9
A Dental Work Force for the Future
What characteristics should the dental work force of the twenty-first century have? Do we now have or are we facing an oversupply or undersupply of dental personnel and services? Anxiety about these issues played a major role in the birth of this study, and the "supply question," as the committee came to call it, was a continuing theme in the public hearing, site visits, and other committee activities. As examined in this chapter, the supply question has several elements. How many dentists and allied dental professionals does the country now have, and what numbers are projected for the future? What will the demand and need for dental services be in the future, and how certain are the answers? Are the composition and distribution of the dental work force satisfactory? Should enrollments in dental schools be increased, decreased, or held steady? The last question was a particular concern of community practitioners and dental society leaders, who referred often to a perceived "busyness" problem (more accurately, the lack of busyness) that resulted from the training of too many dentists after dental schools increased enrollments during the 1970s.
This chapter reviews work force trends and projections for dental practitioners and examines the strengths and limitations of models for work force forecasting. It assesses prospects for an over- or undersupply of dental services and personnel and makes recommendations about work force policies. The chapter is pre-
raised on the principle stated in Chapter 1 that a qualified dental work force is a valuable national resource. Its future is too important to be determined solely by the isolated decisions of individual universities and states.
Earlier sections of this report have also touched on work force issues. Chapter 2 briefly reviews the shift from the 1960s to the 1980s from concerns about an undersupply of dental practitioners to worries about an oversupply. Expansionist policies were adopted and then abandoned in favor of policies of neutrality or contraction. One legacy of the policy turnaround is a set of structures and processes for collecting work force and other data and forecasting future supplies and requirements for dental and other health professionals and services.
Chapter 5 discusses the oral health research work force and notes the shortage of qualified researchers. It cites the recent report of the Office of Science and Engineering Personnel of the National Research Council. That report concluded that at least 200 graduates per year were needed to meet the need for oral health researchers, and it noted that this is roughly four times the current production. The recommendation in Chapter 4 for an increase in the number of general dentistry residencies was intended not to increase the supply of generalists but rather to improve their qualifications.
Work Force Trends and Projections
Dentists
Numbers and Projections
More than 140,000 dentists are in active practice in the United States, and the ratio of dentists to population currently stands at approximately 56:100,000 persons. Forecasts of the numbers of dentists are generally consistent in predicting that the absolute number of dentists in the United States will peak around the year 2000 and then level off before beginning a gradual decline (AADS, 1989; ADA, Bureau of Economic and Behavioral Research, 1991; USDHHS, PHS, 1992). These projections are depicted in Figure 1.2 in Chapter 1. Because the U.S. population continues to grow, the ratio of dentists to the general population will drop earlier and more sharply, falling by 2010 to a estimated level of less than 50:100,000 (or approximately 2,000 people per dentist).
The projections in the dentist work force reflect the combined effect of the retirements of dentists trained in peak enrollment years
and the reduced enrollments of more recent years. As reported earlier, six schools have closed during the last several years, and a majority of the remaining schools have cut enrollments. According to one reckoning, the total enrollment decrease is equivalent to the closure of 20 average-sized dental schools (Consani, 1993).
The cuts in dental school enrollments have primarily affected the supply of generalist dentists. The number of specialty training positions has not increased absolutely, but the ratio of such positions to dental school graduates has increased. Thus, the proportion of dentists who are specialists is projected to increase from about 15 percent in 1985 to more than 25 percent by the second decade of the next century. Despite this growth, general practice still prevails in dentistry, in sharp contrast to the situation in medicine in which more than two-thirds of all physicians are specialists (Kindig et al., 1993).
In its survey of deans, the committee found that three-quarters of those surveyed felt that the supply of dentists today is about right. However, nearly two-thirds believed that the country would be undersupplied with dentists in 15 years (Table 9.1). A majority of respondents reported that the supply of dental hygienists and formally trained dental assistants was too low currently and pro
TABLE 9.1
Deans' Responses to Supply Questions in Institute of Medicine and American Association of Dental Schools Survey
|
For the following questions, please indicate your opinion. |
||||
|
Too Low |
About Right |
Too High |
Not Sure |
Question |
|
7 |
42 |
3 |
2 |
The supply of dentists in the U.S. today is ______. |
|
34 |
16 |
2 |
1 |
The supply of dentists in the U.S. 15 years from now is likely to be _______. |
|
4 |
7 |
0 |
3 |
The supply of dental hygienists in the U.S. today is ________. |
|
38 |
8 |
1 |
5 |
The supply of dental hygienists in the U.S. 15 years from now is likely to be ________. |
|
39 |
7 |
0 |
7 |
The supply of formally trained dental assistants is ________. |
|
34 |
16 |
2 |
1 |
The supply of formally trained dental assistant and dental hygienists in the U.S. 15 years from now is likely to be ________. |
|
SOURCE: Institute of Medicine and American Association of Dental Schools, 1994. |
||||
jected that the supply of these allied personnel would be too low in the year 2008.
Regional Variations and Shortage Areas
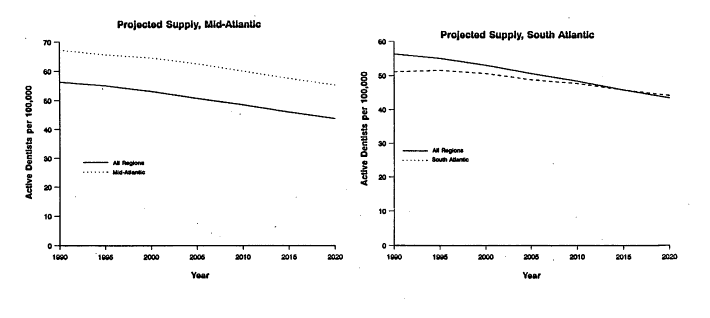
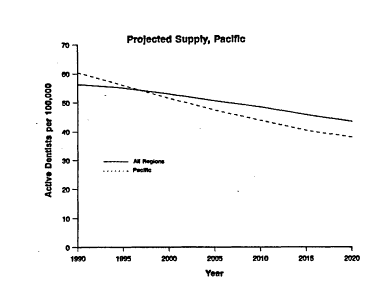
Regional data show considerable variation in dentist-to-population ratios. Figure 9.1 shows trends for three regions. For the New England and the Middle Atlantic regions, the number of active dentists per 100,000 population is projected to remain 10 to 15 dentists more than the national average through 2020, although each ratio is declining (AADS, 1989). In contrast, the dentist-to-population ratio for the Pacific region is expected to move from above to below the national average by the turn of the century while the ratio for the South Atlantic is expected to rise to the national average by 2010. Variations across and within states are even greater than regional variations. In 1993, Alabama had 41 dentists per 100,000 population whereas Connecticut had 75 per 100,000 (or 2,439 persons per dentist in Alabama and 1,370 in Connecticut).
In FY 1993, 1,069 areas were designated as dental health professional shortage areas, and these areas collectively were short 2,087 full-time equivalent dentists (J. Rosetti, personal communication to M. Allukian, April 4, 1994). The Department of Health and Human Services has defined a shortage area as one with a ratio of 5,000 or more people per dentist. It has defined 3,000 people per dentist as a target.
A recent U.S. General Accounting Office (GAO) study found that health professional shortage areas in urban counties report greater needs for full-time general dentists (GAO, 1994) whereas those in rural counties have a greater need for part-time positions (GAO, 1994). Many rural shortage areas would move off the shortage list if they added less than half of a full-time position. Recruiting individuals for part-time practice in shortage areas is, however, particularly difficult.
Composition of Work Force
Dentistry used to be a profession of white males, but that is changing. The proportion of women in the dental work force has grown dramatically since women began entering dental schools in substantial numbers in the 1970s. In 1970, 2 percent of first-year dental students were female compared to 38 percent in 1990. Although only about 10 percent of all dentists are female, nearly 20
percent of those under age 40 are female (ADA, CYP, 1992). With its relatively predictable and manageable work week, attractive financial returns, and moderate length of professional training (compared to medicine), dentistry has many attractions for women interested in both career and family. One drawback is state licensing requirements that complicate interstate moves for two-career couples. As noted in the preceding chapter, such requirements may make it more difficult for dentists to relocate to shortage areas.
The picture for unrepresented racial and ethnic minorities is less encouraging than it is for women. Another Institute of Medicine committee has defined underrepresented racial and ethnic minorities as African-Americans, Hispanics, and Native Americans-groups that are both underrepresented and characterized by a group history of deprivation (IOM, 1994b). Although incomplete American Dental Association (ADA) data on race and ethnicity suggest that perhaps 10 percent of all dentists and 30 percent of dentists under age 40 are minorities, underrepresented minorities make up less than half of this younger group (which is 30 percent Hispanic and 13 percent African-American) (ADA, CYP, 1992).
Since 1971, first-year African-American enrollments in dental school have stayed relatively steady, whereas Asian enrollments have increased substantially and Hispanic enrollments, modestly. As a result, African-Americans now represent less than 25 percent of minority enrollment compared to more than 50 percent in the early 1970s. Attrition rates for African-Americans are approximately twice the rates for whites and Hispanics (ADA, CYP, 1992). According to a 1994 report, African-Americans have not achieved overall population parity in dental school enrollments but are closer to educational parity (GAO, 1994). Population parity compares the percentage of African-Americans in dental schools to the group's percentage of the total population. On a population basis, African-American dental school graduates stood at 37 percent of parity for dental school graduates in 1991 compared 34 percent in 1980. (Full parity equals 100 percent.) Educational parity compares the percentage of the group in dental school to its percentage of the population of college graduates. For dental graduates, the educational parity figures for African-Americans stood at 80 percent in 1991 versus 76 percent in 1980, but for first-year enrollments, the comparable figures were 113 versus 93 percent, respectively. These figures underscore the importance of the strategies described later in this chapter for increasing the pool of college-educated minorities.
Work Force Requirements
Most dental work force models focus only on the supply of practitioners. The econometric model developed by the federal government's Bureau of Health Professions attempts to project prices and utilization, but it does not generate a specific comparison of future supply against future demand (or need) to generate an explicit projection of work force requirements. The background paper by Capilouto et al. notes that the model did not do well in predicting precise dentist supply requirements necessary to maintain stable prices.
The committee did not find specific quantitative projections of population ''requirements" for dental personnel similar to those that have been developed for the physician work force (Feil et al., 1993; Wennberg et al., 1993; Weiner, 1994). This analytic disparity presumably reflects the greater concern of analysts and policymakers about a physician work force that is—compared to the dental work force—much larger, much more specialized, more expensive, and more routinely involved in more diverse practice sites and organizational systems; Most assessments of the physician work force point to a probable aggregate oversupply of physicians, particularly specialists, and most proposals for health care reform would shift the emphasis in medical education from specialists to generalist physicians (Feil et al., 1993; PPRC, 1994). Although there is argument on this point, some believe that the projected supply of generalist physicians is adequate to meet expected demands for care (if there is a continued move to health plans that limit the number of participating physicians) but that the supply of specialists is considerably in excess of what is needed (Weiner, 1994).1 Proposals to limit the
number or proportion of specialist residency positions have provoked considerable controversy.
In dentistry, aggregate work force planning focuses more on predoctoral enrollments than on residency positions. Moreover, most of the concern about residencies focuses on increasing the number of general dentistry positions rather than cutting the absolute number of specialist positions or specifying a percentage split between generalist and specialist positions. One concern in assessing the adequacy of supply to meet requirements for oral health services is the work load of practitioners. ADA survey data (1992f) indicate that the average general dentist works 48 weeks a year and spends an average of 37 hours per week in practice (33.6 hours treating patients). The average appointment wait time was about seven days. One ADA analysis suggests that less than two-thirds of available "capacity in dentistry" has been used in recent years. That number was derived by assuming that all dentists could provide the volume of service provided by the top quartile of dentists (ADA, 1993a).
Similarly, a study comparing educational costs and incomes for professionals reported fewer hours worked annually for dentists than for primary care and procedure-based specialty physicians, lawyers, and business people with M.B.A. degrees (Weeks et al., 1994). For example, for professionals aged 36-45, annual hours worked were 1,613 for dentists (patient care hours only, generalists and specialists); 1,893 for lawyers; 2,520 for business people; 2,674 for primary care physicians (patient care only); and 2,730 for specialists (patient care only). Differences in data definitions and sources undoubtedly account for some of this variation, and professional interpretations of terms such as "patient care hours" may vary. Nonetheless, the numbers raise the possibility of some reserve capacity in the dental work force, although differences in work load may reflect different choices about lifestyle, income, and other factors that might limit the extent to which dentists would increase their work load in response in an increase in the demand for their services.
Whatever the national supply picture, state or regional circumstances may differ. As described in the background paper by Capilouto et al., some research has attempted to assess work force requirements within states based on information and judgments about supply, demand, and need. Several regional organizations exist to assist states with higher education planning and policy. These organizations, which include the Western Interstate Commission for Higher Education, the New England Board of Higher Educa-
tion, and the Southern Regional Education Board, provide policymakers with region-specific work force analyses and comparisons (see, for example, Hebbeler, 1984 and McPheeters, 1987). With appropriate funding, health services researchers in dental schools could also undertake such regional or state studies.
Allied Dental Personnel
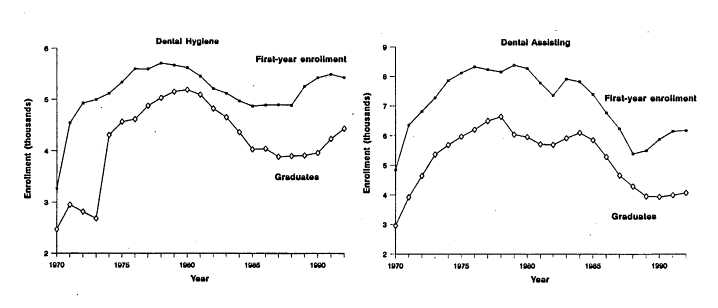
In 1989, the American Dental Hygienists' Association (ADHA) reported 98,000 currently licensed and 71,540 actively practicing dental hygienists. The Bureau of Health Professions estimated that 201,400 dental assistants and 70,000 dental laboratory technologists were active in the work force in 1990 (USDHHS, PHS, 1992). Figure 9.2 shows historic trends in dental hygiene, dental assisting, and dental laboratory technology enrollments. Enrollments grew sharply in the late 1960s and most of the 1970s, then declined in the 1980s. Neither the growth nor the decline was, however, as sharp as that for dentists. Most of the deans surveyed by this committee believed that the current supply of dental hygienists and formally trained dental assistants was too low now and would still be too low in 15 years (see Table 9.1).
Although no government or private organization routinely makes formal projections of trends in the supply of hygienists, assistants, or laboratory technologists, the Bureau of Health Professions predicts the number of jobs that will be available for hygienists in the future. The bureau has projected that the number of hygienists' jobs would grow twice as fast as jobs for the dentists who employ them (IOM, 1989a). These estimates are derived from surveys of incorporated dentist offices and, thus, omit hygienists employed by unincorporated dentists. Moreover, because many hygienists may work in more than one office, the figures do not translate directly into statements about the number of employed hygienists.
Forecasting Models and Their Limitations
The background paper prepared for this study by Capilouto et al. examines models and data used by four organizations to project the supply, demand, and need for dentists. Two of these organizations, the American Dental Association and the American Association of Dental Schools, are private, and two, the Bureau of Health Professions. and the Bureau of Labor Statistics, are agencies of the federal government. The proprietary or nonpublic ele-
ments of some models limited examination of their features. The following discussion draws heavily on this background paper.
Although the models agree in the pattern they forecast, the actual numerical predictions differ as shown in Table 9.2. Each model has tended in the past to produce estimates in excess of actual numbers. Such disagreement is not unique to these forecasts. A recent analysis of estimates of physician supply describes similar variations and concludes that there is ''little scientific basis on which to claim that one projection is more credible than another" (Feil et al., 1993, p. 2863).
Forecasts may vary for several reasons including differences in data sources, definitions, choices of variables to include in models, and assumptions about those variables. Although models and data can be refined, uncertainty about the future is a given. Thus, the mechanical use of models and predictions land, indeed, any planning. and decisionmaking tool) is risky. Even when reasonably good data are available, they may be ignored. For example, the background paper by Capilouto et al. reviews data showing positive income trends for dentists compared with other professions, especially when inflation was considered. In contrast, the media have portrayed declining incomes due to a surfeit of dentists. Because perceptions do influence behavior, they may have to be considered in formulating assumptions for models or presenting their results.
TABLE 9.2
Projection of Active U.S. Dentists by Year of Published Prediction
|
|
Year Prediction Published |
Year Predicted |
|
|
|
|
Organization |
|
1990 |
2000 |
2010 |
2020 |
|
American Association of Dental Schools |
1988 |
149,680 |
154,007 |
148,187 |
137,365 |
|
1989 |
140,699 |
142,379 |
137,197 |
133,214 |
|
|
American Dental Association |
1988 |
149,970 |
156,611 |
|
|
|
1989 |
140,842 |
143,057 |
|
|
|
|
(1990 Census) |
|
(150,762) |
|
|
|
|
|
1991 |
140,543 |
142,793 |
140,611 |
|
|
Bureau of Health |
1988 |
150,300 |
154,700 |
145,800 |
|
|
Professions |
1990 |
149,700 |
154,600 |
151,200 |
140,700 |
|
|
1992 |
148,800 |
154,500 |
149,800 |
138,500 |
|
SOURCE: Table excerpted from Tables 3-5 of the background paper by Capilouto et al. Notes omitted. |
|||||
Supply Estimates
For supply models, the major uncertainties involve assumptions about future dental school enrollments, graduation rates, and retirement from practice. In recent years, different models have projected declines in dental school enrollment ranging from less than 1 to approximately 5 percent per year and educational attrition rates ranging from 5 to 12 percent.
As an example of the prediction errors that can arise from incorrect assumptions, the 1978 Bureau of Health Professions overestimated supply because it incorrectly assumed that the decline in school enrollments would level off in the early 1980s. Because enrollments continued to drop instead, the resulting enrollment estimate was too high by 7,500 over an eight-year period. Similarly, none of the forecasts examined in the background paper by Capilouto et al. anticipated the sharp growth in numbers of international dental graduates admitted to advanced standing in several private dental schools, and current projections still do not account for this development. Thus, even though estimates of future supply are considered more reliable than estimates of demand or need, they are still subject to error. Sometimes accurate predictions result from offsetting errors in assumptions.
In addition, models focus on the supply of practitioners (or jobs) rather than on the supply of services. They tend not to incorporate information or assumptions about productivity (services per practitioner) that result from differences in practice styles, use of allied dental personnel, and other factors. Changes in such factors can significantly affect the supply of services available from the same number of dentists. As the background paper by Bader and Shugars notes, dentistry—like medicine—is characterized by significant unexplained variations in practice patterns.
Demand and Need Estimates
Demand is commonly defined as the willingness and ability to purchase a good or service whereas as need, in a clinical context, refers to phenomena that require clinical attention or treatment (Donabedian, 1973). Demand without need leads to overuse of medical services; need without demand leads to underuse of services. In principle, work force planning models that consider both demand and need for service are more appropriate than models that rely on simple practitioner-to-population ratios and statistical norms for establishing work force "requirements." In practice,
such models are sufficiently subjective and vulnerable to changing events and data limitations that they are less useful as specific numbers than as means of illuminating supply-demand dynamics and helping plan for uncertainty.
The difficulties encountered in projecting current and future requirements for dental personnel and services include the subjectivity of dental diagnoses, the lack of evidence on outcomes and lack of agreement on appropriate interventions for different conditions, and the limited number of conditions for which any data are available. In addition, although the demand for dental services is sometimes measured. by utilization of office visits, this measure does not reveal variations in the quantity and types of service that may be delivered during a visit. (For further discussion, see the background papers on oral health status by White et al. and on outcomes and effectiveness by Bader and Shugars.)
Projected into the future, estimates for demand and need encounter additional problems. In particular, the timing and impact of scientific or technological advances—the future equivalent of the fluoride "revolution" of the 1950s and 1960s—are not easily factored into estimation models. The technological basis for caries vaccine is, for example, on the horizon, but neither its introduction into practice, its acceptance by patients, nor its overall effectiveness can be predicted with any precision. Nor can it be readily predicted whether the preponderance of scientific or technical advances will involve relatively simple, demand-reducing preventive measures (similar to water fluoridation or childhood vaccinations) or whether they will stimulate demand for better therapies (e.g., tissue regeneration as treatment for periodontal disease).
To the extent that a scientific or technological breakthrough only gradually diffuses or changes the demand or need for a service or the way it is produced, routine processes for updating forecasting models and adjusting estimates would be timely enough to warn those who make or implement work force policies. In contrast, a breakthrough that diffuses rapidly and that quickly changes the demand or need for a service (or the way that service is produced) could catch planners and policymakers unprepared. In the background paper by Greenspan and elsewhere, the committee found no evidence suggesting such breakthroughs in caries or periodontal prevention or management.
Given a more than decade-long period in which health care reform was not an active policy issue, it was reasonable for
demand forecasting models to ignore policy options for dental coverage that are now being actively debated. Some policies, notably the inclusion of dental benefits in a universally available benefit package, would likely increase demand for care. Other policies, such as the end of tax exclusions for employer-paid dental benefits, could decrease the demand for dental services. As final revisions were being made in this report, the prospects for health care reform in the next few years were quite uncertain.
In sum, the committee found a very mixed picture of the future adequacy of the supply of dental services. Some factors point to a shortage based on the declining ratio of dentists to the general population and the increasing elderly population (with more teeth at risk for dental problems than preceding generations). Extension of existing preventive measures (e.g., fluoridated water, dental sealants) could continue to reduce the need for restorative services in the younger population. Scientific and technological developments could, on balance, increase or decrease demand depending on the extent to which they favored prevention rather than more intensive treatment. Whether the availability of better treatments would translate into more demand for care would depend on the extent to which they required more time and the extent to which patients could afford to pay for them. The prospect for increased insurance coverage of dental services is uncertain, but an expansion of public or private coverage could increase demand, especially if additional efforts are made to reach those · with significant unmet needs. The presence of reserve capacity in the current dental work force could, however, absorb some or all of any increased demand.
Planning for Uncertainty
The desire of dental educators and public officials for technical models and analyses that provide specific quantitative estimates of the "right" size of the future work force is understandable. Educators and policymakers have no choice but to plan for the future and make choices that may affect the supply of dental services. Using historical experience and quantitative models of the future, they must assess trends, identify options, and project possible best and worst consequences of different actions given alternative future conditions.
Although forecasting models cannot provide firm bases for many important policy decisions, they are still useful monitoring and
analysis tools.2 They help planners and policymakers formulate alternative hypotheses about the future and assess how alternative strategies would fare under these different futures. The models also guide the monitoring and analysis of trend data and encourage analysts to be alert to events that might affect trends. For example, the closure of a large number of dental schools for financial reasons would require a reassessment of the future supply of oral health services and the appropriateness of compensating actions.
Continued investments by government agencies and private organizations in the forecasting models and analyses are prudent as are similar investments in the quality and scope of data used in the models. This, in turn, implies a more sustained investment in a comprehensive oral health data infrastructure than has been evident over the last decade. Although the committee recognizes the tensions that may arise in supporting information resources at the expense of other, more tangible health objectives, it believes that the former ultimately serves the latter.
Three Possible Futures
Based on its review of work force models and projections and analyses of scientific, policy, and other trends, the committee concluded that there is not a compelling case for predicting either a oversupply or an undersupply of dental practitioners in the next quarter century. Recognizing, however, that educators and public officials must look to the future and consider options however uncertain the future appears, the committee considered three broad possibilities for the future supply of dental personnel and services and the ways that dental educators and policymakers might respond. The three possible futures are that the supply might be too high, too low, or within an acceptable range.
Prospects for an Oversupply of Dentists
A decade ago after the substantial increase in dental schools enrollments, the prospect of an oversupply of dentists was a ma
jor concern for many in dentistry, and many of those interviewed for this study believed the current supply of dentists is too high. Population and educational trends described earlier assure that there will be fewer dentists relative to the population after the turn of the century. This ratio could nonetheless be ''too high" under some circumstances, for example, unexpected, dramatic improvements in preventive strategies could change the picture.
Should an oversupply of dentists once again become a worry, strategies proposed to shrink the supply of physicians might apply to dentistry (Wennberg et al., 1993). These strategies include barriers to entry (e.g., further cuts in predoctoral enrollments and specialty residencies) and incentives for early retirement of employed dentists or relocation to underserved areas.
Prospects for an Undersupply of Dentists
As reported earlier, supply forecasts show a downturn in the dentist-to-population ratio, and a majority of dental school deans believe that a shortage of dentists is likely in the future. The committee was not convinced of this point, but it recognized that unexpected but not inconceivable events (e.g., independent actions by several universities to close their dental schools) could change the picture considerably—not only within a state or region but for the nation as a whole.
How might decisionmakers respond to projections of a future shortage? The traditional options have been to increase the supply of dentists or allied dental personnel or to increase work force productivity or both.
Increased Dental School Enrollments. Although concerned about a possible future shortage of dentists, few deans in the committee's survey believed that their school should increase its enrollment. Even fewer believed that they should cut enrollments. Some schools would, in any case, find it difficult to increase enrollments substantially without compromising student quality or incurring significant expansion costs.
The last broad increase in enrollments in health professions schools was spurred by increased federal and state funding, a simple replication of which seems highly unlikely given current fiscal stringency and past government experience with this strategy. Compared to most other fields, an increase in predoctoral dental school enrollments makes heavy demands for specialized and expensive physical space, and many schools that have cut enrollments say they have given up space to other university divisions
that could not be easily reclaimed. Nonetheless, it is reasonable for dental educators to maintain some sense of the extent to which schools could collectively accommodate modest increases in enrollments should the need be convincingly demonstrated.
Increased Productivity of the Dental Team. The most frequently mentioned responses to any future excess of the demand for dental services over their supply involve the productivity of dental personnel. Although, as noted earlier, few data exist to document the point, it is likely that some dentists could considerably increase their individual output of services, for example, by working several more hours each week and seeing more patients. Although not all dentists would choose such a schedule, some surely would. Faced with high demand for their services, some dentists might also seek to free up time for medically needed care by encouraging fewer purely cosmetic services such as bleaching of teeth.
A broader productivity strategy focuses not just on dentists but on the entire dental team (AADS, 1993c; ADA, 1993g; ADHA, 1993). As described by one proponent (Nash, 1993), the "high-performance" dental team of the future would provide "new and challenging roles" for
- dental hygienists in treating periodontal disease and educating patients in and beyond the dental office;
- dental assistants in acting as dentist-extenders, especially for rehabilitative services;
- dental laboratory technicians in providing complete denture services; and
- dentists in providing the leadership that helps every member of the team to perform effectively.
These roles involve a mix of new responsibilities and old responsibilities more intensively exercised. Studies suggest that dentists trained to work with allied dental personnel are more productive and that allied personnel working in less restrictive delivery systems can provide high-quality care within their areas of competency (Burt and Eklund, 1992; Freed and Perry, 1992; see also the background paper by Tedesco).
A team strategy is not without problems, however (Bader et al., 1989; IOM, 1989a; DeVore, 1993; Pew Health Professions Commission, 1993; Robinson, 1993). First, as noted in Chapter 8, state practice acts limit the scope and efficiency of services that allied personnel can provide. For example, a sizable minority of
states require that dentists directly supervise certain hygienist services (i.e., a dentist must be physically present when the services are provided). At least nine states forbid the employment of more than two hygienists in a dental office (ADHA, 1993). The restrictions on dental assistants (e.g., whether they can apply topical fluorides or pit-and-fissure sealants) vary greatly from state to state.
State practice acts are heavily shaped by the economic interests of the dominant professional groups (Starr, 1982; Friedland and Valachovic, 1991; Burt and Eklund, 1992). Efforts to increase the output of the dental "team" through better use of allied dental personnel were attempted in the 1970s but abandoned in the face of a threatened oversupply of dentists. Dentists remain wary of these strategies and might oppose policies to implement them even in the face of an evident shortage of services. Funding for innovative programs to build on the team strategies tested in the 1970s is virtually nonexistent at the federal level. In Chapter 4, the committee suggests further study of the role of existing and new categories of dental personnel in the context of a closer integration of medicine and dentistry.
A second problem with the team strategy is that many hygienist abandon the field after a few years (IOM, 1989a; Miller, 1990). Their reasons include boredom, unsatisfactory pay and benefits, limited opportunities for career advancement, and concern about workplace conditions that increase risk of infection. The ADHA has argued that the perceived shortage of hygienists (as revealed in the committee's survey of deans) is more accurately described as a failure to use the existing work force appropriately (ADHA, 1989, cited in ADHA, 1993). Although dental hygiene enrollments have recently increased, inadequate recruitment for a broad range of allied health fields is still a concern (IOM, 1989a; Pew Health Professions Commission, 1993). To be successful, a team strategy would have to deliver on its promises to allied dental professionals—including increased responsibilities and levels of decisionmaking commensurate with education.
A third issue is the variability in educational background, the declining proportion of university-trained hygienists, and possible shifts in the type of individuals recruited. Each of these factors raises questions about how well dental hygiene education prepares students for increasingly complex oral health problems and suggests that more, rather than less, education is necessary for dental hygienists to meet these challenges (Kraemer, 1985; DeVore, 1993). Similar questions apply for dental assistants.
In 1989, another Institute of Medicine (IOM, 1989a) committee made several relevant and reasonable recommendations to strengthen the dental hygiene and other allied health professions. Among the group's recommendations were that
- the Department of Health and Human Services should "convene an interagency task force . . . to work toward increasing the amount and improving the quality of data needed to inform [decisions] about the allied health occupations" (p. 4);
- "students should be sought in less traditional applicant pools" (p. 7) and "alternative pathways to entry-level practice . . . and mobility between community college and baccalaureate programs" should be encouraged whenever feasible" (pp. 7-8);
- employers should "strive to increase the supply of allied health practitioners . . . [through means including] increasing compensation and developing mechanisms for . . . prolonging their attachment to their fields" (p. 9); and
- "flexibility in licensure" and reliance on "statutory certification" (pp. 11-12) should be accepted to the extent consistent with the public interest.
It is worth observing that physicians or nurse practitioners might, in principle, enlarge the supply of some oral health services, particularly as medical management of oral health problems becomes more important. At this time, however, physicians do not appear inclined by either education or interest to assume a larger role in oral health services, a reluctance reinforced by the modest levels of insurance for such services. Although this committee did not systematically investigate how generalist or specialist physicians might provide oral health services in the event of undersupply of dental professionals, Chapters 3 and 4 of this report have called for increased attention by physicians to oral health concerns.
Reducing the Use of Dental Care. Another set of responses to an undersupply of dental services could target the utilization of dental services. Reductions in service use could come through cutting consumer demand for services, for example, by increasing cost-sharing requirements in dental insurance plans or improving health habits. Reductions could also be achieved by changing provider behavior, for example, by instituting capitated payment to providers to eliminate possible incentives for overtreatment of insured patients.
Strategies targeting the demand for care or the provision of services raise concerns, first, that they would affect both inappropriate and appropriate care and, second, that they would discrimi-
nate against poorer or less sophisticated patients and consumers. For example, increased insurance deductibles and coinsurance levels could prompt patients, especially those with lower incomes, to forgo both needed and unneeded services. Such concerns are not restricted to an "undersupply" scenario as current debates over strategies to contain health care costs attest. They reinforce the committee's call for intensified efforts to measure oral health outcomes and to distinguish clearly beneficial interventions from those that are harmful or ineffective.
Prospects for Supply in Balance with Requirements
A third possible projection is that the future supply of dental services would be essentially in balance with requirements for those services overall. In practical terms, this may seem similar to the committee's conclusion that it could not confidently predict either an oversupply or an undersupply of services. The major difference is that the latter conclusion reflects uncertainty rather than a positive judgment. The implications for policymakers are, however, essentially the same—that caution should govern steps to increase or decrease the future dental work force.
A projection of supply in balance with requirements still leaves a number of work force concerns for planners and policymakers. These include the geographical distribution of practitioners, the composition of the work force, and the productivity of dental personnel. The first two topics are discussed below; the last has been discussed earlier.
Work Force Distribution and Composition
Geographic Distribution of Personnel and Services
The discussion to this point has emphasized the total supply of dental personnel, but the committee has indicated concern about two other important issues: geographic distribution of personnel and work force composition. Past policies to deal with maldistribution problems by increasing the overall supply of personnel have been abandoned because the increased supply of physicians has done little to reduce shortage problems in many rural and inner-city locales (GAO, 1994). Greater competition in health care might reduce the demand for services in oversupplied areas and propel more practitioners to relocate in shortage areas, but this remains to be demonstrated.
To attract health personnel to undersupplied areas, more targeted strategies have been developed. In Britain, for example, a negative incentive denies physicians a list of publicly insured patients (almost the entire population) if they locate in oversupplied areas such as London. The United States has tried positive incentives in the form of the National Health Service Corps (NHSC). The NHSC includes loan repayment features for health professionals that serve in designated shortage areas, and it encourages personnel to remain in these areas after their service period is finished. These strategies are attractive because they address both the shortage problem and the problem of student debt repayment. The General Accounting Office, however, concluded recently that the impact of these programs on underserved areas is difficult to establish (GAO, 1994). It found, however, that the increased total supply of primary care physicians and dentists in the past decade has not been accompanied by increases in ''those urban and rural areas where the greatest shortages exist" (p. 2). The Department of Health and Human Services developed an oral health initiative in FY 1994 in response to Senate concerns about limited access to "primary care oral health services" and inadequate identification of affected areas and populations (U.S. Senate Appropriations Committee, 1994, p. 41). The GAO report concluded that "these actions are not likely to have much impact, at least in the short run" (1994, p. 2].
One problem with the NHSC and related programs is restricted funding. Of the 1,069 designated dental shortage areas in 1993, only 356 had been updated since 1988 and thereby made eligible for assistance through the NHSC (J. Rosetti, personal communication to M. Allukian, April 4, 1994). Moreover, the U.S. Health Resources and Services Administration has approved only 75 dental vacancies for loan repayment participants, and at the time information was provided to this committee, only 23 positions had been filled. One report states that there are no "ready" sites available for additional dental school placements (AADS, 1994c). Such sites have the equipment, salary, and staff to support an NHSC participant. One additional problem cited earlier is that many shortage areas call for part-time positions, and such positions are particularly difficult to fill.
Representativeness of the Work Force
As noted earlier, the composition of the dental student body and the dental work force has changed rather dramatically in some
respects. In particular, the proportion of women and those of Asian background has risen sharply. The proportion of African-Americans has, in contrast, not grown. Recent declines in the number of African-Americans entering and completing college will make it difficult for dentistry and other professional and graduate programs to meet their recruitment goals for this group (New York Times, 1994). Hispanic and Native American populations are also underrepresented.
Since the 1960s, the health professions have focused on the objective and the problems of achieving racial and ethnic diversity, particularly in medicine, dentistry, and nursing. A recent ADA report focused specifically on minority and female representation in dentistry (ADA, 1992f), and another IOM committee recently examined the issue (IOM, 1994a). The latter report emphasized strategies to broaden the "pipeline" of minority students. The GAO figures on population versus educational parity for African-American enrollments in dental schools underscore the importance of increasing the flow of individuals academically prepared from their earliest educational experiences to choose a health professions career. Reform of science and math education from elementary through collegiate stages is a particularly crucial element of the pipeline strategy.
Among the set of supportive attitudes and mechanisms cited by the IOM (1994a, p. 66) study, mentoring was particularly recognized as a critical component with a "proven track record of helping minorities pursue their aspirations and achieve their career goals." To attract and support youths interested in the health professions, academic health centers should enlist the aid of corporations, other educational institutions, foundations, and government in developing mentoring programs; information networks; positive messages for talented students; and other projects. Another supportive step would be for universities to recognize "some level of community service among the criteria for academic recognition and advancement, in addition to the time-honored measures of scholarly and clinical achievement." Clearly, efforts to increase minority representation in dentistry must reach far beyond the dental school and involve practitioners, educators at all levels, policymakers, foundations, and corporations.
A recent California report also recommended a series of outreach programs and other actions to build a "strong educational pipeline" (University of California, 1993, p. ix). These steps included "working to bolster science curricula, developing feeder networks of health sciences high schools and undergraduate col-
leges, keeping health sciences professions within the financial reach of all students, and fostering a supportive learning environment within the health professions programs."
The committee on dental education was encouraged to see many dental educators recognizing and attempting to help implement strategies such as those described above. It notes, however, that medical schools are already attracting a very large percentage of minority science graduates (IOM, 1994a). Thus, recruitment aimed primarily at these graduates is not very promising if dental schools want to do more than "steal" applicants from other health or science careers. The problem of minority attrition after recruitment to dental school warrants particular attention.
Findings and Recommendations
After reviewing work force models and projections and their underlying assumptions, the committee found no compelling case, at this juncture, that the overall production of dentists will, in the next quarter century, prove too high or too low to meet public demand for oral health services. Accordingly, it found no responsible basis for recommending that total dental school enrollments should be pushed higher or lower.
However, even in the absence of compelling evidence that the nation faces either an oversupply or an undersupply of dentists, decisionmakers cannot abandon interest in either prospect. Scientific, economic, political, and other uncertainties warrant active surveillance and monitoring of developments that could change trends in supply, demand, or need. If a shortage in dental services is identified in the future, policymakers should look first to these options and increase enrollments at the predoctoral level only if these strategies prove insufficient.
In Chapter 4, the committee recommended that opportunities for advanced education in general dentistry be expanded, a step that would not affect the total supply of dentists but that would strengthen generalist practice. Chapter 5 endorsed increases in the oral health research work force.
The committee notes the persistence of dental professional shortage areas and the limited reach of federal programs to alleviate these shortages. The underrepresentation of African-Americans and certain other minorities in the dental work force is another continuing concern.
Because the prospects for a future oversupply or undersupply of dental personnel are uncertain and subject to unpredictable scientific, public policy, or other developments, the committee recommends that public and private agencies
- avoid policies to increase or decrease overall dental school enrollments;
- maintain and strengthen programs to forecast and monitor trends in the supply of dental personnel and to analyze information on factors affecting the need and demand for oral health care.
To respond to any future shortage of dental services and to improve the effectiveness, efficiency, and availability of dental care generally, educators and policymakers should
- continue efforts to increase the productivity of the dental work force, including appropriately credentialed and trained allied dental personnel;
- support research to identify and eliminate unnecessary or inappropriate dental services; and
- exercise restraint in increasing dental school enrollments unless other, less costly strategies fail to meet demands for oral health care.
To improve the availability of dental care in underserved areas and to limit the negative effects of high student debt, Congress and the states should act to increase the number of dentists serving in the National Health Service Corps and other federal or state programs that link financial assistance to work in underserved areas.
To build a dental work force that reflects the nation's diversity, dental schools should initiate or participate in efforts to expand the recruitment of underrepresented minority students, faculty and staff, including
- broad-based efforts to enlarge the pool of candidates through information, counseling, financial aid, and other supportive programs for precollegiate, collegiate, predoctoral, and advanced students; and
- national and community programs to improve precollegiate education in science and mathematics, especially for underrepresented minorities.
Summary
Work force planning is a source of continual frustration for policymakers and educators. The failures or unintended consequences of past work force policies have left considerable wariness about proposed solutions to work force problems, and the limitations of forecasting models and data preclude confident predictions about the future. Another legacy of past policies is tension between the education and practice communities that extends beyond enrollment questions to complicate efforts to broaden and enrich the educational and patient care programs of dental schools. This chapter has argued for caution in changing dental school enrollments and for continued efforts to reshape the distribution and composition of the dental work force. It also has reinforced arguments in other chapters for increased effort to make more productive use of the entire dental team.