4
U.S. Funding for the PEPFAR Initiative
The President’s Emergency Plan for AIDS Relief (PEPFAR) is the largest global health initiative focused on a single disease ever undertaken, and the United States is the single largest donor to global HIV/AIDS efforts in the world (Donnelly, 2012c; OGAC, 2009d).The committee reviewed PEPFAR funding because it represents one of the most direct measures of the U.S. government’s (USG’s) investment to address the global AIDS pandemic and, as such, is an important metric by which to understand and assess the program’s impact. It also represents a critical input for answering the questions pertaining to PEPFAR’s effects that were considered in the evaluation of programmatic areas using the program impact pathway framework described in Chapter 2. The distribution of PEPFAR funding over time can provide insight into HIV prevention, treatment, and care programs as well as into additional broader goals, such as country ownership, sustainability, and the strengthening of health systems.
To describe the investments that the USG has made through PEPFAR and to assess the relationship between these investments and program’s effects, the committee examined, to the extent possible, the level of funding over time and how the funds were budgeted and distributed. Unfortunately, because of limitations in the available financial data that are described more fully in this chapter, it was not feasible to make all of the assessments that the committee set out to make. In particular, it was difficult to describe the distribution of the annual direct expenditure of PEPFAR in partner
countries, to comprehensively match accounting budget codes to programmatic activities, and to fully follow the types of partners that ultimately receive funding and implement PEPFAR-supported activities. Nonetheless, the funding data that were available did allow for the insights and observations that were important information for the evaluation, and these finding are presented in this chapter.
As described in Chapter 2, the committee focused most of its data collection and its assessment on the 31 countries that were writing Country Operational Plans (COPs) when the IOM evaluation study process began in 2009.1 As such, in some cases the committee’s examination of PEPFAR funding in this chapter is limited to this subset of 31 countries. These countries represented 96 percent of PEPFAR planned funding in FY 2011 (OGAC, 2011d).2 In addition, although the committee reviewed data on PEPFAR funding over time to contribute to this evaluation, the committee was not charged to conduct a financial audit of PEPFAR; that function is performed by the Offices of Inspectors General at the USG agencies responsible for the implementation of PEPFAR programs and activities, including the Department of State (DoS), the Department of Health and Human Services (HHS), and the U.S. Agency for International Development (USAID).
This chapter begins with a brief discussion of the broader global funding environment for HIV/AIDS within which PEPFAR operates as a reflection of the context in which PEPFAR contributes to the HIV response in partner countries. This is followed by an overview of the USG budget and PEPFAR funding processes and a presentation of PEPFAR financial data describing the amount and distribution of funding over time as well as the characteristics of the partner countries that have been recipients of PEPFAR funding. The chapter then presents a brief discussion of the strategic use of PEPFAR resources. The chapter also discusses some questions of interest to the committee that could not be addressed because of limited availability of quality data.
__________________
1 The 31 PEPFAR countries submitting Country Operational Plans at the time were the original 15 focus countries (Botswana, Republic of Côte d’Ivoire, Federal Democratic Republic of Ethiopia, Cooperative Republic of Guyana, Republic of Haiti, Republic of Kenya, Republic of Mozambique, Republic of Namibia, Federal Republic of Nigeria, Republic of Rwanda, Republic of South Africa, United Republic of Tanzania, Republic of Uganda, Socialist Republic of Vietnam, and Republic of Zambia) plus the following additional countries: Republic of Angola, Kingdom of Cambodia, People’s Republic of China, Democratic Republic of the Congo, Dominican Republic, Republic of Ghana, Republic of India, Republic of Indonesia, Kingdom of Lesotho, Republic of Malawi, Russian Federation, Republic of the Sudan, Kingdom of Swaziland, Kingdom of Thailand, the Ukraine, and the Republic of Zimbabwe.
2 Planned/approved funding as reported in the FY 2011 PEPFAR Operational Plan. The committee’s sources for this and other types of funding information will be explained throughout the chapter.
The primary focus of this chapter is on funding processes within PEPFAR. The committee recognizes that in the response to HIV in PEPFAR partner countries there is an inherent interconnectedness among PEPFAR, partner countries, and other donors. This is touched upon briefly in this chapter, but the primary discussion can be found in the section on financing in Chapter 9, which discusses health systems strengthening, and in Chapter 10, which discusses progress toward a sustainable response in partner countries.
PEPFAR’S CONTRIBUTION RELATIVE TO OTHER DONORS
In most countries PEPFAR is situated within a broader landscape of global funding for HIV/AIDS, which includes partner country governments; other donor governments; the Global Fund to Fight AIDS, Tuberculosis, and Malaria (the Global Fund); the World Bank; and other multilateral institutions.3 The committee sought data on other sources of funding for HIV/AIDS in order to understand the context in which PEPFAR is implemented and to contribute to an assessment of the USG’s relative HIV/AIDS investment. Unfortunately, few data were available to examine the financial contribution of partner countries to national HIV/AIDS responses. The committee reviewed data from National Health Accounts and National AIDS Spending Assessments for the 31 countries that are the focus of this evaluation, but it was unable to address partner country contribution because data are unavailable for many countries and years. Thus, the data presented here focus on the contribution of PEPFAR only in the context of external donor assistance for HIV/AIDS. Chapter 9 provides a more thorough discussion of domestic financing for national HIV/AIDS responses and the implications of these data limitations.
To contextualize PEPFAR’s financial contribution within the broader external donor funding landscape, the committee examined disbursement data on official development assistance for HIV/AIDS, as reported to the Organisation for Economic Co-operation and Development Creditor Reporting System. For the 31 countries in the committee’s analysis, total donor disbursements for HIV/AIDS were $21.8 billion from 2004 to 2010 (OECD, 2012b).4 As shown in Figure 4-1, total disbursements for HIV/AIDS increased each year, from $1.3 billion in 2004 to $4.7 billion in 2010. Disbursements increased over time from all types of donors, including USG
__________________
3 Multilateral institutions are “international institutions with governmental membership” (OECD, 2012a). In the context of development assistance, multilateral institutions pool donor contributions and disburse funding at their own discretion.
4 This 7-year period of time captures donor funding from the beginning of PEPFAR implementation to the most recent year available.
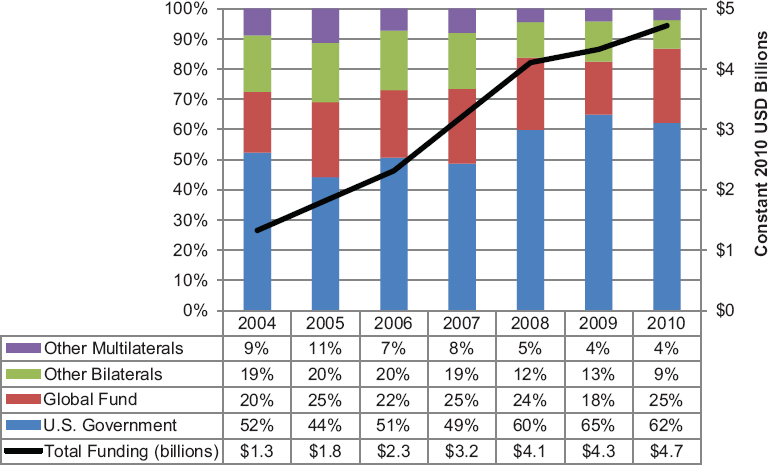
FIGURE 4-1 Total donor disbursements for HIV/AIDS in PEPFAR partner countries (constant 2010 USD billions).
NOTE: Figure presents disbursements for the 31 PEPFAR countries that were writing COPs when the IOM evaluation study process began in 2009. Disbursements represent the sum of two OECD sector codes: STD (sexually transmitted disease) control, including HIV/AIDS, and social mitigation of HIV/AIDS. Funding from the U.S. government and other bilaterals represents only bilateral funding (funding from a donor government to a partner country) and not contributions to the Global Fund.
SOURCE: OECD, 2012b.
bilateral funding for PEPFAR, the Global Fund, other bilateral government donors, and other multilateral organizations.5 The largest proportion of donor funding over this period was provided by the USG through bilateral funding for PEPFAR, followed by the Global Fund, for which the USG is the largest contributor (Goosby et al., 2012). During this time period, the proportion of donor funding from other bilateral donors and multilateral organizations decreased, while the proportions from the USG and the Global Fund increased.
As these data indicate, the USG’s bilateral investments implemented through PEPFAR constitute the largest external source of funding in the response to the HIV epidemic across these 31 countries, providing almost two-thirds of the external funding for HIV in 2010. Although these descriptive data do not demonstrate a causal relationship between funding and impacts on the epidemic, it is reasonable to conclude from the magnitude of PEPFAR’s investment and the proportion of HIV funding that it represents
__________________
5 Bilateral funding is provided to an aid-recipient country directly from a donor country (OECD, 2012a).
that PEPFAR funding did contribute to changes in the trajectory of the HIV epidemic and in HIV-related outcomes. Using the approach of the program impact pathway described in Chapter 2, this evaluation report presents the committee’s assessment of the effects of the activities and programs supported with these funds.
PEPFAR funding has represented a historic contribution in countries with few resources and a great need for support in their response to HIV. The dominance of one external donor, however, also brings with it the possibility that this one donor will drive the agenda and that the response in countries will be vulnerable to changes in that one donor’s investment or policies. These issues are discussed throughout this report, and, in particular, the role of donor funding in supporting the response to HIV in partner countries, along with the additional factors of national investments, health systems financing, and implications for future sustainable management of the HIV pandemic, are discussed in Chapters 9 and 10.
OVERVIEW OF THE PEPFAR FUNDING PROCESS
Through review of publicly available documents and interviews with the Office of the U.S. Global AIDS Coordinator (OGAC) and other USG stakeholders, the committee developed a framework to represent the flow of PEPFAR funding and how it is ultimately used for the implementation of programs in partner countries. Figure 4-2 represents a simplified overview of this flow (NCV-1-USG; NCV-11-USG) (IOM and NRC, 2010).6 In most respects, it mirrors the administrative and programmatic structure of PEPFAR as described in Chapter 3. The rest of this section expands on the subcomponents represented in Figure 4-2, describing the processes for the major steps within the framework. Box 4-1 provides definitions for key terms used in this chapter as part of the description of the U.S. federal budget process and PEPFAR’s budgeting, planning, and programming.
__________________
6 Country Visit Exit Synthesis Key: Country # + ES Country Visit Interview Citation Key: Country # + Interview # + Organization Type Non-Country Visit Interview Citation Key: “NCV” + Interview # + Organization Type Organization Types: United States: USG = U.S. Government; USNGO = U.S. Nongovernmental Organization; USPS = U.S. Private Sector; USACA = U.S. Academia; Partner Country: PCGOV = Partner Country Government; PCNGO = Partner Country NGO; PCPS = Partner Country Private Sector; PCACA = Partner Country Academia; Other: CCM = Country Coordinating Mechanism; ML = Multilateral Organization; OBL = Other (non-U.S. and non-Partner Country) Bilateral; OGOV = Other Government; ONGO = Other Country NGO.
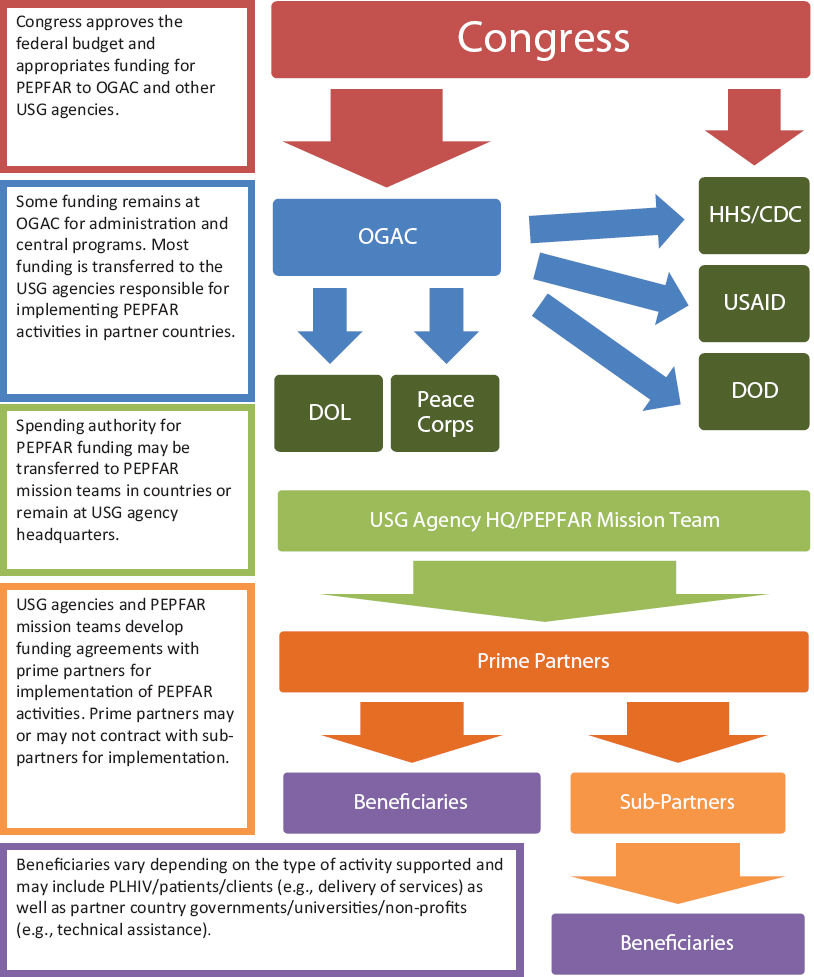
FIGURE 4-2 PEPFAR overall funding flows framework.
NOTE: CDC = U.S. Centers for Disease Control and Prevention; DoD = U.S. Department of Defense; DoL = U.S. Department of Labor; HHS = U.S. Department of Health and Human Services; HQ = headquarters; OGAC= Office of the U.S. Global AIDS Coordinator; PLHIV = people living with HIV/AIDS; USAID = U.S. Agency for International Development; USG = U.S. government.
SOURCE: Developed by the committee after document review and consultations with OGAC.
BOX 4-1
Definitions for Selected Financial Terms
Appropriations:“An appropriations measure provides budget authority to an agency for specified purposes. Budget authority allows federal agencies to incur obligations and authorizes payments to be made out of the Treasury” (Heniff, 2008, p. 2).
Authorization: “An authorizing measure can establish, continue, or modify an agency or program for a fixed or indefinite period of time” and “authorizes the enactment of appropriations for an agency or program” (Heniff, 2008, p. 2).
Obligations: Commitments of funding, such as placing an order or awarding a contract, made by USG agencies in order to implement and carry out programs, projects, and activities.
Outlays: Payments from the U.S. Treasury, usually in the form of cash or check, for goods or services.
Planned/Approved Funding: How OGAC and PEPFAR mission teams plan to obligate and outlay funds, documented in annual operational plans.
SOURCES: OGAC, 2011d; OMB, 2011.
Congressional Authorization and Appropriations
The United States Leadership Against HIV/AIDS, Tuberculosis, and Malaria Act of 2003 (the Leadership Act)7 authorized up to $15 billion in funding, including funds for bilateral PEPFAR efforts and annual yearly contributions to the Global Fund, for fiscal years (FYs) 2004 through 2008.8 In 2008 the U.S. Congress reauthorized PEPFAR for an additional 5 years (FY 2009–FY 2013) for up to $48 billion: $39 billion for bilateral HIV/AIDS programs and contributions to the Global Fund and $9 billion for bilateral tuberculosis and malaria programs.9 These two pieces of legislation authorized Congress to appropriate up to a maximum level of funding in a 5-year period, but PEPFAR’s annual budget is still dependent on the annual federal budget process. Congress may appropriate less or more than
__________________
7 United States Leadership Against HIV/AIDS, Tuberculosis, and Malaria Act of 2003, P.L. 108-25, 108th Cong., 1st sess. (May 27, 2003).
8Ibid., ![]() 401(a).
401(a).
9 Tom Lantos and Henry J. Hyde United States Global Leadership Against HIV/AIDS, Tuberculosis, and Malaria Reauthorization Act of 2008, P.L. 110-293, 110th Cong., 2nd sess. (July 30, 2008).
what is authorized. Early each year, the President prepares a budget for the following year and submits it to the Congress. The Global AIDS Coordinator requests a certain level of funding for each recipient country, and these requests are included in the President’s budget proposal. Congress reviews the President’s budget proposals, determines the final revenue and spending plan for the country, and eventually passes appropriations measures that provide budget authority to USG agencies (Heniff, 2008; OMB, 2011). The annual amount of PEPFAR funding is decided during this budget process.
The red arrows in Figure 4-2 represent the appropriations process whereby Congress appropriates a specific level of funding for USG agencies to implement PEPFAR programs and activities. The greater part of PEPFAR funding is initially appropriated by Congress directly to OGAC at the Department of State, and then most is eventually transferred to the other USG agencies responsible for implementing programs in partner countries (represented by the blue arrows in Figure 4-2). USAID, HHS and the Centers for Disease Control and Prevention (CDC), and the Department of Defense (DoD) may also receive direct appropriations of PEPFAR funding through separate appropriations acts.
All PEPFAR funding, regardless of the agency to which it is appropriated or transferred, is planned and coordinated through an interagency process overseen and led by OGAC (NCV-1-USG; NCV-4-USACA). Each year the USG agencies responsible for implementing PEPFAR work together to develop the PEPFAR Operational Plan as well as country and regional operational plans that include descriptions of previous achievements, proposals for new and continued activities, and funding requests for implementation of these activities. These plans are based on the amount of money requested by OGAC in the President’s budget proposal, and operational plans must be approved by the Global AIDS Coordinator (NCV-1-USG; NCV-4-USACA). As described above, the ultimate amount of PEPFAR funding for each year is determined through the congressional budget and appropriations processes. The PEPFAR Operational Plan provides information about the planned distribution of congressionally appropriated funding to USG agencies for PEPFAR activities as well as details about how the funding that remains at OGAC is used for central programs, oversight, and administration. COPs provide further information about which USG agencies will receive funding for implementation of specific activities and the mechanisms for disbursing that funding to implementing partners. Together, these operational plans document summary budget information regarding the planned and approved use of PEPFAR funding, including which activities will be implemented by which agencies, as determined during the interagency planning process (OGAC, 2011d).
Stakeholders interviewed for this evaluation identified challenges to program planning and implementation as a result of this annual USG fund-
ing process. In particular, interviewees indicated that long-term planning is often difficult for U.S. mission teams, partner countries, and implementing partners because of uncertainty from year to year about whether they will receive funding and how much they will receive (NCV-4-USACA; NCV-9-USG; NCV-11-USG; 166-10-USNGO; 166-13-PCGOV; 935-2-USG; 935-8-PCGOV; 396-16-PCGOV; 240-33-USG). These challenges are considered further in Chapters 9 and 10, where health systems financing and achieving sustainable management of the response are discussed.
Obligations and Outlays
Once Congress has appropriated funding for a given year and the headquarters and country-level planning processes are complete, PEPFAR funding is available to be obligated and outlaid for program implementation. Obligations are commitments of funding, such as awarding a contract, made by USG agencies in order to implement and carry out programs, projects, and activities (OMB, 2011). Outlays are the actual payments made from the U.S. Treasury (OMB, 2011). USG agencies obligate and outlay PEPFAR funding to prime partners. Prime partners may be nonprofit organizations, academic institutions, for-profit firms, multilateral organizations, partner country governments, or USG agencies. PEPFAR funding is obligated when a USG agency enters into a legally binding agreement (also known as an implementing mechanism) such as a contract, grant, or cooperative agreement with a prime partner. PEPFAR funding is outlaid when the U.S. Treasury actually makes a payment to a prime partner. Prime partners implement PEPFAR activities either directly or through subpartners.
Historically, most PEPFAR funding appropriated to OGAC has been “no-year” money that will never “expire”; that is, funding appropriated in any given fiscal year could be obligated or outlaid in that year or any year that follows (OGAC, 2008c). This type of funding remains available until expended and provides OGAC with some flexibility (Sessions, 2006). In FY 2012, a 5-year limit was put in place for the obligation of this funding (Donnelly, 2012b; OGAC, 2013a).10 Funding that is directly appropriated to other USG agencies, including USAID, HHS, and DoD, may be subject to different periods of availability as determined by the relevant appropriations acts (OGAC, 2010e).
__________________
10 Department of State, Foreign Operations, and Related Programs Appropriations Act, 2012, P.L. 112-74, 112th Cong., 1st sess. (December 23, 2011), 392.
PEPFAR FUNDING LEVELS AND DISTRIBUTION BY PROGRAMS AND PARTNERS
To understand the level of investment and the allocation and distribution of PEPFAR resources, the committee collected data from multiple available sources on appropriations, which reflect congressional intent; obligations, which represent programmatic intent; and outlays, which represent the disbursement of funding for implementation. The following sections present the committee’s findings, to the extent that data were available, at each level within the overall framework for the flow of PEPFAR funding (Figure 4-2). Although the committee was interested in understanding the flow of funding through all levels, data were only available to the level of distribution of funds to prime partners, as discussed in more detail below.
Because the committee was charged with evaluating PEPFAR since its inception, FY 2004 was used as the baseline for assessing the financial data, and the following section presents financial data through the last complete year of data available during the timeframe of the evaluation, typically FY 2011. It is important to note that although FY 2004 was the first year of funding for PEPFAR, it was not the first year of USG funding for global HIV/AIDS efforts. Rather, USG assistance for global HIV/AIDS efforts began in 1986, with an initial investment of $1 million. By 2000, annual funding had grown to just more than $360 million, and it reached about $1.5 billion in 2003 (Kates and Summers, 2004). Compared to this prior funding, PEPFAR represented a major scale-up and expansion of U.S. support, authorizing up to $15 billion for bilateral programs over its first 5-year period and creating a new position in the DoS for the coordination of the USG global HIV/AIDS response.11 What follows is a presentation of financial data for FYs 2004 through 2011 (where available).
Congressional Appropriations
Appropriations reflect the level of congressional commitment for PEPFAR programs. From 2004 to 2011, more than $38 billion (current USD) was appropriated to USG agencies for PEPFAR programs and the Global Fund (OGAC, 2011a). During PEPFAR I (FY 2004–FY 2008), actual congressional appropriations surpassed the $15 billion authorized in the Leadership Act. Total congressional appropriations over the 5-year period were $18.3 billion for bilateral HIV/AIDS programs and contributions to the Global Fund (excluding funding for tuberculosis and malaria) (OGAC, 2009a). In the first 3 years of PEPFAR II, actual appropriations totaled $19.8 billion, just more than half of the $39 billion authorized
__________________
11Supra, at note 7, ![]() 102(a)(2), 22 U.S.C. 2651a(f).
102(a)(2), 22 U.S.C. 2651a(f).
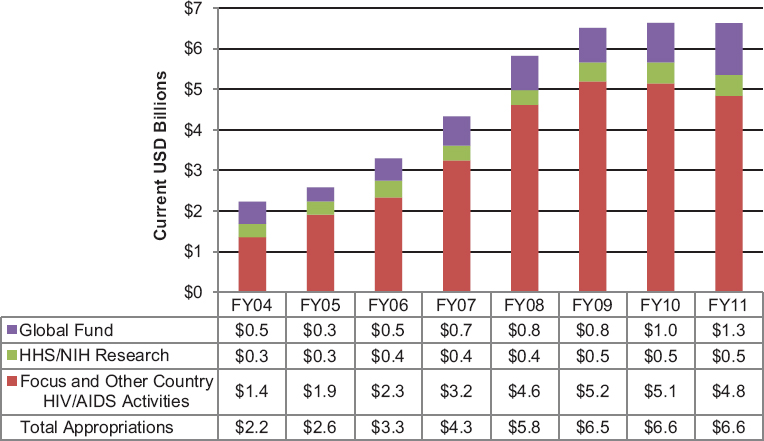
FIGURE 4-3 Congressional appropriations for PEPFAR, FY 2004–FY 2011 (current USD billions).
NOTE: Data represent total funding appropriated (made available) for all PEPFAR countries within each U.S. fiscal year (October 1–September 30) in current USD billions. HHS = U.S. Department of Health and Human Services; NIH = National Institutes of Health.
SOURCES: OGAC, 2004, 2006a, 2007a, 2008a, 2009a, 2010a,b, 2011a.
through FY 2013 (OGAC, 2011a). From FY 2004 to FY 2011, $28.6 billion, or the greater part of PEPFAR funding, was appropriated for support of PEPFAR country programs. Approximately $3.3 billion was appropriated for research at the U.S. National Institutes of Health (NIH), and $6.1 billion was appropriated for the Global Fund (OGAC, 2004, 2006a, 2007a, 2008a, 2009a, 2010a,b, 2011a). Figure 4-3 shows the annual appropriations for each of those categories from FY 2004 to FY 2011.
Cumulative Obligations and Outlays
To understand the level of PEPFAR investment intended by Congress that has been spent to support PEPFAR activities over time, the committee first assessed how appropriated funds have been obligated and outlaid over time. Figure 4-4 summarizes the cumulative funds made available, obligated, and outlaid for PEPFAR programs in all partner countries.
For the funds shown in Figure 4-4, Figure 4-5 provides more detail on the proportions that have been obligated and outlaid at the end of each fiscal year. As of the end of FY 2011, 72 percent of the total funding made available for PEPFAR through congressional appropriations had been outlaid, 17 percent had been obligated but not yet outlaid, and 11 percent had yet to be obligated or outlaid. The cumulative amount of available PEPFAR
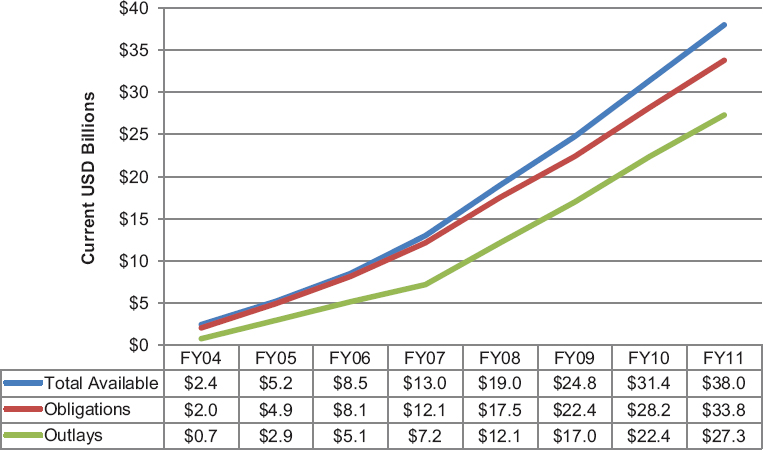
FIGURE 4-4 Cumulative obligations and outlays, FY 2004–FY 2011 (current USD billions).
NOTE: Outlays are a subset of obligations, which are a subset of total funding available.
SOURCES: OGAC, 2004, 2006a, 2007a, 2008a, 2009a, 2010a,b, 2011a.
funding not outlaid at the end of each fiscal year has increased from $1.7 billion at the end of FY 2004 to $10.7 billion at the end of FY 2011; during this time, the total amount of cumulative available funding increased from $2.2 billion to $38 billion (see Figure 4-4) (OGAC, 2004, 2006a, 2007a, 2008a, 2009a, 2010a,b, 2011a).
The cumulative increase in funds not outlaid is the result of funds made available in the current year and prior years that have yet to be expended; some cumulative increase in funds not outlaid is to be expected for large-scale development assistance programs. As a proportion of cumulative PEPFAR funding available at the end of each fiscal year, the amount of funding that has not been outlaid (the sum of the red and blue bars in Figure 4-5) has decreased from 69 percent at the end of FY 2004 to 28 percent at the end of FY 2011 (OGAC, 2004, 2011a).
These funds that have been appropriated and not yet spent are described as being in the “pipeline” (Donnelly, 2012b,c). In March 2012, OGAC reported $9 billion in the pipeline, $7.6 billion of which was “earmarked for programs or is within the acceptable range of 12 to 18 months worth of money in reserve for overseas development programs” (Donnelly, 2012c, p. 2). Global AIDS Coordinator Eric Goosby has explained that a 12- to 18-month funding reserve is reasonable because it allows services to continue in the case of a delay in congressional appropriations (Donnelly, 2012b). The remaining $1.46 billion has been described as a “bad pipeline”
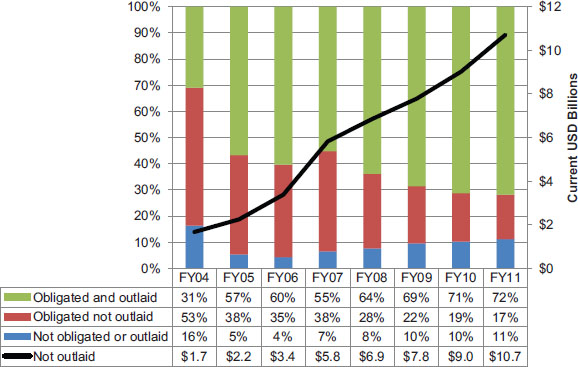
FIGURE 4-5 Proportion of cumulative available PEPFAR funding by obligation and outlay status at the end of each fiscal year (bars) and the cumulative total of funding that has not been outlaid (line) (current USD billions).
NOTE: The black line represents the cumulative amount of PEPFAR funding that has been appropriated but not outlaid; it is the sum of funding that has been obligated but not outlaid and funding that has not been obligated.
SOURCES: OGAC, 2004, 2006a, 2007a, 2008a, 2009a, 2010a,b, 2011a.
by USG officials, which means it has remained unexpended for too long (Donnelly, 2012c). More than two-thirds of this $1.46 billion pipeline is the result of delayed spending in five countries: Kenya, Tanzania, Ethiopia, Mozambique, and Zambia (Donnelly, 2012c).
Since 2011, OGAC has reviewed country and central budgets to identify unspent funds and has taken “corrective action to make sure the pipeline is considered” before allocating future funding to country programs (Donnelly, 2012b, p. 2). The USG currently plans to remove funding in the “bad pipeline” from country ledgers (Donnelly, 2012c) and reinvest these funds in other areas such as commodities, systems and institutions, and program strengthening for greater impact—“three major areas in which PEPFAR already has large investments and a track record of success” (Donnelly, 2012a, p. 1).
There are several factors related to partner countries, USG contracting processes, and implementing partners that may contribute to the increasing size of the pipeline. Ambassador Goosby attributed the unspent $1.46 billion to “inefficient bureaucracies; major reductions in the cost of AIDS treatment; delays due to long negotiations on realigning programs with
recipient country priorities; and a slowdown in a few countries because the AIDS problem was much smaller than originally estimated” (Donnelly, 2012c, p. 2). At the partner country level in Kenya, for example, the large backlog of unspent funds is partially the result of inefficiencies due to “its two ministries of health, which were set up as part of a negotiated settlement following post-election violence in 2008” (Donnelly, 2012c, p. 2).
During interviews conducted by the IOM committee, interviewees from PEPFAR mission teams and implementing partners identified challenges or barriers to obligating and outlaying money in a manner that would facilitate a steady and timely funding flow. Bottlenecks may result from delays in disbursements and contracting at many steps in the PEPFAR funding flow process (including the release of funding from Congress to OGAC, the transfer of funding from OGAC to implementing agencies, and USG contracting), which may lead to gaps between partner contracts in countries (196-23-PCGOV; 196-24-PCNGO; 196-ES; 331-17-USG; 331-18-USNGO; 331-ES; 934-29-USNGO; 934-35-PCNGO; 116-24-USG; 935-20-PCNGO; 587-14-PCGOV; 587-23-USG; 166-17-USG; 396-9-PCGOV; 240-12-USG; 240-29-USNGO; 461-13-USACA). According to one interviewee:
“One of our biggest challenges is receiving our money in time. I think that one becomes a major challenge on our side. You know you make a plan and you are actually like four or five months behind. I’ll give you a typical example now. [. . .] We are in July; we are coming to the end of July. Fiscal year for PEPFAR for this grant started first April. I have no funds.” (461-13-USACA)12
There can also be longer-than-projected timelines for project initiation, for example, the time for prime partners or umbrella grant managers to identify and contract with grantees and subpartners (196-9-USNGO; 240-ES; 331-17-USNGO; 166-17-USG; 636-16-USG; 396-41-PCGOV). As one interviewee said:
“The sub-grantees process, for a prime partner like [them], is a challenge, even though it’s a headache they have always had. From a management perspective, the process is very good, but it is also cumbersome and has too many delays. They often need to build capacity of organizations before the organizations are able to respond to [. . .] service or activity subcontracts. Prime partners need easier and more flexible mechanisms for easier roll-out of funds to organizations or sub-grantees.” (331-18-USNGO)
__________________
12 Single quotations denote an interviewee’s perspective with wording extracted from transcribed notes written during the interview. Double quotations denote an exact quote from an interviewee either confirmed by listening to the audio-recording of the interview or extracted from a full transcript of the audio-recording.
In addition, challenges with capacity can limit the rate at which local implementing partners can spend funding (240-21-PCGOV; 240-ES; 240-3-USG; 934-29-USNGO; 116-12-PCNGO; 116-24-USNGO; 196-9-USNGO). These issues are discussed in more detail in Chapter 9. Short-term contracts or other funding agreements for only 1-or 2-year terms with implementing partners can compound the difficulties associated with delays in disbursement and capacity challenges and lead to other challenges with planning for long-term implementation (116-24-USG; 166-10-USNGO; 166-ES; 240-26-PCNGO; 240-29-USNGO; 240-ES; 396-6-PCGOV; 396-16-PCGOV; 396-41-PCGOV; 396-8-PCNGO; 935-20-PCNGO).
More broadly, at the country program level an independent and external audit of PEPFAR funding for FY 2007 and FY 2008 revealed that, because of the timeline for development and review of country operational plans, OGAC generally distributed PEPFAR funds to implementing agencies in April—7 months after the start of the fiscal year (DoS OIG, 2010). Additionally, PEPFAR’s reauthorizing legislation instituted new congressional requirements that must be met prior to disbursement of funding and, for FY 2010 funding, the need to meet these requirements has delayed outlays across the program (Kates et al., 2011).
Annual Expenditures
In addition to the cumulative outlay of funding over time, the committee was also interested in understanding how much money was actually spent by PEPFAR within each year, regardless of the year in which the money was appropriated or obligated. To achieve this, the ideal approach would have been to access the best possible estimate of the actual financial input toward activities in each year, with a breakdown by country, by partner, and by programmatic area; this corresponds to the first step in the program impact pathway framework described in Chapter 2. However, it is difficult to follow the funding actually spent in a given year because PEPFAR mission teams can simultaneously spend funding that was originally made available in multiple prior fiscal years (NCV-1-USG) and the financial data are reported as cumulative expenditures that do not readily reflect annual expenditures.
In an attempt to overcome this challenge, the committee requested the available reported financial data and worked with OGAC to determine an appropriate methodology for converting these reported data into annual expenditures. This is described in brief here; the request for these data and the methods used are described in more detail in Appendix C.
OGAC provided data that had been reported as cumulative expenditures for each fiscal year, from 2004 to 2011. These data were captured in a total of 78 Excel spreadsheets containing financial data for six agencies: DoD, the Department of Labor, HHS, the Peace Corps, USAID, and the
Department of State, which included five bureaus that reported their data directly (Bureau of African Affairs; Bureau of East Asian and Pacific Affairs; OGAC; Bureau of Population, Refugees, and Migration; and Bureau of Western Hemisphere Affairs). These spreadsheets included data by country for every reporting year that each agency or bureau had participated in the PEPFAR program; for most agencies this represented 8 years of data (FY 2004–FY 2011). The totals recorded available, obligated, and outlaid funds by budget year (when the funds were made available) and reporting year (cumulative funding by that year). The data sent from each agency and bureau were organized so that each year’s report contained data from its first year in the program until the year of the report. For example, the report for 2006 would contain the budget totals for each country for FY 2004, FY 2005, and FY 2006 on that sheet.
To convert these data into annual expenditures required two major steps. First, the data were harmonized across all 78 spreadsheets into a single dataset to ensure that the data could be used together to comprehensively represent PEPFAR spending across agencies, in total and by country. Second, cumulative expenditures were converted into annual expenditures. To get the annual expenditure for within a given fiscal year, all prior year outlays were subtracted from the cumulative total outlays reported for that year.
One challenge that emerged with these data was that there were many discrepancies identified when the countries’ available totals were compiled and compared from their inception year to the following year across annual reports up until 2011. In particular, the major discrepancies came when the dollar amounts reported as available for a given budget year changed in subsequent reporting years (both increases and decreases were observed), although one would expect the amount made available in a budget year to be a fixed constant after that year. These discrepancies ranged in magnitude up to a maximum case of a $214 million difference between two reports for one budget year for one agency. As a result, it was difficult to determine the correct figures for the total amounts made available. Overall, the number of discrepancies and the magnitude of the changes from year to year decreased in later reporting years, and the reporting of the outlays did not exhibit the same degree of discrepancy. To have one consistent source for the calculations of annual expenditures and to base the calculations on the most recent data available, the FY 2011 reports were used as the source of data for all of the fiscal years.
Table 4-1 presents the total annual expenditure across PEPFAR agencies, disaggregated by the budget year in which those funds were originally made available. For example, in FY 2011 a total of $3.3 billion was expended; of this, $8 million had been made available originally in FY 2004, $18 million had been made available in FY 2005, and so forth. PEPFAR’s
| Reporting Year | ||||||||
| Budget Year | FY 2004 | FY 2005 | FY 2006 | FY 2007 | FY 2008 | FY 2009 | FY 2010 | FY 2011 |
| FY 2004 | <$0.1a | $231.0 | $10.9 | $536.8 | –$2.3b | $5.9 | $16.5 | $8.3 |
| FY 2005 | $151.2 | $234.1 | $805.9 | $53.3 | $28.2 | $19.7 | $18.3 | |
| FY 2006 | $124.8 | $907.7 | $409.4 | $86.4 | $109.9 | $26.2 | ||
| FY 2007 | $224.9 | $1,242.9 | $688.6 | $447.7 | $36.9 | |||
| FY 2008 | $246.4 | $1,649.9 | $1,436.1 | $451.2 | ||||
| FY 2009 | $181.6 | $1,700.4 | $1,484.3 | |||||
| FY 2010 | $275.5 | $1,100.5 | ||||||
| FY 2011 | $176.4 | |||||||
| Total outlays for reporting year | <$0.1 | $382.2 | $369.9 | $2,475.4 | $1,949.6 | $2,640.5 | $5,005.7 | $3,302.2 |
| Total outlays for FY 2004-FY 2011: | $15,125.6 | |||||||
NOTE: Funding presented in current USD millions.
aThe actual number corresponding to budget year and reporting year FY 2004 is $7,198 in dollars (not millions).
bThe combination of budget year FY 2004 and reporting year FY 2008 ends up negative as a result of changes to amounts in later-year reports.
SOURCE: Financial data provided by OGAC.
total actual expenditures through FY 2011 on programs in partner countries managed by and reported through these agencies were $15 billion.
It is worth noting that these numbers do not match other publicly reported data sources on PEPFAR outlays; the total expended through FY 2011 as calculated from these data received from OGAC, $15 billion, is less than the total cumulative outlays shown in Figures 4-4 and 4-5, $27.3 billion, which is what is reported in OGAC’s publicly available FY 2011 summary financial status report (OGAC, 2011a). This difference is because the data provided for this analysis include only expenditures through activities allocated to country programs using funding made available to the individual agencies and reported to OGAC. It does not include funds being expended through central activities or through central management, such as funds for central Track 1.0 contracts, the Headquarters Operational Plan, international partnerships (Global Fund and UNAIDS contributions), and NIH Research (OGAC, 2013a).
Table 4-2 shows the annual expenditure disaggregated by subsets of countries, representing successively larger portions of the total geographic scope of PEPFAR funding. The original focus countries and the additional COP countries that are the focus of this evaluation represent most of the PEPFAR expenditures over time.
Although the committee recognizes the complexity and the burden of tracking expenditures across multiple USG agencies and hundreds of diverse implementing partners, the lack of accessible data on actual annual expenditures, regardless of the year in which the money was appropriated or obligated, represents a significant data gap for PEPFAR. Annual expenditures would be a direct measure of the actual, real-time investment of the USG in the programs and activities supported by PEPFAR. These data are not available in a readily accessible repository to external stakeholders or to PEPFAR itself. This is a major limitation for conducting a thorough assessment of the impact of the PEPFAR investment, through either descriptive or statistical analyses, that could incorporate a direct measure of the annual investment by country, by partner, and by programmatic area with annual data on variables such as overall mortality, HIV mortality, HIV prevalence, or antiretroviral therapy (ART) coverage, health outcomes, and other outcome and explanatory variables. Appendix C includes a more in-depth description of opportunities and limitations for analyses that the committee explored that could be feasible, valid, and informative; these could be considered in the future if reliable sources of data were available.
Planned/Approved Funding
Ideally, the committee would have liked to assess the distribution of PEPFAR outlays and annual expenditures among different types of pro-
| Reporting Year | |||||||||
| FY 2004 | FY 2005 | FY 2006 | FY 2007 | FY 2008 | FY 2009 | FY 2010 | FY 2011 | TOTAL | |
| Focus countries (15 total) | <$0.1c | $324.4 | $326.9 | $1,907.2 | $1,691.8 | $2,350.3 | $3,620.9 | $2,840.7 | $13,062.3 |
| COP countries as of 2009 (31 total)a | <$0.1c | $369.5 | $358.7 | $2,206.2 | $1,849.9 | $2,538.1 | $3,893.6 | $3,174.5 | $14,390.4 |
| All countries | <$0.1c | $375.3 | $363.1 | $2,336.8 | $1,906.8 | $2,605.5 | $3,969.4 | $3,244.2 | $14,801.1 |
| All countries and regionsb | <$0.1c | $382.2 | $369.9 | $2,475.4 | $1,949.6 | $2,640.5 | $4,005.7 | $3,302.2 | $15,125.6 |
| Total outlays for all countries and regions, FY 2004–FY 2011: | $15,125.6 | ||||||||
NOTE: Funding presented in current USD millions. Each row is inclusive of the preceding rows.
aThese 31 countries represent those defined as the primary focus of this evaluation (as described in Chapter 2). These figures include funding to non-focus countries in years prior to becoming COP countries.
bRegions refer to programs that support activities in countries but are managed/reported as multi-country regions.
cThe actual number corresponding to FY 2004 is $7,198 in dollars (not millions).
SOURCE: Financial data provided by OGAC.
grams and partners directly in terms of the inputs to the activities supported and who has implemented them. However, because these financial data are not available according to these parameters, the committee used the closest available approximation, which is the planned and approved PEPFAR funding documented through the operational plan budgeting process that was described previously. Each year, OGAC releases the PEPFAR Operational Plan, which provides more detail on how congressional appropriations will be used for program implementation. The PEPFAR Operational Plan includes summary budget information regarding the planned and approved use of PEPFAR funding, including which activities will be implemented by which agencies, as determined during the interagency planning process (OGAC, 2011d). Planned/approved funding reflects how OGAC and PEPFAR mission teams plan to obligate and outlay funds. The committee examined data on the distribution of planned/approved PEPFAR funding in order to understand how the program was intended to be implemented.
Planned/Approved Funding to USG Implementing Agencies
As described earlier, although the Congress appropriates the greater part of PEPFAR funding to the DoS, OGAC transfers most of this funding to other USG agencies for the implementation of programs, services, and activities. This interagency implementation approach was described in Chapter 3. USAID and CDC are the primary implementers of country programs, and the bulk of planned/approved funding is directed to these agencies through direct congressional appropriations or interagency transfers. For example, between FY 2005 and FY 2011, a total of 54 percent of PEPFAR funding was implemented through USAID, and 41 percent was implemented through CDC. Figure 4-6 shows the breakdown of planned/approved funding among the USG implementing agencies each year.
Planned/Approved Funding by PEPFAR Operational Plan Types of Programs
The PEPFAR Operational Plan also provides information on the planned/approved funding for different types of programs and activities that are classified by OGAC in the following categories: country activities, headquarters (HQ) programs (at OGAC and other USG agencies), and multilateral partners. Figure 4-7 displays the proportion of planned/approved funding for each type of program over time, and Figure 4-8 provides a 1-year snapshot from FY 2011 of the distribution of total planned/approved funding among the three broad types of programs, including subcategories. The next three sections will describe, in turn, the activities that fall within each of these three types of programs and provide a further
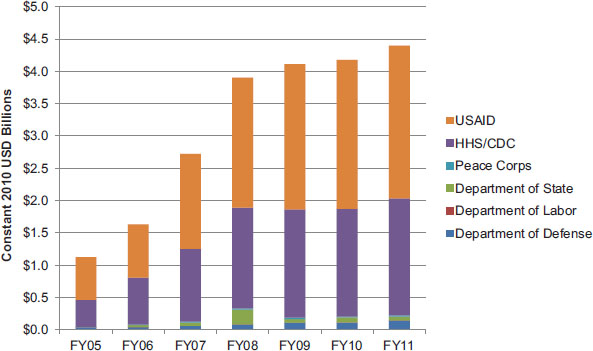
FIGURE 4-6 Planned/approved funding for USG implementing agencies, FY 2005–FY 2011 (constant 2010 USD billions).
SOURCES: OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d.
breakdown of the funding distribution over time by additional subcategories. Each of these types of programs can include activities across PEPFAR’s different programmatic and technical areas, which are discussed in more detail later in this chapter.
OGAC made some changes to how these categories are used to report planned/approved funding after the first phase of the program. To examine funding trends with as much consistency as possible, the committee used the FY 2011 categories to analyze all data; if necessary, programs and funding prior to FY 2011 were re-categorized to the FY 2011 categories.
Country activities Country activities include field programs, central programs, and other country programs. Funding for field programs represents the planned/approved funding for activities planned by mission teams in COPs or regional operational plans; other country programs is funding for programs in those countries that do not prepare COPs or regional operational plans. Central programs are funded and managed centrally by agency HQ yet implemented in partner countries (usually by large nongovernmental organizations, faith-based organizations, and academic institutions). Figure 4-9 shows the planned/approved funding over time for each of these
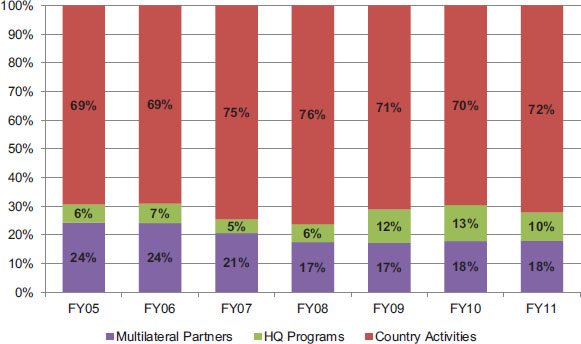
FIGURE 4-7 Proportion of planned/approved funding for PEPFAR operational plan programs, FY 2005–FY 2011.
NOTE: HQ = headquarters.
SOURCES: OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d.
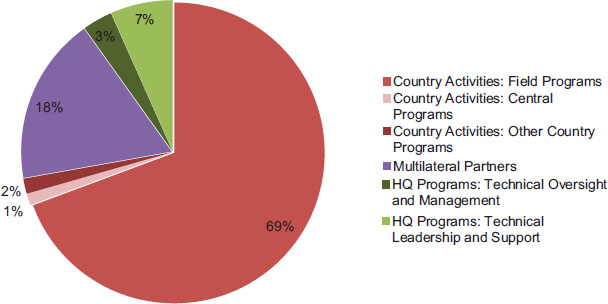
FIGURE 4-8 FY 2011 PEPFAR operational plan program funding summary.
NOTE: Data represent the planned/approved use of funding appropriated for PEPFAR in FY 2011.
HQ = headquarters.
SOURCE: OGAC, 2011d.
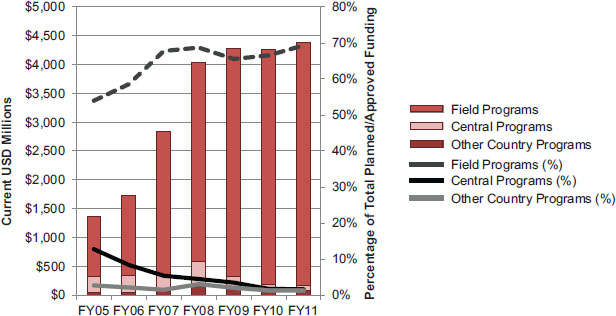
FIGURE 4-9 Planned/approved funding for PEPFAR country activities in current USD millions (left axis and bars) and as a percentage of total planned/approved funding (right axis and lines).
NOTE: Funding for field programs represents the planned/approved funding for activities planned in COPs or regional operational plans; other country programs include funding for those countries that do not prepare COPs or regional operational plans. Funding for central programs includes programs that are funded and managed by OGAC HQ yet implemented in partner countries (usually by large nongovernmental organizations, faith-based organizations, and academic institutions).
SOURCES: OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d.
subcategories of PEPFAR country activities as well as the proportion of total planned/approved funding that each subcategory represents.13
As a proportion of total funding, funding for all country activities has remained fairly steady throughout the period of PEPFAR at approximately 70 percent, peaking at 76 percent in FY 2008; most of this funding for country activities is accounted for by field programs (OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d). Most PEPFAR funding for country activities is approved for field and central programs within countries that prepare COPs. During much of the first phase of PEPFAR, this funding was limited to the 15 focus countries. By FY 2009, when the scope of this evaluation was established, 31 countries were preparing COPs, and by FY 2011, this had increased to 33 (GAO, 2011).
While programs implemented in partner countries have consistently represented the largest share of PEPFAR’s funding, the way in which pro-
__________________
13From FY 2005 to FY 2008, OGAC classified the following as central programs within country activities: New Partner Initiative, Supply Chain Management, Technical Leadership Support, and Twinning. In FY 2009, OGAC reclassified these as HQ programs. To maintain consistency and comparability over time, for all data presentations the committee included all funding for these four programs for all years as HQ programs (which are discussed in the next section).
grams in countries were funded has shifted. In the early years of PEPFAR, more funding was directed to central country programs. In 2005, for example, funding for central programs was 13 percent of planned/approved funding; by 2011 it had dropped to 2 percent (OGAC, 2005, 2011d). The decrease in funding for central programs may reflect increased national and local capacity and changing funding requirements for PEPFAR partners. When country programs were started, there was often no infrastructure, no mechanisms, and no processes that could be used to obligate large sums of money to entities within partner countries, including governments, for program and service implementation. In order to provide service delivery at the needed scale during PEPFAR I, a number of grants went to technical partners that were capable of supporting rapid scale-up of services in the focus countries; these were known as Track 1.0 partners. The Track 1.0 partners were centrally funded to implement antiretroviral therapy, orphans and vulnerable children programs, and prevention activities in multiple partner countries.
As PEPFAR programs in partner countries matured, systems were built and entities were strengthened to facilitate the obligation and outlay of PEPFAR funding to prime partners responsible for programs, projects, and activities within partner countries. As of FY 2009, Track 1.0 partners were required to transition their programs to national or local management (OGAC, 2009c). By FY 2011 only one central program remained (antiretroviral therapy), and funding for this program accounted for just 4 percent of all planned/approved funding (OGAC, 2011d).
HQ programs In FY 2011 funding for HQ programs included two components: technical oversight and management, and technical leadership and support. The category of technical oversight and management captures administrative costs for each of the USG agencies responsible for implementing PEPFAR, such as salary, benefits, travel, supplies, professional services, and equipment. The technical leadership and support category includes funding for technical assistance at all levels (e.g., USG agencies, implementing partners, and partner country governments), supply chain management, and HQ-level strategic information activities (e.g., public health evaluations and inspectors general activities) (OGAC, 2011d). Funding is also captured here for some large-scale capacity-building initiatives that are implemented in multiple countries and are classified as HQ programs. From FY 2005 to FY 2008, several technical leadership and support activities were considered central programs within country activities (described in the preceding section); where possible, the committee has retroactively classified these as HQ programs in order to examine funding trends consistently.
During PEPFAR I, funding for
HQ programs accounted for 6 percent of total planned/approved funding; from FY 2009 to FY 2011, funding for HQ programs increased to 11 percent of total planned/approved funding (see Figure 4-10). This increase is largely a reflection of greater funding for technical leadership and support, which has increased since FY 2007, peaking at 9.6 percent of total planned/approved funding in FY 2010. However, as a proportion of total planned/approved funding, technical oversight and management has remained fairly steady around 3 percent. The increase in funding for technical leadership and support reflects PEPFAR II’s greater emphasis on capacity building and the initiation of programs such as the New Partners Initiative (described further in Chapter 10), as well as the Medical Education Partnership Initiative, and the Nursing Education Partnership Initiative (described further in Chapter 9). Funding for these capacity-building initiatives reflects OGAC’s objective to transition “PEPFAR support from direct service provision to increased provision of technical assistance to governments” (OGAC, 2009b, p. 4).
Multilateral partners Since FY 2005, almost $6 billion has been planned for multilateral partners. Most funding in the category of multilateral support has been directed to the Global Fund, which channels international financing for efforts against AIDS, tuberculosis, and malaria. The Leader-
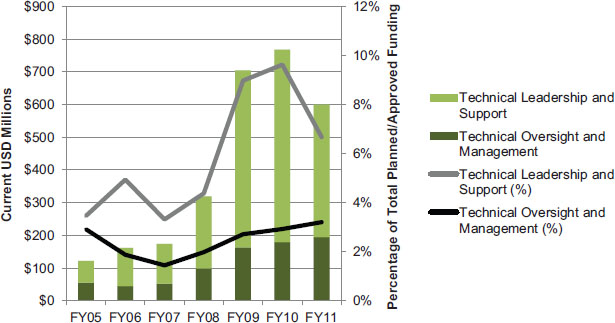
FIGURE 4-10 Planned/approved funding for PEPFAR HQ programs in current USD millions (left axis and bars) and as a percentage of total planned/approved funding (right axis and lines).
NOTE: Technical oversight and management captures administrative and management costs. Technical leadership and support includes funding for strategic information/evaluation activities, supply chain management, twinning, the New Partners Initiative/Local Capacity Initiative, the Medical Education Partnership Initiative, and the Nursing Education Partnership Initiative.
SOURCES: OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d.
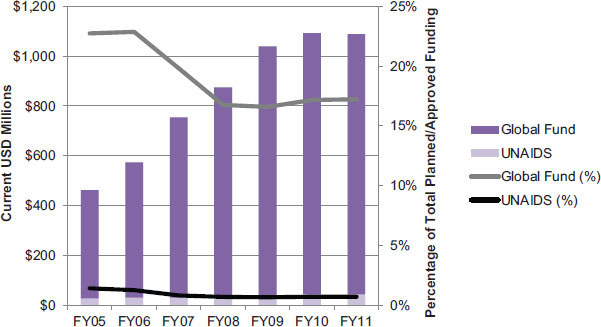
FIGURE 4-11 Planned/approved funding for multilateral partners in current USD millions (left axis and bars) and as a percentage of total planned/approved funding (right axis and lines).
NOTE: Global Fund = Global Fund to Fight AIDS, Tuberculosis, and Malaria; UNAIDS = Joint United Nations Program on HIV/AIDS. The World Health Organization also received $2 million in FY 2005, but this amount was too small to be displayed in this graph.
SOURCES: OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d.
ship Act and the Lantos-Hyde Act authorized the use of PEPFAR funds for the USG contribution to the Global Fund, provided that USG contributions not exceed 33 percent of total contributions to the Global Fund.14 Also represented in this category is funding for the Joint United Nations Program on HIV/AIDS (UNAIDS). The USG is one of the largest contributors to UNAIDS, a partnership of 10 United Nations agencies that leads the international response to HIV/AIDS through advocacy on behalf of those living with HIV/AIDS, technical support for country-led responses to HIV/AIDS, and monitoring global progress toward achieving universal access to HIV prevention, treatment, care and support (OGAC, n.d.; UNAIDS, 2010b). Funding for the Global Fund and UNAIDS increased each year between FY 2005 and FY 2010, when funding peaked at $1.05 billion and $43 million, respectively, and then dropped slightly in 2011 (see Figure 4-11). In FY 2005, OGAC also provided $2 million of multilateral support to the World Health Organization (WHO) to support efforts to coordinate and consolidate USG and WHO efforts to address tuberculosis in people living with HIV/AIDS (OGAC, 2005).
__________________
14Supra, at notes 4 and 7.
Planned/Approved Funding by Technical and Program Areas
The committee was also interested in understanding how PEPFAR funding is distributed among the different services and activities that PEPFAR supports. The PEPFAR operational plans report planned/approved funding for four technical areas that correspond with the primary categories of HIV/AIDS services and systems strengthening efforts: prevention, care, treatment, and other. These data, disaggregated by technical area, represent funding for country activities in countries that prepare COPs or regional operational plans, including the field and central programs described in the previous section. Figure 4-12a shows PEPFAR funding for these technical areas over time. Treatment and prevention have received the most funding over time.
Through FY 2009, treatment received the largest amount of funding, but in the past 2 years, funding for prevention has surpassed funding for treatment. Figure 4-12b displays the proportions of funding for these technical areas over time. During PEPFAR I, the highest proportion of funding was approved for treatment and prevention activities. During PEPFAR II, beginning in FY 2009, the proportion of funding for treatment activities declined, while the proportion of funding for prevention activities increased slightly. Funding for care activities remained relatively steady. The proportion of funding for other activities, which include health systems strengthening, laboratory infrastructure, and strategic information activities, increased over time; this was largely driven by a continuous increase in funding for health systems strengthening.
PEPFAR funding is planned through budget codes, which capture exclusive funding information about more specific activities within these categories. The technical areas shown here may contain funding from as many as eight budget codes, described in Box 4-2. The funding within these categories is presented and discussed in the subsequent chapters of this report, which assess PEPFAR’s efforts in specific technical and program areas.
In general, budget codes have been fairly uniform and stable, but there have been some specific changes over time. Since 2005, new budget codes have been added, and the definitions for some budget codes have been changed. Each fiscal year’s budget codes are unique to that year; OGAC and other USG programs do not go back and change how activities were coded when budget codes are changed or added. The budget codes provide one way of looking at PEPFAR-funded activities, but the interpretation of these trends is complex. For example, in FY 2010 a number of countries shifted funding from the treatment and laboratory infrastructure budget codes to health systems strengthening as a reflection of the increased emphasis on systems strengthening described in the reauthorization legislation and PEPFAR’s second Five-Year Strategy. In some cases these funding shifts
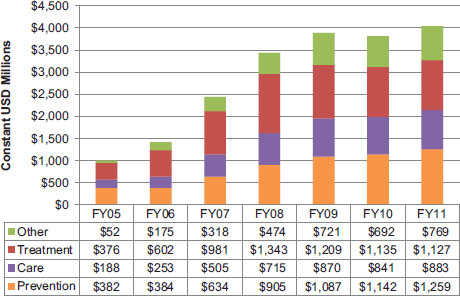
FIGURE 4-12a Planned/approved funding by technical area (constant 2010 USD millions). NOTE: The totals were calculated by retroactively categorizing budget codes as reported in FY 2011 to ensure consistency. The Other technical area includes health systems strengthening, laboratory infrastructure, and strategic information activities. Management and staffing costs were excluded from this analysis.
SOURCES: OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d.
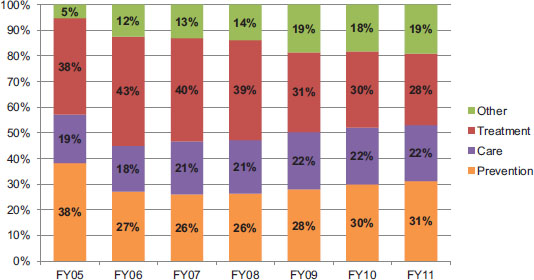
FIGURE 4-12b Proportion of planned/approved funding by technical area.
NOTE: The proportions above were calculated by retroactively categorizing budget codes as reported in FY 2011 to ensure consistency. The Other technical area includes health systems strengthening, laboratory infrastructure, and strategic information activities. Management and staffing costs were excluded from this analysis.
SOURCES: OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d.
were interpreted as decreased support for service delivery, but it is more likely that the same activities intended to strengthen the quality and delivery of treatment or laboratory services were simply re-categorized (NCV-1-USG) (OGAC, 2010c).
As a standard approach to managing these inconsistencies described above, in Figure 4-12 and in the planned/approved funding data presented throughout this report the committee examined funding for budget codes as defined and categorized in FY 2011. As a result of the changing definitions, shifts in the way funding was programmed, and variability in how country programs interpreted the budget codes, PEPFAR’s budget codes do not necessarily track funding consistently across countries and over time. This limited the committee’s ability to draw major conclusions about the distribution of PEPFAR funding beyond descriptive findings; the limitations in tracking funding over time will also be discussed, where relevant, when funding for specific budget codes are presented and discussed in the subsequent chapters of this report.
BOX 4-2
FY 2011 PEPFAR Budget Code Definitions by Technical Area
Prevention
Prevention of Mother-to-Child Transmission (PMTCT): activities (including training) aimed at preventing mother-to-child HIV transmission, including ARV [antiretroviral] prophylaxis for HIV-infected pregnant women and newborns and counseling and support for maternal nutrition. PMTCT-plus ART [antiretroviral therapy] activities should be described under ARV Drugs and Adult Treatment. Funding for HIV counseling and testing in the context of preventing mother-to-child transmission can be coded under PMTCT or Counseling and Testing; targets should be included in PMTCT. Early infant diagnosis should be included under Pediatric Care.
Abstinence and Be Faithful: activities (including training) to promote abstinence, including delay of sexual activity or secondary abstinence, fidelity, reducing multiple and concurrent partners, and related social and community norms that impact these behaviors. Activities should address programming for both adolescents and adults.
Other Sexual Prevention: other activities (including training) aimed at preventing HIV transmission including purchase and promotion of condoms, STI [sexually transmitted infection] management (if not in palliative care settings/context), messages/programs to reduce other risks of persons engaged in high-risk behaviors. Prevention services should be focused on target populations such as alcohol users; at risk youth; men who have sex with men (MSM); mobile populations, including migrant workers, truck drivers, and members of military and other uniformed services (e.g. police); and persons who exchange sex for money and/or other goods with multiple or concurrent sex partners, including persons engaged in prostitution and/or transactional sexual partnerships.
Blood Safety: activities supporting a nationally-coordinated blood program to ensure a safe and adequate blood supply including infrastructure and policies; donor-recruitment activities; blood collection, testing for transfusion-transmissible infections, component preparation, storage and distribution; appropriate clinical use of blood, transfusion procedures and hemovigilance; training and human resource development; monitoring and evaluation; and development of sustainable systems.
Injection Safety: policies, training, waste-management systems, advocacy and other activities to promote medical injection safety, including distribution/supply chain, cost and appropriate disposal of injection equipment and other related equipment and supplies.
Prevention Among Injecting and Non-Injecting Drug Users: activities including policy reform, training, message development, community mobilization and comprehensive approaches including medication assistance therapy to reduce injecting drug use. Procurement of methadone and other medical-assisted therapy drugs should be included under this program area budget code. Programs for prevention of sexual transmission within IDUs [people who inject drugs] should be included in this category. Please refer to the July 2010 Revised Guidance on Comprehensive HIV Prevention for People Who Inject Drugs for more information. [This budget code was adopted in FY 2009.]
Voluntary Medical Male Circumcision: policy, training, outreach, message development, service delivery, quality assurance, and equipment and commodities related to male circumcision. All MC [male circumcision] services should include the minimum package; HIV testing and counseling provided on site; age-appropriate pre- and post-operative sexual risk reduction counseling; active exclusion of symptomatic STIs and syndromic treatment when indicated; provision and promotion of correct and consistent use of condoms; circumcision surgery in accordance with national standards and international guidance; counseling on the need for abstinence from sexual activity during wound healing; wound care instructions; and post-operative clinical assessments and care. HIV counseling and testing associated with male circumcision can be included in either counseling and testing or male circumcision. [This budget code was adopted in FY 2009.]
Counseling and Testing: includes activities in which both HIV counseling and testing are provided for those who seek to know their HIV status (as in traditional VCT [voluntary counseling and testing]) or provider-initiated testing and counseling. Funding for testing and counseling in the context of preventing mother-to-child transmission can be included under PMTCT or Counseling and Testing; targets should be included in PMTCT.
Care
Adult Care and Support: all facility-based and home/community-based activities for HIV-infected adults and their families aimed at extending and optimizing quality of life for HIV-infected clients and their families throughout the continuum of illness through provision of clinical, psychological, spiritual, social, and prevention services. Clinical care should include prevention and treatment of OIs [opportunistic infections] (excluding TB [tuberculosis]) and other HIV/AIDS-related complications including malaria and diarrhea (providing access to commodities such as pharmaceuticals, insecticide-treated nets, safe water interventions and related laboratory services), pain and symptom relief, and nutritional assessment and support including food. Psychological and spiritual support may include group and individual counseling and culturally-appropriate end-of-life care and bereavement services. Social support may include vocational training, income-generating activities, social and legal protection, and training and support of caregivers. Prevention services may include “prevention for positives” behavioral counseling and counseling and testing of family members. The purchase of OI drugs (excluding TB drugs) should be included under Adult Care and Treatment. ARV treatment should be coded under Adult Treatment and ARV Drugs.
Pediatric Care and Support: all health facility-based care for HIV-exposed children aimed at extending and optimizing quality of life for HIV-infected clients and their families throughout the continuum of illness through provision of clinical, psychological, spiritual, social, and prevention services. Clinical care should include early infant diagnosis, prevention and treatment of OIs (excluding TB) and other HIV/AIDS-related complications including malaria and diarrhea (providing access to commodities such as pharmaceuticals, insecticide treated nets, safe water interventions and related laboratory services), pain and symptom relief, and nutritional assessment and support including targeted food interventions. Other services—psychological, social, spiritual, and prevention services—should be provided as appropriate. Pediatric care and support services should be counted if they are provided at a facility; community services should be included within programs for orphans and vulnerable children (OVC). [This budget code was adopted in FY 2009.]
TB/HIV: includes exams, clinical monitoring, related laboratory services, treatment and prevention of tuberculosis (including medications), HIV testing and clinical care of clients in TB service locations, TB screening, and diagnosis, treatment and prevention of TB in PLWHA. Funding for these activities, including commodities and laboratory, should be included in the TB/HIV budget code rather than other budget codes. The location of HIV/TB activities can include general medical settings, HIV/AIDS clinics, home-based care and traditional TB clinics and hospitals. Pediatric TB/HIV services should be included in this budget code.
Orphans and Vulnerable Children: activities are aimed at improving the lives of orphans and other vulnerable children (OVC) affected by HIV/AIDS, and doing so in a measurable way. Services to children (0–17 years) should be based on the actual needs of the child and could include ensuring access to basic education (from early childhood development through secondary level), basic health care services, targeted food and nutrition support, including support for safe infant feeding and weaning practices, protection, mitigation of factors that place children at risk, legal aid, economic strengthening, training of caregivers in HIV prevention and home-based care, etc. Household-centered approaches that link OVC services with HIV-affected families (linkages with PMTCT, palliative care, treatment, etc.) and strengthen the capacity of the family unit (caregiver) are included along with strengthening community structures which protect and promote healthy child development (schools, churches, clinics, child protection committees, etc.) and investments in local and national government capacity to identify, monitor and track children’s well-being. Programs may be included which strengthen the transition from residential OVC care to more family-centered models.
Treatment
ARV Drugs: including procurement, delivery, and in-freight of ARV drugs. All antiretroviral Post-Exposure Prophylaxis procurement for rape victims should be included within this program area. Distribution/supply chain/logistics, pharmaceutical management and related systems strengthening inputs, including training, are to be included in the Health Systems Strengthening section.
Adult Treatment: including infrastructure, training clinicians and other providers, exams, clinical monitoring, related laboratory services, and community-adherence activities. Clinical monitoring and management of opportunistic infections is classified under Adult Care and Support.
Pediatric Treatment: including infrastructure, training clinicians and other providers, exams, clinical monitoring, related laboratory services, and community-adherence activities. Clinical monitoring and management of opportunistic infections is classified under Pediatric Care and Support. [This budget code was adopted in FY 2009.]
Other
Health Systems Strengthening: include activities that contribute to national, regional or district level health systems by supporting finance, leadership and governance (including broad policy reform efforts including stigma, gender etc.), human resources for health, institutional capacity building, supply chain or procurement systems, information systems, Global Fund programs and donor coordination. The HSS Steering Committee has identified the following areas for current emphasis: (1) focus on building government capacities to manage a health system that effectively serves its people; (2) invest more strategically to develop human resources for health; (3) continue transition to indigenous implementing partners; (4) invest in a formal health systems assessment process for each country; (5) put greater emphasis on innovative strategies for the private sector to become a more important part of a country’s health system strengthening plan; (6) expand PEPFAR’s emphasis on monitoring of HIV services to including strategies to monitor broad health system changes over time; and (7) staff for success, in other words assess the skill mix in-country and fill staffing gaps aggressively and thoughtfully.
Laboratory Infrastructure: development and strengthening of laboratory systems and facilities to support HIV/AIDS-related activities including purchase of equipment and commodities and provision of quality assurance, staff training and other technical assistance. Specific laboratory services supporting TB testing goes under TB/HIV. Laboratory services supporting counseling should go under Counseling and Testing or PMTCT. Laboratory services supporting care should go under Adult or Pediatric Care and Support. Laboratory services supporting treatment should be included under Pediatric or Adult Treatment Services.
Strategic Information: HIV/AIDS behavioral and biological surveillance, facility surveys, monitoring partner results, reporting results, supporting health information systems, assisting countries to establish and/or strengthen such systems, and related analyses and data dissemination activities fall under strategic information. Program area–specific monitoring and routine evaluation should be incorporated under the specific program area.
SOURCE: OGAC, 2010d, pp. 20–24.
PEPFAR Funding to Prime Partners
Within countries, PEPFAR activities and services are implemented by a variety of different partners, including local (partner country) and international nonprofit organizations (also known as nongovernmental organizations), for-profit firms or organizations, academic institutions, and partner country governments. Although in some cases USG agencies implement activities directly, for most PEPFAR-supported activities prime partners receive PEPFAR funding from USG agencies through grants, contracts, or cooperative agreements. A grant is used to transfer resources to a prime partner to carry out activities without substantial involvement from USG agencies. A cooperative agreement is used to transfer resources when substantial USG involvement is necessary to achieve a goal or objective. A contract is used to purchase goods or services (OGAC, 2011b). Prime partners may contract with and outlay funds to subpartners to implement services or activities (GAO, 2012).
The committee wanted to explore funding to prime partners and subpartners in order to understand the different kinds of actors that have been responsible for implementing PEPFAR services and activities over time. However, the committee’s analysis in this area was limited by the unavailability of quality data. OGAC has not consistently tracked funding to prime partners across the whole of the program, and although some tracking of this information occurs at the HQ level, OGAC was unable to provide these data to the committee for the evaluation. In addition, USG agencies and PEPFAR mission teams are not required to report sub-partner funding to OGAC, so the committee was unable to examine funding flows through the sub-partner level (NCV-1-USG).
To examine this question, the committee was able to compile some limited data on PEPFAR funding to prime partners using a variety of publicly available sources, including a dataset previously released by the Department of State (for FYs 2004, 2005, and 2006), PEPFAR partner lists (for FYs 2007 and 2008), and COPs (for FYs 2009 and 2010) (CGD, 2008; OGAC, 2012a, 2013c). The process of extracting and compiling these data was time intensive, so to be feasible within the resources and time available for the study the committee’s analysis was limited to a subset of partner countries. The committee chose to compile these data for the same 13 countries purposefully selected for country visits. Within this subset of 13 countries, to the extent that the data sources above were complete, the committee was able to compare partner data and planned/approved PEPFAR funding for those that were focus countries for FY 2004 through FY 2010 and for non-focus countries for FY 2008 through FY 2010. The number of prime partners for which data were available varied by country (from 4 to 176); during the time period for which data were available, focus countries had
an average of 99 total partners and non-focus countries had an average of 19 total partners. For more information on the data sources and their limitations, the methods for this data extraction, and the committee’s selection process for the 13 countries, see Appendix C.
To examine funding trends over time, the committee categorized each of the prime partners by origin and location of the organization’s headquarters (U.S.-based, partner country, and other) and type (academia, nonprofit, for-profit, and government). A separate category was created for multilateral organizations such as the World Health Organization (WHO) and the United Nations Children’s Fund (UNICEF). Based on the subset of data available to the committee for review, there has been a shift in PEPFAR funding over time from U.S.-based to non-U.S.-based prime partners (see Figure 4-13). For this subset of countries and years, prime partners based in partner countries received an average of 33 percent of PEPFAR funding across all years, increasing from 22 percent in 2004 to 36 percent in 2010. U.S.-based prime partners received an average of 63 percent of PEPFAR funding, declining from 75 percent in 2004 to 61 percent in 2010. Prime partners based in other countries (i.e., not the United States or the partner country) received an average of 3 percent, and multilateral organizations received an average of 1 percent. It is important to note that these data do not represent the ultimate distribution of funds to partner
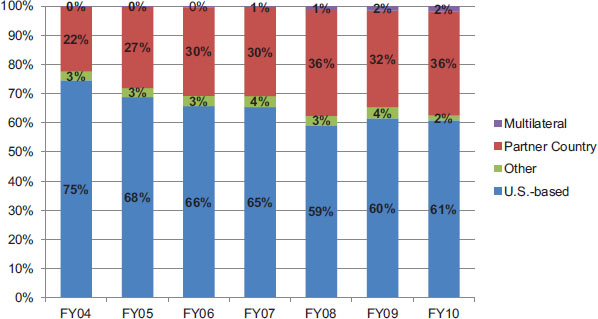
FIGURE 4-13 Proportion of PEPFAR funding by origin of prime partner in 13 PEPFAR partner countries.
NOTE: These data represent, based on the available sources, the proportion of PEPFAR funding directed to prime partners based in the United States, partner countries, other countries, or multilateral organizations.
SOURCE: Select country data extracted by IOM from PEPFAR Country Operational Plans, PEPFAR partner lists, and the Center for Global Development PEPFAR funding dataset (CGD, 2008; OGAC, 2012a).
country implementers, because many U.S.-based prime partners contract with subpartners that are partner country–based organizations, including governments at the national and sub-national level; nongovernmental for-profit, nonprofit, and civil society organizations; and academia. As described previously, the committee was not able to assess the distribution of funds at the sub-partner level.
The committee also examined the distribution of funding among types of prime partners, shown in Figure 4-14. Throughout the duration of the program, the distribution among different types of partners has been variable from year to year, but nonprofit partners have consistently received a greater share of prime partner funding than any other category. On average, nonprofit organizations received the largest share of PEPFAR prime partners funding (49 percent), followed by academic prime partners (20 percent), governmental prime partners (17 percent), for-profit prime partners (13 percent), and multilateral organizations (1 percent). In Figure 4-14, types of partners are not disaggregated by origin; for example, the category of government prime partners includes partner country governments, USG agencies such as CDC and USAID (when these agencies are directly responsible for delivering technical assistance or implementing activities), and, very rarely, other country governments.
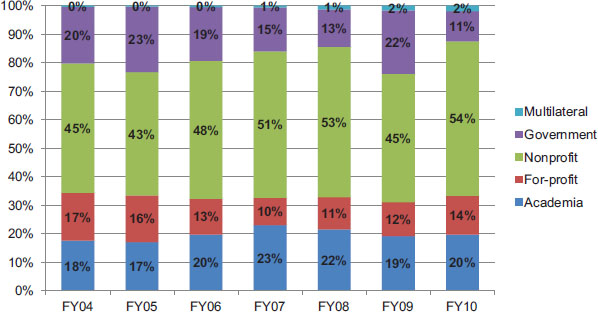
FIGURE 4-14 Percentage of PEPFAR funding by type of prime partner in 13 PEPFAR partner countries.
NOTE: These data represent, based on the available sources, the proportion of PEPFAR funding directed to governments, for-profit entities or firms, nongovernmental organizations (nonprofit organizations), academic institutions, and multilateral organizations, regardless of origin (see above).
SOURCE: Select country data extracted by the IOM from PEPFAR Country Operational Plans, PEPFAR partner lists, and the Center for Global Development PEPFAR funding dataset (CGD, 2008; OGAC, 2012a).
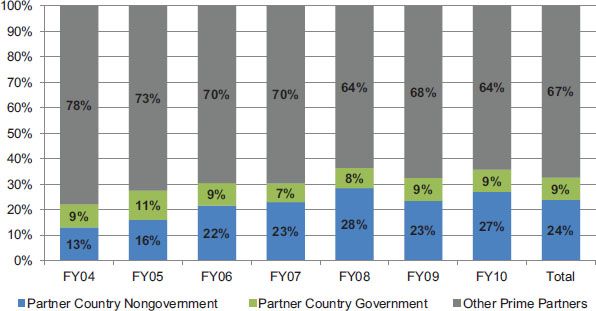
FIGURE 4-15 PEPFAR funding for local prime partners.
NOTE: Other prime partners include prime partners that are based in the United States or other countries as well as multilateral organizations.
SOURCE: Select country data extracted by the IOM from PEPFAR Country Operational Plans, PEPFAR partner lists, and the Center for Global Development PEPFAR funding dataset (CGD, 2008; OGAC, 2012a).
As described above, an increasing share of funding has been directed to local prime partners with headquarters based in partner countries. To better understand how this funding has been distributed among the types of partners within partner countries, the committee examined the breakdown of local prime partner funding between government and nongovernment entities (see Figure 4-15). In this subset of countries and available data, the proportion of funding going to local governments as prime partners has remained relatively stable over time and generally under 10 percent of total funding. The increase in local prime partner funding is mostly accounted for by nongovernmental entities. OGAC has stated that it has the goal of transitioning funding to more local prime partners that are based in partner countries in order to increase the sustainability of PEPFAR programs. These efforts are described further in the discussions of the health systems financing in Chapter 9 and of sustainability in Chapter 10.
Conclusion: The greater part of PEPFAR’s funding has always gone to support programs and activities implemented in partner countries. Consistent with one aspect of PEPFAR’s articulated strategy to move toward sustainability, more PEPFAR funding over time has been directed to local prime partners. Based on an analysis of a subset of data and countries, the increase in local prime partner funding has been driven primarily by increased funding to nongovernmental entities based in partner countries; the proportion
of funding to partner country governments as prime partners has remained relatively stable over time.
As described in this part of the chapter, which focused on PEPFAR funding levels and distribution, the committee aimed to come to a full understanding of the amount and distribution of the annual direct investment of PEPFAR in partner countries, which is a critical input to assess in order to understand the performance of the program. However, limitations in the available financial data made this very difficult. In particular, there are limitations to understanding the amount and distribution of funds outlaid on an annual basis, with data only readily available for annual congressional appropriations and cumulative obligations and outlays. Furthermore, these data are not available disaggregated by type of activity or by type of partner. Thus, the committee used data on what was planned/approved in annual budgets to look at how PEPFAR funding is distributed at the country, program, and partner levels. Even within this planned/approved funding, there are limitations to matching the data in the reported budget codes to the program’s activities, and data are limited on the types of partners that ultimately receive the funding.
Until recently, OGAC has been unable to track and assess how PEPFAR funds have moved from congressional appropriations to OGAC to the implementing agencies to prime partners to subcontractors, because USG implementing agencies were not required to report on expenditures at all levels of the program (Donnelly, 2012b). In May 2012 OGAC requested approval from the U.S. Office of Management and Budget (OMB) to require all partners receiving PEPFAR funding to report annual program expenditures using an electronic template (60-Day Notice, 2012). It is important to note, however, that while this will improve the availability of useful financial data, requiring more financial reporting may also create additional reporting burden for partners and country teams (NCV-4-USACA). OGAC initially estimated that recipients of PEPFAR funding would need an average of 12 hours each year to comply with the new reporting requirements, but based on public comments received during the Paperwork Reduction Act approval process, the average burden estimate was increased to 24 hours (30-Day Notice, 2012; 60-Day Notice, 2012). The estimate was calculated by surveying diverse partners that participated in pilot expenditure analyses from 2009 to 2011 and taking an average of the responses; OGAC has noted that the time will vary considerably depending on the size of partners and the portfolio of programs they implement (OGAC, 2013b). OGAC anticipates the burden to be reduced over time as partners familiarize themselves with the data collection process. The current estimate of 24 hours will be reassessed in 2014, 2 years after OMB’s approval of the reporting form in November 2012. The reassessment will account for improvements
in the data collection interface and greater experience with the data collection for partners.15
Conclusion: Because of limitations in the available financial data, it is difficult to fully assess the amount and distribution by program area and partner type of the annual direct investment of PEPFAR in partner countries. PEPFAR would benefit from the collection and reporting of financial data that not only serves for accounting purposes but also are more closely aligned with programmatic data and program implementation. These data are critical for PEPFAR and external stakeholders to more easily and effectively understand how well PEPFAR is being implemented and how PEPFAR’s investment relates to both the targets and goals of PEPFAR-supported programs and the broader goal of transitioning to more sustainable management of the response to HIV in partner countries. To this end, the committee, while acknowledging the realities of the additional reporting burden, supports OGAC’s request to collect more information from implementing partners on PEPFAR program expenditures.
PEPFAR FUNDING BY COUNTRY CHARACTERISTICS
As described above, most PEPFAR funding is appropriated and budgeted for activities within partner countries. In addition to understanding how PEPFAR funding is distributed among the different program priorities and different mechanisms and partners for implementation, the committee was interested in assessing the characteristics of the countries that have received PEPFAR funding over time and the distribution of funding across these countries. PEPFAR’s authorizing legislation recognized the need “to turn the tide against AIDS” in African and Caribbean countries most affected by HIV/AIDS.16 The legislation stated that the required Five-Year Strategy should “establish priorities for the distribution of resources based on factors such as the size and demographics of the population with HIV/AIDS [. . .] and the needs of that population and the existing infrastructure or funding levels that may exist.”17 As described in Chapter 1, at PEPFAR’s inception bilateral USG HIV/AIDS programs encompassed activities in more than 100 countries, and since FY 2004, at least 112 countries have received PEPFAR support. However, the authorizing legislation designated 14 specific countries in which all USG HIV-related activities should be
__________________
15Ibid.
16Supra, note 7 at ![]() 2(28).
2(28).
17Supra, note 7 at ![]() 101(a)(9).
101(a)(9).
under the direct authority of the newly established U.S. Global AIDS Coordinator, along with “other countries designated by the President.”18 The 14 countries had been previously chosen for the Mother-and-Child HIV Prevention Initiative, and these countries were among those with the highest HIV prevalence rates at the time and were home to nearly 70 percent of those living with HIV in Africa and the Caribbean (White House Office of the Press Secretary, 2003). The implementation of PEPFAR was focused on these countries as well as Vietnam, which was added subsequent to the legislation. Most of the investment was concentrated in these 15 “focus” countries, which together had HIV/AIDS burdens that accounted for more than 50 percent of global HIV prevalence (Goosby et al., 2012).
The reauthorization legislation in 2008 specified that in designating additional countries for this direct authority, priority should be given to “those countries in which there is a high prevalence of HIV or risk of significantly increasing incidence of HIV within the general population and inadequate financial means within the country.”19 Those countries with the highest levels of investment that are under the direct authority of OGAC submit COPs to OGAC. Over time the COP countries—and, in a few cases, coordinated regions—have expanded from the original focus countries. At the time of the planning of this evaluation, there were 31 individual countries submitting COPs; these countries comprise the major focus of the committee’s assessment.
To gain a more detailed understanding of the characteristics of these countries, the committee chose to examine how PEPFAR funding, as reflected in the total annual planned/approved funding reported by OGAC in the annual PEPFAR Operational Plans, is distributed using specific metrics for these 31 partner countries. As described in the sections that follow, in order to examine PEPFAR funding by the severity of the epidemic, the committee calculated summary statistics for three groups of countries based on HIV prevalence in 2009 as well as average PEPFAR funding per person living with HIV (PLHIV) from FY 2005 to FY 2011. Because low-income countries are most in need of external assistance with HIV/AIDS epidemics, the committee also looked at PEPFAR funding to countries by income level. As described previously, complete and consistent data sources across countries are not available to reflect internal resources for the HIV response in partner countries; as a result, this was not included in this analysis despite being one of the criteria for prioritization in the legislation. Chapter 9 provides a more thorough discussion of domestic financing for national HIV/AIDS responses and the implications of these data limitations.
__________________
18Supra, note 7 at ![]() 102(a)(2), 22 U.S.C. 2651a(f)(2)(B)(ii)(VII).
102(a)(2), 22 U.S.C. 2651a(f)(2)(B)(ii)(VII).
19Supra, note 9 at ![]() 102(2)(E)(iii), 22 U.S.C. 2651a(f)(2)(B)(ii)(IX).
102(2)(E)(iii), 22 U.S.C. 2651a(f)(2)(B)(ii)(IX).
PEPFAR Funding by HIV Prevalence
Although PEPFAR is focused on low- and middle-income countries with a high burden of HIV, PEPFAR funding provides support for the response to HIV to countries with a wide range of epidemiological profiles and HIV/AIDS prevalence levels. The committee used 2009 prevalence to group the 31 countries that were the focus of this evaluation into three categories; this year was chosen because it represented the most complete year for which prevalence data were available, and few countries would shift categories if another year were used. Information about PEPFAR’s approved funding over time in these prevalence groupings is shown in Figure 4-16 and Table 4-3. Almost all PEPFAR-approved funding (95 percent) over the FY 2005–2011 period went to countries with high HIV prevalence (>1 percent of the general population). From FY 2005 to FY 2011 the greatest share of PEPFAR funding (60 percent) was approved for 16 countries with adult HIV prevalence rates between 1 and 10 percent. During the same time period PEPFAR funded nine countries with prevalence rates of 10 percent or greater; this subset of countries received approximately one-third of total funding (35 percent) and also had the highest median funding level and included the highest maximum in the range of funding per country. Six countries with national prevalence rates below 1 percent received 5 percent of total funding (OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d). Globally, there were nine countries with HIV prevalence rates greater than
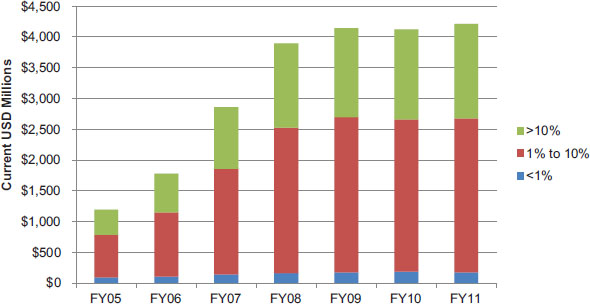
FIGURE 4-16 PEPFAR planned/approved funding by 2009 prevalence groupings in 31 PEPFAR partner countries (current USD millions).
SOURCES: OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d.
TABLE 4-3 PEPFAR Countries Grouped by 2009 Prevalence
| Prevalence | Totals (FY 2005–2011) | |
| <1% | Number of countries | 6 |
| Median funding | $17.5 | |
| Funding range (min, max) | ($4.0, $97.8) | |
| Total funding | $1,034.6 | |
| 1–10% | Number of countries | 16 |
| Median funding | $39.1 | |
| Funding range (min, max) | ($4.0, $565.0) | |
| Total funding | $13,319.9 | |
| >10% | Number of countries | 9 |
| Median funding | $62.5 | |
| Funding range (min, max) | ($6.5, $590.9) | |
| Total funding | $7,850.8 | |
| All 31 Countries | Number of countries | 31 |
| Median funding | $33.0 | |
| Funding range (min, max) | ($4.0, $590.9) | |
| Total funding | $22,205.4 | |
NOTE: Funding data are presented in current USD millions.
SOURCES: OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d; UNAIDS, 2010.
10 percent in 2009, and PEPFAR funded all of them (UNAIDS, 2012a). There were 41 countries with HIV prevalence rates between 1 and 10 percent; in 2009 PEPFAR provided funding to 25 of these countries, including 16 that prepare COPs and are included in this analysis. This distribution of funding is consistent with the congressional and programmatic intent to focus primarily, although not exclusively, on countries with a high burden of HIV. Indeed, Ambassador Goosby has recently said that OGAC has “aggressively tried to re-equilibrate more appropriate allocations to prevalence rates” (Donnelly, 2012b).
PEPFAR Funding per PLHIV
Another measure for examining PEPFAR funding by severity of the epidemic is average PEPFAR funding per PLHIV. Although the number of PLHIV is not a perfect proxy for the HIV prevention, care, and treatment needs in a country, this approach does provide a reasonable approximation of the funding relative to the burden, which allows for a richer assessment of the distribution of funding than simply the HIV prevalence level. The committee used planned/approved PEPFAR funding and yearly estimates of PLHIV from UNAIDS to calculate the average PEPFAR funding per PLHIV (age 15+) from FY 2005 to FY 2010 (UNAIDS, 2010a). Table 4-4 shows this calculation, which for context is presented alongside the population
TABLE 4-4 Average PEPFAR Funding per PLHIV (Current USD)
| Population Size | 2009 HIV Prevalence Grouping | Average PEPFAR Funding per Estimated PLHIV (FY 2005–FY 2011) | ||
| Guyana | 753,013 | 1-10% | $3,842.7 | Greater than $250 per PLHIV |
| Haiti | 9,864,241 | 1-10% | $806.5 | |
| Rwanda | 10,311,275 | 1-10% | $632.8 | |
| Namibia | 2,242,078 | >10% | $469.2 | |
| Ethiopia | 81,187,751 | 1-10% | $368.3 | |
| Cambodia | 13,977,903 | <1% | $275.4 | |
| Kenya | 39,462,188 | 1-10% | $270.8 | |
| Vietnam | 86,901,173 | <1% | $252.4 | |
| Botswana | 1,981,576 | >10% | $242.7 | Between $100 and $250 per PLHIV |
| Zambia | 12,723,746 | >10% | $224.7 | |
| Uganda | 32,367,909 | 1-10% | $206.2 | |
| Côte d'Ivoire | 19,350,026 | 1-10% | $186.2 | |
| Dominican Republic | 9,796,852 | <1% | $173.7 | |
| Tanzania | 43,524,738 | 1-10% | $173.1 | |
| Mozambique | 22,858,607 | >10% | $132.4 | |
| Nigeria | 154,488,072 | 1-10% | $99.4 | Between $20 and $100 per PLHIV |
| Swaziland | 1,168,345 | >10% | $99.2 | |
| South Africa | 49,751,503 | >10% | $73.8 | |
| Lesotho | 2,149,201 | >10% | $55.3 | |
| Angola | 18,555,115 | 1-10% | $51.1 | |
| Indonesia | 237,414,495 | <1% | $42.0 | |
| Ghana | 23,824,402 | 1-10% | $37.9 | |
| Dem. Repub. Congo | 64,204,304 | 1-10% | $36.1 | |
| Sudan | 42,478,309 | 1-10% | $35.7 | |
| Malawi | 14,442,290 | >10% | $32.1 | |
| Zimbabwe | 12,473,992 | >10% | $25.0 | |
| Ukraine | 45,715,010 | 1-10% | $19.9 | Less than $20 per PLHIV |
| China | 1,334,908,820 | <1% | $13.8 | |
| Russia | 143,064,078 | 1-10% | $12.7 | |
| India | 1,207,740,408 | <1% | $12.1 | |
| Thailand | 68,706,122 | 1-10% | $11.8 | |
SOURCES: OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d; UNAIDS, 2012b.
of each country and the HIV prevalence grouping as a reflection of the disease burden.
The funding per PLHIV varied significantly, from $11.84 in Thailand to $3,842.71 in Guyana (see Table 4-4). Guyana received by far the most funding per PLHIV. Seven other countries received greater than $250 per PLHIV, including two countries from the East Asia and Pacific region with concentrated epidemics (Vietnam and Cambodia). Seven countries received between $100 and $250 per PLHIV, 11 countries received between $20 and $100 per PLHIV, and 5 countries received less than $20 per PLHIV. Based on the committee’s assessment and the perspectives expressed by stakeholders interviewed for this evaluation, there are a number of factors worth discussing that may contribute to the distribution of funding per PLHIV, although it is not possible to draw causal conclusions about the relationship between the funding and these factors.
Although there are exceptions, many of the largest countries (by population) have received less funding per PLHIV, while many smaller African countries with high disease burden have received higher investments per PLHIV. Some small countries may require higher investments per PLHIV for a similar level of programming and services because, although initial startup costs to initiate a robust response to HIV may be either greater in larger countries or similar regardless of population size, larger countries subsequently have more opportunities to achieve economies of scale and to reduce per-person costs of the provision of services. Not all small countries are in the higher grouping, however, which may be because in some countries the available infrastructure had more initial readiness to support service delivery at lower per-person costs. In addition, regardless of size, the country’s own resources, capacity, and infrastructure may affect the necessary balance between PEPFAR’s support for higher-cost direct service delivery programs versus lower-cost technical assistance programs.
Countries with different prevalence groupings are distributed across different levels of funding per PLHIV. Some countries in lower prevalence groupings receive among the highest levels of funding. Lower-prevalence countries may receive high levels of funding per PLHIV for various reasons, including political or foreign policy considerations; availability of other external donor and country resources for the HIV/AIDS response, which in some cases may be influenced by how active a role the country government takes in the response; lack of economies of scale for service delivery; and initial or existing capacity levels and infrastructure development that affect the costs of service delivery.
PEPFAR Funding by Income Level
Finally, to assess how PEPFAR funding is distributed by resource needs, the committee calculated summary statistics for planned/approved PEPFAR funding by partner country income level as a proxy for resources available. Of the 31 countries included in the committee’s analysis, 19 were classified by the World Bank in 2004 as low-income, 9 as lower-middle-income, and 3 as upper-middle-income.20 From FY 2005 to FY 2011, most planned/approved PEPFAR funding (78 percent) was directed to 19 low-income countries. Nine lower-middle-income countries have received 6 percent of planned/approved funding, and three upper-middle-income countries have received 16 percent (see Figure 4-17 and Table 4-5).
Summary of PEPFAR Funding By Country Characteristics
In order to understand the distribution of PEPFAR funding among countries, the committee considered funding levels by disease burden, income level, and funding per PLHIV, which have been described in the preceding sections and are put together in Table 4-6. The patterns of distribution of PEPFAR funding by disease severity and income level in partner countries are variable. Overall, PEPFAR funding has predominantly gone to support low-income countries with a high burden of HIV. Five countries fall into both the lowest income grouping and the highest prevalence grouping, and about half of the total number of partner countries (16 of 31) are both low-income and have a high prevalence, at greater than 1 percent. Four other countries that receive funding but are not in the lowest income grouping (Namibia, Swaziland, South Africa, and Botswana) are priority partner countries for investment because of their very high prevalence of HIV. As described previously in this chapter and in Chapter 1, this is consistent with the legislative intent to focus on high-burden countries with limited resources. Countries that are not in the income category of greatest need nor in the highest prevalence grouping, as well as those with concentrated epidemics that are in the lowest income category, may have been selected as recipients of PEPFAR funding for other reasons, including the need for external support for a robust HIV response due to limited resources or a limited engagement of country governments in the response.
The level of PEPFAR funding per PLHIV varies across partner countries; the reasons for this may include level of governmental commitment and the levels of other available country resources and external donor
__________________
20 The World Bank categorizes economies based on gross national income (GNI) per capita and in 2004 used the following criteria: GNI per capita of $735 or less = low-income; $736–$2,935 = lower-middle-income; $2,936–$9,075 = upper-middle-income; greater than $9,075 = high-income (World Bank, 2012).
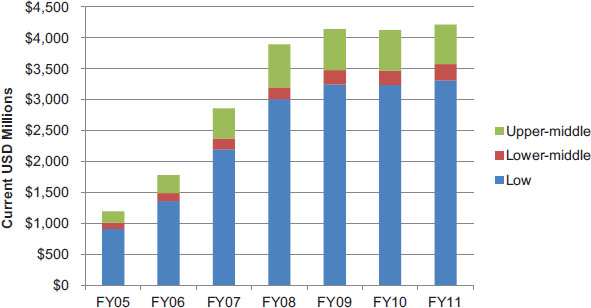
FIGURE 4-17 PEPFAR planned/approved funding by income level in 31 PEPFAR partner countries (current USD millions).
NOTE: Countries were categorized based on income level in 2004 (the year that PEPFAR began).
SOURCES: OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d; World Bank, 2012.
TABLE 4-5 PEPFAR Countries Grouped by 2004 Income Level
| Income Level | Totals (FY 2005–FY 2011) | |
| Low income | Number of countries | 19 |
| Median funding | $75.7 | |
| Funding range (min, max) | ($4.0, $565.0) | |
| Total funding | $17,284.0 | |
| Lower-middle income | Number of countries | 9 |
| Median funding | $9.8 | |
| Funding range (min, max) | ($4.0, $108.9) | |
| Total funding | $1,308.9 | |
| Upper-middle income | Number of countries | 3 |
| Median funding | $84.4 | |
| Funding range (min, max) | ($5.0, $590.9) | |
| Total funding | $3,612.5 | |
| All 31 countries | Number of countries | 31 |
| Median funding | $33.0 | |
| Funding range (min, max) | ($4.0, $590.9) | |
| Total funding | $22,205.4 | |
NOTE: Funding data are presented in current USD millions.
SOURCES: OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d; World Bank, 2012.
| Income Level | |||||||
| Low Income | Lower-middle Income | Upper-middle Income | |||||
| HIV Prevalence | <1% | India | $12.1 | China | $13.8 | ||
| Vietnam* | $252.4 | Indonesia | $42.0 | ||||
| Cambodia | $275.4 | Dominican Republic | $173.7 | ||||
| 1-10% | Nigeria* | $99.4 | Thailand | $11.8 | Russia | $12.74 | |
| Ethiopia* | $368.3 | Ukraine | $19.9 | ||||
| Dem. Repub. Congo | $36.1 | Angola | $51.1 | ||||
| Tanzania* | $173.1 | Guyana* | $3,842.7 | ||||
| Sudan | $35.7 | ||||||
| Kenya* | $270.8 | ||||||
| Uganda* | $206.2 | ||||||
| Ghana | $37.9 | ||||||
| Côte d'Ivoire* | $186.2 | ||||||
| Rwanda* | $632.8 | ||||||
| Haiti* | $806.5 | ||||||
| >10% | Mozambique* | $132.4 | Namibia* | $469.2 | South Africa* | $73.76 | |
| Malawi | $32.1 | Swaziland | $99.2 | Botswana* | $242.71 | ||
| Zambia* | $224.7 | ||||||
| Zimbabwe | $25.0 | ||||||
| Lesotho | $55.3 | ||||||
NOTE: Income levels are from 2004; HIV prevalences are from 2009. *= original focus country. Within each box (e.g., <1% and low-income), countries are sorted by population from largest to smallest.
SOURCES: OGAC, 2005, 2006b, 2007c, 2008c, 2010e, 2011c,d; UNAIDS, 2010a; 2012b; United Nations, 2011.
resources, such as the Global Fund and other bilateral donors, as well as factors of size, capacity, and infrastructure that can affect what types of assistance is needed and how costly services are in the country (NCV-3-USG; NCV-9-USG; NCV-12-USG) (GHI, 2012). In addition to differences in the costs and scale of programs and the types of programmatic support needed, foreign policy, geopolitical, or other factors can be strategic drivers for supporting bilateral engagement and investment in some countries, and past or current political instability or uncertainty may contribute to decisions about foreign assistance investment (NCV-3-USG; NVC-9-USG; NCV-12-USG) (GHI, 2012). Different models of PEPFAR assistance and how they are determined are discussed in more depth in Chapter 10.
Conclusion: Although there is variability in how the distribution of PEPFAR funding relates to country characteristics of disease severity and income level, PEPFAR funding overall has predominantly, but not exclusively, gone to support low-income countries with a high burden of HIV.
STRATEGIC USE OF PEPFAR RESOURCES
In addition to describing the amount and distribution of PEPFAR funding over time, the committee assessed some available information about how decisions are made about the allocation of PEPFAR resources, including mechanisms and efforts to try to maximize the strategic and efficient use of PEPFAR resources as a contribution to the response to HIV in partner countries. This is becoming increasingly important as a part of the future plans for the evolving implementation of USG funding for global HIV, especially in the context of an increasingly resource-constrained environment (NCV-5-USACA; NCV-6-USNGO; NCV-9-USG; NCV-21-ML; NCV-27-ML). A few key topics in this area are described in brief here; the primary discussion of these topics can be found in the section on financing in Chapter 9, which discusses health systems strengthening, and in Chapter 10, which is a discussion of progress toward a sustainable response in partner countries.
In 2011, OGAC launched PEPFAR’s Impact and Efficiency Acceleration Plan, which is “a framework for making smart investments” (Goosby, 2012b, p. S45). This plan calls for the generation and use of economic and financial data; the allocation of resources based on their anticipated impact; collaboration with governments, the Global Fund, and others to align programs; and streamlining of business processes to maximize the impact of PEPFAR resources. As discussed below, these strategies have been in place to some extent through the history of the program but have been receiving greater emphasis in more recent years.
Generation and Use of Economic and Financial Data
To support better decision making, OGAC has prioritized the generation and use of financial data, as discussed earlier in this chapter, as well as economic data such as costing studies, expenditure analysis, and support for partner country governments to understand national funding streams (Goosby, 2012b; Holmes et al., 2012).
In one recent initiative to support enhanced partner management and improve the efficiency of program implementation at the country level, OGAC has piloted different types of expenditure analysis in partner countries (Goosby, 2012b; Holmes et al., 2012; PEPFAR, 2012). From 2009 to 2012, the PEPFAR Expenditure Analysis Initiative collected data on PEPFAR expenditures in eight partner countries. By linking expenditure data to HIV/AIDS program results, the results of these analyses are intended to inform internal PEPFAR partner management, PEPFAR portfolio allocations and budget projections, program planning, and country-level harmonization of expenditure tracking and coordination of resources with governments. For example, PEPFAR has supported the estimation of per-patient expenditure for treatment services in South Africa, Mozambique, and Zambia; for HIV testing and counseling in Mozambique; for different behavioral prevention services in Uganda; and for prevention of mother-to-child transmission (testing, treatment, and care services) in Nigeria (PEPFAR, 2012; Rosen, 2011). In South Africa, the PEPFAR mission team mapped PEPFAR expenditures to the objectives of the National Strategic Plan and is using these data to facilitate planning with the national and provincial government (PEPFAR, 2012). The results of these expenditure analyses are also intended to help inform global budgeting and resource allocation at the headquarters level by estimating the PEPFAR costs to support HIV/AIDS programs (PEPFAR, 2012).
PEPFAR’s support for efforts to track and assess expenditures, costs, resource needs, and funding streams in partner countries is discussed in more detail in Chapter 9 in the section on PEPFAR’s efforts in the area of health systems financing in partner countries.
Allocation of Resources Based on Anticipated Impact
In addition to understanding program costs, OGAC calls on PEPFAR mission teams and partners to use scientific evidence as a guide for allocating resources to the interventions that will have the most impact within each country (Goosby, 2012b). Operational and programmatic guidance from headquarters helps mission teams with the allocation of resources based on evidence for likely impact (NCV-7-USG). In addition to guidance on what activities are priorities for implementation, PEPFAR’s mechanisms for
program monitoring and evaluation are also intended to provide an ongoing assessment of program performance and to therefore inform the future allocation of resources. The reporting and guidance specific to different programmatic areas supported by PEPFAR are discussed in the relevant subsequent chapters of this report.
In addition to using routine program monitoring data, the Expenditure Analysis Initiative described above has also contributed to resource allocation based on impact. In Mozambique, for example, the expenditure data on HIV counseling and testing were used to shift investments to target populations and modalities that were most likely to identify HIV-positive people (PEPFAR, 2012). OGAC expects that better access to economic, financial, and indicator data will allow governments and partners to avoid inefficient allocation of resources (OGAC, 2011e).
Interviewees noted that an increasingly resource-constrained environment in the second phase of PEPFAR has required prioritizing activities that are aligned with guidance and that are reported on (NCV-2-USG; NCV-9-USG). Interviewees shared a common perspective that ‘what gets measured gets done’ (NCV-2-USG; NCV-23-USNGO; 272-36-USG; 396-1920-USG). In some countries, interviewees felt that the emphasis on showing results forced them to focus on interventions for which impact could be measured quickly (272-12-USNGO). Across countries, interviewees also mentioned the need to target PEPFAR resources to populations that are most vulnerable, in need, or at risk as a current or needed strategy for making the best use of resources (587-ES; 166-17-USG; 396-7-PCGOV; 331-ES; 240-ES; 196-ES; 542-ES). The role of PEPFAR’s monitoring and evaluation and other data collection efforts in guiding program priorities is discussed in much more detail in Chapter 11.
Collaboration with Governments, Other Donors, and the Global Fund to Align Programs
OGAC has also identified the importance of working with partner country governments, the Global Fund, other donors, and other stakeholders involved in the HIV/AIDS response to ensure that PEPFAR resources complement funding from domestic and external sources and that interventions are aligned with partner country HIV/AIDS strategies (Goosby, 2012b). Interviewees from several countries and across stakeholder types identified coordination and non-duplication as strategies to make the best use of resources (331-ES; 587-10-USG; 196-ES). Beyond coordination and non-duplication, PEPFAR has in some cases leveraged funding in order to mobilize more resources for the HIV/AIDS response. For example, PEPFAR may provide funding to roll out an intervention in one geographic region
and use that to leverage other donor and partner country resources to fund other geographic regions, or PEPFAR may commit to making investments and use that to elicit matched funding for similar investments from other sources (NCV-9-USG; 240-ES; 542-ES; 396-ES; 935-ES; 166-4-USG).
Collaboration with Partner Country Governments
OGAC has instructed PEPFAR mission teams to align and harmonize PEPFAR planning processes with national planning for the HIV/AIDS response. Further, mission teams must consult with partner country governments to get their buy-in, and the partner country governments must approve the strategic direction of the PEPFAR program (OGAC, 2011b). In some cases the alignment process may happen primarily through a broader arena than direct dialog between PEPFAR and the partner country government, such as through donor forums of the kind described in the next section. In many countries representatives from the PEPFAR mission team meet regularly with representatives from the partner country government to share information and to discuss joint planning for the HIV response and issues that arise; from both perspectives, collaboration and alignment were seen as improving over time and helping the HIV response (240-5-PCGOV; 331-4-PCGOV; 196-6-USG; 587-12-USG; 166-8-USG; 166-13-PCGOV; 272-36-USG; 396-55-USG; NCV-6-USNGO; 116-2-USG; 116-4-USG; 240-7-PCGOV; 240-15-USG; 587-7-PCGOV; 396-57-USG). In some countries, in addition to the mission team, PEPFAR implementing partners are also actively involved in regional- or district-level planning and/or coordinating processes (240-15-USG; 461-14-USG; 331-30-USPS; 196-28-USG; 166-5-USG; 272-36-USG; 935-23-PCNGO; 542-8-USNGO), which was described as having improved alignment (240-15-USG; 396-39-USG; 272-7-USG). However, partner country governments have also experienced a lack of information about PEPFAR-supported activities in some countries, which poses a challenge to collaboration for planning (272-36-USG; 166-16-PCGOV; 166-19-PCGOV; 240-33-USG; 396-16-PCGOV; 461-8-PCGOV), and some government representatives described dissatisfaction with the approach to collaboration, specifically when presented with the COP only after it had been drafted (116-11-PCGOV; 166-13-PCGOV). The sharing of information between PEPFAR and partner country governments and other stakeholders is discussed in more depth in Chapter 11 on knowledge management.
PEPFAR mission teams described struggling to collaborate with partner country governments with competing priorities or those that did not view the HIV/AIDS response as a priority; interviewees noted in some cases that PEPFAR was providing a lot of funding for the HIV response while the government really needed or wanted funding for a broader approach to health (240-1-USG; 934-5-USG; 542-2-USG). For example, in one country where PEPFAR and Global Fund funding comprise a very large proportion of the government’s total budget for health, the partner country government felt that
PEPFAR was driving the priorities of the HIV response (240-2-USG; 240-21-PCGOV). Other examples of challenges for alignment with partner country priorities described by interviewees included government priorities that do not match OGAC guidance or PEPFAR focus areas (935-17-USG), lack of engagement by the partner country government (461-4-USG), incomplete or underdeveloped national strategies (240-3-USG), a lack of joint planning processes with government and other donors (587-2-USG), a lack of national commitment from ministries of health for coordinating partners (636-9-USACA; 636-16-USG; 272-15-PCNGO; 396-18-USG), and no mapping of who does what in the HIV response (636-9-USACA; 331-6-CCM). Although there were examples of misalignment of priorities (240-1-USG; 240-7-PCGOV; 331-6-CCM), there were also instances in which PEPFAR was described as supporting the government’s vision (240-2-USG; 636-3-USG; 331-15-USG).
Alignment and collaboration between PEPFAR and partner country governments is discussed further in the section on leadership and governance in Chapter 9 and in Chapter 10, which discusses the sustainability of the response.
Collaboration with Other Donors
Many countries have at least one mechanism for coordination and collaboration among donors and partners, such as donor forums, technical working groups, or other joint processes for the review and planning of allocation of resources and programming (240-5-PCGOV; 331-2-USG; 331-4-PCGOV; 331-ES; 196-6-USG; 196-ES; 636-9-USACA; 636-16-USG; 116-2-USG; 116-4-USG; 272-2-USG; 272-ES; 166-12-USG; 116-5-PCGOV). These coordination efforts can be led by external donors, by multilateral organizations such as UNAIDS, by Global Fund Country Coordinating Mechanisms, or by the partner country government. In most countries, representatives from PEPFAR mission teams or implementing partners are actively involved in these groups (240-5-PCGOV; 240-7-PCGOV; 240-15-USG; 331-4-PCGOV; 587-7-PCGOV; 196-6-USG; 196-20-PCNGO; 636-9-USACA; 116-2-USG; 116-4-USG; 166-12-USG; 272-6-ML; 934-2-USG). The process of developing Partnership Frameworks has also provided an opportunity to engage all stakeholders (331-5-ML; 116-2-USG; 396-57-USG). As one interviewee observed:
“I think that the Partnership Frameworks changed the way we interacted and the openness to listening to folks on the other side who could say, you know, we’re really appreciative of the resources that you’re bringing in through the HIV window, but let’s think about how we can do this in a more comprehensive manner. And in that conversation, it’s not all about just our resources. And it’s about, okay, so, government, this is what you’re bringing to the table. Other partners, this is what you’re bringing to the table. So let’s think collectively.” (116-2-USG)
In addition to more formal processes of engagement, interviewees also described informal methods (e.g., meeting over coffee) of coordinating with other donors (331-2-USG; 196-8-ML; 240-2-USG). Interviewees in several countries also mentioned “gap-filling”—targeting resources to populations or services not addressed by the national response or other partners—as a strategy to make the best use of resources (331-ES; 272-22-USG; 396-ES; 934-ES; 196-ES; 935-8-PCGOV; NCV-21-ML). The process of collaboration and coordination among donors is discussed further in both Chapters 9 and 10.
Collaboration with Global Fund
In some countries, PEPFAR and the Global Fund provide 90 percent of total funding for HIV/AIDS responses, yet the planning and implementation processes of the two donors are not always aligned. Recently, PEPFAR has started planning country programs in greater coordination with the Global Fund, and Ambassador Goosby has stated that he foresees significant cost savings as the two donors become more aligned (Donnelly, 2012b). Many interviewees described PEPFAR efforts to coordinate activities with the Global Fund (240-3-USG; 196-ES; 636-ES; 543-ES); in some countries, non-duplication is formalized through a memorandum of understanding between the two donors and partner country governments (KFF, 2009). In one example of coordination, Global Fund resources may be used to procure first-line ARV drugs while PEPFAR supports procurement of second-line ARVs (NCV-21-ML; 587-22-USG). In Angola and South Sudan, Global Fund finances procurement of ARVs and PEPFAR supports the delivery of ARVs to patients and health worker training (Goosby, 2012a). In Malawi, PEPFAR funding is targeted to urban areas and Global Fund financing supports rural communities, while PEPFAR and UNICEF (with Global Fund financing) jointly support different elements of the PMTCT program (Goosby, 2012a). A recent article described improved communication, sharing of information, and coordination of activities in Tanzania between PEPFAR and the Global Fund (Bilimoria, 2012). Interviewees believed that coordination between PEPFAR and the Global Fund could be improved in some countries (240-5-PCGOV; 587-1-USG; 272-ES). Some PEPFAR countries with fewer donors or smaller programs described fewer challenges with coordination and cooperation (196-1-USG; 196-8-ML; 636-2-USG). PEPFAR’s collaboration with the Global Fund is discussed further in both Chapters 9 and 10.
Streamlining of PEPFAR Business Processes
The final element of OGAC’s plan to maximize PEPFAR resources calls for USG implementing agencies and PEPFAR partners to improve effectiveness and efficiency and adjust the size of and staffing of country programs
to match the needs of the national response (Goosby, 2012b). Efforts to improve routine business practices for the whole of the program have resulted in considerable cost savings (Donnelly, 2012b). Several strategies for streamlining processes are described here.
Cost Reductions for Drugs Procured by PEPFAR
Systemic changes in the selection and procurement of ARVs has contributed to dramatic reductions in the cost of treatment; per-patient treatment costs have fallen from more than $1,100 per year to approximately $335 (OGAC, 2012c). To ensure quality, ARVs purchased with PEPFAR funding must be approved by the U.S. Food and Drug Administration (FDA) or another acceptable regulatory authority. When PEPFAR began, only proprietary/brand name ARVs had been approved by FDA, which resulted in significantly higher costs for first-line regimens (up to $450 more per patient per year) compared to the lowest-priced generics available in focus countries and/or provided by other global HIV/AIDS initiatives (GAO, 2005). To increase the availability of generic ARVs for purchase with PEPFAR funding, FDA modified an expedited review process—FDA tentative approval—to rapidly evaluate the quality of generic ARVs (Holmes et al., 2010). The percentage of generic ARVs purchased with PEPFAR funding increased from 16 percent in 2005 to 89 percent in 2008, reducing drug costs by more than $323 million; in 2010, 97 percent of ARVs procured by PEPFAR were generic (El-Sadr et al., 2012; Holmes et al., 2010). The Supply Chain Management System estimates that switching to generics has saved $1.1 billion through September 2011 (SCMS, 2012).
In addition to decreased costs due to use of generic ARVs, pooled procurement of commodities (including ARV drugs as well as other commodities such as laboratory reagents) within, across, and between countries has led to savings in the form of discounts from suppliers. Changing the methods by which these ARVs are procured and delivered has also achieved significant cost savings (Jamieson, 2011). Through FY 2011 PEPFAR saved more than $59 million by using sea and road freight instead of air freight (SCMS, 2012).
USG Interagency Implementation Process
A key feature of PEPFAR (and the Global Health Initiative) is that programs are to be implemented through a “whole-of-government” approach with the aim that agencies will focus on their core competencies and coordinate efforts to maximize the effectiveness of PEPFAR funding (OGAC, 2009d). Within PEPFAR mission teams, OGAC has mandated that all USG agencies be involved in the annual COP process (described briefly above)
(OGAC, 2007b, 2008b). This interagency implementation approach was also described in Chapter 3.
Stakeholders in partner countries had mixed perspectives on the “whole-of-government” approach. In some countries, interviewees reported competition for funding among USG agencies (934-40-ML; 935-17-USG; 461-4-USG; 272-ES). One interviewee described situations where CDC and USAID put out competing funding announcements and another situation in which representatives from both agencies ‘looked like fools in front of the government because they were fighting with each other’ (NCV-6-USNGO).
Many interviewees from PEPFAR mission teams described challenges with interagency coordination (240-3-USG; 272-1-USG; 272-36-USG; 461-4-USG; 935-17-USG) and struggles to reduce duplication and overlap of activities by USG agencies (240-8-USG; 587-2-USG; 272-1-USG; 272-33-USG; 272-ES). In some cases the time spent on interagency coordination was described as a burden that took away from other responsibilities (461-4-USG; 396-47-USNGO; 166-4-USG; 331-3-USG) and an inefficient use of resources (587-25-ML; 396-47-USNGO; 331-3-USG). The following comments are representative:
“I think what that’s also meant is we spent a lot of our time doing coordination and collaboration. And you could see that as a good thing, or you could see that as a potentially inefficient thing. A lot of time and energy and effort and probably money is spent making sure that everyone under the PEPFAR umbrella, all included, all said their say, all harmonized. And it takes up a lot of time. And it’s definitely, I think we all would have examples of where it’s obstructed the pace or the results of implementation, for sure.” (396-47-USNGO)
‘The PEPFAR team feels under-resourced for coordination. The USG staff often feels burdened by huge workloads and limited time.’ (166-4-USG)
The COP preparation and submission process for interagency mission teams was also described in multiple countries as a significant burden of time and effort, especially as the size and scope of PEPFAR-supported programs has grown, resulting in lengthy COPs and time-consuming preparation (240-1-USG; 240-3-USG; 331-48-USG; 636-16-USG; 166-4-USG; 272-24-USG; 542-3-USG; 396-1-USG). To help address this, OGAC has recently streamlined the COP process by shifting to a 2-year framework with a reduced COP every other year (OGAC, 2010c). At least two mission teams remarked that the new streamlined COP process was an improvement (240-1-USG; 240-33-USG; 272-24-USG).
The relationship and decision-making status between country programs and USG HQ was also noted as part of the challenge. For example, interviewees asserted that ‘OGAC does not promote interagency cooperation,
no leadership in this area’ (331-3-USG), noted ‘a lack of clear guidance from DC [HQ] regarding what USAID should be doing versus CDC’ (240-3-USG), and described the “one USG” philosophy as ‘theoretical’ (587-2-USG). Interviewees provided contrasting solutions to these challenges:
‘HQ should leave the division of labor to the country office to work out. HQ can influence discussions about activities with a mentality of, “Our agency portfolio should look like this.”’ (240-8-USG)
‘Why not have the fights over money and resources at the DC [HQ] level not transfer the coordination burden to every country. If the money was earmarked to the agencies in DC [HQ], then it would lead to less planning burden in the country and more time to do development thinking.’ (461-4-USG)
‘Would prefer funding decisions made at a higher level. Would rather trust DC to make the funding decisions than fight it out on the country team level.’ (331-3-USG)
Despite the challenges described with the interagency process, some interviewees described interagency cooperation and coordination as at least partially successful or as having improved over time (396-57-USG; 116-27-USG; 636-16-USG; 934-1-USG; 461-19-USG; 935-10-USG; 935-28-USG). Interviewees highlighted some examples of successful efforts to use and improve the interagency process to more strategically use PEPFAR funds. In some countries, having multiple technical working groups with representatives across agencies was described as helpful for coordinating the planning and implementation of activities (396-57-USG; 461-4-USG). Interviewees in some cases described efforts that had been put in place or were planned to identify the comparative advantages of each USG agency and assign responsibility for projects accordingly (240-8-USG; 331-2-USG; 331-15-USG; 272-36-USG). Some countries conducted a review of the PEPFAR portfolio or processes to identify areas of overlap and opportunities to reduce duplication (587-2-USG; 587-12-USG; 272-36-USG). One team mentioned that the Partnership Framework process helped its program identify what each agency was doing (116-7-USG). Other interviewees believed that successful interagency collaboration is dependent on the personalities and leadership of the staff involved (636-16-USG; 934-1-USG).
Coordination of Implementing Partners
Another ongoing approach or future opportunity for more strategic and effective use of resources that emerged from country visit interviews is improving coordination among PEPFAR implementing partners. Although
the number of implementing partners varies by country, some partner country programs have more than 100 prime partners and at least that many subpartners. The sheer number of implementing partners in some countries was described as a challenge (240-5-PCGOV; 240-21-PCGOV; 272-5-PCGOV). In some countries, multiple implementing partners are funded to deliver the same services (e.g., ART) or to conduct similar activities (e.g., capacity building), and this duplication or overlap was seen as a challenge (636-ES; 272-5-PCGOV; 272-36-USG; 196-11-USNGO; 196-12-PCGOV; 240-15-USG). An implementing partner that shares technical assistance responsibilities with another implementing partner noted that ‘there are two projects, with two chiefs of party, two finance directors, two offices, two monitoring and evaluation processes, two head offices [. . . it] is not effective and efficient—it is a duplication of positions’ (196-11-USNGO). In one country multiple partners are funded to provide different yet related services (e.g., prevention of mother-to-child transmission, HIV care, TB/HIV) within the same district, which has caused challenges for integration; the implementing partner interviewed expressed a desire to be responsible for all the services within a district (636-9-USACA).
To address these challenges, some PEPFAR mission teams have convened partners meetings, done portfolio reviews, or used other approaches to reduce overlap and duplication among implementing partners (636-6-USG; 935-ES; 461-18-USG; 587-23-USG; 272-36-USG). In one country, for example, PEPFAR partners were described by a partner country government interviewee as ‘well-coordinated’ (240-7-PCGOV). Several PEPFAR mission teams described various reasons for choosing to fund multiple implementing partners for related activities, such as having different partners provide comprehensive services within certain geographic regions (935-2-USG; 461-18-USG) or specific facilities (166-20-USG) and ensuring that a specific service or activity receives the necessary funding and attention:
‘It’s difficult to have one implementing partner do everything, because some things get lost. In previous PEPFAR-funded programs, capacity building wasn’t getting the attention it needed. Therefore, they decided to split into two PEPFAR implementing partners, one of which would focus explicitly on organizational capacity building, and the other would focus on technical assistance.’ (196-28-USG)
Another challenge was that partners may be funded by multiple USG agencies (396-47-USNGO; 636-11-PCNGO; 636-21-USNGO). In one case where there are few local organizations, these local partners may be funded by multiple USG agencies through multiple funding streams (as high as four); there was a concern that these organizations may not have the capacity to address the reporting needs of multiple funders (636-11-PCNGO; 636-21-USNGO).
Public–Private Partnerships
PEPFAR’s authorizing and reauthorizing legislation specified that public–private partnerships (PPPs) should be an element of the U.S. strategy against HIV/AIDS; in some cases these offer another way of making strategic use of partnerships and resources. PPPs are part of a “broader trend in global health and development practice that began in the 1980s” (Sturchio and Cohen, 2012, p. 1451). OGAC has created multiple partnerships across program areas and agencies that typically involve a 50–50 joint investment by the USG and a private-sector partner. The private-sector partner usually contributes expertise and in-kind resources such as training (Sturchio and Cohen, 2012). Some examples of PPPs that have introduced efficiencies or reductions in resource use are
• Supply Chain Management System (SCMS), managed by the Partnership for Supply Chain Management (a legal entity established by JSI Research & Training Institute, Inc., and Management Sciences for Health) is “a network of commercial private-sector organizations, nonprofits, academic institutions, and faith-based organizations with a wide range of capabilities [brought together] to expand and strengthen global supply chains for antiretrovirals, HIV test kits, laboratory supplies, and other products” (Sturchio and Cohen, 2012, p. 1452). In 2011, 71 percent of ARVs funded by PEPFAR were delivered by SCMS (SCMS, 2012).
• In 2012, PEPFAR, USAID, UNITAID, and the Bill & Melinda Gates Foundation partnered to increase access to a new rapid test to diagnose tuberculosis. Funding provided through this PPP reduces the cost of the rapid test for high-burden and developing countries by 40 percent for 10 years (through 2022) (OGAC, 2012b).
Conclusion: PEPFAR is increasingly emphasizing a range of efforts to use its resources more strategically and efficiently through the generation and use of economic and financial data; the allocation of resources based on anticipated impact; improved collaboration with partner country governments, other donors, and the Global Fund to align priorities and programs; and the streamlining of business processes. PEPFAR has started to see some gains from these efforts. Continuing to identify and implement opportunities for more strategic and efficient use of resources will be critical for making progress toward optimal return on investment in the response to HIV in partner countries.
The committee reviewed the overall PEPFAR funding process and data on PEPFAR funding over time as an important means by which to understand how the program is implemented and as a critical input for answering questions pertaining to the effects of PEPFAR-supported programs. The United States is the single largest donor to global HIV/AIDS efforts in the world, and between 2004 and 2011 the U.S. Congress appropriated more than $38 billion (current USD) for PEPFAR, of which $28.6 billion was designated for programs in partner countries. PEPFAR spending has been invested primarily, although not exclusively, in countries with low incomes and high disease burden.
Because of limitations in the available financial data, it is difficult to fully describe the distribution of the annual direct investment of PEPFAR in partner countries, to match the accounting budget codes to programmatic activities, and to follow the types of partners that ultimately receive the funding and implement PEPFAR-supported activities. This led the committee to conclude that PEPFAR would benefit from the collection and reporting of financial data that not only serve an accounting purpose but also are more closely aligned with programmatic data and program implementation. These data could thus be more easily and effectively used to understand and assess how PEPFAR is being implemented and the relationships between the amount and distribution of the investment and the targets and goals for PEPFAR-supported programs. PEPFAR has begun to take steps in this direction.
30-Day Notice. 2012. 30-Day Notice of Proposed Information Collection: Form DS–4213, PEPFAR Program Expenditures; OMB Control Number 1405–XXXX (notice of request for public comment and submission to OMB of proposed collection of information). Federal Register 77(153):47489-47490.
60-Day Notice. 2012. 60-Day Notice of Proposed Information Collection: Form DS–4213, PEPFAR Program Expenditures; OMB Control Number 1405–XXXX (notice of request for public comments). Federal Register 77(90):27266.
Bilimoria, N. F. 2012. Lessons learned from a decade of partnership between PEPFAR and the Global Fund: A case study from Tanzania. Health Affairs (Millwood) 31(7):1415-1421. CGD (Center for Global Development). 2008. PEPFARFundingData-fullDataset.xls. Washington, DC: CGD.
Donnelly, J. 2012a. PEPFAR’s broad guidelines for spending $1.5 billion backlog. http://www.globalpost.com/dispatches/globalpost-blogs/global-pulse/pepfars-broad-guidelines-spending-15-billion-backlog (accessed September 4, 2012).
Donnelly, J. 2012b. A Q&A with US Global AIDS Coordinator Eric Goosby. http://www.globalpost.com/dispatches/globalpost-blogs/global-pulse/qa-us-global-aids-coordinator-eric-goosby (accessed September 4, 2012).
Donnelly, J. 2012c. US reveals nearly $1.5 billion in unspent AIDS money. http://www.globalpost.com/dispatch/news/health/us-reveals-nearly-15-billion-unspent-aids-money (accessed August 17, 2012).
DoS OIG (U.S. Department of State Office of Inspector General). 2010. Audit of sources and uses of Global HIV/AIDS Initiative Global Health and Child Survival funds related to the President’s Emergency Plan for AIDS Relief (PEPFAR) for FYs 2007 and 2008. Report number AUD/SI-11-10. Washington, DC: U.S. Department of State and the Broadcasting Board of Governors Office of Inspector General.
El-Sadr, W., C. Holmes, P. Mugyenyi, H. Thirumurthy, T. Ellerbrock, R. Ferris, I. Sanne, A. Asiimwe, G. Hirnschall, R. Nkambule, L. Stabinski, M. Affrunti, C. Teasdale, I. Zulu, and A. Whiteside. 2012. Scale-up of HIV treatment through PEPFAR: A historic public health achievement. Journal of Acquired Immune Deficiency Syndromes 60(Suppl 3):S96-S104.
GAO (U.S. Government Accountability Office). 2005. Selection of antiretroviral medications provided under U.S. emergency plan is limited. GAO-05-133. Washington, DC: GAO.
GAO. 2011. PEPFAR program planning and reporting. GAO-11-785. Washington, DC: GAO.
GAO. 2012. President’s Emergency Plan for AIDS Relief—agencies can enhance evaluation quality, planning, and dissemination: Report to congressional committees. Washington, DC: GAO.
GHI (Global Health Initiative). 2012. Interagency paper on country ownership. Washington, DC: GHI.
Goosby, E. 2012a. An update from the Global Fund board meeting in Geneva. In DipNote: U.S. Department of State Official Blog. Washington, DC: U.S. Department of State.
Goosby, E. 2012b. The way forward: Maximizing our impact through shared responsibility and smart investments. Journal of Acquired Immune Deficiency Syndromes 60(Suppl 2):S44-S47.
Goosby, E., M. Dybul, A. S. Fauci, J. Fu, T. Walsh, R. Needle, and P. Bouey. 2012. The United States President’s Emergency Plan for AIDS Relief: A story of partnerships and smart investments to turn the tide of the global AIDS pandemic. Journal of Acquired Immune Deficiency Syndromes 60(Suppl 3):S51-S56.
Heniff, B. 2008. Overview of the authorization-appropriations process. CRS Report for Congress. Order Code RS20371.
Holmes, C. B., W. Coggin, D. Jamieson, H. Mihm, R. Granich, P. Savio, M. Hope, C. Ryan, M. Moloney-Kitts, E. P. Goosby, and M. Dybul. 2010. Use of generic antiretroviral agents and cost savings in PEPFAR treatment programs. Journal of the American Medical Association 304(3):313-320.
Holmes, C. B., J. M. Blandford, N. Sangrujee, S. R. Stewart, A. DuBois, T. R. Smith, J. C. Martin, A. Gavaghan, C. A. Ryan, and E. P. Goosby. 2012. PEPFAR’S past and future efforts to cut costs, improve efficiency, and increase the impact of global HIV programs. Health Affairs 31(7):1553-1560.
IOM and NRC (Institute of Medicine and National Research Council). 2010. Strategic approach to the evaluation of programs implemented under the Tom Lantos and Henry J. Hyde U.S. Global Leadership Against HIV/AIDS, Tuberculosis, and Malaria Reauthorization Act of 2008. Washington, DC: The National Academies Press.
Jamieson, D. 2011. Efficiency gains through smarter transportation and pooled procurement. Paper presented at PEPFAR’s Smart Investments to Save More Lives: Efficiencies, Innovation, Impact, Washington, DC, February 10.
Kates, J., and T. Summers. 2004. HIV/AIDS policy brief: U.S. government funding for global HIV/AIDS through FY 2005. Washington, DC: Kaiser Family Foundation.
Kates, J., A. Wexler, E. Lief, C. Avila, and B. Gobet. 2011. Financing the response to AIDS in low- and middle-income countries: International assistance from donor governments in 2010. Washington, DC: Kaiser Family Foundation and UNAIDS.
KFF (Kaiser Family Foundation). 2009. Fact sheet: The U.S. & the Global Fund to Fight AIDS, Tuberculosis, and Malaria. http://www.kff.org/globalhealth/upload/8003.pdf (accessed February 14, 2013).
OECD (Organisation for Economic Co-operation and Development). 2012a. DAC glossary of key terms and concepts. http://www.oecd.org/dac/glossary (accessed December 11, 2012).
OECD. 2012b. OECD.Stat (database). Paris: OECD.
OGAC (Office of the U.S. Global AIDS Coordinator). 2004. The Emergency Plan for AIDS Relief: Summary financial status as of September 30, 2004. Year one of implementation. Washington, DC: OGAC.
OGAC. 2005. Emergency Plan for AIDS Relief fiscal year 2005 operational plan: June 2005 update. Washington, DC: OGAC.
OGAC. 2006a. The Emergency Plan for AIDS Relief: Summary financial status as of September 30, 2005. Year two of implementation. Data represents all of FY 2004 and FY 2005 through Q4. Washington, DC: OGAC.
OGAC. 2006b. The U.S. President’s Emergency Plan for AIDS Relief fiscal year 2006: Operational plan. 2006 August update. Washington, DC: OGAC.
OGAC. 2007a. The Emergency Plan for AIDS Relief: Summary financial status as of September 30, 2006 (4th quarter—FY 2006). Data for FY 2004–2006 appropriations. Washington, DC: OGAC.
OGAC. 2007b. The President’s Emergency Plan for AIDS Relief: FY 2008 country operational plan guidance. Washington, DC: OGAC.
OGAC. 2007c. The U.S. President’s Emergency Plan for AIDS Relief fiscal year 2007: Operational plan. 2007 June update. Washington, DC: OGAC.
OGAC. 2008a. The Emergency Plan for AIDS Relief: Summary financial status as of September 30, 2007 (4th quarter—FY 2007). Data for FY 2004–2007 appropriations. Washington, DC: OGAC.
OGAC. 2008b. The President’s Emergency Plan for AIDS Relief: FY 2009 country operational plan guidance. Washington, DC: OGAC.
OGAC. 2008c. The U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) fiscal year 2008: PEPFAR operational plan. June 2008. Washington, DC: OGAC.
OGAC. 2009a. The Emergency Plan for AIDS Relief: Summary financial status as of September 30, 2008 (4th quarter—FY 2008). Data for FY 2004–2008 appropriations. Washington, DC: OGAC.
OGAC. 2009b. Guidance for PEPFAR partnership frameworks and partnership framework implementation plans. Version 2.0. Washington, DC: OGAC.
OGAC. 2009c. The President’s Emergency Plan for AIDS Relief: FY 2010 country operational plan guidance. Washington, DC: OGAC.
OGAC. 2009d. The U.S. President’s Emergency Plan for AIDS Relief: Five-year strategy. Washington, DC: OGAC.
OGAC. 2010a. The Emergency Plan for AIDS Relief: Summary financial status as of September 30, 2009 (4th quarter—FY 2009). Data for FYs 2004–2009 appropriations. Washington, DC: OGAC.
OGAC. 2010b. The Emergency Plan for AIDS Relief: Summary financial status as of September 30, 2010 (4th quarter—FY 2010). Data for FYs 2004–2010 appropriations. Washington, DC: OGAC.
OGAC. 2010c. The President’s Emergency Plan for AIDS Relief: FY 2011 country operational plan guidance. Washington, DC: OGAC.
OGAC. 2010d. The President’s Emergency Plan for AIDS Relief: FY 2011 country operational plan guidance appendices. Washington, DC: OGAC.
OGAC. 2010e. The U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) fiscal year 2009: PEPFAR operational plan. November 2010. Washington, DC: OGAC.
OGAC. 2011a. The Emergency Plan for AIDS Relief: Summary financial status as of September 30, 2011 (4th quarter—FY 2011). Data for FYs 2004–2011 appropriations. Washington, DC: OGAC.
OGAC. 2011b. The President’s Emergency Plan for AIDS Relief: FY 2012 country operational plan guidance. Washington, DC: OGAC.
OGAC. 2011c. The U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) fiscal year 2010: PEPFAR operational plan. April 2011. Washington, DC: OGAC.
OGAC. 2011d. The U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) Fiscal Year 2011: PEPFAR operational plan. December 2011. Washington, DC: OGAC.
OGAC. 2011e. The U.S. President’s Emergency Plan for AIDS Relief: Seventh annual report to Congress. Washington, DC: OGAC.
OGAC. 2012a. Countries. http://www.pepfar.gov/countries (accessed July 31, 2012).
OGAC. 2012b. Public-private partnership announces immediate 40 percent cost reduction for rapid TB test. http://www.pepfar.gov/press/releases/2012/196090.htm (accessed September 11, 2012).
OGAC. 2012c. Report on costs of treatment in the President’s Emergency Plan for AIDS Relief (PEPFAR). Washington, DC: OGAC.
OGAC. 2013a. Email communication between OGAC staff and IOM: “Follow-up to IOM questions for clarification.” Washington, DC: OGAC.
OGAC. 2013b. Email communication between OGAC staff and IOM: “IOM questions for clarification.” Washington, DC: OGAC.
OGAC. 2013c. Partners. http://www.pepfar.gov/funding/budget/partners/index.htm (accessed May 31, 2013).
OGAC. n.d. Collaboration with UNAIDS. http://www.pepfar.gov/partnerships/coop/unaids/index.htm (accessed January 14, 2013).
OMB (Office of Management and Budget). 2011. OMB circular No. A–11: Preparation, submission, and execution of the budget. Washington, DC: OMB.
PEPFAR (President’s Emergency Plan for AIDS Relief). 2012. Report on pilot expenditure analysis of PEPFAR programs in 6 countries. Washington, DC: OGAC.
Rosen, S. 2011. Innovations in costing health care delivery models: Boston University’s experience. Paper presented at PEPFAR’s Smart Investments to Save More Lives: Efficiencies, Innovation, Impact, Washington, DC, February 10.
SCMS (Supply Chain Management System). 2012. Six years of saving lives through stronger public health supply chains: A report on SCMS contributions to PEPFAR results. Arlington, VA: SCMS.
Sessions, M. 2006. Overview of the President’s Emergency Plan for AIDS Relief (PEPFAR). Washington, DC: CGD.
Sturchio, J. L., and G. M. Cohen. 2012. How PEPFAR’s public–private partnerships achieved ambitious goals, from improving labs to strengthening supply chains. Health Affairs (Millwood) 31(7):1450-1458.
UNAIDS (Joint United Nations Programme on HIV and AIDS). 2010a. Global report: UNAIDS report on the global AIDS epidemic 2010. Geneva: UNAIDS.
UNAIDS. 2010b. UNAIDS vision and mission. Geneva: UNAIDS.
UNAIDS. 2012a. AIDSinfo: Estimated HIV Prevalence. http://www.unaids.org/en/dataanalysis/datatools/aidsinfo (accessed September 24, 2012).
UNAIDS. 2012b. AIDSinfo: People living with HIV. Source: UNAIDS_Estimate_2010. http://www.unaids.org/en/dataanalysis/datatools/aidsinfo (accessed September 24, 2012).
United Nations. 2011. Population Division world population prospects: The 2010 revision, CD-ROM Edition. Geneva: United Nations, Department of Economic and Social Affairs.
White House Office of the Press Secretary. 2003. Fact sheet: The President’s Emergency Plan for AIDS Relief. http://georgewbush-whitehouse.archives.gov/news/releases/2003/01/20030129-1.html (accessed September 17, 2012).
World Bank. 2012. World Bank GNI per capita operational guidelines and analytical classifications. Washington, DC: The World Bank.