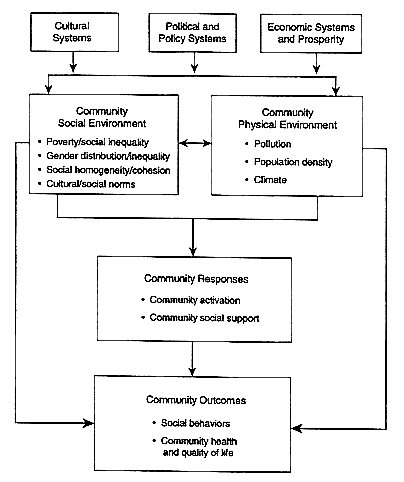
Figure 2
An organizing framework for studying community and health (illustrative factors for community social environment and community physical environment).
Source: From D.L. Patrick and T.M. Wickizer, "Community and Health," p. 67, in Society and Health, B.C. Amick et al., eds. Copyright 1995 by B.C. Amick et al. Used by permission of Oxford University Press, Inc.
Community Experience with Performance Monitoring
The committee heard presentations from five panelists describing health improvement programs in their communities. A moderator-led discussion followed the presentations.
McHenry County Project for Local Assessment of Need6
The McHenry County Project for Local Assessment of Need (McPLAN) is a framework for improving the community's health. McHenry County is the fastest growing county in Illinois and consists of 29 individual municipal areas. Although the county enjoys good health overall, certain subpopulations have less favorable health indicators.
The panelist noted that the State of Illinois was a pioneer in local community health assessment and planning through its network of local health departments. In 1993 and 1994, the Illinois Department of Public Health (IDHP), using a process patterned after the Assessment Protocol for Excellence in Public Health (APEXPH) (NACHO, 1991), coordinated a statewide project to assess the needs of local populations. McPLAN is part of this initiative. The process involved local health agencies and other health-related community organizations that promote health or work in related areas that contribute to health (e.g., education, jobs, housing). Institutionalization of the assessment process now requires that local health departments respond to local health priorities and maintain services in four basic areas (communicable disease, private sewage, private water, and food protection) rather than offer a standard set of 10 programs specified by the state. IDPH provides training and has developed a data system to better enable local health departments to conduct an effective assessment process.
In developing and implementing McPLAN, the McHenry County Department of Health has applied its experience over the past nine years in performance-based budgeting and community health needs assessment. These processes have been empowering for staff as well as community stakeholders. In the budgeting process, problem statements are developed based on local needs assessment, and indicators are selected to serve as markers for appropriate public health interventions. Staffing and other resources needed to address these problems plus an annual review of the health department's mission and goals become the basis for developing a program budget. Each quarter, a review of indicator status and resource utilization allows further refinement of staffing and resource needs. Under McPLAN, both staff and community representatives are active participants in the process through advisory committees and the Community Health Committee. The health priorities selected for the county through the first application of the McPLAN process were environmental health, unintentional injuries, and cardiovascular disease.
The performance-based budgeting process has been used to incorporate health assessment findings into local public health programming and other stakeholder organization initiatives. The use of such a process over the past nine years in McHenry County has (1) aided in the training, focus, confidence, and
perspective of staff; (2) led to a clearer understanding of the roles of the Board of Health, County Board, and related community organizations; (3) allowed movement toward allocation of a more appropriate level of resources to address identified issues (grants, appropriate fees, etc.); (4) led to greater involvement and understanding of other community providers; and (5) resulted in community-wide efforts to address childhood immunizations, improve access to health care for the medically indigent, develop joint grant applications, and begin discussion about a community-wide human services needs assessment in McHenry County.
City of Escondido Health Care and Community Services Project7
The goal of the Health Care and Community Services Project is to reduce the harmful effects of alcohol and other drug use in the community of Escondido, California (population, 120,000; county population, 2.6 million). The project coordinates a cross section of community services, including law enforcement, hospital emergency rooms, and community agencies. Integration of data systems, administrative coordination, financing, and training are other integral elements of the project's success. The municipal government functions as a facilitator for the community collaboration but does not provide services directly. Its interest is to reduce the cost of alcohol and drug use to the city and to improve the city's health.
Unlike most alcohol or drug control programs, which target individuals who are already dependent on alcohol or drugs, the Escondido project seeks to identify users who are at high risk of becoming dependent in the future. The objective is to influence drinking behavior before it reaches a critically destructive level, not to identify those already in need of specialized services (although such referrals are made when necessary). This approach is consistent with population data showing that the majority of alcohol and drug incidents involve users, not addicts. The program involves routine screening for alcohol-or drug use in high-volume, high-risk situations. It includes a three-to five-minute screening interview and brief intervention. It is administered to all adults in hospital emergency rooms, health centers, and law enforcement settings. A new component of the program is the "Sobering Service," which provides services to individuals who would otherwise be sent to the police or to the emergency room for alcohol-or drug-related care.
Three important lessons were emphasized to the committee. First, the ability to cross sectors and create an integrated program made it possible to capture savings in one sector and make these resources available to the program. For example, the city is saving the money normally spent on booking people for
alcohol-related offenses and investing it in the project. The project may become self-sustaining, because local private funds may soon be raised from managed care firms and combined with ongoing public funding for uninsured participants. (Initial funding for the project came from local city general funds, county government funds, and a matching grant from The Robert Wood Johnson Foundation.)
Second, the importance of data was emphasized. The availability of data helped to identify the stakeholders and to create a collaborative value system, based on community participation. Third, development of a data system will be important in monitoring and maintaining the integration of screening and brief intervention services within multiple collaborating agencies.
North Shore Community Health Network Area8
The Massachusetts state health department has designated 27 Community Health Network Areas (CHNAs) across the state with the goal of improving health at the community level. In each CHNA, representatives from provider groups, boards of health, community health centers, and neighborhoods work together to review community health needs, set priorities for health interventions, and help implement those interventions. The state is making available to the CHNAs data on community characteristics and health status that can be used in assessing health needs and setting priorities.
Experiences of the North Shore Community Health Network Area (NSCHNA), which encompasses eight towns north of boston, were reviewed with the committee. The NSCHNA was one of three pilot efforts for the CHNA initiative, which began in 1992. It serves as an advocate for public health ideals, strengthens the public health team, focuses on the consumer, increases affiliations by integrating services with larger health systems, and deemphasizes specific illnesses. It was noted that through the NSCHNA it has been possible to pool resources, which has stretched funds and may make more money available for efforts in areas such as prevention.
A variety of traditional health status indicators are monitored by the NSCHNA. These include economic and demographic statistics, cause-specific mortality, incidence of infectious diseases, maternal and child health indices, substance abuse rates, and hospital discharge data. High rates of lung cancer deaths and asthma hospitalization pointed to tobacco use as an area of particular concern. Thus, tobacco control emerged as the NSCHNA's initial priority. Activities that have achieved some success include promoting the removal of cigarette vending machines from areas accessible to children and adolescents and promoting expansion of smoke-free space in establishments such as malls
and restaurants. Other CHNAs in the state have chosen to focus on issues such as immunization and a reduction in sexually transmitted diseases among 15- to 19-year olds.
Arizona Partnership for Infant Immunization9
The goal of the Arizona Partnership for Infant Immunization is to improve the preschool immunization rate in Arizona by influencing provider behavior. In 1991, initial efforts were made to address immunization of preschool children. Available data showed that providers' perceptions that they were immunizing all their patients were inaccurate. Despite a historic lack of collaboration between the physician and HMO communities, representatives from each sector were convened as stakeholders. Other identified stakeholders were advocacy groups, businesses, and foundations. Participation by pediatricians was high. Because influencing 2,000 providers directly would be very difficult attention was focused on the state's 25 health plans, hoping to influence providers via the payers.
To take further action, a formal partnership, the Arizona Partnership for Infant Immunization (TAPII), was formed. Collecting data on immunization rates was recognized as essential to the project, but reaching agreement on measurement methodology was difficult. Finally, CASA (Clinic Assessment Software Application), a tool of the Centers for Disease Control and Prevention (CDC, 1992), was chosen. Once a methodology was chosen, data collection and interventions were relatively easy to plan. Health plans are now using HEDIS (NCQA, 1993) and CASA methodologies to measure and collect data.
In 1993, only 46 percent of 2-year-olds were fully immunized. In 1994, the rates increased by 10 percent. These rates were determined from medical records but may have understated immunization levels if vaccine doses given by other providers were not recorded. In 1995, immunization rates measured by the National Immunization Survey were 77 percent.10 Provider education is a key component of the program. Once an immunization rate of 80–90 percent is reached, TAPII activities may be expanded to include parent education.
The panelist emphasized the importance of clearly defining a problem that motivated stakeholders to work together. Partners in the coalition have not yet agreed to work together on other problems but have been able to collaborate effectively on this clearly defined task.





