3
Using Indicators to Monitor National Objectives for Health Care
As noted earlier, the committee believes that assessing access to health care requires more than a simple tally of the use of services. The content and appropriateness of those services also must be estimated. Implicit in the committee's definition of access is the idea that certain services improve health. Thus, for many, if not most, personal health care services, there is an expectation of benefit, and that benefit extends beyond such obviously important outcomes as avoiding death to more subtle quality-of-life values like physical and social functioning.
With these concepts in mind, the committee focused on access problems that it believes, if corrected, are most likely to lead to improved health outcomes on a wide scale. Indicators were then identified that could be used to measure changes in the degree of access to specific health care services. After considerable discussion, the committee agreed on a list of 15 indicators, which were grouped into several distinct categories. The categories define a set of national objectives for the personal health care system, with each set of indicators providing a means of assessing progress toward a specific objective. The objectives are as follows: (1) promoting successful birth outcomes; (2) reducing the incidence of vaccine-preventable childhood diseases; (3) early detection and diagnosis of treatable diseases; (4) reducing the effects of chronic diseases and prolonging life; and (5) reducing morbidity and pain through providing timely and appropriate treatment. Table 3-1 shows for each objective the related indicators, how they are measured, and the latest year for which data are available.
TABLE 3-1 Access Indicators
|
Objective/Indicator |
Measure |
Latest Data Available |
|
1. Promoting successful birth outcomes |
||
|
Adequacy of prenatal care (u) |
Percentage of pregnant women obtaining adequate care |
1988 |
|
Infant mortality (o) |
Children who die before first birthday (per 1,000 live births) |
1990 |
|
Low birthweight (o) |
Percentage of infants born weighing less than 2,500 grams |
1988 |
|
Congenital syphilis (o) |
Cases per 100,000 population |
1990 |
|
2. Reducing the incidence of vaccine-preventable preventable childhood diseases |
||
|
Immunization rates (u) |
Percentage of preschool children vaccinated |
1985 |
|
Incidence of preventable childhood communicable diseases (diphtheria, measles, mumps, pertussis, polio, rubella, and tetanus) (o) |
Cases per 100,000 population |
1989 |
|
3. Early detection and diagnosis of treatable diseases |
||
|
Breast and cervical cancer screening (u) |
Percentage of women undergoing procedure in given period |
|
|
|
• Clinical breast exam |
1987 |
|
|
• Mammogram |
1990 |
|
|
• Pap test |
1987 |
|
Incidence of late-stage breast and cervical cancers (o) |
Percentage of tumors diagnosed at late stages |
|
|
|
• Breast cancer |
1983–1987 |
|
|
• Cervical cancer |
1983–1987 |
|
Objective/Indicator |
Measure |
Latest Data Available |
|
4. Reducing the effects of chronic diseases and prolonging life |
||
|
Chronic disease follow-up care (u) |
Average number of physician contacts annually by those in fair to poor health; proportion with no physician contacts in previous year |
1989 |
|
Use of high-cost discretionary care (u) |
Admissions for referral-sensitive surgeries |
1988 |
|
Avoidable hospitalization for chronic diseases (o) |
Admissions for ambulatory-care-sensitive chronic conditions |
1988 |
|
Access-related excess mortality (o) |
Number of deaths per 100,000 population estimated to be due to access problems |
1988 |
|
5. Reducing morbidity and pain through timely and appropriate treatment |
||
|
Acute medical care (u) |
Percentage of individuals with acute illness who have no physician contact |
1989 |
|
Dental services (u) |
Average number of dental visits per year |
1989 |
|
Avoidable hospitalization for acute conditions (o) |
Admissions for ambulatory-care-sensitive conditions |
1988 |
|
u, utilization; o, outcome. |
||
The sections that follow discuss one or more utilization and outcome indicators for each objective. An indicator is first defined and the rationale for including it in the report is presented. This is followed by a subsection on measurement and an analysis of any methodological or measurement problems. A third subsection discusses overall trends in the data related to the particular indicator and, where possible, includes specific information on racial and ethnic groups. It also describes and provides data on barriers to access faced by various groups (the uninsured, the less educated, etc.) in the population. The final subsection contains the committee's recommendations.
The committee did not attempt to develop its own quantitative goals for the indicator measures. Where possible, the Year 2000 Health Objectives for the Nation goals are cited as a benchmark and to indicate existing consensus about the desired levels of service use or health status. Time series data are explored to indicate improvement or lack of improvement over the past decade. Finally, comparisons among population subgroups are made and constitute a major focus for interpretations.
OBJECTIVE 1: PROMOTING SUCCESSFUL BIRTH OUTCOMES
Utilization Indicator: Adequacy of Prenatal Care
Prenatal care consists of medical services and procedures intended to monitor and maintain the health of mother and fetus from conception to delivery. For the purposes of this report, prenatal care at a minimum consists of periodic examinations to screen for and manage health risks to the mother and developing fetus. Prenatal visits comprise an accurate medical history, physical exam (including a check of blood pressure), and laboratory tests (including tests for serum glucose levels, sexually transmitted diseases, and cervical cancer).
The results of these periodic visits will determine the necessary degree of monitoring and intervention. For example, a woman found to have gestational diabetes, abnormal weight gain, signs of premature labor, or preeclampsia (hypertension of pregnancy) may require more frequent visits to the obstetrician or certain nonstandard medical procedures or tests. Women at high risk for poor pregnancy outcomes—such as those who smoke, those who suffer from malnutrition or nutritional imbalance, or those who are addicted to drugs or alcohol—may need to take part in a wide range of medical, health education, and social service programs. The content of prenatal care can vary widely depending on the patient's needs, what health care services are available, and which of the available services the patient chooses to take advantage of.
Extensive efforts have been made to evaluate the components of prenatal care. The Public Health Service's Expert Panel on the Content of Prenatal
Care has analyzed a large constellation of services and procedures that constitute prenatal care. The panel reviewed the scientific and medical literature to determine the efficacy and appropriate timing of more than 130 individual components of prenatal care (Public Health Service Expert Panel on the Content of Prenatal Care, 1989). Another major recent effort to define the content of prenatal care is the seventh edition of Standards for Obstetric-Gynecological Services published in 1989 by the American College of Obstetricians and Gynecologists. Numerous studies have shown the link between the timing, amount, and content of prenatal care and successful birth outcomes. Prenatal care also has been shown to be cost effective, particularly for poorly educated, low-income women who otherwise might incur significant direct medical expenses for the care of their low birthweight infants (Institute of Medicine, 1985, 1988; Office of Technology Assessment, 1988).
The committee realizes that a woman's general health status prior to becoming pregnant has a significant impact on the course and outcome of her pregnancy. Nevertheless, the prenatal period is of critical importance because a host of interventions are known to make a significant difference in the outcome of a pregnancy, regardless of the mother's prior health history.
Two aspects of a woman's access to health care services and her health-seeking behavior prior to pregnancy are worth noting. First is the use and content of so-called preconception medical care, which has been shown to have a direct influence on the later use of prenatal care services. Women are much more likely to use prenatal care services during their pregnancy when the pregnancy is planned (and the child is wanted) than when it is unplanned or mistimed (and the child is unwanted). Noting that more than half of all pregnancies in the United States are unwanted, the IOM Committee to Study Outreach for Prenatal Care concluded that more extensive use of family planning services (a ''preconception" service) would result in reduced rates of late entry into prenatal care (Institute of Medicine, 1988).
The second aspect is the role, indirect and direct, that nutrition services, particularly the Special Supplemental Food Program for Women, Infants, and Children (WIC), play in improving maternal and infant health. WIC is among those services ancillary to prenatal care that have great potential for enhancing the outcome of pregnancy. There is considerable evidence that WIC participation reduces rates of low birthweight and infant mortality (Caan et al., 1987; Centers for Disease Control, 1978; Coit, 1977; Collins et al., 1985; Food Research Action Center, 1991; Kennedy and Kotelchuck, 1984; Rush et al., 1988b; Schramm, 1986). Other research (Kotelchuck et al., 1984; Rush et al., 1988a; U.S. Department of Agriculture, 1990) has shown that women who participate in the WIC program enter early prenatal care more often than women who are eligible but do not participate. A large proportion of women who are eligible to participate in the WIC program
do not do so. In 1984, for example, although some 7.5 million women, infants, and children were eligible, only slightly more than 3 million received WIC benefits (U.S. Department of Agriculture, 1987). It is generally believed that lack of knowledge about available benefits and administrative barriers to enrollment are in great measure to blame for lack of access to the program.
Measuring the Indicator
The primary source for data on prenatal care is the birth certificate. The data are reported by states annually to the National Center for Health Statistics (NCHS). Another important source of information about prenatal care is the 1988 National Maternal and Infant Health Survey (National Center for Health Statistics, 1991), which gathered data from mothers and their health care providers.
There are two aspects of prenatal care that are frequently measured: its initiation and frequency. When a woman first obtains prenatal care is important because care initiated early in a pregnancy has the best chance of preventing or treating medical conditions that could potentially harm the mother or fetus. Similarly, how often a women receives prenatal care is important, too, because periodic monitoring (with frequency determined by need) is essential for ensuring a good pregnancy outcome.
Because many insurance plans do not cover prenatal care and because Medicaid does not reimburse for these services at levels high enough to encourage all providers to participate, income is an important barrier to access. However, securing direct evidence of the link between income and access to care on a routine basis is difficult since income information is not reported on birth certificates. The Health Resources and Services Administration is testing the feasibility of combining the information provided on birth certificates with income data by zip code from the Census Bureau to estimate the income levels of women who use varying quantities of prenatal care services. Preliminary results from a pilot study in New York City indicate that living in lower-income neighborhoods is correlated with less use of prenatal care (Zeitel et al., 1991).
Several factors may affect the accuracy and usefulness of various measures of prenatal care. For example, none of the several measurement methodologies in widespread use defines in any precise way the components of a typical prenatal care visit (Institute of Medicine, 1988). In addition, several measurement methods rely for data collection on the memories of pregnant women or on their medical records, both of which can be faulty. Even the accuracy of birth certificates, used by the NCHS to generate most of the available information about prenatal care, has been called into question (National Center for Health Statistics, 1983; see also NCHS, 1980a).
In addition to these generic problems, each of the three most common approaches to assessing the use of prenatal care has specific limitations. Studies that simply count the number of prenatal care visits tell nothing about the distribution of those visits throughout the pregnancy. Analyses that focus on when prenatal care was begun fail to reveal whether that care had any continuity. Moreover, indices of prenatal care that combine the number of visits and timing of prenatal care with other variables (in the case of the modified Kessner index, for example, with gestational age) can be confounded by incomplete or missing data for one or more variables (Alexander et al., 1991). In short, no currently available method for measuring the use of prenatal care services is without its drawbacks.
Trends in the Data
The committee decided that the most valuable overall indicator of utilization is the percentage of women receiving adequate prenatal care as measured by the modified Kessner index. Although it recognizes the problems with the Kessner index, the committee believes that by combining early initiation of care with the number of visits (adjusted for gestation), the index provides the most appropriate standard of the measures currently and widely available.
Table 3-2 displays the percent distribution of births by adequacy of care for 1986–1988 as measured by the modified Kessner index. For all races, slightly less than 70 percent of all women received adequate prenatal care in each of the three years. In each year nearly three-quarters of white women but only one-half of black women received adequate care. Comparable national data from earlier years are not available. Although the relative differences are small, improvement was greater for whites (0.9 percent) than for blacks (0.1 percent)—a trend that should be watched closely in future years. The NCHS plans to update the Kessner index annually. Beginning in 1989, all states are reporting the data necessary to construct the index.
Trend data are available to indicate the percentage of women who begin prenatal care in the first trimester, a key component of the modified Kessner Index. As Table 3-3 indicates, approximately 75 percent of all U.S. women begin prenatal care at that time. The comparable figure for white women is approximately 80 percent and for black women 60 percent. The table also shows that the percentage of women receiving early care increased steadily during the 1970s (from 67.9 percent for all races in 1970 to 75.9 percent in 1979) but remained static between 1980 and 1988. As the final column in the table indicates, the gap in the use of early prenatal services between white and black women, after decreasing rapidly during the 1970s, has worsened slightly since 1980.
Table 3-4 indicates the percentage of women, by race/ethnicity of the
TABLE 3-2 Percent Distribution of U.S. Births by Adequacy of Care (Modified Kessner Index), 1986–1988
|
Care Level |
All Races |
Black |
White |
|
Adequate |
|
|
|
|
1986 |
68.4 |
50.6 |
72.6 |
|
1987 |
68.7 |
50.7 |
73.2 |
|
1988 |
68.9 |
50.7 |
73.5 |
|
Intermediate |
|
|
|
|
1986 |
23.6 |
34.2 |
21.0 |
|
1987 |
23.2 |
33.6 |
20.6 |
|
1988 |
23.1 |
33.8 |
20.4 |
|
Inadequate |
|
|
|
|
1986 |
8.0 |
15.3 |
6.3 |
|
1987 |
8.1 |
15.7 |
6.2 |
|
1988 |
8.0 |
15.5 |
6.1 |
|
SOURCE: National Center for Health Statistics, based on data from 49 reporting states and the District of Columbia. |
|||
mother, seeking early prenatal care. The percentage for all races for 1988 was 75.9; however, the percentages by ethnic group varied from less than 60 percent for Native Americans and Mexican Americans and 61.1 percent for blacks to 82.4 percent for Chinese, 83.4 percent for Cubans, and 86.3 percent for Japanese. Less than 65 percent of Puerto Rican and Central and South American women living in the United States had early prenatal visits in 1988. The wide variations by race and ethnicity have been constant over the past decade (U.S. Public Health Service, 1991).
The existence of a broad range of barriers to the use of prenatal care services has been extensively documented. Indeed, several years ago IOM prepared a review of much of the relevant literature, grouping the barriers into four categories: (1) financial (including insurance or lack thereof, eligibility for insurance coverage, scope and depth of insurance coverage, and Medicaid coverage); (2) inadequate capacity of the personal health care system (including not only private physicians but also factors influencing such organized health care settings as hospital outpatient departments and community and migrant health centers); (3) organizational aspects of prenatal services (including links among various programs that furnish prenatal care); and (4) cultural and personal factors (including care-seeking behavior, views about the importance of prenatal care, and drug and alcohol abuse) (Institute of Medicine, 1988).
Measuring the organizational factors that influence the quality and content
TABLE 3-3 Percentage of U.S. Women Receiving Early Prenatal Care,a by Race, 1970–1988
of prenatal care is clearly an important task, and it remains a major challenge for researchers (Culpepper, 1991). For example, where women first receive prenatal care varies according to race. Data from 1982 and 1983, collected during cycle III of the National Survey of Family Growth, show that 80 percent of white women who began prenatal care during the first trimester visited a personal, private physician (as opposed to a hospital, health department, or clinic), whereas only 48 percent of black women receiving early prenatal care did so (National Center for Health Statistics, 1988). Further work is needed to sort out the implications of these and other organizational differences—both in terms of positive and negative consequences.
Recommendations
Improved Data from the Revised Standard Birth Certificate and the 1988 National Maternal and Infant Health Survey. The standard birth certificate
TABLE 3-4 Percentage of Women Receiving Early Prenatal Care,a by Race/Ethnicity, 1988
|
Race/Ethnicity |
Percentage |
|
All races |
75.9b |
|
American Indian |
58.1 |
|
Black |
61.1b |
|
Central/South American |
63.1 |
|
Chinese |
82.4 |
|
Cuban |
83.4 |
|
Filipino |
78.4 |
|
Japanese |
86.3 |
|
Mexican American |
58.3 |
|
Puerto Rican |
63.3 |
|
White |
79.4b |
|
a Early prenatal care is defined as care beginning in the first trimester. b Data received directly from the National Center for Health Statistics' Vital Statistics System. SOURCE: National Center for Health Statistics (1990c). |
|
has been revised to include more information on risk factors that affect pregnancy. The form now allows check-box entries for each of 16 medical risk factors. More research and analysis are needed to relate prenatal care and birth outcomes to these risk factors.
The 1988 National Maternal and Infant Health Survey (NMIHS; National Center for Health Statistics, 1991) obtained information from mothers, hospitals, and providers on pregnancies, pregnancy outcomes, and early infant health. In addition, a longitudinal follow-up study was begun in 1990. The study will provide more information on the dynamics of prenatal care; child development; and the effects of low birthweight, child nutrition, and exposure to environmental hazards.
The committee supports these efforts and recommends that NCHS expedite the analysis and release of these data. In addition, the committee recommends that research be undertaken to determine the accuracy of birth certificate data through a comparison of those data with data from the NMIHS. Finally, given the importance of financial barriers to access to prenatal care, the committee recommends that the NCHS consider further revision of the birth certificate to include income class and insurance information.
Content and Timing of Prenatal Services. The committee recommends the continuation of research into the measurement of the content of prenatal care, especially for high-risk pregnancies. This research is likely to improve our understanding of the relationship between prenatal care and successful
birth outcomes. In this regard the committee supports the National Fetal and Infant Mortality Review Program established by the American College of Obstetrics and Gynecology. This program is designed to assist communities in identifying specific causes of infant and fetal mortality and the barriers that need to be addressed. Community-based studies will also help clarify how the constellation of available resources and the way they are organized affect outcomes.
Financial Barriers to Access. The committee recommends the continuation of efforts to develop a better understanding of the relationship between income and access to prenatal care. The committee was encouraged by the results of a pilot project in New York City that linked birth certificate data with Census Bureau income data by zip code. States should subscribe to the long-term objective of computerizing their birth and death records in ways that will promote small-area analyses and needs assessment—not only in terms of income but also in relation to other characteristics of local communities.
Improved Measurement of Prenatal Services. Although the committee has chosen to use the modified Kessner index as a measure of the adequacy of prenatal care, this method is not without its problems. Federal agencies and the states need to continue to develop better indices of adequate prenatal care. The federal Bureau of Maternal and Child Health, for example, has supported state efforts to develop a common outcome-oriented minimum data set and a standard definition of adequate prenatal care. Efforts should be made to develop an index that measures the timing, sensitivity, content, and quality of prenatal care and that accounts for the effects of various risk factors in determining adequacy.
Outcome Indicator: Infant Mortality
Infant mortality refers to children who die before their first birthday. Subcomponent measures of infant mortality are derived by dividing the first year after birth into two stages: neonatal (28 days old or younger) and postneonatal (between 28 days and 1 year of age). Each measure may provide potentially useful information about barriers to health care access. Dividing the first year of life into two parts allows identification of the most appropriate health interventions for specific infant age groups. Reducing neonatal mortality requires not only that steps be taken during pregnancy to increase birthweight but also that intrapartum and newborn care be improved. To achieved the latter, reorganized perinatal services have been put in place. Interventions intended to reduce postneonatal mortality must focus on improving well- and sick-child care and on intensive follow-up of high-risk infants (Centers for Disease Control, 1989b).
Infant mortality data have been widely collected throughout the world, primarily as a way to assess the success or failure of national health care systems. Infant mortality is a useful, although indirect, indicator of the adequacy of prenatal care and of access to neonatal intensive care units (NICUs) and care in the first year of life. The relationship between inadequate prenatal care and infant mortality has become less precise, however, as NICUs have become more widely available and new therapeutic methods for improving the survivability of premature babies have been developed.
Measuring the Indicator
Infant mortality is expressed as the number of deaths per 1,000 live births. National data on infant deaths are compiled by the NCHS. Unfortunately, most of the routinely available data on infant mortality do not provide information about access barriers, which inhibits our ability to better understand the relationship between financial, structural, and personal barriers and outcomes. To analyze factors that contribute to infant mortality, death certificates frequently are "linked" to birth records, which contain information about the mother's use of prenatal care services and other factors that influence the outcome of pregnancy. As noted previously, the revised birth certificate has space for information on 16 medical risk factors. The new certificate also provides space for physicians to record information on obstetrical procedures, method of delivery, and abnormal conditions of the newborn. This kind of information should make the linking of birth and death certificates of even greater value in understanding the causes of infant mortality.
Trends in the Data
Table 3-5 displays infant mortality rates, by race, for selected years from 1970 to 1990. Rates through 1988 are based on complete records and include information on race. Provisional data for 1989 and 1990 are based on a 10 percent sample of deaths. Given the 1987 and 1988 experiences, those provisional rates are likely to be very close to the actual rates.
Infant death rates in the United States have been halved over the past 20 years, from 20 per 1,000 live births in 1970 to 9.1 per 1,000 live births in 1990. The 1990 rate is about 7 percent lower than the 1989 rate and is the lowest ever for the United States. The greatest improvement was seen for neonatal mortality; the greatest reduction in deaths was seen for respiratory distress syndrome, as a result of improved forms of treatment (National Center for Health Statistics, 1990a).
The 7 percent reduction between 1989 and 1990 was significantly higher than in previous years during the 1980s, when the average yearly decline
TABLE 3-5 Infant Mortality Rates by Race and Black/White Ratios, Selected Years, 1970–1990
|
Year |
All Races |
White |
All Nonwhite |
Black |
Ratio, Black/White |
|
Infant Mortality Ratesa |
|||||
|
1970 |
20.0 |
17.8 |
30.9 |
32.6 |
1.83 |
|
1975 |
16.1 |
14.2 |
24.2 |
26.2 |
1.84 |
|
1980 |
12.6 |
11.0 |
19.1 |
21.4 |
1.94 |
|
1981 |
11.9 |
10.5 |
17.8 |
20.0 |
1.90 |
|
1982 |
11.5 |
10.1 |
17.3 |
19.6 |
1.94 |
|
1983 |
11.2 |
9.7 |
16.8 |
19.2 |
1.98 |
|
1984 |
10.8 |
9.4 |
16.1 |
18.4 |
1.96 |
|
1985 |
10.6 |
9.3 |
15.8 |
18.2 |
1.96 |
|
1986 |
10.4 |
8.9 |
15.7 |
18.0 |
2.02 |
|
1987 |
10.1 |
8.6 |
15.4 |
17.9 |
2.08 |
|
1988 |
10.0 |
8.5 |
15.0 |
17.6 |
2.07 |
|
1989 |
9.7b |
N.a. |
N.a. |
N.a. |
|
|
1990 |
9.1b |
N.a. |
N.a. |
N.a. |
|
|
Neonatal Mortality Ratesc |
|||||
|
1970 |
15.1 |
13.8 |
21.4 |
22.8 |
1.65 |
|
1975 |
11.6 |
10.4 |
16.8 |
18.3 |
1.76 |
|
1980 |
8.5 |
7.5 |
12.5 |
14.1 |
1.88 |
|
1981 |
8.0 |
7.1 |
11.8 |
13.4 |
1.89 |
|
1982 |
7.7 |
6.8 |
11.3 |
13.1 |
1.93 |
|
1983 |
7.3 |
6.4 |
10.8 |
12.4 |
1.94 |
|
1984 |
7.0 |
6.2 |
10.2 |
11.8 |
1.90 |
|
1985 |
7.0 |
6.1 |
10.3 |
12.1 |
1.98 |
|
1986 |
6.7 |
5.8 |
10.1 |
11.7 |
2.02 |
|
1987 |
6.5 |
5.5 |
10.0 |
11.7 |
2.13 |
|
1988 |
6.3 |
5.4 |
9.7 |
11.5 |
2.13 |
|
1989 |
6.3b |
N.a. |
N.a. |
N.a. |
|
|
1990 |
5.7b |
N.a. |
N.a. |
N.a. |
|
|
Postneonatal Mortality Rated |
|||||
|
1970 |
4.9 |
4.0 |
9.5 |
9.9 |
2.48 |
|
1975 |
4.5 |
3.8 |
7.5 |
7.9 |
2.08 |
|
1980 |
4.1 |
3.5 |
6.6 |
7.3 |
2.08 |
|
1981 |
3.9 |
3.4 |
6.0 |
6.6 |
1.94 |
|
1982 |
3.8 |
3.3 |
5.9 |
6.6 |
2.00 |
|
1983 |
3.9 |
3.3 |
6.0 |
6.8 |
2.06 |
|
1984 |
3.8 |
3.3 |
5.8 |
6.5 |
1.97 |
|
1985 |
3.7 |
3.2 |
5.5 |
6.1 |
1.90 |
|
1986 |
3.6 |
3.1 |
5.6 |
6.3 |
2.03 |
|
1987 |
3.6 |
3.1 |
5.4 |
6.1 |
1.97 |
|
1988 |
3.6 |
3.1 |
5.4 |
6.2 |
2.00 |
|
1989 |
3.5b |
N.a. |
N.a. |
N.a. |
|
|
1990 |
3.3b |
N.a. |
N.a. |
N.a. |
|
was less than 3 percent. The average rate of decline during the 1980s was well below the 4.7 percent experienced during the 1970s.
As the table shows, the past 20 years have also seen a dramatic decrease in the neonatal mortality rate, from 15.1 per 1,000 live births in 1970 to a provisional 5.7 per 1,000 in 1990. Over the same period, the decline in the postneonatal rate was less striking; it fell from 4.9 percent to a provisional 3.3 percent. During the 1980s, a 28 percent reduction occurred in the overall infant mortality rate, with the greatest decrease (33 percent) arising from improved neonatal mortality rates and the smallest (19 percent) stemming from improvements in postneonatal mortality. The comparable figures for the 1970s were 37 percent, 44 percent, and 16 percent for improvements in overall mortality, neonatal mortality, and postneonatal mortality, respectively.
A striking aspect of infant mortality data is the contrast between the white and black populations. As Table 3-5 shows, infant mortality rates for blacks are much higher than for whites. The absolute differences in rates between the races have narrowed, from approximately 15 more black deaths per 1,000 live births in 1970 to approximately 9 more deaths in 1988; however, the ratio of black to white infant deaths has increased substantially. In 1970 blacks were 85 percent more likely than whites to die during the first year after birth. By 1988 black infants were more than twice as likely as whites to die during their first year. In 1970 blacks were 65 percent more likely than whites to die during the first month after birth; by 1988 they were more than twice as likely to die. In 1975 blacks were twice as likely as whites to die during the postneonatal period, a difference that remained largely unchanged through 1988.
Table 3-6 provides data on infant mortality according to the race or ethnicity of the mother. The data are derived from the linked birth and death records for 1983–1985. Using linked birth and death records addresses the inconsistencies between the information on the two records. Although this information is quite constant for blacks and whites, it can vary
TABLE 3-6 Infant Mortality Ratesa According to Race/Ethnicity of the Mother, 1983–1985 Birth Cohorts
|
Race/Ethnicityb |
Neonatal |
Postneonatal |
Infant Mortality |
|
American Indian |
6.7 |
7.2 |
13.9 |
|
Black |
12.2 |
6.4 |
18.7 |
|
Central/South American |
5.7 |
2.5 |
8.2 |
|
Chinese |
4.3 |
3.1 |
7.4 |
|
Cuban |
5.9 |
2.2 |
8.0 |
|
Filipino |
5.3 |
2.9 |
8.2 |
|
Japanese |
3.4 |
2.6 |
6.0 |
|
Mexican American |
5.7 |
3.2 |
8.8 |
|
Puerto Rican |
8.3 |
4.0 |
12.3 |
|
White |
5.9 |
3.1 |
9.0 |
|
a Deaths per 1,000 live births. b Hispanic data were collected from 23 states and District of Columbia. SOURCE: National Center for Health Statistics (1990c). |
|||
by as much as 25 to 40 percent for American Indians and for some Asian and Pacific Island groups. For this reason the annual records can be misleading, and conclusions must be drawn with caution.
American Indians and Puerto Ricans (as well as blacks) have infant mortality rates that are well above the national averages. For Puerto Ricans, higher infant mortality rates are a result of both high neonatal and postneonatal mortality rates. The high rate among American Indians is primarily due to the group's higher postneonatal death rate. Unfortunately, more recent data are not currently available (National Center for Health Statistics, 1990a).
The U.S. Department of Health and Human Services' (DHHS) Health Objectives for the Year 2000 set a national target of no more than 7 infant deaths per 1,000 live births for the year 2000 (U.S. Public Health Service, 1991). The target for blacks is 11 deaths per 1,000 births; for American Indians, 8.5 deaths per 1,000 live births; and for Puerto Ricans, 8 deaths per 1,000 live births.
Recommendations
Financial and Insurance Barriers. The committee supports NCHS's plans to continue to link birth and death records but also believes that efforts should be made to add source-of-payment information to both records. In the interim the committee recommends efforts to use zip codes to link information from birth certificates to income information from census data.
Access-Sensitive Measures of Infant Mortality. The problem with infant mortality rates as an indicator of access is that they include causes of death, which at present cannot be affected by the personal health care system. The committee believes that there is a need for additional efforts to determine how best to aggregate the specific International Classification of Diseases (9th revision; U.S. Department of Health and Human Services, 1991) categories listed on death certificates into overall classes, which can be categorized as preventable or nonpreventable.
Hispanic Data by Subgroup. The committee encourages NCHS's plans to use the linked birth and infant death files to produce infant death information by specific racial and ethnic subgroups. This proposal is particularly important for Hispanics, whose mortality rates range from well above average for Puerto Ricans to below average for Cubans.
Black-White Gap in Infant Mortality. The committee recommends further research into the contribution of access barriers to the unacceptably large and widening gap in infant mortality between whites and blacks. Particular attention should be focused on the role of financial and insurance barriers as well as the linkage between personal health services and key social services.
Outcome Indicator: Low Birthweight
Infants weighing less than 2,500 grams (5.5 pounds) are considered to be of low birthweight. Very-low-birthweight infants, weigh less than 1,500 grams (3.3 pounds) at birth.
The most important predictor of infant survival is birthweight; survival improves exponentially as birthweight increases to its optimum level (Centers for Disease Control, 1989b). However, a successful birth is one that not only produces a live baby but also a healthy one. Compared with infants weighing more than 2,500 grams, low birthweight and very-low-birthweight babies are much more likely to die during the first year of life and to be hospitalized more frequently. They also have a higher incidence of acute infections and suffer from a range of developmental, behavioral, and physical disabilities. Births of low birthweight and very-low-birthweight infants frequently are associated with inadequate prenatal care and lack of access to nutrition services. Unlike infant mortality (which may be influenced both by the health care services received by the mother during pregnancy and the care received by the infant up to one year after delivery), low birthweight and very low birthweight are outcome indicators specific to the services that the mother received prior to giving birth.
Measuring the Indicator
Low birthweight and very low birthweight are expressed as the percentage of live births weighing less than 2,500 grams and 1,500 grams, respectively. The major source of data on low birthweight and very low birthweight is the birth certificate. Information from birth records is sent by the states to NCHS. The 1988 NMIHS (National Center for Health Statistics, 1991) provides more detailed information about the extent of prenatal care and risk factors associated with low birthweight and very low birthweight.
Additional understanding of the low birthweight problem should be possible when 1989 birth certificate data become available for analysis. The revised birth certificate includes information on medical risk factors and maternal behavior during pregnancy (tobacco and alcohol use) as well as low maternal weight gain—all factors that have been associated with low birthweight.
Efforts to monitor changes in low birthweight are hindered by the considerable time lag between data collection and publication. Similar delays are present in the availability of national linked birth and death certificate data, which are the best source for determining the relationship between low birthweight and poor health outcomes (Miller et al., 1989). In addition, as is true for all events dependent on birth records, no data are available on the source of payment for care.
Trends in the Data
Table 3-7 displays the percentage of infants of low birthweight by race in the United States for selected years from 1970 through 1988, the last year for which data are available. What is most striking is how little change there has been over time. Although there was some decline in low birthweight births during the 1970s, no improvement was apparent during the 1980s. The percentage of low birthweight black infants also deserves note. The ratio of black to white low birthweight births in 1970 was 2.04. A slow but steady increase in the disparity has occurred over the past 20 years, until by 1988 the ratio reached 2.32. The percentage of low birthweight babies born to nonwhites in 1988 was the same as in 1976. Table 3-8 shows low birthweight births for 1988 by racial and ethnic groups. Unlike the previous table, these data are based on the race/ethnicity of the mother rather than the infant.
Table 3-8 reveals the heterogeneity of the Hispanic population. The percentage of low birthweight infants varies from 5.6 per 1,000 live births for Mexican American and Central and South American women to 9.4 per 1,000 live births for Puerto Rican women. The incidence of low birthweight among Puerto Ricans was approximately two-thirds higher than that of white women.
TABLE 3-7 Percentage of Low Birthweight Infants, by Race, Selected Years, 1970–1988
|
Year |
All Races |
All White |
Nonwhite |
Black |
Ratio, Black/White |
|
1970 |
7.9 |
6.8 |
13.9 |
13.3 |
2.04 |
|
1971 |
7.7 |
6.6 |
13.4 |
12.7 |
2.03 |
|
1972 |
7.7 |
6.5 |
13.6 |
12.9 |
2.09 |
|
1973 |
7.6 |
6.4 |
13.3 |
12.5 |
2.08 |
|
1974 |
7.4 |
6.3 |
13.1 |
12.4 |
2.08 |
|
1975 |
7.4 |
6.3 |
13.1 |
12.2 |
2.08 |
|
1976 |
7.3 |
6.1 |
13.0 |
12.1 |
2.13 |
|
1977 |
7.1 |
5.9 |
12.8 |
11.9 |
2.17 |
|
1978 |
7.1 |
5.9 |
12.8 |
11.9 |
2.17 |
|
1979 |
6.9 |
5.8 |
12.6 |
11.6 |
2.17 |
|
1980 |
6.8 |
5.7 |
12.5 |
11.5 |
2.19 |
|
1981 |
6.8 |
5.7 |
12.5 |
11.4 |
2.19 |
|
1982 |
6.8 |
5.6 |
12.4 |
11.2 |
2.21 |
|
1983 |
6.8 |
5.6 |
12.6 |
11.2 |
2.25 |
|
1984 |
6.7 |
5.6 |
12.4 |
11.1 |
2.21 |
|
1985 |
6.8 |
5.6 |
12.4 |
11.1 |
2.21 |
|
1986 |
6.8 |
5.6 |
12.5 |
11.2 |
2.23 |
|
1987 |
6.9 |
5.7 |
12.7 |
11.3 |
2.23 |
|
1988 |
6.9 |
5.6 |
13.0 |
11.5 |
2.32 |
|
SOURCE: Rosenbaum et al. (1991). |
|||||
The national picture is even less encouraging for very-low-birthweight babies. This indicator has shown little change, increasing from 1.15 percent of total births in 1979 to 1.24 percent of the total in 1988 (Rosenbaum et al., 1991). Among blacks the rate rose from 2.37 percent in 1979 to 2.78 percent in 1988.1 In 1988 black women were three times as likely as white women to have a very-low-birthweight baby, and Puerto Rican women were about 80 percent more likely. Other racial and ethnic groups had approximately the same risk of having a very-low-birthweight infant as whites (National Center for Health Statistics, 1990a).
The DHHS's Health Objectives for the Year 2000 set a goal of reducing the incidence of low birthweight to 5 per 1,000 live births, the same rate proposed in the department's health plan for 1990 (U.S. Public Health Service, 1991). For very-low-birthweight infants, the Year 2000 goal is 1 per
TABLE 3-8 Percentage of Low Birthweight Infants by Race/Ethnicity of Mother, 1988
|
Race/Ethnicitya |
Percentage |
|
American Indian |
6.0 |
|
Black |
13.3 |
|
Central/South American |
5.6 |
|
Chinese |
4.6 |
|
Cuban |
59 |
|
Filipino |
7.1 |
|
Japanese |
6.7 |
|
Mexican American |
5.6 |
|
Puerto Rican |
9.4 |
|
White |
5.7 |
|
a Hispanic data were collected from 30 states and the District of Columbia. SOURCE: National Center for Health Statistics (1990b). |
|
100 live births. The Year 2000 objectives set a separate target for blacks of 9 for low birthweight and 2 for very low birthweight. Blacks were the only racial or ethnic group that failed to meet the department's 1990 goal of reducing the low birthweight rate to 9 percent or less.
To understand access barriers that are likely to contribute to the incidence of low birthweight, it is helpful to begin with the known correlates. A variety of factors are correlated with low birthweight and very low birthweight; they have been divided into several categories, including demographic characteristics, medical risks before and during the current pregnancy, and behavioral and environmental risks (Institute of Medicine, 1985). Demographic characteristics that may predispose an infant to low birthweight include low socioeconomic status, limited formal education, bearing children either at a young age (under 17) or an older age (over 34), and being unmarried. Medical risks include such factors as poor obstetrical history, certain diseases and conditions, poor nutritional status, poor weight gain, and short interpregnancy interval. Behavioral and environmental risks include personal behaviors such as smoking, alcohol and drug abuse, and environmental exposure to toxic substances. Also counted under this rubric is inadequate or no prenatal care.
A significant amount of research attention has focused on whether the disparity in the rates of low birthweight between white and blacks can be explained solely by differences in access barriers and maternal risk factors. The manner in which birthweight data have been analyzed seems to indicate that low birthweight is significantly related to race. However, whether
race, per se, is causally related to low birthweight or whether it is a proxy for differences in medical access and socioeconomic status is a matter currently under debate. By controlling for factors other than race, at least one study has shown that the higher rates of prematurity (a birth outcome closely linked to low birthweight) experienced by blacks are attributable to specific medical and socioeconomic characteristics rather than race (Lieberman et al., 1987). These results, however, must be confirmed by other studies with larger samples (Behrman, 1987).
Recommendations
Racial and Ethnic Differences in Low Birthweight. The committee believes that research and analysis should focus on determining the reasons for the large, persistent, and apparently increasing differences in the incidence of low birthweight and very low birthweight among blacks and other racial and ethnic minority groups. It is important that these efforts identify how various barriers affect access to care and that they determine the impact of medical risk factors and socioeconomic factors. It is hoped that data from the revised birth certificate and the 1988 NMIHS (and its 1990 follow-up) will provide greater understanding of this most significant problem.
Financial Barriers. The committee believes that the effects on low birthweight of insurance status and income need to be examined in greater detail. Analyses that use data from the NMIHS or, if available, comparisons of selected states that have linked Medicaid and birth certificate data could provide useful information about the impact of insurance coverage. Data on maternal income may come out of efforts to link zip code data to income information from the Census Bureau.
Delays in Data Availability. There have been concerns that the time lag between data collection and publication of NCHS findings is unnecessarily long and that this lag significantly interferes with the ability to plan, implement, and evaluate public policies. The committee recommends that the Public Health Service investigate these complaints and determine whether efforts to improve the timeliness of NCHS reports are warranted. Consideration should be given to publishing NCHS data as they are received, on a rolling, monthly basis.
Impact of Culture. Recent analysis of the Hispanic Health and Nutrition Examination Survey shows that first-generation Mexican American women have better low birthweight experiences than those born in the United States (Scribner and Dwyer, 1989). The opposite has been shown to be true for Southeast Asian immigrants (Li et al., 1990). It is as yet unclear whether
cultural factors, underreporting of deaths, or other factors may be governing these outcomes. Further research on this topic is warranted.
Outcome Indicator: Congenital Syphilis
Syphilis is a chronic contagious disease caused by a spirochete of Treponema palladium, a bacterium. In adults the disease goes through three stages: the development of skin lesions (primary syphilis); the spread, within two to six months, of lesions into the organs and tissues (secondary syphilis); and the development of skin ulcers and tumors, often with involvement of the skeletal, cardiovascular, and nervous systems (tertiary syphilis). Infants can develop congenital syphilis if infected by their mother during pregnancy or at the time of delivery. Although syphilis may cause rapid onset of severe illness or death in infants (up to 40 percent), the disease responds well to treatment with penicillin.
Each case of congenital syphilis indicates either a lack of any prenatal care (even one prenatal care visit should alert the health care provider to the need for treatment) or a lack of adequate care (a prenatal visit at which an infected mother is not diagnosed is inadequate). In most cases, treatment of syphilis at least 30 days prior to delivery should prevent infection in the infant.
A 1990 editorial in the American Journal of Public Health had this comment:
Congenital syphilis should be a disease of the past. It is fully preventable by treating infected women with penicillin early in pregnancy, provided that infection or reinfection late in pregnancy does not occur. It is therefore a sentinel health condition: its occurrence marks the failure of both the syphilis control program and the prenatal care system.
The recent rise in rates of congenital syphilis in certain geographic areas of the United States is thought to be due in part to the increase in cocaine use (particularly ''crack" cocaine), with its attendant transmission of sexually transmitted diseases. Rates of congenital syphilis, therefore, may also indicate a lack of available, acceptable drug treatment services for pregnant women.
Measuring the Indicator
The incidence of congenital syphilis is measured in numbers of cases per 100,000 population. The presence of the condition can be determined by one of several serologic tests. Test results are reported by physicians to their state health departments, which then forward the results to the Centers for Disease Control (CDC).
The change in 1988 of CDC's case definition for reporting congenital syphilis makes it difficult to interpret changes in the data before that year. The new definition broadened and simplified the reporting criteria. The earlier, more complex reporting requirements depended on extensive physical and laboratory findings at birth and during subsequent follow-up visits. They did not call for including stillborn fetuses with the disease in the overall tally of syphilis incidence.
The new definition is certain to result in an increase in reported cases of congenital syphilis during the short transition period between use of the old and use of the new definition. In one study, based on cases reported in Los Angeles County in 1987, the new definition resulted in a fivefold increase in cases, from 39 to 205 (Cohen et al., 1990).
Counterbalancing the increase in rates expected under the new CDC case definition is the belief that the incidence of congenital syphilis may be underreported because of the failure of physicians to diagnose the disease. In some instances, serologic tests may fail to detect infection in an infant at the time of birth. This may be because the child, although infected, has not yet produced syphilis antibodies on which the test relies for a positive result. The diagnosis of congenital syphilis may also be missed if only the mother is tested (Cohen, 1991). Even when both mother and infant test negative for syphilis at delivery, infection cannot be ruled out because a mother's acquisition of syphilis late in pregnancy may not be detected (Dorfman and Glaser, 1990).
Trends in the Data
Table 3-9 displays the total number of cases of syphilis and cases per 100,000 population for both adult (primary and secondary) and congenital syphilis for selected years from 1970 through 1990. Information on both primary and secondary syphilis is included because the incidence of congenital syphilis closely mirrors the rate of primary and secondary infection in women and because treatment of infected women is the only way to prevent congenital syphilis. The relationship appears graphically in Figure 3-1, which shows the yearly cases of congenital syphilis and the rate of primary and secondary syphilis in women and in men.
The incidence of primary and secondary syphilis in the United States declined from 16.73 per 100,000 in 1950 to 11.45 cases per 100,000 in 1985. It increased steadily through 1990, however, when it reached 20.10, the highest level in the past 40 years.
There are marked differences in the incidence of syphilis among whites, blacks, and other racial and ethnic groups in the United States. Although the incidence for both whites and blacks fell between 1982 and 1985, in 1986 the rates for blacks began to increase. Between 1985 and 1989 the
TABLE 3-9 Disease Rates for Primary, Secondary, and Congenital Syphilis, Selected Years, 1970–1990
|
|
Adult Syphilis, Primary and Secondary |
|
|
|||
|
|
Men and Women |
Women Only |
Congenital Syphilis |
|||
|
Year |
No. of Cases |
Cases/ 100,000 Population |
No. of Cases |
Cases/ 100,000 Population |
No. of Cases |
Cases/ 100,000 Population |
|
1970 |
21,982 |
10.89 |
N.a. |
N.a. |
1,953 |
0.97 |
|
1980 |
27,204 |
12.06 |
N.a. |
N.a. |
277 |
0.12 |
|
1985 |
27,131 |
11.45 |
N.a. |
N.a. |
329 |
0.14 |
|
1986 |
27,883 |
11.65 |
9,197 |
7.5 |
410 |
0.17 |
|
1987 |
35,147 |
14.54 |
13,257 |
10.6 |
681 |
0.28 |
|
1988 |
40,117 |
16.43 |
16,172 |
12.9 |
751 |
0.30 |
|
1989 |
44,540 |
18.07 |
19,047 |
15.0 |
941 |
0.38 |
|
1990 |
50,223 |
20.10 |
22,106 |
17.3 |
2,899 |
1.16 |
|
N.a., not available. SOURCES: National Center for Health Statistics (1990c); Centers for Disease Control data. |
||||||
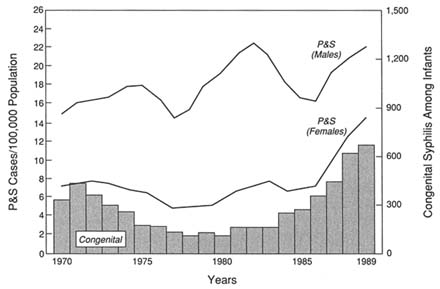
FIGURE 3-1 Cases of congenital syphilis among infants under one year of age and cases of primary and secondary syphilis (P&S) per 100,000 population, by sex, 1970–1989. SOURCE: Centers for Disease Control (1989c).
rate for blacks increased by 132 percent, from 52.6 to 121.8 cases per 100,000 population. It more than doubled in 22 states and the District of Columbia and rose more than fourfold in 10 states. Between 1981 and 1989 the black-to-white incidence rate ratio increased from 14.5 to 47.8. Incidence rates for Asian Americans and Pacific Islanders paralleled those for whites through 1989, whereas the rates for Hispanics remained between the rates for whites and blacks (Rolfs and Nakashima, 1990).
A number of studies have linked the spread of syphilis to increased drug use, particularly cocaine, which often is tied to drug-related high-risk sexual behaviors such as prostitution (Fullilove et al., 1990; McLaughlin et al., 1989; Schwarcz et al., 1989). It also appears that drug use is directly associated with low levels of prenatal care utilization. One study of mothers infected with syphilis who also used cocaine found that 75.8 percent had received no prenatal care (Nanda et al., 1990).
The Year 2000 Health Objective for primary and secondary syphilis in adults is 10 per 100,000 population. For blacks a separate goal is laid out: 65 per 100,000 population. The reasons for the extreme disparity between syphilis incidence rates for blacks and whites are unclear.
Recommendations
Black-White Disparities. The committee recommends that additional research and analyses be conducted to better understand the large disparity between the incidence of primary and secondary syphilis for blacks and whites. Particular emphasis should be placed on the role of barriers to access to health care services.
Drug Use and Prenatal Care Services. The committee also believes that research should be conducted to examine the relationships among drug use, sexually transmitted diseases, and the use of prenatal care services. Such research may shed light on ways of making prenatal care and substance abuse treatment more accessible to this extremely high-risk population and lead to better measures of structural barriers to access.
OBJECTIVE 2: REDUCING THE INCIDENCE OF VACCINE-PREVENTABLE CHILDHOOD DISEASES
Utilization Indicator: Preschool Immunization
Immunization provides protection from infectious diseases, including some that are potentially life threatening. Generally, a vaccine is made up of key parts of a disease organism, or the entire organism is modified so as not to cause disease. Once introduced into the human body, the vaccine
stimulates the production of antibodies and lymphocytes capable of recognizing and destroying the disease-causing microbe.
The immunization of children against polio, measles, mumps, rubella, diphtheria, pertussis, and tetanus has gained wide acceptance in the United States and other countries, both as a means for providing protection to individuals and as a public health measure. (Haemophilus influenzae type b [HIB] encephalitis immunization, while also important, has not been recommended for a sufficient period of time for data to be available.) Routine immunization schedules for children are shown in Table 3-10.
When carried out on a wide scale, immunization programs can dramatically reduce the incidence of certain childhood diseases. Immunization carried out incompletely or only in select population groups, however, can result in higher rates of preventable illness and death than would be expected with more complete vaccine coverage. There is an acknowledged public-private responsibility for immunizing children in the United States. For school-age children, vaccination is required by law in most jurisdictions, but it is generally not required for younger children. Low rates of immunization may indicate the presence of important barriers to other preventive health care services as well. Although nearly all children are vaccinated by the time they begin school (because of statutory requirements), the key access question is whether children are being immunized in accordance with recommended schedules, which require the first immunization at 2 months of age.
Measuring the Indicator
Immunization rates are expressed as the percentage of preschool-age children (ages 1–4) who have been vaccinated. Rates are reported by disease for purposes of access monitoring.
A major problem with state and national efforts to vaccinate children against disease is that there is currently no ongoing routine method of monitoring immunization levels of preschool children. The national immunization survey has not been conducted since 1985; thus, our nationwide estimates are increasingly out of date. Even the accuracy of data obtained in this type of survey is questionable because survey respondents are often expected to recall specific events that happened many years before. This task is made doubly difficult if respondents have more than one child.
Trends in the Data
Table 3-11 displays unpublished survey data on vaccination rates for U.S. children ages 1–4 for selected years from 1970 to 1985. In 1985 the immunization rates ranged from 55.3 percent for polio to 64.9 percent for
TABLE 3-10 Recommended Immunization Schedule for Children
|
Age |
Vaccines |
|
2 Months |
DPTa (first) |
|
|
TOPVb (first) |
|
4 Months |
DPT (second) |
|
|
TOPV (second) |
|
6 Months |
DPT (third) |
|
15 Months |
Measlesc |
|
|
Mumpsc |
|
|
Rubellac |
|
|
DPT (fourth) |
|
|
TOPV (third) |
|
18 Months |
HIB conjugated |
|
At school entry |
MMR, DPT (fifth) |
|
(4–6 Years) |
TOPV (fourth) |
|
a DPT, diphtheria and pertussis and tetanus toxoids vaccine adsorbed; five doses recommended. b TOPV, trivalent oral polio vaccine (live); four doses recommended; however, some physicians may elect to give one additional doses at 6 months of age. c May be combined as a single injection vaccine (MMR). dHaemophilus influenzae type b conjugate vaccine. SOURCE: Hinman (1990). |
|
DPT. The survey indicated declines in vaccination levels of DPT and polio since 1970 and some variation but no clear trends in vaccination rates for the other diseases (particularly during 1983–1985). The same general patterns apply when one considers vaccination by race and by place of residence (inside or outside a metropolitan statistical area, or MSA). However, whites were much more likely to have been vaccinated than children of other races. In addition, beginning in 1976, the survey found that children in the central-city portion of an MSA were less likely to be vaccinated than children in other MSA areas, including the suburbs, or those living outside the MSA altogether.
Even taking into account the possibility of some underreporting, U.S. vaccination rates for children are well below those in some European countries. For example, in 1987 in Denmark, West Germany, and the Netherlands, and in 1986 in France, polio immunization levels among children
TABLE 3-11 Vaccinations of Children 1–4 Years of Age (as percentage of population) for Selected Diseases, by Race and Residence in Metropolitan Statistical Area (MSA), 1970, 1976, and 1983–1985
|
|
|
Race |
|
Inside MSA |
|
|
|
Vaccination and Year |
Total |
White |
All Other |
Central City |
Remaining Areas |
Outside MSA |
|
|
|
|
|
|
|
|
|
1970 |
76.1 |
79.7 |
58.8 |
68.9 |
80.7 |
77.1 |
|
1976 |
71.4 |
75.3 |
53.2 |
64.1 |
75.7 |
72.9 |
|
1983 |
65.7 |
70.1 |
47.7 |
55.4 |
69.4 |
69.4 |
|
1984 |
65.7 |
69.1 |
51.3 |
57.9 |
66.6 |
69.8 |
|
1985 |
64.9 |
68.7 |
48.7 |
55.5 |
68.4 |
67.9 |
|
Measles |
|
|
|
|
|
|
|
1970 |
57.2 |
60.4 |
41.9 |
55.2 |
61.7 |
54.3 |
|
1976 |
65.9 |
68.3 |
54.8 |
62.5 |
67.2 |
67.3 |
|
1983 |
64.9 |
66.8 |
57.2 |
60.4 |
66.3 |
66.7 |
|
1984 |
62.8 |
65.4 |
52.0 |
56.6 |
63.3 |
66.4 |
|
1985 |
60.8 |
63.6 |
48.8 |
55.5 |
63.3 |
61.9 |
|
Mumps |
|
|
|
|
|
|
|
1970 |
N.a. |
N.a. |
N.a. |
N.a. |
N.a. |
N.a. |
|
1976 |
48.3 |
50.3 |
38.7 |
45.6 |
50.7 |
47.9 |
|
1983 |
59.5 |
61.8 |
50.0 |
52.6 |
60.2 |
63.6 |
|
1984 |
58.7 |
61.3 |
47.7 |
51.8 |
58.3 |
63.6 |
|
1985 |
58.9 |
61.8 |
47.0 |
52.4 |
61.0 |
61.4 |
|
Poliob |
|
|
|
|
|
|
|
1970 |
65.9 |
69.2 |
50.1 |
61.0 |
70.8 |
64.7 |
|
1976 |
61.6 |
66.2 |
39.9 |
53.8 |
65.3 |
63.9 |
|
1983 |
57.0 |
61.9 |
36.7 |
47.7 |
60.3 |
60.3 |
|
1984 |
54.8 |
58.4 |
39.9 |
48.7 |
55.2 |
58.5 |
|
1985 |
55.3 |
58.9 |
40.1 |
47.1 |
58.4 |
58.0 |
|
Rubella |
|
|
|
|
|
|
|
1970 |
37.2 |
38.3 |
31.8 |
38.3 |
39.2 |
34.3 |
|
1976 |
61.7 |
63.8 |
51.5 |
59.5 |
63.5 |
61.5 |
|
1983 |
64.0 |
66.3 |
54.7 |
59.5 |
65.2 |
66.0 |
|
1984 |
60.9 |
63.9 |
48.3 |
56.1 |
60.4 |
64.6 |
|
1985 |
58.9 |
61.6 |
47.7 |
53.9 |
61.0 |
60.3 |
|
Respondents consulting vaccination records, 1985c |
|
|
|
|
|
|
|
87.0 |
88.5 |
75.2 |
79.6 |
89.7 |
88.6 |
|
|
Measles |
76.9 |
78.1 |
67.2 |
73.5 |
76.7 |
79.0 |
|
Mumps |
75.5 |
77.1 |
62.7 |
70.5 |
76.8 |
77.0 |
|
Poliob |
75.7 |
77.5 |
61.5 |
68.9 |
79.6 |
75.9 |
|
Rubella |
73.8 |
75.0 |
64.1 |
70.4 |
75.0 |
74.6 |
3 years old or younger exceeded 95 percent. The same success rate was achieved by France, West Germany, and the Netherlands with the DPT vaccine (Williams, 1990). The DHHS in its Health Objectives for the Year 2000 (U.S. Public Health Service, 1991) adopted a goal of immunization for 90 percent of U.S. preschoolers.
Immunization levels for children between the ages of 5 and 6 are significantly higher than those for preschoolers. The reason is that laws in every state require up-to-date vaccinations as a prerequisite to school entry. Provisional data for the 1989–1990 school year indicate that at least 97 percent of students in kindergarten through first grade had received a full course of DPT, polio, and measles-mumps-rubella vaccines (Hinman, 1991). The rates for younger children enrolled in day care centers (95 percent for all vaccines) and Head Start programs (between 94 and 97 percent for all vaccines) were slightly lower. For school-age children and children in day care who must meet the vaccination requirements, the DHHS's Year 2000 Health Objective of at least 95 percent coverage for the basic immunization series has been achieved.
A major barrier to vaccination is financial in that private-sector administration of vaccines currently costs about $300 ($200 for vaccines and $100 for physician visits) before children can enter school. Public-sector prices for the vaccines are approximately $90 (Hinman, 1991). Because parents generally are not charged the full cost of the vaccines, federal support and state willingness to appropriate funds for vaccination have been the deciding factors in whether health departments and nonprofit agencies can vaccinate all those needing the service.
A 1986 survey of health care accessibility found that children of the poor and the near poor were 50 percent more likely than those of higher-income groups not to have up-to-date immunizations. The survey found
that lack of insurance was even more of a barrier. Only 1 percent and 6 percent of children with Medicaid or private insurance, respectively, lacked up-to-date immunization, compared with 19 percent of those not insured (Wood et al., 1990). Medicaid covers immunizations, either on its own or through its Early Periodic Screening, Diagnosis, and Treatment program; some but not all private insurers offer this coverage. These findings thus show the importance of health insurance coverage for specific services.
In addition to these economic barriers, a number of organizational and structural impediments lie in the way of access to immunization. Key among them is the lack of a comprehensive system in the United States for identifying and notifying individuals who need immunization. Health care providers, for various reasons, may fail to administer all indicated vaccines at a single visit. The process of seeking immunizations itself may contain disincentives if, for example, vaccination is conducted on an appointment–only basis or at times that are inconvenient. Finally, physicians who insist on performing vaccinations only during well-child visits (a laudable goal) may as a result delay immunization for weeks or months, given the backlog of such appointments in many medical offices (Hinman, 1991). In fact, pediatricians and family physicians appear to be more and more reluctant to provide immunizations in the office setting. A survey in Dallas, Texas, found that an increasing number of patients were being referred to public facilities. The reasons included inability of patients to pay, the cost of vaccines to physicians, and, in the case of family practitioners, concern over liability (Schulte et al., 1991).
Recommendations
Immunization Surveys. The CDC has addressed the lack of current data on preschool immunization by adding items to the 1991 National Health Interview Survey and by sponsoring a program of research and demonstration projects targeting specific barriers to immunization. While these activities will fill the immediate need for better insight into immunization status, the committee believes that a long-term solution, based on compiled immunization records (see the next recommendation), will provide more reliable data for the future.
School–Based Reporting System. In most, if not all, school systems, parents are required to submit immunization records prior to enrolling their children. These records contain the dates of specific immunizations, which could be reported to state health departments (and, in turn, to the CDC) in a standard format. This reporting would permit a retrospective analysis of whether the school-age cohort received scheduled vaccinations on time. Consideration should be given to the extent of the burden of including
additional information such as place of immunization. The committee recognizes that there may be some drawbacks to the approach in terms of additional paperwork, delayed reporting, and difficulty in linking the data to other types of information that can be obtained through surveys. Nevertheless, the committee believes that the potential of this strategy for improving the accuracy of vaccination reporting is substantial.
Research on Special Populations. Research is needed to understand particular problems in determining the immunization status of special populations (e.g., undocumented aliens) and how barriers discourage specific groups from receiving necessary immunizations.
Outcome Indicator: Incidence of Vaccine-Preventable Childhood Diseases
Measles, mumps, rubella, diphtheria, pertussis, polio, and tetanus are among the most preventable of infectious diseases. (HIB encephalitis immunization, which recently became available, will be recommended for future monitoring.) Although the incidence of these diseases in the United States is low (because of widespread immunization), periodic outbreaks occur because of lapses in immunization coverage. In countries in which effective vaccines are not routinely available, these diseases still cause significant levels of illness and death.
Some countries monitor the immunization status of all age groups. In the United States, however, only the immunization status of entering school-age children is routinely monitored. Although a large percentage of children are vaccinated by the time they begin school, preschool children (under age 5) and immigrants often are not immunized. Inadequate levels of vaccination in these two groups are believed to contribute to outbreaks of vaccine-preventable diseases. Absent a system for monitoring the immunization status of the entire U.S. population, the incidence of vaccine-preventable diseases is a good indicator of access problems related to vaccination, a key preventive health service.
Measuring the Indicator
States report data on the seven selected vaccine-preventable diseases noted above to the CDC, which has developed a set of standardized case definitions for notifiable diseases (Chorba et al., 1990). Incidence can be expressed both as the total number of cases and as cases per 100,000 population. Data are normally collected by month and year; outbreaks of infectious disease, however, typically occur in cycles, once every several years. A low rate of disease in a given year does not indicate the absence of a
problem; rather, the disease's magnitude must be interpreted in relation to its natural history. This makes year-to-year comparisons of the number of cases of a particular disease problematic, because a small number of cases in one year may mask a problem with immunization rates.
Any outbreak is an indication of a problem in immunization. Comparing the number of outbreaks, their duration, and the total number of people infected over the course of the outbreak provides the most useful information. To prevent an outbreak, enough people in a given population must be immunized to establish what is termed ''herd immunity." An outbreak means that the level of immunity—and thus the level of immunization—in the population is below a certain minimum rate.
A major problem in tracking incidence accurately is that reporting for many of these diseases is incomplete. For diseases that are now rare, nonreporting may occur as a result of incorrect diagnosis. During an outbreak of a disease, individual physicians may become lax in their reporting as more cases surface. This latter problem tends to obscure the magnitude of an outbreak. The current infectious disease reporting system is particularly unreliable for data on the incidence of diseases in special populations. The accuracy of information about incidence among minorities, for example, is influenced by variations in the reporting systems of different states and by variations in the quality and completeness of reporting, which may reflect differences in access to medical care (Buehler et al., 1989).
Trends in the Data
Table 3-12 provides data on the occurrence of the seven vaccine-preventable diseases from 1980 through 1989. The number of cases of diphtheria and paralytic polio was quite small throughout the decade. (The return of these diseases would be a serious sentinel event.) The number of cases of tetanus dropped from 95 in 1980 to 53 in 1989; the number of cases of rubella fell from nearly 4,000 in 1980 to around 400 in 1989. The number of cases of mumps declined from approximately 8,600 in 1980 to below 3,000 in 1985 but then increased in succeeding years, sometimes dramatically. Cases of measles declined substantially in the early 1980s, from 13,500 in 1980 to fewer than 3,000 annually from 1982 through 1985. Measles cases increased to more than 6,000 in 1986; however, after subsiding in 1987 and 1988, measles cases rose to approximately 18,000 in 1989.
The incidence of measles increased more than fivefold from 1988 to 1989, from 1.38 cases per 100,000 to 7.33 per 100,000. The current outbreak saw another escalation in 1990, when more than 25,000 cases were detected. (The actual number may be even higher because it is possible that, as cases of measles became more common, medical facilities became less likely to report them.) The outbreak has focused renewed attention on
TABLE 3-12 Reported Cases of Vaccine-Preventable Diseases, Selected Years, 1970–1989
|
|
Diphtheria |
Measles |
Mumps |
Pertussis |
Polio |
Rubella |
Tetanus |
|||||||
|
Year |
No. of Cases |
Cases/ 100,000 |
No. of Cases |
Cases/ 100,000 |
No. of Cases |
Cases/ 100,000 |
No. of Cases |
Cases/ 100,000 |
No. of Cases |
Cases/ 100,000 |
No. of Cases |
Cases/ 100,000 |
No. of Cases |
Cases/ 100,000 |
|
1970 |
435 |
0.21 |
47,351 |
23.23 |
104,953 |
5.55 |
4,249 |
2.08 |
31 |
0.02 |
56,552 |
27.75 |
109 |
0.06 |
|
1975 |
307 |
0.14 |
24,379 |
11.44 |
59,647 |
27.99 |
4,249 |
2.08 |
31 |
0.02 |
16,652 |
7.81 |
252 |
0.12 |
|
1980 |
3 |
0.0 |
13,506 |
5.96 |
8,576 |
3.86 |
1,73 0 |
0.82 |
8 |
0.00 |
3,904 |
1.72 |
95 |
0.04 |
|
1981 |
5 |
0.0 |
3,124 |
1.36 |
4,941 |
2.20 |
1,248 |
0.54 |
6 |
0.00 |
2,077 |
0.91 |
72 |
0.03 |
|
1982 |
2 |
0.0 |
1,714 |
0.74 |
5,270 |
2.46 |
1,895 |
0.82 |
8 |
0.00 |
2,325 |
1.00 |
88 |
0.04 |
|
1983 |
5 |
0.0 |
1,497 |
0.64 |
3,355 |
1.55 |
2,463 |
1.05 |
15 |
0.01 |
970 |
0.41 |
91 |
0.04 |
|
1984 |
1 |
0.0 |
2,587 |
1.10 |
3,021 |
1.32 |
2,276 |
0.96 |
8 |
0.00 |
752 |
0.32 |
74 |
0.03 |
|
1985 |
3 |
0.0 |
2,822 |
1.18 |
2,982 |
1.30 |
3,589 |
1.50 |
7 |
0.00 |
630 |
0.26 |
83 |
0.03 |
|
1986 |
— |
0.0 |
6,282 |
1.61 |
7,790 |
3.37 |
4,1 95 |
1.74 |
6 |
0.00 |
551 |
0.23 |
64 |
0.03 |
|
1987 |
3 |
0.0 |
3,655 |
1.50 |
12,848 |
5.43 |
2,82 3 |
1.16 |
6 |
0.00 |
306 |
0.13 |
48 |
0.02 |
|
1988 |
2 |
0.0 |
3,396 |
1.38 |
4,866 |
2.05 |
3,450 |
1.40 |
9 |
0.00 |
396 |
0.16 |
53 |
0.02 |
|
1989 |
3 |
0.0 |
18,193 |
7.33 |
5,712 |
2.34 |
4,15 7 |
1.67 |
5 |
0.00 |
396 |
0.16 |
53 |
0.02 |
|
SOURCE: Centers for Disease Control (1989c). |
||||||||||||||
the problem of inadequate vaccine coverage among young children, particularly minority children and children living in inner cities (National Vaccine Advisory Committee, 1991).
Although the increase in measles cases should serve as a warning of the need for early and widespread immunization, it should not obscure the major progress that has been made in reducing the incidence of this and other vaccine-preventable diseases over the past several decades. There were 435 cases of diphtheria, 47,351 cases of measles, nearly 105,000 cases of mumps, 56,552 cases of rubella, and 109 cases of tetanus in 1970. Only cases of pertussis, after declining for most of the 1970s and 1980s, have risen to a level comparable to that in 1970.
The DHHS's Health Objectives for the Year 2000 propose the eradication of diphtheria and tetanus (in the under-25 age group) and all cases of polio, measles, and rubella. For mumps the Year 2000 goal is 500 cases; for pertussis it is 1,000 cases.
Case reporting of preventable childhood diseases among racial and ethnic minorities is largely incomplete. In one study approximately 40 percent of case reports did not specify the race or ethnicity of the patient. Existing data indicate that minority children, compared with white children, exhibit higher rates of infectious diseases during an epidemic. For example, in 1987 the incidence of measles among Hispanics (2.24 per 100,000 population) was four to five times higher than for other groups (Buehler et al., 1989). The reporting of information about insurance status, family income, and other barriers to access also is incomplete. Moreover, if it is true, as some believe, that private physicians are increasingly reluctant to give immunizations, the site of immunization will be an additional important clue to the barriers that may need to be overcome.
Recommendations
Increased Surveillance. The committee recommends that disease surveillance activities be increased to monitor outbreaks of infectious disease. The data gathered by such efforts should be used to determine whether higher-than-expected rates of preventable diseases are due to identifiable access-related problems. For example, outbreaks provide an opportunity to understand in greater depth how financial and structural barriers faced by vulnerable populations interfere with their ability to obtain preventive services, including immunization.
Provider Education. The committee recommends that CDC intensify its efforts to alert physicians and local health agencies to the importance of reporting cases of infectious diseases. To that end, CDC surveillance activities should be strengthened.
OBJECTIVE 3: EARLY DETECTION AND DIAGNOSIS OF TREATABLE DISEASES
Utilization Indicators: Breast and Cervical Cancer Screening Procedures
There are a number of diseases for which early detection is important enough to justify screening large segments of the population. For the screening to be worthwhile, an effective medical intervention must be available that can treat the disease of interest at an early stage. (However, not all of the screening tests that are justified in clinical practice are useful as access indicators.)
Two sets of screening tests—clinical breast examinations (physical palpation by a health care professional) and mammography for detecting breast cancer, and Pap smears for detecting cervical dysplasia and the less commonly occurring invasive cervical carcinoma—have high sensitivity and high yield; they also detect conditions with high prevalence. Moreover, morbidity and mortality from these cancers are reduced when they are detected at an early stage and the patient is treated appropriately. The timing of the screening tests depends on the age and risk profile of the woman being tested. In most cases the earlier in its progression that the disease is detected, the greater the chance of preventing cancer-related mortality.
For some women less than optimal use of these screening tests indicates the presence of one or more barriers to primary health care services. Yet for other women the failure to undergo a recommended screening test may reflect a lack of knowledge about the test's benefits or insufficient counseling by the woman's health care provider. These latter circumstances are less clearly a problem of access to health care than an indication of poor quality or inadequate medical care. If specific groups consistently receive substandard care, however, this could indicate the presence of an access barrier.
Measuring the Indicator
The measure of utilization of breast cancer and cervical cancer screening tests is the percentage of women in specific age groups who undergo the procedures during a given time period. Two of the primary sources of data for monitoring the use of cancer screening services are the National Health Interview Survey (NHIS), conducted periodically by the National Center for Health Statistics, and the Behavioral Risk Factor Surveillance System, a state-based program of periodic surveys sponsored by the CDC. The most recent data on mammography come from a special survey completed in 1990, the Mammography Attitudes and Usage Study.
Because Objective 3 focuses on routine preventive screening services, we report data from the NHIS that distinguish screening procedures from the same tests that are also ordered for patients who require diagnostic workups as a follow-up to specific health problems. In interpreting trend data it is important to determine whether the data include both categories of patients. Because there has been special interest in the effects of language and culture on the use of screening services, the NHIS breaks out data for Hispanics.
One problem of interpreting data on the use of screening services is the difficulties involved in separating medical access problems from concerns about the quality or adequacy of the medical care itself. It may be that access to screening services is tied in complex ways to the structural characteristics of the delivery system, aspects that have not been investigated by researchers. Some of the difficulty in distinguishing true access problems from other influences on screening behavior may be rooted in the surveys themselves, which frequently are composed of open-ended questions rather than questions that force respondents to choose one of several specific answers.
Trends in the Data
Clinical Breast Examination/Mammography. The American Cancer Society and the National Cancer Institute recommend that all women have routine clinical breast examinations, although consensus about the precise frequency of the exams has not as yet been reached.
Table 3-13 shows that only about 60 percent of women over age 40 have had a clinical breast exam within the past three years, with no major differences by race/ethnicity. Blacks and Hispanics, however, were over 11 percent more likely than whites never to have had an exam. Women over
TABLE 3-13 Percentage of Women Age 40 and Older Receiving a Clinical Breast Exam, by Race/Ethnicity, 1987
|
Race |
Had Procedure Within Past 3 Years |
Had Procedure More Than 3 Years Ago |
Had Procedure for Health Problem |
Never Had Procedure |
|
All races |
58.7 |
14.6 |
7.2 |
19.5 |
|
Black (non-Hispanic) |
57.9 |
8.9 |
5.0 |
28.2 |
|
Hispanic |
56.7 |
11.2 |
4.0 |
28.1 |
|
White (non-Hispanic) |
59.3 |
15.8 |
7.8 |
17.0 |
|
SOURCE: Unpublished data from the National Health Interview Survey, National Center for Health Statistics, 1987. |
||||
TABLE 3-14 Percentage of Women Age 40 and Older Who Reported Having Had Mammography, by Race/Ethnicity, 1987
|
Race |
Had Procedure Within Past 3 Years |
Had Procedure More Than 3 Years Ago |
Had Procedure for Health Problem |
Never Had Procedure |
|
All races |
23.0 |
7.3 |
6.6 |
63.1 |
|
Black (non-Hispanic) |
18.1 |
5.9 |
5.6 |
70.3 |
|
Hispanic |
16.0 |
7.1 |
3.1 |
73.8 |
|
White (non-Hispanic) |
24.3 |
7.6 |
7.0 |
61.1 |
|
SOURCE: Unpublished data from the National Health Interview Survey, National Center for Health Statistics, 1987. |
||||
age 70 are generally less likely to have had an exam, a problem that is more pronounced for older blacks and Hispanics. Fifty-one percent of black women and 47 percent of Hispanic women over the age of 70 have never had an exam, compared with 29 percent of comparably aged white women (unpublished data from the NHIS, 1987).
Yet despite age- and race-related differences, the situation has improved over the past 15 years. The increase was most dramatic for black women age 60 to 79, whose use of the exam (in the previous two years) jumped 25 percentage points (from 39.1 percent in 1973 to 64.5 percent in 1985). In all age groups, black women increased their use of breast exams to a greater extent than white women. By 1985, compared with white women, a larger percentage of black women were undergoing the screening procedure (Makuc et al., 1989).
There is general agreement that women over age 50 should receive an annual mammogram. There is considerable disagreement, however, among major health organizations about whether regular or any testing should be done between ages 35 and 49 (U.S. Preventive Services Task Force, 1989; Hayward et al., 1991a).
The 1987 NHIS data (Tables 3–13 and 3–14) show that fewer than half as many women had had a mammogram in the past three years as had had a clinical breast examination. Blacks and Hispanics were less likely to have had the procedure, and the elderly—especially blacks and Hispanics—were less likely to have had it than younger women. Seventy-two percent of white women over age 70 had never had a mammogram—11 percent more than the comparable figure for younger white women. Among black women over age 70, 82.4 percent had never had a mammogram. In 1987 slightly more than 70 percent of all black women age 40 and older had never had a mammogram. Older Hispanic women were the least likely of any group to
have had a mammogram (86.7 had not). Overall, according to the NHIS data, 73.8 percent of Hispanic women age 40 and over had never had a mammogram.
More recent studies seem to indicate a dramatic increase in mammography screening in all groups, although differences persist by age and race. Mammogram screening increased between 1987 and 1990 (Table 3-15), probably as a result of media coverage and enhanced public health promotion efforts. By 1990, among women over age 40, 64 percent reported having ever had a mammogram, nearly twice the proportion of three years earlier (Centers for Disease Control, 1990).
TABLE 3-15 Percentage of Women Who Reported Ever Having Had a Mammogram, by Race, Age, Income, and Education
|
|
MAUS a (N = 980) |
NKAB b (N = 836) |
NHIS c (N = 6,858) |
|||
|
Category |
% |
95% CI d |
% |
95% CI |
% |
95% CI |
|
Race |
||||||
|
White |
65 |
62–68 |
69 |
65–73 |
39 |
38–40 |
|
Black |
58 |
47–69 |
59 |
52–66 |
30 |
28–32 |
|
Age (yrs) |
|
|
|
|
|
|
|
40–49 |
64 |
59–69 |
68 |
62–74 |
41 |
39–43 |
|
50–59 |
71 |
55–77 |
70 |
64–76 |
44 |
42–46 |
|
60–69 |
65 |
59–71 |
71 |
65–77 |
38 |
36–40 |
|
>70 |
56 |
49–63 |
59 |
51–67 |
28 |
27–29 |
|
Annual income |
|
|
|
|
|
|
|
<$25,000 |
60 |
55–65 |
64 |
59–69 |
32 |
31–33 |
|
≥$25,000 |
71 |
67–76 |
74 |
69–79 |
47 |
45–49 |
|
Education |
|
|
|
|
|
|
|
Less than high school |
58 |
50–66 |
58 |
50–66 |
25 |
24-26 |
|
High school |
65 |
60–70 |
67 |
62–72 |
41 |
40-42 |
|
Some college |
72 |
66–78 |
72 |
66–78 |
49 |
47-51 |
|
College degree or more |
74 |
68–80 |
79 |
72–86 |
49 |
47–51 |
|
Total |
64 |
61–67 |
67 |
64–71 |
37 |
36–38 |
|
a Mammography Attitudes and Usage Study, February 1990; weighted to reflect the age-, education-, and race-specific distribution of U.S. women in 1989. b National Knowledge, Attitudes, and Behavior Survey, April 1989–February 1990; weighted to reflect the age-, education-, and race-specific distribution of U.S. women in 1988. c Unpublished data from the National Health Interview Survey, National Center for Health Statistics, 1987. d Confidence interval. SOURCE: Centers for Disease Control (1990). |
||||||
Breast cancer screening varies considerably by region. The 1987 Behavioral Risk Factor Surveillance System, for example, revealed a wide range of mammography usage across the states: from 28.6 percent in New Mexico to 57.5 percent in New Hampshire (Centers for Disease Control, 1989a).
Until recently, with the rise in the number of mammograms, a relatively small proportion of women who had had clinical breast exams went on to have mammograms. For example, data from one large, multisite, survey-based study show that a much higher proportion of women have had a clinical breast exam (between 46 and 76 percent) than have undergone mammography (between 25 and 41 percent; National Cancer Institute, Breast Cancer Screening Consortium, 1990b). Because many women now seem to be self-referring to testing sites, the standard patterns linking clinical exams and mammography may be breaking down, causing some concern about continuity of clinical management.
The DHHS in its Health Objectives for the Year 2000 calls for at least 80 percent of American women age 40 and older to have received a clinical breast exam and a mammogram and 60 percent of women over the age of 50 to have received the two screening tests within the preceding two years (U.S. Public Health Service, 1991). The 1987 baseline rates indicate that only 36 percent of women age 40 and older have ever had both exams and only 25 percent had had both in the previous two years.
The role of economic and noneconomic barriers to screening services needs to be sorted out with further research. In 1985 poor women were 10 to 13 percent less likely than nonpoor women to have undergone a clinical breast exam within the past two years. For most poor women, however, failure to have a clinical breast exam did not appear to be related to a problem of entry into the health care system. For both younger (age 20–39) and older (age 60–79) women, most of the poverty-related differences in the use of screening services occurred among those who had recently visited a health care provider. In fact, data from the NHIS indicate that nearly three-quarters of all women who had not had a breast exam within the past two years reported visiting a physician during that period. Similar results have been obtained from state-based surveys of women's use of health care services (Centers for Disease Control, 1988). These data suggest that even though poor women have contact with the health care system, they may not necessarily receive the services they need, especially screening or preventive services. Whether these data measure poor access to appropriate services or a low quality of care is debatable.
The most frequent reasons for not having a mammogram cited by women in the NHIS were that they had never thought about it or that there was no apparent problem warranting such a procedure. Lack of a recommendation for a mammogram by a physician was the second most frequently cited
TABLE 3-16 Percentage of Women Age 18 and Older Who Reported Having Had a Pap Smear, by Race/Ethnicity, 1987
|
Race |
Had Procedure Within Past 3 Years |
Had Procedure More Than 3 Years Ago |
Had Procedure for Health Problem |
Never Had Procedure |
|
All races |
65.0 |
15.8 |
7.8 |
11.3 |
|
Black (non-Hispanic) |
68.2 |
9.2 |
10.6 |
11.9 |
|
Hispanic |
57.7 |
10.3 |
7.4 |
24.7 |
|
White (non-Hispanic) |
65.7 |
17.7 |
7.6 |
9.0 |
|
SOURCE: Unpublished data from the National Health Interview Survey, National Center for Health Statistics, 1987. |
||||
reason (National Cancer Institute, Breast Cancer Screening Consortium, 1990b). It is not clear how women would have assessed the relative roles of insurance coverage or inability to pay as barriers to access to care because these questions were not specifically asked.
Pap Tests. In the United States the recommended frequency of Pap screening for women over age 18 is every one to three years, according to the discretion of the physician (U.S. Preventive Services Task Force, 1989). As of 1987 about two-thirds of U.S. women over the age of 18 had had a Pap smear in the previous three years (Table 3-16). Hispanic women in general had lower rates of testing, and, as was true for breast cancer screening, women over age 70, particularly black and Hispanic women, were much less likely than white women to have ever had a Pap test or to have had one within the past three years. Elderly white women were more than twice as likely as younger white women never to have had the procedure (22.6 percent had not had the test). About twice this proportion of same-age minority women, 43 percent, reported never having had a Pap smear (analysis of unpublished data from the NHIS, 1987).
Historical trend data on the use of Pap tests are similar to those for the use of clinical breast exams and mammography. From 1973 to 1985 there was a small increase (from 63.8 percent in 1973 to 64.8 percent in 1985) among all women in the use of the test for screening and diagnostic purposes. For black women, use of the test increased 10 percent (Makuc et al., 1989).
One study that analyzed the 1987 NHIS screening data found that 15.1 percent of Hispanic women had never heard of a Pap test, compared with 4.1 percent of black women and 2.1 percent of white women. Similar, though less dramatic, differences were observed in the proportion of women who had undergone the screening procedure. The reason for the gap between
Hispanics and other racial and ethnic groups is unclear, although the authors of the report suggest that cultural avoidance of medical tests by native-Spanish-speakers may be a factor (Harlan et al., 1991). The fault may also lie in a health care delivery system that does not respond appropriately to the health education needs of ethnic communities.
The national health objectives for the year 2000 set a target of increasing to 95 percent the proportion of women 18 and older who have received at least one Pap test. By the year 2000, 80 percent of Hispanic and low-income women should have received a Pap smear within the preceding three years, according to the objectives. The target for women with less than a high school education is 75 percent; for women over age 70, the goal is 70 percent (U.S. Public Health Service, 1991).
As was true for breast cancer screening, data from the NHIS indicate that poor or less educated women are less likely than nonpoor or well-educated women to undergo Pap testing. The majority of reasons cited by women for not obtaining a Pap test reflected a lack of appreciation of the importance of screening rather than cost considerations or lack of access to a physician. A majority (75 percent) of women who had not had the test within the past two years had nevertheless visited a physician during that period. These data raise the question of why the test was not performed during the visit and whether the barrier to screening here is one of poor-quality care rather than access to care.
The usual source of a woman's medical care appears to influence whether she will receive screening for cervical cancer. Women who visited a physician's office were less likely to be screened than those who sought medical care at a health maintenance organization (75.1 percent compared with 85.2 percent, respectively). Only 58.2 percent of women with no regular source of care had had a Pap test within the past three years. Most of the women in this latter group received the test at an outpatient department or public health or community clinic.
A focus-group interview study of physicians found that financial and structural barriers may play an important role in less-than-optimal screening rates. Physicians reported having mixed feelings about pressing poor patients to pay for and undergo screening procedures, particularly if the patients were having difficulty paying their rent. Similarly, when a diabetic patient can barely afford the cost of medication, her physician may be reluctant to urge her to have a mammogram that is expensive and often not covered by insurance. For poor patients, financial problems are exacerbated by the necessity of coping with lack of transportation, child care, and the ability to take time off from work.
An additional aspect that may explain lack of screening is the reluctance of some physicians to perform it, based on their feelings of discomfort or their view that these tests are best left to gynecologists. (Internists
and family practitioners, however, are specifically trained in these procedures during residency.) It could be argued that this is not an access problem or that structural deficiencies in the organization of care make it an access problem that reaches beyond the usual financial barriers.
Recommendations
Improved Survey Instruments. The committee believes that surveys about screening services, like the cancer control supplement of the NHIS, should include questions that explore in greater depth the reasons people do not obtain cancer screening services. Survey questions should focus on the effects of insurance coverage and cost issues.
More Frequent Reporting. In those years in which NHIS prevention or cancer supplements are not administered, the Behavioral Risk Factor Surveillance System (BRFSS) should be used to track trends in the data. To accomplish this, questions should be added to the BRFSS surveys to collect information about insurance status, income, and regular source of care.
Outcome Indicator: Incidence of Late-Stage Breast and Cervical Cancers
Late-stage cancers are those that have invaded contiguous tissues and organs or that have spread through the blood or lymphatic system to other parts of the body. Late-stage cancers present a more difficult clinical treatment challenge than those diagnosed at an earlier stage. Late-stage breast and cervical cancers are invariably fatal—therapy in these cases is palliative and not curative.
Discovery of late-stage cancers may indicate the underuse of an effective screening test. Alternatively, or in addition, late-stage cancer may also reflect inappropriate medical follow-up of a diagnosed disease or progression of the cancer in some cases despite appropriate therapy. A recent review article identifies the many steps at which the cervical cancer detection system may fail:
… starting with the initial clinical examination, continuing with the taking of the smear sample and laboratory errors in screening and interpretation, and ending with the clinician's failure to understand the report or take appropriate action and in some instances, with the patient's failure to follow the guidance of the physician. (Koss, 1989)
A large relative difference in late-stage cancer among different groups is an important clue to the existence of problems with access and, potentially, with subsequent treatment. In the case of breast cancer, the diagnosis of late-stage disease may indicate the failure of patients to undergo clinical
breast examination or mammography at the recommended intervals. Likewise, the diagnosis of late-stage invasive cervical cancer may indicate underuse of the Pap test.
Measuring the Indicator
Clinically, breast and cervical cancers are grouped into four stages. Ranked in increasing order of severity, they are categorized as in situ, localized, regional, and distant. Diagnoses for any population group of cancers at the last two stages suggest a pattern that may be strongly influenced by barriers and, therefore, a problem in equity of access.
Most national data about cancer incidence come from state and regional tumor registries, which report to the National Cancer Institute's SEER (Surveillance, Epidemiology, and End Results) program. Not all registries report their data to SEER; furthermore, cancer registries in general may not provide a representative sample of the U.S. population. Nonetheless, the SEER system does offer information on more than 1.5 million cases of cancer in geographic areas covering almost 10 percent of the U.S. population. Caution must be exercised, however, in using this data base to generalize about subpopulations. Because the geographic areas included in SEER have changed over the years, data from a consistent set of tumor registries also are reported.
A further shortcoming of the SEER system, for purposes of access monitoring, is that it includes no information about patient income levels or insurance status. Consequently, little is known about these barriers. Income data potentially could be imputed from patient zip code data in tumor registries. Differences in cancer incidence among residents of low-and high-income counties are included in the committee's analysis.
Trends in the Data
Breast Cancer. Breast cancer accounts for 28 percent of all newly diagnosed cancers in women and 18 percent of female cancer deaths (American Cancer Society, 1989). In 1988 the incidence of breast cancer was 112.9 per 100,000 among white women and 96.5 per 100,000 among black women. The age-adjusted death rate from breast cancer for white women was 23 per 100,000; for blacks it was 27 per 100,000. Whites also have higher five-year survival rates than blacks (National Center for Health Statistics, 1990b). These discrepancies are generally attributed to later case finding among blacks. Women who undergo breast cancer screening are about 20 percent more likely than unscreened women to survive five years or longer (U.S. Preventive Services Task Force, 1989).
As Tables 3-17A and 3-17B indicate, a gap has persisted between black
TABLE 3-17A Percentage of Breast Cancers Diagnosed at a Late Stagea (total number of staged cases in parentheses) by Period and Race
|
Period |
Whites |
Blacks |
||||||
|
All SEER areas |
|
|
||||||
|
1973–1977 |
47.5 (39,978) |
56.6 (2,659) |
||||||
|
1978–1982 |
47.4 (46,277) |
53.8 (3,511) |
||||||
|
1983–1987 |
39.5 (60,390) |
49.8 (4,787) |
||||||
|
Selected SEER areas b |
|
|
||||||
|
1973–1977 |
48.8 (28,826) |
56.8 (2,566) |
||||||
|
1978–1982 |
47.5 (33,783) |
53.7 (3,417) |
||||||
|
1983–1987 |
39.2 (44,406) |
50.0 (4,644) |
||||||
|
SEER, Surveillance, Epidemiology, and End Results (program). a Includes “regional” and “distant.” Unstaged cancers are excluded from the denominator. b Atlanta, San Francisco/Oakland, Connecticut, Seattle, and Detroit. |
||||||||
and white women in the proportion of breast cancers diagnosed at late stages. According to SEER program data, the decline in the number of late-stage breast cancers diagnosed among whites in the 1980s has not quite been matched in blacks. Initially, the committee was concerned about time-series analysis that did not include the same group of geographic areas with roughly similar racial compositions over time. However, limiting the analysis to selected tumor registries did not alter the findings.
When high- and low-income areas are compared (Table 3–17B), high-income areas have about 8 percent fewer cases of late-stage cancers in the
TABLE 3-17B Percentage of Breast Cancers Diagnosed at a Late Stagea (total number of staged cases in parentheses), by County Per-Capita Income
|
Period |
Lowb |
Highb |
|
1973–1977 |
46.6 (4,270) |
46.0 (4,302) |
|
1978–1982 |
49.2 (4,959) |
45.7 (5,116) |
|
1983–1987 |
43.7 (6,336) |
36.1 (6,757) |
|
a Includes “regional” and “distant.” Unstaged cancers are excluded from the denominator. b Low income is the bottom 10 percent and high income the top 10 percent of all cases grouped by per-capita income of the country of residence. SOURCE: Unpublished data from the SEER program. |
||
most recent period than in the earliest period. Low-income areas improved only about a third as much after a period of increases in the middle period.
Cervical Cancer. Five thousand women die annually from cervical cancer. The incidence was twice as high among black women (15.8 per 100,000) as it was among white women (7.8 per 100,000) from 1983 through 1987. Mortality was nearly three times as high among blacks during the same period (6.4 per 100,000 for blacks compared with 2.3 per 100,000 for whites). From 1981 through 1986 the five-year survival rate for white women was 67.3 percent; for black women it was 57.1 percent.
Early diagnosis is closely linked to reduced rates of invasive cervical cancer. Such diagnosis can reduce the mortality rate by up to 75 percent (U.S. Public Health Service, 1991). In one study the cumulative incidence of invasive cervical cancer was reduced almost 84 percent when Pap tests were conducted every five years; it was reduced nearly 93 percent when the interval between testing was reduced to two years (International Agency for Research on Cancer, Working Group on Evaluation of Cervical Cancer Screening Programmes, 1986).
Among whites the proportion of cases of late-stage (regional and distant) cervical cancer remained approximately the same in the 1970s and 1980s. In contrast, the proportion of late-stage diagnoses for blacks, which was approximately the same as that for whites in the mid-1970s, nearly doubled by the mid-1980s (Table 3-18A). With respect to income levels, only a small difference persists over time, and that gap appears to be narrowing (Table 3-18B). As Figure 3-2 illustrates, survival is strongly linked to the stage of diagnosis.
TABLE 3-18A Percentage of Cervical Cancers Diagnosed at a Late Stage a (total number of staged cases in parentheses), by Period and Race
|
Period |
Whites |
Blacks |
|
All SEER areas |
|
|
|
1973–1977 |
8.5 (19,594) |
8.5 (4,113) |
|
1978–1982 |
9.4 (19,429) |
11.3 (3,681) |
|
1983–1987 |
8.2 (21,585) |
15.0 (3,148) |
|
Selected SEER areas b |
|
|
|
1973–1977 |
8.2 (13,792) |
8.3 (4,014) |
|
1978–1982 |
8.7 (14,312) |
11.3 (3,591) |
|
1983–1987 |
7.8 (15,464) |
15.0 (3,050) |
|
SEER, Surveillance, Epidemiology, and End Results (program). a Includes “regional” and “distant.” Unstaged cancers are excluded from the denominator. b Atlanta, San Francisco/Oakland, Connecticut, Seattle, and Detroit. |
||
TABLE 3-18B Percentage of Cervical Cancers Diagnosed at a Late Stage a (total number of staged cases in parentheses), by County Per-Capita Income
|
Period |
Lowb |
Highb |
|
1973–1977 |
10.3 (2,337) |
7.8 (2,139) |
|
1978–1982 |
10.3 (2,332) |
7.2 (2,064) |
|
1983–1987 |
9.4 (2,627) |
8.5 (2,274) |
|
a Includes “regional” and “distant.” Unstaged cancers are excluded from the denominator. b Low income is the bottom 10 percent and high income the top 20 percent of all cases distributed by per-capita income of the country of residence. SOURCE: Unpublished data from the SEER program. |
||
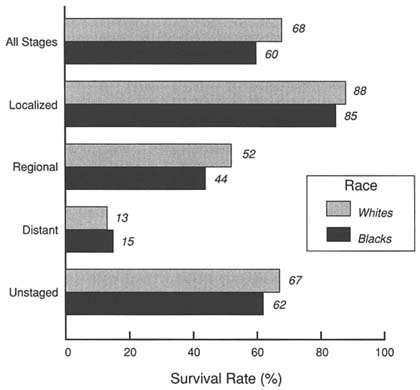
FIGURE 3-2 Five-year survival rates by stage for cancer of the cervix uteri, 1981–1986. SOURCE: National Cancer Institute (1990a).
Recommendations
Enhancing the SEER Data. The SEER data should contain more background information, including the socioeconomic and insurance status of patients. In the interim, zip code analyses to impute income must suffice.
A Clearinghouse for Analyzing Access Problems. The committee believes that the nation needs a clearinghouse of cancer registry data that can be used to analyze access problems. It is beyond the scope of this committee's charge to determine whether this could or should be achieved through expansion of the SEER program or whether some other organizational structure or cooperative arrangement would be better suited to accomplish this objective.
Research Studies. More detailed studies are needed to determine why increases in the use of screening tests by blacks are not reflected in improvements in stage of diagnosis, mortality, and survival.
OBJECTIVE 4: REDUCING THE EFFECTS OF CHRONIC DISEASES AND PROLONGING LIFE
Utilization Indicator: Continuing Care for Chronic Diseases
Many of the reasons people use medical care are related to the treatment of chronic conditions. These diseases are usually not self-limiting and are ongoing over an extended period. Chronic diseases often limit how well a person functions in society. Many chronic diseases include episodes of acute illness followed by quiescent periods.
Diabetes, asthma, congestive heart disease, and hypertension are examples of chronic diseases that, without regular medical management (follow-up care), can result in repeated hospitalization, premature disability, and death. Adverse consequences of chronic conditions can occur with or without regular medical care, but negative consequences are more common when regular care is absent. Even when life cannot be extended, health care can contribute to improved functioning and can minimize discomfort.
Continuing care for a chronic illness may include periodic tests to monitor a patient's health status, nutritional and other types of counseling to reduce or eliminate patient behaviors that may be harmful to health, and necessary medications and medical and surgical procedures. Underuse of the health care system by those with chronic diseases—as reflected by few or irregular physician visits or a less than optimal regimen of care—may indicate an access problem.
Diabetes offers a useful illustration of how a utilization measure (follow-up care) may be applied to a chronic disease condition. Diabetes is a
relatively common illness. Some 7 million people in the United States have been diagnosed with the disease; another 5 million may have it without knowing it (U.S. Public Health Service, 1991). Although few people die from diabetes directly, the disease is a major indirect contributor to mortality in the United States. In 1987 diabetes was the sixth leading underlying cause of death from disease (National Center for Health Statistics, 1987). Two of the most common diabetes-related causes of death are cardiovascular disease (accounting for somewhat more than half of all deaths) and diabetic ketoacidosis.
Standard treatment for diabetes includes diet, exercise, and the administration of insulin or oral hypoglycemic agents. Physicians prescribe one or a mix of these three treatment modalities, depending on the severity of illness and other patient factors (Drury et al., 1981).
Good health practices, such as not smoking and drinking alcohol only in moderation, and the use of preventive health services, such as regular eye and dental exams, stress management of blood pressure, and control of lipid problems, also are important for maintaining the health of the diabetic patient. In addition, because most care for diabetes rests with the individual patient, patient and family knowledge about the disease and compliance with a recommended course of treatment are crucial.
Thus, continuing contact with a regular health care provider is essential for the effective control of diabetes. A breakdown in patient management can have a significant adverse impact on the speed and severity of the disease's effects on a patient's health status. Similar examples can be cited for other chronic illnesses for which regular medical care can have beneficial results.
Measuring the Indicator
There is no direct, routinely available way to measure the use of particular follow-up health care services for specific chronic diseases, like diabetes, that could be used to measure barriers to access. Periodically, however, the extent to which patients with a particular disease have contact with the personal health care system has been documented through supplements to the NHIS. NHIS supplemental data collection on diabetes was performed in 1976 and 1989. The 1989 NHIS also included supplements on mental health services and digestive disorders. However, data from the 1989 supplements were not available in time to analyze them for this report.
Disease-specific surveys with appropriate questions on barriers are the preferred approach for precise monitoring of access problems. Absent such studies, it is possible nonetheless to make inferences about the adequacy of follow-up care for chronic diseases in general. The NHIS can be used to measure physician contacts with persons who judge themselves to be in fair
to poor health as opposed to excellent, very good, and good health. People who rate their health status as fair or poor often are afflicted with serious chronic health conditions that can be helped by medical management. Perceived health status may be the best indirect variable for measuring chronic, serious, yet manageable conditions like diabetes (Pope, 1988). The committee's analysis of the NHIS indicates that nonelderly people who are in fair to poor health, compared with those in good to excellent health, are two-and-a-half times as likely to be unable to carry out major activities of living. They also report four times the number of chronic conditions.
The committee used two measures of physician use in its analysis of chronic illness care. The first was a stringent measure of access to care that focused on entry into the system—that is, whether an individual had had any contact with a physician in the past year. Respondents to the health interview survey were asked to report the interval since the last time they had a physician contact in person or by telephone. The second measure focused on the comparative frequency of use, namely, the average number of contacts per year by insurance status, income level, and other characteristics relevant to access.
Trends in the Data
Having health care coverage makes a major difference in whether persons who rate their health as fair or poor have at least one physician contact within a year. Table 3–19 compares such people with different types of insurance coverage. In 1989 the uninsured were more than twice as likely as those with private health insurance, Medicaid, or Medicare to go without physician contact. Those with both Medicare coverage and supplemental private insurance were even more likely to have had contact with a doctor. In general, there was only a very slight increase in access to physicians for all coverage groups during the 1980s.
For the uninsured in fair to poor health, level of income can be a major factor in determining physician contact (see Table 3–20). The uninsured at the lowest income level are more than twice as likely as those with middle-range incomes not to have had a physician contact in the past year. For most of those with coverage, level of income is only marginally related to physician use, with one exception: Medicare recipients without private insurance are much less likely to contact a physician if they have a low-income.
Once insurance and income are taken into account, other potential barriers to access do not seem to have a consistent effect on who contacts a physician. Differences in the proportions of those without a physician contact according to race, ethnicity, and geographic location generally disappear when income and insurance are taken into account. One exception is
TABLE 3-19 Percentage of People in Poor/Fair Health Who Did Not Contact a Physician in the Past Year, by Health Care Coverage, Selected Years
|
Insurance Coverage a |
1980 |
1986 |
1989 |
|
Uninsured |
24 |
25 |
22 |
|
Private health insurance |
12 |
11 |
9 |
|
Medicaid only |
11 |
6 |
8 |
|
Medicare only |
14 |
11 |
10 |
|
Medicare and private health insurance |
9 |
6 |
5 |
|
All others |
13 |
7 |
8 |
|
a Insurance defination are as follows: Medicaid only—if the person has a current Medicaid card or is covered by Aid to Families with dependent children, Supplemental Security Income, or public assistance and has no other insurance coverage; Medicare plus other health insurance—Medicare plus either private insurance, Medicaid, or CHAMPUS/ Veterans Administration or military health insurance. Private health insurance includes only people who reported private insurance and no other types of insurance. SOURCE: Unpublished data from the National Health Interview Survey, National Center for Health Statistics, 1980, 1986, 1989. |
|||
TABLE 3-20 Percentage of People in Poor/Fair Health Who Did Not Contact a Physician in the Past Year, by Type of Insurance and Income Level, 1989
|
Insurance Coverage a |
Lowest Income |
Lower-Middle Income |
Middle Income |
Highest Income |
|
|
Uninsured |
28 |
19 |
12 |
||
|
Private health insurance |
12 |
11 |
8 |
8 |
|
|
Medicaid only |
10 |
7 |
|||
|
Medicare only |
18 |
12 |
8 |
||
|
Medicare and private health insurance |
6 |
6 |
5 |
5 |
|
|
a Insurance defination are as follows: Medicaid only—if the person has a current Medicaid card or is covered by Aid to Families with dependent children, Supplemental Security Income, or public assistance and has no other insurance coverage; Medicare plus other health insurance—Medicare plus either private insurance, Medicaid, or CHAMPUS/ Veterans Administration or military health insurance. Private health insurance includes only people who reported private insurance and no other types of insurance. * Estimates for which the relative standard error exceeds 30 percent are not reported. SOURCE: Unpublished data from the National Health Interview Survey, National Center for Health Statistics, 1989. |
|||||
rural residents who are both uninsured and at the lowest income level; this is the group that is least likely to have had a physician contact. Thirty-five percent of rural residents had not had a contact, compared with 24 percent of those who lived in similar circumstance but in a metropolitan area.
As Table 3-21 shows, lack of insurance as a barrier is somewhat muted for sick children under age 5. Children over age 5 without insurance, however, are more than twice as likely to have had no physician contact, despite how their health is perceived, than older children who have insurance.
Among persons who rated themselves as being in poor or fair health in 1989 (the committee's indirect indicator of underlying chronic disease), the average number of physician visits per year (estimated from a two-week recall question) by those with private health care coverage (14.8) or Medicaid (16.9) was substantially higher than the number of visits by people without insurance (9.1; Table 3–22). For persons with Medicaid or private health insurance, blacks reported fewer visits than whites with the same health status.
Although a stepwise relationship can be found between physician contacts and income levels, for the most part this relationship is not very strong when health care insurance coverage status is taken into account (Table 3-23). The difference between the high- and low-income categories for the privately insured indicates the probable effect of coinsurance and deductibles. One possible explanation of the high utilization of physician services by Medicaid recipients in the lower middle income group is the likelihood that they have high-cost illnesses that qualify them for the program.
TABLE 3-21 Percentage of People in Poor/Fair Health Who Have Not Contacted a Physician in the Past Year, by Age and Health Care Coverage, 1989
|
Age |
Uninsured |
Medicaid Only |
Private Health Insurance |
|
0–4 |
6 |
1 |
3 |
|
5–17 |
17 |
10 |
8 |
|
18–44 |
24 |
10 |
11 |
|
45–64 |
20 |
6 |
9 |
|
Insurance definitions are as follows: Medicaid only—if the person has a current Medicaid card or is covered by Aid to Families with Dependent Children, Supplemental Security Income, or public assistance and has no other insurance coverage; Medicare plus other health insurance—Medicare plus either private insurance, Medicaid, or CHAMPUS/Veterans Administration or military health insurance. Private health insurance includes only people who reported private insurance and no other types of insurance. SOURCE: Unpublished data from the National Health Interview Survey, National Center for Health Statistics, 1989. |
|||
TABLE 3-22 Average Number of Annual Physician Contacts by Those Who Report Fair/Poor Health, by Health Care Coverage and Race/Ethnicity, 1989
|
Insurance Coverage a |
Total |
White |
Black |
Hispanic |
Non-Hispanic |
|
Uninsured |
9.1 |
9.6 |
7.8 |
9.7 |
6.0 |
|
Private health insurance |
14.8 |
15.6 |
12.0 |
15.2 |
10.7 |
|
Medicaid only |
16.9 |
20.8 |
11.4 |
17.5 |
14.4 |
|
Medicare |
12.9 |
12.8 |
12.7 |
12.7 |
|
|
Medicare and private health insurance |
16.5 |
15.9 |
20.0 |
16.2 |
|
|
a Insurance defination are as follows: Medicaid only—if the person has a current Medicaid card or is covered by Aid to Families with dependent children, Supplemental Security Income, or public assistance and has no other insurance coverage; Medicare plus other health insurance—Medicare plus either private insurance, Medicaid, or CHAMPUS/ Veterans Administration or military health insurance. Private health insurance includes only people who reported private insurance and no other types of insurance. * Estimates for which the relative standard error exceeds 30 percent are not reported. SOURCE: Unpublished data from the National Health Interview Survey, National Center for Health Statistics, 1989. |
|||||
Recommendations
Longitudinal Survey of Individuals with Chronic Diseases. Longitudinal surveys are the most effective way to monitor the effect of access barriers on the ability of chronic disease sufferers to obtain necessary and appropriate care. The epidemiological follow-up studies of the National Health and Nutrition Examination Survey should be explored for their potential to serve this purpose. Several advantages of this approach are detailed below.
-
First, it would be useful to track diseases that are highly prevalent among groups that are likely to face barriers to access. Using the example of diabetes, the Secretary's Task Force on Black and Minority Health noted that "diabetes exemplifies the difference in health status between whites and minority groups…. Blacks, native Americans, Hispanic Americans, and Asian Americans suffer a disproportionate share of the disease, its effects, and the complications that arise from it" (U.S. Department of Health and Human Services, 1986). The task force report identifies demonstration programs that have decreased the adverse consequences of the disease
TABLE 3-23 Average Number of Physician Contacts by Those Who Report Fair/Poor Health, by Family Income and Health Care Coverage, 1989
|
|
|
Levels of Family Income a |
|
|
|
Insurance Coverage b |
Bottom |
Lower Middle |
Middle |
Upper |
|
Uninsured |
7.1 |
11.5 |
7.8 |
|
|
Private health insurance |
13.2 |
13.4 |
16.5 |
19.0 |
|
Medicaid only |
14.7 |
21.4 |
||
|
Medicare only |
14.0 |
13.7 |
16.9 |
|
|
Medicare plus other insurance |
18.1 |
16.1 |
15.5 |
21.8 |
|
Total |
13.5 |
14.7 |
15.8 |
19.3 |
|
a Income grouping are based on family income and are defined separately for people under 65 and for those 65 and older. For those under 65 bottom is less than $9,000 (10.5%), lower middle is $9,000–$24,999 (29.2%), middle is $25,000–$49,999 (39.3%), and upper is $50,000 or more (21.0%). For the elderly, the corresponding figures are bottom, less than $6,000 (9.6%); lower middle, $6,000–$15,999 (51.5%); middle, $16,000–$34,999 (27.3%); and upper, $35,000 or more (11.6%). b Insurance defination are as follows: Medicaid only—if the person has a current Medicaid card or is covered by Aid to Families with dependent children, Supplemental Security Income, or public assistance and has no other insurance coverage; Medicare plus other health insurance—Medicare plus either private insurance, Medicaid, or CHAMPUS/ Veterans Administration or military health insurance. Private health insurance includes only people who reported private insurance and no other types of insurance. * Estimates for which the relative standard error exceeds 30 percent are not reported. SOURCE: Unpublished data from the National Health Interview Survey, National Center for Health Statistics, 1989. |
||||
-
by providing patients with continuing and meaningful contact with the personal health care system.
-
Second, by comparing population groups with the same disease, it is easier to control for severity and changing treatment patterns that may confound analyses of service use.
-
Third, the use of specific services that make a difference for health outcomes can be tracked. For example, diabetics should have their blood pressure and blood serum lipids monitored routinely, and they should visit an ophthalmologist to be checked for proliferative retinopathy.
The committee recommends that the federal government or a foundation support a longitudinal survey of the type described.
Modifications of the NHIS. The lead time for a new national survey can be extensive. In the interim the committee recommends that the regular series of the NHIS be modified to include access-related questions about specific diseases. Among other areas, the questions should address the types of follow-up care known to have a positive effect on prognosis.
The National Center for Health Statistics should determine whether this modification could best be done through changes in core sections of the survey (e.g., supplementary questions to the condition list) or through regularly rotating supplements that include appropriate access questions. The anticipated redesign of the NHIS core will be an opportunity to consider these options.
Utilization Indicator: Use of High-Cost Discretionary Care
For many medical and surgical procedures, there is general agreement in the medical community about the clinical criteria that guide their use. For other procedures, however, physicians may have legitimate disagreements about their appropriate utilization. These latter procedures are termed referral-sensitive because their performance depends on the judgment of the physicians who provide first-contact care and who may or may not decide to refer a patient elsewhere for more specialized treatment. Whether a procedure is indeed performed also depends on the judgment of the surgeon or specialist to whom the patient is referred. The extent to which these referral decisions are influenced, directly or indirectly, by the patient's insurance status, race, or social class may reflect a problem with equity of access.
Some referral-sensitive surgeries, like organ transplantation, can affect patient survival. Other procedures, like hip transplants or breast reconstructions, may improve physical or social functioning without necessarily extending the patient's life span. Although people do not die of osteoarthritis of the hip, the burden of pain and suffering is extremely high. Total hip replacement is not discretionary in the sense of relieving pain and suffering, but it may be treated as such by the medical care system in some cases.
For most of its work, the committee has selected indicators that are agreed to be effective and generally applicable to easily identifiable groups such as women of certain ages or children. In contrast, referral-sensitive procedures constitute a wide area of medical practice in which judgments about effectiveness or appropriateness are difficult to make without a detailed case-by-case review. Yet growing pressure to eliminate ineffective or inappropriate procedures in the name of cost and quality control is working to ensure that these judgments are, indeed, made. An access monitoring tool must be able to measure how these judgments are affecting differential use of discretionary procedures among subpopulations.
As an indicator, referral-sensitive surgeries reach beyond a person's entry into the personal health care system to assess a second level of access—expensive discretionary procedures. That this is a problem worth monitoring emerges from the medical literature, which contains examples of medical and surgical procedures for which there are differences in utilization according to patient health insurance status, race, and other sociodemographic factors.
One national study of hospital discharge abstracts revealed that uninsured patients were between 29 and 75 percent less likely than those with insurance to undergo one of five high-cost or high-discretion procedures: coronary artery bypass surgery, total knee replacement, total hip replacement, stapedectomy, and surgical correction of strabismus (Hadley et al., 1991). Similar findings were reported for the use of angiography, angioplasty, and cardiac bypass grafting among patients treated in Massachusetts hospitals. Low-income patients, the uninsured, and blacks had lower rates of use than their more wealthy, insured white counterparts for all three procedures (Wenneker et al., 1990). In Maryland it was shown that population rates for discretionary orthopedic, vascular, and laryngologic surgery increased with income. Coronary and carotid artery surgery rates were two to three times higher for whites than blacks (Gittelsohn et al., 1991).
Lung cancer treatment also has been shown to vary according to insurance status, both for those who undergo surgical treatment and those who are treated instead with radiation, chemotherapy, or both. Greenberg and colleagues (1988) showed that in both groups those with private insurance were about 50 percent more likely to receive treatment than those without insurance. They also noted that nonclinical factors, such as insurance, may be particularly important in guiding physician choice of treatment in diseases like lung cancer in which the benefit of any therapy is minimal. Surgery and radiation therapy both entail long hospital stays and considerable expense, factors that may discourage their use in patients who lack insurance (Greenberg et al., 1988).
An IOM study of Medicare's end-stage renal disease program documented access problems inherent even in a ''near-universal" entitlement program (Institute of Medicine, 1991). Those ineligible for benefits were found to be disproportionately poor and minority. Various features of the program's organization and payment policies created barriers to access for many patients. One of these barriers is particularly relevant in this discussion because it illustrates the difficulty of interpreting differences in access to referral-sensitive procedures. In a study of dialysis patients and their information-seeking behavior, black patients were at a particular disadvantage in obtaining transplantation. They felt less competent than whites to decide about the procedure, were less inclined to discuss the matter with their nephrologist, and seldom had access to a transplant surgeon. If a
fuller understanding of access barriers is to be gained, more in-depth analysis of the reasons for differential use, especially of discretionary procedures, is needed.
Measuring the Indicator
The committee chose to base its measurement of access to referral-sensitive surgeries on differences in the rates at which these procedures are performed among various subpopulations. The major focus of analysis is the differences among populations of high- and low-income neighborhoods in 11 states (see Table 3-24). The potential effects of race and insurance status on the likelihood of receiving these procedures also are considered.
The committee collaborated in this analysis with the United Hospital Fund Ambulatory Care Access Project (ACAP) and the Codman Research Group. Together, these groups selected a set of five procedures for analysis: hip/joint replacement, breast reconstruction after mastectomy, pacemaker insertion, coronary artery bypass surgery, and coronary angioplasty.
As with many access monitoring indicators, the major methodological issues in the use of referral-sensitive procedures involve the need to control for alternative explanations of differences in utilization rates by income,
TABLE 3-24 Referral-Sensitive Surgeries for Selected Conditions, by Zip Code/Income Groups, 1988, 11 States a
race, and insurance status. As noted previously, these differences may be due not to access barriers but to levels of severity of disease, or of prevalence, patients' social environment, and compliance. Moreover, in view of the discretionary nature of these procedures, patients may forgo the surgery option not because of cost but because of concerns about risks and potential discomfort. The extent to which patient preferences and risk aversion are related to their use of these procedures is not well understood.
Differences in the utilization of certain surgical procedures according to race, income, and other factors have been well documented. What is not clear is what proportion of the differences may be due to overutilization of such procedures by those in the more "favored" groups—whites and those with health insurance, for example.
Research on appropriateness of use suggests that one-quarter to one-third of all medical procedures may be of little or no benefit to patients (Brook and Lohr, 1986). Many third-party payers have instituted utilization management strategies to reduce outlays for inappropriate health care services. Still, because utilization management is in its infancy, there are many procedures for which information about appropriateness is unavailable. The challenge will be to determine whether inappropriate use explains why some groups appear to be underutilizing certain procedures relative to other groups.
Trends in the Data
Because the methodology for this utilization indicator is new, there are no year-to-year trend data. Table 3-24 presents aggregated data for 1988 from the states in the committee's sample of hospital discharge data bases. The ratios in the table represent a comparison of low-income (60 percent or more of the population with incomes below $15,000) and high-income (10 percent or less of the incomes below $15,000) zip codes. A ratio of 1.0 indicates no difference between the two income groups; ratios of less than 1.0 signify that individuals from high-income areas undergo the procedures at a higher rate than those from low-income areas.
The summary figure of 0.62 suggests that, when all the referral-sensitive procedures are combined, people from poor areas appear to be less likely to obtain these services than people from more affluent areas. The most marked differences found were for breast reconstruction (0.20), coronary artery bypass grafts (0.59), and coronary angiography (0.43). The data did not reveal major differences for hip/joint replacement and pacemaker insertion.
The relative rates of admission for referral-sensitive procedures are also comparatively low for zip code areas composed predominantly of black residents, even in those areas with higher-than-average incomes. This confirms
research demonstrating a lower rate of use of cardiac procedures among blacks with private insurance or Medicare compared with whites who are similarly insured (Wenneker and Epstein, 1989). White Medicare recipients are three times more likely than black Medicare recipients to receive coronary artery bypass graft surgery and angioplasty. White Medicare recipients are also more likely than blacks to have magnetic resonance imaging (MRI) scans rather than the less costly computed tomography (CT) scans (Boutwell and Mitchell, 1991).
Recommendations
Standards for Appropriate Use. Increasing attention is being paid to outcomes research and the development of clinical practice guidelines. As techniques become established for determining the appropriateness of use of certain medical procedures, interpreting differences in use among subpopulations will become easier. For example, these techniques will allow us to distinguish problems in access from overutilization of services by specific populations.
Improved Data Availability. Researchers who are seeking improvements in clinical data bases for use in outcomes research should work with those interested in access research to determine whether there are mutually beneficial opportunities for enhancing these data bases. An issue of interest to both groups, for instance, might be the addition of information to the discharge abstract, which would help to measure severity more accurately.
Outcome Indicator: Avoidable Hospitalization for Chronic Diseases
For the purposes of this indicator, "avoidable hospitalizations" are those that might not have occurred had the patient received effective, timely, and continuous outpatient (ambulatory) medical care for certain chronic disease conditions. Although hospital admission rates are generally a utilization measure, they are used here as a proxy for health conditions that have deteriorated to the point where hospitalization is required.
Ongoing medical management can effectively control the severity and progression of a number of chronic diseases, even if the diseases themselves cannot be prevented. An advanced stage of a chronic disease that requires hospitalization may indicate the existence of one or more barriers to access to the personal health care system. Thus, hospital admissions for certain conditions are a potentially useful indicator of the performance of the ambulatory health care system. High rates of admissions for conditions related to treatable chronic diseases in particular may provide indirect evidence of serious patient access problems or deficiencies in outpatient management.
Measuring the Indicator
In the indicator for use of discretionary procedures (discussed above), the committee used hospital discharge data to identify income differences in the utilization of referral-sensitive procedures. The same technique can be used to create an outcome indicator for utilization of ambulatory care. In this case, hospital admission represents a failure in outpatient management rather than use of a service. By comparing different income groups by zip code, one can roughly compare the relative frequency of outpatient management failures by income status.
The committee has identified a specific set of diagnoses representing conditions that, with timely and effective outpatient care, normally would not result in a hospital admission. No matter how timely or effective outpatient medical management may be, a certain amount of hospitalization among patients with chronic diseases is expected. If differences in disease prevalence are taken into account, however, there should be no major differences in hospital admission rates according to income level, insurance status, or race.
Accurate diagnostic data may be obtained by using the disease coding system of the ninth edition of the International Classification of Diseases (ICD-9; U.S. Department of Health and Human Services, 1991), which provides detailed diagnosis information. The aim is to identify diagnoses that are clearly related to the need to treat a patient in the hospital. Furthermore, ICD-9 codes allow fairly precise selection of conditions that are likely to be related to the adequacy of outpatient management.
The source of diagnostic data is the hospital discharge summary. These summaries, at a minimum, provide up to five diagnostic codes (for patients with multiple diagnoses); three procedure codes; and the patient's age, sex, and race. Currently, about two dozen states have centralized hospital discharge data bases, which allows comparisons to be made among all hospitals in a state. Eleven were selected for the committee's analysis.2
Discharge summaries also report a patient's zip code and the expected source of payment. Zip code information permits the matching of diagnosis and procedure with the demographics of the patient's neighborhood, allowing a rough estimate of personal income. Thus, the measure of the avoidable hospitalization indicator is a population-based rate using zip codes grouped by income to approximate differences in the variables of interest (income, insurance, and race). To account for differences among population groupings, the data are adjusted for age and sex. The committee focused initially on admissions for those under age 65, because most of the elderly have Medicare coverage.
As noted in the discussion of the previous indicator, the committee collaborated with the Ambulatory Care Access Project of the United Hospital Fund of New York in selecting a set of chronic-disease-related diagnoses that are potentially sensitive to outpatient care across a range of clinical areas and patient-age cohorts. Appendix D contains a list of those conditions. The Codman Research Group provided hospital discharge data in a form that was suitable for analysis.
Information about household income generally is not collected when a patient enters the hospital. Income can be estimated by matching patient zip codes, which are recorded on hospital discharge summaries, with zip-code-area income-level information available from the Census Bureau. The problem with this indirect approach of measuring patient income is that it is imprecise. Small pockets of the poor in otherwise high-income areas, as well as dispersal of the poor across a wide region, can be particularly problematic.
Although information about health insurance status is included on the standard hospital discharge form, there are no good data on insurance status by geographic area. Without such "denominator" data, it is difficult to know whether hospital admission rates for ambulatory-sensitive conditions are higher than expected, given the levels of insurance in an area. Recent work by Wenneker and colleagues (1990), however, seems to indicate that comparisons by insurance coverage status provide results similar to those of the income analysis, which is probably due to correlation of the two barriers.
Finally, few data are available that shed any light on the relative importance of a variety of factors that appear to contribute to delayed or inadequate outpatient care. One such factor, the criteria used by physicians to admit patients to the hospital, has been examined by the ACAP. It might be expected that many physicians would have a lower threshold for admitting low-income patients than for high-income patients. This might be the case either because of differences in the level of clinical training for physicians in poorer areas or because of physician concerns about lack of access by poor patients to regular outpatient services, their weak family support systems, or their sometimes less-than-optimal compliance with recommended outpatient treatment. However, the ACAP data for New York City indicate that differences in patient severity are unlikely to account for the differences in admission rates seen between low-income and high-income areas (Billings et al., 1991).
Trends in the Data
Table 3-25 lists the discharge diagnoses for the chronic conditions chosen for the analysis, the admission rates (per 1,000 population) for low- and high-income zip codes, and a comparison of those rates in the form of a
TABLE 3-25 Admission Rates for Selected Ambulatory-Care-Sensitive Conditions, by Zip Code/Income Groups, 1988, 11 States a
ratio. All of the ambulatory-care-sensitive admission rates were substantially higher for low-income areas. The greatest differences—ranging in size from six– to sevenfold—were related to admissions for congestive heart failure, hypertension, and asthma. However, even angina, the diagnosis with the lowest ratio (and thus the least difference between rates), showed income differences of almost threefold. The overall average rate of difference was 4.65.
Billings and his colleagues (1991), examining New York City discharge data, looked at the effects of race, substance abuse, and prevalence of disease conditions on the differences between high– and low-income areas. They found that predominantly black middle-income zip codes resembled other middle-class areas but that poor black areas had consistently higher admission rates than comparable white low-income zip codes. By examining secondary diagnoses of alcohol and drug dependence/abuse, they noted that, although alcohol/substance abuse explains some of the differentials for the 22– to 44–year-old population with respect to bacterial pneumonia and tuberculosis, for the most part such abuse has little impact on rates for most
of the conditions chosen for this analysis. Finally, in terms of differences in disease prevalence, the research group looked at asthma and diabetes—two conditions for which data on prevalence are available through the NHIS. Depending on the age group, differences in prevalence between high– and low-income populations ranged from 1.35 to 2.36 times higher for low-income age cohorts with asthma and from 1.15 to 2.96 times higher for low-income cohorts with diabetes. Prevalence thus explains only a portion of the four– to fivefold differences between income groupings for these two conditions.
Recommendations
Hospital Discharge Data Systems. States that do not have centralized hospital discharge data bases should develop them. In addition to their value for the types of analyses suggested by this committee, the data bases will be useful for future research on costs and quality of care.
Expanding Data Elements in the Discharge Abstract. As recommended previously, states should consider the feasibility of adding additional elements to the discharge abstract, especially information to measure the severity of illness and income.
Further Research. The committee believes that more detailed studies of patients and admitting physicians are needed to sort out the relative contribution of the various factors, including access to primary care, that lead to hospitalization for chronic disease-related conditions. Items of particular interest include the timeliness and quality of outpatient care, patient characteristics, and physician admitting practices. Studies focusing on better measurement of continuity of care and the effect of site of care (walk-in clinics, physician's offices, hospital clinics, community health centers, emergency departments) also should be considered.
Outcome Indicator: Access-Related Excess Mortality
The access-related excess mortality rate is the number of deaths per 100,000 population that are thought to be the result of access problems. The estimate is based on a comparison of two groups in the population—one that is believed to have relatively good access and one that is considered likely to experience barriers to access. Because data are available (Stoto, 1992), the population groups of particular focus for this measure are blacks and whites.
It has been well documented that, compared with whites, blacks in the United States have a disproportionately high mortality rate from chronic disease. Some of the difference may be the result of increased levels of
behavioral risk factors among blacks, such as higher rates of smoking (U.S. Public Health Service, 1991). Physiological factors, such as a genetic predisposition to high blood pressure, may also play a role. Problems known to have an effect on access to health care, such as lack of insurance, poverty, and low educational attainment, may be important as well.
If the effects on black mortality of physiological and behavioral risk factors can be statistically "removed," the remaining difference in the death rate between blacks and whites (for diseases that can be managed with medical care) may be attributable, in large part, to differences in access to health care. The statistical calculations necessary to control for the effects of these factors require a number of assumptions that can be questioned. The methodological challenges that must be overcome to enhance the utility of this indicator are discussed below and in the recommendations section. In addition to questions of methodology, some conceptual issues also need to be resolved. Foremost among these is the dilemma of how to handle chronic disease behavioral risk factors—for example, hypertension—that could be ameliorated by treatment or care and whose presence may indicate barriers to access to health care services. Yet despite such conceptual and technical issues, the committee believes that the approach presented here, albeit on a developmental basis, will be an improvement over the unadjusted comparisons of death rates that are frequently cited.
Measuring the Indicator
A critical component in calculating an access-related mortality rate is the adjustment for risk factors. If access were the only factor that distinguished black and white mortality, there would be no need to adjust for risk factors. For example, one would not compare the mortality rates at two hospitals without first adjusting for the relative risks of death for each patient, including age, severity of illness, and procedures undergone. Similarly, one cannot compare how the personal health care system (the hospital in the above analogy) performs for blacks compared with whites (one hospital's patients compared with another's) without first taking into account the differences (in terms of behavior, physiology, and environmental surroundings) between blacks and whites.
Fortunately, the results of epidemiological follow-up studies of health examination surveys performed in the 1970s provide a basis for measuring how six major risk factors interact and affect mortality for the two races. Applying these results to the black mortality rate reveals the level of mortality that blacks would experience if the pattern of their risk factors was the same as that for whites.
In sum, access-related excess mortality is calculated by subtracting two rates. The rate is the actual rate of death in the group with higher mortality
(in this case blacks). The second lower rate is an estimate of what the black death rate would be if blacks had the same pattern of risk factors as whites. This estimate is based on applying "rate ratios" derived from an epidemiological study that compared risk factors among blacks and whites (Otten et al., 1990). The difference between the first and second rates represents the excess mortality of blacks that is related to lack of access to health care services.
Trends in the Data
The 1980 mortality rate from all causes for white males age 35 to 54 was 479.4 per 100,000 population; for same–age white females the rate was 250.3 per 100,000 (National Center for Health Statistics, 1980b). For black males between the ages of 35 and 54, death from all causes stood at 1,048 per 100,000 in 1980; for same–age black females the rate was 527.4 per 100,000. Based on these data, black men and women between the ages of 35 and 54 were 2.2 and 2.1 times more likely, respectively, than their white counterparts to have died in 1980.
By 1988 mortality rates for white males and females age 35 to 54 each had fallen 20 percent, to 381.6 per 100,000 for men and 200.7 per 100,000 for women. The corresponding death rate for black men was 948.4 per 100,000 (a 9.5 percent reduction compared with 1980); for black women the rate was 439.8 per 100,000 (a 16 percent reduction from the 1980 level).
Data on risk factors from the National Health and Nutrition Examination Survey I Epidemiologic Follow-up Study (NHEFS) have been used to calculate the mortality risk ratios of blacks and whites (Otten et al., 1990). The risk ratios were adjusted to remove the influence of six well-established risk factors: smoking, systolic blood pressure, cholesterol level, body-mass index, alcohol intake, and diabetes. In 1980, for men age 35 to 54, the adjusted black-white risk ratio was 1.6; for women of the same age the ratio was 2.3.
Performing the calculations outlined in the measurement section above yields a crude potentially access-related excess mortality rate for blacks (Figure 3-3). In 1980, for men age 35 to 54, the rate was 393 per 100,000. In other words, nearly 39 percent of all deaths among middle-aged black men that year may be attributable to problems in gaining access to the personal health care system. In 1980, for black women age 35 to 54, the access-related death rate was 298.1 per 100,000, accounting for 56 percent of all deaths in this group. These figures must be considered a crude rate at present. As suggested in the recommendations that follow, further research is needed to account for patient characteristics that are not measured by known risk factors.
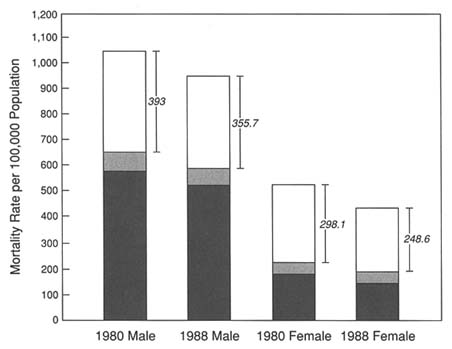
FIGURE 3-3 Estimated excess mortality for blacks, ages 35–54, by sex. 1980 and 1988. The areas indicated are the estimated mortality for blacks if age-specific mortality rates were equal to those of whites &220E; the estimated excess black mortality due to differences in controllable risk factors &1274F; and estimated excess black mortality due to differences in access to personal health care &1274F; SOURCE: Calculated as described in the text above, under ''Measuring the Indicator."
In 1988 it appears that the number of deaths among blacks attributable to access-related problems decreased for both men and women. For black men age 35 to 54, the rate was 355.7 per 100,000; for black women the rate was 248.6 per 100,000. These reductions reflect the overall decline in death rates for blacks and whites and are a continuation of the trend of previous decades. Although they have not been calculated, it is unlikely that the black-white risk ratios for 1988 differ substantially from those determined by Otten for the 1970s when the subjects were surveyed.
Because the calculation of relative risks relies on data from health examination surveys conducted in the 1970s, the drop in excess rates is due solely to changes in black mortality, not changes in risk factor adjustments. It would be desirable, therefore, to have more up-to-date data on risk factors.
Recommendations
Much of the interest in excess mortality has focused on clarifying the role of behavioral and environmental risk factors in producing it, with an eye to designing prevention strategies. More recently, researchers have begun to concentrate on what heretofore had been considered an unexplained residual statistic that now appears to be related to access to and quality of care. The committee believes that this residual deserves further investigation as a potential access measure that can be used in tandem with a better understanding of behavioral and physiological risk factors.
Determining access-related excess mortality raises a number of measurement issues that also deserve further investigation. As mentioned, the rate ratios that are used to adjust for the effect of a set of risk factors for the 1970s were used to calculate access-related excess mortality in 1988. Without new risk data, however, only part of the story can be revealed. Although they might be similar, the actual adjustment for 1988 would not be exactly the same as the adjustment for 1980. It is important to note that most of these risk factors are slow to change. Therefore, changes in risk factors probably have had only a modest effect on changes in death rates during this short period. Moreover, knowing about a change in one risk factor (lower smoking rates, for example) is not sufficient because it is the interaction of the six factors that drives the models.
The measurement of access-related excess mortality is also complicated by the fact that some of the risk factors used in the calculation can be thought of as early stages of disease. For instance, hypertension is an important risk factor for both heart disease and stroke, and it is a disease in itself. "Removing" its effect in an excess mortality calculation removes as well the possible impact that access to medical care earlier in life could have had in preventing hypertension.
Any approach such as this, in which the final result is based on a residual, assumes that appropriate statistical models and data exist to correctly and completely remove the effects of the non-access-related determinants of mortality. It further assumes that all variability in mortality rates that is not attributable to measurable, non-access-related factors is related to access—that is, that there is no "noise" in the data that is not related to risk factors or access. This conclusion cannot be drawn with any certainty.
The current approach does not specifically identify the impact of chronic disease on access-related excess mortality. A rough approximation of this impact, however, can be obtained by studying an age cohort in which the incidence of chronic disease is likely to be quite high (persons age 35 to 54). In addition, the approach does not distinguish those diseases for which access is an important predictor of death from those for which it is not. The impact of the use of health care services is likely to be much greater for
diseases and conditions that are amenable to medical intervention than for those on which such services appear to have little influence (Poikolainen and Eskola, 1986).
The model used by the committee to adjust overall mortality rates to take into account risk factors for disease is an important first step in improving such calculations because it points to clear shortcomings in the available data. The committee believes that research on access-related excess mortality must begin to focus on specific diseases, particularly those amenable to access-related prevention services or amelioration. The present analysis would have been enhanced by the availability of data from a somewhat older age cohort in which chronic diseases were a higher fraction of all deaths. Even better would be data from patient cohorts with specific diseases. It would also be desirable to develop models that compare groups on the basis of factors other than race—for example, income and insurance status.
The National Mortality Followback Survey could be used to explore specific common causes of death related to problems of access. For example, a recent study used data from this survey to analyze differences in the age at death for uninsured and privately insured people between the ages of 25 and 64 who died of acute myocardial infarction (Hadley et al., 1992). This study found that the uninsured were about two years younger at the time of death and that they had significantly less access to care in the year before death (fewer physician visits, greater trouble securing a physician, fewer hospitalizations and hospital days). The investigators controlled for (i.e., "removed") the effects of differences in sex, race, marital status, income, and several risk factors associated with heart attacks. This research also revealed that for most causes of death there were too few cases under the age of 65 included in the followback survey to permit meaningful multivariate analysis. The value of the survey could be enhanced by limiting the number of causes of death surveyed and increasing the numbers of deaths sampled for each of those causes, or by increasing the size of the survey.
The CDC has experimented with a mortality followback pilot study in collaboration with six state diabetes control programs. Among other findings, the study revealed that high blood pressure was not being controlled in a substantial part of the population and that the rate of blood glucose monitoring was relatively low (Bild et al., 1988).
Whatever adjustment model is used, calculations of the risk ratios of blacks compared with whites and those of other ethnic groups (as well as income groups) must be conducted on a more timely basis. Unfortunately, the large-scale epidemiological studies needed to determine trends in excess mortality are too expensive and complex to be replicated every year. It may be possible to derive similar information using mortality rates and risk factor data available through the vital statistics system and regular surveys,
such as the NHIS and the BRFSS. If reliable statistical risk models can be developed, using variables from these two sources but based on data sets like the NHEFS, current mortality rates and current risk factor data can be combined into annual estimates of excess mortality.
OBJECTIVE 5: REDUCING MORBIDITY AND PAIN THROUGH TIMELY AND APPROPRIATE TREATMENT
Utilization Indicator: Percentage of Healthy Individuals Who Do Not Contact a Physician During an Acute Episode of Illness
People who perceive themselves to be in good to excellent health occasionally have an acute illness or a flare-up of a chronic condition that causes them to temporarily limit their normal activities. This could mean staying home from work or school, being restricted to bed, or reducing one's normal activities for more than half a day. During these episodes, a person may believe that his or her symptoms warrant medical attention. Differences among subpopulations in the frequency with which they contact a physician during such episodes could reflect differences in access. Physician contacts refer to consultation either in person or by telephone with a physician or someone (e.g., nurse, physician's assistant) who is supervised by a physician. Data on physician contacts, perceived health status, and restricted activity days are available from the NHIS.
Roughly 800 million physician contacts are made each year by people believing themselves to be in good or excellent health. In addition to requiring treatment for acute care conditions and low-impact chronic conditions, many of these people have undetected chronic diseases that might be aided by prompt medical attention. For example, a 1987 NCHS study estimated that nearly 50 percent of diabetes cases in the United States from 1976 through 1980 went undiagnosed. This indicator contrasts with that for continuing care for chronic disease in that those individuals, perceiving themselves to be in poor health, are more likely to know that they require continuous medical monitoring and care.
Someone who feels ill enough to restrict his or her activities may not necessarily need to seek assistance from a health care provider. For example, many colds and cases of back pain are self-limiting, and the individual can resume normal activities after rest. Thus, choosing not to visit a physician for these conditions may be appropriate utilization. The point of the indicator, however, is that over a broad range of many people and providers, average utilization should not differ among groups by, for example, insurance status. Individual variation in under- and overutilization should be canceled out. In other words, differences among population groups can reflect the presence of access barriers or overuse by groups with high-incomes
or adequate insurance coverage. Because the measurement techniques for this indicator are not well developed, it is not possible to distinguish who may be overusing ambulatory care services. Nonetheless, it is important to monitor systematic differential rates of use by those potentially facing barriers to entering the personal health care system. The results of monitoring utilization must be interpreted in light of related outcome indicators (to follow) and investigated by research studies that explore the issues in greater depth.
Measuring the Indicator
The primary medical concern of the 90 percent of the population who see themselves as being in good health is whether they will be able to see a doctor when needed. This indicator attempts to measure this concern by singling out healthy people who suddenly become so sick that they must reduce their normal activities. The question is whether such characteristics as insurance status, income, and race have an effect on whether they obtain medical attention.
The committee used the NHIS to identify individuals who reported themselves to be in good to excellent health and who had had at least one day of restricted activity in the two weeks prior to being interviewed. Comparisons were then made among those who had potential access barriers.
Trends in the Data
Table 3-26 displays the proportion of healthy individuals who had no physician contacts during a period in which they reduced their activities because of health problems. The majority of people, regardless of whether they had insurance, did not contact a physician by phone or in person. However, people without insurance or Medicare recipients without supplementary policies were less likely than those with private insurance to seek medical care or advice. The differences range from 5 to 10 percentage points. The likelihood of contacting a physician decreases by about 5 percentage points at the lowest income levels both for the uninsured and privately insured, although the differences are not statistically significant. Future monitoring should be alert to signs of whether anticipated out-of-pocket costs are deterring some of the insured from obtaining services.
The committee's data analysis revealed only slight differences between blacks and whites on this indicator (Table 3-26). Uninsured blacks, for example, were about three percentage points more likely not to contact a physician than uninsured whites. The difference between Hispanics and non-Hispanics was also about three percentage points. A 1986 telephone survey documented similar small differences between whites and blacks in
TABLE 3-26 Percentage of Individuals in Good to Excellent Health Who Had No Physician Contact During Period of Restricted Activity
terms of their use of ambulatory care. A higher proportion of blacks (39.3 percent) than whites (33.4 percent) who rated themselves in good to excellent health had gone without an ambulatory care visit during the previous year. However, this survey illustrates the importance of probing further. Blacks' perceptions of the quality of ambulatory care differed significantly from those of whites. For example, 23.3 percent of blacks compared with 9 percent of whites, felt that their physician did not inquire sufficiently about pain; 44.2 percent of blacks, compared with 27.5 percent of whites, felt that their doctors did not adequately explain the seriousness of their illness or injury (Blendon et al., 1989).
Whether generally healthy people are able to see a physician during an acute episode of illness may be related to some extent to their relationship to the personal health care system for routine care. Analysis of the 1986 Robert Wood Johnson Foundation access survey revealed that not having a regular source of care was a risk factor for not receiving recommended medical care. This includes not only cancer screening (as noted in the discussion of a previous indicator) but also whether a person is likely to see a physician for serious medical symptoms such as chest pain during exercise, abnormal bleeding, or loss of consciousness. Survey items that investigate whether people have a "regular source of care" have been relied upon as a global indicator of "access to continuity of care"; however, methodological studies caution against overinterpreting these results because access barriers are only one reason why people may not have a regular source. For example, many people who have insurance and an adequate income nevertheless choose not to have a regular health care provider (Hayward et al., 1991b).
Data from the Hispanic Health and Nutrition Examination Survey (conducted from 1982 through 1984) on the use of health services among Hispanics shows that the frequency of physician visits differed markedly among the three major Hispanic groups living in the United States. Of those who were uninsured, Mexican Americans were three times more likely than Cuban Americans and nearly four times more likely than Puerto Ricans never to have had a routine physical examination (29.5 percent, 9.9 percent, and 7.7 percent, respectively). With the exception of those who had non-Medicare, non-Medicaid public insurance, Mexican Americans were also the least likely among all insured Hispanics to have ever had a physical examination (Trevino et al., 1991).
The 1988 NHIS Child Health Supplement found that a greater proportion of high-income children (92.4 percent for household incomes over $40,000) compared with low-income children (83.8 percent for incomes less than $10,000) had a source of routine medical care. This relationship was equally true when insurance status was taken into account. Insured children were much more likely than uninsured children to have a regular source of care (91.9 percent compared with 79 percent; Bloom, 1988).
Data from the 1982 preventive care supplement to the NHIS revealed a similar correlation among income, insurance status, and the use of routine health services by children age 5 through 16. Children in families with incomes below the poverty line were more likely than their wealthier counterparts to be either nonusers of routine physical, dental, and eye examinations or to be less frequent users of those services. Children with Medicaid were more likely than those without Medicaid or other third-party insurance to use one of the three services. This relationship was particularly strong for physical examinations: 82.7 percent of children with Medicaid, compared with 62.2 percent of those without it, had had such an exam (Newacheck and Halfon, 1988).
Recommendation
National Health Interview Survey Enhancements. In conjunction with efforts to improve monitoring of continuing care for chronic diseases, the NCHS should explore methods to better understand the timely and appropriate use of physician services during episodes of acute illness. Of particular interest are acute illnesses and early stages of chronic illness that have the potential for serious consequences if left untreated.
Utilization Indicator: Dental Services
Annual dental visits include all visits made to a dentist, or to a technician or hygienist under a dentist's supervision, for regular, specialized, or
emergency dental care. Services such as mass screening at schools or other institutions are excluded.
People visit the dentist for many reasons: to have a regular oral examination and checkup, to receive preventive services (such as sealants and fluoride treatment), to obtain emergency treatment for pain, to receive fillings for decayed teeth, to have teeth extracted, or to receive fixed or removable appliances for missing teeth. Dental care can help resolve disease problems and improve functioning, such as the ability to eat and speak; it can also improve appearance. To the extent that dental care can prevent the loss of permanent teeth and help individuals maintain a healthy cosmetic dentition, it plays an important social role in communication and job performance.
There are other important reasons for tracking access to dental services. Since only about a third of Americans are covered by dental insurance, the use of dental services is quite sensitive to income. That is, those in higher-income brackets are more likely to visit a dentist than those less financially well off, regardless of broader health insurance coverage. This relationship has important implications for understanding access more broadly across the health care system.
Part of the committee's mandate was to consider access problems across a wide range of clinical areas. Dentistry constitutes a health service that nearly everyone needs but that is frequently overlooked as a segment of the personal health care system. In the future, in addition to dentistry, access monitoring activities should also focus on barriers to other types of health care, including that provided by nurses and allied health professionals.
Measuring the Indicator
Access to dental services is measured most commonly by the average number of dental visits per person per year. Data on dental visits come from supplements to the NHIS; the most recent NHIS data on dental services are from 1989. Yet the method falls short in two respects: it fails to distinguish differences in the content of visits, and it does not indicate the type, if any, of patient insurance. The poor and many of the uninsured often forgo routine preventive and restorative dental care. Thus, when dental problems become severe, they are more likely to require extractions instead of other more preferable, but expensive, procedures. A monitoring method must be able to disaggregate the content of dental visits to determine when the kind of dental care received is related to problems with access. To sort out the effects of financial barriers, it would be desirable to have more refined information about insurance coverage for dental services. Most surveys identify only those with private insurance, aggregating those with publicly funded insurance, such as Medicaid, and those with no insurance at all.
Trends in the Data
Table 3-27 displays the number of dental visits and percentage of the population that never visited a dentist according to selected patient characteristics. Between 1983 and 1989 the average number of dental visits per person in the United States increased 14 percent, from 1.8 to 2.1. During the same period, the proportion of those who had never visited a dentist fell
TABLE 3-27 Dental Visits, by Selected Patient Characteristics, a 1964, 1983, and 1989
|
|
Dental Visits |
|
Never Visited Dentist |
|||
|
Characteristics |
1964 |
1983 |
1989 |
1964 |
1983 |
1989 |
|
Total |
1.6 |
1.8 |
2.1 |
15.5 |
7.7 |
6.4 |
|
Age (years) |
|
|
|
|
|
|
|
2–14 |
1.3 |
2.0 |
2.1 |
46.6 |
23.5 |
19.7 |
|
15–44 |
1.9 |
1.9 |
2.4 |
4.0 |
1.7 |
1.4 |
|
45–64 |
1.7 |
2.0 |
2.4 |
1.3 |
0.6 |
0.4 |
|
65 and over |
0.8 |
1.5 |
2.0 |
1.5 |
0.9 |
0.5 |
|
Sex |
|
|
|
|
|
|
|
Male |
1.4 |
1.7 |
2.0 |
16.1 |
7.9 |
6.7 |
|
Female |
1.7 |
2.1 |
2.3 |
15.0 |
7.8 |
6.1 |
|
Race |
|
|
|
|
|
|
|
White |
1.7 |
2.0 |
2.3 |
13.8 |
7.2 |
6.1 |
|
Black b |
0.8 |
1.2 |
1.2 |
28.0 |
10.3 |
7.7 |
|
Family income c |
|
|
|
|
|
|
|
Less than $14,000 |
0.9 |
1.2 |
1.3 |
27.4 |
11.2 |
9.5 |
|
$14,000-$24,999 |
0.9 |
1.5 |
1.5 |
22.0 |
9.8 |
7.8 |
|
$25,000-$34,999 |
1.4 |
2.2 |
2.2 |
15.8 |
7.2 |
6.3 |
|
$35,000-$49,999 |
1.9 |
2.5 |
2.7 |
10.9 |
4.5 |
4.5 |
|
$50,000 or more |
2.7 |
2.9 |
3.1 |
7.2 |
3.6 |
3.4 |
|
Location of residence |
|
|
|
|
|
|
|
Within MSA |
1.8 |
2.1 |
2.2 |
14.4 |
7.2 |
6.2 |
|
Outside MSA |
1.2 |
1.6 |
1.7 |
17.9 |
8.6 |
5.8 |
|
MSA, metropolitan statistical area. a Gender, race, family income, and location of residence are age adjusted. b Category of “black” in 1964 includes all nonwhites races. c Family income categories are for 1989. Comparable income categories for 1964 are as follows: less than $2,000; $2,000–$3,999; $4,000–$8,999; and $10,000 or more. For 1983 the categories are less than $10,000; $10,000–$18,999; $19,000–$29,999; $30,000–$39,999; and $40,000 and more. SOURCE: Unpublished data from the National Health Interview Surveys, National Center for Health Statistics, 1964, 1983, 1989. |
||||||
from 7.7 percent to 6.4 percent. However, the black-white disparity in the use of dental services grew, as blacks remained at 1.2 visits per year and white usage increased to 2.3. Those over age 65 have markedly changed their use of dental services, increasing the average number of visits per year from 1.5 in 1983 to 2.0 in 1989. This continues a long-term trend that is related in part to greater numbers of the elderly retaining their teeth longer as they age.
Some indication of the benefit of increased dental visits and greater use of fluoride is apparent in the changing tooth decay experience of U.S. school-children. Compared with the early 1970s, most children in the late 1980s experienced much less tooth decay and thus received fewer fillings and had fewer missing teeth. However, a significant minority of children still experience substantial tooth decay that will compromise their adult dentition if they do not gain access to primary dental care (Office of Technology Assessment, 1990).
Hispanic American adults seem to be at high risk for dental diseases. This group had twice the mean number of untreated decayed teeth of Hispanic children, indicating that lack of access to dental care extends into adult life. The result is that dentate Cuban American and Puerto Rican adults are missing about twice as many teeth as are white, non-Hispanic adults.
The prevalence of gingivitis is also higher among Hispanic Americans than among white non-Hispanics, as estimated during the 1985–1986 survey of employed American adults conducted by the National Institute of Dental Research. Hence, the higher incidence of dental diseases and the presence of high levels of untreated oral conditions suggest that Hispanic American adults experience problems in gaining access to dental care that can compromise the quality of their adult lives (Ismail and Szpunar, 1990).
Household income was directly related to the use of dental services (see Table 3-27). In 1989 people with incomes of more than $50,000 had an average of 3.1 dental visits per year, more than twice the average for those with incomes under $14,000. There was also a small but consistent difference in the number of annual visits made by those living in cities compared with those living outside a metropolitan area, suggesting that people in more rural communities may experience an access barrier.
Not having dental insurance appears to be an important access barrier to dental care. According to the 1986 NHIS, 37.8 percent of those interviewed had dental insurance. Whether one has dental coverage appears to depend on a number of sociodemographic characteristics, including age, race, income, education, and overall health status. For example, people age 25–54 were more likely than those older or younger to have coverage. White were more likely than blacks to have dental insurance (39.3 versus 28.4 percent, respectively), and men were slightly more likely than women
to be insured (38.6 percent of men had coverage). Only 10 percent of those with incomes under $10,000 had dental insurance, compared with 56.6 percent of those with incomes above $35,000. People with more than a high school education were almost three times as likely as those with less than nine years of education to have dental insurance (44.6 versus 15.3 percent, respectively). Those in good to excellent health were nearly twice as likely as those in fair or poor health to have dental insurance (41.5 versus 23.4 percent, respectively).
In 1989 those with dental insurance made an average of about one more visit annually to the dentist than those without insurance (2.7 visits compared with 1.7 visits; Table 3-28). This same insurance-related differential was apparent for both blacks and whites. Regardless of insurance status, whites (2.8 visits by insured, 1.8 visits by uninsured) made more visits than blacks (1.7 visits by insured, 0.9 visits by uninsured). A factor of concern is that the use of dental services among blacks appeared to decline between 1986 and 1989. At each income level, those with insurance made more visits than those without insurance. It is not clear why those with insurance and incomes under $10,000 had such a high number of visits; it may relate to the fact that only a small percentage (10 percent) of this group has insurance.
The committee's analysis of hospital discharge data from 11 states revealed that residents in low-income zip codes are almost three times (2.86) as likely to be admitted to hospitals for dental conditions as those from high-income zip codes. Hospital admission for the specific set of ICD-9
TABLE 3-28 Annual Dental Visits, by Dental Insurance Status and Selected Characteristics, 1986 and 1989
|
|
Private Insurance |
Uncovered |
||
|
Characteristic |
1986 |
1989 |
1986 |
1989 |
|
Total |
2.6 |
2.7 |
1.7 |
1.7 |
|
Race |
|
|
|
|
|
Black |
2.0 |
1.7 |
1.1 |
0.9 |
|
White |
2.7 |
2.8 |
1.8 |
1.8 |
|
Family income |
|
|
|
|
|
Less than $10,000 |
2.9 |
2.1 |
1.2 |
1.2 |
|
$10,000-$19,999 |
1.9 |
2.1 |
1.5 |
1.3 |
|
$20,000-$34,999 |
2.6 |
2.3 |
2.1 |
1.8 |
|
$35,000 or more |
2.9 |
3.1 |
2.4 |
2.5 |
|
SOURCE: Unpublished data from the National Health Interview Surveys, National Center for Health Statistics, 1986 and 1989. |
||||
codes selected by the committee is indicative of advanced dental disease that may be caused by lack of adequate ambulatory dental care. Because admission rates for dental problems are fairly low (less than 0.1 per 1,000 population for the 11 states studied), by itself the measure has limited utility as an outcome indicator.
Two recent studies have shown that Medicaid coverage of dental services appears to impose its own set of access problems on low-income patients. In a review of the Medicaid policies of seven states, the Office of Technology Assessment (1990) found significant differences in the dental services offered. To varying degrees, each state program failed to adequately cover a number of basic dental services. Several specific barriers to dental services were identified, including low Medicaid reimbursement rates, which resulted in inadequate treatment for patients or discouraged dentists from participating in the program; insufficient subsidization of patient transportation costs to the dentist's office; and Medicaid recipients' own lack of awareness of their dental benefits, failure to use their benefits even when aware of them, and negative perceptions about dentistry.
A study of California's Medi-Cal program (Damiano et al., 1990) found a similar set of problems. Medi-Cal reimbursement rates for dental services are significantly lower than the fees charged by private practitioners, which discourages many dentists from treating those covered by the program. Only about 15 percent of all general practice and pediatric dentists in the state accept new Medi-Cal patients; by geographic area, 28 of California's 58 counties had no dentists willing to accept Medi-Cal patients. Overall, the 1,800 dentists in Medi-Cal's dental referral program were responsible for meeting the needs of about 3 million eligible patients across the state.
Recommendations
NHIS Dental Supplements. Questions in future NHIS dental supplements should gather information not only about private insurance coverage but also about publicly funded coverage, such as that provided by Medicaid, Medicare (for oral surgery), the Department of Veterans Affairs, and the military (for dependents). The specific content of care received by patients, including preventive and routine checkups, restorative treatment, extractions, and full or partial dentures, should be captured by the survey. NHIS questions should also probe in greater detail the factors, including cost, that prevent patients from visiting the dentist.
Research Studies. The committee recommends that research be conducted to determine trends in the effect of private insurance on access to various types of dental services.
Outcome Indicator: Avoidable Hospitalization for Acute Conditions
For the purposes of this indicator, hospitalizations are hospital admissions for conditions related to an acute episode of disease. Avoidable hospitalizations are those that probably would not have occurred had the patient received appropriate and timely outpatient (ambulatory) medical care.
People who are in good to excellent health—the population of interest in this objective—may seek medical attention for any number of reasons. (See the discussion for the indicator ''Routine Physician Contacts" above.) The personal health care system in some cases provides only symptomatic relief to patients for conditions that would resolve independent of any medical intervention. In other situations, however, symptoms that are not addressed in a timely fashion can evolve into acute medical problems requiring hospitalization.
For example, a child with pain and fever may be treated by a parent with an over-the-counter cold medication. If the child is from a family with no regular source of medical care and if the symptoms become severe enough, a visit to the emergency room may become necessary. An emergency room physician, unaware that there has been a history of these infections, may release the child to his or her parents. At home the child may get progressively worse and eventually develop severe otitis media requiring hospitalization.
There are many other examples of potential problems faced by people without a regular source of medical care. Someone who experiences frequent urination, a burning sensation, or intermittent pain upon urination, indicating a relatively simple-to-treat urinary tract infection, may, if untreated, be at risk for developing a severe kidney infection. A persistent cough can signal any number of conditions, including tuberculosis or pneumonia. Untreated diarrhea can evolve into severe gastroenteritis.
For the significant segment of the population with no or inadequate health insurance, or who for other reasons have no regular source of medical care, hospital emergency rooms are increasingly being used as walk-in clinics for all manner of health complaints. Although few would maintain that the hospital emergency department is an optimum site for primary care, in the absence of a well-organized system of ambulatory care for those unable to afford private medical care, it is one of the only options. Unfortunately, especially in inner-city hospitals, inpatient bed space is limited. Many emergency rooms overflow not only with patients waiting to be seen by a doctor but also with patients who are already evaluated and are waiting to be assigned a hospital bed. Some evidence suggests that a significant proportion of emergency room patients with serious medical conditions leave the hospital without ever being seen. One of two recent studies found that
11 percent of such patients ended up being hospitalized within the next week (Baker et al., 1991). In the second study, only 4 percent ended up being hospitalized but 27 percent returned to an emergency room (Bindman et al., 1991).
Measuring the Indicator
The committee used the same approach to measure avoidable hospitalization for acute conditions that it used for chronic disease conditions (see Objective 3). The only difference is that a different set of ICD-9 diagnosis codes will be highlighted in the analysis.
The committee chose to examine acute-illness-related data for diagnoses that, with timely and effective outpatient care, normally would not result in a hospital admission. Mild cases of bacterial pneumonia, cellulitis, urinary tract infections, ENT (ear, nose, and throat) infections, and precursor infections leading to pelvic inflammatory disease can often be managed with antibiotics in outpatient settings, preventing the disease from becoming more severe. In selecting specific ICD-9 codes to represent ambulatory-care-sensitive conditions, an effort was made to screen out, where possible, those admissions that would cloud interpretation of the phenomenon of interest: timely and appropriate outpatient care. For example, cases of cellulitis in which a surgical procedure was performed are excluded, because they may be repeat hospitalizations for plastic surgery procedures or trauma cases. Admissions from nursing facilities were also excluded, since these cases have been under at least nominal medical care.
The committee recognizes that the causes behind many hospital admissions for acute conditions are more complex than a delayed outpatient visit. Higher rates of admissions from low-income neighborhoods may be due to lack of health knowledge, comorbidities, or differences in prevalence arising from environmental and social factors related to poverty—all of which can interact with financial barriers to delay care. However, differences in the prevalence of various diseases among the poor, while explaining some portion of admission rate differentials, do not obviate conclusions about the presence of access problems. To counterbalance social factors, equity of access to appropriate care may require more or different types of services for some populations. For instance, these services might include nutrition education for new mothers to lower rates of gastrointestinal diseases, screening young women for venereal disease to lower their rates of pelvic inflammatory disease, or addiction services for alcoholics who are at risk of various medical complications.
As in the previous indicators that use hospital discharge data, this indicator is measured by the ratio of hospital admissions from low-income zip codes to admissions from high-income zip codes. High-income areas are
Table 3-29 Ambulatory-Care-Sensitive Conditions: Acute Disease, 1988 Admission Rates by Zip Code Income Groupings, Nonelderly Population, 11 States
|
Condition |
Low-Income Admissions/1,000 Population |
High-Income Admissions/1,000 Population |
Ratio, Low/High Income |
|
Bacterial pneumonia |
4.39 |
0.81 |
5.42 |
|
Cellulitis |
2.11 |
0.42 |
5.02 |
|
Dehydration as primary diagnosis |
0.59 |
0.28 |
2.11 |
|
Gastroenteritis |
1.30 |
0.68 |
1.91 |
|
Kidney/urinary infection |
1.28 |
0.46 |
2.78 |
|
Severe ear, nose, and throat infections |
0.82 |
0.24 |
3.42 |
|
Skin graft with cellulitis |
0.46 |
0.08 |
5.75 |
|
Total |
10.95 |
2.97 |
3.69 |
|
Source: Joint data and analysis by the Codman Research Group, the Ambulatory Care Access Group (United Hospital Fund of New York), and the IOM Access Monitoring Committee. |
|||
those in which 10 percent or less of families have incomes below $15,000. In low-income areas, 60 percent or more of the families have incomes of $15,000 or less. Again, the focus is on those under 65 years of age.
Trends in the Data
Table 3-29 highlights a number of ambulatory-care-sensitive conditions relevant to the present discussion of hospitalization for acute disease that might have been avoided with timely and appropriate care. For most of the diagnoses in the table, the rates of hospital admissions from low-income zip codes were two to five times higher than rates from high-income zip codes. The overall average ratio was 3.69.
Recommendation
Many patients seen in a hospital emergency room may be unable or unwilling to do what is necessary to recuperate at home from a serious illness. In many cases, such patients have poor social support networks, may live in homes that are overcrowded or without heat, or may be unable
to afford the necessities of life, such as food. Relatives of such a patient may have low-income jobs that make it difficult for them to stay home and provide needed care for the sick person or to pay for needed medications.
For these and other reasons, physicians may be inclined to hospitalize low-income patients more frequently than high-income ones. Current data on hospitalization do not take into account the possibility that physicians may be using different standards to admit patients (Billings et al., 1991). However, Billings' analysis of New York City data did indicate that the severity of illness for patients from the poorest zip codes was equivalent to that of patients from the highest-income zip code.
As was true for chronic-disease-related conditions, the committee believes that more detailed studies of patients and of admitting physicians are needed. These studies should sort out the relative contributions of the various factors that lead to the hospitalization of people without a source of regular medical care. Use of hospital discharge data will be enhanced to the extent that specific diagnoses can be explored in greater depth to determine their utility as indicators of access problems.
REFERENCES
Alexander, G. R., Tompkins, M. E., Peterson, D. J., and Weiss, J. 1991. Source of bias in prenatal care utilization indices: Implications for evaluating the Medicaid expansion. American Journal of Public Health 81:1013–1016.
American Cancer Society. 1989. Cancer Statistics, 1989. CA: A Cancer Journal for Clinicians 39:3–20.
American College of Obstetricians and Gynecologists, Committee on Professional Standards. 1989. Standards for Obstetric-Gynecological Services, Seventh edition. Washington, D.C.: ACOG.
Baker, D. W., Stevens, C. D., and Brook, R. H. 1991. Patients who leave a public hospital emergency department without being seen by a physician. Causes and consequences. Journal of the American Medical Association 266:1085–1090.
Behrman, R. E. 1987. Premature births among back women. New England Journal of Medicine 317:763–765.
Bild, D., Geiss, L. S., Teutsch, S. M., et al. 1988. Sentinel health events surveillance in diabetes. Journal of Clinical Epidemiology 41:999–1006.
Billings, J., Zeitel, L., Lukomnik, J., et al. 1991. Analysis of Variation in Hospital Admission Rates Associated with Area Income in New York City. New York: Ambulatory Care Access Project/United Hospital Fund of New York.
Bindman, A. B., Grumbach, K., Keane, D., Rauch, L., and Luce, J. M. 1991. Consequences of queuing for care at a public hospital emergency department. Journal of the American Medical Association 266:1091–1096.
Blendon, R. J., Aiken, L. H., Freeman, H. E., and Corey, C. R. 1989. Access to medical care for black and white Americans. Journal of the American Medical Association 261:278-281.
Bloom, B. 1988. Health Insurance and Medical Care: Health of our Nation's Children, United States. Advance Data No. 188. Hyattsville, Md.: National Center for Health Statistics.
Boutwell, R. C., and Mitchell, J. B. 1991. Diffusion of new technologies in the Medicare
population: Implications for patient access and program expenditures. Paper presented at a meeting of the Association for Health Services Research, San Diego, July 2.
Brook, R. H., and Lohr, K. N. 1986. Will we need to ration effective health care? Issues in Science and Technology 3(Fall):68–77.
Buehler, J. W., Stroup, D. F., Klaucke, D. N., and Berkelman, R. L. 1989. The reporting of race and ethnicity in the National Notifiable Diseases Surveillance System. Public Health Reports 104:457–465.
Caan, B., Horgen, D., Margen, S., King, J., and Jewell, N. 1987. Benefits associated with WIC supplemental feeding during the interpregnancy interval. The American Journal of Clinical Nutrition 45:29–41.
Centers for Disease Control. 1978. CDC Analysis of Nutritional Indices for Selected WIC Participants. Document No. FNS-176. Atlanta: Centers for Disease Control.
Centers for Disease Control. 1988. Progress in chronic disease prevention: Screening for cervical and breast cancer-Southeastern Kentucky. Morbidity and Mortality Weekly Report 36:845–849.
Centers for Disease Control. 1989a. Behavioral risk factor surveillance-Selected states, 1987. Morbidity and Mortality Weekly Report 38:469–473.
Centers for Disease Control. 1989b. National Infant Mortality Surveillance (NIMS), 1980. Morbidity and Mortality Weekly Report-CDC Surveillance Summaries, Vol. 38, No. SS-3. Atlanta: Centers for Disease Control.
Centers for Disease Control. 1989c. Summaries of notifiable diseases in the United States, 1989. Morbidity and Mortality Weekly Report 38:1–49.
Centers for Disease Control. 1990. Use of mammography-United States, 1990. Morbidity and Mortality Weekly Report 39:621–629.
Chorba, T. L., Berkelman, R. L., Safford, S. K., Gibbs, N. P., and Hull, H. F. 1990. Mandatory reporting of infectious diseases by clinicians. Morbidity and Mortality Weekly Report 39:1–17.
Cohen, D. A. 1991. Congenital syphilis. New England Journal of Medicine 324:1063–1064.
Cohen, D. A., Boyd, D., Prabhudas, I., and Mascola, L. 1990. The effects of case definition in maternal screening and reporting criteria on rates of congenital syphilis. American Journal of Public Health 80:316–317.
Coit, D. 1977. WIC Program Prenatal Data Report. Sacramento: California Department of Health Services.
Collins, T. R., DeMellier, S. T., Leeper, J. D., and Milo, T. 1985. Supplemental Food Program: Effects on health and pregnancy outcome. Southern Medical Journal 78:551–555.
Culpepper, L. 1991. Reducing Infant Mortality: The Research Gaps. Washington, D.C.: Health Resources and Services Administration.
Damiano, C., Brown, R., Johnson, J. D., and Scheetz, J. P. 1990. Access to dental care for Medi-Cal recipients. California Policy Seminar Brief 2(8) June.
Dorfman, D., and Glaser, J. H. 1990. Congenital syphilis present in infants after the newborn period. New England Journal of Medicine 323:1299–1301.
Drury, T. F., Harris, M., and Lipsett, L. F. 1981. Prevalence and management of diabetes. Health, United States, 1981. Washington, D.C.: U.S. Government Printing Office.
Food Research Action Center. 1991. WIC: A Success Story 3rd ed. Washington, D.C.: FRAC.
Fullilove, R. E., Thompson, M. T., Bowser, B. P., and Gross, S. A. 1990. Risk of sexually transmitted disease among black adolescent crack users in Oakland and San Francisco, Calif. Journal of the American Medical Association 263:851–855.
Gittelsohn, A. M., Halpern, J., and Sanchez, R. L. 1991. Income, race, and surgery in Maryland. American Journal of Public Health 81:1435–1441.
Greenberg, E. R., Chute, C. G., Stukel, T., et al. 1988. Special article: Social and economic
factors in the choice of lung cancer treatment-A population-based study in two rural states. New England Journal of Medicine 318:612–617.
Hadley, J., Steinberg, E. P., and Feder, J. 1991. Comparison of uninsured and privately insured hospital patients. Journal of the American Medical Association 265:374–379.
Hadley, J., Steinberg, E., and Klag, M. 1992. A Comparison of Insured Versus Uninsured Individuals Who Died from Acute Myocardial Infarction . Washington, D.C.: Georgetown University Center for Health Policy.
Harlan, L. C., Bernstein, A. B., and Kessler, L. G. 1991. Cervical cancer screening: Who is not screened and why? American Journal of Public Health 81:885–890.
Hayward, R. S., Steinberg, E. P., Ford, D. E., Roizen, M. F., and Roach, K. W. 1991a. Preventive care guidelines: 1991a. Annals of Internal Medicine 114:758–783.
Hayward, R. A., Bernard, A. M., Freeman, H. E., and Corey, C. R. 1991b. Regular source of ambulatory care and access to health services. American Journal of Public Health 81:434–438.
Hinman, A. R. 1990. Immunizations in the U.S. Pediatrics 86(6, pt. 2, Suppl.):1064–1066.
Hinman, A. R. 1991. What will it take to fully protect all American children with vaccines? American Journal of Diseases of Children 145:559–562.
Institute of Medicine. 1985. Preventing Low Birthweight. Washington, D.C.: National Academy Press.
Institute of Medicine. 1988. Prenatal Care-Reaching Mothers, Reaching Infants. Washington, D.C.: National Academy Press.
Institute of Medicine. 1991. Kidney Failure and the Federal Government . R. A. Rettig and N. G. Levinsky, eds. Washington, D.C.: National Academy Press.
International Agency for Research on Cancer, Working Group on Evaluation of Cervical Cancer Screening Programmes. 1986. Screening for squamous cervical cancer: Duration of low risk after negative results of cervical cytology and its implication for screening policies. British Medical Journal 293:659–664.
Ismail, A. I., and Szpunar, S. M. 1990. The prevalence of total tooth loss, dental caries, and periodontal disease among Mexican Americans, Cuban Americans, and Puerto Ricans: Findings from HANES 1983–84. American Journal of Public Health 80(Suppl.):66–70.
Kennedy, E. T., and Kotelchuck, M. 1984. The effect of WIC supplemental feeding on birth weight: A case-control analysis. The American Journal of Clinical Nutrition 40:579–585.
Koss, L. G. 1989. The Papanicolaou test for cervical cancer detection. Journal of the American Medical Association 261:737–743.
Kotelchuck, M., Schwartz, J., Anderka, M., and Finison, K. 1984. Massachusetts Department of Public Health, Division of Family Services. WIC participation and pregnancy outcomes: Massachusetts statewide evaluation project. American Journal of Public Health 74:1086–1092.
Li, D-K., Ni, H., Schwartz, S. M., and Daling, J. R. 1990. Secular change in birthweight among Southeast Asian immigrants to the United States. American Journal of Public Health 80:685–688.
Lieberman, E., Ryan, K. J., Monson, R. R., and Schoenbaum, S. 1987. Risk factors accounting for racial differences in the rate of premature birth. New England Journal of Medicine 317:743–748.
Makuc, D. M., Freid, V. M., and Kleinman, J. C. 1989. National trends in the use of preventive health care by women. American Journal of Public Health 79:21–26.
McLaughlin, M., Wilkes, M., Blum, S., Hermoso, A., Schmid, G. 1989. Risks associated with acquiring chancroid genital ulcerative disease and HIV infection: A case control study. Paper presented at the Fifth International Conference on AIDS in Montreal, Canada, June 4–9.
Miller, C. A., Fine, A., and Adams-Taylor, S. 1989. Monitoring Children's Health: Key indicators, 2nd ed. Washington, D.C.: American Public Health Association.
Nanda, D., Feldman, J., Delke, I., Chintalapally, S., and Minkoff, H. 1990. Syphilis among parturients at an inner-city hospital: Association with cocaine use and implications for congenital syphilis rates. N.Y. State Journal of Medicine 90:488–490.
National Cancer Institute. 1990a. Cancer Statistics Review, 1973–1987 . L. A. G. Ries, B. F. Hankey, and B. K. Edwards, eds. NIH Pub. No. 90–2789. Bethesda, Md.: NCI.
National Cancer Institute, Breast Cancer Screening Consortium. 1990b. Screening mammography: A missed opportunity? Results of the NCI Breast Cancer Screening Consortium and National Health Interview Survey studies. Journal of the American Medical Association 264:54–58.
National Center for Health Statistics. 1980a. Comparability of reporting between the birth certificate and the National Natality Survey. Prepared by L. J. Querec . Vital and Health Statistics, Series 2, No. 83/G. DHEW Pub. No. (PHS) 80–1357. Washington, D.C.: U.S. Government Printing Office.
National Center for Health Statistics. 1980b. Health, United States, 1980. Washington, D.C.: U.S. Government Printing Office.
National Center for Health Statistics. 1983. Birth certificate completion procedures and the accuracy of Missouri birth certificate data. Prepared by G. Land and B. Vaughan. In: Priorities in Health Statistics: Proceedings of the 19thNational Meeting of the Public Health Conference on Records and Statistics. Hyattsville, Md.: U.S. Department of Health and Human Services.
National Center for Health Statistics. 1987. Prevalence of Diagnosed Diabetes, Undiagnosed Diabetes, and Impaired Glucose Tolerance in Adults 20–74 Years of Age, United States, 1976–80. W. C. Hadden and M. I. Harris. Vital and Health Statistics. Series 11, No. 237. DHHS Pub. No. (PHS) 87–1687. Washington, D.C.: U.S. Government Printing Office.
National Center for Health Statistics. 1988. Health Aspects of Pregnancy and Childbirth, United States, 1982-Data from the National Survey of Family Growth. Series 23, No. 16. Hyattsville, Md.: U.S. Department of Health and Human Services.
National Center for Health Statistics. 1990a. Advanced Report of Final Natality Statistics, 1988. Monthly Vital Statistics Report, Vol. 39, No. 7(Suppl.). Hyattsville, Md.: U.S. Department of Health and Human Services.
National Center for Health Statistics. 1990b. Annual Summary of Births, Marriages, Divorces, and Deaths. Monthly Vital Statistics Report, Vol. 39, No. 13. Hyattsville, Md.: U.S. Department of Health and Human Services.
National Center for Health Statistics. 1990c. Health, United States, 1990. Washington, D.C.: U.S. Government Printing Office.
National Center for Health Statistics. 1991. The 1988 National Maternal and Infant Health Survey: Design, content, and data availability. M. Sanderson, P. J. Placek, and K. G. Keppel. Birth 18:26–32.
National Vaccine Advisory Committee. 1991. The measles epidemic: The problems, barriers, and recommendations. Journal of the American Medical Association 266:1547–1552.
Newacheck, P. W., and Halfon, N. 1988. Preventive care used by school-aged children: Differences by socioeconomic status. Pediatrics 82:462–468.
Office of Technology Assessment. 1988. Healthy Children: Investing in the Future. Washington, D.C.: U.S. Government Printing Office.
Office of Technology Assessment. 1990. Children's Dental Services Under the Medicaid Program-Background Paper. Washington, D.C.: U.S. Government Printing Office.
Otten, M. W., Teutsch, S. M., Williamson, D. F., and Marks, J. S. 1990. The effect of known risk factors on the excess mortality of black adults in the United States. Journal of the American Medical Association 263:845–850.
Poikolainen, K., and Eskola, J. 1986. The effect of health services on mortality: Decline in death rates from amenable and nonamenable causes in Finland, 1969–81. Lancet 1(8474):199–202.
Pope, G. C. 1988. Medical conditions, health status, and health services utilization. Health Services Research 22:857–876.
Public Health Service Expert Panel on the Content of Prenatal Care. 1989. Caring for our future: The Content of Prenatal Care. Washington, D.C.: U.S. Public Health Service.
Rolfs, R. T., and Nakashima, A. K. 1990. Epidemiology of primary and secondary syphilis in the United States, 1981 through 1989. Journal of the American Medical Association 264:1432–1437.
Rosenbaum, S., Layton, C., and Liu, J. 1991. The Health of American Children. Washington, D.C.: Children's Defense Fund.
Rush, D., Alvir, J. M., Kenny, D. A., Johnson, S. S., and Horvitz, D. G. 1988a. Historical study of pregnancy outcomes. The American Journal of Clinical Nutrition 48:412–428.
Rush, D., Sloan, N. L., Leighton, J., Alvir, J. M., Horvitz, D. G., Seaver, W. B., et al. 1988b. Longitudinal study of women. The American Journal of Clinical Nutrition 48:439–483.
Schramm, W. 1986. Prenatal participation in WIC related to Medicaid costs for Missouri newborns: 1982 update. Public Health Reports 101:607–615.
Schulte, J. M., Bown, G. R., Zetzman, M. R., Schwartz, B., Green, H. G., Haley, C. E., et al. 1991. Changing immunization referral patterns among pediatricians and family practice physicians, Dallas County, Texas, 1988. Pediatrics 87:204–207.
Schwarcz, S. K., Bolan, G. A., Fullilove, M., McCright, J., and Kohn, R. 1989. Crack cocaine as a risk factor for gonorrhea among black teenagers. Paper presented at the 117th Annual Meeting of the American Public Health Association, Chicago, October 2–26.
Scribner, R., and Dwyer, J. H. 1989. Acculturation and low birthweight among Latinos in the Hispanic HANES. American Journal of Public Health 79:1263–1267.
Stoto, M. 1992. Premature Adult Mortality in Developed Countries: From Description to Explanation. Patper presented at a meeting of the International Union for the Scientific Study of Population, Taormina, Italy, June 1992. London: Oxford University Press.
Trevino, F. M., Moyer, M. E., Valdez, R. B., and Stroup-Benham, C. A. 1991. Health insurance coverage and utilization of health services by Mexican Americans, mainland Puerto Ricans, and Cuban Americans. Journal of the American Medical Association 265:233–237.
U.S. Department of Agriculture. 1987. Estimation of Eligibility for the WIC Program. Washington, D.C.
U.S. Department of Agriculture, Food and Nutrition Service. 1990. The Savings in Medicaid Costs for Newborns and Their Mothers from Prenatal Participation in the WIC Program. Princeton, N.J.: Mathematica Policy Research.
U.S. Department of Health and Human Services. 1986. Report of the Secretary's Task Force on Black and Minority Health, Vol. 7, Chemical Dependency and Diabetes. Washington, D.C.: U.S. Government Printing Office.
U.S. Department of Health and Human Services. 1991. International Classification of Diseases, 9threvision, Clinical Modification, 4th ed. DHHS Pub. No. PHS 91–1260. Washington, D.C.: U.S. Government Printing Office .
U.S. Preventive Services Task Force. 1989. Guide to Clinical Preventive Services. Baltimore: Williams & Wilkins.
U.S. Public Health Service. 1991. Healthy People: National Health Promotion and Disease Prevention Objectives. DHHS Pub. No. (PHS) 91-50212. Washington, D.C.: U.S. Government Printing Office.
Wenneker, M. B., and Epstein, A. M. 1989. Racial inequalities in the use of procedures for patients with ischemic heart disease in Massachusetts. Journal of the American Medical Association 261:253–257.
Wenneker, M. B., Weissman, J. S., and Epstein, A. M. 1990. The association of payer with utilization of cardiac procedures in Massachusetts. Journal of the American Medical Association 264:1255–1260.
Williams, B. C. 1990. Immunization coverage among preschool children: The United States and selected European countries. Child health in 1990: The United States compared to Canada, England and Wales, France, the Netherlands, and Norway. Pediatrics 86(Suppl.):1052–1056.
Wood, D. L., Hayward, R. A., Corey, C. R., Freeman, H. E., Shapiro, M. F. 1990. Access to medical care for children and adolescents in the United States. Pediatrics 86:666–673.
Zeitel, L., Bauer, T. A., and Brooks, P. 1991. Infants at Risk: Solutions Within Our Reach. New York: United Hospital Fund of New York/Greater New York Chapter of the March of Dimes.




















































































