2
Background
MALARIA AS A DISEASE
Malaria in humans is caused by four species of protozoan parasites of the genus Plasmodium: P. falciparum, P. vivax, P. ovale, and P. malariae. Although P. vivax is responsible for most malaria infections in the world, the most severe form of malaria is caused by P. falciparum. The severity of malarial illness depends largely on the immunological status of the person who is infected. Partial immunity develops over time through repeated infection, and without recurrent infection, immunity is relatively short-lived.
The distinction between infection and disease is particularly important in malaria, since infection with the parasite does not necessarily result in disease. Many infected people in areas where malaria is endemic are asymptomatic: they may harbor large numbers of parasites yet exhibit no outward signs and symptoms of the disease. Asymptomatic individuals are major contributors to the transmission of malaria parasites, however.
For reasons not fully understood, the epidemiology of malaria transmission and the severity of the disease vary greatly from region to region, village to village, and even from person to person within a village. Some of these differences are due to the particular species of parasite. The degree of compliance with an antimalarial drug regimen, local patterns of drug resistance, and an individual's age, genetic makeup, and
duration of exposure to infective mosquitoes may also influence the severity of the disease.
Clinical Aspects
The clinical manifestations of malaria are varied. The classic description of an individual progressing episodically from shaking chills through intense fevers to drenching sweats is characteristic but not universal. In areas where malaria is common, infected individuals may have symptoms that mimic other diseases, making a correct diagnosis difficult. The problem of diagnosis is especially difficult in children, who may have high blood levels of parasites but relatively mild symptoms. In areas where health workers are unfamiliar with malaria, or with patients in whom the range of symptoms may not point clearly to malaria, misdiagnosis is a serious problem.
Severe and complicated malaria, generally due to infection with P. falciparum, is a medical emergency. In the absence of prompt intervention, the patient's condition can deteriorate rapidly, often ending in death (Figure 2-1). About 80 percent of deaths from the disease result from cerebral malaria, a state of altered consciousness, sometimes including coma, in patients infected with P. falciparum. Renal failure, hypoglycemia, severe anemia, pulmonary edema, and shock may also play a role in fatal malaria.
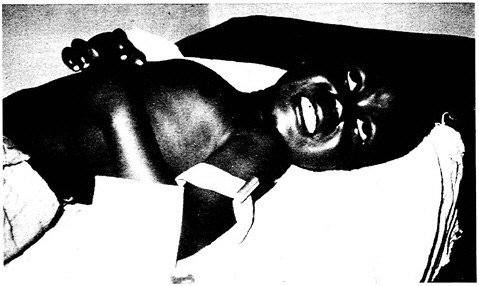
FIGURE 2-1 An African child with severe malaria. (Photo courtesy of Dr. Terrie Taylor, IOM Malaria Committee member)
Malaria during pregnancy can cause miscarriages, fetal death, intrauterine growth retardation, low birth weight, and premature delivery. Women pregnant for the first time and in their third trimester are at particular risk for severe anemia and sometimes even death. The impact of malaria during pregnancy on infant and child development is unknown.
Malarial anemia is an important contributor to P. falciparum-associated morbidity and mortality. Because of the risk of transmitting the human immunodeficiency virus (HIV) and other blood-borne pathogens (including hepatitis B virus and the bacterium that causes syphilis) through contaminated blood, the treatment of malarial anemia with blood transfusions raises serious clinical and safety questions. This risk is of particular concern in areas where screening of donated blood for the presence of HIV and other pathogens is not routine and where blood transfusion equipment is reused without being sterilized.
Immunity
Assuming they survive childhood, people in areas of endemic malaria often acquire a moderate level of immunity to malaria by being infected repeatedly. Although they may experience mild symptoms of the disease, including recurrent fevers, they rarely suffer the more severe and potentially fatal consequences. Without repeated exposure, however, this immunity is relatively short-lived, and although it almost always protects against life-threatening malaria, it does not prevent occasional episodes of fever and chills.
Role of Genetics
Some population groups have genetic characteristics that render them resistant to certain forms of malaria. For example, persons of African descent who lack the so-called Duffy blood group surface antigens cannot be infected with P. vivax. The heterozygous sickle cell trait, often present in people of African descent, partially protects against infection with P. falciparum. Other hereditary abnormalities, such as glucose-6-phosphate dehydrogenase deficiency, are partially protective against malaria.
DIAGNOSIS
Medical personnel should suspect malaria in anyone with a fever who has recently been in a malaria-endemic region. A definitive diagnosis of malaria infection is made by microscopic examination of stained blood smears for the presence of parasites (Figure 2-2). In the early stages of infection and at all stages of infection with P. falciparum, when parasites
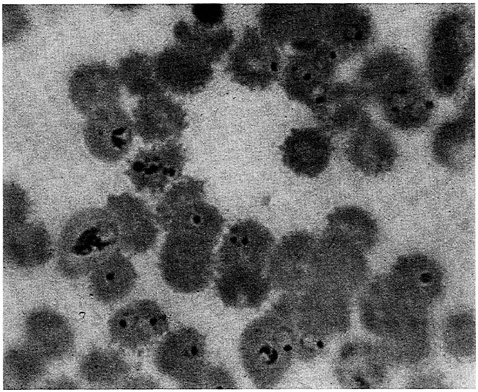
FIGURE 2-2 Photomicrograph of a stained smear of Plasmodium falciparum-infected red blood cells, magnification approximately 1,200×. (Photo courtesy of Dr. Terrie Taylor, IOM Malaria Committee member)
disappear from the peripheral blood during schizogony, few or no parasites may be present in a blood smear; examination of blood smears taken at frequent intervals may be necessary to establish a diagnosis. A positive blood smear taken from a feverish patient living in an endemic region does not conclusively implicate malaria as the cause of illness, because many asymptomatic individuals have circulating parasites in their blood and the fever may be due to other infectious agents.
THE PARASITE
Life Cycle
The life cycle of the malaria parasite is complex (Figure 2-3). The process—three phases in the mosquito and two in the human host—has been divided by scientists into nearly a dozen separate steps. The parasite
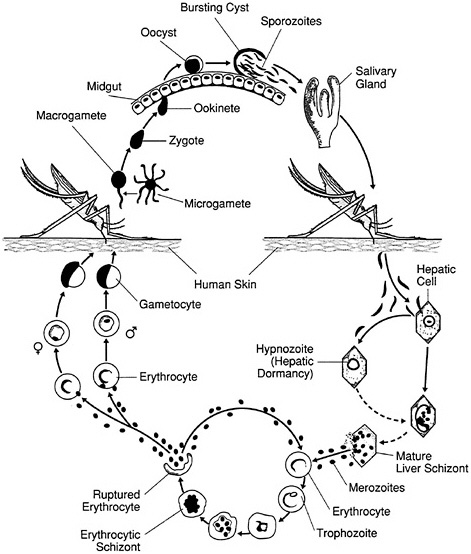
FIGURE 2-3 The life cycle of the malaria parasite. (Adapted from Hospital Practice, September 15, 1990, by permission of HP Publishing, New York)
is transmitted to humans by the sporozoite forms in the saliva of infected female mosquitoes of the genus Anopheles. Soon after entering the human host, the sporozoites invade liver cells, where during the next 5 to 15 days they develop into schizonts. Each schizont contains 10,000 to 30,000 “daughter” parasites called merozoites, which are released and invade the red blood cells. Once inside the red blood cells, each merozoite matures
into a schizont containing 8 to 32 new merozoites. The red blood cell eventually ruptures and releases the merozoites, which are then free to invade additional red blood cells. The rupturing of red blood cells is associated with fever and signals the clinical onset of malaria.
Some merozoites differentiate into sexual forms, gametocytes, which are ingested by a mosquito during its next blood meal. Once in the mosquito, the sexual forms leave the blood cells, and male and female gametes fuse to form a zygote. Over the next 12 to 48 hours, the zygote elongates to form an ookinete. The ookinete penetrates the wall of the insect's stomach and becomes an oocyst. Over the next week or more, depending on the parasite species and ambient temperature, the oocyst enlarges, forming more than 10,000 sporozoites. When the oocyst ruptures, the sporozoites migrate to the mosquito salivary glands, from where they may be injected back into the human host, thus completing the cycle.
Relapse and Recrudescence
Malarial illness may recur months to years after apparently successful treatment. In patients infected with P. vivax and P. ovale, this phenomenon is known as relapse. Relapse is caused by dormant liver-stage forms of the parasite that resume their developmental cycle and release merozoites into the bloodstream. The recurrence of malaria caused by P. falciparum and P. malariae is due to recrudescence, which is caused by surviving blood-stage parasites from an earlier infection.
THE MOSQUITO
Of the more than 2,500 known species of mosquitoes worldwide, only a sub-group of 50 to 60 species belonging to the genus Anopheles are capable of transmitting malaria. Female anophelines require blood meals to reproduce (Figure 2-4). Some anopheline species are indiscriminant feeders; others prefer to feed on animals (zoophilic) or humans (anthropophilic).
Anopheline mosquitoes breed in relatively clean water, with certain species having very specific preferences as to their aquatic environment (Figure 2-5). Understanding these preferences is crucial for targeting effective malaria control interventions. For example, An. stephensi can breed in tin cans and water cisterns, while Anopheles gambiae, the most important malaria vector in Africa south of the Sahara, prefers small, sunlit pools.
Life Cycle
The mosquito undergoes four stages of growth: egg, larva, pupa, and adult (imago). Adult females mate once and store the sperm. The female
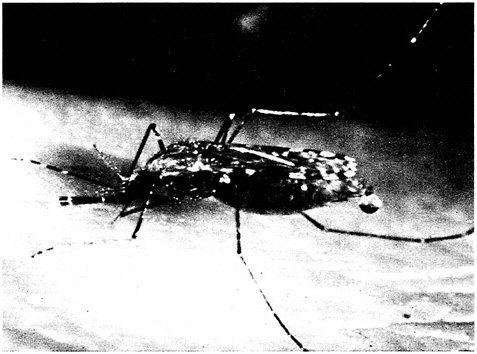
FIGURE 2-4 Female Anopheles gambiae during a blood meal. (Photo courtesy of Dr. Robert Gwadz, NIAID, NIH)
may deposit a total of 200 to 1,000 eggs in three or more batches. Actual egg production is dependent on blood consumption. After hatching, anopheline larvae lie along the water-air interface, where it is thought that they feed on organisms along the surface film. Adult mosquitoes develop from the pupal stage within 2 to 4 days. An adult mosquito will emerge from the egg stage in 7 to 20 days, depending on the species of mosquito and environmental conditions.
Female anopheline mosquitoes can survive at least a month under favorable conditions of high humidity and moderate temperatures. That is sufficient time for them to take a blood meal, for the parasite to develop, and for the mosquito to take another blood meal and thus transmit the parasite to a second human host.
Host-Seeking and Feeding Behavior
Mosquitoes are rarely found more than a few miles from their larval development site. They are readily blown short distances by the wind and have been transported internationally as unintended stowaways on airplanes.
Mosquitoes seek their host in response to a combination of chemical and physical stimuli, including carbon dioxide plumes, certain body odors, warmth, and movement.
Anopheline mosquitoes feed most frequently at night and occasionally in the evening, or in heavily shaded or dark areas during the early morning. During feeding, the mosquito injects a minute amount of salivary fluid into the host to increase blood flow to the area. Sporozoites are transmitted to the host in the salivary fluid.
Anopheles mosquitoes are readily distinguished from other genera by their characteristic stance, in which they appear to be standing on their heads. (Most mosquitoes hold their bodies relatively parallel to the surface on which they are resting.) After feeding, some engorged females seek out cool and humid areas of a house, such as walls and the undersides of furniture, while others find dark, secluded spots outdoors near the ground. Some mosquitoes have modified their resting behavior so as to avoid surfaces treated with pesticides.

FIGURE 2-5 Ideal larval development site for some anopheline mosquitoes. (Photo courtesy of Dr. Pedro Tauil, IOM Malaria Committee member)
THE ENVIRONMENT
Environmental conditions help determine the intensity of malaria transmission. The optimal climate for sporogony, or parasite development in the mosquito, is a temperature of between 20°C and 30°C with humidity in excess of 60 percent. Sporogony ceases at temperatures below 16° C. Temperature also has a significant effect on mosquito development, and consequently affects vector density. Indeed, development from egg to adult may occur in 7 days at 31°C (88°F) but takes about 20 days at 20°C (68°F).
Mosquitoes benefit from rainfall. Even large amounts that flush away mosquito larvae can produce pools of water that serve as future larval development sites. In areas of unstable malaria transmission, such conditions often bring about an explosion of anopheline mosquitoes and frequently contribute to epidemics.
Human modification to the environment also can create larval development sites and “man-made” malaria. For example, massive logging in West Africa has resulted in a proliferation in certain areas of sunlit pools of water, an ideal habitat for An. gambiae. Road building and other types of infrastructure projects, as well as agriculture and irrigation, are among a number of human activities that can spread malaria and other vector-borne diseases. In some regions, human activities can have the opposite effect. For example, deforestation in Thailand has led to the disappearance of malaria in some areas.
EPIDEMIOLOGY
Despite being spread over large regions of the world, malaria is a “focal” disease. That is, because of the complex interactions among the human host, mosquito vector, malaria parasite, and the local environment, malaria affects discrete population groups in different ways. This lack of uniformity is a major reason why it is so difficult to design effective and all-encompassing control strategies.
Geographic Distribution
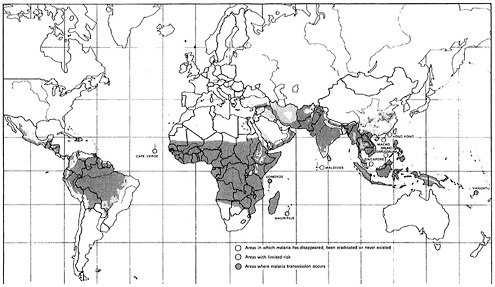
Malaria is primarily a disease of the tropics, but it is also found in many temperate regions of the world, including parts of the Middle East and Asia. Outbreaks are rare in temperate climates where eradication programs have been successful and in regions where environmental conditions are unfavorable for the anopheline mosquitoes, the malaria parasite, or both (Figure 2-6).
Of the four types of human malaria, that caused by P. vivax is the most widely distributed and the most common variety observed in temperate
regions of the world. Plasmodium falciparum, the most clinically dangerous of the malaria parasites, is most widespread in Africa south of the Sahara and throughout the world 's tropics. Plasmodium ovale is found almost exclusively in Africa. Plasmodium malariae has the same geographic range as P. falciparum, although it is much less prevalent and occurs in more restricted zones.
An estimated 2.8 billion people—nearly 60 percent of the world's population—live in areas free from malaria, either because the disease never existed there, because it disappeared as an unintended consequence of human activities, such as road building and urbanization, or because it was eliminated intentionally through eradication efforts. Another 1.7 billion, or slightly more than 30 percent of the population, live in areas where the malaria incidence declined because of eradication efforts but now is making a comeback. Malaria transmission has remained essentially unchanged for 9 percent of the world's inhabitants, about 445 million people. Most in this latter group live in Africa south of the Sahara.
The distribution of malaria within and between geographic regions is greatly influenced by the human population itself. Biological factors such as immune response and genetics, as well as socioeconomic status, living and working conditions, exposure to vectors, and human behavior, all play a critical role in determining a person's risk of infection and illness (Figure 2-7).

FIGURE 2-7 Lean-to housing provides ideal access for mosquitoes. (Photo courtesy of Dr. Pedro Tauil, IOM Malaria Committee member)
Transmission
Epidemiologists have devised a number of ways of classifying the type of malaria transmission in a particular area. Two of the most common are based on levels of endemicity and stability. In contrast to epidemic malaria, in which there is a sudden rise in the number of cases in a defined population, endemic malaria is characterized by a relatively constant and measurable incidence of cases over a number of years. Since there is great variation in the intensity of transmission between and within malaria-endemic regions, regions are categorized as follows:
-
Holoendemic: regions of intense year-round malaria transmission, where the population 's level of immunity is high, particularly among adults.
-
Hyperendemic: regions with seasonal transmission, where the population's level of immunity does not confer adequate protection from disease for all age groups.
-
Mesoendemic: regions that have some malaria transmission, although occasional epidemics constitute a heavy public health burden due to low levels of immunity.
-
Hypoendemic: regions of limited malaria transmission, where the population has little or no immunity to the parasite.
The level of endemicity in a region can be quantified by determining the percentage of children with enlarged spleens and malaria parasites in their blood (Table 2-1). Although widely used, spleen and parasite indices have various limitations. For one, they are poor indicators of morbidity and mortality, which are increasingly recognized to be important measures of the actual burden of disease. In areas where malaria is just one of a number of parasitic diseases, not all enlarged spleens are due to malaria infection. Finally, in holoendemic regions, blood parasite levels can be affected by both the use of antimalarial drugs and the age of the children being tested.
In a holoendemic area, where malaria transmission is intense, virtually everyone in the population is repeatedly infected. Babies are born with maternal protection to the malaria parasite and retain this passive immunity until about six months of age. As passive immunity wanes and as the infant becomes infected with malaria, the risk of severe disease increases. Indeed, malaria-induced morbidity and mortality in holoendemic regions is greatest in children between the ages of one and four. After repeated bouts of infection, children who survive gradually develop a partial immunity to malaria. Although they may have occasional episodes of illness, adults and children over five years of age rarely suffer severe malarial illness. By comparison, in regions of hyperendemic malaria, both children
TABLE 2-1 Classifications of Malaria Endemicity as Defined by Rates in Children Two to Nine Years Old
|
Classification |
Spleen Ratea (%) |
Parasite Rateb (%) |
|
Holoendemic |
>75 |
>75 (in infants) |
|
Hyperendemic |
51-75 |
51-75 |
|
Mesoendemic |
11-50 |
11-50 |
|
Hypoendemic |
0-10 |
<10 |
|
a Originally proposed at the WHO Malaria Conference in Equatorial Africa (1951) and subsequently amended by Molineaux (1988). b Metselaar and van Thiel (1959), as found in Molineaux (1988). |
||
and adults suffer severe disease. In meso- and hypoendemic regions, the frequency of infection is generally low, but epidemics may be devastating.
By definition, stable malaria transmission is intense, robust, and very difficult to interrupt. This type of disease transmission can occur where there are very low densities of mosquitoes, particularly anthropophilic and long-lived vectors such as An. gambiae and those with similar characteristics. In stable malaria transmission, the human population generally acquires a partial immunity to malaria, and morbidity and mortality are largely limited to young children and pregnant women. Conversely, unstable malaria occurs in regions of intermittent malaria transmission where there is little or no acquired population immunity and the risk of epidemic malaria is high. As a rule, as endemicity decreases, transmission becomes less stable and the risk of epidemics increases.
MALARIA CONTROL
Malaria control efforts traditionally have relied on the provision of proven antimalarial drugs, on environmental sanitation, and on the application of insecticides.
Drugs
Antimalarial drugs are used to prevent the onset of disease, to treat clinical cases in individuals, and to prevent disease transmission within populations. Some drugs, including doxycycline, proguanil, pyrimethamine, and primaquine, attack the liver stage, preventing the release of parasites into the bloodstream. Others, such as chloroquine, quinine, sulfadoxinepyrimethamine, and mefloquine, kill the parasite within red blood cells.
The emergence and spread of drug resistant strains of the most dangerous of the four human malaria parasites, P. falciparum, has reemphasized
concerns about the use and efficacy of other available antimalarial drugs. Chloroquine-resistant P. falciparum, first noted in Thailand and Colombia in the 1960s, has since spread to most areas of the world except the Middle East, Central America, and the Caribbean. An additional concern, however, is recent reports of chloroquine-resistant P. vivax. There is also widespread and increasing resistance to other antimalarial drugs.
Source Reduction
Eliminating larval development sites by modifying and manipulating the environment is particularly effective in areas where the spread of malaria has been aided by human activities, such as irrigation, public works, and construction projects. One common but expensive technique is to drain and fill in bodies of water.
Larviciding
There are chemical and biological methods for killing mosquitoes in the larval stage. Chemical larvicides include petroleum oils (Paris green) and pesticides such as temephos and fenthion. Biological methods employ larvivorous fish, such as Gambusia species (minnows) or Lebistes species (guppies), and Bacillus thuringiensis israeliensis, a toxin-producing bacterium.
Spraying
Any intervention that shortens the mosquito's life span should also reduce the likelihood of disease transmission. Residual insecticides applied to the interior of houses are very effective against some mosquitoes but have no effect on those that rest primarily outdoors. For these insects, localized outdoor spraying is sometimes warranted in densely populated areas or where the threat of a malaria epidemic is great. The arsenal of pesticides available includes chlorinated hydrocarbons (DDT, dieldrin), organophosphate compounds (malathion, fenitrothion), carbamates (propoxur), pyrethrins, and pyrethroids. Unfortunately, mosquitoes in many parts of the world have become resistant to some pesticides, and some have adapted so as to avoid insecticide-treated surfaces altogether.
Contact Reduction
Protective clothing, insect repellents, mosquito coils, and bednets can help reduce human-mosquito contact. Pyrethrin-impregnated bednets have been shown recently to reduce cases of clinical malaria in some areas by 50 percent or more, and further evaluations are ongoing.
Vaccines
Much recent research has focused on developing effective malaria vaccines (see Chapter 9). The effort has proved more difficult than anticipated, and it appears unlikely that effective vaccines for widespread use will be available during the next decade.
BIBLIOGRAPHY
The following reference materials are provided as suggested reading for those interested in a more comprehensive examination of the topics discussed in this chapter.
Bruce-Chwatt, L. J. 1985. Essential Malariology, 2nd ed. London: Heinemann.
Metselaar, D., and P. M. van Thiel. 1959. Classification of malaria. Tropical and Geographical Medicine 11:157-161.
Molineaux, L. 1988. The epidemiology of human malaria as an explanation of its distribution, including some implications for its control. Pp. 913-998 in Malaria: Principles and Practice of Malariology, Wernsdorfer, W. H., and I. McGregor, eds. Edinburgh: Churchill Livingstone.
Wernsdorfer, W. H., and I. McGregor, eds. 1988. Malaria: Principles and Practice of Malariology, 1st ed. New York: Churchill Livingstone.
World Health Organization, Division of Control of Tropical Diseases 1990. World malaria situation, 1988. Rapport Trimestriel de Sanitares Mondiales 43:68-79.