8
Monitoring Children’s Mental Health After Disasters
Highlights of Points Made by Individual Speakers
- Anyone who interacts with children after a disaster can be a potential source of assistance and support. However, if they are unprepared or insensitive, they can be a source of further distress.
- A single disaster event is really part of a cascade of other events in a child’s life and results in cumulative impact and stress, even if the prior events are completely unrelated.
- Stigma related to mental health is a still barrier, even in times of national crisis.
- Between 30 and 40 percent of a direct survivor population are at risk for developing a new disorder that they did not have until the index event.
- Traumatic grief is different from the experience of grief in other situations and requires different treatment.
Supporting the mental and behavioral health needs of children in disasters was a recurring statement throughout the workshop. The speakers in this section of the report focused on heightened triage and targeting of vulnerable children for intervention more than demonstrating effective interventions. However, it should be noted that there are not enough data in this area to prove interventions are successful after traumatic events. Definitive guidance requires far more research on the comparative effectiveness of interventions targeting children exposed to traumatic events (Forman-Hoffman et al., 2013). Although earlier chap-
ters covered some of the behavioral health implications for local planners, this section goes deeper into mental health needs and manifestations in children during their recovery period. In addition to a focus on coping and post-disaster processing, there is also the presentation of a tool that schools and other organizations can use to monitor and triage mental health needs in their population.
ENSURING THAT CHILDREN ARE COPING
David Schonfeld, director of the National Center for School Crisis and Bereavement, shared his list of key points for short-term mental health response for children. First, pediatric health care providers play a critical role in the mental health response to disaster. On a daily basis, pediatricians and other pediatric primary care providers are the de facto mental health providers for children in this country. Children are most likely to receive treatment from their primary care physicians for mental health disorders and psychosocial problems, which Schonfeld noted are actually the most common chronic conditions seen in pediatric practices. In the aftermath of a disaster, primary care providers are likely to be the first, and possibly the only responders to provide mental health services to children.
Adults who work with children should understand the likely reactions to disaster and know techniques to help them cope, Schonfeld continued. This includes psychoeducation and supportive services to accelerate the natural healing process. Different types of staff have different relationships with children and can offer different perspectives. As an example, Schonfeld noted that it was cafeteria workers who noticed that girls had been cutting themselves in reaction to a school shooting in which a classmate was killed. They could see this because the girls’ long sleeves would pull back as they reached out with their lunch trays to be served, revealing the cuts on their arms. Anyone who interacts with children after a disaster can be a potential source of assistance and support but, unfortunately, he said, if they are unprepared or insensitive, they can be a source of further distress.
Helping children necessarily includes helping their families and communities as well. For example, parents may need help to take care of themselves in order to be able to be more available to take care of their children. Helping children also means helping health care providers to fulfill their roles. Professional staff members have their own basic needs,
and crisis preparedness and response plans need to consider the professional’s needs as a priority. These professionals may be impacted directly themselves and may have some of the same behavioral and mental health needs as those they serve. Professional self-care is important, but is often neglected. It is distressing to be with children who are in distress. It is critical that staff find ways to have their own personal needs met, and appreciate and address the impact of supporting children who are grieving or traumatized.
Understanding the Timeline of Recovery
Beyond the immediate response, we need to appreciate the timeline for recovery, Schonfeld said. Everyone has a baseline level of function with some highs and lows (see Figure 8-1). When a disaster event occurs people feel vulnerable, their usual coping mechanisms may fail, and they may feel helplessness and hopelessness. As communities respond and provide resources, people start to have improved functioning. This is still a vulnerable period, Schonfeld stressed. Some individuals continue their recovery and return to their baseline functioning, and some even have “posttraumatic growth” and achieve a new baseline of even higher level functioning. But others never return to their original baseline and live in a state of continued impairment. There is often an increase in suicides in this period. Unfortunately, Schonfeld said, children are thought of as “resilient” and support is often withdrawn as soon as there are signs of recovery. Instead, they need to be supported until they return to their baseline level of functioning.
The scope of need is broad, and there is a wide range of reactions and concerns beyond the acute trauma and posttraumatic stress from a disaster. For some children, bereavement is a primary issue if they have lost someone close to them. Other children face a cascade of secondary losses and stressors such as loss of their homes and relocation, loss of their peer network, difficulty integrating into new social networks or bullying at their new school, academic failure, financial stresses on the family, and parental stress, depression, substance use, or increased domestic violence. Schonfeld also pointed out that a single disaster event is really part of a cascade of other events in a child’s life and results in cumulative impact and stress, even if the prior events are completely unrelated. When responding to one event, we are responding to all of the events in the life of the child. As an example, Schonfeld said that after a
busload of children went through a decontamination process for minor exposure to a noxious substance, most children retuned to baseline functioning rapidly, but two girls continued to display significant stress. Further investigation revealed that one had recently seen a family member murdered and the other was being abused at home. Schonfeld also suggested that health care providers need to alter their practice patterns to include trauma history in the overall patient history.
Psychosocial Needs and Stigma
Another point Schonfeld raised is that stigma related to mental health is a still barrier, even in times of national crisis. Parents may not seek assistance because they often underestimate symptoms in their children, or they assume the children are just having normal reactions to abnormal events and professionals would not be interested. Children may withhold complaints because of concerns that they are abnormal, or they want to protect their parents who are visibly upset.
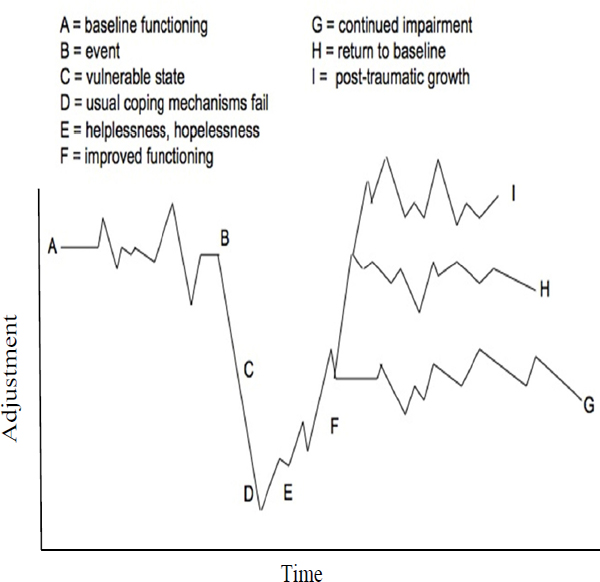
FIGURE 8-1 Adjustment over time in a crisis situation.
SOURCE: Schonfeld presentation, June 11, 2013.
Schonfeld reemphasized the work of the National Centers for Disaster Medicine and Public Health which is developing online training materials that can be used more broadly by the general public, including a module on attending to the psychosocial needs of children. He also mentioned a project with the American Federation of Teachers, the National Education Association, the National Association for School Psychologists, and others, to create materials that would be disseminated to all of their memberships. There are many materials being developed, but facilitating the dissemination and uptake of those materials is a challenge, and he recommended working through professional organizations. Roth urged that the training materials being developed also be made accessible for those with varying needs (e.g., captions on video materials, e-book device accessible).
Merritt Schreiber, director of psychological programs at the Center for Disaster Medicine of the University of California, Irvine, School of Medicine, described a national children’s disaster mental health concept of operations (NCDMH CONOPS) that he developed with funding from the Terrorism and Disaster Center of the National Child Traumatic Stress Network (Schreiber, 2011).
A very large subset of people, including children, experience transitory distress (e.g., insomnia, fears of recurrence, fears of separation). For many, resilience happens without any intervention. However, between 30 and 40 percent of a direct survivor population are at risk for developing a new disorder that they did not have until the index event (posttraumatic stress disorder [PTSD] being the most common). The concept of operations is designed to get to that high-risk subject in a timely way, and offer them evidence-based interventions that have been shown, through randomized controlled studies, to have an impact. The goal is a seamless continuum of triage-to-care incident operation. Schreiber said that there is a critical window at 30 to 45 days post-event in which intervention can reduce or even prevent clinical PTSD. Timely intervention may also reduce the secondary mental health burden on both emergency departments and primary care settings.
Included in the NCDMH CONOPS is the PsySTART Rapid Mental Health Triage and Incident Management System. PsySTART does not measure symptoms (as symptom measurement in acute aftermath of an
event is often unreliable) and is not a diagnostic measure. Rather, it measures exposure, traumatic loss, early emergence of potentially ongoing or persistent stressors, disaster-related injury and illness, and peri-traumatic panic. A triage form prompts staff to collect information from individuals about their experiences (e.g., psychological panic symptom, direct life threat, exposure, trapped, saw bodies, had direct loss of loved ones, home loss). The responses help identify which patients need to be seen first.
Aggregated individual PsySTART data can be used to estimate site-level and population-level impacts of a disaster and develop a total picture of risk (types, locations, number of children at risk). Geographic information system mapping of data from multiple sites enables a common operating picture and near-real-time situational awareness of children’s mental health needs. This is then used to guide incident management, define needs, allocate resources, and facilitate interagency coordination. Schreiber noted that a PsySTART mobile app has recently been developed.
In closing, Schreiber referred participants to another resource from the National Child Traumatic Stress Network, a trauma-focused cognitive behavioral therapy online training course.1 He described it as a high-end intervention for the very-high-risk subset who are not likely to progress to resilience without intervention. Traumatic grief is different from the experience of grief in other situations, he said, and requires different treatment. Triaging high-risk children, while also taking into account important trauma histories and exposure to other incidents can be instrumental in ensuring that children progress through a recovery of timeline along with their peers, and return to their normal baseline after an event or reach further growth potential.
___________________
1Available at http://tfcbt.musc.edu (accessed September 9, 2013).






