9
Prevention of Obesity
The prevention of obesity is a topic that must be considered given the major increases both in the prevalence of obesity and in the mean body weights of people in the United States over the past decade (see Chapter 2). Despite the appeal of prevention as an ideal, it appears that this country as a whole has been unable to prevent obesity. The results of more limited and focused efforts at prevention, described later in this chapter, have hardly been more successful. These facts led a recent review to conclude that "we have not been able to prevent obesity in the past and we do not have the tools to do better in the future" (Stunkard, in press).
It has been proposed that genetic vulnerability may lie at the root of the current epidemic of obesity and the problem of controlling, let alone preventing, obesity (Bouchard, 1994). However, there has been no real change in the gene pool during this period of increasing obesity. The root of the problem, rather, must lie in the powerful social and cultural forces that promote an energy-rich diet and a sedentary lifestyle. But if social and cultural forces can promote obesity, these same forces should be able to control it. Therein lies the still unrealized potential for preventing obesity.
There is some ambiguity of terminology in the prevention literature. The verb prevent implies taking an action or interposing an impediment to stop or keep something from happening. Different ideas about what it is that should be stopped or kept from happening have been suggested in terms of obesity prevention. Is it the incidence of obesity itself? Is it preventing
weight gain among those treated for obesity to prevent progression from a moderate to more severe levels? Does the success of prevention efforts depend upon the effect on comorbid medical disabilities (e.g., diabetes or hypertension)? Is what should be stopped or kept from happening an underlying risk condition or predisposition factor for obesity development?
A recent Institute of Medicine (IOM) report recommends an approach to clarifying definitions of prevention that, although developed in relation to mental disorders, apply to obesity (IOM, 1994). This IOM report reviews existing classification systems for preventive interventions for physical illness. The familiar public health classification system designates three types of prevention: primary, secondary, and tertiary. The goal of primary prevention is to decrease the number of new cases (incidence) of a disorder. In secondary prevention, the goal is to lower the rate of established cases of the disorder in the population (prevalence). Tertiary prevention seeks to stabilize or decrease the amount of disability associated with an existing disorder. For obesity, tertiary prevention could refer to decreasing the progression to more severe obesity or decreasing the likelihood of associated musculoskeletal, metabolic, or vascular disorders (e.g., osteoarthritis, diabetes, or cardiovascular disease).
When this prevention classification system was introduced more than 25 years ago, the implicit disease model was one of an acute condition with a specific and unifactorial cause. It was assumed that mechanisms linking the cause of a specific disease to its subsequent occurrence could be identified. In the intervening years, many chronic diseases prevalent in this country have been recognized as having multifactorial etiologies. Research on these diseases has advanced our knowledge about the complicated relations that exist between risk factors and protective factors for disease and the outcomes of preventive interventions. But this knowledge can breed the pessimistic view that prevention efforts will be futile until the etiologies of diseases are better understood (IOM, 1994).
According to this analysis, the concept of risk reduction is critical to prevention programs and research. Addressing the degrees of risk for a condition supplants the more simplistic concept of prevention in which a disease is simply present or absent. Risk factors refer to those characteristics that, if present for a particular individual, make it more likely that this person (compared to someone selected from the general population) will develop a disorder (Werner and Smith, 1992). Both risk and protective factors are included here. Research also shows that many at-risk individuals have factors in their background or environment that protect against the development of a disorder (Garmezy, 1983).
In furthering the establishment of successful preventive intervention programs, the IOM report recommends instituting a "preventive intervention
research cycle.'' This research cycle consists of, first, description of the interplay between risk and protective factors; next, identification of causal risk factors that may be alterable through interventions; finally, systematic, empirical, and rigorous testing of these interventions, most often in preventive intervention trials.
At the current stage of research into preventing obesity, work is still in the first two phases of this research cycle: identifying high-risk and protective factors for the development of obesity, and determining which factors are malleable and can be altered by preventive interventions. We recommend continuing this early research on the determinants of obesity and pilot-testing promising interventions before funds are allocated for large-scale community prevention trials. Promising research studies that have already appeared in the scientific literature are reviewed later in this chapter.
The recent IOM report also recommended an alternative terminology for physical disease prevention, proposed by Gordon (1987), and we adopt it here (see Figure 9-1). This terminology identifies three types of prevention: universal, selective, and indicated prevention. Each category represents a population group, rather than a disorder or disease state, to whom preventive interventions are directed. Universal preventive measures or interventions are designed for everyone in the eligible population. Selective preventive measures are directed toward a subgroup of the
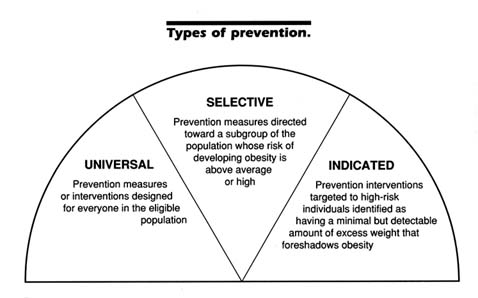
FIGURE 9-1 Adapted from IOM, 1994.
population whose risk of developing the disorder is above average or high. Indicated preventive interventions are targeted to high-risk individuals identified as having minimal but detectable signs or symptoms that foreshadow the disorder, or exhibiting biological markers indicating predisposition, who do not meet the full diagnostic criteria for the disorder itself.
The earlier IOM report reserves the term prevention for those interventions that occur before the onset of a diagnosed disorder. What was previously known as tertiary prevention is redefined as maintenance intervention , whose aim is to reduce the disability associated with an ongoing disorder. Maintenance interventions, which can be supportive, educational, and/or pharmacological, are provided on a long-term basis to reduce relapse and recurrence. Consistent with the IOM definition of prevention (i.e., interventions that occur before onset), we do not include here a discussion of maintenance of weight to prevent the exacerbation of obesity or its complications in those in whom the condition is established. Factors affecting long-term weight management in the obese are discussed in Chapter 7.
The primary aim of obesity prevention is to reduce the number of new cases of obesity. This can be accomplished by means of a risk-reduction model. Even if the obesity outcomes are in the distant future, the decrease in risk factors and increase in protective factors for obesity can be identified. An important secondary aim is to delay the onset of obesity. The goals of indicated prevention programs are harder to define than those of universal and selective prevention programs. They might be framed in terms of reducing the length of time initial weight gain persists beyond certain pre-obese limits and halting its progression before diagnostic criteria for obesity are met. Even if the individual does eventually develop obesity, the prior preventive intervention may still have had an effect by reducing the duration or severity of the disorder.
The remainder of the chapter describes all three areas of prevention with reference to the prevention of obesity. Each area is described with respect to rationale, outcome measures, specific examples of programs, and criteria for evaluating prevention outcomes.
UNIVERSAL PREVENTION
In accord with the traditional concept of primary prevention, universal prevention programs are geared to the general public and all members of specific eligible groups, such as children, the elderly, or pregnant women. Examples of universal prevention measures (which can often be applied without professional assistance) include prenatal care, use of seat belts, prevention of smoking, and consuming a nutritionally adequate
diet (IOM, 1994). Such programs have advantages when their cost per person is low and the intervention is acceptable, low risk, and effective for the population involved. It is important to note that the target population (e.g., the general public) often includes individuals who have already developed the designated disorder.
As discussed in Chapter 2, obesity is becoming more rather than less prevalent in the United States. Universal prevention programs may help stabilize or even reverse the trend toward increased obesity in the general population. Universal programs can be classified into two broad categories: (1) preventive education and skills targeted toward individuals (e.g., programs in various settings designed to enhance nutritional knowledge and increase physical activity, thereby informing the public about the nature of weight change so that uninvolved and unaffected people can avoid negative or adverse consequences); and (2) modification of social and economic policies in an attempt to reduce the population's exposure to the environmental causes of obesity (e.g., mandated changes in food composition, regulation of food advertising, and food labeling). Programs in the first category often are derived from an individual clinical treatment model and evaluated in terms of weight change and the health habits of individual participants. Programs in the second category often are linked with a public health model, and results can be evaluated in terms of changes in the population distribution of body mass index (BMI).
Outcome Measures for Universal Prevention
Six outcome measures for this type of prevention can be identified:
-
reduction in the prevalence of obesity in the general population (this is a logical outcome to use when evaluating universal prevention programs; however, it must be noted that what counts as a reduction in the prevalence of obesity will share in the same arbitrariness as the definition of obesity used [see Stunkard, in press]);
-
an overall reduction in average weight of the U.S. population;
-
improvements in nutritional intake, eating habits, exercise, and other health-related activities;
-
improved knowledge, attitudes, and norms regarding nutrition, weight, eating habits, and exercise;
-
decreased rates of comorbidity problems (e.g., hypertension and diabetes); and
-
public policy and environmental change indices (e.g., regulations concerning food labeling and label claims).
Examples of Universal Prevention Programs
Family-Based Programs
The family context can influence children's eating behavior and risk for obesity in several ways, including parental verbal prompts at mealtime, nonverbal influences such as food purchases and food presentation, modeling influences of adult eating behaviors, and use of food for non-nutritious purposes (Ray and Klesges, 1993). In one study, Pisacano et al. (1978) gave instruction in health education to parents of infants, emphasizing a low-fat, prudent diet. Compared with a usual-care control group, the prevalence of obesity was significantly reduced for intervention group children for a period ranging from 3 months to 3 years. Nader (1993) proposes that the family be an essential part of programs designed to prevent and treat obesity. An example of this type of program, in which overweight children are treated in the family context (Epstein et al., 1990b), is described later in this chapter in the section on indicated prevention.
School-Based Programs
In a recent review of school-based obesity prevention programs, Resnicow (1993) emphasizes the importance of the school environment, pointing out that more than 95 percent of American youth aged 5–17 are enrolled in school and that children eat one to two meals per day there. Most school-based prevention programs include nutrition education and exercise components. Resnicow (1993) reviews six studies showing significant benefits of intervention. Other studies that evaluated the effects of physical education on childhood adiposity show less promise. In an evaluation of one such study, Project SPARK, Sallis et al. (1993) report that children did not significantly reduce their BMI or adiposity after 2 years of participating in a physical activity promotion program.
Work-Site-Based Programs
After completing school, employed people spend more time at work than any other activity. Health-promotion programs at the work site provide access to large numbers of persons who can be reached at relatively low cost. Despite the promise of such programs, a general review of studies in this area is not encouraging. Work-site programs designed to control problems such as hypertension and smoking have been highly successful. By contrast, the results of weight-control programs at the work site have been consistently disappointing (Taylor and Stunkard, 1993).
Community-Wide Programs
Another approach to preventing and reducing the prevalence of obesity is to focus on the entire population within a specified community. Community-based approaches to weight reduction are typically part of broader educational programs focused on cardiovascular risk reduction and helping individuals adopt a healthier lifestyle. The goal of such programs is to achieve at least small changes in most people who live in a particular geographic area. The results of four such projects have been reported: the Stanford Three-Community Study (Farquhar et al., 1977), Stanford Five-City Study (Farquhar et al., 1990), Minnesota Heart Health Program (Luepker et al., 1994), and North Karelia (Finland) Project (Puska et al., 1983).
All four programs were devoted to cardiovascular risk reduction and thus provided the opportunity to compare efforts to control obesity with those to control smoking, hypertension, and blood cholesterol concentrations. Obesity turned out to be far harder to control than the other coronary risk factors. In contrast to the reasonable effectiveness of the other risk-factor reduction efforts, no program interrupted the increase in the prevalence of obesity. The Minnesota and North Karelia projects showed no difference between the experimental and contrast communities in the rate of increase in obesity. In the Stanford Three Community Study, weight did not increase in the experimental community, while it rose 0.45 kg in the contrast community. In the Stanford Five-City Study, the comparable values were increases of 0.54 and 1.25 kg.
Environmental-Change Programs
Any review of universal prevention methods would be incomplete without a brief description of environmental-change programs, some of which touch on public-policy issues. In this approach to universal prevention, the goal is to modify social and economic policies so as to reduce the population's exposure to environmental causes of obesity. Among the prevention strategies that have been proposed or implemented are (1) regulating the abuse potential of food products (e.g., specifying a maximum caloric density and fat or sugar content in processed foods); (2) regulating advertising and other promotional practices for food (e.g., controlling advertising of sugared cereals to children); and (3) modifying economic policies related to food (e.g., increasing excise taxes based on the fat and sugar content of food products). Environmental changes to encourage physical activity include the development of safe bicycle lanes in urban areas, as well as safe and inviting places to walk, and the provision of well-maintained stairwells as options to elevators. Unfortunately,
little or no research has been conducted to document the effects of such changes, so the potential of environmental change from these and related public health approaches to modify individual behaviors remains unknown.
SELECTIVE PREVENTION
High-risk subgroups may be distinguished by age, gender, occupation, family history, and other characteristics. The risk may be imminent or occur over a lifetime; risk groups are identified on the basis of biological, psychological, or social/cultural risk factors that are known to be associated with the onset of the disorder. Examples of interventions for target groups include annual mammograms for women with a positive family history of breast cancer, special immunizations (e.g., yellow fever) for groups who travel in high-risk areas where the disease is still prevalent, preschool programs for all children from poor neighborhoods, and support groups for elderly widows. Obesity prevention programs that target entire high-risk groups (e.g., black adolescent females, children of obese parents, and Native American children living in impoverished communities) meet the definition of selective prevention.
Selective prevention programs and policies are designed for groups at high risk for obesity or already overweight but not yet obese. Treatment programs for children diagnosed as obese are not included, since this represents treatment of an already developed condition (although it is recognized that the treatment of childhood obesity may affect that proportion of adult obesity that is carried over from childhood). Programs that target high-risk but still nonobese children or adolescents in order to develop lifetime behavioral patterns protecting against obesity would quality.
Personal high-risk factors for obesity include predispositional factors at the individual level (e.g., family history of obesity or non-insulin-dependent diabetes mellitus and low resting metabolic rate), personal eating habits and physical activity (e.g., a high-fat diet coupled with a sedentary lifestyle), developmental periods associated with weight gain (e.g., early childhood, prepuberty, ages 25–34, and late adulthood), and critical life events (e.g., pregnancy and menopause). Other demographic risk factors include gender (women are heavier than men, particularly those with lower education and socioeconomic status) and minority status (e.g., overweight is more common in black and Hispanic females) (Sobal and Stunkard, 1989).
Many commercial weight-loss programs and diets are geared to the general population, including a majority of people who are overweight but not necessarily obese. Since studies show that even a relatively small
loss of weight can provide health benefits (see Chapter 2), this large population of dieters may benefit from prevention-based programs (e.g., by developing a healthier lifestyle).
Outcome Measures for Selective Prevention
Selective prevention has three outcome measures:
-
prevention of weight gain in high-risk individuals and groups;
-
decreased excessive dieting among dieters; and
-
improved lifestyle patterns (better nutrition, more exercise, and decreased eating disorders).
Examples of Selective Prevention Programs
Programs That Target Overweight Adolescents in High-Risk Groups
Some school-based programs target populations that are at high risk for obesity. Examples include minority school populations such as Native American and Mexican-American school children. Davis et al. (1993b) describe a school-based program for navajo and Pueblo children from rural elementary schools in New Mexico. Foreyt and Cousins (1993) describe school-based programs for Mexican-American children. Both studies are in progress and no results have been published.
Commercial Weight-Loss Programs and Diets
As described in Chapters 1 and 2, weight loss is big business. However, since not everyone who diets or attends a commercial program is obese, many overweight, nonobese people are involved in these programs. In the face of data showing high relapse rates in follow-ups of commercial diet programs, some programs now deemphasize fixed dietary weight-loss goals in favor of a more balanced, lifestyle-change program focusing, for example, on healthier eating habits, exercise, and maintenance of weight loss (see Table 3-1). These programs may be effective in the selective prevention of obesity among high-risk groups.
INDICATED PREVENTION
In the past, indicated prevention has sometimes been referred to as secondary prevention or early intervention. With regard to obesity prevention, indicated preventive methods or programs can be designed for individuals
(in contrast to entire groups, as in selective prevention) who show biological markers for obesity or who are already overweight but do not meet the diagnostic criteria for obesity. Risk factors for such individuals include a family history of obesity as well as biological markers and the development of early symptoms of the disorder. Although research is still in the preliminary stages of identifying reliable biological markers, programs that target individuals who are already overweight (or whose health risks are increased owing to their weight and/or a sedentary lifestyle) may prove effective.
Outcome Measures for Indicated Prevention Programs
There are two outcome measures for indicated prevention programs:
-
reduction in the number of obese people who go on to develop obesity-related comorbidities (e.g., reduced adult obesity among overweight children receiving intervention in childhood); and
-
increase in the number of obese people who are successful in attaining and maintaining relatively small weight losses (e.g., 10 percent of initial body weight) and a decrease in the number who gain a small amount of weight (e.g., 2 kg).
Examples of Indicated Prevention
Promising results have been reported by Epstein et al. (1990c). Although this study could also be considered a treatment program for obese children (since subjects had to be ≥ 20 percent over ideal body weight for age, height, and sex), its goal was to prevent adult obesity. We include this study as an example because the same approach could be adopted with children who are overweight but not obese. In the study, Epstein and colleagues used a prospective, randomized design to examine the effects of behavioral, family-based treatment on percent overweight and growth over 10 years in obese 6- to 12-year-old children. Obese children with their parents were randomized to three groups that were provided similar diet, exercise, and behavior-management training, but differed in the way in which behavioral reinforcement was provided. In one group, both parent and child were reinforced; in the second only the child was reinforced. The third group was a nonspecific control group in which families were reinforced for attendance only. Children in the first group showed significantly greater decreases in percent overweight after 5 and 10 years (-11.2 and -7.5 percent, respectively) than children in the nonspecific control group (+7.9 and +14.3 percent, respectively). Results of
children in the second group were midway between the other two groups, but not significantly different from either.
This study has been replicated in three additional randomized treatment studies designed to change the diet and exercise behaviors of obese children treated with behavioral family therapy (Epstein et al., 1994). Averaging across all four studies, Epstein and colleagues note that over a 10-year period, 34 percent of their subjects decreased their percent overweight by ≥ 20 percent, and 30 percent were no longer obese. The children did best when both they and their parents were targeted and reinforced for weight loss and when the children were treated with aerobic exercise and exercise was incorporated into their lifestyle. This 10-year success in the treatment of childhood obesity stands in marked contrast to the disappointing long-term results in treating adult obesity (Wilson, 1994a).
CONCLUDING REMARKS
Many approaches to prevent obesity appear promising, though few studies are available to document long-term positive outcomes. Since success in prevention programs is often equated with the absence of future problems, the impact of universal prevention programs that target education and behavior change (e.g., in diet or exercise patterns) is difficult to evaluate except through longitudinal population studies. The recent literature in prevention has focused more on working with groups or individuals who are known to be at risk for a particular disorder. The emphasis on working with high-risk individuals with interventions that are matched or targeted to specific risk factors (as in selective and indicated prevention strategies) appears to have considerable merit. Only a few studies of this type have been conducted in obesity prevention. Future research on the development of prevention programs targeted to those at high risk for obesity is necessary before any conclusions can be drawn concerning this promising new approach.











