Page 58
3
The Utilization Management Industry: Structure and Process
Analyzing the changes brought about by utilization management requires a basic understanding of how utilization management actually works. What decisions do utilization management organizations make and on what basis? To whom are they accountable and for what? How do they try to be effective in controlling costs without harming patients? How standardized are their methods and criteria?
To answer these questions, the committee set out to learn more about the workings of utilization management. What it found about prior review procedures is described in this chapter. Chapter 5 covers high-cost case management. Judgments and recommendations are reserved primarily for Chapter 6.
From the standpoint of the employers or governmental programs that purchase medical care, utilization management can be brought into play in one of three ways. The purchaser can
• engage in utilization management directly, as some Medicaid programs do;
• contract with another organization for utilization management services, as Medicare and many employers do; or
• shift some of the financial risk to another party, such as an insurer, an HMO, or a PPO, which is then faced with the same three choices of doing utilization management directly, contracting for the services, or shifting risk to still another party (for example, physicians or hospitals).
Page 59
The committee did not focus on utilization management activities undertaken directly by employers. Rather, it looked at the broad and varied array of organizations that either contract directly with employers to provide utilization management services or, like some HMOs and insurers, provide utilization management as part of a larger package of services. The products, target markets, philosophies, and technologies of these organizations vary widely, but the industry is evolving so rapidly that summary is difficult. What follows is a snapshot of the field of utilization management.
Industry Overview
In 1980, there was no utilization management industry to speak of, although some of the building blocks existed in HMOs, professional standards review organizations (PSROs), insurance plans, and hospital utilization review programs. Now hundreds of organizations offer utilization management services to thousands of clients who employ perhaps half to two-thirds of all American workers (Foster Higgins, 1987; Gabel et al., 1988). A precise count of utilization management organizations is virtually impossible because the industry is changing constantly, and no single trade association or industry information source exists. A 1987 publication listed 158 private independent utilization review companies (McGraw-Hill, 1987). However, this list did not include the utilization management departments of those commercial insurers and Blue Cross and Blue Shield plans that do not have separate utilization management subsidiaries. Also not included were the internal utilization management departments of HMOs, independent practice associations (IPAs), and PPOs. A 1989 survey by Business Insurance reported 125 review organizations (Business Insurance, 1989). Again, utilization management departments of many insurers were not listed. The companies listed in this second survey covered from 10,000 to over 11 million individuals, and review services accounted for 2 to 100 percent of company revenues. The ten largest firms are listed in Table 3-1.
Figure 3-1 charts the industry's growth, a growth vividly illustrated by the experience of the Mayo Clinic (Mayo Clinic, 1988). In 1984, the Mayo Clinic was dealing with only one utilization management program—precertification for Medicare beneficiaries. Four years later it was working with approximately 1,000 utilization review plans. This does not equate to 1,000 review organizations, however, because many review companies alter some details of their programs to fit particular client preferences. (The Mayo Clinic, for example, reported dealing with over 200 Blue Cross and Blue Shield review programs, but there are fewer than 75 Blue Cross and Blue Shield organizations in existence.) The American Hospital Association (1989) reports that hospitals may deal with from 50 to 250 organizations doing prior and retrospective review.
Page 60
| TABLE 3.1 The 10 Largest General Service Utilization Review Firms | |||||
| No. of Full-Time Staff | |||||
Company (Ownership) | No. of Lives Serviced | Total | Physicians | Registered Nurses | Physicians on Retainer |
| Intracorp (CIGNA Corp.) | 11,500,000 | 600 | NA | NA | NA |
| Corporate Health Strategies (Metropolitan Life Insurance Co.) | 6,200,000 | 243 | 6 | 228 | 7 |
| HealthCare COMPARE Corp. (independent) | 5,000,000 | 433 | 27 | 300 | NA |
| Peer Review Analysis, Inc. (privately held) | 4,000,000 | 45 | 7 | 16 | 65 |
| Corporate Health Care Management (EQUICOR, Inc.) | 3,750,000 | 236 | 9 | 93 | 23 |
| Cost Care, Inc. (independent) | 2,900,000 | 268 | 19 | 136 | 6 |
| Value Health, Inc. (privately held) | 2,800,000 | 119 | 5 | 9 | 7 |
| The Sunderbrunch Corp. (privately held) | 2,683,000 | 293 | 2 | 89 | 0 |
| Western Medical Review (nonprofit) | 2,000,000 | 40 | 1 | 22 | 50 |
| August International Corp. (privately held) | 1,979,750 | 230 | 3 | 48 | 45 |
| NOTE: NA, not available. | |||||
| SOURCE: Business Insurance (1989). | |||||
Some utilization management organizations are spin-offs and descendants of the PSROs developed for Medicare after 1972. Many PSROs had private clients, as do many of the successor PROs. Over three-quarters of the PROs were listed in a 1987 compilation of private independent utilization review companies (McGraw-Hill, 1987), although only a handful appeared in a 1989 directory compiled by Business Insurance (Business Insurance, 1989).
Insurance companies, which are coping with the loss of business that resulted from employers' decisions to self-insure, offer utilization management services both to control costs for underwritten accounts and to provide new products for both insured and self-insured groups. From 1982 to 1986, the percentage of Blue Cross plans reporting prior review programs
Page 61
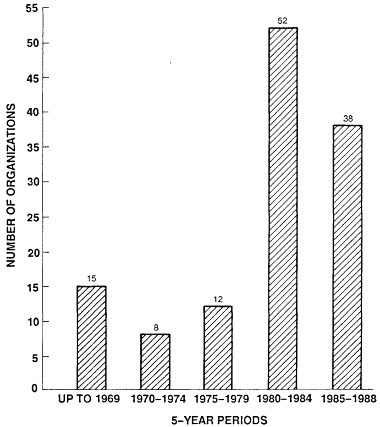
Figure 3-1
Founding years for utilization management organizations. All organizations
founded before 1970 were founded to perform other functions such as insur-
ance or claims administration. Some organizations founded later are subsid-
iaries of older insurance companies or other organizations. Regardless of fou-
nding data, most initiated utilization management services after 1982.Source:
Business Insurance (1988).
jumped from 28 to 95 percent (Scheffler et al., 1988). Third-party administrators, which began by specializing in processing claims for self-insured employers, have also diversified into prior review. In addition, a few community coalitions are administering utilization management programs for employers.
The strategies, lines of business, market niches, and sophistication of organizations in the utilization management field are quite varied. Some organizations specialize in a particular service, such as high-cost case management or review of mental health services, whereas others offer
Page 62
a broad range of services, including underwriting, claims administration, and provider contracting. Certain organizations concentrate on developing software packages for analyzing claims data and assessing the appropriateness of services but actually administer programs for relatively few clients.
The relative youth of utilization management organizations, their limited track records, and the inexperience of purchasers have created a small offshoot industry: firms that review the reviewers. These firms provide consulting services to employers and other purchasers. They also conduct independent audits of hospital medical records and compare their results with those of different review systems or organizations (Milstein et al., 1987).
The description of utilization management that follows is drawn largely from a series of site visits during the summer of 1988 to 12 organizations engaged in utilization management (see Appendix E for summaries of these visits). The organizations visited were selected for variability, not because they were believed to be exemplary. They included both industry leaders and organizations that are not as well known. Site visit teams were made up of two staff members and one or two members of the committee. The visits generally consumed a full day and focused heavily on the details of the operation of preadmission review and high-cost case management programs. The committee asked the utilization management organizations that it visited for examples of contracts with clients. Appendix F in this report presents a review of the agreements that were submitted.
The organizations visited included three independent utilization management companies, three insurance company subsidiaries, two third-party administrators, two PROs engaged in private review, and two HMOs (one staff model and one IPA). This mixture of organizations conveys something of the variety in the utilization management field but not the extent of cross-fertilization that is built into these organizations. The backgrounds of the organizations and their founders includes HMOs, PSROs, the insurance industry, claims administration, employee benefit management, disability management, and academic research. These differences in origins and backgrounds translate in complex and subtle ways into differences in corporate cultures, data systems, computerization, attitudes toward physicians and institutional providers, expectations about what utilization levels can be achieved, and sensitivity to the employee relations issues that utilization management can create for employers.
Although any simple categorizations inevitably oversimplify the situation, it is helpful to define several basic ways in which the utilization management function can relate to the functions of health care delivery, insurance, and benefit plan administration. The following four categories of utilization management are described below: (1) freestanding service,
Page 63
(2) insurer-based service without provider contracts, (3) insurer- or broker-based service with provider contracts, and (4) provider-based service.
In the first category, utilization management is carried out by an organization that (1) does not have contracts or other formal relationships with providers and (2) is not at risk for the costs of medical care services. The party at risk may be an employer, an insurer, or even an HMO or PPO that contracts with the organization for utilization management services. Even though the review function may be freestanding, the organization itself may be a subsidiary or an affiliate of an insurance company or a subdivision of a third-party administrator rather than a completely independent organization. What distinguishes these programs from those that are integrated into the insurance or claims administration function is that they may be marketed as a freestanding product to purchasers that use other companies for insurance or claims administration or that perform those functions themselves.
The organizations that engage in utilization management as a freestanding service have gained so much attention that they are often thought of as constituting the utilization management industry. And, in fact, except for two HMOs, all of the organizations visited in this study—including the PROs—fit into the freestanding category.
In the category of an insurer-based service without provider contracts, utilization management is done by a party that is at risk for the costs of additional medical services but has no contractual relationship with the hospitals or physicians who are subject to its utilization management efforts. Many insurers, acting in their insurance capacity,1 engage in utilization management as a way of controlling claims costs, with the administrative expense for the function built into their premiums. Alternatively, they may offer prior review as a separate option to their customers, but they do not market their service on a freestanding basis to clients whom they do not insure.
The third category of utilization management covers organizations that establish and manage explicit networks or panels of providers. These organizations include some HMOs, some PPOs, and some Blue Cross and Blue Shield plans. The specific arrangements vary from highly integrated group practice HMOs to PPOs and other models with weaker ties between the providers and the broker or other entity that organized the network. The entity that organizes and manages the network may act simply as a broker that does not accept economic risk for the cost of services delivered by network providers. Alternatively, the organization may accept risk, typically
1The implied distinction arises bemuse insurance companies and Blue Cross and Blue Shield plans may either act as an insurer (accepting actuarial risk) or as an entity that provides only administrative services for self-insuring clients.
Page 64
sharing it with the providers in the network. Generally, the provider agrees to initiate the prior review process and to not bill the patient for any claim denied for lack of medical necessity.
When an organization has the kinds of contractual relationships with physicians described above, it has at least three types of potential influence over physicians. The first lies in its control of continuing access to the network's patients, which can be effective with doctors who need the patients furnished by the network more than the network needs access to the services provided by that doctor. Second, because the organization generally has the provider's agreement not to bill patients when claims are denied for lack of medical necessity, the threat of a payment denial can be significant. The organization does not have to face unhappy patients whose bills are not being covered or unhappy clients whose employees are complaining about denied claims. Third, the organization can establish economizing or risk-sharing incentives, for example, capitation or bonuses, as part of its compensation arrangements. (The commissioned paper by Joan B. Trauner and Sybil Tilson in Appendix B describes utilization management in HMOSs in more details.)
Provider-based utilization management, the fourth category, is undertaken out of self-interest by hospitals or other health care organizations that have formal relationships with physicians, for example, employment or admitting privileges. One incentive for health care organizations to undertake utilization management is to reduce the potential for retrospective denial of payment for services judged medically unnecessary. In addition, hospitals paid on a prospective per-case basis have an incentive to minimize costs once a patient is admitted. Institutions may also undertake utilization management as an alternative to having the function performed by an external organization, as may happen with some HMOs or PPOs.
For provider-based utilization management, effectiveness may rest less on the threat of payment denial than on administrative pressure, a perceived mutuality of interest, and the risk that the institution might sever its relationship with the physician, for example, by not renewing an employment contract or by withdrawing admitting privileges. Although several payers (most importantly, Medicare) provide institutions with economic incentives to minimize unnecessary days of care, little documentation is available on the extent to which health care institutions actually use the methods of utilization management (Burda, 1989; Project HOPE, 1987).
The committee notes that those who consider the full research and policy questions raised by utilization management must recognize the existence of provider-based utilization management. The committee, however, has not focused on the utilization management activities of institutional providers of health care for several reasons. Most hospitals have been responsible for utilization review and discharge planning for many years, so hospital-based prior review is a less dramatic change from past prac-
Page 65
tices than are programs undertaken by external organizations. Institutional providers also face comparatively small changes in their legal responsibilities for patient care, which exists independently of any prior review programs.
In theory, the differences among the various organizational contexts of utilization management described above could have important implications for an organization's efficiency and effectiveness, its sensitivity to the complexities and costs created for patients and physicians, its ability to assess the impact of its activities, and the extent to which it is exposed to legal risk. Unfortunately, as described in Chapter 4, virtually no research exists on the effects of these organizational differences. As Appendix B points out, this also holds true for many organizational differences among HMOs.
Even though the organizations visited do not represent the full range of organizations that carry out utilization management activities, the committee found many noteworthy variations in the ways that utilization management is designed and implemented. The description that follows covers several areas of variation in prior review processes. The short history and rapid evolution of the industry and the flux in employer-sponsored health benefits make it impossible to predict how long this description will hold.
The Realities of Prior Review: How is it Actually Done?
"We have the same things that everyone else has ... a book, a WATS line, and nurses."2
Despite certain basic similarities implied by this quote and by the definitions offered in Chapter 1, each utilization management organization's programs are a mixture of invention, imitation, borrowing, and adaptation by an organization that has its own history, market niche, and strengths and weaknesses. Moreover, the industry is subject to little explicit regulation and has not developed any extensive form of self-regulation during its relatively brief existence. For these reasons, it is not surprising to find variations in how such "standard" methods as preadmission and continued-stay review are carried out by different organizations. Even the PROs that contract with Medicare, which are subject to very detailed oversight and performance specifications from the federal government, vary a great deal in their organization and activities (General Accounting Office, 1988).
2Robert E. Becker, M.D., founder of HealthCare COMPARE Corp., at the June 6, 1988, hearing of the Committee on Utilization Management by Third Parties. Dr. Becker followed this characterization with his views on why his company is, in fact, different.
Page 66
Likewise, the means used by HMOs to influence patient care decisions vary widely, as described in Appendix B of this report.
To date, little or no documentation exists regarding the nature, extent, or consequences of such variations. This report attempts to correct some of that descriptive void, but the committee's charter did not and could not include empirical research on the impact of organizational differences.
Certain elements appear to be common to all or most programs in which prior authorization or certification must be obtained from an external organization regarding the necessity or appropriateness (different programs use different terms) of hospitalization or other services. First, all programs offer some or all of the prior review and high-cost case management activities described in Chapter 1.
Second, all rely on telephone rather than face-to-face contact with the patient or physician. The major exception is that some programs for continued-stay review programs use review nurses who are employed by the utilization management organization but who work on-site in the health care facilities that are subject to review. This arrangement was typical of PSROs and continues to be common in PROs. It is also used by HMOs, particularly those that have contractual relationships with a limited number of hospitals. In addition, for admissions planned weeks in advance, written forms may be used, with the telephone used for follow-up as needed.
Third, programs use a two-stage assessment process. In the first stage, the review organization obtains information about the patient and the proposed services; services that pass the screening criteria are certified as necessary or appropriate. This first stage is handled by nurses in most programs, although experienced medical secretaries perform this function in one program that the committee visited. Services that do not pass the screening criteria pass to the second stage, which involves physician review. Nurses may authorize services, but only physicians may deny authorization.
Fourth, the current focus of prior review is on the appropriateness of the site of care, the timing of an admission, or the duration of care. A few organizations examine the need for specific procedures, but most currently do not. During preadmission review, the cost of alternative care is not evaluated on a case-by-case basis. (As described in Chapter 5, high-cost case management includes such an assessment.)
The typical steps in the prior review process are described in Figure 3-2. Beyond these elements, organizations vary widely, as described below.
How Prior Review Is Integrated with Other Administrative Functions
Because utilization management is done by organizations with different purchaser and provider relationships, there are significant differences in the extent to which the prior review function is integrated with other
Page 67
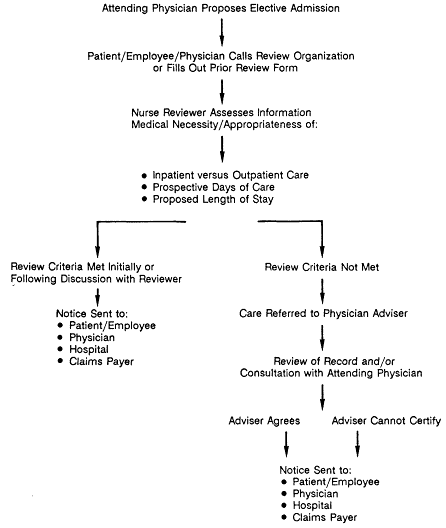
Figure 3-2
Typical basic steps in the prior review process.
Page 68
aspects of benefit plan administration, such as determination of whether a proposed or alternative service falls in a category covered by a patient's benefit plan. Some organizations have no information about benefit plan provisions and thus can make judgments only about the appropriateness of proposed services, not whether a general category of care is covered for a particular patient. Such organizations typically tell the patient or the provider that they must find out from the employer, insurer, or claims administrator whether or not the benefit plan covers the particular services. Even organizations that have information about benefit plan provisions do not always have on-line information about whether a particular patient is still eligible for benefits or has left the employer, been dropped as a dependent, or joined another health plan.
Moreover, some review organizations have no connection with the claims payment function and possess little or no information about the actual use of services. Thus, they can report only on their activities (for example, the numbers of admissions requested and authorized), not on services actually used or paid for. They also cannot readily determine whether adherence to utilization management requirements is being checked during the claims payment process.
At the other extreme are organizations that do both utilization management and claims payment and that have fully integrated data systems. Such integration provides greater certainty that unauthorized services are not paid for inadvertently, a problem that may occur more often when one organization does utilization management and another pays claims. It also makes possible the generation of reports based on actual claims experience. Ready access to particular patients' claims histories, which some organizations possess, may permit more sophisticated judgments about the appropriateness of proposed treatment.
For example, a third-party administrator that the committee visited had a system in which the patient's claims history appeared automatically on the computer screen when the nurse reviewer began to enter data during a telephone request for prior authorization. The example that was demonstrated involved a child for whom a tonsillectomy was proposed—a procedure that was subject to a ''focused second opinion'' program under the insured's health benefits. The child's claims history showed that a series of office visits for tonsillitis had occurred over the previous year. Since this suggested a recurrent problem that was not responding to less intense treatment, the second-opinion requirement was waived because it was likely to concur. This saved the family some inconvenience and the purchaser the cost of the second opinion.
Systems that integrate utilization management with claims information also facilitate identification of potential cases for high-cost case management, for example, by flagging repeat hospitalizations. Integrated systems
Page 69
also make possible, at least in theory, a kind of outcome measurement, because future services will show up in additional claims. Although none of the organizations that were visited reported doing outcome studies, such assessments are not far beyond the capacity of several of them.
Another form of data integration takes place at some utilization management organizations whose activities are highly concentrated in a particular geographic area. PROs, Medicaid programs, Blue Cross and Blue Shield plans, HMOs, and PPOs operate largely in particular states or metropolitan areas, whereas the larger commercial insurance companies, third-party administrators, and independent review organizations often do business nationally and deal with a much more dispersed group of providers. The geographic concentration of a relatively high volume of business provides an opportunity, if data systems are properly organized, to accumulate considerable experience with particular hospitals and physicians and to better target review activities on problem services or providers.
None of the review organizations visited in this study confined their prior review or case management programs to providers who had been identified as problems. However, focusing on problem providers has been an important feature of the retrospective review activities of the PSRO, PRO, and carrier programs conducted for Medicare. One PRO visited by the committee reported that they had tried unsuccessfully to interest their private customers in a focused precertification program.
How Basic Logistical Matters Are Handled
For utilization management organizations, like most service companies, the ways in which basic operations are handled can have a major effect on relations with clients and suppliers. Purchasers often insist on visiting a review organization in an effort to assess how well the program is run, and many ask for periodic reports on service levels, for example, the percentage of telephone calls answered within five rings. Although the impact of logistical differences on benefit costs cannot now be documented empirically, the committee found a number of plan characteristics that are widely regarded as important.
Initiating Review
For organizations that do not have contracts with providers (and for some that do), the enrollee is usually responsible for initiating the review process. Otherwise, the enrollee may incur a financial penalty. One of the biggest challenges for purchasers and suppliers of utilization management services is to educate employees about this responsibility. Mere discussion in a benefits handbook is generally regarded as insufficient, and an array of additional information efforts are often attempted. These include
Page 70
highlighted notices on benefit plan identification cards, discussions during new employee orientation, and information letters that must be returned to the personnel office with a signed acknowledgment of receipt from the employee.3
As a practical matter, physician and hospital offices often make the initial calls to the utilization management organization since they generally end up discussing the case with the reviewer anyway and also want to reduce the risk of a denied claim or bad debt. For many years most hospitals have had standard routines to check a patient's insurance coverage before admission, and contact with review organizations can be incorporated into this process. Some utilization management firms say that they try to obtain all the information they need from the patient or the patient's family, but many make it a practice to talk to the physician's office to confirm the information, obtain additional information, and describe directly their review policies or guidelines.
Handling Telephone Calls
In some utilization management organizations, the calls from patients or providers are answered centrally and passed along to the first available review nurse. In other organizations, review nurses answer calls directly. Before the actual admission takes place, as many as three or four telephone conversations may take place, since review organizations may be notified of a pending admission by more than one party and may have to talk to the physician's office more than once, particularly if the proposed services do not pass the organization's screens for certification.
How quickly the caller gets through to the correct party will depend upon the organization's staffing levels, phone system, and other factors. Some firms with clients nationwide provide a single toll-free 800 number, but calls are automatically routed to different regional offices, depending on where the calls originate. Many but not all review organizations have computerized telephone systems that allow supervisors to monitor telephone waiting time and track how often callers encounter busy signals or hang up because the phone was not answered after several rings. Attention to these matters varies enormously from organization to organization. For example, some organizations lack the equipment for systematic telephone
3For example, the identification card for the indemnity health plan offered by the National Academy of Sciences includes one warning of special plan review requirements on the front of the card (in red capital letters) and two warnings (in boldface capital letters) at the top and the bottom of the card's reverse side. The reverse side also includes brief summaries of the plan requirements and relevant phone numbers.
Page 71
monitoring, whereas others not only have the equipment but also have specific performance standards and incentives. In general, sophisticated phone systems are a high priority for major utilization management organizations.
Computerization
The degree of computerization also varies greatly across utilization management organizations. At one extreme there are organizations that use computers off-line only for recordkeeping purposes. Some organizations have gone to this approach after finding that their software was too slow to be efficient for data entry while the patient or provider was on the telephone. Since flexible and fast software can be very expensive to develop or license, some organizations have been slow to upgrade their systems. At the other extreme are organizations that use networked computers into which are built (1) questions for patients or providers, (2) decision protocols and criteria to assess the information and determine whether to certify care or refer it for further review, (3) details of client benefit plan limitations, (4) individual claims histories, (5) automatic diagnosis and procedure coding, (6) diagnosis or procedure-specific length-of-stay norms, and (7) addresses for practitioners and institutional providers. These systems may also allow the automatic preparation of letters to patients, physicians, and hospitals to confirm the results of the review. These aspects of computerization affect not only the comparative efficiencies of different utilization management programs but also the kinds of analyses and reports that can be generated.
Because multiple calls involving multiple parties may take place, logistics can be important for the patient or provider. In a highly computerized organization, any nurse reviewer or physician adviser can take up a case exactly where it was left on a previous call. Organizations that use pencil and paper or inflexible telephone and computer systems may require the person who took the initial call to take follow-up calls. Since nurse reviewers and physician advisers spend much of their time on the telephone, this means that the hospitals, doctors, or patients who deal with the latter type of organization may have to make many calls before they reach the right individual. Because this can be time-consuming, physicians often turn the function over to employees. Thus, the prior review process often becomes a discussion between a nurse reviewer at the utilization management organization and a secretary or nurse in the physician's office.
How Nurse Reviewers Work
Nurses play an integral role in most prior authorization programs. This role usually includes obtaining all requisite information about the patient and proposed treatment, entering the information into the computer,
Page 72
assigning diagnosis and procedure codes, reviewing the proposed treatment against the organization's criteria of appropriateness, and conveying approval for treatment that conforms to those criteria. Two organizations departed from this pattern. One uses experienced medical secretaries in this role. The other gives staff physicians—assisted by computerized screening criteria—the responsibility for reviewing treatment against approval criteria and conveying approval.
Several organizations report that nurse reviewers handle 40-50 calls per day, doing anywhere from 10 to 20 certifications (certification may require several calls to complete). In most organizations, nurse reviewers do other functions, such as high-cost case management and answering inquiries from beneficiaries. Some organizations assign those functions to a separate group or groups, and others rotate nurses through different functions.
Even in the organizations that use nurses for apparently similar functions, the nature of their authority varies substantially. No organization visited gives nurses the authority to refuse prior certification of care proposed by attending physicians, but most give nurses the authority to try to negotiate conformity with review criteria. However, two organizations instruct nurses not to negotiate with attending physicians or their employees; anything that does not fit the organization's criteria of appropriateness must be referred to a physician consultant. Even in these organizations, the nurse reviewer's questions may prompt the physician to modify a proposed plan of care.
Organizations also vary in whether they direct nurse reviewers not to coach attending physicians on how to gain approval of proposed care. In one organization that the committee visited, the attitude is that attending physicians do not always know the right language to be used to gain approval of an appropriate admission. If nurse reviewers' believe that a patient probably needs to be admitted, they can give the attending physician's office the cues needed to gain approval. Other organizations explicitly instruct nurse reviewers not to do this.
Another area in which nurse reviewers' authority varies from organization to organization is whether they are permitted to make exceptions to review criteria on the basis of their clinical judgment. At least two organizations visited permit review nurses to certify an admission that does not meet review criteria if, in their judgment, it is nevertheless appropriate. Many utilization management organizations do not permit this and require referral of all such cases for review by physicians.
Most organizations prefer to hire nurse reviewers who are registered nurses with at least 5 years of experience; however, one required only one year of experience. Most organizations also prefer reviewers with hospital experience. One mentioned experience in utilization review in hospitals
Page 73
as being important; another prefered nurse reviewers to have emergency room or intensive care unit experience.
The training of new nurse reviewers can be quite variable. Some are trained in one-to-one sessions with a supervisor; others go through formal training periods that last anywhere from 2 to 6 weeks. Most organizations report that after some initial loss of nurses who simply do not like the work, there is very little turnover. Recently, one national association implemented a training and monitoring program to instruct nurse reviewers how to analyze and listen to patient or provider requests and calls, explain insurance plan requirements, pose questions effectively, and manage difficult calls ("New Blues Program to Train Nurse Reviewers," 1989).
How nurse reviewers are monitored also varies. Supervisors in most organizations are responsible for anywhere from 6 to 12 nurse reviewers, but in a few organizations supervision is much less close. One PRO that was visited had 76 nurses and one supervisor. Monitoring ranges from informal oversight done by walking around and overhearing the nurse's end of conversations to very rigorous and systematic monitoring. Several organizations monitor telephone activity by using a computer (which can compute such things as the average length per call and number of calls per day) and by silently listening in on a sample of calls. Several organizations also systematically review a sample of cases handled by nurse reviewers by looking at the appropriateness and consistency of decisions made and the accuracy of coding. In a few organizations, the physicians who receive cases on referral from nurse reviewers play a role in monitoring their performance.
Several of the organizations visited provide incentives for accuracy and productivity. When asked, none reported attaching any rewards to such measures as days or dollars saved or utilization levels achieved.
What Role Do Physician Advisers Play?
All utilization management organizations that were visited refer cases that fail screens to physician advisers. These physician advisers are expected to use their clinical judgment and experience to determine whether the services should be certified as medically appropriate. One organization that was visited noted that under its state's law, this function could be construed to be the practice of medicine and thus must be carried out by a physician who is licensed to practice in the state. All organizations visited said that their physician advisers are not bound by the organization's criteria or rules about what services are appropriate. This is quite consistent with the logic of the entire process—otherwise, decisions not to certify services could be made by computers. Thus, the physician adviser's role is crucial.
Page 74
However, responsibilities and work arrangements vary in some important ways across organizations.
One important source of variation involves the nature and sources of the information on which the physician advisers base their decisions. In most of the organizations visited, the physician advisers call the attending physician to discuss cases that the nurse reviewers cannot certify. Companies say that physician advisers have excellent success in establishing direct contact with attending physicians. One reason for this is that, in at least some companies, the physician adviser calls the patient's physician's office directly, announces himself as Dr. X without disclosing the purpose of the call, and asks to speak with the attending physician. (The committee's site visitors were unable to ascertain physicians' reactions to receiving a call from another physician and finding out when they come on the line that the calling physician was from a review company.) Companies also say that by approaching attending physicians as colleagues, physician advisers, are often able to obtain important additional information that was not provided to the nurse reviewer, and they can work out a satisfactory agreement with the attending physicians about the services that will be certified as appropriate.
Some utilization management organizations, however, use their physician advisers in quite a different way. In a pattern that may be particularly characteristic of PROs, some physician advisers have no contact with attending physicians. Ordinarily, they make their decisions based only on the information obtained by the nurse reviewers and then convey their results to these nurse reviewers, who carry on from there.
The relationship between physician advisers and utilization management organizations varies. Four arrangements were seen during the site visits:
• The medical director and physician advisers are full-time employees of the utilization management organization.
• The medical director and physician advisers are part-time employees and part-time practitioners.
• The medical director is employed by the utilization management organization, and physician advisers are outside consultants.
• The medical director and physician advisers are outside consultants.
In the first arrangement, the medical director and physician advisers are full-time employees who work from the utilization management organization's offices. This requires a certain volume of business to be practical, but it provides advantages in standardizing operations such as recordkeeping, monitoring performance, and developing a corporate culture. A potential danger is that the corporate culture will include a significant degree of cynicism about the abilities and motivations of practicing physicians. Also,
Page 75
this type of arrangement is inconsistent with a strongly held, though nonvalidated, belief of practicing physicians (and some people in the utilization management business) that physicians who leave practice to work as reviewers lose touch with important realities of medical practice. The opposing argument, also unverified, is that physicians who work for a large review firm deal with thousands of clinical situations each year and therefore not only keep current but have a broader and deeper understanding of what goes on in medical practice (such as variations among practitioners).
The second arrangement, the use of reviewers who are part-time employees and part-time practitioners, appears to combine the advantages of the first arrangement while avoiding the criticism about the loss of touch with the realities of medical practice. Of course, the use of part-time physician advisers is a less stable situation, since their practices may grow or they may assume full-time responsibilities elsewhere. However, with the growing physician supply nationally, review organizations in many areas of the country are able to find practitioners who can commit a certain number of hours per week to review. By law, physician advisers for PROs must be in active practice.
The third arrangement involves the use of an in-house medical director who is responsible for the organization's medical decision-making and consults, as needed, with a panel of practicing physicians in particular specialties, most of whom work from their own offices. The medical director may seek advice from these advisers or may refer to them an occasional case that they need to deal with fully, including discussion with the attending physician. Because most decisions and most feedback from practicing physicians pass through a single individual, this arrangement may provide for a comparatively high degree of consistency in the organization's decisions. However, the arrangement also has dangers if the medical director's judgment is idiosyncratic and not balanced by other on-site physicians.
The final arrangement, which was observed in several organizations and may be the most common of all, particularly in small organizations, involves the use of physician advisers (and even medical directors) who do their work for the utilization management firm from their own offices. Although this is probably the least expensive way to organize the function, it has several potential weaknesses. It can be difficult to monitor reviewers' performance, maintain consistency, and develop a corporate culture. Some organizations say that it can be difficult to reach a physician adviser who has a busy practice, to get him or her to attend to cases in a timely fashion, and to produce the necessary documentation. Some organizations have found that physicians who agree to be on their panel are reluctant to call the attending physicians or to raise the necessary questions with them. This reluctance may be a source of the delays in the review process complained of by some attending physicians.
Page 76
Variations among utilization management organizations in the use of local versus nonlocal medical advisers also have important implications. Again, several arrangements exist. First, there are organizations that operate in a relatively confined geographic area, like PROs, and that use local physicians as reviewers. These reviewers may be more reluctant to challenge their peers because of social or professional contacts.
A second variation is for an organization to do prior review on a national basis but draw physician advisers from the areas where the firm's offices are located. (An unusual version of this model involves a large insurance company that uses its own nurse reviewers but contracts with organizations located elsewhere for the services of physician advisers.) During the site visits, such organizations did not complain of having difficulty in getting their physician advisers to make the necessary phone calls. On the other hand, this arrangement can lead to problems when practice standards that are commonplace where the reviewers are located differ from the standards where the attending physician is located. For instance, several organizations reported substantial regional differences in whether surgeons will admit patients on the morning of rather than the day before surgery or whether they will perform tonsillectomies on an outpatient basis.
Probably the least common situation is for a company to do business over a large geographic area with little or no use of local physician advisers. In part, this approach may reflect the logistical difficulties that a review organization can face in developing and monitoring physician advisers scattered around a larger region. In one state that the committee visited, an entrepreneurial group of physicians put together a statewide network of physicians who were wining to do reviews on a contract basis. It can ensure that the physician reviewer who is assigned to a case is from a different part of the state than the attending physician.
There are also major differences among utilization management organizations in how much physicians are involved in prior review. On the low side, the proportion of cases that go to physician advisers for review runs about 1 or 2 percent in two organizations visited and about 10 to 15 percent in five organizations visited. In contrast, 40 percent of cases go to physician advisers in one of the oldest and best established firms, and another firm advertises 100 percent physician review.
Given these differences, it is not surprising that caseloads for physician advisers vary enormously from organization to organization. The physician advisers who work on-site at one organization handle about 10 cases per full-time reviewer per day, whereas those at another organization do 200-250 certifications per day. Note that for a hypothetical 6-hour "review day" the latter rate appears to allow a physician, on average, less than 2 minutes per review. This suggests that many cases may be just scanned and signed in such organizations.
Page 77
Except for the organizations in which the physicians' determinations are based purely upon a written or computerized record, all organizations report that the process of physician review is collegial. Rarely do the attending physician and the reviewing physician fail to reach agreement about a case. Most organizations report that denials of certification are issued in fewer than 1 or 2 percent of all cases, but a much larger proportion of cases involve some modification of proposed services at some stage in the review process. By way of comparison, based on both prospective and retrospective review, PROs deny payment for about 2 percent of all Medicare admissions (PPRC, 1989).
In hiring physician advisers, most organizations that the committee visited state that the main credentials they seek are board certification and experience in practice. Some organizations mention additional factors, such as professional reputation or experience in utilization review. Investigations of qualifications do not appear to be extensive. One organization recruits some reviewers from among the physicians with whom they have contact as subjects of review.
The training of physician advisers is minimal—from 1 day to several days—and performance monitoring varies greatly. In some organizations, up to 10 percent of each reviewer's cases are reviewed either by the medical director or a quality assurance committee. Alternatively, a sample of cases may be exchanged among reviewers for mutual review. One organization uses an outside panel to review a sample of its reviewers' decisions. In contrast, some organizations do not engage in such systematic oversight. They may only review cases in which an attending physician appeals the physician adviser's decision. One organization states that its main review of its physician advisers' performance was by the nurse reviewers to whom the decisions are conveyed.
Physician advisers are paid in several different ways, reflecting the diversity of their arrangements with the review organizations. The basis of payment seen in the site visits included payment per call made, per case, per hour, per month, and by an annual salary. Although explicit or implicit productivity incentives are common, none of the organizations that were visited indicated that they tie payments to physician advisers to such measures as denial rates or the amount of money that they save the purchaser. Virtually all of the organizations visited report little turnover among their physician advisers.
To summarize, the utilization management physicians in whose hands rest decisions about the necessity or appropriateness of services
• may be full-time or part-time employees of either the utilization management organization or a subcontractor;
• may or may not have an active medical practice;
Page 78
• may work from their own offices or from the review organization's office;
• may review only local cases, only cases from other regions of the country, or both;
• may deal directly with attending physicians or may rely completely upon information assembled by nurse reviewers; and
• may review as few as 10 or as many as 200 cases per day.
These differences may well affect such matters as the reviewers' toughness in trying to eliminate inappropriate services, their sympathy with the position of the attending physician, the efficiency of the program, and the consistency of the organization's decisions.
What Style Is Used with Attending Physicians?
Utilization management organizations generally state a preference for negotiating agreement rather than attempting to impose decisions on attending physicians. This preference stems, in part, from reluctance among review organizations to risk legal liability for patient care decisions, but it also may reflect client wishes. In addition, employers who purchase utilization management services vary in their desire to maximize the economizing effects of these activities and in their willingness to risk employee relations problems by backing up negative review decisions. Numerous factors may contribute to these variations, including corporate culture, the composition of the labor force, and competitive pressures. Companies that have an expanding market and a highly educated labor force may put quite different demands on a review organization than may a company whose profits are threatened by health care costs and whose labor force is poorly educated and decentralized.
One organization, most of whose clients had unionized labor forces, particularly stresses its practice of trying hard to convince attending physicians to accept its determinations of appropriateness or agree to a negotiated alternative. They say they want to avoid putting patients in the middle between the provider and the payer. Several organizations stated that some clients want to be contacted before denial letters are issued, presumably so they can make case-by-case decisions about whether to risk employee relations problems.
However, other organizations take pride in backing their reviewers' determinations and believe that their clients expect them to refuse payment authorization for inappropriate services. The impact of such a policy has not been empirically compared with more lenient policies.
Page 79
What Criteria Are Used to Assess Care?
The results of prior review of medical services by utilization management organizations are shaped by criteria—an imprecise term employed here to refer to the written policies, decision rules, or guides used to evaluate what services are appropriate or necessary for patients in different clinical circumstances (Donabedian, 1981). Organizations refer to several different types of criteria, although the boundaries between categories are not necessarily well-defined.
Lists of Procedures
Most utilization management organizations have lists of procedures that are used to target services for assessment. The most common lists involve (1) surgical or diagnostic. procedures for which payment is ordinarily authorized only if the procedure is done on an outpatient basis without an overnight stay in the hospital and (2) surgical procedures or other services for which a second opinion may be required. These lists may be included in the benefit plan information provided to patients to alert them to the general policies of the utilization management program. The utilization management organization then uses the lists in evaluating proposed inpatient services, a step that relieves the patient of keeping track of a long procedure list. (Depending on whether the benefit plan includes preprocedure review, the patient may still need to be aware of outpatient procedures for which second opinions are required.) To consider whether an admission might be warranted for a target procedure, the reviewer relics on exceptions criteria.
Exceptions Criteria
Exceptions criteria specify the circumstances under which certain utilization management policies or requirements might be waived. For procedures that are ordinarily certified only as outpatient procedures, exceptions might include patients with a history of bleeding disorders or heart disease. Also common are defined exceptions to the general rule against authorizing a patient's admission to the hospital prior to the day of surgery. Both of these types of exceptions criteria tend to be generic, and they are applied without reference to the particular diagnosis or procedure for which an admission is proposed.
Hospitalization Criteria
Utilization management organizations use a variety of criteria to determine whether an individual needs inpatient care. Most are based on criteria that were originally developed for retrospective review in the PSRO
Page 80
program or for research on unnecessary use of the hospital (Payne, 1987). These criteria have been refined and are marketed in hard copy or computer disk versions by a handful of major vendors for use in both prospective and retrospective reviews.
Most of the review organizations the committee visited base their hospitalization criteria either on the appropriateness evaluation protocol (AEP) or on the ISD-A criteria set (intensity of services, severity of illness, discharge, and appropriateness screens). These tools, which were originally developed for retrospective research on the extent of inappropriate hospital use, have been adapted for prospective use to discourage inappropriate hospitalization (Restuccia, 1986). A 1987 study of PROs indicated that the AEP and ISD-A criteria are also widely used by PROs (Project HOPE, 1987).
The AEP criteria for adult medical/surgical services and for pediatric and elective surgery, which were initially prepared with federal financial support in the late 1970s, are in the public domain and have been the subject of several studies that have indicated that they are reliable and valid (Gertman and Restuccia, 1981; Strumwasser et al., 1987). More recent work on the AEP has been proprietary, although it is readily available and relatively inexpensive. The ISD-A criteria are proprietary (InterQual, Inc., 1987), and no specific reports on their reliability appear to have been published.
The AEP, which has been revised and expanded since it was developed in the mid-1970s, is comprised of lists of symptoms (such as sudden acute loss of vision) or services (such as the need for vital signs monitoring every 2 hours or more often). The lists are specific to major clinical services (for example, surgery and pediatrics) and are designed so that any one symptom or service suffices to justify a day in the hospital. Table 3-2 includes an excerpt from a recent training manual describing criteria for determining when inpatient surgery is warranted based on respiratory status. The ISD-A criteria operate by a logic similar to that of the AEP but are specific to different body systems.
Most organizations purport to use a modified version of whichever criteria set they have adopted. The committee cannot judge whether these modifications are designed to make the criteria tougher, more appropriate locally, or easier for reviewers to use.
To explore variations in two specific areas, site visitors inquired about the circumstances that would warrant certification of admission to the hospital for combined tonsillectomy and adenoidectomy and for nonsurgical back pain. Some organizations consider their criteria and guidelines to be proprietary, but all responded to these specific questions. As summarized in Table 3-3, the responses varied considerably in content and specificity. It should be noted, however, that tonsillectomy and adenoidectomy and lower
Page 81
| TABLE 3-2 Excerpt from the Surgery Appropriateness Evaluation Protocol Reviewer's Manual | |||||
| V. CRITERIA OF ADMISSION—LOCATION OF SURGERY/RISK FACTOR ASSESSMENT | |||||
| This section includes those factors felt to identify patients and procedures requiring that surgery be performed on an inpatient basis rather than on an ambulatory or day of surgery admission basis. These criteria for determining location fall into three categories: (1) comorbidity (the presence of concurrent medical problems which place the patient at special risk, no matter what kind of surgery is to be done), (2) potential for complications post-operatively, and (3) the need for intensive post-operative care. If any one of these criteria is met, inpatient admission for the surgical procedure is deemed appropriate. Conversely, if none of the criteria are satisfied, inpatient admission is not justified. The reviewer, however, does have the option to override the criteria in either direction (see pages 9-10). | |||||
| Comorbidity | |||||
| The diagnoses or measurements in this section must be documented as being present and the data (whether test results or clinical observations) should be from within the past four months prior to admission. Do not use ''suspected'' diagnoses. | |||||
| A. Respiratory Status | |||||
| 1. Significantly abnormal pulmonary function measurements | |||||
| Independent of what particular respiratory disease is present any one of the following four measures of pulmonary function will suffice: | |||||
| a. Functional Vital Capacity (FVC) of < 1.0 liters | |||||
| b. Forced Expiratory Volume in the First Second (FEV1) of < 50% × FVC | |||||
| c. Arterial pCO2 > mmHg | |||||
| d. Arterial pO2 < 50 mmHg | |||||
| 2. Sleep apnea. | |||||
| Documented as present regardless of how severe or frequent | |||||
| SOURCE: Reprinted with permission from Restuccia (1986). Copyright© 1986 by Restuccia. | |||||
back pain were picked deliberately because the committee knew they were particularly likely to show variation.
Length-Of-Stay Norms
To assess proposed hospital lengths of stays, most utilization management organizations use statistical norms based either on data published by the Commission on Professional and Hospital Activities (CPHA) or on data compiled by the review organization itself. These statistics are generally disaggregated by geographic region and diagnosis. Most of the organizations visited base their continued-stay review on the CPHA's average length of stay for the CPHA Western region, where lengths of stay are shortest. Many review organizations do continued-stay review either on the
Page 82
| TABLE 3-3 Circumstances Warranting Hospital Admission as Identified by Various Organizations Visited by the Committee | |
| Site | Tonsillectomy and Adenoidectomy |
| 1 | Distance from home to facility; complications |
| 2 | Physician insistence on admission |
| 3 | Complications |
| 4 | Age; comorbidities |
| 5 | Physician insistence; high risk; 2 hours or more of travel time |
| 6 | Bleeding disorders; distance |
| 7 | Physician request for admission |
| 8 | Patient's history |
| 9 | None specified |
| 10 | One-night stay permitted |
| 11 | Physician request for admission |
| 12 | No special conditions required |
| Site | Lower Back Pain |
| 1 | Patient requires intramuscular injections for pain control; inability to move |
| 2 | Need for intramuscular injections for pain control; motor defects |
| 3 | Pain; complications |
| 4 | Severe pain; need for traction |
| 5 | Three days of traction allowed for pain |
| 6 | ISD-A criteria |
| 7 | Failure of outpatient treatment |
| 8 | Neurological deficit |
| 9 | If physician requests, having tried outpatient treatment first |
| 10 | Physician insistence on admission |
| 11 | Physician request for admission |
| 12 | Rare, only for intensity of service |
day by which 50 percent of patients with a given diagnosis are discharged in the Western CPHA region or on the day before that. However, one HMO visited initiates continued-stay review on the day when, on average, the first 10 percent of patients are or have been discharged. Most of the organizations visited do not use the length-of-stay norms to certify a specific length of stay as appropriate but, instead, use them as guides for scheduling continued-stay reviews. They then assess whether a patient is ready for discharge based on AEP, ISD-A, or similar criteria. Some organizations do not employ statistical norms for scheduling continued-stay review but rather check back on a regular basis, for example, every third day after admission.
Thus, although some organizations still tell providers and patients how many days of stay they can certify at the outset, others simply state when they will check back to see how the patient is doing. Two reasons have been cited for this practice. First, when a particular length of stay is certified, physicians and patients may interpret it as a fixed limit, not a guide. Patients who do not understand the process may get anxious when they know that 3
Page 83
days of stay have been authorized and then their physician tells them on the third day that they are not ready for discharge. Second, some physicians may regard a statistical norm as a minimum length of stay or may focus on the length-of-stay numbers rather than on the justification for continued hospitalization.
Necessity of a Procedure
The least commonly used criteria at this time are those designed to assess whether a specific procedure (usually surgical, but sometimes diagnostic) is appropriate for a particular patient. Although considerable research evidence has accumulated to suggest that certain procedures— insertion of pacemakers, carotid endarterectomies, and others—are used much more commonly than is medically justifiable, utilization management organizations have moved cautiously to require prior review of procedures based on medical necessity grounds. PROs are now required to review the need for care on a prospective basis for several procedures (see Appendix c). Fear of legal liability undoubtedly contributes to the reluctance of other organizations to accept the responsibility that such determinations would entail. Nevertheless, a growing number of programs are expanding or planning to expand in that direction.
The most commonly mentioned criteria for this kind of review involve the medical review system developed by former Rand Corporation researchers (Value Health Sciences, Inc., 1989). In this system, the review protocols for procedures like tympanotomy tube insertion or knee arthroscopy involve a series of questions on such matters as the chronicity of the patient's problem, prior treatment by drugs or specified nonsurgical options, and physical findings. The answers are evaluated through scaling and other techniques to determine whether the proposed care is indicated (Value Health Sciences, Inc., 1989).
At present, it appears that most organizations that make medical necessity judgments combine prior review with provisions for a nonbinding second-opinion in cases in which the clinical indications for a procedure are dubious. In certain cases in which clinical indications for a specific procedure are nonexistent (based on information provided to the reviewer), some review organizations say they now refuse to certify the necessity of the services.
How Criteria Are Adopted and Modified
Many approaches are used to adopt or modify criteria, but virtually all involve the organization's medical director and physician advisers (or a committee thereof), who are supplemented in some cases by an external advisory group. Some organizations describe a fairly formal and extensive
Page 84
internal process for developing criteria that includes using systematic review of the clinical literature on a topic and consensus panels. However, criteria are often borrowed, licensed, or adapted from outside sources or are developed less formally through discussions among physician advisers.
Utilization management organizations generally report that their criteria are in a continuous process of modification, although some also schedule periodic reviews for particular sets of criteria. The process of modification can be rather informal in smaller organizations. In large organizations in which many different nurses and physicians use the criteria, the process is necessarily more formal.
The decision to revise a criterion may be prompted in several ways. Members of the medical staff may raise an issue because of differences among themselves over how certain situations are being handled, because they are encountering a great deal of resistance from attending physicians, or because new information has come to light in medical literature or conferences. In addition, pressure from customers to reduce medical care utilization may prompt a new examination of criteria to search for areas in which additional savings are possible.
Several organizations mentioned that they revise criteria based on their own utilization data. They may find, for example, that although they are still authorizing hospitalization for a particular procedure, the majority of the patients covered by their program undergo the procedure on an outpatient basis. Length-of-stay criteria may be revised when data show that many patients are being discharged before the scheduled concurrent review. Examples like these suggest that utilization management organizations tend not to be the pioneers in the move to more parsimonious forms of care but are, instead, consolidators of movement in that direction.
How Organizations Use Criteria
Utilization management organizations most commonly use written or explicit criteria to differentiate patient conditions that warrant certification in a first level of review (usually by a nurse reviewer) from those that require more detailed review, usually by a physician based on implicit professional standards. The written criteria are, as a result, often described as screens, although that term is sometimes reserved for computerized edits of claims that flag certain types of claims for more detailed examination by nurse reviewers.
The main users of criteria are the nurse reviewers who are empowered by most (but not all) programs to certify services that conform to the criteria or to negotiate changes in proposed services so that they conform to the criteria. Criteria for outpatient surgery, presurgical days, or appropriate hospital days may be applied more or less strictly, depending on
Page 85
the utilization management organization's philosophy and the purchaser's requirements. In most instances, physician advisers make little direct use of such formal screening criteria. They are expected to make decisions based upon their own clinical judgment. However, physician advisers are expected to be familiar with the formal criteria and not contradict them without sound clinical justification. It does not ordinarily suffice for a physician adviser to certify services on the grounds that he or she does not agree with the criteria.
In some cases, medical directors and physician advisers cannot agree on how particular circumstances should be handled, and it is left to the discretion of the physician adviser who receives the case.4 In some organizations, the nurse reviewers have the power to select the physician adviser to whom a case will be referred. With the passage of time, the nurses can learn a great deal about different physician advisers' tendencies and can make referrals based on their own assessment of whet decision should be made and their knowledge of which physician adviser is most likely to make that decision.
Appeals Processes
The appeals process used by organizations that engage in utilization management are quite diverse, although it appears that all organizations have some mechanism for appeals. Among the organizations visited, variations in these mechanisms appear particularly significant along two dimensions. One dimension is the elaborateness of the process. The other is whether parties external to the organization are involved.
PROs have a very formal and extensive appeals process. (For a brief overview of some general differences between the PRO program and private programs, see Appendix c.) This is a function of the requirements that PROs accept as part of their contracts with the federal government to review care for Medicare beneficiaries.
In most of the organizations the committee visited, an appeal involves a review of the case by a new physician adviser, the medical director, or a
4A particularly interesting situation was described in one review organization visited in which the two specialists to whom a particular type of case was referred had different preferences regarding the two treatment options that were available. Depending upon which physician adviser received the case, either treatment A or treatment B would be authorized. For the organization to send all such cases to either of the physicians would have involved a policy decision that the organization was not prepared to make. The organization decided to alternate cases, without regard for the fit between the therapeutic preferences of the attending physician and the physician adviser. So the luck of the draw determined whether an attending physician received authorization with no difficulty or might not be able to obtain authorization at all.
Page 86
committee. Additional discussion with the attending physician may or may not be a part of the process.
Several organizations indicated that their clients, usually an employer, may get drawn into the appeals process when the issue is whether the proposed service will be covered by the patient's benefit plan. In at least one organization, appeals are shifted directly to the clients.
Reporting and Feedback Mechanisms
In inquiring about the impact of the programs operated by the organizations the committee visited, it became apparent that interpretation of results and comparisons across organizations are extremely difficult. What can be made of information from one organization that the number of hospital days per 1,000 covered individuals ranges from 300 days for one client to 600 days for another and from a second organization that reports a range from 200 to 1,300 days per 1,000? For a third organization, the range is 487 to 1,583 days, but the review organization at least knows that the second number applies to a group of retirees. Despite the well-recognized differences in medical care cost and use experience for different age, sex, and other groups and the considerable variation across employee groups, there are no standard adjustments or reporting conventions used by utilization management organizations to account for these differences.
Organizations that provide review services under contract generally provide their clients with periodic reports on their activities. These reports vary considerably in usefulness. At one extreme are organizations that calculate savings based on the difference between services requested and services authorized. At the other extreme are organizations that can provide detailed analyses of inpatient and outpatient utilization for the covered group. Some firms have clients that demand relatively sophisticated, or at least extensive, data, and they risk losing these clients if they cannot respond to those demands. (Problems with different measures of program results are discussed in Chapter 4.)
Discussions of reporting requirements during the site visits conveyed a clear sense that clients evaluate utilization management organizations based on their apparent success in reducing hospital utilization or holding hospital utilization to comparatively low levels. Client reaction to reports of cost and use experience are, thus, an important feedback mechanism to review organizations.
Review organizations also receive several other kinds of feedback. One source is appeals and objections from physicians and patients regarding the organization's decisions. Criteria that produce too much negative reaction and consume too much of the physician advisers' time may be revised.
None of the organizations that provide utilization management services
Page 87
under contract report any routine mechanism to evaluate the impact that their decisions have on the quality of patient care. For example, no systematic mechanisms are in place to track the experience of patients whose care is shifted from an inpatient to an outpatient basis. Similarly, no organization has any systematic process to assess the burden that their procedures place on providers of care. Some organizations, however, report that they survey patients who have gone through prior review. Also, clients may have (or may be planning) programs to monitor quality of care based, for example, on retrospective reviews of certain types of claims such as those showing rehospitalization within a specified number of days after discharge.
Second-Opinion Requirements
Second-opinion programs were not the subject of much systematic inquiry during the site visits because few of the organizations regard second opinions as a major element in their package of services. Second-opinion programs, which are generally confined to a list of 15-30 surgical procedures, have two major objectives. First, they are intended to save money by reducing the likelihood that unnecessary procedures will be recommended and performed. Second, they are an educational device designed to increase the amount of information available to the patient who is contemplating elective surgery.
There are several types of second-opinion programs. Some employers and insurers have voluntary programs that pay for a second opinion if the patient wants it. Other programs are mandatory, that is, they make obtaining a second opinion a requirement for full payment of benefits, but they do not condition payment on the receipt of a confirming opinion. Some benefit plans require a third opinion if the second opinion does not confirm the first. Most programs, like those for preadmission review, require that the patient initiate the process with a call to the utilization management organization.
Several permutations were encountered in the site visits. For example, organizations vary in whether they refer patients to particular physicians for second opinions. Some have panels of physicians who have agreed to provide second opinions, and these organizations generally offer patients the names of three participating physicians whom they can call for an appointment. Other organizations leave the selection to the patient. With regard to procedures about which there may be differences of opinion across medical specialties (for example, between cardiac surgeons and a cardiologists), some programs require that the second opinion be obtained from the nonsurgical specialist. One organization has a second-opinion program that consists of record reviews and telephone consultations by
Page 88
their regular panel of physician advisers. No face-to-face consultation is required.
Although older second-opinion programs required (with few exceptions) a second opinion for any targeted procedure, several organizations now waive the requirement when preadmission or preservice review determines that the clinical indications for the procedure are clear. A typical example would be a patient with uterine cancer recommended for a hysterectomy. The screening of cases during preadmission or preservice review is intended to reduce the cost and inconvenience of the program. However, by retaining the provision for second opinions for cases in which indications are in doubt, the review organization has a means of dispute resolution that can supplement the usual appeals process.
Legal Issues
In Appendix A of this report is a commissioned paper by William A. Helvestine that discusses the legal implications of utilization review, primarily prior review, and continued-stay review techniques. It describes the general lack of explicit legislative, administrative, or judicial rules involving prior review. It also describes standards of behavior that have been applied by the courts to other aspects of health plan administration that are, in many respects, similar to prior review.
In one well-known case, Wckline v. California, a state court has held that a review organization (in this case the state Medicaid program) could be held liable for "defects in the design and implementation of cost containment mechanisms" that result in the denial of medically necessary services. In this particular instance, the organization was not held liable because the harm to the patient was attributed to the negligence of the attending physician. A later case, Sarchett v. Blue Shield of California, explicitly upheld the right of an insurer to challenge an attending physician's decisions about medically necessary care.
A few states have passed laws regulating private review organizations (American Hospital Association, 1989). Maryland and Arkansas have established (but have not implemented at the time of this writing) a certification process that requires submission by organizations of information about review standards, appeals provisions, personnel, confidentiality policies, information for patients and providers, and accessibility to patients and providers (for example, business hours). The laws do not require detailed disclosure of review criteria. Other states have considered, but not passed, legislation that would require that review physicians be licensed within the state, that no penalties (for example, reductions in benefit payments) be imposed on patients or providers for failing to follow review procedures, and that all reviews (including those now performed by nurses) be done by licensed physicians. The efforts to impose state regulation have been attributed, in part, to concern about controlling a few "bad apples"
Page 89
and getting accountability, especially from the smaller organizations. However, physician resistance to outside review and unwillingness to change challenged practice patterns is also cited (Page, 1989). Some proposed regulations could make operations much more difficult for organizations operating on a nationwide basis, and some might make reviews prohibitively expensive.
Despite the lack of much explicit regulation, the committee found that review organizations are aware of the legal risks inherent in efforts to influence patient care decisions and to operationalize the terms of health benefit contracts. There also appears to be a general appreciation of the conventional—but not infallible—protections offered against liability by good management, good judgment, good faith, and good documentation. The contract provisions analyzed in Appendix F reflect the sensitivity of utilization management firms to these legal issues.
Conclusion
As might be expected for a new and evolving activity, prior review programs are not standardized. Aside from a few common elements—the absence of face-to-face contact with patients, the focus on site, timing, and duration of care, and the requirement that negative determinations be made by a physician—all aspects of the process vary markedly from organization to organization. This variation includes the roles and responsibilities of the nurses and physicians who are involved in the review process, the logistics of the process, the nature and availability of the criteria used in prior review, the types of decisions that are made, the appeals process, and reports of impact.
Although review organizations vary in their inventiveness and willingness to tackle new issues of appropriate use, they generally follow the lead of researchers or medical groups in selecting targets for attention. The evolving focus on assessing the clinical indications for selected procedures is a case in point.
Some variation among review organizations is prompted by clients, some by the origins or roots of the organization. Variations in state regulation, which affect many aspects of insurance company operations, do not account for differences among review organizations since little regulation of these programs exists. One exception involves PROs, which face many requirements for their federal business that also govern their private contracts. However, PROs still vary considerably. It might be expected that the outside consulting firms that assess review programs for employers would have a certain standardizing influence over time, but the committee has seen no obvious evidence of this to date.
Page 90
Through its site visits, the committee developed a clear sense that some organizations have better designed programs or more effectively implemented programs than others. However, as the next chapter reports, the limited evidence on the impact of prior review programs does not include any assessment of the link between differences in program characteristics and differences in program results.
References
American Hospital Association, Private Utilization Review, State Issues Forum Monograph Series, August 1989.
Burda, David, "Changing Physician Practice Patterns," Modern Healthcare, February 17, 1989, pp. 18-26.
Business Insurance Survey, "Directory of Utilization Review Companies," Business Insurance, February 20, 1989, pp. 33-68.
Donabedian, Avedis, "Criteria, Norms and Standards of Quality: What Do They Mean?" American Journal of Public Health, April 1981, pp. 409-412.
Foster Higgins, Health Care Benefits Survey, New York, 1987.
Gabel, Jon, Jajich-Toth, Cindy, de Lissovoy, Gregory, and Cohen, Howard, "The Changing World of Group Health Insurance," Health Affairs, Summer 1988, pp. 48-65.
General Accounting Office, Medicare PROs: Extreme Variation in Organizational Structure and Activities, GAO/PEMD-89-7FS, Washington, DC, November 1988.
Gertman, Paul M., and Restuccia, Joseph D., "The Appropriateness Evaluation Protocol," Medical Care, August 1981, pp. 855-871.
InterQual, Inc., The ISD-A Review System, Chicago, 1987.
Mayo Clinic, "The Cost of Effective Utilization Review Programs," Statement for the Institute of Medicine Committee on Utilization Management by Third Parties, Washington, DC, May 20, 1988.
McGraw-Hill, Inc., Review Resources: Sourcebook of Private Independent UR Companies, Washington, DC, 1987.
Meyer, Harris, "Two States Lead Move to Regulate Utilization Review," American Medical News, April 21, 1989, pp. 1, 45.
Milstein, Arnold, Oehm, Marvis, and Alpert, Geraldine, "Gauging the Performance of Utilization Review," Business and Health, February 1987, pp. 10-12.
"New Blues Program to Rain Nurse Reviewers," American Medical News, April 14, 1989, p. 49.
Page, Leigh, "AMA, Insurers Agree on Guidelines for Hospital Admission Review," American Medical News, July 21, 1989, pp. 3, 34-35.
Payne, Susan M. C., "Identifying and Managing Inappropriate Hospital Use," Health Services Research, December 1987, pp. 706-769.
Physician Payment Review Commission, Annual Report to Congress, Washington, DC, 1989.
Project HOPE, A Study of the Preadmission Review Process, Prepared for the Prospective Payment Assessment Commission, Washington, DC, November 1987.
Restuccia, Joseph, Appropriateness Evaluation Protocol Reviewer's Manual, Boston: Boston University, 1986.
Scheffler, Richard M., Gibbs, James O., and Gurnick, Deborah, The Impact of Medicare's Prospective Payment System and Private Sector Initiatives: Blue Cross Experience 1980-1986, HCFA Grant No. 15-C-98757-50-1, Research Program in Health Economics, University of California, Berkeley, July 1988.
Strumwasser, Ira S., et al., Estimates of Non-Acute Hospitalization, Final Report, HCFA Grant No. 18-C98582/5-01 and 2, Washington, DC: Health Care Financing Administration, 1987.
Value Health Sciences, Inc., Medical Review System, Santa Monica, CA, 1989.

































