3
Computer-Based Patient Record Technologies
User needs, both of individuals and of cohesive communities, are paramount in the design and development of computer-based patient record systems. Designers and vendors of CPR systems must understand such needs, as well as how the systems will be used and what demands users will place on the systems. The discussion of user requirements in Chapter 2 sets the stage for explaining in this chapter the attributes of technologies required to create CPR systems in the 1990s.
This chapter has three main goals: (1) to highlight technologies relevant to CPR systems, (2) to convey what is possible with existing technologies, and (3) to emphasize what will be required to build state-of-the-art CPR systems in the 1990s. The chapter also provides some insight into the current state of existing clinical information systems that possess features crucial to the development of state-of-the-art CPR systems. Finally, it discusses the technological barriers that still must be overcome before CPR systems can become well established.
Technological Building Blocks for CPR Systems
No clinical information system in 1990 is sufficiently comprehensive to serve as a complete model for future CPR systems. That is, no operational clinical information system in 1990 can manage the entire patient care record with all its inherent complexities. A few existing clinical information systems are beginning to approach the CPR system capabilities envisioned by the committee. None of these is yet complete, but some might appropriately be called today's CPR systems. Therefore, the committee sometimes
refers to current CPR systems, meaning those clinical information systems that are beginning to approximate the ideal CPR system envisioned by the committee for the future (see Chapter 2).
The committee selected and reviewed nine technologies that are significant for CPR systems. They include (1) databases and database management systems, (2) workstations, (3) data acquisition and retrieval, (4) text processing, (5) image processing and storage, (6) data-exchange and vocabulary standards, (7) system communications and network infrastructure, (8) system reliability and security, and (9) linkages to secondary databases. This section describes the key attributes of these crucial technologies.
Databases and Database Management Systems
It is important to distinguish between the clinical data—that is, the computer-based patient record, or CPR—and the system that captures and processes those data—that is, the CPR system. CPR functions relate to the collection of data, such as patients' medical problems, diagnoses, treatments, and other important patient information, including follow-up data and quality measures. CPR system functions relate to storage capacity, response time, reliability, security, and other similar attributes, but the system relies on the collection of clinical data, the core CPR, to support virtually all of its activities.
Databases
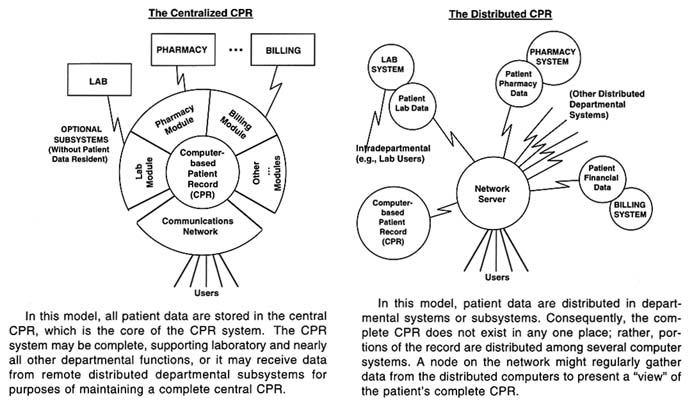
The most desirable database model for CPR systems involves either (1) a distributed database design—that is, a system with physically distributed computers and databases but with logical central control of the entire record; or (2) a centrally integrated physical database design—that is, a centrally located, complete CPR within a single computer-stored database (see Figure 3-1);1 or (3) some hybrid or mix of these two approaches. In any case, the key requirements are central control and organizational integrity of the entire record for each individual patient. Central control permits authorized persons using a terminal located anywhere in the information system to access the entire integrated patient record or any of its parts, regardless of the locations of any other departmental subsystems where the various data items may have originated. (Access is allowed only on the basis of parameters specific to authorized users.)
Although the feasibility of the distributed database design (see the righthand panel of Figure 3-1) has recently gained support from the development of networking technologies, most current clinical information systems that might qualify as CPR systems use a centralized design (the left-hand panel of Figure 3-1). The CPR systems of today cannot as yet acquire and retrieve all patient care data directly. Instead, they rely on data transmitted to the CPR system through interfaces with departmental subsystems; the data are subsequently entered into the CPR using applications programmed on the CPR system. One major factor that differentiates current CPR systems is the extent to which they use local area networks, or LANs, to access departmental subsystems and stand-alone databases containing portions of the CPR.
Today's CPR systems place great emphasis on providing at least a ''view" of a complete, centralized patient record (Hammond et al., 1990). If the patient's clinical data are physically distributed among several computers in a network, a comprehensive view of the record of a given patient can be achieved only by retrieving and assembling the pertinent data from each computer on the network where patient data reside. Although this scenario has a number of advocates and some advantages, it also has several severe problems (Margulies et al., 1989; Hammond et al., 1990).
A careful analysis of the two contrasting models shown in Figure 3-1 may be helpful in understanding the main problems. In the distributed system, the patient record is physically distributed among several computer systems but at the same time is functionally integrated. This means that a variety of distributed patient care applications will generate and use patient care data in the distributed CPR. It also means that individual records may require multiple data structures (or data files), which tends to lengthen data retrieval times. Another problem with a distributed system is that data synchrony—that is, the correct sequencing of a patient's time-stamped data that are entered into the system at the same time but from different sources—must be guaranteed at both the applications and the database management system (DBMS) levels. Perhaps the most significant problem with the distributed database approach, however, is the increased potential it carries for circumventing CPR confidentiality mechanisms. Because portions of the patient's record are distributed among several different computers, ensuring confidentiality becomes more difficult. Every computer has its own vulnerabilities, and each one that is added to a network represents another node that must be protected and another potential entry point for unauthorized access (National Research Council, 1991).
Database Management Systems
A major technological issue is the complexity of the data that will eventually reside in the CPR. The CPR of the future will consist of many
different kinds of data, including text, graphics, images, numerical data, sound, and full-motion video. To design a functionally integrated database system that accommodates such diversity is a sizable technical challenge.
The CPR is so complex that no single database management system is capable of optimally storing and retrieving the full range of patient data (Hammond et al., 1990). As a result, CPR system developers have used a variety of complementary DBMSs to address these complexities. This multiple-DBMS approach is most common when the CPR system uses the distributed database scenario; in that case, each subsystem often uses a different DBMS. Because the CPR is distributed across many connected subsystems, each subsystem will probably use a DBMS that is particularly suited to the kind of data most frequently stored in that subsystem. The collection of appropriate databases that results offers advantages of efficiency in manipulating and storing the CPR complex data. Some CPR system developers have even created their own proprietary database management systems, tailored to the CPR's particular complexities.
The selection or creation of the DBMS that will support the CPR is among the first and most crucial steps in developing a CPR system. Several database management systems or architectures have evolved in recent years. Four important ones developed by commercial vendors are hierarchical, relational, text-oriented, and object-oriented databases. Each of these architectures has its own particular strengths and weaknesses. Architects of current CPR systems (both commercial and private) have mainly used hierarchical, relational, or text-oriented models. Viable object-oriented database management systems have been introduced only recently and are not yet in widespread use.
Workstations
Three general classes of workstations seem likely to prevail in future CPR systems. First, "smart" terminals with data entry pointer/selector devices (e.g., mouse, touch-screen, light-pen, or voice) will be used for data input and retrieval; they may also support "windowing" and medium-resolution imaging. These terminals will use a graphical user interface (GUI) and communicate with file servers, compute servers, and rule servers2 in a local area network
Second, hand-held terminals or computers, or other similar semiportable devices, will facilitate either manual or voice entry of data into the CPR. These relatively portable devices will be used at the bedside by practitioners. Third, fully configured workstations (e.g., complete with a mouse, accelerated processors, GUI, and large storage capacities) may well become one of the more powerful tools ever devised for health care professionals and may ultimately come to be considered indispensable.
Data Acquisition and Data Retrieval
Data Acquisition
Data acquisition for the CPR remains an exceptionally challenging topic within the field of medical informatics.3 Ideally, data in the CPR should be entered at its source (e.g., the site of patient care) by the record's primary user; they should be entered only once, and they should be accessible to all portions of the CPR system that use that particular data item. Data entry at the source by members of the health care team remains a sensitive issue. Yet the most commonly used alternative, data entry by an intermediary (e.g., a clerk or a transcriptionist) has several disadvantages: (1) it often introduces errors because the person who has direct information about the patient is not the person entering the data; (2) it delays the timely availability and transmittal of potentially critical information; (3) it makes immediate feedback to health care professionals (in the form of alerts or alarms generated by detectable errors or conflicting orders) impossible; and (4) it interferes with the decision maker's ability to use linked databases and other on-line knowledge bases designed to assist health care professionals in the clinical decision making process. Two keys to the success of next-generation CPR systems are ease of use and proper incentives for data entry at the data source (Young, 1987; Safran et al., 1989).
Data Retrieval
The organization of data displays that can quickly convey crucial information needed in a particular setting (e.g., in the intensive care unit) or by a certain user (e.g., a surgeon) is also a challenge (Stead and Hammond, 1987; Silva et al., 1990). Because much of the patient record can be presented as text, tables, or graphs (e.g., trends in laboratory values), most CPR systems today display data on low-cost monitors capable of high-resolution
graphics. Although these displays cannot deliver, for example, high-definition radiological images, they can produce hard-copy printouts of display screens, graphs and tables, and signals such as those needed for an electrocardiogram (ECG). A complete on-line CPR reduces the necessity for printing multipart copies of these printouts.
A short response time has proven to be an important factor in successful CPR systems (Bleich and Slack, 1989). This requirement refers primarily to retrieving data, but it is equally important for inputting data. In future CPR systems, the displays and reporting formats of CPR data are likely to be configured or modified by users. Thus, the same data may be presented differently, or in different combinations, to different health care professionals, each of whom has differing "views" or "windows" into the same CPR (see Chapter 2). Customizing data in this way is a difficult capability to implement but will produce a system that is much more attractive to end users.
Text Processing
To establish a diagnosis, physicians and other health care professionals use patient information in a textual form—for example, the patient history and the results of the physical examination. With a CPR system, professionals search for and retrieve such text from database systems using query languages, which in the past were often idiosyncratic to a particular system. In recent years, gradual progress has been made in standardizing such languages.
Natural language understanding, or the ability of the computer system to selectively extract meaning from textual data, has been slower to evolve because of its inherently greater complexity (Obermeier, 1989). Compounding this complexity is the slow development of efforts to encourage a more uniform vocabulary in health care. Automated speech-recognition systems may help to add uniformity and consistency to vocabularies for the CPR by encouraging the speaker to use clinically relevant, yet consistent, terminology.
In the 1990s, text-processing systems for translating the narrative found in discharge summaries and other parts of the CPR are likely to be used to generate codes for billing. As text-processing systems improve in accuracy and performance, they may be used to extract significant phrases or attributes from the CPR that could assist the user in searching related databases. For example, attributes derived from the CPR might be matched against the terms and concepts in the National Library of Medicine's (NLM) Unified Medical Language System (UMLS; Humphreys and Lindberg, 1989). Improved text-processing systems would make it possible to use data from the CPR, in conjunction with the UMLS, to lead practitioners
to an array of related information sources, including medical literature and other pertinent knowledge bases (Lindberg and Humphreys, 1990).
Image Processing and Storage
Medical imaging today includes diagnostic images or pictures obtained by film scanners, computed radiography (CR), magnetic resonance (MR), computed tomography (CT), ultrasound, and nuclear medicine sources. The medical images generated by these technologies and found in today's patient records are typically two-dimensional, still pictures. The increasing digitization of data, however, will expand the capabilities of such technologies. For example, digital data permit varying intensity resolution (number of measurable levels of gray), which allows the computer to display images with medium to high contrast. In the near future, digital images will be routinely available in many radiology departments.
New technological developments are expected to lead to a new generation of picture archiving and communications systems (PACSs), which will be installed in many radiology departments by the mid-1990s. PACSs permit the electronic storage, transmission, and display of medical images throughout a medical facility and offer many advantages not available with conventional film. For example, two or more physicians can simultaneously examine exact duplicates of an image at their respective and sometimes distant locations, discuss the interpretation of the image, and together formulate plans for optimal patient management. Imaging systems in the near future will eliminate concerns about the current status or location of an image, such as "missing" or "in transit."
Imaging is routinely used not only radiologists but also by ophthalmologists, dermatologists, pathologists, dentists, and other specialists. Indeed, images have become an essential part of the complete patient record. Yet although the record is incomplete without images, the typical paper record environment stores images separately from the chart itself. CPR systems of the future, when appropriately linked to PACSs, will allow health care professionals to view images at the computer workstation in a timely fashion.
Data-Exchange and Vocabulary Standards
In today's health care environment, health care professionals, managers, policymakers, regulators, and educators need increasing amounts of accurate health care data in machine-readable form to support intelligent decision making. All such data must be collected, aggregated (when they come from diverse sources), and transmitted among disparate systems. The
aggregation and dissemination of existing and future health care data mandate the development of standards, both to exchange health care data and to encourage more consistent medical vocabulary, especially in those portions of the CPR containing natural language text. Developing such standards requires a coordinated approach.
Efforts to develop data-exchange standards for components of the CPR have only recently gained significant momentum in the United States. Because so much is at stake in this sizable medical market—a market that remains largely untapped from the vendors' point of view—standards take on an even more prominent role in fostering the evolution of the required technologies. Currently, there are several related efforts to standardize and facilitate the exchange of health data. HL 7 and Medix, as well as standards from the American Society for Testing and Materials (ASTM), the American College of Radiologists/National Electrical Manufacturers Association (ACR/NEMA), and others are representative of the current movement to formulate data-exchange standards.4
Several promising vocabulary developments are relevant to CPR systems. These include a planned new edition of the Systematized Nomenclature of Medicine (SNOMED); the Read Clinical Classification in Great Britain; the ASTM Standard Guide for Nosologic Standards and Guides for Construction of New Biomedical Nomenclature, which is now completed and ready for distribution (ASTM, 1989); and the NLM's UMLS project. The overall goal of UMLS is to help users retrieve relevant biomedical
information from multiple machine-readable sources, even though different vocabularies and classifications may have been used in these sources. One of the new knowledge sources being developed to support this goal is a metathesaurus, which will link related terms and concepts from a variety of existing biomedical vocabularies and classifications.
System Communications and Network Infrastructure
Caring for patients naturally requires many health care workers to interact frequently. As discussed in Chapter 2, health care is information-intensive, which implies a strong emphasis on the communication and transmission of information to many people in diverse places. The patient information conveyed is complex and appears in all possible modalities, including text, images, voices and sounds, signals, and video. This board array of information needs to be available in such diverse locations as the bedside, the hospital department, professional offices, emergency settings including mobile units, and the home.
Technologies to support communications of all kinds are evolving at an unprecedented rate. With the advent of fiber optics, in particular, transmitting the diversity of information contained in the CPR will soon be feasible at high-speeds and low-costs.
Of great significance is the evolving Integrated Services Digital Network (ISDN), an all-digital network capable of high-speed transmission of all modalities (data, voice, graphics, or video) over public telephone networks. In the 1990s, the transition from analog to fully digital switches is expected to occur throughout much of the United States. This transition to an all-digital network, when complete, will have wide-ranging implications for improving health care because it will open a new era for communication of all types of information, including that contained in the CPR.
System Reliability and Security
Chapter 2 presented brief explanations of system reliability, system security, and data security. System security is achieved through appropriate system design and the use of physical security measures directed toward protection of the computing environment and equipment. For example, techniques for security include software and hardware features, physical measures such as locks and badges, identification numbers or codes, passwords, and an informed, security-conscious staff (National Research Council, 1991).
A data integrity control policy has at least four essential components: (1) security measures, (2) procedural controls, (3) assigned responsibility, and (4) audit trails. It is especially important to allow access to the CPR system
only to those with a need to know and to certify their identity before permitting access. In addition, the CPR system must be capable of providing different levels of data confidentiality as required for its various users. Audits of all legitimate users of CPR systems must be conducted regularly to remind and assure patients and staff that strict confidentiality is being maintained and measured. Such periodic audits should help deter any attempts by staff to breach confidentiality.
Members of the health care team who record patient data in the record are responsible for such entries, but in a hospital or clinic, physicians typically still have primary responsibility for ensuring the record's accuracy. As documentation of health care shifts from paper to computer-based records, practitioners will maintain their responsibility to document patient care, but the data will reside within CPR systems. Legal, professional, and accrediting standards must be revised to specify appropriate new roles and responsibilities associated with the shift from the paper chart to the CPR.
In the aggregate, current CPR systems seem to use limited measures for ensuring patient confidentiality. Most CPR systems do not approach the levels of security or confidentiality that airlines or banks, for example, maintain to protect their less sensitive information. Future CPR systems must implement stricter measures to protect confidentiality (National Research Council, 1991).
Linkages to Secondary Databases
Many clinically relevant registries and databases have evolved in recent years and are of particular interest to health care professionals as they attempt to improve the quality of patient care. Increasingly, these collections of secondary data will be extracted from primary data in CPRs in such a way as to protect the confidentiality and identity of individual patients. Thus, patient records will collect all data on all problems for a single patient; clinical research databases will collect all data on one problem for many patients. For policymakers, the secondary collection of relevant (nonconfidential) clinical information on large populations of patients will support their development of policy strategies and general assessments of quality and outcomes of care. Hundreds of databases are available or are now evolving; some of these resources should be linked with the CPR to provide clinical decision support when needed.
Some current CPR systems already offer linkages to knowledge and research databases. Most CPR systems, however, lack this capacity, owing primarily to the complexity and cost of developing such linkages. Health care professionals are beginning to appreciate the support offered by timely access to a diverse array of external information sources in providing care.
NLM's GRATEFUL MED,5 for example, gives physicians in their offices ready access to NLM's MEDLINE. For these purposes, it will be important to develop easy-to-use linkages in real time so that feedback to the clinician occurs as part of the decision making process.
Experience with CPR Systems
Health care facilities have been using computers since the 1960s, but that use has primarily focused on business and accounting functions of health care (e.g., patient billing). Many have called these business systems for health care environments either hospital information systems (HISs) or medical information systems (MISs); they have been largely devoid of patient care data. The systems of most interest to this report are clinical information systems, also sometimes known as patient care management systems. Clinical information systems consist of components related to clinical or direct care of patients (Blum, 1986), regardless of the setting (ambulatory, inpatient, institution, or home).
In 1959, two pioneers in health care described a hypothetical health computing system that might be able to address actual clinical problems (Ledley and Lusted, 1960). Almost simultaneously, several other experts began pioneering efforts using computing technologies in clinical settings. By the mid-1960s, Spencer and Vallbona (1965:121) had concluded that at least six areas of medical practice would be affected: "(1) medical diagnosis, (2) hospital medical records, (3) laboratory analysis and functional testing, (4) patient monitoring, (5) hospital communications, and (6) utilization of hospital services and facilities." In 1965, Summerfield and Empey reported that at least 73 hospital and clinical information system projects and 28 projects for storage and retrieval of medical documents and other clinically relevant information were under way. Blum (1984:6) noted that progress through the 1960s was difficult and slow and that "[s]uccesses in information processing during this phase were limited. The Lockheed experience of the late 1960s resulted in the Technicon MIS and a more sobering appraisal of the complexity of clinical information systems."
These early experiences showed that clinical computing offered several distinct challenges that would require significant time to address effectively. A study of clinical systems between 1955 and 1973 by Giebink and
Hurst (1975:xii) revealed that many of the systems planned or developed during the 1960s were "extinct—blunt testimony to the difficulties of implementing computer-based information systems for health care delivery. … Medical computer applications which meet operational criteria are rare except for routine business applications. … Other than in developmental projects, computerized medical records are abstracts of more complete records maintained in hard copy form."
With the advent of less costly mini- and microcomputers, clinical information system development flourished during the 1970s and 1980s. The advances made during these years focused primarily on departmental systems (known today as subsystems) for such areas as the clinical laboratory, radiology, electrocardiology, and the pharmacy. One reason for this flurry of development was that departmental systems were easier and less risky to develop than comprehensive systems covering patient care management.
The 1970s and 1980s also saw the development of systems for clinical decision support (Warner et al., 1972; Shortliffe, 1987). To perform their sophisticated functions, these complex systems require that at least a subset of the CPR be available as input—that is, in machine-readable form. Once the use of CPRs becomes more widespread and more and more patient data are captured, these systems should become increasingly valuable to clinicians.
Virtually all of the current clinical information systems that might qualify as CPR systems have evolved from a strong academic medical center's teaching hospital or clinic records. Examples of this phenomenon include the COSTAR6 (Computer Stored Ambulatory Record; Barnett, 1984) system, which is used by several institutions, including the Harvard Community Health Plan; a system used by the Latter-Day Saints Hospital in Salt Lake City, Utah, known as Health Evaluation through Logical Processing (HELP),7 which was developed by faculty at the University of Utah (Warner et al., 1972; Pryor et al., 1983, 1984); the TMR (The Medical Record) system at Duke University Medical Center (Stead and Hammond, 1988); and the THERESA system at Grady Memorial Hospital, the primary teaching hospital for Emory University's medical school (Walker, 1989).
With few exceptions, software developed in an academic setting is not generally considered to be particularly robust or of an "industrial or commercial grade"; consequently, some experts have been skeptical about the functionality of these and other clinical information systems. Nevertheless, many of these systems have proved their usefulness and viability in supporting the actual delivery of health care in real-world settings. Attributes
of the systems discussed above are presented in subsequent sections of this chapter.
These systems all illustrate the time required to establish operational clinical systems: all of them began development at least a decade ago, and some have been under development for more than two decades. Now, however, their increasingly sophisticated capabilities are being recognized in the marketplace. A variety of commercial organizations, having seen or demonstrated the viability of these systems in one or more hospital or clinic settings, have subsequently negotiated further developmental and marketing rights to these clinical information systems.
An Overview of CPR Systems
A distinguishing feature of the clinical information systems that can rightly be called computer-based patient record systems is their underlying database management system. Generally, for performance reasons, CPR systems have developed their own DBMS and have avoided the use of commercially available products. As a result, they use an approach by which a data dictionary can be expanded to accommodate new data elements to be captured in the CPR. Such flexibility sets these systems apart for two reasons: (1) their databases are not fixed in terms of size and content, and (2) no significant reprogramming is needed to meet the continually changing demands placed on the CPR system by technology innovations and system enhancements.
Much of the effort to automate clinical functions has focused on a single department such as the laboratory or pharmacy; these are not examples of CPR systems. The more noteworthy examples of currently operating CPR systems go well beyond the routine collection, storage, and communication of data provided by one or more departmental systems. Yet, to reiterate, no single health care information system operational in 1990 captures and manipulates the entire CPR. Of those that might qualify as CPR systems, not one is comprehensive enough to serve as a model for the future computer-based systems that will be designed to manage the entire patient care record.
The few clinical information systems that qualify as ''today's CPR systems" share several common traits. First, they maintain a large data dictionary to define the contents of their internal CPRs. Second, all patient data recorded in the CPR are tagged with the time and date of the transaction, thus making the CPR a continuous chronological history of the patient's medical care. Third, the systems retrieve and report data in the CPR in a flexible manner. Finally, the systems offer a research tool for using the CPR data.
Although much remains to be done to design and produce complete, robust CPR systems, significant progress has been made in establishing
state-of-the-art components of CPR systems. Several systems developed in recent years have been designed and tailored to serve the special needs of nearly all members of the health care team in a variety of health care settings.
This section discusses a few key attributes of selected operational clinical systems that effectively utilize some portion of a computer-based patient record. There has been no attempt to provide an exhaustive presentation here of all the clinical systems developed to date. Rather, the discussion below focuses on systems that embody one or more special features crucial to the successful implementation of the complete CPR, especially within certain practice settings. These include (1) physician offices and group practice settings, (2) health maintenance organizations, (3) single hospitals or medical centers, and (4) large multihospital systems. By a large margin, the majority of patient care is provided in the office or group practice setting; as a result, systems that specifically address the needs of practitioners and patients in this environment will probably encounter the most substantial challenges and have the greatest impact. Therefore, although only two systems in this category are discussed below (many others have been developed or are currently under development), it should be understood that this category comprises perhaps the most important settings for CPR systems in terms of the potential for improved care. In addition to the discussion of clinical systems, the section also describes a few international developments of special interest and selected emerging developments.
Physician Offices and Group Practice Settings
The Medical Record
For more than 20 years, the Duke University Medical Center8 has been developing a comprehensive medical information system known as The Medical Record (TMR). The TMR system was first conceived as a tool for clinicians in outpatient settings; it was subsequently expanded to address the needs of clinicians in inpatient settings (Hammond and Stead, 1986). From the outset of the project, the CPR was considered the centerpiece of the TMR system (Stead and Hammond, 1988). The system can store and retrieve and data contained in a traditional paper record in an ambulatory or inpatient setting, with the exception of images such as X-rays. In an inpatient
setting, however, the TMR system can provide a link to such imaging systems.
The TMR system can support a complete list of diagnoses and procedures, as well as subjective and physical findings, laboratory data, and therapeutic interventions. The system also allows multiple "views" of data. For example, patient data may be viewed from any of several perspectives—from a problem, time, task, or encounter orientation. 9 The look and feel of a particular TMR system are controlled by a user-defined, object-oriented data dictionary that separates the parameters, or variables, along which data are being collected from the system features that manipulate those variables. Even users with no programming expertise thus can tailor the TMR to their own needs.
Health Maintenance Organizations
Computer-Stored Ambulatory Record Systems
In 1968 the Laboratory of Computer Science at the Massachusetts General Hospital implemented the COSTAR (Computer Stored Ambulatory Record) system, which became one of the first systems capable of producing a computer-based patient record.10 COSTAR is a medical information management and record system designed as a set of modules for which individual sites can choose the portions of the system they wish to install. COSTAR supports patient registration, scheduling of patient visits, storage and retrieval of clinical information, and billing and accounts receivable (Barnett, 1984).
The first implementation of COSTAR was at the Harvard Community Health Plan (HCHP), which adopted and began testing the COSTAR systems in 1969 (Grossman et al., 1973). By 1987, HCHP had installed 10 minicomputers to support clinical computing in their 9 care facilities, which together serve an active membership of more than 225,000 people. The HCHP COSTAR system now contains individual records for nearly 550,000 people generated over the past 20 years.
The HCHP system supports patient record inquiry, a tumor registry, clinical reminders, and storage and retrieval of demographic data. It also provides clinical reporting, automated appointment scheduling, and diverse management reports and facilitates urgent care. Much of the patient record can be printed on demand by clinicians, and by 1986 more than 4.1 million pages were being printed annually (Harvard Community Health Plan, n.d.). In that same year 1.3 million patient encounters were documented, more than 2.5 million lines of text were dictated and transcribed into the system, and the results of 650,000 laboratory tests were entered.
Two characteristics of COSTAR have made it possible to use the system in a variety of sites. One is modular design: a site need only install a partial set of modules—for example, scheduling and medical record modules but not the accounting module. The other is its substantial, extensible data dictionary. The core of the data dictionary is a controlled vocabulary of clinical terms, which includes the ability to associate modifier terms with the primary name for a clinical concept. These modifiers make the COSTAR controlled vocabulary quite sophisticated: it can provide synonyms and generate specialized terms by combining the modifier with the primary name for a concept. It can also associate specific brand names with the generic names for drugs.
The COSTAR system is comprehensive enough to include all major categories of clinical data, including laboratory results and findings from diagnostic procedures. All data recorded in the patient record are associated with controlled vocabulary terms (and any selected modifiers). The benefits of this approach are seen in clinical care (e.g., for any patient, the system can generate a summary document that contains the most recent information on every COSTAR code in the record); quality assurance (e.g., the system can analyze each patient record to identify patients with certain risk factors for whom an influenza vaccination is indicated); and clinical investigation (e.g., the system can examine the patterns of prescription ordering for hypertension by physicians with different levels of training).
In 1975 the Laboratory of Computer Science rewrote the system and made it available in the public domain. Currently, there is an active COSTAR users' group that provides information about the system, conducts tutorials, and distributes COSTAR manuals and software on diskettes for a nominal fee. A number of commercial vendors also market COSTAR. Current
system users of COSTAR include physician offices, public health departments, ambulatory care clinics, a veterinary teaching clinic, and a consortium of sites for multiple sclerosis research. COSTAR has been implemented in several hundred sites in the United States, Canada, Mexico, Argentina, and Europe.
Single Hospitals or Medical Centers
Theresa System
Atlanta's Grady Memorial Hospital, the primary clinical teaching facility of the Emory University School of Medicine, contracted with Medical Systems Development for the development of its CPR system in 1981. As of 1990 there were 18 million documents on-line. Plans call for completing the system in late 1991, illustrating again the complexity and length of time required to create an operational clinical system.
THERESA,11 as Grady's system is called, is based on a custom-made, object-oriented database management system that was specially designed to address the problems associated with the patient record noted earlier in this report (see Chapter 2). It supports problem-oriented, task-oriented, event-oriented, and time-oriented "views" of the patient record. It also permits users to employ English-like queries to access the complete database. When a user requests complex decision support, the system searches the database, typically requiring from 30 seconds to 3 minutes to respond to the user's request. Since the first modules became operational at Grady in 1983, data on more than 220,000 patient encounters (an encounter is defined as a single hospital stay or clinic visit) have been collected; the patient record includes data on the individual's medical history, physical examination, and diagnosis, as well as orders, results, progress notes, and physician and nursing notes. The system maintains a lifelong record and never deletes clinical data.
Physicians and other members of the health care team enter these data directly using "windowing" terminals (a feature that permits users to look at different data or views of the same data on the terminal screen at the same time). The majority of data are entered using a mouse (i.e., point-and-click technology; Walker, 1989). A recent analysis of one month's medical admissions revealed that practitioners entered complete data on 98 percent of
their patients. THERESA is therefore one of the few clinical systems that have successfully engaged clinicians in direct patient data entry. Grady also appears to have successfully solved the problem of ensuring system access. Although it has not installed expensive special fault-tolerant computer systems,12 for the last seven years a distributed network of standard supermini-computers has provided access to the system 99.95 percent of the time.
Health Evaluation Through Logical Processing
The Intermountain Health Care Corporation's Latter-Day Saints (LDS) Hospital provides another example of the CPR system of today.13 The LDS system, which has been under development for more than 25 years, is known as HELP (Health Evaluation through Logical Processing; Pryor et al., 1983). HELP's primary objective is to provide medical decision support, but it is also a computer-based patient record system. Much of the input to HELP comes directly from medical professionals entering data at terminals, but wherever possible HELP utilizes automated input of the patient's clinical data. Although LDS has conducted experiments using an automated patient history, currently only minimal history and physical examination data are contained in the HELP record. Consequently, at present, HELP maintains both a paper and a computer-based record for each patient.
Developers of HELP have consistently tried to focus on the use of patient data in making decisions about care rather than on merely the storage and communication of these data. To support its decision making goals, HELP contains more than 100,000 rules and statistical processes pertaining to a broad spectrum of health care; it uses these rules and processes to make decisions (including diagnoses)—just as a panel of experts might when presented with similar data. The system makes decisions in both a background monitoring mode and an interactive session with the health care
provider. To maintain constant availability of the system, HELP has been developed to run on special fault-tolerant computers.
Beth Israel and Brigham and Women's Hospital System
The clinical information system at Beth Israel Hospital in Boston, Massachusetts, was developed by the Harvard Medical School's Center for Clinical Computing and has been in continuous use and evolution for more than a decade (Bleich and Slack, 1989).14 The system at Brigham and Women's Hospital in Boston, also from the Clinical Computing Center, was modeled after Beth Israel's system and required approximately four years to develop. More than 800 and more than 1,250 on-line terminals currently operate at Beth Israel and Brigham and Women's hospitals, respectively (Safran et al., 1989). One outstanding attribute of these systems is their extensive use by clinicians and other members of the health care team. At Beth Israel during an average week, for example, 742 departmental and laboratory workers entered or corrected information in computer-based patient records 137,526 times (Bleich et al., 1989). Similarly, during an average week, 532 physicians, 893 nurses, 59 medical students, and 253 health assistants used the computer terminals to examine patient information.
In addition to reporting results, these systems provide other capabilities to clinicians: scheduling, order entry, electronic mail, and bibliographic retrieval through PaperChase. Beth Israel users can also search the growing clinical database. This retrieval capability, called ClinQuery (Safran et al., 1989), is a powerful tool for answering administrative and research questions. Through this system, hospital practitioners can access the Physicians' Desk Reference (PDR) and receive advice from an attached expert system designed to assist practitioners in treating acid-base problems.
Clinical computing systems at these two hospitals are patient centered and integrated rather than networked or interfaced (i.e., they utilize the central database model displayed in Figure 3-1). These systems also store data for hospitalized and ambulatory patients in a common database within each institution. In addition, the systems handle patient billing functions. Indeed, installation of these clinical computing systems has reduced substantially the length of time between provision of service and receipt of payment for the service. (Accounts receivable dropped by 30 days at Beth Israel when the clinical computing system was installed; when that system
also performed the fiscal computing, accounts receivable dropped by 40 days.) The experience of Beth Israel and Brigham and Women's hospitals shows that clinical computer systems can drive nearly all patient billing functions and that they can do so more efficiently than separate machines dedicated only to patient billing. Slack (1989:140) notes that "more than 90% of each patient's charges are now collected as a byproduct of the clinical computing system." This important feature substantiates the dual notions that the CPR is or should be the central feature of all clinical systems and that it is capable of supporting nearly every functional component of the system, including billing.
Lockheed's Early Clinical Information System
One of the earliest demonstrations of a clinical information system came through the development of a system by the Lockheed Corporation between the mid-1960s and 1970s. Technicon, an early clinical system vendor, acquired the system from Lockheed; today, it is owned and marketed by a company called TDS. This system displays two distinct, powerful features crucial to the design of future CPR systems. First, it offers very fast response times (usually less than one second) for nearly all user input; second, it is extremely flexible. For example, it can support the diverse needs of many users at a single site because the system has been tailored to meet the expectations of several simultaneous users.
Large Multihospital Systems
Department of Veterans Affairs
A pioneer and leader in this field, the Department of Veterans Affairs (VA) has been developing its clinical computing system, known as the Decentralized Hospital Computer Program (DHCP), for nearly a decade (Andrews and Beauchamp, 1989). By the late 1980s, the VA had installed DHCP in most of its more than 170 medical centers.15 Outpatient clinics and other care facilities, including nursing homes, operated by the VA gain access to systems through the VA's national network.
The VA's DHCP consists of software grouped into three categories: (1)
system/database management, (2) administrative management, and (3) clinical management. System/database management software consists of software tools that have been constructed by the VA for the support, development, and maintenance of the DHCP. Administrative management software supports all normal hospital administrative tasks, including scheduling. Clinical management software supports clinical information provision in the laboratory, pharmacy, and other departments. It includes a complete surgery module and also partially supports medicine, cardiology, and oncology. The VA is recognized for its use of state-of-the-art technologies in selected radiology departments (Dayhoff et al., 1990).
To advance the clinical aspects of the DHCP, the VA has launched the Clinical Record Project. Clinical record development is under way at several sites and includes modules to support order entry/results reporting, a health summary, a problem index, allergies/adverse reactions, progress notes, crisis warnings, consults information, clinical observations, and clinical measurements. These and other clinical modules represent the VA's commitment to constructing its own state-of-the-art CPR system.
Department of Defense
The Department of Defense (DoD) has contracted for the deployment of a clinical information system at its hundreds of care facilities around the world (General Accounting Office [GAO], 1988, 1990). The system, known as the Composite Health Care System (CHCS), is currently being tested in multiple care facilities in the United States that serve a range of care settings. One example involves health maintenance organization-like settings in Hawaii where hospitals and associated care facilities and clinics are networked. As military personnel visit any of these facilities, the CHCS allows clinicians to gain immediate access to patient care data from previous patient encounters.
The CHCS is an excellent environment and opportunity to design, test, and evaluate certain desirable features of the ideal CPR system, and its potential in this regard may prove vital to accelerating the development of CPR systems generally. For example, the military has established a command structure that permits testing in a closed-loop environment. This means that, within limits, DoD can mandate particular clinician behaviors to evaluate various potentially beneficial methods of providing care and that the CHCS can measure the benefits, if any, that are derived. Currently, the CHCS represents the largest demonstration of actual clinician hands-on data entry to clinical systems: because military facility commanders can require clinicians to input data into the system, alternative input mechanisms may be evaluated. In addition, DoD is testing a prototype professional workstation to facilitate clinicians' interaction with the CHCS.
International Developments
DIOGENE, a system operating in the largest hospital in Geneva, Switzerland, supports a nearly complete CPR and will soon support communication of high-resolution images throughout the hospital complex. The system's unique approach to clinical data capture (Scherrer et al., 1990) may well offer a useful model that could be utilized in other health care organizations.
DIOGENE employs specially trained transcriptionists who can enter text rapidly. A clinician who wants to enter narrative into the patient's computer-based record first identifies or displays the record on a computer terminal near the point of care. He or she then places a call to an available transcriptionist on a nearby telephone and begins dictating. As the dictation proceeds, the typed narrative appears on the terminal display currently being used by the clinician. At the completion of the dictation the clinician suggests any pertinent changes and then approves the text, which becomes a permanent part of the computer-based patient record in DIOGENE.
Even at peak hours, a few specially trained transcriptionists can support all practitioners' dictation. In the future, when clinical workstations can accept direct voice input, transcriptionists will no longer be required.
The Exmouth Project
A large experimental study, known as the Exmouth Project, is being conducted in Exeter, England. The experiment uses patient-carried "smart cards"16 capable of storing critical portions of the complete patient record that are essential in emergency as well as routine care situations. In Exeter, 98 percent of the pharmacies, 70 percent of general practitioners, and all hospitals are able to read and use the credit card-sized patient Care Cards.
This experiment is driven by the belief that information management in health care is a primary key to cost containment. Approximately 9,000 patient Care Cards (which includes cards for all diabetics in the area) are in routine use. Preliminary results of the test released in late 1990 reveal significant reductions in staff time devoted to clerical functions, a significant increase in patient-centered activities by clinicians, and significant reductions in orders for laboratory tests (presumably because recent test results were available from the Care Card). Patients themselves indicated significantly greater satisfaction with the care they have received since introduction of the cards in 1989 (only 2 percent expressed dissatisfaction; Hopkins, 1990).
England has also embarked on a large experiment in which more than 16,000 general practitioners have installed personal computers in their offices to support clinical practice. This figure represents approximately half of all general practitioners in the country and is perhaps the most substantial (in terms of numbers of practitioners) clinical computing experiment undertaken to date. These and other experiments in Europe imply that Europeans have significant experience in developing clinical data standards, perhaps more than most other regions of the world. Further, they indicate the very real need for greater international cooperation in formulating future health care data standards.
Selected Emerging Developments
Once a patient's clinical data are in machine-readable form, many decision making aids will be available to health care professionals to permit them to take advantage of the latest information on problems specific to the patient. In addition, clinical data in the CPR may support other capabilities that can help ensure higher quality care, one beneficial consequence of which may be a reduction in the rate of malpractice suits. Several of these recently developed decision making aids are described below.
Chart Checker
Kaufman and Holbrook (1990) describe Chart Checker, a software package that operates in conjunction with the machine-readable emergency room record. Chart Checker analyzes the emergency room record narrative to alert the emergency room physician to potentially serious diagnoses that he or she may have overlooked or dismissed too quickly. This capability is particularly important for preventing malpractice suits. For example, Kaufman and Holbrook (1990) noted that more than 30 percent of liability cases won against emergency room physicians resulted from missing a myocardial infarction. Chart Checker has been tested using emergency room narratives
for cases in which myocardial infarctions actually occurred, and the package quite accurately suggested the possibility of that diagnosis, as well as other potentially devastating illnesses that apparently had not been seriously considered.
Chart Checker's benefits are so well demonstrated that in certain instances it has led to an across-the-board 20 percent reduction in malpractice insurance premiums for physicians. In Massachusetts, for example, this reduction in premiums (amounting to $2,400 or more per physician) became effective in July 1990 for all emergency room physicians who regularly use Chart Checker (Blau, 1990). This software is representative of many clinical decision support systems that can be expected to evolve in the near future. Such tools cannot be used by health care professionals, however, until clinical data are captured in machine-readable form. In short, the CPR must come first.
Problem-Knowledge Coupler
The problem-knowledge coupler (PKC) is another personal computer-based system designed to assist clinicians in organizing patient data in a variety of care settings (Weed, in press). Weed's system permits the clinician to build a computer-based, problem-oriented patient record; it also uses medical knowledge derived from the literature to provide the clinician with timely suggestions and information specific to the symptoms or problems of the current patient to guide and assist the clinician's decision making. Thus, the PKC presents a nearly complete list of potential causes of a patient's reported problems. Only a few topics in medicine have been covered so far, however, because many couplers have yet to be written.
The PKC is designed to provide practitioners with information they need from the literature when they need it. At the moment, the system supplies references to highly relevant, targeted articles that have been searched beforehand and are directly associated with the patient's problems. Some of the system's architects have proposed that a ready link to MEDLINE at the NLM is the solution to answering clinicians' questions near the time of the patient encounter. Currently, however, that notion may be unrealistic because the time required to formulate and perform an adequate bibliographic search is measured in minutes, not seconds.
Medical Logic Modules
Decision support systems for health care have been successfully demonstrated in recent years, but they too lack a common standard for representing the knowledge they contain, thus limiting exchanges of their contents (Pryor et al., 1984; Miller et al., 1986). As special medical knowledge databases
are developed at different institutions, the ability to share these databases will become important. Anticipating this need, the Center for Medical Informatics at the Columbia Presbyterian Medical Center has been exploring and testing the development of the Arden syntax for medical logic modules (Hripcsak et al., 1990). The Arden syntax is designed to facilitate the sharing of medical knowledge and is especially well suited for the transfer of medical knowledge bases among disparate medical decision support systems.
Clinical data derived from operational CPR systems will contribute significantly to the body of medical knowledge used by future medical decision support systems. Indeed, it is highly probable that CPR systems may realize their full impact only when used in conjunction with medical decision support systems. Similarly, medical decision support systems are likely to mature only when medical knowledge can be readily transferred between systems. Therefore, indirectly, the Arden syntax may be crucial to the rate of CPR system deployment.
Clinician Interaction and Resistance
Perhaps the single greatest challenge that has consistently confronted every clinical system developer is to engage clinicians in direct data entry. Clinical systems have used many different strategies to solve this problem; they range from eliminating the need for clinician input to mandating direct data entry by clinicians.
The LDS Hospital in Salt Lake City, Utah, is a good example of an innovative approach to circumvent resistance to clinician data entry. As discussed earlier in this chapter, the hospital's HELP system directly captures clinical data (from the laboratory, intensive care units, and other departments) virtually without human intervention wherever possible; it uses specially designed data-capture devices attached to conventional medical instruments that convert analog to digital information. Today, most vendors of such medical instruments and devices provide computer-ready output capabilities as standard equipment or as options.
Other systems require data to be typed by clinicians or by some intermediary. Yet the bulk of the patient record is still unstructured text, such as the patient history, the discharge summary, and physical examination findings; this text must be entered into the clinical system either by dictation, which must be transcribed in some timely manner, or by automated speech-recognition systems. Another alternative is for the information to be typed manually into the system. Many system developers have attempted to use typed input, but this approach has generally failed because busy clinicians reject it. The next section discusses possible technical support to overcome clinician resistance to interacting with CPR systems.
Finding appropriate mechanisms to encourage direct clinician input remains
a significant challenge for clinical system architects (Mandell, 1987; Benda, 1989). Experience demonstrates that providing a fee for data entry does have a positive impact. For example, the New England Deaconess Hospital found in an initial test in 1989 that paying $5 to physicians to input their own discharge summaries directly resulted in a 40 percent participation rate. Without escalating payment, 54 percent of the discharge summaries (in some months, as many as 70 percent) were entered into the system directly by physicians during the first six months of 1990 (Zibrak et al., 1990).
Technological Barriers
Several technological barriers still must be overcome before robust CPR systems can be fully realized, although no great technological breakthroughs are needed. The human interface—the place where man and machine meet—remains a major challenge (despite such advances as the graphical user interface and voice inputting) and is closely tied to system performance. As we move further into the 1990s, the major technological barriers to widespread implementation of the CPR include problems with text processing, the lack of appropriate confidentiality or security measures, and inadequate health data-exchange standards.
The Human Interface and System Performance
The lack of sufficiently powerful computing systems at an affordable price has been a major barrier to providing clinicians with an adequate human interface. Now, however, affordable state-of-the-art computer systems have been introduced, which are likely to resolve this problem. Slack (1989) argues that users of clinical systems require a response time of less than a second. Providing a simple-to-use, or nearly intuitive, human interface means dedicating a significant proportion of the computer's resources to that function, which reduces their availability for crucial clinical functions. As a result, clinical system architects in the past have generally been inclined to emphasize clinical function and performance at the expense of the human interface.
The most natural way for humans to communicate is through speech, and a great deal of computer science research has focused for decades on voice-recognition capabilities. Recently introduced, commercially viable systems address this problem in ways that are becoming acceptable to some in the health care sector, but currently available, affordable voice-recognition systems support only a portion of the health care requirements.
Three primary criteria must be met to enable widespread, effective use of such systems. First, the ability to accept and process continuous speech, that is, speaking without pausing between each individual word, is crucial.
Second, systems should be speaker independent; that is, the system should be able to recognize words spoken by any individual who might speak without first ''training" the system to recognize the words spoken by that individual. Third, systems for general medicine require large vocabularies; some domains and subdomains, for example, may require vocabularies in excess of 30,000 words or meaningful phrases. As vocabularies expand, both the costs and error rates generally become intolerable. Emerging voice-recognition technology is likely to ease the inputting of clinical data in future CPR systems, but the successful experiences discussed earlier with such systems as HELP, THERESA, and DIOGENE confirm the existence of currently available alternative approaches to capturing crucial clinical data (including text) in the CPR.
Text Processing
Assuming that text can be conveniently entered into the clinical system through voice-recognition technology or other means, the problem then becomes one of effectively analyzing in an automated way the content and meaning of the textual data. The raw material for epidemiological analysis and for effectiveness and outcomes studies is primarily text from patient records, which must be converted to coded data. For accurate comparisons, patient record data must be correctly transformed into precise, unambiguous codes that represent specific characteristic processes.
Text processing is generally considered to be a complex operation; its application to the data in the CPR, with its special and diverse vocabularies, further complicates the challenge of implementing it as a system capability. Often, the more experienced the practitioner, the more succinct or abbreviated the notes in the record. The notes thus may consist of abbreviations, acronyms, and mnemonics, which could be difficult to interpret, even by other health care professionals. Although text processors have improved markedly in recent years, they can approach but never exceed the quality of written or dictated information. Therefore, the quality of patient records can be improved only through more disciplined approaches to consistent vocabulary in the record. Although technology (voice-input or menu-driven input systems) can artificially impose more consistent terminology, practitioners should be encouraged as a rule to avoid idiosyncratic terminology and to use more formal, well-defined vocabularies. Additional technological research is needed in this area, as well as studies of incentives for behavioral change, before CPR systems can reach their full potential.
Confidentiality and Security
Among the important priorities for the 1990s is the further development
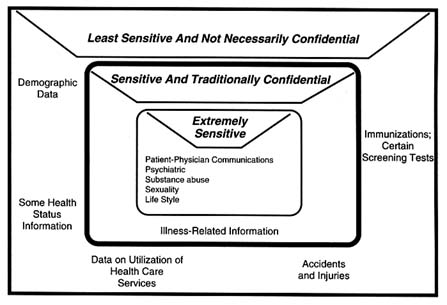
FIGURE 3.2 Three-zone confidentiality model.
of technology to ensure fully the privacy and confidentiality of patient data in the CPR. Indeed, as discussed in Chapter 4, societal and legal concerns about privacy and confidentiality must be satisfactorily resolved before wide-scale implementation of the CPR can occur. Many technologies are available to ensure CPR security and integrity, but, in general, they have not been adequately deployed or embedded in present CPR systems.
Recent research has proposed a three-zone medical confidentiality model (Figure 3-2). In this model, extremely sensitive information, which would always be held confidential, resides in the innermost zone and might not always find its way into the CPR. The outermost zone contains the least sensitive information, which may or may not be confidential. The area between these two zones is the one containing sensitive information, probably related mainly to illnesses and health problems; it is likely to be the largest area in terms of volume of the CPR and the one most frequently associated with traditional medical confidentiality requirements.
The figure illustrates why CPR systems must address confidentiality adequately at multiple levels. Patients should be permitted to name the portions of their record that are to remain totally confidential (i.e., the innermost information zone). Practitioners may also designate elements of the CPR as highly confidential. Most of the emphasis on confidentiality has involved protecting patient-related information in the CPR, but confidentiality
issues may also pertain to others engaged in providing health care. For example, all members of the health care team deserve the same level of protection against unauthorized access or abuse of information in the CPR that applies to the patient.
One important method for ensuring confidentiality, and data and program integrity, is to allow access to the CPR system only to those with a need to know and then to certify positively their identity before granting access. Fortunately, the problem of implementing measures to ensure confidentiality and privacy is not unique to medicine. Confidentiality issues are important in several areas outside health care such as finance and banking, libraries, and communications, and these sectors may offer approaches that could be tailored to the needs of health care users. For example, future CPR systems must be capable of providing different levels of data confidentiality as required by their users. Psychiatric data are a case in point: they must be available only to the patient's psychiatrist. In addition, some sensitive data for drug abuse, alcoholism, and similarly sensitive diagnoses must be protected by legal and professional rules and regulations.
Health Data-Exchange Standards
Progress toward developing acceptable standards for transferring an entire CPR has been slow, primarily because standards development has been largely ad hoc. Still, although such progress is meager in comparison to what is needed, it appears impressive when one considers that it has been accomplished virtually without government funding and without substantial industry-wide commitment. Nevertheless, the lack of funding for and coordination of standards development for CPRs can constitute a major barrier to CPR development, testing, and deployment. What is perhaps of even greater concern, given the current limited support for standards development, is the potential long-term negative impact of premature standards development. Without substantially better coordination and greater funding relatively soon, standards may evolve that may later prove to be inadequate, and neither as well conceived nor as robust as the standards needed to support a broad array of future CPR applications.
Before an actual exchange of clinical data can take place, agreement must be reached on what is being transferred. Many vendors and government agencies have independently developed their own internal clinical data dictionaries. These dictionaries differ in terms of the actual data elements included, naming conventions, definitions, and relationships among data elements. No attempt has yet been made to create a composite clinical data dictionary (CCDD) using input provided by these and other groups interested in the CPR (Figure 3-3). For example, the federal government alone has at least three distinct clinical data dictionaries (namely, those of DoD, the VA, and the Health Care
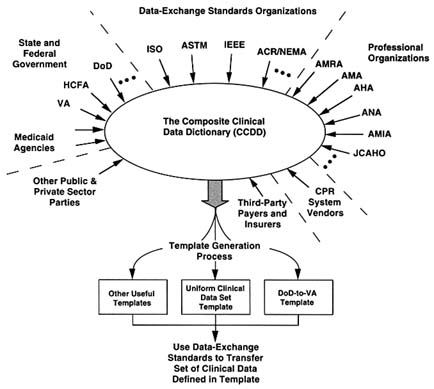
FIGURE 3-3 Concept of a composite clinical data dictionary. Abbreviations: ACR/NEMA, American College of Radiologists/National Electrical Manufacturers Association; AHA, American Hospital Association; AMA, American Medical Association; AMIA, American Medical Informatics Association; AMRA, American Medical Record Association; ANA, American Nurses Association; ASTM, American Society for Testing Materials; DoD, Department of Defense: HCFA, Health Care Financing Administration; IEEE, Institute of Electronic and Electrical Engineers; ISO, International Standards Organization; JCAHO, Joint Commission on Accreditation of Healthcare Organizations; VA, Department of Veterans Affairs.
Financing Administration); each of these has evolved independently and largely without coordination. Because no CCDD yet exists, the evolution of data-exchange standards has been limited and will remain so until a CCDD or some similar coordinating mechanism is developed.
Once a CCDD is created and perpetually maintained, any number of relevant subsets can be generated from this defined universe of clinical content. Standard definitions of subsets (or "templates," as shown in Figure 3-3) can be prepared, and data-exchange standards can then be used to carry
out the actual data transfers. For example, one potential template might be HCFA's Uniform Clinical Data Set (UCDS), a collection of approximately 1,600 data elements (Krakauer, 1990). Over time, many other relevant data sets for varied purposes are likely to be generated using subsets from the universe of data elements defined in the CCDD. For example, emergency room (ER) physicians might designate a small set of clinical data elements from the CCDD (such a subset could be the ER template) that are required to facilitate appropriate care in an emergency setting. This template could then be used to formulate an appropriate health data-exchange standard to perform the actual transfer of patient data between disparate CPR systems.
The diversity of patient record data is likely to continue as a number of different vendors and mix of institutions, service bureaus, reimbursement agencies, and governmental agencies increase their use of clinical data. It is essential, therefore, that development and promotion of standards for data representation and data exchange be major priorities. Without such standards, it will be impossible to support the necessary exchange of CPR data among the different interested organizations and institutions.
Summary
Although progress has been steady over the past two decades in developing complete CPR systems, and although several powerful clinical information systems have become operational in recent years, as yet not one is capable of supporting the complete CPR. Most of the former technological barriers to developing CPR systems have now or are about to disappear, and no technological breakthroughs are needed to implement CPR systems. Nevertheless, further maturation of a few emerging technologies, such as voice-input or voice-recognition and text-processing systems, would facilitate the development of state-of-the-art CPR systems in the 1990s.
Many different standards must be developed, tested, and deployed before the CPR can realize its full potential. Standards to facilitate the exchange of health care data are needed now so that clinical data may be aggregated and analyzed to support improved decision making. When clinical data from CPR systems are pooled in regional and national databases and made available through networks, they will constitute a vast information resource on which to base health care policy, clinical studies of effectiveness and appropriateness, and equitable reimbursement policies.
Standards are also needed for the development of more secure CPR systems. All of this effort should focus on ensuring the integrity of the clinical data in the CPR and on patient confidentiality. Confidentiality of health data in CPR systems is crucial to the success of these systems. Further, confidentiality must be maintained not only for the patient but for all health care professionals and especially for members of the health care team.
Although powerful new technologies and standards will greatly facilitate the realization of the CPR, they alone are not sufficient to overcome the barriers to its routine use. The primary barriers to realizing complete CPR systems are not technical but rather behavioral or organizational in nature. The next chapter explores various means for overcoming such barriers.
References
Andrews, R. D., and C. Beauchamp. 1989. A clinical database management system for improved integration of the Veterans Affairs hospital information system. Journal of Medical Systems 13:309–320.
ASTM (American Society for Testing Materials). 1989. Standard Guide for Nosologic Standards and Guides for Construction of New Biomedical Nomenclature. Report No. E 1284-89. Philadelphia, Pa.
Barnett, G. O. 1984. The application of computer-based medical record systems in ambulatory care. New England Journal of Medicine 310:1643–1650.
Barnett, G. O., R. Zielstorff, J. Piggins, M. McLatchey, M. Morgan, S. Barnett, D. Shusman, K. Brown, F. Weidman-Dahl, and G. McDonnell. 1982. COSTAR: A comprehensive medical information system for ambulatory care. Pp. 8–18 in Proceedings of the Sixth Symposium on Computer Applications in Medical Care, ed. B. I. Blum. Washington, D.C.: IEEE Computer Society Press.
Benda, C. 1989. Are doctors computer-compatible? Are computers physician-friendly? Minnesota Medicine 3:146–150.
Blau, M. L. 1990. Emergency physicians gain malpractice discount. Physicians News Digest 6:2–3.
Bleich, H. L., and W. V. Slack. 1989. Clinical computing. M.D. Computing 6:133–135.
Bleich, H. L., C. Safran, and W. V. Slack. 1989. Departmental and laboratory computing in two hospitals. M.D. Computing 6:149–155.
Blum, B. I., ed. 1984. Information Systems for Patient Care. New York: Springer-Verlag.
Blum, B. I., ed. 1986. Clinical Information Systems. New York: Springer-Verlag.
Canfield, K., B. Bray, and S. Huff. 1990. Representation and database design for clinical information. Pp. 350–353 in Proceedings of the Fourteenth Symposium on Computer Applications in Medical Care, ed. R. A. Miller. Washington, D.C.: IEEE Computer Society Press.
Dayhoff, R. E., D. L. Maloney, and P. M. Kuzmak. 1990. Examination of architectures to allow integration of image data with hospital information systems. Pp. 694–698 in Proceedings of the Fourteenth Symposium on Computer Applications in Medical Care, ed. R. A. Miller. Washington, D.C.: IEEE Computer Society Press.
Friedman, C., G. Hripcsak, S. B. Johnson, J. J. Cimino, and P. D. Clayton. 1990. A generalized relational scheme for an integrated clinical patient database. Pp. 335–339 in Proceedings of the Fourteenth Annual Symposium on Computer Applications in Medical Care, ed. R. A. Miller. Washington, D.C.: IEEE Computer Society Press.
GAO (General Accounting Office). 1988. Use of Information Technology in Hospitals.
Statement of Melroy D. Quasney, Associate Director, Information Management and Technology Division, before the Subcommittee on Education and Health, Joint Economic Committee. T-IMTEC-88-4. Washington, D.C. May 24.
GAO. 1990. Defense's Acquisition of the Composite Health Care System. Statement of Daniel C. White, Special Assistant to the Assistant Comptroller General, before the Subcommittee on Military Personnel and Compensation, Committee on Armed Services, U.S. House of Representatives. T-IMTEC-90-04. March 15.
Giebink, G. A., and L. L. Hurst. 1975. Computer Projects in Health Care. Ann Arbor, Mich.: Health Administration Press.
Greenes, R. A., and E. H. Shortliffe. 1990. Medical informatics: An emerging discipline and institutional priority. Journal of the American Medical Association 263:1114–1120.
Grossman, J. H., G. O. Barnett, and T. D. Koespell. 1973. An automated medical record system. Journal of the American Medical Association 224:1616–1621.
Hammond, W. E., and W. W. Stead. 1986. The evolution of a computerized medical information system. Pp. 147-156 in Proceedings of the Tenth Symposium on Computer Applications in Medical Care, ed. H. F. Orthner. New York: IEEE Computer Society Press.
Hammond, W. E., M. J. Straube, and W. W. Stead. 1990. The synchronization of distributed databases. Pp. 345–349 in Proceedings of the Fourteenth Annual Symposium on Computer Applications in Medical Care, ed. R. A. Miller. Washington, D.C.: IEEE Computer Society Press.
Harvard Community Health Plan. N.d. Automated Medical Record System (unpublished overview). Harvard Community Health Plan, Brookline, Mas.
Hopkins, R. J. 1990. The Exeter care card: A CPB-based global health care record for the United Kingdom's national health care service. Journal of Medical Systems 14:150–154.
Hripcsak, G., P. D. Clayton, T. A. Pryor, P. Haug, O. B. Wigertz, and J. Van der Lei. 1990. The Arden syntax for medical logic modules. Pp. 200–204 in Proceedings of the Fourteenth Annual Symposium on Computer Applications in Medical Care, ed. R. A. Miller. Washington, D.C.: IEEE Computer Society Press.
Humphreys, B. L., and D. A. B. Lindberg. 1989. Building the unified medical language system. Pp. 475–480 in Proceedings of the Thirteenth Annual Symposium on Computer Applications in Medical Care, ed. L. C. Kingsland. New York: IEEE Computer Society Press.
Kaufman, A., and J. Holbrook. 1990. The Computer as Expert. Springfield, Mass.: Mercy Hospital.
Kirby, J. D., M. P. Pickett, W. Boyarsky, and W. W. Stead. 1987. Distributed processing with a mainframe-based hospital information system: A generalized solution. Proceedings of the Eleventh Annual Symposium on Computer Applications in Medical Care, ed. W. W. Stead. Washington, D.C.: IEEE Computer Society Press.
Krakauer, H. 1990. The uniform clinical data set. Pp. 120–123 in Effectiveness and Outcomes in Health Care, ed. K. A. Heithoff and K. N. Lohr. Washington, D.C.: National Academy Press.
Ledley, R. S., and L. B. Lusted. 1960. The use of electronic computers in medical data processing . IRE Transactions in Medical Electronics 7:31–47.
Lindberg, D. A. B., and B. L. Humphreys. 1990. The UMLS knowledge sources: Tools for building better user interfaces. Pp. 121–125 in Proceedings of the Fourteenth Annual Symposium on Computer Applications in Medical Care, ed. R. A. Miller. Washington, D.C.: IEEE Computer Society Press.
Mandell, S. F. 1987. Resistance to computerization: An examination of the relationship between resistance and the cognitive style of the clinician. Journal of Medical Systems 4:311–318.
Margulies, D. M., R. Ribitzy, A. Elkowitz, and D. P. McCallie. 1989. Implementing an integrated hospital information system at Children's Hospital. Pp. 627–631 in Proceedings of the Thirteenth Annual Symposium on Computer Applications in Medical Care, ed. L. C. Kingsland. New York: IEEE Computer Society Press.
McDonald, C. J., L. Blevins, W. M. Tierney, and D. K. Martin. 1988. The Regenstrief medical records. M.D. Computing 5:34–47.
Miller, R. A., M. A. McNeil, S. M. Challinor, F. E. Masarie, and J. D. Myers. 1986. Status report. The INTERNIST-I: Quick medical reference project . Western Journal of Medicine 145:816–822.
National Research Council. 1991. Computers at Risk: Safe Computing in the Information Age. Washington, D.C.: National Academy Press.
Obermeier, K. 1989. Natural Language Processing Technologies in Artificial Intelligence: The Science and Industry Perspective. London: Ellis Horwood Limited.
Pryor, T. A., R. M. Gardner, P. D. Clayton, and H. R. Warner. 1983. The HELP system. Journal of Medical Systems 7:87–102.
Pryor, T. A., R. M. Gardner, P. D. Clayton, and H. R. Warner. 1984. The HELP system. Pp. 109–128 in Information Systems for Patient Care , ed. B. I. Blum. New York: Springer-Verlag.
Safran, C., D. Porter, J. Lightfoot, C. D. Rury, L. H. Underhill, H. L. Bleich, and W. V. Slack. 1989. ClinQuery: A system for on-line searching of data in a teaching hospital. Annals of Internal Medicine 111:751–756.
Scherrer, J. R., R. H. Baud, D. Hochstrasser, and R. Osman. 1990. An integrated hospital information system in Geneva. M.D. Computing 7:81–89.
Shortliffe, E. H. 1987. Computer programs to support clinical decision making. Journal of the American Medical Association 258:61–66.
Silva, J. S., A. J. Zawilski, and J. O'Brian. 1990. The physician workstation: An intelligent "front end" to a hospital information system. Pp. 764–767 in Proceedings of the Fourteenth Symposium on Computer Applications in Medical Care, ed. R. A. Miller. Washington, D.C.: IEEE Computer Society Press.
Slack, W. V. 1989. The soul of a new system: A modern parable. M.D. Computing 6:137–140.
Spencer, W. A., and C. Vallbona. 1965. Applications of computers in clinical practice. Journal of the American Medical Association 191:121–125.
Stead, W. W., and W. E. Hammond. 1987. Demand-oriented medical records: Toward a physician workstation. Pp. 275–280 in Proceedings of the Eleventh Annual Symposium on Computer Applications in Medical Care , ed. W. W. Stead. Washington, D.C.: IEEE Computer Society Press.
Stead, W. W., and W. E. Hammond. 1988. Computer-based medical records: The centerpiece of TMR. M.D. Computing 5:48–62.
Summerfield, A. B., and E. Empey. 1965. Computer-based Information Systems for Medicine: A Survey and Brief Discussion of Current Projects . Santa Monica, Calif.: Systems Development Corporation.
Walker, H. K. 1989. Grady Memorial's integrated database. Computers in Healthcare March:36–42.
Warner, H. R., C. M. Olmsted, and B. D. Rutherford. 1972. HELP: A program for medical decision making. Computers and Biomedical Research 5:65.
Weed, L. L. 1968. Medical records that guide and teach. New England Journal of Medicine 278:593–600, 652–657.
Weed, L. L. (in press). New Premises and New Tools for Medical Practice and Medical Education. New York: Springer-Verlag.
Whiting-O'Keefe, Q. E., A. Whiting, and J. Henke. 1988. The STOR clinical information system. M.D. Computing 5:48–62.
Wiederhold, G. 1986. Views, objects and databases. Computer 19:37–44.
Wilton, R. W., and J. M. McCoy. 1989. Outpatient clinic information system based on distributed database technology. Pp. 372–376 in Proceedings of the Thirteenth Symposium on Computer Applications in Medical Care , ed. L. C. Kingsland. New York: IEEE Computer Society.
Young, D. W. 1987. What makes doctors use computers? Discussion Paper. Pp. 8–14 in Use and Impact of Computers in Clinical Medicine, ed. J. G. Anderson and S. J. Jay. New York: Springer-Verlag.
Zibrak, J. D., M. S. Roberts, L. Nelick-Cohen, and M. Peterson. 1990. Creating an environment conductive to physician participation in a hospital information system. Pp. 779–783 in Proceedings of the Fourteenth Symposium on Computer Applications in Medical Care, ed. R. A. Miller. Washington, D.C.: IEEE Computer Society Press.
Appendix: the Computer-based Patient Record System Vendor Survey
The members of the Institute of Medicine study committee agreed that their deliberations would be enhanced by access to data on commercial clinical information systems and on the perspectives of those who develop and market them. The committee's Technology Subcommittee therefore conducted an informal survey to solicit basic information from vendors active in the computer-based patient record system market. Twelve vendors associated with clinical information systems (including three hardware manufacturers) responded. This appendix briefly summarizes findings and conclusions derived by the subcommittee from the responses to the survey.
General Observations
The range of responses, both to the survey as a whole and to the individual items within it, indicated substantial differences among members of the software development industry about the operational definition of the
computer-based patient record and the data that should be captured in it. Vendor responses suggested that the industry viewed direct data entry as desirable, but they also reflected industry pessimism about whether physicians and nurses could be convinced to actually enter data (although three vendors stated that they had implemented systems in which direct data entry by practitioners was occurring). Other impediments to the immediate implementation of CPRs today, as opposed to in the future, included the cost of the system, general resistance to change within the health care industry, the need for data sharing among many different kinds of systems (including departmental systems), and the lack of a good decision support system.
Vendors showed more agreement in their view of the forces that could propel the medical record environment into the computer age. Most cited the increasingly broad range of medical record users, which mandates a patient record with expanded access. Strong consensus emerged regarding the CPR as a tool with the potential to benefit every aspect of the health care environment. Vendors also voiced some skepticism, however, that the CPR could receive the broad-based, organization-wide support required for its implementation and use in a hospital.
According to the vendor responses, technologies commonly believed to be 5 to 10 years distant are, in fact, already being employed in workable CPR systems. Three vendors claimed that they had implemented a full-scale electronic medical record in a hospital environment: one in a facility of unspecified size, the second in a hospital of 176 beds, and the third in a large, urban teaching hospital of more than 900 beds. Two of these vendors offered decision support systems, one of which was described as a powerful report-writing system and the other as an actual interactive decision support system. The survey responses also indicated that direct data entry by patient care practitioners was feasible, resistance to change notwithstanding, provided the CPR system was user-friendly and was perceived as improving quality and reducing costs for the hospital, clinic, or practice. Taken together, the survey responses appeared to suggest that the environment is right for the implementation of CPRs in hospitals—that is, if enough of the system's beneficiaries can be convinced that such a comprehensive system justifies the difficulties of implementation.
Survey Findings
FINDING 1. Close reading of the responses generates some skepticism about whether all of the named products meet the requirements of a comprehensive CPR system. This may be the case in part because too few of the necessary patient record components have been automated.
FINDING 2. The majority of the systems noted in the survey operate in
multiprocessor environments, a configuration that arises in response to a hospital's demands for flexible implementation and system expandability. This trend can be expected to continue. All but one of the systems are designed to run on the hardware of a particular vendor; the exception is a system adaptable to any hardware that uses UNIX. For the most part, the systems described in the survey do not employ the most advanced terminal technologies, even though these technologies are no longer new on the market. The one exception to this generalization—the vendor whose product is adaptable to many different types of computer hardware—supports both windowing and point-and-click technologies.
FINDING 3. System costs, including installation, are likely to be in the range of $2 million to $6 million for a medium-sized hospital. Annual maintenance costs for each system could be substantial—approximately 10 percent of the purchase or lease price.
FINDING 4. With the exception of a single software vendor, the industry is moving slowing in solving one crucial problem: ease of data entry. Although such devices as the mouse and the light pen are commonly used in other industries, and even in home computing, they are rarely found in health care computing. The only vendor that offers evidence of having solved the problem of convincing physicians and nurses to use the system is the same vendor that has exploited these technologies most fully. The same conclusion may be drawn with regard to flexible output devices: the vendor that offers the most flexible data entry methods also supports the most varied output, including terminal windowing, and has the most flexible hardware requirements.
FINDING 5. The survey responses are informative regarding vendor attitudes toward the state-of-the-art in CPR systems, but they may not be helpful in defining the actual state-of-the-art. The committee found it surprising that the software vendors who responded to the survey should so heavily emphasize hardware improvements as the necessary step in advancing to comprehensive CPRs and CPR systems.
FINDING 6. The last set of findings was based on a group of open-ended questions to which only a few vendors responded. In general, they seem reluctant to lay out in detail imaginative ideas regarding the impact of computerized systems on the industry their systems are intended to serve, namely, the health care industry. Thus, the committee found it disturbing that the vendors appeared pessimistic, perhaps unintentionally, about surmounting the difficulties involved in implementing the CPR—especially given the success that some have had in overcoming certain technological and behavioral problems associated with CPR implementation.