3
Overview
Through its direct impact on health and its indirect effects on such factors as economic development, migration, and military conflict, malaria has played and continues to play an important role in human history. The literature of ancient and modern civilizations contains repeated references to “intermittent” and “malignant” fevers and “agues” consistent with a diagnosis of malaria. As far back as 2700 B.C., the Chinese Canon of Medicine, the Nei Ching, discussed malaria-like symptoms and the relationship between fevers and enlarged spleens. Similarly, cuneiform tablets excavated from Assurbanapli's royal library in Nineveh (what is now Iraq) in the 6th century B.C. mention deadly malaria-like fevers that afflicted the populace of ancient Mesopotamia. The writings of Homer, Aristotle, Plato, Socrates, Horace, Tacitus, Carus, Varro, Chaucer, Pepys, and Shakespeare all mention fevers that were undoubtedly malaria related (Bruce-Chwatt, 1988).
The Greek physician Hippocrates was the first to make a connection between the proximity of stagnant bodies of water and the occurrence of fevers in the local population. The Romans also associated marshes with fever and pioneered early efforts at swamp drainage. Appropriately, the role of standing bodies of water and marshes in causing fevers was described by the Italians as “aria cattiva” (spoiled air) or “mal'aria” (bad air) beginning in the mid-sixteenth century, and the latter term entered the English language as “malaria ” some 200 years later. Like-
wise, the French coined the word “paludisme,” whose root means swamp, to refer to malaria.
Saint Augustine, the first archbishop of Canterbury, died from what was almost certainly malaria in 597 A.D. Dante Alighieri, the Italian poet, died of malignant fever in 1321 A.D. Peter the Great was so upset by the fever-related illness and death that plagued his Russian army in Persia in the early 1720s that he ordered them to stop eating melons, which he believed caused the sickness.
Kings, popes, and paupers alike have been stricken by this parasite-caused disease. Holy Roman Emperor Charles V died of malaria in a monastery in Yuste, Spain, in 1558. Pope Sixtus V died of “marsh fever” in 1590, as did his successor, Urban VII. During the Conclave of 1623, 8 cardinals and 30 scribes and secretaries died of malaria-induced fever, while other members in attendance fell ill (Celli, 1925). In England, King James I, King Charles II, and Cardinal Wolsey all suffered from intermittent fevers consistent with malaria.
PRE-COLUMBIAN HISTORY
Malaria may or may not have been present in the pre-Columbian New World. Some scholars argue that the disease was introduced to the Americas by people who migrated from malaria-endemic regions in Asia, across the now submerged land bridge, into North America. Early European visitors to South America noted the Indian use of cinchona bark, a natural source of quinine, to treat fevers, further supporting the view that malaria may have predated European expeditions to the New World. Whether or not European exploration and colonization of the Americas introduced malaria, they most certainly facilitated the spread of the disease.
MALARIA IN AMERICA
Malaria was one of the most widespread and debilitating diseases of early North America, significantly impeding the development of the colonies (Duffy, 1953). The English introduced two species of malaria, Plasmodium vivax and P. malariae, when they settled Jamestown, Virginia, in 1607, but it was the importation of African slaves beginning in 1620 that brought the more virulent P. falciparum to the continent (Russell, 1968). Indeed, it is thought that the decision in 1699 to move the capital from Jamestown to Williamsburg was motivated by the desire to escape the effects of malaria.
Boston was particularly hard hit by malaria-related illness and death in the seventeenth century. In 1699, Samuel Maverick of New York wrote, “The flux, agues, and fevers, have much rained both in cittie and country,
& many dead, but not yet soe many as last yeare. The like is all N.Engld. over, especially about Boston, where have dyed verry many” (quoted in Duffy, 1953). In 1723, George Hume, a Scottish settler in Virginia, wrote home to his family that “I am now & then troubled with ye fever & ague wch. is a very violent distemper here. This place is only good for doctors & ministers who have good encouragement here” (quoted in Duffy, 1953).
As the pioneers spread into the interior of the country, so did malaria. In the eighteenth and nineteenth centuries, malaria was endemic in the southern and western portions of the colonies. Most settlers in those regions considered it inevitable that they would contract the disease (Ackernecht, 1945). In New England, malaria was less of a problem, primarily because swamps and marshlands were being drained.
During the Civil War, 8,000 combatants died of malaria and there were more than 1.2 million recorded cases of the disease among Confederate and Union troops (Ognibene and Barrett, 1982; Bruce-Chwatt, 1988). As recently as the early 1900s, 500,000 cases of malaria were reported each year in the United States, the majority occurring in the South.
DISCOVERY OF QUININE
South American Indians used cinchona bark as a traditional remedy for malarial fevers long before any treatment was available in Europe. In 1639, Jesuit missionaries brought some of the bark back with them to Europe, where it eventually became the treatment of choice for fevers. It was not until 1820, however, that Pierre Joseph Pelletier and Joseph Bienaime Caventou, two French chemists, identified the alkaloid quinine as the bark's active ingredient (Russell, 1955). Shortly after this discovery, the demand for and use of quinine spread rapidly throughout Europe, North America, and Asia.
DISCOVERY OF THE MALARIA PARASITE AND ITS LIFE CYCLE
In 1846, the Italian physician Giovanni Rasori proposed that a parasite was responsible for the fever and other symptoms associated with the disease we now call malaria. In 1880, a French Army medical officer, Charles Louis Alphonse Laveran, observed live parasites in blood taken from a feverish soldier in Algeria.
Some of the greatest advances in understanding the complex life cycle of malaria parasites were made by the Italians around the turn of the century. In 1898, Giovanni Battista Grassi, Amico Bignami, and Guiseppe Bastianelli documented the transmission of human malaria parasites in
Anopheles claviger and soon after they described the developmental stages of P. falciparum and P. vivax, two of the most important malaria parasite species.
A bitter debate surrounded the discovery that malaria parasites are transmitted by anopheline mosquitoes. Both Grassi and his co-workers, as well as Sir Ronald Ross, a British military doctor working in India, were doing research on the problem at the same time and were influenced by another British scientist, Patrick Manson, who stimulated the working hypothesis that mosquitoes were responsible for malaria transmission. Using avian malaria as a model, Ross was the first to demonstrate the cycle of malaria in mosquitoes. But it was the Italians who definitively documented that only Anopheles mosquitoes can transmit human malaria, and a classic monograph by Grassi in 1900 details the complete development cycle of the parasite in these mosquitoes. In 1902, Ross was awarded the Nobel Prize in Medicine for his work on malaria.
MALARIA AND THE MILITARY
Malaria remains a disease of tremendous concern to the military. Its debilitating effects can often do more damage than the enemy. In a major outbreak during World War I, for example, more than 100,000 British and French troops on the Macedonian front were sidelined. Responding to a 1916 order to attack, an exasperated French general sent a telegram to Paris complaining, “Mon armee est immobilisee dans les hopitaux.” His army had malaria (Wenyon et al., 1921 quoted in Bruce-Chwatt, 1988).
In World War II, both Allied and Axis troops felt the effects of malaria. The U.S. Army alone recorded over 500,000 cases during the war; the Navy and Marine Corps recorded another 90,000 (Ognibene and Barrett, 1982; D. Robinette, Institute of Medicine, personal communication, 1991). “This will be a long war, if for every division I have facing the enemy, I must count on a second division in the hospital with malaria, and a third division convalescing from this debilitating disease,” said General Douglas MacArthur from the Pacific theater (Russell et al., 1946).
Malaria had a major impact on the American war effort in Vietnam, especially at the beginning of the conflict. In late 1965, nearly 10 percent of soldiers had the disease. “During that period, rates for certain units operating in the Ia Drang valley were as high as 600 per 1,000 per year, and at least two maneuver battalions were rendered ineffective by malaria,” General Spurgeon Neel reported in 1973 (Neel, 1973). Over 80,000 cases of malaria were diagnosed in American troops in Vietnam from 1965 to 1971. The overall mortality rate of 1.7 per 1,000 was low, however, because of rapid diagnosis and treatment of cases as they occurred (Canfield, 1972).
MALARIA CONTROL
Credit for the first efforts at malaria control properly belongs to the Greeks and Romans, who in the sixth century B.C. undertook major engineering projects to drain marshy areas. This practice continued well into the Middle Ages and spread throughout Europe and the Middle East. By and large, however, efforts to control malaria prior to the twentieth century met with minimal success. One of the most successful modern attempts at malaria control occurred under the leadership of General William C. Gorgas, who joined the U.S. Army Medical Corps in 1880, shortly after receiving his medical degree. During construction of the Panama Canal (1904-1914), Gorgas oversaw an integrated program of malaria control that included drainage, application of larvicide, and prophylactic treatment with quinine that resulted in the virtual elimination of malaria from the Canal Zone by 1910.
ERADICATION
Background
Starting in the mid-1940s and continuing through the mid-1950s, public health officials began to consider eradicating malaria from all parts of the world. Successful attempts to eradicate the Mediterranean fruit fly from Florida (1930-1931) and An. gambiae from Brazil (1934-1940) and Egypt (1948) made a large campaign against malaria seem feasible. The greatest impetus for malaria eradication came with the development of the powerful insecticide DDT during World War II.
Serious attempts to wipe out malaria in the United States began in 1943. That year, a proposal to eradicate the disease based on a strategy of indoor residual spraying with DDT was presented to the National Malaria Society by the U.S. Public Health Service (PHS) (Mountin, 1944). The result was the National Eradication Program, initiated in 1947 with $7 million in federal funds. Five years later, malaria morbidity and mortality in the United States had dropped to near zero and the program was abandoned (Bradley, 1966).
The years following World War II were unparalleled for the level of international cooperation devoted to combating endemic malaria. The United Nations Rehabilitation and Relief Administration, formed in 1943 as an international emergency organization with the United States as the principal financial backer, was very active in malaria control projects (Russell, 1968). The first Expert Committee on Malaria, established by the Interim Commission of the World Health Organization, met in 1947 (Najera, 1989); the World Health Organization (WHO) was officially formed in 1948.
One of the earliest broad-based proposals for eradication came in 1950 from the Pan American Sanitary Conference (PASC), which later merged with the Pan American Health Organization. In 1954, PASC declared a hemispheric eradication program and solicited support from the United Nations International Children's Emergency Fund (UNICEF), which led to an endorsement of the concept by a joint UNICEF/WHO Health Policy Committee (Soper, 1960). Worldwide malaria eradication seemed truly within reach when George MacDonald, of the Ross Institute in London, developed a mathematical model suggesting that malaria transmission could be interrupted simply by shortening the life span of the mosquito vector, thereby preventing the parasite from developing fully. This approach meant that the total number of mosquitoes could be ignored and justified a strategy of focused, residual insecticide spraying. Accordingly, domestic application of DDT emerged as the single most effective intervention tactic.
Eradication Campaign
In 1955, the Eighth World Health Assembly adopted a plan for worldwide malaria eradication, officially launching the initiative (World Health Organization, 1955). The effort was shadowed from the start by the fear that the vector mosquitoes would develop insecticide resistance before the disease could be wiped out. Historically, resistance developed within 5 to 10 years after an insecticide was in widespread use. Eradication, therefore, was recognized as a time-limited operation. Still, there was optimism. Medical entomologists believed in the efficacy of DDT and expected that their expertise would one day no longer be needed.
The eradication program that finally took shape would last about eight years: a preparatory phase of one year, an attack phase of at least four years, and a consolidation phase of three years. This would be followed by an indefinite maintenance phase (World Health Organization Expert Committee on Malaria, 1957). It was estimated that eradication, using DDT residual spraying, could be accomplished at a cost of 25 cents per person per year and that the cost for the first five years would total $519 million (International Development Advisory Board, 1956).
As the eradication program progressed, serious problems emerged. For one, planning activities often did not adequately address the attitudes of the local populations toward the disease. Often, regional differences in vector behavior, and the earmarking of local and national health resources for the task, were not taken into account (World Health Organization, 1969). In many areas, research could have provided better design strategies, but given the amount already committed to eradication, it was difficult to justify additional expenditures.
Although the eradication effort generated impressive results in North America and Europe, by the mid-1960s there was growing concern that
eradication was not technically or economically feasible in many areas (World Health Organization Expert Committee on Malaria, 1967). In fact, Africa south of the Sahara had been excluded from the eradication plan altogether because of the perceived magnitude of the region 's malaria problem and the lack of technological capability within those countries (Lepes, 1974). The number of malaria cases decreased dramatically in some regions, but most of these successes were recorded in less threatened temperate zones or on island nations, not in the continental tropical countries, where by the late 1960s malaria was still a serious health threat (Brown et al., 1976).
Research had almost no role in the initial years of the eradication effort. Indeed, there was little interest in involving scientists in a field many thought would soon be obsolete. It was only as the complexity of malaria became apparent that research assumed a more prominent place in eradication programs. Recognizing this, WHO in 1965 began to actively encourage malaria research. In 1969, the World Health Assembly passed a formal resolution to stimulate and intensify multidisciplinary malaria research.
The deemphasis of science combined with a decline in the number of malariologists left countries ill prepared for two major, interrelated changes in international health policy: the shift from malaria eradication to malaria control, and the move toward integration of health services.
Financial Support for Eradication
Many countries invested heavily in the eradication effort. In 1958, two powerful U.S. senators, Hubert H. Humphrey from Minnesota and John F. Kennedy from Massachusetts, attached legislation to the Mutual Securities Act that committed the United States for five years to the goal of worldwide malaria eradication (Spielman and Kitron, 1990). An annual appropriation of $23 million was provided, an enormous investment for the time. The United States spent $85 million in just three years (1957-1960), and the worldwide commitment to the project exceeded $100 million in 1960 alone (International Cooperation Administration Expert Panel on Malaria, 1961). WHO obligations to malaria eradication jumped from $768,000 in 1955 to almost $8 million in 1964 (Gramiccia and Beales, 1988). A number of countries also shifted funds within their own health budgets to accommodate the eradication goal. During the mid-1960s, for instance, India devoted 35 percent of its health dollars to malaria. The tremendous resources devoted to malaria eradication throughout the world meant that less could be spent on other important public health projects (Farid, 1980).
Eradication to Control
In 1969, the World Health Assembly revised its global malaria eradication strategy. The new approach emphasized strategies that could be justi-
fied on the basis of health grounds as well as economic considerations, and it encouraged control where eradication was not feasible (World Health Organization, 1969). The shift from malaria eradication to control necessitated a long-term commitment of personnel and financial resources and, unlike eradication, did not offer the potential for time-limited and dramatic results. Politicians were often reluctant to embrace the concept of control, which was not well understood.
The World Health Assembly also urged that malaria control strategies be integrated into the basic health services programs of each country. For some countries, where national malaria services had been run by a centralized organization and a single strategy, this proved to be particularly difficult. The result of this integration was a dramatic decrease in funding for malaria; money was shifted into programs for family planning, smallpox eradication, and multipurpose health services (Farid, 1980). By the early 1970s, changing priorities and responsibilities within the nations that had supported eradication caused a further erosion of support for malaria-related activities. The U.S. Agency for International Development (USAID), with the assistance of the PHS, contributed $375 million to 26 nations over a 20-year period (Howard, 1972). By 1974, the PHS had stopped funding eradication efforts in all but two countries, Nepal and Haiti (Smith, 1974). Similarly, UNICEF's contribution to eradication, which had risen to as much as $8.8 million in one year, began to be phased out by 1973 (Brown et al., 1976).
The combined withdrawal of international funding meant that the financial and technical responsibilities for malaria control would rest almost entirely within individual nations, many of which did not have adequate resources, technical expertise, or the administrative infrastructure to effectively carry out such programs. The situation was particularly serious for countries or regions that had made progress against malaria and for which a drop in technical and financial support would ultimately lead to a resurgence of the disease.
After the 1978 International Congress on Primary Health Care, the responsibility for malaria control in many countries was shifted further to those in the basic health services and to peripheral health workers. This integration was, for the most part, not smooth. Peripheral health workers were overburdened with other tasks and often lacked the technical competence to monitor and direct malaria control operations.
1970 to Present
As the international pool of funding for malaria eradication and control was drying up, a movement in the United States to halt the use of DDT was taking shape. In 1972, under pressure from environmental and conser-
vation groups, the United States banned use of the pesticide for all nonpublic health uses. By 1982, production of DDT in the United States had ceased altogether. The removal of this cheap and effective antimalaria weapon from the U.S. marketplace had a negative impact on malaria control efforts worldwide. Subsequent pesticides (e.g., malathion) have proved to be more expensive and more toxic.
Beginning in the early 1970s and continuing to the present, resistance to important antimalarial drugs has become increasingly prevalent. Particularly disturbing is the resistance to chloroquine, once the treatment of choice for P. falciparum malaria. The progressive spread of P. falciparum into areas where other species of the parasite once predominated adds an unfortunate complication to control efforts. Multidrug resistance has become such a problem in some parts of the world, such as Thailand, that malaria control personnel are hard pressed to institute any effective preventive or treatment regimen.
Political and social instability around the world have played a central role in malaria's comeback. From the decades-long civil war in Ethiopia, with its attendant cycles of famine and drought, to the devastation of Brazil's rain forest by urban resettlement, human impact on and interaction with the environment have facilitated the resurgence of the disease. Matters are made worse by the fact that there is a dwindling pool of technically competent malariologists, both nationally and internationally, equipped to manage the complexities of malaria research and control in the coming years.
On the positive side, important research discoveries, such as the development in 1975 of an in vitro culture system for the blood stage of P. falciparum, have facilitated scientific understanding of the malaria parasite (Trager and Jensen, 1976). A series of studies in the early and mid-1970s proved that humans could be protected for short periods of time from infection after being inoculated with irradiated sporozoites, lending considerable support to the notion that a vaccine against malaria is possible. Much of the early vaccine-related work in the United States has been supported by the USAID, which by the mid-1970s established a formal malaria vaccine research project. The agency continues to be the major source of U.S. malaria vaccine research funding. During this same period and continuing into the 1980s, a number of new antimalarial drugs, such as mefloquine and halofantrine, were discovered and developed, adding to the available chemotherapeutic options for treating and preventing the disease. The Special Programme for Research and Training in Tropical Diseases (TDR), founded in 1976 as a joint project of the United Nations Development Programme (UNDP), the World Bank, and WHO, has added both scientific direction and consistent financial and organizational support to worldwide activities in the area of malaria research and control.
U.S. AND INTERNATIONAL SUPPORT FOR MALARIA ACTIVITIES
A number of governmental and nongovernmental organizations around the world actively support malaria research, prevention, and control programs. No two programs are alike, and each operates within a specific policy framework that governs the choice and level of funding for malaria-related activities.
The United States is just one of many countries that support malaria research and control initiatives. Malaria-endemic countries also fund malaria-related projects, which, as one might expect, are geared overwhelmingly to controlling the spread of the disease within national borders.
In general, for industrialized countries, the national agencies in charge of scientific research have tended to focus on issues of domestic concern, while support for tropical diseases research and control has largely been left to government entities involved in foreign aid and international cooperation. For example, the Overseas Development Administration is the largest and most consistent government supporter of tropical disease research and control activities in the United Kingdom, while the Medical Research Council, the government's health research arm, concentrates primarily on issues of domestic concern.
Multilateral organizations, including the World Bank, the European Commission, and WHO support both malaria control and research activities. The WHO, which contributed almost 30 percent of its annual budget to malaria during the eradication years, currently allocates slightly over 4 percent of its total annual budget to malaria activities. This has amounted to almost $12 million per year for the 15 years 1973-1988. Some programs, like the TDR, predominantly support research and training activities. Out of a total 1990-1991 TDR budget of $73 million, approximately 21 percent or $15 million, is allocated to funding laboratory and field research on malaria (World Health Organization, 1991). A number of non-governmental entities, such as the Rockefeller Foundation, also contribute to both malaria control and research activities; others, like the MacArthur Foundation and the Wellcome Trust (United Kingdom), support both research and training.
Two studies on the funding of malaria activities were commissioned for this report, and both confronted similar problems in data collection and analysis (Ettling, 1990; Guha-Sapir and Hariga, 1991). While the absolute and relative funding allocated to a particular program is a prime indicator of an organization's priorities and interests, few governments or independent funding agencies tally their expenditures for malaria in the same way. Many, for instance, do not separate spending for particular diseases from spending for health in general. The problem of assessing relative contribu-
tions to malaria research and control is further compounded by the variability in the quality and accuracy of the data that are available. Even if accurate data were widely and easily available, they would likely fail to answer three critical questions: Was the amount spent insufficient, sufficient, or excessive? Was it spent well? Did it have an effect?
For all of the reasons discussed above, the committee decided that the danger of presenting somewhat erratic information outweighed any possible benefit. Because the data were easier to obtain and verify, and because U.S. government funding of malaria activities was of particular interest to the committee, the limited discussion that follows focuses on U.S. government funding of malaria.
United States
Four U.S. government agencies fund malaria activities: USAID, the Centers for Disease Control (CDC), the Department of Defense (DOD), and the National Institute of Allergy and Infectious Diseases (NIAID) of the National Institutes of Health (NIH).
U.S. Agency for International Development
Established in 1961 within the Department of State, USAID is the foreign assistance arm of the U.S. government. Highly decentralized, the various USAID offices and regional bureaus involved in malaria projects around the globe include the Office of Health in the Bureau of Science and Technology, and the Health, Nutrition, and Population Offices in the four regional bureaus for Africa, Asia, Latin America and the Caribbean, and the Near East. In addition to the bureaus, USAID has overseas “missions,” each supervised by a mission director, the U.S. country ambassador, and, in Washington, the respective regional bureau. Malaria projects are supported from one or more funding accounts, including the Health Account, Child Survival Fund, the Development Fund for Africa, the Economic Support Fund, Population Account, and the Agriculture, Rural Development, and Nutrition Account. In addition, USAID relies on an estimated 10,000 nongovernmental organizations, consultants, and contractors worldwide to help implement all of its projects.
In fiscal year (FY) 1989, USAID allocated $421 million to health, child survival, and AIDS activities, of which nearly $22 million (5.2 percent) was obligated to malaria research and control. This is fairly consistent with the pattern for each of the last seven fiscal years, during which the agency has allocated between 5 and 7 percent of its health budget to malaria-related activities (Table 3-1).
From 1985 through 1989, a little more than half of USAID malaria funds
TABLE 3-1 USAID Funding for Malaria Research and Control as a Percentage of Overall Obligations for Healtha
|
Funding ($000) |
|||||||
|
Category |
FY 85 |
FY 86 |
FY 87 |
FY 88 |
FY 89 |
FY 90 |
FY 91 |
|
Overall health |
354,433 |
332,733 |
304,887 |
309,517 |
421,278 |
341,326 |
363,219 |
|
Malaria |
25,524 |
17,595 |
21,243 |
20,117 |
21,793 |
16,309 |
27,978 |
|
Malaria as a percentage of overall health |
7.2 |
5.3 |
7.0 |
6.5 |
5.2 |
4.8 |
7.7 |
|
Note: Figures for FY 85 through FY 89 are actual obligations; those for FY 90 and FY 91 are projected obligations. The funding amounts reported here are calculated amounts, based on fiscal year obligations reported in the congressional presentation and on percentage attributions for malaria reported in the annual Health and Child Survival Questionnaires and in the USAID Activity Code/Special Interest System. a All funding accounts SOURCE: Center for International Health Information/ISTI, USAID HealthInformation System. |
|||||||
went to support bilateral programs, all of which targeted some aspect of malaria control. Of the bilateral programs funded in FY 1988 and FY 1989, just over a quarter included a small malaria research component as part of their overall control activities. From 1985 through 1989, nearly 48 percent of USAID malaria money was obligated to vaccine and immunity research (Figure 3-1). As a group, countries in Asia and the Near East receive the greatest share of USAID bilateral malaria funding; African nations received the smallest (Figure 3-2). The geographic allocation of funds is consistent with overall USAID funding, whereby the bulk of the resources are targeted to regions of particular U.S. strategic or political interest.
Centers for Disease Control
CDC is charged with protecting and monitoring the health of U.S. citizens. Over 7 million U.S. citizens travel abroad each year to malarious regions, according to CDC. Over each of the past several years, there have been more than 1,000 cases of malaria reported in the United States, most in U.S. nationals and nearly all acquired overseas.
From FY 1985 through FY 1989, CDC spent approximately $5.5 million for malaria surveillance activities and laboratory investigations (Table 3-2). In addition to its own resources, CDC receives funds from USAID for other malaria-related activities, including vaccine and immunity research, child survival projects, and other malaria research and control activities in malaria-endemic countries. CDC has also received funds from WHO on an intermittent basis (Figure 3-3).
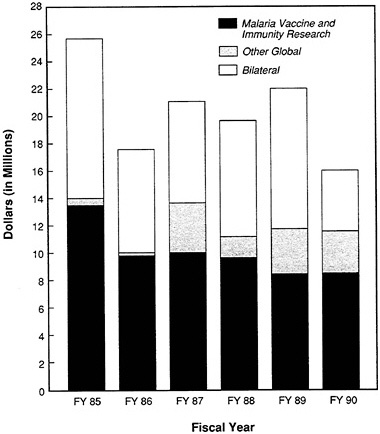
FIGURE 3-1 USAID malaria funding, all accounts (FY 1985 to FY 1990). Note: “Other Global” refers to those projects funded from all accounts, including the Vector Biology and Control Project, Diagnostic Technology for Community Health, Primary Health Care Operations Research, Maternal/Neonatal Health and Nutrition, and Communication for Child Survival, to name but a few. Data source: Center for International Health Information/ISTI, USAID Health Information System.
Department of Defense
DOD's interest in malaria stems from its commitment to protect the health of U.S. military personnel. Malaria exacted a heavy toll on U.S. troops during World War I, World War II, and both the Korean and Vietnam conflicts.
In 1982, Congress directed the United States Army Medical Research and Development Command (USAMRDC) at Fort Detrick, Maryland, to oversee all research on infectious diseases, including malaria, for the military. The Walter Reed Army Institute of Research (WRAIR), part of USAMRDC, and the Naval Medical Research Institute both have active
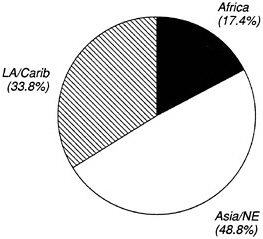
FIGURE 3-2 USAID bilateral malaria program funding (FY 1985 to FY 1989). Note: Over the period 1985-1989, the following countries and areas received funds for malaria activities: Africa (Burkina Faso, Cameroon, Ghana, Kenya, Liberia, Malawi, Mali, Niger, Nigeria, Senegal, Togo, Uganda, Zaire, Zimbabwe); Asia/Near East Region (Afghanistan, Burma, Egypt, India, Morocco, Nepal, Pakistan [received bulk of the funds for this region], South Pacific Region, Sri Lanka, Yemen); and Latin America Region (Belize, Bolivia, Costa Rica, Dominican Republic, Eastern Caribbean Region, Ecuador, Guatemala, Haiti, Honduras, Jamaica, Peru). Source: Center for International Health Information/ISTI, USAID Health Information System.
malaria research programs. In fact, WRAIR is home to the largest antimalarial drug screening program in the world.
The DOD malaria research programs concentrate on vaccine and drug development and, to a lesser extent, vector control. DOD has established field laboratories in Thailand, Kenya, Brazil, Peru, Indonesia, and the Philippines, all of which are involved in the study of malaria and other tropical diseases and are partially supported by malaria vaccine research funds.
Over the four years spanning 1986 through 1989, DOD allocated almost $38 million to malaria activities, including malaria vaccine development, drug development, and vector biology research and control. While funds for vector research and control have held fairly constant over the six years from 1985 to 1990, malaria vaccine funding was reduced by 26 percent between 1988 and 1989, and funds allocated for drug development have been decreasing steadily since 1985 (Table 3-3).
National Institute of Allergy and Infectious Diseases
NIAID is one of 13 institutes at NIH, the medical research branch of the PHS. Like other NIH institutes, NIAID supports both intramural and
TABLE 3-2 CDC Malaria Spending as a Percentage of Total Budget
|
Spending ($000) |
||||||
|
Category |
FY 85 |
FY 86 |
FY 87 |
FY 88 |
FY 89 |
FY 90 |
|
Malariaa |
1,330 |
1,758 |
1,938 |
2,157 |
1,985 |
2,508 |
|
Total budget |
410,000 |
452,000 |
587,000 |
772,000 |
982,000 |
1,121,000 |
|
Malaria as a percentage of total budget |
0.32 |
0.39 |
0.33 |
0.28 |
0.20 |
0.22 |
|
a Includes funds received from USAID and WHO. SOURCES: Office of Financial Management, Division of Parasitic Diseases,and the International Health Program Office, CDC. |
||||||
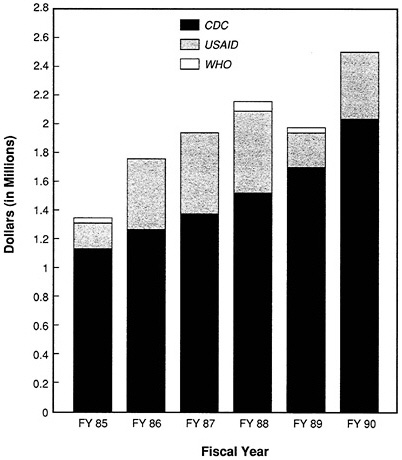
FIGURE 3-3 CDC spending on malaria, by account (FY 1985 to FY 1990). Sources: Division of Parasitic Diseases, Center for Infectious Diseases, and International Health Program Office, CDC.
TABLE 3-3 DOD Malaria Program Funding
|
Funding ($000) |
|||||
|
Category |
FY 86 |
FY 87 |
FY 88 |
FY 89 |
FY 90 |
|
Vaccines |
|||||
|
Technical base |
|||||
|
Army-in-house |
1,352 |
1,252 |
1,210 |
914 |
785 |
|
Army-field sites |
822 |
950 |
738 |
703 |
817 |
|
Navy-in-house |
1,138 |
706 |
1,147 |
996 |
809 |
|
Navy-field sites |
220 |
142 |
193 |
245 |
286 |
|
Extramural |
452 |
457 |
435 |
402 |
425 |
|
Advanced development |
|||||
|
In-house |
587 |
1,321 |
1,164 |
270 |
330 |
|
Extramural |
458 |
834 |
923 |
0 |
0 |
|
Total vaccine funding |
5,029 |
5,662 |
5,810 |
3,530 |
3,452 |
|
Drugs |
2,400 |
2,200 |
2,000 |
1,900 |
1,700 |
|
Vectors |
|||||
|
Research |
|||||
|
In-house |
210 |
220 |
230 |
240 |
250 |
|
Overseas |
320 |
340 |
360 |
380 |
400 |
|
Control |
281 |
189 |
231 |
253 |
212 |
|
Total vector funding |
811 |
749 |
821 |
873 |
862 |
|
Total malaria program |
8,240 |
8,611 |
8,631 |
6,303 |
6,014 |
|
Percent vaccines |
61.0 |
65.8 |
67.3 |
56.0 |
57.4 |
|
Percent drugs |
29.1 |
25.5 |
23.2 |
30.1 |
28.3 |
|
Percent vectors |
9.8 |
8.7 |
9.5 |
13.9 |
14.3 |
|
SOURCES: USAMRDC and U.S. Army Biomedical Research and DevelopmentLaboratory, Fort Detrick; Division of Experimental Therapeutics andDepartment of Entomology, WRAIR. |
|||||
extramural researchers in the basic and clinical sciences and is the only federal entity that actively supports basic research on tropical diseases.
Consistent with overall NIAID and NIH funding patterns, about 20 percent of all tropical disease research monies are spent in-house, with most of the remainder going to U.S. investigators outside NIH through a competitive grants award system. Grants from NIAID to foreign investigators for tropical disease research are relatively rare. Out of a total FY 1989 budget of $831 million, NIAID allocated $8.3 million (1 percent) to malaria (Table 3-4). While funding for tropical diseases as a proportion of the overall NIAID budget has declined over the past four years (largely because of the rapid influx of AIDS research funding), funding for malaria as a proportion of tropical diseases has increased. The bulk of NIAID extramural malaria research support during FY 1987 through FY 1989 went to studies on vaccines and immunity, while research on parasite biology received the next largest share of funds (Figure 3-4).
Overall, the U.S. government has invested nearly $140 million on malaria research and control activities over the past four years (Table 3-5). More than half of that amount was spent by USAID.
TABLE 3-4 NIAID Funding for Tropical Diseases and Malaria, 1986-1990
|
Funding ($000) |
||||
|
Category |
FY 87 |
FY 88 |
FY 89 |
FY 90 |
|
NIAID |
545,433 |
638,521 |
740,239 |
831,181 |
|
Tropical diseasesa |
34,118 |
34,440 |
32,633 |
38,765 |
|
Malaria |
6,122 |
6,803 |
7,467 |
8,337 |
|
Tropical diseases as a percentage of NIAID |
6.3 |
5.4 |
4.4 |
4.7 |
|
Malaria as a percentage of tropical diseases |
17.9 |
19.8 |
22.9 |
21.5 |
|
a This category includes the six tropical diseases (malaria, schistosomiasis, filariasis, trypanosomiasis, leishmaniasis, and leprosy) selected for special emphasis by the UNDP/World Bank/TDR, and training and career development in tropical diseases. SOURCES: U.S. Department of Health and Human Services, NIH, “NIAID Combined Intramural and Extramural Tropical Medicine Activities,” FY 87, FY 88, FY 89, FY 90 (mimeographs). |
||||
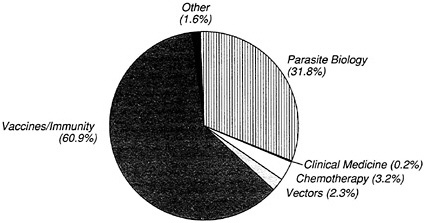
FIGURE 3-4 NIAID extramural malaria funding, by research area (FY 1987 to FY 1989). Source: Office of Tropical Medicine and International Research, NIAID.
TABLE 3-5 Overall U.S. Government Support of Malaria Activities
|
Funding ($000) |
||||||
|
Agency |
FY 87 |
FY 88 |
FY 89 |
FY 90 |
Total |
% |
|
USAID |
21,243 |
20,117 |
21,793 |
16,309 |
79,462 |
57.01 |
|
NIAID |
6,122 |
6,803 |
7,467 |
8,337 |
28,729 |
20.61 |
|
DOD |
7,862 |
7,810 |
5,430 |
5,152 |
26,254 |
18.84 |
|
CDC |
1,105 |
1,151 |
1,214 |
1,471 |
4,941 |
3.54 |
|
Total |
36,332 |
35,881 |
35,904 |
31,269 |
139,386 |
|
|
100.00 |
||||||
|
SOURCE: Compiled using information from other tables in this report. |
||||||
REFERENCES
Ackerknecht, E. H. 1945. Malaria in the Upper Mississippi Valley, 1760-1900. Baltimore: Johns Hopkins Press.
Bradley, G. H. 1966. A review of malaria control and eradication in the United States. Mosquito News 26:462-470.
Brown, A. W. A., J. Haworth, and A. R. Zahar. 1976. Malaria eradication and control from a global standpoint. Journal of Medical Entomology 13:1-25.
Bruce-Chwatt, L.J. 1988. History of malaria from prehistory to eradication. Pp. 1-59 in Malaria: Principles and Practice of Malariology, Wernsdorfer, W. H., and I. McGregor, eds. Edinburgh: Churchill Livingstone.
Canfield, C. J. 1972. Malaria in U.S. military personnel 1965-1971. Proceedings of the Helminthological Society of Washington 39:15-18.
Celli, A. 1925. Storia della malaria nell'agro romano. Academia dei Lincei, Roma.
Duffy, J. 1953. Epidemics in Colonial America. Baton Rouge: Louisiana State University Press.
Ettling, M. B. 1990. Financing of Anti-Malaria Activities in Selected Countries. A paper commissioned by the Committee on Malaria Prevention and Control of the Institute of Medicine, Washington, D.C.
Farid, M. A. 1980. The Malaria Programme—from euphoria to anarchy. World Health Forum 1:8-33.
Gramiccia, G., and P. F. Beales. 1988. The recent history of malaria control and eradication. Pp. 1335-1378 in Malaria: Principles and Practice of Malariology, Wernsdorfer, W. H., and I. MacGregor, eds. Edinburgh: Churchill Livingstone.
Guha-Sapir, D., and F. Hariga. 1991. The Funding of Malaria Research: Where It Goes and Why. A paper commissioned by the Committee on Malaria Prevention and Control of the Institute of Medicine, Washington, D.C.
Howard, L. M. 1972. Basic research priorities from the perspective of national malaria programs in developing countries. Proceedings of the Helminthological Society of Washington 39:10-18.
International Cooperation Administration Expert Panel on Malaria. 1961. Report and recommendations on malaria: a summary. American Journal of Tropical Medicine and Hygiene 10:451-502.
International Development Advisory Board. 1956. Malaria Eradication: Report and Recommendations of the International Development Advisory Board. April 13, 1956.
Lepes, T. 1974. Present status of the Global Malaria Eradication Programme and prospects for the future. Journal of Tropical Medicine and Hygiene 77:47-53.
Mountin, J. W. A. 1944. A program for the eradication of malaria from continental America Journal of the National Malaria Society 3:69-73.
Najera, J. A. 1989. Malaria and the work of the WHO. Bulletin of the World Health Organization 67(3):229-243.
Neel, S. 1973. Medical Support of the U.S. Army in Vietnam, 1965-70. Vietnam Studies. Washington, D.C.: Office of the Surgeon General and Center for Military History, U.S. Army.
Ognibene, A. J., and O. Barrett, eds. 1982. Internal Medicine in Vietnam. Vol. 2.
Washington, D.C.: Office of the Surgeon General and Center for Military History, U.S. Army.
Russell, P. F. 1955. Man's Mastery of Malaria. London: Oxford University Press.
Russell, P. F. 1968. The United States and malaria: debits and credits. Bulletin of the New York Academy of Medicine 44:623-653.
Russell, P. F., C. S. West, and R. D. Manwell. 1946. Practical Malariology. Philadelphia: W.B. Saunders Company.
Smith, E. A. 1974. AID policy on malaria. From a paper presented at the Forty-second Annual Conference of the California Mosquito Control Association, Inc., and the Thirtieth Annual Meeting of the American Mosquito Control Association, Inc., February 24-27, 1974.
Soper, F. L. 1960. The epidemiology of a disappearing disease: malaria. American Journal of Tropical Medicine and Hygiene 9:357-366.
Spielman, A., and U. Kitron. 1990. Rationale and Conceptual Framework for Malaria Eradication: A Historical Overview with an Emphasis on Time-Limitation and the Role of Research A paper commissioned by the Committee on Malaria Prevention and Control of the Institute of Medicine, Washington, D.C.
Trager, W., and J. B. Jensen. 1976. Human malaria parasites in continuous culture. Science 193:673-675.
World Health Organization. 1955. WHA8.30 Malaria Eradication, from the Ninth Plenary Meeting, May 26, 1955. WHO Official Records No. 63, pp. 31-32. Geneva: World Health Organization.
World Health Organization. 1969. Re-examination of the Global Strategy of Malaria Eradication. A report by the Director-General to the 22nd World Health Assembly, May 30, 1969. Annex 13, Part I. WHO Official Records No. 176.
World Health Organization. 1991. Tropical Diseases, Progress in Research 1990-91. Tenth Programme Report of the UNDP/World Bank/WHO Special Programme for Research and Training in Tropical Diseases (TDR). Geneva: World Health Organization.
World Health Organization Expert Committee on Malaria. 1957. Sixth Report. World Health Organization Technical Report Series No. 123. Geneva: World Health Organization.
World Health Organization Expert Committee on Malaria. 1967. Thirteenth Report. WHO Technical Report Series, No. 357. Geneva: World Health Organization.



















