3
Biologic Markers in Neurotoxicology
The purpose of this chapter is to form a bridge between the issues of nervous system structure and function that are the principal subjects of contemporary neuroscience (Chapter 2) and the goals and emerging methods of quantitative risk assessment (Chapter 6). Identification of biologic markers and understanding of their role in cell response and damage can provide information that will be essential for predicting, and therefore preventing, diseases and disability. This chapter applies to the nervous system the important conceptual framework developed recently by the National Research Council's Committee on Biologic Markers and applied in pulmonary toxicology (NRC, 1989a), reproductive and neurodevelopmental toxicology (NRC, 1989b), and immunotoxicology (NRC, 1991a). We believe that the concepts and definitions of the Committee on Biologic Markers constitute a valuable tool that can be applied to neurotoxicology, as described in the following sections.
CONCEPTS AND DEFINITIONS
Biologic markers, broadly defined, are indicators of change or variation in cellular or biochemical components or processes, structures, or functions that are measurable in organisms or samples from those organisms. Understanding the processes, structures, and functions of the nervous system is the starting point for identifying biologic markers. Current interest in the biologic markers of the nervous system stems from a desire to identify the early stages of system impairment and damage and to understand the dynamics of exposure and the basic mechanisms of response to toxic exposure.
There is growing interest in the use of biologic markers in clinical medicine, epidemiology, toxicology, and related biomedical fields to study the human neurologic effects of exposures to environmental toxicants (NRC, 1989a,b). Clinical medicine uses markers to allow earlier detection and treatment of disease; epidemiology uses them as indicators of internal dose or of health effects and for surveillance; and toxicology uses them to help to determine underlying mechanisms of diseases, develop better estimates of dose-response relationships, and improve the technical bases for assessing risks associated with low levels of exposure (see Chapter 6).
The rapid growth of new molecular and biochemical tools in the practice of medicine has resulted in the development of markers
for understanding disease, predicting outcome, and directing treatment. Over the next few years, many of the tools will be used to estimate chemical exposure. Even now, many diseases are defined, not by overt signs and symptoms, but by the detection of biologic markers at the subcellular, molecular, or functional level after exposure to a toxic agent. The identification, validation, and use of markers in neurobiology and medicine depend fundamentally on increased understanding of mechanisms of action and of molecular and biochemical processes. Biologic markers are allowing investigators to gain a better understanding of chemical-receptor interactions. As noted in Chapter 2, for example, some toxicants interfere with ion channels and thus enhance or suppress impulse conduction along nerves. Tetrodotoxin, a puffer fish poison, blocks the sodium ion channel, thereby impairing impulse conduction. However, the insecticidal pyrethroids keep the sodium ion channels open too long, thereby making the nerve hyperactive.
As we use the term here, markers can be signals or indicators of normal physiology, forerunners of nervous system damage, or clinical signs and symptoms of neurologic disease. A specific biologic marker can serve several purposes and is best characterized by the use to which it is put in a particular context. Markers can indicate susceptibility, exposure to an exogenous agent, internal dose, biologically effective dose (dose at a receptor site), early biologic effect, structural or functional alteration, physiologic status, system damage, or disease. Thus, the choice of a marker and its interpretation depend on the purpose of its use, and its intended use depends on characteristics peculiar to a particular exogenous agent, to an individual organism, or to a particular target organ or tissue (see Table 3-1). If the goal is prevention, the major emphasis will be on monitoring markers that
TABLE 3-1 Examples of Characteristics of Exogenous Agents, Organisms, or Targets That Influence Choice of Biologic Marker
|
Agent-specific characteristics |
Organ- or tissue-specific characteristics |
|
Physiochemical properties |
Blood flow |
|
Interactions |
Membrane permeability |
|
Routes of exposure |
Transport |
|
Duration of exposure |
Receptors |
|
Exposure concentration |
Function |
|
Pattern of exposure |
Homeostasis |
|
Metabolism |
Structure |
|
Activation |
Physiologic state |
|
Detoxification |
|
|
Organism-specific characteristics |
|
|
Species |
|
|
Age |
|
|
Sex |
|
|
Physiologic state |
|
|
Pharmacokinetic characteristics |
|
|
Genetic factors |
|
|
Lifestyle factors |
|
|
Source: NRC (1989b). |
|
identify biologic changes in the nervous system that are predictive of health impairment or overt disease, such as the various biochemicals, metabolites, responses, and characteristics listed in Table 3-2.
Markers represent points in a continuum between health and disease. How they are applied to the neurologic sciences might change as our knowledge of the fundamental processes of disease of the nervous system increases. What are perceived at first to be early signals of exposure and of a system's response to a toxicant could come to be considered health impairments themselves, because of their strong predictive relationship to disease. By the time early changes (markers) are detected, it might be difficult to prevent neuropathy from occurring in response to exposure to a toxicant whose effects are progressive and irreversible. But many neurotoxicants produce damage that is reversible if exposure is stopped (e.g., agents that cause CNS depression). Thus, biologic markers related to the nervous system can be valuable in prevention, in estimation of exposure, in early detection of damage, and in early treatment of disease.
The Committee on Biologic Markers found it useful to define three general categories of biologic markers: those of exposure to chemical or physical agents, those of effects of exposure, and those of susceptibility to the effects of exposure (NRC, 1989a,b). In the context of the nervous system, a biologic marker of exposure is an exogenous substance or its metabolite or the product of an interaction between a substance and some target molecule or other nervous system receptor. A biologic marker of effect is a detectable alteration of an endogenous component within the nervous system that, depending on magnitude, can be recognized as a potential or established health impairment or disease. A biologic marker of susceptibility is an indicator of an inherent or acquired limitation of an organism's nervous system's ability to respond to the challenge of exposure to a specific
TABLE 3-2 Selected Markers of Neurotoxicity in Nervous System
|
General neuronal measures |
|
Cell number |
|
Tetanus-toxin binding |
|
Neurofilament protein |
|
Neuronal structure |
|
General glial measures |
|
Glial fibrillary acidic protein |
|
Oligodendrocyte probe |
|
Transmitter systems |
|
Amino Acid |
|
Excitatory |
|
Inhibitory |
|
Cholinergic |
|
Choline acetyltransferase |
|
Muscarinic and nicotinic receptors |
|
Aminergic |
|
Norepinephrine |
|
Serotonin |
|
Dopamine |
|
Peptidergic |
|
Vasoactive intestinal peptide |
|
Substance P |
|
Enkephalin |
|
Cell biologic responses |
|
Second messengers |
|
Cyclic nucleotide |
|
Phosphorylation |
|
Calcium-dependent transmitter release |
|
Voltage-dependent NA+ or Ca2+ uptake |
toxic substance. Organisms might be particularly susceptible to a toxic substance for several reasons, including a genetic predisposition, existing disease, unique metabolic characteristics, or even the consequences of increased stress (see discussion on markers of susceptibility).
Biologic Markers of Exposure
External exposure is the amount or concentration of a substance in the environment of an organism; internal dose is the amount that is transferred or absorbed into the organism (see Figure 3-1). Biologically effective dose, in general terms, is the internal dose that is quantitatively correlated with an identifiable biologic effect; however, it is more precisely considered to be the amount of a substance that has interacted with a critical cellular or tissue receptor or target where the biologic effect is initiated. Because many such receptor sites in the nervous system are not known or not accessible, it is often necessary to use a surrogate site. For example, the neurofilament cross-linking that follows exposure to γ-diketones is accompanied by dimerization of erythrocyte spectrin; blood samples can reveal that a biologically effective dose has been received by the organism (St. Clair et al., 1988) in that these compounds penetrate to the nervous system sites in proportion to concentrations in blood samples.
Markers of exposure can be based on steady-state or pharmacokinetic measures, such as peak circulating concentration, cumulative dose, or plasma half-life. Individual variations in physiologic characteristics—such as sex, age, blood flow, membrane permeability, and respiratory rate—can affect the absorption and distribution of a chemical and its metabolites (Doull, 1980; NRC, 1986). Age and health status, such as disease, can alter the respiratory rate and thus the pulmonary dose of a toxicant (NRC, 1989a). Exposure concentration, size of delivered dose, and dose rate also affect internal dose. When absorption capacities are exceeded, alternate pathways of clearance come into play. High vapor concentrations (e.g., high concentrations of organic solvents) might be exhaled, rather than absorbed. Species and individual differences in metabolism can drastically alter internal doses of reactive metabolites.
The internal dose of a substance can vary with route of exposure, chemical species, and physical form. To make qualitative or quantitative estimates of exposure with biologic markers, the concentration, duration and pattern of exposure, and physicochemical nature of a toxicant must be considered in the selection of an appropriate marker of exposure (Gibaldi and Perrier, 1982). Other environmental factors, such as temperature, can affect exposure by changing amounts of water consumption and thus of waterborne pollutants ingested. Diet alters intestinal motility and gastric emptying time, as well as the transport of specific substances across barriers in the gastrointestinal system. The
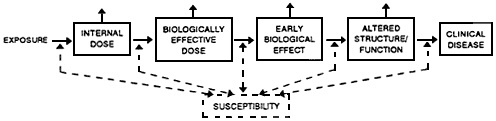
Figure 3-1. Simplified classification of biologic markers (indicated by boxes). Solid lines indicate progression, if it occurs, to the next class of marker. Dashed lines indicate that individual susceptibility influences the rates of progression, as do other variables described in the text. Biologic markers represent a continuum of changes, and the classification of change might not always be distinct. Source: NRC Committee on Biologic Markers, 1987.
formulation or type of mixture that contains a toxicant can affect its transport across protective barriers and membranes in the nervous system.
The presence of active mechanisms of transport into an organ or tissue and the density of nervous system receptor sites can all influence internal dose and biologically effective dose. Metabolism critically affects biologically effective doses of many compounds; the tissue distribution of metabolizing enzymes is an important determinant of effective dose. Many nervous system toxicants act by interfering with neurotransmitter-receptor interactions. Thus, the interpretation of dosimetric data involves an understanding of the role of the receptor in overall cell, organ, or organism function, of coexisting or pre-existing stresses on the organism, and of the existence and availability of repair or compensation during and after exposure (Doull, 1980). These interactive aspects of exposure and response are especially important for the nervous system, which participates in the physiologic regulation of other body systems.
An example of a marker of exposure is the inhibition of blood acetylcholinesterase by organophosphorus pesticides. However, although moderate levels of inhibition—i.e., up to 30%—are not associated with physiologic effects (NRC, 1986), inhibition of blood acetylcholinesterase greater than 30% can be used as a marker of both exposure and effect. As another example, urinary concentrations of 2,5-hexanedione have been suggested as markers of exposure to n-hexane.
Biologic Markers of Effect
For purposes of environmental health research, biologic markers of effects in the nervous system of an organism after exposure to a toxicant are considered in the context of their relationship to health status—normal health, early health impairment and damage, or overt disease (see Figure 3-1). In that context, an effect is defined as any of the following:
-
An alteration in a tissue or organ.
-
An early event in a biologic process that is predictive of the development of a health impairment.
-
A change consistent with early damage to an organ or tissue.
-
A health impairment or clinically recognized disease.
-
A response peripheral or parallel to a disease process, but correlated with it and thus usable in predicting development of a health impairment.
Thus, a biologic marker of a nervous system effect can be any qualitative or quantitative change that is predictive of system impairment or damage resulting from exposure to a substance, e.g., in brainwave recordings, in release of a neurotransmitter (such as dopamine), or in the presence of amyloid in Alzheimer's disease or of neuron-specific enolase in some CNS neoplasms. Markers of early biologic effects include alterations in the functions of target tissues of the nervous system after exposure. As early-warning signals, such markers can be useful dosimeters to guide intervention aimed at reducing or preventing further exposure. Such early-warning signals might also be observed in organs or tissues other than the sites that are critical for toxic action, in that effects on the nervous system can themselves affect the functioning of other organ systems—e.g., caffeine can stimulate the CNS, which can then affect the heart and kidneys.
A tissue affected by a toxicant might exhibit altered function even if the exposed organism has no overt manifestations. Such alteration can in some cases be determined by testing, particularly with the new biochemical probes (e.g., molecular adducts) or
imaging techniques (e.g., magnetic resonance imaging). Biologic markers of functional alterations are most useful if related to specific functions—e.g., acetylcholinesterase for a cholinergic response and epinephrine for a catecholaminergic response.
If the internal dose of a toxicant is great enough, disease will develop, because the biologically effective dose will be sufficient to affect some function irreversibly or produce an effect for a substantial period, as in the case of ethanol. Disease that occurs soon after exposure might be easy to link directly to the toxicant. Disease that occurs long after exposure might be difficult to relate to a specific toxicant, as is postulated for some cases of Alzheimer's disease and other neurodegenerative disorders (Calne et al., 1986), unless the findings are pathognomonic, i.e., are relatively specific to a particular type of exposure (such as γ-diketones and methyl n-butylketone) or are rare in unexposed persons (such as distal axonopathy).
The transition to overt disease can depend on properties of the toxicant, the nature of exposure, the disease process itself, or individual susceptibilities. Because people respond differently to toxicants, it is not surprising that only some members of a population similarly exposed to a given environmental agent will develop a given disease. That is especially true of the nervous system, in which large observed variations in population response to chemical toxicants have been attributed to differences in metabolism, pharmacokinetics, protective mechanisms and barriers, and system complexity.
Although scientists tend to divide biologic markers into groups, there is a continuum between health and disease, and advances in toxicology have demonstrated a continuum between dose and response. Biologic markers are best divided operationally, depending on how they are assessed and how they can be used, but the divisions should not be interpreted to imply mechanistic distinctions (Figure 3-1).
Biologic Markers of Susceptibility
Some biologic markers indicate individual or population factors that can affect response to environmental agents. Those factors are independent of whether exposure has occurred, although exposure sometimes increases susceptibility to the effects of later exposures (e.g., in sensitization to formaldehyde). An intrinsic characteristic or preexisting disease state that increases the internal dose or the biologically effective dose or that amplifies the effect at the target tissue can be a biologic marker of increased susceptibility (NIEHS, 1985; Omenn, 1986). Such markers can include inborn differences in metabolism, variations in immunoglobulin concentrations, low organ reserve capacity, or other identifiable genetically or environmentally induced factors that influence absorption, metabolism, detoxification, and effect of environmental agents. These types of biologic markers are not extensively considered in this report.
VALIDATION OF BIOLOGIC MARKERS
To validate the use of a biologic measurement as a marker, it is necessary to understand the relationship between the marker and the event or condition of interest, e.g., between muscular weakness and exposure to acrylamide. Sensitivity and specificity are critical components of validity (MacMahon and Pugh, 1970). Sensitivity is the ability of a marker to identify correctly those who have been exposed or have a disease or condition of interest; specificity is the ability to identify correctly those who have not been exposed or do not have the disease or condition.
Animal models are useful for understanding the basic mechanistic processes of the expression of markers and the relationships among exposure, early effects, and disease and thus are useful in validating biologic markers (see Chapter 4). If a disease can be satisfactorily induced in experimental animals (e.g., axonopathy in rats exposed to n-hexane), then potential biologic markers for predicting eventual disease can be explored, and early indicators of the disease might be identified for use in human studies (e.g., peripheral neuropathy). A major goal of research with biologic markers is to develop markers that reliably indicate an early stage in the development of a disease process in humans when effective intervention is still possible. That is especially important for the nervous system, where repair is limited and early intervention might offer the only chance of recovery.
One of the most serious challenges for the use of animal models in neurotoxicology is that many expressions in the human central nervous system are quite different from those which can be assessed directly in animal models. Moreover, even for events that appear to be similar, humans might differ from specific experimental animals in their functional reserve capability. Therefore, the degree of impairment required to cause a particular functional deficit could differ for apparently equivalent levels of damage. Use of appropriate biologic markers for changes in neurologic functions that are similar between animals and humans could help determine functionally equivalent amounts of damage. For example, changes in neurotransmitter turnover might provide a basis for interspecies comparability. This application of markers has been useful in neuropharmacology and should find increased application in the development of neurotoxicologic markers. Until recently, such markers were not directly measurable in humans. However, new scanning techniques of positron-emission tomography and magnetic resonance imaging can provide information in vivo on the neurochemistry of humans and experimental animals.
The principal purpose of markers in health research is to identify exposed people, so that risk can be estimated and disease prevented. Particularly critical for marker validation is the strength of biologic plausibility that supports an association between a change in a specified signal (a marker) and the occurrence of a specific exposure or of a change in a specific effect.
Validation of a specific marker depends on its expected use in monitored populations. Biologic markers observed well before the onset of disease might have low predictive value for the disease itself, but function acceptably as criteria for defining exposed populations and thus be useful for long-term followup. For example, heroin addiction in California might be a useful clue of potential exposure to the neurotoxicant MPTP for epidemiologic research, even though its relationship to a parkinsonian syndrome is indirect. Conversely, an effect marker that is expressed long after exposure could be of relatively little use in exposure assessment, but very important in predicting progression of disease or calculating risk. For example, neurobehavioral manifestation of prenatal exposure to methylmercury can persist well into adulthood.
Quality assurance and quality control are fundamental to the objective development and application of accurate and verifiable biologic markers. The objective of laboratory quality-assurance practices is to ensure that findings reported by one laboratory are in fact verifiable and within acceptable limits of measurement error, that they accurately indicate the concentrations or presence of the biologic changes reported to have been found, and that they are objective and free from sources of bias introduced through the analytic process. General issues of quality assurance and quality control have been addressed by documents produced by the
Food and Drug Administration (FDA), the U.S. Environmental Protection Agency, the Organization for Economic Cooperation and Development, and other regulatory organizations. FDA developed a set of guidelines known as good laboratory practices, or GLPs (FDA, 1988), which are now incorporated into the standard procedures of most testing and analytic laboratories for well-established assays. GLPs are intended to reduce the chance of contamination (particularly important in the measurement of biologic markers of exposure) or of changes in biologic variables introduced by sample storage, processing, or measurement (Zeisler et al., 1983). The application of GLPs to analysis of biologic samples, especially human tissue, has been reviewed by operational units of the Centers for Disease Control, the National Institute of Standards and Technology (formerly named the National Bureau of Standards), and various clinical laboratories (ACS, 1980; NCCLS, 1981, 1985). Because most of the biologic markers discussed in this report are still at a research stage, standardized GLP practices regarding them remain to be established for laboratories.
USE OF BIOLOGIC MARKERS IN RISK ASSESSMENT
Cellular and molecular markers can serve as powerful new tools for the assessment of risks associated with exposure to environmental toxicants. Markers that indicate the delivery of an internal dose or a biologically effective dose or the induction of a disease process can be useful in hazard identification—i.e., in the qualitative step by which an environmental agent is causally associated with an adverse effect. Biologic markers can also be used to determine dose-response relationships, especially at the low doses relevant to exposure to many environmental chemicals. In addition, they can be used to quantify actual exposures.
Biologic markers in environmental-health studies offer an opportunity to determine the shape of the lower end of the dose-response curve in humans—an opportunity that has not yet been used extensively in standard human epidemiologic or laboratory animal studies. Nevertheless, it is likely to remain uncommon to have information on concentrations of a toxicant at the site of action within the nervous system.
Many neurotoxic effects can be studied in experiments conducted with doses at which enzymatic detoxification or activation and other biochemical reactions along the causal chain are not saturated—i.e., at which the dose-response relationship is still linear. When dose-response relationships are not linear, measures of dose of active forms of toxicants at relevant sites in the nervous system are important for understanding those relationships. In addition, the use of biologic markers can help to sort out potential nonlinearities with respect to dose and can facilitate approaches to four problems critical in predicting neurotoxicity:
-
Differences in sensitivity of the individual to neurotoxicants at different stages of life. (The previous report on biologic markers in reproductive toxicology contains an extensive discussion of neurologic markers of developmental effects [NRC, 1989b].)
-
Protective mechanisms and barriers that vary with respect to developmental age, location in the nervous system, and degree of metabolic integrity.
-
Repair and compensation processes for types of damage that appear to be at least partly reversible under some conditions of exposure.
-
Differences in pharmacokinetics (absorption, distribution, metabolism, and excretion) between chemicals and between animals and humans.
It has long been recognized that sensitivity to adverse effects during development can differ dramatically over short periods—especially during gestation. Developmental signals might be present over short periods at the intensity required to induce axons to find their targets and for other key physiologic
and biochemical events to occur; these signals might be disrupted by toxic chemicals. Understanding the physiologic basis of temporal differences in sensitivity will be a key to determining over what periods exposures should be aggregated for best experimental and epidemiologic quantification of risks. For example, Marsh et al. (1987) have shown the relationship between the incidence of a variety of fetal methylmercury effects and the time of maximal exposures during gestation, as indicated by sequential mercury concentrations in the hair of the mothers in the Iraqi mass-poisoning incident (see Chapter 1).
It is important to note that, because of the metabolism and the pharmacodynamics of chemical toxicants, there is a continuing need for the development of better and more accurate markers of internal dose that can be used to estimate biologically effective doses. That refinement of dose-response modeling is fundamental to risk assessment.
Neurons do not regenerate in adult life, and some important neurologic conditions (including Alzheimer's disease, Parkinson's disease, and amyotrophic lateral sclerosis) are associated with progressive cumulative loss of specific types of neurons. However, considerable numbers of cells can be lost before clinical signs of impairment are detectable. Thus, exposure to agents causing such loss might proceed without apparent effect for years. Even after symptoms appear, identifying the potentially relevant exposures among those of a lifetime is nearly impossible.
Epidemiologic research on neurodegenerative diseases would be greatly facilitated if either or both of the following types of biologic markers were available:
-
Measures of the past accumulation of relevant damage in people who have not yet developed clinical illness. For example, can our new tools for imaging the brain be applied to develop a census of the relevant cells left in people of different ages with different past exposures? Imaging methods are being applied to studies of people exposed to doses of MPTP that have not yet produced clinical effects. It is analogous to the use of chest x-rays, FEV1, (forced expiratory volume in 1 second), and FVC (forced vital capacity) to assess the accumulation of chronic respiratory damage (NRC, 1989a).
-
Measures of the current rate of loss of the relevant cells. When cells die, do they release measurable amounts of a distinctive form of an enzyme or some other cellular component that could be used as a biologic marker? Distinctive patterns of electric activity in discrete brain regions can be monitored, as can the integrity of neurochemical systems, e.g., receptor binding, synthetic enzyme activity, and glucose utilization.
SUMMARY
In toxicology and epidemiology, biologic markers have several major advantages as means of exploring the relationship between exposures and effects:
-
A more complete scientific understanding than a simple input-output analysis based on external dose and the incidence of disease, by virtue of the incorporation of more relevant information about critical events and molecular mechanisms.
-
The eventual prospect of improving mechanism-based estimations of risk.
-
Improved sensitivity, specificity, and predictive value of detection and quantification of adverse effects at low dose and early in exposure at the cellular or subcellular level.
-
The prospect of confirming exposure-related effects and narrowing the search for exposures.
-
A better understanding of unique susceptibilities in various population groups.
-
A better understanding of disease processes in the nervous system.
Neuroscience and neurotoxicology can be enhanced by directing more research atten-
tion to quantitative questions—''How much?'' "How fast?" "According to what quantitative functional relationship?"—among the series of causal intermediate processes involved. The role of biologic markers is to measure the steps of disease processes at as many different points as is feasible and to aid the development of means to stop and reverse the processes.










