| This page in the original is blank. |
Introduction
Naomi Rothfield
Karen Davis and Cathy Schoen focus on the potential of managed care to provide better care for patients with chronic diseases and on potential for leaving these patients with less or no care. The risks that come with managed care are described; that is, the financial risk that plans attracting the chronically ill will do poorly compared to plans attracting healthy patients; the risk of having physicians unable to act in the best interests of their patients; the risk of patients being denied entry into a plan or dropped; and the risk of limits on referrals or appropirateness of care.
The potential for systemic lupus erythematosus (SLE) or rheumatoid arthritis (RA) patients to have better care could come from having a physician who manages all of the care of that patient. However, currently, the rheumatologist is the primary care giver for most patients with SLE and, as such, coordinates all of the care by all care givers. For patients with rheumatoid arthritis, the rheumatologist may or may not be the primary care giver.
The potential risk for both SLE and RA patients is great. These patients are high users of care and may be terminated from plans or denied access to them. Many of these patients have been denied health insurance, and this has been going on for years. For-profit and nonprofit plans do not want to attract patients such as SLE or RA patients who are chronically ill and will cost the plan money. The plans would much rather attract "healthy" patients so that they can make a profit or at least not have a loss. Thus, having skilled practitioners for the care of SLE or RA patients is not a priority of managed care plans because they might attract patients.
It is widely believed (judging by the New York Times and other newspaper
reports and TV programs) that physicians in some plans are not allowed to act as the patient's advocate and may not be allowed to tell the patient about all therapeutic or diagnostic possibilities.
At present, we are seeing a definite limit on referrals in some managed care plans. Although we do not have adequate data, it is the perception of most physicians and of most patients that physicians having the most experience with a specific disease provide the best care, which leads to the best outcome for the patient.
Research on outcomes of comparable SLE and RA patients treated by rheumatologists and by internists or family physicians is needed to document the above perceptions.
Invited Address
Karen Davis and Cathy Schoen
Today's evolving U.S. health care system poses new risks and uncertainties for access to quality care, particularly for those suffering from chronic disease. Although an era of managed care and more integrated systems in theory offers much promise for those with long-term or complex illness, the chronically ill are likely to face new barriers to access to appropriate care, given current market dynamics and insurance trends. The risks are especially high for the 40 million people without insurance coverage and the 29 million with inadequate or unstable coverage.90
This workshop offers a timely opportunity to discuss access barriers intrinsic to current market dynamics and changing systems as well as ongoing and new challenges to serving vulnerable populations well. This goal of this paper is to stimulate discussion about the likelihood of new barriers to care and policy implications. Throughout, the focus is on those populations with chronic illness that we know are likely to be at high risk: the frail elderly, low-income people, minority Americans, and women. To frame the discussion, the paper is organized into four sections:
- A discussion of characteristics of the chronically ill and new access barriers in an era of competing, capitated, managed care health "systems;"
- An analysis of current coverage and insurance trends that are likely to undermine access and continuity of care, particularly with increased enrollment of the insured in managed care organizations,
-
90
Short, PF, and J Banthin (1995). New estimates of the underinsured younger than 65 years. Journal of the American Medical Association, 274: 1302–1306.
- A review of populations likely to be at particular risk, and
- An outline of policy implications and possible strategies to address emerging concerns.
The paper's central argument is that policy changes are needed to match or anticipate the changing times. Whether or not the nation's changing health care system will evolve to improve health and quality of life for those with chronic illness, particularly the vulnerable populations, is likely to depend critically on policy responses. The paper's concluding remarks suggest directions for change that would hold new organizations accountable, reward efforts to improve health and quality of life, and improve insurance coverage and stability.
The Chronically Ill: Promises and Risks in An Era of Managed Care and Competitive Markets
Chronic Illness
Chronic illness poses particular challenges for medical and health care systems. As noted in a recent paper by Stan Jones, chronically ill patients typically require specialized as well as primary care with a varied team of providers, and needs persist and fluctuate over time.91 Care and treatment of chronic illness tend to focus on preventing or slowing the progression of illness rather than curing disease and require that patients work in partnership with physicians in following often complex care regimes.
For sicker patients, coordination and continuity of care are particularly important factors in access to quality care. To serve and care for patients with chronic illness, medical and health systems need the time to care, the flexibility to combine multiple medical and support services (varying by patient), and the ability to coordinate care, often across multiple sites or types of medical or health services.
For care systems to work well, patients and their families must have the ability to get to and pay for services, and delivery systems must be concerned with maintaining or improving the quality of life and functioning, not just treating disease. Measures of quality care or standards of appropriate care often require subtle distinctions, varying with the particular patient's condition and aimed at avoiding acute care episodes or deterioration in health status, as well as improving health or functioning.
Risk and Current Managed Care Market Dynamics
Given the ongoing and at times extensive use of health care services by the chronically ill, the minority of those in any population group with chronic illness accounts for a substantial share of total health care expenses for the group. As a result, the distribution of health care expenses is highly skewed. For children, for example, recent estimates indicate that the 70 percent of children who are relatively healthy account for only 10 percent of total expenses, whereas the 20 percent of children with minor chronic problems and the 10 percent with serious illness or severe chronic disease account for 90 percent of expenses.92 As a result, children with chronic illness are two to five times more expensive than ''average.''
Costs are similarly and dramatically skewed at the other end of the age spectrum (See Figure 7-1).
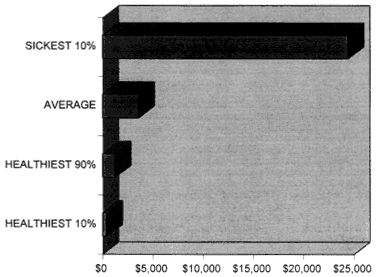
Figure 7-1
Average per capita costs for subgroups of Medicare beneficiaries, 1993 (authors' calculations are based on Health Care Financing Review, Statistical Supplement, 1995).
The sickest 5 percent of Medicare beneficiaries account for half of total spending, while the healthiest 90 percent account for only 30 percent of total spending. Average costs for the sickest 5 percent came to more than $24,000 per person in 1994, compared to $3,561 per person for all Medicare beneficiaries.93 Unlike costs for more episodic illness or accidents, higher costs for care for the chronically ill persist over time, with fluctuations depending on severity.
Managed care and integrated delivery systems should, in theory, offer much promise for the chronically ill. Such plans can move the burden of coordinating care from the patient to case managers and, with capitated payments, allow physicians and case managers to operate under more flexible budgets to arrange and pay for services as needed, without regard to narrowly defined covered benefits or providers. More highly integrated plans also offer the potential of shared medical records and close coordination of care by teams. By taking on the responsibility of providing care over time, managed care organizations should have a significant incentive to invest in improvements in cost-effective care centered on patient concerns and circumstances. In theory, markets could be structured to encourage plans to compete with one another on their reputations for quality as well as costs and to give plans strong incentives to invest in improving care while lowering costs. The emphasis would be on effective care and system improvements.
In practice, current market dynamics are more likely to reward those plans that succeed in avoiding risk and penalize those that gain a reputation for outstanding care for the seriously or chronically ill. With most public and private purchasers paying plans on the basis of average costs, with only minor adjustment for risk (usually age, sex, and disability status), managed care plans have an incentive to attract those at the low end of the expense distribution and, at best, keep quiet about aspects of care systems that in practice, might attract a disproportionate share of the chronically ill,
In today's markets, we are probably just at the beginning of seeing the impact of intense competition among capitated Plans. In most markets across the country, the industry is still relatively new and has enjoyed the favorable risk advantage of relatively new market entrants. The existence of fee-for-service (FFS) plans (whether Medicaid, Medicare, or an employer's residual indemnity plan) as the preferred choice for those with a long-standing provider relationship or in the midst of ongoing care has skewed risk in favor of newer plans and moderated competitive pressures and incentives to adopt more aggressive measures to avoid risk. Studies repeatedly find that when more limited managed care network plans are offered side by side with an FFS option, fee for service, with its broad community coverage, tends to absorb a
disproportionate share of higher-cost, older populations with more chronic, severe conditions.94
Plans to date have also typically sought to offer as broad a network as possible in order to increase market share. Trend data within the health maintenance organization (HMO) field, for example, show almost all the growth has come in broader-based association models. Similarly, among the employed population, the jump from 54 percent enrolled in managed care in 1993 to 70 percent in 1995 has come almost entirely from the growth in preferred provider organization (PPO) enrollment and plans offering point-of-service (POS) options.95
As market penetration deepens in the coming years and a greater proportion of the seriously and chronically are enrolled in managed care plans, competition among managed care organizations is likely to intensify, with individual plans less able to gain advantage through discount arrangements alone. Network composition and control and the health status of plan members will more directly influence each plan's comparative advantages.
It is at this point in market competition that intensified competition among capitated plans threatens to erect new barriers to care. The list of opportunities to market or "de-market" based on expected risk is long and ranges from more subtle to more aggressive.96 Moreover, rather than encouraging investment care advances for the sickest patients, competitive forces may deter investment in managing care well in order to avoid a reputation for being the best for the sickest. Unless purchasers structure payments to adjust for higher expected costs based on health status, plans that seek to compete on the high end of quality and to promote reputations for caring for the chronically ill are likely to be at a competitive disadvantage
Reports from recent efforts of a California purchasing alliance to adjust for risk indicate that a disproportionate share of patients with chronic illness can result in significant pricing disadvantage, outweighing the potential gain from managing care more effectively. The plan with the highest concentration of those with chronic disease or serious illness required a 20 percent adjustment in its premium based on the underlying health status of its membership.97
Capitation: Moving to the Provider Level?
Capitation and competition for patients put in motion a dramatically different set of incentives than fee for service, particularly if risks are shifted downward to physicians or physician groups. Under fee for service, physician income depends on attracting patients in need of care. Generally, the sicker the patient and more intense the care needs, the higher is the physician or physician group income. Capitation at the physician group or individual level reverses this equation. The more care required by patients covered by capitated rates, the more physicians are at risk if they see a sicker mix of patients than their colleagues. The broader the scope of services covered by capitated rates, the greater is the potential for conflict of interest between the health and welfare of the patient and that of the physician.
We have little historical experience with which to judge the future. Today, capitation as a method of paying physicians remains a growing but small share of the managed care market. Group or staff HMOs traditionally have paid physicians salaries, with possible end-of-the-year adjustments depending on overall plan performance. Global budgets and salary payments are essentially neutral regarding delivery of care to individual patients since the physician neither gains nor loses income in deciding what services are necessary. Group or staff model HMOs historically have relied on organizational culture and supply controls to stay within capitated plan payments at the plan level.
As recently as 1994, a Physicians Payment Review Commission (PPRC) survey of plans found that Independent Provider Associations (IPAs) and network HMOs continue to pay specialists on a discounted fee-for-service or fee schedule (often a modification of Medicare's resource-based relative value scale (RBRVS), with capitation spreading mainly for primary care physicians for primary care services. Capitation for primary care services alone, however, leaves in place primary care and specialist incentives to "do more." FFS payment without risk sharing remains the norm for PPOs. Although managed care plans typically require varying mixes of withholds or bonuses to give physicians financial incentives to stay within budget targets, to date, payment incentives at the provider level in IPA or network model HMOs and PPOs continue to reward physicians who see sicker and more complex patients.98
The next few years will offer an opportunity to monitor what happens as plans seek to move risk downward in more mature, managed care markets. Capitation at the physician level, unless adjusted for risk, will give physicians as well as plans incentives to avoid the chronically ill—a major shift in current
care paradigms.
Our ability to monitor quality of care is especially weak as incentives shift from doing more to doing less. Protocols for caring for those with long term or even life-threatening disease are highly dependent on knowing the individual patient's condition and relate to functional status as well as medical condition. A recent study comparing outcomes for frail elderly patients in need of home health care, for example, found that overly restrictive managed care practices reduced care for the chronically ill elderly in need of such care and, as a result, led to poorer outcomes. To detect differences and to control for case mix, however, the study required access to medical records and details of the patients' functional status (ability to feed, dress, etc.) over time to contrast outcomes of those enrolled in managed care with those of more traditional Medicare enrollees.99
Access barriers arising from risk selection are intrinsic to competitive, capitated markets. The challenge we face today is how to encourage and support managed care plans that earn a reputation for providing access and quality care to their enrollees. Even if such plans can demonstrate that they provide lower-cost, higher-quality care for sicker patients, their total plan costs are likely to be higher than average. Without methods and standards to hold plans accountable for access and incentives to enroll and care for the chronically ill, we are likely to see new sets of access concerns in the future.
Standards of Comparison
In the past, managed care plans could be compared to the dominant fee-for-service, indemnity sector as a check point for access and care. Studies finding that managed care enrollees lower ratings for access and for various dimensions of quality of care have helped keep the pressure on plans to improve their performance.
As the FFS sector dwindles and indemnity plan benefit coverage worsens (higher deductibles and copayments), traditional plans will become less useful as a standard of comparison. The task today is to develop standards and measures capable of comparing and differentiating managed care plans and sensitive to the minority of enrollees with chronic and serious illness. Patient reports on caret from those with chronic illness in different managed care plans, as well as comparisons with broad-access FFS coverage are needed to evaluate variations.
A recent Commonwealth Fund study of experiences in three cities, for
example, found significantly different ratings by families with chronic or serious illness when comparing ratings by type of HMO (group ro staff, IPA or network, or mixed model) or PPO (Figure 7-2). Better tracking of markets at the community level will be essential to hold plans to high standards rather than let ratings shift downward.
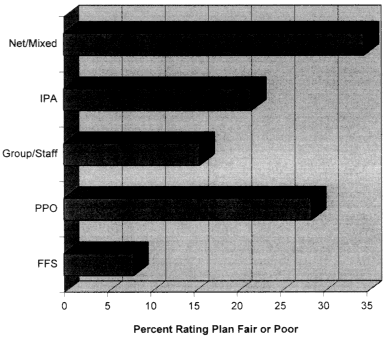
Figure 7-2
Percentage of families in poor health rating access to specialists in their health plan as fair or poor, by type of health plan. SOURCE: Commonwealth Fund Managed Care Survey, 1994.
The National Committee on Quality Assurance (NCQA) is the major organization setting standards for managed care plans. It accredits HMOs and promulgates managed care plan quality indicators known as HEDIS (Health Plan Employer Data and Information Set). Additional development of HEDIS indicators for patients with chronic conditions is an important step.
Inadequately Insured Chronically Ill: A Harsher Future
Broad coverage trends threaten severe access barriers, even if we could solve the problem of risk incentives and accountability standards tomorrow. Efforts by managed care networks and public programs to reduce fees paid for insured patients, combined with the slow but steady increase in the number of uninsured and underinsured, are undermining the capacity of community health systems to provide care for those unable to pay. The inadequately insured face an increasingly bleak and harsh future given current market trends.
Measured over a two-year period, 64 million people were uninsured for at least one month during 1991–1993. More than two-thirds of those with a gap in coverage were uninsured for at least eight months. As of 1994, 40 million people were uninsured during the year, and another 29 million were inadequately protected against costs of a long-term or serious illness,100 In combination, this amounts to one-third of the under-65 population without adequate insurance.
Most of the uninsured lack insurance because they can not afford premium costs and because, if they are employed, their employer does not offer a plan or does not pay for coverage. Incomes are generally low: three in five of the uninsured have incomes below 200 percent of poverty.101 Not surprisingly, given low income and no insurance, studies repeatedly find reports of significant access barriers to care for the uninsured and for those in and out of insurance coverage.
Mounting pressures on safety net health providers—public hospitals, community health centers, and physicians dedicated to providing at least some free care—are rapidly eroding the capacity of communities to subsidize care for the growing ranks of those without adequate insurance. In communities with a high penetration of managed care plans, market forces are cutting deeply into resources for uncompensated care. As these pressures drain resources and the ability to cross-subsidize with revenues from insured patients, we are likely to see significantly greater access barriers, with traditional entry points to free care closing their doors.
For the chronically ill, spells without insurance as well as being uninsured raise access barriers and undermine care. Those with gaps in health insurance are less likely to have a regular source of care and more likely to use multiple,
fragmented sources.102 In an era of managed care, changing jobs or changing plans, moving from Medicaid coverage to private insurance, and spells without insurance increase the likelihood that care and relationships will be disrupted. In contrast to indemnity coverage or traditional Medicaid, changing insurance coverage is no longer merely a matter of changing claims processors and reimbursement rates. Now a change in plans is likely to require a change in physician and a change in referral networks as well.
Several trends in combination are increasing the likelihood that a change in family circumstances or employment will trigger a change in physicians and care systems. Insurance for the working population is still based largely at the employer level, and employers are moving to decrease rather than expand choice of plans. RAND surveys in 1993 found that nearly half of private sector insured employees had only one plan offered by their employer, and only 18 percent had a choice of three or more plans.103 A Commonwealth Fund study found that nearly one-third of those enrolled in managed care plans in three cities did not have a choice of an alternative plan.104 Today even larger employers are seeking to narrow the range of choices in order to minimize administrative complexity, avoid adverse risk issues, and improve control. Employers have not yet moved into larger purchaser alliances capable of offering a broader range of plans meeting group standards. Thus, employer-based coverage typically offers at best a few of the managed care networks operating in each market.
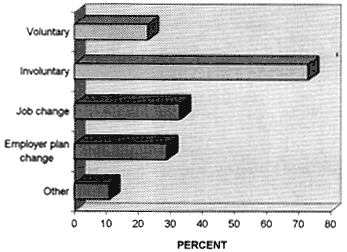
As of 1995, one-third (11.6 million) of Medicaid beneficiaries were enrolled in managed care plans, nearly triple the number enrolled in 1993.105 Beneficiaries move on and off the program frequently due to changing employment (loss or gain of a job, increase or decrease in hours and wages) or family circumstances (poor health, pregnancy, age).106 See Figure 7-3 and Figure 7-4.
Still, many Medicaid managed care plans are not offered on the commercial market, and Medicaid does not contract with all commercial plans. As a result, moving on and off Medicaid, even into a private job with insurance, is likely to mean a change in care networks. More typically, moving off Medicaid means becoming uninsured: nearly two-thirds of low income women leaving Medicaid over a two-year period lost their insurance.107
Recent Commonwealth Fund surveys indicate that frequent, usually involuntary changes in plans today are the norm rather than the exception. In a survey of employed, insured adults in three cities, nearly half of those surveyed had been in their current plan less than three years.108 Three out of four who had changed plans reported that their recent change had been involuntary, due to their employer changing plans, a change in jobs, or a change in family status. Preliminary data from a survey of low-income adults indicate even more frequent plan changes: 57 percent have been in their current plans three years or less.109 Rates of change are similarly high among low-income families whose members have chronic health conditions.
Basing eligibility for health insurance on individual employers, income, and family status has always meant frequent switching of plans and coverage. In an era of managed care and more restricted care networks, frequent change now may regularly disrupt and shift patterns of care systems and, in the process, raise new barriers to continuous care.
At the same time, managed care plans' networks are also in a state of flux. Care systems are being "dis-organized" and recreated, often with fairly high turnover in participating physicians. In newer managed care organizations, financial contracts rather than the patient's past history or immediate concerns tend to set the parameters of referrals. Physicians are now referring patients to specialists on plan lists rather than to past teams used by the physician and her or his patient in the past.
Vulnerable Populations
The time, resources, and care required by patients with chronic illness vary with social, cultural, and economic factors as well as with age and severity of disease. Repeated studies over the past decade have shown that even with
insurance, poor, near-poor, and minority populations tend to lack other resources necessary to access health care. Unless health care systems build in outreach, education, and support services, low-income families may be unable to ''comply'' with health plan rules and medical care instructions, however willing.
Managed care's emphasis on planning ahead to make appointments, calling before using services, and moving care out of hospitals into ambulatory care centers and the home by design poses barriers for low-income families or chronically ill patients (including the frail elderly) living alone. Families without telephones, transportation, other family members with time and training to care, or the ability to take time off from work during the day to get to medical care for themselves or family members are less likely to be able to navigate through to needed care. Inconvenient location of a plan's network providers (including distance to public transportation) or its hours of operation may exacerbate organizational barriers and result either in patients' continuing to rely on the nearest emergency room for episodic care or in missed appointments and delayed or postponed care.
Copayments for services in managed care plans, which seem relatively modest to middle-income families, may erect financial barriers to care for families living on already stretched or poverty budgets. Preliminary results of a Commonwealth Fund survey of families with young children find that low-income families are having trouble paying for the basic needs of their infants (formula, diapers, and clothes), much less medical care.110 Poverty leaves little room for paying even nominal fees, such as copayments for drugs or follow-up visits.
Studies also indicate that low-income and minority populations may be less prepared to negotiate the bureaucracy of managed care. Following referral rules and guidelines for making appointments and getting care may at times require considerable patient or family initiative. An early RAND study and, more recently, the Commonwealth Fund three-city survey found evidence that low-income enrollees fared less well than others enrolled in similar managed care organizations.111
The transition to managed care is likely to require time, education, and outreach efforts to ensure that new enrollees understand plan guidelines and link up with new care systems. Case studies of managed care plans with a long history of caring for lower-income and minority Medicaid populations have found that the adjustment process is a two-way street—managed care
plans discover over time that providing support services is essential to providing medical care.112 The characteristics of frail elderly, low-income, and minority populations that have historically undermined access under more traditional fee-for-service insurance are likely to continue to challenge evolving care systems. Commonwealth Fund and other studies of low-income populations find that low-income and minority populations are accustomed to episodic and fragmented care: they are more likely to cite the emergency room, hospital outpatient department, or urgent care clinics as their regular source of care; less likely to report regular use of preventive care services; and more likely to postpone getting needed care even when insured.113 Commercial plans originally developed to serve a relatively healthy, working population are finding that they need to develop services and skills to serve populations living on low incomes, facing debilitating disease, or facing hurdles due to cultural or ethnic concerns.
In most states, the transition to managed care for Medicaid beneficiaries has been so rapid that neither state agencies, plans, nor beneficiaries have had time to prepare and adjust. The rapid pace of change itself has introduced short-term access concerns that may or may not ease over time.
Minorities are also more likely to report discrimination or feeling "unwelcome" by virtue of race or ethnicity. In a recent Commonwealth Fund survey of minority health, 15 percent of minority adults believed they would have received better care if they were of a different race or ethnic group.114 Only two-thirds of minority adults felt "very" welcome at their doctors' offices. To the extent that community providers have succeeded in building more welcoming systems of care, rupturing relationships will decrease access. On the other hand, if enrollment in new networks removes past stigmas of inferior or second-class care, access may improve.
For those with chronic disease, the challenge of matching care systems for vulnerable populations is doubly complex. With care requiring a varied team of providers, referral and team arrangements—not just the site of the primary care physician—are important to building an ongoing relationship of trust and partnership with primary care providers. Patients are no longer choosing just a personal physician but an entire system of care. Similar challenges exist for serving the frail elderly and homebound.
Policy Implications
The above review of trends in coverage and managed care market dynamics implies that, absent new policies to match the changing times, access barriers are likely to grow worse for the chronically ill, particularly for the poor and those without adequate insurance. In the past, we have relied on a complex system of hidden subsidies to sustain a health care system that was for the most part accessible, at least in an emergency. As public and private purchasers reduce payments for the insured and encourage enrollment in managed care plans, resources to sustain care for those without insurance are at risk. For the insured, the dynamic of competing, capitated plans plus disruptions in coverage could move us rapidly from an era of excessive care to underservice, with plans particularly reluctant to take on care of the chronically ill. Populations that have historically been at risk for barriers to care are likely to be particularly at risk.
Three types of policy initiatives appear necessary to counteract the trend toward increased access barriers:
- incremental expansions of coverage to the uninsured most at risk;
- new methods of paying for care in managed care plans that give plans an incentive or at least neutralize disincentives to provide access and care for the chronically ill; and
- Standards, data reporting, and monitoring to hold plans accountable for quality care for sicker, more vulnerable populations.
| This page in the original is blank. |
Invited Reaction
Leigh F. Callahan
A number of today's speakers present different perspectives, depending on where they are sitting in the medical care community. Fogelman and Eisenberg focused primarily on the role of the physician and the system in this changing health care arena. Brady, Allaire, and Holman certainly highlighted the role of the patient, and Davis has highlighted both groups in looking at the problem of barriers and access to health care for the chronically ill. She noted in her paper the central argument that policy changes are needed to match or anticipate the changing times. Together with Holman's point that the health care system is attempting to deal with a set of problems it was not originally created to deal with, these are two important points to look at when we examine the barriers to health care.
Most of the speakers have focused on chronic illness and the difference between chronic and acute illness. Davis nicely summarized some of the thoughts by pointing out that the care and treatment of chronic illness tend to focus on preventing or slowing the progression of illness, rather than curing disease. The care and treatment of chronic illness require that patients work in partnership with physicians in following often complex care regimens.
That is the area I want to focus on—the complexity of this system and how it affects this issue of care versus cure, the patient's role, and the nature of the services that the patient is being asked to handle. There has been considerable discussion regarding the role of the patient as the director of medical care and the role of the patient in self-management. As Bevra Hahn pointed out, we may be a bit narrow in our thinking about the patient's role, particularly if we focus primarily on Caucasian populations.
There are a number of potential barriers facing vulnerable populations in
the changing health care system. This has been an area of considerable interest to me in rheumatoid arthritis and systemic lupus erythematosus.115 Numerous studies have demonstrated that individuals with lower socioeconomic status have increased prevalence of, and increased morbidity and mortality in, rheumatic disease and most chronic diseases. These associations of lower socioeconomic status and poor health status outcomes have been noted in many different countries with varying health care systems. Individuals with lower socioeconomic status are those individuals who are vulnerable and at risk. They are going to need the most help in dealing with the complexities of the services and the changes. In studies that have looked at potential mediators of the association between socioeconomic status and health status outcomes, measures of psychological status account for a portion of the association. This will influence the capability of the patient as the case manager.
Davis's data, not all of which appear in this volume, show that people who are at risk, who are in the poverty group or lower level, when they are in managed care settings, reported that they were not receiving care (17 percent compared to 11 percent in the FFS sector). Forty-two percent reported that they put off getting needed care. Also, a much smaller percentage of people who were in the poor, more vulnerable populations reported that they had received fair or poor service in fee for service, and the figure was close to 30 percent for some of the managed care models. Tarlov also pointed out that the nonpoor group had better outcomes in prepaid systems, whereas the poverty group had better outcomes in the fee-for-service system.
We are seeing differences in outcomes according to the type of population. We have to look at the differences in these vulnerable populations and evaluate what needs to be addressed as we change the health care system. Clearly, a lot of the issues that were brought out in terms of the role of the patient are very important. However, when we have a varied population of patients—not simply the white, upper middle class model that has been looked at so frequently in the self-management role—we are going to have to look at what the role of the system is going to be and what policy initiatives are necessary to target those at-risk and vulnerable groups.
Invited Reaction
Norman G. Levinsky
I would like to combine my two interests (a very amateur ethicist but a professional nephrologist) and say a word about some of the ethical issues I perceive in managed care, and then share with you certain analogies that I think are not too far-fetched between another chronic illness—namely, end stage renal disease—and some of the issues you were discussing with regard to rheumatic diseases.
First of all, it seems to me that managed care really is management of physicians. This isn't usually the way it is described, but the key to managed care is to manage physician behavior, physician time, and all other aspects of what physicians do as professionals. This inserts into the traditional dyad between physician and patient, where the physician's ethics determine the most appropriate care, a third party—one that has a different set of motivations.
The for-profit organization has obvious responsibilities to stockholders, but even a not-for-profit organization has responsibilities to manage costs within a set premium. A marketplace morality can be exerted in important ways by limiting what physicians can do, for example, through threats such as disenrollment, through limitation of access to a plan's patients, and through bribes (i.e., large payments for limiting care). Thus, there is an opportunity for a third party to insert a nonprofessional morality into the interchange between a physician and a patient.
What I think is especially relevant to the management of patients with chronic illnesses is the management of physician time. In most plans, physicians work on a relatively tight schedule—certainly in staff model HMOs—and managers tell them how much time they can spend with patients. As a quick anecdote, I would point out that my wife, who is a mental health
professional, receives a significant minority of her patients from one of the largest managed care programs in Massachusetts. That program allows three 20-minute visits for patients with anxiety. Fortunately for both my wife and the patient, these patients are willing and able to pay for additional counseling from her.
There are also market forces, of course, even in the fee-for-service environment. For example, we all are aware of some of the ethical tensions in recommending hip prosthesis for patients who choose hip replacements. There are prostheses varying from a few hundred dollars to several thousand dollars in cost. Because the diagnosis related group (DRG) payment for hospitals is fixed, hospital administrators have leaned on orthopedic surgeons to select prostheses without informing the patient about which prosthesis they will use or the criteria for the choice.
As I mentioned, we have had an experiment in managed care in end stage renal disease for the last 23 years. In 1973, the federal government undertook to care for virtually all Americans with end stag,: renal disease. There are a couple of points about patients on chronic dialysis that are perhaps worth comparison with rheumatic diseases. In effect, the cost of dialysis has been capitated for the past 23 years, although other aspects of the care of these patients is on a fee-for-service basis. The facilities that perform dialysis and the physicians who supervise it are paid a set sum for each of the three weekly dialysis episodes. This is really an annual managed care fee. The fee has never been adjusted upward for inflation. In fact, it has been adjusted downward in absolute dollars twice in the last 23 years. So, if one looks at it in inflation-corrected dollars, the fees now paid are 30 percent of those that were paid in 1973. What has been the response of the medical care system in caring for patients with chronic disease?
First, and most importantly in terms of patient outcome perhaps, there has been a gradual reduction in the amount of time for each episode of dialysis. This, of course, permits a given group of nurses to dialyze more patients, because each patient is dialyzed for a shorter period of time. Secondly, many units moved from having nurses deliver dialysis to having technicians deliver dialysis. Technicians are quite competent to perform the mechanics of dialysis, but they aren't clinicians and they can't handle some of the clinical issues. Third, social work support and nutritional support, which are very important for these patients, have been minimized to the point where there is really a slapdash, minimalist type of access for patients in these very important areas. There is some, although controversial, evidence that all of these changes have resulted in increases in mortality and increases in hospitalization.
In all of this 23-year period with a single payer and with access to information about all patients, there has been no real measurement of quality in the program until very recently. We know from cost reports that dialysis facilities are required to file that mortality varies from 30 percent less than the
mean to 30 percent more than the mean among different units—a 60 percent swing in mortality from the best to the worst. Similarly, the cost of a single dialysis treatment varies from $35 less than the federal payment to $35 more than the federal payment among different units. No one has tried to link these two pieces of information and see whether those facilities that cost more provide better service or simply skim off money and make a profit. 70 percent of the units doing dialysis are for-profit units).
| This page in the original is blank. |
Discussion
JOHN ROWE: Karen, you showed data that indicated that a small proportion of beneficiaries is responsible for a very large proportion of health care utilization. In the case you mentioned, 10 percent of the Medicare population used 70 percent of the dollars. This can lead to the assumption that because these are the sickest patients, they must have chronic disease. I wonder if a lot of those patients are not acutely ill—whether a lot of that utilization is not by chronically ill elderly people but by people who were previously well and had a heart attack or emergency major surgery or something similar.
KAREN DAVIS: The studies are underway, but I don't really have any answers for you. Gerard Anderson at Johns Hopkins is looking at the Medicare database and trying to sort out the health conditions of those who are in the costliest I0 percent. We have also sponsored some work by Alan Barker at the National Bureau of Economic Research on the persistence of large outlays over time. They are finding that the patients that have big expenses this year are those who will have big expenses next year. However, there is some regression to the mean, meaning that some of the people who are high health care users today are low tomorrow, and some of those who are low health care users today are high tomorrow. Therefore, if you look at three-year expenses, you don't get quite the same 10 percent of patients accounting for 70 percent of expenses, but there is still a fair amount of persistence of this high-cost-today, high-cost-tomorrow kind of patient.
NORMAN LEVINSKY: It happens that we are studying a related issue, the high-cost elderly, using the 1992 Medicare database. I can answer part of
what you asked based on unpublished data: 50 percent of the cost incurred by the most costly patients—the 5 percent who account for 50 percent of the total cost of the Medicare system—is for hospital care. About 70 percent of that 50 percent appears to be related to general medical diseases. Only 30 percent is for episodes involving a procedure, for example, a myocardial infarct followed by angioplasty or something like that.
LEIGH CALLAHAN: When you look at a specific rheumatic condition, a small percentage of the individuals account for a large percentage of the cost, even when you are just looking within the chronic disease.
DEBORAH FREUND: We heard the anecdote from someone about how specialists under carve-outs don't want to refer patients back to primary care physicians. Karen Davis told us about the barriers to access that face the elderly and the poor. Now we have heard about endstage renal disease, which in its own way and time involved a carve-out plan.
My question for Karen, and whoever else may want to answer, is the following: Is there any evidence in the Medicaid data that when you carve some subset of patients out of managed care, especially at-risk populations with chronic diseases, they do any better than if they were not carved out? Is there any relation to whether the carve-out is prepaid in and of itself?
KAREN DAVIS: I don't believe that there is a lot of literature on that yet. I think of this as merely a financial arrangement—just a different way in which the state Medicaid program would pay a health plan for care of patients with a particular disease. It would not necessarily mean that these patients would shift their sources of care.
However, in following the New York Times coverage of this issue, certainly you get a sense that many HIV patients are not faring very well in managed care plans because they can't get to their infectious disease specialists or their physicians haven't had enough experience with HIV patients and aren't up on the latest techniques.
WILLIAM HAZZARD: The exponential rise in cost per capita in the sickest resembles the exponential rise in cost per capita in the final illness. To what extent do the Medicare concentrations of cost represent terminal illness, and does that apply to rheumatological disease?
KAREN DAVIS: About 6 percent of Medicare beneficiaries die in a given year and account for 24 percent of Medicare outlays, so they don't explain the entire phenomenon of high-cost patients. Obviously part of those terminally ill do fall within the high-cost patient populations, but approximately 20
percent of those who die have not been hospitalized in the last year. So, it is not the case that everyone who dies does so in a very expensive way.
RONALD MACKENZIE: This question is perhaps best directed at Dr. Davis. It concerns the problem of accountability. Managed care companies seem to be in the process of enhancing the vulnerability of our already vulnerable patients with rheumatic diseases. Do you think that as managed care participates more in Medicare and Medicaid, which are institutions that may be a little more sensitive to the political process, we will see some redressing or influence on the broader base of managed care and the way patients are being insured?
KAREN DAVIS: I am optimistic that Medicare and also Medicaid, at least in some states, will provide a leadership role in setting regulations or rules of the game that govern managed care practice. I think that should be required for accreditation of HMOs participating in Medicare and Medicaid by an organization such as the National Committee on Quality Accreditation (NCQA). The Health Care Financing Administration (HCFA) ought to require that plans submit the HEDIS indicators. They are not currently required to submit such data. HCFA should also require the data be audited and that the results of the audit be publicly available.
HCFA has in fact worked with NCQA to develop Medicaid-specific HEDIS indicators. For example, there is a glycosylated hemoglobin test for diabetics, so they are starting to develop some specific indicators for specific conditions. I haven't seen anything yet on Medicare HEDIS, but I know that it is under development. I think it is beginning to move us in the right direction. Basically we need accreditation, quality measures, reporting of those quality measures, right of patients to appeal, a grievance process, some right to care in an emergency situation without waiting to have it approved by a plan, right of physicians to act in their patients' best interests, and appropriate payment methods for managed care plans—methods that eliminate financial disincentives or penalties for caring for the chronically ill. This is basically my list of the rules that are needed. I think that Medicare and Medicaid may well help us to move that agenda along.
BEVRA HAHN: Given that it is cheapest for people to die quickly, what would the members of the panel see as optimal measures of value?
NORMAN LEVINSKY: It seems to me that value must ultimately lie in the patients' perceptions that they are receiving something that contributes to their quality of life and ability to function. In the renal disease literature there is a well-known study that contrasts patients' perception of their functional status and quality of life with the judgment of outside observers using well-known
psychometric and other tests. The two perceptions are totally disparate. The objective analysis indicates that dialysis patients are closer to dead than to normal, whereas the patients rate themselves on a par with the average person in the United States. That is why I would focus on the patient's perception.
THEODORE FIELDS: Dr. Davis, you mentioned that it is probably not in the interests of managed care companies to advertise that they have services for the chronically ill, particularly if an expensive service is involved. How would we go about making sure that patients in managed care, particularly the chronically ill, get the information about which companies are connected with which services? Someone else previously mentioned the importance of having centers of specialized service. This may be a way in which such patients are kept away from those services, because they are not advertised.
KAREN DAVIS: In a broad way, again, in marketing for Medicare and Medicaid, I think the enrollment process should be managed by the Medicare and Medicaid programs. They are the ones that should be providing equal information on all of the plans and their capacity, quality, specialists available, credentials, and so forth, rather than door-to-door marketing or a lot of these decisions being swayed by advertising. We are a long way away from being there.
JEREMIAH BARONDESS: As clinical decisions get modified by nonphysicians and, for that matter, by nonclinicians and by computer programs, is there any information about the inclusion of managed care entities in the tort system with regard to malpractice or liability issues? If a system says that you can't have a magnetic resonance image (MRI) for a suspected acoustic neuroma, only have a computed tomography (CT) scan, and it misses the tumor, who is legally responsible?
NORMAN LEVINSKY: Actually, some very striking legal judgments have already indicated that not only HMOs but physicians are liable for their actions, even when the plan prevents them from taking the action they think is in the patient's best interests. I don't know how far that will spread or whether it will become a mechanism for improving the clinical process in some of these plans.
JOHN ROWE: There is another answer emerging as well. In the State of Maine, if you come to the emergency room as a patient with a head injury and the physician follows the approved Maine practice guideline in deciding whether you get a CT scan, the physician cannot be sued, regardless of the outcome. That experiment has been going on now for a couple of years, and the State of Florida is beginning to consider it. This approach uses practice
guidelines to immunize clinicians against inevitable, but unpredictable, adverse effects and their legal consequence.
KAREN DAVIS: Let me add one thing to that last point. In fee for service, when something is denied under Medicare the physician is often the patient's best advocate, explaining why it is really needed. In managed care the physician no longer advocates on behalf of the patient, and the patient must try to go through a grievance procedure without such help.
| This page in the original is blank. |