4
Clinical Trials of FIAC at Memorial Sloan-Kettering Cancer Center
Although the toxic side effects that led to the formation of this Institute of Medicine committee were related to the administration of the drug fialuridine (FIAU), a review of experience with the closely related parent drug fiacitabine (FIAC) is relevant (although it should be emphasized that each of these drugs is a separate chemical entity, and therapeutic efficacy and toxicity need to be studied individually for each). The early trials of FIAC were carried out to a large extent in seriously ill patients suffering from underlying neoplastic disease or immunosuppressive conditions in the early 1980s at the Memorial Sloan-Kettering Cancer Center (MSKC). The following summarizes the available published information and pharmaceutical company summaries on these five trials. This commentary is based solely on the material available in the aforementioned sources; the committee did not review the individual patient records at MSKC.
Fiacitabine (FIAC),2'-deoxy-2'-fluoro-1-β-D-arabinofuranosyl-5-iodo-cystosine (Figure 1), is a pyrimidine nucleoside analog synthesized by Fox and his colleagues at MSKC in the 1970s. It was found to be highly active in vitro against several of the clinically important human herpes viruses (Lopez, Watanabe and Fox, 1980) and shortly thereafter against hepadnaviruses, inhibiting in its triphosphate form the DNA polymerases of human and woodchuck hepatitis viruses (Hantz, Allaudeen, Ooka, De Clercq and Trepo, 1984). It was studied at MSKC in the early 1980s in the treatment of herpes group (herpes simplex virus [HSV] types 1 and 2, varicella-zoster virus [VZV], and cytomegalovirus [CMV]) infections. Clinical studies were performed under Investigational New Drug application 20,496, and the results were published in several papers in the mid-1980s (Young, Schneider, Leyland-Jones, Armstrong, Tan, Lopez, Watanabe, Fox, and Philips, 1983; Leyland-Jones, Donnelly, Groshen, Myskowski, Donner, Fanucchi, and Fox, 1986) by the MSKC Antiviral Working Group. This group included, among others, a virologist (Carlos Lopez) and the chief of the Infectious Disease Division at MSKC and professor of Medicine at Cornell Medical College (Donald Armstrong).
The rationale for these studies involving compromised hosts was (1) the common and morbidity-producing occurrence of clinically active herpes group viral infections in patients with immunocompromise because of either their underlying disease or immunosuppressive therapy for neoplastic disease and (2) the prior demonstration of potent anti-herpes group virus activity by FIAC in cell culture systems and in mice that had been inoculated with ordinarily lethal doses of HSV-1. Additionally, the availability at the time of only one drug, one with substantial side effects, adenine arabinoside (Ara-A), made these studies of possible therapy
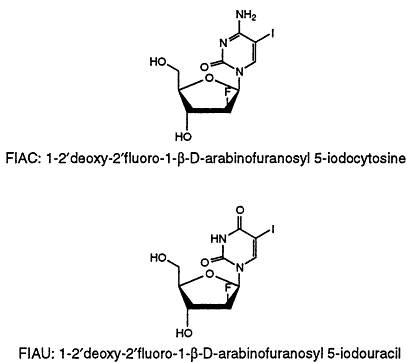
FIGURE 4-1 Structure of fiacitabine (FIAC) and fialuridine (FIAU).
for HSV and VZV infections more cogent. Preclinical toxicological studies indicated that FIAC was well tolerated in short-term dosing experiments in mice; for example, LD50 (the lethal dose for half of the animals) of 1,000 mg/kg/day for 5 days was 10 to 100 times the effective dose range. The antiviral activity was believed to be due to phosphorylation by the pyrimidine nucleoside kinases induced by the virus in infected cells (and then cellular conversion to di-and triphosphates) and subsequent inhibition of virus-encoded DNA polymerases (Lopez et al., 1980).
Pharmacokinetic studies by the mid-1980s (Leyland-Jones, Donnelly, Groshen, Myskowski, Donner, Fanucchi and Fox, 1986) indicated that in humans FIAC was cleared from the blood, after biotransformation in the liver, kidney, and peripheral blood, with a terminal-phase half-life of 1.3 hours after intravenous administration. The principal metabolite is fialuridine (FIAU), 2'-deoxy-2'-fluoro-1-β-D-arabinofuranosyl-5-iodo-uracil, which was later shown by high performance liquid chromatography to have a terminal-phase half-life of about 4 hours (Oclassen, 1989). Development of a highly specific and much more sensitive radioimmunoassay for FIAU in 1993 has permitted detection of a very prolonged elimination phase for FIAU in healthy volunteers with a mean elimination half-life of 29.3 hours (Bowsher, Compton, Kirkwood, Place, Jones, Mabry, Hyslop, Hatcher and DeSante, 1994).
After IV administration of FIAC in humans only 12 percent appears unchanged in the urine and 45 percent is excreted as FIAU (Bowsher, Compton, Kirkwood, Place, Jones, Mabry, Hyslop, Hatcher, DeSante, 1994). Small amounts of FAU (1-2'-deoxy-2'-fluoro-1-β-D
arabinofuranosyl-5-uracil), FAC (1-2'-deoxy-2'-fluoro-1-β-arabinofuranosyl-5-cytosine), and FMAU (1-2'-deoxy-2'-fluoro-1-β-arabinofuranosyl-5-methyluracil) have been detected in the urine along with FIAU in other studies, the exact amounts and proportions dependent upon the species. Thus, FIAC and FIAU appear to have a metabolically stable N-glycosyl sugar linkage, leaving deiodination and deamination of the pyrimidine moiety as the major routes of metabolism. Since the termination of clinical trials and the development of the sensitive RIA assay, incorporation of FIAU into DNA, which implies conversion to FIAU-triphosphate, has been observed in spleen, liver, pancreas, jejunum, heart and skeletal muscle, although it was time, species and tissue dependent. Attempts to determine if FMAU and FAU were present in DNA with high concentrations of FIAU have been inconclusive. See Chapter 13 for further information on mechanism of action.
PHASE I EVALUATION OF FIAC IN IMMUNOSUPPRESSED PATIENTS WITH HERPES VIRUS INFECTION
This trial (Young, Schneider, Leyland-Jones, Armstrong, Tan, Lopez, Watanabe, Fox, and Philips, 1983) involved 32 immunocompromised patients (30 with leukemia, lymphoma, or solid tumors and 2 with AIDS) who had active herpes group virus infections (29 were infected with VZV, 3 were infected with HSV) that had shown clinical progression in the previous 48 hours. None of the patients received myelosuppressive therapy concurrently, but 10 percent of them had received cytotoxic chemotherapy or radiation within 21 days prior to entry into the study. Hematologic abnormalities were not considered as exclusionary grounds since herpes group virus infection in such patients with neoplastic disease commonly involves pancytopenia. The institutional review board of MSKC approved the study design and consent procedures, and signed informed consents were obtained from all participants (or a responsible guardian in the case of children). The median performance (Karnofsky) score status of the study patients was only 60 and the principal justifications offered for a clinical trial involving such poorly performing patients were that the study was being carried out before the approval of acyclovir for the treatment of such patients and that FIAC showed minimal toxicity at therapeutic doses in the murine HSV model system.
The design was one of an acute study; dosing of patients was at 60, 120, 240, 400, or 600 mg/m2/day (two divided doses) IV for 7 days in a dose escalation sequence. Cessation of progression of lesions occurred within 48 to 72 hours (followed promptly by healing) in all 24 patients who entered the FIAC trial without visceral dissemination and who received FIAC at > 120 mg/m2/day. Spread of disease was not observed in patients with initially localized disease. In patients who had pain before therapy, improvement was noted within 48 to 96 hours. Only two patients developed postherpetic neuralgia, and both had locally advanced zoster with evident sensory nerve involvement before entry into the study. Two patients, both with visceral dissemination of VZV at the time of entry into the study, received the ineffective dose of 60 mg/m2/day and died of multisystem failure on days 6 and 15 of the trial (autopsy information was not provided). Only one patient had recrudescent zoster after the completion of 7 days of FIAC treatment. The three patients with HSV-1 or HSV-2 infection who entered the study had visceral involvement, and all three patients died. In two patients follow-up viral
cultures became negative within 4 days, but they died of their underlying diseases. The third patient with presumed systemic HSV infection showed no new skin lesions after 96 hours of FIAC therapy but died of respiratory insufficiency on the final day of treatment (an autopsy was not performed). The patients in this trial were severely ill, as indicated by their poor Karnofsky scores. In addition, those patients with visceral involvement were particularly ill, and as a consequence their deaths were not unexpected.
The investigators reported that FIAC was generally well tolerated. At the highest dose levels used, the most common side effects were mild to moderate nausea (10 of 13 patients) and vomiting (7 of 13 patients). The second toxicity was myelosuppression, specifically, decreases in both white blood cell (WBC) and platelet counts under FIAC treatment. Nadirs in the WBC count ranged between 60 and 90 percent of normal, but consistent leukopenia was not seen at any dose. A mild but consistent platelet depression (mean level at a nadir of 42,000) was noted at a dose of 600 mg/m2/day. These indications of myelodepression were attributed to FIAC since it was observed in patients who had received no other myelosuppressive therapy.
Comment
The rationale and design of the study were reasonable, and the justification for a trial involving immunocompromised patients with VZV (a group at high risk for disseminated infection) deemed acceptable. A therapeutic benefit was shown in the treatment of VZV infections in immunosuppressed cancer patients with FIAC at a dose of 400 mg/m2/day IV for 7 days. The toxic side effects noted were mild hematopoietic depression (decreases in WBC and platelet counts).
The nature of the trial, with only a short-term follow-up, seems reasonable in view of the short course of infection and what was known at the time about the side effects of this class of drugs. Five deaths occurred among the 24 patients without visceral involvement at the time of entry into the trial. Deaths ascribed to multisystem failure (on the sixth day of treatment and 8 days after completing treatment) occurred in two patients whose VZV infection spread to the viscera and appear likely to have been due to the extensive nature of the viral infections. Two other patients, with HSV infections, died of their underlying diseases after their viral cultures had become negative within 4 days of initiating treatment with FIAC. The fifth death occurred in a patient with presumed systemic VZV infection (skin, esophagus, pulmonary infiltrates) in whom treatment with FIAC was begun on the eighth day of VZV infection. No new skin lesions appeared after 96 hours of therapy, but the patient died of respiratory insufficiency on day 7 of treatment. Autopsies were apparently not performed on any of these patients, and it is not possible to know whether hepatic microsteatosis had developed. From the available limited clinical descriptions it is not possible to ascertain whether lactic acidosis (or an anion gap acidosis) developed terminally. However, it seems to the committee that there were no clear indications in these short-term trials of the type of toxicity that was to develop in 1993 in the trial of chronic dosing with FIAU in the treatment of chronic hepatitis B virus infection.
PHASE I STUDY OF AIDS PATIENTS WITH PRESUMPTIVE OR PROVEN HERPES GROUP VIRUS INFECTION
Eleven patients with AIDS were treated in this study for probable opportunistic herpes group virus infections with FIAC (200-600 mg/m2/day given IV for up to 7 days)(Oclassen Pharmaceuticals, Inc., 1989; Gold, Leyland-Jones, Urmacher and Armstrong, 1984).
Six very ill patients (Karnofsky scores of 20-50) with a variety of opportunistic infections and one patient with Kaposi's sarcoma (Karnofsky score of 90) and perirectal HSV infection were treated with FIAC. Clinical improvement or resolution was observed during FIAC treatment of several patients with HSV infection and one patient with CMV pneumonia. However, five patients died within 15 days (four patients died within 6 days) of initiating therapy. Confusion, lethargy, tremulousness, myoclonic jerking, and/or seizures were observed after the receipt of 5 to 10 FIAC doses in three patients. These neurologic findings cleared within 2 days of omitting FIAC. Acute hypotension, pulmonary edema or pulmonary infiltrates, and/or renal failure also developed in three patients during therapy (or within 2 days of its completion). At autopsy these three patients had disseminated CMV disease (frequently accompanied by Pneumocystis and Mycobacterium avium infections). Two patients developed neutrophil counts of <<1,000/mm3, and one patient developed thrombocytopenia (20,000/mm3). Three of the five patients for whom data were available had aspartate aminotransferase (AST) increases of >300 IU/liter.
Another four patients with AIDS and Kaposi's sarcoma were treated with FIAC (600 mg/m2/day) at a time (1984) when CMV was believed to have a possible direct etiologic role in producing this neoplasm. FIAC was well tolerated without significant leukopenia, thrombocytopenia, or neurologic complications in these patients with Karnofsky scores of 70-90.
Comment
Significant neurologic complications were observed in three patients, and pulmonary complications were observed in five patients. The resolution of the neurologic findings within 2 days of discontinuing FIAC treatment suggests a drug-related side effect. Neurotoxicity had not been observed in any of the 80 other patients with cancer treated previously for HSV, CMV, or VZV infections.
The pulmonary complications or sudden clinical deterioration observed in five patients may have reflected the natural course of their AIDS-associated infections. However, the severity of the deterioration in previously stable patients and the temporal relation of this toxicity with FIAC administration were evident and led the investigators to think that FIAC was responsible. Although several infectious agents (P. carinii, M. avium-intracellulare) were responsible for the pneumonias, in all autopsied patients widespread infection with CMV was present. The possibility that FIAC therapy might be associated with worsening of CMV pneumonia was raised by the investigators. They felt that the temporal relationship between FIAC treatment and the neurologic and pulmonary complications noted in this trial warranted caution in undertaking antiviral therapy in patients with AIDS.
As in the other MSKC studies of FIAC, evidence of some marrow suppression, primarily in the sickest patients, was observed. In the sickest patients with systemic opportunistic infections (often multiple), significant elevations in AST levels occurred, but the relative contributions of the infections and of FIAC are difficult to sort out. The committee has found no mention in the publications describing these patients of microvesicular steatosis in the livers of the patients who died. The neurologic and pulmonary complications noted in these patients with AIDS treated with FIAC appear to be different than the hepatotoxicity and pancreatitis later noted in patients with hepatitis B virus infection treated with FIAU.
PHASE I STUDY OF FIAC IN BONE MARROW TRANSPLANT PATIENTS WITH HERPES GROUP VIRUS INFECTIONS
This unpublished study, carried out by members of the Antiviral Working Group of MSKC, involved 15 bone marrow transplant (BMT) recipients who received 60-400 mg of FIAC per m2 IV daily for complicating VZV or CMV infections (Oclassen Pharmaceuticals, Inc., 1989). Five patients received 120-200 mg/m2/day for 5 to 7 days for the treatment of cutaneous or visceral disseminated VZV. All five patients had good initial responses. In two of those with VZV, recurrence of lesions occurred immediately posttreatment, and retreatment was successful. The other 10 patients were treated for proven or probable CMV pneumonitis. Two patients were moribund on respirators and died after receiving only one or two doses of FIAC. The remaining patients were very seriously ill (pretreatment Karnofsky scores of 20-40, except for one patient with a score of 70). Modest clinical or radiological improvement was observed for 3 to 5 days in three patients after starting FIAC (120-800 mg/m2/day for 5-14 days), but the clinical course was progressively downhill; death supervened in 6-20 days following the cessation of treatment in 9 of the 10 patients. Transient improvement in retinitis occurred in one patient, but death was due to disseminated CMV infection. Another patient died on the 12th day after completing therapy and had disseminated CMV disease which included brain involvement. In two patients receiving 300-400 mg of FIAC per m2/day, sudden hypotension and pulmonary edema occurred after 9 and 14 doses had been administered respectively. In the one surviving patient in the group with CMV infection, urine cultures became negative after treatment, but a lung biopsy showed only adenovirus and P. carinii infection, casting doubt on the original diagnosis of CMV infection.
Hematologic and liver function parameters were followed in these 15 study participants. Three VZV patients with well-established grafts (and another treated within 4 weeks of engraftment) did not have clinically significant drops in WBC or platelet counts. Of the eight patients with CMV infections who received more than two doses, six had well-established grafts when they were treated with FIAC. Depression in WBC counts occurred in all of these patients, but in only one of them was the neutropenia <<1,000 cells/mm3. This patient was one with severe graft-versus-host hepatitis in whom platelets also dropped from 39,000/mm3 to 3,000/mm3 eight days after completing 10 doses of FIAC (300 mg/m2/day). This patient died of a massive gastrointestinal hemorrhage. In four of the remaining five patients platelet counts dropped to less than 20,000/mm3 from pretreatment levels of 28,000-97,000/mm3
Increases in AST levels of at least 50 IU/liter occurred in 5 of 13 patients completing treatment (1 with VZV and 4 with CMV), and 8 of 13 patients had bilirubin increases of >1 mg/dl.
Comment
The patients with VZV infection appeared to respond to FIAC at the dosage used, but two patients had relapses and required retreatment. Response to FIAC in patients with CMV infection was more problematic, since these patients were severely ill on entering the trial (Karnofsky scores of 20-40) and only one patient survived beyond 21 days of beginning treatment. The principal side effects noted were drops in WBC and platelet counts, but baseline levels in these BMT recipients were already low. Increases in AST and serum bilirubin levels were noted in more than one-third of the patients, but these were not dose related. It seems likely to this committee that the putative explanations offered for the liver function abnormalities, that is, graft-versus-host disease or CMV hepatitis, were correct in view of the fact that all but the immediate postengraftment patients were already receiving suppressive therapy with steroids for this and in view of the autopsy-confirmed CMV hepatitis in three patients.
PHASE I ORAL DOSE RANGING FIAC STUDY IN IMMUNOCOMPROMISED PATIENTS WITH VZV AND HSV INFECTIONS
This study of oral FIAC therapy in 26 patients with VZV or HSV infections was carried out at MSKC by members of the Antiviral Working Group (Oclassen Pharmaceuticals, Inc., 1989; Fanucchi, Leyland-Jones, Young, Burchenal, Watanabe, and Fox, 1984). All of these patients had underlying neoplastic disease (n = 24), principally hematologic or lymphoproliferative, or AIDS (n = 2). Localized zoster was present in 17 patients, another 7 had cutaneous dissemination, 1 patient had visceral involvement (hepatitis) in the course of disseminated disease, and in 1 patient HSV infection was disseminated on the skin.
Initial dosing was 100 or 1,000 mg/m2 orally twice daily in 11 patients. Nausea and vomiting followed dosing in 9 of the 11 patients, and this led to decreased but more frequent daily dosing: 11 patients received 30, 90, or 150 mg/m2/day in aliquots three times daily. Nausea and vomiting occurred in two of five patients taking 150 mg/m2 daily. Among the six patients taking the lower daily doses only three reported mild nausea and rarely required antiemetics.
The response of VZV infections to oral FIAC therapy was excellent, and no new cutaneous lesions were observed after 72 hours of therapy in 24 of 26 patients. One patient receiving 30 mg/m2/day continued to have cutaneous progression through the fourth day of therapy.
The toxicity observed in this oral trial, like that in the prior IV trials, primarily involved the hematopoietic system. In 15 patients receiving the higher doses the median WBC count dropped 30-50 percent and the median platelet count dropped 15-40 percent of the baseline
values. One patient with disseminated VZV infection and hepatitis had a baseline AST level of 63 IU/liter, which rose to 395 after 3 days of FIAC at 150 mg/m2/day given orally, and then rapidly declined while treatment was continued for the rest of the 7-day course of treatment.
Comment
Dosing with FIAC orally was limited to less than 200 mg/m2/day because of nausea and vomiting. The response of VZV infection to FIAC at 30 to 200 mg/m2/day was excellent. The main toxicity was mild to moderate, but temporary, leukopenia and thrombocytopenia. In addition, elevated AST levels were observed in one patient who entered the study with VZV hepatitis.
PHASE I/II TRIAL OF FIAC EFFICACY IN IMMUNOSUPPRESSED PATIENTS WITH VZV INFECTION
This trial, the results of which were reported by Leyland-Jones, et al (1986) involved 34 immunosuppressed individuals (advanced malignancy or severe immunodeficiency associated with lymphoproliferative disease or cancer) who developed recurrent infection with VZV and who had shown progression of viral lesions in the 24 hours before entering the study. Study entry required a serum creatinine level of <2.0 mg/dl, but there were no limitations of age, hepatic function, or blood counts. The rationale for this study was the significant incidence of dissemination (7-26 percent in several Series) in patients with such underlying disease and the life-threatening nature of these infections with visceral involvement.
The trial was designed as a randomized, double-blind comparison of FIAC with Ara-A, a drug which had been standard therapy for VZV infections in immunosuppressed patients. Patients were stratified by spread of disease (local, disseminated or visceral) and delay to treatment ( <72 or >72 hours). FIAC was administered for 5 days at a dosage of 400 mg/m2/day IV, and Ara-A was given IV at a daily dosage of 400 mg/m2.
Results were evaluable for 31 of the 34 subjects. In those subjects treated with FIAC the clinical response was superior to the response with Ara-A: the median time to formation of the last new vesicle was reduced by approximately 3 days, crusting occurred in a significantly greater proportion of patients within the first 72 hours after the initiation of treatment, the disappearance of pain occurred earlier, and the cutaneous dissemination of zoster occurred less frequently (in 0 of 17 patients receiving FIAC versus 2 of 16 treated with Ara-A).
FIAC produced few toxic reactions in this study, and all were judged to be mild. Fatigue (evaluated on the fourth day of treatment) was noted in 57 percent of those receiving FIAC, and this figure did not differ significantly in those receiving Ara-A. More nausea and vomiting occurred in those receiving FIAC, but the difference was not statistically significant. Hematologic changes observed in the first FIAC trial were again observed, but the median decreases in WBC (37.5 percent) and platelet (42 percent) counts observed did not differ significantly from the decreases observed in the patients receiving Ara-A. Changes in serum
bilirubin, alkaline phosphatase, and creatinine levels also did not differ statistically between the two treatment groups. However, a transient rise in AST levels was observed in 54 percent of those treated with FIAC and in only 14 percent of those receiving Ara-A (P = .046).
Comment
The clinical response of VZV infection to FIAC was better than the response to Ara-A, the available drug therapy at that time. The toxic side effects noted included nausea, vomiting and fatigue, but their frequency in FIAC-treated patients did not differ statistically from that in those receiving Ara-A. However, a transient rise in AST levels was significantly more frequent (P = 046) among those receiving FIAC than those receiving Ara-A. Overall, the toxic reactions were considered mild.
SUMMARY OF ALL THE FIAC CLINICAL STUDIES AT MSKC
FIAC orally given or IV had a beneficial effect in the treatment of VZV infections. Its efficacy against CMV was unclear because of the uncertainty of the diagnosis in many patients and the steady downhill course of many of the seriously ill patients. Toxicity appeared to be manifested primarily as hematopoietic suppression and a mild elevation in AST levels. However, in several severely ill patients with AIDS acute, reversible neurotoxicity developed during FIAC administration. Such toxicity was not observed in treatment groups with underlying neoplastic disease. The pulmonary complications, clinical deterioration, and deaths occurring in the group of patients severely ill with AIDS (and multiple opportunistic infections, including CMV) were temporally related to FIAC therapy. Whether IV administration of FIAC may have contributed to any of the acute deaths in the study cannot be determined from the available information; the underlying disease with disseminated superimposed infections in these ill patients may have been the main factor in the demises. Since dosing was only for short periods in these trials, the potential for toxicity with long-term use would not have been discernible. However the IV doses of FIAC used were very high compared with those used orally in later trials (see the section below on the Oclassen R-89-001 trial). The extremely high dose may be relevant, despite the short course of therapy, in view of what is now known of the long half-life of the principal metabolite, FIAU.
Further clinical trials of FIAC were not carried out at the time, probably because of the emergence of an effective, relatively nontoxic nucleoside analog (acyclovir) for the treatment of HSV and VZV infections. Thus, the return to clinical study of FIAC in 1989 (R89-001-01: Efficacy and Safety of Oral FIAC in AIDS Patients with Cytomegalovirus Infection—A Dose Ranging Study) under the sponsorship of Oclassen Pharmaceuticals seems to have been reasonable in view of the drug's in vitro activity against CMV (an important viral infection in patients with HIV infection and for which there was need of effective oral antiviral drugs).









