3
Physicians and Physicists: The Interdisciplinary Introduction of the Laser to Medicine
JOANNE SPETZ
The laser was heralded by professionals and the press, even before the first one was built in 1960. Although it was initially unclear to researchers what the laser's uses might be, there was much excitement in both the creation of the laser and the subsequent development of applications. The laser's potential in surgery was envisioned almost immediately by some of its developers owing to its ability to burn through materials; still, it is surprising that only one year after the laser's invention, it was used by an ophthalmologist to repair a retina. Most medical doctors are not educated in the principles of quantum physics, nor are physicists and engineers fully trained in the biological sciences. What institutions and relationships resulted in the development of the laser photocoagulator? The answer to this question lies in the story of the laser's development.
Scientists from many disciplines became involved in laser research in the 1960s; the laser was studied for applications in measurement, industrial production, spectroscopy, weaponry, and medicine. Such widespread interest in the laser largely resulted from the fact that the laser's creation was an interdisciplinary enterprise. The invention of the laser required the collaboration of physicists and engineers, most of which occurred in private companies. The subsequent development of laser applications followed this pattern of interdisciplinary research. The willingness of private industry to aggressively organize relationships between scientists and engineers led to the rapid introduction of the laser to medicine. By understanding the nature of these relationships and the factors that influenced them, we might better understand how new medical technologies are conceived and created.
THE LASER'S INVENTION
The demonstration of a working ruby laser by Theodore Maiman at Hughes Aircraft Corporation (see Maiman, 1960) was the culmination of over a decade of research in the stimulation of radiation, which began early in this century. In 1916, Albert Einstein laid the foundation for the invention of the laser and its predecessor, the maser, in a proof of Planck's law of radiation.1 In 1900 the German physicist Max Planck had proposed a formula relating atoms to the spontaneous emission of electromagnetic energy. Einstein sought to relate Planck's proof to his own theories of quantum mechanics; he suggested that photon emission could be stimulated, not just spontaneously produced (see the technical appendix for a detailed explanation of laser theory). Einstein's proposal was ignored, however, until after World War II.
During World War II, several laboratories were established to develop radar. The most prominent laboratories were the Massachusetts Institute of Technology (MIT) Radiation Laboratory and the Columbia University Radiation Laboratory in the physics department. These research sites were enormously successful, and in 1946 the Joint Services Electronics Program (JSEP) was established to continue laboratory funding in peacetime. The main recipients of JSEP funds were MIT and Columbia University, and JSEP founded laboratories at Harvard in 1946 and Stanford in 1947. A variety of military projects were funded at these laboratories; one of the beneficiaries of JSEP was Charles Townes of Columbia University.
Townes had worked on radar bombing systems at Bell Laboratories in New Jersey during World War II and was a founding father of molecular and millimeter-wave spectroscopy. He became deeply involved in spectroscopy after the war, and military experts thought his work could be used in radar. Prior research of the electromagnetic spectrum had been sequential; the longest waves (electric current) were studied first, followed by shorter radio waves and then microwaves. It seemed logical to physicists to continue this pattern of development, so many projects sought to conquer waves of millimeter length. Waves with a higher frequency would be more compact than radar waves and had the potential to provide greater secrecy in communication. In 1950, the U.S. Office of Naval Research asked Townes to organize the Advisory Committee on Millimeter Wave Generation. The following year, while in Washington, D.C., to attend this committee meeting, Townes was inspired with an idea while sitting on a park bench. He thought that an oscillator made with deuterated ammonia (ND3) might cause the emission and amplification of microwaves (10-3 to 1 meter wavelengths).2
Townes' colleagues were skeptical of this idea and argued that a high-frequency emission could not result from Townes' device. Despite the lukewarm reception of his ideas, Townes began work on an oscillator with Herbert J. Zeiger, a postdoctoral student, and James P. Gordon, a doctoral candidate, in the fall of 1951.
Zeiger and Gordon began to build what Townes later called a MASER—Microwave Amplification by Stimulated Emission of Radiation—in 1952. Construction was supported by the Army Signal Corps, the U.S. Air Force, and the Office of Naval Research through JSEP. Zeiger left the project in February 1953 when his postdoctoral appointment ended but Gordon continued working with Townes. They demonstrated the amplification of microwaves by the end of the year and, in April 1954, generated a microwave oscillation with a power output of 0.01 microwatt. An explosion of MASER (now "maser") research followed their announcement.
Part of Townes' success with the maser can be attributed to his education as an electrical engineer. His approach to his work involved a combination of physics theory and engineering application. Once he was convinced that a maser could work, he focused on the task of engineering a device to prove his theory. Townes' association with several corporations through the Carbide and Carbon Chemicals Corporation Post-graduate Fellows Program at Columbia's Radiation Laboratory was also a result of his engineering background. This was one of the ways he kept abreast of the commercial possibilities of his research. He was aware that the maser could prove useful in many industrial and military applications.
Following the invention of the maser, many researchers began to develop applications for it. Government agencies explored several uses for the maser. Because a very narrow band of wavelengths are emitted by a maser, the maser was an attractive candidate for measurement applications such as a frequency standard or an atomic clock.3 Private companies, especially those with close ties to the military, sought to reap profit from Townes' invention. The military was interested in having a portable generator of a frequency standard for guided missiles and the Army Signal Corps Engineering Laboratory provided funding to the Jet Propulsion Laboratory in Pasadena, California, to research this.4 Hughes Aircraft's Research and Development Laboratory hired the former chief of the Microwave Standards Section of the National Bureau of Standards to improve Hughes' competitiveness for military contracts.
A result of maser research was a closer relationship between engineering and
physics. Private companies hired both engineers and physicists for their new millimeter-wave research laboratories and as engineers entered the field they made significant contributions in the development of maser systems. Because the maser made understanding quantum mechanics necessary for electrical engineering, engineering curricula were altered throughout the United States in the late 1950s. Schools decided to diversify engineering education and to increase the scientific content of course work. Older graduate students and professors had to learn new material to remain at the forefront of engineering.5 Interdisciplinary educations and collaborations were key to the inventions of both the maser and the laser and to the development of applications for them.
After conquering the emission of waves in the radio and microwave spectra, many scientists viewed the infrared region (10-6 to 10-3 meters) as the next step. Millimeter and submillimeter waves became the focus of radio engineering research in the late 1950s. Many ideas came from the maser principle and proposals for tackling this region were issued by universities, private laboratories, and Department of Defense-sponsored laboratories. At the end of the summer of 1957, Townes began a serious study of the infrared maser. As he developed ideas, he leapt over the infrared frequencies and focused on visible light (4 × 10-7 to 7 × 10-7 meter wavelengths). He began to create design ideas for an ''optical maser" and contacted Arthur Schawlow of Bell Labs, where Townes was a consultant.6 They agreed to work together and Bell Labs filed a patent application for their optical maser proposal a year later. Schawlow and Townes sent a manuscript of their theoretical calculations to Physics Review, which published their paper that year (Schawlow and Townes, 1958).
At the same time that Townes began work with Schawlow, Townes met R. Gordon Gould, a graduate student at Columbia University. Gould was working on a doctoral thesis on the energy level of excited thallium and was familiar with the parallel reflecting plates called Fabry-Perot etalons which Schawlow envisioned using for the optical maser. Gould and Townes had conversations on the general subject of radiation emission and Gould made notes about his ideas for a LASER (Light Amplification by Stimulated Emission of Radiation) in November 1957 and had them notarized.7 His notes included possible applications for a laser, such as spectrometry, interferometry, radar, and nuclear fusion. In March 1958 he took a job at Technical Research Group (TRG) without finishing his dissertation with the agreement that any inventions he had dated before his hiring date would remain his property. In July of that year, TRG gave Gould free time to work on his doctoral thesis. Gould worked on the laser instead.
He wrote detailed plans for the creation of such a device and filed a patent application in April 1959. Bell Labs won the patent in 1960 and were then
challenged by TRG and Gould. This conflict continued for several years, with Bell as the ultimate victor.8
Meanwhile, after the publication of the Schawlow and Townes (1958) paper on the optical maser, a race had begun to construct the first working laser. At least six laboratories, most in private companies, were involved in this research: Columbia University, Bell Labs, TRG, IBM, Hughes, and American Optical Corporation. The private companies expected a laser to have many applications, although there was little substantial discussion of uses for the laser until after its invention.
The first "lasing" of a substance was achieved by Theodore Maiman at Hughes on May 16, 1960, with a ruby crystal laser small enough to hold with one hand. His breakthrough was published in Nature in July of that year (Maiman, 1960) and before the year ended three other materials were lased. The new laser exhibited several previously unknown physical effects, and it was clear to scientists that much research could be done about and with the laser. The desire to develop applications for this invention led to a flurry of research, primarily by private-sector companies. Firms hoped to obtain patents for laser uses and to win military contracts before their competitors did. It is estimated that 400 to 500 laboratories were studying the laser in the early 1960s. Laser manufacturers proposed laser applications that would expand their markets: Bell Labs studied optical communications, Martin-Marietta worked on laser target designators, and Hughes Aircraft designed optical radars.
In 1963, the Proceedings of the Institute of Electronics and Electrical Engineers contained an article about the laser that reviewed anticipated applications, including medical, industrial, photographic, scientific, and communications uses (Proceedings of the IEEE, 1963). The laser was also celebrated in the popular press. Time, U.S. News and World Report, and the Wall Street Journal published articles in the early 1960s about the laser's promise for the future. In 1963 the Wall Street Journal predicted that the laser could reach $1 billion in sales by 1973 (cited in Bromberg, 1991). Such proclamations resulted in a rush of venture capital to the new laser industry. Established firms and new companies marketed commercial lasers, with the first ones being sold in 1961. By 1963, about 20 firms were selling lasers. While the sales volume was low, the availability of lasers encouraged research throughout the country.
It was during this early heyday of laser development that medical uses were envisioned and research began in New York and California. This research was a continuation of two trends in medical research: that of photocoagulation and that of studying the dangers of radiation. Relationships between medical doctors and physicists led to the introduction of the laser to these trends and the resultant production of the first medical laser device, the laser photocoagulator.
PHOTOCOAGULATION
Medical research with the laser was largely the result of a connection between the ongoing work of ophthalmologists and the laser's providing a powerful light source. In 1954 a German ophthalmologist, Gerd Meyer-Schwickerath, introduced photocoagulation to the treatment of retinal disease (see Meyer-Schwickerath, 1967, 1973). He created a device that concentrated the sun's light to a small focal point and used this light energy to create a lesion in the retina. These lesions served as welds to prevent retinal detachment which was then the leading cause of blindness despite the existence of this procedure. Before Meyer-Schwickerath's discovery, coagulation of the retina required the ophthalmologist to either apply energy on the surface of the eye with a diathermy machine or turn the eye around after loosening muscles to bore a hole in the sclera and use an inflammatory material such as lye to create an adhesion. This procedure required an inpatient hospital stay and significant recuperation time and was, as Dr. Francis L'Esperance commented, "really barbaric" (see Hecht, 1986).
In the mid-1950s, xenon high-pressure arc lamps became available. They had been developed by the American Optical Corporation in Southbridge, Massachusetts, for a movie producer and were so bright that the light would coagulate the back of the eye if a person looked at it. Zeiss Laboratories in Oberlochen, Germany, began to manufacture a photocoagulator with the xenon lamp. The first three Zeiss coagulators arrived in the United States in 1959. The recipients included the Edward S. Harkness Eye Institute at Columbia-Presbyterian Medical Center in New York and the Stanford University Medical Center.
The Zeiss photocoagulator was a great advance in the treatment of retinal disease but it had several disadvantages. Zeiss treatment requires the dilation of the pupil, and the lesions produced by the Zeiss are large since the light beams emitted are wide. Patients experience pain during the half-second treatment because, as Dr. Milton Flocks of Stanford University explained, "in half a second … the iris contracts and comes down hard, and that hurts" (personal communication, Milton Flocks, March 20, 1992). Ophthalmologists wanted a better light source for photocoagulation, and several companies experimented with improved lamps.
Photocoagulation was highly publicized, so it is not surprising that some developers of the laser recognized that their invention might provide an appropriate light source for ophthalmological treatment. Early demonstrations of the laser by Schawlow included one with a dark balloon inside a clear balloon. When he aimed the laser at the pair the light passed through the clear balloon and popped the dark one.9 He later commented that it was obvious that "once you
had a brighter light, it was worth trying" for retinal surgery (reported in Hecht, 1992). Townes also recognized this potential in ophthalmology and wrote a paper in the early 1960s about possible medical and biological uses of the laser (Townes, 1962). But before the laser was considered for therapeutic work, researchers studied the potential danger of the laser to the eye.
FEAR OF INJURY
The physicists and engineers who invented and worked with the laser recognized its danger immediately. Accounts of retinal damage caused by staring at eclipses were reported by Plato and, more recently, many people had experienced retinal burns from watching the nuclear explosions at Hiroshima and Nagasaki. When doctors began treating vision-impaired residents of Japan they conducted systematic research on flash burns of the retina. Among these researchers were William Ham, Jr., and his associates at the Medical College of Virginia. His group, with support from the Defense Atomic Support Agency, studied flash burns on rabbit retinae in the late 1950s (Ham, Jr., et al., 1963). This research alerted ophthalmologists to the dangers of powerful light sources and resulted in government sponsorship of studies of the laser's effects. The government was interested both in ensuring the safety of scientists and technicians and in developing a laser weapon.
The first papers about the laser's risks appeared in Science on November 10, 1961. Two articles were published, one by Leonard Solon, Raphael Aronson, and Gordon Gould of TRG (Solon et al., 1961) and the other by Milton M. Zaret and his associates at the New York University Medical Center (Zaret et al., 1961). Zaret served as a medical consultant to TRG and Bell Labs and was pursuing two careers: one as an ophthalmologist and one as a researcher on the effects of radiation on humans. His primary interest was (and is) the relationship between nonionized radiation and cancer, and he had been a consultant to the military for radar and microwave research. His positions at TRG and Bell required that he examine the employees of these companies to determine what levels of exposure workers had to radiation. Because he communicated directly with the companies' researchers, he heard about new and ongoing research projects. He became aware of laser research in 1959 and understood the potential optical effects of a laser; he also understood the risk of injury the laser posed, especially to the eye. Zaret had "more than a casual knowledge of physics" (personal communication, Milton M. Zaret, May 1, 1992). He had been trained as an engineer during his military service in World War II and had written a graduate chemistry thesis on the structure of the atom, a subject that would now be in the realm of atomic physics. This interdisciplinary scientific education enabled him to fully understand the laser and its effects on human tissue; every ophthalmologist who developed laser photocoagulation systems in the early 1960s had a similarly strong knowledge of physics.
Immediately after Maiman's announcement (Maiman, 1960), Zaret began to study the ruby laser's effects on human tissue. He was able to access laser equipment because of his contact with Bell Labs and TRG. He studied the lesions induced on a rabbit's retina and iris and determined that the ruby laser could cause significant damage to the human eye. The first paper on his findings was published in Science in 1961 (Zaret et al., 1961). He also recognized that this damage could be therapeutic, as photocoagulation. The accompanying article by Solon and his colleagues (1961) contained theoretical calculations of the laser's effect on the retina. Solon concluded that the ruby laser had the energy density of viewing the sun directly for 30 seconds, which is six times the density needed to burn the retina. The implication of these publications was that the laser presented a physical risk and that more research was needed to understand the laser's effects on humans. Zaret continued to study this throughout the 1960s (see Zaret et al., 1962, 1963).
Further quantitative research was conducted by Ham and his associates in the mid-1960s. Their work was funded by the U.S. Army Medical Research and Development Command, the Office of the Surgeon General, and the Defense Atomic Support Agency. They noted in a 1963 paper that there was a "recognized need to study the biological effect of lasers, especially due to the ocular hazard of retinal burns" (Ham et al., 1963). Ham's group built a ruby laser and identified thresholds for irreversible injury. The conclusion was that the ruby laser produced four levels of short-term damage to the retina: (1) blanching of the retina, (2) cavitation or bubble formation, (3) breakthrough of the vitreous, and (4) hemorrhage in addition to the first three effects. While the results of Zaret's and Ham's research might have been viewed pessimistically by those with little knowledge of medicine, the identification and description of the dangers of the laser were necessary to facilitate its development as a therapeutic tool.
POTENTIAL IN OPHTHALMOLOGY
Two groups of researchers independently began work with the laser as a therapeutic device at roughly the same time. The first group to commence experimentation was that of Dr. Charles J. Campbell of the Institute of Ophthalmology at Columbia-Presbyterian Medical Center in Manhattan and Dr. Charles Koester of the above-mentioned American Optical Corporation in Southbridge, Massachusetts. The other group was based at Stanford University and was headed by Drs. Milton Flocks and Christian Zweng. Flocks was a half-time researcher on the clinical faculty at Stanford and Zweng was a practicing ophthalmologist at the Palo Alto Medical Foundation while holding a faculty position. They collaborated with Dr. Narinder Kapany, a physicist who founded Optics Technology, Incorporated, in 1960.
These groups were similar in both their composition and their research. Both the New York and the California group were comprised of researchers from
private industry and from academic medical centers. The two companies involved, American Optical and Optics Technology, developed relationships with medical researchers in order to design and test new medical devices. The ophthalmologists did not have the means to create the laser photocoagulator without the resources of private industry, but both Charles Campbell and Milton Flocks had educations that enabled them to understand the laser. Campbell had earned a master's degree in optics from the Institute of Optics of the University of Rochester before beginning his residency in ophthalmology (personal communication, Charles Koester, April 29, 1993). Flocks had taken a graduate course in atomic physics while in college. He also had studied pathology under a Heed Fellowship at the Armed Forces Institute of Pathology before he moved to California. Lastly, Charles Campbell, Milton Flocks, and Christian Zweng had conducted research with the Zeiss photocoagulators their medical centers received in 1959.
American Optical established its laser research program in 1959 by hiring Elias Snitzer. Snitzer was a specialist in fiber optics and had developed military electro-optics in the 1950s. Shortly after Maiman's announcement of the ruby laser in 1960, Snitzer constructed one for his own experimentation. Charles Koester was simultaneously developing an improved photocoagulator with a mercury arc lamp. Since Snitzer knew of Koester's project, he realized that the laser had potential for photocoagulation. Sometime in late 1960, Snitzer asked Koester if the ruby laser would be a suitable light source. Koester made some calculations based on the energy and wavelength of the laser and "concluded it made sense" (see Bromberg, 1984). American Optical started a research program on laser photocoagulation before the end of 1960.
Koester contacted Charles Campbell, then a medical consultant for American Optical, for a medical opinion and to conduct clinical experiments. In the fall of 1961 they used a prototype ruby laser photocoagulator on a patient for the first time, destroying a retinal tumor. The results of this experiment were publicized in a press release which, at the request of Dr. Campbell, named only Dr. Koester. Articles were published in the New York Times and the Wall Street Journal on December 22, 1961. In the spring of 1962, Koester, Snitzer, and Campbell presented a paper on their work at a meeting of the Optical Society of America (Koester et al., 1962). Milton Zaret also discussed his rabbit experiments at the meeting (Zaret et al., 1962). Koester and Campbell were unaware of Zaret's work until the Optical Society of America meeting. They also did not know that Milton Flocks and Christian Zweng were in the early stages of their laser research in 1961.
Flocks and Zweng had written one paper together before attending a conference in 1955 at which Gerd Meyer-Schwickerath described the Zeiss photo-coagulator. After hearing Meyer-Schwickerath's presentation, Zweng and Flocks applied for and received a grant from the National Institutes of Health to obtain a Zeiss instrument. Zweng and Flocks' research with the photo-coagulator was publicized throughout the San Francisco area.
In 1962 a Stanford scientist showed Flocks a "little ruby laser the size of a pencil" and told Flocks it could produce more light than the Zeiss instrument (personal communication, Milton Flocks, March 20, 1992). According to Flocks, the scientist who took the laser to the medical school was unaware of other medical research involving the laser. Shortly after this meeting, Flocks and Zweng contacted someone in the physics department at Stanford who built a ruby laser for them to conduct preliminary research. Zweng also consulted with Milton Zaret, as Zaret was assisting several researchers in the development of laser research laboratories. Zweng and Flocks began working with rabbits, monkeys, and cats and published the results of their research on a rabbit and a cat in July 1963. Flocks and Zweng used the instrument on a human for the first time in August 1963 (Kapany et al., 1963; Zweng et al., 1964).
By 1964 a large amount of research had been conducted by the California and New York groups (see, for example, Campbell et al., 1963a,b; Koester et al., 1962; Zweng and Flocks, 1965). Their research became known to the medical community primarily through conferences and publications. Koester and Campbell and Milton Zaret had presented papers at the aforementioned Optical Society of America meeting in the spring of 1962. Campbell presented a paper on laser coagulation at the Southeastern Section meeting of the American Association for Research in Ophthalmology (AARO) in March of that year. At the AARO meeting, Campbell stated that their study "demonstrates clearly that a laser photocoagulator has potential as a safe clinical device." At the American Medical Association meeting of June 1964, Flocks and Zweng described 25 patients who had been treated exclusively with the ruby laser. The reaction from the medical community was strong; as Flocks recalls, "All these doctors didn't even know what a laser was. They'd never heard the word, most of them … and after that [the presentation at the conference] it went like wildfire." Still, a voice of caution remained in the medical profession. After Flocks and Zweng's presentation, Milton Zaret rose to discuss their paper and stated that it was irresponsible of them to use the laser on human subjects given that they didn't know the laser's long-term effects. Zaret also expressed concern about the danger of the laser to the laser operator and assistant, since these people would be exposed to its radiation repeatedly. Since much of Zaret's other research was focused on the long-term effects of radiation, his concerns were well-founded. Much more research was needed before the laser would be accepted by ophthalmologists.
PHOTOCOAGULATORS AND THE PRIVATE SECTOR
After the laser's initial clinical trials by Flocks and Zweng and by Campbell, research on photocoagulation took a new form. The indications for and limitations of laser photocoagulation needed determination, as it was clear that the technique could be valuable to the treatment of eye disease. More importantly, sophisticated equipment was needed to provide doctors with greater control over
the beam. Medical doctors actively collaborated with laser manufacturers to design equipment specifically for medical use; American Optical sponsored the first use of a laser photocoagulator on a human subject and subsequently began to develop a commercial device, and Milton Flocks and Christian Zweng began work with Optics Technology shortly after their first experiments with the laser photocoagulator. Zweng also co-authored the first book on laser photocoagulation in 1969 (see Zweng et al., 1969).
As mentioned earlier, Optics Technology, Incorporated, was founded in 1960 by Narinder Kapany, a physicist educated in India. Kapany is "generally acknowledged to be the originator of fiber optics" (Laser Focus, 1967). His doctoral thesis sought to prove that one could send an image through fibers much as one could deliver other electronic signals; it laid the groundwork for the development of the fiberoptic endoscope. He used Optics Technology as a vehicle for research on the application of new technologies.10
Who initiated the collaboration between Drs. Zweng and Flocks and Dr. Kapany is unclear. Flocks and Zweng, after their initial research on rabbits, found that the laser they had received from the physics department was not ideal. The physics department was unable to assist them in producing better equipment, so they sought a private laser supplier. In 1961 Kapany received a grant from the National Institutes of Health (the first given to a private company) titled "Applications of Modern Optics in Medicine." He cultivated relationships with cardiologists, gastroenterologists, proctologists, radiologists, and ophthalmologists. Flocks and Zweng were among those who received lasers from and consulted with Kapany.
According to Kapany, a project was planned to test laser interaction with human tissue (see Cunningham, 1986; personal communication, Narinder Kapany, May 14, 1992). Kapany asked an employee, Dr. Ig Liu, to build a laser for this project. A device composed of a steel tube with a ruby rod and flash-lamps was suggested, and when Liu showed Kapany the product Kapany immediately suggested that an ophthalmic head be added to it. This equipment was the basis for Optics Technology's photocoagulator. Zweng, Flocks, and scientists at Optics Technology defined their specifications: constant energy output, protection of the laser operator, viewing capability, easy aiming, the ability to create a useful lesion, variation in the laser pulse, maneuverability of the instrument, and the ability to change the size of the focal point of the beam. By early 1963 a prototype had been developed, and it may have been this photocoagulator that Zweng and Flocks used on their first human subject.
Kapany made a public announcement of this experimental photocoagulator and selected 20 ophthalmologists to purchase the instrument and provide clinical data to Optics Technology. As the success of laser treatment became apparent to
the medical community, Optics Technology was able to sell many photocoagulation devices. American Optical's photocoagulator reached the marketplace in late 1963. Campbell and Koester developed the device with funding from the National Institute of Neurological Diseases and Blindness and the U.S. Public Health Service. Their device was more sophisticated and more expensive than that of Optics Technology (personal communication, Charles Koester, April 29, 1993) and sold at the rate of about a dozen per year. According to Kapany, Optics Technology and American Optical "didn't have any competitors until almost the year 1968 when Coherent Radiation came out with an argon photocoagulator" (reported in Cunningham, 1986).
The argon laser was invented in 1964 and within a year researchers used this light source for photocoagulation. The laser was a great improvement over the Zeiss instrument in many cases, especially since the laser's brief exposure time reduced pain and its monochromatic light was more easily controlled than white light. Patients could be treated on an outpatient basis and no anesthesia was needed. Still, the ruby laser photocoagulator had several disadvantages and was not used for some retinal disorders. The major complaints against the ruby laser were that the laser pulsed in a slightly irregular fashion, the intensity of the output was difficult to control, and the beam diameter varied (Campbell et al., 1963). A laser that could create similar lesions in the eye without these disadvantages was desired and was found in the argon laser.
In early 1965 Dr. Francis L'Esperance of the Columbia-Presbyterian Medical Center presented his first paper on treating diabetic retinopathy (then the leading cause of blindness in people 20 to 64 years old) with a ruby laser at a conference in New York. L'Esperance, like Zaret, Flocks, and Campbell, had a remarkably strong knowledge of physics; he says he "had taken every physics and chemistry course at Dartmouth College" (reported in Hecht, 1986). He became interested in laser photocoagulation after hearing about the early research of Flocks, Zweng, and Campbell. L'Esperance bought the third ruby laser made by Optics Technology for $5,500 in 1963 and began research on humans the following year. In his 1965 presentation on the ruby laser, L'Esperance noted that doctors needed a blue-green laser since its wavelength would be likely to produce therapeutic lesions. In the discussion following the presentation, Flocks said he had just seen an argon laser in a Palo Alto company's research laboratory (personal communication, Milton Flocks, March 20, 1992).
Shortly after the 1965 conference, L'Esperance learned from a patient that Bell Laboratories had developed a blue-green laser. L'Esperance began placing phone calls immediately. He contacted Eugene Gordon and Edward Labuda of Bell Labs and had "a very stiff meeting" at which Gordon and Labuda sought to determine the specifications L'Esperance wanted (reported in Hecht, 1986). L'Esperance could not provide such information; since the argon laser was new, L'Esperance had no sense of its effects on the eye. The three men met several more times, but Gordon and Labuda were reluctant to pursue a project with
L'Esperance because Bell Labs' charter is for auditory, not visual, devices. They found an excuse to work on optical applications when they saw someone working on a prototype picturephone; at that point "things started changing" (Hecht, 1986). As with the development of the ruby laser, the collaboration of academic and private-sector researchers proved fruitful.
Gordon loaned L'Esperance several laser discharge tubes and L'Esperance began to determine what power levels were necessary for successful photocoagulation. Raytheon developed the most powerful argon ion laser in existence for L'Esperance's work and in early 1966 studies were initiated on animals. The first human was treated with the argon laser in February 1968, at which time L'Esperance decided to design a device for ophthalmological clinics. He called the John A. Hartford Foundation of New York, a private foundation that provides funding for medical research. After hearing L'Esperance's description of the project, the director of the foundation replied, "Forget all the preliminary stuff. All I want is the budget" (quoted in Hecht, 1986). L'Esperance received $287,000 to begin work with Bell Labs in 1968.11
In 1968 and 1969, with Gordon and Labuda, L'Esperance developed three delivery systems for ophthalmologists. A fourth system was created in association with the American Optical Corporation. An indirect delivery device and an articulated-arm manipulator that allowed one to hold the laser like a scalpel were among the new instruments. L'Esperance published the designs so they went into the public domain and tested them clinically with Dr. Felix Shiffman12 (see L'Esperance, 1968, 1973; L'Esperance et al., 1969). The argon laser proved superior to the ruby laser and, according to Flocks, "as soon as the argon was developed, everything else disappeared." In 1969, Coherent Incorporated decided to produce and market the Bell designs, which are still the standard for photocoagulators.
Coherent's profitable sales of the argon laser were not surprising to those working on laser photocoagulation. First, lasers were clearly superior to conventional white light sources for photocoagulation. Further, most ophthalmological laser researchers, according to Elias Snitzer, "were aware of the fact that it was necessary to shift the wavelength into the green" (reported in Bromberg, 1984). American Optical did not pursue the argon coagulator because they did not have a research program on argon lasers in place (personal communication, Charles Koester, April 29, 1993) and because the ruby laser photocoagulator had not been profitable (Bromberg, 1984). Optics Technology also did not design an argon device, leaving the market completely available to Coherent.
By 1971, Christian Zweng and other doctors were teaching argon laser photocoagulation courses throughout the United States. Diabetic retinopathy was no longer a major threat to eyesight and, thus far, there have been no systemic negative effects of laser treatment in ophthalmology. The laser is used by ophthalmologists for glaucoma treatment, retinal reattachment, and the ablation of tumors. As Leon Goldman noted in Laser Focus, (1967), ''eye surgery … is now almost accepted as routine by nearly everybody." In 1990, 95 percent of ophthalmologists surveyed by Arthur D. Little, Inc., agreed that they "recognize the laser as a legitimate medical tool and use it when it is the superior method of treatment" (Arthur D. Little Decision Resources, Inc., 1989; Halter, 1985). Research of the laser's effects on other parts of the body has progressed more slowly than ophthalmological research owing to the difficulty of working with more complex tissue structures. What advancement has occurred is not strictly the result of ophthalmology's success being transferred to other specialties; significant research was performed by doctors in other fields in the early 1960s.
MORE EARLY MEDICAL LASER RESEARCH
In 1986, John L. Ratz wrote in the introduction to a textbook on lasers in nonophthalmological medicine that "the birth of laser medicine in the early 1960s was largely due to the hard work and persistence of Leon Goldman, M.D." (Ratz, 1986). Given the breadth of work conducted and supervised by Goldman at the University of Cincinnati, this statement is probably not an exaggeration. He was the first person to use the ruby laser in dermatology and has been dubbed the "father of lasers in medicine and surgery" by the medical profession.13 His studies involved almost every laser developed and most parts of the human (and animal) body. Because Goldman studies a wide range of biologic effects, many medical specialties benefited from his lifelong work.
Goldman's laser research began in 1962 when the Occupational Health Division of the U.S. Public Health Service and the Hartford Foundation provided funding to the department of dermatology at the University of Cincinnati to establish a medical laser laboratory. The laboratory was placed under Dr. Goldman's leadership at the Cincinnati General Hospital. According to Milton Zaret, Goldman consulted Zaret for assistance in the early stages of the laboratory's development (personal communication, Milton M. Zaret, May 1, 1992). The purpose of the laser laboratory was "to study the occupational hazards of the laser … primarily the dangers to physicists and technicians in laser laboratories."14
This laboratory's early work focused on laser safety, particularly the proper
construction of facilities and the protection of workers. Goldman's first published medical study appeared in the Journal of Investigative Dermatology in January 1963 (Goldman et al., 1963a). He presented a summary of the effects of the laser on white and black skin and rabbit eyes. The most significant finding was that the ruby laser's effect on tissue depends on the skin's melanin content and degree of vascularization; darker-colored tissues exhibit more damage than light-colored tissue. Goldman concluded his paper by noting that he was studying the laser's effect on red cells, capillaries, pigmented nevi, basal cell carcinomas, and tattoos.
Shortly after the founding of Goldman's laser laboratory, the Hartford Foundation and the National Institutes of Health (NIH) provided him with another grant to develop an applied medical laser laboratory. The particular interest of the Hartford Foundation, NIH, and Goldman was to develop surgical instrumentation for basic research and clinical studies. By 1965 the new medical laser laboratory was considered "one of the best-equipped laser research laboratories in the U.S.A." (Laser Focus, 1965). It contained 10 rooms, eight lasers, and an interdisciplinary staff of 30 biologists, histologists, cytologists, physicists, and instrument design engineers.
Goldman's laboratory completed important investigations regarding the laser in hematology, cytology, protein and enzyme research, dentistry, retinal coagulation, and dermatology. Procedures for treating skin cancers and for removing tattoos and warts were developed by Goldman. Goldman supervised experiments of whether the laser produced malignancies in animals and whether the vapor resulting from laser contact with tissue was harmful. He also recognized that the transmission of laser beams through rods would be significant to medicine, and his laboratory was the first to report delivery of ruby laser beams to skin with a fiberoptic device (see Goldman et al., 1963a,b).
Much of Goldman's interest in this new, larger laboratory came from the realization that laser instrumentation for surgery was "primitive" and that "laser manufacturers are not interested in the production of equipment for medical purposes" (Laser Focus, 1965). Companies were reluctant to enter the medical laser market for at least three reasons: development costs were high, the laser companies were not familiar with medical buyers, and small companies could not protect their inventions from larger corporations. The solution to this reluctance was a large infusion of government money, particularly from the NIH and the military.
Early laser research was occurring in what Susan Bartlett Foote (1992) called "the heyday of federal biomedical support," and the Armed Forces became interested in using the laser as a beam weapon. Milton Flocks, Milton Zaret, and Charles Koester commented on the military's interest in identifying the threshold to damage from the laser in preparation for using it as a weapon. Flocks commented that such research "was not of much interest to me," and Milton Zaret, who received grants from the Air Force Systems Command, concurs. Military
interest in the laser was not exhibited strictly through grants; in 1965 Laser Focus reported that the Army Missile Command at the Redstone Arsenal was developing a high-energy laser medical unit. The project reportedly began when Dr. John P. Minton of the National Cancer Institute was searching for a high-powered laser and learned that the military could provide one. Dr. James R. Dearman of Redstone called this program "the result of a unique marriage between the military and medicine" (Laser Focus, 1965). The U.S. government's and military's interest in the laser was beneficial to medicine resulting in a large volume of important research from government-supported projects.
Medical laser research developed an audience from the large number of medical and laser conferences in the 1960s. It was through these events that the medical profession informed laser developers of their needs. At the Boston Laser Conference in August 1964, Goldman and Zaret reported on the dangers of the laser to scientists, while Captain Martin S. Litwin of the Army Medical Research and Development Command stated that biological researchers needed continuous lasers, especially at wavelengths shorter than 5900 angstroms. The 1965 Northeast Electronics Research and Engineering Meeting included 10 papers on medical uses, including one by Goldman. The watershed event for medical research may have been the First Annual Biomedical Conference on Laser Research, organized by Dr. Paul E. McGuff of Tufts New England Medical Center, and featuring 36 talks. In 1965, Goldman began to bring his work to doctors more directly; he inquired in Laser Focus whether medical professionals were interested in a course on the use of lasers.
Other projects involving the laser were few in the early 1960s. Dentists began examining the laser's effect on teeth in 1964, with studies focusing on human enamel, dentin, and dental restorative materials. While this research was needed to understand the laser's effects on human tissue, it produced no immediate advances for dentistry. Marginally more successful were studies of the laser's potential in surgery (Wolbarsht, 1971).
Dr. McGuff published reports on the use of the laser in surgery in 1963. By 1964, with David Prushnell of Raytheon, he vaporized a human carcinoma that had been transplanted to a hamster. Early cancer studies were the mechanism by which the vaporization and cutting abilities of the laser became fully known. A flurry of research on laser treatments for cancer occurred in the mid-1960s, but cancer treatment studies became less common after scientists discovered that the ablation was scattering malignant cells to other sites (Bromberg, 1991).
Laser surgery equipment began to appear in the medical marketplace in 1965 with the development of microsurgical equipment by M.C. Bessis and others at the National Transfusion Center in Paris. In 1967, Laser Incorporated, a spin-off from and subsidiary of American Optical Corporation, introduced a portable surgical device designed for operating room use. Prototypes were tested on dogs at the Montefiore Hospital Medical Center in New York.
By the mid-1960s there were many types of lasers available for researchers;
the neodymium-doped yttrium-aluminum-garnet (Nd:YAG) laser had been developed in 1964 by Bell Labs, as had the carbon dioxide (CO2) laser in 1965. It was known that the CO2 laser vaporized tissue, the Nd:YAG created a coagulative necrosis within tissue, and the visible lasers (ruby, argon, etc.) served as hemostatic coagulators. Because the biological effect of a laser is dependent on the laser's wavelength, energy density, and tissue absorption, doctors needed to develop an understanding of the principles of light transmission, scatter, reflection, and absorption. Theoretically, surgeons could manipulate the laser beam's width and energy density to obtain a desired effect, but medical scientists did not understand the laser well enough to define these parameters. The determination of the indications for and best method of use of the laser has been the focus of laser research since 1965.
THE MEDICAL LASER INDUSTRY TODAY
Even over 30 years after Zaret's preliminary paper (Zaret et al., 1961) on the laser, new medical uses for the laser are announced frequently. Current proposals include using the laser for lithotripsy (the breaking up of kidney stones), phototherapy treatment of cancer, recanalization of arteries, and Doppler-shift measurement of blood velocity (see Forrester, 1988; Hall, 1990; Ratz, 1986; Sanborn, 1988; Sliney and Wolbarsht, 1989; White, 1988). The laser is now commonly used in ophthalmology, in otolaryngology to treat benign lesions in the throat, in gynecological surgery to treat endometriosis and remove cervical dysplasia, in gastroenterology, and in dermatology (see Table 3-1), which are a few of the fields that have had either established clinical experience with the laser or randomized controlled trials (see Table 3-2). More importantly, the laser has been proven the best treatment for some indications, especially in ophthalmology (see Table 3-2). New research is made possible by an active medical technology industry in the United States, although this industry's success is often affected by forces beyond its control.
During the end of the 1960s the laser marketplace underwent significant changes. The laser shifted to mostly civilian use and the Mansfield Amendment of 1969 prohibited defense agencies from supporting basic research. NIH began to focus more on scientific research than on technological development. Most research and development received its funding from outside the public sector and entrepreneurial individuals sought venture capital for their ideas. New companies were created frequently as engineers tried to capitalize on the laser's popularity. They obtained funds from private investors but encountered many difficulties entering the medical industry due to the particularities of its institutions and regulations.
Medical device development is generally less expensive than pharmaceutical development because of the comparative simplicity of mechanical and electrical design. Medical devices, however, are less protectable by patents, making many
TABLE 3-1 Rate of Laser Penetration by Specialty,a 1985–1990
researchers reluctant to devote resources to the creation of a new medical tool. The Food and Drug Administration's (FDA) oversight of the licensing process of medical devices further hinders innovation. The FDA began to regulate devices stringently with the 1976 Medical Device Amendments, codifying requirements for the testing and approval of new devices (Kessler et al., 1987). Although many researchers complain about the FDA approval process, Dr. Jacob Dagan of Advanced Surgical Technologies, Inc., Dr. Leroy Sutter of Directed Energy, Inc., and Kenneth Nilsson of Cooper Lasersonics, Inc., agree that "FDA regulations have been of minimum detriment" to the success of lasers in medicine (Akerley, 1985).
Federal policies for financing health care also affect the medical laser device market. When Medicare and Medicaid were established in 1965, payments were made to doctors and hospitals on a fee-for-service basis. In 1984, the Health Care Financing Administration (HCFA, which oversees Medicare and Medicaid) established the Prospective Payment System (PPS) to control health care costs. PPS divides hospital inpatient diagnoses into 480 categories, each of which is reimbursed at a fixed rate. Medical treatments that cost more than the fixed rate are not used, as the hospital would lose money implementing the technology. Since HCFA is the largest third-party payer of health care in the United States, this reform has greatly affected the entire medical community.
In order to evade the PPS controls, many hospitals are moving operative
TABLE 3-2 Judgments of Effectiveness of Medical Applications of Lasers
|
Procedure |
Established Clinical Experience |
Randomized Controlled Trial |
Probably Cost Effective |
Proven Cost Effective |
|
Dermatology |
|
|
|
|
|
Port-wine stain |
x |
|
|
|
|
Tattoos |
x |
|
|
|
|
Telangiectasia |
x |
|
|
|
|
Warts |
x |
|
|
|
|
Ophthalmology |
|
|
|
|
|
Diabetic retinopathy |
|
x |
x |
x |
|
Retinal detachment |
x |
|
|
|
|
Retinal vein occlusion |
|
x |
x |
|
|
Trabeculoplasty for glaucoma |
|
x |
x |
|
|
Senile macular degeneration |
|
x |
x |
|
|
Posterior capsulotomy |
|
x |
x |
|
|
Otolaryngology |
|
|
|
|
|
Respiratory papillomatosis |
x |
|
x |
|
|
Pharyngeal pouch |
x |
|
x |
|
|
Tongue resections |
x |
|
x |
|
|
Pulmonology |
|
|
|
|
|
Palliation of advanced lung cancer |
x |
|
x |
|
|
Gastroenterology |
|
|
|
|
|
Hemostasis of gastric ulcer |
|
|
x |
|
|
Hemostasis of intestinal vascular malformation |
x |
|
|
|
|
Cancer palliation of esophagus |
x |
|
x |
|
|
Cancer palliation of colon |
x |
|
x |
|
|
Sessile villous adenomas |
x |
|
|
|
|
Hemorrhoids |
x |
|
x |
|
|
Urology |
|
|
|
|
|
Bladder cancer |
x |
|
x |
|
|
Penile carcinoma |
x |
|
x |
|
|
Condyloma |
x |
|
x |
|
|
Laser lithotripsy |
x |
|
x |
|
|
Gynecology |
|
|
|
|
|
Cervical intra-epithelial neoplasia excision |
x |
|
x |
|
|
Fallopian tube reconstruction |
x |
|
|
|
|
Endometriosis |
x |
|
|
|
|
Condyloma |
x |
|
|
|
|
SOURCE: Banta et al., 1992. |
||||
procedures to the outpatient setting, which is still reimbursed on a fee-for-service basis. The resultant trend is "minimally invasive surgery" (MIS), which includes endoscopic procedures, minor operations, and many emergency room treatments. MIS is usually cost-effective, safer, and more convenient for patients, further encouraging its development. The laser may be an important tool in this trend because its surgical effects can be very precise, minimizing damage to tissue, and because lasers can be transmitted via fiber optics with endoscopic devices. The lower costs associated with several laser procedures may lead to their adoption in the inpatient setting as well. A three-year study at Cooper Hospital/University Medical Center in Camden, New Jersey, found that lasers reduced the direct cost for gastrointestinal (GI) applications by $3,500 per patient. GI operating room expenses were reduced by 40 percent, and the average length of a hospital stay dropped from 17.7 days to 14. Similar results were found in a study of neurosurgical, gynecological, and outpatient applications (Cerne, 1988). Still, many doctors are reluctant to use lasers; as noted about the carbon dioxide laser, "successful commercialization … requires the device to overcome several major hurdles, including user resistance to high system prices as well as a reluctance by physicians to replace traditional scalpels with tools requiring extensive training" (see Akerley, 1985).
Despite institutional hurdles, the medical sector is one of the fastest growing segments of the laser industry (see Table 3-3). Collaboration between laser manufacturers and clinicians has boosted medical research and equipment sales,
TABLE 3-3 Laser Sales (in million dollars)
|
|
1985 |
1987 |
1988 |
1989 |
1990 |
1991 |
Percent Change, 1985–1991 |
|
Material processing |
127.0 |
128.6 |
146.7 |
173.9 |
256.4 |
337.6 |
166 |
|
Medicine |
83.7 |
81.0 |
102.8 |
200.2 |
209.5 |
233.8 |
179 |
|
R&D |
104.1 |
123.4 |
141.7 |
216.5 |
218.4 |
190.0 |
83 |
|
Printing |
34.2 |
35.8 |
46.5 |
53.2 |
50.8 |
40.0 |
17 |
|
Platemaking/color separation |
14.2 |
15.4 |
10.9 |
11.4 |
14.1 |
8.4 |
–41 |
|
Communications |
44.0 |
60.0 |
70.1 |
76.4 |
112.1 |
111.2 |
153 |
|
Optical memories |
21.4 |
89.0 |
53.5 |
70.9 |
73.8 |
76.9 |
259 |
|
Barcode scanners |
4.5 |
11.9 |
18.6 |
29.0 |
30.7 |
26.3 |
484 |
|
Alignment, control |
2.0 |
0.9 |
5.9 |
7.1 |
7.0 |
10.9 |
445 |
|
Test and measurement |
21.0 |
20.0 |
28.7 |
35.6 |
39.9 |
34.3 |
63 |
|
Entertainment |
3.5 |
5.2 |
8.0 |
8.4 |
12.0 |
9.7 |
177 |
|
TOTAL |
459.6 |
570 |
633.5 |
882.6 |
1,024.7 |
1,079.1 |
135 |
|
SOURCE: Laser Focus/Electro-Optics, 1986, 1988–1992. |
|||||||
and several journals have been established for this industry.15 Such interdisciplinary collaboration between firms and academic medical doctors was essential to the success of ophthalmological lasers. No single vendor dominates the medical laser market (with the exception of argon-laser ophthalmic systems), and over 100 companies supply lasers to the medical community. In 1991, over 31,000 laser units were sold for medical and diagnostic use. Although this was less than 0.1 percent of the total number of laser units sold in the United States, the dollar value of these sales has been estimated to range from $233 million to $325 million—over 20 percent of cash sales in lasers. Ophthalmological applications dominate this purchasing, comprising $70 million of the $220 million of sales in 1988. In the United States in 1991, less than 1 percent of surgeries were performed with the laser. Advocates say that up to 50 percent could be done with laser devices (Bromberg, 1991), but recent developments have indicated that the medical market for lasers will not grow to be as large as many researchers once hoped. In 1987, C. Breck Hitz described the medical laser market as being "profitless" (Hitz, 1987) and Laser Focus/Electro-Optics noted that the industry had "slim profit margins" in 1989 (p. 98). The cost of bringing a new medical laser product to the consumer is still high, although the cost may decline as laser manufacturing becomes less expensive. For this reason, the laser is still considered to be in its embryonic stages in medicine.
From a laboratory in southern California, the laser has moved into nearly every medical specialty. The laser's success in ophthalmology can be traced to the research conducted by Koester and Campbell, Zaret, and Flocks, Kapany, and Zweng. These men laid the foundation for the implementation of laser techniques in medicine. They were able to do so because they had the opportunity to utilize several established methods of communication between researchers. The most important of these was the use of medical consultants by private companies. The consultancies brought physicians, physicists, and engineers together to create useful technologies for medicine. Academic medical researchers rarely have the resources or the incentive to bring a new technology to market; private companies are driven by the need to produce new devices. Also necessary in the development of the laser photocoagulator were the broad science educations obtained by Flocks, Zaret, and Campbell. Encouraging this type of education in universities could foster further collaboration between medicine and industry. Lastly, the existence of conferences and journals that cater to many scientists supported communication among and between laser developers and medical researchers.
Transferring new technological discoveries into useful medical tools is not a
deterministic process. Some dimension of serendipity is involved in the inspiration of any idea. But, as is clearly exemplified by the introduction of the laser to medicine, particular institutional structures and relationships are necessary to foster the development of medical technology. In the case of laser photocoagulation, we can thank the researchers who established relationships between private laser producers and academic medical centers for launching the development of an important tool in medicine.
ACKNOWLEDGMENTS
I am grateful to the late Milton Flocks, Narinder Kapany, Elias Snitzer, and Milton Zaret for allowing me to interview them, to Charles Koester for his correspondence, and to the Neils Bohr Library, Center for History of Physics, at the American Institute of Physics for a transcript of Joan Bromberg's interview with Elias Snitzer and a questionnaire from Charles Koester. Nathan Rosenberg and Victor Fuchs provided many useful comments. I thank the National Science Foundation for financial support.
REFERENCES
Akerley, B. H. 1985. Outlook for medical laser market strong as sales surge. Laser Focus/Electro-Optics 21:62–72.
Andrews, A. H., Jr. 1984. The use of the carbon dioxide laser in otolaryngology: 10 years experience. Lasers in Surgery and Medicine 4:305–310.
Banta, H. D., Schou, I., Vondeling, H., and de Wit, A. 1992. Economic appraisal of laser applications in health care. Report of a project. Lasers in Medical Science 7:9–21.
Bromberg, J. L. 1984. Interview for the Laser History Project of Elias Snitzer. August 6. New York: Neils Bohr Library, American Institute of Physics.
Bromberg, J. L. 1991. The Laser in America, 1950–1970. Cambridge, Mass.: The MIT Press.
Campbell, C. J., Koester, C., Curtice, V., Noyori, K., and Rittler, M. C. 1965. Clinical studies in laser photocoagulation. Archives of Ophthalmology 74:57–65.
Campbell, C. J., Noyori, K., Rittler, M. C., and Koester, C. 1963a. Intraocular temperature changes produced by laser coagulation. Acta Ophthalmologica 76(suppl.):22–31.
Campbell, C. J., Rittler, M. C., and Koester, C. J. 1963b. The optical maser as a retinal coagulator: An evaluation. Transactions: American Academy of Ophthalmology and Otolaryngology 67:58–67.
Cerne, F. 1988. Can lasers cut hospital costs? Hospitals 62:63.
Choy, D. S. J. 1988. History of lasers in medicine. Thoracic and CV Surgeon 36(suppl.2):114–117.
Cunningham, R.1986. Applications pioneer interview: Narinder Kapany. Lasers and Applications 5(7):65–68.
Dunnington, J. H., Regan, E. F., and L'Esperance, F. A. 1963. Progress in Ophthalmic surgery, part 2. New England Journal of Medicine 269:417–413.
Foote, S. B. 1992. Managing the Medical Arms Race: Public Policy and Medical Device Innovation. Berkeley, Calif.: University of California Press.
Forrester, J. S. 1988. Laser angioplasty: Now and in the future. Circulation 78:777–779.
Goldman, L., Blaney, D., Kindel, D., and Franke, E. K. 1963a. Effect of the laser beam on the skin. Journal of Investigative Dermatology 40:121–122.
Goldman, L., Blaney, D. Kindel, D. J., Jr., et al. 1963b. Pathology of the effect of the laser beam on the skin. Nature 197:912–914.
Hall, L. T. 1990. Cardiovascular lasers: A look into the future. American Journal of Nursing 90(July):27–30.
Halliday, D., and Resnick, R. 1978. Physics: Part 2. New York: John Wiley and Sons.
Halter, P. 1985. The medical laser market waits for R & D to deliver. Lasers and Applications 4(October):55–57.
Ham, W. T., Jr., Williams, R. C., Geeraets, W. J., Ruffin, R. S., and Mueller, H. A. 1963. Optical masers (lasers). Acta Ophthalmologica 76(suppl.):60–78.
Hecht, J. 1986. Applications pioneer interview: Francis L'Esperance. Lasers and Applications 5(5):79–83.
Hecht, J. 1992. Laser Pioneers. Boston, Mass.: Academic Press, Inc.
Hitz, C. B. 1987. Medical lasers: A paradox of profitless prosperity. Laser Focus/Electro-Optics 23:76–79.
Kapany, N. S., Peppers, N. A., Zweng, H. C., and Flocks, M. 1963. Retinal photocoagulation by lasers. Nature 199:146–149.
Kessler, D. A., Pape, S., and Sundwall, D. N. 1987. The federal regulation of medical devices. New England Journal of Medicine 317:357–365.
Koester, C. J., Snitzer, E., Campbell, C. J., and Rittler, M. C. 1962. Experimental laser retina photocoagulation. Journal of the Optical Society of America 52:607.
Laser Focus. 1965, 1967. Volumes 1, 3.
Laser Focus/Electro-Optics. 1986, 1988-1992. Volumes 22, 24–28.
L'Esperance, F. A., Jr. 1968. An ophthalmic argon laser photocoagulation system. Transactions of the American Ophthalmological Society 66:827–904.
L'Esperance, F. A. 1973. Argon laser photocoagulation of diabetic retinal neovascularization (a five year appraisal). Transactions: American Academy of Ophthalmology and Otolaryngology 77:OP6–OP24.
L'Esperance, F. A., Labuda, E. F., and Johnson, A. M. 1969. Photocoagulation delivery systems for continuous-wave lasers. British Journal of Ophthalmology 53:310–322.
Little, Arthur D. Decision Resources, Inc. 1989. New Medical Laser Applications—Industry Report. No. 948451. March 22.
Maiman, T. H. 1960. Stimulated optical radiation in ruby. Nature 187:493.
Meyer-Schwickerath, G. 1967. The history and development of photocoagulation. American Journal of Ophthalmology 63:1812–1814.
Meyer-Schwickerath, G. 1973. 25 years of photocoagulation. Transactions: American Academy of Ophthalmology and Otolaryngology 77:OP3–OP5.
New York Times. December 22, 1961. Light beam used in eye operation.
The Otolaryngologic Clinics of North America. 1990. Volume 23.
Proceedings of the IEEE. 1963. 57:1847–1852.
Ratz, J. L., ed. 1986. Lasers in Cutaneous Medicine and Surgery. Chicago: Year Book Medical Publishers, Inc.
Sanborn, T. A. 1988. Laser angioplasty: What has been learned from experimental studies and clinical trials? Circulation 78:769–774.
Schawlow, A. L. 1961. Optical masers. Scientific American 204(June):52.
Schawlow, A. L., and Townes, C. H. 1958. Infrared and optical masers. Physics Review 112:1940.
Sliney, D. H., and Wolbarsht, M. L. 1989. Future applications of lasers in surgery and medicine: A review. Journal of the Royal Society of Medicine 82:293–296.
Solon, L. R., Aronson, R., and Gould, G. 1961. Physiological implications of laser beams. Science 134:1506–1508.
Townes, C. 1962. Optical masers and their possible applications to biology. Biophysics Journal 2:325.
Trokel, S. L. 1990. Development of the excimer laser in ophthalmology. Refractive and Corneal Surgery 6:357–362.
Wall Street Journal. December 22, 1961. Intense beam of light from laser used successfully to treat tumor in human eye.
White, G. H. 1988. Angioscopy and lasers in CV surgery. Australian and New Zealand Journal of Surgery 58:271–274.
Wolbarsht, M. L., ed. 1971. Laser Applications in Medicine and Biology . New York: Plenum Press.
Zaret, M. M., Breinin, G. M., Schmidt, et al. 1961. Ocular lesions produced by an optical maser. Science 134:1525–1526.
Zaret, M. M., Ripps, H., Siegel, I. M., and Breinin, G. M. 1962. Biomedical experimentation with optical masers. Journal of the Optical Society of America 52:607.
Zaret, M. M., Ripps, H., Siegel, I. M., and Breinin, G. M. 1963. Laser photocoagulation of the eye. Archives of Ophthalmology 69:97–104.
Zweng, H. C., and Flocks, M. 1965. Clinical experiences with laser photocoagulation . Federation Proceedings 24:S65–S70.
Zweng, H. C., Flocks, M., and Kapany, N. S. 1964. Experimental laser photocoagulation. American Journal of Ophthalmology 58:353–362.
Zweng, H. C., Little, H. L., and Peabody, R. R. 1969. Laser Photocoagulation and Retinal Angiography. Saint Louis, Mo.: C. V. Mosby Company.
TECHNICAL APPENDIX
Until 1900, the study of light was limited to examining its behavior. Scientists had identified light sources but they did not know how light was generated. Light is commonly radiated from heated solids and gases through which an electric current is passing. Another light source is the cavity radiator, constructed of blocks of tungsten, tantalum, or molybdenum. When the blocks are heated uniformly to a high temperature, they will emit light. Max Planck (1858–1947) studied cavity radiators and from his observations defined a relation between the ''radiancy" of a frequency of light, temperature, and frequency.
Planck wanted to devise a theory that would explain his formula after it was published in 1900. He believed the atoms that comprised the walls of his cavity radiator behaved like electromagnetic oscillators which emitted and absorbed electromagnetic energy. This idea led to the theory that electromagnetic oscillators (atoms) emit and absorb energy in discrete quantities. The emission and absorption of these quantities is characterized by the oscillator moving from one quantized state to another (see Halliday and Resnick, 1978).
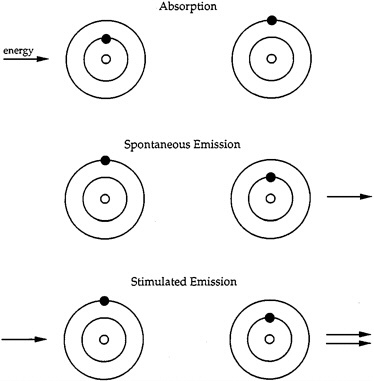
When an electron of an atom moves from a higher quantum level (of energy, measured discretely) to a lower quantum level, a photon of energy, viewed as electromagnetic radiation, is spontaneously emitted (see figure 3-A1). Similarly, a photon of energy can be absorbed by an electron, moving the electron to a higher quantum state. In Albert Einstein's 1916 proof of Planck's law, Einstein suggested that a photon emission might be stimulated. This idea was essentially ignored until Charles Townes proposed the maser, which was a feedback oscillator from which microwaves were emitted.
By bombarding deuterated ammonia with energy, Townes forced many of the electrons of the ND3 atoms into higher quantum states than they normally exhibit. These atoms were enclosed in a resonator which sustained the frequency of electromagnetic emissions. The stimulated emissions were reflected back to the atoms, maintaining the high quantum states. At high levels of radiation, the device broke into self-oscillation, producing millimeter-waves continuously.
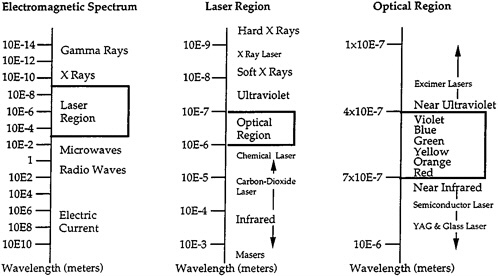
The laser is constructed in the same way as the maser described above, but with a material whose emissions produce visible light. The difficulties of creating the laser were finding an appropriate material and building a resonant chamber that would maintain the energy level of the material. Because the maser principle can be applied to many solids and gases, a wide variety of lasers exists. Each laser material produces a different wavelength of electromagnetic emission; thus, many "colors" of light can be produced with lasers (see Figure 3-A2).