15
Falls in Older Persons Risk Factors and Prevention
Falls are a marker of frailty, immobility, and acute and chronic health impairment in older persons. Falls in turn diminish function by causing injury, activity limitations, fear of falling, and loss of mobility. Most injuries in the elderly are the result of falls; fractures of the hip, forearm, humerus, and pelvis usually result from the combined effect of falls and osteoporosis.
Prevention of falls must span the spectrum of ages and health states within the older population and address the diversity of causes of falls without unnecessarily compromising quality of life and independence. Intrinsic risk factors for falls have been found in controlled studies, which allow the identification of those at risk and suggest potential preventive interventions. Elderly individuals with multiple health impairments are at greatest risk, but many healthy older persons also fall each year. Current understanding of the etiology of postural instability and falling is limited, and there is little information about the effectiveness of interventions to prevent falls.
A fall is an unintentional event that results in the person coming to rest on the ground or another lower level.56 Falls can be described in terms of three phases. The first phase is an initiating event that displaces the body's center of mass beyond its base of support. Initiating events involve extrinsic factors such as environmental hazards; intrinsic factors such as unstable joints, muscle weakness, and unreliable postural reflexes; and physical activities in progress at
the time of the fall. The second phase of a fall involves a failure of the systems for maintaining upright posture to detect and correct this displacement in time to avoid a fall. This failure is generally due to factors intrinsic to the individual, such as loss of sensory function, impaired central processing, and muscle weakness. The third phase is an impact of the body on environmental surfaces, usually the floor or ground, which results in the transmission of forces to body tissue and organs. The potential for injury is a function of the magnitude and direction of the forces and the susceptibility of tissues and organs to damage. A fourth phase, although not part of a fall, concerns the medical, psychological, and health care sequelae of the fall and attendant injuries. These sequelae effect the degree of damage and disability resulting from the fall. Approaches to preventing falls and their consequences should focus on factors related to each of these phases.
Falls with certain initiating characteristics (e.g., loss of consciousness, stroke, overwhelming external force from a motor vehicle accident, or violence) are often excluded from the definition of falls in older persons.56 The causes of these falls are different from the typical fall associated with neuromuscular and sensory impairment in an older person and are therefore a distinct topic. The committee concurs in this exclusion; consequently, such falls will not be covered in this chapter.
THE HEALTH BURDEN OF FALLS AND FALL-RELATED INJURIES IN OLDER PERSONS
Mortality
In 1986, there were 8,313 deaths from falls reported in the United States for persons aged 65 and older, making falls the leading cause of death from injury in the elderly.94 This number, derived from death certificates, may underestimate the number of deaths in which falls are a contributing factor.27,49 The rate of fall-related deaths rises rapidly with age for whites aged 70 and older; it rises less dramatically for nonwhites 75 and older (Figure 15-1). By age 85, approximately two-thirds of all reported injury-related deaths are due to falls.6 Older men are more likely than older women to die from a fall; the highest mortality rate occurs in white men aged 85 and over (171 per 100,000), followed by white women aged 85 and over (127 per 100,000). The rate of mortality from falls has declined in recent decades77 (Figure 15-2), which may reflect increased survival of hip fracture patients92 and improved trauma care.95 Some studies suggest
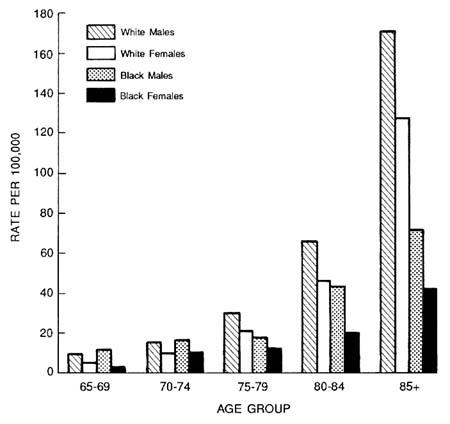
FIGURE 15-1 Death rates from falls per 100,000 persons by age, sex, and race: United States 1986. Source: National Center for Health Statistics annual mortality data tapes reporting external underlying cause of death.
that falls in the frail elderly, especially falls with a ''long lie" (a long waiting time on the ground after a fall before help arrives), are associated with increased mortality independent of injury severity;36,112 this finding, however, is still uncertain.16
Fall-related Injuries
In general, fractures are the most common serious injury resulting from falls in older persons. Specifically, fractures of the hip, wrist, humerus, and pelvis in this age group result from the combined effects of falls, osteoporosis, and other factors that increase susceptibility to injury.21,65 Each year in the United States there are approximately
220,000 each of hip and wrist fractures in persons over the age of 6573 (see Chapter 6). Although precise estimates are not available, there are several times as many fractures of other bones in persons aged 65 and older as there are hip and wrist fractures.29,33,81 The proportions of some frequently occurring fractures (e.g., those of the rib, hand, foot, and ankle) that result from falls versus other types of trauma are also uncertain. The epidemiology of fracture is reviewed in greater detail in Chapter 6.
Other serious injuries resulting from falls include hematoma, joint dislocation, severe laceration, sprain, and other disabling soft tissue injury. There are few data on fall-related injuries other than fracture in the U.S. population. In a regional study in northeastern Ohio, the rate of emergency room treatment of fall-related injuries in persons aged 75 and older approached 80 per 1,000 per year in women and 60 per 1,000 per year in men.29 Another recent study in Dade County, Florida, found an exponential increase with age in the rate of fall injuries that received hospital and emergency room treatment among persons aged 65 and older. These rates were higher in women than men at all ages.95 Among those over age 75, fall injury rates in women exceeded 100 per 1,000 per year; in men they exceeded 80 per
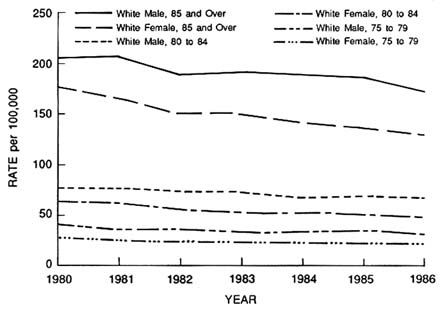
FIGURE 15-2 Death rates from falls per 100,000 persons by age, sex, and year: United States. Source: National Center for Health Statistics annual mortality data tapes reporting external underlying cause of death.
1,000 per year. About 40 percent of treated fall injuries were fractures.
Most falls, however, do not cause sufficient injury to receive medical attention. Only 3 to 5 percent of falls in elderly persons who reside in the community and in nursing homes result in fractures, with fewer than 1 percent of falls causing hip fractures.36,75,93,103 Only about 5 to 10 percent of falls cause other serious injuries requiring medical care.36,102 Between 30 and 50 percent of falls result in a variety of minor soft tissue injuries that do not receive medical attention; the remainder cause no injury or only trivial damage.36,75,82
Frequency of Falls
The few large community surveys of falls in this country and elsewhere have been retrospective, asking respondents about falls in the past year. This focus probably results in significant underreporting and misclassification.22,75 Nevertheless, these studies find that about one-quarter of persons aged 65 to 74 and a third or more of those aged 75 and older report a fall in the previous year,17,84,92 figures that are roughly consistent with 12-month recall data from the National Health Interview Survey (Figure 15-3). About half of those elderly persons (of all ages) who report falling in the previous year fall two or
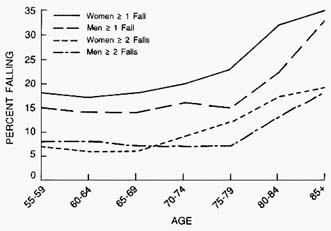
FIGURE 15-3 Percentage of older individuals reporting falls in the previous 12 months by age and sex: United States. Source: National Health Interview Survey's 1984 Supplement on Aging.
more times, a finding consistent with recent prospective studies.75,103 The rate of falls is even higher in health care institutions, with an annual average incidence of about 1,600 per 1,000 nursing home patients.93
Disability
Estimates from the National Health Interview Survey indicate that, among persons aged 65 and older in 1986, there were 5.8 million acute injuries of all types associated with 58.9 million days of restricted activity and 18.8 million bed days.74 Falls probably account for a large part of this total injury burden. About one-quarter of falls in the community result in an activity limitation owing to injury or fear of falling.75,103 Disabilities resulting from hip, wrist, and other fractures in the elderly are substantial (see Chapter 6), but there are few data on disability-associated fall injuries other than fracture. One study found that about half of those persons aged 65 and older living at home who are hospitalized for a fall injury are not discharged to their home;95 this group also includes one-third of those with injuries other than a hip fracture.
The psychological and functional consequences of falls can be severe whether or not an injury occurs, but such consequences have received insufficient attention and study. Postural instability or a fall can lead to fear of falling and anxiety about normal activities on the part of the older person at risk, as well as among family members and care givers. The result may be a reduction in activity, decreased mobility, and increased dependence, often self-imposed but sometimes originating from others (e.g., family members, care givers). Fear of falling, or "postfall syndrome," may contribute to nursing home admissions109 and loss of independence.56
Costs
Meaningful estimates of the medical and other economic costs of falls in the elderly are not possible. Fall-related fractures, however, constitute the major portion of the costs of osteoporosis, which have recently been estimated at $7 to 10 billion annually.81 For example, about 90 percent of the estimated $5.2 billion in direct medical costs for osteoporosis in 1986 were attributable to hospital and nursing home care; 66 percent of hospitalizations and 82 percent of nursing home care admissions for osteoporosis involve fractures in which a fall is usually the source of trauma in an elderly person.83 Studies are needed of the costs of fall injuries other than fractures, of fall
injuries treated on an outpatient basis, of nursing home admissions triggered by fear of falling, and of activity limitations and disability owing to falls.
DETERMINANTS OF FALLS: RISK FACTORS AND CAUSES
Current prospects for the prevention of falls are uncertain, although several intrinsic and pharmacologic factors that are associated with an increased risk of falls have been identified. Many falls in the elderly are probably multifactorial, resulting from the convergence of several intrinsic, pharmacologic, environmental, behavioral, and activity-related factors. However, knowledge regarding the etiologic mechanisms of these risk factors and how they combine to produce falls remains limited. Perhaps even more limited is an understanding of situational and environmental factors that precipitate a fall in persons with predisposing characteristics. Situational and environmental factors may be among the most important determinants of risk in healthy older persons. Finally, a better understanding is needed of factors that affect the risk of injury and other adverse outcomes of a fall.
Intrinsic Risk Factors
Falls are a recognized marker of frailty and mobility impairment in the elderly. The presence and severity of functional disability is a useful indicator of the risk of falling in individuals and populations (Table 15-1). Data from the National Health Interview Survey's 1984 Supplement on Aging indicate that persons aged 75 to 84 who require help with activities of daily living are 14 times more likely, and those with limitations in walking, transfer, and balance activities are 10 times more likely, to report having two or more falls in the previous 12 months compared with persons with no limitations.43 The association of falls with frailty and functional disabilities in the elderly is also evident in the high rates of falls reported in nursing homes.93 The design of effective preventive measures, however, requires knowledge of treatable impairments and conditions that contribute to functional disability, frailty, and falls in older populations.
Normal gait and postural stability depend on the proper functioning of sensory, neuromuscular, and musculoskeletal systems. Limb proprioceptive and tactile input, visual input, and vestibular input are critical for maintaining the body's center of gravity within
TABLE 15-1 Selected Intrinsic Risk Factors for Falls
|
Type of Risk Factor |
Measure (Studies) |
Strength of Evidencea |
|
Demographic |
Strong Inconsistent |
|
|
General health and functioning |
ADL, IADL, mobility impairment (17,31,62,75,90,103,105,111); Reduced physical activity/exercise (15,75,103); Past history of falls (15,55,75,103,105,112) |
Strong; Weak; Strong |
|
Medical conditions |
Arthritis (9,14,32,75,90,103,105); Stroke (15,62,75,84); Parkinson's disease (15,32,75); Dementia (13,14,32,68); Incontinence (55,62,75,90,103,105); Postural hypotension (15,17,75,90,103,105) |
Moderate; Moderate; Strong; Strong; Strong; Inconsistent |
|
Musculosketal and neuromuscular |
Reduced knee, hip, or ankle strength (14,15,75,90,104,105,110,112); Reduced grip strength (9,15,75,110); Hip or knee pain/arthritis; Foot problems (9,31,75,82,103); Impaired knee/plantar reflexes; (31,75,90); Slowed reaction time (1,31,75) |
Strong; Strong; Moderate; Inconsistent; Weak; Weak |
|
Sensory |
Impaired visual acuity (11,15,17,75,82,90,103,105); Reduced depth perception (75); Visual perceptual error (15,89,106); Impaired lower extremity sensory function (11,14,75,90,97,103,105) |
Strong; Weak; Weak; Inconsistent |
|
Other neurologic signs |
Frontal cortex/release (90,105); Cerebellar, pyramidal, extrapyramidal (75,90) |
Weak; Weak |
|
Gait, balance, physical performance |
Gait "abnormalities" (37,75,90,103,105,112); Reduced walking speed (15,37,52,75); Postural sway (11,15,75,89); Impaired dynamic balance (75,89,90,103,105,112,113); Impaired tandem gait, one leg balance (14,75,103); Difficulty arising from chair (15,75,103,104) |
Strong; Strong; Moderate; Strong; Moderate; Strong |
|
Cognitive, psychological |
Reduced mental status test score (13,15,17,55,69,75,84,90,103,105,112); Depression (17,32,69,75,103,105) |
Strong; Strong |
|
Type of Risk Factor |
Measure (Studies) |
Strength of Evidencea |
|
Medication use |
Sedatives, hypnotics, anxiolytics (9,15,17,32,55,62,75,84,86,90,97,103,105,111,112); Antidepressants (9,17,62,75,86); Cardiovascular (9,15,17,32,75,84,90,103,105); NSAIDS* (15,32); Number of medications (9,14,15,32,90,105) |
Strong; Moderate; Inconsistent; Weak; Strong |
|
Note: ADL = Activities of Daily Living; IADL = Instrumental Activities of Daily Living. Numbers in parentheses indicate references. a Strong = association in multiple studies; at least two of which are prospective; moderate = association in multiple studies, only one of which is prospective—some studies are negative; Weak = association in only a few studies, none of which are prospective—some studies are negative; Inconsistent = generally conflicting and inconsistent findings in multiple studies. * NSAIDS = National Health Interview Survey Supplement on Aging, 1984. |
||
its base of support, and these sensory pathways may be compromised by age and disease.114 In addition, age-related disturbances in the organization and central neurological integration of sensory and motor functions may impair the speed, effectiveness, and reliability of postural reflexes, leading to falls.99,115 Age-related slowing of postural reflexes may increase the muscular force required for an effective response to postural disturbances,99 but the strength of skeletal muscles involved in postural control and walking declines with increasing age.12,35,117 Weak muscles and unstable or painful joints may also initiate postural disturbances during voluntary movement.
Several studies have found that impaired vision, lower extremity sensory impairment, reduced lower extremity strength, and reduced grip strength are associated with the risk of falls (see Table 15-1). Arthritis in lower extremity joints and foot disorders contribute to gait and balance problems and are also associated with falls in several studies (Table 15-1). Other sensory problems that may contribute to falls, including cervical mechanoreceptor116 and vestibular disorders,72 and the role of impaired central processing in postural instability and falls,53 need more investigation. A few studies have assessed the association of falls with slowed reaction time, impaired reflexes, and other neurologic signs, with inconclusive results (Table 15-1).
Performance-based measures of gait, balance, and neuromuscular function are strong predictors of falls (Table 15-1), probably because they reflect the combined effect of sensory, neurological, and musculoskeletal impairments on postural stability during the activities in which falls commonly occur.38,103 Impaired cognitive function and depression are associated with an increased risk of falls in several studies. Whether the association of cognitive impairment and falls reflects neurological and psychomotor causes of falls, or behavioral factors related to mental and psychological states, is uncertain.70
It is suspected that psychotropic, diuretic, antihypertensive, and antiparkinsonian medications, especially when inappropriately dosed, may contribute to falls in the elderly by decreasing alertness, depressing psychomotor function, or causing fatigue, dizziness, and postural hypotension.60 Evidence is strongest for an association of falls with the use of hypnotic-anxiolytic drugs, particularly benzodiazepines85 (Table 15-1). The role of diuretic and antihypertensive medications in increasing the risk of postural hypotension and falls needs further investigation.85 Several studies have found an association of falls with the number of medications being taken. Research is needed to determine possible synergistic effects among drugs that might increase postural instability.10
Several common chronic medical conditions, including arthritis, dementia of the Alzheimer's type, stroke, cataracts, and urinary incontinence, as well as such uncommon conditions as Parkinson's disease, are associated with falls in one or more studies (Table 15-1). Although most studies have not found an association of falls with chronic cardiovascular conditions, including postural hypotension, their role as risk factors remains uncertain. Falls may also be a nonspecific manifestation of a variety of chronic and acute conditions.102
In sum, many impairments, disabilities, and conditions repeatedly have been found to be associated with the risk of falls in the elderly. This risk appears to increase with the number of risk factors a person has,76,103 so that those persons most likely to fall can be identified. Additional research is needed, however, including controlled trials, to determine which treatable risk factors are causal.
Situational and Extrinsic Risk Factors
The risk of falls in apparently healthy older persons is substantial,76,103 suggesting that behavioral, psychosocial, activity-related, and environmental factors are important in the etiology of falls and
may combine with intrinsic risk factors to increase risk. For example, minor environmental hazards that are easily negotiated by a healthy individual can become major obstacles to mobility and safety for a person with gait or balance impairments. More generally, the physical demands of certain activities or tasks may exceed the competence of the individual, resulting in a fall.47 Although potentially an important area of inquiry, current understanding of this type of fall risk factor is quite limited.
In healthy, active older persons, situational and extrinsic factors may be the predominant determinants of risk. Compared with frail and impaired elderly persons, falls among the individuals in this group are thought more often to involve overt environmental hazards, risk-taking activities like climbing ladders, hurrying, or running; in addition, they are more often likely to occur away from home.56 Exposure to fall risks is spread over a wide range of physical environments and activities. In contrast, falls in health-impaired older persons are thought to occur during routine ambulation and transfer maneuvers, usually without an overt environmental hazard, and to occur at home. Among the functionally impaired elderly, fall risks are focused on activities required for basic mobility within a familiar environment.
If these contrasting patterns of fall risk are valid, then preventive efforts may need to be tailored to the health level of the population.54 In addition, the two contrasting patterns of risk define a continuum along which many people move with advancing age and declining function. Behavioral, cognitive, and psychological factors that influence how an individual perceives and adapts to the dynamic and changing fit between his or her capabilities and environmental and task demands are a potentially important focus for fall prevention.47,50,106 Additional research in this area is needed to guide the design of behavior-oriented prevention efforts.
Individual adaptations to increasing fall risks range from avoidance of specific high-risk activities and removal of environmental hazards, to enhancement of personal and environmental resources to maintain desired activities, to general curtailment of mobility and activities. Modification of activities and behaviors aimed at reducing risk is often appropriate; however, a delicate balance must always be struck between reduction in risk and maintenance of quality of life and independence. Although drastic reductions in activity may decrease falls in the short-term by reducing exposure, over the long-term, reduced self-confidence and physical deconditioning may only increase risk.
Environmental Factors
Environmental hazards potentially include poor stairway design and disrepair, inadequate lighting, clutter, slippery floors, unsecured mats and rugs, and lack of nonskid surfaces in bathtubs, among many others. Environmental factors are implicated by self-report as contributing to one-third to one-half of falls,56,76,93,103 but most studies do not compare exposure to environmental hazards in those who fall with a control group. Only a few prospective studies have assessed hazards in the home as risk factors, with inconclusive results.76,103 No studies have assessed hazards outside the home or quantified exposure to hazards (in terms of frequency, duration, and intensity) to develop a true estimate of risk; the usual approach is simply to note the presence of hazards in the homes of subjects. In addition, definitions of environmental hazards and methods for assessing them are difficult to standardize.91
The contribution of environmental factors to falls depends on both intrinsic risk factors and other situational variables, but these interactions are poorly understood. Persons with functional disabilities may be especially susceptible to a cluttered, poorly designed, or poorly illuminated environment. In addition, postural stability in an older person may be affected by subtle environmental cues such as lighting and visual and spatial design.80,99,107,115 Although previous experience or familiarity with a particular environmental obstacle may reduce the risk per exposure,102 factors that suddenly precipitate a misstep or trip in these familiar contexts are poorly understood, and methods to study such questions are needed.
Determinants of Injury and Other Outcomes of Falls
For injuries resulting from mechanical energy, such as a fall, the severity of impact, the resistance of the body through inertial forces, the elastic capacity of tissue, and the viscous tolerance of the body organs play an important role in the risk of injury.18 Because of declines in the strength and resiliency of muscle, bone, and other tissues, older persons have an increased risk of injury compared with a younger person subjected to similar impact forces.94 For example, bone mineral density is highly correlated with bone strength; after age 50, bone density declines about 1 percent per year at key sites such as the proximal femur.65 The risk of fractures of the hip, forearm, and other sites increases with decreasing bone density independently of age.20,51,63 Other factors that contribute to the risk of fracture owing to a fall include the orientation of the fall, the speed and effectiveness of protective responses, the ability of skin, fat,
muscle, and environmental surfaces to absorb and distribute mechanical energy, and the architecture of bone.20,64 A better understanding of biomechanical and other factors affecting the risk of fall injuries is needed.
Older people often have a worse outcome than younger people from the same injury because of impaired tissue regeneration, decreased functional reserves, and poorer immunologic function.18,48 The psychosocial sequelae of falls are a poorly understood but potentially important outcome because they may influence functional recovery from fall injuries as well as the risk of further falls. Very little is known about factors that precipitate a ''postfall syndrome" of extreme fear and anxiety.
PREVENTABILITY OF BURDEN
Research on risk factors for falls and the causes of postural instability suggests many preventive interventions, although at present there is almost no direct evidence of the effectiveness of any approach to preventing falls.46 This situation will soon change as a result of studies now in progress. For the moment, however, one can only speculate about which approaches are most promising. In a few instances, evidence regarding modifications of intermediate variables that are risk factors for falls provides a limited basis for speculation.
Exercise and Physical Activity
Skeletal muscle strength and mass decline with age57,58,71 and immobility.12 Impaired strength is a strong predictor of falls in most studies (Table 15-1) and may also increase the risk of injury from a fall. Exercise might prevent falls and injury by strengthening muscles and increasing endurance; maintaining and improving posture, joint motion, and postural reflexes; stimulating cardiorespiratory function; and improving alertness.41 A growing body of evidence indicates that the elderly respond to exercise training and that this response (which may include increased muscle strength and mass and increased aerobic capacity24) continues at very old ages and extremes of frailty.3,25 Weight-bearing exercise may also help preserve bone mass, although this benefit is uncertain.43,81 Exercise and physical activity are positively associated with physical and mental function in cross-sectional studies, but whether exercise training in the elderly can improve physical function, postural reflexes, mental function, or general health and well-being is uncertain.43
The type, level, intensity, and duration of exercise required to
achieve a given health objective are controversial.42 In particular, the effects of low-level exercise and physical activity, such as walking, on muscle strength, bone mass, postural reflexes and other factors affecting fall injuries are uncertain.12 Because low-level exercises are popular, conducive to increased compliance, especially in frail subjects, and less likely to cause adverse effects,41 they should be considered for inclusion in prevention trials along with high-intensity, focused training regimes. Nutritional causes of skeletal muscle weakness should also be considered as targets for intervention.93
There are no controlled studies specifically of exercise to prevent falls, though exercise has been included as a component of a few undifferentiated multiple risk factor interventions.50,78 Exercise, and strength training regimes in particular, will be a key feature of future trials of fall prevention. These studies must address important issues of content, cost, safety, acceptability, and compliance, particularly as these apply to a frail older population with multiple chronic conditions. Techniques for minimizing the risk of exercise-induced injury are needed. Methods are also needed to control for possible increased exposure to situational and environmental fall risks resulting from exercise and physical activity programs, and to differentiate the psychosocial and the physiological effects of exercise interventions.
Rehabilitative Therapies: Balance and Gait Training
Balance and gait abnormalities are associated with falls (Table 15-1) and may be modified through focused rehabilitative interventions.106 Rehabilitative strategies include strength training targeted to impaired muscle groups, habituation exercises for persons with vestibular problems, motor coordination and proprioception exercises for persons with balance problems, and gait training for individuals with gait abnormalities.37,96,106 A few studies suggest it may be possible to improve balance with focused exercise or repetition of specific voluntary movements associated with instability.8,45,106 Additional controlled studies are needed to test the effect of rehabilitative therapies on balance, gait, and falls.
Medications
More than 70 percent of persons 65 and older living at home currently have at least one prescribed medication,44 and the percentage is even higher among nursing home residents.7 Randomized trials to determine whether adherence to conservative guidelines for use of psychotropic medications prevents falls are clearly warranted. Such
guidelines include "a) careful assessment of the need for a psychotropic drug with consideration of nonpharmacologic therapy, b) use of drugs with fewer potential side effects, c) use of the lowest effective dose, d) use of drug for the shortest possible duration,"85 and reduction of other drugs when initiating treatment with psychotropic medications.10 The efficacy of such an approach is unknown. However, there is evidence that the prescribing habits of physicians can be modified.40,87 Educational efforts emphasizing the dangers of self-medication and tinkering with prescribed doses may also be of value5,34 and should be tested. More research is needed to determine the contribution of cardiovascular medications to the risk of falling.
Environmental and Behavioral Interventions
Although there is little epidemiologic evidence linking environmental hazards to the risk of falling, environmental factors remain a promising focus for intervention. Common sense suggests many modifiable factors that affect the safety of both the home and community environments, ranging from sidewalks and stairways in disrepair, to grossly inadequate lighting, to unsafe footwear, to safety measures like grab bars and nonskid surfaces in bathrooms.56,100 More subtle environmental factors (e.g., the shape and positioning of handrails, the design of furniture, storage space, and bathrooms) may also be important.2 Environmental assessment and modification appears feasible as a component of clinic, community-based, and institutional programs.50,93 However, there is a large range of difficulties and costs of environmental and design modifications; in addition, methods for overcoming psychological and economic barriers to implementation must be considered.
Because falls tend to occur where people spend the most time, a home-oriented prevention strategy is important. Numerous checklists are available to help identify environmental hazards in the home,56,100 but there is little information to help prioritize remediation of the many hazards that may be found. Studies are needed to identify where falls occur in the home and the prevalence of various home hazards. Studies of the risk attributable to each of these home hazards, especially in relation to the person's time at risk and their functional disabilities, are critical to the design of prevention strategies. An approach that combines medical and physical therapy evaluation with a home environment assessment may be particularly effective owing to the fact that physical disabilities and environmental factors interact to cause many falls.93,102
Education is an essential element of the prevention of falls
because the perception of health risk supports health action. Educating patients and the public to recognize potential hazards in the home and to distinguish safe from risk-taking behavior may have benefits in terms of the perception of risk and the adoption of safety practices. Some hazards can be addressed by behavioral changes alone—for example, avoiding darkened stairways or such risky activities as standing on chairs. In one study a majority of older persons who had suffered falls felt that their falls were preventable by changes in their own or another's behavior.50 Involving the older person at risk in any assessment of the home environment is an important educational tool that will support compliance with the expert's recommendations. A better understanding of how psychological and cognitive factors affect the success of behavioral and environmental interventions to reduce fall risks would help focus supportive education and counseling.106 Mechanisms for developing community resources and delivering them to elderly persons in need of help in making environmental or behavioral changes should be designed and tested.
Finally, physical restraints are sometimes used with institutionalized patients to prevent falls,23 but no studies have determined whether this approach is successful or whether alternative strategies of managing fall-prone patients would be equally or more effective.
Frameworks for Multiple Risk Factor Interventions
Because of the multifactorial nature of falls and the wide range of factors involved, it is possible that the most effective clinic or community-based interventions will address several types of risk factors and involve diverse disciplines.56,93,102 Intensive clinical evaluation of elderly individuals with instability problems often finds multiple conditions that could contribute to falls and that may be treatable.30,93,102 To prevent falls, however, medical evaluation and treatment may need to target those impairments that are most likely to cause falls and include pharmacologic, rehabilitative, psychosocial, and environmental components in a treatment plan.
Multidisciplinary geriatric assessment and treatment programs suggest one model for multiple risk factor interventions: "Comprehensive geriatric assessment generally includes evaluation of the patient in several domains. . . physical, mental, social, economic, functional and environmental" with the goal of guiding the selection of interventions to restore or preserve health.19 Geriatric assessment in rehabilitation and inpatient settings has demonstrated effectiveness in prolonging survival and reducing hospital and nursing home admissions; there is also some evidence it may improve functional
status.19 Preliminary results from one study suggest that a modest reduction in falls is also possible (Lawrence Rubenstein, VA Medical Center, Sepulveda, California, personal communication, 1989). Performance-oriented assessment and intervention may also be a useful model for fall prevention in medical care settings. In this approach, physical performance and mobility are evaluated in the context of the usual activities of daily living, preferably in the residential setting; those impairments that contribute to functional and mobility problems are targeted for medical, rehabilitative, or environmental remediation.61,101,102
Whether falls can be prevented by aggressive diagnosis, treatment, and rehabilitation of multiple risk factors, either in traditional medical settings or in settings guided by principles of geriatric medicine, remains to be tested. The cost-effectiveness of such an approach and the willingness and ability of third-party payers to finance it must also be carefully evaluated.
Although intrinsic risk factors may be most effectively addressed through clinical interventions, environmental, educational, behavioral, and low-level exercise and physical activity interventions can be implemented through community-based programs. Educational programs may encourage changes on the individual level, as well as on the level of governmental action and public awareness. For example, an increased awareness of the importance of safe access by the elderly and disabled to the broader physical environment is important for increased mobility and may be a factor in the prevention of falls. The effectiveness of community-based fall prevention programs may depend as much on social, political, and psychological factors as on the inherent value of the intervention. Therefore, trials of such programs should include in-depth process as well as outcome evaluation.
Targeting Interventions
There is substantial heterogeneity in the health and functional status of elderly populations, and the diverse causes of falls reflect this heterogeneity. The success of preventive efforts may depend on the ability to target interventions toward those risk factors that are most important in subgroups of the population. Medical and rehabilitative approaches may be most beneficial in the very impaired elderly and those living in nursing homes, whereas environmental and behavioral interventions may have most value among healthy older persons living in the community. Nevertheless, these contrasting approaches may only imply different emphases on a common
set of factors, with intrinsic, environmental, and situational factors combining to cause most falls in both healthy and impaired persons. For example, slowed postural reflexes may increase the risk of falls owing to slips and trips in otherwise healthy persons, and it is possible that postural reflexes can be improved by training and exercise.
The goal of prevention should be not only to reduce falls but to reduce injury and other sequelae of falls. The risk of injury from a fall is the product of a sequence of risks, including the probability of falling, the effectiveness of protective responses, protection by local shock absorbers, including environmental surfaces, and the strength and resiliency of tissue and organs.64 Thus, preventive efforts should address each of the phases in the injury sequence.18 Approaches to decreasing susceptibility to fall injuries are currently limited to therapy to prevent bone loss (see Chapter 6). Environmental surfaces that cushion the impact of a fall, as well as learned protective responses, should also be explored. Finally, improved approaches to treatment and rehabilitation of injuries in the elderly should be emphasized.18
RECOMMENDATIONS
Research
-
Randomized trials of fall prevention interventions are a high priority. Agencies of the National Institutes of Health are currently sponsoring a program of such research, and consideration should be given to increasing funding to support a greater number of trials. Interventions that should be given a high priority for randomized trials include the following:
-
focused exercise and strength training regimes;
-
physical therapy, rehabilitation, and training for specific balance and gait impairments;
-
comprehensive medical diagnosis and treatment focused on neuromuscular, musculoskeletal, and sensory impairments thought to cause falls;
-
adherence to conservative guidelines for use of hypnotic-anxiolytic drugs;
-
improved vision care and updated lens prescriptions;
-
modification of environmental risks in the home;
-
behavioral/educational interventions focusing on risk awareness and risk-taking behaviors; and
-
multiple risk factor interventions.
-
-
Intervention trials should provide information on the effectiveness of distinct treatment components, either by focusing on a single component or, when multifactor interventions are used, through a "crossed" or "matrix" design. Where appropriate, investigators should also provide data on the costs and benefits of the program. Trials should be undertaken in both community-dwelling and institutionalized populations.
-
Support should be provided for observational studies of falls that will expand the knowledge base for future intervention designs by increasing understanding of the etiologic mechanisms of falls and of interactions among risk factors. High priority should be given to the following:
-
better understanding of situational risk factors (behavioral, psychosocial, activity-related, and environmental variables) and how these interact with gait, balance, and other impairments in causing falls;
-
better understanding of the pathophysiology of postural control abnormalities in the elderly to identify new leads for therapy;
-
studies of the effect of psychosocial factors on adaptation and on the coping strategies of older persons adjusting to physical impairments, postural instability, and falls;
-
greater understanding of the effects of injury on the psychological function and quality of life of older persons;
-
studies of where falls occur in the home and of the location and prevalence of various home hazards;
-
studies of the risk attributable to specific home hazards, especially in relation to the person's time at risk to these exposures and their functional disabilities;
-
in cognitively impaired and demented patients, an increased understanding of the respective roles of neurological and behavioral factors in causing falls;
-
studies of diuretic and antihypertensive therapy and falls that examine specific drug types, underlying cardiovascular conditions, and new versus established use, and that have the power to detect moderate increases in risk;
-
studies of the distribution and determinants of risk factors for falls in populations, especially neuromuscular, sensory, gait, and balance impairments; and
-
monitoring of new drugs and postmarketing surveillance in elderly patients for side effects that cause postural instability and falls.
-
-
Support should be provided for studies that address methodological issues in research on falls, including the following:
-
use of intermediate outcome variables, such as balance and strength measures, to estimate the effectiveness of interventions in preventing falls and injuries;
-
reliable methods of self-report ascertainment and description of falls in community-dwelling populations;
-
development of reliable falls surveillance mechanisms for institutionalized and cognitively impaired populations, including accelerometers and other technological approaches;
-
methods for quantifying exposure to fall risk, especially environmental and activity-related risk factors, which are important in assessing the efficacy of interventions that increase exposure by increasing physical activity and mobility; and
-
methods for describing and classifying the full range of fall injuries and other adverse sequelae, including fear of falling and activity limitations.
-
-
The recommendation made in the National Research Council/Institute of Medicine report Injury in America for the use of E-codes (from the World Health Organization's International Classification of Diseases , "External Causes of Injury") in medical records, including hospital discharge records, should be implemented. This practice would allow better tracking of national health objectives, the performance of analytic studies, and evaluation of the effectiveness of proposed preventive measures. Indeed, implementation of this objective would benefit a broad range of injury research and prevention activities.
-
Studies of the biomechanical and other determinants of fall injuries, particularly the understanding of impact responses and tolerances, should be emphasized as a potential means of preventing fall injuries through the environmental control of mechanical energy. Increased research in this area might lead to the design of energy-absorbing surfaces or unobtrusive protective clothing for high-risk older persons.
-
Support should be provided for studies of the economic costs of fall-related injuries other than fractures, of outpatient treatment of fall injuries, and of nursing home admissions related to falls.
Education and Services
-
Support should be allocated for community-based demonstration projects in injury prevention in general and in prevention of
-
falls in particular, stressing education, reduction of environmental risks, and changes in risk-taking behavior. As part of these projects, methods for coordinating existing public- and private-sector organizations and mobilizing new community injury control resources (e.g., retired firemen, building trades workers) should be developed and evaluated.
-
State-of-the-art fall prevention techniques should be integrated into existing national/local injury control programs.
-
Public education aimed at both the older population and society at large should provide information on risk factors for falls and injuries, ways to modify risks, and sources of assistance in risk reduction. These activities should make aggressive use of several media, including television, radio, and the health care delivery system.
-
Treatment and rehabilitation programs addressing the psychological ("post-fall syndrome") and disability outcomes of falls should be developed and tested.
-
The general topic of injury prevention for the older person should be a required part of the core curriculum of training and continuing education of health professionals. Curriculum areas should include the significance of injury (and falls in particular) as a public health problem, risk factors for injury, and presumptive and demonstrated injury control strategies.
-
Professional training in architecture, city planning, product design, and human factors engineering should include information on the range of capabilities and limitations of the older population so that these factors can be incorporated into designs, standards, and plans.
-
Agencies that set and enforce architectural, building, and safety standards affecting the environments of older persons should take into account the range of capabilities in the elderly population. Applied multidisciplinary studies that address the intersection of standards for the built environment, human factors, and aging should be supported.
-
Adequate reimbursement for injury prevention efforts should be sought, including reimbursement for clinical evaluation and interventions to decrease the risk of falling.
Other Areas
In addition to implementation of the recommendations for prevention of osteoporosis outlined in Chapter 6, the recommendations of the surgeon general's 1988 Workshop on Health Promotion and Aging regarding injury control, medications, and physical activity
should also be implemented, with particular emphasis on the following:
-
research and evaluation of promising approaches to improving the understanding and effective use of medications in the elderly, including medication profiles and diaries, color-coding, special packaging, large print, pictographs, and messages adapted to social, cultural, and educational differences;
-
education of patients, family members, and health care providers in proper use, monitoring of side effects, and management of multiple medications for the older individual;
-
continued research on the full spectrum of physiological, functional, and psychosocial effects of exercise regimes and regular physical activity, including strength, endurance, bone mass, agility, coordination, flexibility, and well-being; and
-
research to determine the appropriate type, intensity, frequency, and duration of exercise necessary to achieve the potential benefits in health and functional capacity across a wide age span and range of health status and abilities.
REFERENCES
1. Adelsberg, S., Pitman, M., and Alexander, H. Lower extremity fractures: Relationship to reaction time and coordination time . Archives of Physical Medicine and Rehabilitation 1970; 70:737-739.
2. American Institute of Architects Foundation. Design for Aging: An Architect's Guide. Washington, D.C.: American Institute of Architects Press, 1986.
3. Aniansson, A., Ljungberg, P., Rundgren, A., and Wettereqvist, H. Effect of a training programme for pensioners on condition and muscular strength. Archives of Gerontology and Geriatrics 1984; 3:229-241.
4. Aniansson, A., and Gustafsson, E. Physical training in elderly men with special reference to quadriceps muscle strength and morphology. Clinical Physiology 1981; 1:87-98.
5. Ascione, F. J., and Shrimp, L. A. The effectiveness of four education strategies in the elderly. Drug Intelligence and Clinical Pharmacy 1984; 18:126-131.
6. Baker, S., O'Neill, B., and Karpf, R. S. The Injury Fact Book. Cambridge, Mass.: Lexington Books, 1984.
7. Beers, M., Avorn, J., Soumerai, S. B., Everitt, D. E., Sherman, D. S., and Salem, S. Psychoactive medication use in intermediate-care facility residents. Journal of the American Medical Association 1988; 260:3016-3020.
8. Black, F. O., Wall, C. III, Rockette, H. E., Jr., and Kitch, R. Normal subject postural sway during the Romberg test. American Journal of Otolaryngology 1982; 3:309-318.
9. Blake, A. J., Morgan, K., Bendall, M. J., Dallosso, H., Ebrahim, S. B. J., Arie, T. H. D., Fentem, P. H., and Bassey, E. J. Falls by elderly people at home: Prevalence and associated factors. Age and Ageing 1988; 17:365-372.
10. Blumenthal, M. D., and Davie, J. W. Dizziness and falling in elderly psychiatric outpatients. American Journal of Psychiatry 1980; 173(2):173-203.
11. Brocklehurst, J., Robertson, D., and Groom, J. Clinical correlates of sway in old age. Age and Ageing 1982; 11:1-10.
12. Buchner, D. M. Strategies to improve functional status in older adults by increasing skeletal muscle strength: Rationale and design. In: R. Weindruch and M. Ory (eds.), Frailty Reconsidered: Reducing Frailty and Fall-related Injuries in the Elderly. Springfield, Ill.: Charles C Thomas, in press.
13. Buchner, D. M., and Larson, E. B. Transfer bias and the association of cognitive impairment with falls. Journal of General Internal Medicine 1988; 3:254-259.
14. Buchner, D. M., and Larson, E. B. Falls and fractures in patients with Alzheimer's type dementia. Journal of the American Medical Association 1987; 257(11):1492-1495.
15. Campbell, A., Borrie, M. J., and Spears, G. F. Risk factors for falls in a community-based prospective study of people 70 years and older. Journal of Gerontology 1989; 44(4):112-117.
16. Campbell, A. J., Diep, C., Reinken, J., and McCosh, L. Factors predicting mortality in a total population sample of the elderly. Journal of Epidemiology and Community Health 1985; 39:337-342.
17. Campbell, A., Reinken, J., Allan, B., et al. Falls in old age: A study of frequency and related clinical factors. Age and Ageing 1981; 10:264-270.
18. Committee on Trauma Research, Commission on Life Sciences, National Research Council/ Institute of Medicine. Injury in America. Washington, D.C.: National Academy Press, 1985.
19. Consensus Development Panel. National Institutes of Health Consensus Development Conference statement: Geriatric assessment methods for clinical decision-making. Journal of the American Geriatrics Society 1988; 36:342-347.
20. Cummings, S. R., Black, D. M., Nevitt, M. C., et al. Appendicular bone density and age predict hip fracture in women. Journal of the American Medical Association, in press.
21. Cummings, S. R., and Nevitt, M. C. A hypothesis: The causes of hip fractures. Journal of Gerontology 1989; 44(4):107-111.
22. Cummings, S. R., Nevitt, M. C. and Kidd, S. Forgetting falls: The limited accuracy of recall of falls in the elderly. Journal of the American Geriatrics Society 1988; 36:613-616.
23. Evans, L. K., and Strumpf, N. E. Tying down the elderly: A review of the literature on physical restraint. Journal of the American Geriatrics Society 1989; 37:65-74.
24. Evans, W. J. Exercise and muscle function in the frail elderly. In: R. Weindruch and M. Ory (eds.), Frailty Reconsidered: Reducing Frailty and Fall-related Injuries in the Elderly. Springfield, Ill.: Charles C Thomas, in press.
25. Evans, W. J. Exercise and muscle metabolism in the elderly. In: M. L. Hutchinson and H. N. Munro (eds.), Nutrition and Aging. New York: Academic Press, 1986, pp. 179-191.
26. Fernie, G., Gryfe, C., Holliday, P., et al. The relationship of postural sway in standing to the incidence of falls in geriatric subjects. Age and Ageing 1981; 11:11-16.
27. Fife, D. Injuries and deaths among elderly persons. American Journal of Epidemiology 1987; 126(5):936-941.
28. Fife, D., and Barancik, J. I. Northeastern Ohio trauma study. III. Incidence of fractures. Annals of Emergency Medicine 1985; 14(3):244-248.
29. Fife, D., Barancik, J. I., and Chatterjee, M. S. Northeastern Ohio trauma study. II. Injury rates by age, sex and cause. American Journal of Public Health 1984; 74(5):473-478.
30. Foley, C. J., and Wolf-Klein, G. P. Prevention of falls in the geriatric patient with osteoporosis. In: Clinical Rheumatology in Practice. New York: Le Jacq, 1986, pp. 136-143.
31. Gabell, A., Simons, M. A., and Nayak, U. S. L. Falls in the healthy elderly: Predisposing causes. Ergonomics 1985; 28(7):965-975.
32. Granek, E., Baker, S. P., Abbey, H., et al. Medications and diagnoses in relation to falls in a long-term care facility. Journal of the American Geriatrics Society 1987; 35:503-511.
33. Grazier, K. L., Holbrook, T. L., Kelsey, J. L., et al. The Frequency of Occurrence, Impact, and Cost of Musculoskeletal Conditions in the United States. Chicago: American Academy of Orthopedic Surgeons, 1984.
34. Green, L. W., Mullen, P. D., and Stainbrook, G. L. Programs to reduce drug errors in the elderly: Direct and indirect evidence from patient education. Journal of Geriatric Drug Therapy 1986; 1:3-18.
35. Grimby, G., and Saltin, B. Mini-review: The aging muscle. Clinical Physiology 1983; 3:209-218.
36. Gryfe, C., Amies, A., and Ashley, M. A. longitudinal study of falls in an elderly population. I. Incidence and morbidity. Age and Ageing 1977; 6:201-210.
37. Guimaraes, R. M., and Isaacs, B. Characteristics of the gait in old people who fall. International Rehabilitation Medicine 1980; 2:177-180.
38. Guralnik, J. M., Branch, L. G., Cummings, S. R., and Curb, J. D. Physical performance measures in aging research. Journal on Gerontology 1989; 44(5):141-146.
39. Haddon, W., and Baker, S. Injury control. In: D. Clark and B. MacMahon (eds.), Preventive and Community Medicine. New York: Little, Brown and Co., 1981, pp. 109-140.
40. Hanlon, J. T., Andolsek, K. M., Clapp-Channing, N. E., et al. Drug prescribing in a family medicine residency program with a pharmacotherapeutics curriculum. Journal of Medical Education 1986; 61:64-67.
41. Harris, R. Fitness and the aging process. In: R. Harris (ed.), Guide to Fitness After Fifty. New York: Plenum Press, 1977.
42. Harris, S. S., Caspersen, C. J., DeFriese, G. H., and Estes, H., Jr. Physical activity counseling for healthy adults as a primary preventive intervention in the clinical setting. Journal of the American Medical Association 1989; 261(24):3590-3598.
43. Harris, T., and Kovar, M. G. National statistics on the functional status of older persons. In: R. Weindruch and M. Ory (eds.), Frailty Reconsidered: Reducing Frailty and Fall-related Injuries in the Elderly. Springfield, Ill.: Charles C Thomas, in press.
44. Havlik, R. J., Liu, B.M., Kovar, M. G., Suzman, R., Feldman, J. J., Harris, T., and Van Nostrand, J. Health Statistics on Older Persons, United States, 1986. DHHS Publ. No. (PHS) 87-1409. Hyattsville, Md.: National Center for Health Statistics, 1987.
45. Hecker, H. C., Haug, C. O., and Herndon, J. W. Treatment of vertiginous patients using Cawthorne's vestibular exercises. Laryngoscope 1974; 84:2065.
46. Hindmarsh, J. J., and Estes, E. H., Jr. Falls in older persons: Causes and interventions. Archives of Internal Medicine 1989; 149:2217-2222.
47. Hogue, C. Falls risk: The importance of psychosocial factors. In: R. Weindruch and M. Ory (eds.), Frailty Reconsidered: Reducing Frailty and Fall-related Injuries in the Elderly. Springfield, Ill.: Charles C Thomas, in press.
48. Hogue, C. Injury in late life. Part I. Epidemiology. Journal of the American Geriatrics Society 1982; 30(3):183-190.
49. Hongladarom, G. C., Miller, W. F., Jones, J. M., et al. Analysis of the Cause and Prevention of Injuries Attributed to Falls. Olympia, Wash.: Office of Environmental Health Programs, Department of Social and Health Services, 1977.
50. Hornbrook, M. C., Wingfield, D. J., Stevens, V. J., Hollis, J. F., and Greenlick, M. R. Behavioral and environmental antecedents of falls among the community dwelling elderly: What can we learn from self-report data? In: R. Weindruch and M. Ory (eds.), Frailty Reconsidered: Reducing Frailty and Fall-related Injuries in the Elderly. Springfield, Ill.: Charles C Thomas, in press.
51. Hui, S. L., Slemeda, C. W., and Johnston, C. C. Baseline measurement of bone mass predicts fracture in white women. Annals of Internal Medicine 1989; 111:355-361.
52. Imms, F., and Edholm, O. Studies of gait and mobility in the elderly. Age and Ageing 1981; 10:147-156.
53. Isaacs, B. Clinical and laboratory studies of falls in old people: Prospects for prevention. Clinics in Geriatric Medicine 1985; 1(3):513-524.
54. Isaacs, B. Are falls a manifestation of brain failure? Age and Ageing 1978; 7(Suppl.):97-111.
55. Janken, J. K., Reynolds, B. A., and Swiech, K. Patient falls in the acute care setting: Identifying risk factors. Nursing Research 1986; 35(4):215-219.
56. Kellogg International Work Group on the Prevention of Falls by the Elderly. The prevention of falls in later life. Danish Medical Bulletin 1987; 34(4):1-24.
57. Larsson, L., Grimby, G., and Karlsson, J. Muscle strength and speed of movement in relation to age and muscle morphology. Applied Physiology 1979; 46:451-456.
58. Larsson, L., and Karlsson, J. Isometric and dynamic endurance as a function of age and skeletal muscle characteristics. Acta Physiologica Scandinavica 1978; 104:129-136.
59. Lipsitz, L. A. Orthostatic hypotension in the elderly. New England Journal of Medicine 1989; 321:952-957.
60. Macdonald, J. B. The role of drugs in falls in the elderly. Clinics in Geriatric Medicine 1985; 1(3):621-636.
61. Mathias, S., Nayak, U. S. L., and Isaacs, B. Balance in elderly patients: The ''get-up and go" test. Archives of Physical Medicine and Rehabilitation 1986; 67:387-389.
62. Mayo, N. E., Korner-Bitensky, N., Becker, R., and Georges, P. Predicting falls among patients in a rehabilitation hospital. Archives of Physical Medicine and Rehabilitation 1989; 68(3):139-146.
63. Melton, L. J. III, Kan, S. H., Wahner, H. W., and Riggs, B. L. Lifetime fracture risk: An approach to hip fracture risk assessment based on bone mineral density and age. Journal of Clinical Epidemiology 1988; 41(10):985-994.
64. Melton, L. J. III, and Cummings, S. R. Heterogeneity of age-related fractures: Implications for epidemiology. Bone and Mineral 1987; 2:321-331.
65. Melton, L. J. III, Wahner, H. W., Richelson, L. S., O'Fallon, W. M., and Riggs, B. L. Osteoporosis and the risk of hip fractures. American Journal of Epidemiology 1986; 124:254-261.
66. Melton, L. J. III, and Riggs, B. L. Risk factors for injury after a fall. Clinics in Geriatric Medicine 1985; 1(3):525-530.
67. Mion, L. C., Gregor, S., Buettner, M., Chwirchak, D., Lee, O., and Paras, W. Falls in the rehabilitation setting: Incidence and characteristics. Rehabilitation Nursing 1989; 14(1):17-22.
68. Morris, J. C., Rubin, E. H., Morris, E. J., and Mandel, S. A. Senile dementia of the Alzheimer's type: An important risk factor for serious falls. Journal of Gerontology 1987; 42:412-417.
69. Morse, J. M., Tylko, S. J., and Dixon, H. A. Characteristics of the fall-prone patient. Gerontologist 1987; 27(4):516-522.
70. Mossey, J. M. Social and psychologic factors related to falls among the elderly. Clinics in Geriatric Medicine 1985; 1(3):541-554.
71. Murray, M. P., Duthie, E. F., Jr., Gambert, S. R., et al. Age-related decline in knee muscle strength in normal women. Journal of Gerontology 1985; 40:275-280.
72. Nashner, L. M., Black, F. O., and Wall, C. Adaptation to altered support and visual conditions during stance: Patients with vestibular deficits. Journal of the Neurological Sciences 1982; 2:536-544.
73. National Center for Health Statistics. 1987 Summary: National Hospital Discharge Survey. Vital and Health Statistics, No. 159 (Rev.). Washington, D.C.: U.S. Government Printing Office, 1988.
74. National Center for Health Statistics. Current estimates from the National Health Interview Survey, United States, 1986. Vital and Health Statistics, Series 10, No. 164, pp. 16-52. Washington, D.C.: U.S. Government Printing Office, 1987.
75. Nevitt, M. C., Cummings, S. R., Kidd, S., and Black, D. Risk factors for recurrent nonsyncopal falls: A prospective study. Journal of the American Medical Association 1989; 261(18):2663-2668.
76. Nevitt, M. C. Ascertainment and description of falls. In: R. Weindruch and M. Ory (eds.), Frailty Reconsidered: Reducing Frailty and Fall-related Injuries in the Elderly. Springfield, Ill.: Charles C Thomas, in press.
77. Nickens, H. W. A review of factors affecting the occurrence and outcome of hip fracture, with special reference to psychosocial issues. Journal of the American Geriatric Society 1983; 31(3):166-170.
78. Obonyo, T., Drummond, M., and Isaacs, B. Domiciliary physiotherapy for old people who have fallen. International Rehabilitation Medicine 1984; 5:157-160.
79. Overstall, P., Exton-Smith, A., Imms, F., et al. Falls in the elderly related to postural imbalance. British Medicine Journal 1977; 1:261-264.
80. Owen, D. H. Maintaining posture and avoid tripping. Clinics in Geriatric Medicine 1985; 1(3):581-600.
81. Peck, W. A., Riggs, B. L., Bell, N. H., et al. Research directions in osteoporosis. American Journal of Medicine 1988; 84:275-282.
82. Perry, B. Falls among the elderly living in high-rise apartments. Journal of Family Practice 1982; 14(6):1069-1073.
83. Phillips, S., Fox, N., Jacobs, J., and Wright, W. E. The direct medical costs of
osteoporosis for American women aged 45 and older, 1986. Bone 1988; 9:271-279.
84. Prudham, D., and Evans, J. Factors associated with falls in the elderly: A community study. Age and Ageing 1981; 10:141-146.
85. Ray, W. A., and Griffin, M. R. Prescribed medications, falling, and fall-related injuries. In: R. Weindruch and M. Ory (eds.), Frailty Reconsidered: Reducing Frailty and Fall-related Injuries in the Elderly. Springfield, Ill.: Charles C Thomas, in press.
86. Ray, W. A., Griffin, M. R., Schaffner, W., et al. Psychotropic drug use and the risk of hip fracture. New England Journal of Medicine 1987; 316(7):363-369.
87. Ray, W. A., Blazer, D. G., Schaffner, W., et al. Reducing long-term diazepam prescribing in office practice: A controlled trial of educational visits. Journal of the American Medical Association 1986; 256:2536-2539.
88. Reinsch, S., and Tobis, J. S. Intervention strategies to optimize health behaviors and environment: A cognitive-behavioral approach. In: R. Weindruch and M. Ory (eds.), Frailty Reconsidered: Reducing Frailty and Fall-related Injuries in the Elderly. Springfield, Ill.: Charles C Thomas, in press.
89. Ring, C., Nayak, U. S. L., and Isaacs, B. Balance function in elderly people who have and who have not fallen. Archives of Physical Medicine and Rehabilitation 1988; 69:261-264.
90. Robbins, A. S., Rubenstein, L. Z., Josephson, K. R., Schulman, B. L., Osterweil, D., and Fine, G. Predictors of falls among elderly people: Results of two population-based studies. Archives of Internal Medicine 1989; 194:1628-1633.
91. Rodriguez, J. G., Sattin, R. W., DeVito, C. A., and Wingo, P. A. Developing an environmental hazards assessment instrument for falls among the elderly. In: R. Weindruch and M. Ory (eds.), Frailty Reconsidered: Reducing Frailty and Fall-related Injuries in the Elderly. Springfield, Ill.: Charles C Thomas, in press.
92. Rodriguez, J. G., Sattin, R. W., and Waxweiler, R. J. Incidence of hip fractures, United States, 1970-83. American Journal of Preventive Medicine 1989; 5(3)175-181.
93. Rubenstein, L. Z., Robbins, A. S., Schulman, B. L., Rosado, J., Osterweil, D., and Josephson, K. R. Falls and instability in the elderly. Journal of the American Geriatric Society 1988; 36(3):266-278.
94. Sattin, R. W., and Nevitt, M. C. Injuries in later life: Epidemiology and environmental aspects. In: Oxford Textbook of Geriatric Medicine. New York: Oxford University Press, in press.
95. Sattin, R. W., Rodriguez, J. G., DeVito, C. A., Lambert, D. A., and Stevens, J. A. The epidemiology of fall-related injuries among older persons. In: R. Weindruch and M. Ory (eds.), Frailty Reconsidered: Reducing Frailty and Fall-related Injuries in the Elderly. Springfield, Ill.: Charles C Thomas, in press.
96. Shumway-Cook, A., and Horak, F. B. Vestibular rehabilitation: An exercise approach to managing symptoms of vestibular dysfunction. Seminars in Hearing 1989; 10(2):196-209.
97. Sorock, G. S., and Shimkin, E. E. Benzodiazepine sedatives and the risk of falling in a community-dwelling elderly cohort. Archives of Internal Medicine 1988; 148:2411-2444.
98. Stelmach, C. E., Phillips, J., DiFabio, R. P., and Teasdale, N. Age, functional
postural reflexes, and voluntary sway. Journal of Gerontology 1989; 44(4):B100-B106.
99. Stelmach, C. E., and Worringham, C. J. Sensorimotor deficits related to postural stability: Implications for falling in the elderly. Clinics in Geriatric Medicine 1985; 1(3):679-694.
100. Tideiksaar, R. Preventing falls: Home hazard checklists to help older patients protect themselves. Geriatrics 1986; 41(5):26-28.
101. Tideiksaar, R., and Kay, A. D. What causes falls? A logical diagnostic procedure. Geriatrics 1986; 41(12):32-50.
102. Tinetti, M. E., and M. Speechley. Prevention of falls among the elderly. New England Journal of Medicine 1989; 320(16):1055-1059.
103. Tinetti, M. E., Speechley, M., and Ginter, S. F. Risk factors for falls among elderly persons living in the community. New England Journal of Medicine 1988; 319(26):1701-1707.
104. Tinetti, M. E. Performance-oriented assessment of mobility problems in the elderly. Journal of the American Geriatrics Society 1986; 34(2):119-126.
105. Tinetti, M. E., Williams, F. T., and Mayewski, R. A fall risk index for elderly patients based on number of chronic disabilities. American Journal of Medicine 1986; 80:429-434.
106. Tobis, J. S., and Reinsch, S. Postural instability in the elderly: Contributing factors and suggestions for rehabilitation. Critical Reviews in Physical Rehabilitation Medicine 1989; 1(2):59-65.
107. Tobis, J. S., Reinsch, S., Swanson, J. M., Byrd, M., and Scharf, T. Visual perception dominance of fallers among community-dwelling older adults. Journal of the American Geriatrics Society 1985; 33(5):330-333.
108. U.S. Preventive Services Task Force. Recommendations for physical exercise in primary prevention. Journal of the American Medical Association 1989; 261(24):3588-3589.
109. Vellas, B., Cayla, F., Bocquet, H., dePemille, F., and Albarede, J. L. Prospective study of restriction of activity in old people after falls. Age and Ageing 1987; 16:189-193.
110. Whipple, R. H., Wolfson, L. I., and Amerman, P. M. The relationship of knee and ankle weakness to falls in nursing home residents: An isokinetic study. Journal of the American Geriatrics Society 1987; 35:13-20.
111. Wickham, C., Cooper, C., Margetts, B. M., and Barker, D. J. P. Muscle strength, activity, housing and the risk of falls in elderly people. Age and Ageing 1989; 18:47-51.
112. Wild, D., Nayak, U., and Isaacs, B. How dangerous are falls in old people at home? British Medical Journal 1981; 282:266-268.
113. Wolfson, L. I., Whipple, R., and Amerman, P. Stressing the postural response: A quantitative method for resting balance. Journal of the American Geriatrics Society, 1986; 335:845-850.
114. Wolfson, L. I., Whipple, R., and Amerman, P. Gait and balance in the elderly: Two functional capacities that link sensory and motor ability to falls. Clinics in Geriatric Medicine 1985; 1(3):649-660.
115. Woollacott, M. H., Shumway-Cook, A., and Nashner, L. Postural reflexes and aging. In: J. A. Mortimer, F. J. Pirozzolo, and G. J. Maletta (eds.), The Aging Motor System. New York: Praeger Publishers, 1982.
116. Wyke, B. Cervical articular contributions to posture and gait: Their relations to senile disequilibrium. Age and Ageing 1979; 8:251-257.
117. Young, A., Stokes, M., and Crowe, M. Size and strength of the quadriceps muscles of old and young women. European Journal of Clinical Investigation 1984; 14:282-287.




























