Important Points Made by Individual Speakers
- Reviews of the research evidence suggest that nutrition education is effective overall, even if it is not effective across the board in all individual studies and individual behaviors.
- The outcomes of nutrition education should be stated in behavioral terms, whether related to health, food systems, food safety, or other relevant issues.
- Nutrition education needs to enhance the motivation to act and facilitate the ability to engage in behaviors that promote and support health and food-related concerns.
- Between 40 and 50 hours of education are needed to change general knowledge, practices, and attitudes.
- Of all the institutions that influence eating behaviors, schools may have the greatest potential effect.
The development and implementation of national nutrition education curriculum standards would not occur in a vacuum. Two workshop presenters described research that they and others have done on past nutrition education and the lessons that can be drawn from that research.
LESSONS FROM PAST RESEARCH
Is nutrition education effective, or should attention be devoted primarily to changing access to food and the food environment to change eating behaviors? Isobel Contento, the Mary Swartz Rose Professor of Nutrition Education and Coordinator of the Program in Nutrition at Teachers College, Columbia University, summarized the results of past research to answer this question.
A recent meta-analysis by Waters et al. (2011), which looked at 55 studies of obesity prevention interventions in more than 27,000 children through age 18, found an overall reduction in body mass index of 0.15 kg/m2, with the greatest reduction (of 0.26 kg/m2) among children aged 0 through 5 years. The authors concluded that one of the promising strategies was school curriculum that includes healthy eating, physical activity, and body image. Similarly, a meta-analysis by Katz et al. (2008), which looked at the effects of nutrition education along with physical activity and a reduction in television watching in 10,752 children aged 5 through 18 in 8 separate studies, found significant reductions in body weight compared with controls, Contento noted. Subsets of the eight studies that were less comprehensive had smaller effects, but even these subsets were effective in reducing weight.
These meta-analyses found positive effects overall despite the fact that the results of individual studies in terms of specific behaviors related to energy-balance (and hence weight) have been mixed. These behaviors include consumption of sweetened drinks, snacks, fast foods, fruits and vegetables, as well as physical activity, or sedentary behaviors. Some studies have resulted in desired changes for some of these behaviors but not all, and others did so for one gender only or one particular age group.
A review of school-based fruit and vegetable interventions found a range of effect sizes, from medium to large (Howerton et al., 2007), though all the changes were positive. Interventions led by the researchers had a larger effect than those led by teachers, suggesting the importance of effective implementation of education programs. Furthermore, even relatively small changes in servings can represent a large effect if spread across millions of children, Contento observed.
Individual studies of fruit and vegetable consumption also have produced promising results. In a study of 15 interventions promoting children’s fruit and vegetable consumption, Knai et al. (2006) found that 9 of 11 elementary school programs and 1 of 4 high school programs were effective at significantly increasing daily consumption of fruit and vegetables by 0.3 to 0.99 servings. Moreover, three of the studies had effect sizes of between 0.7 and 0.9 servings.
Contento described an earlier systematic review she did of 40 studies of
children mostly in grades three through nine. Eight of 17 studies directed at general nutrition education were effective, while 18 of 23 directed at behavioral changes were effective at achieving behavior change (Contento et al., 1995). This is important, said Contento, because changing behavior is more difficult than changing knowledge and behavioral change should be the goal of nutrition education.
Finally, a meta-analysis of 12 meta-analyses found a positive effect on health behavior changes in eating and physical activity (Johnson et al., 2010).
“On balance,” Contento concluded, “reviews of evidence suggest that nutrition education is effective overall, even if it is not across the board in all individual studies and individual behaviors and the effects are often modest.”
Contento also included an older study because at that point the researchers were able to divide the studies between those that focused on general nutrition education topics versus studies that focused on specific behaviors. Whitehead (1973) did a systematic review of nutrition education with school-aged children conducted between 1900 and 1970 and identified several elements of effective programs:
- Changing behavior was clearly specified as the goal.
- Educational methods were appropriate to the goal.
- Individuals themselves were involved in problem solving.
- An integrated community approach was used.
Similarly, in a comprehensive and systematic review of 40 studies between 1980 and 1995 involving children primarily in grades three through nine, Contento and colleagues (1995) found that some behavior change was achieved in 18 of 23 behaviorally focused nutrition education interventions, but only in 8 of 17 studies directed at general nutrition education. This is important, said Contento, because changing behavior is more difficult than changing knowledge, and behavioral change (supported by knowledge and skills) should be the goal of nutrition education. This review concluded that the outcomes of nutrition education should be stated in behavioral terms (whether related to health, food systems, or food safety). Education standards tend to focus on knowledge rather than behaviors, Contento said.
Elements contributing to the effectiveness of nutrition education include
- Eating and educational strategies based on both theory and evidence, including
ο Cognitive dimensions (involving concepts and skills),
ο Affective dimensions (involving motivations, beliefs, values, and emotions), and
ο Behavioral dimensions (involving personalized self-assessments, decision making, and behavioral-change strategies).
- Adequate duration and intensity (Box 3-1 discusses the critical issue of how much nutrition education is needed to change behaviors.)
- Sequential and coherent
- Involve intervening in the school environment
- Parent involvement, particularly for younger children
- Community involvement
- Coordinated with the school curriculum and school meals
Box 3-2 looks at the National Health Education Standards as a model for national nutrition education standards.
Katz et al. (2008), Knai et al. (2006), and Waters et al. (2011) also derived lists of promising policies and strategies, from which Contento abstracted several elements that are common to all the lists:
- Curricula should focus on healthy eating and physical activity.
- Specific behaviors should be the goals.
- Programs should be active and participatory and include exposure to healthy food.
- Attention should be devoted to cultural and diversity issues.
- Teachers need to be given support.
- Schools, families, and communities should be involved.
In general, she said, these elements constitute a social ecological model for both individuals and the environment (Contento, 2010). Nutrition education needs to enhance the motivation to act and facilitate the ability to engage in behaviors that promote and support health and food-related concerns. Cerin et al. (2009), in a review of seven school-based interventions that fit their criteria, found that effective mediators of behavioral change were beliefs about outcomes (which affected motivations), behavioral-change and goal-setting skills (which helped students change behaviors through enhanced self-efficacy) and habit. Nutrition education also needs to provide a universe of concepts and skills while fitting with the educational mandates and the needs and constraints of teachers, including the time limits on nutrition education. “Obviously, we have a lot of challenges,” Contento said.
Enhancing motivation involves knowledge, values, attitudes, and social norms. People may have outcome expectations based on scientific evidence, but they also can be motivated by risks, concerns, preferences, attitudes, and self-efficacy. Similarly, people need food- and nutrition-related knowledge and skills to act, but they also need self-regulation skills in such areas as self-assessment, decision making, planning, and self-monitoring.
Finally, Contento described what nutrition education programs look like in practice. Accessibility to healthy foods is important but is not enough. As an example, she cited Cookshop, which is an ongoing program in 500 schools. In the initial effectiveness study, when provided with whole grains and vegetables, only those students who received nutrition education in the classroom, and particularly cooking instruction, improved their eating (Liquori et al., 1998). In another study, younger children who received plates of vegetables and fruit were more likely to consume those foods if they also received cartoons of children their age eating those foods along with stickers for eating them. Even after the cartoons and rewards were stopped, the targeted children were eating more fruits and vegetables 6 months later (Horne et al., 2004). “They needed something to get them to become familiar with the fruits and vegetables, and then once they were familiar [with] them, the behavior seemed to continue.”
People who are directly involved with nutrition have large stores of nutrition science knowledge, and “we love all that information,” said Contento. As a result, they often try to include as much information as possible in introductory nutrition education presentations and lessons. While their enthusiasm for the subject is laudable, the developers of nutrition education standards will need to be careful not to include too much specific nutrition science information. Rather, the standards need to enhance motivation to act and facilitate the ability to act on behaviors that promote and support health and other food-related concerns. Standards can be comprehensive while still avoiding too much detail. Contento argued for an emphasis on functional knowledge—information that people can use to change behaviors, such as knowing how much sugar a particular beverage contains. “Our teachers are going to have less time, and they need to have information that is going to be practical.” Also, the integration of nutrition education into other subjects will be different in elementary schools, where topics are more integrated, than in middle and high schools.
An issue that came up in the discussion following Contento’s presentation is how to define nutrition education. The word nutrition technically covers the entire diet, but it also can be interpreted to refer specifically to nutrients. One possibility would be to refer to food and nutrition education. Another possibility is to refer to food literacy, which could be interpreted to include physical activity.
SCHOOL-BASED NUTRITION INTERVENTIONS: FINDINGS FROM THE LITERATURE
Between the ages of 5 and 17, 95 percent of children and adolescents are educated by U.S. schools (U.S. Census Bureau, 2011). Of all the institutions that influence eating behaviors—including government, industry,
BOX 3-1
How Much Time Should Be Spent on Nutrition Education?
In her presentation, Contento suggested that between 40 and 50 hours of nutrition education may be needed for that education to be effective. This number comes from a study done by Connell et al. (1985) of more than 1,000 classrooms in which four model curricula were tested on 30,000 students in grades four through seven (see Figure 3-1). Evaluation instruments found that program-specific knowledge increased substantially during the first 15 hours of classroom instruction, but general knowledge, practices, and attitudes did not increase to their maximal levels until after 40-50 hours of classroom instruction. In contrast, the School Heath and Programs Study of 2006 found that nutrition and dietary behavior topics consume a median of 3.4 hours in elementary schools, 4.2 hours in middle schools, and 5.9 hours in high schools (Kann et al., 2007). The total hours will be somewhat greater. Other studies have found 8-12 hours devoted to nutrition education.
As was observed later in the workshop, the typical school year includes about 1,000 hours of instruction. Nutrition education may need 40-50 hours of time to have optimal effects, but if other subjects outside of the standard curriculum require comparable amounts of time, teachers may be hard pressed to include everything they are asked to include. Thus, some of the hours may need to come from other school venues.
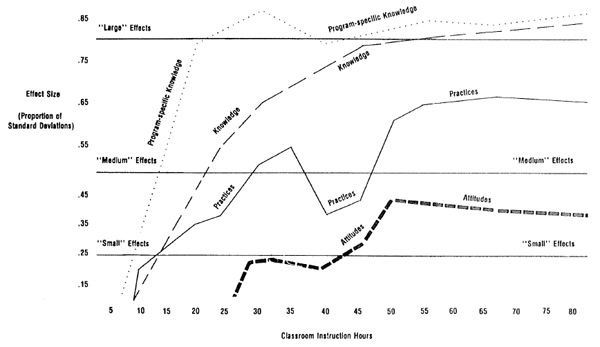
FIGURE 3-1 Knowledge, practices, and attitudes do not undergo large changes until after 40-50 hours of instruction. SOURCE: Connell, D. B., R. R. Turner, and E. F. Mason. 1985. Results of the School Health Education Evaluation: Health promotion effectiveness, implementation, and costs. Journal of School Health 55(8):316-321. Reprinted with the permission of the Journal of School Health.
BOX 3-2
The National Health Education Standards
Contento called attention to the National Health Education Standards as a model for the development of nutrition education standards. These standards call for the following:
- Comprehend concepts related to enhancing health.
- Analyze the influences of family, peers, culture, media, and technology on health behaviors.
- Access and analyze valid information, products, and services to enhance health.
- Use interpersonal communication skills to enhance health, reduce or avoid health risks, or both.
- Use decision-making skills to enhance health.
- Use goal setting to enhance health.
- Practice behaviors to reduce risk and promote health.
- Promote and support personal, family, and community health.
Also associated with the National Health Education Standards are a Health Education Curriculum Analysis Tool, which includes a healthy eating module (CDC, 2007), and guidelines for school programs to promote lifelong healthy eating. The guidelines cover the following:
- School policy on nutrition;
- Curriculum: preschool through secondary school as part of a sequential coordinated school health education curriculum designed to help health students adopt healthy eating behaviors;
- Instruction for students: developmentally appropriate, culturally relevant, fun activities that involve social learning strategies;
- Integration of school food service and nutrition education;
- Training for school staff;
- Family and community involvement; and
- Program evaluation.
SOURCE: CDC, 1997.
and the media—schools may have the greatest potential effect, said Mary Roseman, associate professor in the Department of Nutrition and Hospitality Management at the University of Mississippi.
In 2011, Roseman and two colleagues published a content analysis of 26 K-12 school-based nutrition interventions (Roseman et al., 2011). They used 12 school-based nutrition intervention reviews published between 1995 and 2000 to derive 10 general recommendations for school-based nutrition interventions, and then they used those 10 recommendations to
TABLE 3-1 Components of the School-Based Nutrition Interventions
|
|
|
| Component | Percentage |
|
|
|
| Incorporating classroom curriculum | 85 |
| Involving parents at home | 62 |
| Training teachers on classroom nutrition education | 42 |
| Disseminating physical education materials | 42 |
| Increasing fruits and vegetables | 38 |
| Providing incentives for students or families | 38 |
| Lowering fat | 31 |
| Training school nutrition staff | 31 |
| Involving student peers | 27 |
| Establishing physical activity goals | 27 |
| Establishing school food service guidelines | 15 |
| Providing school incentives | 12 |
| Involving parents at school | 8 |
|
|
|
| SOURCE: Roseman et al., 2011. | |
analyze 26 new studies of obesity- or health-related school interventions published between 2000 and 2008. These 26 studies had many differences and used a wide variety of approaches (see Table 3-1), but collectively they provide a valuable overview of what has been done in the past.
At the workshop, Roseman stepped through the 10 recommendations and examined their relevance to possible future nutrition interventions:
- Nutrition interventions are most effective when they are behaviorally focused. All of the 26 interventions studied were behaviorally focused, despite many other differences in the studies. Eighty-five percent had both knowledge-based and behaviorally focused components of school-based nutrition interventions, whereas 15 percent were focused on behaviors only.
- The use of multicomponent interventions that address multiple influences on health behavior is important. Eighty-eight percent of the studies addressed multiple components, but relatively few—only 27 percent—included physical activity goals. “I think we all would like to see that a bit higher,” Roseman said.
- Healthful changes in the food and school environment can improve behavior changes at the population level. These changes may affect lunch and breakfast programs, à la carte food, vending machines,
school stores, marketing, and advertising but seemingly smaller changes also make a difference, Roseman noted, such as educators eating with their students to set good examples and recognition and rewards for students based on their fruit and vegetable consumption.
4. Family involvement enhances the effectiveness of school-based programs. Family involvement was common—in 62 percent of the interventions—but Roseman also pointed to the difficulties involved in working with families. Nevertheless, families are critical because of their influence on what is eaten at home, how much physical activity takes place, and what kinds of role models exist for students.
5. Incorporation of student self-assessments containing a feedback component is effective in middle school or older students. Such assessments occurred in a third of the studies of middle and high school students. Especially important is teaching children how to assess their diet and how to make appropriate changes to create an improved diet.
6. Inclusion of quantitative evaluation measures that capture food-related behaviors, eating patterns, and anthropometric measures is important. The studies used a variety of evaluation methods, which tend not to be standardized, resulting in large variations in reporting across the studies. Roseman also emphasized the value of qualitative data, including interviews of students, staffs, and faculty; parent interviews; and focus groups.
7. Interventions with links to the larger community can enhance school nutrition interventions. Such involvement occurred in only 15 percent of studies, but several valuable models for such links exist, such as the community and school health program model provided by the Centers for Disease Control and Prevention.
8. More studies should include ethnic and cultural groups to determine effective strategies and approaches for specific groups versus using entire school populations. Only 15 percent of the studies looked at ethnic groups. In general, the literature lacks studies of minorities, Roseman noted.
9. Use of innovative multimedia technology tools may enhance children’s engagement in the intervention. Children are proficient with new technologies—which were incorporated in about one-third of the studies—and these technologies offer many potential benefits, ranging from Web-based instruction to celebrity videos to excite and motivate children.
10. Nutrition education should be sequential, with sufficient duration and intensity, and include developmentally appropriate strategies. Forty-two percent of the interventions studied extended for at least 6 months, but challenges in this area are great in the school environment, and more consistent and effective reporting and methods are needed.
Of the 26 nutrition interventions covered by the study, they were conducted in only 16 states, and 4 states—California, Florida, Minnesota, and North Carolina—had multiple interventions (see Figure 3-2). Only one intervention published in the 9-year period from 2000 to 2008 came from one of the 8 states (NSCH, 2007) with the highest obesity rates among youth ages 10 to 17. According to Roseman, this observation may suggest a lack of funding for new researchers trying to enter the field.
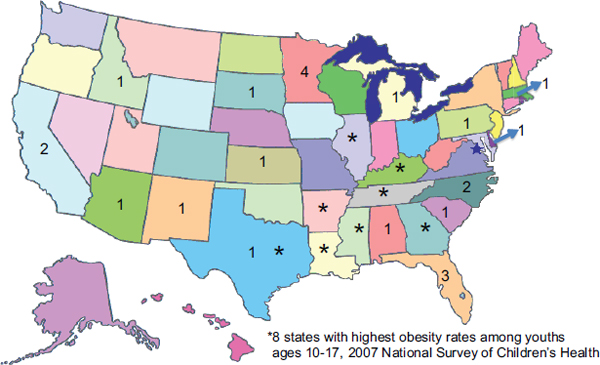
FIGURE 3-2 Eighteen of 26 nutrition interventions occurred in just 16 states and in only 1 of the 8 states with the highest obesity rates among youth.
NOTE: Data on interventions from Roseman et al., 2011 (Table 1). Eight of the 26 interventions studied did not report state information.
SOURCE: Roseman, 2013.












