4
Effects of Exercise and Heat on Gastrointestinal Function
Carl V. Gisolfi1
INTRODUCTION
Compared with cardiorespiratory function, little is known about the effects of exercise-heat stress on gastrointestinal (GI) function. Much of the information is anecdotal, and many of the studies lack adequate controls and quantitation of the exercise response. Most of the information in this area, in recent years, has come from studies on endurance athletes (Brouns et al., 1987; Eichner, 1989; Lorber, 1983; Moses, 1990). This chapter reviews recent prospective studies in this field and the results of a study from this laboratory that evaluated the effects of exercise on intestinal absorption. Because most studies have not isolated the effects of high environmental or internal body temperature per se, the combined effects of exercise and heat stress are discussed. The questions to be addressed include the following:
-
What GI symptoms are manifested during exercise-heat stress?
-
Are these symptoms intensified with increased exercise intensity, duration, or increased heat stress?
-
What are the effects of exercise-heat stress on gastric emptying and intestinal absorption of water?
-
What morphological changes occur in the GI system associated with exercise-heat stress?
-
Do GI symptoms and morphological changes associated with exercise-heat stress persist or do they subside quickly without functional impairment?
GASTROINTESTINAL SYMPTOMS
One of the first and most dramatic accounts of GI distress came from Derek Clayton (Benyo and Clayton, 1979) after he ran the marathon in 2:08:33.6. He commented:
Two hours later, the elation had worn off. I was urinating quite large clots of blood, and I was vomiting black mucus and had a lot of black diarrhea. I don't think too many people can understand what I went through for the next 48 hours.
Table 4-1 lists the common GI symptoms experienced by runners, although these have also been observed in other athletes (Eichner, 1989).
TABLE 4-1 Gastrointestinal Disturbances Associated with Long-Distance Running
|
Abdominal cramps |
|
Belching |
|
Gastrointestinal reflux |
|
Flatulence |
|
Bloody stools |
|
Vomiting |
|
Diarrhea |
|
Nausea |
They are most often observed with overtraining, dehydration, and the use of aspirin. Another contributing factor may be high ascorbic acid intake (Sharman, 1982). These GI symptoms may be reduced by treatment with cimetidine (Baska et al., 1990) or consumption of an elemental diet (Bounous et al., 1967).
IMPORTANCE OF GI MANIFESTATIONS WITH EXERCISE-HEAT STRESS
Severe heat exposure simulates hemorrhage and intestinal ischemia because blood pools in the cutaneous capacitance vessels, central blood volume and splanchnic blood flow decline, and mean arterial pressure falls because increased heart rate cannot fully compensate for a declining stroke volume that causes cardiac output to fall. Hemorrhage and intestinal ischemia
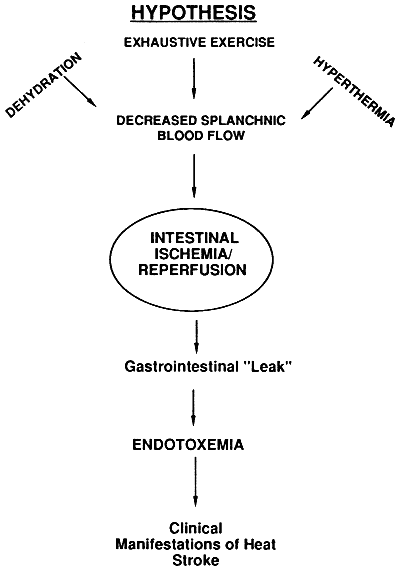
increase capillary permeability (Granger et al., 1981) and have been reported to produce mucosal lesions in the small intestine of humans (Klemperer et al., 1940), dogs (Chiu et al., 1970), rats (Bacalzo et al., 1971), and cats (Haglurid and Lundgren, 1973). The pathogenesis of the rise in capillary permeability has been attributed to the production of superoxide radicals (Granger et al., 1981), and the pathogenesis of the mucosal lesions has been attributed to hypoxia (Ahren and Haglund, 1973). Thus, it has been hypothesized that severe hyperthermia (a) produces mucosal lesions in the small intestine from tissue hypoxia, (b) increases capillary permeability, and (c) results in endotoxemia (see Figure 4-1). Systemic endotoxemia has been shown in human heat stroke victims (Coridis et al., 1972; Graber et al., 1971), in ultramarathon runners who collapsed during competition in the heat (Brock-Utne et al., 1988), and following strenuous exercise (Bosenberg et al., 1988).
The diarrhea that occurs in marathon runners, if coincident with bleeding, may be a clinical manifestation of ischemic enteropathy (Bounous and McArdle, 1980). The effects of exercise-heat stress on GI function and performance can range from mild discomfort to serious impairment. For example, GI bleeding, which is often coincident with diarrhea, may be trivial (Eichner, 1989) or lethal (Thompson et al., 1982).
Gaudin et al. (1990) performed a standard endoscopy examination on seven runners 15 minutes before and 12 hours after they performed a maximal distance training run (18 to 50 km). Because the race was not competitive, stress was not considered to be a factor. Mucosal biopsy specimens of the upper digestive track revealed histologically pathological features in all runners (Table 4–2). These features included vascular lesions, ranging from congestion to hemorrhage, and evidence of reduced mucosal secretion (estimated from PAS [para -aminosalicylic acid] staining). The intensity of the lesions was independent of running distance, and a measure of running intensity was not provided. The prevalence of the lesions was independent of clinical symptoms.
Schwartz et al. (1990) studied 41 runners who completed the 1988 Chicago Marathon. Nine of the runners experienced GI bleeding, and three of these consented to esophagogastroduodenoscopy and colonoscopy within 48 hours after the race. Four other runners consented to these procedures 4 to 30 days after the race. Of the three runners examined within 48 hours, two had oozing gastric antral erosions, and the third had patchy areas of hyperemic and eroded mucosa limited to the splenic flexure. The latter portion of the colon is a circulatory watershed area, which suggests that a condition of reduced blood flow may contribute to necrosis of the colonic mucosa. Thus, injury can occur in both upper and lower segments of the GI track. There were no endoscopic findings in the four runners examined three or more days after the race, which suggests that restoration of the
TABLE 4-2 Histological Observations of Runners After a Maximal Distance Training Run (18 to 50 km)
|
Vascular lesions |
|
Extravasation |
|
Petechiae |
|
Reduced mucosal secretion |
|
Reduced mucopolysaccharide epithelial coating |
|
Subepithelial capillary dilation |
|
Edema of lamina propria |
|
SOURCE: Gaudin et al. (1990) and Schwartz et al. (1990). |
resting state allows this form of injury to heal quickly. As a cautionary note, the lesions found in this study are similar to those observed with the use of nonsteroidal antiinflammatory drugs (NSAIDs), which are frequently taken by runners with musculoskeletal injuries (Andron, 1991). In the study by Schwartz et al. (1990), 60 percent of the runners in the ''bleeding group'' used NSAIDs.
The extent of these GI injuries can be more severe. Acute ischemic enteropathy could produce endotoxemia and the cardiovascular manifestations of heat stroke. Of 89 exhausted runners who required admission to the medical tent for treatment in the 1986 Comrades Marathon (89.4 km), 81 percent had endotoxemia that significantly correlated with the occurrence of nausea, vomiting, and diarrhea (Brock-Utne, 1988). It was hypothesized that the intestinal wall was damaged by reduced blood flow, hypoxia, and/or hyperthermia. This damage in turn led to excessive leakage of endotoxin into the portal circulation (Brock-Utne et al., 1988). This hypothesis is supported by the observation that a nonabsorbable antibiotic (kanamycin, 15 mg per kg) administered over a 5-day period to primates before heat exposure prevented the endotoxemia that was observed in control animals heated to a core temperature of 44.5°C (Gathiram et al., 1987).
GASTRIC EMPTYING
Is there any evidence that environmental temperature, or a rise in core body temperature, adversely affects the rate at which the stomach empties? The observation that gastric emptying (GE) is reduced in the heat was first made by Owen et al. (1986). These investigators found that during treadmill exercise (65 percent ![]() [maximal oxygen uptake]) in a 25°C environment) subjects emptied 79 percent of the water they ingested (1 liter) com-
[maximal oxygen uptake]) in a 25°C environment) subjects emptied 79 percent of the water they ingested (1 liter) com-
TABLE 4-3 Gastric Emptying During Ingestion of Different Beverages
|
Beverage (environment) |
Gastric Residual Volume (ml) |
% Drink Emptied |
|
|
mean ± SEM |
|
|
Glucose polymer (35°C) |
487.6 ± 12.3 |
51.3 ± 1.2 |
|
Glucose (35°C) |
587.0 ± 98.1* |
41.3 ± 9.8* |
|
Water (35°C) |
412.1 ± 84.7 |
58.8 ± 8.5 |
|
Water (25°C) |
208.8 ± 65.5 |
79.1 ± 6.5 |
|
* Significantly different (p < 0.05) from all other runs. SOURCE: Adapted from Owen et al. (1986). |
||
pared with only 59 percent when they performed the same exercise and ingested the same volume of water in the heat (35°C) (see Table 4–3). Neufer et al. (1989) made a similar observation and found a significant negative correlation between GE and rectal temperature. These investigators also found that hypohydration significantly reduced GE. The mechanism responsible for this reduction is unclear, but it is probably related to the thermal strain associated with hypohydration and exercise-heat stress. Exercise reduces splanchnic blood flow (Rowell et al., 1968) and elevates plasma beta-endorphin levels (Kelso et al., 1984), both of which could reduce GE (Konturek, 1980; Kowalewski et al., 1976). Also, it is known that elevations in core body temperature can reduce stomach and intestinal motility (Tsuchiya and Iriki, 1980; Tsuchiya et al., 1974).
INTESTINAL ABSORPTION
Is there any evidence that intestinal absorption is compromised during exercise-heat stress? Using the plasma accumulation of 3-O-methyl-D-glucose (active) and D-xylose (passive) from a solution ingested orally as measures of intestinal absorption, Williams et al. (1964) found that prolonged (4.5 hour) treadmill exercise (3.0 miles per hour) in the heat (38/27°C dry bulb/wet bulb) reduced active but not passive carbohydrate absorption. Maughan et al. (1990) also found evidence of reduced intestinal absorption during exercise. They measured the rate of plasma D2O accumulation from a beverage labeled with D2O and found that exercise at 61 percent ![]() reduced absorption measured at rest, and that absorption at 80 percent
reduced absorption measured at rest, and that absorption at 80 percent ![]() was less than at 42 percent and 61 percent
was less than at 42 percent and 61 percent ![]() .
.
Also, Barclay and Tumberg (1988) reported that mild (heart rate = 103 beats per minute) exercise significantly reduced water and electrolyte absorption compared with rest; however, the solution they used contained no carbohydrate, which reduced the rate of intestinal absorption to 2 ml per hour per cm compared with a value of 13 to 15 ml per hour per cm for a carbohydrate-electrolyte solution (Gisolfi et al., 1991).
In contrast to these observations, Fordtran and Saltin (1967) found no effect of exercise (74 percent ![]() ) on either active or passive absorption using the more direct technique of segmental perfusion. Moreover, this author's most recent results (Gisolfi et al., 1991), also using the segmental perfusion technique, show no effect of either exercise intensity (30 to 70 percent
) on either active or passive absorption using the more direct technique of segmental perfusion. Moreover, this author's most recent results (Gisolfi et al., 1991), also using the segmental perfusion technique, show no effect of either exercise intensity (30 to 70 percent ![]() ) or duration (60 to 90 minutes) on fluid absorption (see Figure 4-2 on following page).
) or duration (60 to 90 minutes) on fluid absorption (see Figure 4-2 on following page).
PREVENTION AND MANAGEMENT
Although there is much to be learned about GI function during exercise-heat stress, the following suggestions are offered to help prevent or manage GI distress under such conditions:
-
GI symptoms, GI bleeding, and endotoxemia seem to be related to exercise intensity, exercise duration, high thermal stress, and sharp increments in training. They also seem to occur among individuals who are poorly trained and who engage in endurance exercise. Thus, it would be prudent to be well conditioned and heat acclimated if thermal stress is anticipated. Also, sharp increments in physical work performed in the heat should be avoided.
-
Nonsteroidal antiinflammatory drugs have been known to produce upper GI lesions and should be avoided 12 to 24 hours prior to hard exercise in the heat. Aspirin has a potent and long lasting antiplatelet action and should be avoided for 2 or 3 clays prior to severe exercise in the heat. Aspirin is often taken 30 minutes before exercise by individuals with joint pain. If taken immediately before exercise, aspirin can produce marked cramping and related GI discomfort. High doses of ascorbic acid (vitamin C), which are sometimes taken by athletes, can produce diarrhea and should be avoided.
-
Prefeeding an elemental semihydrolyzed diet might reduce the incidence and severity of intestinal discomfort in endurance athletes. If gastrids or upper GI ulceration is the source of GI symptoms, therapy with antacids or H2 blockers may provide relief and allow soldiers to function normally.
-
When GI symptoms do occur as a result of exercise per heat stress, they usually abate quickly (within days) with rest.
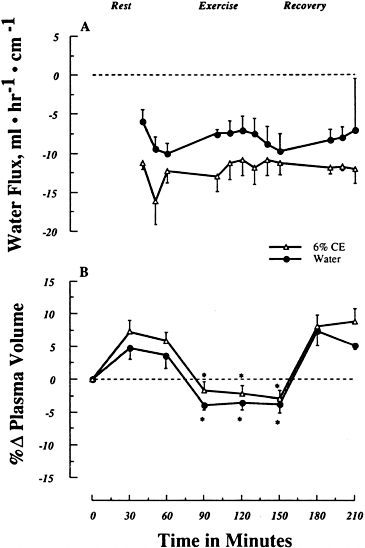
FIGURE 4-2 (A) Net water flux (mean ± SE) across a 40 cm segment of the duodenojejunum during the perfusion (15 ml per min) of water or a 6 percent carbohydrate-electrolyte (CE) solution at rest, during 90 min of exercise at 70 percent ![]() , and during 60 min of recovery. Infusion began at time 0. Negative values indicate absorption. (B) Percent change in plasma volume during rest, exercise, and recovery for perfusion of water and the 6 percent GE solution. Different from rest and recovery values (p < 0.05). SOURCE: Gisolfi et al. (1991).
, and during 60 min of recovery. Infusion began at time 0. Negative values indicate absorption. (B) Percent change in plasma volume during rest, exercise, and recovery for perfusion of water and the 6 percent GE solution. Different from rest and recovery values (p < 0.05). SOURCE: Gisolfi et al. (1991).
REFERENCES
Ahren, C., and U. Haglund 1973 Mucosal lesions in the small intestine of the cat during low flow. Acta Physiol. Scand. 88:541–550.
Andron, R.I. 1991 Gastrointestinal bleeding in runners. Ann. Intern. Med. 114(5):429.
Bacalzo, L.V., A.L. Cary, L.D. Miller, and W.M. Parkins 1971 Methods and critical uptake volume for hemorrhagic shock in rats. Surgery 70:555–560.
Barclay, G.R., and L.A. Turnberg 1988 Effect of moderate exercise on salt and water transport in the human jejunum. Gut 29:816–820.
Baska, R.S., F.M. Moses, and P.A. Deuste 1990 Cimetidine reduces running-associated gastrointestinal bleeding. Dig. Dis. Sci. 35(8):956–960.
Benyo, R., and D. Clayton 1979 The world's fastest marathoner. Runners World 66–73.
Bosenberg, A.T., J.G. Brock-Utne, S.L. Gaffin, M.T.B. Wells, and G.T W. Blake 1988 Strenuous exercise causes systemic endotoxemia. J. Appl. Physiol. 65(1):106–108.
Bounous, G., and A.H. McArdle 1980 Marathon runners: The intestinal handicap. Med. Hypotheses 33:261–264.
Bounous, G., N.G. Sutherland, A.H. McArdle, and F.N. Gurd 1967 The prophylactic use of an "elemental" diet in experimental hemorrhagic shock and intestinal ischemia. Ann. Surg. 166:312–342.
Brock-Utne, J.G., S.L. Gaffin, M.T. Wells, P. Gathiram, E. Sohar, M.F. James, D.F. Morrell, and R.J. Norman 1988 Endotoxemia in exhausted runners after a long-distance race. S. Afr. Med. J. 73:533–536.
Brouns, F., W.H.M. Saris, and N.J. Rehrer 1987 Abdominal complaints and gastrointestinal function during long-lasting exercise. Int. J. Sports Med. 8:175–189.
Chiu, C.-J., A.H. McArdle, R. Brown, H.J. Scott, and F.N. Gurd 1970 Intestinal mucosal lesion in low flow states. Arch. Surg. 101:478–483.
Coridis, D.T., R.B. Reinhold, P.W. Woodruff, and J. Fine 1972 Endotoxemia in man. Lancet 1:1381–1386.
Eichner, E.R. 1989 Gastrointestinal bleeding in athletes. Physician Sportsmed. 17:128–140.
Fordtran, J.S., and B. Saltin 1967 Gastric emptying and intestinal absorption during prolonged severe exercise. J. Appl. Physiol. 23:331–335.
Gathiram, P., M.T. Wells, J.G. Brock-Utne, B.C. Wessels, and S. L. Gaffin 1987 Prevention of endotoxemia by non-absorbable antibiotics in heat stress. J. Clin. Pathol. 40:1364–1368.
Gaudin, C., E. Zerath, and C.Y. Guezennec 1990 Gastric lesions secondary to long-distance running. Dig. Dis. Sci. 35(10):1239–1243.
Gisolfi, C.V., K.J. Spranger, R.W. Summers, H.P. Schedl, and T. L. Bleiler 1991 Effects of cycle exercise on intestinal absorption in humans. J. Appl. Physiol. 71:2518–2587.
Graber, C.D., R.B. Reinhold, and J.G. Breman 1971 Fatal heatstroke. J. Am. Med. Assoc. 216:1195–1196.
Granger, D.N., G. Rutili, and J.M. McCord 1981 Superoxide radicals in feline intestinal ischemia. Gastroenterology 81:22–29.
Haglund, U., and O. Lundgren 1973 The effects of vasoconstrictor fibre stimulation on consecutive vascular sections of cat small intestine during hemorrhagic hypotension . Acta Physiol. Scand. 88:95–108.
Kelso, T.B., W.G. Herbert, F.C. Gwazdauskas, F.L. Goss and J.L. Hess 1984 Exercise-thermoregulatory stress and increased plasma b-endorphin/b-lipotropin in humans. J. Appl. Physiol. 57:444–449.
Klemperer, P., A. Penner, and A.I. Bernheim 1940 The gastro-intestinal manifestations of shock. Am. J. Dig. Dis. 7:410–413.
Konturek, S.J. 1980 Opiates and the gastrointestinal tract. Am. J. Gastroenterol. 74:285–291.
Kowalewski, K., S. Zajac, and A. Kolodej 1976 Effect of ischemic anoxia on electrical and mechanical activity of the totally isolated porcine stomach. Eur. Surg. Res. 8:12–25.
Lorber, S.H. 1983 Gastrointestinal disorders and exercise. Pp. 279–290 in Exercise Medicine: Physiological Principles and Clinical Applications. New York: Academic Press.
Maughan, R.J., J.B. Leiper, and B.A. McGaw 1990 Effects of exercise intensity on absorption of ingested fluids in man. Exp. Physiol. 75:419–421.
Moses, F.M. 1990 The effect of exercise on the gastrointestinal tract. Sports Med. 9(3): 159–172.
Neufer, P.D., A.J. Young, and M.N. Sawka 1989 Gastric emptying during exercise: Effects of heat stress and hypohydration. Eur. J. Appl. Physiol. 58:433–439.
Owen, M.D., K.C. Kregel, P.T. Wall, and C.V. Gisolfi 1986 Effects of ingesting carbohydrate beverages during exercise in the heat. Med. Sci. Sports Exerc. 18(5):568–575.
Rowell, L.B., G.L. Brengelmann, J.R. Blackmon, R.D. Twiss, and F. Kusumi 1968 Splanchnic blood flow and metabolism in heat-stressed man. J. Appl. Physiol. 24:475–484.
Schwartz, A.E., A. Vanagunas, and P.L. Kamel 1990 Endoscopy to evaluate gastrointestinal bleeding in marathon runners. Ann. Intern. Med. 113(8):632–633.
Sharman, I.M. 1982 Gastrointestinal disturbances in runners. Br. J. Sports Med. 16(2): 179.
Thompson, P.D., E.J. Funk, and R.A. Carleton 1982 Incidence of death during jogging in Rhode Island from 1975 through 1980. J. Am. Med. Assoc. 247(18):2535–2538.
Tsuchiya, K., and M. Iriki 1980 Effects of spinal cord cooling and heating on gastrointestinal motility in spinalintact and acutely spinalized dogs. Ital. J. Gastroenterol. 12:255–259.
Tsuchiya, K., E. Kozawa, and M. Iriki 1974 Changes of gastrointestinal motility evoked by spinal cord cooling and heating. Pflugers Arch. 351:275–286.
Williams, J.H., M. Mager, and E.D. Jacobsen 1964 Relationship of mesenteric blood flow to intestinal absorption of carbohydrates. J. Lab. Clin. Med. 63(5):853–863.
Discussion
PARTICIPANT: This damage is associated with running or is it associated with other types of activity as well?
DR. GISOLFI: It is primarily associated with running, but has been observed in triathletes and elite cyclists.
I think it is important that over at least a 90-minute period of intense exercise, we had one subject reach a core temperature of 40°C and observed no reduction in intestinal absorption of either active or passive solutes nor did we observe any change in fluid absorption.
If you exceed 90 minutes of strenuous exercise, especially if it is performed in a warm environment, I don't know the consequences on the GI tract. There is no data.
PARTICIPANT: Would you care to speculate on the differences between indirect and direct evidence on the deuterated water versus the sampling from the intestine?
DR. GISOLFI: This is a good point. Using the direct method of segmental perfusion you are looking at absorption from just a segment of the intestine. Using the indirect method of D2O accumulation in the blood, you are looking at absorption from the entire intestine.
Some studies have demonstrated that deuterium oxide is taken up by the stomach. How much this contributes to overall absorption is not clear.
When you look at the accumulation of a substance in the blood, you need to know the rate at which the substance is coming into the vascular compartment and the rate at which it is leaving. How is it being distributed to different organs? At what rate is it moving from the vascular compartment into the interstitial fluid compartment and at what rate is it being filtered off by the kidney? Without knowing the dynamics of that situation, it is difficult to say what the accumulation in the vascular compartment really means.