4
The Mission of Education
The most visible mission of dental education is to develop future practitioners. Broadly stated, its basic goals are to (1) educate students to serve their patients and communities well and (2) prepare students to continue to grow in skill and knowledge over their lifetime in practice. This report throughout refers to ''education'' rather than "training" to emphasize that dentistry as a profession demands both intellectual and technical skills that depend on clinically relevant education in the basic sciences and scientifically informed education in clinical care.
This chapter starts by putting current curriculum critiques in historical context. It then discusses several major curriculum concerns within the framework of principles established in Chapter 1. Then, because a sound curriculum means little without capable faculty and students, two major sections consider the people who constitute the heart of a dental school and whose careful recruitment and continued development are essential to the educational changes proposed in this chapter. Although the emphasis is on predoctoral education, this chapter also examines the critical relationship between predoctoral and advanced education in general dentistry. Continuing education, sometimes viewed as part of a university's service mission, is here considered to be one more stage of a lifelong learning process that professionals must pursue and dental schools must support. Research and patient care, which are
examined in Chapters 5 and 6, are critical in their own right but are also crucial contributors to the kind of educational enterprise recommended in this chapter.
The discussion below tends to focus on dental schools as discrete entities. The committee did not, however, intend to understate the role of organizations such as the American Association of Dental Schools (AADS) or limited-purpose consortia of several dental schools as promoters of change. These groups serve many valuable purposes, for example, by stimulating discussion, facilitating communication about innovative programs, devising model approaches to common problems, providing technical support, collecting and analyzing information, and promoting good relationships with organized dentistry and others. Collective as well as individual effort is essential if the changes recommended are to be achieved.
Curriculum in Context
A curriculum embodies the values and vision of an institution and a discipline. As expressed in the principles stated in Chapter 1, dental education should be scientifically based, clinically relevant, medically informed, and socially responsible. It should emphasize outcomes as well as services, efficiency as well as effectiveness, and community as well as individual needs. It should prepare students to critically assess both new and old technologies and practices throughout their careers.
Traditionally, faculty have largely controlled school and department decisions about what is taught, by whom, and in what fashion. As discussed in a later section of this chapter, among the most important and difficult factors affecting the direction and pace of curriculum change are those involving the composition, power, and disciplinary organization of faculty.
Seventy Years of Curriculum Critiques
In the course of this study, the committee heard a lively debate about the strengths and weaknesses of current curricula and the values and vision that curriculum reform should reflect. As the background paper by Tedesco underscores, most critiques of the dental curriculum are long-standing. The core concepts behind changes that are still being advocated date back several decades.
Moreover, if the word "medical" were changed to "dental," the basic points of several persistent critiques of undergraduate medi-
cal education could easily apply to dentistry (Enarson and Burg, 1992). The links between the Flexner report (1910) on medical education and the Gies report (1926) on dental education have already been cited in Chapter 2. In the 1960s, the report Planning for Medical Progress Through Education (Coggeshall; 1965) fore-shadowed the 1993 recommendations of the Pew Health Professions Commission. For example, it envisioned medical education as a "continuum" that begins with preprofessional years (secondary and collegiate), is marked by the M.D. degree as a "midpoint," and extends with continuous education and reeducation "until the professional life of the practitioner is finished'' (pp. 39-40). The Coggeshall report also stressed (as does this report) the importance of health professions schools as integral parts of the university. More recently, the 1992 report Medical Education in Transition (sponsored by the Robert Wood Johnson Foundation) argued that "there is [an] . . . urgent need for students to appreciate the relevance—and, indeed, the excitement—of applying today's scientific advances to the practice of medicine" (Marston and Jones, 1992, p. vi). That theme likewise runs throughout this report.
One lesson of past reports is that the dental curriculum is not alone as a target for criticism. A more sobering lesson is that it is much easier to analyze and recommend than to act.1 The practical, political, and procedural demands of major shifts in course offerings and content test the stamina of those attempting change (AAMC, 1992; Hendrickson et al., 1993). As one educator put it, "Most deans would rather take a daily physical beating than try to make significant changes in the traditional [curriculum]" (Garrison, 1993, p. 344).
Recognizing the difficulties of change, various organizations have tried to assist planning processes, demonstration projects, and other activities in dental schools. The Pew National Dental Education Program offers a model of this kind of private support. It funded strategic planning processes in 21 schools and implementation
activities in 6 (University of California, San Francisco; Columbia University; University of Florida; University of Maryland; Oregon Health Sciences University; and University of Southern California). These projects are summarized in the background paper by Tedesco, and an initial evaluation of the programs is reported in Feldman et al. (1991).
This committee's findings and recommendations are intended to provide additional guidance and leverage for those with the desire and the will to seek further and more widespread reform of dental school curricula. They are also intended to reflect the interconnections of the education, research, and patient care missions of the dental school and to place curriculum objectives in the context of changing concerns about faculty, students, financing, regulatory practices, and work force planning.
Background Data
The major source of quantitative data on the dental school curriculum is a series of annual education surveys conducted and published by the American Dental Association (ADA). The background paper by Tedesco presents additional historical data from many sources. Information from the survey of deans by the Institute of Medicine (IOM) and the American Association of Dental Schools is also included here.
Through its site visits, survey of deans, public hearing, and other activities, the committee sought to supplement quantitative and written information with a more qualitative sense of the curriculum as experienced by students, faculty, and to a limited degree, patients. In some respects, this qualitative sense is another label for realism, an understanding of the practical and political challenges of change.
Variations in Program Length and Density
The dominant model of dental education is a four-year predoctoral program. One school (the last of a group of 16 that tried a three-year schedule during the 1970s) offers a three-calendar-year predoctoral program, and another has offered a five-calendar-year program that it is planning to reduce to four years. The predoctoral program is generally preceded by a baccalaureate degree with appropriate preprofessional coursework in the sciences. For the majority of dental graduates, it is followed by advanced education in general dentistry or a specialty.
Beyond that common base lies substantial variability in program length and density. The length of the predoctoral program ranges from 120 to 187 weeks, with a mean length of 158 weeks.2 The number of weeks of instruction for the fourth year of dental school averages 38, with a range from 28 to 49 weeks (a 75 percent difference). Summers have increasingly been filled with academic requirements.
For the four-year programs, total clock hours3 range from 3,450 to 6,635—an almost twofold difference. Clock hours per week range from 20 to 41; the median number of clock hours per week is 30.
Many schools offer optional programs that allow qualifying students to combine baccalaureate and predoctoral coursework in a structured six- or seven-year program. Some schools cooperate with other university programs to offer joint degrees, for example, a D.D.S. and a master's degree in public health, business, or public policy.
Variations in Instructional Allocations
The variability in length of the total dental curriculum extends to individual components. Table 4.1 summarizes the two- to sevenfold differences among schools in hours devoted to basic, clinical, and behavioral sciences. The background paper by Tedesco reveals similar variation among schools in the hours allocated for 19. basic science, 24 clinical science, and 5 behavioral science categories.
The background paper also summarizes historical data on clock hours and their distributions over the past 30 years. These data suggest a gradual increase in curriculum requirements. This committee did not chart statistical changes in clock hours by individual school, but the survey of deans, the site visits, and other information once again suggest considerable variation across schools.
In the deans' survey, a near majority of dental school deans (25 of 54) estimated that overall clock hours of instruction had remained about the same for the past 10 years. Only five suggested that
TABLE 4.1
Variability in Curriculum Requirements—Basic Sciences, Clinical Sciences, and Behavioral Sciences
|
|
Total Clock Hours |
Percentage of Total Hours |
||||
|
Curriculum |
Low |
Median |
High |
Low |
Mean |
High |
|
Basic Sciences |
||||||
|
Didactic |
447 |
574 |
1,770 |
|
|
|
|
Laboratory |
52 |
206 |
584 |
|
|
|
|
Total |
563 |
787 |
2,103 |
12 |
17 |
34 |
|
Clinical Sciences |
||||||
|
Didactic |
678 |
1,001 |
1,535 |
|
|
|
|
Laboratory |
398 |
726 |
1,208 |
|
|
|
|
Patient careintramural |
415 |
1,938 |
2,740 |
|
|
|
|
Patient care extramural |
8 |
119 |
1,798 |
|
|
|
|
Total |
2,567 |
3,844 |
5,400 |
64 |
80 |
87 |
|
Behavioral Sciences |
||||||
|
Didactic |
57 |
115 |
373 |
|
|
|
|
Laboratory |
2 |
12 |
120 |
|
|
|
|
Total |
57 |
123 |
373 |
1 |
3 |
5 |
|
SOURCE: Excerpted from American Dental Association, 1994c. |
||||||
hours had increased rather than decreased. A majority of deans reported some or substantial increases in clock hours in clinical sciences, practice management, research methods, and behavioral science instruction. For the next 15 years, a majority expected further increases in these areas, in clinical training at nontraditional sites, and in working with allied personnel. Twelve deans reported decreases in basic science hours, compared to 10 reporting increases. Decreases in preclinical instruction were reported by 14 deans, but 5 reported increases. A majority of deans (30) predicted that preclinical hours of instruction would drop further. The committee could not determine whether decreases in basic science hours represented a desirable pruning of marginally relevant material or a deemphasis of the scientific foundation of dentistry at a time when that base is becoming more important.
Accreditation Standards and Curriculum Guidelines
Curriculum content is influenced by the standards of the Commission on Dental Accreditation and the curriculum guidelines developed independently by the AADS. Curriculum guidelines, which are not enforceable in the same way as accreditation standards, are intended to provide useful models for dental schools
that neither stifle innovation nor mire schools in detailed regulatory requirements. As described in more depth in the background by Tedesco, the AADS is redrafting the guidelines to focus on competencies that comprise a mix of skills, practices, and attitudes (or understanding) needed by dental practitioners.
The accreditation standards (and the accompanying discussion) emphasize preparation for lifelong learning (5.1.1), education in scientific reasoning and problem solving (5.1.2), and application of basic science principles to clinical care (5.2.1). Patient assessment and coordinated treatment planning are also stressed (5.3). The charge that accreditation standards stifle innovation focuses, in part, on the detailed specifications in clinical areas and on the standard that "early specialization must not be permitted until the student has achieved a standard of minimal clinical competency in all areas necessary to the practice of general dentistry" (5.1.3) (CDA, 1993a, p. 489).
The committee heard the accreditation standards commended for promoting many of the directions discussed below. It also heard complaints that the standards discouraged innovation. As discussed in Chapter 8, the committee's sense is that both arguments have merit.
Issues and Controversies
As noted earlier, 70 years of surveys and reports have identified curriculum problems that persist to a considerable extent today. Most criticisms can be grouped into at least five broad concerns. First, basic science concepts and methods are weakly linked to students' clinical education and experience. Second, the curriculum is insufficiently attuned to current and emerging dental science and practice. Third, many problems remain in implementing comprehensive patient care as a model for clinical education. Fourth, linkages between dentistry and medicine are weak. Fifth, the overcrowded dental curriculum gives students too little time to consolidate concepts and develop critical thinking skills that prepare them for lifelong learning.
Integrating the Basic and Clinical Sciences
Curriculum Structure
As described in Chapter 2 and in the background paper by Tedesco, the 1910 Flexner report and the 1926 report by William Gies called
for curricula that embodied the scientific basis of medicine, including dentistry. Intervening years have broadened the case for basic science education to prepare students to become practitioners who can critically appraise new strategies for patient care and apply them when appropriate and who can understand the relevant biological bases of oral health and disease. Education in the basic sciences should also provide the vocabulary and basic concepts for researchers and clinicians to communicate with each other (Ten Cate, 1986).
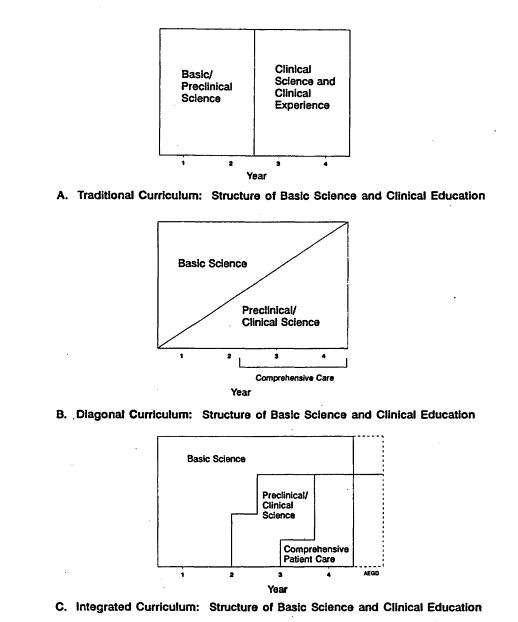
Figure 4.1 (derived from Formicola, 1991) depicts graphically the traditional Flexner-Gies organizational scheme.4 It also presents two alternative models that illustrate curriculum innovations adopted after World War II by medical schools at Cornell, Colorado, and what is now Case Western Reserve (Marston and Jones., 1992). These new models also contain other innovative concepts including comprehensive patient care.
The Flexner-Gies model concentrated basic science education in the early part of the medical and dental school curriculum. Over time, as dental schools settled into a four-year schedule, the first two years of the curriculum also incorporated preclinical instruction (e.g., tooth preparation for restorations).
The traditional curriculum, although a great advance over the nonscientific curriculum that preceded it, has been criticized severely for divorcing basic science from clinical practice to such an extent that many students view basic science as a largely irrelevant hurdle that has to be passed before their "real" training begins (Neidle, 1986a; Prockop, 1992). "Preclinical curricula are stuffed with too many courses, too many lectures, and too many faculty hobby horses that leave students at the end of two years exhausted [and] disgruntled" (Petersdorf, 1987, p. 19).
More specific criticisms include the following (see Vevier, 1987; Marston and Jones, 1992; Prockop, 1992; Pew Health Professions Commission, 1993). First, expectations that students can master the core basic science disciplines in the equivalent of four semesters are unsustainable and counterproductive given the explosion of scientific knowledge. Second, the emphasis on mastering facts
|
4 |
This model is also called the horizontal model because it has often been graphed with years on the vertical axis so that the last two years of clinical science are stacked horizontally above the first two years of basic science. Figure 4.1A shows a vertical rather than horizontal division because school years are consistently placed on the horizontal axis for each model. |
still prevails over mastering principles and methods. Third, Ph.D.-trained basic scientists are not, in isolation, well prepared to focus their courses on the concepts and knowledge that are most clinically relevant. Fourth, the preparation and focus of National Board examinations, despite revisions, reinforce these problems. Fifth, some of the more esoteric areas of the basic sciences are not really relevant to clinicians and should be identified and dropped.
Although these criticisms have been directed at both medical and dental education, dental students face additional burdens under a traditional curriculum. Besides the basic science courses, they must fit a considerable volume of preclinical laboratory work into their first two years.
More generally, it was suggested to the committee that locating basic science faculty in the medical school can contribute to a lack of accountability to the dental school and thereby to curriculum immobility and low research productivity. For the majority of dental schools (29 in 1992), the basic science faculty are shared with the medical school, and instruction for dental and other health professions students is negotiated (ADA, 1993f). Although these dental schools may contribute 10 to 20 percent of their budgets to medical schools for basic science faculty positions, they do not have direct control over the faculty, and this may make it difficult for them to influence course content, for example, the inclusion of clinically relevant topics and examples. Some interviews suggested that schools may receive little in return beyond instructional hours (e.g., no participation in research related to oral health issues). If more shared faculty can be interested in oral health issues, then the larger and more diverse pool of basic scientists available on such a basis may be an asset. Such a pool is also created when academic health centers organize all basic science faculty in a separate unit.
Alternatives to the traditional curriculum propose a more gradual shift in emphasis from basic science to clinical education. The objectives, which this committee endorses, are to reduce the disjuncture between instruction in the basic and clinical sciences and to encourage more "correlation" between the two throughout the predoctoral program. As depicted simply in Figure 4.1B, the goal is a gradual shift in educational emphasis rather than an abrupt chronological divide. In actuality, because coursework is generally blocked into discrete units (e.g., hours), the shift is better depicted as a stepwise rather than a continuous progression (Figure 4.1C). The revised figure still oversimplifies by omitting coursework in areas such as the behavioral sciences.
Curriculum reorganization can do only so much, however. The link between science and practice must be demonstrated by faculty in both the classroom and the clinic. Thus, the modes as well as the content of education are important.
Modes of Education
Another shift from the traditional curriculum involves the introduction of instructional methods that attempt to reduce student alienation and disinterest by melding basic science principles and information with realistic analyses of clinical dental problems. Problem-based learning is perhaps the most notable example of such new approaches. Rather than view dental students as ''repositories of facts with psychomotor skills" (Tedesco et al., 1992), advocates of problem-based learning see students as acquiring an intellectual framework for practice and an understanding of the scientific method. In a sense, education is "what you have left after you've forgotten the facts" [Smith, 1985, cited by DePaola, 1986).
At the risk of some oversimplification, traditional instruction and problem-based learning can be contrasted as follows.
|
Traditional Instruction |
Problem-Based Learning |
|
Fact-oriented science |
Concept- and problem-oriented science |
|
Discipline-focused courses |
Interdisciplinary education |
|
Abstract knowledge |
Clinically related problems |
|
Larger classes |
Smaller classes |
|
Lectures |
Guided discussions |
|
Multiple-choice examinations |
Analytic examinations |
A number of dental schools have introduced problem-based learning in recent years, but little research documents its educational outcomes to date. Some medical schools, however, have up to 20 years experience with the approach. Two recent reviews of research on outcomes of problem-based versus traditional instructional methods indicate that the former was associated with greater student satisfaction; higher faculty evaluations; better clinical functioning; better performance on Part III of the medical board examinations (the problem-solving segment); and poorer performance on the Part I (fact-based) examination (Albanese and Mitchell, 1993; Vernon and Blake, 1993; see also Norman and Schmidt, 1992, and the background paper by Tedesco). One of these re-
views (Albanese and Mitchell) recommended caution in curriculum-wide conversion to the strategy until more evidence is available on costs and effectiveness of different methods of problem-based learning, in particular, more and less directive approaches.
If problem-based learning is successful in encouraging critical thinking, it should prompt students and faculty to question variations in approaches to different clinical problems and to become more focused on the outcomes of alternative patterns of care. The committee learned that some schools, in an effort to standardize some aspects of clinical instruction and reduce inconsistent assessments of student performance, have begun to identify variations among faculty in clinical preferences and practices; to secure agreement on preferred practices by using scientific evidence and formal consensus processes; and to develop the case for acceptable variations. Such processes are politically sensitive and time consuming. Furthermore, the paucity of outcomes research and systematically developed practice guidelines is a problem. Chapter 3 has already discussed this deficiency and recommended increased support for both outcomes research and practice guidelines. The background paper by Bader and Shugars explores these topics in depth. It notes research indicating that dental faculty are as variable in their clinical preferences and practices as other dentists.
Computer-based and other self-paced instructional materials and the use of standardized patients can also help in encouraging critical thinking and relating basic science principles to clinical examples. 5 They generally involve conscious, multidisciplinary efforts to construct learning opportunities that are less dependent than traditional instruction on the talents and biases of individual faculty.
The committee recognizes that costs are a barrier to the introduction of new instructional methods that may require additional spending for faculty to develop and teach smaller classes, acquisition of computer hardware and software, physical space reconfiguration, and faculty training in new teaching methods. In some cases, however, computer-based instruction might replace some faculty instruction, and reductions in total curriculum hours, as recom-
mended below, should free some resources for new uses. Further, special appeals to alumni and industry may attract funds for capital investments in up-to-date computer capacity that would not be forthcoming for other purposes.
Current Concepts and Practice
The committee heard arguments that dental school curricula—and faculty—are too often oriented to past oral health problems and practices. Specifically, curricula have not kept pace with changes in oral health problems (e.g., the increasing proportion of patients with complex medical conditions); scientific knowledge and technologies (e.g., in areas such as pharmacology and implants); information management tools and techniques; and society's expectations for health professionals (e.g., attention to informing patients about their choices).
In addition, the committee was impressed with arguments that students spend too much time on preclinical and laboratory activities (e.g., fabrication of crowns and prostheses) that today are most often performed by technicians and other personnel. More generally, financial and other constraints mean that many students receive an inadequate education in effective and efficient team practice with dental hygienists, assistants, and technicians.
An annual AADS survey of dental school seniors (Solomon and Whiton, 1991; AADS, 1992) asks for their views on curriculum components that were under- and overstressed. As presented in Figure 4.2, the 1992 survey found that a quarter or more students rated curriculum attention to orthodontics, practice administration, geriatric dentistry, emergency treatment, and community dentistry as inadequate. Attention to dental materials, basic medical science, and periodontics was rated as excessive by more than 10 percent of the respondents.
In the committee's view, several factors contribute to resistance to curriculum change. They include faculty conservatism, slow change in licensure examinations, and economic limits on changes that require capital expenditures or recruitment of additional personnel.
Faculty conservatism can be attributed to at least three factors beyond personal attachment to familiar arrangements and anxiety about the possible negative consequences of change. First, despite the recent growth of advanced education programs in general dentistry, many generalist faculty lack such training and are also not involved with advanced students who should be better prepared than predoctoral students to question traditional prac-
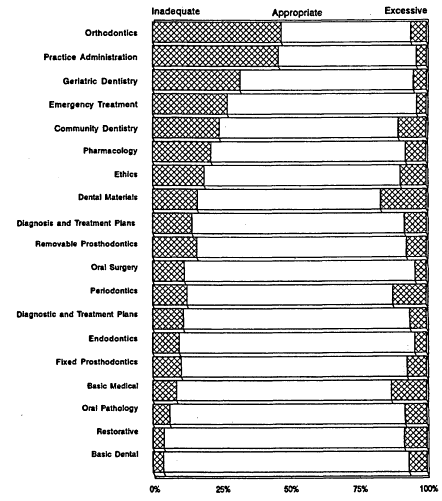
Figure 4.2
Survey of dental school seniors: Ratings of curriculum emphasis.
Source: American Association of Dental Schools, 1992.
tices. Second, some clinical faculty are unable or unwilling to participate in faculty practice plans or interact clinically with those in private, community-based practice, which may limit their exposure to current practice and expectations. Third, clinical faculty who are not involved in research may be less familiar with scientific and technological advances. On occasion, the committee heard that some full-time faculty are viewed as not conversant with newer materials, techniques, and debates. By default,
students may look to part-time faculty as models for up-to-date practice. Whether these perceptions have a basis in fact or are just one more sign of tensions between educators and practitioners, they were disquieting to the committee and warrant attention from educators, for example, through continuing education or alumni and community relations programs.
As noted earlier, one problem with oral health services (indeed, health services generally) is limited evidence about the effectiveness of many preventive, diagnostic, and therapeutic interventions. As the evidence base related to both new and established dental procedures and technologies expands and as more Science-based practice guidelines are developed, dental educators will be better positioned to assess and shape current practice. Well-designed and presented outcomes studies and practice guidelines should, in the future, prove to be useful educational tools (IOM, 1992).
Comprehensive Patient Care
Traditionally, dental schools organize clinical experience for students through rotations in discipline-based clinics. That is, students spend fixed amounts of time in up to nine specialty clinics (e.g., fixed prosthodontics, periodontics) supervised by specialty faculty.
In contrast, the premise of the comprehensive care model of clinical education is that students should learn to provide patient care in a manner and setting similar to those found in an efficient dental practice (Vining, 1984; see, generally, Journal of Dental Education , June 1984 supplement). The continuum of care learned by predoctoral students should be that provided by the general dentist including (1) patient examination and evaluation; (2) diagnosis and treatment planning; (3) direct treatment for a range of common dental problems; (4) use of allied dental personnel; and (5) referral to dental specialists, physicians, or others as appropriate.
Again at the risk of oversimplifying, the traditional and comprehensive care approaches to clinical education can be contrasted as follows:
|
Traditional Care |
Comprehensive Care |
|
Specialist role model |
Generalist role model |
|
Student-centered instruction |
Patient-centered education |
|
Segmented patient care |
Continuity of patient care |
|
Procedure focus |
Evaluation and management focus |
|
Numerical requirements |
Competency criteria |
Chapter 6 argues that these tenets of comprehensive care are supportive of the patient care mission of the dental school and better prepare students to be sensitive to patient needs and less narrowly focused on technique. It argues further that unless academic programs offer patient-centered education, they will fare poorly in the restructured health care system of the future.
Although many schools have adopted some elements of comprehensive care, most have considerable progress to make in providing patient-centered, continuous care and in evaluating students based on competency rather than numerical requirements. A 1993 survey estimated that 40 dental schools had comprehensive care programs, up from 25 schools identified in 1989 (Baughan et al., 1993; Dodge et al., 1998). The structure of these programs varied substantially with respect to the features listed above. Nor example, some drew faculty from specialty departments, whereas others relied on faculty from departments of general practice; numerical criteria for evaluating student performance remain commonplace. One innovative variant of the comprehensive care model, the ''Pennsylvania experiment," took a subset of students out of the large school-based clinic and linked them to faculty-based private practices (Cohen et al., 1985, 1991). In general, differences in the way schools implement comprehensive care involve both practical realities and pedagogical concerns.
The practical challenges of implementing comprehensive care in dental schools are taxing. They involve (1) finding and financing appropriate physical space; (2) recruiting patients and matching patient needs with individual student needs to gain competency in specific procedures; (3) increasing faculty work loads and accountability; (4) locating and integrating qualified part-time faculty; and (5) managing disciplinary tensions. Many of these challenges are discussed further in Chapter 6, which considers the patient care activities of the dental school from a patient's rather than a student's perspective. In general, "some features of practice, such as the total management of each patient, the care of large and diverse groups of patients, and the operation of a dental office are not easily simulated in a dental school" (AADS and Kellogg Foundation, 1980, p. 20).
Most of the schools visited by the committee acknowledged that their implementation of comprehensive care involved less-than-ideal compromises—political, logistical, and financial. For example, the University of Pennsylvania dental school, despite concluding that its experimental practice was educationally desir-
able and financially feasible on a small scale, has not found it feasible to expand the model to cover all students (Cohen et al., 1991).
Columbia University concluded both that introduction to comprehensive care in the third dental year was premature and that a single (fourth) year of comprehensive care was insufficient preparation for entry-level practice (Formicola, 1991). Accordingly, Columbia concluded, as did Pennsylvania, that a postgraduate year was an essential supplement to its predoctoral comprehensive care program (Cohen, 1985; Formicola, 1991). A later section of this chapter discusses the need for a postgraduate year of education in general dentistry.
A pedagogic debate in comprehensive care focuses on the use of general faculty to instruct students in basic specialty procedures that are frequently performed by general dentists (Hasler, 1984). Some dental educators argue that few generalist faculty have advanced training in the procedures they supervise. Others are concerned that "calibrating" assessments of student competency will be difficult if comprehensive care faculty come from different disciplines. This is a particular issue in comprehensive care clinics because of their greater attention to the nonprocedural elements of care (e.g., evaluation and treatment planning) (Baughan et al., 1993).
Educational Inefficiencies
Although dental schools vary considerably and detailed comparative data are generally unavailable, the committee became concerned that many if not most dental students learn in settings that are neither clinically nor educationally efficient. Students stand in line for supplies, collect patient payments, lack assistance from allied personnel, wait for faculty review of their work, and undertake clerical functions neither essential to their education nor routine in practice. The emphasis on procedures rather than on patient care means that students may be assigned to complete procedures from start to finish even when they are so inexperienced that hours of extra time are required. In some schools, outdated arrangements of facilities produce some gross wastes of student time (for example, in one school, students must run up and down the escalators from the clinic floor to the cashier floor to handle patient payments).
These inefficiencies add to the student's overcrowded week, squander patient time, and provide an inappropriate model of patient care. Dental educators recognized the minimal educational value of having students collect patient payments, but clinic managers
told the committee that they could not afford to hire clerks to handle this responsibility and that patient payment before receipt of service was essential to financial survival. Similarly, educators often acknowledged that student clinics are generally understaffed with allied dental professionals but argued that they would further increase the clinic deficit by hiring more such personnel. Several of the schools visited by the committee were acutely aware of physical plant problems and had substantial renovations of their patient care space planned, under way, or recently completed.
Chapter 6, which looks at these circumstances from a patient's perspective, argues that dental schools must change their approach to patient care for ethical and practical reasons. In a health care environment marked by significant restructuring and serious challenges to the economic position of academic health centers, dental school clinics are poorly positioned to attract the growing numbers of insured patients (with or without health care reform) and to help the academic health center compete for health plan contracts.
In the broader context of the university and academic health center, efficiency considerations may argue for studies to determine whether consolidation of some aspects of the dental curriculum with other educational programs could generate administrative and personnel savings with no harm to (and, possibly, enhancement of) educational objectives. Although not a matter of efficiency per se, opening some dental school courses to students from other programs such as physical anthropology would make a modest contribution to reducing the isolation of dental schools, as discussed further in Chapter 7.
Rebalancing an Overcrowded Curriculum
The combination of scientific and technological advances, academic traditions, and commitment to a four-year program has generated a curriculum widely regarded as overcrowded. With the conventional 40-hour work week used for comparison, the average dental student spends 30 hours in scheduled lectures, laboratory, or clinic work and has just 10 (theoretically) unscheduled daytime hours. Little of the formal curriculum is organized around the active learning strategies described earlier, and little time is left for critical reflection, consolidation of concepts and information, supplementary reading, or consultation with faculty.
The year as well as the week is packed with requirements. Only a handful of schools leave summers free for students to refresh themselves physically and mentally or to enlarge their
education through discretionary research projects or off-campus clinical experience. Free summers would also allow students to earn money for tuition and might alleviate the need for outside employment during the school year.
Virtually every dean who met with committee members spoke of efforts to reevaluate and redesign the curriculum so as to reduce-inappropriate duplication or overlap among courses; to set priorities for identifying content that has greater relevance for today's students and tomorrow's practitioners; and to find more time-efficient ways of teaching. Severe financial pressure can stimulate "downsizing," but the political realities of academia may lead to cuts based more on the relative power of different disciplines and individuals than on expectations about the educational needs of future practitioners. In its site visits, the committee found instances in which the curriculum had been pruned, but efforts to prevent regrowth were not always successful. That is, if a curriculum committee was successful in cutting back in certain areas, the pressure to add elsewhere was difficult to resist.
One challenge in curriculum change involves the cost—or even the feasibility—of obtaining data, for example, that (1) identify the specific courses in a given school that have overlapping material; (2) correlate the emphases in clinical instruction with the actual and desirable content of current dental practice; and (3) document the effectiveness (related to cost) of alternative instructional methods. As described in the background paper by Bader and Shugars and in Chapter 8, the third task is complicated by questions about the validity and reliability of measures of professional competency. Other obstacles relate to shortages of faculty trained to employ new teaching methods and limited availability of instructional software and related hardware tailored to the particular requirements of dental education (which constitutes a relatively small market).
These difficulties notwithstanding, the committee concluded that curriculum restructuring should be a high priority. Among the emphases should be the balance between facts and concepts in basic science courses, and the reexamination of heavy work loads in preclinical technique.
Dentistry and Medicine
The environmental changes alluded to above are among the factors contributing to new interest in the relationship between dentistry and medicine. Debates about this relationship are centuries old. In Europe, dentistry was often a specialty of medicine, and all
dentists had medical degrees, but the recent trend has been toward separate programs and degrees as found in the United States.
Since the first U.S. dental school was founded a century and a half ago, medical and dental schools have been separate. Integration of classes and other experiences exists in some institutions. For example, the University of Connecticut has completely integrated education in the basic sciences, and Columbia University has integrated most of the lecture portion of basic science education but still groups dental students together for smaller seminars and work groups. Several dental schools provide elective medical clerkships directed by internists. At the graduate level, hospital-based residency programs typically require residents to take medical rotations, and many oral and maxillofacial surgery programs award a medical degree after five years of training.
The scientific, clinical, and epidemiological literature and the committee's interviews with deans, faculty, students, and leaders of dental professional organizations—all point to changes in oral health care that will make the acquisition of additional knowledge of systemic disease and medical interventions more important in the future. Among these changes are the following:
- 'The technology used to prevent and treat oral diseases will increasingly involve diagnostic, pharmacological, and other interventions that demand medical knowledge. As described in Chapter 3 and in the background papers, advances in the biomedical and clinical sciences will almost certainly accelerate this trend.
- Medically complicated or compromised patients, particularly the elderly, are becoming a larger segment of dental practice. Treatment for these patients must take their systemic health problems and their typical use of multiple prescription drugs and nonprescription drugs into account.
- A growing number of dentists will be employed or practicing in large multispecialty practices, staff and group model health maintenance organizations (HMOs), and similar settings. Appropriate clinical experience in medicine may help them function more comfortably in these environments, particularly if the stress is on a broad scope of generalist care.
Meeting the challenges of changing technology, patient mix, and work setting will require changes in the relationship between dentistry and medicine. The options range from marginal change in dental education to complete integration. The committee discussed this relationship at length. It concluded that marginal change is insufficient but beyond this found considerable disagreement
on directions. Although the discussion below focuses on the relationship between medicine and dentistry, the committee notes the important relationships between dentistry and other health professions, a point emphasized in Chapter 3. That chapter recommends that dental educators work with colleagues in the other health professions to emphasize these relationships and to experiment with new strategies in didactic and clinical instruction.
Closer Integration as an Alternative. In the view of most committee members, closer integration of dentistry and medicine is a reasonable and desirable objective, one that might take a number of specific forms and one that a few schools have already adopted in some form. The committee's emphasis was not on institutional arrangements or degrees but on educational and clinical substance.
Although many variants on the details are possible, closer integration would generally involve the following elements. First, dental students would take basic science courses that would be the same as or similar to those taken by medical students and that would generally be taught by the same faculty. The content of courses, whether taught on a separate or an integrated basis, would reflect the principles of clinical relevance and critical thinking discussed earlier in this chapter. Second, basic science courses for dental and medical students, whether or not taught jointly, would include conditions or problems relevant to oral disease and would not, in any case, be divorced from clinical care. Early exposure to patients would, whenever Possible, be joint with medical students and thus include a wide range of patients. Third, dental students would have required clerkships in relevant areas of medicine (e.g., physical evaluation of hospitalized and ambulatory patients, urgent care and emergency medicine, pediatrics, and geriatrics), with options for additional training. Fourth, dental faculty would have sufficient experience in clinical medicine so that they—and not just physicians—could impart medical knowledge to dental students and serve as role models for them. Fifth, dental licensure examinations would be redesigned to increase the emphasis on critical thinking and clinically relevant knowledge of systemic disease and physiology. This change is desirable in any case.
Whatever the form, closer integration of dentistry with medicine would still entail fundamental changes for students, faculty, and institutions. These changes would be demanding to plan and implement and could not be expected to occur quickly or painlessly. During site visits, university and dental school
officials sympathetic to the concept of closer integration explained to committee members why they were not moving more quickly or fully to integrate medical and dental education. From a purely practical perspective, the lack of large enough classrooms and the complexities of class scheduling are important barriers to joint education. Likewise, building medical knowledge within the dental faculty takes time and money and would likely require a combination of faculty development and recruitment of new faculty.
Another concern involves the preparation of entering students. Entering medical students have higher grade point averages—3.45 compared with 3.09 for dental students (on a 4-point scale) (Jonas et al., 1993). Eighty-six percent of medical students have a baccalaureate degree as their highest degree compared to 65 percent of dental students. Such differences may put dental students at a disadvantage in shared courses. In addition, if dental students still were differentiated by a heavy load of preclinical courses, then they would be at a further disadvantage compared with medical students. The committee has already argued that the necessity of this work load needs to be reexamined.
Student qualifications aside, even educators who favored joint predoctoral education argued that some differentiation in curriculum was essential. Oral biology and other topics of special relevance to dental practitioners require special emphasis.
Although more of the burden of change might fall on dental schools, medical schools would also have to make curriculum adjustments and widen their perspectives so that future generalist and specialty physicians would regard oral health as a part of their concern with total health. With or without further integration and as already argued, it is this committee's sense that basic science faculty affiliated with medical schools need to be more accountable for the education of dental students and any other nonmedical students they teach. The research implications of current organizational structures are discussed in Chapter 5, and the financial aspects of various kinds of consolidation are discussed in Chapter 7.
Even without such additional challenges, change in medical schools is not easy. Early on, this chapter noted that medical education as currently organized has been seriously criticized for inadequacies in predoctoral basic science education and overspecialization in graduate medical education. Moreover, many medical schools are likely to be preoccupied in coming years with the pressures created by health care restructuring (as discussed more
generally in Chapter 6). Many of these changes should, however, bring the schools closer to the prevention and primary care orientation of dentistry.
Despite its recognition of the difficulties of more closely integrating dental and medical education, the majority of the committee believed that such integration is necessary to prepare dental practitioners for a future characterized by more medical management of oral health problems and more patients with complex medical problems. Within the general framework suggested above, dental and medical educators have a variety of options they can test and revise.
Dentistry as a Medical Specialty? The most far-reaching option is for dentistry to become a medical specialty fully integrated with medicine in the way that otolaryngology and ophthalmology are. Although some committee members believed this was a desirable long-term direction, the majority of the committee disagreed or was unconvinced. Despite this disagreement, however, the committee felt that steps by individual universities and states to test this or similar approaches would be desirable and instructive if undertaken with foundation or government support for a formal, integrated evaluation of the effort.
The case for this option rests, in large part, on the scientific, demographic, and organizational trends noted above. Combining courses and faculty also could help counter what some see as unsustainable increases in the cost of medical and dental education. In addition, as dentistry moves closer to medicine and as medicine moves toward generalist practice, practitioners will become better prepared to work as part of a health care team in a more integrated health care system.
Against complete integration are arguments that clinical, organizational, legal, economic, and cultural considerations make the objective sufficiently unrealistic that it would distract attention from more achievable but still major changes. These considerations include the need for significant, politically difficult revisions of state practice acts; the requirement that major university components be restructured; the realignment of responsibilities across existing and possibly new professional categories; and the uncertain impact of such realignments on the quality of care. A further argument against converting dentistry to a medical specialty that requires additional years of specialty training (following the pattern of ophthalmology or otolaryngology) is that the cost of education for general dental practice could increase substantially, which, in turn, could lead to higher fees for dentists' services.
To reduce the length of the total pre- and postdoctoral program for those who sought careers in dentistry and thereby trim educational costs, an alternative to the traditional medical model might be devised that would create an early specialization track for dentistry at the predoctoral level. Medicine and dentistry have, generally, rejected predoctoral specialization, so this would be a considerable innovation. In any case, it is not clear whether a special track for dentistry within medical schools would qualify as ''complete integration" rather than "closer integration" of medicine and dentistry.
A more conventional (but still controversial) approach to cost concerns would be to delegate more care to allied dental personnel working under the supervision of dentist physicians who provide more complex medical and surgical services. Proponents of this view cite evidence that existing or new categories of allied dental practitioners can be trained to perform safely and effectively some of the more common tasks now performed by dentists (Burt and Eklund, 1992; Freed and Perry, 1992; see also the background paper by Tedesco). A more complex and difficult alternative would be the creation of a new category of advanced allied dental professionals whose education and scope of practice include many restorative services and whose education might involve a five-year baccalaureate program similar to that for pharmacists.
Although some redefinition of professional roles appears crucial to the feasibility of converting dentistry into a medical specialty, this committee did not have the resources to estimate the net effects on costs and quality of care of the options suggested above. It encourages the appropriate government agencies to pursue these questions and to support further testing of these and other strategies for the use of allied dental personnel. The committee was also unanimous in encouraging dental and medical schools to continue and expand experiments with combined medicine-dentistry programs for interested students and residents. This combination of experiments with new steps and extensions of previously tested strategies should help prepare future policymakers and educators to make more informed judgments about the oral health work force in the face of continued scientific, technological, economic, and other changes.
Advanced Education
Today, dental school graduates have two broad options in pursuing advanced clinical training—one that focuses on general dentistry and the other, on education in one of the dental specialties.
The first option was the subject of the most controversy and attention during the committee's work.
Currently, first-year postdoctoral positions are available for approximately 60 percent of graduating dentists. These positions are split about evenly between eight specialist and two general dentistry categories (Table 4.2). Virtually all of the growth in the number of positions has been accounted for by the growth in general dentistry positions. The total number of specialty positions has stayed essentially steady. However, because the number of dental graduates has decreased since the 1970s, the proportion of all dentists who are specialists has been increasing.
Advanced Education in General Dentistry
In contrast to medicine, substantial numbers of dental students do not pursue residency training alter graduation. Yet, the emphasis in most dental schools on preparing students to be competent, entry-level general practitioners upon graduation puts a considerable burden on both schools and students. As discussed earlier, some have concluded that students need a postgraduate year of broad but supervised experience in general dentistry to make the transition from dental graduate to competent entry-level practitioner.
History and Development
Hospital-based general practice residency (GPR) programs have been formally evaluated and accredited since the late 1940s, although such residencies date back at least to the 1920s (Santangelo, 1987; AADS, 1994a). Other postgraduate programs in specialty areas were not explicitly approved until the 1960s. In 1977, the AADS urged that programs of advanced education in general dentistry (AEGD) be approved for nonhospital sites, consistent with dentistry's focus on comprehensive care and care outside the inpatient setting. In 1979, the ADA authorized this step.
The concept of advanced education in general dentistry was given a strong boost in 1980 by an AADS task force funded by the W.H. Kellogg Foundation. That group recommended that "the number of positions in general practice residencies and other advanced dental education programs ... be increased to accommodate approximately one-half of the dental school graduates by the mid-1980s" (AADS and W.K. Kellogg Foundation, 1980, p. 6).
The postgraduate year in general dentistry (PGY1) has sometimes been referred to as a fifth year, but this terminology implies
TABLE 4.2
First-Year Enrollment in Advanced General and Specialty Education Programs
to many a fifth predoctoral year (Gray, 1987). As recommended by this committee, neither the AEGD nor the GPR should be regarded as an extension or revision of the predoctoral curriculum; rather, each should provide a period of greater independence and responsibility for complex patient care.
Although GPR positions outnumber AEGD positions, the number of GPR slots has been declining, and changes in Medicare payments for graduate medical education may lead to further declines. Since 1978, the federal government has invested nearly $40 million in support of postgraduate general dentistry (Handelman et al., 1993). For FY 1993, the appropriation for this area was $3,730,000.
It does not appear that advanced education in general dentistry serves as a prelude to specialization. One recent study indicates that nearly 90 percent of graduates with such training remained in general practice (Handelman et al., 1993).
Britain now requires dental graduates to participate in what is termed a ''vocational" year of office-based training before they begin general practice, and other European nations appear to be moving in this direction (AADS, 1994a). Many advocate a similar requirement for this country under the AEGD or PGY1 label.
Issues and Controversies
As described in an earlier section, the existing predoctoral curriculum is so burdened with coursework and acquisition of technical skills that students have little time to integrate their skills and knowledge as envisioned in the concept of comprehensive patient care. This deficiency is a particular problem for general dentists, whose responsibilities for primary care require comprehensive management of all patient care, whether it is provided directly or referred to specialists as appropriate. The problem is analogous to that in medicine before graduate medical education was universally accepted. A year of postgraduate or advanced education in general dentistry would allow students to gain speed and confidence in procedures, broaden their patient management skills to cover more complex problems, and mature in the nontechnical aspects of patient care.
Curriculum reform that emphasizes comprehensive patient care and other restructuring and pruning of the dental curriculum should improve student readiness to enter practice. The postgraduate year should not be seen as a way of avoiding such reform. Conversely, predoctoral curriculum change is not a substitute for a postgraduate year. This committee believes that all graduates of U.S. dental schools should have the opportunity to round out and
refine their predoctoral work through a supervised and accredited postgraduate experience. This is not possible now.
One estimate is that demand for AEGD or GPR positions exceeds supply by about 400 positions (AADS, 1994a). During site visits, liaison panel meetings, and other activities, the committee often heard that those most in need of the advanced year were the least successful in competing for available positions (see also Little St. Simons Conference, 1993). The demand for AEGD and general practice residencies is cited by some as evidence that students do not feel adequately prepared for practice (Garrison, 1993).
An exception to this supply-demand imbalance was reported by the U.S. Department of Defense (DOD) in its testimony to the committee (Martin, 1993). In contrast to the past, the department now cannot fill all its one-year GPR positions. The testimony cited the increased number of residencies in the civilian sector (often in more appealing locations) as well as DOD's relatively low salaries and limited provisions for scholarships or loan forgiveness. Dental educators and DOD officials have a mutual interest in identifying how unfilled residencies might be made more attractive, for example, through changes in federal or other policies regarding loan forgiveness or payback arrangements.
The expectation of postgraduate experience would increase the flexibility of dental schools to modify their predoctoral curricula to encompass advances in dental practice and research. More than three-quarters of the deans agreed that building or sustaining a strong postdoctoral general dentistry program was a priority, although a slightly higher percentage agreed that a strong postdoctoral specialty program was a priority. Slightly more than 60 percent of deans surveyed for this report agreed that a year of postgraduate training should be required by 2005.
The qualifications to the endorsement of a required postgraduate year are primarily practical not philosophical. The major obstacles to such a requirement and indeed to the more modest recommendation of this committee are fiscal. Financial pressures on hospitals have resulted in a modest decline in the number of hospital-based general dentistry programs, and uncertainties over future funding for graduate medical education may have Some spillover effects on dentistry.6 Startup funding from the U.S. Pub-
lic Health Service is often available for AEGD programs, but continued funding generally requires creative efforts to supplement routine patient care revenues with additional funding sources including federal and state programs for disadvantaged groups. To the extent that faculty practice plans expand their patient base and revenues, they may also offer opportunities for postgraduate training. Creating appropriately structured, stipend-paying residency positions demands a substantial investment of administrative and faculty time—and favorable local conditions.
In addition, to make postgraduate education a requirement for licensure, each state would have to revise its statutes, a daunting prospect. Another consideration is student resistance; some students say they do not need additional training and balk at the economic opportunity cost of delaying their entrance into private practice. In light of these concerns, the committee chose to recommend increased opportunities rather than requirements for residencies. As these opportunities are expanded and their relative benefits and costs are studied further, the case for or against a requirement should become clearer.
Other concerns involve the availability of general practice faculty to teach advanced students and a shortage of patients with treatment needs consistent with students' educational program. The latter is already a problem for some predoctoral student clinics. Although expanded coverage of dental care under health care reform might not make predoctoral clinics more attractive, AEGD clinics might very well be able to attract patients newly able to afford dental care. Two models proposed to expand the availability of postgraduate positions would place students in university-affiliated private offices and in community clinics such as those funded by the federal government to provide care in underserved areas. In some instances, the development of additional sites for advanced education may lay the foundation for schools to use the same sites for extramural predoctoral education.
Advanced Specialty Education
As described in Chapter 2, the first specialty programs were established a century ago, but they were slow to proliferate. Specialty standards were first developed in the 1940s but an accreditation program did not begin until the 1960s. Today, eight recognized dental specialties have 421 accredited programs in dental schools and other institutions. Table 4.2 lists the specialties and
their first-year enrollments. Chapter 8 and the background paper consider regulatory issues related to dental specialties.
Many of the issues raised in the discussion of predoctoral education apply broadly to all aspects of dental education and practice. These issues can be rephrased so that they speak to the importance of advanced specialty education that
- emphasizes the scientific basis of the Specialty;
- promotes critical thinking about the effectiveness of alternative treatments including the options of generalist care or continued observation;
- focuses on the patient not the procedure; and
- prepares practitioners to treat medically complicated patients and work with medical specialists and generalists as appropriate.
As presented to this committee, the primary concerns about the distinctive content and quality of specialist education dealt with how they prepared individuals for research or teaching rather than clinical careers. Although most specialist curricula include exposure to the scientific method and literature, the primary focus is clinical proficiency, not the generation or evaluation of new knowledge. Some schools provide more scientific training in programs leading to a master's degree than in programs leading to a specialty certificate, but this is not universal. Such programs may help prepare clinical faculty to teach with a greater appreciation of dentistry's science base and to participate as partners in clinical research under the direction of full-fledged researchers. Notwithstanding these benefits, such program do not and should not be expected to prepare students for a research career.
Accordingly, those involved in faculty recruitment and development should not mistake acquisition of a master's degree with academic preparation for a research career. Likewise, educators interested in developing a serious research training component within a dental school should focus on programs leading to a doctorate not a master's degree. This argument is reinforced in Chapter 5.
In presentations to the committee, some groups were worried that insufficient numbers were being trained in particular specialties, for instance, pediatric and public health dentistry (AAPD, 1993; AAPHD, 1993; ABDPH, 1993; ASTDD, 1993).7 In site vis-
its, schools expressed concern about the availability of oral pathologists. More common was a concern that the proportion of specialists was increasing in dentistry because the number of specialists being trained had remained fairly steady while the number of dental graduates had dropped. These concerns do not relate, for the most part, to specialty curricula but to work force issues. In Chapter 9, the committee cautions against a decrease in dental schools' focus on generalist education, but it found few data or analyses on which to base conclusions about requirements for individual specialties. Unlike medicine, restrictions on dental specialty training have not figured in the debates about health care reform.
A quite different set of concerns about advanced specialty education related to its reinforcing of faculty organization by specialty category. The committee heard arguments that curriculum reform is impeded by this organizational structure and by faculty interests and attachments to particular specialties. Further, legitimate questions can be asked about whether disproportionate resources are devoted to graduate specialty education. The committee found few data on the allocation of resources between predoctoral and advanced dental education. One dean reported that 30 percent of faculty effort at his school is directed to advanced education, which accounts for 10 percent of enrollment<m>but 45 percent of clinic revenues (Hunt, 1993). An expert in financial administration reported that the cost of educating a graduate specialty student is 70 percent higher than the cost of educating a predoctoral student (Consani, 1993). Whether these figures are typical or, in any case, whether they represent disproportionate emphasis, the committee could not determine.
Continuing education
One of the guiding Principles for this study was that learning is a lifelong enterprise for dental practitioners. It cannot stop with the awarding of a degree or the completion of a residency pro
|
|
with less than average health status) not clinical services for individuals. Because their work constitutes a public good and because the income expectations for public health dentist are comparatively low, subsidized education programs in this specialty were cited as especially important. Congress reauthorized dental public health training in 1992 but adequate funding is in doubt. Oral pathology is another specialty that does not emphasize individual patient care. |
gram. Continuing dental education is part of the continuum of education, and dental schools are obvious sources of continuing education that covers advances in relevant scientific fields, provides critical appraisals of new technologies, and incorporates an evaluation component that draws on faculty research skills to assess the impact of different approaches to continuing education. Interest in the effectiveness of continuing education is likely to grow as more public attention focuses on methods of documenting and continuously improving the performance of established practitioners (Nash et al., 1993; Horn and Hopkins, 1994). Although evidence of the positive—or negative—effects of traditional programs is limited (Bader, 1987; Davis et al., 1992), the issue for educators and policymakers is not whether continuing education is necessary but what methods or formats are most effective in reaching particular educational objectives.
In the deans' survey, continuing education was rated as highly or very highly important for 41 of the 54 schools. Only one dean reported it low in importance, and 12 responded that it was moderately important. Thirty-two deans (59 percent) responded that continuing education would be either more or much more important in the future. None of the deans reported that providing continuing education would be less important in the future. Questions remain, however, about whether dental and medical schools are prepared to invest resources in lifelong learning programs for dental professionals that are based on practitioners' concerns, patients' needs, and practice realities (Chambers, 1992b; Davis and Parboosingh, 1993).
Options for Continuing Education
The committee found a range of continuing education offerings, representing wide differences in intensity and scope. The offerings are not easily ranked in quality and depth. Some obviously provide more complete education and evaluation than others, and some might actually be harmful if they provide inadequate instruction but give participants a false sense of competency. Some programs include clinical experience; others are purely didactic. Not all qualify for continuing education credits.
The array of course media includes audio and video cassettes, computer modules, cable TV programs, and personal instruction. Instruction may occur in quite disparate settings. Some involve weekend or day courses at hotels or resorts or sessions at professional conferences. Informal study clubs may meet in partici-
pants' homes or offices. Dental schools offer a variety of programs both on-site and in outlying locations arranged by the schools. Every major general dentistry and specialty organization, many producers of dental equipment and other products, and a variety of other organizations sponsor continuing education courses.
In its site visits, the committee found varying levels of dental school involvement in continuing education. School location, traditions, faculty interest, and available market influence school decisions. One school visited by the committee was increasing its continuing education programs to improve relations between alumni and practitioner. Continuing education programs may, like faculty practice plans, provide a way to supplement faculty salaries. Some schools, however, reported that the costs of providing continuing education exceeded the revenues generated from course fees, making it a financial drain on the school when it was expected to generate a surplus.
In principle, dental schools have the advantage of facilities specifically designed for clinical education and ready access to a diverse faculty including educators, researchers, and practitioners. In actuality, they may not successfully mobilize or build upon these advantages to serve and attract practitioners (Chambers, 1992b). In the future, educational and other support might come in unconventional formats such as computer-based information or interactive consulting services. Improved communication links between schools and practitioners also may offer a base for extending research opportunities as discussed in Chapter 5.
Active state support for the area health education centers (AHEC) program facilitates dental school involvement in continuing education. At the University of North Carolina (UNC) at Chapel Hill, for example, the AHEC program supports continuing health professions education by deploying the university's faculty throughout the state. The state has designated specific funds for a portion of faculty time, facilities, transportation, and similar costs. Because the AHEC program is academic health center wide, it also links the dental school to other health professions schools at the UNC. In Washington State, which also has a strong AHEC program, the University of Washington dental school is extensively involved in continuing dental education.
Accreditation and Evaluation
Following the path of other health professions, the AADS section on continuing education has endorsed a set of accreditation
standards for sponsors and providers (AADS, 1992).8 In 1989, the ADA Board of Trustees adopted a resolution to consider an evaluation and approval mechanism for continuing education that would address concerns about quality and the need for certification of programs and instructors (ADA, 1992c). After considerable work on an initial proposal by the Council on Dental Education, the ADA board appointed a committee to work with representatives from each of the specialties, the American Association of Dental Examiners (AADE), the AADS, and the Academy of General Dentistry (AGD) to develop a continuing dental education Provider Recognition Program (PRP). That committee recommended adoption of a PRP that would certify providers or programs, not individual courses, to ensure quality and reputability. The committee also recommended establishment of a PRP steering committee and a review committee on continuing dental education. In early 1993, the Continuing Education Recognition Program was established under the auspices of the ADA in cooperation with 11 other national dental organizations (ADA, CERP, 1993a).
As noted above, little is known about the effectiveness of alternative methods of continuing education or about the specific methods best suited for topics as diverse as patient education and implant materials and techniques. Moreover, the availability of a sound continuing education course does not guarantee that those who enroll will actually participate, learn, and then practice what they learn. Skepticism about the value of participation in continuing education courses as a proxy for competency in practice is common, even among its supporters. This skepticism echoes more general reservations about the impact of education and information as vehicles for influencing practitioner behavior (Eisenberg, 1986; Lomas, 1991; Kibbe et al., 1994). It reinforces the call for a stronger emphasis on evaluation of the effectiveness of different methods and formats; such evaluation should, in turn, provide dental faculty with additional research opportunities.
Requirements for Continuing Education
Prior to 1980, only 9 of the 52 states and territories (including the District of Columbia and Puerto Rico) required continued education for dentists (ADA, Department of State Government Affairs, 1994). By January 1994, 40 of 52 dental boards required—as a condition for relicensure—some sort of continuing education credit hours for dentists over a one- to five-year period; 43 required such credits of dental hygienists. Continuing education requirements are relatively uncontroversial among practitioners compared to other measures such as periodic written or clinical examinations or review of patient records.
Although the committee viewed continuing education as part of the process of continued professional development, it also believed that state boards should move beyond continuing education requirements as a measure of continued competency. Boards should work with others in the dental community to develop pilot projects to identify practical methods of measuring professional performance for established practitioners. A recent draft report from the AADE describes several alternatives including inoffice audits, simulated case evaluations, the AGD's fellowship examination, and the diplomate examinations administered by specialty societies (AADE, 1993a). Chapter 8 examines this issue in the context of state licensure requirements.
Faculty
The day-to-day fulfillment of the educational mission of dental schools depends on the quality and commitment of their faculty. Whether students enter practice with appropriate clinical skills and with critical thinking skills to guide them throughout their careers and whether they leave with positive attitudes about dental education depend largely on faculty. In addition, faculty contribute significantly to the development of new knowledge in oral health and to the care of patients.
It is the sense of this committee that several of the problems described in this report arise, in part, because dental faculty are too little involved with educational, clinical, and scientific contacts outside their clinical or basic science departments. They are thus isolated
- from the rest of the university and academic health center;
- from researchers in government, industry, and other universities;
- from the challenges and demands of active patient care; and
- from dentist colleagues in the community.
The task of reducing isolation is addressed throughout this report. This section focuses on initiatives by dental schools to achieve new relationships among faculty and between faculty and university administration. Among the dental schools visited by the committee, such initiatives had included the consolidation of traditional departments into larger units, the establishment of active curriculum committees, the formal study of the content and interrelationships of courses, the introduction or expansion of faculty development programs, and even the adoption of early retirement programs.
Such structural and procedural changes have the potential positive effects of focusing governance arguments on the relative contribution of parts to the whole rather than on the merits of the parts in isolation. If carefully implemented, they may reduce the administrative costs associated with small departments, make it easier to gather empirical information about what is actually happening in the school, and disturb practices justified mainly by their long existence.
Even if undertaken in a spirit of sensitivity and cooperation, however, these initiatives have potential negative effects as well. For example, they may create new organizational layers, interests, and paperwork. Some steps, such as early retirement programs, may divert resources away from other, perhaps better, uses and may create jealousy. Departmental consolidation may hamper recruitment of talented individuals who see traditional units as providing greater autonomy and control over resources. Restructuring may have the added p purpose of saving money, but such savings may prove elusive. If the changes do not work as promised, they may reinforce the not inconsiderable cynicism that already exists inside and outside the university about proposals for educational restructuring and reform.
Provisions for tenure and legal prohibitions against mandatory retirement make it difficult to restructure the faculty, particularly during periods of relative stasis or decline in resources. Universities like most organizations have considerable reluctance to disrupt current personnel and constituencies in favor of personnel and constituencies whose influence—indeed existence—lies largely in the future.
The discussion below starts with a statistical profile of the dental faculty and continues with an overview of several central issues including faculty isolation, scholarship, tenure, and faculty development.
Statistical Profile
In 1968, before the surge in dental school enrollments, the 52 existing dental schools had about 2,800 full-time basic science and clinical faculty, not quite 4,400 part-time faculty, and 15,400 students. Eighty-five percent of the part-time faculty—about 925 full-time equivalent positions—were clinical (AADS, 1993b).
In 1992, after the number of schools had grown to 60 and then fallen back to 55, dental schools had more than 3,300 full-time faculty in the basic and clinical sciences, more than 6,700 part-time faculty, and slightly less than 16,000 students. About 93 percent of the part-time faculty (or 1,275 full-time equivalents [FTEs]) were on the clinical side. As a percentage of full-time faculty, those in basic science dropped from 42 to 25 percent of the total during the same period.
Figure 4.3 show trends in the numbers of full-time and part-time faculty in the sciences. As a percentage of FTE clinical positions, part-time faculty dropped from 36 percent of the total in 1968 to 28 percent in 1992. ADA figures for 1992-1993 show that
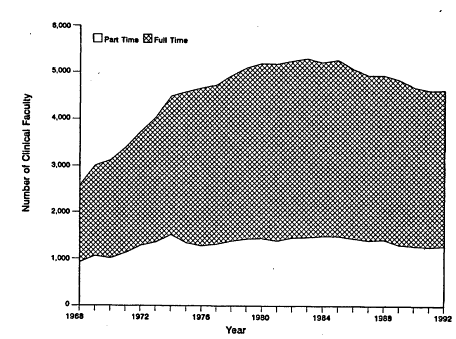
Figure 4.3
Trends in numbers of full-time and part-time clinical faculty.
Source: American Association of Dental Schools, 1993b.
part-time clinical faculty range from lows of 0 and 17 percent of the total clinical faculty at the University of North Carolina and the University of Florida (both public schools) to highs of 93 and 94 percent at Tufts University and the University of Southern California (both private schools).
According to AADS figures, in 1992, 19 percent of dental school faculty were women, and the percentages varied little between full-time and part-time faculty. About 4 percent of faculty were African-Americans; other minorities comprised about 8 percent.
Issues
Dental school faculty are clearly a diverse group with quite varied training, responsibilities, and concerns. Basic science and clinical faculty tend to have quite different responsibilities, work loads, and interactions with students. In general, clinical faculty spend more hours teaching or supervising clinic work and, thus, spend more time with students. The combination of these hours and any hours spent in a faculty practice plan will tend to leave clinical faculty with less time for research compared with basic science faculty.
Among clinical faculty, some have dental degrees, others have Ph.D.s, and some have both. Some have postgraduate specialty training; others have none. Some teach full-time; others, part-time. Some full-time faculty participate in faculty practice plans; others have no patients for whom they are directly responsible. Some are active researchers, but many clinical faculty have little or no involvement in research. Some have close ties to organized dentistry and local practitioners; others find such involvement uncomfortable. Faculty diversity enriches education, research, and patient care, but managing this diversity to achieve a balanced, high-quality faculty is a demanding task.
Faculty Development
One commentary recently observed that most schools spend a lot of time on recruitment, what they called the ''fish-and-catch'' phase of managing faculty resources (Bland and Ridky, 1993). The support and continual development of faculty once they are hired (i.e., caught) have been relatively neglected, with the major postrecruitment effort focused on tenure decisions. The reasons for this neglect of faculty development include lack of interest, and even resistance, from faculty themselves; management inat-
tention; funding problems; and methodological questions that are both typical of educational efforts generally and specific to those aimed at faculty (Blackburn, 1991). Evaluations of faculty development strategies are limited.
The development or even retraining of faculty at all stages of their careers is, however, becoming a practical if not a philosophical concern of the university and the dental school as they have had to cope with resource limitations, increased public scrutiny, deteriorating faculty morale, and faculty composition influenced by tenure as well as educational needs (Schuster and Wheeler, 1990; Parker, 1991). Because many current faculty are products of the very educational approaches critiqued in this chapter, implementation of new strategies may require that faculty be educated both to understand the rationales for change and to learn new skills. The same argument holds for the new expectations with respect to research and patient care outlined in Chapters 5 and 6.
The importance of faculty development is increasingly being recognized in dental schools. In 1990, the AADS identified faculty development as an action priority (see, generally, the Journal of Dental Education , October 1991). The standards of the Commission on Dental Accreditation state that "there must be a professional development program available for full-time faculty of dental schools" (CDA, 1993a, p. 4). In the committee's survey one question asked deans to rate priorities for faculty development over the next 15 years. Table 4.3 presents their responses. In an added
TABLE 4.3
Survey of Deans' Priorities for Dental School Faculty Development over the Next 15 Years
|
Weighted Rank |
Area |
|
In the next 15 years, what priority would you place on faculty development in these areas? |
|
|
1 |
a. Increasing sensitivity to student needs and concerns |
|
8 |
b. Developing administrative and management skills |
|
7 |
c. Developing facility with problem-based learning or similar strategies |
|
4 |
d. Developing competency-based evaluations of student clinical skills |
|
6 |
e. Using computer-based instructional tools |
|
3 |
f. Improving instructional tools |
|
5 |
g. Improving research skills |
|
2 |
h. Increasing emphasis on patient outcomes assessment |
|
SOURCE: Institute of Medicine and American Association of Dental Schools, 1994. |
|
comment, one dean noted that faculty development demanded a very heavy commitment of resources. Not only does it require resources to plan, develop, staff, and evaluate internal activities or to send faculty to outside programs, the more intensive efforts—for example, research training—may require that faculty be freed from other obligations. This, in turn, may require schools to bring in clinicians from the community to fill in for absent clinical faculty (Dirksen, 1992). Finding the appropriate person may. be difficult, particularly in smaller communities. These difficulties notwithstanding, the committee believes that faculty development programs are an important part of dental school efforts to adapt to a changing and resource-constrained environment.
As was evident in the committee's site visits and other activities, faculty development can take many forms and focus on a variety of objectives. The forms include seminars, workshops, written materials, editorial or technical assistance, peer assessment and guidance, and mentoring (Wheeler, 1991; Stritter, 1993). The broad objectives may be to develop teaching abilities, writing skills, research capabilities, or leadership talents. Less tangible than any of these objectives and methods is a much broader and more complex aim—building and sustaining talented and energetic faculty that are committed to the multiple missions of the dental school and the larger university and are intent on communicating their knowledge, enthusiasm, and dedication to students.
Faculty as Role Models
A related philosophical issue involves the ways in which faculty should serve as role models for students. To the extent that clinical faculty are not themselves engaged in patient care beyond the student clinic, they are often criticized as poor role models for their students, the great majority of whom will become full-time practitioners. Faculty who practice what they teach should find it easier to keep abreast of changing technologies and patient expectations. Being teachers as well as dentists, however, clinical faculty are particularly obligated to serve as role models of critical thinking in practice.
Faculty practice plans were recommended to the committee as a dual-purpose strategy to strengthen dental school faculties. On the one hand, they permit faculty salaries to be supplemented and made more competitive with private practice. On the other hand, they enhance faculty stature and experience by keeping them in
touch with the realities of practice and the challenges of critical thinking in that environment.
Two other dimensions of faculty as role models involve research, which is covered in the next chapter, and responsibility for student education in comprehensive patient care. As noted earlier, the committee heard competing views about the latter issue. One argument is that generalist faculty should take the lead in educating students in comprehensive patient care because they can best exemplify the general practice model and philosophy that is the foundation of most predoctoral programs. The competing view is that instruction in the kinds of periodontic, endodontic, and other conditions seen by general dentists—and either created by them or referred—requires faculty with advanced training. It is likely that both models can work if designed, implemented, and evaluated carefully.
In any case, the committee urges that one objective of faculty recruitment and development efforts be the establishing of faculty who are regarded as master clinicians in general practice, that is, qualified beyond the average general dentist. This objective, unfortunately, may conflict with the conventions of academic employment, in particular, compensation levels and tenure. More generally, because dental students tend to emerge from predoctoral and advanced education programs with very high levels of debt, graduates interested in academic careers may find that an entry-level academic appointment will make debt repayment difficult. Once they are established in private practice, these individuals may be reluctant to relinquish its pecuniary rewards even after they have reduced or eliminated their education debt. A number of the schools visited by the committee noted the irony of not being able to afford to hire their own top—but highly indebted—graduates.
Compensation
In common with other professional schools, dental schools can face difficulties in attracting qualified clinicians as educators and researchers because such individuals generally earn substantially higher incomes in private practice. Salary levels are typically higher in professional schools than elsewhere in universities, which may create jealousies elsewhere on campus.
Although the nonpecuniary benefits of teaching the next generation and of generating and disseminating new knowledge must be valued by faculty and nurtured by university and public offi-
cials, competitive salaries and benefits are essential. Unfortunately, in combination with the physical plant and equipment requirements of dental education, such compensation helps make dental schools expensive parts of their parent universities and academic health centers.
In medical schools, a major strategy for augmenting salaries for clinical faculties has been the faculty practice plan. This strategy, already mentioned in the discussion of role models, is examined further in the discussion of financing dental education in Chapter 7. That discussion notes that most revenues generated by practice plans are consumed either in patient care expenses or in supplements to faculty salaries, with little left for other educational purposes. Faculty practice also has nonfinancial benefits, particularly, as noted above, the increased involvement of faculty in actual patient care, not just in the supervision of patient care.
Tenure
In 1992, the percentage of full-time clinical faculty in dental schools who were tenured ranged from a low of 7 percent at Loma Linda University to a high of 96 percent at the State University of New York at Stony Brook. On average, about half of all such faculty are tenured. The percentage of full-time clinical faculty not eligible for tenure ranged from less than 5 percent at five schools to at least 50 percent at five other schools. Both the low end and the high end of the tenure continuum raised concerns for the committee. Earlier sections of this chapter have noted that tenure limits the flexibility of dental school in adapting to change and in restructuring the curriculum to remedy long-standing problems, and tenure may also act as a constraint on recruitment of a faculty that is more representative of the country's population. Very low levels of tenure combined with high ratios of part-time faculty may, however, deprive a school of a core of faculty committed primarily to the missions of the dental school rather than to the exigencies of private practice.
In principle, tenure rewards academic quality and protects intellectual freedom. The guiding statement on tenure, issued in 1940 by the American Association of University Professors, entitled "Statement of Principles on Academic Freedom and Tenure," refers to careful consideration of "accomplishments in teaching, scholarship, and college or university service" (AAUP, 1990). For health professions schools, the concept of service includes service to individual patients, and for higher education in general, the
concept now more generally includes service to the community and nation.
Most educators acknowledge that very few faculty can be "triple threats," excelling in research, teaching, and service, and those who excel primarily in the latter areas often have not fared well in tenure decisions. For that reason, many schools have altered tenure practices. One approach has been to revise the criteria for tenure to grant more recognition to teaching and service. If the principle of scholarly excellence is to be maintained and if "teaching [is] to be equal to research," then it must be ''vigorously assessed," a step that requires better methods for measuring performance (Boyer, 1990, p. 37; Stritter, 1993). Likewise, service must be assessed on the basis of academic as well as social relevance. In some cases, it is not clear what academic standards are being applied. The result may be a perception that teaching and patient care are relegated to second-class status (Scheetz and Mendel, 1993). The concern about how to assess performance in teaching for tenure-related purposes reinforces questions about measuring educational outcomes that are troublesome in many contexts including curriculum reform, licensure policies, and accreditation standards.
Rather than revise the terms of tenure, a second strategy has been to devise alternatives to tenure that may, to varying degrees, coexist with it and with institutional standards of excellence. These alternatives are highly varied, ranging from renewable contracts to increased reliance on part-time faculty to more generous sabbatical policies and other benefits for those who forgo tenure (Honan, 1994a).
Concerns about tenure have been intensified by the 1986 Age Discrimination in Employment Act, which prohibits mandatory retirement for most workers. Until 1994, colleges and universities were allowed to maintain mandatory retirement at age 70. A congressionally mandated study by the National Academy of Sciences concluded that most faculty would retire before age 70 at most institutions but that some research universities might have a high proportion of faculty working beyond that age (NRC, 1991). The study concluded that age itself did not affect institutional quality but that reduced faculty turnover and limited hiring flexibility did. They also affect efforts to create a faculty more representative of the broader population. Another 1991 study suggested that up to 10 percent of faculty at both private and public institutions of higher education would be over age 70 by the year 2000 (Honan, 1994b).
In this study's survey of deans, slightly more than 60 percent reported that their institutions had modified tenure criteria or adopted alternatives, and another 10 percent reported that they
were being considered. Nearly 80 percent of the deans favored alternative tracks.
Students
A historic and not always fair charge against colleges, universities, and academic health science centers is that students are often viewed as a peripheral burden by administrators and faculty, who are preoccupied with organizational charts, salaries and benefits, research, private practice or consulting activities, and academic politics. The committee was not surprised to hear this charge sometimes directed at dental schools, often by faculty and administrators as well as practitioners. Indeed, research on medical and dental student perceptions suggests that an unpleasant atmosphere created by clinical faculty is among the most stressful aspects of school life (Wolff et al., 1992; Westerman et al., 1993).
That dental educators have been reexamining their attitudes, practices, and objectives about students is suggested by responses to the committee's survey of deans cited above in Table 4.3. The most uniformly cited priority for faculty development was programs to increase faculty sensitivity to student needs and concerns: of 54 deans, 43 rated such programs a high priority, and 8 a moderate priority.
Regardless of the merits of charges about past behavior, several factors have made careful regard for students a priority for universities generally and dental schools in particular. Demographics— notably, the so-called baby bust and its accompanying "shortage" in the pool of young adults—has prompted educators to work harder to attract and retain students. The 1980s saw a substantial decrease in applications for admission to dental school combined with a decline in the "quality" of applicants as measured by grades and test scores, which are admittedly limited—although widely used—measures of qualifications. Schools risked closure if they could not attract a sufficient number and quality of students to satisfy university academic standards and maintain tuition revenues. Without the influx of women students described below, the situation would be much worse.
Statistical Profile
In 1993, 54 dental schools enrolled nearly 16,000 predoctoral dental students and graduated more than 3,800 (AADS, 1993b). An array of postdoctoral programs in both university and nonuniversity (e.g., hospital) settings enrolls nearly 4,600 students. In Table 4.2, first-year enrollments in advanced programs are listed. In
addition, university, community college, and other programs enroll about 10,000 dental hygienists, 6,000 dental assistants, and 1,000 dental laboratory technicians (AADS, 1993b).
In 1992, total predoctoral enrollment of dental students ranged from lows of 109 and 111 at Harvard and the State University of New York at Stony Brook, respectively (excluding Loyola, which closed in 1993), to highs of 520 and 1,145 at the University of Southern California and New York University, respectively.9 Figure 4.4 graphs dental schools grouped according to enrollment.
Among the 54 schools currently in operation, predoctoral enrollment has decreased since 1983 for 45 schools and increased for 9; all but 2 of the latter are private or private state-related schools. Between 1982 and 1992, total enrollment dropped 30 percent— from 22,235 to 15,980. The decreases are negligible for several schools, but others have cut enrollment by a quarter or even a half. Of the six public schools with more than 500 predoctoral students in 1983, none has as many as 400 students now. Of the seven private or private state-related schools with more than 500 students in 1983, two have closed, one has remained roughly steady in size, three have downsized by more than 20 percent, and one has increased its total enrollment by 80 percent.
Student enrollment statistics show great variability in state residence, gender, race, ethnicity, and graduation from foreign dental schools (ADA, 1993a, b, c). Nonresident enrollments range from 0 to 60 percent among public schools and from 7 to 94 percent among private and private state-related schools. The proportion of female students ranges from less than 15 percent at one school to slightly more than 50 percent at two schools. Two schools have majority African-American enrollments, but no other schools appear to have African-American enrollments equal to the group's representation in the general population. A few schools have near-majority enrollments of students of Asian origin, and Hispanic students constitute more than 20 percent of enrollment at a few schools. In Chapter 9, which considers a dental work force for the future, strategies to increase participation by underrepresented minorities are discussed.
Enrollment of foreign dental graduates ranges from a low of 0 in 20 schools (and only one or two students at 11 more schools) to
highs of 17 percent in two schools and 41 percent at one school (ADA, 1993e). The last school alone accounted for nearly half of all enrolled foreign dental graduates, and two-thirds of such graduates were enrolled in just four private institutions. As noted in the background paper by Capilouto et al., the number of foreign dental graduates admitted with advanced standing to U.S. dental schools has grown sharply, nearly doubling from 1990 to 1992.
Quality of Applicants and Graduates
Improving the quality of applicants and admitted students was clearly a priority (either self-chosen or externally dictated) at several of the schools visited by the committee. These schools pointed to recent improvements in student credentials but acknowledged that they could not say whether these improvements reflected their recruiting efforts or other factors such as the decreasing attractiveness of M.B.A. programs.
In the 1970s, increases in the number of dental school applicants and the ratio of applicants to enrollees were accompanied by increases in grade point averages and dental admission test scores (AADS, 1993b). The 1980s saw decreases in each area. Recent trends indicate improvements in applicant ratios and grade point averages. In addition, the attrition rate has dropped. In their survey responses, three-quarters of dental school deans agreed that dental school applicants were "better" today than five years ago. Although grade point averages were often mentioned during site visits and other meetings, the committee concluded that dental educators' views on shifts in student quality were not limited to this indicator but were also based on their first-hand experience with students over the course of many years.
The earlier apparent drop-off in student qualifications may now be reverberating in initially higher failure rates on board and licensure examinations. For example, the percentage of U.S. graduates failing Part I of the National Board examinations increased fairly steadily from 9.6 in 1982 to 16.0 in 1992; for Part II, the failure rate went from 8.0 to 13.2 percent during the same period (ADA, 1993d).10 These trends may be another factor prompting schools
to pay more attention to how they recruit and educate their students. The relationships among the entering qualifications of dental students, their achievements in dental school, their success on licensure examinations, their subsequent performance in dental practice, and school evaluations during the accreditation process are discussed further in Chapter 8.
In considering the quality of dental students and graduates, the committee developed some particular questions about graduates of foreign dental schools. ADA data indicate that these students are more likely to fail the National Board Dental Examinations (ADA, 1993c). For example, 48 and 39 percent failed the 1992 Part I and H examinations, compared to 16 and 13 percent of U.S. students, respectively.11 The committee found no data on the proportions of foreign dental graduates who never passed the examination and no follow-up data on those who eventually did pass. Information on clinical examination performance is not available.
The committee recognizes that foreign dental graduates who do become licensed in the United States may provide needed services, and it opposes discrimination on the basis of nationality. Nonetheless, as discussed further in Chapter 8, the committee is troubled by shortcomings in the processes for assessing student performance and graduate competency, and it is concerned that these shortcomings may be even more serious for foreign dental graduates who enter with advanced standing. The committee urges dental educators, accrediting organizations, and related groups to assess current policies for the admission, education, graduation, and licensure of graduates of foreign dental schools and to eliminate admissions policies or other practices that may exploit these students or threaten the quality of patient care.
Tuition and Debt Load
In its visits to dental schools, the committee heard countervailing worries about tuition. On the one hand, tuition cannot continue to go up at the same rate as in the past; on the other hand, tuition is a major source of revenue for many schools.
High student tuition is one of the most acute quality-of-life problems for many dental students and a major worry for dental educators. Figure 4.5 shows the change in tuition (in constant dollars) charged by public and private dental schools from 1970 to 1991. In 1970, tuition ranged from $67 dollars for in-state students at the least expensive school to $2,750 for all students at the most expensive. In 1991, the range was from $3,126 to $33,195. Other fees and living expenses add to total costs. For example, instrument purchase or rental can add thousands of dollars to students' costs. Not surprisingly, many dental students leave school with considerable debt, as illustrated in Figure 4.6. The high cost of dental education contributes to concerns that students from low- and middle-income families will lose access and that only those from wealthy families and those poor enough to qualify for substantial income-based financial aid will be able to afford dental school.
In addition to considering the implications of the tuition and debt situations for both students and schools, the committee was
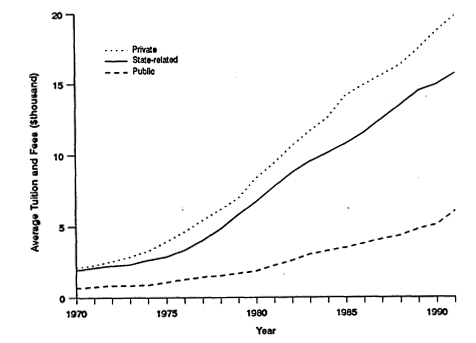
Figure 4.5
Average resident tuition and fees in constant dollars by school type.
Source: American Association of Dental Schools, 1992.
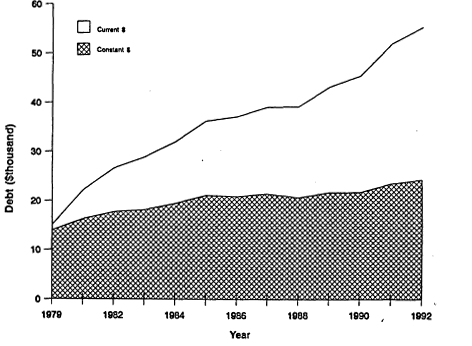
Figure 4.6
Student debt in constant dollars.
Source: American Association of Dental Schools, 1993b.
concerned about the implications for practitioners and patients. During almost every site visit, the committee heard students admit that debt limited their options after graduation. Among the options discouraged are rural practice, short-term or career military service, practice in low-income areas, and academic or research careers. Several of these options involve settings with a shortage of practitioners. For example, the Department of Defense (1993, p. l) testified to the committee that ''the high level of indebtedness . . . [means that] many . . . who would consider serving in the armed services . . . cannot afford such a career. . .. All three services are well short of their recruiting needs."
Some students who would prefer to go into practice say they opt for advanced education in part to put off debt repayment. For some but not all loan categories, interest charges are suspended during the training period. An additional incentive is the prospect of higher income with which to repay debt. Conversely, other students feel that they must start earning immediately after
graduation, even if they would prefer a general practice residency or postgraduate specialty training. The fact that several categories of postgraduate training in dentistry neither pay a stipend nor waive tuition only adds to the difficulty. (Stipends are the norm in hospital-based programs, primarily for oral and maxillofacial surgery and general practice residencies; they axe common if not universal in pediatrics and advanced general dentistry.)
In simple numerical terms, existing programs fall short as either debt relief or access improvement. Between FY 1991 and FY 1993, the National Health Service Corps (NHSC) increased the number of loan repayment positions from 11 to 55 (J. Rosetti, personal communication to M. Allukian, April 4, 1994). For 1994, 75 loan repayment positions were approved, but approximately 350 dentists were on a waiting list. Between FY 1991 and FY 1993, the number of scholarships decreased from 22 to 5, and none are projected in the future. In fact, the brochure describing the NHSC scholarship program does not even mention dentistry (AADS, 1994b).
Efforts to control tuition and educational costs generally are discussed in Chapter 7 and in the background paper by Douglass and Fein. In addition to trying to control tuition costs, policymakers may ameliorate the debt problem to some degree by adopting or expanding programs of national service that link debt forgiveness to a period of practice in underserved areas.12
In FY 1993, the Health Resource Services Administration listed more than 1,000 dental shortage areas in need of over 2,000 dentists. The limitations of the NHSC program as a vehicle for improving access to care in underserved areas are discussed further in Chapter 9. Without greater public funding of this program, it will meet neither the primary goal of improved access nor the important secondary goal of helping students who are not wealthy retain access to dental education.
Quality of Student Life
During site visits, several specific initiatives to improve student instruction and quality of life were cited. Most of these initiatives were also expected to improve the quality of education. Specifically,
- upgraded admission standards would avoid the distress created for and by students who are not academically qualified (given available resources and reasonable expectations for special remediation programs) to tackle predoctoral coursework;
- revisions in instructional methods would discourage authoritarian and rote teaching, thereby reducing the stress associated with numerical requirements and factual recall;
- attempts to rebalance the curriculum would provide more stimulating education and more time to reflect on it; and
- efforts to create a sense of community among health professions students and to expand student exposure to the broader offerings of university life would improve the quality of life for dental students.
The second and third of these directions—instructional and curriculum changes—have already been discussed. The fourth area reflects an acknowledgment that although the insularity of most professional schools—and dental schools in particular—has its comforts, isolation can be stifling. The committee was impressed by what it heard of efforts to create a sense of community among health professions students. These efforts are designed, in part, to increase the quality of services and support available to students by pooling library, housing, and other resources or activities and, in part, to enrich student life. Joint teaching of dental and other health professions students is intended to broaden the educational experience and promote the concept of health care as an enterprise involving teamwork and consultation. Enrichment of the dental school experience stretches beyond the health professions
in the form of joint degrees and coursework involving a range of other schools and programs such as engineering, business, and health administration.
A self-interested reason for dental educators to improve the quality of student life is that unhappy student memories may mean meager alumni contributions. Although such contributions are a relatively small part of school budgets they can relieve some of the pressure caused by cutbacks in public funding and greater competition for research funds. More generally, if practitioners retain negative feelings alter they graduate, this may contribute to the tensions between the education and the practice communities noted elsewhere in this report.
Findings and Recommendations
Because education is the most visible mission of dental schools, the committee commissioned a background paper on curriculum by Tedesco and focused many of its information collection activities on issues related to curriculum, faculty, and students. The committee examined extensive analyses of dental education. It also consulted numerous analyses of medical education to identify parallels and contrasts. The persistence of several common themes is striking and underscores the challenge of achieving change.
The committee feels confident that most of those involved in dental education would agree that the following problems persist. Basic and clinical science teaching do not stress the basic sciences as a relevant foundation for clinical practice. Individual courses and the overall curriculum often reflect past rather than current practice and knowledge. Comprehensive care is more an ideal than a reality in clinical education, and instruction still focuses too heavily on procedures. Linkages between medicine and dentistry are insufficient to prepare students to comprehend and apply the growing medical core of dental practice. The curriculum is crowded with redundant or marginally useful material and gives students too little time to consolidate concepts or to develop critical thinking skills. Lack of flexible tenure and promotion policies and of adequate resources for faculty development limits efforts to match the faculty to educational needs. Despite progress, insensitivity to student needs is still a concern. All of these weaknesses undermine efforts to prepare students for lifelong learning.
Many other reports have argued for movement away from these traditions and problems and have suggested specific alternatives including curriculum reform, education using active learning strategies
such as problem-based learning, closer relationships between dentistry and medicine, new approaches to comprehensive care, and revised accreditation standards. The problem is not so much agreement on directions for change but difficulty in overcoming the obstacles to change. These include lack of specific information on course content, limited evaluation of educational impact, university policy restrictions, faculty conservatism, and regulatory and financial constraints. Suggestions and recommendations here or in other chapters address most of these obstacles, but each institution will have to tailor strategies to its specific circumstances. More generally, the kind of leadership and commitment emphasized in Chapter 7 is not something that can be transmitted through a report, although this report may—as stated early in this chapter—provide guidance and some leverage.
The following recommendations emphasize curriculum reform, closer relationships with medicine, clinical experience in efficient practice settings, and student debt. They offer a mix of aspirations and instrumental actions to move toward desired goals. They need to be considered in conjunction with Chapter 6's recommendations about the patient care mission of dental schools, Chapter 8's consideration of licensure and accreditation policies, and Chapter 9's discussion of work force policies.
To stimulate progress toward curriculum goals long endorsed in dental education, the committee recommends that dental schools set explicit targets, procedures, and timetables for modernizing courses, eliminating marginally useful and redundant course content, and reducing excessive course loads. The process should include steps to
- design an integrated basic and clinical science curriculum that provides clinically relevant education in the basic sciences and scientifically based education in clinical care;
- incorporate in all educational activities a focus on outcomes and an emphasis on the relevance of scientific knowledge and thinking to clinical choices;
- shift more curriculum hours from lectures to guided seminars and other active learning strategies that develop critical thinking and problem-solving skills;
- identify and decrease the hours spent in low priority preclinical technique, clinical laboratory work, and lectures; and
- complement clinic hours with scheduled time for discussion of specific diagnosis, planning, and treatment-completion issues that arise in clinic sessions.
To prepare future practitioners for more medically based modes of oral health care and more medically complicated patients, dental educators should work with their colleagues in medical schools and academic health centers to
- move toward integrated basic science education for dental and medical students;
- require and provide for dental students at least one rotation, clerkship, or equivalent experience in relevant areas of medicine, and offer opportunities for additional elective experience in hospitals, nursing homes, ambulatory care clinics, and other settings;
- continue and expand experiments with combined M.D.D.D.S. programs and similar programs for interested students and residents; and
- increase the experience of dental faculty in clinical medicine so that they—and not just physicians—can impart medical knowledge to dental students and serve as role models for them.
To prepare students and faculty for an environment that will demand increasing efficiency, accountability, and evidence of effectiveness, the committee recommends that dental students and faculty participate in efficiently managed clinics and faculty practices in which
- patient-centered, comprehensive care is the norm;
- patients' preferences and their social, economic, and emotional circumstances are sensitively considered;
- teamwork and cost-effective use of well-trained allied dental personnel are stressed;
- evaluations of practice patterns and of the outcomes of care guide actions to improve both the quality and the efficiency of such care;
- general dentists serve as role models in the appropriate treatment and referral of patients needing advanced therapies; and
- larger numbers of patients, including those with more diverse characteristics and clinical problems, are served.
The committee recommends that postdoctoral education in a general dentistry or specialty program be available for every dental graduate, that the goal be to achieve this within five to ten years, and that the emphasis be on creating new positions in advanced general dentistry and discouraging ad-
ditional specialty residencies unless warranted by shortages of services that cannot be provided effectively by other personnel.
To permit faculty hiring and promotion practices that better reflect educational objectives and changing needs, the committee recommends that dental schools and their universities supplement tenure-track positions with other full-time nontenured clinical or research positions that provide greater flexibility in achieving teaching, research, and patient care objectives.
To improve the availability of dental care in underserved areas and to limit the negative effects of high student debt, Congress and the states should act to increase the number of dentists serving in the National Health Service Corps and other federal or state programs that link financial assistance to work in underserved areas.
Summary
The education of future practitioners is the central mission of dental schools. The content and method of dental education have been the subject of many criticisms over the years related to the weak links between basic science and clinical education or experience, the overcrowded dental curriculum, and the isolation of faculty both individually and collectively from the world beyond departmental boundaries. Linkages between dentistry and medicine are weaker than the nature of oral health problems and the growth of medically oriented interventions warrant. Problems remain in implementing comprehensive patient-centered care. The persistence of these problems testifies to the difficulty of change. Although the next two chapters of this report catalog yet more problems in the areas of research and patient care, their recommendations focus on steps that would address not only those problems but also some identified in this chapter. For example, greater research involvement by clinical faculty would almost certainly reinforce the links between basic science and clinic education, and revitalization of the patient care mission would likewise help make clinically current and patient-centered education a reality.