2
Nurturing Clinical Researchers
Despite the tremendous advances made over the past 50 years in the ability to understand, diagnose, and treat human disease, there is a growing and legitimate concern that the pace of clinical research will be significantly hampered at a time when some of the most exciting research developments in the history of medical science are ready for human testing. As more and more is understood about fundamental cellular and molecular biology from the study of cells and animal systems, many questions about basic human biology arise, and these questions can only be answered in human subject studies, or what Ahrens refers to as basic patient-oriented research (Ahrens, 1992). Furthermore, over the past two decades the measures for assessing medical practice and determining medical outcomes have been refined progressively, and this field of research stands on the crest of rapid implementation to improve the practice and delivery of effective health care (Wennberg, 1990).
Clinical investigation in the United States is currently threatened by fundamental changes in the organization of health care, major efforts to contain health care expenditures, the high costs of performing clinical studies, such as those associated with drug development, that add to the growing health care budget, and a perceived reduction in the number of individuals pursuing careers in patient-based research. It should be noted that new knowledge gained through scientific investigation is a public good (Pool, 1991). Thus, there is an inherent penalty for those who fund research and a reward for those who let others support it. There is grave danger in a cost-conscious health care reform environment that people will have the notion that clinical research is something
that should be supported by someone else. However, society and the payers as society's representatives must recognize the value to all society of support for clinical research. The committee fears that a health care environment that focuses solely on costs or the effort to contain costs will increase the disincentive to invest in clinical research.
Current medical practice and health care rely on sound scientific principles. Clinical research into new therapies, diagnostics, prevention strategies, as well as outcomes assessment of current medical practice requires methods every bit as sophisticated as those required to isolate and clone genes. To develop a sound scientific basis for health practices, a thorough understanding of hypothesis testing and knowledge base in areas such as biochemistry, pharmacology, cellular and molecular biology, statistical methodology, economics, medical informatics, and the social and behavioral sciences is necessary. Design of clinical research without attention to preclinical studies is inappropriate.
Identifying and enrolling suitable patients into clinical research protocols is very time consuming. It is estimated that in many studies only 20 percent of the pool of apparently suitable patients are actually appropriate candidates (Friedman, 1987; Hunter et al., 1987; Martin et al., 1984). Thus, considerable effort is expended by the physician member of a research team who screens patients to enroll suitable subjects into research protocols. Many feel that this time commitment is underappreciated by other scientists and research administrators.
Although clinical investigators are commonly sought for academic departments, highly skilled and talented individuals who understand and can perform complex human studies are also needed by industry and government agencies (Shaw, 1992; Spilker, 1992). Career trajectories are vague, however, and clinical research funding appears tenuous when compared with the funding base for laboratory-based research (Wyngaarden, 1983). For many, the lengthy periods of training required to become skilled in providing high-quality health care conflict with the time demands of becoming outstanding researchers. High levels of educational debt, pressures to develop a unique academic practice and earn one's salary, obligations to family, responsibility to serve on numerous committees, and other commitments add to the pressures confronting junior faculty. On top of these pressures, faculty often find that the institutional paperwork required for different committees overseeing human research activities is virtually endless. Although these are just a few of the barriers and obstacles confronting individuals who choose to perform a human study in academic institutions, these and other problems affect investigators in both the federal government and the private sector.
The academic model in the past was the "triple-threat" faculty member who was expected to be an outstanding researcher, teacher, and clinician simultaneously. Because of the increasing complexity in all three realms, many
now believe that the triple-threat is no longer feasible and that a clinician can focus on being outstanding in only one, or possibly two, of these areas. This chapter explores the number of faculty available for performing clinical research, examines some of the barriers to careers in clinical research, and suggests some solutions for overcoming the impediments to these career paths.
ENVIRONMENT FOR CLINICAL RESEARCH
Clinical research can be conducted in numerous sites, but the primary locus of most clinical research has been the academic medical center. There are currently 126 accredited allopathic medical schools in the United States, 14 of which are free standing and 112 of which are affiliated with a university. In addition, some academic medical centers are closely affiliated with schools of nursing, pharmacy, or allied health. To trace the course of development to the modern academically based clinical research environment, it is useful to reflect on the history of academic medical centers.
Prior to this century, medical education was the province of voluntary private practitioners. Over the past 100 years, medical education in the United States has undergone vast changes. At the turn of the century there were approximately 155 medical schools in the United States and Canada, and there were three predominant models: the hospital-based clinical model, in which students were trained through programs similar to apprenticeships; the university-based model; and the proprietary or for-profit schools (Burke, 1992). In 1910 Abraham Flexner published a report, "Medical Education in the United States and Canada," based on personal visits and surveys of medical schools (Flexner, 1910). By the time Flexner issued his report, the university-based teaching model was beginning to gain broad acceptance in the United States. Flexner endorsed this model and recommended that the responsibility of medical education be delegated to full-time faculty members who would also be involved in advancing knowledge in medical science as well as training physicians. Moreover, Flexner's description of the for-profit medical schools and the low educational standards of these schools led to the closure of many schools and reforms in a large number of the schools that remained. Flexner's report may thus have served as the catalyst for the shift to staff clinical departments with full-time faculty. This change to full-time faculty in the university-based medical centers, combined with an academic organization similar to those in the other parts of universities, made the medical school more like the rest of the university, with a greater emphasis on scholarly achievement (Fye, 1991).
Largely as a result of the Flexner report, the number of medical schools in the United States dropped to 80 by 1925. Following World War II, the number of medical schools began to rise again as a result of a variety of forces. In 1940 there were about 2,800 full-time medical school faculty. By 1950, the number
of faculty had grown by more than 50 percent, to nearly 4,200, and it more than doubled again during the next decade, to reach 11,300 by 1960 (Burke, 1992). This rapid rate of growth was fueled by several policy changes by the federal government, most notably the surge in federal research monies flowing to universities, the government's decision to push for training of more doctors, and the concomitant funding made available for building new medical school facilities throughout the 1960s (Ahrens, 1992; Institute of Medicine, 1990). The number of medical schools grew to 95 by 1969 and to 127 by 1982. There has been only one closure, leaving the present total of 126 medical schools of which 74 are publicly supported institutions and 53 are private (Ahrens, 1992).
CLINICAL RESEARCH WORKFORCE
Obtaining demographic data on the subset of academic faculty performing patient-oriented clinical research is hampered by the lack of a database for recording these data, the heterogeneity of the disciplines engaged in clinical research, and the inability to separate clinical investigator faculty from those with predominantly laboratory-based research or clinical care responsibilities. Furthermore, many faculty may be involved in more than one of these areas, possibly both laboratory and human research or human research and patient care. Unlike the Doctorate Record File database maintained by the National Research Council, which records the doctorates conferred on all graduates of U.S. institutions and gives some indication of the talent pool for biomedical research, comparable listings for medical or dental school graduates do not provide insight into the potential researcher pool in these professions (National Research Council, 1989a). Also, Vaitukaitis has shown that almost half of all grant awards to investigators indicating the use of humans or human materials are to Ph.D.s (Vaitukaitis, 1991). Because clinicians are trained primarily to provide health care, they have alternate career options available if research pathways appear unappealing because of difficulties in funding or other reasons. In addition, there is no way to quantify the reserve pool of clinical investigator talent—the number of adequately trained clinicians who might apply for research funding if the chances for garnering funds were somewhat better.
To gain a clearer understanding of the physician-investigator workforce, it is useful to look at the total pool of U.S. physicians and its subsets, particularly those on the faculties of medical schools, where the majority of academically based clinical investigators are believed to be employed. According to the American Medical Association (AMA) Physician Masterfile, there were more than 615,000 M.D.s in the United States in 1990, of whom about 90 percent were active in medical practice (American Medical Association, 1992). What is very striking is that the number of women physicians has quadrupled since 1970, from 25,401 (7.6 percent of the 334,038 physicians in 1970) to 104,194 (16.9
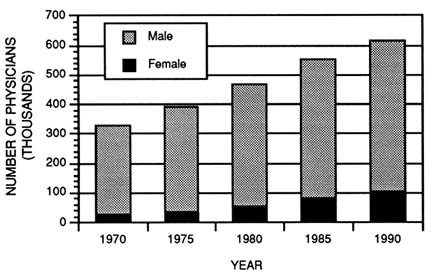
FIGURE 2-1 Total number of U.S. physicians by gender for selected years, 1970–1990. (Source: American Medical Association, 1991.)
percent) in 1990 (Figure 2-1) (American Medical Association, 1991). Moreover, women constitute more than 28 percent of the estimated 134,872 physicians under the age of 35. The growing number of women in the physician workforce implies that particular attention should be paid to clinical research career pathways for this subset as well.
Both the AMA and the Association of American Medical Colleges (AAMC) collect data on medical school faculty, and both sets of data are useful in describing the clinical research workforce. Data collected by the AMA for the Liaison Committee for Medical Education reveal that there were 80,086 medical school faculty in the 1991–1992 academic year (Jolin et al., 1992). The AAMC, however, reports that there were about 75,144 medical school faculty in 1993. Of the latter, 44,838 (59.7 percent) were M.D.s, another 5.4 percent (4,076) were M.D.-Ph.D.s or M.D.s with another health degree (for example, D.Sc., D.P.H., and the like), and the remainder had either a Ph.D. (19,589) or another degree (6,641) (Figure 2-2) (Association of American Medical Colleges, 1993).
Using Institute of Medicine, AMA, and National Institutes of Health (NIH) data, Ahrens has shown that distribution of faculty between clinical and preclinical departments is about 80 percent and 20 percent, respectively (Table 2-1) (Ahrens, 1992). Moreover, the proportion of Ph.D.s on medical school faculties has remained fairly stable, at about 29 percent, since 1970. Whereas
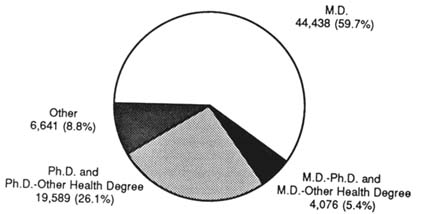
FIGURE 2-2 Distribution of U.S. medical school faculty (Total =75,144) by degree in 1993. (Source: Reprinted, with permission, from Association of American Medical Colleges [1993], p.4. Copyright 1993 by Association of American Medical Colleges.)
M.D.s have always been clustered in the clinical departments and more than 90 percent are so assigned, nearly half of the Ph.D.s now have their primary appointment in a clinical department (Ahrens, 1992; Herman, 1986). This represents about a 36 percent increase since 1970, but there is variability in the employment practices among medical schools as well as among departments. What is not known is how many faculty, M.D.s or Ph.D.s, have dual appointments in both the preclinical and clinical sciences, partially because of the inability to track investigators' appointments with any current database. Gaps also exist in quantifying the number of investigators, basic as well as clinical, who are employed by independent teaching hospitals and independent research institutions without medical school affiliations.
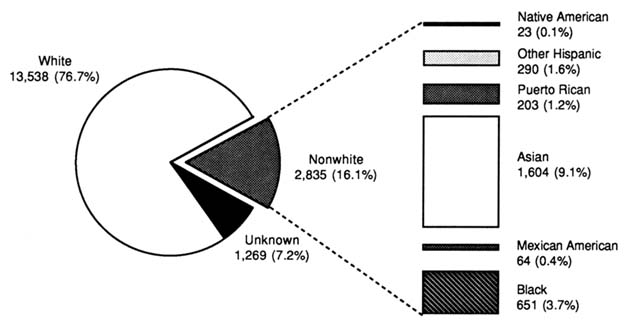
Also of interest is the gender, racial, and ethnic distributions of the faculty (Eisenberg, 1989; Grant, 1988). According to the AAMC data, women make up about 23.5 percent of medical school faculty (17,642 of the 75,144 total faculty) (Figure 2-3) (Association of American Medical Colleges, 1993). About 9,666 or slightly more than half (54.8 percent), of women medical school faculty are M.D.s (including M.D.s with Ph.D.s or other health degrees) compared with 68.7 percent (39,181 of 57,007) of male faculty who have an M.D. The proportion of women physicians on medical school faculty exceeds their representation in the overall population of physicians—about about 23 percent versus 17 percent, respectively (see Figures 2-1 and 2-3). Most of the women faculty, however, are clustered in the lower ranks of the faculty (Figure 2-4).
TABLE 2-1 Full-time Faculty in All U.S. Medical Schools, 1961–1989
|
|
|
Number of Awards |
|
|
|
|
Fiscal Year |
Number of Schools |
Total |
Preclinical Departments |
Clinical Departments |
Percent in Clinical Departments |
|
1961 1962 1963 1964 1965 |
86 86 87 88 89 |
11,224 12,040 13,602 15,015 15,882 |
4,023 4,342 4,693 5,541 5,233 |
7,201 7,698 8,909 9,474 10,649 |
64.2 63.9 66.0 63.1 67.1 |
|
1966 1967 1968 1969 1970 |
89 92 99 101 103 |
17,118 19,297 22,293 23,034 24,093 |
5,671 5,877 6,639 7,048 7,287 |
11,447 13,420 15,654 15,986 16,806 |
66.9 69.5 70.2 69.4 69.8 |
|
1971 1972 1973 1974 1975 |
108 112 114 114 114 |
27,539 30,170 33,265 34,878 37,010 |
8,283 8,714 9,381 9,928 10,164 |
19,256 21,456 23,884 24,950 26,846 |
69.9 71.1 71.8 71.5 72.5 |
|
1976 1977 1978 1979 1980 |
116 122 125 126 126 |
39,346 41,650 44,358 46,662 49,446 |
10,743 11,031 11,736 12,605 12,831 |
28,603 30,349 32,622 34,057 36,665 |
72.7 72.9 73.5 73.0 74.2 |
|
1981 1982 1983 1984 1985 |
126 127 127 127 127 |
50,532 53,371 55,525 57,003 58,774 |
12,816 13,223 13,587 13,560 13,767 |
37,716 40,148 41,938 43,443 45,007 |
74.6 75.2 75.5 76.2 76.6 |
|
1986 1987 1988 1989 |
127 127 127 127 |
61,397 63,313 66,798 70,308 |
14,204 14,479 14,580 14,832 |
47,193 48,834 52,218 55,476 |
76.9 77.1 78.2 78.9 |
|
Average Annual Growth Rate 1961–1989 |
1.4% |
6.7% |
4.8% |
7.6% |
|
|
Source: Reprinted, with permission, from Ahrens [1992], p. 21. Copyright 1992 by the Oxford University Press, Inc. |
|||||
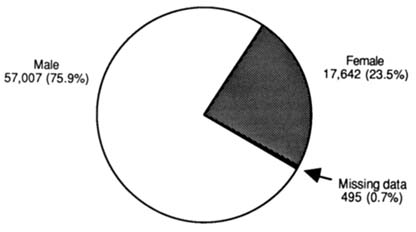
FIGURE 2-3 Distribution of U.S. medical school faculty (Total=75,144) by gender in 1993. (Source: Association of American Medical Colleges, 1993.)
For example, only 9 percent are full professors, 19 percent are associate professors, and 50 percent are assistant professors. The remainder are listed as instructors (18 percent) or have other types of appointments. By comparison, the male faculty are almost evenly stratified among professors (31 percent), associate professors (25 percent), and assistant professors (35 percent).
The reasons for women being clustered in the lower professional ranks remain unclear, but several suggestions have been postulated (Bickel, 1988; Bickell and Whiting, 1991; Cotton, 1992a and 1992b; Dwyer et al., 1991; Graves and Thomas, 1985; Levinson and Weiner, 1991). For example, women did not begin to enter medical schools in significant numbers until the 1970s. Thus, the age profile of faculty shows that women faculty are younger than their male counterparts. For example, 36 percent of women faculty are under the age of 39, compared with 23 percent of male faculty. Only 22 percent of the women faculty are between the ages of 50 and 69, whereas 36 percent of the male faculty are in the same age bracket (Association of American Medical Colleges, 1993). Women are only now beginning to enter the top ranks of medical school faculties in large numbers. There has also been a perceived bias on the part of promotion committees, which have been dominated by men in the past.
Another apparent barrier to clinical research careers for women is balancing the responsibilities of family with the demands of a professional career (Cole and Zuckerman, 1989; Levinson et al., 1989). It is estimated that nearly 75 percent of women physicians are currently married (American Medical Association, 1991). Of these, 93 percent of the spouses of married women
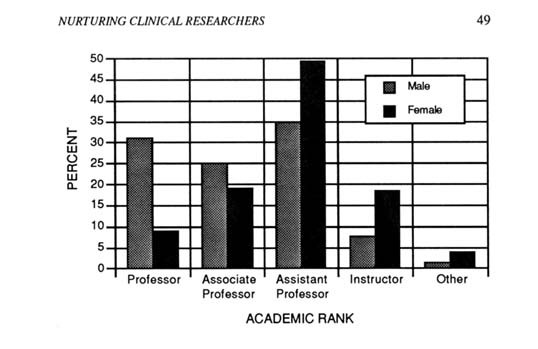
FIGURE 2-4 Distribution of U.S. medical school faculty by genderand academic rank for 1993. (Source: Reprinted, with permission, from Associationof American Medical Colleges [1993], p. 8. Copyright 1993 by the Associationof American Medical Colleges.)
physicians are employed outside the home, compared with 45 percent for married male physicians. Among married women physicians under the age of 40, about 45 percent are married to other physicians, while less than 10 percent of male married physicians in the same age bracket are married to physicians (American Medical Association, 1991). Another fraction is married to individuals in other professions who are as dedicated to their careers as physicians are. Moreover, about 85 percent of women physicians who are married have children. To maintain competence in their profession, it is believed that physicians must maintain continuity in their practices and that they do not exit and reenter the job market. For those pursuing research careers as well, it is nearly impossible to maintain active participation in research on a part-time or intermittent basis. Thus, the balancing of two-career families and the juggling of two-career families with children can often lead to career compromises by one or both of the parents. It is believed that women, even those in two-professional families, shoulder a disproportionately larger share of the responsibilities of child-rearing and household duties than their male spouses. No reliable data are available to substantiate whether these concerns affect women physicians more than male physicians, however.
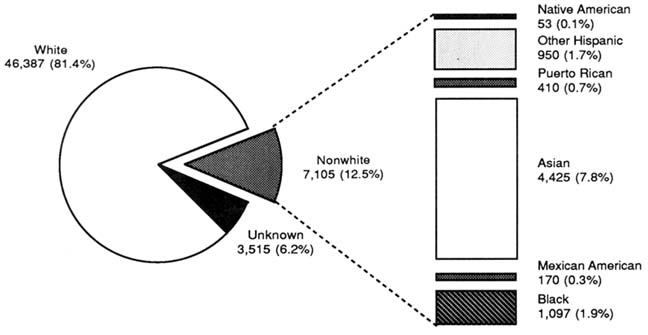
Of the 17,642 women faculty, 2,835 (16.1 percent) are nonwhite (Figure 2-5). Most of this fraction are of Asian or Pacific Island descent (more than 9 percent of the total). Of the 57,007 male faculty, 7,105, or about 12.5 percent, are nonwhite (Figure 2-6). Here, too, most of the nonwhite male faculty (almost 8 percent of the total) is of Asian or Pacific Island descent. Only a small fraction of the men or women faculty are African American (1.9 and 3.7 percent, respectively).
RESEARCH INVOLVEMENT OF FACULTY
Data on the research involvement of medical school faculty are sparse. The only comprehensive study of faculty research activity was conducted in 1986 by the Association of Professors of Medicine in conjunction with the AAMC, Research Activity of Full-Time Faculty in Departments of Medicine (Beaty et al., 1986; Association of American Medical Colleges, 1987). The parameters of research involvement were effort, funding, laboratory space, and publications. The study concluded that the median research effort of M.D. faculty in departments of medicine was 25 percent, compared with the 95 percent effort of Ph.D.s in the same departments. About 45 percent of the M.D.s and 68 percent of the M.D.-Ph.D.s reported that more than 20 percent of their effort was devoted to research. While 68 percent of the M.D. faculty had some form of external funding to support their research, only 23 percent of the M.D. faculty were principal investigators on an NIH grant. Twenty-five percent reported no research funding. Moreover, 34 percent of the M.D.s and 22 percent of the M.D.-Ph.D.s reported that they had no laboratory space. More striking was the fact that nearly half of the M.D. faculty had not published an original, peer-reviewed article (Association of American Medical Colleges, 1987). Ahrens has also reported that half of the clinical faculty in three departments of his three-department analysis did not publish at least one research article (Ahrens, 1992).
A 1989 follow-up study of internal medicine faculty revealed that there was no difference among M.D., M.D.-Ph.D., and Ph.D. faculty who had been or were principal investigators on a peer-reviewed research grant application (60, 61, and 58 percent, respectively). Although 52 percent of those conducting research were doing laboratory research, only 7 percent were performing patient-related research; 29 percent were involved in both (Levey et al., 1988).
ACADEMIC RECOGNITION
Promotions committees, and particularly tenure committees at competitive medical schools, require proof of a candidate's scholarly contributions.
However, what constitutes scholarship is not clearly defined. Although Boyer has suggested a broadening of what constitutes scholarly activity, over the past few decades scholarship in biomedicine has become equated with research, particularly laboratory-based research that frequently allows rapid data collection and publication (Boyer, 1987). Scholarship is, in turn, measured by one's ability to obtain competitive grant funds and publish results in peer-reviewed journal articles (Abrahamson, 1991; Applegate, 1990). Laboratory investigators, who devote all their time to research, usually have protected time to pursue research that is secured by grant funds. Clinical investigators, however, less frequently have grants to support their salaries and protect a segment of time to perform research activity. Thus, defining reliable measures of scholarship based on research activities for clinical investigators is much more difficult than for bench scientists (Bickel, 1991; Bickel and Whiting, 1991).
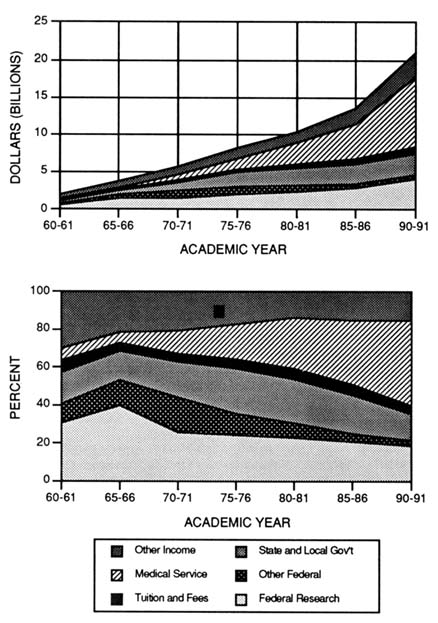
Physician faculty in clinical departments have certain patient care responsibilities that are distinctly different from those of physicians in independent research institutes, private industry, or preclinical departments (Blackburn, 1979). Clinical research faculty are generally hired to care for patients and teach clinical medicine to students, house staff, and clinical fellows—demands that are not made on nonclinical faculty. The economic necessity of maintaining a clinical department in financial balance has placed a greater emphasis on the clinical care component of a department's activities (Chin, 1985). Although a large portion of medical school revenues were previously derived from research funds, a review of medical school financing demonstrates that a growing fraction of medical school revenues are derived from professional practice plans (Hughes et al., 1991). During the late 1980s the revenues from professional services began to exceed those derived from research sources (Figure 2-7) (Ahrens, 1992; Jolin et al., 1992).
Although junior faculty members are recruited with the expectation that they will develop creative lines of investigation, the pressures of starting an academic practice, building a referral base, and contributing to departmental coffers can be overwhelming (Applegate, 1990; Jones et al., 1985). Academic health centers have contributed to these pressures and problems by imposing expanded funding expectations on young physician-investigators. It is believed that these investigators can support themselves with clinical income while performing pilot research studies and until they gain grant support. This also reinforces the disincentive to pursue clinical research when funding appears tenuous and encourages young investigators to pursue more secure career opportunities in bench research.
The perception that laboratory-based research is more scholarly and leads more readily to promotion lures junior faculty away from patient-based research. Moreover, while NIH and industry provide substantial sums of money for large, multi-institutional clinical studies and clinical trials, the principal investigators
are, of necessity, generally well-established senior investigators. For a newly independent junior faculty member, the inability to compete successfully for NIH funding, identify a unique research niche, and develop one's research independence seem to be insurmountable obstacles (Cohen, 1991). In addition, the necessity to participate in multicenter projects that require a large team approach is unappealing. Moreover, it takes many months for scientific and human protection committees to review and approve a human study protocol before patients can be enrolled in a clinical study. The new congressional requirement for subgroup analysis of women and minorities will also increase the size and cost of each clinical trial as well as the difficulty of enrolling patients into each trial. The time required to initiate, implement, and publish a human study is thus prolonged and arduous, and the potential number of publications from these studies over a similar period of effort is perceived to be fewer than that for laboratory-based research. Therefore, junior faculty perceive that the best route to promotion is development of a laboratory-based research effort. Laboratory experiments with well-established controls often can be completed rapidly; determining the clinical correlates in a patient-based clinical study can take years. Consequently, clinical research publications are frequently case reports or descriptive reviews of patients (Cadman, 1993).
FACULTY TRACKS
Perceptions of second-class faculty status abound in both camps of the medical school faculty. Some physicians feel that their laboratory-based Ph.D. colleagues regard them as having inferior training in scientific methods and, therefore, as being less sophisticated scientists. At the same time, the Ph.D. community sometimes feels that it is perceived as second-class faculty by its physician colleagues, particularly those with a primary appointment in a clinical department. Even Ph.D.s in clinical departments feel that they are viewed as outcasts by their Ph.D. colleagues in the preclinical departments. Although it is nearly impossible to diminish these perceptions, no empirical data exist to support the conjecture that one group is superior to or more productive than the other in conducting research. Each clearly has unique contributions to make to expanding the knowledge base of medical science.
Institutions have dealt with these issues through different means. Some institutions have established multiple career tracks for the physician faculty to recognize their different scholarly contributions (Bickel, 1991; Bickel and Whiting, 1991). For example, the Department of Internal Medicine at the University of Michigan initiated a two-track system for tenurable clinical faculty that is intended to define the expectations of departmental faculty by the department's leadership (Kelley and Stross, 1992). In addition to the nontenurable, full-time clinical faculty, tenurable faculty are divided into
physician-scientists and clinician-scholars. Although both groups are required to commit approximately 20 percent of their effort to teaching, the remaining time commitment is different for the two tracks. Physician-scientists are expected to commit the remaining 80 percent of their effort to research and receive departmental support for start-up, space, and personnel for initiating their research activities. Clinician-scholars are expected to spend 50 percent of their effort in the direct care of patients without a teaching component and 30 percent of their effort in research. Although clinician-scholars are not provided laboratory space, they do receive support for personnel, travel, computers, and other activities. The obvious advantages of a well-delineated multiple-track system are acknowledgment of the range of scholarly contributions that can be made by the clinical faculty and the fact that the expectations of performance and scholarship for all faculty groups are clearly defined at the outset.
Other institutions have remained committed to a single-track system, holding all faculty to the same academic standards for promotion. For example, Batshaw and others (1988) undertook an analysis of the single-track system at Johns Hopkins University School of Medicine to determine whether clinician-teachers were less likely to be promoted than the research-intensive faculty (Batshaw et al., 1988). The study concluded that there were no significant differences between the probabilities that clinical and research faculty would be promoted to either associate or full professor at Johns Hopkins University School of Medicine. Probably more significant was the fact that those who were promoted published nearly twice as many articles in peer-reviewed journals as those who were not promoted. No distinction was made between publishing clinical or basic science articles.
There is no easy way to change the perceptions about promotion and tenure. Each group has made significant contributions to building the knowledge base for medical care—basic scientists for their contributions in understanding fundamental biological processes, physician-scientists for translating new technologies to clinical practice, and clinician-scholars for their ability to implement new approaches based on sound scientific knowledge. Whether an institution has multiple tracks or not should not detract from the overall balance of objectives of the academic health center.
The committee believes that one avenue might be to encourage each group to gain an appreciation for the other's contributions. At least one institution, Tufts University School of Medicine, has implemented a course to provide Ph.D.s with the perspective of clinical sciences (Arias, 1989). The course is not intended to train Ph.D.s to become clinicians; its goal is to facilitate a dialogue between basic scientists and clinical investigators. Some professional societies are also adding symposia and instructional courses to the agendas of their annual meetings in an attempt to bridge the chasm between basic scientists and clinicians. For example, the American Federation of Clinical Research, the American Society for Clinical Investigation, and the American Association of
Physicians sponsor annual symposia on molecular biology for the nonmolecular biologist and clinical epidemiology and health services research for the novice. It is hoped that courses such as this will create a synergism from which new and exciting collaborations will ultimately flow. These types of linkages will become even more critical as the fruits of the biological revolution move toward human applications and the need to evaluate these new medical care practices grows.
COMPETING TIME DEMANDS
To reserve research time, an investigator must be able to garner research funds. To be competitive, an investigator must demonstrate competence in designing and conducting a research project. Even a small clinical study can require considerable funds and resources, including computers, data managers, research nurses, computers, and patients. Thus, protected time and a recruitment package, similar to those offered to junior laboratory-based investigators, must be made available to clinical investigators.
The ability to be a triple-threat (physician, teacher, scientist) may be limited in today's academic health care environment. Clinical faculty at all levels are required to maintain competence in their field of specialty or subspecialty to be board certified. The effects of the new policies regarding time-limited recertification recently implemented by many boards may have unintended negative consequences on clinical investigative careers. Clinical investigators need to be specialists in their areas of investigation and strive for academic recognition through scholarly contributions to the medical knowledge base. Recertification will require that a physician be competent in treating the broad spectrum of maladies in a particular subspecialty. However, this requirement seems to be in direct conflict with the goals of academic medicine, by which academically based physicians are frequently narrowly focused within the subspecialty in which they work to impart new knowledge about a particular disease or treatment thereof. Were they not so focused, it would be difficult to assess their scholarly contributions.
CLINICAL RESEARCH TRAINING
The training of clinical investigators has been fragmented and diverse (Levey, 1988). Many have had no specific research training other than the design and analysis of a research project during a subspecialty fellowship under the supervision of a mentor (Neinstein and Mackenzie, 1989; Burke, 1986). Some who are interested in epidemiology and outcomes assessment may have completed master's programs in public health either before or after obtaining
their M.D. degrees. The model that many clinical investigators have followed, however, is one or more years of laboratory-based research. In the efficient transfer of technology from the laboratory to the bedside and in the development of laboratory-based research to study questions arising in the clinical environment, an understanding of laboratory investigation can be invaluable (Littlefield, 1986). Although this model has been effective in allowing physicians to gain basic skills in research design and hypothesis testing, its effectiveness in providing the requisite skills for clinical research is unknown. It is believed that laboratory experience, however, is inadequate preparation for designing and conducting clinical research, which has its own set of methods, techniques, and ways of posing and answering relevant scientific questions using humans subjects (Feinstein, 1985a and 1985b; Fletcher et al., 1982; Janowsky et al., 1986; Nathan, 1988; Stolley, 1988).
Physicians who are trained exclusively in laboratory techniques may not be appropriately prepared to design and execute clinical studies without further clinical research training in fields such as biostatistics, ethics, regulatory issues, patents and licensing, pharmacology, and medical economics or other bridging disciplines. NIH supports a myriad of training programs that are available to physicians in various stages of training. As elucidated in Chapter 4, however, the overwhelming majority of programs are directed toward laboratory research. A few programs focus on human research or clinical epidemiology, such as the Robert Wood Johnson Clinical Scholars program, but outcomes data from these programs are sparse. The problem may be circular, in that the paucity of funds, perceived or real, for human studies, in turn, places a low priority on clinical research training. Therefore, resources are not allocated and clinical research training programs are not funded.
MENTORING
The importance of mentors and role models in the training pathways for research scientists of all types cannot be understated (Cameron, 1981). Although the literature is laden with the educational and training needs for physicians pursuing research career paths, scant attention has been paid to the roles and influences of mentors, advisers, or role models. Each of these is believed to play a crucial role in stimulating individuals to pursue a particular career path, shaping the content of their training, socializing them in the research environment, and providing support and guidance in the formative stages of their career (Swazey, 1994). Whereas being a role model is largely passive, the development of a mentor-protégé relationship is a gradual, interactive process that builds on interpersonal relationships. Unfortunately, few empirical data exist on the effects of mentoring, and adequate elucidation of what constitutes effective relationships between a mentors and trainees, and the effects of
mentoring on the developing clinical investigator have not been adequately addressed. Judith Swazey's white paper ''Advisors, Mentors, and Role Models in Graduate and Professional Education: Implications for the Recruitment, Training, and Retention of Physician-Investigators" (Swazey, 1994), explores the nature of each of these relationships in shaping a clinical investigator.
When internal medicine faculty were asked what factors most influenced their career choice to be a physician-investigator, a mentor was considered among the most important (Levey et al., 1988). A vigorous evaluation of the components of a successful academic career confirms the value of a mentor. The study by Levey et al. (1988) documented that the supporting and nurturing roles of a mentor during the first few years of faculty member's research experience were critical for launching a productive career. In addition to providing ongoing supervision and training and introducing the junior faculty member to the mechanics of being a successful investigator, the most respected mentors also offered emotional support.
Although many agree that mentoring is a significant force shaping the careers of young investigators, there is little consensus in the literature on the roles or responsibilities of a mentor (Calkins and Wakeford, 1982). Vance (1982) has encapsulated the essence of a mentor as "someone who serves as a career role model and who actively advises, guides, and promotes another's career and training" (p. 10). As Swazey points out in her paper a broad range of qualities, characteristics, and functions is ascribed to mentors (Swazey, 1994). A mentor can function as a coach, counselor, teacher, advocate, protector, sponsor, guide, and confidant. To this end, a mentor's activities include teaching cognitive knowledge and technical skills; developing the protégé's intellectual abilities; providing advice, encouragement, and criticism; helping their protégé learn risk-taking behavior, effective communications skills, and institutional and professional skills; fostering involvement in research and scholarly productivity; and facilitating entry into postgraduate or initial career positions and career advancement (Swazey, 1994). Swazey summarizes a good or successful mentor as one who is self-confident, willing to share, patient, understanding, available and accessible, willing to commit time and emotion to the mentor-protégé relationship, influential in one's field, and genuinely interested in the professional development of the protégé. Conversely, mentors should not be overprotective or supervise too closely, be harshly harshly critical or focus on inadequacies, be manipulative, withhold information, take over projects, or exploit the protégé. In conclusion, and effective mentor knows when to encourage independence and derives personal satisfaction in providing assistance and advice to help shape the career of a trainee without the expectation of being a part of the published accomplishments.
LIFESTYLE ISSUES
Similar to individuals in other professional careers, physicians in training pursue various career paths with the expectation that they will have rewarding employment opportunities upon completion of their training. The pathway to being a successful clinical investigator is not an easy one. It requires energy, drive, ambition, devotion, initiative, entrepreneurship, individualism as well as team work, and plenty of hard work (Rahmitoola, 1990). In return, fair compensation is essential to afford adequate housing, provide for a family, and purchase a reliable automobile, particularly at the junior faculty level.
Many trainees and junior faculty, however, perceive the financial security of an academic career as ephemeral. For many who have incurred large educational debt burdens during college and medical school, the financial insecurity of an academic career serves as a disincentive for choosing this career path. Many believe that the large educational debt, the discrepancy between the incomes of academically based physicians compared with those of physicians in private practice, the difficulty of garnering competitive research funding from NIH and other sources for basic as well as clinical research, and obstacles to advancement in the academic community discourage trainees from pursuing academic career paths (Hughes et al., 1991; Institute of Medicine, 1988a). The implications of debt and career choices will be covered more thoroughly in Chapter 4.
CONCLUSIONS
In conclusion, the committee believes that there are numerous hurdles confronting clinical investigators at all levels of faculty career development. Recognition in the academic health center includes promotion, protected time, and financial support. The scholarship of the successful clinical investigator should be appropriately recognized in the academic setting. This includes recognition that the nature of the clinical investigator's research, the sources of the funding, and the journals in which investigators publish may differ substantially from those of fundamental investigators.
Leadership at all levels within these institutions must define their expectations of junior faculty and support them so that these young men and women can meet and exceed the expectations. Teaching and serving as role models, advisers, and mentors are important in attracting students to careers in clinical investigation. These faculty activities, therefore, must be recognized and rewarded.
In addition to well-trained and adequately funded patient-based clinical investigators, the successful execution of patient-based clinical research requires a suitable institutional infrastructure. Similar to newly independent, laboratory-based
researchers, recruitment packages for clinical investigators should include protected time for setting up and conducting clinical studies as well as resources such as space, computer equipment, data management, and research support personnel.
University-based and research-intensive medical centers should develop mechanisms to achieve the optimal infrastructure to support inpatient-and outpatient-based clinical research. The features of such an infrastructure may include a clinical practice that is structured to deliver health care in a scholarly and investigative fashion and the integration of students, residents, fellows, and other health care professionals into human research activities. In addition, multidisciplinary facilities are required at universities to support core requirements for clinical research; these might include such elements as biostatistics, data management, and an opportunity to work with other health professionals. Creative start-up efforts through university mechanisms to establish core facilities that will seek continued funding through extramural sources represent important activities that should be strongly encouraged within the academic setting.
The committee believes strongly that the translation and application of advances in research to patient care require a strong partnership between academic institutions and industry. Facilitation of technology transfer by both parties is important and deserves special support. The relationship between faculty, the academic institution, and industry is changing dramatically and represents a new paradigm. This will require new standards in the definition and resolution of conflicts of interests at all levels in support of this change. Academia-industry relationships are covered more thoroughly in Chapter 5.