7
Medical Demography: Interaction of Disability Dynamics and Mortality
Kenneth G. Manton and Eric Stallard
As the elderly have become an ever-growing proportion of the American population, and as society has assumed some responsibility for their health, understanding the relationships among the factors that affect health has become crucial to policy makers. In this chapter we seek to build a framework for examining the interactions among the health-related behavior of individuals, genetic predispositions, the incidence of disease and fatality, the aging of the population, and levels of mortality and morbidity. Particularly crucial to policy makers is the relation between disability and mortality: When the incidence of disease or injury falls, so does the incidence of disability; and when death rates for people with a particular disability fall, that condition becomes more prevalent and thus demands on the health care system intensify.
To focus on the elderly demands a special approach because the mortality and health of the elderly and of younger people differ dramatically. The likelihood that someone suffers from multiple diseases, and from functional limitations, increases with age. Moreover, death in the old is due mostly to chronic diseases, with long histories. The models that apply to younger people, therefore, are not suitable for the analysis of the old.
Mortality is often studied with life tables estimated from vital statistics and census data. Life tables are useful for analysis of health policy and for social, epidemiological, and biomedical research. But they are deficient for refined analysis because they often lack information on the risks an individual faces. Everyone in a cohort—consisting, say, of all women, or of all
people aged 45 to 64—is assumed to face the same risks as everyone else; thus, such studies cannot be used to analyze such things as the change in the health of given individuals, nor are they useful for assessing the efficacy and cost of interventions.
Medical demography, the study of chronic disease, disability, and mortality in mature and aging populations, has roots in actuarial and biometric models of mortality and insurance of health-contingent events (Spiegelman, 1968). The tradition includes Graunt's ''bills of mortality" (1662), Bernoulli's life-table models of smallpox vaccination (1760), and the models of adult mortality devised by Gompertz (1825), Makeham (1867), Perks (1932), and Beard (1963a,b). Other well known examples include Clarke's use of "bioactuarial" models to isolate mortality associated with old age from mortality from exogenous causes (1950), and Bourgeois-Pichat's (1952, 1978) and others attempts to estimate the biological "limits" to life expectancy.
But medical demography lost impetus as research into the epidemiology of chronic disease specialized. That work, however, had its limitations in its reliance on case-control studies or studies of occupational cohorts and on longitudinal studies of selected populations from which it was difficult to estimate national rates of health events.
Recently, medical demography regained impetus for several reasons. First, concern has arisen because federal forecasts of mortality and population growth show biases with important implications for Social Security, Medicare, and other federal programs. The Social Security "crisis" of 1982-1983 showed that the population aged 65 and older was consistently underestimated, a bias that may still exist (Myers et al., 1987; Preston, 1993). Second, forecasts of the effects of disease on populations and of the health- and cost-effectiveness of interventions were often inaccurate (Walker, 1982; Frank et al., 1992). Third, the need to assess health trends and to characterize the natural history of chronic disease in the very old—those 85 or older— has intensified as life expectancy has lengthened and as that group has grown. Finally, longitudinal surveys of changes in the health of elderly Americans became available that were linked to Medicare data whose age reporting was better than that in decennial censuses (for example, the 1982, 1984, and 1989 National Long-Term Care Surveys, NLTCS).
Medical demography requires biomedically detailed models of the relation of age to health, to change in the ability to function, and to mortality in individuals. Biologically naive models do not accurately anticipate change in health or in the population health burden or the effects of intervention (Evens et al., 1992; Frank et al., 1992; Selikoff 1981; Tsevat et al., 1991). This is especially the case for the very old because of the special nature of the health processes of this group: they experience comorbidity—combinations of problems—impairment of function, a decrease in the ability to maintain biological stability with emergent nonlinearities in the change of
population health parameters. Such complex processes are often modeled using parameters estimated from multiple data sets, each with specific sets of biological measures.
Medical demography is crucial in research about aging populations and in analyses of policies affecting them because mortality and health are dramatically different among the elderly than they are among younger people. Thus, demographic models, developed initially for younger populations, must be modified to describe and forecast health changes at late ages. For example, mortality in the old is due mostly to chronic diseases with long natural histories. Furthermore, the likelihood that a person has multiple concurrent diseases, and functional limitations, increases with age. Standard life tables are not designed to model such processes; for one thing, cause-elimination life tables assume that diseases operate independently—an assumption that may better approximate the effects infectious diseases have on the mortality of younger people. To model processes that become more complex with age also requires data that are not available from the usual demographic sources—for example, combinations of data on mortality from vital statistics with data on health from longitudinal health surveys.
The need for medical-demographic analyses to describe health changes in the old has two aspects. First, to describe the effects of preventative and other public health interventions we need models that can both identify relevant inputs—say, risk factors for chronic diseases and the provision of health services—and accurately predict the influence of those inputs on health. Second, anticipating health and functional changes calls both for measures to describe the special health problems of the elderly noted above and for models to anticipate how observed health factors translate into future changes. For chronic diseases in the elderly these requirements entail a long time horizon because the latency of chronic disease ranges, for example, from 7 years for premenopausal breast cancer to 50 years for asbestos-determined lung cancer. Thus, one must recognize that the health of the elderly is subject both to biological inertia and to changes brought about by ongoing interventions, such as the National Cholesterol Education Program (Johnson et al., 1993; Sempos et al., 1993). Recognition of these factors will affect both models of health changes in elderly populations and models of their needs for services.
We explore these issues in the four sections of this chapter. First, we review methodological issues in modeling chronic disease processes such as the nature of hazard functions for chronic disease, the effects of time-varying covariates on health processes, cohort effects, and the mathematical relation of health changes in individuals and in aggregate populations. Second, we examine processes for individuals, relating the interactions of the natural history of a chronic disease with life stage. Doing so is necessary to make the models biologically realistic so that they can accurately predict
the effects of interventions. Third, we discuss the relation of disability and mortality; the measurement of disability in elderly persons; and the effects on measurement of using duration-based indicators of disability such as "active life expectancy." This discussion highlights the complexity of the health and functional status of elderly persons which requires assessments of multiple dimensions of function and the effects of comorbidity. Finally, we examine the role of genetics in shaping health in old age, which is different from its role at earlier ages because most lethal genetic defects are expressed by middle age. In elderly populations, health effects are polygenically determined and interact with environmental factors. Throughout, we discuss the use of primary data in estimation and of secondary data in determining model structure, because seldom will a single data set have the information necessary to estimate all relevant parameters for models of chronic disease and functional loss. This presentation assumes the reader has been exposed to the use of life tables, survival functions, hazard models, and common matrix and vector notation used in regression analysis.
Cohort Analysis and Time-Varying Covariates
The concepts of age, period, and cohort are basic in assessing the effect chronic disease has on the population. But they need careful definition to avoid the confounding that arises because cohorts are the interaction of age and period. We present, therefore, two definitions of a cohort. One is a "set" of persons who were all born in a particular year and thus are all the same age at any given point in time. Here the dynamics are demographic turnover—for example, passing age 65 or death. This is the standard concept of a cohort and is often used in gerontological and demographic research, though this work is hampered by the methodological problem of identifying age, period, and cohort parameters from aggregate data (see Schaie, 1983; Mason et al., 1981; and Hastings and Berry, 1979).
The second concept groups individuals, whatever their age, according to their exposure to a common experience at a specific time or place. A cohort might consist of the group of individuals who received a polio vaccination. This concept uses longitudinal microdata to estimate the parameters of a multidimensional, stochastic process that describes developments in the health of individuals. Mechanisms that are functions of the time lived represent aging. Period effects are exogenously generated perturbations, localized in time. Exogenous factors that permanently alter individual parameters are cohort effects. Thus, age, period, and cohort are identified with the temporal dependence of the parameters of processes of change in individual health. The designation of parameters to decompose the temporally changing correlations of multiple health variables permits the identification of the effects of age, period, and cohort (Feskens et al., 1991, 1992).
One cannot identify aggregate parameters for these factors using the variation of a single dependent measure—I.Q., for example—because within-cell variation is assumed to be "error." By relating age, period, and cohort parameters to individual health changes, one can construct a state-space model in which "state" is the individual's state of health measured by certain variables at a point in time and "error" is uncertainty about an individual's state. The variation in one individual's state from another's, or in his own over time, identifies the effects of cohort, age, and period.
These issues are illustrated by the individual failure process implicit in hazard models and explicit in state-space models. In a hazard model, the dependent variable is time to death for individual i (t i). In Figure 7-1, A, B, C, and D are hazards describing changes in the distribution of ti as fixed covariates are added. One could stratify the hazard on age, then period, and then cohort. As more covariates are added, the hazard approaches that for an individual—the "ultimate" stratification, described by curve D, that is, a "spike," or infinite hazard, at ti. As a consequence of adding covariates, the shape parameter, which controls the hazard's curvature with time, increases. When ti is known, the hazard is zero up to ti, and then it is infinite. The distribution function of ti, identical for everyone, is a distribution of the effects of unobserved variables over time. The individual's failure process is uninformative in these models (that is, mortality rates go from 0.0 to 8 instantaneously). The probability that, prospectively, ti can be determined exactly is vanishingly small; such models are not valid for predicting change.
Conditions for curve D occur frequently, as in aggregate data when the model is "saturated"—that is the number of data cells showing age by period effects and the number of parameters are the same—or when a hazard, estimated by maximum likelihood from ti's, degenerates into spikes when too many parameters are estimated. This situation can develop unexpectedly if ti is reported, not as a truly continuous variable, but grouped in temporal categories. Such "clumping" was found in data on unemployment duration when labor force reentry clustered at 13, 26, 39, 52 weeks, and so on, when unemployment benefits ran out (Heckman and Singer, 1984a,b). If not "adjusted" by, say, using dummy variables to filter out quarterly effects, the estimation of additional parameters caused the likelihood value to go to infinity. Problems also appear if the hazard rates change too rapidly, for example, declines in infant mortality in the first week, or month, of life may be so rapid that the actual information, and thus the degrees of freedom, is more limited than the sample size suggests (Potthoff et al., 1992). Both problems involve misspecification of the hazard function (Manton et al., 1992).
If continuous hazard functions with specific parameters are to be used to analyze health events, they must be substantively rationalized. The Weibull hazard function assumes that an event emerges after an individual takes m
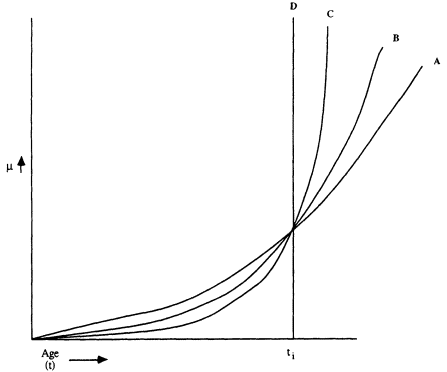
Figure 7-1 Illustrative hazard function for aggregate data. The hazard function µ(t) is the mortality rate for the infinitesimal interval ( t,t+Δt). Hence, µ(t)At is the probability of death between t and t+Δt for persons alive at t. The survival function S(t) is obtained from ![]()
The distribution function F(t), obtained from F(t) = 1-S(t), is the probability that death occurs at or before age t.
"hits."1 In carcinogenesis, hits are mutations in the genes in a cell controlling its growth and function. If, as for colon cancer, the number of mutations is known, then the shape parameter value, or possibly its range is known (Ashley, 1969; Fearon and Vogelstein, 1990). Using biological data to establish the shape parameter prevents hazard from going to infinity. Without ancillary data to fix the value (or range) of the shape parameter,
the hazard may become infinite. Thus, using a hazard model without a theoretical rationale relies on chance to avoid parametric saturation and a degenerate likelihood (Trussell et al., 1992).
To biologically justify a hazard function requires specification of a mathematical relation between the failure process for an individual and the distribution of times to death in a population. Using a Weibull, the times to tumor onset in a population have the same distribution as the time for the first cell, in an organ's population of cells, to acquire m errors. Functions with these special mathematical properties generate extreme-value distributions (for example, the Weibull and Gompertz; see Mann et al., 1974).
A hazard can be generalized by assuming that each person has his own scale parameter, (see, for example, the work of Vaupel et al. (1979) on modelling frailty). Then, no matter how a population is stratified, tihas irreducible variance. "Mixed" hazards use the marginal distribution of risk factors estimated from national surveys to identify fixed, and random, heterogeneity effects on mortality (Manton et al., 1993a). Slower age increases of the population hazard, assuming the individual hazard is a Weibull (cancer) or a Gompertz (total mortality), are produced both by the scale parameter being distributed over individuals (Manton et al., 1986), and by relating individual risks to a distribution of marginal risk factors. If the hazard is a convex function of risk factors, then the age trajectories of population and individual hazards are related by Jensen's inequality—E(µ(![]() )) = µ(E(
)) = µ(E(![]() ))—the average risk in a heterogeneous population (risk factors are represented by the vector
))—the average risk in a heterogeneous population (risk factors are represented by the vector ![]() ) is greater than (or equal to) the risk at the means of the risk factors E (
) is greater than (or equal to) the risk at the means of the risk factors E (![]() ). Because survivors have more favorable values of
). Because survivors have more favorable values of ![]() s, heterogeneity, regardless of its distribution, acts to decrease population risk with time.
s, heterogeneity, regardless of its distribution, acts to decrease population risk with time.
A hazard function implicitly has a parameter space with two dimensions, persons and time. In the extreme, there is either a time-dependent hazard with no individual heterogeneity, or a time-constant hazard with individual heterogeneity. To identify parameters, information on either individual failure, or risk differences, is needed. The correlation of parameters provides information on the relation of scale and shape parameters of the Gompertz (or other hazard) across populations or over species (Finch, 1990). In a stochastic process, risk-factors are time varying.
Macrolevel Models
Long time series of mortality—for, say, cancer deaths in the United States from 1950 on—can be used to model how vulnerable to specific diseases given cohorts have been. Trends in the causes of death must be distinguished from changes in the causes noted on death certificates; one example of the latter changes is the shift during the 1980s from listing
emphysema, bronchitis, and asthma to listing "chronic obstructive pulmonary disease." If conclusions made from these data are to be meaningful, the hazards must be carefully defined.
Mortality data are often used to complement biologically detailed models of health events in select, longitudinally followed populations because few longitudinal data sets are large enough to precisely estimate cohort trends for specific diseases to late ages. Carey et al. (1992) showed that distinguishing between mortality patterns at late ages requires a sample of 100,000 or more. Few longitudinal studies meet this requirement. Conversely, mortality data are insufficient to study survival at late ages when age reporting error may significantly affect the distribution of times of age at death (Kestenbaum, 1992).
The failure process for "mixed" hazards can be described by a "compartment model," that is, a discrete-state, continuous-time, stochastic process in which transitions to unobserved health states are estimated using biologically plausible functions to infer prior health changes from the age distribution of mortality. Compartment models were developed to assess multistate drug metabolism (Jacquez, 1972) and biological experiments (Matis and Wehrly, 1979). They can also be applied to cohort data to study a population's health "metabolism"—the rate at which persons move through specific, but unobserved, health states. For example, to evaluate the utility of mammography, cohort mortality from breast cancer for American women from 1950 to 1988 was modeled as a mix of early, premenopausal, disease and late, postmenopausal, disease: The characteristics of the former are that it is histologically aggressive, that it involves a strong family history, that it is estrogen receptor negative, and that is has a short latency, of 7 years. The characteristics of the latter are that it is fertility sensitive, that it involves a weak family history of the disease, that it is less histologically aggressive, that it is estrogen receptor positive, and that is has a longer latency, 14 years. Data on cohort mortality were combined with data from the National Cancer Institute's Surveillance of Epidemiological and End Results (SEER) program to estimate stage-specific survival rates in order to simulate the efficacy of different age and time schedules for mammographic screening; the measure of efficacy was changes in the proportion of females identified with Stage I disease. By distinguishing early and late disease, with different latencies and age-incidence patterns, different screening schedules were evaluated (Manton and Stallard, 1992a). Second, data on the mortality from lung cancer of cohorts of American men from 1950 to 1988 were linked to data from the National Health Interview Survey (NHIS) on smoking (Harris, 1983). Using the marginal cohort distribution of cigarette consumption, cohort-specific relative risks for smokers and the rate at which persons quit smoking were estimated (Manton et al., 1993a). Third, cohort mortality rates for lung cancer, and for all other causes, were estimated
simultaneously (Manton et al., 1993b). Fourth, U.S. mortality data organized by cohort were combined with (1) Weibull functions estimated from the incidence of mesothelioma (a type of lung cancer; Peto et al., 1982); (2), SEER-recorded incidence rates for mesothelioma (1975 to 1989); and (3) reported starts of asbestos exposure arranged in age by date matrices. The lack of detailed data on asbestos exposure necessitated the use of multiple data sources. Early exposures, in "insulation work equivalents" (assuming a linear dose response) were estimated using Weibull functions for specific cohorts to relate 15 years of mesothelioma incidence to reported "age by date" first responses. This assumes the validity of the multihit (Weibull) model of carcinogenesis for mesothelioma (Armitage and Doll, 1961). The use of time since first exposure, rather than age, in the Weibull, assumes that mesothelioma is due only to asbestos, and that other causes of death are elevated for persons with asbestos exposure (due to nonasbestos toxic work exposures). A table of estimated age by date of first exposure is used to forecast other asbestos-related diseases.
Thus, in these examples, combining data sources permitted analyses of specific diseases—though with limitations. Maximum likelihood procedures may not be optimal here because large samples may require smoothing parameter estimates for young and old cohorts with truncated mortality distributions (Manton and Stallard, 1992b). This is because sampling error is small relative to measurement error, and biases, such as right censoring of mortality and age changes in disease mechanisms, may dominate the variation of parameter estimates across cohorts. Second, a model's validity is based on its biological rationale. If there is no biological rationale to constrain model choice, a model fitting the data can always be found because of the inability to identify hazard functions in mortality data (Manton et al., 1994a).
Using clinical and experimental information to specify a model, and assessing it with cohort mortality data, depends on Bayesian principles because parameters are estimated conditionally on ancillary data. This approach differs from meta-analysis, which assesses the consistency of parameters across studies (Thompson and Pocock, 1991). A compartment model is tested against external data, say, cohort mortality rates from specific causes. Compartment models are exclusive: only the "best" studies are used in model development. Meta-analyses use all studies meeting specific criteria, which must be carefully examined to ensure that the selection is not biased. For example, "successful trials" are more likely to be published, and thus overrepresented in the literature, than are trials with negative results. Thus, the studies available in the literature may disproportionately represent certain outcomes. Second, the criteria used to select published studies influence the outcomes of meta-analysis. For example, meta-analysis was used to examine the relation of cholesterol to adverse health effects.
No study has yet shown a significant decline in total mortality produced by reducing serum cholesterol using drug therapy, though positive outcomes are shown for circulatory disease. Ravnskov (1992) argued that meta-analyses of cholesterol health effects are biased "samples" of studies.
Microlevel Models
Complementing mortality models are analyses of longitudinal microdata, in which the individual is modeled as a complex system whose evolution is governed by time-dependent processes operating at different levels of biological organization. In this view, aging is the loss of system integration—that is, increased entropy—and of homeostatic control of multiple linked processes (Firth, 1991; Goldberg et al., 1992). This type of model contains two types of jointly dependent processes. First, systems of autoregressive equations describe linked changes in J state variables, that is, xijt, (or the vector ![]() ), where j = 1, 2, ..., J and i indexes individuals,
), where j = 1, 2, ..., J and i indexes individuals,
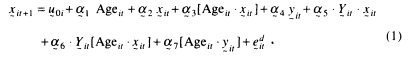
Ageit denotes the age of person i at t, ![]() are stochastic shocks,
are stochastic shocks, ![]() are exogenous variables, and
are exogenous variables, and ![]() is a matrix formed from the
is a matrix formed from the ![]() . The J trajectories described by (1) represent both fixed and stochastic effects. Fixed effects due either to genetics or to exposures to a risk prior to the study are represented by constants, (for example,
. The J trajectories described by (1) represent both fixed and stochastic effects. Fixed effects due either to genetics or to exposures to a risk prior to the study are represented by constants, (for example, ![]() ) or age changes (that is,
) or age changes (that is, ![]() ) of
) of ![]() . The expression
. The expression ![]() · Ageit may describe genetic age changes; for example, the age rate of loss of hepatic low-density lipoprotein receptors. These changes can be sex specific (Hazzard, 1990). Estimating an individual constant,
· Ageit may describe genetic age changes; for example, the age rate of loss of hepatic low-density lipoprotein receptors. These changes can be sex specific (Hazzard, 1990). Estimating an individual constant, ![]() , (or parameters of its distribution) requires multiple measures on each i, or assumptions about the distribution of
, (or parameters of its distribution) requires multiple measures on each i, or assumptions about the distribution of ![]() (or
(or ![]() ) over persons. Parameters might be estimated from longitudinal data on identical twins. Genetic disease may manifest itself early in a person's life; that is, the stronger the effect of a gene on disease, the higher the rate of early death (Beregi et al., 1991; Marriotti et al., 1992; Takata et al., 1987; Thieszen et al., 1990). For example, the risk of genetic dyslipidemic hypertension is manifest by age 40 and declines with age (Reed et al., 1991). Strong selection can generate a rapid rise in mortality in "mid" age (e.g., age 30-80), with mortality approaching a constant at late ages (Perks, 1932; Thatcher, 1992). Such age patterns, found by Carey et al. (1992) and Curtsinger et al. (1992) in insect models, are manifest in human populations for specific diseases, such as breast and lung cancer, and possibly for total mortality (Lew and Garfinkel, 1990).
) over persons. Parameters might be estimated from longitudinal data on identical twins. Genetic disease may manifest itself early in a person's life; that is, the stronger the effect of a gene on disease, the higher the rate of early death (Beregi et al., 1991; Marriotti et al., 1992; Takata et al., 1987; Thieszen et al., 1990). For example, the risk of genetic dyslipidemic hypertension is manifest by age 40 and declines with age (Reed et al., 1991). Strong selection can generate a rapid rise in mortality in "mid" age (e.g., age 30-80), with mortality approaching a constant at late ages (Perks, 1932; Thatcher, 1992). Such age patterns, found by Carey et al. (1992) and Curtsinger et al. (1992) in insect models, are manifest in human populations for specific diseases, such as breast and lung cancer, and possibly for total mortality (Lew and Garfinkel, 1990).
The term ![]() [Ageit ×
[Ageit × ![]() ] represents the alteration by risk factors of the age expression of genotype. For example, testosterone reduces hepatic LDL receptors and stimulates abdominal fat cells, which are more insulin resistant than are other fat cells (McKeigue et al., 1991). Insulin resistance may raise cholesterol and stimulate hyperinsulemia (Modan et al., 1991). The increase may be mitigated by the value (and age trajectory) of other variables, the body mass index (BMI) or the hematocrit.2 Differences in age trajectories of hematocrit may maintain sex differences in mortality at late ages (Heikinheimo et al., 1985; Sullivan, 1991).
] represents the alteration by risk factors of the age expression of genotype. For example, testosterone reduces hepatic LDL receptors and stimulates abdominal fat cells, which are more insulin resistant than are other fat cells (McKeigue et al., 1991). Insulin resistance may raise cholesterol and stimulate hyperinsulemia (Modan et al., 1991). The increase may be mitigated by the value (and age trajectory) of other variables, the body mass index (BMI) or the hematocrit.2 Differences in age trajectories of hematocrit may maintain sex differences in mortality at late ages (Heikinheimo et al., 1985; Sullivan, 1991).
The term ![]() represents sets of K exogenous factors,
represents sets of K exogenous factors, ![]() , k = 1,...,K. If K= 1,
, k = 1,...,K. If K= 1, ![]() is a scalar:
is a scalar: ![]() =
= ![]() . If K > 1,
. If K > 1, ![]() is a vertical "stack" of K, JxJ diagonal matrices, where the J diagonal elements of the kth matrix are
is a vertical "stack" of K, JxJ diagonal matrices, where the J diagonal elements of the kth matrix are ![]() . To conform with
. To conform with ![]() , a5 and a6 have J rows and JxK columns so the products a5 ×
, a5 and a6 have J rows and JxK columns so the products a5 × ![]() and ×
and × ![]() are JxJ. The term a5 ×
are JxJ. The term a5 × ![]() ×
× ![]() is the interaction of exogenous factors with state variables; a6 ×
is the interaction of exogenous factors with state variables; a6 × ![]() [Ageit ×
[Ageit × ![]() ] is the interaction of exogenous factors with age changes in state variables. If there is a "normal" trajectory of cholesterol metabolism, and it is affected by other characteristics, then
] is the interaction of exogenous factors with age changes in state variables. If there is a "normal" trajectory of cholesterol metabolism, and it is affected by other characteristics, then ![]() might reflect pharmaceutical control, that is, a drug's effect may be modulated by, say, BMI and age changes in lipid metabolism (Knapp et al., 1992). These interactions determine whether interventions affect mortality at late ages. Clinical studies suggest that some risk factors are significant to late ages; (in one example, treatment of isolated systolic hypertension reduced the risk of stroke; SHEP Cooperative Research Group, 1991).
might reflect pharmaceutical control, that is, a drug's effect may be modulated by, say, BMI and age changes in lipid metabolism (Knapp et al., 1992). These interactions determine whether interventions affect mortality at late ages. Clinical studies suggest that some risk factors are significant to late ages; (in one example, treatment of isolated systolic hypertension reduced the risk of stroke; SHEP Cooperative Research Group, 1991).
The terms in equation (1) involving ![]() reflect the effect of prior states on future states,
reflect the effect of prior states on future states, ![]() , that is, state dynamics. Diffusion (
, that is, state dynamics. Diffusion (![]() , where d is an age-dependent scale parameter) prevents ti from being "known." Unobserved stochastic processes,
, where d is an age-dependent scale parameter) prevents ti from being "known." Unobserved stochastic processes, ![]() ,also influence
,also influence ![]() . Inversely, temporal changes in
. Inversely, temporal changes in ![]() covariances may be used to infer the characteristics of
covariances may be used to infer the characteristics of ![]() , especially if
, especially if ![]() are measured often. The variables
are measured often. The variables ![]() may be manifest as high-order lags in equation (1) (Manton et al., 1993c). Lags may be described by integrating exposures to risk factors over time, for example, the number of years smoked multiplied by the average number of packs of cigarettes smoked— the "pack years"—reflects cumulative "damage."
may be manifest as high-order lags in equation (1) (Manton et al., 1993c). Lags may be described by integrating exposures to risk factors over time, for example, the number of years smoked multiplied by the average number of packs of cigarettes smoked— the "pack years"—reflects cumulative "damage."
The second type of process is described by a mortality function,
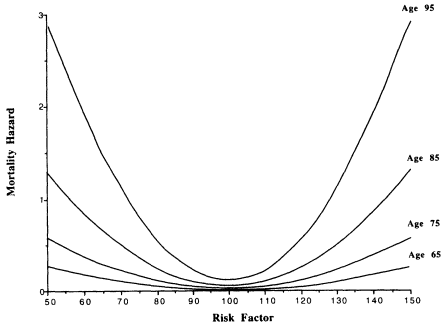
Figure 7-2 Univariate quadratic hazard function for a single risk factor ( x), for a fixed value θ = 0.0805, but at different ages. The quadratic hazard is drawn with the following parameter settings: µ(x) = (0.01+[(x-x*)/100]2)exp[0.0805(Age-65)], and x* = 100.
Equation (2) is a ''Gompertz" with the scale parameter replaced by a quadratic function of the realizations, ![]() , of the stochastic process in equation (1). In other words, equation (2) is dependent on time-varying covariates. The quadratic can be decomposed into terms for each of M diseases to allow risk factors to relate differently to different diseases (i.e., the
, of the stochastic process in equation (1). In other words, equation (2) is dependent on time-varying covariates. The quadratic can be decomposed into terms for each of M diseases to allow risk factors to relate differently to different diseases (i.e., the ![]() can be different). If θ represents the effects of unobserved age-related variables (
can be different). If θ represents the effects of unobserved age-related variables (![]() ) on mortality, senescence can be explicated by improving the measurements of the state variables
) on mortality, senescence can be explicated by improving the measurements of the state variables ![]() . Alternatively, a cause may have its own θm due to unobserved variable effects specific to m. θ declines in value as more of the age dependence due to senescence measured by θ is assignable to state variables (
. Alternatively, a cause may have its own θm due to unobserved variable effects specific to m. θ declines in value as more of the age dependence due to senescence measured by θ is assignable to state variables (![]() become more informative).
become more informative).
A quadratic function is used for several reasons. A U- or J-shaped function describes the relation of mortality to many risk factors (Jacobs et al., 1992; Neaton et al., 1992). The curvature of the quadratic is a function of θ, so the rate of change of risk factor effects on mortality that is related to age reflects interactions with unobserved variables, ![]() . The function with θ = 0.0805 is shown for select ages in Figure 7-2. The horizontal axis
. The function with θ = 0.0805 is shown for select ages in Figure 7-2. The horizontal axis
represents x; x°is a value producing the lowest mortality; for example, µ(x°) = .01 at age 65. The vertical axis is the mortality level. As age increases from 65-95, with θ and ![]() fixed, mortality increases.
fixed, mortality increases.
Changes in θ are illustrated in Table 7-1 for the 34-year follow-up of 10 risk factors from the Framingham Study: 7 dimensions identified from 27 functional and physical performance items for the 1982-1984 NLTCS and mortality for 1982-1986; and 7 dimensions from the 1982-1984-1989 NLTCS and mortality for 1982-1991. For Framingham, risk factors reduce the male θ form 9.4 percent to 8.1 percent, a relative decline of 14 percent. For females, the relative decline in θ is 19 percent, from 10.0 to 8.1 percent. The relative decline of θ using 1982-1984 NLTCS functional scores is 51 to 61 percent. Thus, functional scores described the age dependence of death better than risk factors (Campbell et al., 1985; Dontas et al., 1991; Grand et al., 1990). This finding is consistent with decreased physical activity being a major risk factor at late ages: 56 percent of deaths in a population whose mean age was 84.5 years were due to pulmonary embolism, congestive heart failure, or pneumonia—all diseases associated with reduced activity (Gross et al., 1988). Conditioning θ on functional status, suggests that mortality rises 3.6 to 4.0 percent per year of age (thus it doubles in 17-19 years) compared with a doubling of mortality in 6.9 years for a θ of 10 percent. Controlling income and education, as well as function, reduced θ to 2.6 percent. For the 1982-1984-1989 NLTCS, the relative decline in θ is smaller (35 to 48 percent) because, over the longer period 1984-1989, intermediate transitions cause information in the 1984 scores to decay.
A second measure of information is the proportion of χ2 explained by ![]() (that is, test 2, with θ = 0.0). In the Framingham study, risk factors explain 70 percent of the χ2 due to age in the mortality model. In the 1982-1984 NLTCS, 92-95 percent of the χ2due to age is explained. In the 1982-1989 NLTCS, function accounts for 79 percent and 87 percent (for males and females, respectively) of the χ2 explained by age. The decline in the age variation of mortality explained by function for 1982-1989 data is smaller (14 and 7 percent for males and females) than the relative changes in θ, 24.1 and 23.3 percent. Thus, loss of the ability to explain the age dependence of mortality between 2- to 5-year intervals is moderate and similar to that for other types of survey error. θ adjusts for differences in the quantity and type of
(that is, test 2, with θ = 0.0). In the Framingham study, risk factors explain 70 percent of the χ2 due to age in the mortality model. In the 1982-1984 NLTCS, 92-95 percent of the χ2due to age is explained. In the 1982-1989 NLTCS, function accounts for 79 percent and 87 percent (for males and females, respectively) of the χ2 explained by age. The decline in the age variation of mortality explained by function for 1982-1989 data is smaller (14 and 7 percent for males and females) than the relative changes in θ, 24.1 and 23.3 percent. Thus, loss of the ability to explain the age dependence of mortality between 2- to 5-year intervals is moderate and similar to that for other types of survey error. θ adjusts for differences in the quantity and type of ![]() to better embed the estimated discrete-time process in the underlying continuous-time process, and thus reduces bias.
to better embed the estimated discrete-time process in the underlying continuous-time process, and thus reduces bias.
Other reasons for using a quadratic is that it describes homeostasis in an organism (that is, negative feedback keeps an individual's state within viable regions of ![]() ). The quadratic defines a point at which mortality is minimized:
). The quadratic defines a point at which mortality is minimized:
TABLE 7-1 Chi-Squared Values Associated with the State Variables, ![]() , and with the Senescence Process θ in Cause-Specific and Total Mortality Functions
, and with the Senescence Process θ in Cause-Specific and Total Mortality Functions
|
Data Source, Test |
Males |
Females |
||
|
Number (n), and Descriptiona |
χ2n |
χ2n/χ21(%) |
χ2n |
χ2n/χ21(%) |
|
Framingham: 10 risk factors |
||||
|
1. Full process |
2,174.8 |
100.0 |
2,047.8 |
100.0 |
|
2. |
1,518.8 |
69.8 |
1,445.5 |
70.6 |
|
3. Effect of θ |
656.0 |
30.2 |
602.3 |
29.4 |
|
|
(θ = 0.0805) |
|
(θ = 0.0812) |
|
|
4. θ alone, no |
1,350.4 |
62.1 |
1,406.1 |
68.7 |
|
|
(θ = 0.0939) |
|
(θ = 0.1002) |
|
|
1982-1984 NLTCS: 7 functional scores (based on 27 attributes) |
||||
|
1. Full process |
3,206.5 |
100.0 |
4,728.1 |
100.0 |
|
2. |
2,945.9 |
91.8 |
4,467.5 |
94.5 |
|
3. Effect of θ |
260.6 |
8.2 |
260.6 |
5.5 |
|
|
(θ = 0.0401) |
|
(θ = 0.0364) |
|
|
4. θ alone, no |
1,163.6 |
36.3 |
2,210.6 |
46.8 |
|
|
(θ = 0.0811) |
|
(θ = 0.0937) |
|
|
1982-1984-1989 NLTCS: 7 functional scores (based on 27 attributes) |
||||
|
1. Full process |
4,837.9 |
100.0 |
7,493.8 |
100.0 |
|
2. |
3,821.5 |
78.9 |
6,550.5 |
87.4 |
|
3. Effect of θ |
1,016.4 |
21.1 |
943.3 |
12.6 |
|
|
(θ = 0.0528) |
|
(θ = 0.0475) |
|
|
4. θ alone, no |
2,662.2 |
55.0 |
4,466.0 |
59.6 |
|
|
(θ = 0.0815) |
|
(θ = 0.0910) |
|
|
a For tests 1, 2, and 4, the baseline model for comparison assumes constant mortality for all ages and risk factor values. Test 3 compares the models in tests 1 and 2. SOURCE: Data are from the Framingham Heart Study and the 1982, 1984, and 1989 National Long-Term Care Surveys. |
||||
The second expression arises if Ageit is not in ![]() , (for example, if age's effects are represented by θ), with the implication that
, (for example, if age's effects are represented by θ), with the implication that ![]() is constant. If age is in
is constant. If age is in ![]() ,
, ![]() is a linear function of age. It is also unlikely that a hazard with greater than second-order terms can be estimated in most data sets. The multivariate normal distribution of
is a linear function of age. It is also unlikely that a hazard with greater than second-order terms can be estimated in most data sets. The multivariate normal distribution of ![]() , implied by a quadratic hazard, is the statistically most conservative estimator of a multivariate distribution with higher-order moments (>2) because it has the maximum entropy of any distribution with a fixed covariance matrix.
, implied by a quadratic hazard, is the statistically most conservative estimator of a multivariate distribution with higher-order moments (>2) because it has the maximum entropy of any distribution with a fixed covariance matrix.
The interaction of a quadratic hazard and linear dynamics preserves properties of the ![]() distribution that other hazard functions do not. The quadratic mortality matrix
distribution that other hazard functions do not. The quadratic mortality matrix ![]() =
= ![]() + ... +
+ ... + ![]() reduces the variance-covariance matrix of
reduces the variance-covariance matrix of ![]() in each measurement interval for each of M causes: it naturally parameterizes cause-specific mortality changes. The logistic only approximates a hazard (the dependent variable is the log of the odds ratio, p/(1-p), where p is the event probability). If one decomposes data by time, or cause of death, a logistic estimated for each interval, or cause, cannot be recomposed to generate a logistic for total time, or mortality, because the product of logistics is not logistic (Woodbury et al., 1981). Estimates from the Cox model (1972) are not consistent if cause-specific rates are not proportional over age; if, for example, exponential hazards are estimated for three causes, (say, cardiovascular disease (CVD), cancer, and other), the three functions produce a sum of exponentials so coefficients for total mortality cannot be compared with coefficients in cause-specific functions. The Cox model also assumes that the population is risk homogeneous and that competing risks are independent (Gill, 1992). Furthermore, in the quadratic the matrix of second-order partial derivatives of µ(·) is independent of
in each measurement interval for each of M causes: it naturally parameterizes cause-specific mortality changes. The logistic only approximates a hazard (the dependent variable is the log of the odds ratio, p/(1-p), where p is the event probability). If one decomposes data by time, or cause of death, a logistic estimated for each interval, or cause, cannot be recomposed to generate a logistic for total time, or mortality, because the product of logistics is not logistic (Woodbury et al., 1981). Estimates from the Cox model (1972) are not consistent if cause-specific rates are not proportional over age; if, for example, exponential hazards are estimated for three causes, (say, cardiovascular disease (CVD), cancer, and other), the three functions produce a sum of exponentials so coefficients for total mortality cannot be compared with coefficients in cause-specific functions. The Cox model also assumes that the population is risk homogeneous and that competing risks are independent (Gill, 1992). Furthermore, in the quadratic the matrix of second-order partial derivatives of µ(·) is independent of ![]() , that is,
, that is,
Thus, interactions of risk factors are constant within age strata. Since the inverse of equation (4) appears in equation (3), all these interactions are represented in ![]() . Introducing quadratic terms in a Cox model does not preserve these properties, for one thing, quadratic effects are scale dependent.
. Introducing quadratic terms in a Cox model does not preserve these properties, for one thing, quadratic effects are scale dependent.
Estimation of equations (1) and (2) assumed that the likelihood for a longitudinal study can be factored conditionally on ![]() . To integrate parameter estimates from (1) and (2) in life tables, difference equations are needed. Three describe mortality dynamics. Survival is
. To integrate parameter estimates from (1) and (2) in life tables, difference equations are needed. Three describe mortality dynamics. Survival is

where ![]() =
= ![]() ,
, ![]() =
= ![]() , and
, and ![]() =
= ![]() are from (2),
are from (2), ![]() are risk-factor means, and
are risk-factor means, and ![]() is the risk-factor covariance matrix at t. The vector of mortality-adjusted risk factor means is
is the risk-factor covariance matrix at t. The vector of mortality-adjusted risk factor means is
Mortality-adjusted variances are
After adjusting for mortality, the ![]() of survivors changes:
of survivors changes:
where ![]() and
and ![]() are coefficients in (1). The covariance matrix adjusted for dynamics is
are coefficients in (1). The covariance matrix adjusted for dynamics is
where ![]() is the error covariance matrix at age t + 1. For functional scores, which sum to 1.0 and are nonnegative, diagonals of
is the error covariance matrix at age t + 1. For functional scores, which sum to 1.0 and are nonnegative, diagonals of ![]() are bounded by Bernoulli variance requiring constraints in equation (9) and on
are bounded by Bernoulli variance requiring constraints in equation (9) and on ![]() in equation (1) (Manton et al., 1993c). Equations (5) through (9) are used in health forecasts and simulations.
in equation (1) (Manton et al., 1993c). Equations (5) through (9) are used in health forecasts and simulations.
To test the model, first, standard errors of coefficients in equations (1) and (2) are calculated. Second, trajectories of the ![]() and
and ![]() are compared with external data. Examining these trajectories requires more data, and is more stringent, than evaluating a hazard's prediction of ti. In Table 7-2, we illustrate the effects of state dynamics. The life tables used parameters estimated from the 25-year follow-up of the Finnish East-West study in equations (5)-(9) (Pekkanen et al., 1992). If life tables are calculated with both
are compared with external data. Examining these trajectories requires more data, and is more stringent, than evaluating a hazard's prediction of ti. In Table 7-2, we illustrate the effects of state dynamics. The life tables used parameters estimated from the 25-year follow-up of the Finnish East-West study in equations (5)-(9) (Pekkanen et al., 1992). If life tables are calculated with both ![]() fixed and
fixed and ![]() =0.0, (assumption 1) there is a 32-33 percent upward bias in life expectancy. With only
=0.0, (assumption 1) there is a 32-33 percent upward bias in life expectancy. With only ![]() = 0.0 (assumption 2) the bias is 10-15 percent. The addition of time-varying covariates (assumption 3) reduces error to 0.4-0.6 percent.
= 0.0 (assumption 2) the bias is 10-15 percent. The addition of time-varying covariates (assumption 3) reduces error to 0.4-0.6 percent.
The importance of time-varying covariates, and the effects of specific hazard functions on results, is now realized by epidemiologists. In Gordon et al. (1989), identification of the importance of HDL cholesterol in U.S., but not British, studies was traced to the use of different hazard models. Regression dilution is believed to have caused the effects of cholesterol on mortality to be underestimated (Cooper et al., 1992; Davis et al., 1990;
TABLE 7-2 Life Expectancy at Age 40 Under Alternative Assumptions About Risk Factor Dynamics in 25-Year Follow-up of Finnish East-West Study
|
|
Life Expectancy, e40 (years) |
||
|
Assumption |
East Finland |
West Finland |
Description |
|
|
29.5 |
31.8 |
Life table |
|
1 |
39.0 |
42.2 |
Risk estimated for baseline |
|
|
(+32.2%) |
(+32.7%) |
risk factor measurements |
|
2 |
32.5 |
36.6 |
Risk estimated from risk |
|
|
(+10.1%) |
(+14.9%) |
factor means and variances/ covariances |
|
3 |
29.6 |
32.0 |
Risk factor distribution |
|
|
(+0.4%) |
(+0.6%) |
changes according to regression estimates |
|
SOURCE: Data from Pekkanen et al. (1992). |
|||
Jacobs et al., 1992), emphasizing the need for multiple measurements to better identify their true level.
θ can be used to adjust ![]() for unobserved health differences between populations so that national mortality data that are unbiased, but uninformative about disease mechanisms, can be integrated with longitudinal select population data that may be biased for the national population being studied. Thus, the state-space model can reduce bias in integrating multiple survey and demographic data sources in cross-national studies (Dowd and Manton, 1990). Initial age- and sex-specific risk-factor conditions (
for unobserved health differences between populations so that national mortality data that are unbiased, but uninformative about disease mechanisms, can be integrated with longitudinal select population data that may be biased for the national population being studied. Thus, the state-space model can reduce bias in integrating multiple survey and demographic data sources in cross-national studies (Dowd and Manton, 1990). Initial age- and sex-specific risk-factor conditions (![]() and
and ![]() ) can be estimated from cross-sectional survey data. From national vital statistics, the proportion of mortality for each of M causes can be determined. Because θ represents the average age-related effects of
) can be estimated from cross-sectional survey data. From national vital statistics, the proportion of mortality for each of M causes can be determined. Because θ represents the average age-related effects of ![]() , it reflects unmeasured differences between sources of population data just as it adjusts for unobserved variable effects when different risk factors, or measurement intervals, are used.
, it reflects unmeasured differences between sources of population data just as it adjusts for unobserved variable effects when different risk factors, or measurement intervals, are used.
Dependent risks can be identified using time-varying state variables measured before death (Tsiatis, 1975). Assessment of dependence suggests that prevention can, by changing xijt, affect other risk factors and several causes of death and thus affect health more than would a treatment that reduces mortality from a specific cause. The dependence of diseases does not have a large effect until mortality risks are high enough to deplete the
high-risk groups. Thus, dependence is important at late ages, when most deaths occur and the trajectory of mortality is uncertain. The existence of cause dependency and risk-factor interactions suggests that traditional cohort methods need strong assumptions to reconstruct mortality at late ages. Counts of deaths at late ages, by definition, are small and uncertain, and they reflect nonlinear state dynamics.
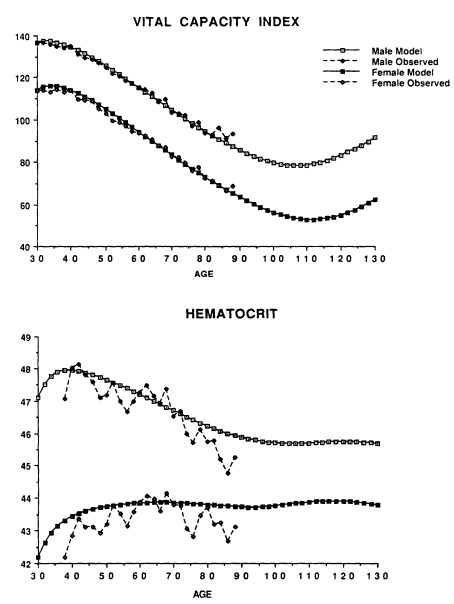
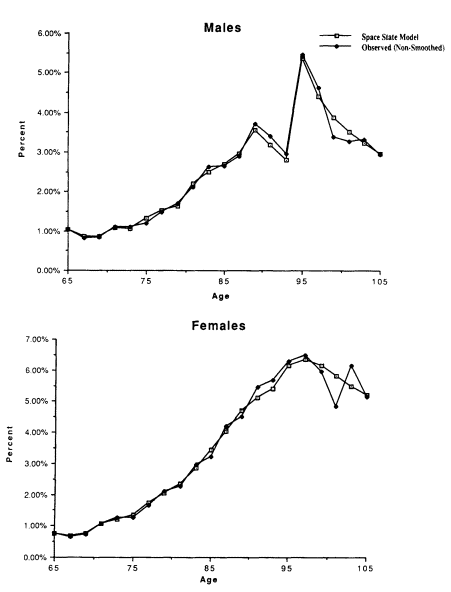
Although equation (1) is linear, its use in equations (5) through (9) can produce nonlinear effects, like sex-specific age changes of the means of hematocrit and the vital capacity index (VCI). In Figure 7-3a, the VCI means decline, as expected, until age 105. This pattern is due to the exponential increase of mortality with age which, by 95, is so large that risk-factor means for survivors (![]() ) must approach
) must approach ![]() . In Figure 7-3b, the hematocrit means for females remain lower, even postmenopausally, than male hematocrit means, which decline after reaching a peak (Sullivan, 1991).
. In Figure 7-3b, the hematocrit means for females remain lower, even postmenopausally, than male hematocrit means, which decline after reaching a peak (Sullivan, 1991).
Failure to understand risk-factor interactions and dynamics may be why prevention trials do not reduce mortality by the amount suggested in population studies. A logistic coefficient does not show how intervention changes other risk factors over time. In a state-space model, the dynamic equations describe how changes in risk factors interact over time. Indirect risk-factor effects may be positive or negative. Diuretic use in diabetics decreases blood pressure, but elevates cholesterol and blood glucose: one risk factor is reduced, but several increase. In postmenopausal women with osteoporosis and reduced estrogen, atherogenesis accelerates because increased cholesterol and calcium release into the blood, raises the calcification rate of arterial plaques (Moon et al., 1992). Treatment of osteoporosis with estrogens has beneficial effects on multiple risk factors and outcomes and may produce improvements larger than those measured in population studies (Stampfer et al., 1992).
Because of diffusion, the uncertainly of forecasts from state-space models is higher than is the uncertainty of forecasts from aggregate models. This difference can be represented in aggregate forecasts using empirical Bayes methods (see, for example, Manton et al., 1989). Uncertainty may be dealt with by imposing a utility function on the outcome distribution, discounting the costs of some and increasing costs of others. Confidence in a decision may increase when outcomes are weighted. For example, the answer to the question of whether shortfalls in Social Security trust funds are as important as, or more important than, excesses could reduce uncertainty about decisions on marginal tax rates.
Thus, to deal with cohort effects in medical demography, one needs both macrolevel compartment models represented by differential equations with parameters specified from biomedical data, or microlevel state-space models estimated from longitudinal data in which measurements of multiple risk factors are made. The procedures are complementary. Estimates from
the one may be used to help specify and estimate the parameters of the other.
DISEASE STAGES, NATURAL HISTORY, AND THE LIFE-CYCLE
Because chronic diseases take a long time to develop, they cannot be treated as events. They must be modeled as processes, with characteristic (and lengthy) natural histories whose evolution interacts with the characteristics of the person suffering from the disease. Representing these effects by the age dependence of mortality presents problems because changes in the age dependence may not be recognized for several reasons: reliance on standard hazards like the Gompertz, analyses of the logarithm of rates—a transformation that hides significant deviations, and the use of statistically inefficient estimators (like ordinary least squares). Despite improvements in the quality of data for late ages, reliance on assumptions about the age trajectory of mortality is common. (See, for example, National Center for Health Statistics, 1987; Lee and Carter, 1992). Human mortality at advanced ages often deviates from the Gompertz (Bayo and Faber, 1985; Kestenbaum, 1992; Thatcher, 1992).3 Although human data are subject to age misreporting 4, that alone does not explain all deviations from a Gompertz. Making assumptions about the tail of the distribution of human ages at death is similar to designing experiments assuming that the Gompertz is valid, and making studies large enough to estimate Gompertz parameters but not large enough to test alternative models. Even if a Gompertz fits cohort data, it is not clear what to expect in cross-sectional data representing a changing mix of cohorts with different parameters (Manton et al., 1986).
Not all risks of chronic disease increase monotonically with age. Osteo-arthritis, for example, decreases after age 75 (Bagge et al., 1992); and if they survive to middle age, persons with familial high cholesterol appear to have normal survival. Furthermore, persons predisposed to a disease are selected out of the population or, if not selected out, have the disease controlled. As diseases are controlled, the age trajectory of mortality changes shape.
Medical demography is concerned not only with the lifetime distribution of health events, but also with their distribution within life stages, in
which health is dominated by specific diseases. Disease models with differing time scales, and with more detail about the effects of age on mortality and risk-factor processes, are required to design interventions. Prevention or treatment may have larger effects if introduced before significant organ damage occurs (as they do in the case of osteoporosis, Overgaard et al., 1992), and renal function loss in diabetics (Chan et al., 1992). Diseases once limited to a certain life stage may become lifelong, with multiple recurrences, and require medical surveillance and intermittent treatment. Early-stage, premenopausal breast cancer, treated successfully, may recur 30 years later if the disease reflects immunological defects. Below we briefly review the characteristics of several chronic conditions or syndromes important in elderly populations.
Dementia
Diseases that are prevalent at late ages include Alzheimer's and related dementias. Alzheimer's has a long natural history, with death often due to comorbidity; in one study, 70 percent of deaths were due to pneumonia (Burns et al., 1990). Data from the Baltimore study of aging suggests that dementia cases, with good care, may live nearly normal life spans. Two difficulties in studying Alzheimer's disease are that its progression is indicated by slow changes on multiple cognitive dimensions and that it often coexists with other types of dementia.
Heart Disease
Heart disease progresses over time. Onset of the disease at early ages is often caused by genetic factors. Factors that affect heart disease between ages 30-50 may be quite different to those affecting the older population.5 Treatment is effective early in a heart attack. Besides improving function, coronary bypass surgery in patients over age 80 did much better than medical treatment in increasing 3-year survival: the ratios were 77.4 percent and 55.2 percent, respectively (Ko et al., 1992). As procedures have improved, the benefits of surgery have increased (Muhlbaier et al., 1992). If persons survive early heart disease, they may later develop chronic health failure
(CHF) and left ventricular hypertrophy (LVH) because of the interaction of reduced peripheral circulation, reduced cardiovascular efficiency, and hypertension (Kitzman and Edwards, 1990; Lakatta, 1985). The age-standardized U.S. hospitalization rate for CHF from 1973-1986 increased 60 percent (Ghali et al., 1990). Now both CHF and LVH are treatable using ACE-II inhibitors (SOLVD Investigators, 1991; Weber and Brilla, 1991).
The effect of cholesterol on CVD varies with age, especially for women (Jacobsen et al., 1992; Knapp et al., 1992). This variation may be due to a U-shaped relation of cholesterol to total mortality and to the fact that some premenopausal women have cholesterol low enough to raise other disease risks (see, for example, Neaton et al., 1992). Thus, when cholesterol rises postmenopausally for some women, risks could decline.6
Nutritionally Related Disorders: Systemic Factors
A newly appreciated aspect of chronic disease is the effect of nutrition on antenatal development. The data suggest that maternal malnutrition, which produces low birth and placental weight, affects the fetal development of multiple organs and that these effects become manifest above age 65 as chronic diseases (Barker, 1990; Barker and Martyn, 1992; Barker et al., 1989, 1991a,b, 1992a,b,c). Fetal physiology requires the brain to receive nutrition at the expense of other organs. The liver can be damaged, affecting fibrinogen and other hemostatic factors and increasing CVD risk (Barker et al., 1992a; Barker and Martyn, 1992). Lung and pancreatic function can be impaired, so that chronic lung disease and adult-onset diabetes mellitus appear.
The effects of antenatal nutrition on chronic disease may explain long-term changes in the risks of chronic disease. Despite literature suggesting that chronic diseases are consequences of industrialized society (Dubos, 1965; Omran, 1971), declines of some of those diseases started long before major prevention efforts. Antihypertensive therapy was first introduced in the 1950s, and a national program did not begin until 1972-1973. Yet, U.S. mortality from stroke declined after 1900—41.7 percent from 1900-1948, for example. An analysis of diagnostic practices and coding on death certificates suggests that declines were real by 1925 (Lanska and Mi, 1993).
Research by Fogel at the University of Chicago shows that chronic disease rates were higher for Civil War veterans aged 65 in 1910 than for veterans over age 65 in the 1985-1988 NHIS. The decline per decade in chronic disease was 6 percent over the 75 years—a decline that correlated with changes in body mass and stature. Heart disease was 2.9 times more common in the 1910 cohort of veterans than it was for veterans in 1985-1988. This work, for which Fogel won the 1993 Nobel Prize in economics, is consistent with the antenatal nutrition model.
Micronutrients may have long-term effects on disease. Zinc governs birth weight, and males are susceptible to gestational zinc deficiency (Andrews, 1992; Hales et al., 1991). Zinc deficiency affects both adult-onset diabetes mellitus and schizophrenia, diseases whose incidence is correlated. Recently, it was recommended that women of child-bearing age take folic acid supplements because deficiency early in fetal development is responsible for 60 percent of birth defects of the neural tube—spina bifida, for example, Vitamin B and other deficiencies may be related to late-age dementia (Zaman et al., 1992; Martin et al., 1992). Thus, there is a linkage of health in the antenatal and later life stages due to deprivation of both macro- and micro-nutrients at childbearing ages. If maternal nutrition varies over cohorts (and, within cohorts, by socioeconomic status at childbearing ages), then those effects must be distinguished from genetic factors. What look like genetic effects could be the effects of low socioeconomic and cultural status that persist in families from one generation to another.
Immunologically Related Diseases: Interactions of Viral and Nutritional Factors
Nutrition affects the immune system. Some chronic diseases, are due to early viral infections; for example, cytomegalia virus is implicated in CVD (Mozar et al., 1990). Viruses may trigger autoimmune diseases (like rheumatoid arthritis and systemic lupus erthymatosis). Some of these diseases may moderate with age. Other diseases like humoral autoimmunity (i.e., the prevalence of antinuclear antibodies) or multiple myeloma (a form of cancer) may increase with age (Beregi et al., 1991). Nutritional supplements may be important in changing immunological responses with age. For example, age-related loss of gastric immunity is reversed by supplementation with vitamins A, C, and E (Penn et al., 1991a,b).7 Other examples include recent studies showing significant effects, starting after 1 or
2 years, of antioxidant supplements—beta carotene, vitamin E, and selenium—on total, cancer, and stroke mortality (Blot et al., 1993).
Nutritional and other types of supplementation for the elderly is complex because of the need to maintain homeostasis. CVD is reduced by estrogen replacement, a result correlated with improvement in status on multiple risk factors (Nabulsi et al., 1993). However, when that therapy is combined with vitamin D, lean women showed no improvement in cholesterol (Mysrup et al., 1992). Hypercalcemia, produced by vitamin D, raised CVD risk without an increase in cholesterol (Moon et al., 1992). Thus, though nutritional and hormonal supplementation are important at late ages, its parameters, and their linkage, are not yet clear. Furthermore, the most biologically active form of many micronutrients is not known.8 Consequently, trials of nutritional interventions must rely heavily on laboratory data (Prasad and Edwards-Prasad, 1992).
Multiple Diseases, Host Factors, and Their Interactions at Late Ages
Analysis of age differences in disease and risk-factor processes requires biologically detailed models in which failure is multidimensional, each dimension potentially having its own time scale. A state-space model has this capability if a θ is assumed for each disease. For breast cancer and Alzheimer's disease, one must identify early and late disease with different etiologies, genetic determinants, and rates of progression. In Manton et al. (1993c) the quadratic estimated from all deaths behaved differently from a quadratic that was the sum of three disease-specific functions (with a single θ). Time functions can differ by disease: the quadratic for cancer could be estimated with a Weibull—not a Gompertz. M causes, with different θs, can be summed if the causes are disjoint (Manton and Stallard, 1988).
Some life-cycle effects, if ![]() explains much of the variation associated with θ, can be represented in equation (1). For example, adult-onset DM lowers the age at death for multiple conditions (Goldstein et al., 1978; Jones, 1956). So, DM could be expressed as a rapid increase of blood glucose (and its variance) with age in (1), which increases mortality by raising risk-factor levels in (2). For persons treated for DM, a person's variability of blood glucose is an important measure of risk—even, possibly, for dementia (Sachon et al., 1992).
explains much of the variation associated with θ, can be represented in equation (1). For example, adult-onset DM lowers the age at death for multiple conditions (Goldstein et al., 1978; Jones, 1956). So, DM could be expressed as a rapid increase of blood glucose (and its variance) with age in (1), which increases mortality by raising risk-factor levels in (2). For persons treated for DM, a person's variability of blood glucose is an important measure of risk—even, possibly, for dementia (Sachon et al., 1992).
Exogenous factors, whose effects vary with age, may be used to link health and socioeconomic factors. The adverse effect of low income on health may be represented by the effect of ![]() on risk factors. If health
on risk factors. If health
affects retirement, then retirement could be both an outcome and a cause of a change in health. Thus, a state-space model can represent exogenous inputs influencing health and nonlinear risk-factor processes.
Life-cycle effects differ by sex and race. Fertility may affect mortality from chronic diseases, like CVD and breast cancer (Beral, 1985; MacMahon, 1973). Postmenopausally, lower estrogen levels lead to female osteoporosis and atherosclerosis. African-Americans have elevated risks of hypertension and of renal failure, which peak in late mid-life (Walker et al., 1992; Brancati et al., 1992).9
DISABILITY AND MORTALITY
Disability is a complex phenomenon that manifests itself in many ways and that evolves over a long time. Thus, the definition of disability is subject to measurement and conceptual difficulties. But the attempt to measure disability is important because, given its relation to Medicare use and costs, and to morbidity and mortality, disability has strong predictive validity (Manton et al., 1993c). Moreover, functional impairment is important because of its prevalence at late ages and its association with decreased autonomy and increased demand for long-term care (LTC). One measure of functioning is the number of years one can expect to live free of disability, that is Active Life Expectancy (ALE) (Katz et al., 1983). ALE can be calculated from single- or multiple-decrement life tables and from cross-sectional or longitudinal surveys (Sullivan, 1971; Crimmins et al., 1989; Rogers et al., 1989; Manton and Stallard, 1991).
The assessment of the population impact of disability needs refinement. In most studies, a discrete threshold for disability, constant across age, is used to define the ''impaired" population as those who require help in the activities of daily living (ADLs)—dressing, bathing, eating, and so on; or instrumental activities of daily living (IADLs) (Lawton and Brody, 1969). A "threshold" model of disability has two limitations. First, there will be people who are close to the threshold, but above or below it. They will
have higher misclassification rates than do persons with no disability or with severe disability. Depending on where the threshold is set, large proportions of persons may be misclassified if the time derivative of the age distribution of disability is large. Second, the oldest-old will have a high prevalence of partial disability, though only a small proportion may be severely disabled: some disability, after all, is due to treatable or preventable conditions (Marx et al., 1992; Taylor, 1993).10
To deal with measurement error, and with different types and intensities of disability, multivariate procedures can be used to estimate scores for disability dimensions affecting persons at different ages due to different diseases. When multiple discrete measures of disability are projected onto a multidimensional "fuzzy" state space (Manton and Stallard, 1991), if, say, one of 27 disability items is miscoded, an individual's score changes incrementally: he does not jump from a disabled to a nondisabled state. Scores more precisely assess the type and intensity of disability (see Maddox and Clark, 1992). And, they better describe covariate effects; for example, disability for a fixed level of physical disease may be negatively correlated with education as in the case of osteoarthritis (Hannan et al., 1992). Scores may better describe short episodes of disability and improvements in functional status for individuals. With scores, changes in the intensity of disability can be described in autoregressive functions like equation (1).
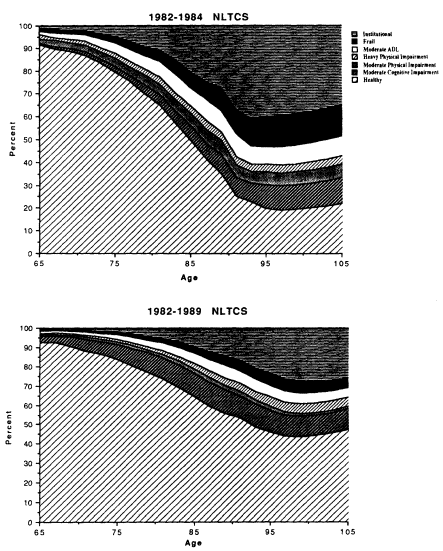
Scores (properly scaled) can be used to partition life expectancy into components specific to disability type. By representing within-class heterogeneity they behave better stochastically because diffusion, though bounded, is continuous. In the NLTCS, scores were calculated from 10 ADL, 8 IADL, and 9 physical performance items (like difficulty in climbing stairs and in holding a 10-pound package). We estimated male and female life tables (for the 1982-1989 NLTCS and mortality for 1982-1991) for seven dimensions identified from the 27 items for models in which a person is a member of one class (a discrete-state model) or has partial membership in multiple classes (a fuzzy-state model). A discrete-state model was implemented by fixing the covariance matrix in equations (6) and (8) at 0.0. Doing so yields a homogeneous population process comparable to the heterogeneous population process modeled in equations (5) through (9) except for the effects of altering the covariances. Alternatively, a Markov transition model could be constructed by classifying individuals into the state in which they had the highest disability score. Since that model does not use equations (5) through (9), differences in outcomes are confounded with differences in model structure.
In Table 7-3 we combined the seven dimensions, into four groups.
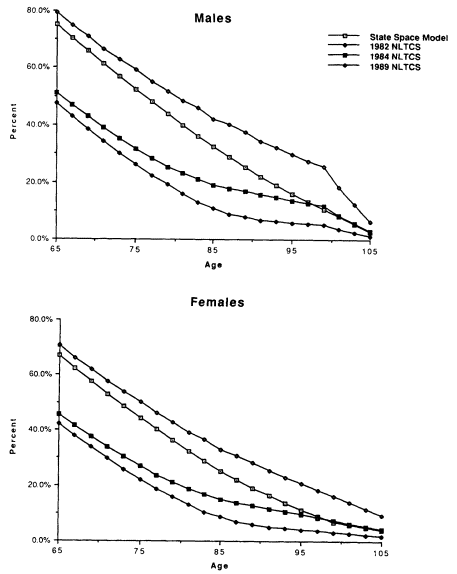
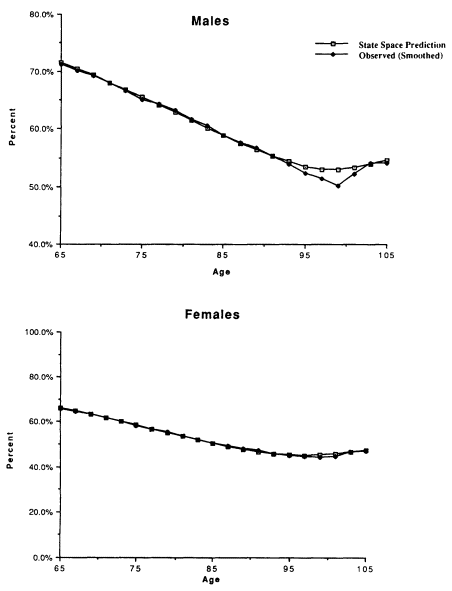
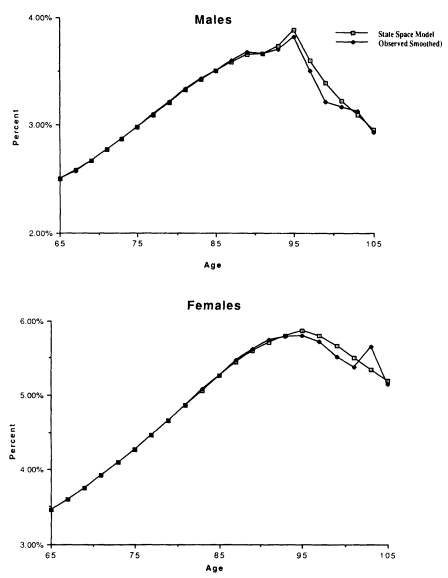
Although life expectancy at 65 is similar if not identical for the two models, survival declines less rapidly for the discrete-state model for both sexes to age 75. The prevalence of disability increases faster in the discrete-state model because, with only between-class heterogeneity, mortality increases only when a person "jumps" to a more disabled state. In the fuzzy-state model there is within-class heterogeneity that mortality selects against; that is, as a person's scores on severely disabled dimensions increase with age, interactions for the pair wise (but partial) occupancy of states allows mortality to increase continuously with age. In the discrete-state model, mortality is downwardly biased until sufficient proportions move into states with high mortality. The discrete-state model generated increases in the proportion in severely impaired and institutional groups inconsistent with the 1984-1986 Longitudinal Study of Aging (LSOA).11
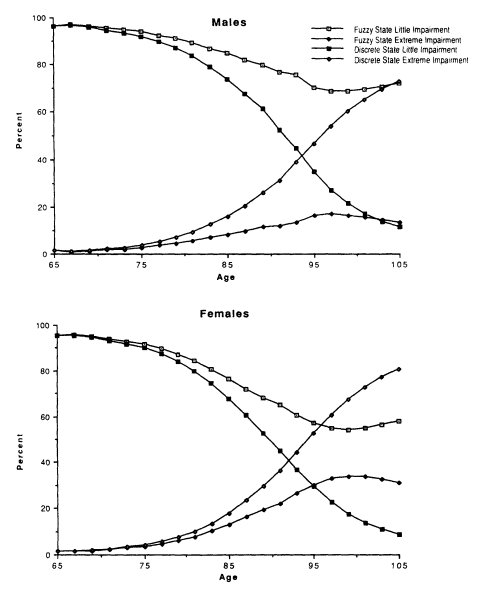
The age trajectories for the two models are shown in Figure 7-4 for the least and the most impaired classes. The two discrete-state trajectories for males converge faster than the fuzzy-state trajectories starting at age 75. For females, convergence is also faster in the discrete-state model, though it occurs later. The slower covergence for males is consistent with their shorter survival time at any disability level and age. For both sexes, the age-specific prevalences of low and high disability cross over in the discrete-state model. Fuzzy-state trajectories do not. The fuzzy-state model illustrates the effects of interactions of nonlinear age increases in mortality and linear disability dynamics produced in equations (5) through (9). With age, the "average" health of the population approaches stable points in a convex state space because of the moving equilibria of prevalence on multiple disability dimensions and increases in states with high mortality. The equilibria models, like extreme-value hazard models, represent isomorphisms between the statistical mechanics of population health and the kinetics of aging for individuals. Thus, the "strange attractor" (nonlinear change) behavior observed at late ages is due to failure mechanisms becoming more complex with age. At early ages, death is often due to the catastrophic failure of one system. At late ages, it reflects the overwhelming of homeostasis by the accumulation of loss of function in multiple organs. This is why the age trajectory of functional loss predicts mortality well.
Analyses of the NLTCS indicate that the prevalence of disability de-
TABLE 7-3 Cohort Life Tables and Disability Scores for Males and Females, With and Without Heterogeneity Within Classes Eliminated; Estimates for Persons Reaching Age 65 in Mid-1980s
|
|
|
|
|
Percent of Life Expectancy at Age t in Class |
|||
|
Age t |
Model Typea |
Proportion Age t, lt(%) Surviving to |
Life Expectancy at Age t, et (years) |
Little Impairment; No Physical and Mild or no Cognitive Disability |
Moderate Physical Impairment: |
Heavy Physical Impairment |
Extreme Impairment Moderate ADL, Frail, and Institutionalized |
|
Males |
|
|
|
|
|
|
|
|
65 |
Fuzzy state |
100.0 |
15.6 |
96.3 |
0.7 |
0.6 |
2.4 |
|
|
Discrete state |
100.0 |
15.4 |
93.3 |
0.7 |
0.6 |
2.4 |
|
75 |
Fuzzy state |
69.2 |
10.3 |
94.0 |
0.8 |
1.0 |
4.3 |
|
|
Discrete state |
69.7 |
9.8 |
92.1 |
1.0 |
1.3 |
5.7 |
|
85 |
Fuzzy state |
33.0 |
6.1 |
84.7 |
1.3 |
2.4 |
11.6 |
|
|
Discrete state |
32.5 |
5.3 |
73.9 |
2.0 |
3.7 |
20.5 |
|
95 |
Fuzzy state |
6.3 |
3.4 |
70.1 |
1.6 |
5.3 |
23.0 |
|
|
Discrete state |
4.0 |
2.3 |
34.6 |
2.8 |
8.6 |
54.0 |
|
105 |
Fuzzy state |
0.3 |
2.4 |
72.0 |
0.2 |
3.5 |
24.3 |
|
|
Discrete state |
0.0 |
1.1 |
11.3 |
0.9 |
4.9 |
82.8 |
|
Females |
|
|
|
|
|
|
|
|
65 |
Fuzzy state |
100.0 |
20.9 |
95.6 |
1.0 |
0.7 |
2.7 |
|
|
Discrete state |
100.0 |
20.9 |
95.6 |
1.0 |
0.7 |
2.7 |
|
75 |
Fuzzy state |
82.6 |
14.1 |
91.8 |
1.3 |
1.2 |
5.7 |
|
|
Discrete state |
83.3 |
14.0 |
90.1 |
1.6 |
1.4 |
6.8 |
|
85 |
Fuzzy state |
55.2 |
8.5 |
76.6 |
2.2 |
2.8 |
18.5 |
|
|
Discrete state |
56.7 |
8.0 |
67.9 |
3.2 |
3.5 |
25.4 |
|
95 |
Fuzzy state |
19.5 |
5.0 |
57.4 |
1.9 |
5.0 |
35.7 |
|
|
Discrete state |
18.7 |
4.0 |
29.4 |
3.3 |
6.1 |
91.3 |
|
105 |
Fuzzy state |
2.5 |
3.8 |
58.1 |
1.1 |
5.0 |
35.8 |
|
|
Discrete state |
1.1 |
2.3 |
8.8 |
1.6 |
3.7 |
85.9 |
|
a In the fuzzy state model, an individual can belong to more than one class. SOURCE: Data are from the 1982, 1984, and 1989 National Long-Term Care Surveys. |
|||||||
TABLE 7-4 The 1982, 1984, and 1989 Prevalence of Chronic Disability in the U.S. Population Age 65 and Over Estimated from the 1982, 1984, and 1989 National Long-Term Care Surveys
creased from 1982-1989 (Manton et al., 1993a). In Table 7-4 are estimates of prevalence in 1982, 1984, and 1989 for six groups: (1) not disabled; (2) disabled only for IADLs; (3) disabled on 1 or 2 ADLs; (4) disabled on 3 of 4 ADLs; (5) disabled on 5 or 6 ADLs; and (6) institutionalized. The 1.1 percent increase in the proportion of nondisabled from 1982 to 1989 is significant. It represents a 4.7 percent relative decline in the prevalence of disability. Because the U.S. elderly population grew 14.7 percent between 1982 and 1989, and also became older, the age-standardized rate of disability declined 1.7 percent; the age-and sex-standardized rate declined 2.8 percent. Reductions in the incidence of disability were large at late ages—even adjusted for mortality. At age 85 the mortality-adjusted likelihood of becoming disabled in 5 years declined 23.2 percent between 1982-1984 and 1984-1989 (Manton et al., 1993a).
The prevalences in Table 7-4 require no assumptions about between-surveys transitions or calculations of scores. The validity of these declines may be examined by comparing them with covariates with known trends. They are consistent with declines in population-weighted proxy response rates (indicative of severe impairment) from 19.8 percent (1982) to 17.6 percent (1989). Because the use of a proxy is determined before an interview, rates are unlikely to be affected by the reassessment of an individual. The use solely of equipment to cope with disability increased both absolutely and relatively from 1982 to 1989—suggesting a reduction in disability and an increase in social autonomy within the disabled population (Manton et al., 1993b). The use of equipment with personal assistance increased. Only the use of personal assistance by itself declined. Thus, decreases in informal care due to higher participation by women in the labor force and to smaller family size may be compensated for by use of equipment.
The 1982, 1984, and 1989 NLTCS and the 1982-1991 Medicare mortality data were used to construct cohort life tables based on disability scores. Cohort life expectancy at age 65 was 15.6 years for males and 20.9 years for females in 1989—increases from 14.2 years and 18.6 years, respectively, in 1982-1984. These life expectancies are projected to be achieved in 1993 for males and by 2010 for females in Census mid-range projections (Day, 1993), and in the low-mortality variant for females by 2003. Thus, the male values are conservative. The age trajectories of the seven disability dimensions, with mortality effects removed, are shown in Figure 7-5 by sex for 1982-1984 and 1982-1989. Before comparing results, we first note procedural differences. The results are based on changes in disability between 1982 and 1984 surveys and mortality between 1982-1986. The 1982-1989 analysis had to deal with different follow-up intervals (2 versus 5 years). This difference was handled by assuming that scores estimated for a survey are constant over the follow-up interval. While this practice permits estimates to be made on a monthly basis, with equal intervals, a strong
mortality gradient makes the imputed population appear healthier at late ages. However, estimating mortality coefficients with the imputed monthly data to remove survival bias yields accurate life tables. Bias in health scores is less of a problem if it is recognized that the scores describe a mixture of the current state of the population, and the state at a previous survey date (an average of 1 or 2 1/2 years earlier). Thus, changes in Figure 7-5 reflect the effects of improvements from 1982 to 1989 (Table 7-4) and the use of imputed monthly data. We investigated several methods for imputing monthly disability data using other dynamic assumptions and found that the results were similar (Manton et al., 1994b). Estimates of disability for 1982-1989 increase less rapidly with age than do those for 1982-1984—similar to the slowing of mortality age increases in Carey et al. (1992) and Curtsinger et al. (1992). This finding may reflect diseases associated with different life stages. Disabling conditions have peak effects at different ages; for example, DM peaks before 65 to 70; osteoarthritis before 75; and Alzheimer's disease before 90. For DM, this pattern is related to a lower life expectancy; for osteoarthritis, it may be due to the trajectory of the disease process; for Alzheimer's, the cause may be the exhaustion of susceptible persons.
In analyses of the Longitudinal Study of Aging, education was significantly related to robustness. Persons with 9 or more years of education had 2.1 to 2.4 times the likelihood of remaining robust than persons with 6 or fewer years had. Thus, declines in disability are consistent with cohort changes in education in Table 7-5. Above age 85, life expectancy and active life expectancy increased for the group with low education (8 or fewer years). Life expectancy for males in this group increased a year while active life expectancy increased 1.9 years—nearly twice as fast. Life expectancy for better-educated males increased a year; active life expectancy 0.4 year. Life expectancy and active life expectancy were absolutely higher in high-education groups (4.8 versus 7.3 years) in 1982-1989. Females manifest similar patterns. Overall life expectancy and active life expectancy increased for women more than for men for each education group because of the rapid growth of high-education groups above 85. Between 1980 and 2015 the proportion of persons 85 to 89 with 8 or fewer years of education is projected to decline significantly (Preston, 1992). Consequently, because education and function are associated, active life expectancy is expected to improve (Maddox and Clark, 1992; Suzman et al., 1992).12
Our model can be compared with disability data weighted by time of exposure. Figure 7-6 presents observed data (including imputed monthly data) and model-generated age trajectories for the least disabled for 1982-1989. The model fits the data well: there is little trend in the residuals for either sex. For both sexes, there is a flattening, and then a slight increase, for the least disabled at late ages. One source of this pattern is suggested by the trajectories for the most disabled community residents (Figure 7-7). The prevalence of the most disabled class declines above age 95, similar to risk-factor dynamics: the force of mortality is so high for the oldest old in this group that they cannot survive ill for very long.
Figure 7-8 plots sex-specific age trajectories for the least disabled group, as observed and as modeled, for each survey year. To smooth these data we plotted scores averaged over ages t to 105:
At 65, we plot the average score for 65 to 105; then the average for ages 67 to 105, and so on. The trajectory of model-generated scores for the least disabled fits the data well. In Figures 7-9 and 7-10 we plot the trajectories for the least and most disabled using smoothed data for males and females. The data and the model results are similar. In both, severe disability declines at late ages. These results, unlike the prevalences reported in Table 7-4, depend on model assumptions. The scores are more reliable because they are a weighted average of multiple functional items. Figure 7-5 can be compared with the results of a model in which groups are defined by IADL-only disability, 1 to 2 ADLs, 3 to 4 ADLs, 5 to 6 ADLs (physical performance is not represented). The 5-year transition matrix for persons age 65 is given in Table 7-6. The extrapolation of these transitions (by multiplying the four transition matrices for persons age 65, 70, 75, and 80) produces the distribution in Table 7-7. The proportion remaining nondisabled is, adjusting for mortality, 58 percent—close to the value for the least disabled at age 85 depicted in Figure 7-5. Thus, discrete-state changes are similar to score trajectories for times and ages where a comparison is possible.
TABLE 7-5 Life Expectancy and Active Life Expectancy for Males and Females 1982-1984 and 1982-1989 at Age 85; Total and Stratified by Education
|
|
Males |
Females |
||||||
|
Period |
Percentage of Life Years Expected to be Lived at a Given Education Level |
Life Expectancy (years) |
ALE (years) |
Proportion of Life Active (%) |
Percentage of Life Years Expected to Be Lived at a Given Education Level |
Life Expectancy (years) |
ALE (years) |
Proportion of Life Active (%) |
|
Total |
|
|
|
|
|
|
|
|
|
1982-1984 |
— |
5.0 |
3.1 |
61.8 |
— |
6.3 |
3.1 |
49.6 |
|
1982-1989 |
— |
6.1 |
4.4 |
72.5 |
— |
8.5 |
5.5 |
64.3 |
|
Change |
— |
+1.1 |
+1.3 |
|
— |
+2.2 |
+1.4 |
|
|
Low educationa |
|
|
|
|
|
|
|
|
|
1982-1984 |
64.7 |
3.8 |
1.2 |
30.8 |
81.7 |
4.6 |
0.9 |
19.6 |
|
1982-1989 |
40.8 |
4.8 |
3.5 |
72.9 |
62.5 |
5.6 |
3.6 |
64.2 |
|
Change |
-23.9 |
+1.0 |
+1.9 |
|
-19.2 |
+1.0 |
+2.7 |
|
|
High educationb |
|
|
|
|
|
|
|
|
|
1982-1984 |
35.5 |
6.3 |
5.0 |
79.1 |
18.3 |
9.3 |
6.4 |
68.7 |
|
1982-1989 |
59.2 |
7.3 |
5.4 |
74.0 |
37.5 |
10.3 |
6.7 |
70.9 |
|
Change |
+23.9 |
+1.0 |
+0.4 |
|
+19.2 |
+1.0 |
+0.3 |
|
|
a Eight years or less of education. b Nine years or more of education. SOURCE: Data are from the 1982, 1984, and 1989 National Long-Term Care Surveys. |
||||||||
GENETICS
Models and Methods
The effects of genetics on longevity are complex. Models in which a single gene controls biological senescence are obsolete. Genetic influences are polygenic, and the expression of genetically determined traits depends on environment. To estimate the effects of genetics on population health
one must posit a model of these effects and compare the actual to the theoretical distribution of events. Such model-based integration of data, and indirect inference, is often used in medical demography. Often, problems involving latent variables must be dealt with in genetic models: some are time-constant effects such as fixed genetic factors, and some are time-variable effects. Though the terminology changes with the topic being addressed, the mathematics and statistics are similar (for example, the assumption of local independence, Suppes and Zanotti, 1981; or the missing-
TABLE 7-6 Five-Year Transition Probabilities from Age 65-70 Estimated from the 1984 to 1989 NLTCS, With and Without Mortality Adjustments
|
Status at Age |
Status Age 70 in 1989 |
||||||
|
65 in 1984 |
Nondisabled |
IADL Only |
1-2 ADLs |
3-4 ADLs |
5-6 ADLs |
Institutional |
Dead |
|
Nondisabled +age-ins |
.800 |
.026 |
.032 |
.012 |
.011 |
.009 |
.111 |
|
(excluding dead) |
.900 |
.029 |
.036 |
.014 |
.012 |
.010 |
— |
|
IADL only |
.228 |
.158 |
.220 |
.049 |
.031 |
.043 |
.272 |
|
(excluding dead) |
.314 |
.217 |
.302 |
.067 |
.042 |
.059 |
— |
|
1-2 ADLs |
.147 |
.074 |
.250 |
.136 |
.050 |
.073 |
.270 |
|
(excluding dead) |
.202 |
.101 |
.343 |
.187 |
.069 |
.100 |
— |
|
3-4 ADLs |
.015 |
.042 |
.200 |
.199 |
.154 |
.050 |
.339 |
|
(excluding dead) |
.023 |
.063 |
.303 |
.301 |
.234 |
.076 |
— |
|
5-6 ADLs |
.038 |
.019 |
.082 |
.089 |
.156 |
.096 |
.520 |
|
(excluding dead) |
.079 |
.040 |
.171 |
.185 |
.325 |
.200 |
— |
|
Institutional |
.000 |
.019 |
.011 |
.012 |
.012 |
.553 |
.393 |
|
(excluding dead) |
.000 |
.031 |
.018 |
.019 |
.020 |
.912 |
— |
|
SOURCE: Data are from the 1984 and 1989 National Long-Term Care Surveys. |
|||||||
TABLE 7-7 Twenty-Year Transition Probabilities for Age 65-85 Estimated from the 1984 to 1989 NLTCS, With and Without Mortality Adjustments
|
|
Status at Age 85 |
||||||
|
Status at Age 65 |
Nondisabled |
IADL Only |
1-2 ADLs |
3-4 ADLs |
5-6 ADLs |
Institutional |
Dead |
|
Nondisabled +age-ins |
.218 |
.024 |
.041 |
.025 |
.019 |
.047 |
.626 |
|
(excluding dead) |
.583 |
.063 |
.110 |
.066 |
.050 |
.127 |
— |
|
IADL only |
.088 |
.012 |
.026 |
.018 |
.013 |
.035 |
.808 |
|
(excluding dead) |
.456 |
.065 |
.134 |
.092 |
.069 |
.184 |
— |
|
1-2 ADLs |
.063 |
.010 |
.023 |
.016 |
.012 |
.034 |
.841 |
|
(excluding dead) |
.397 |
.064 |
.142 |
.104 |
.077 |
.217 |
— |
|
3-4 ADLs |
.025 |
.006 |
.016 |
.013 |
.010 |
.028 |
.901 |
|
(excluding dead) |
.253 |
.063 |
.166 |
.134 |
.100 |
.285 |
— |
|
5-6 ADLs |
.021 |
.004 |
.011 |
.008 |
.006 |
.020 |
.930 |
|
(excluding dead) |
.296 |
.060 |
.151 |
.116 |
.089 |
.289 |
— |
|
Institutional |
.006 |
.002 |
.007 |
.004 |
.003 |
.030 |
.947 |
|
(excluding dead) |
.114 |
.038 |
.125 |
.081 |
.066 |
.577 |
— |
|
SOURCE: Data are from the 1984 and 1989 National Long-Term Care Surveys. Estimates are the results of multiplying the 5-year transition matrices for ages 65 (see Table 7-6), 70, 75, and 80. |
|||||||
information principle; Orchard and Woodbury, 1971). A combination of models from the two areas could be beneficial. One possibility would be to combine analyses of the genetic control of aging with stochastic-process models using fuzzy-state mapping of discrete traits to allow evaluation of high-dimensional discrete spaces, and their mapping to nonstationary stochastic processes, without Gaussian assumptions.
Weiss (1990) reviewed standard approaches for analyzing the genetics of chronic diseases. One method assumes that phenotype is controlled by the additive effects of a gene locus (G), a component representing all other genetic determinants (PG), and environment (E). The distribution is
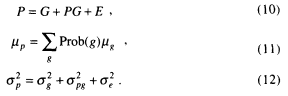
(See, for example, Elston, 1981, 1986). This does not produce a one-to-one mapping of genotype and phenotype. The population is composed of subsets of individuals for each genotype with mean µg and variance (spg2 + se2). The presence of a gene locus produces a nonnormal distribution. This model can be fitted to family disease pedigrees with µ's and s's estimated by maximum likelihood to identify genetic effects. A limitation of the model is the effect of individual differences in exposures. Exposure effects can be assumed to be normally distributed if independently generated. This assumption fails if there are interactions between genotype and environment (G x E). These may be studied in experiments using animal models with well-characterized genetic traits (for example, Curtsinger et al., 1992) or in human studies of identical twins (a natural experiment in which genetic endowment is identical but must be contrasted with same-sex fraternal twins to control for environmental variation). Effects, however, are not identifiable in this case unless the gene loci are identified.
Thus, identifying the genetic effects on health can require multiple data sets, such as laboratory analyses identifying genes, family history, or data on identical twins. The problems are more complex when one gene affects multiple phenotypes, that is, pleiotropy. For example, the genetic control of an enzyme, 5 alpha reductase, which converts testosterone into dihydrotestosterone, affects the risk of both baldness and prostate cancer. The correlation of trait expression can be used to analyze how a gene of interest is related to genes whose location on o chromosome is known (Ott, 1985). Modifications of the Elston-Shinant algorithm can represent covariates in these relations. A model based on the correlation of continuously distributed risk factors between a random pair of relatives and its effect on the probability of being affected by a risk factor, modeled as a logistic, is less
computationally burdensome (Hopper and Carlin, 1992). A moderately frequent appearance of a disease in a family over time may imply strong familial risk factors.
Hazard functions are often nuisance parameters in genetic epidemiology. In medical demography the age dependence of health events is often a primary concern, for example, the rectangularization of the survival curve, the compression of morbidity, and the plasticity of aging. Weiss (1990) suggests that, to analyze age effects, one must relate genotype to disease risk by defining a hazard with the distribution of risk factors conditional on genotype modeled as a separate factor, or,
This mixed hazard can be related to multivariate trait selection. A gap exists between population models of multiple quantitative traits and identification of classical Mendelian genes (Hartl and Clark, 1989). Random genetic drift has been represented by differential equations (Kimura, 1955). An approximation (assuming Markovity) uses a diffusion process to obtain φ(x,t), the distribution of x alleles at t. Phenotype and genotype are assumed to be Gaussian distributed with selection of one phenotype over another altering φ's moments. If zn is the phenotypic value of the nth trait, the vector of traits ![]() is
is
where ![]() are genetic differences for N traits and
are genetic differences for N traits and ![]() are environmental effects. If
are environmental effects. If ![]() ,
, ![]() , and
, and ![]() are covariance matrices for
are covariance matrices for ![]() ,
, ![]() , and
, and ![]() , then the fitness (probability of survival) is,
, then the fitness (probability of survival) is,
The mean phenotype after selection (environmental effect mean is assumed 0.0) is,
where g(x) is the distribution of genetic effects and ![]() (
(![]() ) is the mean fitness of genotype
) is the mean fitness of genotype ![]() . The change in the mean genotype is
. The change in the mean genotype is
Applying the del(∇) operator to the mean fitness function produces a gradient,

where ![]() is the vector of selection differentials,
is the vector of selection differentials,
or,
In (20a), ![]() are average phenotypic changes,
are average phenotypic changes, ![]() are selection differentials, and
are selection differentials, and ![]() is the fraction of phenotypic variation that is additive genetic variance. Changes in
is the fraction of phenotypic variation that is additive genetic variance. Changes in ![]() for "weak" selection are
for "weak" selection are
where ![]() (see equation 18) (Hartl and Clark, 1989). To relate this to the state-space model, we substitute equation (3) into equation (6):
(see equation 18) (Hartl and Clark, 1989). To relate this to the state-space model, we substitute equation (3) into equation (6):
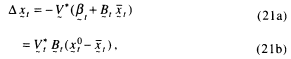
where ![]() corresponds to
corresponds to ![]() ,
, ![]() is a quadratic matrix (as is
is a quadratic matrix (as is ![]() ); and x0t -
); and x0t - ![]() is the vector of deviations from optimal values (corresponding to
is the vector of deviations from optimal values (corresponding to ![]() ). Thus, the diffusion model of quantitative traits with selection for fitness is related to the state-space model—except the force of selection in the state-space model has a specific form (quadratic); and deterministic and stochastic age-variable components of change in phenotypic variation are explicit. In equation (1), fixed components represent
). Thus, the diffusion model of quantitative traits with selection for fitness is related to the state-space model—except the force of selection in the state-space model has a specific form (quadratic); and deterministic and stochastic age-variable components of change in phenotypic variation are explicit. In equation (1), fixed components represent ![]() variation. Time-varying components generalize
variation. Time-varying components generalize ![]() to
to ![]() where time dependency is multivariate. The state-space model allows
where time dependency is multivariate. The state-space model allows ![]() to vary with time; that is, the age variation of genotypic risk is a mix of risk-factor-specific hazards, multiplied by the probability of having a given risk-factor value, given a genetic factor (g). In the state-space model, Prob
to vary with time; that is, the age variation of genotypic risk is a mix of risk-factor-specific hazards, multiplied by the probability of having a given risk-factor value, given a genetic factor (g). In the state-space model, Prob![]() in (13) is replaced by a multivariate process for
in (13) is replaced by a multivariate process for ![]() , with genetic variance represented by fixed effects (for example,
, with genetic variance represented by fixed effects (for example, ![]() ). The interaction of G with E is represented by exogenous processes,
). The interaction of G with E is represented by exogenous processes, ![]() and interactions with fixed effects. The identifiability of components of the state-space model depends on the length of follow-up and measurement density. In the hazard model, in addition to risk conditional on
and interactions with fixed effects. The identifiability of components of the state-space model depends on the length of follow-up and measurement density. In the hazard model, in addition to risk conditional on ![]() , θ represents the average age effects of unobserved factors on
, θ represents the average age effects of unobserved factors on ![]() with µ0t(=µ0 · eθt) representing senescence. Genetic effects are represented by the dependence of mortality on
with µ0t(=µ0 · eθt) representing senescence. Genetic effects are represented by the dependence of mortality on ![]() or
or ![]() in the dynamics, for example, for a one-step forecast, t to t+l,
in the dynamics, for example, for a one-step forecast, t to t+l,
The interaction of dynamics and mortality leads to multistep forecast equations like (5) through (9).
Examples of Genetic Analysis in Studying Chronic Disease and Aging
As indicated above, the effects of genetic differences are not directly observed in human populations but must be inferred. Examples of genetic analysis in studying chronic disease and aging are Knudson's (1971) work on the effects of genes on the cancer retinoblastoma; other researchers have shown that the risk of early breast cancer is strongly related to family pedigree: (the relative risk is 50 to 1 for a woman whose mother and a sister have had early breast cancer); but late-onset breast cancer bears no strong relation to family history (Lynch and Watson, 1990; Mettlin et al., 1990; Roseman et al., 1990).
Genetic analyses are often not adjusted for cohort, or heterogeneity, effects. Failure to recognize cohort trends can produce biased estimates— and compromise genetic inferences. For example, U.S. lung cancer mortality has been increasing over birth cohorts, which makes cross-sectional estimates of m too large.
Experimental studies can identify genetic factors. For example, Farrar et al.'s (1990) work on the effect of aluminum on Alzheimer's risk suggests that a genetic defect in the blood-brain barrier allowed, experimentally, gallium (an element chemically similar to aluminum) transfer in both Down's and Alzheimer's patients. Head injuries, another Alzheimer's risk factor, might also damage the blood-brain barrier (Graves et al., 1990).
Genetic heterogeneity at ages 90 or 100 and more is not much different from that for persons, say, age 50 (Thieszen et al., 1990; Beregi et al., 1991; Takata et al., 1987; Marriotti et al., 1992).13 Models in which senescence is controlled by a few genes regulating the number of cell replications such as the Hayflick limit are too simple to explain longevity, though some believe genes controlling growth factors regulating cell death may be significant, (see Hayflick and Moorhead, 1961; Finch, 1990; Cristofalo et al., 1989).
Studies suggest that genetic diseases are important at early ages. For example, Reed (1990) found that the concordance rate for CVD risk factors decreased with age. As discussed above, genetically determined breast cancer is expressed early. And, most genetically determined lung cancer is manifest before age 70 (Sellers et al., 1990).
We need new multivariate-process models to detect the stochastic generation of mutations in DNA with age over the life span and to distinguish those from genetic endowment. If free-radical damage to DNA accumulates with age, the fidelity of DNA replication is affected (Cutler, 1991). This could be modeled as a stochastic process with a diffuse effect on genes emerging at late ages, (such as plasma cell abnormalities of unknown significance; Alexanian et al., 1988). Free-radical damage at advanced ages may affect mitochondrial, DNA, rather than nuclear DNA, thus affecting energy production. Thus, DNA changes may be involved in aging—but not necessarily through inheritance; the effects could be similar to neoplasia, in which fidelity of function is lost as DNA errors accumulate.
CONCLUSION
Because of the very high costs of caring for people with health impairments, models that demonstrate the potential impact of various health policies and that accurately project changes in disability rates are extremely valuable tools for policy makers.
In this chapter we have discussed the tools of medical demography and the areas of research to which they may be applied. Many of these tools require the development of biologically detailed models of changes in the health of populations. We have discussed the factors affecting the use of such models to describe changes in health between two elderly populations at a given point in time and changes in the health of a given population as they age through time. We need to understand better the processes related to age that affect health, and we need to learn how to exploit longitudinal and demographic data to describe those effects. Because biomedical science is advancing so rapidly, so must the evolution of models. We can accomplish this evolution by using a general state-space model that can be elaborated as more refined data become available.
Medical demography is conceptually and procedurally distinct from the epidemiology of chronic disease. The epidemiologist attempts to discern causal relations between risk factors and disease endpoints, often using general statistical models to test the significance of relations. To investigate causality requires experimental designs and randomized trials. The medical demographer uses estimates of epidemiological and clinical relations in population models to asses their implications, with and without interventions, for both current and future populations. However, in performing those tasks, the validity of the basic epidemiological relations are tested at the population level, and the result may be estimates of population effects with implications for the interpretation of epidemiological data. In addition, it may be necessary to estimate different types of models of complex health processes whose parameters may require evaluation in multiple
data sets. Finally, the biostatistician is often interested in assessing the effects of clinical interventions—usually for relatively short periods of time. Thus, many biostatistical methods do not deal with the long-term age changes that are the focus of medical demography.
Of greater importance to the medical demographer than to epidemiologists or biostatisticians is the effect of functional change in the population. Analysis of such changes involves endpoints that are difficult to measure and that evolve over long periods of time. The medical demographer is also more concerned with cohort and life-cycle effects and with the use of longitudinal survey data to assess changes in health over time without significant population bias. Designs of longitudinal surveys appropriate for assessing complex changes in the health of the elderly will require methodological research. A state-space model such as we have detailed here may aid this development. The effects of length of time between measurements, and the effects of the detail of measurement, can be examined by considering changes in θ over design parameters.
Thus, medical demography is an endeavor to synthesize scientific insights from multiple disciplines to explain and forecast change in the health outcomes of populations that are attributable to age. It thus relies on multivariate, stochastic models to represent the interactions of disease, disability, and mortality as they change over time, and as they affect people as people age. Recent evidence indicates that these dynamics are more complex than once supposed and that simple hazards do not describe them. This finding is not surprising. These dynamics are the consequences of changes in the health of individuals as they age, related to declines in mortality and to increases in life expectancy, which permit manifestation of nonlinear behavior. Clearly, what is called for is much more research on these processes before interventions can be carefully coordinated with simultaneous changes in health.
REFERENCES
Alexanian, R., B. Barlogie, and D. Dixon 1988 Prognosis of asymptomatic multiple myeloma. Archives of Internal Medicine 148:1963-1965.
Andrews, R.C.R. 1992 Diabetes and schizophrenia: Genes or zinc deficiency? Lancet 340:1160.
Armitage, P., and R. Doll 1961 Stochastic models for carcinogenesis. Pp. 19-38 in J. Neyman, ed., Proceedings of the Fourth Berkeley Symposium on Mathematical Statistics and Probability. Vol. IV: Biology and Problems of Health. Berkeley: University of California Press.
Ashley, D.J. 1969 The two ''hit" and multiple "hit" theories of carcinogenesis. British Journal of Cancer 23:313-328.
Bagge, E., A. Bjelle, S. Eden, and A. Svanborg 1992 A longitudinal study of the occurrence of joint complaints in elderly people. Age and Ageing 21:160-167.
Barker, D.J. 1990 The intrauterine origins of cardiovascular and obstructive lung disease in adult Life. Journal of the Royal College of Physicians of London 25(2):129-133.
Barker, D.J.P., and C.N. Martyn 1992 The maternal and fetal origins of cardiovascular disease. Journal of Epidemiology and Community Health 46:8-11.
Barker, D.J.P., P.D. Winter, C. Osmond, B. Margetts, and S.J. Simmonds 1989 Weight in infancy and death from ischaemic heart disease. Lancet 8663:577-579.
Barker, D.J.P., A.R. Bull, C. Osmond, and S.J. Simmonds 1991a Fetal and placental size and risk of hypertension in adult life. British Medical Journal 301:259-262.
Barker, D.J.P., K.M. Godfrey, C. Fall, C. Osmond, P.D. Winter, and S.O. Shaheen 1991b Relation of birth weight and childhood respiratory infection to adult lung function and death from chronic obstructive airways disease. British Medical Journal 303:672-675.
Barker, D.J.P., K.M. Godfrey, C. Osmond, and A. Bull 1992a The relation of fetal length, ponderal index and head circumference to blood pressure and the risk of hypertension in adult life. Pediatric and Perinatal Epidemiology 6:35-44.
Barker, D.J.P., T.W. Meade, C.H.D. Fall, A. Lee, C. Osmond, K. Phipps, and Y. Stirling 1992b Relation of fetal and infant growth to plasma fibrinogen and factor vii concentrations in adult life. British Medical Journal 304:148-152.
Barker, M.E., S.I. McClean, J.J. Strain, and K.A. Thompson 1992c Dietary behaviour and health in Northern Ireland: An exploration of biochemical and haematological associations. Journal of Epidemiology and Community Health 46:151-156.
Bayo F.R., and J.F. Faber 1985 Mortality rates around age one hundred. Transactions of the Society of Actuaries 35:37-59.
Beard, R.E. 1963a A theory of mortality based on actuarial, biological and medical considerations. Proceedings of the International Population Conference, New York. 1961, Vol. 1. London: International Union for the Scientific Study of Population.
1963b Actuarial methods of mortality analysis: Adaptation to changes in the age and cause pattern. Proceedings of the Royal Society B 159:56.
Beral, V. 1985 Long term effects of childbearing on health. Journal of Epidemiology and Community Health 39:343-346.
Beregi, E., O. Regius, and K. Rajczy 1991 Comparative study of the morphological changes in lymphocytes of elderly individuals and centenarians. Age and Ageing 20:55-59.
Bernoulli, D. 1760 Essai d'une nouvelle analyse de la mortalité causée par la petite vérole, et des avantages de l'inoculation pour le prévenir. Pp. 1-45 in Historie avec les Mémoirs, Académie Royle des Sciences. Paris.
Blot, W.J., J.T. Li, P.R. Taylor, W. Guo, S. Dawsey, G.Q. Wang, C.S. Yang, S.F. Zheng, M. Gail, G.Y. Li, Y. Yu, B.Q. Liu, J. Tangrea, Y.H. Sun, F. Liu, J.F. Fraumeni, Y.H. Zheng, and B. Li 1993 Nutrition intervention trials in Linxian, China: Supplementaion with specific vitamin/mineral combinations, cancer incidence, and disease-specific mortality in the general population. Journal of the National Cancer Institute 85(18): 1483-1492.
Bourgeois-Pichat, J. 1952 Essai sur la mortalite "biologique" de l'homme. Population 7:381-394.
1978 Future outlook for mortality declines in the world. Population Bulletin of the United Nations. No. 11. New York.
Brancati, F.L., J.C. Whittle, P.K. Whelton, A.J. Seidler, and M.J. Klag 1992 The excess incidence of diabetic end-stage renal disease among blacks: A population based study of potential explanatory factors. Journal of the American Medical Association 268:3079-3084.
Branch, L.G., and L. Ku 1989 Transition probabilities to dependency, institutionalization, and death among the elderly over a decade. Journal of Aging and Health 1:370-408.
Burns, A., R. Jacoby, P. Luthert, and R. Levy 1990 Cause of death in Alzheimer's disease. Age and Ageing 19:341-344.
Campbell, A.J., J. Reinken, C. Diep, and I. McCosh 1985 Factors predicting mortality in a total population sample of the elderly. Journal of Epidemiology and Community Health 39:337-342.
Carey, J.R., P. Liedo, D. Orozco, and J.W. Vaupel 1992 Slowing of mortality rates at older ages in large medfly cohorts. Science 258:457-461.
Chan, J.C.N., C.S. Cockram, M.G. Nicholls, C.K. Cheung, and R. Swaminathan 1992 Comparison of enalapril and nifedipine in treating non-insulin dependent diabetes associated with hypertension: One year analysis. British Medical Journal 2(305):981-985.
Chandra, R.K. 1992 Effect of vitamin and trace-element supplementation on immune responses and infection in elderly subjects. Lancet 340:1124-1127.
Clarke, R.D. 1950 A bio-actuarial approach to forecasting rates of mortality. Proceedings of the Centenary Assembly of the Institute of Actuaries 2:12.
Cooper, G.R., G.L. Myers, S.J. Smith, and R.C. Schlant 1992 Blood lipid measurements: Variations and practical utility. Journal of the American Medical Association 267(12): 1652-1660.
Cox, D.R. 1972 Regression models and life tables. Journal of the Royal Statistical Society, Series B 34:187-202.
Crimmins, E., Y. Saito, and D. Ingegneri 1989 Changes in life expectancy and disability-free life expectancy in the United States. Population and Development Review 15:235-267.
Cristofalo, V.J., P.D. Phillips, T. Sorger, and G. Gerhard 1989 Alterations in the responsiveness of senescent cells to growth factors. Journal of Gerontology 44(6):55-62.
Curtsinger, J.W., H. Fukui, D. Townsend, and J.W. Vaupel 1992 Demography of genotypes: Failure of the limited-lifespan paradigm in Drosophila melanogaster. Science 258:461-464.
Cutler, R.G. 1991 Antioxidants and aging. American Journal of Clinical Nutrition 53:373S-379S.
Davis, C.E., R.M. Rifkind, H. Brenner, and D.J. Gordon 1990 A single cholesterol measurement underestimates the risk of coronary heart disease: An empirical example from the Lipid Research Clinics Mortality Follow-up Study. Journal of the American Medical Association 264:3044-3046.
Day, J.C. 1993 Population Projections of the United States, by Age, Sex, Race, and Hispanic Origin: 1993 to 2050. Current Population Reports, Series P25-1104. Washington, D.C: U.S. Department of Commerce.
Dontas, A.S., A. Tzonou, P. Kasviki-Charvati, G.L. Georgiades, G. Christakis, and D. Trichopoulos 1991 Survival in a residential home: An eleven-year longitudinal study. Journal of the American Geriatrics Society 39:641-649.
Dowd, J.E., and K.G. Manton 1990 Forecasting chronic disease risks in developing countries. International Journal of Epidemiology 19(4): 1018-1036.
Dubos, R. 1965 Man Adapting. New Haven and London: Yale University Press.
Elston, R.C. 1981 Segregation analysis. Pp. 63-120 in H. Harris and K. Hirschhorn, eds., Advances in Human Genetics. New York: Plenum.
1986 Modern methods of segregation analysis. Pp. 213-224 in S.H. Moolgavkar and R.L. Prentice, eds., Modern Statistical Methods in Chronic Disease Epidemiology. New York: John Wiley & Sons.
Evans, D.A., P.A. Scherr, N.R. Cook, M.S. Albert, N.H. Funkenstein, L.A. Smith, L.E. Hebert, T.T. Wetle, L.G. Branch, M. Chown, C.H. Hennekens, and J.O. Taylor 1992 The impact of Alzheimer's disease in the United States population. Pp. 283-302 in R. Suzman, D. Willis, and K.G. Manton, eds., The Oldest-Old. New York: Oxford University Press.
Farrar, G., P. Altmann, S. Welch, O. Wychrij, B. Chose, J. Lejeune, J. Corbett, V. Prasher, and J.A. Blair 1990 Defective gallium-transferrin binding in Alzheimer disease and Down syndrome: Possible mechanism for accumulation of aluminum in brain. Lancet 335:747-750.
Fearon, E.R., and B. Vogelstein 1990 A genetic model for colorectal tumorigenesis. Cell 61:759-767.
Feskens, E.J., C.H. Bowles, and D. Kromhout 1991 Intra- and interindividual variability of glucose tolerance in an elderly population. Journal of Clinical Epidemiology 44:947-953.
1992 A longitudinal study on glucose tolerance and other cardiovascular risk factors: Associations within an elderly population. Journal of Clinical Epidemiology 45(3):293-300.
Finch, C.E. 1990 Longevity, Senescence, and the Genome. Chicago: University of Chicago Press.
Firth, W.J. 1991 Chaos—Predicting the unpredictable. British Medical Journal 303:1565-1568.
Frank, J.W., D.M. Reed, J.S. Grove, and R. Benfante 1992 Will lowering population levels of serum cholesterol affect total mortality? Expectations from the Honolulu heart program. Journal of Clinical Epidemiology 45(4):333-346.
Gerkins, V.R., A. Ting, H.T. Menck, J.T. Casagrande, P.I. Terasaki, M.C. Pike, and B.E. Henderson 1974 HL-A heterozygosity as a genetic marker of long-term survival. Journal of the National Cancer Institute 52:1909-1911.
Ghali, J.K., R. Cooper, and E. Ford 1990 Trends in hospitalization rates for heart failure in the United States, 1973-1986 . Archives of Internal Medicine 150:769-776.
Gill, R.D. 1992 Multistate life-tables and regression models. Mathematical Population Studies 3(4):259-276.
Glueck, C.J., P. Gartside, R.W. Fallat, J. Sielski, and P.M. Steiner 1976 Longevity syndromes: Familial hypobeta and familial hyperalpha lipoproteinemia. Journal of Laboratory and Clinical Medicine 88:941-957.
Goldberg, K.C., A.J. Hartz, S.J. Jacobsen, H. Krakauer, and A.A. Rimm 1992 Racial and community factors influencing coronary artery bypass graft surgery rates for all 1986 medicare patients Journal of the American Medical Association 267(11): 1473-1477.
Goldstein, S., E.J. Moerman, J.S. Soeldner, R.E. Gleason, and D.M. Barnett 1978 Chronologic and physiologic age affect replicative life-span of fibroblasts from diabetic, prediabetic and normal donors. Science 199:781-782.
Golino, P., F. Piscione, J.T. Willerson, M. Cappelli-Bigazzi, A. Focaccio, B. Villari, C. Indolfi, E. Russolillo, M. Condorelli, and M. Chiariello 1991 Divergent effects of serotonin on coronary-artery dimensions and blood flow in patients with coronary atherosclerosis and control patients. New England Journal of Medicine 324:641-687.
Gompertz, B. 1825 On the nature of the function expressive of the law of human mortality. Philosophical Transactions, Royal Society of London 114:513.
Gordon, D.J., J.L. Pobstfield, R.J. Garrison, J.D. Neaton, W.P. Castelli, J.D. Knoke, D.R. Jacobs, S. Bangdiwala, H.A. Tyroler 1989 High-density lipoprotein cholesterol and cardiovascular disease: Four prospective American studies. Circulation 79:8-15.
Grand, A., P. Grosclaude, H. Bocquet, J. Pous, and J.L. Albarede 1990 Disability, psychosocial factors and mortality among the elderly in a rural French population. Journal of Clinical Epidemiology 43(8):773-782.
Graunt, J. 1662 Natural and Political Observations Made upon the Bills of Mortality. (Reprinted by the Johns Hopkins University Press, 1939.)
Graves, A.B., E. White, T.D. Koepsell, B.V. Reifler, G. van Belle, E.B. Larson, and M. Raskind 1990 The association between head trauma and Alzheimer's disease. American Journal of Epidemiology 131:491-501.
Gross, P.A., G.V. Quinnan, M. Rodstein, J.R. LaMontagne, R.A. Kaslow, A.J. Saah, S. Wallenstein, R. Neufeld, C. Denning, and P. Gaerlan 1988 Association of influenza immunization with reduction in mortality in an elderly population: A prospective study. Archives of Internal Medicine 148:562-565.
Gutstein, W.H. 1988 The central nervous system and atherogenesis: Endothelial injury. Atherosclerosis 70:145-154.
Haffner, S.M., K.K. Gruber, P.A. Morales, H.P. Hazuda, R.A. Valdez, B.D. Mitchell, and M.P. Stern 1992 Lipoprotein(a) concentration in Mexican-Americans and Non-Hispanic whites: The San Antonio Heart Study. American Journal of Epidemiology 136(9): 1060-1068.
Hales, C.N., D.J.P. Barker, P.M.S. Clark, L.J. Cox, C. Fall, C. Osmond, and P.D. Winter 1991 Fetal and infant growth and impaired glucose tolerance at age 64. British Medical Journal 303:1019-1022.
Hannan, M.T., J.J. Anderson, T. Pincus, and D.T. Felson 1992 Educational attainment and osteoarthritis: Differential associations with radiographic changes and symptom reporting. Journal Clinical Epidemiology 45(2):139-147.
Harris, J.E. 1983 Cigarette smoking and successive birth cohorts of men and women in the United States during 1900-80. Journal of the National Cancer Institute 71:473-479.
Hartl, D.L., and A.G. Clark 1989 Principles of Population Genetics. Sunderland, Mass.: Sinauer Associates.
Hastings, D., and L. Berry 1979 Cohort Analysis: A Collection of Interdisciplinary Readings. Oxford, Ohio: Scripps Foundation.
Hayflick, L., and P.S. Moorhead 1961 The serial cultivation of human diploid cell strains. Experimental Cell Research 37:614.
Hazzard, W.R. 1990 A central role of sex hormones in the sex differentials in lipoprotein metabolism, atherosclerosis, and longevity. Pp. 87-108 in M.G. Ory and H.R. Warner, eds., Gender, Health, and Longevity: Multidisciplinary Perspectives. Springer: New York.
Heckman, J., and B. Singer 1984a The identifiability of the proportional hazards model. Review of Economic Studies 51:231-241.
1984b A method for minimizing the impact of distributional assumptions in econometric models for duration data. Econometrics 52:271-320.
Heikinheimo, R.J., M.V. Haavisto, K.J. Mattila, and S.A. Rajala 1985 Mortality and high hematocrit in the very aged. Age and Ageing 14:159-162.
Hopper, J.L., and J.B. Carlin 1992 Familial aggregation of a disease consequent upon correlation between relatives in a risk factor measured on a continuous scale. American Journal of Epidemiology 136(9):1138-1147.
Jacobs, D., H. Blackburn, M. Higgins, et al. 1992 Report of the conference on low blood cholesterol: Mortality association. Circulation 86(3):1046-1060.
Jacobsen, S.J., D.S. Freedman, R.G. Hoffmann, H.W. Gruchow, A.J. Anderson, and J.J. Barboriak 1992 Cholesterol and coronary artery disease: Age as an effect modifier. Journal of Clinical Epidemiology 45(10): 1053-1059.
Jacquez, J.A. 1972 Compartmental Analysis in Biology and Medicine. Amsterdam: Elsevier.
Johnson, C.L., B.M. Rifkind, C.T. Sempos, M.D. Carroll, P.S. Bachorik, R.R. Briefel, D.J. Gordon, V.L. Burt, C.D. Brown, K. Lippel, and J.I. Cleeman 1993 Declining serum total cholesterol levels among U.S. adults: The National Health and Nutrition Examination Surveys. Journal of the American Medical Association 269(23):3002-3008.
Jones, H.B. 1956 A special consideration of the aging process, disease and life expectancy. Advanced Biological Medical Physics 4:281-337.
Katz, S., L.G. Branch, M.H. Branson, J.A. Papsidero, J.C. Beck, and D.S. Greer 1983 Active life expectancy. New England Journal of Medicine 309:1218-1223.
Kestenbaum, B. 1992 A description of the extreme aged population based on improved Medicare enrollment data. Demography 29(4):565-580.
Kimura, M. 1955 Solution of a process of random genetic drift with a continuous model. Proceedings of the National Academy of Sciences USA 41:144-150.
Kitagawa, E.M., and P.M. Hausner 1973 Differential Morality in the United States: A Study in Socioeconomic Epidemiology. Cambridge, Mass.: Harvard University Press.
Kitzman, D.W., and W.D. Edwards 1990 Minireview: Age-related changes in the anatomy of the normal human heart. Journal of Gerontology 45:M33-M39.
Knapp, R.G., S.E. Sutherland, J.E. Keil, P.F. Rust, and D.T. Lackland 1992 A comparison of the effects of cholesterol on CHD mortality in black and white women: Twenty-eight years of follow-up in the Charleston Heart Study. Journal of Clinical Epidemiology 45(10): 1119-1129.
Knudson, A.J. 1971 Mutation and cancer: Statistical study of retinoblastoma. Proceedings of the National Academy of Sciences USA 68:820-823.
Ko, W., J.P. Gold, R. Lazzaro, J.A. Zelano, S. Lang, O.W. Isom, and K.H. Krieger 1992 Survival analysis of octogenarian patients with coronary artery disease managed by elective coronary artery bypass surgery versus conventional medical treatment. Circulation 86(5):II-101-II-197.
Lakatta, E.G. 1985 Health, disease, and cardiovascular aging. Pp. 73-104 in America's Aging: Health in An Older Society. Institute of Medicine, National Research Council. Washington, D.C.: National Academy Press.
Lanska, D.J., and X. Mi 1993 Decline in U.S. stroke mortality in the era before antihypertensive therapy. Stroke 24(9): 1382-1388.
Lawton, M.P., and E.M. Brody 1969 Assessment of older people: Self-maintaining and instrumental activities of daily living. Gerontologist 9:179-186.
Lee, R.D., and L.R. Carter 1992 Modeling and forecasting U.S. mortality. Journal of the American Statistical Association 87:659-675.
Lew, E.A., and L. Garfinkel 1990 Mortality at ages 75 and older in the Cancer Prevention Study (CPSI) Ca-A Cancer Journal for Clinicians 40:210-224.
Lynch, H.T., and P. Watson 1990 Editorial commentary: Early age at breast cancer onset—A genetic and oncologic perspective. American Journal of Epidemiology 131:984-986.
MacMahon, B., P. Cole, and J. Brown 1973 Etiology of human breast cancer: A review. Journal of the National Cancer Institute 50:21-42.
Maddox, G.L., and D.O. Clark 1992 Trajectories of functional impairment in later life. Journal of Health and Social Behavior 33:114-125.
Makeham, W.M. 1867 On the law of mortality and construction of annuity tables. Journal of the Institute of Actuaries 8:301.
Mann, N.R., R.E. Schafer, and N.D. Singpurwalla 1974 Methods for Statistical Analysis of Reliability and Life Data. New York: John Wiley & Sons.
Manton, K.G., and E. Stallard 1988 Chronic Disease Modeling: Measurement and Evaluation of the Risks of Chronic Disease Processes. London: Charles Griffin.
1991 Cross-sectional estimates of active life expectancy for the U.S. elderly and oldest-old populations. Journal of Gerontology 48:S170-S182.
1992a Demographics (1950-1987) of breast cancer in birth cohorts of older women. Journal of Gerontology 47 (Special Issue):32-42.
1992b Compartment model of the temporal variation of population lung cancer risks. Pp. 75-81 in Biomedical Modeling and Simulation (Proceedings of the 13th IMACS World Congress on Computation and Applied Mathematics). Amsterdam: North-Holland, Elsevier Science Publishers B.V.
Manton, K.G., E. Stallard, and J.W. Vaupel 1986 Alternative models for the heterogeneity of mortality risks among the aged. Journal of the American Statistical Association 81:635-644.
Manton, K.G., M.A. Woodbury, E. Stallard, W.B. Riggan, J.P. Creason, and A. Pellom 1989 Empirical Bayes procedures for stabilizing maps of U.S. cancer mortality rates. Journal of the American Statistical Association 84:637-650.
Manton, K.G., B. Singer, M.A. Woodbury 1992 Some issues in the quantitative characterization of heterogeneous populations. In J. Trussell, R. Hankinson, J. Tilton, eds., Demographic Applications of Event History Analysis. Oxford: Clarendon Press.
Manton, K.G., L.S. Corder, and E. Stallard 1993a Changes in the use of personal assistance and special equipment 1982 to 1989: Results from the 1982 and 1989 NLTCS. The Gerontologist 33:168-176.
1993b Estimates of change in chronic disability and institutional incidence and prevalence rates in the U.S. elderly population from the 1982, 1984 and 1989 National Long-Term Care Survey. Journal of Gerontology: Social Sciences 47:S153-S166.
Manton, K.G., E. Stallard, and B.H. Singer 1993c Projecting the future size and health status of the U.S. elderly population. In D. Wise, ed. The Economics of Aging. Chicago: University of Chicago Press.
Manton, K.G., M.A. Woodbury, and H.D. Tolley 1994a Statistical Procedures for the Application of Fuzzy Set Models to High Dimensional Discrete Response Data. New York: John Wiley & Sons, forthcoming.
Manton, K.G., E. Stallard, M.A. Woodbury, and J.E. Dowd 1994b Time varying covariated human mortality and aging: Multidimensional generalization of the Gompertz. Journal of Gerontology: Biological Sciences.
Marriotti, S., P. Sansoni, G. Barbesino, P. Caturegli, D. Monti, A. Cossarizza, T. Giacomelli, G. Passeri, U. Fagiolo, A. Pinchera, and C. Franceschi 1992 Thyroid and other organ-specific autoantibodies in healthy centenarians. Lancet 339:1506-1508.
Martin, D.C., J. Francis, J. Protetch, and F.J. Hoff 1992 Time dependency of cognitive recovery with cobalamia replacement: Report of a pilot study. Journal of the American Geriatrics Society 40:168-172.
Marx, M.S., P. Werner, J. Cohen-Mansfield, and R. Feldman 1992 The relationship between low vision and performance of ADLs in nursing home residents. Journal of the American Geriatric Society 40:1018-1020.
Mason, T.J., J.F. Fraumeni, R.N. Hoover, and W.J. Blot 1981 An Atlas of Mortality from Selected Diseases. Washington, D.C.: U.S. Government Printing Office.
Matis, J.H., and T.E. Wehrly 1979 Stochastic models of compartmental systems. Biometrics 35:199-220.
McCord, J.M. 1991 Is iron sufficiency a risk factor in ischemic heart disease? Circulation 83(3): 1112-1113.
McKeigue, P.M., B. Shah, and M.G. Marmot 1991 Relation of central obesity and insulin resistance with high diabetes prevalence and cardiovascular risk in South Asians. Lancet 337:382-386.
Mettlin, C., I. Croghan, N. Natarajan, and W. Lane 1990 The association of age and familial risk in a case-control study of breast cancer. American Journal of Epidemiology 131:973-983.
Modan, M,. J. Or, A. Karasik, Y. Drory, Z. Fuchs, A. Lusky, A. Chetrit, and H. Halkin 1991 Hyperinsulinemia, sex and risk of atherosclerotic cardiovascular disease. Circulation 84(3): 1165-1175.
Moon, J., B. Bandy, and A.J. Davidson 1992 Hypothesis: Etiology of atherosclerosis and osteoporosis: Are imbalances in the calciferol endocrine system implicated? Journal of the American College of Nutrition 11:567-583.
Mooradian, A.D., and N.C. Wong 1991a Molecular biology of aging. Part I: An introduction to laboratory techniques of molecular biology. Journal of the American Geriatrics Society 39:717-723.
1991b Molecular biology of aging. Part II: A synopsis of current research. Journal of the American Geriatrics Society 39:717-723.
Mozar, H.N., D.G. Bal, and S.A. Farag 1990 The natural history of atherosclerosis: An ecologic perspective. Atherosclerosis 82:157-164.
Muhlbaier, L.H., D.B. Pryor, J.S. Rankin, L.R. Smith, D.B. Mark, R.H. Jones, D.D. Glower, F.E. Harrell, Jr., K.L. Lee, R.M. Califf, and D.C. Sabiston 1992 Observational comparison of event-free survival with medical and surgical therapy in patients with coronary artery disease. Circulation 86(5):198-204.
Myers, G.C., K.G. Manton, and H. Bacellar 1987 Sociodemographic aspects of future unpaid productive roles. Pp. 110-147 in America's Aging: Productive Roles in an Older Society. Washington, D.C.: National Academy Press.
Mysrup, B., G.F. Jensen, and P. McNair 1992 Cardiovascular risk factors during estrogen-norethindrone and cholecalciferol treatment. Archives of Internal Medicine 152:2265-2268.
Nabulsi, A., A. Folsom, A. White, W. Patsch, G. Heiss, K. Wu, M. Szklo 1993 Association of hormone-replacement therapy with various cardiovascular risk factors in postmenopausal women. New England Journal of Medicine 328(15)1069-1075.
National Center for Health Statistics 1987 The Supplement on Aging to the 1984 National Health Interview Survey. Vital and Health Statistics, Series 1, No. 21. DHHS Pub. No. (PHS) 87-1323. Public Health Service. Washington, D.C.: U.S. Government Printing Office.
Neaton, J.D., H. Blackburn, D. Jacobs, L. Kuller, D.J. Lee, R. Sherwin, J. Shih, J. Stamler, D. Wentworth, and Multiple Risk Factor Intervention Trial Research Group 1992 Serum cholesterol level and mortality findings for men screened in the multiple risk factor intervention trial. Archives of Internal Medicine 152:1490-1500.
Omran, A.R. 1971 The epidemiologic transition: A theory of the epidemiology of population change. Milbank Memorial Fund Quarterly 49:509-538.
Orchard, R., and M.A. Woodbury 1971 A missing information principle: Theory and application. Pp. 697-715 in L.M. LeCam, J. Neyman, and E.L. Scott, eds., Proceedings Sixth Berkeley Symposium on Mathematical Statistics and Probability. Berkeley: University of California Press.
Ott, J. 1985 Analysis of Human Genetic Linkage. Baltimore, Md.: Johns Hopkins University Press.
Overgaard, K., M. Hansen, S. Jensen, and C. Christiansen 1992 Effect of salcatonin given intranasally on bone mass and fracture rates in established osteoporosis: A dose-response study. British Medical Journal 305:556-561.
Pekkanen, J., K.G. Manton, E. Stallard, A. Nissinen, and M.J. Karvonen 1992 Risk factor dynamics, mortality and life expectancy differences between eastern and western Finland: The Finnish cohorts of the Seven Countries Study. International Journal of Epidemiology 21:406-419.
Penn, N.D., L. Purkins, J. Kelleher, R.V. Heatley, and B.H. Masie-Taylor 1991a Ageing and duodenal mucosal immunity. Age and Ageing 20:33-36.
Penn, N.D., L. Purkins, J. Kelleher, R.V. Heatley, B.H. Masie-Taylor, and P.W. Belfield 1991b The effect of dietary supplementation with vitamins A, C and E on cell-mediated immune function in elderly long-stay patients: A randomized controlled trial. Age and Ageing 20:169-174.
Perks, W. 1932 On some experiments in the graduation of mortality statistics. Journal of the Institute of Actuaries 63:12.
Peto, J., H. Seidman, and I.J. Selikoff 1982 Mesothelioma incidence among asbestos workers: Implications for models of carcinogenesis and risk assessment calculations. British Journal of Medicine 45:124-135.
Potthoff, R.F., M.A. Woodbury, and K.G. Manton 1992 Equivalent sample size and equivalent degrees of freedom refinements for inference using survey weights under superpopulation models . Journal of the American Statistical Association, Theory and Methods 87:383-396.
Prasad, K.N., and J. Edwards-Prasad 1992 Vitamin E and cancer prevention: Recent advances and future potentials. Journal of the American College of Nutrition 11(5):487-500.
Preston, S.H. 1992 Cohort succession and the future of the oldest old. Pp. 50-57 in R.M. Suzman, D.P. Willis, and K.G. Manton, eds., The Oldest Old. New York: Oxford University Press.
1993 Demographic changes in the United States, 1970 to 2050. In K.G. Manton, B.H.
Singer, and R.M. Suzman, eds., Forecasting the Health of Elderly Populations. New York: Springer-Verlag.
Qualheim, R.E., S.G. Rostand, K.A. Kirk, and R.G. Luke 1991 Changing patterns of end-stage renal disease due to hypertension. American Journal of Kidney Disease 18:336-343.
Ravnskov, U. 1992 Cholesterol lowering trials on coronary heart disease: Frequency of citation and outcome. British Medical Journal 305:15-19.
Reed, D.M. 1990 The paradox of high risk of stroke in populations with low risk of coronary heart disease . American Journal of Epidemiology 131:579-588.
Reed, T., J. Quiroga, J.V. Selby, D. Carmelli, J.C. Christian, R.R. Fabsitz, and C.E. Grim 1991 Concordance of ischemic heart disease in the NHLBI Twin Study after 14-18 years of follow-up. Journal of Clinical Epidemiology 44:797-805.
Rogers, A., R.G. Rogers, and L.G. Branch 1989 A multistate analysis of active life expectancy. Public Heath Reports 104:222-225.
Roseman, D.L., A.K. Strauss, and W. Shorey 1990 A positive history of breast cancer: Does its effect diminish with age? Archives of Internal Medicine 150:191-194.
Sachon, C., A. Grimaldi, J.P. Digy, B. Pillon, B. Dubois, and F. Thervet 1992 Cognitive function, insulin-dependent diabetes and hypoglycaemia. Journal of Internal Medicine 231:471-475.
Schaie, K.W. 1983 Longitudinal Studies of Adult Psychological Development. New York, London: Guilford Press.
Selikoff, I.J. 1981 Disability Compensation for Asbestos-Associated Disease in the United States. Report to the U.S. Department of Labor, Contract No. J-9-M-8-0165. Environmental Sciences Laboratory, Mount Sinai School of Medicine, City University of New York.
Sellers, T.A., J.E. Bailey-Wilson, R.C. Elston, A.F. Wilson, G.Z. Elston, W.L. Ooi, and H. Rothschild 1990 Evidence for Mendelian inheritance in the pathogenesis of lung cancer. Journal of the National Cancer Institute 82:1272-1279.
Sempos, C., J. Cleeman, M. Carroll, C. Johnson, P. Bachorik, D. Gordon, V. Burt, R. Briefel, C. Brown, K. Lippel, and B. Rifkind 1993 Prevalence of high blood cholesterol among U.S. adults: An update based on guidelines from the Second Report of the National Cholesterol Education Program Adult Treatment Panel. Journal of the American Medical Association 269(23):3009-3014.
SHEP Cooperative Research Group 1991 Prevention of stroke by antihypertensive drug treatment in older persons with isolated systolic hypertension. Journal of the American Medical Association 265:3255-3264.
SOLVD Investigators 1991 Effect of enalapril on survival in patients with reduced left ventricular ejection fractions and congestive heart failure. New England Journal of Medicine 325:293-302.
Spiegelman, M. 1968 Introduction to Demography. Cambridge, Mass.: Harvard University Press.
Stampfer, M.J., R. Malinow, W.C. Willett, L.M. Newcomer, B. Upson, D. Ullmann, P.V. Tishler, and C.H. Hennekens 1992 A prospective study of plasma homocyst(e)ine and risk of myocardial infarction in U.S. physicians. Journal of the American Medical Association 268(7):877-881.
Sullivan, D.F. 1971 A single index of mortality and morbidity HSMHA Health Reports 86:347-354.
Sullivan, J.L. 1991 Antioxidant and coronary heart disease. Lancet 337:432-433.
Suppes, P., and M. Zanotti 1981 When are probabilistic explanations possible? Synthese 48:191-199.
Suzman, R.M., T. Harris, E.C. Hadley, M.G. Kovar, and R. Weindruch 1992 The robust oldest-old: Optimistic perspectives for increasing healthy life expectancy. Pp. 341-358 in R.M. Suzman, D.P. Willis, and K.G. Manton, eds., The Oldest Old. New York: Oxford University Press.
Takata, H., M. Suzuki, T. Ishii, S. Sekiguchi, and H. Iri 1987 Influence of major histocompatibility complex region genes on human longevity among Okinawan-Japanese centenarians and nonagenarians. Lancet 824-826 (editorial, 835-836).
Taylor, A. 1993 Cataract: Relationships between nutrition and oxidation. Journal of the American College of Nutrition 12(2):138-146.
Thatcher, A.R. 1992 Trends in numbers and mortality at high ages in England and Wales. Population Studies 46(3):411-426.
Thieszen, S.L., J.E. Hixson, D.J. Nagengast, J.E. Wilson, and B.M. McManus 1990 Lipid phenotypes, apolipoprotein genotypes and cardiovascular risk in nonagenarians. Atherosclerosis 83:137-146.
Thompson, S.G., and S.J. Pocock 1991 Can meta-analysis be trusted? Lancet 338:1127-1130.
Trussell, J., G. Rodriguez, and B. Vaughan 1992 Union dissolution in Sweden. Pp. 39-60 in J. Trussell, R. Hankinson, J. Tilton, eds., Demographic Applications of Event History Analysis. Oxford: Clarendon Press.
Tsevat, J., M.C. Weinstein, L.W. Williams, A.N. Tosteson, and L. Goldman 1991 Expected gains in life expectancy from various coronary heart disease risk factor modifications. Circulation 83:1194-1201.
Tsiatis, A.A. 1975 A nonidentifiability aspect of the problem of competing risks. Proceedings of the National Academy of Sciences USA 72:20-22.
Vaupel, J.W., K.G. Manton, and E. Stallard 1979 The impact of heterogeneity in individual frailty on the dynamics of mortality. Demography 16:439-454.
Walker, A.M. 1982 Projections of Asbestos-Related Disease 1980-2009. Final Report, Epidemiology Resources, Chestnut Hill, Mass.
Walker, W.G., J.D. Neaton, J.A. Cutler, R. Neuwirth, and J.D. Cohen 1992 Renal function change in hypertensive members of the Multiple Risk Factor Intervention Trial: Racial and treatment effects. Journal of the American Medical Association 268(21):3085-3091.
Weber, K.T., and C.G. Brilla 1991 Pathological hypertrophy and cardiac interstitium. Circulation 83:1849-1865.
Weiss, K.M. 1990 The biodemography of variation in human frailty. Demography 27:185-206.
Woodbury, M.A., K.G. Manton, and E. Stallard 1981 Longitudinal models for chronic disease risk: An evaluation of logistic multiple regression and alternatives. International Journal of Epidemiology 10:187-197.
Yeung, A.C., V.I. Vekshtein, D.S. Krantz, J.A. Vita, T.J. Ryan, P. Ganz, and A.P. Selwyn 1991 The effects of atherosclerosis on the vasomotor response of coronary arteries to mental stress. New England Journal of Medicine 325:1551-1556.
Zaman, Z., S. Roche, P. Fielden, P. Frost, D. Niriella, and A. Cayley 1992 Plasma concentrations of vitamins A and E carotenoids in Alzheimer's disease. Age and Ageing 21(2):91-94.
Zheng, Z.X., Z.S. Wang, H.M. Zhu, J.Y. Yang, H.Y. Peng, L.X. Wang, J. Li, X.W. Jiang, and Y.F. Yu 1993 Survey of 160 centenarians in Shanghai. Age and Ageing 22:16-19.