7 The Effects of Needle Exchange Programs
This chapter assesses the effects of needle exchange programs on HIV infections and drug use behaviors. Five major sources provide the evidentiary basis for the panel's assessment: (1) a 1991 review carried out by congressional request of the effectiveness of needle exchange programs (U.S. General Accounting Office, 1993), (2) a second comprehensive evaluation carried out by University of California researchers for the Centers for Disease Control and Prevention (Lurie et al., 1993), (3) selected studies published since the two 1993 literature reviews, (4) detailed examination of a set of recent studies in New Haven, Connecticut, and (5) detailed examination of a set of recent studies in Tacoma, Washington. This chapter concludes with the panel's conclusions and recommendations, which are based on the evidence presented in the chapter and throughout the report.
Evaluations of needle exchange programs have been published by Stimson et al. (1988), Des Jarlais (1985), the U.S. General Accounting Office (GAO) (1993), and the University of California (Lurie et al., 1993). We highlight the findings of the latter two reports, which were commissioned specifically by the federal government as evaluations of needle exchange programs. Both were published in 1993 and deal with needle exchange programs as they existed up to that time.
Needle exchange programs operate in a rapidly changing environment, and the panel reviews a number of studies that were published subsequent to the major reviews by GAO and the University of California.
Two strong lines of evidence emerged from the panel's examination of recent research on the effects of needle exchange programs on the spread of
HIV infection: studies from New Haven and Tacoma. These two sets of studies were selected on the basis of the wealth of published information available about the programs they analyze. That is, not only do they provide a sizable amount of information on various endpoints of interest (i.e., incident infection and risk behaviors), but they also have carefully addressed potential alternative explanations for their reported findings.
POTENTIAL OUTCOMES
At the outset, it is important to recognize that the effects of needle exchange programs can be viewed from a number of different perspectives. Some of these perspectives involve outcomes relevant to improving the health status of injection drug users, and others reflect community-level concerns regarding potential negative effects that may be associated with the implementation of such programs. The following section identifies the outcome domains that are relevant to those distinct perspectives and are most germane to the panel's task of assessing the effects of needle exchange programs.
Possible Positive Outcomes
Needle exchanges are established in order to: (1) increase the availability of sterile injection equipment and (2) at the same time, remove contaminated needles from circulation among the program participants. Operation of the exchange, then, is expected to result in a supply of needles with reduced potential for infecting program participants with HIV and also to reduce sharing between individuals because of easier access to clean needles for any program participant. Typical exchanges also maintain such services as education concerning risk behaviors, referral to drug treatment programs (a step toward eliminating the route for all infection), and distribution of condoms. These measures offer independent prospects for reducing the spread of HIV. Appraisal of the success of a needle exchange program may involve measuring, for example, the numbers of needles exchanged; the cleanliness of circulating needles; the prevalence and incidence of HIV and other needle-borne diseases; referrals to drug treatment programs; enrollments in treatment programs; and changes in the risk behaviors of needle exchange participants. An observed pattern of favorable outcomes would reflect health benefits from the operation of the program.
Possible Negative Outcomes
The possibility of negative results from needle exchange program operations also demands attention. One possible negative outcome is an increase
TABLE 7.1 Possible Outcomes and Expectations of Successful Needle Exchange Programs
|
Possible Positive Outcomes: |
Possible Negative Outcomes: |
|
Reduction in pool of infected needles |
Increase in drug use among needle exchange program clients |
|
Reduction in drug-related risk behavior |
Increase in new initiates to injection drug use |
|
Reduction in sexual risk behavior |
Increase in drug use in wider community |
|
Increase in referrals to drug abuse treatment |
Increase in number of contaminated needles unsafely discarded (e.g., on streets) |
|
Reduction in new infections among client population |
|
in the number of improperly discarded used needles. Another possibility is that the issuance of injection equipment, condoned by government, will "send a message" undercutting efforts at combatting illegal drug use and will promote more drug use (with more attendant HIV incidence). A third possible negative outcome is that needle exchanges will lower the perception of risk of injection drug use and thus attract more users to inject drugs and to other forms of illegal drug use.
Appraisal of the success of a needle exchange program, then, should also attend to measures of these possible negative outcomes. An observed pattern of negative outcomes would weigh against the idea that needle exchange programs are beneficial.
Assessment of the effects of needle exchanges involves the simultaneous consideration of a number of intended positive and unintended negative outcomes (Table 7.1). Ideally, a successful exchange program would reduce the risk of new infection among injection drug users without increasing drug use and health risks to the public.
THE PANEL'S APPROACH TO THE EVIDENCE
The purpose of this section is to clearly explain the panel's perspective in assessing the effectiveness of needle exchange programs. We first briefly review the basis for the traditional review procedures. We then outline the argument for a different approach—one that examines the patterns of evidence in order to assess effectiveness.
The Traditional Approach: Considering the Preponderance of the Evidence
Traditional reviews of experimental analysis search for studies with well-controlled research designs. By well-controlled designs, we mean ones
that can substantially protect against the introduction of systematic influences (i.e., bias) other than the intervention condition under consideration. High ratings on credibility are usually given to comparative designs that involve: (1) random assignment of participants to conditions (i.e., needle exchange program versus "usual services"); (2) minimal attrition of participants from being measured; (3) measurement procedures that minimize the role of response biases; and (4) sufficient statistical sensitivity (i.e., statistical power).
It is unlikely that evaluations of needle exchange programs will ever be carried out with ideal controls that warrant high confidence in the conclusions that can be drawn from a single definitive study. There are at least two broad reasons for this: (1) multiple actions generally are initiated in a given community setting, making it difficult to separate the effects of a needle exchange program from those of other prevention efforts by studying time trends and (2) the development of a comparative research design that relies on random assignment of individuals to receive needle exchange program services (or not) has technical, ethical, and logistical difficulties. Given these limitations, it seems reasonable to explore alternative means of assessing the credibility of the evidence's underlying claims about the effectiveness of needle exchange programs. Before doing so, however, it is useful to examine how previous research reviews have attempted to incorporate the traditional emphasis on design-induced control.
Two reviews were commissioned by the federal government and published in 1993: one by the U.S. General Accounting Office (1993) and one by the University of California at San Francisco (Lurie et al., 1993). Prior to 1993, a number of other studies were published (Des Jarlais et al., 1985; Stimson et al., 1988).
A close examination of the manner in which these studies were conducted strongly suggests their reliance on the quality of the evidence in individual studies, which is based on the strength of their research designs. The language of the assessments also reflects the expectation that, when they are taken as a collective across studies, even though the designs are less than ideal, the preponderance of evidence will weigh in favor of or against a definitive conclusion about needle exchange programs.
Taken together, these studies tend to suggest that needle exchange programs are either neutral or positive in terms of potential positive effects and that they do not demonstrate any potential negative effects. However, each study's conclusions are often less than firm because of its methodological limitations.
An Alternative Approach: Looking at the Patterns of Evidence
When the designs of a group of studies are limited, little inferential clarity is gained by looking at the preponderance of evidence, even if it
converges across all available studies. At a minimum, there must be a sufficient number of higher-quality (i.e., high-credibility) studies within the pool of studies to assess whether the evidence from the lower-quality studies is biased in a particular fashion.
Rationale
For well-designed interventions with well-designed experimental assessment procedures, examining each outcome one at a time is obviously justifiable on statistical and logical grounds. However, in light of the fact that most studies that have attempted to assess the effectiveness of needle exchange programs have limited study designs and that there are serious practical constraints associated with conducting a randomized control trial, some may conclude that it is impossible to ever determine whether needle exchange programs are effective. In the panel's view, however, such a conclusion is both poor scientific judgment and bad public health policy. Indeed, to adopt the position that evidence short of a randomized trial is useless amounts to denying the possibility of learning from experience—which, though often difficult, is not impossible.
In many areas of social sciences and public health research, the so-called definitive study—a randomized control experiment (that is, a randomized double-blind placebo controlled trial)—is an ideal that cannot be implemented. For example, it is unethical to consider use of a clinical trial design to show that smoking causes lung cancer (Hill, 1965). Scientific judgment develops instead through a series of studies using cross-sectional retrospective and prospective designs, in which later research avoids the flaws of earlier work but may introduce problems of its own. The improbability of being able to carry out the definitive study of the effects of certain HIV and AIDS prevention programs, including needle exchange programs, does not necessarily preclude the possibility of making confident scientific judgments about the effects of such prevention programs. As A. Bradford Hill (1965:300), one of this century's foremost biostatisticians, commented three decades ago:
All scientific work is incomplete—whether it be observational or experimental. All scientific work is liable to be upset or modified by advancing knowledge. That does not confer upon us a freedom to ignore the knowledge we already have, or to postpone the action that it appears to demand at a given time.
Sooner or later there comes a time for decision on the basis of evidence in hand. In the case of the efficacy of needle exchange programs, urgency is added because the disease in question—AIDS—is fatal, is contagious, and has been seen to spread rapidly in various settings. Previous assessments
of individual studies (as well as the panel's own) did not rate them as highly conclusive, because none of them used the gold standard of randomized controlled research designs. The panel therefore elected to rely on an approach that assesses the pattern of evidence in determining the effects of these HIV and AIDS prevention programs rather than relying on a preponderance of evidence approach.
In this approach to assessing the effects of needle exchange programs and the credibility of evidence surrounding a needle exchange program, we look at the consistency of the pattern of evidence that is available from multiple data sources about the same program. Taking this approach greatly expands the depth and breadth of the evidentiary base, because we try to understand the relationships among the parts of the intervention model, the process, and their outcomes. Rather than interpreting the effects of the intervention on individual outcomes, in isolation, the pattern of evidence approach considers interrelated conditions, such as intermediate outcomes (Cordray, 1986).
For example, consider the evaluation of a needle exchange program that reveals a reduction in new HIV infections over time among injection drug users who used the program. By traditional standards, this design would be classified as relatively weak because there is no control or comparison condition. Without further information, it is not possible to confidently conclude that the introduction of the needle exchange program is responsible for the observed decline on the basis of this one piece of evidence (the observed decline) alone.
Ruling In Plausibility
By examining whether certain required conditions were present, it is possible to probe the plausibility that the needle exchange program was responsible, at least in part, for the reduction. This type of assessment requires the specification of a series of if-then propositions. That is, if there is a real connection between the introduction of the needle exchange program and the observed decline in new infections, then a series of conditions must be present in order to increase confidence in the conclusion that the program is at least partially responsible for the observed outcome. The conclusion that the needle exchange program is plausibly connected to the decrease in new HIV infections is more credible if there is evidence that, as the putative causal agent, it was actually present in the community. This means that there must be an empirical pattern of evidence that, in effect, rules in its plausibility. Programmatically, the pattern of evidence might include:
-
information that the needle exchange program was established;
-
data that it exchanged a sufficient number of needles;
-
data that it provided needles to a substantial enough portion of the injection drug users in the community;
-
data that those who used the needle exchange reduced their level of drug-use risk behaviors (e.g., sharing, use of bleach); and
-
data that those who used the needle exchange most intensively show a greater level of risk reduction.
The argument that undergirds this approach is that programs have a structure and mechanisms that establish a logical pattern of expectations that can be tested empirically. To the extent that the empirical evidence supports these propositions, the plausibility that the needle exchange program was responsible for the observed change should increase. That is, the plausibility increases through repeated assessments. As a simple example, if there is a reduction in HIV incidence but the needle exchange program failed to exchange a single needle, it is not reasonable to conclude that the needle exchange program was responsible for the decline, regardless of the strength of the design underlying the HIV incidence data. However, through multiple assessments, involving a logical network of evidence, it may be possible to derive a portrait of the plausibility that the needle exchange program is implicated in the change process.
Ruling in the plausibility that the needle exchange program is a causal agent, through empirical assessment, is only half the story. It is still possible that other features of the program or research process contain biases that affect the HIV incidence. In traditional discussions of causal analysis, the notion of excluding (or rendering implausible) rival explanations has been the hallmark of competent experimental analysis. To the extent that repeated efforts to probe the results fail to disconfirm the plausibility that the intervention was at least partially responsible, its plausibility should be enhanced. Therefore, an assessment of the pattern of evidence not only entails ruling in the plausibility that the needle exchange program is a causal agent, but also requires ruling out plausible alternative explanations.
The Panel's Synthesis
The panel analyzed the patterns of evidence from five sources: two evaluations of the research published before 1993, the findings of studies published since 1993, and two sets of studies that provide the best available detailed account of how needle exchange programs impact risk behaviors and viral infections—one on New Haven, the other on Tacoma.
The process of selecting studies for detailed examination involved a comprehensive analysis of the research findings of individual needle exchange and bleach distribution projects. The panel generated a list of published
papers and presentations on needle exchange evaluation projects in the United States, Canada, and Europe. A meeting was held to judge which reports included data that might be used in a review. The projects were subsequently grouped by city and divided among panel members so that each city project had two independent reviewers. The studies from each city were reviewed, annotated on a formal evaluation form, and then discussed with the full panel at a subsequent meeting. Following this review, at a separate meeting, the panel decided to limit itself to studies conducted in the United States, because the legal and cultural environments of other countries are sufficiently different to raise questions about whether data are applicable to the United States. Two U.S. cities, New Haven and Tacoma, were found to have a sufficient number of data published from a variety of perspectives (e.g., incident infection, behavioral risk) to warrant inclusion in this review.
Various criteria were used in deciding to pursue the New Haven and Tacoma sets of studies. Consistent with the logic of the patterns of evidence approach, the first criterion applied in selecting studies was that the site or project had to have been comprehensively studied. That is, there had to be empirical evidence establishing that the needle exchange program was operational, that the mechanisms of the exchange process had been studied, and that there was an estimate of HIV incidence or, as in the case of New Haven, a proxy measure.
The level of activity in the prevention environment can make it difficult to isolate the influence of the needle exchange program. A second criterion was that, in the sites and projects selected, the needle exchange program had to be the predominant (if not the only) intervention ongoing at the time of the assessment. This criterion implies a selection process that focuses on high-contrast sites (i.e., the needle exchange program intervention dominates prevention activities in the area), thus yielding estimated effects of needle exchange that cannot readily be attributed to other prevention activities reaching the program participants.
U.S. GENERAL ACCOUNTING OFFICE REVIEW
In late 1991, the House Select Committee on Narcotics Abuse and Control requested that the U.S. General Accounting Office carry out a review of the effectiveness of needle exchange programs.1
Procedure
GAO researchers carried out an extensive review of the literature to identify empirical evaluation studies that had appeared in refereed or peer-reviewed
journals. They conducted site visits to programs located in Tacoma, Washington, and New Haven, Connecticut. Their review identified a total of 20 published studies and 21 abstracts on evaluations of needle exchange programs originating from nine distinct research projects, all but one of which (the Tacoma study) involved programs outside the United States. Among the nine research projects were one from Australia, one from Canada, two from the Netherlands, one from Sweden, and three from the United Kingdom.
The GAO team developed a list of eight relevant outcome measures: (1) rate of needle sharing; (2) prevalence of injection drug use; (3) frequency of injection; (4) rate of new HIV infections; (5) rate of new entrants to injection drug use; (6) incidence rate of other blood-borne infections; (7) rate of other HIV risk behaviors; and (8) risk to the public's health. They also identified three methodological criteria that had to be satisfied before findings could be considered: (1) the findings had to have been published in a scientific journal or government research monograph; (2) they had to have reached statistical significance; and (3) the reported effects of the needle exchange program could not have been attributed by the authors to any other source. Of the eight listed outcome measures, only three outcomes met the methodological standard of evidence set by the GAO team: (1) rate of needle sharing, (2) prevalence of injection drug use, and (3) frequency of injection. The GAO team summarized descriptive information, whenever it was available, on the ability of needle exchange programs to reach out to injection drug users and refer them to drug treatment and other health services.
Results
Tables 7.2 and 7.3 summarize the GAO findings. Regarding the potential positive outcomes, of the nine research projects reviewed, two reported a reduction in needle sharing, and a third reported an increase. It should be noted that the increase in sharing by needle exchange participants resulted from their passing on more used injection equipment (Klee et al., 1991); this finding was not replicated in a follow-up report by the same investigator (Klee and Morris, 1994). The earlier finding from that study appears to have been a transient effect that occurred before the needle exchange programs in the area reached full operation; that is, needle exchange participants were being used as a source of needles among their respective networks of injection drug users (Klee and Morris, 1994). The researchers concluded, moreover, based on the data available from six of the nine projects, that the needle exchange programs were successful in reaching injection drug users and providing a link to drug treatment and other health services.
Regarding potential negative outcomes of needle exchange programs,
TABLE 7.2 GAO Review: Results of Needle Exchange Program Study Projects
all five projects that reported findings on injection drug use by program participants—four on frequency of injection and one on prevalence of use—found that use did not increase. (Note that three of these findings did not reach statistical significance.) This led GAO to conclude that ''some research suggests programs may reduce AIDS-related risk behavior" (p. 6) and "most projects suggest that programs do not increase injection drug use" (p. 8). GAO reported that there was sufficient evidence to suggest that needle exchange programs "hold some promise as an AIDS prevention strategy" (p. 4).
In summary, the GAO report, which was the first government report to evaluate needle exchange programs, concluded that such programs hold promise as interventions to limit HIV transmission. The criteria for assessing the validity of the study findings and for including reports in the review were quite stringent. In particular, the criterion of statistical significance means that studies that showed no difference in the frequency of injection or needle sharing were excluded. Therefore, the argument that needle exchange programs cause no harm is not fully characterized because studies
TABLE 7.3 GAO Review: Needle Exchange Program Outcomes Measured and Reported
|
Project Number by Country |
Attracted Injection Drug Users Not in Treatment |
Referred Injection Drug User to Drug Treatment |
Referred Injection Drug User to Other Health Services |
|
Australia |
|
|
|
|
1 |
|
|
|
|
Canada |
|
|
|
|
2 |
|
Yes |
Yes |
|
Netherlands |
|
|
|
|
3 |
|
|
|
|
4 |
Yes |
|
|
|
Sweden |
|
|
|
|
5 |
Yes |
|
Yes |
|
United Kingdom |
|
|
|
|
6 |
Yes |
|
|
|
7 |
Yes |
Yes |
Yes |
|
8 |
|
|
|
|
United States |
|
|
|
|
9 |
Yes |
Yes |
|
|
SOURCE: Adapted from Needle Exchange Programs: Research Suggests Promise as an AIDS Prevention Strategy (U.S. General Accounting Office, 1993:10). |
|||
with high level of statistical power that showed no difference were excluded.
UNIVERSITY OF CALIFORNIA REPORT
In September 1993, a second government report, The Public Health Impact of Needle Exchange Programs in the United States and Abroad , was published by the University of California for the Centers for Disease Control and Prevention (CDC). This report consists of a summary volume with two supporting volumes and addresses a number of the questions that this panel was asked to address.
Procedure
The University of California report was the work of a team of 12 individuals with expertise in clinical medicine, nursing, psychology, anthropology, sociology, cost-benefit modeling, and epidemiology. None of the team
members was identified in published writings as either in favor of or opposed to needle exchange programs. In a process that included discussions with an advisory committee, public health officials, needle exchange program staff members, researchers, experts in drug abuse treatment and injection drug use, and community leaders, a list of 14 research questions was generated: (1) How and why did needle exchange programs develop? (2) How do needle exchange programs operate? (3) Do needle exchange programs act as bridges to public health services? (4) How much does it cost to operate needle exchange programs? (5) Who are the injection drug users who use needle exchange programs? (6) What proportion of all injecting drug users in a community uses the needle exchange program? (7) What are the community responses to needle exchange programs? (8) Do needle exchange programs result in changes in community levels of drug use? (9) Do needle exchange programs affect the number of discarded syringes? (10) Do needle exchange programs affect rates of HIV drug and/or sex risk behaviors? (11) What is the role of studies of syringes in injection drug use research? (12) Do needle exchange programs affect rates of diseases related to injection drug use other than HIV? (13) Do needle exchange programs affect HIV infection rates? and (14) Are needle exchange programs cost-effective in preventing HIV infection?
The investigators conducted a formal review of existing research; made site visits and sent mail surveys to needle exchange programs; formed focus groups with injection drug users; and applied statistical modeling techniques. Data collected from each approach were sorted into 1 of the 14 questions about impact of needle exchange programs. The aim of the literature review was to identify a maximum of written works relating to the effectiveness of needle exchange programs. Computer searches of AIDS line and Medline provided a first cut and were augmented by items from the bibliographies of articles found therein. In addition, the research team reviewed abstracts from the annual International Conference on AIDS from 1988 to 1993 and the annual meetings of the American Public Health Association from 1987 to 1992. To identify unpublished materials, needle exchange program staff were contacted about internal reports, and a search was made for newspaper and magazine clippings, government and institutional reports, and relevant book chapters.
From this effort, 1,972 data sources were identified, which included 475 journal articles, 381 conference abstracts, 236 reports, 159 unpublished materials, 499 newspaper and magazine articles, 94 books or chapters, and 128 personal communications or other sources. All materials were reviewed and coded according to which research question(s) they addressed. Project members were assigned responsibility for synthesizing information for each of the 14 research questions. Each of the studies was assessed using a standardized format and ranked on a scale from 1 to 5:
-
incomplete, inadequate, or not relevant to the research question;
-
unacceptable: contains flaws in design or reporting that make interpretation unreliable;
-
acceptable: provides credible evidence but has limited detail, precision, or generalizability;
-
well done: provides detailed, precise, and persuasive evidence; and
-
excellent: compelling and complete.
The final ranking of an article was determined by agreement of at least two project members. Only studies ranked 3 or higher were used in the synthesis.
In addition to the review of existing research, the University of California team conducted site visits to 15 cities, 10 of which were in the United States, 3 in Canada, and 2 in Europe.2 The sites were selected on the basis of a published list of programs and reflected the range of existing needle exchange programs with respect to size, legal status, geographical location, injection drug users' HIV seroprevalence, and extent of prior evaluation research. (CDC was consulted during the selection process.) At each site, the research team used multiple data collection methods with multiple iterations, consisting of interviews, focus groups, and observation using a formal qualitative research strategy.
The methodology was codified in a manual. Standardized training of the research staff was provided. In the 15 cities, 33 needle exchange sites were visited and a total of 239 interviews with needle exchange directors and staff, public health officials, injection drug use researchers, community leaders, program participants (11 focus groups), and injection drug users not enrolled in programs (7 focus groups) were completed. Observation guidelines were pretested at two sites and the results were compared qualitatively for interrater reliability before adopting the final guidelines.
Results
Of the nine outcomes and expectations for successful needle exchange programs listed in Table 7.1, the University of California report addressed eight. That is, research findings concerning four of the five possible positive outcome domains were reviewed: reduction in drug-related and sexual risk behaviors, increase in referrals to drug abuse treatment, and reduction in HIV and other infection rates. The report addressed all four possible negative outcomes: increases in (1) drug use by program participants; (2) new initiates to injection drug use; (3) drug use in the community in general; and (4) the number of contaminated needles discarded.
Possible Positive Outcomes
Reduction in High-Risk Behavior
The University of California report reviewed data on reported needle-sharing frequency in studies of needle exchange programs. Of the 26 evaluations addressing behavior change associated with the use of needle exchange programs that were identified, 16 were deemed of acceptable quality (rating 3 or higher). Of the 16 studies, 14 presented data on the frequency of needle sharing; 9 of these had comparison groups reported. As Table 7.4 indicates, 10 of the 14 studies showed a beneficial effect of the needle exchange programs on reported frequency of needle sharing; 4 showed a mixed or neutral effect; and none showed an increased frequency of needle sharing. Regarding sexual risk behavior change, the report concluded that the findings were neutral. That is, four studies reported beneficial effects of needle exchange programs relating to sexual risk associated with number of partners and two reported mixed or neutral effects. When reviewing studies that addressed risk associated with partner choice, three showed beneficial effects and two reported mixed or neutral effects. Finally, beneficial effects of needle exchange programs relating to condom use were observed in one study, mixed or neutral results in another, and adverse effects in three studies.
Increased Referrals to Drug Treatment
The University of California report noted that 17 of 18 U.S. and Canadian programs visited stated that they provide referrals to drug treatment. Of 33 U.S. programs surveyed, 3 reported treatment services on site. The extent to which referrals enter treatment and are retained was described—the 6 programs that collect data on referrals reported 2,208—but was not studied. The report noted (Lurie et al., 1993:236) that the paucity of drug abuse treatment slots in many cities limits the usefulness of needle exchange program referrals to drug abuse treatment. This affects the likelihood that a needle exchange program will refer and that a referral will link a client with treatment.
Reduction in HIV Infection Rates
The University of California report identified 21 studies that were relevant to the issue of whether needle exchange programs impact rates of HIV infection: 2 case studies, 7 serial community cross-sectional studies, 6 serial needle exchange program cross-sectional studies, 1 case-control study,
TABLE 7.4 University of California Report: Studies of Behavior Change With Quality Rating of Three or Greater
|
Outcome Measure |
Beneficial Needle Exchange Program Effect |
Mixed or Neutral Needle Exchange Program Effect |
Adverse Needle Exchange Program Effect |
|
Drug risk sharing frequency |
Amsterdama,b (Hartgers et al., 1989); London/SW Englanda (Dolan et al., 1991) (Donoghoe et al., 1991); New South Wales (Schwartzkoff, 1989); New York City (Paone et al., 1993); Portlanda (Oliver et al., 1991) (Oliver et al., 1992) (Des Jarlais and Maynard, 1992); San Franciscoa (Watters and Cheng, 1991) (Guydish et al., 1989) (Feldman et al., 1989); Tacoma (Hagan et al., 1991b) (Hagan et al., 1992a); Tacoma (Hagan et al., 1993); Walesa (Stimson et al., 1991) |
Amsterdama (Hartgers et al., 1992) Amsterdama (van Ameijden et al., 1993) England/Scotlanda (Donoghoe et al., 1989) (Stimson et al., 1988) (Stimson et al., 1989) Manchestera (Klee et al., 1991) |
|
|
Giving away used needles |
London/SW Englanda (Dolan et al., 1991) (Donoghoe et al., 1991); Tacoma (Hagan et al., 1991b) (Hagan et al., 1992a); Tacoma (Hagan et al., 1993) |
Amsterdam (van Ameijden et al., 1993) |
Manchestera (Klee et al., 1991) |
|
Needle cleaning |
New South Wales (Schwartzkoff, 1989); Portlanda (Oliver et al., 1991) (Oliver et al., 1992) (Des Jarlais and Maynard, 1992); Tacoma (Hagan et al., 1993) |
Amsterdam (Hartgers et al., 1992) |
|
|
Outcome Measure |
Beneficial Needle Exchange Program Effect |
Mixed or Neutral Exchange Program Effect |
Adverse Needle Exchange Program Effect |
|
Injection frequency |
Amsterdama,c (Hartgers et al., 1989); Tacoma (Hagan et al., 1991b) (Hagan et al., 1992a); Walesa (Stimson et al., 1991) |
New York City (Paone et al., 1993); San Francisco (Watters and Cheng, 1991) (Guydish et al., 1989) (Feldman et al., 1989); San Francisco (Guydish et al., 1993); Tacoma (Hagan et al, 1993) |
London/SW Englanda (Dolan et al., 1991) (Donoghoe et al., 1991) |
|
Sex risk Number of partners |
England/Scotlanda (Donoghoe et al., 1989) (Stimson et al., 1988) (Stimson et al., 1989); New South Wales (Schwartzkoff, 1989) |
London/SW Englanda (Dolan et al., 1991) (Donoghoe et al., 1991) |
|
|
Partner choice |
England/Scotlanda (Donoghoe et al., 1989) (Stimson et al., 1988) (Stimson et al., 1989) |
London/SW Englanda (Dolan et al., 1991) (Donoghoe et al., 1991) |
|
|
Condom use |
New South Wales (Schwartzkoff, 1989) |
Walesa (Stimson et al., 1991) |
England/Scotlanda (Donoghoe et al., 1989); (Stimson et al., 1988) (Stimson et al., 1989) |
|
NOTE: SW = southwest. a Compared with control group(s). b Cross-sectional component. c Retrospective component. SOURCE: The Public Health Impact of Needle Exchange Programs in the United States and Abroad, Volume 1 (Lurie et al., 1993:414). |
|||
and 3 prospective studies. The quality of studies was rated on a 5-point scale ranging from a low of 1 (not valid) to a high of 5 (excellent) and a mid-point of 3 (acceptable). Only two of the studies received a quality rating of 3 or higher, and two others were rated between 2 and 3. None of the studies showed increased prevalence or incidence of HIV infection among needle exchange participants.
Given the quality rating of the studies, it is not surprising that the University of California report concluded that the studies available up to the time of the report (Lurie et al., 1993) do not, and for methodological reasons probably cannot, provide clear evidence that needle exchange programs decrease HIV infection rates. However, needle exchange programs do not appear to be associated with increased rates of infection.
It is intrinsically difficult to measure effects of intervention on the incidence of new infections of rare diseases, whose victims ordinarily do not show symptoms at the time of infection. Although most of the early studies used prevalent infection as the outcome measure, the more appropriate measure is incident or new infection. However, a further complication is that incidence is low in most locations, thereby requiring larger study populations to demonstrate program effects. The University of California report noted (Lurie et al., 1993:465) appropriately:
Well-conducted, sufficiently large case-control studies offer the best combination of scientific rigor and feasibility for assessing the effect of needle exchange programs on HIV rates.
Possible Negative Outcomes
Increase in Program Participant Drug Use
The University of California report noted that eight "acceptable" studies were identified that presented data on the issue of reported injection frequency. As Table 7.4 shows, three studies found reductions in injection associated with needle exchange programs; four found mixed or no effects; and one found an increase in injection compared with controls. This last study also found reduced needle sharing reported among needle exchange participants. This study noted that the apparent increase in injection could be attributed to several other factors, including the differential dropout of low-level injectors. The report also reviewed the methodological limitations of the studies, including the potential for socially acceptable responses by injection drug users. On balance, because of methodological problems, the report drew no strong conclusions about levels of injection drug use.
Increase in New Initiates to Injection Drug Use
The University of California report reviewed a variety of studies and used focus groups to understand whether needle exchange programs could encourage persons to initiate injection drug use. In reviewing the demographic data from the programs, the report noted that the median age of participants across programs ranged from 33 to 41, and the median duration of injection drug use from 7 to 20 years. This suggests that most participants initiated injection drug use prior to using the needle exchange program.
A review of serial cross-sectional studies of injection drug users in San Francisco noted an increase in the mean age of the samples over time from 34 in 1986 to 40 in 1990, suggesting that there was not an increase in young new injectors over time. Researchers in Amsterdam used a capture-recapture method to estimate the number of injection drug users between 1983 and 1988. Despite initiation of a needle exchange program in 1984, no change in the number of injection drug users was reported, and the average age of drug users increased over time. Furthermore, the number of drug users under age 22 decreased from 14 percent in 1983 to 3 percent in 1988. The authors concluded that there was no increase in the number of new initiates into injection drug use.
The report concluded, on the basis of evidence from surveys, that (Lurie et al., 1993:357) "needle exchange programs are not associated with an increase in community levels of injecting."
Focus groups were consulted. Of 10 focus groups from needle exchange programs, comprising 65 injection drug users, 2 individuals thought needle exchange programs could encourage nonparenteral drug users to start injecting. Among seven nonprogram focus groups comprising 47 injection drug users, 2 individuals thought needle exchange programs could encourage nonparenteral drug users to start injecting. The focus group data were viewed as corroborating evidence for the data available from surveys arguing against an effect of needle exchange programs on increasing the community levels of injection drug use.
Increased Drug Use in the Community
The University of California report addressed the potential for increased drug use in the community by reviewing the studies noted in the previous section. Researchers searched for additional data by examining established data sets of drug abuse indicators and answers to additional questions asked of focus groups of injection drug users.
The University of California researchers attempted to relate the presence (or absence) of needle exchange programs to ongoing statistical series
like the Drug Abuse Warning Network (DAWN), Drug Use Forecasting (DUF), and Uniformed Crime Reports (UCR), which might reflect altered patterns of drug-related events, such as drug cases in hospital emergency rooms, positive urine drug screens, and drug-related arrests, respectively. The report noted wide variation in these drug-use indicators over time, which suggests inherent lack of precision and limits the manifestation of patterns—if any—relating to needle exchange.
The University of California report also noted that, because needle exchange programs are relatively new, changes in drug use might yet appear with longer follow-up. The report concluded that (Lurie et al., 1993:357) "currently available (national indicator) data provide no evidence of change in overall community levels of drug use associated with needle exchange programs."
The report also noted that the San Francisco and Amsterdam surveys described above provide (Lurie et al., 1993:357) "some evidence that needle exchange programs are not associated with an increase in community levels of injecting or overall drug use."
Increase in Number of Contaminated Needles Unsafely Discarded
The University of California report noted that adverse community responses to needle exchange programs are likely to be centered on the issue of discarded needles and the risk to the public of accidental needlestick injury. However, the report noted that one-for-one exchange rules cannot, in theory, increase the total number of discarded needles, although programs could affect the geographic distribution of discarded syringes. Data on a surveillance project with the Portland, Oregon, needle exchange program noted a decrease in the prevalence of discarded syringes near the program (Lurie et al., 1993:386). Passive surveillance of health or police department reports over time indicated either declines or small increases in needlestick injuries, with the trends due to changes in reporting patterns. The University of California report concluded that needle exchange programs "have not increased the total number of discarded syringes" and, if structured as a one-for-one exchange with no starter needles, "they cannot increase the total number of discarded needles" (Lurie et al., 1993:395).
Summary
Using multiple data sources, the University of California reviewed a number of questions about needle exchange programs. As far as possible positive outcomes are concerned, the report concluded that the data available at the time of the report "do not … provide clear evidence that needle exchange programs decrease HIV infection rates," (p. 20) but that "the
majority of studies of [program] clients demonstrate decreased risk of HIV drug risk behavior, but not decreased rates of HIV sex risk behavior'' (p. 18) In addition, "all but one of the 18 US and Canadian needle exchanges visited … stated that they provide referrals to drug abuse treatment" (p. 10) Finally, regarding possible negative outcomes, the report concluded that needle exchange programs have not increased the total number of discarded used needles and syringes (p. 16). The report goes on to state that there is no evidence that drug use among program participants increased, and there is no evidence of change in overall community levels of noninjection or injection drug use (Lurie et al., 1993:15).
EVIDENCE FROM RECENT STUDIES
This section is organized into topical areas that parallel the summaries of the GAO and University of California reports. Study findings are categorized according to the outcomes and expectations of program effects listed in Table 7.1; both possible positive and possible negative effects are reviewed. The information sources for this update comprise: (1) a review of abstracts from the 1994 International Conference on AIDS; (2) the 1994 American Public Health Association conference; (3) papers presented at the National Research Council/Institute of Medicine's Workshop on Needle Exchange and Bleach Distribution Programs (1994); and (4) articles appearing in refereed journals following the release of the University of California report. Since the University of California report was issued, a number of studies on the impact of needle exchange programs have been presented or published. These studies utilize a variety of designs, including an ecological design; a comparison of prevalence rates between injection drug users who use and those who do not use needle exchange programs; HIV incidence rates among needle exchange program attenders; and, using data collected prospectively, a comparison of HIV incidence rates between injection drug users who attend and those who do not attend a needle exchange program.
Possible Positive Outcomes
Reduction in Risk Behavior
Recent publications on needle exchange programs in San Francisco, New York City, and Portland, Oregon, have addressed the issue of the impact of the programs on HIV drug-use risk behaviors and sexual risk behaviors (Watters et al., 1994; Watters, 1994; Lewis and Watters, 1994; Des Jarlais et al., 1994a, 1994b, 1995; Paone et al., 1994a, 1994b; Oliver et al., 1994).
In an ecological study in San Francisco, Watters (1994) examined the
trends in risk behaviors and HIV seroprevalence over a 6.5-year period among heterosexual injection drug users over 13 cross-sectional surveys between 1986 and 1992. Interviews (5,956) were conducted with injectors in street settings and drug detoxification clinics. During that time period, multiple prevention efforts targeting injection drug users had been implemented (including outreach, education, voluntary HIV testing and counseling, bleach and condom distribution, and needle exchange programs). Among injection drug users who reported sharing needles, the proportion of those who reported ever using bleach increased from 3 percent in 1986 to 89 percent by 1988 and remained relatively constant at that level through fall 1992.
Sexually active heterosexual male injectors also reported significant changes in condom use (i.e., injection drug users reported using a condom 4.5 percent of the time in 1986, compared with 31 percent of the time in late 1992). However, Lewis and Watters (1994) found that a substantial proportion of sexually active male drug injectors, including heterosexuals, bisexuals, and homosexuals, reported frequently engaging in unprotected sex (i.e., reported condom use was low in all three groups). That is, 56 percent of the heterosexuals who had vaginal sex in the prior 6 months reported no condom use; one-third of the homosexuals who engaged in anal intercourse with male partners reported no condom use; and 41 percent of the bisexual men reported no condom use while engaging in vaginal sex and approximately half (52 percent) reported no condom use while engaging in anal or oral sex with females and/or males.
In another ecological report from New York City, Des Jarlais and colleagues (Des Jarlais et al., 1994a) examined trends in reported risk behaviors and seroprevalence among injection drug users for 1984 and 1990 to 1992 by comparing results of two surveys of injection drug users entering a drug detoxification program. Several trends in drug-use risk behaviors were reported. In 1984, for example, 65 percent of injection drug users reported having used shooting galleries in the preceding 2 years; in the 1990 to 1992 survey, only 3 percent reported injecting in shooting galleries in the preceding 6 months. Substantial reductions in sharing behavior were also observed. Use of potentially contaminated needles declined from 51 to 7 percent of injections. Moreover, an increasing proportion of injection drug users entering the detoxification program reported using the needle exchange programs since they opened in 1990. For the 1990 to 1992 period, results also show that needle exchange participation was associated with a downward trend in the proportion of subjects reporting any injection with needles that had been used by someone else and a reduction in the percentage of study participants reporting having passed on used needles to others. The extent to which the reductions in risk behaviors reported in the two surveys can be attributed to the needle exchange program itself is limited by the fact
that the data are ecological trends. Other prevention efforts were occurring in New York City between the two time intervals. Therefore, although the results are consistent with an inference of reduction in risk behaviors following the introduction of a needle exchange program, the study design does not exclude the possibility of contributing or alternate explanations.
In the San Francisco needle exchange program evaluation, Watters (1994) compared frequent needle exchange participants with two comparison groups—injection drug users who used the exchange less frequently and a group who did not use it at all. These researchers found a 47 percent decline (from 66 to 35 percent) in reported sharing behavior among injection drug user study participants between spring 1987 and spring 1992. More refined analyses revealed that frequent needle exchange participants (i.e., used the program more than 25 times in the past year) were less likely to report needle sharing in the past 30 days than study participants who used the needle exchange program less frequently or not at all. In contrast, over the 3-year study period, no change in reported rates of sharing behavior was observed among those not using the program.
In New York City, Paone et al. (1994a) conducted a pre-post analysis that examined the drug-use risk behaviors of 1,752 needle exchange program participants 30 days prior to using the exchange and during their most recent 30 days in the program. Participants reported a two-thirds decline in the proportion of time they injected with previously used needles (12 percent before participating in the needle exchange program, compared with 4 percent in the last 30 days while participating in the program). Similar reductions in renting or buying used needles (73 percent decline) were observed, and similar reductions in the number of participants who reported borrowing used needles were found (59 percent decline). The number of participants who reported using alcohol pads increased from 30 percent before participating in the needle exchange program to 80 percent in the most recent 30 days in the exchange. Although the reduction in high-risk behaviors was based on self-reports of exchange users and no comparison of injection drug users not using the exchange was included in this report, this pattern of reduction in drug-use risk behaviors was found to be relatively stable in recent updates (Des Jarlais et al., 1994b; Des Jarlais et al., 1995; Paone et al., 1994b). These authors also note in their recent updates that minimal changes in sexual risk behaviors were reported. For example, always using a condom with a primary sexual partner increased from 36 percent in the 30 days prior to first using the needle exchange program to 37 percent for the last 30 days while using the program; whereas always using a condom with a casual sexual partner increased from 56 percent in the 30 days prior to first using the exchange program to 60 percent in the last 30 days while using the exchange. However, due to design constraints,
it cannot be stated what portion of the reduction in risk behaviors is due to the needle exchange program.
An evaluation of the Portland needle exchange program (Oliver et al., 1994) assessed change in risk behaviors among 753 needle exchange program participants by comparing data collected on each study participant during an intake interview and a 6-month follow-up interview. Significant declines in sharing behaviors (rent needles and syringes: intake = 9 percent compared with 3 percent at follow-up; borrowed needles and syringes: intake = 20 percent compared with 7 percent at follow-up) and increased use of bleach (intake = 51 percent compared with 65 percent at follow-up) were observed. When drug-use risk behaviors of frequent attenders (attended four or more times) were compared with risk behaviors of those who attended three or fewer times, frequent attenders reported greater risk reduction on borrowing and returning used needles to the program. To supplement the pre-post analysis, needle exchange participants were also compared with another group of drug injectors, clients of Portland's National AIDS Demonstration Research (NADR) program (i.e., all received bleach and HIV education and a subset also received counseling). Frequent needle exchange participants were found to be less likely to reuse needles without cleaning or to improperly dispose of used needles than were the NADR clients. The two groups were not found to differ on other risk behaviors assessed. It is worth noting that there was little overlap between the two groups (11 percent). The two interventions apparently are recruiting different participants.
In sum, from the earliest studies of needle exchanges, there has been a dominant trend in the data showing significant and meaningful associations between participation in needle exchange programs and lower levels of drug-use risk behaviors, and small or no change in sexual risk behaviors. The most recent data continue to reflect this trend. Moreover, this pattern of findings has also been observed in foreign cities (Davoli et al., 1995; Hunter et al., 1995).
Reduction in HIV Infection Rates
Two recent ecological studies examined trends in HIV seroprevalence rates among injection drug users, one in New York City and the other in San Francisco (Des Jarlais et al., 1994a; Watters, 1994). Both reported a stabilization of HIV seroprevalence rates that coincided with reductions in high-risk behaviors and the implementation of various prevention programs (including outreach, education, testing and counseling, bleach and condom distribution, and needle exchange programs). Although these ecological studies do not provide direct causal evidence of the effect of such programs, they nonetheless document a pattern in behavioral risk reduction that corresponds
with stabilization of seroprevalence rates in distinct populations of injection drug users.
Hagan and colleagues (1994b) reported seroprevalence rates of needle exchange participants and nonparticipants. The cross-sectional sample of needle exchange participants (n = 426) was found to have a 2 percent HIV prevalence rate, compared with an 8 percent rate for the cross-sectional sample of nonparticipants (n = 159). Because the outcome measured in this study was prevalent infection, temporal associations cannot be established with certainty, and the possibility that the results might reflect that the needle exchange program attracts lower-risk injection drug users cannot be dismissed out of hand. However, the results are consistent with the inference that needle exchange programs are associated with a lower risk of infection.
On the basis of recent updates from the 1994 International Conference on AIDS, Des Jarlais (1994; in press) provided descriptive information on HIV incidence among injection drug users who participate in needle exchange programs across 14 different cities (Table 7.5). Some of these incidence rates were measured directly by testing cohorts of needle exchange participants; others were based on self-reports of prior serological tests; still others were derived from statistical modeling techniques (e.g., New Haven).
An examination of the data reveals that, with the exception of data from Montréal, HIV incidence is uniformly low among needle exchange program participants; that is, regardless of whether HIV prevalence is low, moderate, high, or very high among the community of injection drug users in a city, HIV incidence among program participants is consistently low across cities. These findings are consistent with the premise that an AIDS prevention program (e.g., needle exchange program or other outreach intervention) that is able to reach and successfully modify the behavior of injection drug users who are at high risk of becoming infected or of transmitting HIV to others is capable of maintaining a low level of new infections in the population of injection drug users in a community.
The high HIV incidence among needle exchange program participants observed in Montréal is disconcerting. The reader is referred to Appendix A for a detailed discussion of Montréal data. Although the prevalence is moderate and has remained stable, the observed incidence is high among the needle exchange cohort being studied. If the high incidence accurately reflects the rate of new infections in the population of injection drug users in Montréal, an increasing prevalence over time would be expected—it is not possible to think that mortality is as high as the observed incidence. A rational explanation (again, if the prevalence and incidence estimates are unbiased population estimates) could be that Montréal's needle exchange program is attracting a high-risk group of users (selection bias).
TABLE 7.5 HIV Incidence Estimates Among Needle Exchange Participants in Select Cities
|
City |
HIV Prevalencea |
Measured HIV Seroconversionsb |
Estimated HIV Seroconversionsc |
|
Lund, Sweden |
Low |
0 |
|
|
Glasgow, Scotland |
Low |
|
0-1 (2) |
|
Sydney, Australia |
Low |
|
0-1 (2) |
|
Toronto, Canada |
Low |
|
1-2 (2) |
|
England and Wales (except London) |
Low |
|
0-1 (1) |
|
Kathmandu, Nepal |
Low |
0 |
|
|
Tacoma, WA, USA |
Low |
<1 |
|
|
Portland, OR, USA |
Low |
<1 |
|
|
Montréal, Canada |
Moderate |
13 |
|
|
London, England |
Moderate |
|
1-2 (4) |
|
Amsterdam, The Netherlands |
High |
4 |
|
|
Chicago, IL, USA |
High |
0 |
|
|
New York, NY, USA |
Very high |
2 |
|
|
New Haven, CT, USA |
Very high |
|
0 (3) |
|
a Low = 0 to 5 percent; moderate = 6 to 20 percent; high = 21 to 40 percent; very high = 41 + percent. b Cohort study and/or repeated testing of participants in per 100 person years at risk. c Estimated from: (1) stable, very low <2 percent seroprevalence in area; (2) self-reports of previous seronegative test and a current HIV blood/saliva test; (3) HIV testing of syringes collected at exchange per 100 person years at risk; and (4) stable or declining seroprevalence. SOURCE: Adapted from Current Findings in Syringe Exchange Research: A Report to the Task Force to Review Services for Drug Misusers (Des Jarlais, 1994). |
|||
Recent reports from Montréal (Hankins et al., 1994; Lamothe et al., 1993; Bruneau et al., 1995) suggest that needle exchange participants still frequently engage in high-risk behaviors, including unsafe cocaine injection and prostitution. The program is located in an area of the city noted for prostitution, and the program operates in the middle of the night, which makes it prone to recruiting high-risk users. Moreover, injection drug users in Montréal who elect to purchase sterile needles in pharmacies can do so without a prescription (further biasing the representation of those who elect to acquire their needles in the middle of the night at the exchange program). Recent epidemiologic data from Montréal (Bruneau et al., 1995) highlight the complex nature of the observed association between sources of sterile needles and HIV seroincidence (see Appendix A). That is, although the risk of seroconversion was found to be higher among needle exchange participants when compared to nonparticipants, injection drug users who used the
needle exchange program as their exclusive source of sterile needles were found to be at substantially lower risk than those who used diverse sources of sterile needles. Furthermore, the needle exchange program limit of 15 needles per visit may not be sufficient to properly address drug-use risk behaviors of individuals who inject large amounts of cocaine. There is also a high level of male prostitution among the needle exchange participants.
If the infection rate estimates accurately reflect the population parameters, it would appear that the services offered by the Montréal needle exchange program are insufficient to control HIV transmission in that cohort. Specific ethnographic studies are needed to better understand the primary routes of transmission implicated and their dynamics (e.g., sex, specific drug-use risk behaviors). This would allow the program to better tailor its services (e.g., add new services) and/or the relative intensity of the service delivery according to needs of participants (i.e., primary risks).
The potential ability of needle exchanges to attract injection drug users that are at high risk of seroconversion was also recently reported in the United States by a San Francisco research team (Hahn et al., 1995; see Appendix A for a detailed review of the San Francisco study). Although the disparities in observed seroincidence rates between needle exchange participants and nonparticipants could not be attributed to having been exposed to the needle exchange program, the program appeared to serve a relatively high-risk subset of injection drug users. The authors concluded that the San Francisco program provides a unique setting for intervention because it provides direct access to a population that is at high risk.
Other cities with needle exchange programs that have high seroprevalence data (e.g., New Haven, Chicago, New York) report a low level of HIV seroconversion. The high seroconversion rate in Montréal therefore appears to be the exception, rather than the rule. These data are consistent with the premise that AIDS prevention programs (e.g., needle exchange) are able to stabilize HIV prevalence and very low seroincidence. Obviously, these results are descriptive in nature (there are no comparison groups) and, as a consequence, cannot in themselves provide evidence of the direct causal effect of needle exchange programs on HIV incidence rates. Nonetheless, they do provide valuable insight into HIV incidence rates among needle exchange participants in cities with varying levels of HIV seroprevalence among the local populations of injection drug users.
Other recent reports from New York City (Des Jarlais et al., 1994b, 1995; Paone et al., 1994b) have compared seroconversion rates of various injection drug user groups in the city. The HIV seroconversion rate among high-frequency drug injectors not using the needle exchange programs ranged from 4 to 7 per 100 person years at risk, compared with needle exchange participant groups with seroconversion rates ranging from 1 to 2 per 100 person years at risk. These findings suggest that the use of needle exchange
programs has a substantial protective effect for preventing new HIV infections. However, the results need to be interpreted with care. That is, nonequivalence across groups being compared (needle exchange users versus nonusers) precludes making strong causal inferences about the direct effect of the needle exchange on HIV incidence rates. Nonetheless, these data do reflect a significant association between needle exchange participation and HIV infection (Des Jarlais et al., 1994b, 1995).
Possible Negative Outcomes
Program Participant Drug Use
The most recent studies that have examined drug-use behaviors among needle exchange participants show either stable levels of reported drug injection frequency or even slight declines over time among injection drug users who continue to participate in needle exchange programs (Watters et al., 1994; Paone et al., 1994a; Des Jarlais et al., 1994a; Oliver et al., 1994). In the recent New York City study, Paone et al. (1994a) reported a statistically significant decrease in injection frequency among needle exchange participants, from 95 times in the 30 days preceding program participation to 86 times in the 30 days prior to participants' being interviewed.
The only exception to this reported trend comes from an unpublished research manuscript from Chicago researchers (O'Brien et al., 1995a). As noted in the Preface, as the panel was concluding its deliberations, the Assistant Secretary for Health made public statements that a number of unpublished needle exchange evaluation reports had raised doubts in his mind about the effectiveness of these programs. The panel deemed these statements to be significant in the public debate, therefore necessitating appropriate consideration in order for the panel to be fully responsive to its charge. The panel therefore reviewed the unpublished studies, one of which was the aforementioned O'Brien et al. (1995a) Chicago study. As unpublished findings, this research lacks the authority provided by the peer review and publication process. For this reason, the panel gave special attention to scrutinizing and describing in detail results reported by the researchers, as well as appraising their probative value (see Appendix A).
The investigators infer from their findings that those who participate in needle exchange programs spend more money and inject more frequently than nonparticipants as a result of their participation in the program. Their assertion is based on data that, according to these authors, support the contention that program participation is economically driven (i.e., by the cost of needles). The panel's review raised serious concerns about the tenability of their inferences. For instance, a clearly insufficient theoretical and empirical development of the underlying models is used. That is, there are
numerous other plausible models that could explain their data. From an economic standpoint, it would seem that individual socioeconomic status may be causally related to both drug abuse and use of the needle exchange program, rather than to the explanation that needle exchange programs cause drug use. Nonetheless, the authors do not test any alternative plausible models to assess the relative fit of their models compared with other viable competing models. Moreover, a weak theoretical justification is provided of their postulated model (e.g., cost of needles is the underlying driving force for using the needle exchange, but that cost is minute compared with other expenses, such as the cost of the drugs themselves).
The empirical information provided on key variables is inadequate. Properties of the distributions of key variables are absent and aggregate summary statistics are used in various models without attention to the possible adverse effect of outliers. The presence of such outliers can severely distort the results and challenges the viability of the inferences drawn by these investigators. Substantial inconsistencies between data on key variables (self-report) presented in the manuscript and information extracted from the needle exchange program records raised serious concerns among panel members. Moreover, as discussed in some detail in Appendix A, the panel had serious reservations about the appropriateness of the modeling techniques as implemented by these researchers.
Although this particular study suffers from serious limitations, the conclusions reached by the authors raise interesting questions and hypotheses that should be subjected to sound empirical testing. These issues should be further studied with adequate designs, measures, and analytical methods. In the meantime, in the panel's opinion, these difficulties are serious enough to preclude making causal inferences about the effect of needle exchange programs.
New Initiates to Injection Drug Use
The concern that having the opportunity to use a needle exchange may lead persons who are not currently injecting to begin injecting demands attention, and some information about this is available.
If the opportunity to participate in needle exchange programs were to lead to an increase in the number of new injection drug users, one would expect to see relatively large numbers of young newer injectors at the needle exchange programs. This has not been observed in any of the earlier studies (e.g., Lurie et al., 1993), or in the most recent publications (Paone et al., 1994a, 1994b; Des Jarlais et al., 1994b; Watters et al., 1994).
Investigators in Amsterdam have recently published data that permit examination of the hypothesis that "mixing" of injecting and noninjecting drug users at needle exchanges will lead noninjectors to begin injecting
behavior (van Ameijden et al., 1994). Many of the Amsterdam needle exchanges are operated out of the "low-threshold" methadone programs. These programs provide services to both heroin injectors and heroin smokers and do not require abstinence from illicit drug use as a condition for remaining in the program. Thus, these combined methadone treatment and needle exchange sites do provide frequent opportunities for social interactions between heroin injectors and heroin smokers. Despite this, the proportions of heroin users who smoke and those who inject have remained constant since the exchanges were implemented.
Recent U.S. data also support the conclusion that needle exchange programs do not lead to any detectable increase in drug injection. The recent San Francisco study (Watters, 1994) found an increase in the mean age of injection drug users in the city during the years of operation of the needle exchange programs (i.e., mean age in 1986 was 36 compared with 42 in 1992). Moreover, the author reported that during that 5.5-year period, the median reported frequency of injection declined from 1.9 to 0.7 injection per day and that the percentage of new initiates into injection drug use decreased from 3 to 1 percent. In Portland (Oliver et al., 1994), under 2 percent of program participants had histories of injecting of less than a year. The average duration of injection drug use was 14 years, and more than 75 percent had been injecting for 5 years or more. The presence of a needle exchange program does not appear to cause any increase in the number of new initiates to drug injection. Identifying what factors lead individuals to initiate injection drug use, despite knowing about AIDS, remains an important question for future research.
Discarded Needles and Syringes
Since the University of California report was issued, only one study has dealt with needle exchange programs and improperly discarded needles. Doherty et al.. (1995) conducted a survey of a random sample of city blocks in areas of high drug use in Baltimore before and after implementation of the needle exchange program; their results are consistent with the University of California conclusion that needle exchange programs do not increase the total number of discarded syringes.
THE NEW HAVEN STUDIES
After extended legislative debate, Public Act 90-214 allowed the City of New Haven, Connecticut, to implement—on an experimental basis—a legal needle exchange for injection drug users. On November 13, 1990, the New Haven Needle Exchange Program began operation. This program operated
from a van, typically 6 hours a day, 4 days a week, and traveled to specific sites known to involve high levels of drug activity.
The needle exchange program operated on an anonymous basis. Specifically, participants were assigned a fictitious name as a means of identification and tracking. New enrollees who did not have a needle and syringe to exchange at their first encounter with the needle exchange program were provided with a single ''rig." After that, exchanges were conducted on a one-for-one basis, with a maximum of five needles and syringes issued on each occasion. Syringes that were distributed were coded to enable tracking and evaluation. The program accepted syringes that had not originated from the program. All returned equipment was placed in a metal canister, and all returned equipment was turned over to an evaluation team at Yale University for assessment. In particular, a sample of returned syringes were assessed for the prevalence of HIV.
In addition to exchanging used sterile equipment, program staff provided AIDS education and information on risk reduction. Condoms and bleach packets were provided to all participants at each encounter. All participants were also provided information on drug treatment and a broad range of other relevant services (e.g., tuberculosis and sexually transmitted disease screening through clinics, HIV testing, maternal and child health services); outreach workers also provided participants with direct assistance in accessing drug treatment and other services.
In July 1992, syringe possession without a prescription was decriminalized. This was followed by a reduction in the monthly volume of exchanges at the program (from about 4,000 to a little more than half that number).
The importance of the evidence from the New Haven studies is twofold. They provide: (1) direct evidence of lower levels of HIV infection among needles in use and (2) indirect, model-based estimates of changes in the incidence of new HIV infections among needle exchange program participants.
The direct evidence involves the impact of the needle exchange program on the critical features of program process. Specifically, the evaluation reveals significant and substantial reductions in the infectivity of the syringes exchanged through the needle exchange program. The data also reveal increases in referral to drug treatment and no change in the number of injection drug users.
Prior to the distribution of sterile injection equipment, extremely sensitive DNA analyses using the polymerase chain reaction (PCR) to detect the presence of HIV-infected peripheral blood cells in the returned syringes of existing "street" syringes showed an HIV-positive rate of 0.675; needles from shooting galleries revealed a rate of 0.917; and needles from an underground exchange showed a rate of 0.628. During the first month of the
exchange, HIV-positive rate for needles turned into the exchange was 0.639; within 3 months, this rate declined to 0.406 and remained relatively constant (with an increase to 0.485 at the end of the year—November-December 1991). That is, the prevalence of HIV in needles decreased by one-third.
Program Implementation
Measures of syringe infectivity gradually declined over time, with the sharpest decline occurring in the first 3 months after the implementation of the needle exchange program. If the reduction in the infectivity of needles is due to the activities of the program, it is reasonable to expect changes in program operations that parallel the pattern of reductions in needle infectivity. Data about program operations tend to support the plausibility that reductions in infectivity are connected to the activities of the clients of the needle exchange program and the program itself.
In particular, the number of visits increased more rapidly than the number of clients, suggesting that the same clients were exchanging needles more frequently. Specifically, in December 1990 there were about 100 clients and 150 visits. By June 1992 there were 300 clients and 900 visits.
Program data are also consistent with a fundamental concept of the circulation theory advanced by Kaplan—namely, the law of conservation of needles. Specifically, there was a close match between the number of inbound and outbound needles, and there was a substantial increase in the volume of exchanges between December 1990 and June 1992. That is, the volume of exchanges increased from less than 500 to over 4,000 in June 1992. (After decriminalization in 1992, the volume of exchanges decreased to between 2,000 and 2,500.) Over the entire study period (November 1990 through June 1993), a total of 80,292 needles were distributed; for the same period, the total number of needles that were returned was 78,067. That is, 97.2 percent of the total number of needles distributed were returned to the needle exchange program. It appears that these figures include the "return" of nonprogram needles. In other papers (e.g., Kaplan and Heimer, 1994), return probabilities of about .7 are shown.
Using estimates of the size of the population of injection drug users in New Haven derived by Kaplan and Soloshatz (1993), it appears that about half of the injection drug users have had contact with the needle exchange program (Lurie et al., 1993).
Central to the circulation theory advanced by Kaplan is the notion that "more frequent exchanging should lead to a reduction in mean needle circulation times" (1994b:226). Data obtained from the syringe tracking system confirm this expectation. In December 1990, the mean circulation time for
syringes was about 7 days. (It should be noted that Kaplan's linear regression results project an estimated preprogram circulation time of 23.5 days; according to the plot in Figure 4 of Kaplan (1994b), the empirically based mean circulation time of 7 days is associated with the third month of operation.) Over the course of the intervention, circulation time declined steadily, to about 3 days in September 1991. Circulation time stabilized between 2 and 3 days thereafter (through June 1992). This appears to be consistent with the linear regression estimates provided in Figure 4 of Kaplan (1994b:248). Kaplan concluded that the needle exchange program "appears to be interrupting the needle circulation process in the manner intended" (1994b:25).
To summarize the empirical results so far, evaluation data reveal: (1) increased exchange rates per injection drug user and (2) increased return of program syringes, resulting in a decrease in mean circulation time for each syringe. Because needles are in circulation for shorter periods, there is a decline in the probability of infection. Taken together, these data indicate that the New Haven needle exchange program, a substantial intervention effort, was a plausible contributor to reductions in the infectivity level of needles.
Estimated Effects on HIV Incidence
Kaplan and colleagues (Kaplan and Heimer, 1992; Kaplan and O'Keefe, 1993) could not directly observe HIV infection in needle exchange program clients (as they could in needles) and, as a consequence, turned to a mathematical modeling approach. They estimated the relative effects (the proportionate reduction of incidence per year) and the absolute impact (number of infections prevented per client year) of the New Haven needle exchange program. It was estimated from these models that the project was associated with a relative reduction in HIV incidence of 33 percent.3
It was further estimated that between 1 and 3 infections per 100 participant years were prevented annually.4 A completely different modeling approach (Kaplan and Heimer, 1994b), based on a change point model, yielded a maximum likelihood incidence estimate of zero, with a relatively large confidence interval for that estimated incidence rate (i.e., 0 to 10.2). An update of this rate of new HIV infections among participants yielded a revised maximum likelihood incidence estimate of 1.63 infections per 100 drug injectors per year (Kaplan and Heimer, 1994b, in press), with a 95 percent confidence interval ranging from 0 through 7.2. Moreover, a test of the null hypothesis that no new infections had occurred could not be rejected, providing further support for the efficacy of New Haven's needle exchange program.
Assessment of the Models
Because these assessments are based on mathematical models that, of necessity, must rely on various assumptions, the validity of the resulting estimates hinges critically on the validity of the assumptions that had to be made. Two scientific reviews of the procedures and assumptions embodied in Kaplan's models issued in recent years (U.S. General Accounting Office, 1993; Lurie et al., 1993) provided concordant views regarding Kaplan's models. GAO summarized Kaplan's work as follows (p. 23):
Both our experts found that the mathematical specifications used in both equations appropriately express the dynamic process of HIV transmission among injection drug users via infected needles. They agree in their assessment that the model is technically sound and incorporates all key parameters.
The University of California review states (p. 478):
The circulation model is a very significant contribution to NEP [needle exchange program] evaluation efforts. By focusing on how NEP needles alter the characteristics of needles in circulation, the model circumvents reliance on injection drug user self-reports of behavior change. Rather, the model uses syringe tracking and testing data to demonstrate that even if injection drug users made no effort to change behavior (aside from obtaining needles at the NEP), HIV incidence would drop as a result of lower HIV prevalence in the needles. Any additional reduction in risk behavior (such as cessation of sharing or increased bleaching) would reduce HIV incidence even further.
Concerning the numerical estimates, from applying the model to the study data in New Haven, the GAO review concludes (pp. 23-24):
Our experts agreed that Dr. Kaplan's assumptions serve to underestimate the impact of the New Haven program on the rate of new HIV infections. The expert reviewers strongly believe that 33 percent understates the true percentage reduction in new infections attributable to the program.
The data used in the model were primarily obtained from three sources: (1) data developed from the program's syringe tracking and testing system, (2) self-reports from injection drug users participating in the program, and (3) data developed from other AIDS research studies. Our experts noted that the data values used from these sources are reasonable and produce a conservative estimate of the program's impact on the rate of new HIV transmissions.
The model's estimate that the New Haven needle exchange program results in a reduction of new HIV infections among participants over 1 year is defensible as a minimal estimate of the program's impact. The 33 percent difference is strictly attributable to the reduction in levels of infection in
needles due to the shorter length of time that needles are in use (or needle circulation time).
The University of California concludes (p. 484):
Relative impact would decrease modestly if different values were used for certain model parameters. However, if the model incorporated behavioral risk reductions, relative impact would increase substantially from the 33% published value.
Absolute impact would probably decrease below the published value of 0.021 infections averted per client-year, because the estimate of non-NEP HIV incidence appears to be too high.
The panel's view is that these models provide important qualitative insight into why needle exchange programs should work. However, conclusions from modeling a complex process can rarely have the force of absolute proof. Kaplan and his colleagues recognize this, offering a range of calculations based on competing assumptions, parameter values, and models. Despite these admirable efforts, it is true that unmodeled features of the needle exchange program process might make the efficacy estimates either too high or too low. For example, the Kaplan model does not take account of changes in the percentage of infected participants that result if disproportionately many dropouts from the program population were infected (or were not infected). Likewise, if new entrants to the needle exchange program population were less infected (or more) that would artificially raise (or lower) the apparent effectiveness of the needle exchange program. Therefore, we must regard numerical estimates from these models with some caution.
In summary, the model-based evaluation of the New Haven needle exchange program provides important insights into the dynamics of such programs and useful preliminary estimates of their efficacy. We cannot attach the same level of confidence to these model-based estimates as we could to evaluation programs that included a suitable control group in which individuals were tested (directly) for HIV infection. Unfortunately, such an evaluation program would face formidable obstacles because of concerns about privacy and confidentiality, difficulties ingeniously (and conscientiously) sidestepped by Kaplan's study methods.
Several other outcome variables were also studied at the New Haven needle exchange program, and these are described below.
New Initiates to Injection Drug Use
If needle exchange programs attracted new initiates to injection drug use, a drop in the average age of program participants who enroll over time would be expected to be observed, coupled with a downward shift in the
average number of years of injection drug use. Using demographic data obtained from needle exchange program enrollees over the course of the program operation (November 1990 to December 1991), Heimer and colleagues (Heimer et al., 1993) show that the mean age and mean duration of injection did not change over time. Throughout the study period, male and female enrollees were, on average, approximately 33 to 34 years old. Male enrollees reported using injection drugs for about 10 years; female self-reports on duration showed more month-to-month variability (averaging about 5 to 10 years). From this set of indicators, it would appear that the needle exchange program did not increase the number of new initiates.
The authors also provided an additional observation that counters the argument that needle exchange programs encourage the initiation of injection drug use. They argued that, if the presence of a needle exchange program did enhance use, an increase in the number of new initiates to injection drug use would be most prominent following public disclosure of the first report on the effects of the program. But, at the time of the report's release (and publicity), there was "no increase in the percentage of enrolling clients with very short durations of intravenous drug use" (p. 219).
Enrollment in Drug Treatment
Participants requested drug treatment at a nearly constant rate (25 percent) throughout the study period. The percentage entering treatment increased from 15 percent (first 7 months) to 18 percent (end of 1991). Another noteworthy observation is that a substantial proportion of people who visit the program's van are not needle exchange participants but are visiting the van because they are seeking treatment for drug abuse (Heimer, 1994).
Alternative Explanations
As we have noted in our critique of the model-based estimates of HIV incidence, the change in outcomes (especially the infectivity of needles) might possibly be due to changes in the population served. It is possible that the reduction in the infectivity of needles and syringes could be due to changes in the risk characteristics of participants. But little of the available evidence indicates such client population shifts (Kaplan and Heimer, 1994a). The mean age of enrollees and the mean duration of drug use did not change over the course of the program. The percentage of women remained constant at 20 percent over the course of the study (November 1990 to June 1992). Self-reported drug behaviors were not associated with enrollment date. Analyses of changes over time in frequency of injection, use of shooting galleries, injections shared, using cocaine, and risky injection frequency
failed to show any statistically significant trends. (More sophisticated, multivariate models were also used, with similar results.)
Although drug behaviors and gender remained statistically constant over time, Kaplan and colleagues (Heimer et al., 1993; Kaplan, 1994a) reported that the racial composition of the study population did change over time; the percentage of white participants steadily increased (from 17 to 39 percent). Because white participants are less at risk, the change in HIV prevalence might be due to the change in the composition of the population served, but, as the authors note, this does not appear to be a viable plausible explanation for the decline in the infectivity of needles. The decline occurred in the first 120 days and then stabilized. The number of white participants steadily increased throughout the duration of the project. The magnitude of the change in composition is also not great enough to explain the reduction in HIV seropositivity. Specifically, the authors state (Heimer et al. 1993:219):5
At the start of the program, 83% of the participants were nonwhite and 67.5% of the syringes were infected. After 7 months, 62% of the clients were nonwhite and 43% of the syringes were infected. If needle exchange were without effect, then 87.3% of the syringes returned by nonwhites ought to test positive, a plausible result. However, -29.2% of the syringes returned by whites would need to test positive, clearly an impossible result.
Also, Heimer et al. (1993) argue that the decrease in prevalence was not the result of reduced needle sharing, because the fraction of syringes assigned to one person but returned by someone else did not change. As noted by the authors, because of the manner in which the exchange operated, it is not possible to know with certainty whether discordant needles (i.e., exchanged by one individual and returned by a different person) had been shared or whether they were simply exchanged by someone else.
Finally, Kaplan and others (Kaplan, 1994a; O'Keefe et al., 1991) report that up to 60 percent of the New Haven needle exchange program participants dropped out. Although the status of those who dropped out was not always clear, as noted above, a small fraction of these participants were known to have entered drug treatment. Kaplan (1994a) argues that even short-term exposure to the needle exchange program could contribute to its aggregate impact.
Summary
The pattern of evidence surrounding the New Haven needle exchange program involves a set of models, driven in large measure by empirical data gathered from participants and the needles they exchanged. Although the
estimates of relative and absolute reduction in HIV incidence are based on mathematical models, Kaplan and his colleagues have explored the computational implications of a range of parameter values. These varied models provide estimates that are not dramatically different, lending credibility to the methods. Nevertheless, the models are not infallible.
The most compelling evidence from this set of evaluation studies is the direct evidence from the actual testing of syringes for the presence of HIV positivity. Here the empirical results of monthly assessments show about a one-third reduction in the rates of infected needles. These empirical results are consistent with those produced by the models underlying Kaplan's circulation theory. Furthermore, evidence about the actual operation of the needle exchange program reveals that the mechanisms necessary for change were in place. A substantial number of needles were exchanged (removed from circulation), the frequency of exchanging increased, and the mean circulation time of needles declined. Had these changes not occurred or had there been observed changes in the composition of the study population, the plausibility of the observed effect (i.e., reduction in the rate of infected needles) attributable to the program would have been undercut. Evidence about the program processes strongly suggests that the reduction in the rate of infected needles is plausibly due to the program. Similarly, reduction in the rate of infected needles strongly suggests (but does not directly test) that there should be a reduction in HIV incidence on the order of magnitude projected by Kaplan's models.
In the panel's view, the empirical data clearly indicate that needles used by program participants have a lower probability of being infected and, consequently, program participants are less likely to become infected.
THE TACOMA STUDIES
The first legally authorized needle exchange program in the United States was implemented in Tacoma, Washington, in 1988. There are several reasons for examining the research on the Tacoma needle exchange in some detail. The needle exchange was the dominant HIV prevention effort in the local area, so there is less confounding with other simultaneous HIV prevention efforts than in other geographic areas. Also, several studies have been conducted on the Tacoma needle exchange program, making it possible to assess consistency across different outcome measures and study designs. As a U.S. city with an ethnically diverse population of injection drug users and high rates of both heroin and cocaine injection, Tacoma may be more relevant to the circumstances of other U.S. cities than the European and Australian cities in which other needle exchange programs have been implemented.
The importance of the Tacoma studies on needle exchange programs is
the fact that they provide direct evidence of the incidence of a blood-borne viral disease, spread by needles and sexual contact, among individuals who attended and those who did not attend a needle exchange program. In Tacoma, the prevalence of HIV infection among injection drug users was low, indicative that incident HIV infections would be expected to be rare. However, the rates of two other blood-borne infections, hepatitis B (HBV) and hepatitis C (HCV), were higher and therefore considered as surrogates for HIV infection.
The Program
The Tacoma needle exchange program began operating "unofficially" in August 1988. After informing city officials that a needle exchange would be opening, a community-based organization set up a folding table on a sidewalk in an area of downtown Tacoma where there was a visible concentration of drug users and began exchanging syringes. The unofficial program was officially sanctioned and funded by the local health department beginning in January 1989. A few months later, the health department filed a lawsuit to settle the issue of the legality of the program in view of existing drug paraphernalia laws. In early 1990, a Pierce County Superior Court judge declared that needle exchange was legal in the county. During the past 6 years, the needle exchange has developed into a broad public health program of prevention and education for injection drug users.
At present, the Tacoma needle exchange program consists of two fixed outdoor exchange sites, one located two blocks from the original location and another in a Tacoma neighborhood. Both fixed sites are located near shelters or food kitchens that provide services to homeless persons and operate in areas of the city where there are many injecting drug users. The fixed outdoor sites are open 5 hours per day, 5 days per week. In addition, a community-based organization also operates a mobile needle exchange that can be accessed by phoning exchange workers and arranging to meet and exchange syringes at a mutually agreed-on location within the county. The mobile exchange can be reached during business hours weekdays and Saturdays; exchanges are arranged before or after the fixed sites' hours of operation. A van is used to transport supplies and staff to each of these exchange sites. Syringe exchange is also available within the local public health department clinic pharmacy for 8 hours each weekday.
There are few regulations governing the Tacoma needle exchanges. Participants do not need to register or show identification or proof of drug injection to participate in any exchange program. However, all programs operate on a strict one-for-one basis, and participants must return a syringe for each new syringe they receive. At the pharmacy exchange, a maximum of 20 syringes may be exchanged at any time. At the fixed outdoor and
mobile exchanges, there is no maximum number of syringes that may be exchanged at any time, and single exchanges of more than 1,000 syringes have been recorded. The purpose of imposing no limit on the number of syringes is to encourage injection drug users to build up a large reserve of clean syringes to perhaps enable them to better avoid high-risk situations when they have exhausted their supply. It is estimated that 900,000 syringes were exchanged in Tacoma needle exchange programs in 1994 (90,000 from the pharmacy, the remainder from the fixed outdoor and mobile programs).6
Assistance from injection drug users willing to act as "secondary exchangers" is encouraged, and several have been identified via the mobile exchange program. They have included representatives from groups of gay and bisexual injection drug users and other injection drug user groups who report they are fearful of being exposed as drug injectors if they come to the fixed sites. With each of the secondary exchanges, there is an explicitly stated expectation that syringes will not be sold. Although for a few months in 1993 the pharmacy exchange asked needle exchange participants for donations, at present there is no cost for syringes or any services provided directly by any exchange.
The Tacoma needle exchange program has been the primary source of AIDS education for injection drug users in the county. Exchange workers spend time each day talking with individuals about their own and other injection drug users' behavior in relation to risk of exposure to HIV and other pathogens and about specific prevention strategies. When it was apparent that the exchange was a better setting for one-to-one education than were ad hoc encounters on street corners, the local health department's small-scale "bleach and teach" outreach campaign moved to the needle exchange site. Eventually, needle exchange staff assumed responsibility for providing one-to-one education and counseling to local injection drug users, primarily because regular and frequent visits to the exchange by their clientele offered an opportunity for follow-up contact and counseling. From January to November 1994, a monthly average of 511 one-to-one contacts were made (range 411-724), which consisted of individualized education, counseling, and referral to other services.
Condoms and sexual risk reduction education have been included among the basic services since the program began. The fixed outdoor exchange sites are both within police-defined areas of prostitution in the city, and there are many female and male sex workers among needle exchange participants. In the first 11 months of 1994, approximately 2,900 condoms (range from 2,100 to 3,900) were distributed each month at the exchange sites.
The fixed needle exchange sites have become the primary locations in the county for bringing health and social services to local injection drug
users. Since 1990, a public health nurse has been stationed at the fixed outdoor sites to administer tuberculosis screening tests (the PPD skin test). Those who are given the screening test return to the exchange to have their results read, and further medical workup is arranged for those with positive skin tests. Patients who require antituberculosis medications are scheduled to receive directly observed therapy at the needle exchange. Tuberculosis prevention education is provided to all needle exchange participants through one-to-one counseling and a small-media approach. An average of 175 tuberculosis screening tests are administered to exchange participants each year (Hagan et al., 1992b:8).
HIV testing has also been provided to exchange participants to a limited extent; full implementation has been hindered by the physical setting of the exchange. Both asymptomatic HIV-positive participants and those who have progressed to AIDS are eligible to receive AIDS case management services. The support services given to case management clients provide stability in housing and health care access.
The needle exchange has also become an important source of referral to drug treatment programs in the community. In the first 11 months of 1994, an average of 65 persons were referred to treatment each month. Methadone drug treatment programs, in particular, noted that recruitment at the exchange resulted in enrolling a higher proportion of injection drug users with no previous history of treatment. Furthermore, in 1991 and 1992, the needle exchange was the largest single source of recruitment to methadone treatment programs in the county (Hagan et al., 1993:1694-1695). Since that period, referrals to methadone treatment from the exchange have increased, but program capacity has not kept up with the demand as the number of low-cost, publicly funded treatment slots has plateaued.
In the Tacoma community, the exchange's function of safe disposal of contaminated injection equipment has been considered important. In fact, the local police chief cited public safety and protection of his officers from accidental needlestick injury as the basis for his support of the exchange program (affidavit of Raymond Fjetland, in Tacoma Pierce County Health Department v. City of Tacoma). In addition, a maintenance supervisor responsible for keeping public areas in the vicinity of one of the fixed outdoor sites free of trash and litter noted a dramatic decline in the number of discarded syringes picked up by his crews (affidavit of James Burgess, in Tacoma Pierce County Health Department v. City of Tacoma). In 1990, a sample of returned syringes was collected from the exchange and tested for HIV (Hagan et al., 1991). The virus was detected in 1 percent of 1,200 syringes tested; 2 percent of syringes with visible blood or dirt were HIV-positive. That year, approximately 120,000 used syringes were collected and safely disposed of by the needle exchange.
In Table 7.6 appears a list of five studies that examine various aspects
TABLE 7.6 Tacoma Studies
|
Study |
Design |
Results |
Alternative Explanation |
|
HIV seroprevalencea |
• CDC non-link 5-year survey protocol; • Injection drug user entering methadone treatment; • N = 1,109; • To 1992 |
2 to 4 percent over 5 years' time |
• Low HIV prevalence and incidence imply no presence of transmission risk; needle exchange program does not matter; • Other HIV interventions |
|
Hepatitis surveillance case reportinga |
• CDC sentinel pre-post needle exchange program; • To 1990 |
1985—HBV injection drug user = 40 Sex = 9 Unknown = 13 1990—HBV injection drug user = 7 Sex = 12 Unknown = 6 |
• Due to normal fluctuation in incidence; saturation in injection drug user community (exhaustion of susceptibles); • Local health department implemented other prevention interventions |
|
Hepatitis B and C case controlb |
Case from injection drug user CDC sentinel surveillance 28 injection drug user—HBV 20 injection drug user—HCV; Control from injection drug user from • HIV testing and counseling • Treatment; 38 injection drug user no serologic markers HBV; 26 injection drug user no serologic markers HCV |
HBV • Case—75 percent never used needle exchange program; • Control—26 percent never used needle exchange program; • OR = 8.4; HCV • Case = 75 percent never used needle exchange program; • Control = 26 percent never used needle exchange program; • OR = 8.1 |
• Case control not equivalent groups; • Controls are a bias sample; • Self-selection bias in use of needle exchange program |
|
Interview study 1b |
• To 1989; • Retrospective pre-post; • N = 204 random selection of needle exchange program participants |
Overall unsafe injection Pre = 58 percent Post = 33 percent; Past used Pre = 100 per month Post = 62 per month; Rent Pre = 56 per month Post = 30 per month; Bleach Pre = 69 per month Post = 105 per month |
• Decline in self-report data due to response bias (social desirability); • Self-selection |
|
Interview study 2b |
• To 1991; • Cross-sectional; • Exchange users N = 265; • Non-exchange N = 93; • Random selection of needle exchange participants |
Frequency injection no change; Unsafe injection; Needle exchange program users = 21 percent; Non-needle exchange program = 45 percent; HIV Needle exchange program users = 2 percent; Non-needle exchange program = 7 percent; HIV rates remained stable at follow-up |
• Decline in self-report data due to response bias (social desirability); • Self-selection |
|
NOTE: OR = odds ratio. a Community-level data. b Individual drug user-level data. |
|||
of the Tacoma needle exchange program experience. We consider these studies in the order shown there.
HIV Seroprevalence Studies
Beginning in June 1988, individual entering the health department's methadone drug treatment program were enrolled in an HIV seroprevalence study conducted as part of the CDC Family of HIV Seroprevalence Surveys. A nonlinked design was used in accordance with the CDC unlinked survey protocols, with all eligible clients being enrolled so that an unbiased estimate of seroprevalence is obtained. Eligible clients included those who were not coming to the methadone clinic solely for HIV testing and who had not been previously admitted during the survey period, which corresponded to the calendar year. Demographic and risk behavior information was abstracted from data routinely collected for client records. All persons entering drug treatment were required to have a Venereal Disease Research Laboratory test, and any remaining serum was tested for HIV (Hagan and Hale, 1993).
From June 1988 through December 1992, 1,109 drug treatment clients were enrolled in the seroprevalence survey. HIV seroprevalence remained between 2 and 4 percent during each year of the 5-year period. There was no variation in seroprevalence in relation to gender, age, or race/ethnicity (Hagan and Hale, 1993:10).
The continued maintenance of such a low HIV seroprevalence in a population of injection drug users cannot be unequivocally attributed to the needle exchange program and its many program components. However, this stands in sharp contrast with experience in many places, where no systematic prevention programs were in place and seroprevalence among injection drug users was observed to rise rapidly from low to high levels.
Hepatitis Surveillance and Case Reporting
Pierce County has been one of four U.S. counties participating in the CDC's sentinel hepatitis surveillance system since the late 1970s (Alter et al., 1990a, 1990b).7 The stimulated reporting system includes laboratory-based reporting of serologic findings suggestive of hepatitis and contact with physicians, hospitals, and other health care providers in the community. All confirmed and suspected cases are reported to the local health department's hepatitis surveillance clinic. Public health nurses at the clinic conduct the case investigations and, using a standardized questionnaire, they interview cases and collect demographic and risk-factor information in accordance with the sentinel county study protocol. Hepatitis serologies are performed to specify type of infection.
The surveillance case definition for hepatitis B has included the presence in serum of hepatitis B surface antigen (HBsAg), elevated liver enzymes (SGOT or SGPT) greater than 2.5 times the upper limits of normal, and no other possible causes of liver injury. For hepatitis C, the case definition included absence in sera of both HBsAg and hepatitis A virus immunoglobulin (HAV-IgM), in conjunction with elevated liver enzymes greater than 2.5 times the upper limits of normal and all other possible causes of liver injury ruled out. Hepatitis C cases were presumptively classified as non-A non-B hepatitis until hepatitis C virus antibody (anti-HCV) assays were introduced to diagnose acute illness. The majority of both hepatitis B and hepatitis C cases were symptomatic at the time they were reported.
An outbreak of hepatitis B was observed among injection drug users in Pierce County beginning in 1985:43 incident cases as of December 1985 (Figure 7.1). The incident cases of hepatitis B among injection drug users persisted until several months after the needle exchange opened (i.e., August
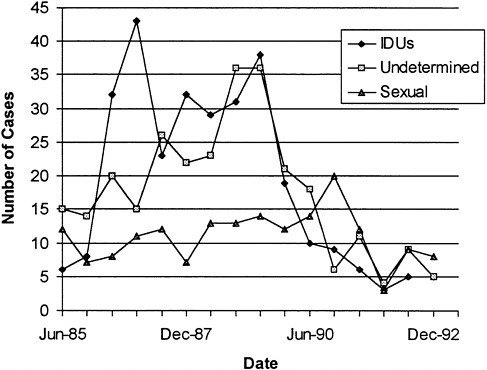
FIGURE 7.1 Hepatitis B incident cases by 6-month intervals, between January 1985 and December 1992.
NOTE: IDU = injection drug user. SOURCE: Adapted from Hagan et al. (1991c:1647).
1988) and then declined rapidly (Hagan et al., 1991c). That is, incident cases peaked in December 1986:43 incident cases among injection drug users were reported, declining to 39 incident cases in December 1989, and further declining to 9 cases as of December 1990. A similar pattern was observed among cases whose source of infection was not identified, whereas the incidence of those cases for which sexual exposure was identified as the primary mode of exposure remained relatively stable over that time period (ranging between 12 and 20 incident cases per 6-month interval between June 1985 and December 1990).
The fact that the reduction of new HBV cases coincided with the introduction of the needle exchange program suggests a plausible positive impact of the exchange. These ecological data alone are subject to alternative explanations. However, when combined with other data from Tacoma, the data support the pattern of evidence suggesting that the abrupt (rather than gradual) reduction in new hepatitis B infections among injection drug users following the opening of the needle exchange program could be in part due to the exchange.
Hepatitis B and C Case-Control Study
Injection drug users who reported to the sentinel hepatitis surveillance system in Pierce County from January 1991 to December 1993 and who met the hepatitis B or hepatitis C case definition (see the previous section) were included in the case series (Hagan et al., in press). Male cases who reported sexual contact with another male were excluded from the study because they may have acquired hepatitis as a result of sexual rather than parenteral exposure to the virus. Cases reporting other risk factors for hepatitis B or C (blood transfusion, health care employment with frequent blood contact, hemodialysis, or sexual or household contact with a confirmed case of hepatitis B or C) were also excluded. In addition to items included in the surveillance questionnaire, a supplemental question was asked about previous use of the needle exchange (Hagan et al., 1994a:5-8).
Control subjects were injection drug users from either of two other health department services, including those attending the HIV-testing center or enrolling in a methadone drug treatment program. Controls were enrolled during the time the cases were being reported. As with the cases, potential controls who were males reporting sexual contact with another male were excluded, and those referred to either health department service by the needle exchange program were also excluded. In addition, hepatitis B controls had to have an absence of any serologic evidence of previous exposure to hepatitis B (negative for HBsAg, antibody to hepatitis B core antigen (anti-HBc), and IgM anti-HBc). Similarly, hepatitis C controls had to have an absence of any serologic evidence of exposure to hepatitis C
(anti-HCV negative). Demographic and behavioral data and serum specimens were collected for routine purposes and recorded on client records. Data were abstracted from client records by study personnel. Residual sera were tested for hepatitis B and C markers at the CDC Hepatitis Reference Laboratory in Atlanta, Georgia.
A total of 28 injection drug users with acute hepatitis B and 20 with acute hepatitis C who met study eligibility criteria were reported to the sentinel surveillance system in Pierce County during the time period 1991 to 1993 (Hagan et al., 1994a:8-9). Controls were 38 injection drug users with no serologic markers of exposure to hepatitis B and 26 with no markers for hepatitis C who were attending health department services during the same calendar period and met all study criteria. Of the hepatitis B cases, 75 percent had never used the needle exchange program, compared with 26 percent of hepatitis B seronegative controls (unadjusted odds ratio = 8.4, with a 95 percent confidence interval [CI] 2.4-30.2). Similarly, the risk of hepatitis C was higher among those who never used the exchange (unadjusted odds ratio = 8.1, with a 95 percent CI 1.8-38.7). For both hepatitis B and C infections, there were no differences between cases and controls in the distributions of gender or race. Injection drug users with hepatitis B were somewhat younger and had injected for fewer years than hepatitis B controls. For hepatitis C, there were no differences between cases and controls in relation to age or duration of injection. Adjusted for gender, race, age, and duration of injection, the odds ratio for the association between nonuse of the exchange and hepatitis B was 5.5, with a 95 percent CI 1.5-20.4. For hepatitis C, the adjusted odds ratio was 7.3, with a 95 percent CI 1.6-32.8 (Hagan et al., 1994a:9-10). These case-control studies indicate a powerful retardant effect of needle exchange program attendance on infection with two blood-borne viral infections, offering support to the wholly independent indications from the New Haven study.
Interview Studies with Injection Drug Users
The first interview study with injection drug users in the county was carried out between November 1988 and December 1989. A systematic random sample of 204 injection drug users attending the needle exchange was drawn and asked to participate in a brief interview (Hagan et al., 1993:1692-1693). Subjects were asked about their behavior during the month prior to their enrollment into the needle exchange program and their behavior during the most recent month following their enrollment. Pre-versus postexchange behavior was compared for individual study subjects.
In the pre-versus postexchange comparison of behavior among exchange users, there were no changes in the rate of injection. However, there were statistically significant declines in the frequency of unsafe injections.
Study subjects reported a mean of 155 injections per month before first use of the exchange compared with 152 injections per month while participating. The number of injections with rented or borrowed syringes declined from 56 per month pre-exchange to 30 per month while participating. The number of occasions when a used syringe was given to another injector also declined from a mean of 100 times to 62 times per month (Hagan et al., 1993:1693-1695). The number of times when bleach was used to disinfect syringes also increased from 69 to 105 times per month. The proportion of exchange users reporting any unsafe injections also decreased, pre-versus postparticipation, from 58 percent to 33 percent (Hagan et al., 1994b:26 and 32).
From 1990 to 1991, a referent group of Pierce County injection drug users not participating in the exchange (nonexchangers) was enrolled in a cross-sectional study (Hagan et al., 1991b). The systematic sampling scheme used in the pre-versus postexchange study was used to select exchange users for the referent group study. Nonexchangers were recruited from health care and social service agencies and street locations in areas where the exchange did not operate. In addition, chain-referral sampling was used to increase the sample size of nonexchangers. Data were collected from both exchange users and nonexchangers through interview and HIV testing. Analysis compared recent behavior reported by exchange users (while participating in the program) with recent behavior reported by nonexchangers during the same calendar period.
In their second interview study, 265 exchange users were compared with 93 nonexchangers. Significantly fewer exchange users (21 percent) reported any unsafe injections than nonexchangers (45 percent) (Hagan et al., 1991b:3 and 5). And 2 percent of exchange users versus 7 percent of nonexchangers were HIV positive. A larger proportion of exchange users were living on the street or in shelters (20 percent) than nonexchangers (8 percent) (Hagan et al., 1991b:3 and 4). There have been no HIV seroconversions detected in either exchange users or nonexchangers in follow-up HIV testing (67 person years follow-up for nonexchangers, 223 person years for exchange users) (Hagan et al., 1994b:27).
Potential Alternative Explanations
We now discuss one or more alternative explanations for the results in each of the separate studies (Table 7.6). First, it should be noted that the magnitude of the observed effects in each of the studies is relatively large, and that the findings are consistent across different potential outcome measures and methodological approaches. HIV seroprevalence has remained low and stable in the area, implying low community seroincidence. HIV seroincidence in a cohort of injection drug users enrolled in the needle
exchange program is low, less than 0.5 per 100 person years at risk. Incidence of acute hepatitis B among injection drug users in the county abruptly declined by 75 percent shortly following the opening of the needle exchange program, whereas incident cases attributable to sexual exposure remained relatively constant.
The case-control studies of incident hepatitis B and C among injection drug users show use of the exchange to be a strong protective factor, and this finding persists after controlling for other potential confounding variables.
The comparison of self-reported risk behavior before and after beginning to use the exchange shows a reduction of almost half. Injection drug users attending the exchange report substantially fewer unsafe injections than those not using it. Those using the exchange also have a substantially lower prevalence of HIV infection.
Although there is at least one alternative explanation for each of the findings from the Tacoma studies, there is no single alternative explanation that could consistently explain the findings across the different studies. Indeed, the possible alternative explanation for one study is often contracted by findings from another study. For example, low community HIV prevalence and the low incidence of HIV infection in the needle exchange cohort study might have been found simply because the conditions for rapid HIV transmission did not exist in Tacoma even before the needle exchange was implemented. This alternative explanation would not explain, however, why the community rate of hepatitis B virus infections among injection drug users fell dramatically after the implementation of the needle exchange or why the exchange users reported large reductions in risk behavior.
Other potential contributing factors may have been legal sales of syringes by pharmacies or saturation of hepatitis infections in the population of injection drug users. However, by taking into account the results of the two interview studies (i.e., reduction in risk behaviors) and the case-control study (protective effect of the needle exchange program), the credibility of the program having a beneficial effect on hepatitis incidence in the county is strengthened. An outbreak of HBV that abruptly subsides several months after the start of the needle exchange program (while sexual cases remain stable) is consistent with a program effect. In outbreaks, an abrupt downward slope in the epidemic curve suggests the impact of an intervention, whereas exhaustion of susceptible or other epidemic features is usually associated with a more gradual decline. This is a generalization, but it piques interest in the data.
An important alternative explanation is that the health department geared up and achieved momentum in case finding and contact tracing and delivered hepatitis B hyperimmune globulin and HBV vaccine. However, this
potential rival explanation still would not explain why no such abrupt decline was observed with the sexually transmitted cases. Moreover, as stated earlier, Pierce County has been part of CDC's hepatitis surveillance system since the late 1970s, and no changes in protocol have been implemented since then. Furthermore, no hepatitis vaccine campaign was ever undertaken in the county (H. Hagan, personal communication, January 1995).
Social desirability effects (telling the interviewer what you believe he or she wants to hear) might explain why needle exchange users report large reductions in their risk behavior and lower frequencies of injection risk behavior than injection drug users not using the exchange (even though the interviews were conducted by research staff separate from the exchange staff). The alternative explanation of social desirability for self-reported risk behavior does not match the findings from the hepatitis case-control studies (Hagan et al., in press), in which injection drug users who used the exchange were much less likely to have been recently infected with hepatitis B and hepatitis C viruses.
Self-selection or volunteer bias might explain why the injection drug users who use the exchange report low levels of current risk behavior and have low incidence of HIV, hepatitis B, and hepatitis C virus infections. The exchange might simply have attracted injection drug users who were concerned about health and were practicing safer injection prior to the implementation of the needle exchange. However, this alternative explanation is not consistent with the exchange users' report of their frequent risk behavior prior to beginning use of the exchange and the community-wide reduction in hepatitis B incidence and the low community prevalence rate of HIV infection.
Case-control studies are always open to the objection that cases and controls may differ in important respects. If cases and controls in the Tacoma study (Hagan et al., in press) were not arising from the same source population, it would result in biased estimates of the associations between needle exchange participation and incident cases of hepatitis B and C. Nonequivalence between controls and cases was not detected on measured demographic characteristics for hepatitis C (sex, race, age, and duration of injection). Hepatitis B cases and controls differed regarding age and duration of injection. Nonetheless, after statistically controlling for such disparities, the association between needle exchange participation and hepatitis B was still found to be significant.
Another concern that may arise is that hepatitis B cases may not be representative of nonselected cases in the community because they were symptomatic. It is true that immunocompromised individuals (e.g., from renal dialysis, steroid use, HIV, and age extremes) are less likely to be symptomatic. However, given the low HIV prevalence, the age range of
study cases, and other factors, these seem unlikely to be a major factor operating in the Tacoma study.
The case-control study report (Hagan et al., in press) can be viewed as having design issues that affect confidence in the inferences that can be drawn. One is the selection of controls.
Controls for this study were injection drug users who were ascertained through entry into drug treatment or enrollment in the county's HIV testing program. Although cases in this study can be argued to be representative of all cases for hepatitis B (Pierce County is a CDC sentinel surveillance site), the selection of controls through the two stated mechanisms raises questions. The underlying issue is the extent to which new drug treatment admissions or enrollees for HIV testing are ''representative" of the overall uninfected population (including those not in treatment or uninterested in HIV testing). The descriptive epidemiologic literature on the characteristics of persons with a history of treatment versus no history of treatment suggests demographic differences; this literature hints at the possibility for bias when limiting ascertainment to treatment or testing programs (Alcabes, 1993). However, analyses of drug-use risk factors for infection for those in treatment compared with those out of treatment indicate that, despite differences in distribution of certain characteristics, patterns of drug-use risk behaviors and infection are similar for both groups. This argues that treatment samples are not biased as far as susceptibility to infections is concerned (Alcabes et al., 1993). Also, prospective studies of factors associated with entry into treatment note similar injection risk behaviors, but increased complications of drug abuse in those entering treatment (Schütz et al., 1994); this suggests that the effect of sampling treatment entrants for the purpose of studying viral infection is likely to be minor.
Nevertheless, the issue of potential of bias for controls selected among treatment entrants and injection drug users who arrive for HIV testing could be real if the needle exchange program makes active referrals into treatment and HIV testing. In the case of the Tacoma study, this apparently occurred, but the researchers made explicit the point that direct referrals were identified and excluded from analysis.
The issue remains whether the probability that controls who were picked from treatment and testing were somehow more likely to have used needle exchange than HBV-seronegative drug users not going into treatment or testing. If the proportion of drug users in a community that used needle exchange was small (e.g., 5 percent) and the proportion in this sample was high, then the discrepancy might be attributed to sampling. However, as Hagan and colleagues note, the proportion of the entire Tacoma community of injection drug users that has been estimated to be enrolled or covered by needle exchange is high (i.e., 50 to 70 percent; see Hagan et al., 1994:10-11)
and not inconsistent with the proportion estimated in the controls in this study. This suggests that the effect of selection bias is probably minor.
In sum, the choice of controls for the study of hepatitis B and C virus infections and needle exchange in Tacoma is intuitively open to criticism. A broader cross section of approaches to sample injection drug users might add confidence in the inferences drawn. However, on closer inspection, there is evidence from other studies to suggest that (1) the sampling approach is not obviously biased; (2) the investigators excluded those who might have biased the sample (referrals); (3) the sample estimates and population estimates for use of needle exchange are not dissimilar; and (4) no mechanism for differential bias could be identified. Taken together, these suggest that, whereas it is prudent to be cautious about the results of any case-control study, the effect of selection bias in this situation is likely to be minimal.
The lack of any consistent alternative explanation for the Tacoma findings leads the panel to accept the primary hypothesis that implementation of the needle exchange program led to substantial risk reduction among local injection drug users, which then led to reduced transmission of blood-borne viruses (both HIV and hepatitis). Although different study designs were used, there was consistency among the results; under these circumstances, it is less likely that the findings are due to bias (Rothman, 1986). Thus, the panel concludes that the Tacoma studies show that a needle exchange program can lead to behavior change and reduced transmission of blood-borne viruses.
Program Effects on New Initiates to Drug Use or Abuse
The Tacoma and New Haven studies and previous reviews had few, if any, empirical data on the impact of needle exchange programs on drug initiation or drug abuse among noninjection drug users. This leaves any conclusion regarding the impact of such programs on nondrug users to be theoretical at best. Although few empirical data are available on how these programs may impact overall drug use in communities that choose to implement such programs, a sizable literature does exit on the etiology of drug use. In this section we first briefly summarize what factors have been found to influence drug-use initiation and progression to drug abuse. Based on that knowledge base we attempt to foresee how needle exchange programs may potentially impact drug-use initiation and/or progression to drug abuse.
Some research suggests that the reasons people begin using drugs are different from the reasons they continue or escalate their use, which is to say, the factors that influence initiation are different from those that influence progression to more serious use (e.g., injection drug use). Several
researchers have found that initiation is often strongly tied to social and peer influences, whereas biological and psychological processes appear to be associated with abuse (Carman, 1979; Kandel et al., 1978; Newcomb and Bentler, 1990; Paton et al., 1977). Even though data may as yet be too sparse to establish firmly that the causes of use are different from the causes of abuse, the evidence consistent with this hypothesis is accumulating (Glantz and Pickens, 1992).
Moreover, the more risk factors to which someone is exposed that encourage use, the more likely he or she is to use or abuse drugs. Exposure to a greater number of risk factors is not only a reliable correlate of use, but it also influences the increase in drug use over time, implying a true causal role for those variables that together make for increased risk (Schreier and Newcomb, 1991). It appears that the presence of particular factors that can encourage drug use are not as important as the accumulation and interaction of such factors in a person's life.
The existing knowledge about risk and protective factors suggests that certain social influences to use drugs have the potential to be impacted by needle exchange programs (Hawkins et al., in press; Clayton and Leukefeld, 1994). Impacting such factors can theoretically either increase or decrease the risk of nondrug users moving from nonuse to use and abuse. Known risk factors include peers who use drugs, current involvement of parents and siblings in drug use, favorable societal and community norms regarding drug use, and favorable personal attitudes toward drug use, which include perceived risk of harm. The effect of needle exchange programs on other risk and protective factors is not likely.
On the positive side, needle exchange and bleach distribution programs may decrease the number of new initiates to drug use or abuse. As described earlier in this chapter, treatment referral and entrance has been a documented result of such programs. Since parental and peer drug use are risk factors for drug initiation and abuse, needle exchange and bleach distribution program participants who are referred to treatment and become abstinent are likely to reduce the likelihood that their children and their close family and friends make the transition from nondrug to drug user.
On the negative side, the presence of needle exchange programs may affect risk factors for drug use and abuse. This includes an increase in favorable community or personal norms and attitudes toward drug use. An increase in clean needles and syringes may lead to a reduction in the perceived risk of AIDS and other blood-borne diseases associated with injection drug use. Furthermore, changes in federal regulations banning the use of federal funds for needle exchange programs may result in the perception that societal resolve against drug use is weakened. However, there is no evidence of an impact of needle exchange programs on these community attitudes and, in general, little evidence of an increase in the number of
nondrug users that move to drug use as a result of such programs in their community. If the effect of needle exchange programs on nondrug users is evident only over the long term because of an extended temporal causal chain—including weakened societal antidrug abuse resolve first affecting community norms and personal attitudes, which, in turn, affect the transition from nonuse to use—then the effect on nondrug users may not be evident in the short term. Although this long-term effect may be possible and should be investigated, there is also reason to believe that the existing evidence of no effect will hold in more controlled and long-term investigations. The relationship between drug-use norms and perceived risk of drug use indicates that the effect of these norms and attitudes is drug specific (Bachman et al., 1990). Since needle exchange programs are likely to affect only risk due to injection, and because nondrug users are extremely unlikely to begin their drug-using careers by using injectable drugs (Kandel et al., 1978, 1992), it is not likely that changes in community or personal norms and attitudes as a result of having needle exchange and bleach distribution programs will increase the risk of the transition of nondrug users into drug use.
Alternatively, it may be possible to curtail the emergence of these theoretical potential negative effects of needle exchange programs on norms and attitudes. There is evidence that drug-use norms and attitudes are manipulable by intervention (Hansen et al., 1988; Hansen and Graham, 1991), and it may be possible, through active norm change strategies, to avoid the potential negative effects of needle exchange programs on norms and attitudes. By stressing to the public the fact that these programs are health approaches taken to curb the spread of contagious diseases (e.g., AIDS, HBV, HCV), rather than remaining neutral or leaving interpretation solely to community and personal impressions, it may be possible to avoid potentially adverse community norm changes.
All of these issues need to be properly addressed in future research to clarify whether possible long-term harms associated with the implementation of needle exchange programs are tenable.
SUMMARY
The following conclusions and recommendations are necessarily built on the progressive presentation of information and research data found in this and earlier chapters. This presentation reflects the cumulative development of the panel's understanding about issues inherent in the establishment of needle exchange and bleach distribution programs and, ultimately, their anticipated effects, based on the pattern of evidence discerned by the panel from its collective activities, primarily its reviews of pertinent studies.
Conclusions
The panel found sufficient evidence among the studies reviewed to reach the following conclusions:
-
Needle exchange programs increase the availability of sterile injection equipment.
-
For the participants in a needle exchange program, the fraction of needles in circulation that are contaminated is lowered by this increased availability. This amounts to a reduction in an important risk factor for HIV transmission.
-
The lower the fraction of needles in circulation that are contaminated, the lower the risk of new HIV infections.
The first two conclusions are amply supported by empirical evidence. The third is a logical consequence: if a needle has a lower probability of being contaminated, then it necessarily has a smaller chance of infecting the user. Direct empirical evidence (from a case-control study) confirms this proposition when hepatitis B virus and hepatitis C virus (more virulent than HIV) are the infections in question. HBV and HCV are spread by contaminated needles in the same population, and needle exchange was shown to reduce the incidence of new cases of these (less rare) blood-borne viral infections.
The panel further concludes that:
-
Additional possible positive outcomes are reported by the users of needle exchange programs, including:
-
increased cleaning of used needles;
-
decreased sharing of needles; and
-
uncertain and probably small improvements in risky sexual behaviors (fewer partners, more condom use).
-
-
Needle exchange programs report increased referrals to drug abuse treatment and, in the few studies that examined this issue, no increase in the number of dirty needles discarded in public places (e.g., parks, streets, alleys).
Unfavorable aspects of needle exchange and bleach distribution programs also demand consideration. The act of giving a needle—however clean—to an injection drug user has a powerful symbolism that has sparked fears about the potential negative effects of needle exchange programs. Similar fears sometimes appear in response to proposals to distribute bleach
to injection drug users. However, the record shows little evidence in support of these concerns.
-
There is no credible evidence to date that drug use is increased among participants as a result of programs that provide legal access to sterile equipment. (Long-term effects are necessarily not yet known, providing a reason for continued monitoring for potential negative effects.)
-
The available scientific literature provides evidence based on self-reports that needle exchange programs:
-
do not increase the frequency of injection among program participants and
-
do not increase the number of new initiates to injection drug use.
-
-
The available scientific literature provides evidence that needle exchange programs:
-
have public support, depending on locality, and
-
have public support that tends to increase over time (where trend data are available).
-
The high level of concern about potential negative effects of needle exchange and bleach distribution programs cannot be ignored, despite the paucity of supporting evidence. Communities wracked with drug abuse and addiction, AIDS, crime, and poverty may well resent the institution of needle exchange and bleach distribution programs, seeing the programs as a wholly inadequate response to the key problems. Attention to comprehensive responses to the drug epidemic is clearly important, especially the expansion of drug treatment to make it more available. Needle exchange programs should be regarded as a public health promotion and disease prevention strategy that fits within the broader harm reduction approach to public health.
It is essential that prevention programs (including initiation of needle exchange programs) must vary regionally and locally to reflect those infected or at risk in any area. Thus, although the panel supports the use of needle exchange and bleach distribution programs as part of a nationwide HIV prevention strategy, it is absolutely critical that their use should be driven by the nature of the epidemic in different locales.
Recommendations
The specific charge to this panel was to examine the effectiveness of syringe exchange and bleach distribution as methods of reducing HIV transmission.
This necessarily led to some consideration of other methods of reducing HIV transmission.
Reducing drug use would serve to reduce HIV transmission as well as to achieve other important social and public health goals. Comprehensive drug treatment is one important way to reduce drug use. However, (1) treatment, especially comprehensive treatment, is inadequately available; (2) treatment does not work for all individuals who enter it; and (3) not all drug abusers currently are willing ("wish") to enter treatment.
For all of these reasons, researchers have explored the efficacy of more limited programs, such as needle exchange and bleach distribution, as a means of reducing the risk of HIV infection by providing users not able to undertake drug treatment access to uncontaminated injection equipment.
Based on a comprehensive review of the research literature, the panel concludes that well-implemented needle exchange programs can be effective in preventing the spread of HIV and do not increase the use of illegal drugs. Hence, we recommend that:
-
The Surgeon General make the determination called for in P.L. 102-394, section 514, 1993, necessary to rescind the present prohibition against applying any federal funds to support needle exchange programs.
Observe that the panel does not recommend a mandated national program of needle exchange and bleach distribution. As documented in this report, regional variation in prevalence of HIV infection, the extent and kind of drug use, the presence of other AIDS programs, operational characteristics of existing needle exchange programs, and the attitudes and needs of local communities all influence the potential effects of needle exchange programs and militate against such a mandate. The recommendation is to allow communities that desire such programs to institute them, using resources at their disposal and unencumbered by the specific funding handicap that is now in place.
If needle exchange programs become available tools of public health and disease prevention, certain implementation measures become desirable. In particular, the panel recommends that:
-
Local community members (e.g., police, church, treatment providers, pharmacists, local public health authorities) should be involved in determining whether such programs should be implemented locally and how they should be institutionalized.
-
Attention must be given to the development of site-specific programs that are community based, culturally sensitive, and capable of demonstrating respect for the concerns of the communities in which they are to
-
be based. The importance of flexibility and community control is strongly emphasized.
-
Appropriate health agencies should make available technical assistance and relevant epidemiologic data to local organizations and groups within the communities to assist them in making informed decisions about needle exchange and bleach distribution programs.
-
Needle exchange programs should promote HIV prevention not only by providing sterile equipment, but also by means of education, drug treatment referral, and materials, including bleach, alcohol pads, and condoms.
-
Needle exchange programs should make special efforts to reach and retain hard-to reach subgroups of injection drug users, such as young injection drug users and women.
-
The National Institutes of Health, the Centers for Disease Control and Prevention, and the Agency for Health Care Policy and Research should support evaluation research examining the programs and the key outcomes, including HIV risk behavior and reduced HIV transmission.
The panel further recommends that in meeting the need for increasing the treatment capacity, as described above,
-
Incremental funds for needle exchange programs and other AIDS prevention strategies should be appropriated but should not be taken from resources now supporting drug treatment programs.
In addition, such a diversion of funds would be unwise because drug treatment programs have been shown to be effective in treating the underlying disorder of drug abuse and can be effective in curtailing HIV risk behaviors. Moreover, for many program participants, needle exchange and bleach distribution programs have been found to serve as a bridge to drug treatment for many needle exchange program clients. Indeed, the panel further recommends that:
-
The appropriate legislative bodies should enact legislation (and should appropriate monies) to increase drug treatment capacity and establish better links between treatment and AIDS prevention programs that target injection drug users.
Finally, the panel recommends that:
-
The National Institutes of Health (e.g., National Institute on Drug Abuse) and the Centers for Disease Control and Prevention should support research that evaluates the effect of needle exchange and bleach distribution
-
programs on the severity of abuse and addiction among needle exchange and bleach distribution program participants.
-
A better monitoring system should be established for assessing long-term societal changes in drug use at the community level due to needle exchange programs.
NOTES
REFERENCES
Alcabes, P., E.E. Schoenbaum, and R.S. Klein 1993 Correlates of rate of decline of CD4+ lymphocytes among intravenous drug users infected with human immunodeficiency virus. American Journal of Epidemiology 137:989-1000.
Alter, M.J., A. Mares, S.C. Hadler, and J.E. Maynard 1987 The effect of underreporting on the apparent incidence and epidemiology of acute viral hepatitis. American Journal of Epidemiology 125:133-139.
Alter, M.J., S.C. Hadler, and H.S. Margolis 1990a The changing epidemiology of hepatitis B in the United States. Journal of the American Medical Association 263:1218-1222.
Alter, M.J., S.C. Hadler, and F.N. Judson 1990b Risk factors for acute non-A, non-B hepatitis in the United States and association with hepatitis C virus infection. Journal of the American Medical Association 264:2231-2235.
Bachman, J.G., L.D. Johnston, and P.M. O'Malley 1990 Explaining the recent decline in cocaine use among young adults: Further evidence that perceived risks and disapproval lead to reduced drug use. Journal of Health and Social Behavior 3(June):173-184.
Bruneau, J., F. Lamothe, E. Franco, N. Lachance, J. Vincelette, and J. Stoto 1995 Needle Exchange Program (NEP) Attendance and HIV-1 Infection in Montréal: Report of a Paradoxical Association. Abstract for International Conference on the Reduction of Drug Related Harm, Palazzo dei Congressi, Florence, Italy, March 26-30.
Carman, R.S. 1979 Motivations for drug use and problematic outcomes among rural junior high school students. Addictive Behaviors 4:91-93.
Clayton, R.R., and C.G. Leukefeld 1994 Drug Use and Its Progression to Drug Abuse and Drug Dependence: Implications for Needle Exchange and Bleach Distribution Programs. Paper commissioned by
the Panel on Needle Exchange and Bleach Distribution Programs, National Research Council and Institute of Medicine.
Cordray, D.S. 1986 Quasi-experimental analysis: A mixture of methods and judgment. New Directions for Program Evaluation 31:9-27.
Davoli, M., C.A. Perucci, D.D. Abeni, M. Arcà, G. Brancato, F. Forastiere, P.M. Montiroli, and F. Zampieri 1995 HIV risk-related behaviors among injection drug users in Rome: Differences between 1990 and 1992. American Journal of Public Health 85(6):829-832.
Des Jarlais, D.C. 1994 Current Findings in Syringe Exchange Research: A Report to the Task Force to Review Services for Drug Misusers. United Kingdom: Department of Health. in press HIV epidemiology and interventions among injecting drug users. Journal of the Royal Society of Medicine.
Des Jarlais, D.C., and H. Maynard 1992 Evaluation of Needle Exchange Program on HIV Risk Behaviors: Supplemental Final Report. American Foundation for AIDS Research. September 10.
Des Jarlais, D.C., S.R. Friedman, and W. Hopkins 1985 Risk reduction for the acquired immunodeficiency syndrome among intravenous drug users. Annals of Internal Medicine 103:755-759.
Des Jarlais, D.C., S.R. Friedman, J.L. Sotheran, J. Wenston, M. Marmor, S.R. Yancovitz, B. Frank, S. Beatrice, and D. Mildvan 1994a Continuity and change within an HIV epidemic: Injecting drug users in New York City, 1984 through 1992. Journal of the American Medical Association 271(2):121-127.
Des Jarlais, D.C., D. Paone, M. Marmor, S. Titus, J.L. Sotheran, and S.R. Friedman 1994b New York City Syringe Evaluation: The New York City Syringe Exchange Program: Evaluation of a Public Health Intervention. Paper presented at a Conference of the American Public Health Association, Washington, DC, November.
Des Jarlais, D.D., D. Paone, M. Marmor, S. Titus, Q. Shi, T. Perlis, J.L. Sotheran, and S.R. Friedman 1995 New York City Syringe Evaluation: HIV Risk Behavior and Seroincidence Among Injecting Drug Users in the New York City Syringe Exchange Programs. Paper submitted for publication.
Doherty, M.C., R.S. Garfein, B. Junge, P. Beilenson, and D. Vlahov 1995 Discarded Needles Do Not Increase With a Needle Exchange Program. Paper presented at The Second National Conference on Human Retroviruses and Related Infections, American Society for Microbiology, Washington, DC.
Dolan, K., M. Donoghoe, S. Jones, and Stimson, G. 1991 A Cohort Study of Syringe Exchange Clients and Other Drug Injectors in England, 1989 to 1990. The Centre for Research on Drugs and Health Behaviour. April.
Donoghoe, M.C. G.V. Stimson, K. Dolan, and L. Alldritt 1989 Changes in HIV risk behavior in clients of syringe-exchange schemes in England and Scotland. AIDS 3:267-272.
Donoghoe, M., K. Dolan, and G. Stimson 1991 Changes in Injectors' HIV Risk Behavior and Syringe Supply in UK 1987-90. Abstract ThC 45 in Final Program and Abstracts of the VII International Conference on AIDS, Florence.
Feldman, H. P. Biernacki, T. Knapp, and E. Margolis 1989 Modification of Needle Use in Out-of-Treatment Intravenous Drug Users. Abstract
ThDP 62 in Final Program and Abstracts of the V International Conference on AIDS, Montréal.
Glantz, M.D., and R.W. Pickens 1992 Vulnerability to drug abuse: Introduction and overview. Pp. 1-14 in M. Glantz and R. Pickens, eds., Vulnerability to Drug Abuse . Washington, DC: American Psychological Association.
Guydish, J. A. Abramowitz, W. Woods, J. Newmeyer, G. Clark, and J. Sorensen 1989 Sharing Needles: Risk Reduction Among Intravenous Drug Users in San Francisco. Abstract ThDP 34 in Final Program and Abstracts of the V International Conference on AIDS, Montréal.
Guydish, J. J. Bucardo, M. Young, W. Woods, O. Grinstead, and W. Clark 1993 Evaluating needle exchange: Are there negative effects? AIDS 7:871-876.
Hagan, H., and C.B. Hale 1993 HIV-1 Seroprevalence Surveys in Pierce County. Report available from Tacoma-Pierce County Health Department.
Hagan, H., D.C. Des Jarlais, D. Purchase, S.R. Friedman, T. Damrow, R. Ip, N. Mellor, T.R. Reid, and D. Villareal 1991a Syringe seroprevalence in relation to seroprevalence among syringe exchange users and accidental HIV transmission. Proceedings of the 119th Meeting of the American Public Health Association, November 10-14, Atlanta, GA.
Hagan, H., D.C. Des Jarlais, D. Purchase, T.R. Reid, and S.R. Friedman 1991b Lower HIV Seroprevalence, Declining HBV and Safer Injection in Relation to the Tacoma Syringe Exchange. Abstract WC 3291 in Final Program and Abstracts of the VII International Conference on AIDS, Florence.
Hagan, H., D.C. Des Jarlais, D. Purchase, S.R. Friedman, T.R. Reid, and T.A. Bell 1991c The incidence of HBV infection and syringe exchange programs [letter]. Journal of the American Medical Association 266:1646-1647.
Hagan, H., D.C. Des Jarlais, S.R. Friedman, D. Purchase, and T. Bell 1992a Oral presentation at Kaiser Foundation Conference, Menlo Park, CA.
Hagan, H., D.C. Des Jarlais, S.R. Friedman, D. Purchase, and T.R. Reid 1992b Potential for multiple public health functions of a syringe exchange. Proceedings of the 120th Annual Meeting of the American Public Health Association, November, Washington DC.
Hagan, H., D.C. Des Jarlais, D. Purchase, S.R. Friedman, T.R. Reid, and T.A. Bell 1993 An interview study of participants in the Tacoma, Washington, syringe exchange. Addiction 88:1691-1697.
Hagan, H., D.C. Des Jarlais, S.R. Friedman, D. Purchase, and M.J. Alter 1994a Reduced risk of hepatitis B and hepatitis C among injecting drug users participating in the Tacoma syringe exchange program. Manuscript submitted for review.
Hagan, H., D.C. Den Jarlais, S.R. Friedman, and D. Purchase 1994b Risk for human immunodeficiency virus and hepatitis B virus in users of the Tacoma syringe exchange program. Pp. 24-34 in Proceedings, Workshop on Needle Exchange and Bleach Distribution Programs. National Research Council and Institute of Medicine. Washington, DC: National Academy Press.
Hagan, H. D.C. Des Jarlais, S.R. Friedman, D. Purchase, and M.J. Alter in press Reduced risk of hepatitis B and hepatitis C among injecting drug users participating in the Tacoma syringe exchange program. American Journal of Public Health.
Hankins, C., S. Gendron, J. Bruneau, and E. Roy 1994 Evaluating Montréal's needle exchange CACTUS-Montréal. Pp. 83-90 in Proceedings, Workshop on Needle Exchange and Bleach Distribution Programs. National Research Council and Institute of Medicine. Washington, DC: National Academy Press.
Hansen, W.B., and J.W. Graham 1991 Preventing alcohol, marijuana, and cigarette use among adolescents: Peer pressure resistance training versus establishing conservative norms. Preventive Medicine 20(3):414-430.
Hansen, W.B., J.W. Graham, B.H. Wolkenstein, B.Z. Lundy, J. Pearson, B.R. Flay, and C.A. Johnson 1988 Differential impact of three alcohol prevention curricula on hypothesized mediating variables. Journal of Drug Education 18(2):143-153.
Hartgers, C., E.C. Buning, G.W. van Santen, A.D. Verster, and R.A. Coutinho 1989 The impact of the needle and syringe-exchange programme in Amsterdam on injecting risk behaviour. AIDS 3:571-576.
Hartgers, C., E. van Ameijden, J. van den Hoek, and R. Coutinho 1992 Needle sharing and participation in the Amsterdam syringe exchange among HIV-seronegative injecting drug users. Public Health Reports 107:675-681.
Hawkins, D., M.W. Arthur, and R.F. Catalano in press Preventing substance abuse. In D. Farrington and M. Tonry, eds., Crime and Justice: A Review of Research, Vol. 18. Crime Prevention. Chicago: University of Chicago Press.
Hawkins, J.D., R.F. Catalano, and J.L. Miller 1992 Risk and protective factors for alcohol and other drug problems in adolescence and early adulthood: Implications for substance abuse prevention. Psychological Bulletin 112(1):65-105.
Heimer, R. 1994 Presentation at Focus Group on HIV and Substance Abuse, July 28, Washington, DC.
Heimer, R., E.H. Kaplan, K. Khoshnood, B. Jariwala, and E.C. Cadman 1993 Needle exchange decreases the prevalence of HIV-1 proviral DNA in returned syringes in New Haven, Connecticut. American Journal of Medicine 95(2):214-220.
Hill, A.B. 1965 The environment and disease: Association or causation? President's address at January 14 meeting. Proceedings of the Royal Society of Medicine 163(series B):295-300.
Hunter, G.M., M.C. Donoghoe, G.V. Stimson, T. Rhodes, and C.P. Chalmers 1995 Changes in the injecting risk behaviour of injecting drug users in London, 1990-1993. AIDS 9:493-501.
Kandel, D.B., R.C. Kessler, and R.S. Margulies 1978 Antecedents of adolescent initiation into stages of drug use: A developmental analysis. Journal of Youth and Adolescence 7:13-40.
Kandel, D.B., K. Yamaguchi, and K. Chen 1992 Stages of progression in drug involvement from adolescence to adulthood. Journal of Studies on Alcohol 53(5):447-457.
Kaplan, E.H. 1994a A method for evaluating needle exchange programmes. Statistics in Medicine 13:2179-2187.
1994b Operational modeling of needle exchange programs. Pp. 202-249 in Proceedings, Workshop on Needle Exchange and Bleach Distribution Programs. National Research Council and Institute of Medicine. Washington, DC: National Academy Press. in press Probability Models of Needle Exchange Programs. Operations Research.
Kaplan, E.H., and R. Heimer 1992 HIV prevalence among intravenous drug users: Model-based estimates from New Haven's legal needle exchange. Journal of Acquired Immune Deficiency Syndromes 5:163-169.
Kaplan, E.H. and R. Heimer 1994a A circulation theory of needle exchange. AIDS 8(5):567-574.
1994b HIV incidence among needle exchange participants: Estimated from syringe tracking and testing data. Journal of Acquired Immune Deficiency Syndromes 7(2):182-189. in press HIV incidence among New Haven needle exchange participants: Updated estimates from syringe tracking and testing data. Journal of Acquired Immune Deficiency Syndromes.
Kaplan, E.H., and E. O'Keefe 1993 Let the needles do the talking! Evaluating the New Haven needle exchange. Interfaces 23:7-26.
Kaplan, E.H., and D. Soloshatz 1993 How many drug injectors are there in New Haven? Answers from AIDS data. Mathematical and Computer Modelling 17:109-115.
Klee, H., and J. Morris 1994 Needle Exchange Schemes: Increasing the Potential for Harm Reduction Among Injecting Drug Users. In Tenth International Conference on AIDS, Yokohama, Japan.
Klee, H., J. Faugier, C. Hayes, and J. Morris 1991 The sharing of injecting equipment among drug users attending prescribing clinics and those using needle-exchanges. British Journal of Addiction 86:217-223.
Lamothe, F., J. Bruneau, R. Coates, J.G. Rankin, J. Soto, R. Arshinoff, M. Brabant, J. Vincelette, and M. Fauvel 1993 Seroprevalence of and risk factors for HIV-1 infection in injection drug users in Montréal and Toronto: A collaborative study. Canadian Medical Association Journal 149(7):945-951.
Lange, W.R., F.R. Snyder, D. Lozovsky, V. Kaistha, M.A. Kaczaniuk, and J.H. Jaffe 1988 Geographic distribution of human immunodeficiency virus markers in parenteral drug abusers. American Journal of Public Health 78(4):443-446.
Lewis, D.K., and J. K. Watters 1994 Sexual behavior and sexual identity in male injection drug users. Journal of Acquired Immune Deficiency Syndromes 7:190-198.
Lurie, P., A.L. Reingold, B. Bowser, D. Chen, J. Foley, J. Guydish, J.G. Kahn, S. Lane, and J. Sorensen 1993 The Public Health Impact of Needle Exchange Programs in the United States and Abroad, Volume 1. San Francisco, CA: University of California.
National Research Council and Institute of Medicine 1994 Proceedings, Workshop on Needle Exchange and Bleach Distribution Programs. Washington, DC: National Academy Press.
Newcomb, M.D., and P.M. Bentler 1990 Antecedents and consequences of cocaine use: An eight-year study from early adolescence to young adulthood. Pp. 158-181 in L. Robins, ed., Straight and Devious Pathways from Childhood to Adulthood. Cambridge, Mass.: Cambridge Press.
O'Brien, M.U., J. Murray, F. Cannarozzi, A. Jimenez, W. Johnson, L. Ouellet, and W. Wiebel 1995 Needle Exchange in Chicago: The Demand for Free Needles and Their Effect on Injecting Frequency and Needle Use. Draft manuscript.
O'Keefe, E., E. Kaplan, and K. Khoshnood 1991 Preliminary Report: City of New Haven Needle Exchange Program. City of New Haven, July 31.
Oliver, K. S.R. Friedman, H. Maynard, and D.C. Des Jarlais 1991 Behavioral Impact of the Portland Syringe Exchange Program: Some Preliminary Results. Presentation at Third National AIDS Demonstration Research Conference.
Oliver, K., S. Friedman, H. Maynard, D. Des Jarlais, and D. Fleming 1992 Comparison of Behavioral Impacts of Syringe Exchange, and Community Impacts of an Exchange. Abstract PoC 4284 in Final Program and Abstracts of the VII International Conference on AIDS, Amsterdam.
Oliver, K., H. Maynard, S.R. Friedman, and D.C. Des Jarlais 1994 Behavioral and community impact of the Portland syringe exchange program. Pp. 35-46 in Proceedings, Workshop on Needle Exchange and Bleach Distribution Programs. National Research Council and Institute of Medicine. Washington, DC: National Academy Press.
Paone, D., D.C. Des Jarlais, S. Caloir, and P. Friedmann 1993 AIDS Risk Reduction Behaviors Among Participants of Syringe Exchange Programs in New York City, USA. Abstract PO-C24-3188 in Final Program and Abstracts of the IX International Conference on AIDS, Berlin.
Paone, D., D.C. Des Jarlais, S. Caloir, P. Friedmann, I. Ness, and S.R. Friedman 1994a New York City syringe exchange: An overview. Pp. 47-63 in Proceedings, Workshop on Needle Exchange and Bleach Distribution Programs. National Research Council and Institute of Medicine. Washington, DC: National Academy Press.
Paone, D., D.C. Des Jarlais, S. Caloir, B. Jose, and S.R. Friedman 1994b New York City Syringe Exchange: Expansion, Risk Reduction, and Seroincidence. Abstract for Tenth International Conference on AIDS and STD, Yokohama, Japan, August 7-12.
Paton, S., R.C. Kessler, and D.B. Kandel 1977 Depressive mood and illegal drug use: A longitudinal analysis. Journal of Genetic Psychology 131:267-289.
Rothman, K. 1986 Modern Epidemiology. Boston, MA: Little, Brown and Company.
Schreier, L.M., and M.D. Newcomb 1991 Psychological predictors of drug use initiation and escalation: An expansion of the multiple risk factors hypothesis using longitudinal data. Contemporary Drug Problems 18:31-37.
Schutz, C.G., D. Vlahov, J.C. Anthony, and N.M. Graham 1994 Comparison of self-reported injection frequencies for past 30 days and 6 months among intravenous drug users. Journal of Clinical Epidemiology 47(2):191-195.
Schwartzkoff, J. 1989 Evaluation of the New South Wales Needle and Syringe Exchange Program. Department of Health. November.
Stimson, G.V., L.J. Aldritt, K.A. Dolan, M.C. Donoghoe, and R.A. Lart 1988 Injecting Equipment Exchange Schemes: Final Report. The Centre for Research on Drugs and Health Behaviours.
Stimson, G., M. Donoghoe, and K. Dolan 1989 Changes in HIV Risk Behavior in Drug Injectors Attending Syringe-Exchange Projects in England and Scotland. Abstract WAP 108 in Final Program and Abstracts of the V International Conference on AIDS, Montréal.
Stimson, G.V., J. Keene, N. Parry-Langdon, and S. Jones 1991 Evaluation of the Syringe Exchange Programme in Wales, 1990-91: Final Report to Welsh Office. Centre for Research on Drugs and Health Behaviour. December.
U.S. General Accounting Office 1993 Needle Exchange Programs: Research Suggests Promise as an AIDS Prevention Strategy. (GAO/HRD-93-60). Washington, DC: U.S. Government Printing Office.
van Ameijden, E.J.C., J.A.R. van den Hoek, and R.A. Coutinho 1993 A Major Decline in Risk Behavior Over 6 Years Among IDUs. Abstract WS-C21-2 in Final Program and Abstracts of the IX International Conference on AIDS, Berlin.
van Ameijden, E.J.C., J.A.R. van den Hoek, C. Hartgers, and R.A. Coutinho 1994 Risk factors for the transition from noninjection to injection drug use and accompanying AIDS risk behavior in a cohort of drug users. American Journal of Epidemiology 139:1153-1163.
Watters, J.K. 1994 Trends in risk behavior and HIV seroprevalence in heterosexual injection drug users in San Francisco, 1986-1992. Journal of Acquired Immune Deficiency Syndromes 7:1276-1281.
Watters, J., and Y. Cheng 1991 Syringe Exchange in San Francisco: Preliminary Findings. Abstract ThC 99 in Final Program and Abstracts of the VII International Conference on AIDS, Florence.
Watters, J.K., M.J. Estilo, G.L. Clark, and J. Lorvick 1994 Syringe and needle exchange as HIV/AIDS prevention for injection drug users. Journal of the American Medical Association 271(2):115-120.

































































