7
Nonmalignant Respiratory Effects of Mustard Agents and Lewisite
It is well documented that inhalation of sulfur mustard or Lewisite causes acute damage to the respiratory tract. In fact, pulmonary injury is the principal cause of mortality in the first few days to weeks after exposure to sufficiently high concentrations of sulfur mustard (Hosseini et al., 1989; Papirmeister et al., 1991; Willems, 1989).
The primary question at issue in this report, however, is whether repeated daily exposures to these agents, at the concentrations used in the World War II (WWII) testing programs, are associated with long-term respiratory effects. If a risk of chronic effects is judged to exist among these human subjects, a secondary question arises as to whether an acute response is a necessary precursor to the development of long-term respiratory effects.
There are few directly relevant studies available for answering these questions and, as discussed in Chapter 3, the long-term health status of the subjects has not been followed. Nevertheless, some data do exist on the chronic health effects among populations exposed to sulfur and nitrogen mustards in far different contexts. To make inferences to the WWII testing program experiments, however, would require knowing the exposure levels present in each of the contexts. Thus, the conclusions reached in Chapter 3 regarding the possible exposure levels of human subjects in the WWII testing programs become key aspects of this assessment.
This chapter deals with chronic, nonmalignant respiratory effects. It is based primarily on a review of the epidemiologic and clinical literature on chronic effects of exposures incurred in the manufacture of mustard agents, in combat, and in medical therapeutic situations. Finally, in an
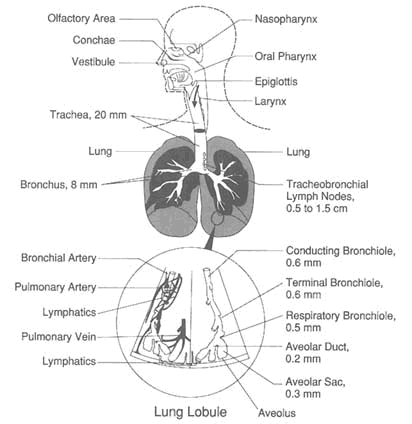
FIGURE 7-1 Structure of the respiratory tract. SOURCE: National Research Council, 1979.
attempt to understand the relationship between the acute and chronic responses to these agents, other respiratory hazards known to cause both acute and chronic effects are also reviewed.
PHYSIOLOGY AND ANATOMY
The basic anatomy of the respiratory tract is illustrated in Figure 7-1. The respiratory tract is lined with epithelial cells of different types, depending on their location and functions. A stratified squamous epithelium lines the nasal vestibule, followed by pseudostratified ciliated and ciliated columnar to cuboidal epithelium that lines the remainder of the nose, trachea, bronchi, and bronchioles (Figure 7-2). These cells are interspersed with nonciliated goblet and Clara cells. The cells are coated with a thin layer of mucus secreted by the goblet cells and
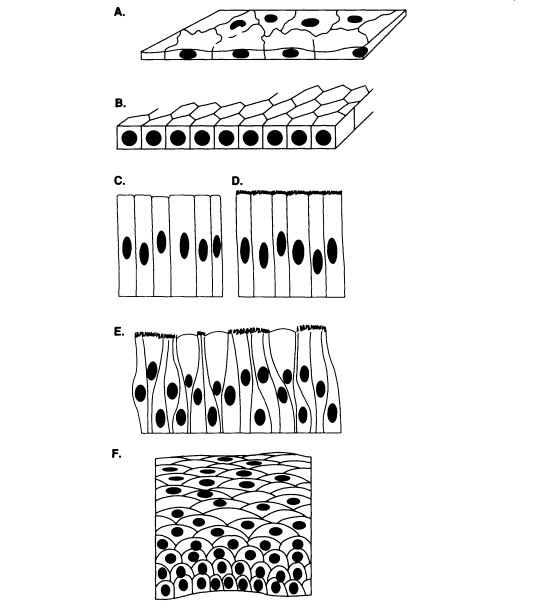
FIGURE 7-2 Illustration of the various types of cellular arrangements of epithelium that line internal body passages, including the respiratory system. Specialized cells, such as goblet cells, that secrete mucus into the passages are often interspersed with the epithelial cells. Clara cells take the place of goblet cells in certain parts of the respiratory system. A: simple squamous; B: simple cuboidal; C: simple columnar; D: ciliated columnar; E: pseudostratified ciliated columnar with goblet cells; and F: stratified squamous. SOURCE: Adapted from Stedman's Medical Dictionary, 1976, with permission from Williams & Wilkins.
mucous glands. The ciliated cells and the mucus serve as an escalator to move materials from the deep lung to the oral cavity where they are swallowed and excreted.
The conducting airways extend through the respiratory bronchioles, which terminate into the acini, consisting of alveolar ducts, alveolar sacs, alveoli and associated blood vessels, lymphatic tissues, supportive tissues, and nerve endings. The alveoli are the primary site of gas exchange with the blood, and are lined by two specialized types of epithelial cells (Type I and Type II alveolar epithelial cells). The total alveolar surface area in the adult human is about 100 m 2 during deep inspiration (Menzel and Amdur, 1986; Phalen and Prasad, 1988).
The most important type of inhalation exposure of the respiratory tract to sulfur mustard or Lewisite, including the chamber tests and field trials, has been to vapors of these compounds (Papirmeister et al., 1991). Inhaled vapors rapidly contact airway surfaces by the process of molecular diffusion (Lippmann, 1992). Surface uptake of the vapor then depends on the chemical properties of the inhaled compound. Highly reactive compounds with characteristics similar to sulfur mustard are generally removed higher in the respiratory tract and, thus, cause most of their damage in nasal, laryngeal and bronchial regions of the respiratory tract (Dahl, 1990; Dahl et al., 1991; Lippmann, 1992).
ACUTE EFFECTS AND BIOLOGICAL MECHANISMS
The inhalation of sulfur mustard or Lewisite causes acute damage to the respiratory tract, but the symptoms of exposure are not immediate and develop over a period of several days. Pulmonary injury is in fact the principal cause of mortality in the first few days to weeks after exposure to sulfur mustard (Hosseini et al., 1989; Papirmeister et al., 1991; Willems, 1989). The signs and symptoms of respiratory tract damage following inhalation of various levels of sulfur mustard are summarized in Table 7-1.
Damage to the respiratory tract involves acute edema (swelling), inflammation, and destruction of the airway epithelial lining. Depending on the dose, the destruction may be mild to severe. Severe damage includes destruction of the epithelium with subsequent formation of pseudomembranes (such as those formed in diphtheria infections), which may slough and obstruct the airway, resulting in death. In most cases, the injury is most severe in the larynx, trachea, and bronchi, with small bronchi less affected than large bronchi. The basement membranes that underlie the epithelium are edematous and are infiltrated by white blood cells. In some cases, presumably with high exposures, damage extends into the deeper alveolar regions, resulting in generalized edema of the lung. Finally, allergic hypersensitivity reactions to inhaled sulfur
TABLE 7-1 Effects of Acute Sulfur Mustard Vapor Exposure on the Human Respiratory Tract (at 16°C-27°C unless otherwise noted)
|
Estimated Exposure |
Effects |
Latency |
Reference |
|
12-70 mg·min/m3 |
Hoarseness; nasal mucosa irritation; nondisabling; recovery in approximately 2 weeks |
12 hours to 2 days |
Project Coordination Staff, 1946 |
|
100-500 mgmin/m3 |
Pulmonary effects evident (very little data) |
Not available |
Sidell, 1990 |
|
200 mg·min/m3 |
Median incapacitating Ct (ICt50). Upper airway effects of sneezing, lacrimation, rhinorrhea, sore throat, hoarseness, nosebleed, from which recovery usually occurs after two weeks. Lower airway effects of tracheobronchitis, hacking cough, rapid breathing, and pseudomembrane formation. Pulmonary edema, bronchial pneumonia, and other secondary infections may develop after 36-48 hours. Prolonged recovery (1-2 months), particularly after infections. |
4 to 6 hours |
Ganas, 1969; Stepanov and Popov, 1962 |
|
1,000-1,500 mg·min/m3 |
1,500 mg·min/m3 is estimated median lethal Ct (LCt50). Injuries as for ICt50 above, progressing to edema in pharynx and tracheobronchial tree; death due to severe edema, secondary infection or necrotic bronchopneumonia. Incapacitating for survivors; recovery over period of several mnths. |
24 to 48 hours |
Robinson, 1967; Sidell, 1990; Stepanov and Popov, 1962; U.S. Army, 1974; U.S. Army CRDEC, 1990; U.S. Army and U.S. Air Force, 1975; WHO, 1970 |
|
150 mg/m3 (10 min) 1,500 mg·min/m3 |
Reported human lethal concentration; no temperature data |
Not available |
Back et al., 1972 |
|
70 mg/m3 (30 min) 2,100 mg·min/m3 |
Reported human lethal concentration; no temperature data |
Not available |
Inada et al., 1972 |
|
SOURCE: Adapted from Papirmeister et al., 1991; Watson and Griffin, 1992. |
|||
mustard vapors have not been well studied, but could be involved in cases of chronic exposures to sulfur mustard (Morgenstern et al., 1947; Papirmeister et al., 1991).
Infection of the respiratory tract resulting in bronchopneumonia is a common complication of respiratory tract injury from inhaled sulfur mustard. It appears that most deaths following inhalation of sulfur mustard result, at least in part, from pulmonary infection, often complicated by septicemia (Hosseini et al., 1989; Keshmiri, 1989; Papirmeister et al., 1991; Willems, 1989). Immunosuppression from systemic absorption of sulfur mustard probably plays a major role in the pathogenesis of these infections, although its importance relative to the local pulmonary injury is not well understood. Pulmonary infection and septicemia, despite modern antibiotic therapy, were still significant causes of death in Iranians taken to Europe for treatment (Willems, 1989).
The above descriptions of the acute effects come primarily from humans who died following World War I (WWI) gas attacks and from animals that died as a result of experimentally induced lesions (Papirmeister et al., 1991). There is little contemporary information regarding the pathogenesis of the respiratory lesions or few data from people or animals exposed to nonlethal concentrations of sulfur mustard vapor. There are even fewer studies in which the histopathology of the recovery process has been studied in animals exposed to sulfur mustard. However, two studies conducted during WWI suggest that low-level exposure or survivable exposures in dogs and rabbits may produce scar tissue following small ulcerations in the trachea and larynx, causing contractions of these areas (Warthin and Weller, 1919; Winternitz, 1919). Nevertheless, the descriptions of the more severe lesions of the respiratory tract of animals exposed to sulfur mustard vapor and those in humans appear to be quite similar in type and location (Papirmeister et al., 1991). Thus, further studies in animals conducted to follow the repair of the acute respiratory tract lesions from nonlethal, inhaled sulfur mustard vapor would be of value in determining the persistence and course of such lesions in people. However, it has been difficult to induce a chronic bronchitis that persists following cessation of exposure in animals (Greene et al., 1984).
The acute effects of inhaled Lewisite vapors are similar to those discussed above for inhaled sulfur mustard vapor. A major exception is that the irritating effect of Lewisite is immediately detectable by the exposed person. Data on the histopathological lesions in the respiratory tract from inhaled Lewisite are available only from animals, but the reported lesions are generally very similar to those discussed above for sulfur mustard. However, at high concentrations, Lewisite-induced pulmonary edema appears to be more prominent than with sulfur mustard. Hemoconcentration, presumably due to this pulmonary
edema, has also been reported to be a prominent finding following inhalation of Lewisite (Urbanetti, 1988).
EVIDENCE OF LONG-TERM HEALTH EFFECTS
Animal Studies
Inhaled sulfur mustard vapor produces destruction of the epithelium of the respiratory tract. Apparently, much of the vapor is removed higher in the respiratory tract: the nasal, laryngeal, and tracheobronchial regions appear to be the most severely affected (Papirmeister et al., 1991). Many of the animal studies of toxicity from inhaled sulfur mustard were conducted during WWI. In rabbits, inhalation of sulfur mustard produced damage that was particularly prominent in the upper respiratory tract, including the nasal passages, pharynx, larynx, trachea, and large bronchi (Warthin and Weller, 1919). The damage increased with increasing exposure concentrations. Low levels of exposure caused congestion of these areas without hemorrhage. Degeneration of mucous cells was observed in the pharynx and larynx. The highest levels of exposure caused necrosis of the epithelium, infiltration of white blood cells, and the formation of diphtheritic-like pseudomembranes.
Experiments in dogs showed necrosis of the epithelium of the upper respiratory passages with pseudomembrane formation. This usually extended to the bronchioles. Animals that died from two to ten days following exposure had evidence of necrotizing pneumonia. Animals sacrificed at later times showed localized ulceration or constriction of the trachea (Winternitz, 1919).
Lung damage also occurred following intravenous injection of sulfur mustard into animals (Office of Scientific Research and Development, 1946). Intravenous injection of a solution of sulfur mustard in either propylene glycol or thiodiglycol was reported to cause diffuse pulmonary congestion and edema, but pure sulfur mustard given rapidly caused more serious necrotic and hemorrhagic lesions of the lung. However, these authors attributed this lung damage from injected sulfur mustard to localization of particulate sulfur mustard in the pulmonary capillaries, because pulmonary injury was not observed with other parenteral routes of administration.
Sulfur mustard is absorbed through the skin into the systemic circulation. Following intravenous administration of radiolabeled sulfur mustard in rabbits, the level of radioactivity in tissue was highest in kidney, followed by lung and then liver (Boursnell et al., 1946). Thus, it is conceivable that some sulfur mustard exposure of respiratory tract tissue with subsequent biological effects could occur following systemic absorption from skin exposure.
Human Studies
The clinical and epidemiologic literature on health effects of sulfur mustard covers three types of exposure situations: (1) chronic occupational exposures incurred in the manufacture of the mustard agent; (2) acute combat exposures; and (3) medical use as antitumor drugs.
Occupational Exposure
There is some relatively recent epidemiologic literature on occupational exposure to mustard agents in British and Japanese munitions factories. Several studies suggest that workers who were chronically exposed to mustard agents developed chronic nonmalignant respiratory effects (Easton et al., 1988; Manning et al., 1981; Nishimoto et al., 1970). In the British population, chronic respiratory disease has been reported to occur even among workers with only a few years of employment (Easton et al., 1988).
In a cohort mortality study of 511 employees at a manufacturing plant in England, a significant excess of deaths due to pneumonia was found (Manning et al., 1981). In a more extensive examination of this same plant, Easton examined the mortality patterns of an enlarged cohort of 3,500 workers and reported standardized mortality ratios (SMRs, measures of relative risk) for specific causes of death (Easton et al., 1988). Findings included statistically significant excesses of nonmalignant respiratory disease (SMR = 143), including subcategories of influenza and pneumonia (SMR = 143), bronchitis (SMR = 159), and asthma (SMR = 151). These excesses were present even among those with less than three years of employment at the plant, and were not related to duration of employment. The finding of excess mortality due to nonmalignant respiratory disease observed shortly after initial exposure is consistent with the follow-up studies of combat survivors, in which bronchitis and emphysema were found to be present within months of the acute exposure (see below).
Workers exposed to sulfur mustard and Lewisite in a Japanese production plant were surveyed for respiratory morbidity 25 years after production had ceased (Nishimoto et al., 1970). The survey included chronic symptoms and pulmonary function assessments, that is, forced vital capacity (FVC) and forced expiratory volume in 1 second (FEV1). The study group of 1,403 represented 62 percent of those identified from among the 5,000 total former employees of the plant. Based on an internal comparison, more highly exposed workers reported more chronic bronchitis and had slightly lower FEV1/FVC than either a less-exposed or unexposed clerical group of coworkers. Compared to groups of unexposed patients at a Chicago respiratory clinic and
''ordinary" patients at a Japanese clinic, the group exposed to mustard agent and Lewisite had more chronic bronchitis, chronic cough, and reduced FEV1/FVC. Among nonsmokers, almost half of those previously exposed to mustard agents or Lewisite reported persistent productive cough, compared to 30 percent in the unexposed group. The former poison gas workers showed a more bronchitic type of airway obstructive pattern than did the ordinary patients with chronic obstructive pulmonary disease (COPD); however, they did not have less anatomical evidence of emphysema.1 Based on this literature, the Agency for Toxic Substances and Disease Registry (ATSDR) concluded in the recent Toxicological Profile for Mustard "Gas" (1991) that, "when the vapors are breathed for a prolonged period, other respiratory diseases, such as chronic bronchitis . . . can eventually occur."
None of the epidemiologic studies of occupational exposures provided estimates of exposure level. It has been reported that worker protection was inadequate in the Japanese factories and that employees were exposed to significant levels of sulfur mustard, and to a lesser extent to Lewisite (Wada et al., 1962). Conditions may have been better, but still relatively poor, in British munitions factories (Haber, 1986). It is difficult to judge the safety conditions, however. For example, as discussed in Chapter 3, all sulfur mustard and Lewisite production in the United States was accomplished at military bases controlled by the Chemical Warfare Service. This group's safety record was the worst in the military during the peak years of production, with hundreds and probably thousands2 of documented injuries resulting from sulfur mustard and Lewisite (Brophy and Fisher, 1959; Cochrane, 1946). Given this high incidence of injury, it is surprising that follow-up studies of chemical warfare production workers have not been conducted on the U.S. worker populations.
Battlefield Exposure
The risks associated with acute combat exposures are probably more relevant for predicting the likely long-term effects of the experimental chamber exposures. Chamber exposures were delivered over a period of
days to weeks and were designed to simulate combat exposures in terms of concentration, humidity, and temperature.
World War I. In a 1922 clinical study of 83 pensioners with recognized disability due to gas poisoning, the principal symptom was shortness of breath (Sandall, 1922). Persistent cough, expectoration, and chest tightness were also frequent. Sandall reported that, on physical examination, 26 percent showed signs of "emphysema," while another 20 percent had some definite signs of bronchitis.
A similar clinical study published in the same year involved 166 sanatorium patients, who gave a definite history of having been gassed during the war and hospitalized for at least 20 days (Hankins and Klotz, 1922). Of these young adults, 25 percent gave a history of influenza or pneumonia, and all reported having never regained their health since the gassing. Shortness of breath, cough, and expectoration were common, as were asthmatic symptoms. Based on X-ray findings, the clinical picture was one of chronic peribronchitis, resulting from a permanent thickening of the bronchial mucous membrane.
Berghoff reported clinical data based on 2,000 U.S. servicemen who had been gassed with chlorine or sulfur mustard and were examined in the course of their related discharge (Berghoff, 1919). Of those exposed to sulfur mustard, most had been exposed in an explosive attack three to four months prior to discharge. Of the total group, 30 percent were diagnosed to have bronchitis, characterized by prolonged expiration and coarse moist rales. Another 22 percent had characteristics associated with emphysema, including a rigid chest, limited diaphragm movement, and impaired expansion.
Gilchrist and Matz (1933) selected 89 living and 53 deceased cases from among 1,016 U.S. servicemen who had been gassed with sulfur mustard during World War I. The 89 living cases were examined clinically and roentgenologically eight to ten years after exposure to sulfur mustard. The basis for selection of cases was the availability of full and well-documented histories of exposure to sulfur mustard, based on military records, and the severity of the effects, also from information in military records. These investigators concluded that 27 of the 89 men who were examined nine to ten years after gassing had evidence of anatomic or symptomatic disease attributable to their exposure to sulfur mustard. The residual effects on the respiratory tract they noted were chronic bronchitis, emphysema, and bronchial asthma.
There is also evidence that British soldiers exposed to mustard gas during combat in WWI had a higher incidence of chronic bronchitis than the general population (Case and Lea, 1955). One study, designed to examine for lung cancer, identified a group of 1,267 war pensioners who had suffered from sulfur mustard poisoning; 80 percent of the group had
chronic bronchitis. Although this study group may not have been representative of the entire cohort of veterans with exposure to sulfur mustard, the findings strongly suggest an elevated risk of chronic bronchitis associated with combat exposure.
Iran-Iraq War. There are several more recent reports of chronic respiratory effects among people with combat exposure in the Iran-Iraq war. Hosseini and colleagues described 61 victims of sulfur mustard injury, between the ages of 15 and 30, seen two to four weeks following exposure (Hosseini et al., 1989). Twenty-one of these patients were followed for 15 months with spirometry and X-rays. The symptomatic profile of the patients indicated that all 61 had cough, 75 percent had sputum, and 62 percent experienced shortness of breath. An improvement in symptoms during follow-up was observed for one subject. Only 20 percent appeared to have "normal" patterns of pulmonary function, defined as predicted FVC and FEV1/FVC values greater than 80 percent. The FVC was less than this for 71 percent of those followed, and the FEV1/FVC was below this figure in 52 percent of the cases. The authors were unable to explain this observed inconsistent pattern of abnormalities. In another report of survivors of the Iran-Iraq conflict, Somani and Babu (1989) described delayed effects, present two years after the exposure, which included chronic bronchitis and recurrent pneumonia.
In summary, the literature on the longer-term respiratory effects of acute combat exposures suggests the presence of significant chronic lung disease of both an obstructive and a restrictive nature. Yet, most of these studies were based on individuals who had sustained an initial acute injury with documented symptomatology. There is no direct examination of whether such chronic effects can occur in the absence of an observable acute response.
Medical Therapeutic Exposure
A variety of chemicals, including antitumor drugs with similarities to sulfur mustard, are known to damage lung tissue following systemic administration. Table 7-2 is a listing of antitumor drugs for which there is good evidence of pulmonary toxicity, particularly pulmonary fibrosis, following their administration in patients (Muggia, 1983; Rosenow et al., 1985; Smith and Walker, 1990; Weiss and Muggia, 1980). Although five of these drugs are alkylating agents (as is sulfur mustard), the alkylating agents nitrogen mustard and thio TEPA have not been reported to produce pulmonary fibrosis (Weiss and Muggia, 1980). Thus, the question of pulmonary effects following absorption of sulfur mustard, or
TABLE 7-2 Antitumor Drugs That Produce Pulmonary Fibrosis
|
Classical Alkylating Agents |
Antibiotics |
Nitrosoureas |
Miscellaneous |
|
Busulfan |
Bleomycin |
Carmustine |
Cytosine arabinoside |
|
Chlorambucil |
Mitomycin |
Semustine |
Methotrexate |
|
Cyclophosphamide |
Zinostatin |
Chlorozotocin |
6-Mercaptopurine |
|
Melphalan |
|
Lomustine |
Procarbazine |
|
Uracil mustard |
|
|
VM-26 Vinblastine Vincristine |
|
SOURCES: Muggia, 1983; Rosenow et al., 1985; Smith and Walker, 1990. |
|||
for that matter for Lewisite, from systemic absorption following an exposure to skin, cannot be answered with available information.
RELATIONSHIP BETWEEN ACUTE AND CHRONIC EFFECTS CAUSED BY EXPOSURES TO OTHER RESPIRATORY HAZARDS
There is clear evidence from descriptions of severe overexposure to sulfur mustard that exposure can cause both acute and chronic respiratory disease. However, there is little information available on the effects of lower levels of acute exposure, and apparently no information on the relatively brief exposures to levels that typify the experience in the chamber and some field studies.
Even in the absence of follow-up studies that directly address the question, however, it can still be pursued by examining indirect evidence from studies of compounds that might behave similarly. To evaluate the respiratory health risk associated with repeated brief overexposures at nonlethal levels, the committee requested an expert review of indirect evidence focusing on the link between acute and chronic respiratory responses to similar agents (see Appendix J). The review included exposures to irritant gases (chlorine, sulfur dioxide, and combustion products), materials of plant origin (cotton), chemicals (isocyanates), and inorganic dusts (silica, beryllium, and asbestos).
Sources of similar exposures include accidental overexposures to irritant gases, which have occurred in the workplace as well as the general community. Becklake and colleagues have reviewed the literature on acute and chronic effects associated with massive accidental exposures to sulfur dioxide, chloride, and oxides of nitrogen (Becklake et al., 1988). In 16 studies of sulfur dioxide, persistent abnormalities were consistently reported, including airflow limitation, with symptoms lasting up to 10 years following a single overexposure (Haskonen et al., 1979). For oxides of nitrogen, persistent abnormalities were less consis-
tent; for overexposure to chlorine, abnormalities were found to be rarely persistent. In a community study based on a population exposure to chlorine, subjects exposed during the derailment of a tank car were followed up six years after the accident. The rate of annual decline in FEV1 was found to be unrelated to the initial clinical status of the subjects (Jones et al., 1986).
Becklake concludes that none of the many case reports, nor the one community study, provides evidence to suggest that the pathophysiologic process induced by the exposure to an irritant gas was progressive. Persistent pulmonary damage did not appear to be determined by the degree of acute response at the time of the exposure, or by the extent of initial recovery that occurred during the several months following the exposure.
Exposures to cotton dust or components of the dust have been noted to cause both acute and chronic effects. The acute effects are represented by both a disabling respiratory syndrome (byssinosis) and a cross-shift decrement in FEV1. Chronic effects include both accelerated annual decrements in FEV1 and chronic bronchitis. The acute syndrome does not necessarily remit on removal from exposure, and there is a growing body of evidence to suggest a relationship between the acute effects and chronic airflow limitation. There is evidence that short-term exposures result in acute effects (Castellan et al., 1987; Martin and Higgins, 1976), but no evidence for whether such exposures, with or without an acute response, ultimately lead to chronic effects.
Isocyanates have been noted to cause several acute conditions, including chemical bronchitis and allergic bronchoconstriction (Axford et al., 1976; Brooks et al., 1985) and large dose-related cross-shift losses in FEV1 (Peters et al., 1968). The chronic respiratory effects caused by isocyanates include accelerated loss in pulmonary function over several years, suggesting the development of chronic airway limitation, and irreversible asthma (Peters and Wegman, 1975). There is also evidence that the presence of acute effects predicts both the development of chronic asthma and an accelerated rate of loss in lung function in nonasthmatics. Finally, there is evidence that short-term exposures to isocyanates can cause acute responses that are irreversible and progressive, but there is no evidence as to whether such short-term exposures without acute response result in irreversible respiratory effects.
Beryllium exposures have also been associated with both acute and chronic pulmonary disease, both of which have been shown to be disabling (AMA Archives of Industrial Health, 1959). Relevant to the present question, beryllium exposures, in one instance as brief as one week and in several instances occurring for less than ten weeks, have resulted in disease certified for inclusion in the registry of cases of
beryllium disease established at the Massachusetts General Hospital (Hall et al., 1959).
Silica exposures are generally considered important only for chronic disease production. However, the condition of acute silicosis is caused by relatively short-term, high-intensity exposures to very fine silica particulate (Jones et al., 1975). Exposures as brief as six months have been associated with acute silicosis. Yet even in the absence of such severe overexposures and acute clinical disease, there is evidence that low-level exposures, not associated with clinical symptoms or chest X-ray abnormality, can result in irreversible pathology (Craighead and Vallyathan, 1980).
Similarly, asbestos exposures are noted for causing chronic respiratory illness, as well as cancer. Brief high exposures are not recognized to cause respiratory complaints. However, relatively short-term exposures of less than four years have been associated with increased respiratory symptoms and decreased vital capacity (Rodriques-Roisin et al., 1986).
It should be noted that beryllium, asbestos, and silica are relatively insoluble particles that remain in the lungs for months to years following inhalation. Thus even a brief exposure results in a chronic exposure of lung tissue to the agent.
Based on this review, a set of answers has been suggested for the following key questions regarding sulfur mustard and Lewisite exposure and chronic nonmalignant pulmonary disease. However, it should be kept in mind that there is a striking absence of knowledge about the early stages of environmentally related pulmonary diseases and almost no knowledge on the natural (longitudinal) evolution of the clinical conditions. Thus, there is little to guide us towards the appropriate disease model or towards identification of the relevant pattern(s) of exposure for disease etiology.
Does the occurrence of an acute pulmonary reaction following exposure to toxic chemicals identify an individual at risk for long-term respiratory sequelae? Ample evidence has been provided for all of the agents reviewed that a significant portion of individuals who react acutely to short, high exposures (and even some to short, relatively low exposures) go on to develop a variety of long-term respiratory effects. The agents differ in the probability of long-term adverse outcomes, but none appear to be free of this risk. The literature reviewed does not allow identification of a minimum magnitude of acute response necessary in order for there to be long-term sequelae.
If acute pulmonary reactions can identify individuals at risk for long-term sequelae of chemical exposures, can the probability or degree of damage be predicted from the magnitude of the acute
response? This question has not been adequately studied. An association with dose is found for acute as well as chronic responses, which provides support for the association, but not for a relationship between the magnitude of the acute response and the magnitude of the chronic response. If the disease model invoked requires the acute exposure to cause acute irreversible damage, then one might reasonably expect the magnitude of acute response to predict the magnitude of the chronic response. However, if another disease model is invoked, one in which the acute exposure results in or leads to an alteration in individual risk factors, then it is quite likely that the magnitude of the acute and chronic responses would be unrelated.
What assurance is there that the absence of an acute pulmonary reaction identifies chemically exposed individuals who will not develop long-term sequelae? This may be the most important question to ask and, unfortunately, the one for which no direct evidence could be found. The indirect evidence, however, would suggest the need to invoke an unusual disease model, one in which changes in individual risk factors could be excluded from the list of possible mechanisms, so that the absence of an acute reaction would eliminate the possibility of any chronic effects related to a short-term or acute exposure.
SUMMARY
Gaps
There are few directly relevant data for evaluating the risk of chronic nonmalignant respiratory disease associated with the specific exposure conditions present in the WWII chamber and field studies. The range of exposure concentrations that were actually inhaled by the subjects can be only crudely estimated, but they may have reached the levels experienced by those exposed in combat or production facilities. Without precise knowledge about the exposures, the only way to estimate the true risk would be to identify the cohort of test subjects and follow them for the occurrence of respiratory morbidity. To date, the entire cohort of subjects has not been identified, nor has any subset of them been followed for long-term health effects. The absence of a follow-up study of the experimental subjects from the WWII testing programs is the single largest gap in the literature relevant to the assessment of chronic nonmalignant respiratory disease risk in individuals experiencing short-term exposures to sulfur mustard or Lewisite.
Conclusions
The evidence indicates a causal relation between exposure to sufficient concentrations of sulfur mustard (and presumably nitrogen mustard and Lewisite) and chronic nonreversible respiratory effects in humans. It is well known that pulmonary injury is the principal cause of mortality in the first few days to weeks after intense exposure to sulfur mustard. In addition, the evidence is consistent with a causal relationship between occupational exposure to these agents and chronic obstructive lung diseases, including chronic bronchitis, asthma, and pneumonia. Finally, evidence from studies of combat survivors of gas attacks is consistent with a causal relationship between acute overexposure and bronchitis and emphysema. Further, given the likely exposure levels outlined in Chapter 3, the evidence is consistent with a causal relation between the concentrations of sulfur mustard (and Lewisite) used in the WWII experiments and chronic nonreversible lung diseases.
Indirect evidence, based on a review of the relationships between acute and chronic effects caused by other substances, suggests that the likelihood of long-term respiratory effects may not necessarily be linked to the presence of an acute respiratory response. Review of the evidence does not support a minimum magnitude of acute response necessary in order for there to be long-term sequelae. Further, if the disease model requires the acute exposure to cause acute irreversible damage, then the magnitude of acute response might well predict the magnitude of the chronic response. However, if acute exposure led to an alteration in individual risk factors, then it is possible that the magnitude of the acute and chronic responses would be unrelated. Finally, indirect evidence suggests that only an unusual disease model would exclude the possible mechanism of change in individual risk factors so that the absence of an acute reaction would eliminate the possibility of a chronic effect related to an acute exposure. Thus, there is insufficient evidence to conclude that long-term respiratory responses occur only in cases where an earlier acute response has been documented.
References
Agency for Toxic Substances and Disease Registry (ATSDR). 1991. Draft, Toxicological Profile for Mustard "Gas." U.S. Department of Health and Human Services.
AMA Archives of Industrial Health. 1959. Beryllium disease and its control. Conference held at Massachusetts Institute of Technology, Sept. 30-Oct. 1, 1958. AMA Archives of Industrial Health 19.
Axford AT, McKerrow CB, Jones AP, Le Quesne PM. 1976. Accidental exposure to isocyanate fumes in a group of firemen. British Journal of Industrial Medicine 33:65-71.
Back KC, Thomas AA, MacEwen JD. 1972. Reclassification of material listed as transportation
health hazards.Office of Hazardous Materials of the Assistant Secretary for Safety and Consumer Affairs, Department of Transportation. TSA-2072-3. PB-214 270/1.
Becklake MR, Bourbeau J, Menzies R, Ernst P. 1988. The relationship between acute and chronic airway responses to occupational exposure. In: Current Pulmonology. Chicago: Year Book Medical Publishers.
Berghoff RS. 1919. The more common gases: their effect on the respiratory tract. Observation on two thousand cases. Archives of Internal Medicine 24:678-684.
Boursnell JC, Francis GE, Wormall A. 1946. Studies on mustard gas (ß,ß-dichlorodiethylsulphide) and some related compounds. 6. The fate of injected ß,ß-dichlordiethylsulphone and b,b-dichlorodiethylsulphoxide (containing radioactive sulphur) in the animal body. Biochemical Journal 40:765-768.
Brooks SM, Weiss MA, Bernstein IL. 1985. Reactive airways dysfunction syndrome (RADS). Chest 88:376-384.
Brophy LP, Fisher G. 1959. The Chemical Warfare Service: Organizing for War. United States Army in World War II: The Technical Services. Washington, DC: Office of the Chief of Military History, Department of the Army.
Case RM, Lea AJ. 1955. Mustard gas poisoning, chronic bronchitis, and lung cancer: an investigation into the possibility that poisoning by mustard gas in the 1914-1918 war might be a factor in the production of neoplasia. British Journal of Preventive and Social Medicine 9:62-72.
Castellan RM, Olenchock SA, Kinsley KB, Hankinson JL. 1987. Inhaled endotoxin and decreased spirometric values. New England Journal of Medicine 317:605-610.
Cochrane RC. [1946]. Medical research in chemical warfare. Available through the U.S. Army Chemical Defense Research, Development and Engineering Center, Aberdeen Proving Ground, MD.
Craighead JE, Vallyathan NV. 1980. Cryptic pulmonary lesions in workers occupationally exposed to dust containing silica. Journal of the American Medical Association 244:1939-1941.
Dahl AR. 1990. Contemporary issues in toxicology. Toxicology and Applied Pharmacology 103:185-197.
Dahl AR, Schlesinger RB, Heck HD, Medinsky MA, Lucier GW. 1991. Comparative dosimetry of inhaled materials: differences among animal species and extrapolation to man. Fundamental and Applied Toxicology 16:1-13.
Easton D, Peto J, Doll R. 1988. Cancers of the respiratory tract in mustard gas workers. British Journal of Industrial Medicine 45:652-659.
Ganas P. 1969. New developments in chemical and biological warfare. Forces Aeriennes Francaises 24:449-475.
Gilchrist HL, Matz PB. 1933. The Residual Effects of Warfare Gases. Washington, DC: U.S. Government Printing Office.
Greene SA, Wolff RK, Hahn FF, Henderson RF, Mauderly JL, Lundgren DL. 1984. Sulfur dioxide induced chronic bronchitis in beagle dogs. Journal of Toxicology and Environmental Health 13:945-958
Haber L. 1986. The Poisonous Cloud. Oxford: Clarendon Press. 250-257 . Hall TC, Wood CH, Stoeckle JD, Tepper LB. 1959. Case data from the beryllium registry. AMA Archives of Industrial Health 19:100-103.
Hankins JL, Klotz WC. 1922. Permanent pulmonary effects of gas in warfare . American Review of Tuberculosis 6:571-574.
Haskonen H, Nordman H, Korhonen O. 1979. Long-term effects of exposure to sulfur dioxide: lung function four years after a pyrite dust explosion. American Review of Respiratory Diseases 119:555-560.
Hosseini K, Moradi A, Mansouri A, Vessal K. 1989. Pulmonary manifestations of mustard gas injury: a review of 61 cases. Iranian Journal of Medical Sciences 14:20-26.
Inada S, Hiragun K, Seo K, Yamura T. 1978. Multiple Bowen's disease observed in former workers of a poison gas factory in Japan with special reference to mustard gas exposure. Journal of Dermatology 5:49-60.
Jones RN, Weill H, Ziskind M. 1975. Pulmonary function in sandblasters' silicosis. Bulletin de Physio-Pathologie Respiratoire 11:589-595.
Jones RN, Hughes JM, Glindmeyer H, Weill H. 1986. Lung function after acute chlorine exposure. American Review of Respiratory Disease 134:1190-1195.
Keshmiri M. 1989. Pulmonary cause of death from chemical warfare agents: the Halabche experience. Iranian Journal of Medical Sciences 14:10-19.
Lippman M, ed. 1992. Environmental Toxicants, Human Exposures and Their Health Effects. New York: Van Nostrand Reinhold.
Manning KP, Skegg DCG, Stell PM, Doll R. 1981. Cancer of the larynx and other occupational hazards of mustard gas workers. Clinical Otolaryngology and Allied Sciences 6:165-170.
Martin CVF, Higgins JE. 1976. Byssinosis and other respiratory ailments. Journal of Occupational Medicine 16:455-462.
Menzel DB, Amdur MO. 1986. Toxicology responses of the respiratory system. In: Klaassen CD, Amdur MO, Doull J, eds. Casarett and Doull's Toxicology. 3rd ed. New York: Macmillan.
Morgenstern P, Koss FR, Alexander WW. 1947. Residual mustard gas bronchitis: effects of prolonged exposure to low concentrations of mustard gas. Annals of Internal Medicine 26:27-40.
Muggia FM. 1983. Pulmonary toxicity of anti-tumor agents. Cancer Treatment Reviews 10:221-243.
National Research Council. 1979. Airborne Particles. Baltimore: University Park Press.
Nishimoto Y, Burrows B, Miyanishi M, Katsuta S, Shigenobu T, Kettel LJ. 1970. Chronic obstructive lung disease in Japanese poison gas workers. American Review of Respiratory Disease 102:173-179.
Office of Scientific Research and Development. National Defense Research Committee. 1946. Summary Technical Report of Division 9, NDRC. Chemical Warfare Agents and Related Chemical Problems. Parts I-VI. Washington, DC: NDRC. AD-234 249.
Papirmeister B, Feister AJ, Robinson SI, Ford RD. 1991. Medical Defense Against Mustard Gas: Toxic Mechanisms and Pharmacological Implications. Boca Raton, FL: CRC Press.
Peters JM, Wegman DH. 1975. Epidemiology of toluene diisocyanate (TDI) induced respiratory disease. Environmental Health Perspectives 11:97-100.
Peters JM, Murphy RLH, Pagnotto LD, Van Ganse WF. 1968. Acute respiratory effects in workers exposed to low levels of toluene diisocyanate (TDI). Archives of Environmental Health 16:642-647.
Phalen RF, Prasad SB. 1988. Morphology of the respiratory tract. In: McClellan RO, Henderson RF, eds. Concepts in Inhalation Toxicology. New York: Hemisphere.
Project Coordination Staff, Chemical Warfare Service. 1946. Technical Aspects of Chemical Warfare in the Field. 2 vols. Washington, DC: Chemical Warfare Service.
Robinson JP. 1967. Chemical warfare. Science Journal 4:33-40.
Rodriques-Roisin R, Picado C, Roca J, Arrigo S, Agusti-Vidal A. 1986. Early lung function changes after short heavy exposure to chrysotile asbestos in non-smoking women. Bulletin Europeen de Physiopathologie Respiratoire 22:225-229.
Rosenow EC, Wilson WR, Cockerill FR. 1985. Pulmonary disease in the immunocompromised host . Mayo Clinic Proceedings 60:473-487.
Sandall TE. 1922. The later effects of gas poisoning. Lancet 2:857-859.
Sidell FR. 1990. Clinical Notes on Chemical Casualty Care. USAMRICD Technical Memorandum 90-1. Aberdeen Proving Ground, MD: U.S. Army Medical Research Institute of Chemical Defense.
Smith G, Walker J. 1990. The histopathology of pulmonary reactions to drugs. Clinics in Chest Medicine 11:95-117.
Somani SM, Babu SR. 1989. Toxicodynamics of sulfur mustard. International Journal of Clinical Pharmacology, Therapy and Toxicology. 27:419-435.
Stedman's Medical Dictionary. 1976. 23rd ed. Baltimore: Williams & Wilkins.
Stepanov AA, Popov VN. 1962. [Chemical Weapons and Principles of Antichemical Defense]. Translated by Joint Publications Research Service. JPRS 15107. Washington, DC: JPRS.
Urbanetti JS. 1988. Battlefield chemical injury. In: Loke J, ed. Pathophysiology and Treatment of Inhalation Injuries. New York: Marcel Dekker. 281-348.
U.S. Army. 1974. Chemical agent data sheets, Vol. 1. Technical Report EO-SR-74001. Edgewood Arsenal, Maryland.
U.S. Army Chemical Research, Development, and Engineering Center (CRDEC). 1990. HD and THD. Material Safety Data Sheet. HCSDS No. 20058A. Aberdeen Proving Ground, MD: U.S. Army Chemical Research, Development and Engineering Center.
U.S. Army and U.S. Air Force. 1975. Military chemistry and chemical compounds. Field Manual No. FM3-9, Regulation No. AFR 355-7.
Wada S, Nishimoto Y, Miyanishi M, Katsuta S, Nishiki M. 1962. Review of Okuno-jima poison gas factory regarding occupational environment. Hiroshima Journal of Medical Sciences 11:75-80.
Warthin AS, Weller CV. 1919. The lesions of the respiratory and gastrointestinal tract produced by mustard gas (dichlorethyl sulphide). Journal of Laboratory and Clinical Medicine 4:229-264.
Weiss RB, Muggia FM. 1980. Cytotoxic drug-induced pulmonary disease: update 1980. American Journal of medicinae 68:259-266.
Willems JL. 1989. Clinical management of mustard gas casualties. Annales Medicine Militaris Belgicae 3:S1-61.
Winternitz MC. 1919. Anatomical changes in the respiratory tract initiated by irritating gases. Military Surgeon 44:476-493.
World Health Organization (WHO). 1970. Health Aspects of Chemical and Biological Weapons: Report of a WHO Group of Consultants. Geneva: WHO.



















