Chapter 4
DIET AND CHRONIC DISEASE IN THE UNITED STATES
Humans have recognized that there is a connection between diet and health for centuries. As far back as 400 B.C., Hippocrates wrote about the relationship of diet to health: "The power of nutriment reaches to bone and to all parts of bone, to sinew, to vein, to artery, to muscle, to membrane, to flesh, fat, blood, phlegm, marrow, brain, spinal marrow, the intestines and all their parts. It reaches to heat, breath, and moisture."
In 1796 the British Navy instituted what was perhaps the first dietary cure for a human disease: sailors were given lime juice while at sea to cure scurvy. At the time, no one knew about vitamin C or the body's need for it, but people had made the observation that citrus fruits could prevent this life-threatening disease. But only in the past hundred years or so have we come to accept the modern concept of nutrition—that human life depends on a steady intake of a variety of specific dietary components in defined amounts. And it
was not until 1932 that scientists finally isolated vitamin C from lemon juice.
Scurvy was only one of several nutritional diseases that affected many people in the United States. Others included anemia (iron deficiency), goiter (iodine deficiency), rickets (vitamin D deficiency), and pellagra (niacin deficiency). For the most part, these diseases were eradicated in the United States in the first half of this century. The introduction of "iodized" salt, for example, virtually eliminated goiter, and milk fortified with vitamin D did a great deal to solve the problem of rickets.
Today, the diet-related diseases we face are very different. They develop over a much longer time than the vitamin deficiencies of earlier times. The insidious nature of these chronic, or slow-to-develop, diseases is what makes it all the more important to pay attention to what you eat now.
How important is it for us as a nation—and you as an individual—to change our eating habits? Of the 10 leading killer diseases in the United States, 6 are connected in some way to what we eat or drink. Combined, these 6—heart disease, cancer, stroke, diabetes mellitus, chronic liver disease and cirrhosis, and atherosclerosis—accounted for nearly 1.5 million deaths in 1987, nearly 70 percent of all deaths in the United States that year (see Figure 4.1). Alcohol ingestion plays a role in two leading causes of death—accidents and suicide. Only two of the leading causes of death are not connected to what we eat or drink—chronic obstructive lung disease, and pneumonia and influenza.
This is not to say that bad eating habits alone caused 1.5 million deaths in 1987, for diet is not the only factor that causes these diseases to develop. But changing our diet for the better could go a long way to reducing the disease toll significantly.
Improving the nation's diet could also do a great deal to reduce the number of people suffering from illnesses that are serious but not immediately life-threatening. High blood pressure, obesity, dental diseases, osteoporosis, and gallstones
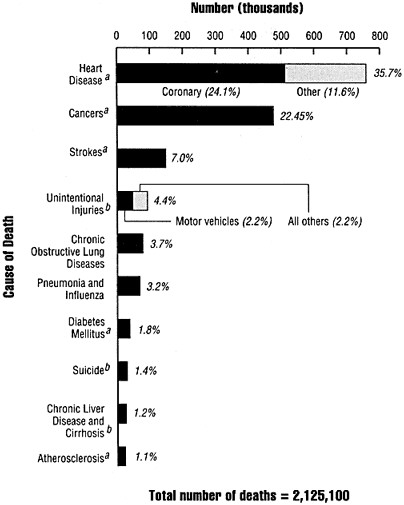
FIGURE 4.1 Estimated deaths and percent of total deaths for the 10 leading causes of death in the United States, 1987. SOURCE: U.S. Department of Health and Human Services. 1988. The Surgeon General's Report on Nutrition and Health. U.S. Government Printing Office, Washington, D.C.
a indicates causes of death in which diet plays a part.
b indicates causes of death in which excessive alcohol consumption plays a part.
fall into this category of diet-related chronic diseases. Over 57 million people in the United States have high blood pressure. Obesity affects 34 million people, osteoporosis 15 to 20 million. Nearly one-half million people were operated on in 1987 because of gallstones. And dental disorders, while rarely fatal, added over $21 billion to the nation's medical bill in that
year. In addition, over 60 million Americans have high blood cholesterol levels, a risk factor for heart disease.
This chapter will explain what these diseases are, who gets them, and—when known—how they develop. The next five chapters will show how various nutritional factors play important roles in the development of these major chronic diseases.
ATHEROSCLEROSIS (HARDENING OF THE ARTERIES)
The number one killer in the United States is heart disease, and the number one cause of heart disease is atherosclerosis, or "hardening of the arteries." Atherosclerosis also contributes to a majority of strokes, the third leading cause of death. Therefore let's begin our discussion by examining how arteries become clogged.
Atherosclerosis is a condition of adulthood, but it starts when we are children. Lipids, particularly cholesterol and cholesterol linked to fatty acids, begin building up in the muscular walls of the arteries that carry blood throughout the body. The places where lipids accumulate are called fatty streaks.
In adolescence, fatty streaks can grow as more and more cholesterol is incorporated into the arterial walls. The body responds to the presence of fatty streaks by covering them with hard, stiff fibrous tissue and muscle, forming what are called fibrous plaques.
As we move into middle age, the fibrous plaques can continue to grow, accumulating cholesterol, fibrous tissue, and muscle cells. At some point, plaques can begin to calcify—calcium deposits form, and the plaques harden. The arteries begin to narrow, and blood has a harder time flowing through them.
At this stage, several things can happen. The worst (and a relatively common) case is when a stiff, brittle plaque
cracks, causing a blood clot to form over the already obstructing deposit. Often, the additional bulk of the blood clot is enough to block the artery, which prevents blood—and the oxygen and nutrients it carries—from reaching tissues downstream from the obstruction. The tissues downstream will then die.
Fortunately, there are indications that the plaque-forming process can be prevented through dietary changes. The continued incorporation of cholesterol into the vessel walls can be arrested and may occasionally even be reversed. When that happens, plaques can actually shrink.
The key to atherosclerosis and its reversal lies with the two major carriers of cholesterol—low-density lipoprotein (LDL) and high-density lipoprotein (HDL). LDL particles carry about 60 to 70 percent of the cholesterol circulating through the blood stream, and HDL particles hold between 20 and 30 percent of the total serum cholesterol.
It turns out that LDL-cholesterol and HDL-cholesterol have quite different roles in the body. LDL-cholesterol delivers cholesterol from the liver to the millions of cells in the body. HDL-cholesterol can help to remove cholesterol from the millions of cells in the body and return it to the liver.
In the simplest terms, too much LDL-cholesterol causes cholesterol to accumulate on the walls of blood vessels, leading to fatty streaks, plaques, and blocked arteries. In societies in which the population is at a high risk of developing atherosclerosis—such as affluent Western societies—most people have relatively elevated LDL and total cholesterol levels. In addition, the level of HDL-cholesterol is an important factor in individual risk. Lowering the amount of LDL-cholesterol in the blood, and raising the level of HDL-cholesterol, can help to remove cholesterol from plaques and fatty streaks, preventing further narrowing of arteries. As is shown in Chapter 6, the levels of both LDL-cholesterol and HDL-cholesterol in the blood are important factors in whether you are at risk for heart disease, peripheral artery disease, and stroke.
HEART DISEASE
When atherosclerosis occurs in the arteries that supply blood to the heart muscle itself (the coronary arteries), the result is often coronary heart disease. Like other organs, the heart muscle needs an adequate supply of blood. If that supply is partially blocked by arterial plaque, the heart muscle does not get enough oxygen, and chest pain (called angina pectoris) can occur.
In this case, open but narrowed arteries may not be able to deliver the additional oxygen that the heart muscle requires at times of emotional excitement or physical exertion. Climbing stairs, for example, can trigger an angina attack; the pain is no different than that produced by any other muscle when it is taxed beyond its capacity.
The heart can compensate for atherosclerosis to a degree by rerouting blood from other coronary vessels, but if atherosclerosis continues unchecked even this will not keep the heart healthy. When a coronary artery becomes blocked, usually when a clot forms at a plaque deposit, the tissues downstream from the obstruction die, and this is called a myocardial infarction, or a heart attack.
About one-third of all people who suffer a heart attack die suddenly because the heart simply stops beating with any regularity. In many instances, prompt medical treatment can restore the heart's rhythm enough to keep the heart attack victim alive. Other people have a nonfatal heart attack in which the heart is damaged but does not stop beating. Within the first few hours after the heart attack, the affected part of the heart dies, and the body begins replacing the dead muscle with connective tissue. Other parts of the heart, if their blood supply is not restricted, eventually grow larger to compensate for the missing muscle.
Approximately 6.7 million people in the United States have coronary heart disease, and in 1987 over 500,000 people died from a heart attack, making it the leading cause of death.
In addition, another 725,000 people suffered a heart attack and survived. Men are more likely than women to develop coronary heart disease and suffer a fatal heart attack at a younger age, but the risk rises rapidly for women after menopause. Women get coronary heart disease about 10 years later than men, but, overall, as many women as men die from coronary heart disease in the United States. The risk of death from heart disease is greater for white men than for black men, but higher for black women than for white women.
The situation is improving, however, and the number of deaths has dropped from its high in 1967. This is true among all U.S. population groups. At least part of the reduced death toll from heart disease—some health experts estimate as much as 30 percent—can be tied to better eating habits among the U.S. public. The death rate from heart disease has also dropped, thanks in part to improved medical treatment and because fewer people are smoking cigarettes.
PERIPHERAL ARTERY DISEASE
Muscle damage from atherosclerosis can also happen in the chest, abdomen, legs, and feet, a disorder known as peripheral artery disease. If the blood supply to the legs or feet is restricted, the result is muscle tiredness, and pain upon exertion. When the blood supply to the legs and feet is completely blocked, tissue dies and gangrene results. In the chest and abdominal areas, atherosclerosis can cause the aorta—the main artery—to balloon and rupture, producing life-threatening internal bleeding.
In 1987, slightly more than 23,000 people died from peripheral artery disease, making it the tenth leading cause of death. But since peripheral artery disease is not usually a direct cause of death—it more often leads to other disorders such as aneurysms that can be fatal—health officials believe it is a larger health problem than the death toll suggests.
STROKE
When atherosclerosis affects the arteries supplying blood to the brain, a stroke can result. One type of stroke, called a cerebral thrombosis, occurs when a blood clot forms on top of an arterial plaque in a blood vessel in the neck or head. This shuts off or seriously restricts the blood supply to a part of the brain, killing the tissue there in a matter of minutes. This type of stroke typically causes paralysis on one side of the body or disturbances of speech, vision, hearing, or memory.
The exact signs and symptoms of the stroke depend on the specific parts of the brain that are affected. With physical therapy, another part of the brain can sometimes be trained to take over the task once controlled by the damaged area, restoring most or all of the lost functions. A cerebral thrombosis can be fatal, however, if the damage occurs in an area of the brain responsible for breathing.
Atherosclerosis can also cause a second type of stroke—a cerebral hemorrhage—if a plaque-covered artery becomes weak enough to rupture. This happens more frequently in people with high blood pressure, and large parts of the brain can die if the bleeding is severe enough. Cerebral hemorrhage strokes have many of the same symptoms as strokes caused by blood clots, but cerebral hemorrhages are more likely to be fatal.
About 2.7 million people in the United States have atherosclerosis of brain arteries, and in 1987 nearly 150,000 people died from a stroke, making it the third leading cause of death. Another 350,000 survive a stroke each year, and all told there are about 2 million stroke survivors in the United States. The risk of death from stroke is twice as great in blacks as whites. Even more than heart attacks, the number of deaths from stroke has declined greatly in the last 20 years, mainly due to effective control of hypertension.
HIGH BLOOD PRESSURE (HYPERTENSION)
Hardening of the brain arteries is one ingredient in the recipe for stroke. The second major element is high blood pressure, also known as hypertension. High blood pressure damages the heart, kidneys, and nervous system and increases the risk for heart attack, stroke, peripheral artery disease, and kidney disease.
Blood pressure is the force of blood against the walls of arteries. This pressure is created by the heart as it pumps blood through the body. The smaller arteries of the circulatory system are responsible for controlling blood pressure. When they contract, blood cannot pass easily through them, and so the heart must pump harder to push the blood through. This increased push increases the blood pressure in the arteries. If the blood pressure increases above normal and remains elevated, the result is high blood pressure.
In most cases, high blood pressure is apparently caused by the interaction between genetic susceptibility and lifestyle influences including high-salt diets, alcohol, and obesity. In a few cases, high blood pressure is a symptom of an underlying problem, such as kidney disease.
Whatever the cause, high blood pressure is bad because it adds to the workload of the heart and damages the lining of arteries. When the heart is forced to work harder than normal for a long period of time, it tends to become bigger. A slightly enlarged heart may function just fine, but a heart that is much larger than normal has a difficult time keeping up with the demands placed on it.
Arteries also show the wear and tear of high blood pressure. Eventually, damage to the arterial wall may contribute to the formation of arterial plaques. Eventually, the increased pressure on plaques already formed can cause them to rupture as well.
There are few apparent symptoms of high blood pressure,
but it is easy to detect with a familiar device called a sphygmomanometer, or blood pressure cuff. The cuff is wrapped around the upper arm and inflated with air. This causes the cuff to squeeze against and compress a large artery in the arm, momentarily stopping the blood flow.
As the air is released from the cuff, the pressure drops to the point when blood begins to flow, the doctor or nurse listens with a stethoscope to the sound of the blood pushing through the artery. While listening and watching a gauge, two measurements are recorded: the pressure when the blood flow first is heard in the artery—the systolic pressure—and the pressure when the flow of blood becomes continuous between heartbeats—the diastolic pressure.
Both numbers, the systolic and diastolic pressures, make up a blood pressure measurement—110/70, for example. The more difficult it is for the blood to flow, the higher the numbers. Two or more readings greater than 140/90 are considered to indicate the presence of high blood pressure.
Blood pressure varies to a certain extent from day to day, and, in fact, the anxiety of being in a doctor's office can raise blood pressure. Thus doctors measure a patient's blood pressure on at least two occasions before making a diagnosis of high blood pressure. Though most cases of high blood pressure affect the diastolic pressure, some show a diastolic pressure below 90 but elevated systolic pressure. Criteria for diagnosing both cases are shown in Figure 4.2.
As many as 58 million people in the United States are thought to have high blood pressure. Some are taking medication to control high blood pressure, and others are not yet diagnosed. High blood pressure is more common among black adults than white adults and is especially high in black women.
Because of widespread publicity about the dangers of high blood pressure, the number of undiagnosed cases has dropped in the past quarter of a century, and more and more people are controlling their high blood pressure successfully. Medical experts estimate that if all cases of high blood pressure
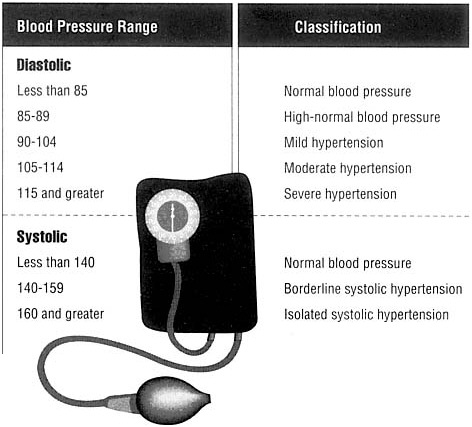
FIGURE 4.2 Criteria used to diagnose high blood pressure.
SOURCE: U.S. Department of Health and Human Services. 1988. The Surgeon General's Report on Nutrition and Health. U.S. Government Printing Office, Washington, D.C.
in this country were brought under control, there would be a 20 percent drop in the total number of deaths among whites, a 30 percent drop among black men, and a 45 percent decline among black women.
CANCER
In 1987, more than 480,000 people in the United States died from cancer, making this most feared disease the number two killer. In addition, almost a million new cases of cancer were diagnosed that year. Cancer rates tend to be higher in the northeast United States and lower in rural areas, except for stomach cancer, where the reverse is true. Some cancers are more common in women, others in men.
Cancer is actually a group of diseases that have one thing in common: groups of cells multiplying out of control.
Normally, about 10 million cells in the body divide every minute under exacting control of the cells' genetic material. This process of cell division is necessary for growth and repair of all body tissues.
But on rare occasions, something goes amiss. A particular control fails, and a cell begins replicating at will, growing, dividing, growing, dividing. The body has mechanisms for spotting and destroying out-of-control cells, but, again on rare occasions, a cluster of such cells escapes detection. Eventually, the cells are growing and dividing so rapidly that they begin causing problems. Depending on where the cells are located, specific symptoms appear.
Doctors diagnose cancer in many ways, but the ultimate diagnosis comes after a sample of the suspect cells is removed from the body and examined under a microscope; cancer cells have a characteristic appearance that distinguishes them from normal cells. Cancers are classified largely according to the site at which they appear—lung cancer, liver cancer, ovarian cancer, and so on.
Some cancers have no connection to diet, or at least none that has been identified as yet. Also, diet is not presumed to be the only factor playing a role in the development of cancer. Nevertheless, as is discussed in the chapters that follow, diet does seem to affect the development of a number of cancers. Those whose development is suspected of being influenced by diet include cancers of the esophagus, stomach, colon and rectum (usually grouped together as colorectal cancer), breast, lung, liver, pancreas, endometrium, ovaries, bladder, and prostate.
Some scientists estimate that 30 to 40 percent of cancers in men and 60 percent of cancers in women are affected by dietary practices. Other researchers have predicted that between 10 and 70 percent of the deaths from cancer are related to diet. This wide range indicates that the scientific evidence is not sufficient to precisely quantify the contribution of diet to the overall risk of cancer. It is also difficult to
predict how large the reduction in risk might be if everyone adopted the eating pattern recommended in Eat for Life. It is noteworthy, though, that several countries with dietary patterns similar to the pattern recommended in the Eat for Life guidelines have about one-half the U.S. mortality rates for cancers associated with diet.
DIABETES
Like cancer, diabetes mellitus—diabetes for short—is a group of diseases with a common biochemical characteristic. In diabetes, the common feature is abnormal metabolism of carbohydrates, particularly glucose. This can lead, over many years, to kidney disease, atherosclerosis, heart attack, stroke, gangrene, and other complications including blindness. In fact, diabetes is the third leading cause of blindness in the United States.
All types of diabetes have something to do with insulin, a hormone produced by special cells in the pancreas, called islets of Langerhans. Insulin is one of several compounds the body uses to control the levels of glucose in the blood. Without insulin, blood sugar levels rise dangerously high. The same thing can happen if the body loses its ability to respond to insulin.
There are two main types of diabetes. The most serious is called insulin-dependent diabetes. In this disorder, the insulin-producing cells of the islets of Langerhans are destroyed, depriving the body of insulin. In most cases, this destruction seems to occur by the body's own hand—cells of the immune system, for some unknown reason, come to see the islets cells as being invaders, and therefore the immune system destroys the cells as it would any foreign object. Diet is not thought to be a cause of this disease.
Insulin-dependent diabetes usually appears well before the age of 40. The only treatment is regular injections of insulin.
About 10 percent of all diabetics—about 1.1 million people in the United States—have insulin-dependent diabetes.
The more common form of diabetes is called noninsulin-dependent diabetes. It is closely linked to the resistance to the action of insulin that occurs in obesity. It accounts for about 90 percent of diabetes cases, or nearly 10 million people in the United States. Noninsulin-dependent diabetes usually appears in middle or old age, particularly in people who are overweight. As many as 9 percent of people 65 and older may have this disease. Genetic, environmental, and lifestyle factors can place a person at increased risk for developing noninsulin-dependent diabetes. The most important risk factors are increasing age, family history of diabetes, and obesity—especially fat carried in the abdomen. Researchers have found that fasting blood sugar levels tend to increase as body weight increases, but exactly how these risk factors contribute to the development of noninsulin-dependent diabetes is still the subject of research.
OBESITY
For more than 50 years, life insurance companies have pointed out that greatly increased body weight is associated with an above-average death rate. In the course of investigating why this is so, researchers have developed a number of ways of judging whether people weigh more than they should for optimal health. The two most important factors associated with the risk of developing several chronic diseases are (1) total body fat, most often estimated by the ratio of body weight to height, and (2) distribution of that fat, on the stomach or on the hips and legs.
Two terms are applied to people who weigh more than they should. ''Overweight" indicates an excess amount of weight for a given height above some standard. "Obese" indicates an excessively high amount of body fat compared to muscle and bone.
A way of determining whether your weight is appropriate for your height is called the body mass index. Body mass index is calculated as follows: body weight (in kilograms) divided by the square of the height (in meters). It is simple to determine your body mass index by using the nomogram shown in Figure 4.3. The most desirable body mass
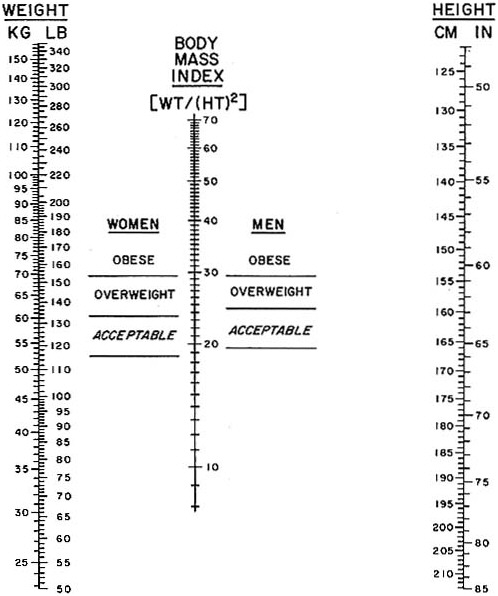
FIGURE 4.3 Nomogram used to determine body mass index. Determine your height without shoes and your weight without clothes. Place a ruler on the nomogram connecting weight on the left with height on the right. The place where it crosses the scale in the center is your body mass index.
SOURCE: Copyright 1978, George A. Bray. Used by permission.
index depends on your age, as shown in Table 4.1. A body mass index greater than 30, regardless of age, is considered overweight.
Another way of judging whether you are too fat or too thin is to compare your weight and height to a table based on body mass index and presented in the measurements we are used to using—feet and inches for height and pounds for weight. The weights for heights shown in Table 4.2 are the suggested ranges based on the body mass indexes in Table 4.1. Ranges of weights are given in the table because people of the same height may have equal amounts of body fat but differ in muscle and bone. The higher weights are suggested for people with more muscle and bone. Weights above the range are believed to be unhealthy for most people. Weights slightly below the range may be healthy for some small-boned people but are sometimes linked to health problems, especially if sudden weight loss has occurred.
The distribution of fat on the body is another important variable in the relationship between being overweight and being at risk for chronic diseases. People who deposit fat in the abdominal area are at greater risk of developing strokes,
TABLE 4.1 Desirable Body Mass Indexes by Age Group
|
Age Group |
Body Mass Index |
|
19-24 |
19-24 |
|
25-34 |
20-25 |
|
35-44 |
21-26 |
|
45-54 |
22-27 |
|
55-65 |
23-28 |
|
Over 65 |
24-29 |
|
SOURCE: National Research Council. 1989. Diet and Health: Implications for Reducing Chronic Disease Risk. National Academy Press, Washington, D.C. |
|
TABLE 4.2 Suggested Weights for Adults
|
|
||
|
Heighta |
19 to 34 Years |
35 Years and Over |
|
5'0" |
97-128 |
108-138 |
|
5'1" |
101-132 |
111-143 |
|
5'2" |
104-137 |
115-148 |
|
5'3" |
107-141 |
119-152 |
|
5'4" |
111-146 |
122-157 |
|
5'5" |
114-150 |
126-162 |
|
5'6" |
118-155 |
130-167 |
|
5'7" |
121-160 |
134-172 |
|
5'8" |
125-164 |
138-178 |
|
5'9" |
129-169 |
142-183 |
|
5'10" |
132-174 |
146-188 |
|
5'11" |
136-179 |
151-194 |
|
6'0" |
140-184 |
155-199 |
|
6'1" |
144-189 |
159-205 |
|
6'2" |
148-195 |
164-210 |
|
6'3" |
152-200 |
168-216 |
|
6'4" |
156-205 |
173-222 |
|
6'5" |
160-211 |
177-228 |
|
6'6" |
164-216 |
182-234 |
|
a Without shoes. b Without clothes. c The higher weights in the ranges generally apply to men, who tend to have more muscle and bone; the lower weights more often apply to women, who have less muscle and bone. SOURCE: U.S. Department of Agriculture and U.S. Department of Health and Human Services. 1990. Dietary Guidelines for Americans, third edition. U.S. Government Printing Office, Washington, D.C. |
||
coronary heart disease, and diabetes than people who tend to deposit fat in their hips and thighs—called the "femero-gluteal" area. The most common method for determining fat distribution is called the waist-to-hip ratio. You can determine that easily by using the nomogram shown in Figure 4.4.
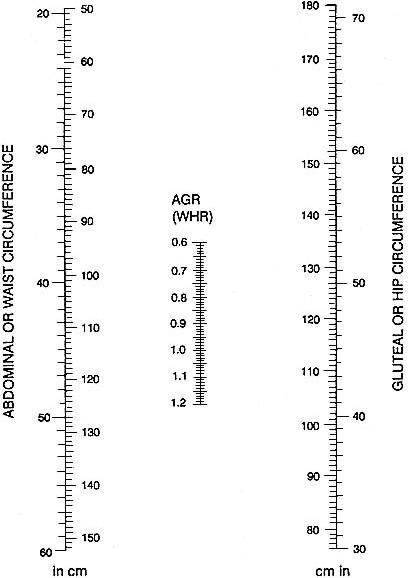
FIGURE 4.4 Nomogram used to determine waist-to-hip ratio. Using a tape measure, measure your waist at the smallest point below your ribs but above your naval. Next, measure your hips at the largest part of your buttocks. Place a ruler on the nomogram connecting size of your waist on the left with size of the hips on the right. Read your abdominal-to-gluteal ratio off the scale in the middle of the nomogram. SOURCE: National Research Council. 1989. Diet and Health: Implications for Reducing Chronic Disease Risk. National Academy Press, Washington, D.C.
Waist-to-hip ratios close to or higher than one are linked to a greater risk for several chronic diseases. If your weight for your height is above the suggested range and your waist-to-hip ratio is high, you should consult your doctor to determine a healthy weight for you and set some reasonable weight loss goals.
Approximately 34 million adults in the United States between ages 20 and 74 are overweight, and of these over 12
million are obese. More women are overweight than men, and black people are overweight more often than whites. And, as a whole, the country is gaining weight. With these figures in mind, it should come as no surprise that 27 percent of all men and 46 percent of all women say they are trying to lose weight.
OSTEOPOROSIS
Osteoporosis is a disease in which the bones become fragile. In severe osteoporosis, bone loss can be so bad that bones fracture with very little stress. The most common bones to fracture in osteoporosis are the hip, vertebrae in the spine, forearm, upper arm, pelvis, and ribs.
Bone is composed primarily of calcium, phosphate, and a porous material called collagen. Though bone seems stable, it is constantly being formed and broken down, or reabsorbed. In childhood, adolescence, and young adulthood, more bone is formed than is broken down. In normal adult bones, these two processes are in balance—when one of these activities increases or decreases, so does the other—and the amount of bone remains constant. Then, sometime between ages 35 and 45, bone starts to resorb faster than it forms, so that the amount of bone begins to decrease. In most cases, the difference is very small, less than one-half percent each year.
Women have a special problem, however. For about 8 to 10 years immediately before and after menopause, bone resorbs some 10 times faster than at younger ages. During that period, women can lose between 2 and 5 percent of their bone each year.
About 15 to 20 million people in the United States, the majority of them elderly women, have osteoporosis. People with osteoporosis suffer an estimated 1.3 million bone fractures each year.
GALLSTONES
Gallstones are small, hard pellets that form in the gallbladder. They can block the bile duct, which transports bile from the liver to the small intestine. The major symptom of gallstones is severe pain.
Bile is a mixture of compounds, including cholesterol, that aids digestion by breaking globs of fat in the intestine into tiny droplets, which can then be absorbed into the blood stream. The liver makes bile and stores it in the gallbladder.
There are two major varieties of gallstones: those composed primarily of cholesterol and those made of various pigments derived from hemoglobin, the oxygen-carrying substance of red blood cells. About 80 percent of the gallstones in the United States are the cholesterol variety. They form when bile contains too much cholesterol; the cholesterol then solidifies to form stones.
About 10 percent of all adults in the United States have gallstones. Women are twice as likely as men to develop them. Native Americans are particularly prone to gallstones, with as much as 65 percent of some groups suffering from this disease.
Obesity increases the risk of gallstones by increasing cholesterol secretion into bile. It seems logical that a high cholesterol intake would increase cholesterol secretion into the bile and increase the risk of gallstones, but there is no firm evidence from studies in humans that the concentration of cholesterol in bile is increased by high intakes of cholesterol.
CIRRHOSIS OF THE LIVER
The liver is susceptible to injury from a variety of causes. Cirrhosis of the liver is a chronic disease whose relentless progression destroys normal liver structure and function. Eventually, the liver fails and death results. Cirrhosis may be caused by viral hepatitis, hemachromatosis (a disease in which excess iron accumulates in the liver), obstruction of the biliary system,




















