3 Needle Exchange and Bleach Distribution Programs in the United States
INTRODUCTION
In an effort to curb the rate of HIV infection among injection drug users in the United States, needle exchange programs have been instituted in 20 states. In September 1993, a total of 33 active needle exchange programs were reported by the University of California/Centers for Disease Control and Prevention (Lurie et al., 1993a) to be operating in the United States. Since that time, new programs have opened in Baltimore, Boston, Milwaukee, and Dallas, and legislation has been passed to establish needle exchange programs in Minnesota and Rhode Island. A survey conducted in October 1994 reported 76 needle exchange programs in 55 U.S. cities (North American Syringe Exchange Network, 1994).
To date, no systematic survey of bleach distribution programs in the United States has been reported. However, information about bleach distribution is described in a report by the National Institute on Drug Abuse (NIDA), which covers 41 projects in 50 cities nationwide (National Institute on Drug Abuse, 1994).
The purpose of this chapter is to describe the needle exchange and bleach distribution programs that are currently active in the United States, their operational characteristics, and the on-site services offered. In addition, whenever available, the demographic characteristics of program participants are described.
Although information about individual programs is accessible, comparative
studies across programs are sparse. It also is clear from the data on individual programs that some recruit small and others large numbers of participants. If prevention programs are to be effective, it seems reasonable to suggest that they need to be able to recruit large numbers of individuals at risk. Another purpose of this chapter is therefore to summarize case studies of selected programs to examine organizational characteristics that might affect their recruitment of participants. The chapter includes a brief discussion of the cost associated with operating a needle exchange program and cost-effectiveness estimates from the literature.
The material presented in this chapter contributes to the panel's overall assessment of the effectiveness of needle exchange and bleach distribution programs, and its findings and conclusions are integrated in the recommendations that appear in Chapter 7. As stated in the Introduction, this approach reflects the development of the panel's deliberations on the issues.
NEEDLE EXCHANGE PROGRAMS
Needle exchange programs either distribute sterile needles or exchange used needles for new ones. (The first programs were initiated by activists and advocacy groups in violation of prescription drug laws and drug paraphernalia laws.) Most also offer a variety of other services and/or referrals, including HIV screening and counseling, screening for tuberculosis and sexually transmitted diseases, substance abuse counseling, primary medical care, case management, health education, and condom and bleach distribution.
The primary sources for the information that follows are a report prepared by the School of Public Health, University of California, Berkeley, and the Institute for Health Policy Studies, University of California, San Francisco (Lurie et al., 1993a, 1993b), and reports on the Washington, D.C., and Baltimore needle exchange programs, which opened subsequent to the University of California report.
Legal Issues
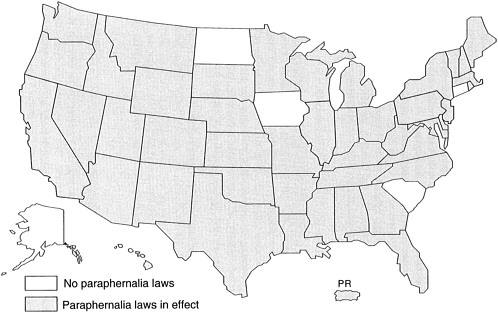
The status of needle exchange programs according to existing laws primarily determines their characteristics. The most important laws affecting needle exchange programs are drug paraphernalia and prescription drug laws. A total of 45 states and the District of Columbia (Valleroy et al., in press) have paraphernalia laws that prohibit the possession of needles and syringes for the purpose of using illicit drugs (Figure 3.1). Of the states operating needle exchange programs, Alaska is the only one not restricted by such a law.
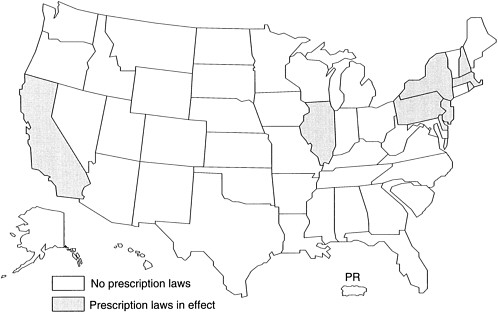
Nine states and the District of Columbia (Valleroy et al., in press) have
laws requiring a prescription to purchase needles and syringes (Figure 3.2). Four of these states—California, Illinois, Massachusetts, and New York—have needle exchange programs. In this report, a needle exchange program is defined as legally authorized when it has been specifically authorized by statute, regulation, or case law in the state.
Other laws affecting the operation of needle exchange programs involve drug-free zones and prostitution-free zones. These are city ordinances that prohibit persons convicted of a drug-related crime or prostitution from entering certain areas during certain times of the day. They tend to be areas with high drug trafficking, which are precisely the areas that needle exchange programs target in order to reach the most people. The ordinances impede injection drug users from obtaining sterile injection equipment from needle exchange programs operating in these areas and limit the operating capabilities of the programs (see Chapter 5 for an in-depth discussion of legal issues).
The administrative structures and funding sources of the programs are closely related to whether they are legally authorized. The programs that are not legally authorized tend to be operated by activists and funded by private donations and, occasionally, by foundation grants; however, this is not universal. Although legally authorized needle exchange programs are more likely than those not legally authorized to receive local or state government funding, not all of them do. Activists continue to administer many of the currently operating programs. The remainder are administered by either government agencies or community-based organizations, some with and some without local or state government involvement.
Program Operations
Sites
As described by Lurie et al. (1993a), needle exchange sites can be broadly classified into two categories: fixed and mobile. Fixed sites operate at a consistent and predictable location at the same time each week. Mobile sites include deliveries and persons roving either on foot or in a vehicle. Roving sites usually cover a specific geographic area and often follow a consistent route, but they do not stay at any one location for very long. Fixed sites have the advantage of being relatively predictable, whereas mobile sites can cover a greater geographic area and can more readily accommodate changes in local conditions.
In their systematic survey, Lurie et al. (1993a) identified seven types of exchange sites: four types of fixed sites (stationary van, storefront, street, and health facility) and three types of mobile sites (walk route, deliveries, and roving van).
A stationary van site consists of a van parked at a predictable location at a predictable time. One van may visit multiple fixed sites in a single outing. A van exchange is a way for needle exchange programs to provide the benefits of both a fixed and a mobile site. It can provide shelter for staff, some privacy for clients, and consistent service while covering a large geographic area.
A storefront program provides shelter for participants and staff. It can also provide privacy for injection drug users, especially if the storefront houses other programs and services not directly related to injection drug use. Storefront sites can also house telephones, facsimile machines, computers, desks, and chairs, which can make it easier for needle exchange program staff to provide services to injection drug users and facilitate referrals to other services. Storefront needle exchange programs may involve significant rental costs.
A street site is located on a sidewalk with either a card table to hold the items to be distributed or persons holding bags containing the items. Participants can blend in with the foot traffic as they approach the table to pick up condoms, peruse the available literature, or ask a question about AIDS. Injection drug users are not the only persons to approach the needle exchange program table and thus their privacy can be protected.
Housing a needle exchange program in a health facility can also provide shelter and privacy. Such sites also facilitate referral of injection drug users to other services, especially if these services are also provided within the health facility. However, health facilities can present geographic and psychological barriers to injection drug users. The needle exchange program may be located in a public health building in an area of low injection drug use activity. Many injection drug users may not feel comfortable entering institutional buildings, particularly ones in close proximity to other government buildings (e.g., police headquarters).
Needle exchange program services provided on walk routes generally target areas known to have high concentrations of injection drug users. A roving site of this sort generally follows a relatively consistent route, although it can change in response to immediate neighborhood conditions (e.g., increased police presence) or to incorporate additional populations of injection drug users.
Deliveries bring needle exchange program services directly to injection drug users. In many ways, deliveries are the most private type of site, in that they meet the injection drug user at a location of his or her choice. However, deliveries require access to transportation, are labor intensive, and may present many logistical challenges.
Roving vans allow a needle exchange program to cover a greater geographic area. A roving site keeps staff members relatively inconspicuous to neighbors, local businesspeople, and police officers.
In summary, needle exchange programs are operated from a variety of locations, some mobile, some fixed, and some with both fixed and mobile sites. Sites range from health department pharmacies to mobile vans to tables set up on city sidewalks.
Staffing
The plurality of the programs are staffed by a combination of paid employees and volunteers. As with funding, the staffing mix is related to whether exchanges are legally authorized and the administering body of the programs. Programs administered by activists are typically staffed by volunteers. Only legally authorized programs that are administered by either local or state government agencies or community-based organizations are predominantly operated by paid staff.
Policies
According to Lurie et al. (1993a), needle exchange policies restrict the exchange of syringes, or limit eligibility to use the needle exchange programs, or both. These policies alleviate potential staff-participant conflicts by clearly delineating procedural rules that must be followed. In general, the policies seek to establish an optimal balance among the following criteria: remaining convenient to the participant, maintaining frequent contact with the participant, and alleviating community concerns over the potential of needle exchange programs to facilitate drug use or increase the numbers of needles discarded in public places.
At a one-for-one exchange, a new syringe is given out for each used syringe turned in. A needle exchange program that adheres to a strict one-for-one exchange rule cannot increase the total number of discarded syringes if it provides no starter needles. Starter needles are those distributed to participants at their first visits, even if they do not have any needles to exchange. This rule removes a potential barrier to entering a needle exchange program. The Lurie et al. (1993a) report classified needle exchange programs that give out starter needles but thereafter have a strict one-for-one exchange rule as having both rules.
An exchange maximum is a limit placed on the number of needles that can be exchanged per visit or per unit time. Some needle exchange programs impose an exchange maximum solely because of limited supplies. An argument sometimes offered in favor of an exchange maximum is that it brings participants back to the needle exchange program more frequently, thus increasing staff-participant contact and providing more opportunities to refer injection drug users to drug treatment and other public health services. However, an exchange maximum might lead to an increase in the reuse of
dirty syringes and may be inconvenient for injection drug users who have to travel long distances to use the needle exchange program.
A minimum age requirement for exchanging is generally imposed in response to the concern that the needle exchange program may encourage young people to start injecting illicit drugs. A countervailing concern is that young injection drug users may have difficulties gaining access to sterile needles.
Requiring a participant to show needle ''track" marks (visibly scarred veins due to repeated injection) in order to use the needle exchange program is intended to limit clientele to active users. This rule is, in part, a response to the concern that needle exchange programs may encourage noninjection drug users to start injecting drugs, but it can also be used to prevent noninjection drug users from selling syringes for a profit. However, some programs note that participants who do not have tracks may be neither new injectors nor profiteers, but may instead be surrogates exchanging syringes for friends or family members. Some programs actively encourage surrogate exchangers, believing that they act as important sources of sterile needles and, perhaps, of education for otherwise hidden injection drug user populations.
Hours of Operation
Of the surveyed programs (Lurie et al., 1993a), the number of operating hours per week, not including deliveries, typically ranged from 8 to 168, with a median of 10. Hours of operation was also found to be related to whether programs are legally authorized: legally authorized exchanges are open more hours per week.
On-Site Services Offered
The range of services offered by needle exchange programs includes
-
education,
-
HIV testing and counseling,
-
tuberculosis screening,
-
screening for sexually transmitted diseases,
-
primary medical care,
-
substance abuse treatment, and
-
case management.
Services to educate and inform injection drug users regarding injection practices, safety steps, nonsharing behavior, and other risk reduction methods are an important part of a needle exchange program. The ability and
capacity to provide such a service are somewhat dependent on site of operation (roving van versus a storefront, for example) and types and number of staff. A critical component of education involves sexual behaviors and practices and the use of condoms. The majority of the programs surveyed by Lurie et al. (1993a) reported that they distribute educational materials most often in the form of health pamphlets. The need for and value of targeted education and behavior modification efforts directed at injection drug users at risk of HIV transmission have been clearly demonstrated in programs that do not include needle exchange (Wiebel et al., 1993).
Additional services include HIV testing and counseling, tuberculosis screening, screening and treatment of sexually transmitted diseases, primary medical care and case management, drug treatment, assertiveness training focused on negotiation skills, and other health and social services. The ability to provide these additional services on site is related to space and available personnel, which are in turn related to funding and whether programs are legally authorized. At the time of the Lurie et al. (1993a) report, the only two programs to offer all of these above services were The Works (Boulder, Colorado) and the Tacoma-Pierce County Health Department (Tacoma, Washington). Both of these programs are legally authorized, are government administered and funded, have paid staff, and are open more than 10 hours per week.
For the most part, the needle exchange programs that offer primary medical care and/or substance abuse treatment have paid staff. HIV testing and counseling, however, are provided by both paid and volunteer employees.
Although a minority of programs have the capacity to provide all of the services mentioned above, the majority do refer participants to services. For instance, of all U.S. programs surveyed by Lurie et al. (1993a, 1993b), all but one program provided referrals to drug abuse treatment.
Items Distributed
In addition to sterile needles, the programs distribute other paraphernalia and supplies. These typically include cotton, sterile cookers, sterile water bottles, and alcohol wipes. With a few exceptions, all programs also distribute bleach, condoms, and health pamphlets. Because of concerns about the efficacy of bleach in inactivating HIV in injection equipment, some of the providers are reluctant to provide it (see Chapter 6).
Characteristics of Program Participants
The variation in the demographic characteristics of needle exchange program participants is one of the most notable features of the programs
overall. Data from published accounts of data collection efforts at 10 U.S. programs are presented in Table 3.1. The data are notable in several respects.
Needle exchange programs attract males predominantly: the proportion of participants who are female ranges from 15 to 34 percent. However, as noted in Chapters 1 and 2, female injection drug users in general tend to show higher HIV seroincidence than their male counterparts, suggesting that the programs may not be targeting high-risk women. The sex profile of needle exchange programs is similar to that of drug abuse treatment programs and other populations used to sample injection drug users.
Needle exchange programs vary considerably in their racial/ethnic distributions. As Table 3.1 shows, the proportion of program participants who are African American ranges from 8 to 100 percent; Asian participants range from 0 to 12 percent; Hispanic participants range from 0 to 53 percent; white participants range from 0 to 70 percent; and others (primarily Native Americans) range from 0 to 28 percent. This variation across programs to some extent reflects regional differences.
The mean age at entry into needle exchange programs tends to be similar across programs, ranging from age 33 to 41.
The mean duration of injection drug use ranges from 7 to 20 years. Combined with the information available on age, these data suggest that needle exchange programs do not tend to attract recent initiates into injection drug use. A more recent report from San Francisco noted that less than 1 percent of needle exchange program participants were under age 18 (Watters et al., 1994). These data could be considered as indirect evidence that needle exchange does not encourage the initiation of injection drug use. However, considered in conjunction with the data presented in Chapter 2 on the prevalence of injection drug use by age, the overall data suggest that these programs may not be attracting the young injectors who, according to available estimates, represent a sizable portion of the injection drug user population. This is especially disconcerting in light of the findings reported in several studies that show that the risk of HIV infection is higher among younger and more recent initiates.
Before firm conclusion are drawn, it is important to note that the data presented here mostly reflect samples of program participants who agreed to be interviewed. The published descriptions of sampling procedures are incomplete, so the extent to which potential biases could have operated cannot be assessed.
When needle exchange participants were compared with nonparticipants, the participants were found to be more likely to be male and older, and less likely to be African American and to have been in drug treatment (Hagan et al., 1991; Joseph, 1989; Watters and Case, 1989).
TABLE 3.1 Demographic Characteristics of Needle Exchange Participants
Original Data Sources:
The Chicago Recovery Alliance
1992 Individuals Concerned with Addiction, Recovery, and HIV Disease. Risk Reduction Outreach with Syringe Exchange: Guidelines and Operating Procedures. June 24.
Clark, G., D. Garcia, J. Guydish, and P. Case
1991 Street-Based Survey of Needle Exchange Clients. Abstract WC 3295 in Final Program and Abstracts of the VII International Conference on AIDS, Florence, Italy.
Demographics Among 700 Drug Injectors. Unpublished material. Department of Health, State of Hawaii
1992 Needle Exchange Evaluation Report. January 1.
Guilfoile, A., D. Lenaway, and V. Harris
1991 Boulder County Health Department Needle Exchange Program. Unpublished material. October 15.
Hagan, H., D.C. Des Jarlais, S.R. Friedman, D. Purchase, and T.R. Reid
1992 Multiple Outcome Measures of the Impact of the Tacoma Syringe Exchange. Abstract 4283 in Final Program and Abstracts of the VIII International Conference on AIDS, Amsterdam, Netherlands.
Harris, N.V., M.J. Fields, D.C. Gordon, et al.
1991 HIV and Related Risk Behaviors Among Inmates and Needle Exchange and Drug Treatment Clients. Abstract WC 3362 in Final Program and Abstracts of the VII International Conference on AIDS, Florence, Italy.
Joseph, S.C.
1989 A bridge to treatment: The needle exchange pilot program in New York City. AIDS Education and Prevention 1:340-345.
O'Keefe, E., E. Kaplan, and K. Khoshnood
1991 City of New Haven. Preliminary Report: City of New Haven Needle Exchange Program. July 31.
Oliver, K., S.R. Friedman, H. Maynard, and D.C. Des Jarlais
1991 Behavioral Impact of the Portland Syringe Exchange Program: Some Preliminary Results. Presentation in Third National AIDS Demonstration Research Conference.
SOURCE: Adapted from The Public Health Impact of Needle Exchange Programs in the United States and Abroad, Volume 1 (Lurie et al., 1993a:274).
Cost and Cost-Effectiveness
The cost of operating a needle exchange program was estimated in the University of California/Centers for Disease Control and Prevention report (Lurie et al., 1993a). Briefly, their report noted wide variation in annual cost across the 18 programs sampled, ranging from $18,628 in the Tacoma Pharmacy Exchange to $393,951 in the Lower East Side, New York City, Exchange. The median annual cost of operating a needle exchange was $168,650. The budgets reflect actual plus donated resources for personnel, consultants, equipment, supplies, transportation, travel, and space rental. The proportion of the budget specifically allocated to syringes ranged from 2 percent in Boston and New Haven to 47 percent in the Tacoma Pharmacy Exchange (median = 7 percent), with the proportion per program reflecting the volume of needles exchanged. The largest proportion of the budget was for personnel, ranging from 27 percent in Berkeley's NEED exchange to 79 to 80 percent in the Boulder, New Haven, and Portland exchange programs (median = 66 percent).
In an attempt to measure the productivity of needle exchange programs, the University of California team of investigators used the annual budget, the number of participant contacts, the number of syringes distributed, and the hours of operation for each program to calculate the cost per participant contact, the cost per syringe distributed, and the cost per hour open. The median cost per participant contact across the seven programs with available data was $17; the median cost per syringe distributed was $1.35; and the median cost per hour of program operation was $145. The median number of syringes distributed per hour was 205.
The variability across sites was attributed to differences in exchange rates of needles: higher costs per needle, contact, and hours of operation were related to activities that do not contribute directly to needle exchange. For example, Boston's ACT-UP project spent considerable time attempting to engage a scattered clientele under continual police scrutiny and had exchanged 9 syringes per hour, considerably below the median of 205.
In an attempt to measure the cost-effectiveness of programs, the University of California research team estimated absolute impact (number of HIV infections averted) and associated cost-effectiveness (program cost divided by number of HIV infections averted) on the basis of three different models. The three models included a simplified circulation model formula (Kaplan, 1993), a behavior change model (Kahn et al., 1992), and a combined circulation and behavior change model (Lurie et al., 1993a:496-499). The results summarized here are based on a hypothetical needle exchange program with specific characteristics (e.g., high volume of needle exchange, limited counseling and referrals to other services) and HIV risk determinants (e.g., high prevalence and incidence, drug and sexual risk behaviors).
Although the three models differ in many ways, the primary distinguishing factors are as follows. The simplified circulation model focuses on obtaining estimates of averted HIV infections among program participants, based on a 1-year time frame, attributable to transmission from sharing contaminated needles. The behavior change model estimates averted infections among all injection drug users in the community as well as their sexual partners and offspring over a 5-year time interval, attributable to transmissions from both sharing and sexual behavior. The combined circulation and behavior change model incorporates characteristics of both models.
As depicted in Table 3.2, all models estimated that the hypothetical needle exchange program had a substantial impact on averted HIV infections and reported significantly lower costs per HIV infection averted than the $119,000 estimated lifetime HIV medical costs associated with treating a person infected with HIV (Hellinger, 1993). One noticeable disparity is the substantially different estimates in the number of infections averted over 5 years reported by the behavior change model compared with the combined model. This disparity is due mainly to the fact, as with the circulation model, that the combined model limits its estimates to infections averted among program participants only (participants are assumed to share only with each other).
These are obviously crude estimates of the cost-effectiveness of needle exchange programs and are of limited value in assisting health policy makers
TABLE 3.2 Comparison of Three Model Estimates of Needle Exchange Impact and Cost-Effectiveness
|
|
Simplified Circulation Model |
Behavior Change Model |
Combined Model |
|
Absolute HIV infection averted |
50 |
46 |
53 |
|
Additional absolute HIV infection averteda |
0 |
113 |
11 |
|
Cost per HIV infection avertedb |
$12,000 |
$3,773 |
$9,375 |
|
a Estimated drug-related (i.e., direct sharing) HIV infections averted in program participants during 1 year of program participation. b Estimated drug-related and sexually related HIV infections averted among program clients, their drug and sexual partners, and their offspring over 5 years. That is, 1 year of program operation and 4 years of delayed effects (averted infections during the 1 year of program operation among program participants due to sharing are not included). SOURCE: Adapted from The Public Health Impact of Needle Exchange Programs in the United States and Abroad, Volume 1 (Lurie et al., 1993a:499). |
|||
set priorities for allocating resources across various health promotion and disease prevention programs. Nonetheless, these estimates demonstrate that multiple models lead to the conclusion that needle exchanges reduce the number of new HIV infections at a cost per infection averted far below the $119,000 lifetime cost of treating an HIV-infected person.
In order for cost-effectiveness analysis to be a useful tool in guiding the setting of priorities for the use of scarce financial resource allocations for AIDS prevention, certain critical information is needed:
-
measures of program effectiveness on meaningful health outcome measures,
-
estimates of costs, as well as discounting and variable cost rates, and
-
a set of independent AIDS prevention programs from which to choose, each having an expected degree of effectiveness and an associated cost.
Once these elements are known, policy makers will be able to maximize program effectiveness by allocating financial resources to programs according to their respective cost-effectiveness ratio. Numerous uncertainties surround these elements, such as the parameter estimates that should be included in the models, the tenability of the underlying assumptions used to derive those estimates, the necessary level of precision, and whether collateral program effects should be included (e.g., on crime, sexually transmitted diseases, drug use). Although these issues must be carefully addressed in cost-effectiveness analyses of AIDS prevention programs, they are beyond the scope of this report. For a more detailed treatment of benefit-cost analysis of AIDS prevention programs, the interested reader is referred to a previous National Research Council report (Turner et al., 1989:471-499).
Moreover, Kaplan (1995, in press) in a recent paper provides various models for estimating the cost and benefits of HIV prevention programs and uses data from the New Haven needle exchange to illustrate how such models can assist policy makers in making resource allocation decisions. In particular, the proposed models do provide some guidance for addressing pragmatic issues, such as how a given needle exchange program, in a specific epidemiologic environment, can optimize its cost-effectiveness ratio (i.e., cost per infection averted), within a budget constraint. The author also depicts how these ratios are a function of critical program parameters (e.g., number of program participants, number of needles exchanged per participant, HIV incidence in population being served).
Organization Characteristics
Although brief descriptions of needle exchange programs along selected dimensions are available, few studies thus far have examined the organizational characteristics of needle exchange programs themselves as potential determinants of the behavior of the injection drug users participating in the exchange. Since needle exchanges are service delivery organizations, it is reasonable to expect that the particular mode of organizing the services may in itself be a very important determinant of the HIV and AIDS risk behavior of the participants in the exchange.
In this section we review existing research on the organizational characteristics of needle exchange programs and outline possible directions for future research. Before reviewing the few available comparative studies of the organization of needle exchange programs, we briefly examine five case studies in which organizational issues were found to be critical to the effectiveness—or ineffectiveness—of needle exchange programs in reducing HIV risk behavior.
Three Simple Case Studies
Dundee-Wishart, Scotland Many of the earliest needle exchange programs implemented in the United Kingdom were operated by preexisting drug service agencies that, in some cases, were lacking both the resources and the appropriate training for this challenging new task. Perhaps the clearest example of these problems was in the experience of the needle exchange program that operated from the premises of the Wishart Drug Problems Centre in Dundee-Wishart, Scotland, in summer 1988 (Stimson et al., 1988). At that time, the Dundee-Wishart facility was not only understaffed in relation to an already full caseload, but also encumbered with an ill-suited and overly rigid set of rules for a fledgling needle exchange. In addition, it was being operated by the staff of an abstinence-oriented treatment program who clearly felt overwhelmed by the sudden influx of injection drug users seeking only to exchange used needles for new ones and who plainly did not desire abstinence treatment. Indeed, injection drug users in the area came to perceive the primary aim of the exchange as recruiting them into the treatment program. Hence, very few participated in the exchange, causing it to close within 6 weeks.
New York City The first legally authorized needle exchange program in New York City opened in 1988 as a single-site operation, although it had originally been designed and proposed as a pilot study that aimed to compare injection risk behavior and the rates of entry into treatment among injection drug users seen at four different sites (Anderson, 1991; Joseph and
Des Jarlais, 1989). Two of these planned locations were to offer needle exchange services, and two were not. Subjects were to be recruited from the waiting lists of drug treatment programs in order to better compare rates of actual entry into treatment and to place a prearranged limit on length of needle exchange participation (which was to end as soon as a treatment slot became available for the subject.)
When the scheduled opening of the needle exchange program was announced, however, the ensuing controversy led to a political compromise that no needle exchange would be located "within 1,000 feet of a school." This, however, precluded all four of the originally planned sites. Indeed, the only site that both 9a) met the school distance criterion and (b) was under the control of the City Health Department was in the Health Department's own Lower Manhattan headquarters, which happened to be in an area that was not only inconvenient for injection drug users, but also conspicuously near police headquarters and the Manhattan criminal courts. Moreover, the registration procedures themselves lasted several hours and included tuberculosis screening, administration of a detailed questionnaire on risk behavior, and issuance of a photo ID card. A strict one-for-one exchange rule was in effect, whereby only one syringe at a time could be exchanged.
In a little over a year of operation, 317 injection drug users participated in the program. Many were placed into treatment programs quickly, and too few participated long enough to enable researchers to make pre-and post-program comparisons of risk behavior. Plans were being made to expand the exchange operations into areas more convenient to drug users but, at the end of 1989, a decision was made by a new mayor to close the exchange.
Washington, D.C. The Washington, D.C., program had many similarities to the first legally authorized New York City exchange program. First, the program design itself was actually the product of a delicate compromise with political opponents of needle exchange on the District of Columbia City Council. In addition, as in New York: (1) the program was obliged to operate out of a single site, a drug abuse treatment program, (2) participant eligibility was restricted to those already on a waiting list for drug abuse treatment, and (3) the cumbersome entry procedure required hours of participant and staff time (Vlahov et al., 1994). Also, as in Dundee-Wishart, some of the treatment program staff at the designated site were adamantly opposed to any distribution of needles in a treatment setting. Moreover, the Washington, D.C., needle exchange program was permitted to operate for only 60 days, during which time it was able to enroll a total of 31 injection drug users in the first month and 2 in the second month from the District's estimated 16,000 injection drug users. It was then closed, in keeping with the original agreement, while public health officials assessed the experience.
The Vlahov et al. (1994) evaluation study also noted that the program was supplying both syringes and needles in a size incompatible with those used by injection drug users in the local community.
Discussion None of these three needle exchange programs would be considered user-friendly (a concept discussed below). Some of the unfriendliness in program operation stemmed from concessions to political opponents of needle exchange and some from research design requirements. Other aspects of the unfriendliness, such as tuberculosis screening, were required in a sincere belief that they were in the best interests of the participants. None of these three programs appears to have had any impact on HIV transmission in the local area, and it is not even likely that any of them had any meaningful impact on the HIV/AIDS risk behavior of the small numbers of people who participated.
Nonetheless, these three programs may provide valuable learning experiences for future exchanges. The New York City exchange in particular was the first to demonstrate that a needle exchange program could serve as a bridge to treatment (New York City Department of Health, 1989). The many similarities between the first legally authorized New York City needle exchange program (1988) and the Washington, D.C., program 4 years later (August 1992), however, raise the question of how the program planners can learn about important organizational issues from past experiences.
Two Complex Case Studies
The primary lesson to be drawn from the above three cases histories, of course, is that a needle exchange program needs to be user-friendly in order to attract participants and to have a public-health-level impact on HIV and AIDS risk behavior. This somewhat straightforward organizational lesson, however, does not illustrate any of the possible complexities involved in the organizational characteristics of a needle exchange program and its possible effectiveness. The following two case histories show some of the possible complexities.
Manchester In 1988, Klee conducted an interview study of HIV/AIDS risk behavior among injection drug users in Manchester, United Kingdom, and published results somewhat later (Klee et al., 1991). She found that some of the local injection drug users who had participated in the local needle exchange program had become known among the drug user community as sources of injection equipment. These injection drug users themselves were often socially pressured by other injection drug users to pass on injection equipment, and they actually did pass on their used injection equipment more frequently than did a comparison group of injection drug users who
were not using the exchange. In the U.S. General Accounting Office (1993) review of needle exchange studies, this study was classified as showing an association between participation in a needle exchange program and increased sharing of drug injection equipment. (Indeed, this was the only study so classified.)
Klee, however, disputes this classification of her findings. She notes that the data from this study were collected at a time when local needle exchange programs were just being implemented and before they had engaged a large number of participants. Klee conducted a later study, after needle exchange programs in Manchester had reached a larger number of participants, in which she did not find that users of the exchange were more likely to pass on used injection equipment (Klee, personal communication, February 1994). Thus, the apparent relationship between participation in the program and the sharing of used injection equipment had changed from the early to the later period of the lengthy program implementation process.
Tagging Syringes in New York City Several underground needle exchanges operated in New York City between the time that the first legally authorized needle exchange program was closed in 1989 and the legal authorization of community-based organization (CBO) exchanges, which began in 1992. Three of the underground exchanges tagged the syringes they exchanged (Paone et al., 1994b); that is, marking pens or paint were used to draw a circle around the barrel of each syringe. The tagged syringes served both as a reminder to injection drug users to inject safely and as an advertisement for the needle exchanges. Rough counts of the tagged syringes that were returned also provided a means for estimating the percentages of syringes that were returned to the exchanges out of the total number of tagged syringes that had been distributed. (The exchanges also accepted syringes that drug injectors had acquired by other means.)
The legal authorization of the underground exchanges was accompanied by increased funding and regulation. The newly authorized exchange programs had to operate within regulations issued by the New York State Department of Health. The original intention of the Health Department's regulations was to require continued tagging of syringes issued through the now legally authorized exchanges, and this stipulation was included in the first versions of the regulations. The tagging, it was reasoned, would both provide information about the percentage of issued syringes that were returned to the exchanges and help law enforcement personnel to distinguish between possession of syringes obtained from legally authorized sources and those obtained from other sources of distribution.
Moreover, with the start of legalization and increased funding, there was also a wide expansion of needle exchange programs. Two of the underground exchanges, which had been serving approximately 1,000 injection
drug users per year before being legally authorized, increased to serve nearly 8,000 injection drug users within the first 12 months afterward (Paone et al., 1993, 1994a, 1994b). This expansion led to considerable logistical problems in continuing to tag syringes. The volunteer staff, who did the actual tagging, complained that they were now spending all of their time tagging syringes and no longer had time to interact with the injection drug users coming to the exchanges. This personal interaction was viewed as a major benefit to the injection drug users and a primary opportunity for the volunteers to obtain a palpable sense of accomplishment.
Staff of the two largest legally authorized exchange programs in New York City had begun refusing to continue tagging when a negotiated compromise was reached between the State Health Department and the programs. An evaluation team offered to conduct a special tagging alternative study to determine the syringe return rates and thereby no longer require the programs to tag the syringes they were issuing. In this instance, then, an exchange procedure that had earlier appeared to be highly functional for small underground exchanges clearly became dysfunctional when the exchanges underwent rapid expansion.
Discussion Both the Manchester and the New York City tagging studies suggest the need to examine the organizational characteristics of needle exchange programs within the context of their entire developmental history, as well as in the larger context of drug injection and HIV and AIDS risk behavior in the surrounding community. These two case histories illustrate the possibility that a conclusion drawn from data collected at one point in time may be totally inappropriate for other points in time.
Comparisons Across Programs
It would of course be useful to compare organizational characteristics across programs. To date only two such comparative studies have been conducted (Table 3.3). Stimson and colleagues conducted an evaluation of the national system of needle exchange programs that was implemented in the United Kingdom from 1987 to 1988 (Stimson et al., 1988); it was the first to elaborate on the concept of user-friendliness in syringe exchange. Although they did not conduct formal quantitative analyses, they were able to show that user-friendliness was associated with both attracting and retaining injection drug users in needle exchange programs. (It should be noted that the participation of injection drug users in the U.K. needle exchanges was within a context of legal authorization that permitted both over-the-counter sales of needles and syringes and personal possession of equipment to inject illicit drugs.) As indicated in the first three case histories
TABLE 3.3 Organizational Characteristics of Needle Exchange Programs
|
Comparative Study |
Characteristics |
Components |
|
Stimson et al. (1988) |
User-friendliness |
—Nonjudgmental staff attitude; —Convenient location; —Convenient hours of operation; —Willingness to exchange large numbers of syringes at one time |
|
Lurie et al. (1993a) |
Legal status |
—Legal; —Illegal—tolerated; —Illegal—underground |
|
|
Administrative body |
—Activist run; —Community-based organization run; —Community-based organization with government support; —Government run |
|
|
Funding source |
—Private donations; —Foundation grants; —Community-based organization; —City, county, and/or state government |
|
|
Sites |
—Fixed sites; —Stationary van; —Streetfront; —Street; —Health facility; —Mobile sites; —Walk route; —Deliveries; —Roving van |
|
|
Staff |
—Paid; —Volunteers; —Both paid and volunteers |
|
|
On-site services |
—Educational material; —HIV testing and counseling; —Primary medical care; —Tuberculosis screening; —Sexually transmitted diseases screening; —Drug treatment; —Referrals to above services; —Referrals to social services |
|
|
On-site items provided |
—Needles/syringes; —Bleach; —Alcohol wipes; —Cotton; —Cookers; —Water; —Condoms; —Lubricant |
presented above, the concept of user-friendliness appears to be fundamental to at least the initial effectiveness of needle exchange programs.
The University of California, San Francisco, collected organizational data on 33 U.S. and 4 Canadian needle exchange programs (Lurie et al., 1993a). As the table shows, this study arrayed the programs according to a number of different organizational characteristics (e.g., status of legal authorization, funding sources, staffing) and was able to show some meaningful associations among them. Unfortunately, this study was not able to associate any of the organizational characteristics with any measures of effectiveness in behavior change or HIV transmission.
Although valuable in depicting the diversity in the type of needle exchange programs, there are certain limitations of this study that should be noted. First, the cost data used in the descriptions and analyses did not separate the costs of exchanging needles from the costs of other services. For this reason, these cost data should be used with extreme caution. Second, given the rapidly changing circumstances of needle exchange programs in the United States, the information provided by this study, as with any cross-sectional survey, represents a snapshot of a complex picture in a state of flux. As of October 1994, there were at least 76 needle exchange programs in the United States—a 130 percent increase over the number of exchanges itemized in the 1993 University of California, San Francisco, report (North American Syringe Exchange Network, 1994). In addition, many of the needle exchange programs included in the study have since undergone substantial changes. Data for the New York City exchanges, for example, do not take account of the legal authorization and expansion noted in the tagging case study presented above.
BLEACH DISTRIBUTION PROGRAMS
Unlike the situation for needle exchange programs, to date there has been no comprehensive survey of the total number of programs in the United States to distribute bleach or other disinfectants for the purpose of cleaning needles and syringes between uses. An extensive review of the literature has resulted in multiple studies that questioned injecting drug users about needle-cleaning practices, but these reports typically do not include descriptions of the characteristics of the bleach distribution programs per se (Longshore et al., 1993; Neaigus et al., 1990).
The most systematic information about bleach distribution programs in the United States comes from the National AIDS Demonstration Research (NADR) program, which was initiated in 1987 by NIDA.
The purpose of NADR was to assess the efficacy of different strategies of AIDS prevention with out-of-treatment injection drug users and their sexual partners. All these strategies—except those initiated in New Jersey—were
to make use of the newly developed bleach distribution technology. All were to rely on the skills of ex-addict staff trained to conduct case finding and engagement and to provide AIDS prevention materials and counseling. NADR came to involve a total of 41 projects in nearly 50 cities nationwide. Over the life of the program, data were collected on more than 43,000 injection drug users and nearly 10,000 sexual partners, although many more tens of thousands of participants received outreach and intervention services (AIDS prevention services) but were not referred for study (Brown and Beschner, 1993).
Characteristics of Program Participants
The demographic characteristics of NADR program participants vary considerably across participating program sites. Data from 13,475 participants in the 28 sites that contributed demographic data for the final data analysis indicate that the average age of participants is 35. On average, participants had been injecting drugs for 14 years (ranging from 10 to 19 years across sites). NADR recruited predominantly men: 74 percent of the sample at intake were men. The proportion of women by site ranges from 12 to 37 percent.
NADR participants also vary considerably by site in their racial/ethnic distributions. The proportion of African American participants ranges from 9 to 95 percent; Hispanic participants range from 0 to 81 percent; and white participants range from 3 to 65 percent. As is the case with needle exchange programs, this variation across sites to some extent reflects regional differences. Overall the sample was 51 percent African American, 25 percent Latino, and 22 percent white.
Other noteworthy observations are that 81 percent of NADR participants had spent time in jail or prison, 41 percent had never been in a drug treatment program, and participants reported an average of 12 different sex partners in the past 6 months. However, it is again important to note that the demographic data presented here mostly reflect the demographics of participants who provided data for the final NADR analysis and, as a consequence, there may be a bias in the representation of the original NADR sites. Moreover, descriptions of sampling procedures (outreach workers recruited out-of-treatment injection drug users) make it unlikely that the studied sample is statistically representative of the out-of-treatment injection drug user population in this country. Nonetheless, this effort is the most extensive description of the demographic characteristics of out-of-treatment drug users to date. The similarity in demographic patterns, between NADR participants and the needle exchange participants reported earlier in this chapter, is notable.
Outreach Strategies
The outreach strategies used in bleach distribution programs are characterized by their emphasis either on (a) the development of individual behavioral skills to limit risk taking or (b) the modification of community norms to support changed behavior. Those concerned with the former are focused on counseling and behavioral skills training, and those concerned with the latter are focused on peer intervention and social contagion.
For programs that emphasize counseling and behavioral skills training, outreach mainly involves referring injection drug users to a community site at which they typically receive structured counseling and skills-building sessions (Rhodes, 1993). For programs that emphasize the peer intervention and social contagion approach, outreach workers, chosen for their knowledge of and status in the injection drug-using community, play a key role in the work of HIV and AIDS prevention by inserting themselves into the social network of injection drug users (Wiebel et al., 1993).
Outreach at the sites in the NADR project varied in terms of techniques used, from written instructions about the use of bleach to disinfect injection equipment, to demonstration of the technique in person, reverse demonstration (by the drug user to measure comprehension and competence), and videotapes. Information summarized from eight NADR sites is presented in Table 3.4. Two cities—San Francisco and Denver—reported ancillary techniques to promote the use of bleach to disinfect needles. In San Francisco, an individual was costumed as an 8-foot-tall superhero named ''Bleachman," with a plastic bottle for a head and a Clorox logo on his torso. Bleachman appeared on city streets to distribute small bottles of bleach (Broadhead, 1991). In Denver, outdoor murals were painted in the city to encourage risk reduction and the bleaching of needles and syringes.
There are limitations on the NADR data, which are discussed in Chapter 6. Although the NADR program provides information to describe and evaluate bleach distribution programs in the United States, it does not describe all existing bleach distribution programs. Also, the NADR programs used outreach workers to establish trust and rapport with injection drug users outside treatment for drug abuse; bleach distribution is thus intertwined with the intervention of community health outreach workers. Other bleach distribution occurs in the setting of needle exchange programs. The panel found no instance in the literature of self-service bleach bottles with printed instructions as the sole intervention.
One further limitation: reports from San Francisco describe the instructions provided by the NADR projects for the use of bleach to disinfect needles. Undiluted bleach was packaged in 1-ounce vials, to be flushed through a used syringe twice before injecting and following each bleach flushing with a flushing of water. The extent to which instructions varied
TABLE 3.4 Percentage of Clients Receiving Intervention Components
|
|
|
Site |
|
|
|
|
|
|
|
|
Intervention Components |
Total (n = 3,886) |
1 |
2 |
3 |
4 |
5 |
6 |
7 |
8 |
|
Give bleach |
82 |
33 |
100 |
100 |
100 |
100 |
35 |
100 |
100 |
|
Demonstrate bleach use |
61 |
33 |
100 |
100 |
51 |
44 |
34 |
37 |
100 |
|
Practice condom use |
61 |
33 |
100 |
100 |
49 |
44 |
34 |
37 |
100 |
|
Give condom |
91 |
100 |
100 |
100 |
100 |
100 |
34 |
100 |
100 |
|
Demonstrate condom use |
61 |
33 |
100 |
100 |
51 |
44 |
34 |
37 |
100 |
|
Practice condom use |
61 |
33 |
100 |
100 |
49 |
44 |
34 |
37 |
100 |
|
Video/slide presentation |
67 |
44 |
100 |
100 |
73 |
100 |
34 |
37 |
54 |
|
One-on-one session |
72 |
100 |
— |
100 |
100 |
— |
100 |
100 |
46 |
|
Group session (not specific) |
10 |
43 |
— |
— |
— |
— |
34 |
— |
— |
|
Group session: problem solving |
26 |
30 |
— |
41 |
— |
46 |
45 |
— |
54 |
|
Group session: risk avoidance |
29 |
33 |
— |
41 |
— |
100 |
23 |
— |
54 |
|
Group session: negotiation |
27 |
— |
100 |
36 |
— |
46 |
— |
— |
54 |
|
Role-playing: problem solving |
24 |
— |
38 |
35 |
24 |
— |
45 |
— |
54 |
|
Role-playing: risk avoidance |
22 |
— |
43 |
— |
48 |
46 |
— |
— |
54 |
|
Role-playing: negotiation |
23 |
— |
35 |
35 |
24 |
46 |
— |
— |
54 |
|
Didactic session: risk avoidance |
73 |
— |
100 |
37 |
100 |
100 |
100 |
100 |
54 |
|
Booklet/brochure |
50 |
— |
100 |
100 |
100 |
— |
— |
100 |
100 |
|
Referral (HIV or non-HIV) |
49 |
— |
100 |
100 |
100 |
— |
— |
37 |
54 |
|
SOURCE: Outreach/Risk Reduction Strategies for Changing HIV-Related Risk Behaviors Among Injection Drug Users: The National AIDS Demonstration Research (NADR) Project (National Institute on Drug Abuse, 1994:58). |
|||||||||
from this at other sites before 1993 has not been summarized systematically.
CONCLUSIONS
-
By 1994, 76 needle exchange programs had been established in the United States, an increase from 33 at the time of the University of California report in 1993. More are planned.
-
Needle exchange programs vary considerably in terms of whether they are legally authorized, their sources of funding, site characteristics, on-site services offered, and other items distributed.
-
Needle exchange programs vary in terms of the racial/ethnic distributions of the participants served. The majority served are men. The distribution of participants by age and duration of drug use shows that a wide cross section of drug injectors are attracted to needle exchange.
-
The cost of needle exchange programs varies widely, depending on their organizational aspects. The median annual cost for operation of a needle exchange program has been estimated at $168,650.
-
Needle exchange programs vary in their ability to attract clients. Factors that promote recruitment of participants include:
-
An "ideal" needle exchange and bleach distribution site. This should be (1) in an area frequented by injection drug users, (2) unlikely to be noticed by passersby, (3) unlikely to engender opposition from local residents or businesses, (4) able to provide privacy for injection drug users and protection from the weather, (5) in a predictable location, (6) accessible to diverse communities of injection drug users, and (7) able to be relocated easily, if necessary. Some of these characteristics may be mutually incompatible.
-
Programs that provide for an exchange of injection equipment, not a unilateral distribution. This greatly increases the likelihood that the programs will reduce the number of discarded syringes found in parks and alleys and other public sites. It also helps to ensure that existing injection drug users, not new users, are the ones using the program. Conducting the programs as an exchange also increases the possibilities for evaluating program effectiveness through tracking exchanged syringes and conducting surveys of exchange participants to ensure safe practices (Lurie et al., 1993a).
-
User-friendly policies and procedures and staff that are nonjudgmental and flexible.
-
-
Bleach distribution and needle exchange programs are not and should not be viewed as discrete entities. They typically include a variety of prevention services (including outreach and education) that are intertwined.
REFERENCES
Anderson, W. 1991 The New York needle trial: The politics of public health in the age of AIDS. American Journal of Public Health 81(11):1506-1517.
Broadhead, R.S. 1991 Social constructions of bleach in combating AIDS among injection drug users. Journal of Drug Issues 21:713-737.
Brown, B.S., and G.M. Beschner, eds. 1993 Handbook on Risk of AIDS: Injection Drug Users and Sexual Partners . Westport, CT: Greenwood Press.
Hagan, H., D. Des Jarlais, D. Purchase, T. Reid, and S.R. Friedman 1991 The Tacoma syringe exchange. Journal of Addictive Diseases 10:81-88.
Hellinger, F.J. 1993 The lifetime cost of treating a person with HIV. Journal of the American Medical Association 270(4):474-478.
Jones, T.S. 1994 Update on Upcoming Research Activities Pertaining to Needle Exchange and Bleach Distribution. Presentation at the September meeting of the Panel on Needle Exchange and Bleach Distribution Programs, Woods Hole, MA.
Joseph, S.C. 1989 A bridge to treatment: The needle exchange pilot program in New York City. AIDS Education and Prevention 1:340-345.
Joseph, S.C., and D.C. Des Jarlais 1989 Needle and syringe exchange as a method of AIDS epidemic control. AIDS Updates 2(5):1-8.
Kahn, J.G., A.E. Washington, J.A. Sowstack, M. Berlin, and K. Phillips 1992 Updated Estimates of the Impact and Cost of HIV Prevention in Injection Drug Users. San Francisco, CA: Institute for Health Policy Studies, University of California.
Kaplan, E.H. 1993 Back-of-the-Envelope Estimates of Needle Exchange Effectiveness. Unpublished material. in press Economic analysis of needle exchange. AIDS. 9:1113-1119, 1995.
Klee, H., J. Faugier, C. Hayes, and J. Morris 1991 The sharing of injecting equipment among drug users attending prescribing clinics and those using needle-exchanges. British Journal of Addiction 86:217-223.
Longshore, D., M.D. Anglin, K. Annon, and S. Hsiehs 1993 Trends in self-reported HIV risk behavior: Injection drug users in Los Angeles. Journal of Acquired Immune Deficiency Syndromes 6:82-90.
Lurie, P., A.L. Reingold, B. Bowser, D. Chen, J. Foley, J. Guydish, J.G. Kahn, S. Land, and J. Sorensen 1993a The Public Health Impact of Needle Exchange Programs in the United States and Abroad, Volume 1. San Francisco, CA: University of California.
Lurie, P., A.L. Reingold, B. Bowser, D. Chen, J. Foley, J. Guydish, J.G. Kahn, S. Land, and J. Sorensen 1993b The Public Health Impact of Needle Exchange Programs in the United States and Abroad: Volume 2. San Francisco, CA: University of California, San Francisco.
National Institute on Drug Abuse 1994 Outreach/Risk Reduction Strategies for Changing HIV-Related Risk Behaviors Among Injection Drug Users: The National AIDS Demonstration Research (NADR) Project. NIH Publication No. 94-3726. Bethesda, MD: National Institutes of Health.
Neaigus, A., M. Sufian, S.R. Friedman, D.S. Goldsmith, B. Stepherson, P. Mota, J. Pascal, and D.C. Des Jarlais 1990 Effects of outreach intervention on AIDS risk reduction among injection drug users. AIDS Education and Prevention 2:253-271.
New York City Department of Health 1989 The Pilot Needle Exchange Study in New York City: A Bridge to Treatment. A Report on the First Ten Months of Operation. New York: New York City Department of Health.
North American Syringe Exchange Network 1994 Surveys, surveys, surveys. Newsworks 3(December 16):1.
Paone, D., D.C. Des Jarlais, S. Caloir, and P.B. Friedmann 1993 AIDS risk reduction behaviors among participants of syringe-exchange programs in New York City. Presented at the Ninth International Conference on AIDS, Berlin, June 6-11 [abstract PO-C24-3188].
Paone, D., D.C. Des Jarlais, S. Caloir, P.B. Friedmann, I. Ness, and S.R. Friedman 1994a New York City syringe exchange: An Overview. Pp. 47-63 in Proceedings, Workshop on Needle Exchange and Bleach Distribution Programs. Washington, DC: National Academy Press.
Paone, D., S. Caloir, J. Clark, E. Gonzalez, B. Jose, and D.C. Des Jarlais 1994b Tagging Alternative Study (TAS): A Substudy of the New York City Syringe Exchange Evaluation. Presented at the North American Needle Exchange Network Conference, Santa Cruz, CA, March 3-5.
Rhodes, F. 1993 The Behavioral Counseling Model for Injection Drug Users. Rockville, MD: National Institute on Drug Abuse.
Stimson, G.V., L.J. Aldritt, K.A. Dolan, M.S. Donoghoe, and R.A. Lart 1988 Injecting Equipment Exchange Schemes. Final Report. London: Monitoring Research Group, Goldsmith's College.
Turner, C.F., H.G. Miller, and L.E. Moses, eds. 1989 AIDS: Sexual Behavior and Intravenous Drug Use. Washington, DC: National Academy Press.
U.S. General Accounting Office 1993 Needle Exchange Programs: Research Suggests Promise as an AIDS Prevention Strategy. Washington, DC: U.S. Government Printing Office.
Valleroy, L.A., B. Weinstein, T.S. Jones, S.L. Groseclose, R.T. Rolfs, and W.J. Kassler in press Impact of increased legal access to needles and syringes on community pharmacies' needle and syringe sales—Connecticut, 1992-1993. Journal of Acquired Immune Deficiency Syndromes.
Vlahov, D., C. Ryan, L. Solomon, S. Cohn, M.R. Holt, and M.N. Akhter 1994 A pilot syringe exchange program in Washington, D.C. American Journal of Public Health 84(2):303-304.
Watters, J.K. 1994 Trends in risk behavior and HIV seroprevalence in heterosexual injection drug users in San Francisco, 1986-1992. Journal of Acquired Immune Deficiency Syndromes 7:1276-1281.
Watters, J.K., and P. Case 1989 Preliminary Study of an Illicit Needle Exchange Program in San Francisco. Presentation in American Public Health Association Annual Meeting, Chicago.
Watters, J.K., M. Downing, P. Casse, J. Lorvick, T.Y. Cheng, and B. Fergusson 1990 AIDS prevention for injection drug users in the community: Street-based education and risk behavior. American Journal of Community Psychology 18:587-596.
Wiebel, W., A. Jimenez, W. Johnson, L. Ouellet, T. Lampinen, J. Murray, B. Jovanovic, and M.U. O'Brien 1993 Positive Effect on HIV Seroconversion on Street-Outreach Intervention with IDU in Chicago: 1988-1992. Paper presented at the Ninth International Conference on AIDS, June 6-11.