3
Who are the Recipients of Treatment?
Policymakers and the interested public have a number of questions about heroin use and addiction. These questions include the following. How large is the population of heroin users and addicts? Does it appear to be growing or shrinking? How are heroin addicts distributed geographically and demographically in the population? What other substances do heroin addicts use that are detrimental to their well-being? What concurrent medical and social problems do heroin addicts have for which they need services? How persistent is heroin addiction if untreated? How likely are heroin addicts to seek treatment? What are the characteristics of those who do and do not seek treatment?
The major sources of information about the frequency of heroin use and addiction are general and special population surveys and information obtained from persons arrested for possession or sale of illegal drugs and those in treatment. Each data source has its limitations and no single source provides all the information that might be desired. Consequently, following this introductory discussion this chapter discusses respectively, data from population-oriented, addict-oriented, and treatment-oriented information sources.
The limitations of data about illicit substance abuse are intertwined with issues of concept and definition. There is no official psychiatric diagnosis termed "opiate addiction," the disorder that methadone programs treat. Instead, the newly published DSM-IV offers the following diagnoses: opiate dependence, opiate abuse, opiate intoxication, opiate withdrawal. Dependence requires three or more of the following symptoms occurring within a 12-month period: tolerance; withdrawal; taking larger amounts or taking amounts over a longer period than was intended; persistent desire or failed efforts to reduce or control use of the substance; spending a great deal of time obtaining the substance, using it, or recovering from its use; giving up important social, occupational, or recreational activities because of substance use; and continued
use despite knowledge of a persistent physical or psychological problem likely to have been caused by use of the substance.
Addiction, as defined by Dorland's Medical Dictionary, would fall within the dependence diagnosis, but would be somewhat more severe. It requires, in addition to regular heavy use, four symptoms. One of these is dependence (physical or psychological); the others are a tendency to increase dosage (which is equivalent to tolerance in the dependence diagnosis), an overwhelming desire or need (compulsion) to continue use and to obtain the drug by any means (which appears in the DSM-IV definition of dependence as use in larger amounts than intended and inability to stop use, even when the drug's detrimental effects are known), and a detrimental effect on the individual and society (which appears in the DSM-IV definition of dependence as giving up social, recreational, and occupational activities to use the drug).
In addition to these efforts to definition the states experienced by individuals (e.g., tolerance, dependence, addiction) there are also various descriptions of a continuum regarding the use or consumption of drugs, legal and illicit. These descriptions include (1) "occasional use to regular use" (CDC, 1987), (2) "use, abuse, dependence, and recovery" (Gerstein and Harwood, 1990), and (3) "general use versus problematic use" (Reuter, 1993). For the purposes of this chapter, we will adopt a similar approach to analyzing the data. Specifically, we will discuss the continuum of those who ever used opiates, those who ever become dependent on opiates, those who become addicted, and those addicts who have been treated.
The data, drawn from multiple sources, show a steady reduction in numbers along this continuum. The vast majority of Americans have never used a self-administered, nonprescribed opiate. Of those who have used one, about half do not proceed beyond occasional use. Others progress to a relatively brief period of dependence (Biernackie, 1986) and cease use without treatment.
At the other end of the continuum, however, are those who engage in substantial use over long periods, become dependent, and fail at voluntarily ending their dependence. These are the addicts for whom methadone treatment is intended, treatment that has given rise to the methadone regulations. Although they represent a relatively small percentage of the total users of opiates, addicts constitute a large absolute number who contribute disportionately to drug-related crime and threats to the public health. Much more is known about the heroin addict group than about those who use heroin occasionally or are briefly dependent on it, because it is the addicts who generally come to the attention of treatment and criminal justice personnel.
Heroin Use and Dependence
Population-based surveys covering the use of all illicit drugs often do not assess dependence or addiction at all. Estimates based on such surveys indicate that only about 1 percent of the U.S. population has ever tried heroin. The few studies that have measured dependence find that less than half of this 1 percent who try heroin ever develop dependence. The percentage currently dependent is not known precisely. Nor is it known what proportion of those currently dependent would qualify for methadone maintenance programs by having been daily users for a year or longer and unable to cease on their own or with medical supervision. But the proportion of the population who could be candidates for methadone maintenance must be smaller than the 0.5 percent who have ever been dependent. We discuss below some findings from epidemiologic studies that put upper bounds on the number of addicts in the population.
Available epidemiological data on heroin use and dependence, coupled with data from other sources about the addict population, provide a background for placing methadone treatment in context and answering a number of specific questions that affect the committee's charge.
Prevalence of Heroin Use
While the use of other drugs has varied considerably over time, the number of persons who reported that they had ever used heroin, a number which soared about 1969, appears to have been quite stable since then at just below 1 percent of the general population. This stability is demonstrated in Lloyd Johnston's graphs, showing results from Monitoring the Future, a nationwide longitudinal, cohort study (Johnston, et al., 1993). In this study, each year 12,000 to 18,000 adolescents, selected from senior classes in a national sample of high schools, are surveyed; of those graduating from 1978 to 1991, representative samples of 2,400 have been selected for follow-up each year. The 2,400 are randomly divided in half and 1,200 are followed every two years on even years, 1,200 every two years on odd years. Thus, the sample of young adults being surveyed in recent years includes every age from 19 to 32.
This study found a stable rate of heroin use by young adults initially surveyed as high school seniors since 1986 (see Figure 3-1). The low flat curve for heroin use contrasts with that for crack cocaine use, which has been declining since 1986. In this study, Johnston and colleagues found rates of ever having tried heroin differed with age—1.2 percent of the 18-year-olds compared to 3 percent of those 31–32-years-old. Interestingly, none of the older group with heroin experience admitted any heroin use in the year before
the interview. In no age group did the proportion using in the last month rise above 0.3 percent, and it was less than 0.1 percent in those 25 or older. The fact that less than a quarter of those who report ever having used heroin also report use in the last month suggests either that use by high school seniors does not often lead to dependence or that dependence is typically brief, or both. Since the proportion of subjects who used any heroin at all in the last month is less than 0.2 percent, the proportion currently addicted to heroin has to be below that figure. However, this conclusion should be interpreted with caution, as persons who reach the senior year of high school, having shown a capacity to manage their school careers, may be less susceptible to the serious consequences of heroin use than others their age not in school.
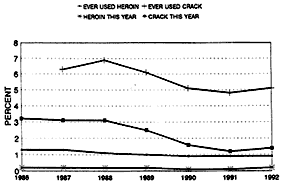
Figure 3-1
Changes in drug use over time by young adults—heroin compared to crack cocaine.
SOURCE: Johnston et al. (1993).
Another important epidemiological study of drug use is the National Household Survey, which interviews persons 12-years-old and older in a national sample of household residents every year or two. In the 1992 National
Household Survey, the proportion of interviewed household members who had ever used heroin was 0.9 percent and use in the last year was 0.2 percent. The age group with the highest lifetime rate of having ever used heroin was the 26–34-year-olds (1.6 percent) and of having recent use was the 18–25-year-olds (0.5 percent). These data support Johnston's finding that most of those who ever used heroin no longer use it.
From Use to Dependence
Neither Monitoring the Future nor the National Household Survey assesses dependence on or addiction to heroin, only the amount of use. Indeed, population surveys that provide rates of dependence on heroin are scarce. Even in these surveys, when the population sampled is limited to household residents, questions can be raised about the prevalence estimates for dependence because not all addicts live in households and those in households may be unwilling to be interviewed. Therefore, estimates of the number of heroin-dependent individuals based on household surveys must be considered minimum estimates.
Four general population studies have assessed dependence on heroin as well as use. In a small study (N = 235) of young African-American men born and brought up in St. Louis (conducted in 1965), 13 percent had used heroin, with use generally beginning between ages 16 and 23 (around 1950). Ten percent of the sample, or 79 percent of the men who reported using heroin, said they had become addicted to it (Robins and Murphy, 1967), by which they meant they were heavy users and had experienced withdrawal symptoms. In 1973, in a follow-up of a random sample of Army enlisted men (N = 900) who had been in Vietnam at the height of the heroin epidemic there in 1970–1971, about 44 percent reported having tried an opiate while there, and 20 percent became addicted, again defined as heavy use plus persistent withdrawal symptoms when they stopped. Thus they had a 45 percent risk of dependence if they used (Robins, 1974). In 1982, the Epidemiological Catchment Area (ECA), a large study of mental disorders in the general population, interviewed 18,000 persons 18 years of age and older, including the institutionalized. When weighted to make the sample representative of the total U.S. population over 18, 1.3 percent had tried heroin six times or more and 48 percent of these more-than-experimental users had become dependent according to DSM-III criteria (Anthony and Helzer, 1991). Finally, in the recent National Comorbidity Study, 8,098 household residents aged 15–54 were asked if they had ever used heroin even once; one percent had used, and only 23 percent of users qualified as ever dependent according to DSM-III-R criteria (NCS, 1994). The last two studies, which are studies of the general
adult population, find lifetime rates of heroin dependence of 0.6 percent and 0.2 percent. The proportion who are candidates for methadone treatment, because their dependence was severe enough to qualify as addiction and for whom the addiction is currently active, must be smaller than these figures.
The first of these four studies was conducted in 1965, the most recent in 1992. Although they differ in populations studied, methods of sampling, and questions asked, they agree that many who try heroin do not become dependent on it. The rates of use and dependence suggest that the risk of becoming dependent if heroin is tried may have declined over the 30 years the studies span.
However, there is no guarantee that the stability (or possible decline) of dependence among heroin users will continue. In the late 1980s, the price of heroin fell sharply and the purity of street heroin rose. Although most heroin addicts use injection into the vein as their method of ingestion, the quality of heroin in some areas of the country is now high enough to allow smoking or snorting as a route of administration, thus removing a major barrier to heroin use. These changes may lead to both an increase in users and a higher probability that users will become addicted.
How Persistent is Heroin Dependence?
Although estimates of the typical duration of dependence are not precise, these studies suggest that dependence often ends without treatment. The study of young African-American St. Louis men found only 3 out of 22 self-described one-time "addicts" still using heroin in their early thirties, although only 4 had any treatment. Only 12 percent of the Vietnam veterans who reported having been "addicted" in Vietnam reported relapse in the first three years after their return to the United States, and these self-reports were confirmed by almost uniformly negative urine tests for opiates at 1 and 3 years after their return. In the ECA, which evaluated dependence according to DSM-III criteria, the St. Louis sample was asked whether problems had been experienced with each drug used in the last year. Among the St. Louis ECA subjects who had ever been dependent on heroin, only 5 percent reported having had any of the symptoms of heroin dependence in the current year.
The above paragraph in no way denies the importance, and the needs, of the significant group of those who become dependent and progress to addiction and who find it impossible to quit without help. This addict population is a subset of the general heroin user population and differs from it in important ways.
Information about the addict group is available from several long-term natural history studies of addicts known to treatment or the courts, including
Vaillant (1973), Simpson et al. (1986), and Hser et al. (1993). This last study followed 581 male heroin addicts from about 1962–1964, when the average age of this group was 25.4 years and they had been addicted nearly six years, through 1986, when they had an average age of 47.6 years. Over this 24-year period, 28 percent had died. At interview in 1986, 18 percent were incarcerated, 23 percent had urines positive for heroin, only 29 percent were urine negative, and only 20 percent reported having been heroin-abstinent during the previous three years.
The Hser findings were similar to those of the other two studies, which found that death, incarceration, or continued addiction was the course of the majority of addicts identified in treatment or criminal justice settings. Once heroin addiction is established, in many cases even for a relatively short period, it tends to persist and most addicts relapse repeatedly. It is this group of chronic addicts for whom methadone programs provide opportunities for living a productive life.
Age, Gender, and Ethnicity
General population surveys identify some relationships between individual demographic characteristics and heroin dependence. Most of these relationships are confirmed in special population studies (see below), but some change when only the treated addict population is considered.
Age
Heroin-dependent individuals in the 1990s are mostly under 40 years of age. Their youth can be explained in three ways: First, few people now over 50 have ever tried heroin, which became generally available around 1970 but has been initiated almost exclusively before age 30, thus leaving out persons over 30 when it first appeared. Second, the death rate among heroin addicts is high, decimating those who continue their addiction for 10 years or longer. Third, chances of recovery increase with age, so that those who try to quit are increasingly successful as they mature. Thus, heroin dependence typically began in the early 20s among persons born after 1945 and eventuated either in death or recovery by age 40.
Gender
Gender is less strongly related to use and dependence than is age, but the relationship is still substantial. There is good agreement across studies that
heroin dependence is predominantly male. Rates in men were 2.5 times that in women in the National Comorbidity Study. In the ECA, male rates were almost 5 times that in women. However, the ECA found that dependent women are slightly more likely to recover than men (55 percent versus 47 percent).
Ethnicity
Heroin is somewhat more popular with African-Americans than whites, although differences are small. In the National Household Survey, 1 percent of African-Americans and 0.9 percent of whites had tried heroin. Among high school seniors followed into adulthood, 2 percent of African-Americans and 1.2 percent of whites 26–32-years-old had ever tried heroin (Johnston et al., 1993). The association of minority status is much less pronounced than the association of either age or gender with the use of heroin. There were too few minority users in the ECA to allow reliable comparisons of races with respect to the chance that users would become dependent.
What Other Substances Do Heroin Users Consume?
Every population study in the last 30 years has found that heroin-dependent persons typically use and become dependent on a variety of other substances, both legal and illegal, in addition to heroin. In the Vietnam study for example, those who used heroin after their return to the United States on average used 8 different illicit drugs. Men dependent on heroin were asked what their main drug was after their return from Vietnam; 40 percent named alcohol, marijuana, or some drug other than heroin. Among heroin-dependent persons in the ECA, conducted in the early 1980s, more than 40 percent also had problems with cannabis and sedatives and almost as many had problems with stimulants (39 percent). The ECA showed that 48 percent of heroin-dependent persons were also alcohol-dependent.
The main national shift in consumption of illicit drugs in the 1980s is certainly to cocaine. The 1982 ECA sample contained 6.5 times as many heroin users as users of cocaine. In 1992, the National Comorbidity Study found the relationship had reversed—there were over 6 times as many cocaine users as heroin users.
These results suggest that heroin-addicted persons in treatment will have dependencies on a variety of other substances and that problems with drugs other than heroin may be as responsible as heroin for their distress and maladjustment. Data from community, arrestee, and treatment populations
presented below confirm these results. Indeed, the presence of severe problems due to drug use is an increasingly frequent characteristic of heroin addicts, according to clinicians.
Other Medical and Social Problems of Heroin-Dependent Persons
Heroin-dependent persons typically have a variety of psychiatric, medical, and social problems in addition to their substance dependence. As compared to persons their own age and sex, heroin-dependent individuals in the ECA had an excess of depression and other serious psychiatric disorders. ECA data for the 248 men under 40 who ever met the criteria for heroin dependence showed dramatic rates of comorbidities compared with the remaining 3,800 men in the same age group. Depression was found in 19 percent of the former compared with 4 percent of the remainder; schizophrenic symptoms in 9 percent versus 2 percent; panic disorder in 5 percent versus 2 percent; and a manic episode in 4 percent versus 1 percent of other young men. Whether or not these disorders are the result of the heroin dependence, or independent of it, it is clear that persons dependent on heroin need psychiatric assessment and treatment.
The heroin-dependent person frequently has many medical problems in addition to his or her dependence. Some of these problems stem from the way in which heroin is administered and its illegal status, rather than from the effects of heroin itself. It is injection that accounts primarily for infections, hepatitis, and AIDS. It is the illegal status of heroin that accounts for the elevated risks of homicide and injury associated with its purchase and sale, and for overdose death or poisoning due to variations in the strength and purity of the drug as purchased on the street. Methadone maintenance treatment makes a major contribution to the addict's health and to public health in general by eliminating or reducing injection and the purchase and sale of heroin in the illicit market, and by substituting a drug of known strength and quality for street drugs.
Despite their liability to ill health as a result of infections or the drug itself, heroin-dependent persons are not heavy users of routine or primary medical services. In the ECA, heroin-dependent persons were no more likely than others to have seen a doctor in the last 6 months. When these individuals do seek medical care, it is often at hospital emergency rooms and when their medical problems have reached an advanced stage. Thus, dependent persons, and certainly heroin addicts among them, appear to be a particularly medically underserved population.
Heroin-dependent persons have a number of social problems, including difficulty in holding jobs, obeying laws, maintaining stable marriages, making
and keeping friends, and functioning as caring and responsible parents. These difficulties are related to the fact that getting and using drugs leaves little time for other activities. In addition, heroin addicts commit a large number of crimes in order to support their addiction.
Many who become heroin-dependent had, while still children and before any drug use, behaviors that forecast adult social problems in non-drug-users as well as in heroin addicts. For example, there was frequently a childhood and early adolescent history of school problems and truancy, delinquency, drinking, lying, running away from home, and fighting. The fact that these early behaviors predict adult social problems independent of drug dependence means that once the heroin addiction is controlled through methadone treatment, the addict's social problems are likely to decline but not vanish. Many addicts will still be socially incompetent and continue to be involved in illegal behaviors, because they had these tendencies before their addiction.
When considering what methadone treatment is likely to accomplish, then, it is important to remember that the heroin-dependent person who has progressed to addiction brings many medical and social problems to the treatment setting, in addition to addiction, that pose a challenge to the treatment system going well beyond treating drug addiction. Many clinicians believe that these other problems have become more severe in today's patient.
How Likely Are Heroin Addicts to Use Treatment?
What proportion of all addicts enter treatment? According to self-report data in the ECA, 37 percent of heroin-dependent persons have ever attended a drug treatment program, a proportion that does not vary with age. Dependent men, on the other hand, were less likely to attend than dependent women (32 percent versus 51 percent). But the greatest difference was found by ethnic background. Only 28 percent of white heroin-dependent persons had attended a specialized drug treatment program, although 50 percent of minority heroin-dependent persons had done so (calculated for the committee from ECA tapes). The result is that minorities are more overrepresented in treated populations than in the total user population.
What characteristics of an addict are associated with the decision to enter treatment? Those persons who enter treatment are older and have been more severely addicted for a longer time than heroin-dependent persons who do not enter treatment. Although treated addicts, like the general population of heroin users, are disproportionately young males, this disproportion is less striking than in the general heroin population. The greater representation of older addicts in treatment is explained both by the fact that it is only after some years that the disadvantages of addiction relative to its pleasures become
apparent and drive the addict to seek help, and by the fact that the first treatment episode often fails, which means that the treated population includes a large number of repeaters, i.e., those who have relapsed to heroin use and have then returned to treatment. The greater representation of female addicts in treatment may be explained by the fact that, in general, women are more likely than men to seek medical care (Fiorentine and Anglin, 1993).
Characteristics of Untreated and Treated Heroin Addicts
This section shifts the focus from population-based surveys to surveys of heroin addicts. Empirical data are presented that characterize what is known about contemporary populations of untreated and treated addicts.
If one moves from examining the characteristics of users and addicts that are demarcated by general population epidemiological studies, which have been discussed earlier, to characteristics as demarcated by epidemiological studies specific to addicts, then the chronicity of addiction and the dysfunctional nature of addict lifestyles becomes quite clear. Table 3-1 provides such addict-specific information by drawing on data from samples or subsamples within two multiple-site national studies. The first is the National AIDS Demonstration Research (NADR) program, funded by NIDA in 59 sites across the nation. Results from a NADR subsample were among the most salient in indicating the large proportion of heroin addicts who have never received formal treatment. The second is the Drug Use Forecasting (DUF) program, funded by NIJ for calendar year 1990 in 24 cities across the United States. Each quarter, DUF staff selects booked arrestees and interviews them about their drug use histories. Unlike most other surveys of addicts, DUF also requests voluntary urine samples—which are provided in 85–90 percent of cases—which are objectively tested for the presence of 10 drugs. Given their extensive geographic coverage, access to heroin addicts, and large sample sizes, these two studies (which are also discussed in Chapter 4) provide very useful data related to untreated and treated heroin addicts.
The interpretation of the data provided in Table 3-1 should focus primarily on the pattern of responses within each study, and only limited comparisons should be made across the studies. This is necessary because study methodologies access different samples, and define somewhat different measures for the variables represented.
The first study, the NADR study, included a fairly large subsample of primary heroin addicts (about 16,500) accessed through nontraditional access mechanisms (i.e., they were not drawn from treatment programs or criminal justice populations). The three groups within this subsample are large, each
exceeding 5,000, being evenly distributed across addicts who report no treatment history (34 percent), those who report a treatment history exclusive of methadone (32 percent), and those who report any methadone maintenance history (34 percent). Data from this study recapitulate a number of the findings reported earlier for general population studies of heroin users and addicts. These include the finding that the proportion of women among those reporting methadone maintenance histories is higher than the proportion of women among those reporting any nonmethadone treatment history or no treatment history. While proportions of African-Americans are equivalent across all three groups at about 42–44 percent, the proportion of Hispanics decreases steadily across the three groups and the proportion of whites increases steadily. The mean age also increases across the three groups from 33 years in the group reporting no treatment history to 37 years in those reporting some prior exposure to methadone maintenance. Similarly, the proportions of those over 30-years-old in each group increase steadily to a maximum of 87 percent in the methadone maintenance treatment group. In contrast to the no-treatment-history group, those with a treatment history, particularly those with a methadone maintenance history, report more prior contact with the criminal justice system and have longer reported years of addiction. The methadone group reports higher rates of prior treatment than the nonmethadone treatment group. The methadone maintenance group reports slightly less employment before interview, and slightly more criminal involvement, than the other groups. Rates of cocaine use are similar across all three groups, while rates of marijuana use are less in the methadone maintenance group.
The DUF data cover approximately the same period as do the NADR data. The sample size reported for 1990 is reasonably large, at about 3,000 cases. As might be expected with an arrestee population, over 60 percent report no treatment history. A caution in interpreting the DUF data is important here. Any arrestee who reported prior opiate dependence or whose urine was opiate-positive at the time of interview was included in the opiate user or addict category. Therefore, that group may include some few opiate users who were not addicted. Furthermore, this data base did not distinguish between methadone maintenance and other types of drug treatment.
Replicating earlier patterns described in this chapter, the sample shows that those reporting a treatment history are somewhat more likely to be women, to be white, and to be older. Rates of reported legal income in the period before interview are surprisingly high and involvement in criminal activity is significant, with the treated group somewhat less employed and more criminally involved. Use of other substances is similar across the two groups, but the treated group reports slightly more cocaine use, and slightly less marijuana use.
In sum, opiate users accessing treatment have more extensive histories of opiate addiction, have more prior treatment failures, and are marginal in terms of employment, criminal activities, and polysubstance abuse. The population of untreated and previously treated opiate addicts together comprises the pool of active users who may need, may seek, and may utilize methadone maintenance treatment. This brings us to our third source of information about heroin use, dependence, addiction, and treatment: addicts now in methadone maintenance treatment.
Methadone Patient Characteristics
The following section presents data on historical tends and current characteristics of those heroin addicts now in methadone maintenance treatment. We examine most closely methadone maintenance clients, and briefly describe methadone detoxification clients. As noted above, there are some significant differences between the general heroin-addicted population and the patient population. Overall, addicts who enter into a methadone treatment program either maintenance or detoxification, are more desperate, more physically and mentally ill, poorer, and more disabled than the general addict population. In addition there are regional differences in patient characteristics as well as differences between patients in publicly funded treatment programs, and in programs relying on private (usually client paid fee-for-service) funds.
Historical Trends
Three nationwide studies of drug abusers entering treatment have been conducted that provide information as to historical trends in methadone maintenance treatment admissions over the last three decades. The first of these was a series of studies collectively called the Drug Abuse Reporting Program (DARP) research on drug treatment admissions during the years 1969 through 1973. The second series of studies was known as the Treatment Outcomes Prospective Studies (TOPS), which yielded characteristics of patients entering methadone maintenance during the years 1979 through 1981 (see Flynn et al., 1994). The most recent nationwide study, known as the Drug Abuse Treatment Outcome Studies (DATOS), examined methadone patient characteristics for the years 1991 through 1993 (see Flynn et al., 1994). Finally, special computer runs in 1993 by SAMHSA's Office of Applied Studies detail characteristics of methadone maintenance admissions for the 26 states reporting admissions for calendar year 1992. Table 3-2 shows basic characteristics of methadone maintenance patient across the time periods represented by the data.
TABLE 3-1 Characteristics of Heroin Users and Addicts at Percentage Occurrences Within Untreated and Treated Groups
|
|
NADR Sample (total N = ~16,500) |
|
DUF Sample (total N = ~3,000) |
||
|
Characteristic |
No Treatment (N = 5,542; 34% of total) |
Some Nonmethadone Treatment History (N = 5,296; 32% of total) |
Some Methadone Maintenance History (N = 5,662; 34% of total) |
No Treatment History (N = 1,092; 63% of total) |
Any Treatment History (N = 1,095; 37% of total) |
|
Female |
27 |
25 |
32 |
32 |
38 |
|
African-American |
43 |
42 |
44 |
48 |
41 |
|
Hispanic |
42 |
36 |
30 |
25 |
22 |
|
Mean agea |
33 |
34 |
37 |
31 |
34 |
|
Over 30-years-old |
66 |
72 |
87 |
57 |
70 |
|
High school graduate |
48 |
56 |
61 |
58 |
61 |
|
Ever married |
— |
— |
— |
38 |
48 |
|
Prior incarceration |
75 |
85 |
91 |
— |
— |
|
Years addicteda |
12 |
14 |
18 |
— |
— |
|
|
NADR Sample (total N = ~16,500) |
|
DUF Sample (total N = ~3,000) |
||
|
Characteristic |
No Treatment (N = 5,542; 34% of total) |
Some Nonmethadone Treatment History (N = 5,296; 32% of total) |
Some Methadone Maintenance History (N = 5,662; 34% of total) |
No Treatment History (N = 1,092; 63% of total) |
Any Treatment History (N = 1,095; 37% of total) |
|
3 or more prior |
0 |
43 |
77 |
— |
— |
|
Court referred |
— |
— |
— |
— |
— |
|
On legal supervision |
23 |
28 |
30 |
— |
— |
|
Employed |
28 |
28 |
28 |
71b |
65b |
|
Criminal activity |
44 |
49 |
53 |
30c |
42c |
|
Cocaine used |
81 |
84 |
79 |
70 |
76 |
|
Marijuana used |
39 |
37 |
28 |
28 |
22 |
|
NOTE: NADR = National AIDS Demonstration Research programs; interviewers were heroin addicts not accessed through treatment treatment programs or the criminal justice system. DUF = Drug Use Forecasting program; interviewers were arrestees categorized as opiate users or addicts. NADR data are for 1989–1990; DUF data are for 1990. a Data in this row are mean years. b Percentage reporting legal income sources in past month. c Percentage reporting illegal income sources in past month. d Reported as a secondary drug problem. SOURCE: Complied from data from the NADR program and the DUF program by Mel Widawski, Senior Statistician at the Drug Abuse Research Center of the University of California, Los Angeles. |
|||||
In examining the data presented in Table 3-2 it should be kept in mind that the first study depicted, DARP for the years 1969–1973, occurred primarily in the years before federal regulations were instituted (see chapter 5). The second and third studies, TOPS and DATOS, occurred after the institution of federal, and subsequently State, regulations, at approximately 10-year intervals. The final column includes data from the Client Data System (CDS) maintained currently by the Substance Abuse Mental Health Services Administration, Office of Applied Studies. These data are not from a research study, as were the prior three, but are instead from a drug treatment admission monitoring system, which is discussed in more detail below. Of most importance for methadone regulation purposes are the DARP, TOPS, and DATOS study. The CDS information is presented primarily as a confirmation of the accuracy with which the DATOS sample represents the full population of methadone admissions for about the same period.
The following changes across the three studies are worth noting. First, the proportion of women in methadone treatment increased steadily from 22 percent in the DARP studies to 39 percent in the DATOS studies. Second, the proportion of African-Americans decreased from 58 percent in DARP to 28 percent in DATOS; the proportion of Hispanics grew from 10 percent in DARP to 24 percent in DATOS; and the percent of those who are white has increased by approximately nine years across the three studies, and the proportion of patients over 30-years-old reached 80 percent in the DATOS studies. In the DARP studies the average years addicted for methadone admissions was 9–10; this rose to 13 by the early 1990s (i.e., by the time of the DATOS studies). The proportion receiving previous treatment was approximately 50 percent during the DARP period, a rate which rose to about 75 percent for the subsequent study periods. Similarly the proportion with three or more treatments was only 13 percent for DARP, increasing to 44 percent and 40 percent for the subsequent two studies respectively. The percentage of admissions with prior incarceration histories remained in excess of 50 percent, and the percentage under legal supervision at program entry varied but represented a significant minority over all three study periods, as did the level of criminal involvement among patients. The percentage of employed patients dropped somewhat from the DARP period to the subsequent two study periods, demonstrating the marginal employability of more recent methadone admission populations. Cocaine use was 25–35 percent of the admission population in the DARP and TOPS studies and nearly 50 percent of the DATOS admissions. Marijuana use as a secondary drug problem declined in recent study periods, as did use of alcohol.
The similarity in the patient characteristics across the three series of studies is quite striking. Generally, patients entering methadone maintenance treatment are dysfunctional in a number of behavioral domains, show long
histories of chronic addiction, have serious involvement with the criminal justice system, and typically access treatment repeatedly after their first episode is complete.
Current Patient Characteristics
As of December 1993, there were 759 methadone maintenance programs in the United States (FDA tabulation). These programs typically maintain a census of some 115,000 patients. Only one national data base, the Client Data System mentioned above, which is maintained by SAMHSA's Office of Applied Studies, contains information of definitive patient characteristics, and the data collected are limited. Even so, the CDS provides a great deal of information about the annual number of admissions. However, its data are more complete for publicly funded treatment programs than for private, proprietary programs; comprehensive information about all treatment programs is not available at this time. Similar limitations characterize the California Alcohol and Drug Data System, whose data are used in further discussions below.
The CDS is based upon admissions data on methadone patients in treatment programs as reported by 31 of the 42 reporting states.1 (During 1992, as discussed earlier and shown on Table 3-2, 26 states reported admission for methadone maintenance treatment. Reports and numbers of admissions for detoxification treatment are counted separately. See further discussion below.) This data base offers some information about the age, sex, and race of patients upon entry into a treatment program, and allows discovering regional differences. However, in any one year a single patient may have more than one admission reported to CDS. To reduce the error introduced by counting patients multiple times, admissions designated as transfers are excluded from consideration. Still, patients may drop out of a program and later return for a new episode of treatment in the same or a different program. Data are presented below in three areas: first, any admission to methadone treatment; second, methadone detoxification; and, finally, methadone maintenance.
TABLE 3-2 Methadone Maintenance Patient Characteristics as Percentage Occurrences Within Programs, 1969–1993
|
Characteristic |
DARP, 1969–1973 (N = 11,023; 34 programs) |
TOPS, 1969–1973 (N = 4,184; 17 programs) |
DATOS, 1969–73 (N = 1,540; 29 programs) |
CDS (1992) (N = 41,509; 26 states reporting) |
|
Female |
22 |
32 |
39 |
36 |
|
African-American |
58 |
37 |
28 |
33 |
|
Hispanic |
25 |
21 |
24 |
27 |
|
White |
15 |
20 |
25 |
25 |
|
Mean agea |
28 |
31 |
37 |
— |
|
Over 30-years-old |
30 |
40 |
80 |
79 |
|
High school graduate |
37 |
48 |
64 |
69 |
|
Ever married |
46 |
56 |
69 |
51 |
|
Prior incarceration |
50 |
80 |
63 |
— |
|
Years addicteda |
9–10 |
12 |
13 |
— |
|
3 or more prior treatments |
13 |
44 |
40 |
36 |
|
Court referred |
7 |
3 |
2 |
6 |
|
On legal supervision (preinterview) |
30 |
18 |
21 |
— |
|
Characteristic |
DARP, 1969–1973 (N = 11,023; 34 programs) |
TOPS, 1969–1973 (N = 4,184; 17 programs) |
DATOS, 1969–73 (N = 1,540; 29 programs) |
CDS (1992) (N = 41,509; 26 states reporting) |
|
Employed |
36 |
24 |
16 |
21 |
|
Criminal activity |
47–52 |
33 |
48 |
— |
|
Cocaine useb |
<34 |
28 |
42 |
52 |
|
Marijuana useb |
<55 |
55 |
18 |
Court referred |
|
NOTE: DARP = Drug Abuse Reporting Program; TOPS = Treatment Outcomes Prospective Studies; DATOS = Drug Abuse Treatment Outcome Studies; CDS = Client Data System maintained by SAMHSA's office of Applied Studies (OAS). a Data in this row are mean years. b Reported as secondary drug problem. SOURCE: Sampson et al. (1976) (DARP); Hubbard et al. (1989) and Flynn et al. (1994) (TOPS and DATOS); special computer runs by SAMHSA-OAS (CDS). |
||||
Methadone in Drug Treatment: General
Overall, in fiscal year 1992, 97,519 admissions for both detoxification and methadone maintenance were reported by 31 of the 42 reporting states as having been assigned to receive methadone as part of treatment.2 Although methadone maintenance is the treatment for persistent opiate dependence with the best evidence of effectiveness, it appears to be infrequently utilized in many states treatment systems. Even in those states where such programs exist, the utilization of methadone treatment by opiate-dependent individuals varies dramatically. Five of the reporting jurisdictions (California, District of Columbia, New Jersey, New York, and Rhode Island) predominate in the methadone maintenance treatment data, each accounting for more than 10 percent of the nation's methadone treatment admissions. Eight states reported fewer than 100 admissions. Nationally, admissions to methadone maintenance or detoxification were 64 percent male, and 46 percent were white, 12 percent African-American, and 38 percent Hispanic. The modal ages were 35 to 44 years of age (44 percent of admissions). Among the 23 states reporting at least 100 admissions, 47 percent of those admitted had three or more prior treatment episodes, and 42 percent reported that cocaine was a secondary substance of abuse.
Of particular interest are the differences between states in the treatment settings that use methadone. For example, in the state of Pennsylvania, 26 percent of admissions for treatment utilizing methadone occurred in hospital inpatient detoxification settings, a considerably greater percentage than in New York and Texas, where only 10 percent and 14 percent, respectively, of admissions were for inpatient detoxification. Most other states appeared not to use methadone in inpatient or residential settings at all. Minnesota is an exception; there, methadone was used extensively in residential settings (68 percent of admissions—19 percent hospital-based, 49 percent nonhospital). Generally, methadone is provided in ambulatory outpatient settings, but states differ significantly here as well. All of Connecticut's methadone admissions were into intensive outpatient programs, as were 32 percent of admissions in Minnesota and 10 percent in North Carolina. Most other states, however, reported that nonintensive outpatient services only were utilized, or that outpatient detoxification services were utilized. In this last regard, state policies again differed. For example, in California, 81 percent of all methadone admissions were to outpatient detoxification programs and only 17 percent
were to methadone maintenance programs. This pattern was also true in Hawaii (78 percent and 17 percent). By contrast, 97 percent of admissions in Illinois were to methadone maintenance programs, as were 88 percent in the District of Columbia, and 82 percent in New York. These figures highlight the variation in the use methadone treatment across states (see also chapter 6).
Use of Methadone in Detoxification
Of the 42,615 admissions to detoxification treatment reported by 12 states in fiscal year 1992, the great majority (86 percent) were in California. New Jersey accounted for 10 percent and Maryland for 2 percent. No other state reporting to the CDS had more than 300 admissions for detoxification. Of the nationwide admissions for detoxification treatment, 65 percent were male; 43 percent were white, 18 percent African-American, and 35 percent Hispanic. The high percentage of Hispanic admissions probably reflects the domination of the detoxification figures by the California data. Forty-three percent were between 35 and 44 years of age.
Use of Methadone in Maintenance Treatment
The 41,509 admissions reported by 26 states for methadone maintenance also showed a different distribution by state. In fiscal year 1992, New York led with 33 percent of the total, followed by California with 19 percent, New Jersey with 8 percent, Massachusetts with 7 percent, and the District of Columbia with 6 percent. No other state reported more than 2,500 admissions, with a range of 7 to 2,409.
The gender distribution was similar to that seen in detoxification admissions, with males accounting for 64 percent. The ethnic breakdown was somewhat different: 38 percent white, 33 percent African-American, and 27 percent Hispanic. As with detoxification admissions, 46 percent were between 35 and 44 years of age.
Contrast between Detoxification and Maintenance Patient Admissions
Characteristics of detoxification and maintenance patient admissions are similar, except in the following areas: There are more repeaters among those detoxified, where 42 percent reported 5 or more prior treatment episodes compared to 19 percent for methadone maintenance admissions.
Referrals by the criminal justice system account for a smaller proportion of detoxification admissions (1 percent) than of maintenance (6 percent). In
fact, referrals to detoxification are almost entirely self-referrals (93 percent). More of those admitted for detoxification than for maintenance reported injection as the primary route of administration (91 percent versus 74 percent). Inhalation is reported by only 8 percent of those admitted for detoxification admissions compared with 24 percent of those admitted for maintenance (probably because New York and New Jersey provide maintenance treatment to large numbers of addicts and it is in these two states where inhalation, or snorting, is on the rise).
Nearly all persons admitted for detoxification (98 percent) are daily users of opiates compared to 85 percent of maintenance admissions. Forty percent of those admitted for detoxification report secondary substance abuse, and 30 percent report cocaine use. Among those admitted for maintenance, the corresponding figures are 57 percent and 52 percent. Persons admitted for maintenance treatment report more psychiatric problems (7 percent) than those admitted for detoxification (1 percent). More women admitted to maintenance treatment are pregnant (10 percent) than are women admitted to detoxification (1 percent).
Only about one-third of methadone patients are currently employed, whether admitted to detoxification or maintenance treatment. Finally, while more of those admitted for maintenance than for detoxification admissions have been married (61 percent versus 39 percent), only one in five in either group is currently married.
To provide more detailed information on the use of methadone in maintenance treatment, we present data from two states with large maintenance populations, New York and California.
Maintenance Patients in New York State; 1992
Some one-third of the methadone maintenance treatment population of the United States is in New York State programs. The census of patients in these programs as of January 1, 1992, was 39,340; two-thirds were male.
Unlike the general addict population, two-thirds of these methadone patients were over age 35. As of January 1994, the mean age of the treated population was 39.5 years—39.6 for males and 36.9 for females.
Heroin use generally began during their teens. Fifty-seven percent reported beginning heroin use by age nineteen; 20 percent started use by age fifteen. Conversely, less than 10 percent reported starting heroin use after age twenty nine.
With regard to race-ethnic status, these New York State male methadone patients were almost evenly composed of three groups: African-American (27 percent); Hispanic (36 percent); and white (35 percent). The distribution
among female patients was still more evenly balanced: African-American (34 percent); Hispanic (34 percent); and white (31 percent).
Almost all (96 percent) of the patients in methadone maintenance programs in New York State reported that heroin was their primary drug of abuse before treatment. Interestingly, unlike any other state, almost a thousand patients reported that street methadone was their chief drug of abuse prior to treatment; use of street methadone, then, accounted for some 3 percent of admissions.
Data concerning route of drug administration for the 1992 New York State active treatment population (approximately 30,000) indicate that intravenous use (injecting) has declined from prior years. (NIDA has established the following routes of administration for minimum data set purposes: oral, smoking, inhalation (snorting), injection, and other.) Of the male methadone maintenance patients, 74 percent reported at admission that injecting was their common route of use, 24 percent reported inhalation (snorting), and 2 percent reported other routes (oral, smoking, other). The females, however, were less likely than the males to be intravenous drug users: among female patients, 66 percent reported injecting, 24 percent inhalation, and 15 percent other routes. In both sexes, primarily intravenous use has notably declined in the past several years, from 82 percent of admissions in 1986 to 57 percent in 1992 (approximately 11,000).
In addition to a long history of opiate abuse, most of these methadone maintenance patients have abused other drugs as well. Overall, the secondary drugs of abuse for males and females were quite similar; over half of both male and female patients report cocaine use.
Most (75 percent) of the methadone maintenance patients in treatment in New York State had one or more prior treatments for drug abuse. These prior treatments included detoxification and therapeutic communities, as well as methadone maintenance and other modalities.
Maintenance Patients in California, 1992
The California Alcohol and Drug Data System (CADDS) contains data from all methadone treatment programs except those in Department of Veterans Affairs hospitals. The system includes the data required for reporting to CDS (see discussion above) as well as other information collected for state use. California limits the number of methadone detoxification slots, and limits Medi-Cal reimbursement to a maximum of 21 days per detoxification treatment episode. Admissions for methadone detoxification during calendar year 1992 were 30,981 for men and 15,924 for women. Discharges were 30,806 and 15,826, respectively, resulting in a January 1, 1993, census of 1,209 men and
666 women. (These treatment census figures are substantially below the licensed detoxification capacity due to lags in reporting by some large counties.)
In California, detoxification patients are similar to maintenance patients, except they are more often male. Women admitted to detoxification report pregnancy less often than those admitted for maintenance. Detoxification admissions report fewer prior treatment episodes than do maintenance admissions. The differences are due, in part, to state regulations that require at least two prior treatment failures for maintenance admissions, but not for detoxification admissions. In addition, high rates of prior treatment among those admitted for detoxification are partly explained by the way treatment is reimbursed in California. Although limited in length, detoxification is fully reimbursed (i.e., no copayment) by Medi-Cal for the majority of admissions, while maintenance treatment is reimbursed only in specific cases, such as pregnant women, HIV-positive patients, and limited other groups.
As of January 1, 1992, there were 15,896 patients being served by California methadone maintenance programs. This group was 57 percent male, for whom the average age was 38.7 years with three-fourths being age 33 or older. For females, the average age was 34.9 years with three-fourths being age 30 or older. Whites made up the largest proportion of clients for both males (53 percent) and females (61 percent), while Hispanics made up the next largest proportion (35 percent for males and 26 percent for females). African-Americans constituted the vast majority of the remaining admissions.
The majority of clients were ''self-referred'' into treatment: 83 percent of males and 78 percent of females. Referrals from alcohol/drug programs or from the court/criminal justice system accounted for just under 10 percent each for both males and females. Approximately 20 percent of both males and females had some type of involvement with the criminal justice program at the time of admission. One-third of the males and 41 percent of females had less than 12 years of education. Employment (including part time) was 13.6 percent among males and 7.1 percent among females.
Finally, as is to be expected because current state regulations require at least two treatment failures before maintenance admission, except for emergency admissions, which require no prior treatment failures, only 1 percent of the males and 1.8 percent of the females reported no prior treatment. This is in contrast to New York methadone maintenance patients, 25 percent of whom have reported no prior treatment.
Nearly all methadone maintenance clients claimed heroin as their primary drug (98 percent for both males and females), and injection as the main route of administration (about 96 percent) for both. A large proportion were daily users (85.9 percent and 82.9 percent for males and females, respectively). A very small proportion of the sample reported street methadone as their main
drug (0.2 percent for both males and females). The average age of first opiate use was 20.9 for males and 21.5 for females, with half of the males beginning use on or before age 19 and half of the females beginning use on or before age 20.
Just over half of the males and about three-fifths of the females were using cocaine as a secondary drug, with over half using it on a daily basis. Of those using cocaine, 12.2 percent of the males and 18.6 percent of the females were using crack. Alcohol was the next most popular secondary drug of abuse among males (24.4 percent) and females (16.8 percent).
Differences Between New York and California
The previous paragraphs described in detail the methadone maintenance data for the two states that together serve the majority of methadone maintenance patients in the United States. The data from New York and California allow some summary data to be extracted which highlight the differences between the two systems. Although the specific data are informative, a contrast of some overall system parameters indicates the extent to which state and local government policy affects treatment availability, utilization, and outcome.
Table 3-3 shows the most recent data available for both states with respect to their methadone maintenance patient census as of January 1 in 1992 and 1993; their rates of admission and discharge during the year; the percentage of system growth over the year; and the rate of patient movement into and out of treatment, measure as a "turnover rate" (calculated by dividing the total 1992 discharges by the January 1, 1992, patient census).
Before discussing specific differences, a comparison of each state's overall government policies toward methadone is informative. New York State, particularly New York City, has been troubled by heroin addiction since World War II, and has the longest history of comprehensive government-sponsored interventions to address the problem. New York State and its local governments subsidize the majority of methadone maintenance treatment programs and have few restrictions on dosing or duration of treatment.
It was in New York City that the pioneering research of Dole and Nyswander (see, e.g., Dole and Nyswander, 1965) established methadone maintenance as a legitimate pharmacotherapy for opiate addiction in the mid-1960s. New York's practitioners probably accept to a larger extent than those in other states the proposition that relatively high doses of methadone are required to provide a blockade against the euphoria provided by heroin. Methadone providers in New York tend to subscribe to a blockade model of maintenance, in which the methadone dose is increased until it prevents
withdrawal symptoms for a full 24-hour period, rather than being limited to preset maximum dose. Finally, in New York, detoxification is viewed as a short-term intervention, typically necessary where there are medical complications or mixed addictions present. In general, it is seen there as an adjunct to treatment and is not regarded as a desirable or reasonable alternative to long-term methadone maintenance.
California did not establish methadone maintenance programs until the early 1970s. The first state oversight agency, the Research Advisory Panel (RAP), viewed methadone as appropriate for detoxification but regarded methadone maintenance as a "treatment of last resort." This view continued under the Department of Alcohol and Drug Programs, which assumed administrative responsibility later in the 1970s, and led to an emphasis during the 1980s on low-dose treatment of limited duration. The majority of methadone providers in California during the 1970s and 1980s maintained average dose levels of around 40 mg, a level considerably under the 60 mg average recommended by NIDA. More recently, state dosing policies have changed, so that by early 1994, only 18 percent of patients received a dose under 40 mg, some 28 percent received doses between 40 and 59 mg, about 45 percent received doses between 60 and 80 mg, and about 8 percent were on doses greater than 80 mg.
Independently, as local government budgets were constrained in 1976 and thereafter as a result of Proposition 13, many California counties began to withdraw their subsidy of methadone maintenance treatment programs. By the mid-1980s, the majority of methadone treatment funds were provided out-of-pocket by clients' fees (see chapter 6). However, for several years California has subsidized methadone treatment for addicted women who are pregnant or postpartum, for addicts who are HIV-positive patients, and for certain other specified groups of addicts.
The results of these state policies are evident in the data discussed above and highlighted in Table 3-3. First, many more opiate addicts receive methadone maintenance in New York than in California. Second, the California emphasis on subsidized treatment for pregnant and postpartum addicts has resulted in women making up 43 percent of the January 1, 1992, patient census in that state, compared to only 34 percent of the census in New York State. Finally, a comparison of the censuses for January 1, 1992, and January 1, 1993, indicates that while New York increased methadone treatment slots by 6 percent, California increased its slots by about 1 percent. Furthermore, the turnover of maintenance slots in California (number of discharges in 1992 divided by the January 1, 1992 census) is more than twice that of New York, even when discharge numbers are reduced by removing "satisfactory discharges" and inter-program transfers.
TABLE 3-3 California and New York Methadone Maintenance Patient Flow in 1992
|
|
California |
New York |
||||||||||
|
|
Males |
Females |
Total |
Males |
Females |
Total |
||||||
|
|
N |
% |
N |
% |
N |
% |
N |
% |
N |
% |
N |
% |
|
January 1992 Census |
9,024 |
56.8 |
6,872 |
43.2 |
15,896 |
100 |
26,088 |
66.3 |
13,252 |
33.7 |
39,340 |
100 |
|
Admissions |
7,592 |
57.0 |
5,936 |
43.0 |
13,328 |
100 |
9,657 |
68.7 |
4,400 |
31.3 |
14,057 |
100 |
|
All Discharges |
6,822 |
57.0 |
5,139 |
43.0 |
11,961 |
100 |
8,007 |
68.7 |
3,642 |
31.3 |
11,649 |
100 |
|
January 1993 Census |
9,095 |
56.6 |
6,988 |
43.4 |
16,083 |
100 |
27,692 |
66.4 |
13,987 |
33.6 |
41,679 |
100 |
|
Growth |
71 |
0.8 |
116 |
1.7 |
187 |
1.2 |
1,604 |
6.2 |
735 |
5.6 |
2,339 |
6.0 |
|
Uncorrected Turnover |
— |
75.0 |
— |
73.5 |
— |
74.4 |
— |
30.7 |
— |
27.5 |
— |
29.6 |
|
Satisfactory discharge |
510 |
7.5 |
437 |
8.5 |
947 |
7.9 |
541 |
6.8 |
250 |
6.9 |
791 |
6.8 |
|
Transferred |
716 |
10.5 |
862 |
16.8 |
1,578 |
13.2 |
946 |
11.8 |
552 |
15.2 |
1,498 |
12.9 |
|
Turnover |
|
67.7 |
|
62.2 |
|
65.3 |
|
.271 |
|
.233 |
|
.258 |
|
Turnover |
|
62.0 |
|
55.9 |
|
59.4 |
|
.250 |
|
.214 |
|
.238 |
|
SOURCES: California Department of Alcohol and Drug Programs; New York State Office of Alcoholism and Substance Abuse Services. |
||||||||||||
Although New York and California, respectively, treat the largest number of opiate addicts, they differ in the number of patients served, the number of women in treatment, the type of treatment provided and subsidized, and dosing policies. These differences are due to individual state philosophies, policies, and regulations, which are also reflected in general differences in public subsidies. These state differences suggest a useful research opportunity to study the consequences of alternative financing and regulatory approaches to methadone maintenance, the results of which could inform the drafting of new regulations or clinical practice guidelines.
Summary
This chapter presents data that show that heroin use occurs, along a continuum including those who have ever used opiates, those who ever become dependent on opiates, those who become addicted, and those who are treated for addiction. However, no effort has been made to estimate the size of the heroin addict population, even though this figure is of great interest to policymakers.
There is considerable uncertainty about the size of the heroin addict population. Almost all analysts believe the total number of heroin addicts to be at least 500,000, though estimates that range up to one million are sometimes mentioned. A committee of the National Research Council (NRC) in 1989 analyzed the estimates of the prevalence of intravenous drug use (IVDU), which is dominated by heroin use. B.D. Spencer, who was asked by the NRC committee to evaluate the accuracy of the IVDU estimates, concluded: "The accuracy of the estimates of the number of [users] is not objectively ascertainable, but the estimate (of about 1 million) could well be off by a factor of 2; that is, the true number could conceivably be smaller than 500,000 or greater than 2 million. The closeness of several of the estimates is not persuasive because they cannot be regarded as independent estimates" (Spencer, 1989).
Reuter (1993) reviewed the literature regarding the prevalence of heroin addiction and concluded: "Since the HPI [Heroin Problems Index]-based estimate in 1981, there has been only one formal estimate of the number of heroin addicts nationally (Cooley et al. 1990), which used DAWN's [Drug Abuse Warning Network's] heroin-related ER mentions to produce a figure of 853,000 for 1987. This number, developed by an adaptation of the HPI technique, has not acquired much authority; the sensitivity to highly uncertain anchor city estimates is probably the primary reason."
Gerstein and Harwood (1990) estimated the population of all drug users clearly in need of treatment at 1.5 million. They did not make a separate estimate of heroin addicts in need of treatment.
The lower range of the estimates of the total addict population does not appear to be in question. The figure is high enough to make the point that the estimated 115,000 methadone patients in maintenance treatment is modest relative to the size of the addict population.3
References
Anglin, MD, and McGlothlin, WH. 1985. Methadone maintenance in California: A decade's experience. In: L. Brill and C. Winick (eds.), The Yearbook of Substance Use and Abuse. Vol. 3. New York: Human Sciences Press.
Anthony, JC, Warner, LA, and Kessler, RC. 1994. Comparative epidemiology of dependence of tobacco, alcohol, controlled substances, and inhalants: Basic findings from the National Comorbidity Study. Clinical and Experimental Psychopharmacology. (in press.)
Anthony, JC, and Helzer, JE. 1991. Syndromes of drug abuse and dependence. In: L. N. Robins and D. A. Regier (eds.), Psychiatric Disorder in America. New York: The Free Press.
Ball, JC and Greberman, SB. 1994. Lifetime arrest rates of heroin addicts in Baltimore. In: Problems of Drug Dependence, 1993: Proceedings of the 55th Annual Scientific Meeting of the College on Problems of Drug Dependence, L.S. Harris, ed., Vol. 2: Abstracts. NIDA Research Monograph 141, Rockville, Md. P. 42.
Ball, JC, and Ross, A. 1991. The Effectiveness of Methadone Maintenance Treatment: Patients, Programs, Services, and Outcomes. New York: Springer-Verlag.
Biernacki, P. 1986. Pathways from Heroin Addiction: Recovery Without Treatment. Philadelphia: Temple University Press.
Courtwright, DT. 1982. Dark Paradise: Opiate Addiction in America Before 1940. Cambridge, Mass.: Harvard University Press.
Dole, VP, and Nyswander, M. 1965. A medical treatment for diacetylmorphine (heroin) addiction. Journal of the American Medical Association. 193:80–84.
Fiorentine, R, and Anglin, MD. 1993. Perceiving need for drug treatment: A look at eight hypotheses. Unpublished manuscript. Los Angeles: University of California, Drug Abuse Research Center.
Flynn, PM, Craddock, S, Gail, MS, Luckey, JW, and Hubbard, RL. 1994. Client Characteristics Among Admissions to Methadone Treatment Programs in Two National Samples: 1979–981, 1991–993. Research Triangle Park, NC.
General Accounting Office. 1990. Methadone Maintenance: Some Treatment Programs Are Not Effective; Greater Federal Oversight Needed. Washington, D.C.: U.S. Government Printing Office.
Gerstein, Dr, and Harwood, HJ (eds.). 1990. Treating Drug Problems . Vol. I Washington, D.C.: National Academy Press.
Hser, Y, Anglin, MD, and Powers, K. 1993. A 24 year follow-up of California narcotics addicts. Archives of General Psychiatry 50:577–584.
Johnston, LD, O'Malley, PM, and Bachman, JG. 1993. National Survey Results on Drug Use from the Monitoring the Future Study, 1975–1992 . Vol. 2 College Students and Young Adults. Rockville, Md. National Institute on Drug Abuse.
Musto, DF. 1973, 1987. The American Disease: Origins of Narcotic Control. New York: Oxford University Press.
National Institute on Alcohol Abuse and Alcoholism. 1994. Eighth Special Report to the U.S. Congress on Alcohol and Health. NIH Publication No. 94-3699. Rockville, Md. NIAA, DHHS.
O'Donnel, JA, Voss, HL, Clayton, RR, Slatin, GT, and Room, R. 1976. Young Men and Drugs: A Nationwide Survey. NIDA Research Monograph 5, DHEW Publication No. (ADM) 76-311, Washington, D.C.
Reuter, P. 1993. Prevalence estimation and policy formulation. Journal of Drug Issues 23(2):167–184.
Rhodes, P. 1993. Synthetic estimation applied to the prevalence of drug use. Journal of Drug Issues 23(2):297–322.
Rittenhouse, JD. 1977. The Epidemiology of Heroin and Other Narcotics . NIDA Research Monograph 16, Rockville, Md.
Robins, LN. 1974. The Vietnam Drug User Returns. Special Action Office Monograph, Series A, No. 2. Washington, D.C.: U.S. Government Printing Office.
Robins, LN, and Murphy, GE. 1967. Drug use in a normal population of young Negro men. American Journal of Public Health 57:1580–1596.
Simpson, DD, Joe, GW, Lehman, WEK, and Sells, SB. 1986. Addiction careers: Etiology, treatment, and 12-year follow-up procedures. Journal of Drug Issues 16:107–121.
Simpson, DD, and Savage, LJ. 1980. Treatment re-entry and outcomes of opioid addicts during a four-year follow-up after drug abuse treatment in the United States. Bulletin on Narcotics 32(4):1–10.































