community process that includes identification of stakeholders, adoption of a shared conceptual framework to analyze the community's health, selection of indicators appropriate to fundamental concerns, operational development of indicators, and field testing of indicators. Indicators should be descriptive; reliable, valid, and sensitive to changes in the community's health; important to stakeholders; sensitive to declines in the health of vulnerable subpopulations; and useful in monitoring health initiatives.
Determinants of Health4
Health encompasses physical and psychosocial well-being, not simply the absence of disease. Because many factors influence health and well-being, understanding the nature and scope of these determining factors is an essential element in developing health improvement strategies and in determining what indicators may be appropriate elements of a performance monitoring effort. The workshop's opening presentation used the framework of the Health Field Model for examining the determinants of health.
Health Field Model
A model of the determinants of health proposed by Evans and Stoddart—the health field model—provides a broad conceptual framework for considering the factors that influence health in a community (Evans and Stoddart, 1990). Unlike a biomedical model that views health as the absence of disease, the field model includes functional capacity and well-being as health outcomes of interest (see Figure 1). The model also emphasizes general factors that affect many diseases or the health of large segments of the population, rather than specific factors that account for small changes in health at the individual level. It takes a multidisciplinary approach, uniting biomedical sciences, public health, psychology, statistics and epidemiology, economics, sociology, education, and other disciplines. Social, environmental, economic, and genetic factors are seen as contributing to differences in health status and, therefore, as presenting opportunities to intervene.
Although this type of model is not an entirely new paradigm, its implications for designing health improvement programs deserve attention. For example, the way in which (health) behavior is understood fundamentally changes. Rather than a voluntary act amenable to direct intervention, behavior can be seen as an intermediate factor that is itself shaped by multiple forces, particularly the social and physical environments and genetic endowment. At the same time, behavior remains a relevant target for intervention. The model
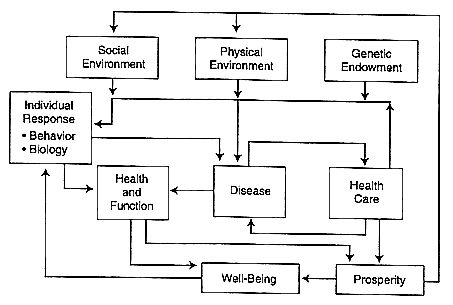
Figure 1
A model of the determinants of health. Source: Reprinted from R.G. Evans and G.L. Stoddart, ''Producing Health, Consuming Health Care,'' Social Science and Medicine 31:1359, with permission from Elsevier Science Ltd, Kidlington, UK.
also differentiates among disease, health and function, and well-being. They are affected by separate but overlapping factors, and therefore, indicators selected to monitor health improvement programs may need to differ depending on which outcome is of primary interest. The model also reinforces the interrelatedness of many factors. Outcomes are the product of complex interactions of factors rather than of individual factors operating in isolation. It was suggested that the interactions among factors may prove to be more important than the actions of any single factor.
Each of the factors included in the model is considered briefly in turn.
Social Environment
Among the elements of the social environment that have been linked to health are family structure, the educational system, social networks, social class, work setting, and level of prosperity.
Family structure, for example, is known to affect children's physical and mental health. On average, children in single-parent families do not do as well on measures of development, performance, and mental health as children in two-parent families. Children's relationships with their parents, social support, nurturance, and sense of self-efficacy have been shown to be related to their mental and physical health and even to their future economic productivity (Schor and Menaghan, 1995).
Education has an effect on health status separate from its influence on income. Years of formal education are strongly related to age-adjusted mortality in countries as disparate as Hungary, Norway, and England and Wales (Valkonen, 1989). Although most research is based on years of formal schooling, evidence suggests a broader relationship that includes the preschool period. An assessment at age 19 of participants in the Perry Preschool Study, which randomized children into a Head Start-like program, showed that participation in the preschool program was correlated with better school performance, attending college, and avoiding involvement with the criminal justice system (Weikart, 1989). Critical periods for education, particularly at young ages, may prove to be important in determining health. In addition, studies show that maternal educational attainment is a key determinant of child welfare and survival (Zill and Brim, 1983).
"Social networks" is a term that refers to an individual's integration into a self-defined community and the degree of connectedness to other individuals and to institutions. There is a strong inverse correlation between the number and frequency of close contacts and mortality from all causes, with odds ratios of 2:1 or higher and a clear "dose–response" relationship (Berkman and Syme, 1979). Although it is possible to see the impact of social networks on health, the pathways responsible for those effects are not yet known.
Social class is another well-described determinant of health, independent of income. Major studies have been done in Britain, where social class is defined more explicitly than in the United States. In the Whitehall study of British civil servants, Marmot et al. (1987) demonstrated a clear relationship between social class (based on job classification) and mortality. The relationship persists throughout the social hierarchy and is unchanged after adjusting for income and smoking. The effect of social class may raise uncomfortable issues in the United States but is important to consider in dealing with issues of health and equity.
The health effects of work-related factors are seen in studies of job decision latitude, autonomy, and cardiovascular mortality (Karasek and Theorell, 1990). Involuntary unemployment negatively affects both mental and physical health. Economic prosperity is also correlated with better health. Throughout history, the poor have, on average, died at younger ages than the rich. The relationship between prosperity and health holds across the economic spectrum. For every decile, quintile, or quartile of income, from lowest to highest, there is a decline in overall age-adjusted mortality. In international comparisons by the
Organization for Economic Cooperation and Development, the difference in income between the highest and lowest deciles of income shows a stronger relationship with overall mortality rates than does median income (Wilkinson, 1992, 1994).
Genetic Endowment
Genetic factors are recognized as having a significant influence on health, and it will be important to gain a better understanding of these influences. For the most part, genetic factors are currently understood as contributing to a greater or lesser risk for health outcomes, rather than determining them with certainty. Briefly highlighted in the presentation was the link seen between genetics and behavior. Studies of twins separated at birth demonstrate a high concordance rate in alcoholism, schizophrenia, and affective disorders (Baird, 1994). Even so-called voluntary behaviors such as smoking and eating habits may be subject to genetic predispositions (e.g., Carmelli et al., 1992; de Castro, 1993; Falciglia and Norton, 1994). Health behaviors are complex, and the influences that determine them are likely to be extremely complex.
Genetic factors also interact with social and environmental factors to influence health and disease. It will be important to understand these interactions to learn why certain individuals with similar environmental exposures develop diseases whereas others do not (e.g., why most smokers do not develop lung cancer).
Physical Environment
The physical environment affects health and disease in diverse ways. Examples include exposures to toxic substances that produce lung disease or cancers; safety at home and work, which influences injury rates; poor housing conditions and overcrowding, which can increase the likelihood of violence, transmission of infectious diseases, and mental health problems; and urban–rural differences in cancer rates.
Behavior
In the field model framework, behavior is a response to the other determinants and can be seen as an "intermediate" determinant of health. It is shaped by many forces, particularly the social and physical environments and genetic endowment, as previously described. Behaviors related to health care, such as adherence to treatment regimens, are influenced by these forces as are behaviors that directly influence health, such as smoking.




