8
Ocular Effects of Mustard Agents and Lewisite
The external eye is uniquely vulnerable to injury by mustard compounds and Lewisite. Over 90 percent of patients exposed to sulfur mustard in World War I (WWI) sustained injury to the conjunctiva; about 10 percent of these injuries were severe, involving the cornea as well. Animal studies suggest that these acute injuries can be followed by recurrent or delayed symptoms, including ulceration, inflammation, and corneal erosion. Many WWI veterans in fact developed such symptoms some 8 to 25 years after their initial injuries. As with pulmonary injuries (Chapter 7), however, there have been no long-term studies of the ocular status of World War II human subjects.
PHYSIOLOGY AND ANATOMY OF THE EYE
The housing of the eye is a fibrous envelope composed of clear cornea over the front one-sixth and opaque sclera surrounding the rest (Figure 8-1). The sclera is covered by the conjunctiva, a transparent mucous membrane that also covers the inner surface of the eyelids. Both the cornea and the conjunctiva are covered with squamous epithelium, six to seven and three to four layers thick, respectively. A three-layered tear film (lipid, aqueous, and mucoprotein) bathes the surface cells constantly, providing the eye with lubrication and protection. The lids also close to protect the eye, and in doing so they periodically replenish the tear film lost from evaporation and lacrimal drainage.
The cornea itself is a layered structure. Underlying the corneal epithelium is a specialized region of collagen tissue. The rest of the corneal collagen is organized into lamellae, or layers, that are very
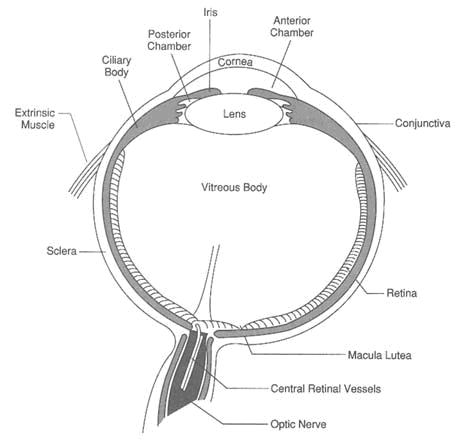
FIGURE 8-1 Anatomy of the eye.
regularly oriented and contribute significantly to corneal clarity. The inner surface of the cornea is lined with a single layer of endothelium, a metabolically active cellular layer that pumps electrolytes, water, and metabolites out of the cornea. The corneal epithelium is derived from a specific group of stem cells, encircling the cornea, that multiply and ultimately form mature corneal cells. A different population of stem cells, in the conjunctival fornices, give rise to the conjunctival epithelium.
Corneal nutrition is supplied almost exclusively by the aqueous humor circulating behind the cornea in the front of the eye. This allows the cornea to obtain its nutrition in the absence of blood vessels, an obvious aid to clarity. When blood vessels do enter the cornea (in disease or injury), scarring occurs, with a loss of transparency and consequently loss of vision.
ACUTE EFFECTS AND BIOLOGICAL MECHANISMS
Dose-Related Considerations
Because of the constant presence of a tear film over its surface and mucous membranes, the eye is more sensitive to sulfur mustard than any other organ of the body. The fact that fluid is present in the eye at all times probably accounts for the fact that varying conditions of humidity do not influence the degree of injury as compared, for example, to skin. Table 8-1 summarizes dose-related effects of sulfur mustard on eyes at 16°C-7°C. The degree of visual loss depends on the concentration and exposure time to sulfur mustard. Concentrations of less than 50 to 100 mg·min/m3 cause simple conjunctivitis (inflammation of the conjunctiva) that, at most, can disable an individual for one to two weeks (Papirmeister et al., 1991). When doses exceed 200 mg·min/m3, however, corneal edema or swelling occurs. At even higher doses, severe corneal damage takes place, with significant loss of vision (Papirmeister et al., 1991).
Ocular injury with sulfur mustard liquid increases the risk of perforation of the cornea and thus is far more damaging to the cornea than vapor-induced injury. Some permanent loss of vision is also more likely as the severity of such exposure is increased.
The time between injury and the appearance of clinical symptoms varies, depending on the severity and duration of exposure. The less severe the injury, the longer is this latency period. With conjunctival injury alone, the latent period is 4 to 12 hours. After more severe exposures in which the cornea is damaged, this latent period may be decreased to as little as 1 to 3 hours. The latency period after liquid sulfur mustard injury is less than 1 hour (Papirmeister et al., 1991).
The exquisite sensitivity of the eye, compared to respiratory tract and skin, to sulfur mustard is evident in the data previously presented in Table 3-4. Symptoms appear in the eye before most other tissues. As the concentration of sulfur mustard increases, however, the injury to the eye parallels that of the respiratory tract. Unlike sulfur mustard, Lewisite exposure causes immediate pain and blepharospasm (spasm of eyelid muscle), especially when the agent is aerosolized (Adler and Leopold, 1945). Eye morbidity from liquid and vapor Lewisite is summarized in detail in Table 8-2.
Clinical Observations
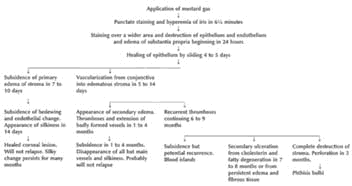
The acute clinical course of severe sulfur mustard injuries of the eye has been well described in the rabbit (Figure 8-2). Hughes (1942) described five stages following severe damage to the cornea in rabbit and man:
TABLE 8-1 Effects of Acute Sulfur Mustard Exposure on the Human Eye at (16°C-27°C unless otherwise noted)
|
Estimated Exposure |
Effects |
Latency |
Reference |
|
Vapor (Ct of mg·min/m3) 2 (=32ºC) |
Threshold for conjunctivitis and reddening; nondisabling; Not available maximum safe Ct for eyes |
Not available |
McNamara et al., 1975; U.S. Army CRDEC, 1990 |
|
=12 |
Threshold for conjunctivitis and reddening; nondisabling |
Several hours to several days |
McNamara et al., 1975; Project Coordination Staff, 1946 |
|
12 |
Marginal effects |
Not available |
U.S. Army, 1974 |
|
30 (60 min) |
Conjunctivitis |
Not available |
Reed, 1920 |
|
50-100 |
Conjunctivitis, sensation of grittiness under eyelids, tearing, light sensitivity; nondisabling; healing of injury 2-7 days (14 days if severe) |
4-12 hours |
Gates and Moore, 1946; McNamara et al., 1975; Project Coordination Staff, 1946 |
|
70 |
Reddening, no incapacitation |
Not available |
U.S. Army, 1974 |
|
90 |
Reddening, mild incapacitation |
Not available |
U.S. Army, 1974 |
|
200 |
Median incapacitating Ct (ICt50); corneal edema and clouding; eyelid edema, photophobia, severe blepharospasm (temporary blindness); healing of injury over several weeks; some hypersensitivity for months |
3-12 hours |
Project Coordination Staff, 1946; Urbanetti, 1988; U.S. Army, 1974; U.S. Army and U.S. Air Force, 1975 |
|
400-800 |
Corneal damage with possible ulceration and secondary infection; incapacitating; eye damage may be permanent; possible prolonged hospitalization (several months) |
1-4 hours |
Karnofsky and Nolen, 1944 |
|
>800 |
Severe corneal damage with possible permanent loss of vision; possible systemic effects; incapacitating; possible prolonged hospitalization |
1-3 hours |
Papirmeister et al., 1991; Stepanov and Popov, 1962 |
|
Liquid |
|||
|
Unknown (droplets or liquid splash) |
Severe pain; edema; corneal damage; possible corneal perforation; incapacitating, possible permanent eye damage or loss (rare); hospitalization required |
<1 hour |
Maumenee and Scholz, 1948; Papirmeister et al., 1991 |
|
SOURCE: Adapted from Papirmeister et al., 1991; Watson and Griffin, 1992. |
|||
TABLE 8-2 Effects of Acute Lewisite Exposure on the Mammalian Eye
|
Estimated Exposure |
Species |
Effects |
Exposure time (min) |
References |
|
Vapor (mg/m3) |
||||
|
0.8 |
Man |
No irritation (estimate) |
Not reported |
A.D. Little, 1986 |
|
1.0 |
Rabbit |
Permanent lesions (minimum effective dose) |
30 |
Gates et al., 1946 |
|
1.0 |
Man |
Lesions |
30 |
U.S. Army, 1974 |
|
1.5 |
Man |
Severe (estimate) |
Not reported |
Gates et al., 1946 |
|
2 |
Man |
Threshold of irritation |
Not reported |
A.D. Little, 1986 |
|
10 |
Man |
Inflammation |
15 |
Ottinger, 1973 |
|
10-30 |
Man |
Irritation |
1 |
A.D. Little, 1986 |
|
20 |
Dog |
Permanent lesions (minimum effective dose) |
30 |
Gates et al., 1946 |
|
Saturated |
Rabbit |
Perforation |
22.5 |
Hughes, 1942 |
|
Vapor (mg·min/m3) |
||||
|
<300 |
Man |
Median incapacitating Ct (ICt50) |
Not reported |
U.S. Army CRDEC, 1990 |
|
Liquid (mg) |
||||
|
0.005 |
Rabbit |
Mild |
Not reported |
Wallen et al., 1943 |
|
0.01-0.02 |
Rabbit |
Permanent damage |
Not reported |
Wallen et al., 1943 |
|
0.1 |
Rabbit |
75% perforated |
Not reported |
Wallen et al., 1943 |
|
0.1 |
Man |
Severe (estimated) |
Not reported |
Gates et al., 1946 |
|
12 |
Rabbit |
Destruction |
Not reported |
Irwin, 1954 |
|
SOURCE: Adapted from Solana, unpublished. |
||||
-
Immediate damage to the corneal epithelium, with edematous clouding and necrosis of the stroma.
-
After five hours, dense infiltration of polymorphonuclear neutrophils at the sclerocorneal junction, extending into the corneal stroma.
-
Clinical improvement of the opacity after five to seven days, with diminished edema of the stroma in less severe injuries.
-
Progressive vascularization of the cornea extending in from the limbal vessels. This process may continue for several weeks.
-
Persistent ulceration of the cornea for weeks or recurrent ulceration after a latent period of years.
Over 90 percent of patients exposed to sulfur mustard in World War I sustained conjunctival injury. Corneal changes were apparent in a much smaller group and were likely due to vapor, as opposed to liquid, exposure. All those exposed, however, had photophobia and blepharospasm. Hughes (1945b) divides these patients into three categories:
-
Class I: about 75 percent had mild symptoms without corneal involvement.
-
Class II: about 15 percent were moderately affected, the corneal
-
epithelium was mildly injured, but would return to normal in one or two days.
-
Class III: about 10 percent had severely affected eyes, both the cornea and the conjunctiva being involved. Class III was subdivided into IIIa (mild corneal changes with a prognosis of return to active duty in six weeks to three months) and IIIb (severe corneal changes resulted in disability of more than three months). It is from members of the latter 10 percent of Class III that ''delayed keratitis" developed 8 to 25 years later (see below).
Experience with Lewisite eye injuries is much less extensive. However, Lewisite can produce some changes similar to those of sulfur mustard (Goldman and Dacre, 1989; Mann et al., 1946; also see Table 8-3). Although severe visual loss occurs with Lewisite exposure, no long-term ocular effects were reported by Mann and colleagues (1946). However, animals in the Mann study were only followed for 30 days following exposure.
Physiology and Histopathology of Injury
The corneal epithelium continues to appear viable and respond in a normal manner for hours after exposure to sulfur mustard, even if the epithelium is separated from the underlying layers of the cornea. However, even very low doses of sulfur and nitrogen mustard cause cessation of mitotic activity in the corneal epithelium. Exposed cells in mitosis complete their cell division normally. If exposed to the poison before the onset of mitosis, however, the mitosis is either greatly prolonged or completely suppressed (Friedenwald, 1945). This is consistent with the effects of these agents on all rapidly proliferating cells.
Mann and Pirie (as cited in Friedenwald, 1945) found that corneal collagen reacts with sulfur mustard and, in the presence of an excess of sulfur mustard, more molecules of sulfur mustard are bound by the protein than the number of sulfhydryl groups present in the material before exposure. Further they reported that collagen was abnormally resistant to attack by pepsin after reacting with the agent. This suggests that a specific physical or chemical reaction occurred between the collagen and the sulfur mustard, namely, a denaturation of collagen, potentially making it more vulnerable to degradative enzymes.
The histological changes taking place after sulfur mustard injury of the eye have been summarized by Scholz (1945). Thirty to 60 minutes after exposure, the first change noted was edema of the basal epithelial cells of the cornea. At one to two hours, the basal nuclei relocated toward the central portion of the cell. Between two and 12 hours, the goblet cells had lost their mucus and were sloughed off, followed shortly
TABLE 8-3 Characteristics of Sulfur Mustard and Lewisite Ocular Lesions
|
Types |
Sulfur Mustard |
Lewisite |
|
Onset of ocular action |
No initial reaction; symptoms do not appear for some hours. |
Immediate and painful reaction. |
|
Pupillary reaction |
Not affected. |
Immediate strong miotic action. |
|
Vascularization |
Never occurs unless limbus is damaged. |
Independent of the site of the primary lesion; occurs when a sufficient dose reaches the cornea or limbus. |
|
Vascular lesions |
Do not all perforate; tend to be chronic, to relapse, and to show intracorneal hemorrhages from newly formed vessels; vessels have peculiar and characteristic form. |
Not all vascular lesions perforate; there are no relapses and no recurrent hemorrhages. |
|
Cholesterin and other lipoid scars |
Follow some vascular lesions, and subsequently these tend to break down (delayed mustard gas keratitis). |
Do not occur, and there is no late breakdown due to them. |
|
Perforation and loss of an eye |
Caused by relatively large doses (0.005 cc), and even then are long delayed. Perforation never occurs as a primary lesion before the stage of vascularization. |
Caused by relatively small doses (0.001 cc); perforation may occur within a few days without vascularization, or later after the entry of blood vessels. |
|
Edema |
Edema of the conjunctiva and cornea is present, but not excessive. |
Edema of the lids and conjunctiva is immediate and severe. Edema of the cornea is extreme in all but the smallest doses. |
|
Iris and ciliary body |
Relatively little involvement. No late effect on pigment. |
Early and severe involvement, followed by gradual depigmentation and shrinkage of the iris stroma. |
|
Vessel formation |
Characteristic vessels form in cornea and conjunctiva. |
Corneal vessels do not show the characteristic varicosities of mustard vessels. |
|
SOURCE: Adapted from Mann et al., 1946. |
||
by loss of the conjunctival and corneal epithelial cells. Edema of the stroma developed as a consequence of endothelial cell damage and loss. From 12 to 24 hours after exposure, the conjunctiva was edematous, the endothelium of the blood vessels was lost, and an infiltrate accumulated, composed primarily of neutrophils.
The conjunctival epithelium began to regenerate two days after injury. If the corneal and limbal epithelium had been lost, conjunctival epithelium was observed to cross the limbus to resurface the cornea.
Conjunctival epithelium thickened in one to two weeks postinjury, but the corneal epithelial layer remained very thin, often with "skip" areas referred to as defects. When such defects were long-lasting, necrotic ulcers, with or without bacterial infection, often supervened. Depending on the severity of the original injury, a scarring, or "hazing," of the corneal stroma was noted.
Lewisite injuries cause necrosis of the deep corneal layers with loss of nuclei of all keratocytes and loss of normal staining characteristics in collagen fibers (Adler et al., 1947). Neutrophils invade the stroma at 24 hours but are replaced by round, chronic inflammatory cells at the end of 10 days. Corneal vascularization is not visible until 5 days after the injury, becoming intense at 14 days. Topical British Anti-Lewisite treatment diminished the severity of these injuries only if given within two to five minutes of injury (Hughes, 1946).
EVIDENCE OF LONG-TERM HEALTH EFFECTS
Animal Data and Cellular Bioassay
Long-term studies of the effect of sulfur mustard were conducted by Mann and Pullinger (1944). Over a period of 18 months they intermittently examined 138 rabbits injured by sulfur mustard (Figure 8-2). Based on the lifetime of a rabbit as one-tenth that of man, an observation period of 18 months would be sufficient time to develop delayed keratitis in this experimental animal. The results showed that, similar to the human condition, migration of fatty or cholesterin deposits to the surface of the eye could occur after 7 to 8 months and cause recurrent secondary ulceration. In these models of severe burns, it can be concluded that delayed and recurrent keratitis is demonstrable and reproducible.
Comparison of sulfur mustard injuries to those sustained with Lewisite is summarized in Table 8-3. A summary of the toxicology of Lewisite liquid and vapor is separately tabulated in Table 8-2. Many of the rabbits in the Lewisite study were watched for more than one year; no secondary lipoid degeneration or cholesterin deposition was noted, nor any long-term effect, in particular (Mann et al., 1946).
Human Studies
Occupational Exposure
A large number of injuries occurred in the production of sulfur mustard. A summary of the toxic accidents in all three mustard gas production factories in England showed that 10.4 percent of 939 eye
casualties showed improvement of the cornea, and only 1 percent had severe Class IIIb corneal lesions (Hughes, 1945a). A report of 1,097 patients treated at Edgewood Arsenal during the 17 months preceding March 1, 1943, showed that 91 percent of the injuries were due to mustard agent vapor, and of that number 78 percent had eye burns (Uhde, 1946). Eighty of these patients were exposed to a sudden break in the shell filling line, which released large quantities of mustard agent vapor. The remaining 93 percent were exposed to slow leaks that were not detected by smell. Unfortunately, there have been no long-term studies of these patients to determine their ocular status many years after exposure.
Battlefield Exposure
The British reported many thousands of eye casualties during World War I. Sulfur mustard was responsible for 77 percent of all gas injuries in WWI; of these, 75 percent were relatively mild conjunctival irritations, forcing hospital care for an average of two weeks before return to active duty (Gilchrist and Matz, 1933; Hughes, 1942). Another 15 percent were described as intermediate, with incapacitation for four to six weeks. Finally, 10 percent were severe, requiring hospitalization or rehabilitation for a four- to six-month period before stabilizing (Hughes, 1942). A total of 51 British soldiers were reported as blinded, and there were 180 vision-related pensions (Phillips, 1940). Phillips (as cited in Hughes, 1945a) also reported 80 patients with late recurrent ulceration of the cornea following exposure to sulfur mustard in WWI. He stated that there were a total of 300 reported cases of delayed keratitis as of 1939.
Two French reports describe only a handful of ocular lesions. Teulieres (as cited in Hughes, 1942) reported on 1,500 mustard gas casualties, of which only 23 patients sustained ocular lesions severe enough to necessitate observation. Of these, 3 patients showed ulceration of the cornea and 1 developed inflammation of the entire eye (panophthalmitis). In a parallel report of 1,800 sulfur mustard casualties, Beauvieux (1920) found only 2 patients in whom severe corneal ulceration developed; both cases ultimately recovered useful vision. Beauvieux also examined the retinal blood vessels and condition of the retina in 120 cases of severe generalized sulfur mustard lesions and noted venous dilatations in 34 percent and hyperemia of the optic disk in 23 percent.
If all of these reports are combined, up to 90 percent of casualties would be expected to have ocular involvement, with symptoms peaking 6 to 12 hours after exposure. However, 90 percent of these cases would have no significant corneal involvement. Common symptoms included gritty sensation, conjunctivitis, chemosis (edema of the conjunctiva
causing swelling around rim of cornea), lid edema, blepharospasm, photophobia, blurred vision, and tearing. The 10 percent of patients with corneal involvement exhibited corneal edema, keratitis, ocular pain, temporary blindness, tissue necrosis, iridocyclitis (inflammation of iris and ciliary body), glaucoma, vascularization, and, rarely, ulceration or perforation of the eye.
Anatomical investigations by Ashoff and colleagues, cited in Oswald (1920), have shown that sulfur mustard poisoning probably causes blood clots in the precapillary arterioles of the eye. This might explain a report of progressive narrowing of the retinal blood vessels in a 34-year-old man who had sustained a relatively mild exposure to sulfur mustard in 1917 that nevertheless resulted in bilateral blindness (Oswald, 1920).
Chronic Course
Many patients continue to have recurrent corneal erosions and inflammatory keratitis for an indefinite number of years after the serious corneal injury. Approximately 243 cases of late recurrent ulceration of the cornea have been reported following severe sulfur mustard burns in WWI (Scholz and Woods, 1945).
In the acute stage the limbal region frequently presents a marbled appearance in which porcelain-like areas of ischemia (decreased or blocked blood flow) are surrounded by blood vessels of irregular diameter. Later, the vascularized scars of the cornea often contain deposits of cholesterin, calcium, and fat. There were reports of a sudden increase in these symptoms and findings some 8 to 25 years after the initial injury. This information first appeared in the U.S. literature in a 1947 article by Scholz and Woods, but many such cases had already been reported in the British, French, and German literature (Genet, 1925; Heckford, 1937; Moore and Heckford, 1929; Proceedings of the Royal Society of Medicine, 1940; Rohrschneider, 1937; Sourdille, 1936; Weill, 1939).
Phillips, who collected 70 cases, called attention to the delayed keratitis due to sulfur mustard exposure (Proceedings of the Royal Society of Medicine, 1940). He noted that, after the initial early and intermediate hospitalization from 4 to 6 months, these patients were often symptom free for 10 to 13 years, whereupon delayed keratitis developed, characterized by photophobia, lacrimation, and failing vision. Superficial ulcerations also occurred in these patients, and the sensitivity of the cornea to touch and other stimuli was reduced. Marbling of the cornea appeared in the acute stage of these cases along with additional linear marks referred to as "skate marks on fresh ice." Also found were pale triangular patches on either side of the cornea,
indicating an absence of small conjunctival and episcleral blood vessels that left large areas of the sclera bare. In each of these cases there was a history of a severe corneal and perilimbal burn that involved an extensive amount of the perilimbal conjunctiva. This corresponds to Class III injuries in which there is (a) damage to the limbal blood supply, associated with moderate corneal edema, superficial collections of inflammatory cells, with or without superficial corneal vascularization; or (b) ischemic necrosis of the limbal regions, marked and persistent corneal edema, deep corneal inflammatory cells, and deep blood vessel ingrowth into the cornea (vascularization).
The problem of delayed keratitis was neither trivial nor infrequent in the severe injuries. Mann's studies of 84 cases in 1944 showed that an inflammatory keratitis (inflammation of the cornea) developed intermittently in the most severely injured veterans for a period of 17 years after initial exposure (Mann, 1944); however, during the next 7- to 8-year period, a sudden substantial increase in these numbers was observed.
The use of Lewisite as a wartime gas was much less common. A combination of sulfur mustard and Lewisite was reported to have been used in the Japanese attack on Ichang in 1941 (SIPRI, 1971). No medical reports are available to document the short- or long-term effects to the health of survivors. No large-scale reports of pure Lewisite eye injury to humans are noted in the literature.
Medical Therapeutic Exposure
Sulfur mustard has not been used to treat eye disease. However, other alkylating agents, such as cyclophosphamide and chlorambucil, have been shown to be effective in arresting a number of eye diseases, including peripheral ulcerative keratitis, Mooren's corneal ulcer, some ulcerative and nonulcerative scleral diseases, and recalcitrant uveitis (inflammation of the iris, ciliary body, and choroid). Each of these diseases is regarded as, or has been proven to be, an autoimmune process. There are no reports of secondary cancers developing as a consequence of immunosuppression from treatment of eye disease.
SUMMARY
Gaps in Knowledge
Limbal Vascular Damage
The whitened appearance of perilimbal ocular tissues after sulfur mustard injury suggested to early investigators that destruction of the limbal vasculature resulted in the disastrous effects on the cornea and
the late development of recurrent keratitis. This hypothesis was based on the presumption that the cornea derived its entire nutritional supply from these vessels. Since then it has been discovered that corneal nutrition is principally derived from the aqueous humor and probably receives only a small facultative supply from perilimbal vessels. It is unknown whether sulfur mustard can damage blood vessels in the ciliary body—the only way that nutrition of the cornea could be influenced.
Ocular Epithelial Damage
The most trying and difficult problems associated with mustard gas injuries are the corneal complications that can occur in the early, intermediate, but especially the late phases after exposure. Recent research suggests that the loss of ocular epithelium is a key factor in persistent epithelial defects of the cornea, giving rise to new disease entities called "ocular surface disease" and "stem cell disease." Even when the cornea itself has not been damaged, loss of stem cells can result in persistent epithelial defects that will encourage inflammatory cell invasion, vascularization, and scarring. When corneal scarring interferes with vision, corneal transplantation is hazardous in the absence or with a deficiency of stem cells.
The concept of corneal stem cell injury and destruction has become of central importance in a variety of diseases of the eye, especially severe alkali and acid injuries. Frequently in these cases all corneal, limbal, and extensive conjunctival epithelium is lost.
No clinical trial has been initiated to study this problem, but numerous individual reports and clinical observations have shown that small conjunctival transplants from the limbus of an unaffected eye to the injured eye can eliminate these recurrent erosions and inflammatory propensities and restore the injured eye to full function (Kenyon and Tseng, 1989). When the injury is bilateral it is possible that conjunctival stem cell transplants from a donor eye would survive in these injured eyes to create a stable epithelial surface. If the corneal problem is one of constant epithelial breakdown, then stem cell transplant should stabilize the epithelial surface and thereby improve vision. In those patients who show severe tear film instability, irremediable eyelid malappositions, recurrent corneal transplant failures, and severe distortions of the anterior segment, a keratoprosthesis (artificial cornea) is an option to provide some vision when live corneal tissue consistently fails. Patients with severe corneal opacities also benefit from modern techniques of corneal transplantation and postoperative management.
Protection of the Corneal Epithelium with a Contact Lens
Mechanical protection of the corneal epithelium has been shown to reduce the irritation and improve the vision in a large series of cases of recurrent keratitis. The large and cumbersome scleral lenses were difficult to make, could only be worn for short periods by most individuals, and gave only a limited but welcome response. The development of soft contact lenses has dramatically improved our ability to protect the corneal epithelium in those patients when it is fragile (Pfister, 1986). Research to study the effect of soft contact lenses on the chronic relapsing keratitis after sulfur mustard injuries might provide an updated approach to mechanical protective devices.
Sulfur Mustard Compared to Alkali Injury: The Stromal Component
Sulfur mustard injuries bear distinct similarities to alkali or very strong acid injuries of the eye. If these two injuries present similar problems, then treatments that have been initiated for alkali burns of the eye might well be effective in mustard gas or Lewisite injuries. An animal model of the alkali-injured eye has yielded significant data showing that sodium citrate and sodium ascorbate, when applied topically to the eye, significantly reduce the incidence of corneal ulceration and perforation (Pfister and Paterson, 1980; Pfister et al., 1981, 1982). A national clinical trial on the treatment of human alkali-injured eyes with ascorbate and citrate is currently in progress. Other chelators that inactivate metalloproteases, such as collagenases, are also available. These metalloprotease inhibitors interfere with the enzymes leading to corneal ulceration. Although there is no clear-cut evidence available, it seems likely that this treatment could be quite effective in sulfur mustard injuries of the eye.
CONCLUSIONS
Acute, severe injury of the eye with sulfur mustard might result in recurrent corneal ulcerative disease for the remainder of the patient's life, with a maximum incidence occurring 15 to 20 years after the injury. Based on extensive data, there is a causal relationship between severe exposure to sulfur mustard and the development of delayed recurrent keratitis.
There is a causal relationship between exposure to sulfur mustard and the development of prolonged, intractable conjunctivitis.
There is evidence, in laboratory animals, to indicate that no causal relation is present between exposure to Lewisite and any long-term ocular disease process. However, any corneal scarring or vasculariza-
tion occurring soon after the injury will persist. In spite of the arsenical nature of Lewisite, no association has been noted between Lewisite and the development of neoplasia of the eye.
REFERENCES
Adler FH, Leopold IH. 1945. The toxicity of Lewisite for the eye. In: National Research Council. Division of Medical Sciences, Committee on Treatment of Gas Casualties, comp. Fasciculus on Chemical Warfare Medicine. Volume I, Eye. Washington, DC: Prepared for the Committee on Medical Research of the Office of Scientific Research and Development. 279-288.
Adler FH, Fry WE, Leopold IH. 1947. Pathologic study of ocular lesions due to Lewisite (beta-chlorovinyldichloroarsine). Archives of Ophthalmology 38:89-108.
Beauvieux. 1920. Ocular lesions caused by vesicant gases. Archives d'Ophtalmologie 37:597-619. [In French]
Friedenwald JS. 1945. The pathological physiology of mustard damage to the cornea. In: National Research Council. Division of Medical Sciences, Committee on Treatment of Gas Casualties, comp. Fasciculus on Chemical Warfare Medicine. Volume I, Eye. Washington, DC: Prepared for the Committee on Medical Research of the Office of Scientific Research and Development. 214-235.
Gates M, Moore S. 1946. Mustard gas and other sulfur mustards. In: Division 9, National Defense Research Committee. Chemical Warfare Agents, and Related Chemical Problems. Summary Technical Report of Division 9, NDRC. Washington, DC: Office of Scientific Research and Development. 30-58.
Gates M, Williams JW, Zapp JA. 1946. Arsenicals. In: Division 9, National Defense Research Committee. Chemical Warfare Agents, and Related Chemical Problems. Summary Technical Report of Division 9, NDRC. Washington, DC: Office of Scientific Research and Development. 83-114.
Genet L. 1925. Ocular burns from yperite gas: persistent sequelae seven years after injury. Case study. Lyon Medical 136:388-391. [In French]
Gilchrist HL, Matz PB. 1933. The Residual Effects of Warfare Gases. Washington, DC: U.S. Government Printing Office.
Goldman M, Dacre J. 1989. Lewisite: its chemistry, toxicology, and biological effects. Reviews of Environmental Contamination and Toxicology 110:75-115.
Heckford F 1937. Delayed corneal ulceration following mustard gas burns. Proceedings of the Royal Society of Medicine 30:949.
Hughes WF Jr. 1942. Mustard gas injuries to the eyes. Archives of Ophthalmology 27:582-601.
Hughes WF Jr. 1945a. The importance of mustard burns of the eye as judged by World War I statistics and recent accidents. In: National Research Council. Division of Medical Sciences, Committee on Treatment of Gas Casualties, comp. Fasciculus on Chemical Warfare Medicine. Volume I, Eye. Washington, DC: Prepared for the Committee on Medical Research of the Office of Scientific Research and Development. 79-90.
Hughes WF Jr. 1945b. The symptomatology and diagnosis of mustard gas injuries of the eyes. In: National Research Council. Division of Medical Sciences, Committee on Treatment of Gas Casualties, comp. Fasciculus on Chemical Warfare Medicine. Volume I, Eye. Washington, DC: Prepared for the Committee on Medical Research of the Office of Scientific Research and Development. 91-109.
Hughes WF Jr. 1946. Treatment of Lewisite burns of the eye with BAL. Journal of Clinical Investigation (July):541-548.
Irwin. 1954. As cited in: Solana RP. 1992. Toxicology of Lewisite. Presentation to the
Institute of Medicine Committee to Survey the Health Effects of Mustard Gas and Lewisite, June 11, 1992. Unpublished.
Karnofsky DA, Nolen JT. 1944. Report on mustard vapor casualties occurring at Bushnell, Fla., 6 June 1944. As cited in: Papirmeister B, Feister AJ, Robinson SI, Ford RD. 1991. Medical Defense Against Mustard Gas: Toxic Mechanisms and Pharmacological Implications. Boca Raton, FL: CRC Press. 42.
Kenyon KR, Tseng SC. 1989. Limbal autograft transplantation for ocular surface disorders. Ophthalmology 96:709.
Little AD Inc. 1986. As cited in: Solana RP. 1992. Toxicology of Lewisite. Presentation to the Institute of Medicine Committee to Survey the Health Effects of Mustard Gas and Lewisite, June 11, 1992. Unpublished.
Mann I. 1944. A study of eighty-four cases of delayed mustard gas keratitis fitted with contact lenses. British Journal of Ophthalmology 28:441-447.
Mann I, Pullinger BD. 1944. A study of mustard gas lesions of the eyes of rabbits and men. American Journal of Ophthalmology 26:1253-1277.
Mann I, Pirie A, Pullinger BD. 1946. Study of Lewisite lesions of the eyes of rabbits. American Journal of Ophthalmology 29:1215-1227.
Maumenee AE, Scholz RO. 1948. The histopathology of the ocular lesions produced by sulfur and nitrogen mustards. Bulletin of Johns Hopkins Hospital 82:121-147.
McNamara BP, Owens EJ, Christensen MK, Vocci FJ, Ford DF, Rozimarek H. 1975. Toxicological Basis for Controlling Levels of Mustard in the Environment. Edgewood Arsenal Special Publication EB-SP-74030. Aberdeen Proving Ground, Maryland: U.S. Army Armament Command. Edgewood Arsenal Biomedical Laboratory.
Moore RF, Heckford F. 1929. Delayed corneal ulceration from mustard gas. British Medical Journal 1:497-498.
Oswald A. 1920. Collapse of the double-sided closure of the central artery as a consequence of blister gas poisoning. Klinische Monatsblatter fur Augenheilkunde 64:381387. [In German]
Ottinger RS, Blumenthal JL, Dal Porto DF, Gruber GI, Santy MJ, Smith CC. 1973. Recommended Methods of Reduction, Neutralization, Recovery or Disposal of Hazardous Waste. Vol. 2, Toxicologic Summary. EPA-670/2-73-053-b. As cited in: Solana RP. 1992. Toxicology of Lewisite. Presentation to the Institute of Medicine Committee to Survey the Health Effects of Mustard Gas and Lewisite, June 11, 1992. Unpublished.
Papirmeister B, Feister AJ, Robinson SI, Ford RD. 1991. Medical Defense Against Mustard Gas: Toxic Mechanisms and Pharmacological Implications. Boca Raton, FL: CRC Press.
Pfister RR. 1986. The biology of persistent epithelial defects of the cornea. In: Brightbill, FS, ed. Corneal Surgery: Theory, Technique, and Tissue. Papers from the First International Cornea and Eye Banking Symposium . St. Louis: Mosby. 582-593.
Pfister RR, Paterson CA. 1980. Ascorbic acid in the treatment of alkali burns of the eye. Ophthalmology 87:1050-1057.
Pfister RR, Nicloaro ML, Paterson CA. 1981. Sodium citrate reduces the incidence of corneal ulcerations and perforations in extreme alkali burned eyes: acetylcysteine and ascorbate have no favorable effect. Investigative Ophthalmology 21:486-490.
Pfister RR, Haddox J, Paterson CA. 1982. The efficacy of sodium citrate in the treatment of severe alkali burns of the eye is influenced by the route of administration. Cornea 1:205-211.
Phillips TJ. 1940. The delayed action of mustard gas and the treatment. Proceedings of the Royal Society of Medicine 33:229-232.
Proceedings of the Royal Society of Medicine. 1940. Discussion on gas injuries to the eye. 33:225-236.
Project Coordination Staff, Chemical Warfare Service. 1946. Technical Aspects of Chemical Warfare in the Field. 2 vols. Washington, DC: Chemical Warfare Service.
Reed CI. 1920. The minimum concentration of dichlorethylsulphide (mustard gas) effective for the eyes of man. Journal of Pharmacology and Experimental Therapeutics 15:77-80.
Rohrschneider W. 1937. Late ocular lesions (keratitis) following yellow cross (dichloroethylsulfide) poisoning. Klinische Monatsblatter fur Augenheilkunde 99:447-455. [In German]
Scholz RO. 1945. Clinical and pathological studies of ocular mustard gas burns. In: National Research Council. Division of Medical Sciences, Committee on Treatment of Gas Casualties, comp. Fasciculus on Chemical Warfare Medicine. Volume I, Eye. Washington, DC: Prepared for the Committee on Medical Research of the Office of Scientific Research and Development. 155-191.
Scholz RO, Woods AC. 1945. Relapsing and chronic mustard gas lesions of the eyes. In: National Research Council. Division of Medical Sciences, Committee on Treatment of Gas Casualties, comp. Fasciculus on Chemical Warfare Medicine. Volume I, Eye. Washington, DC: Prepared for the Committee on Medical Research of the Office of Scientific Research and Development. 260-278.
Scholz RO, Woods AC. 1947. Relapsing and chronic ocular lesions following mustard gas burns. Archives of Ophthalmology 37:137-148.
Solana RP. 1992. Toxicology of Lewisite. Presentation to the Institute of Medicine Committee to Survey the Health Effects of Mustard Gas and Lewisite, June 11, 1992. Unpublished .
Sourdille GP. 1936. Lesions of cornea, especially marginal vascular lesions by yperite. Bulletin de la Societe d'Ophtalmologie de Paris 799-801. [In French]
Stepanov AA, Popov VN. 1962. [Chemical Weapons and Principles of Antichemical Defense]. Translated by Joint Publications Research Service. JPRS 15107. Washington, DC: JPRS.
Stockholm International Peace Research Institute (SIPRI). 1971. The Problem of Chemical and Biological Warfare: A Study of the Historical, Technical, Military, Legal, and Political Aspects of Chemical and Biological Warfare and Possible Disarmament Measures. Vol. 1, The Rise of Chemical and Biological Weapons. Stockholm: Almqvist & Wiksell.
Uhde GJ. 1946. Mustard gas (dichloroethyl sulfide) burns of human eyes in World War II. American Journal of Ophthalmology 29:929.
Urbanetti JS. 1988. Battlefield chemical injury. In: Loke J, ed. Pathophysiology and Treatment of Inhalation Injuries. New York: Marcel Dekker.
U.S. Army. 1974. Chemical agent data sheets, Vol. 1. Technical Report EO-SR-74001. Edgewood Arsenal, Maryland.
U.S. Army Chemical Research, Development, and Engineering Center (CRDEC). 1990. HD and THD. Material Safety Data Sheet. HCSDS No. 20058A. Aberdeen Proving Ground, MD: U.S. Army Chemical Research, Development and Engineering Center.
U.S. Army and U.S. Air Force. 1975. Military chemistry and chemical compounds. Field Manual No. FM3-9, Regulation No. AFR 355-7.
Wallen LJ, Horton RG, Ferguson RL. 1943. L, HN-1, H and HQ: effects of 0.1 mg drops on eyes of rabbits. Project A10.3. TRLR 18. Edgewood Arsenal, MD: Toxicological Research Laboratory. As cited in: Solana RP. 1992. Toxicology of Lewisite. Presentation to the Institute of Medicine Committee to Survey the Health Effects of Mustard Gas and Lewisite, June 11, 1992. Unpublished.
Watson AP, Griffin GD. 1992. Toxicity of vesicant agents scheduled for destruction by the Chemical Stockpile Disposal Program. Environmental Health Perspectives. Publication in process.
Weill G. 1939. Corneal ulcers after dichloroethylsulfide poisoning: case. Bulletin de la Societe d'Ophtalmologie de Paris 51:281-282. [In French]