
13 Polynuclear Aromatic Hydrocarbon (PAH) Toxicity
|
Environmental ALERT…
|
This monograph is one in a series of self-instructional publications designed to increase the primary care provider’s knowledge of hazardous substances in the environment and to aid in the evaluation of potentially exposed patients. The Agency for Toxic Substances and Disease Registry (ATSDR) and the Centers for Disease Control (CDC) designate this continuing medical education activity for 1 credit hour in Category 1 of the Physician’s Recognition Award of the American Medical Association and 0.1 continuing education units for other health professionals. See pages 17 to 19 for further information.
|
Guest Contributor: |
Jacek Brudzewski, MD |
|
Guest Editor: |
Dennis Shusterman, MD, MPH |
|
Peer Reviewers: |
Charles Becker, MD; Jonathan Borak, MD; Joseph Cannella, MD; Bernard Goldstein, MD; Alan Hall, MD; Richard J.Jackson, MD, MPH; Jonathan Rodnick, MD; Robert Wheater, MS; Brian Wummer, MD |

U.S. DEPARTMENT OF HEALTH & HUMAN SERVICES
Public Health Service
Agency for Toxic Substances and Disease Registry
Case Study
Dyspnea, weight loss, and weakness in a 52-year-old incinerator worker
A 52-year-old man is seen at your office for a health evaluation, his first in 3 years. While trying to assure you that he is in reasonably good health, he admits that this visit was prompted by his wife, who is concerned about his weight loss, lack of stamina, and weakness in the shoulders and arms. Chart review indicates a weight loss of 30 pounds since his last visit. The patient also describes shortness of breath with moderate activity. He is a lifelong nonsmoker and drinks alcohol only occasionally. He is taking no medications. Past history is noncontributory. Review of systems reveals the patient also has a chronic, intermittently productive cough and constipation of 1 month’s duration.
Social history indicates that the patient has worked at a municipal incineration plant for the past 34 years and has been a lifelong resident of an urban industrial neighborhood approximately 1 mile from where he works. He has been married for 25 years; his wife and adult daughter are in good health.
On physical examination, vital signs are normal. Inspection of the skin reveals multiple dry, scaly, hyper-pigmented macules involving the forehead, temporoparietal areas, eyelids and brows, and several hyperkeratotic papillomata about the face, neck, upper chest, forearms, and hands. On palpation of the right supraclavicular area, a 2×3-cm firm, nontender fixed lymph node is detected. Auscultation discloses intermittent, scattered right-sided wheezes and dry bibasilar crackles. The remainder of the exam is unremarkable.
Laboratory results are remarkable for the following: hemoglobin 12.9 g/dL (normal 14 to 18 g/dL), hematocrit 36% (normal 42 to 52%), leukocyte count 2.9×103/µL (normal 3.9 to 11×103/µL), serum calcium 12.9 mg/dL (normal 8.5 to 10.5 mg/dL), alkaline phosphatase 483 IU/L (normal 30 to 125 IU/L) with concomitant elevation of GGTP (GGT), SGOT (AST) 121 IU/L (normal 7 to 45), and SGPT (ALT) 129 IU/L (normal 7 to 35 IU/L). The chest X ray reveals a 3.3-cm central, thick-walled, cavitating lesion with irregular, spicular margins in the right upper lobe, and atelectasis and prominence of the right hilar lymphatics.
![]()
(a) What should be included on this patient’s problem list?
_________________________________________________________________
(b) What is the differential diagnosis?
_________________________________________________________________
(c) What treatment would you recommend for this patient?
_________________________________________________________________
Answers to the Pretest can be found in Challenge answers (5) through (7) on page 15.
Exposure Pathways
❑ PAHs are a class of organic compounds produced by incomplete combustion or high-pressure processes.
❑ PAHs are ubiquitous in the environment.
Polycyclic aromatic hydrocarbons (PAHs) are organic compounds consisting of three or more fused benzene rings containing only carbon and hydrogen (Figure 1). PAHs form when complex organic substances are exposed to high temperatures or pressures. Hundreds of such compounds exist. They are a natural component of most fossil fuels.
Figure 1. Structural formulas of selected polyaromatic hydrocarbons (PAHs). The arrows indicate “bay” regions (discussed on page 6).
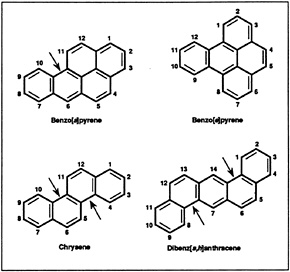
At room temperature, PAHs are solids with low volatility. They are soluble in many organic solvents and are relatively insoluble in water. Most PAHs can be photo-oxidized and degraded to simpler substances.
PAHs are ubiquitous in the environment. Also known as polynuclear aromatics (PNAs) or polycyclic organic matter (POM), the more common PAHs include benzo(a)pyrene, benzo(e)pyrene,
❑ Cigarette smoke contains numerous PAHs.
benzo(a)anthracene, chrysene, pyrene, benzo(k)fluoranthene, benzo(g,h,i)perylene, coronene, dibenz(a,h)anthracene, and dibenz(a,h)acridine. Benzo(a)pyrene (B[a]P) is the most carcinogenic PAH studied.
Although PAHs are produced naturally by forest fires and volcanoes, most PAHs in ambient air are the result of burning coal, wood, petroleum, petroleum products, or oil; and of coke production, refuse burning, and motor vehicle exhaust. PAHs are found in industries that produce or use coal tar, coke, or bitumen (asphalt); they are also produced in coal gasification plants, smokehouses, municipal incinerators, and some aluminum production facilities. In cities with coke ovens the concentration of airborne PAHs may reach 150 nanograms per cubic meter of air (ng/m3). (The permissible workplace exposure limit for coke oven emissions is 150,000 ng/m3.) Coal tar pitch and creosote, which are complex mixtures of liquid and solid aromatic hydrocarbons produced in coke ovens, contain significant amounts of B(a)P and other PAHs.
Water and soil contain measurable amounts of PAHs, primarily from airborne fallout. Water contamination also occurs from industrial effluents and accidental spills during oil shipment at sea. Documented levels of PAHs in soil near oil refineries have been as high as 200 nanograms per kilogram (ng/kg) of dried soil; those from soil samples obtained near cities and areas with heavy traffic typically are greater by tenfold. PAHs can leach from soil into water. Concentrations of B(a)P in drinking water are generally lower than those in untreated water and about a hundredfold lower than the U.S. Environmental Protection Agency’s (EPA) proposed drinking water standard. (EPA’s proposed maximum contaminant level goal [MCLG] for B(a)P in drinking water is 0.2 parts per billion [ppb].)
PAH concentrations in foodstuffs vary. Charring meat or barbecuing food over a charcoal fire greatly increases the concentration of PAHs. Cooked and smoked meats and fish are higher in PAHs than uncooked products, with up to 2.0 micrograms per kilogram (µg/kg) of B(a)P detected in smoked fish. Roasted peanuts and coffee, refined vegetable oil, and many other foodstuffs contain PAHs, and some crops such as wheat, rye, and lentils may synthesize PAHs.
Cigarette smoke contains numerous PAHs. According to one study, a cigarette yields 10 to 50 ng B(a)P, 18 ng chrysene, 40 ng dibenz(a,h)anthracene, and 12 to 140 ng benz(a)anthracene. Filtered cigarettes remove some, but not all, PAHs from cigarette smoke inhaled by the smoker.
|
(1) What are likely sources of PAHs for the patient described in the case study? _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ |
Who’s at Risk
❑ Persons working with coal and coal products have a greater likelihood of exposure to PAHs.
❑ AHH-inducible persons may be at greater risk from PAHs’ effects.
Percival Pott, an English surgeon, was the first to report a connection between occupation and cancer. In 1775, he described an unusually high incidence of scrotal cancer among London chimney sweeps and suggested this was due to their exposure to soot and ash. Since then other coal tar-related cancers have been induced in laboratory animals and noted in humans. The PAH benzo(a)pyrene, which was isolated from coal tar in the 1930s, was determined to be carcinogenic when applied to the skin of test animals. Since then, hundreds of PAHs have been described; many of them are carcinogenic.
Workers in industries or trades using or producing coal or coal products are at highest risk of PAH exposure and include, but are not limited to, the following:
aluminum workers
asphalt workers
carbon black workers
chimney sweeps
coal-gas workers
coke oven workers
fishermen (coal tar on nets)
graphite electrode workers
machinists
mechanics, auto and diesel engine
printers
road (pavement workers)
roofers
steel foundry workers
tire and rubber manufacturing workers
workers exposed to creosote:
carpenters
farmers
railroad workers
tunnel construction workers
utility workers
Fetuses may be at risk of PAHs’ effects. Various animal studies have confirmed that PAHs and metabolites cross the placenta, affecting the offspring. Animals exposed to PAHs in utero show
a decrease in the number of functional oocytes, often to the point of infertility. Because PAHs are excreted in breast milk, nursing infants of exposed mothers can be secondarily exposed.
Persons with a high degree of aryl hydrocarbon hydroxylase (AHH) inducibility may constitute a high-risk population. Genetic variation in AHH inducibility has been implicated as a determining factor for susceptibility to lung and laryngeal cancer. Several studies support the hypothesis that persons with lung cancer have higher AHH inducibility in cultured lymphocytes or in peripheral lung tissue than those who do not develop lung cancer.
|
(2) Besides the patient, who in the case study may be at risk of PAH exposure? _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ |
Biologic Fate
❑ PAHs are metabolized in a number of organs and are excreted in bile and urine.
❑ PAHs are excreted in breast milk and are stored to a limited degree in adipose tissue.
PAHs are absorbed through ingestion, inhalation, and dermal contact. Although no precise data regarding the metabolic fate of PAHs exists for humans, information on absorption, distribution, and elimination of these substances is available from animal studies. After absorption, PAHs enter the lymph, circulate in the blood, are metabolized primarily in the liver and kidney, and are excreted in both bile and urine. Because of their lipophilic nature, PAHs can accumulate in breast milk and adipose tissue; however, biliary and urinary excretion of PAHs is relatively efficient because of the wide distribution of enzymes that transform PAHs into polar metabolites.
In addition to the liver and kidneys, metabolism of PAHs occurs in adrenal glands, testes, thyroid, lungs, skin, sebaceous glands, and small intestine. PAHs are probably transformed initially to epoxides, which are converted to dihydrodiol derivatives and phenols. Glucuronide and sulfate conjugates of these metabolites
are excreted in the bile; glutathione conjugates are further metabolized to mercapturic acids in the kidney and are excreted in the urine. Metabolism is a prerequisite for hepatobiliary excretion and elimination through the feces, regardless of route of entry.
Some parent PAHs are weak carcinogens and require metabolism to become more potent carcinogens. Diol epoxides, proposed PAH intermediate metabolites, are presumed to be mutagenic and may affect normal cell replication when they react with DNA to form adducts. The bay region theory states that an epoxide will be highly reactive if it is located in the “bay” region of the PAH molecule (Figure 1).
|
(3) Additional information for the case study: the patient’s daughter, who has lived in his household all her life, recently gave birth to a daughter. Is the newborn at risk from PAH exposure? _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ |
Physiologic Effects
❑ The most significant endpoint of PAH toxicity is cancer.
PAHs generally have a low degree of acute toxicity to humans. Many PAHs are only sightly mutagenic or even nonmutagenic in vitro; however, their metabolites or derivatives can be potent mutagens. Interaction of PAH metabolites with DNA is believed to be the mechanism of PAH-related carcinogenesis.
The carcinogenicity of certain PAHs is well established in laboratory animals; increased incidence of skin, lung, liver, and stomach cancer have been reported, as well as injection-site sarcomas. Animal studies indicate that certain PAHs also can affect the hematopoietic and immune systems, and can produce reproductive and developmental effects.
Carcinogenicity
❑ Increased incidences of lung, skin, GI, and genitourinary cancers are associated with occupational exposure to PAHs.
Epidemiologic reports of PAH-exposed workers have noted increased incidences of skin, lung, bladder, and gastrointestinal cancers. These reports, however, provide only qualitative evidence of the carcinogenic potential of PAHs in humans due to the presence of multiple PAH compounds and other putative carcinogens and indicate the lack of quantitative monitoring data.
The earliest human PAH-related epidemiologic study was reported in 1936 by investigators in Japan and England who studied lung cancer mortality among workers in coal carbonization and gasification processes. Subsequent U.S. studies among coke oven workers confirmed an excess of lung cancer mortality with the suggestion of excessive genitourinary system cancer mortality. Later experimental studies showed PAHs in soot were probably responsible for the increased incidence of scrotal cancer among London chimney sweeps noted by Percival Pott.
PAH-induced carcinogenesis may result when a PAH-DNA adduct forms at a site critical to the regulation of cell differentiation or growth. A mutation occurs during cell replication if the aberration remains unrepaired. Cells affected most significantly by acute PAH exposure appear to be those with rapid replicative turnover, such as those in bone marrow, skin, and lung tissue. Tissues with slower turnover rates, such as liver tissue, are less susceptible.
|
(4) How could you document that the work environment of the patient described in the case study contributed to his risk of lung cancer? _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ |
Clinical Evaluation
History and Physical Examination
❑ Physical examination includes review of all systems.
Pertinent history includes the patient’s occupational history, occupation of spouse and other household members, medications including coal tar-containing dermatologic preparations, and diet, especially charbroiled meats, alcohol consumption, and smoking habits. Hobbies and activities may reveal additional evidence of exposure to PAH-containing mixtures.
Physical examination should include review of all systems, keeping in mind that cancer is the most significant endpoint of chronic PAH toxicity. If PAH exposure is suspected, the clinician should be alert to malignant transformation of actinic skin lesions. The bucal mucosa and oropharynx should be inspected for malignant changes. Inspection of sun-exposed areas for evidence of hyperpigmentation in response to sunlight is advised. Patients who chronically inhale PAHs should have periodic chest X rays and pulmonary function tests.
Signs and Symptoms
Acute Exposure
❑ Acute effects attributed to PAH exposure are probably caused by other agents.
PAHs have low acute toxicity. Other, more toxic agents probably cause those acute symptoms attributed to PAHs. Hydrogen sulfide in roofing tars and sulfur dioxide in foundries are examples of concomitant, acutely toxic contaminants.
Chronic Exposure
❑ Effects reported from occupational exposure to PAHs include chronic bronchitis, dermatitis, cutaneous photosensitization, and pilosebaceous reactions.
The following is a list of reported effects associated with chronic exposure to coal tar and its byproducts:
Skin: erythema, burns, warts on sun-exposed areas with progression to cancer. Toxic effects of coal tar are enhanced by exposure to ultraviolet light.
Eyes: irritation and photosensitivity.
Respiratory system: cough, bronchitis, and bronchogenic cancer.
Gastrointestinal system: leukoplakia, bucal-pharyngeal cancer, and cancer of the lip.
Hematopoietic system: leukemia (inconclusive) and lymphoma.
Genitourinary: hematuria, kidney and bladder cancers.
Laboratory Tests
Direct Biologic Indicators
❑ Direct biologic measurement of PAHs is neither cost-effective nor clinically useful.
Although researchers have examined PAHs directly in the blood and tissues of experimental animals, these methods have not been widely used for human samples. High costs of testing and lack of knowledge of normal background levels in humans limit their clinical usefulness.
Indirect Biologic Indicators
❑ A recently developed technique measures serum antibodies to PAH-DNA adducts.
The most common tests for determining exposure to PAHs involve examining tissues, blood, and urine for the presence of metabolites. For example, tissue in culture can be labeled with radioactive phosphorus and analyzed by thin-layer chromatography and scintillation to identify and quantify the DNA adducts formed. Also, an immunoassay technique, for which a patent is pending, has been developed to detect antibodies to the PAH-DNA adducts in blood.
Recently it has been established that PAH diol epoxides form adducts with hemoglobin in the red blood cells; the adducts can be quantified using fluorescence spectroscopy. This technique is limited in its potential usefulness, however, due to individual differences in PAH metabolism and the limited specificity of the technique itself.
In general, biologic monitoring can be useful in determining whether exposure to PAHs has occurred, but it is not clinically useful for evaluating individual patients because normal or toxic levels have not been determined. Individual variability, confounding effects of drugs or cigarettes, and nonspecificity of techniques are likely to complicate the interpretation of the results, especially in low-level environmental exposures.
|
(5) Before his present employment, the patient was employed as a laborer on a farm. He denies exposure to pulmonary toxic agents such as asbestos or silica. What is the problem list and differential diagnosis for the patient described in the case study? _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ (6) What is the significance of elevated levels of aryl hydrocarbon hydroxylase? _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ |
Treatment and Management
Acute Exposure
❑ Decontamination and life-support measures are the primary objectives after acute PAH exposure.
Contaminated clothing should be removed from victims as soon as possible. The skin should be decontaminated by gently scrubbing with soap and water. Ocular contamination should be treated with irrigation and a complete eye examination. In the event of an acute inhalation exposure, ventilatory support should be tailored to the patient’s clinical condition. Most acute respiratory injury in PAH-containing work environments occurs from exposure to gases, fumes, and dusts containing various toxic agents rather than to PAHs.
Chronic Exposure
❑ Treatment of chronic PAH toxicity is symptomatic. ❑ Education is an important aspect of patient care.
Treatment of PAH-related disease begins with patient education. Persons exposed to potentially significant levels of PAHs should be aware of the increased risk of cancer and the additive effect of cigarette smoke and other toxic agents. Periodic evaluation of healthy patients who have been significantly exposed to PAHs, even in the absence of symptoms, is recommended to facilitate early diagnosis and intervention should a malignancy develop.
Predicting the carcinogenicity of a complex chemical mixture on the basis of one or several of its components is difficult because of possible interactions among the components. Interactions of various PAHs have been shown to produce both synergistic and antagonistic effects in mutagenicity tests in vitro. Because estimation of additional risk due to PAH exposure is often impossible, the challenge to the clinician is maintaining a balance between appropriate concern and undue alarm.
|
(7) The diagnosis for the patient described in the case study is lung cancer with classification T2, N3, M0. What treatment do you recommend? _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ (8) In general, what can you do to decrease the risk of lung cancer among your patients? _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ |
Standards and Regulations
Workplace
Air
❑ The OSHA PEL for PAHs in the workplace is 0.2 mg/m3.
The PAH workroom air standard mandated by the Occupational Safety and Health Administration (OSHA) is an 8-hour time-weighted average (TWA) permissible exposure limit (PEL) of 0.2 mg/m3, measured as the benzene-soluble fraction of coal tar pitch volatiles. The OSHA standard for coke oven emissions is 0.15 mg/m3. The National Institute for Occupational Safety and Health (NIOSH) has recommended that the workplace exposure limit for PAHs be set at the lowest detectable concentration, which was 0.1 µg/m3 at the time of the recommendation. The standards and regulations for PAHs are summarized in Table 1.
Table 1. Standards and regulations for PAHs
|
Agency |
Focus |
Level |
Comments |
|
ACGIH |
Air-Workplace |
0.2 mg/m3 |
Advisory; TWA† |
|
NIOSH |
Air-Workplace |
0.1 mg/m3 |
Advisory; Recommended exposure limit |
|
OSHA |
Air-Workplace |
0.2 mg/m3 |
Regulation; (Benzene soluble fraction of coal tar volatiles) PEL§ over 8-hour workday |
|
EPA |
Water |
0.2 ppb |
Proposed maximum contaminant level goal (MCLG) for B(a)P; Proposed MCLG for PAHs is zero |
|
*ACGIH=American Conference of Governmental Industrial Hygienists; EPA=Environmental Protection Agency; NIOSH=National Institute for Occupational Safety and Health; OSHA= Occupational Safety and Health Administration †TWA (Time-Weighted Average)=time-weighted average concentration for a normal 8-hour workday and 40-hour workweek to which nearly all workers may be repeatedly exposed. §PEL (Permissible Exposure Limit)=highest level in air, averaged over a normal workday, to which a worker may be exposed. |
|||
Environment
Water
❑ The maximum contaminant level goal for B(a)P in drinking water is 0.2 ppb.
In 1980, EPA developed ambient water quality criteria to protect human health from the carcinogenic effects of PAH exposure. The recommendation was a zero (nondetectable) level for carcinogenic PAHs in ambient water. Because attainment of this level may be currently impossible, EPA will recommend maximum contaminant level goals (MCLG) for individual PAHs in June 1990. The MCLG for B(a)P, the most carcinogenic PAH, will be 0.2 ppb. EPA is also considering setting MCLGs for five additional carcinogenic PAHs: benz(a)anthracene, benzo(k)fluoranthene, chrysene, dibenz(a,h)anthracene, and indenopyrene.
Food
No standards for governing the PAH content of foodstuffs have been established by the Food and Drug Administration.
|
(9) Would you consider the patient described in the case study a sentinel case requiring notification of public health agencies? Explain. _________________________________________________________________ _________________________________________________________________ _________________________________________________________________ |
Suggested Reading List
Reviews
Zedeck MS. Polycyclic aromatic hydrocarbons: a review. J Environ Pathol Toxicol 1980;3:537–67.
Biologic Testing
Harris CC, Newman MJ, Weston A, Mann DL. Identification of human antibodies to polycyclic aromatic hydrocarbon-DNA adducts. Clin Res 1986;34:690A.
Haugen A, Becher G, Benestad C et al. Determination of polycyclic aromatic hydrocarbons in the urine, benzo(a)pyrene diol epoxide-DNA adducts in lymphocyte DNA, and antibodies to the adducts in sera from coke oven workers exposed to measured amounts of polycyclic aromatic hydrocarbons in the work atmosphere. Cancer Res 1986;46:4178–83.
Jongeneelen FJ, Bos RP, Anzion RBM, Theuws JL, Henderson PT. Biological monitoring of polycyclic aromatic hydrocarbons: metabolites in urine. Scand J Work Environ Health 1986;12:137–43.
Metabolism and Carcinogenesis
Levin W, Wood A, Chang RL, et al. Oxidative metabolism of polycyclic aromatic hydrocarbons to ultimate carcinogens. Drug Metab Rev 1982;13:555–80.
Related Government Documents
Agency for Toxic Substances and Disease Registry. Toxicological profile for polycyclic aromatic hydrocarbons (draft). Atlanta: US Department of Health and Human Services, Public Health Service, 1990.
Agency for Toxic Substances and Disease Registry. Toxicological profile for benzo(a)pyrene. Atlanta: US Department of Health and Human Services, Public Health Service, 1988.
Agency for Toxic Substances and Disease Registry. Toxicological profile for dibenz(a,h)anthracene. Atlanta: US Department of Health and Human Services, Public Health Service, 1988.
Agency for Toxic Substances and Disease Registry. Toxicological profile for benz(a)anthracene. Atlanta: US Department of Health and Human Services, Public Health Service, 1988.
Agency for Toxic Substances and Disease Registry. Toxicological profile for benzo(b)fluoranthene. Atlanta: US Department of Health and Human Services, Public Health Service, 1988.
Environmental Protection Agency. Health effects assessment for polycyclic aromatic hydrocarbons (PAH). Cincinnati: Environmental Criteria and Assessment Office, 1984. EPA report no. 540/1–86–013.
Environmental Protection Agency. An exposure and risk assessment for benzo(a)pyrene and other polycyclic aromatic hydrocarbons. Vol IV. Washington DC: Office of Water Quality. Report no. EPA 4–85–020–V4.
Answers to Pretest and Challenge Questions
-
The patient may have been exposed to incinerator-generated pollutants at his work for over 34 years. Moreover, if his home and immediate environs are in the prevailing downwind direction from the incinerator plant, there may be ambient air contamination from ash, dust, soot, and smoke. The patient may have been exposed to PAHs by all three routes: inhalation, ingestion, and direct cutaneous contact.
-
Workers at the incinerator plant and residents in the community downwind from the incinerator may be exposed to PAHs. The patient’s family members may have added exposure if the patient carried these compounds home on his skin and work clothes.
-
Yes, if the patient’s daughter breathed contaminated air in and around the house, engaged in various household chores such as laundering, dusting, and general cleaning of the contaminated home or her father’s work clothing, then the baby could have been exposed in utero. PAHs absorbed into the mother’s system may continue to be transferred to the infant via breast milk. The newborn may also be breathing contaminated air, thereby increasing her exposure.
-
The role of the workplace in the patient’s PAH exposure can be determined by area sampling at the work site, individual monitoring, medical surveillance of coworkers, and air sampling within the immediate community. A first step would be to determine if this data is available through sources at the incinerator plant and local, state, or federal agencies. While this information most likely will not aid the diagnosis or influence the treatment or outcome of a specific case, it may have legal and financial implications in workers’ compensation issues.
-
The patient’s problem list includes weight loss, fatigue, muscle weakness, skin lesions on exposed areas, exertional dyspnea, and a roentgenographically identified cavitating lesion in the right upper lobe with associated lymphadenopathy. The differential diagnosis includes carcinoma of the lung, tuberculosis, fungal lung infection, and lung abscess.
-
Aryl hydrocarbon hydroxylase (AHH) inducibility is genetically determined. An elevation in pulmonary and serum levels of this enzyme signifies an additional risk factor for the development of pulmonary and laryngeal carcinoma. The test, however, is a research tool and is not readily available.
-
The patient has squamous cell carcinoma and his condition is considered inoperable. Treatment options would consist of radiation or radiation with chemotherapy.
-
The main objective is to educate patients about cancer prevention. You should try to stimulate changes in their work habits and lifestyle that will decrease the risk of developing cancer. A risk assessment can identify elements in a person’s workplace, family history, medical history, and lifestyle that may be controllable risk factors.
For example, between 75% and 80% of all cases of bronchogenic carcinoma are due to cigarette smoking and are therefore preventable. Of the remaining 20% to 25%, many are occupationally or environmentally related and could therefore be prevented by appropriate workplace or environmental controls. Education for smoking prevention, improved working conditions, substitution of less hazardous materials in work processes and building materials, and increased awareness of personal risk factors may decrease the incidence of lung cancer.
-
Squamous cell carcinoma does not require a report to any public health agency or authority. However, in view of the patient’s medical, social, occupational, and family history, workplace and environmental factors emerge as the most likely causal factors in the development of his neoplastic disease. When the potential exists for others to be exposed, serious illness related to occupational or environmental factors should be reported to the appropriate state and federal authorities. For example, OSHA would have responsibility for PAHs in the workplace air at the incinerator site, and EPA would have responsibility for the level of emissions to the ambient air or water. Inclusion of this case in a tumor registry should also be considered.
Sources of Information
More information on the adverse effects of PAHs and the treatment and management of PAH-exposed persons can be obtained from ATSDR, your state and local health departments, and university medical centers. Case Studies in Environmental Medicine: Polyaromatic Hydrocarbons (PAHs) Toxicity is one of a series. For other publications in this series, please use the order form on the back cover. For clinical inquiries, contact ATSDR, Division of Health Education, Office of Director, at (404) 639–0730.

















