Vision Performance With Contact Lenses
Robert B. Mandell
Visual acuity is a very complex subject in itself, even without regard to contact lens wear. I think that the primary question for us, however, is whether there is any loss in vision performance in changing from spectacles to contact lenses. This brings us to the problem of sorting out what aspects of visual performance must be considered, particularly the task involved in flight.
The first aspect that must be considered is how visual acuity is measured and defined. I shall begin by describing the various ways of defining the test parameters.
VISUAL ACUITY MEASURES
Let us begin by considering various characteristic of contact lenses that might contribute to changes in visual acuity. Although aberrations are the primary concern, residual astigmatism, which is probably the more important aspect of contact lenses, must also be considered.
The real world has, of course, many low-contrast objects in addition to the high-contrast ones normally found on a visual acuity chart. Actually, a number of people have come up with very innovative ways of testing these low-contrast visual functions.
You may be more familiar with what is the common method of using this particular testing procedure. The test can be viewed as a variant of visual acuity testing. It incorporates a threshold testing situation in which the patient views gratings of different spatial frequencies and different contrasts. The threshold detection of these different gratings yields a contrast measure. Measuring an individual's ability to detect these gratings typically results in a plot that looks something like that shown in Figure 1
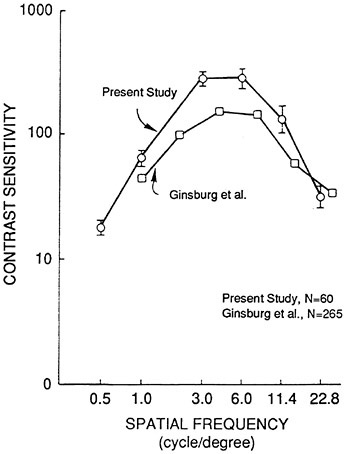
FIGURE 1 Mean contrast sensitivity function for 60 observers of Long and Penn (1986) and Ginsburg et al. (1984). Brackets indicate standard errors.
One of the problems in this test is the interpretation of just what is being measured when a contrast sensitivity test is performed and how the results can be transferred to our visual interpretation of the real world.
There has been a lot of discussion and a lot of disagreement about how valid the contrast sensitivity test is in terms of reproducibility. Figure 2 for example, shows the results from two runs on the same group of individuals. What exactly does a small difference in the response in this particular test mean in terms of some real interpretable measurement?
Recently, some people have tried to measure the same kind of function but by using the more traditional visual acuity testing procedures —namely, modified Snellen-type testing charts. The information obtained from these tests is in traditional terms that can be understood a little more readily than some of the results from psychophysical testing methods.
Figure 3 illustrates another new chart, designed by Bailey and Lovie. It
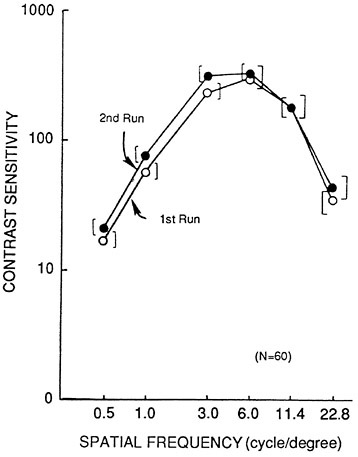
FIGURE 2 Mean CSF for 60 college-age observers in two separate test runs. The brackets around each date in point indicate two standard errors above and below that point. Based on data from Long and Penn (1986).
has a number of advantages in that there are an equal number of letters per row. The sizes of the letters in the rows are determined on a basis that has some meaning in terms of graduation; it allows a simpler scaling and so forth.
These new charts offer a number of advantages. Untrained operators can conduct the test fairly easily, and the results can be interpreted fairly simply.
ACUITY CHANGES
Guillon and co-workers measured visual acuity changes in a group of subjects first with spectacle correction and then with contact lens correction. The group consisted of five near-ametropes who all had small amounts of astigmatism. They wore four different soft contact lenses for the test.
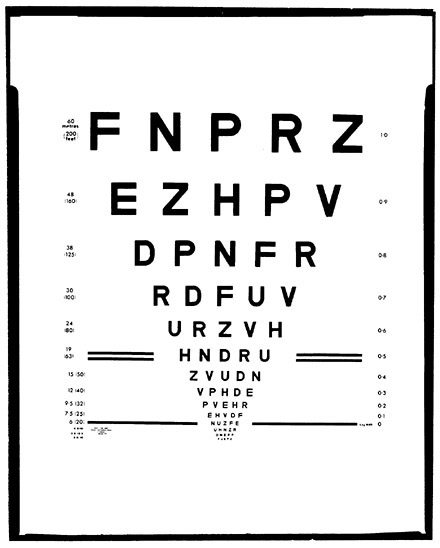
FIGURE 3 Bailey and Lovie chart for contrast sensitivity testing.
In general, there was a reduction of visual acuity with a reduction in contrast as well as a reduction in visual acuity as the luminance was reduced (Figure 4). Guillon et al. concluded that there were visual acuity differences between different contact lenses. However, conclusions of this type are often found in the literature, and they are statistically but not clinically significant.
A careful review of the literature reveals that from one study to the next there can be just about any conclusion one wants regarding the effects of contact lenses on acuity. The more recent studies show that contrast sensi-
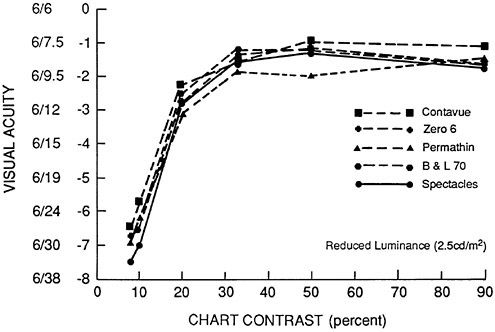
FIGURE 4 Visual acuity results for four contact lenses and spectacles at reduced luminance (2.5 CD/M2). Based on data from Guillon et al. (1988).
tivity function is better with contact lenses than with spectacles. Other studies show just the opposite. Usually the differences between results obtained by the two forms of correction are so small that it makes no practical difference. When there is a “significant” difference between the two types of corrections—contact lenses and spectacles—it can usually be attributed to the fact that there was residual astigmatism present when the subjects were wearing contact lenses. I think that the result is very meaningful, however, in terms of what results might be anticipated with contact lenses worn by military personnel.
SPHERICAL ABERRATION
The aberrations that are normally encountered in the wearing of contact lens are usually not considered a serious problem. Generally speaking, spherical aberration is the only aberration considered significant.
Contact lenses are very interesting in that they offer the potential for changing the eye's spherical aberration. Some researchers have viewed this phenomenon as a possible method of improving visual acuity beyond normal or of getting “super” visual acuity. Unfortunately, there are very few experiments where this was carried out under controlled conditions.
Some contact lens manufacturers have found that certain aspherical designs produce enough spherical aberration that visual acuity is actually degraded. Most of the time this problem is not one to be concerned about because the manufacturer does not make the lens available. Unfortunately, much of the time this information has been restricted to within the organization and the data are thus never published.
RESIDUAL ASTIGMATISM
Residual astigmatism which remains when the contact lens is in place, is a very real problem with regard to fitting military personnel with contact lenses. The task is to fit a group of subjects with an unknown distribution of refractive errors, and without knowing precisely the incidence of astigmatism. If these subjects are to be fit with soft contact lenses, there will be a significant number of people who are going to have enough residual astigmatism that it will cause a reduction in visual acuity. Even if we knew the population numbers, they would not necessarily apply to the military sample of pilots. It certainly must be recognized ahead of time that this will be a significant problem.
If you decide to fit all military personnel needing a refractive correction with soft contact lenses, there are going to be, based on the occurrence of residual astigmatism, a certain number of people who will have to have an alternative lens.
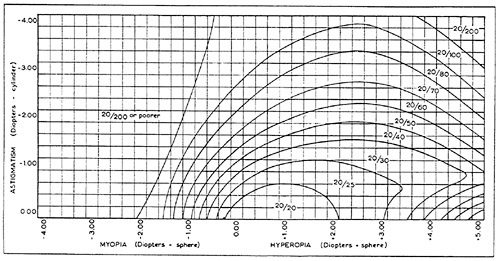
FIGURE 5 Relation between unconnected astigmatism and visual acuity. Based on data from Blum et al. (1959).
Figure 5 shows the distribution of spherical refractive error against astigmatism and the amount of reduction that is to be expected in visual acuity. This information permits prediction of the amount of visual acuity loss that can be expected to occur in a certain percentage of pilots. Residual astigmatism is something that the military will have to contend with in the selection of contact lenses. It will almost have to be an individualized situation as far as fitting is concerned. For an individual who has a certain amount of astigmatism, it cannot always be predicted what type of lens will produce the best visual acuity for that person.
In conclusion, the military's policy toward contact lenses cannot really restrict the lens type to soft contact lenses and expect to provide an optimal correction for the majority of potential pilots. On the other hand, it certainly seems that the military should restrict the number of lenses to certain types. There is going to have to be a broad representation if the needs of all pilots are to be addressed.
REFERENCES
Bailey, I. no date Contrast Sensitivity Visual Acuity Chart. Available from Multimedia Productions, School of Optometry, University of California.
Blum, H.L., et al. 1959 Vision Screening for Elementary Schools: “The Orinda Study.” Berkeley: University of California Press.
Ginsburg, A.P., D.W. Evan, N.W. Cannon, Jr., C. Owsley, and P. Mulvanny 1984 Large-sample norms for contrast sensitivity. American Journal of Optometry and Physiological Optics 61:80–84.
Guillon, M., D.P.M. Lydon, and R.T. Solman 1988 Effect of target contrast and illuminance on soft contact lens and spectacle visual performance. Current Eye Research 7(7):635–648.
Long, G.M., and D.L. Penn 1986 Normative contrast sensitivity functions: the problems of comparison American Journal of Optometry and Physiological Optics 64(2):131–135.







