1
Introduction
Most Americans spend a majority of their time indoors. For many, this can be nearly 24 hours per day, including time in transit (Figure 1-1; NRC, 1981; Spengler and Sexton, 1983). The quality of indoor air, therefore, is at least as important to health as the quality of outdoor air, and in recent years concerns have increased about possible adverse health effects from indoor allergens (i.e., biological or chemical substances that cause allergic reactions). In fact, there is a growing perception that allergy has been underestimated as a public health problem. For example, indoor allergens such as those from dust mites, house pets, cockroaches, and fungi are thought to be responsible for much of the acute asthma in adults under age 50. Using asthma as an example of severe allergic disease, it is apparent that indoor allergens adversely affect the quality of life for a significant fraction (more than 10 percent) of the population (Burge and Platts-Mills, 1991). In addition, asthma was the first-listed diagnosis for more than 450,000 hospitalizations in 1987 (NHLBI, 1991). There is also a rising rate of mortality associated with asthma—especially among African Americans (NHLBI, 1991). Depending on age, African Americans are 3–5 times more likely than Caucasians to die from asthma. In 1988, a total of 4,580 people died from asthma in the United States.
The severity of asthma and the fact that it is often more easily identified than some other allergy-related conditions have led to better statistics on the effects and outcomes than are available for other allergy-related conditions. Nevertheless, most such figures are necessarily expressed as estimates. For example, recent estimates have put the total annual cost to
U.S. society from asthma at more than $6.2 billion (K. B. Weiss et al., 1992b), an increase of 39 percent over the estimated cost of the disease in 1985. Despite the lack of exactitude, the size of these costs and the fact that they represent an increasing trend argue for careful attention not only to the effects of allergy in causing asthma but also to the litany of other conditions that are more commonly thought to be associated with ''allergies." Allergic rhinitis (hay fever), for example, is a disease of dramatic proportions in this country; although not life-threatening, it nevertheless is estimated to affect some 35 million Americans (17 percent of the population) at some point in their lives. The direct and indirect costs associated with such a burden of disease are not trivial and point to the importance of serious consideration of the effects of indoor allergens on the public's health.
To a majority of people, the indoor environment has always been considered a refuge from the dangers of the outdoors, offering protection from weather, wild animals, and, in modern times, air pollution—long seen as primarily an outdoor phenomenon. In more recent times, however, reduced ventilation in energy-efficient buildings has stimulated debate and concern about increasing indoor pollutant concentrations. Much of the concern has focused on potential carcinogens, with radon and environmental tobacco smoke being good examples. But other agents and potential health effects are beginning to receive increasing consideration, and among these are the indoor allergens.
Evidence is mounting that allergy has a fundamental, causal relationship
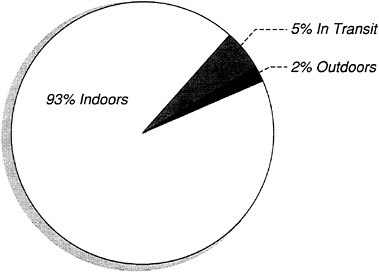
FIGURE 1-1 Amount of time spent indoors, outdoors, and in transit by most Americans.
Sources: NRC, 1981; Spengler and Sexton, 1983.
to many diseases and that aeroallergens—allergens that are airborne—are important in disease pathogenesis. For example, allergy to house dust mites and cats increases the risk of childhood asthma four- to sixfold.
There is a coherence to the body of research on these effects that now deserves emphasis: Exposure to indoor allergens is common, as are resultant sensitization and allergic disease. One hundred million Americans are immunologically sensitized to allergens; that is, they have been exposed to a substance that has raised the sensitivity of their immune system in such a way that the system will produce an "allergic response" when it encounters the allergen on subsequent occasions. The number of Americans so sensitized is fourfold more than the number with hypertension; 50 million people in this country will have a disease related to allergy at some time in their life.
With increasing levels of interest and concern about the potential health effects of indoor air, the Environmental Protection Agency's Office of Air and Radiation, in conjunction with the Agency for Toxic Substances and Disease Registry, and three of the institutes at the National Institutes of Health—the National Institute of Allergy and Infectious Diseases, the National Institute of Environmental Health Sciences, and the National Heart, Lung, and Blood Institute—requested that the Institute of Medicine (IOM) conduct an independent assessment of the public health significance of indoor allergens. Specifically, the IOM was asked to perform the following tasks:
-
Examine and characterize what is known about the adverse effects on human health caused by indoor allergens and chemicals that elicit allergic reactions.
-
Characterize the magnitude of these problems nationally and the populations that are commonly affected.
-
Identify the specific causative agents and their sources.
-
Assess testing methodologies for indoor allergens, including their applicability and interpretation.
-
Evaluate the adequacy of the knowledge base that is currently available to physicians on this topic and the need for additional information and research.
The IOM Board on Health Promotion and Disease Prevention responded to the request by establishing a committee with expertise in allergy and immunology, epidemiology, industrial hygiene, mycology, pulmonology, general and family medical practice, engineering, education, and public policy. This report, the product of the committee's deliberations, reviews published epidemiological reports, describes risk factors, and estimates the health impacts of exposure to indoor allergens. It examines clinical diagnostic practices and the measurement of indoor allergen exposures, and discusses the
need for increased awareness and knowledge of indoor allergens among primary care physicians, allergists, patients, and others.
Because of the large number of people affected by allergic disease, the committee anticipates that this report will be of interest to a broad array of readers (e.g., medical practitioners, public policymakers, members of the public whose health is adversely affected by the indoor environment). Consequently, several sections of background material are presented in this chapter; they should be useful to readers in understanding the rest of the report. The sections below present a brief historical perspective on allergies, the indoor environment, and the twentieth-century innovations that have contributed to current concerns; several concepts and definitions that the committee used as a framework for its discussions are also discussed. The chapter concludes with a brief statement regarding the report's scope and organization.
ALLERGENS AND THE INDOOR ENVIRONMENT
For more than 5,000 years, observers have recorded episodes of disease and demise that today are recognized as allergic reactions. For example, the death of King Menes of Memphis in about 3000 B.C. was the result either of anaphylaxis from the sting of a hornet or of being trampled by a hippopotamus. (A question arises because hornet and hippo share the same ancient Egyptian word.) During the sixteenth, seventeenth, and eighteenth centuries, reactions were noted (mostly to foods) that were surely allergic in nature, and some surprisingly intuitive observations were made regarding cause and effect. During this period, cats, dogs, horses, feathers, and many foods were suspected of causing asthma. In the early nineteenth century, it was recognized that pollen caused "hay fever" and that dust from beaten carpets produced similar symptoms. The first experimental challenges with pollen apparently were done by Kirkman in 1835, followed by Blackley's extensive investigations into both allergy and aerobiology in the 1870s (Blackley, 1873).
More recently, much progress has been made in recognizing specific causes of asthma and hay fever and in defining the mechanisms by which symptoms are elicited. Yet in spite of increasing knowledge of the mechanisms of allergic disease and of the agents that cause sensitization and symptoms, we have modified indoor environments in ways that may contribute significantly to exposure to these agents and to the development of allergic disease. For example, we have adopted central heating on a broad scale, which means that we heat all parts of our houses, even when they are not occupied. By the late 1960s and 1970s it became obvious that much energy was wasted in houses and other buildings owing to excessive heat transfer through surfaces such as walls, ceilings, and windows or through
"cracks." This waste inspired a federally sponsored campaign to make houses and other buildings both better insulated and "tighter." Insulation may not directly affect the levels and kinds of allergens in the indoor environment (as long as it remains dry), but decreased ventilation encourages their accumulation and may increase relative humidity, leading to conditions that favor the growth of biological allergen sources (e.g., microbes and mites).
Other twentieth-century amenities have also contributed to increased allergen exposure. The invention and widespread use of the vacuum cleaner have been followed by the practice of installing wall-to-wall carpeting in homes, schools, hospitals, and offices, despite the fact that the vacuum cleaner is probably not effective for removing skin scales, mites, and excess moisture from carpeting. In fact, vacuum cleaning is quite effective in dispersing and suspending allergens and other particles in the air. Heating, ventilating, and air-conditioning (HVAC) systems, which have become widespread in this country, can also create problems in terms of indoor allergens. On the one hand, HVAC systems allow windows to remain closed, filter out outdoor particulate material, and decrease relative humidity, thus lowering the risk of microbial and mite contamination. On the other hand, if air-conditioning units are not maintained properly, they can be sources of microbial contamination and have caused more than one major epidemic of infectious disease (Fraser et al., 1977). In addition to these factors, pets in the home are a major source of allergens and can play a large role in sensitization and allergic disease (Mathison et al., 1982; Ohman et al., 1977; Reed and Swanson, 1987; Swanson et al., 1989). Thus, lifestyle changes have influenced indoor air pollution both positively and negatively. Overall, indoor air quality is better than it was in the Middle Ages, when straw was used as a floor covering, sanitation was nonexistent, and burning fuels created a smoky environment. In modern times, however, homes and buildings still harbor the potential for severe allergic problems.
Over the past 25 years, a steady increase in our knowledge of the biological sources (sensitizing agents) that give rise to immunological sensitization has allowed us to identify specific health risks and to establish methods for measuring some of the indoor agents that are thought to cause hypersensitivity disease (i.e., "allergies"). For most agents, it is clear that exposure creates a risk, but insufficient data are available to propose threshold or risk levels. For a few sensitizing agents, it has been possible to propose specific levels of exposure that constitute a risk for sensitization and symptom development (Platts-Mills and Chapman, 1987). Most research on indoor air quality, however, has focused on the same pollutants that are found in outdoor air (nitrogen oxides, carbon monoxide, etc.) and a few other nonbiological agents that are either relatively easy to measure (e.g., asbestos, radon) or that have stimulated major controversy (e.g., environmental tobacco smoke). Very little research has been directed toward
the health effects, prevalence, or relative risks of allergens, toxins, and volatile irritants of biological origin in indoor air.
The major sources of indoor allergens include house dust mites, molds, and animal dander. These and other potential sources of allergens are the focus of this report and are covered in detail in the chapters that follow. Also emphasized are several specific allergic diseases of the upper and lower airways: rhinitis, asthma, and hypersensitivity pneumonitis. Before proceeding to this discussion, however, several concepts and definitions are described that will be useful to an understanding of the material that follows. Readers are also encouraged to consult the glossary, which follows the references at the end of the main text of the volume.
CONCEPTS AND DEFINITIONS
Allergy, generally speaking, is the state of immune hypersensitivity that exists in an individual who has been exposed to an allergen and has responded with an overproduction of certain immune system components such as immunoglobulin E (IgE) antibodies (defined below). More specifically, common use of the term allergy usually refers to a type I hypersensitivity reaction (the type I reaction is also called the anaphylactic type or immediate type of allergic reaction). It is the common type of allergic reaction caused by IgE antibody and results in the common allergic diseases such as hay fever, allergic asthma, allergic urticaria, and the less common but potentially fatal anaphylactic reaction. About 40 percent of the population have IgE antibodies against environmental allergens, 20 percent have clinical allergic disease, and 10 percent have significant or severe allergic disease.
Gell and Coombs (1968) classified hypersensitivity reactions into four major types, according to the immune mechanisms involved (see Table 1-1). For the purposes of this report (and unless noted otherwise), the term allergic reaction means the immediate hypersensitivity response that occurs when a sensitized individual is exposed to an allergen, that is, a type I, IgE-mediated reaction. Although these reactions against indoor allergens are our primary focus, some attention is also given to allergic diseases that operate through different mechanisms, for example, hypersensitivity pneumonitis—a disease that involves IgG antibodies and reactive lymphocytes. Chapter 4 describes the mechanisms of the immune function in technical detail.
There are two major components of the immune system that respond to allergens: antibodies, which are specific proteins of the immunoglobulin E (IgE) type, and mast cells, which carry receptors for IgE and release chemicals such as histamine. The initial phase of the immune response, known as sensitization, sets up the mechanisms for an allergic reaction (Figure 1-2).
TABLE 1-1 Four Types of Immunologic Reactions to Indoor Allergens that Cause Pulmonary Disease in Humans
|
Type of Hypersensitivity Reactiona |
Immunologic Mediation |
Antigen |
Method of Study |
|
Type I (anaphylactic) |
IgE antibody |
Proteins such as animal allergens |
Correlation of skin tests or in vitro measurement of antibody with symptoms |
|
Type II (cytolytic) |
IgG antibody against cells haptenized with allergenic chemicals |
Allergenic chemicals: acid anhydrides and isocyanates |
Theoretical concepts under research study |
|
Type III (antigen-antibody complex) |
Antigen-antibody complex and inflammatory cells |
Proteins such as avian proteins |
Precipitating antibody correlated with exposures and symptoms |
|
Type IV (lymphocyte-mediated) |
Lymphocyte-mediated reactions in lung against antigen |
Avian and microbial proteins, for example |
Correlation of clinical disease with lymphocyte activation and cytokine release after antigen exposure |
|
a Gell and Coombs's (1968) classification. |
|||
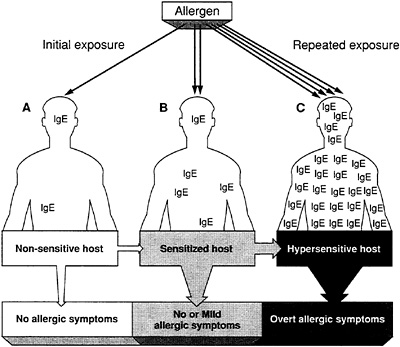
FIGURE 1-2 Hypersensitivity and IgE-mediated allergy. (A) Upon initial exposure to an allergen, there will be no overt manifestations of allergic disease because the patient is nonsensitized. However, this allergen will initiate an immune response that results in the synthesis of IgE and sensitization of the susceptible (atopic) host. (B) Upon subsequent, repeated exposures, this sensitized individual will synthesize increased amounts of IgE, thus becoming hypersensitive, although mild allergic symptoms may or may not be present. (C) From this point onward, reexposure to this specific allergen will provoke the overt manifestations of allergic disease. Source: Fireman and Slavin, 1991.
During sensitization (in the case of airborne allergens, this occurs in the airways or on the skin), the immune system of a susceptible person encounters an allergen in the form of an antigen (a substance that stimulates the production of an antibody). The system responds by producing IgE specific to that antigen1—that is, an IgE that will recognize and react with that specific antigen when they meet again. During the sensitization process, the antigen-specific IgE that is produced attaches to receptors on mast cells2—completing the sensitization process. When the "sensitized individual" is
exposed again to the allergen, the IgE on the mast cells binds the antigen, triggering the mast cells to release histamine and other chemicals from their cytoplasm. These chemicals interact with surrounding tissues, producing inflammation and the typical allergic reaction. IgE antibody production can last for many years, sensitizing the mast cells. Thus, for example, someone who had an allergic reaction to penicillin as a child could still be allergic to the drug as an adult.
Another important term is atopy. Atopy is generally defined as the state of having one or more of a defined group of diseases (allergic rhinoconjunctivitis, allergic asthma, and atopic dermatitis) that are caused by the genetic propensity to produce IgE antibodies to environmental allergens (predominantly from pollens, molds, dust mites, animals, and foods) encountered through inhalation, ingestion, and possibly skin contact. Although everyone produces some IgE, people with a genetic predisposition to allergy (i.e., atopy) produce significant quantities of it.
For epidemiological surveys, atopy is sometimes defined differently, that is, solely by the presence of IgE antibodies to one or more allergens—whether or not clinical disease is present. The population identified by this definition is considerably larger than that defined by disease because a sizable number of asymptomatic persons have such antibodies (this condition is known as asymptomatic atopy).
Thus, an atopic individual is defined differently in different settings and by different researchers as either a person with a particular disease described under atopy or a person with IgE antibody (i.e., positive skin tests). It is obviously important, therefore, that the context and use of the term be well defined in its particular applications and settings. In discussing the published literature in this report, the meaning of the term will correspond to that used in the study being considered.
SCOPE AND ORGANIZATION OF THE REPORT
In addressing the tasks described earlier in the chapter, the committee used the following guidelines to define the scope of its deliberations. First, it focused on airborne allergens, although contact allergens (e.g., cosmetics) and food allergens are also in the home (the second major focus). A second major focus in the scope was the residential environment; the broad topic of industrial/occupational allergens was deemed to be beyond the scope of this report and was not covered in depth. Some attention is given, however, to allergens that are found in nonindustrial work sites such as office buildings, hospitals, and schools. Similarly, some attention is given to selected nonbiological chemicals that have been shown to be allergenic and that are found in residential or nonindustrial work sites (e.g., trimellitic
anhydride and isocyanates). Primarily, however, the report focuses on airborne allergenic agents of biological origin.
In-depth consideration of multiple chemical sensitivity (MCS) reactions was excluded from the scope of this report because of a lack of data showing immune mechanisms. As stated in a recent NRC report (NRC, 1992a, p. 138), "there is insufficient evidence to ascribe an immune etiology to this disorder." For information on the topic of MCS the reader is directed to the recently published proceedings of a workshop and compilation of individually authored papers (NRC, 1992b).
The remaining seven chapters of this volume present the committee's findings, conclusions, and recommendations on several aspects of the problem of indoor allergens. Chapter 2 discusses the magnitude and dimensions of allergen-caused disease, and Chapter 3 presents a detailed discussion of allergen sources and their distribution. Chapter 4 describes the mechanisms of immune function. A discussion of test methods, with particular attention to their applicability, reliability, and interpretation appears in Chapter 5. Chapter 6 discusses the assessment of exposure and risk. The report concludes with an examination in Chapter 7 of engineering control strategies and the role of education in Chapter 8.
In preparing this report, the committee identified and developed a list of research agenda items and 15 priority recommendations. The recommendations focus primarily on the need to improve awareness and education, and as such are also relatively inexpensive and easy to implement compared to the research agenda items. The research agenda focuses on the longer term, more expensive, and more technical aspects of fundamental research and data collection.
Although cost-benefit analyses were beyond the scope of the committee's charge in conducting this study the committee's findings have been separated into recommendations and research agenda items, as described above, based on relative ease of implementation and estimations of associated costs. Policy development and further priority setting, however, should be based on investigations of the probable costs and benefits of the various strategies for prevention and control. The cost analyses should include both direct and indirect costs (i.e., medical costs as well as lost work), and benefits should include a full assessment of the effects on improving the quality of life and on reducing morbidity and mortality.
All of the committee's recommendations and research agenda items are compiled in the Executive Summary. In the body of the report they are presented in their individually relevant chapters and chapter sections.










