Immunological Mechanisms of Disease and the Multiple Chemical Sensitivity Syndrome
William J. Meggs
INTRODUCTION
The Multiple Chemical Sensitivity Syndrome (MCS) is a highly controversial illness which afflicts an unknown number of people. The very existence of this syndrome is questioned, but it is dear from the experience of physicians from several specialties that a population of patients exists that goes to great lengths to avoid a group of odorous organic chemicals at levels that are known to occur in contemporary homes, schools, and offices. These chemicals include the products of combustion, cleaning products, fragrances, pesticides; outgassing from synthetic materials used for clothing, furnishing and building products and are commonly found in the indoor air.
This type of sensitivity is colloquially called "allergy" but differs from traditional allergic reactions. At the present time the mechanism of this intolerance of chemicals is as controversial as the syndrome itself, but it is important to consider hypothetical mechanisms at this early stage of scientific scrutiny. Some say there is not scientific evidence that this syndrome exists, but the syndrome exists bemuse the patient population exists, and in extreme cases these people are disabled and no longer able to function productively in society. What is expressed by disclaimers is a belief that the mechanism of the syndrome is a mental disturbance such as somatization, and at this stage the somatization hypothesis is one of several to be considered by investigators designing clinical research protocols.
This article will discuss proposed and hypothetical immunological mechanisms for the Multiple Chemical Sensitivity Syndrome. In the next section, descriptions of this syndrome will be discussed, and the syndrome will be described in terms of a chemical stress syndrome. Known immunological mechanisms for the pathophysiology of established diseases will then be discussed and compared with MCS to see if any are feasible explanations. Finally, the hypothesis that the mechanism of MCS involves neuroimmunology, the interplay between the immune and nervous systems, will be presented.
DESCRIPTIONS OF THE MULTIPLE CHEMICAL SENSITIVITY SYNDROME
An option that exposure to environmental organic chemicals could lead to illnesses was expressed in 1962 in a short book, Human Ecology and Susceptibility to the Chemical Environment, written by a Chicago allergist (Randolph, 1962). The characterization of this illness is presented in Table 1, and this type of sensitivity was presented as being distinct from classical allergic sensitization. Notable features of this description include an adaptation phenomenon, with: (a) sensitive individuals having chronic symptoms while living in the chemical environment which resolve several days after removal from the chemicals, (b) withdrawal symptoms upon removal and (c) "shock reactions" when these individuals are reexposed to chemicals. Patients affected by this disorder have a variety of physical and mental illnesses which can be managed by avoiding incriminated chemicals. A spreading phenomenon was described in which affected individuals become progressively sensitive to more and more chemicals found in indoor air, water, and foods. A set of chemicals which were found in clinical practice to cause illness in some patients is given in Table 2. This work was presented as an opinion based upon the clinical practice of having patients avoid chemicals and foods using trial and error, and no scientific data such as double-blinded studies were presented to substantiate this point of view.
TABLE 1
|
Randolph's Description of Chemical Sensitivity Disease |
|
Acquired, often after chronic insidious or acute exposure to a petrochemical. |
|
Chemical exposures trigger physical (arthritis, asthma, colitis, etc.) or mental (depression, difficulty with concentration, mania, psychosis, etc.) symptoms. |
|
Specific Adaptation Syndrome. Adaptation to specific chemicals with chronic exposure is followed by maladaptation and chronic illness, withdrawal symptoms when removed from the chemical environment, and "shock reactions" on reexposure. |
|
Spreading phenomena. As an individual becomes maladapted to the chemical environment, intolerance to increasing numbers of environmental chemicals develops. |
|
Avoidance. By avoiding the chemical environment, chronic illnesses may resolve. |
A case definition of the Multiple chemical Sensitivity Syndrome based on the experience of occupational medicine specialists around the country has been presented (Cullen, 1989). Table 3 gives the seven criteria presented in this case definition. Common of Tables I and 3 shows considerable overlap, and a discussion of the relationship between the two will be given below.
An operational definition of MCS has been given (Ashford and Miller, 1989, 1991),
TABLE 2
|
Chemicals Alleged to Cause Reactions in chemically Sensitive Individuals (From Randolph, 1962) |
|
Indoor air contaminants |
|
utility gas |
|
coal smoke |
|
fumes from fresh paint, turpentine, mineral spirits, detergents |
|
fragrances from toiletries and perfumes |
|
cleaning products such as bleach, ammonia, disinfectants |
|
inspect sprays and repellants |
|
odorous synthetic carpets, pads, adhesives, and building materials |
|
Outdoor air contaminants |
|
automobile and diesel exhaust |
|
industrial air pollutants |
|
paint manufacturing and sulfur-processing fumes |
|
fumes from roof tar and roads |
|
Chemical additives and contaminants of food and water |
|
insecticides and fumigant residues |
|
some chemical preservatives |
|
sulfur residues |
|
chemical flavoring and sweetening agents |
|
plastic conformers and lined tins |
|
chloride in water |
|
Synthetic drugs, cosmetics, and miscellaneous chemicals |
|
medications, including aspirin, sulfonamides, synthetic vitamins |
|
allergic extracts or other biologic materials that contain phenol |
|
cosmetics |
|
synthetic textiles |
|
bed linens washed with detergents, dried in gas driers, or impregnated with |
|
synthetic starch or sizing |
that "The patient with multiple chemical sensitivities can be discovered by removal from the suspected offending agents and by revenge, after an appropriate interval, under strictly controlled environmental conditions. Causality is inferred by the clearing of symptoms with removal from the offending environment and recurrence of symptoms with specific challenge."
A description of this syndrome is best given in the context of what we call the "Hypothetical Chemical Stress Syndrome", a concept which is not original and draws heavily on the work of others (Selye, 1946; Randolph, 1962). The word "hypothetical" is used because at the present time there is insufficient data to establish a consensus about the role
TABLE 3
|
Examples of Host Responses that Must Also Be Considered Immunological |
|
Endothelial cell reactions |
|
Activation of C cascades in the absence of antibody |
|
Activation of procoagulant activity |
|
Acute phase reactant responses |
|
Aracidonic acid metabolism |
|
NK cell enhancement |
|
Lysosomal enzyme release |
|
Generation of toxic oxygen radicals |
|
IL-1 effect on the hypothalamus |
|
Beta-endorphin activity |
|
Generation of neuropeptides |
of this syndrome in human disease. The word "chemical" is used because our focus is on the stress of exposure to environmental chemicals, though some would argue that emotional and other stresses eau "cross react" with chemical exposures.
The stages of the Hypothetical Chemical Stress Syadrome (HCSS) are given in Figure One. Individuals in Stage 0 tolerate chemical exposures without difficulty. Progression from Stage 0 to Stage 1 occurs when an individual is chemically stressed either by an acute high-dose chemical exposure, or by a chronic insidious exposure. Individuals in Stage I have symptoms on exposure to chemicals, but no physical findings on physical examination. Hence, Stage 1 is the "-algia" stage, with-algia being the Greek suffix used in medicine to denotes pain; e.g., arthralgia denotes joint pain while myalgia denotes muscle pain.
Stage 2 is reached when an individual develops loci of inflammation from chemical exposures. It is at this stage that both findings on physical examination appear and a medical diagnosis can be given. The specific medical diagnoses which might be amenable to this approach are discussed elsewhere in these proceedings (Meggs, 1991). This stage is referred to as the "-itis" stage, with-itis being the Greek medical suffix denoting inflammation. Arthritis is inflammation of joints, myositis is inflammation of muscle, and so forth. The progression from Stage I to Stage 2 again follows increasing chemical exposures, and if tissue damage has not occurred, the inflammation can be reversed by removal of the chemical stimuli. That is, progression between Stages 1 and 2 is a two way process, with progression from Stage 2 to Stage 1 being possible if chemicals are avoided. The inflammation of Stage 2 can be reduced by medications such as corticosteroids and the non-steroidal anti-inflammatory agents, but these medications are not curative. If the chemical stimuli are not removed, there is immediate relapse of inflammation. Further, these medications do not prevent the progression from Stage 2 to Stage 3.
Stage 3 occurs if an individual suffers damage to tissue, so this stage can be
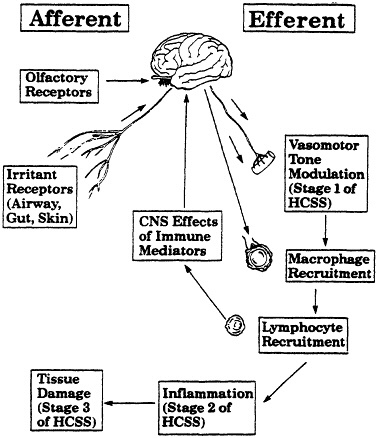
Figure 1 Hypothetical chemical stress syndrome.
characterized by "-osis". In medicine, the Greek suffix-osis denotes a change in living tissue; e.g., necrosis means death of tissue and fibrosis means the replacement of functional tissue by scar tissue. Unfortunately, once tissue is damaged there is little hope in current medical practice for a reversal, and organ function is lost.
Generally, the progression into Stages 2 and 3 occurs in one organ system, such as the skin, joints, or lungs. Later, a second organ system may become involved. It may still be important to remove an individual who has reached the irreversible tissue damage of Stage 3 from the chemical environment because it may be that inflammation can occur in other tissues.
What many clinicians call the Multiple Chemical Sensitivity Syndrome is Stage 1 of the Hypothetical Chemical Stress Syndrome. These patients have multiple complaints which they attribute to chemical exposures, but little if any findings on physical examination. Hence, it is easy to regard these patients as having a somatization disorder with no real medical illness. It is important that studies of adverse reactions to environmental chemicals include patients with diagnosable medical conditions, that is Stage 2 and 3 patients, and that the hypothesized progression between these stages be studied. In this regard, longitudinal studies will be very important.
The concept of a stress syndrome was originally introduced as the "Generalized
Adaptation Syndrome" to explain observations in animal models of disease (Selye, 1946). In this syndrome, laboratory animals exposed to stresses progress through stages of adaptation similar to the stages described above. The syndrome was initially discovered while exposing animals to chemical stresses, and the word "generalized" was introduced in the name of this syndrome because other stresses, for example the stress of confinement, was observed to lead to similar results.
The "Specific Adaptation Syndrome" has been described in humans to differ from the "Generalized Adaptation Syndrome" in that maladaptation can occur to one specific stress, in particular a single chemical (Randolph, 1962). The extent to which these stress syndromes are equivalent can be debated, but in any event they are very similar. The purpose of formulating the Hypothetical Chemical Stress Syndrome is to develop a specific hypothesis for studying adverse reactions to environmental chemicals such as those found in the indoor air.
IMMUNOPATHOGENESIS OF DISEASE AND CHEMICAL SENSITIVITIES
It is well known that the interaction of the immune system with environmental chemicals can cause disease. In this section, the known immunological mechanisms of disease will be reviewed, and their possible relationship to the multiple chemical sensitivity syndrome will be discussed. The function of the immune system is to protect the organism from invasion by pathogens such as bacteria, fungi, viruses, and parasites. It is known that the immune system has different arms, or branches, as listed in Table 4, which are recruited to deal with different types of pathogens. We know that these branches are distinct and recent investigations suggest that activation of one branch can actually deactivate another (Moore et al., 1990).
TABLE 4
|
Branches of the Immune System and Their Function |
|
|
Branch |
Function |
|
IgE-eosinophil system |
Destruction of tissue parasites |
|
IgG-neutrophil/macrophage system |
Destruction of encapsulated bacteria |
|
lymphocyte system |
Destruction of fungi and viruses |
|
IgA-secretory system |
Destruction of pathogens at mucosal surfaces |
Further, activation of the immune system can lead to inflammation, disease, and tissue damage. IgE mediated reactions arise when foreign proteins or low molecular weight compounds such as drugs bound to foreign proteins interact with IgE bound to the surface of mast cells to release histamine and other immune mediators, leading to the classical allergic reactions to foods, aeroallergens, pharmaceuticals, and insect venoms. Clinical manifestations of these reactions are asthma, urticaria, rhinitis, anaphylactic shock, or gastrointestinal problems. Some of the mediators released in allergic reactions are chemotactic factors, that is, they attract white blood cells into the tissues. Some patients with MCS report flushing and itching after chemical exposures, and a minority of patients report that they developed classical allergic disease after the onset of MCS. These anecdotes do not change the fact that MCS is distinct from classical allergy, as originally stated by Randolph.
Immune complexes are high molecular weight aggregates of antigen and antibody which can deposit in vessel walls, activate complement, and lead to inflammation and tissue damage, with serum sickness being the classical and experimental form of immune complex disease. The clinical picture of serum sickness is distinct, with fever, urticaria, fatigue and malaise, arthritis, and sometime renal failure. Immune complexes have been associated with autoimmune diseases and a host of other clinical conditions (Cochran, 1988). While they do not. play a role in MCS, they may play a role in stage 2 and 3 illnesses of fag. 1 related to chemicals.
Delayed type hypersensitivity, also sometimes referred to as cellular immunity and mediated by T-lymphocytes, can lead to inflammatory changes in tissues after a sensitizing exposure followed by reexposure. The initial exposure leads to antigen-specific T-cells which become activated on reexposure and release cytokines. Experimentally this is most commonly demonstrated in the skin, and contact dermatitis in humans arising from organic chemicals is mediated by cellular immunity. Of the known types of immune reactivity, cellular immunity is the one most likely to play a direct role in adverse reactions to environmental chemicals. The delayed or withdrawal nature of the inflammatory symptoms described in these patients is similar to the delay seen in cellular inflammation. Two of the interleukins (IL-1 and IL-2) are known to have effects on the central nervous system (Obal et al., 1990 and De Sarro et al., 1990). Several authors have claimed abnormalities of cellular immunity in these patients, such as alterations of helper and suppressor ratios and the presence of activated lyumphocytes in peripheral blood, as discussed below.
There are at least theoretical analogies in immunology to the spreading phenomena discussed for patients with multiple chemical sensitivities. The concept of an environmental adjuvant has been introduced to describe substances which induce an immune response to other substances. In immunology, an adjuvant is a substance which potentiates an immune response to other substances. An example of an adjuvant is alum, for an animal injected with alum mixed with a protein will begin producing IgE specific for the protein. Examples of inhaled environmental adjuvants in experimental models include sulfur dioxide, which can induce allergic asthma to co-administered aeroallergens in a guinea pig model (Riedel et al, 1988), and ozone, which has been shown to potentiate platinum sensitivity in monkey (Biagini et al., 1986).
The mechanism of environmental adjuvancy may be that inflamed tissue processes antigen. Substances like sulfur dioxide and ozone produce tissue irritation, which then leads to inflammation with the recruitment of macrophages to the area. Macrophages then present antigens in the area to lymphocytes to produce an immune response to the antigen. Subsequent exposure to either the adjuvant or the antigen could produce further
inflammation and processing of other antigens. The process may be initiated by the interaction of chemical irritants with sensory nerves. The repertoire of triggers of inflammation would grow, with increased risk of more substances becoming triggers. Such an immunological spreading phenomena has not been demonstrated to my knowledge but is theoretically possible.
REVIEW OF SELECTED PUBLISHED DATA ON IMMUNE ABNORMALITIES IN CHEMICALLY SENSITIVE PATIENTS
Studies have appeared which attempt to establish an immunological basis for patients with multiple chemical sensitivities, as described in Table 5. There are studies depicting increases in T4/T8 ratios in chemically sensitive patients, decreases in this ratio, and no abnormalities in this ratio. It is important to note, however, that the patient populations differ in these studies. One study described three groups of chemically sensitive patients, those with vascular dysfunction (vasculitis), asthma, and rheumatoid arthritis (Rea et al.,-+1986). Chemical sensitivity was verified by chemical challenges in these study patients. Rea's patients would be considered stage 2 and 3 patients in the Hypothetical Chemical Stress Syndrome discussed in section I above. Statistically sign cast decreases in T8 (suppressor) cells and increases in the T4/T8 (helper: suppressor ratio) were found in patients with vasculitis and rheumatoid arthritis but not in asthmatics.
Levin and Byer (1989) have looked at populations of patients who have had documented environmental exposures to chemicals such as trichlorethylene exposure, PCB's, or a mixture of industrial dyes, solvents, and pesticides. These patients were said to be chemically sensitive following these exposures, and may represent Stage 1 patients in the HCSS. This study found decreased T4:T8 ratios in these patients.
Terr examined the medical records of 50 patients referred by the California Worker's Compensation Board of Appeals who claimed to have difficulties with workplace chemicals and found no consistent pattern of immunological abnormality. In contrast to the patients studied by Rea and his collaborators, these patients had a variety of medical diagnoses and no attempt was made to challenge them with chemical exposures to see if they were sensitive to chemicals. Rather, it was concluded that, since another medical diagnosis could be given, they did not have chemical sensitivities and instead had a somatization disorder.
These three studies obtain conflicting results on the T4:T8 ratio in chemically sensitive populations, but the patient populations differ dramatically. Rea's group studied patients with known inflammatory diseases which improved when isolated from the chemical environment, Levin and Byer studied populations environmentally exposed to organic chemicals, and Terr studied patients claiming chemical sensitivity who had had a claim for worker's compensation rejected. These studies illustrate the importance of using well-designed clinical research protocols to assess chemically sensitive patients, using well-defined patient populations. It can be argued that the expression multiple chemically sensitivity is best used as an etiology, not as a medical diagnosis. The hypothesis presented in Section II is that a number of inflammatory conditions can arise from the chronic stress of exposure to environmental chemicals, and it may be that the various conditions developing from chemical exposures may have different immunological profiles reflecting the medical diagnosis rather than the chemical etiology.
One group of investigators has proposed that antibodies to formaldehyde coupled to
TABLE 5 Selected Published Data on Immune Abnormalities in Chemically Exposed Patients
|
Reference |
Patient Group |
Number |
Abnormality |
|
Rea et al., 1986 |
Vasculitis Asthma Rheumatoid arthritis |
70 27 7 |
T8 decreaseda, T4/T8 increaseda T4% decreasedb |
|
Terr, 1986 |
Worker's comp. appeals |
50 |
No immunological abnormality |
|
Broughton & Thrasher, 1988 |
Formaldehyde exposure |
67 |
Antibodies to formaldehyde albumin Increased CD26 cells |
|
Levin & Byers, 1989 |
TCE exposure Industrial Chemical Exposure PCB exposure Electronic workers |
25 10 21 78 |
T4/T8 decreasedd T4/T8 decreasede T4/T8 decreasede T4/T8 decreasede |
|
Patterson et al, 1989 |
Chemically sensitive Dialysis patients |
|
No antibodies to formaldehyde-albumin Antibodies to formaldehyde-albumin |
|
McConnachie & Zahalsky, 1991 |
Chlordane/heptachlor |
27 |
Increased CD26, decreased CD45R/T4 Decreased Con A mitogen response Decreased mixed lymphocyte response |
|
a p<0.0001 b p<0.05 c p<0.001 d p<10-8 e p<10-6 |
|||
human serum album (f-HSA) may be a good marker for chemical sensitivity (Broughton and Thrasher, 1988; Thrasher et al., 1988; Thrasher et al., 1989). These investigators found low level IgG, IgE, and IgM titers to f-HSA, in the 1:4 to 1:16 range, in chemically sensitive patients. Well-established associations between diseases and antibody titers, such as the association of systemic lupus erythematosis with anti-DNA titers, are characterized by
extremely high titers of 1:1,000 or higher. Non-specific binding at the high serum concentrations found in low titer wells make low-titer associations with disease of dubious clinical significance. Another group has found no association between formaldehyde conjugates and chemical sensitivity, but has found titers to be a possible marker of exposure to formaldehyde in renal dialysis patients (Patterson et al., 1989).
An increased frequency of the CD26 lymphocyte marker in chemical sensitivity individuals has been reported (Broughton and Thrasher, 1988). This marker has also been reported with greater frequency in chlordane/heptachlor exposed individuals (MeConnachie and Zahalsky, 1991), though the issue of chemical sensitivity is not addressed in this study. Since CD26 is a lymphocyte activation marker, the notion that chronic activation of cellular immunity by chemical exposures is an attractive one which deserves further study.
Neuroimmunology and Chemical Sensitivities
Over the past decade there has been an increased appreciation of the numerous interactions between the nervous system and the immune system. It is tempting to speculation that an understanding of chemical sensitivity may be found in the study of neuroimmunology, given the neurological and behaviorally abnormalities in this patient population and the altered reactivity to normally harmless levels of environmental chemicals reminiscent of immune mediated phenomena. In this section we propose a hypothetical model of disease based on the interactions of the immune and nervous systems, as depicted in Fig. 2. Odorous chemicals excite the nervous system in two ways, through olfactory nerves and irritant nerve fibers in the airway. According to the hypothetical tenet of neuroimmunology, given in Table 6, stimulation of irritant fibers in the airway by volatile organic chemicals leads to inflammation. Normal volunteers exposed for four hours to a mixture of volatile organic chemicals were found to have increased numbers of polymorphonuclear cells in nasal lavage washings eighteen hours (Koren et al., 1990), suggesting an association between irritant chemicals and inflammation.
TABLE 6 The Hypothetical Tenets of Neuroimmunology
|
Tenet 1. Irritancy leads to inflammation and vasomotor abnormalities. |
|
Tenet 2. Inflammation provokes an immune response, that is inflamed tissue processes antigen. |
|
Tenet 3. Immune mediators modulate the central nervous system. |
As the airway becomes inflamed, macrophages are recruited to the area and begin to process antigens, including organic chemicals bound to tissue proteins, for presentation to lymphocytes. We propose that this process leads to sensitized lymphocytes specific for the chemicals which were present in the airway. Subsequent exposure to these chemicals can
Hypothetical Chemical Stress Syndrome
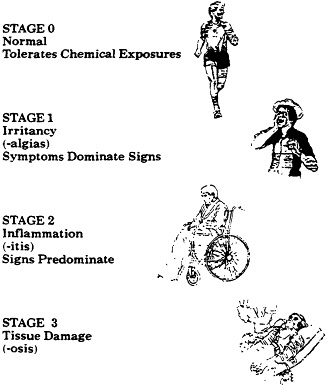
Figure 2
lead to the production of cytokines which can have systemic effects and may effect the central nervous system. Two interleukins, IL-1 (Obal et al., 1990) and IL-2 (De Sarro et al., 1990) are known to have activity on the central nervous system. Perhaps the difficulty with concentration that is reported by chemically sensitive individuals following exposures is related to the release of interleukins with central nervous system activity.
Blood flow in vessels throughout the body is modulated by the contraction and relaxation of smooth muscles in the blood vessel walls, or vasomotor tone, and the tone of these muscles is controlled by the nervous system. Tenet Number 1 in Table 6 proposes that stimulation of irritant receptors by chemicals can alter blood flow by dilating or constricting vessels. Clinical manifestations would include headache, nasal congestion, and rhinorrhea. It is interesting to speculate if neuronal pathways can be acquired so that stimulation by chemicals in the airway might lead to vasomotor phenomena in other organs. One would then have the possibility of protean manifestations of chemical exposures depending on one's ''learned'' or acquired responses.
It is instructive to discuss the Hypothetical Chemical Stress Syndrome of fig. i in terms of the neuroimmunological mechanisms proposed in fig. 2. Stage 1 patients in the HCSS have an exaggerated vasomotor response to the stimulation of irritant receptors in the
airway, with vasomotor tone alterations in organs other than the airway. Stage 2 patients arc those who have developed recurrent loci of inflammation resulting from chemical exposures. Stage 3 arises when tissue is destroyed by the inflammatory products including free radicals released by macrophages and neutrophils.
SUMMARY
We have presented a speculative but comprehensive and mechanistic model to explain the alleged adverse reactions to environmental chemicals. The multiple chemical sensitivity syndrome must be discussed in the broader context of stress syndromes. The patient with multiple complaints related to chemicals but few objective signs of disease manifests an early stage of chemical induced disease. We believe that the stimulation of irritant receptors by chemicals, primarily in the airway, leads to modulations of vasomotor tone. In the chemically sensitive patient, this response is exaggerated and can occur various organs through acquired neuronal pathways.
As the disease progresses, foci on inflammation develop, with infiltrations of macrophages, polymorphonuclear cells, and perhaps lymphocytes into the affected tissue. At this point, the patient develops a diagnosable disease and is traditionally treated with corticosteroids, non-steroidal anti-inflammatory agents, bronchodilators, or other pharmaceuticals as appropriate. The inflammation can be reversed by avoiding the causative chemicals if tissue damage has not occurred.
The inflammatory response leads to processing antigen and specific immunological responses to chemicals. Immune mediators then cause further symptomatology including effects on the central nervous system. Tissue destruction can be a final outcome of chemical sensitivity.
This speculative model must be subjected to several tests. Do patients with chemical sensitivities, including those with diagnosable disorders such as rheumatoid arthritis and multiple sclerosis, progress through the stages of the stress syndrome when their chemical environments are manipulated? This question can be answered by placing patients with candidate diseases in an Environmental Control Unit and studying clinical and laboratory changes in their health.
Are the mechanisms proposed above operative in chemically sensitive patients? This question can be addressed by measuring immune parameters, neurological parameters, and mediators in blood and urine while patients' chemical environments are manipulated. An Environmental Control Unit will be necessary for this type of work Animal models may be helpful in studying the details of the response to chemical exposures depicted in figure 2.
REFERENCES
Ashford, N. A., and Miller, C.S. 1990. Multiple chemical Sensitivities. Report to the New Jersey Department of the Environment.
Ashford, N. A., and Miller, C.S. 1991. Chemical Exposures: Low Levels and high Stakes. Van Nostrand Reinhold, New York.
Bingini, R. E., W. J. Moorman, T. R. Lewis, and I. L. Bernstein. 1986. Ozone enhancement of platinum asthma in a primate model. Am. Rev. Respir. Dis. 134:719-725.
Broughton, A., and J. D. Thrasher. 1988. Antibodies and altered cell mediated immunity in formaldehyde exposed humans . Clinical Toxicology 2, 155-174, 1988.
Cochran, C. G. 1988. Immune Complex Diseases, In J. B. Wyngaarden and L. H. Smith, Jr., ed., Cecil Textbook of Medicine, 18th edition, W. B. Saunders, Philadelphia. chapter 424, p 1960.
Cullen, M. 1989. "The Worker with Multiple Chemical Sensitivities: An Overview." In, Cullen, M. (ed.) Workers with Multiple Chemical Sensitivities. Occupational Medicine: State of the Art Reviews. 2(4):655-662. Hanley & Belfus, Philadelphia.
De Sarro, G. B., Y. Masuda, C. Ascioti, M. G. Audino, G. Nistico. 1990. Behavioral and ECoG spectrum changes induced by intracerebral infusion of interferons and interleukin 2 in rats are antagonized by naloxone. Neuropharmacology 29:167-79.
Korea, H. S., R. B. Devlin, D. Hourse, S. Steingold, and D. E. Graham. The inflammatory response to the human upper airways to volatile organic compounds. 1990. Proceedings of the 5th International conference on indoor air quality and climate. Ottawa, p. 325.
Levin, A. S. & V. S. Byers. 1989. Environmental illness: a disorder of immune regulation. In M. R. Cullen, ed., Workers with multiple chemical sensitivities. State of the art reviews: Occupational Medicine. 2(4)669-681.
Meggs, W. J. "Development of a Clinical Research Protocol for the Multiple Chemical Sensitivity Syndrome."
Moore K. W., P. Vieira, D.F. Fiorentino, M. L. Trounstine, T. A. Khan, T. R. Mosmann. 1990. Homology of cytokine synthesis inhibitory factor (IL-10) to the Epstein-Barr virus gene BCRFI. Science 248:1230-4.
Obal, F. Jr., M. Opp, A. B. Cady, L Johannsen, A. E. Postlethwaite, H. M. Poppleton, J. M. Seyer, and J. M. Krueger. 1990. Interleukin 1 alpha and an interleukin 1 beta fragment are somnogenic. Amer Jour Physiology 259:R439-46.
Patterson, R. et al. 1989. IgG antibodies against formaldehyde human serum proteins: a comparison of other IgG antibodies against inhalant proteins and reactive chemicals. J
Allergy Clin Immunol 84:359-366.
Randolph, T. G. 1962. Human Ecology and Susceptibility to the Chemical Environment. Charles C Thomas, Springfield, IL.
Rea, W. J., A. R. Johnson, S. Youdim, et al., 1986. T&B lymphocyte parameters measured in chemically sensitive patients and controls. Clinical Ecology 4, 11.
Riedel,, F., M. Kramer, C. Scheibenbogen, and C. H. Rieger. 1988. Effects of SO2 exposure on allergic sensitization in the guinea pig. Sour Allergy Clin. Immunol. 82:527-534.
Terr, A. I. 1986. Environmental Illness: a clinical review of 50 cases. Arch Int Meal 146














