11
Tobacco Control Policy Strategies: Lessons from Western Developed Countries
John P. Pierce
Introduction
Tobacco usage, particularly daily consumption of multiple cigarettes, has been identified as the most preventable cause of disease in the developed world (U.S. Department of Health and Human Services, 1989). Tobacco is one of the few products on the legal market which, when used explicitly as the manufacturer intended, leads to untimely death and disability. Worse still, this negative health impact is not restricted to the consumer, but extends to others who are exposed to environmental tobacco smoke (U.S. Environmental Protection Agency, 1992). In the United States alone, it is estimated that consumption of tobacco is associated with over 400,000 deaths each year. The estimated direct health care costs per smoker per year in California in 1993 were $793, using the prevalence method of cost accounting (Rice and Max, 1993).
The very size of this health impact has forced many developed nations to formulate public policies related to tobacco usage. If the product were new on the market today, it could never meet the regulatory requirements for legal production and marketing for sale. However, tobacco was introduced into Europe five centuries ago, and it now plays an important role in many national and provincial economies. No country has sought to delegalize all tobacco products. The preferred public policy has been to use public monies to convince citizens not to smoke. This policy is broadly referred to as tobacco control.
Tobacco control aims to influence citizens' behavior related to smoking. The goals of tobacco control programs are very clear:
- To protect nonsmokers in society.
- To reduce prevalence
-
-
-
by encouraging smokers to quit and
-
-
by discouraging nonsmokers from starting to smoke.
-
The objective of this chapter is to identify generalizable elements from existing tobacco control programs in Western developed countries that might usefully be employed in the NIS.
The next section of the chapter reviews the current situation and trends in tobacco use in the NIS. This is followed by a look at the context for a tobacco control program, including the natural history of smoking behavior and the role of advertising in increasing tobacco consumption. The chapter then examines the various components of a tobacco control program. The final section addresses the application of these components to the NIS.
Current Situation and Trends in Tobacco Use in the New Independent States
Tobacco Use in the New Independent States
The history of tobacco in Eastern Europe throughout the major part of this century has been marked by government-controlled production and sale of tobacco products. Throughout the 1980s, cigarette production in the region grew by around 1 percent per year. However, per capita consumption was relatively stable at around 1,600 smoking pieces per person per year between 1982 and 1988. This is approximately half the per capita consumption level of the United States.
In the 1980s, approximately half the adult men in the Soviet Union smoked, compared with less than 15 percent of the women (Zaridze et al., 1986); however, there were marked differences by age, as shown in Figure 11-1. The highest prevalence was among men aged 20 to 39, over 60 percent of whom were smokers. Prevalence among men between ages 40 and 70 was around 40 percent. There appeared to be an educational gradient, with the better-educated men smoking less than the less educated (30 vs. 60 percent). The highest prevalence among women also occurred in the age group 20 to 39 years, at 20 percent. By comparison, in the United States in 1987, around 31 percent of men and 26 percent of women smoked. There was also a marked difference in prevalence for the better and less educated (16 vs. 35 percent).1
Tobacco Products in the New Independent States
The tobacco industry in Central and Eastern Europe has changed markedly in recent years in both structure and ownership (see also Prokhorov, in this volume).
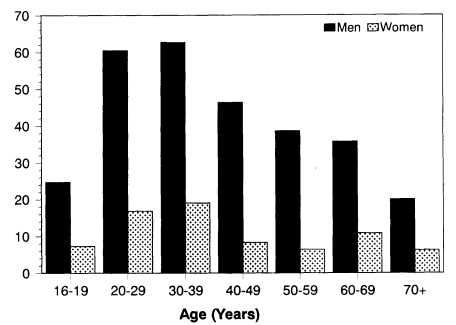
Figure 11-1
Prevalence of smoking by gender and age: Soviet Union, 1981.
SOURCE: Zaridze et al. (1986).
Privatization has occurred very quickly, with purchasers being the major transnational tobacco companies. The impetus for this change in the tobacco industry started in 1990, when the rapidly developing economic crisis led to the temporary closing of 50 percent of tobacco factories in the Soviet Union. During this time, the worsening currency problem made large-scale importation of cigarettes very expensive. There was civil unrest resulting from the shortage of cigarettes. The transnational tobacco companies agreed to provide the region with a total of 38 billion cigarettes at enormously discounted rates. Since then, these tobacco companies have acquired major interests in 34 former state monopolies in Central and Eastern Europe, with 12 being owned outright. Table 11-1 shows recent investment by transnational tobacco companies in Central and Eastern Europe.
The entry of the transnational tobacco industry giants into the economy and politics of the region has changed expectations for consumption over the next decade. In 1988, per capita consumption projections for the Soviet Union foresaw a negligible increase through 1998, with some projected brand switching toward filtered cigarettes (60 percent of market in 1988 to 80 percent in 1998) and a move toward milder cigarettes preferred by younger consumers and women. These projections were made with the knowledge that tobacco advertising had been banned in 1980 and that government regulation was likely to remain in
TABLE 11-1 Recent Transnational Tobacco Company Investments in Central and Eastern Europe
|
Region |
Plants |
Percent Ownership |
Cigarette Production Capacity (billions) |
|
Russia |
10 |
49-100 |
127 |
|
Other NIS |
17 |
51-97 |
66 |
|
Baltic |
3 |
45-65 |
16 |
|
Other Eastern Europe |
16 |
10-100 |
148 |
|
NIS = New Independent States. SOURCE: Connolly (1994). |
|||
force. The entrance of the transnational tobacco companies significantly changed that scenario.
In purchasing tobacco plants in Central and Eastern Europe, the transnational tobacco companies have significantly increased their manufacturing capabilities.2 It is expected that the long-term goals of the companies are to expand cigarette production within the region, to expand per capita consumption levels toward those seen in the United States, and to increase the level of profitability for each cigarette sold.3
To promote higher consumption levels, the industry might be expected to follow the prescription that has been so successful in other countries: large marketing expenditures and the use of their economic might to create pressure. Indeed, the new tobacco industry in the region has moved quickly to begin stimulating demand for major brands of cigarettes produced by the transnational tobacco companies. The industry has started by completely ignoring the advertising ban. Connolly (1994) reports that of the 6,723 billboards in Moscow, 70 percent advertise tobacco products—almost exclusively key multinational brands. Indirect advertising of Marlboro and Rothman's is widespread on Moscow television. During one feature film, three commercial breaks advertised Lucky Strikes. In July of 1993, the Moscow City Council took its own action to ban tobacco advertising, and a similar ban passed in the Russian Parliament. However, the Press Ministry has refused to enforce the ban, citing the importance of the advertising revenue. Prokhorov and Alexandrov (1994) report that the Moscow Department of Public Transportation has noted an enormous expansion of protected bus stops featuring tobacco advertising. Further, the Moscow Trade Department has indicated that there will be a significant increase in ''brand-name" tobacco kiosks in Moscow, thus increasing the ease of access to Western-brand cigarettes.
Recent evidence suggests, moreover, that there has been a rapid increase in smoking prevalence among young adult women in the NIS, with prevalence
already much closer to the high rates observed among men of the same age. There is also evidence suggesting a rapid recent rise in smoking among adolescents, with one study reporting 20 percent smoking rates among 12 year olds (Alexandrov et al., unpublished data, no date).
Thus, the situation in the NIS suggests that without effective tobacco control programs, there will be a major increase in tobacco use over the next few years, with the smoking-related disease epidemic worsening significantly over the next generation (see also Prokhorov, in this volume).
Context for Tobacco Control
The majority of tobacco control programs that have been undertaken have focused on influencing individual behavior and reducing smoking prevalence. Accordingly, this discussion of the context for tobacco control starts with a review of the natural history of smoking behavior.
One of the peculiarities of tobacco control is the existence of a major industrial group that seeks to influence behavior in a way that is directly contradictory to the goals of tobacco control programs. A significant goal for tobacco control is thus to reduce the effectiveness of tobacco industry efforts to stimulate demand for tobacco. Therefore, this section also reviews the evidence for the effectiveness of tobacco marketing in increasing smoking among different population groups.
The Natural History of Smoking Behavior
Most societies measure the level of smoking behavior by assessing its prevalence in the community at a particular point in time and comparing this with per capita consumption (U.S. Department of Health and Human Services, 1989). Changes in the prevalence of smoking are effected either by a reduction in the proportion of nonsmokers who start to smoke, or an increase in the proportion of smokers who quit smoking, or a change in the in-out migration ratio of smokers to nonsmokers. Tobacco control focuses on the first two of these: it aims to reduce the uptake of smoking among nonsmokers and to increase successful quitting among smokers.
The uptake of smoking has been studied extensively over the past 20 years (U.S. Department of Health and Human Services, 1989, 1994a). From these studies, there is consensus that it is a time-dependent process that starts with the development of a susceptibility to smoking (U.S. Department of Health, Education and Welfare, 1964). A nonsmoker is considered susceptible once he or she has formed attitudes and beliefs about the utility of smoking. It is this susceptibility to smoking, which occurs prior to any experimentation with cigarettes, that is the focus of many tobacco control approaches. Recent evidence from California in the United States (Evans et al., 1992) supports earlier studies in Great
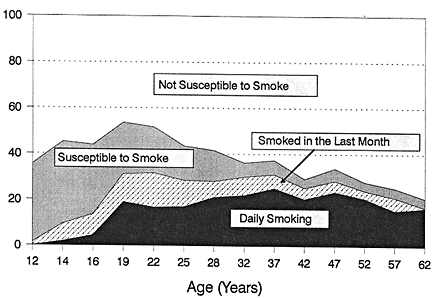
Figure 11-2
Different measures of smoking behavior for Californian females, 1992. SOURCE: Pierce et al. (1994a).
Britain (Russell, 1978) indicating that 70 percent of those who experiment with cigarettes develop an addictive habit, as shown in Figure 11-2.
Cigarette smoking fits all the criteria for an addictive behavior (U.S. Department of Health and Human Services, 1988). Nicotine has a psychoactive effect that is generally regarded as pleasant. Most individuals who smoke have built up tolerance, and their smoking behavior is highly controlled and compulsive. They have become physically dependent on the drug so that cessation of its use is associated with unpleasant physical withdrawal symptoms. The majority of attempts to quit smoking end in relapse (Gilpin and Pierce, 1994). In the United States, from one-third to one-half of smokers try to quit in any given year; however, over 90 percent of these attempts end in failure, with over half of these quitters relapsing in the first 4 days.
Quitting is not an all-or-nothing event, but a time-dependent process. Studies of successful quitting demonstrate that there are two variables that predict the probability of success: the level of addiction of the smoker and the individual's recent experience or practice in overcoming withdrawal symptoms. Thus, successful quitting of smoking can be likened to successfully completing a long-distance run. It depends on the level of fitness of the runner (read the level of addiction) and the recent practice the runner has had in overcoming the hurdles or difficulties involved in the race. Just as in the race, the smoker with the least chance of success is the one who goes into a quit attempt with a high level of
addiction and no recent practice at overcoming withdrawal. The smoker who is better prepared on both of these counts has a sixfold better chance at long-term success in quitting (Farkas et al., 1996a, 1996b).
The Role of Advertising in Increasing Tobacco Consumption
Advertising is used both to attract new consumers to tobacco products (U.S. Department of Health and Human Services, 1994a) and to convince users of alternative or competing products to switch brands (Ray, 1982). Most of the interest in tobacco advertising has focused on whether it attracts new consumers who are adolescents or minors (Albright et al., 1988; Altman et al., 1987; King et al., 1991; Mazis et al., 1992; Schooler and Basil, 1990; Schooler et al., 1991). There is little public support for the encouragement of adolescents and children to start an addictive habit, before they are old enough to appreciate its consequences. The tobacco industry strongly argues that it does not use advertising to promote smoking among minors, although it has produced little evidence to support this argument.
A recent historical analysis of cigarette advertising and the uptake of smoking in the United States examines four periods in history associated with major, different advertising campaigns.4 Cigarettes were advertised to males in two of these periods and to females in the other two. Strong evidence of the effectiveness of tobacco advertising is shown by the association of the timing of each campaign with a major increase in the uptake of smoking among the targeted gender-specific group (Pierce and Gilpin, 1995).
In recent research, we investigated the association between adolescent responsiveness to tobacco marketing and susceptibility to smoking among those who have never tried a cigarette (Pierce and Gilpin, 1995). We defined an index of receptivity that includes having a favorite cigarette advertisement and being prepared to use an item of clothing that displays a cigarette advertising logo. With this index, we demonstrated that receptivity to advertising is considerably more powerful than exposure to smokers in predicting which never-smokers will be susceptible to initiating smoking.
Components of a Tobacco Control Program
A viable tobacco control movement requires widespread acceptance of and concern about the health consequences of smoking (U.S. Department of Agriculture, 1985, 1989). Dissemination of information about the health effects of smoking and environmental tobacco smoke is a key element in building a constituency for tobacco control. Health professionals and schools have important roles in this dissemination process.
Societal-level interventions, such as the use of mass media, can also be an important influence. Many tobacco control programs aim to reconstruct societal
norms and rules to reduce the likelihood that smoking behavior will be associated with positive social benefits. Tobacco control seeks to influence the price of cigarettes, limit the access of the young, and encourage places where nonsmokers will be protected from the harmful effects of environmental tobacco smoke. In most successful programs, the use of the mass media has been crucial to these efforts (Pierce et al., 1990, 1994a; Flynn et al., 1992; Farquhar et al., 1977). One strategy has been to use paid counteradvertising and other forms of social marketing.
This section examines the various components of a tobacco control program, including the implementation of policies to restrict advertising, efforts to influence beliefs about the health consequences of smoking and environmental tobacco smoke, the role of health professionals, school-based smoking prevention programs, the use of cigarette pricing for tobacco control, efforts to control access by minors, use of mass media for counteradvertising, and the role of restrictions on smoking behavior.
The Implementation of Policies to Restrict Advertising
Advertising Bans and Their Impact on Tobacco Consumption and Smoking Uptake
A number of approaches to restricting tobacco marketing have been tried. The first approach undertaken in the United States was to ban tobacco advertising from the broadcast media (U.S. Department of Health and Human Services, 1989). A number of other countries have further restricted the rights of the tobacco companies to advertise, extending the ban to all print media as well.
In the United States, the ban on tobacco advertising in the broadcast media took effect in early 1971 (Whiteside, 1971). The impact of this ban on per capita cigarette consumption is shown in Figure 11-3. From 1900 through the release of the first Surgeon General's report on smoking and health in 1964, per capita consumption of cigarettes in the United States increased almost every year, from a level of 54 cigarettes per capita in 1900 to 4,345 in 1963. Declines occurred in 1964 and again in each year from 1967 through 1970, the years of television counteradvertising. The consistent annual decline in per capita consumption started in 1973 (U.S. Department of Health and Human Services, 1989).
For boys and girls aged 10 through 20, the first consistent decline in smoking initiation started in 1973, also approximately 2 years after the broadcast advertising ban. Before 1973, the incidence of smoking initiation among girls had sharply increased, a rise associated with the strong tobacco advertising campaign targeting women noted above. Between 1973 and 1978, the incidence rate among boys declined by approximately 25 percent and among girls by approximately 10 percent (Gilpin et al., 1994).
Can we claim that the broadcast advertising ban rather than some other
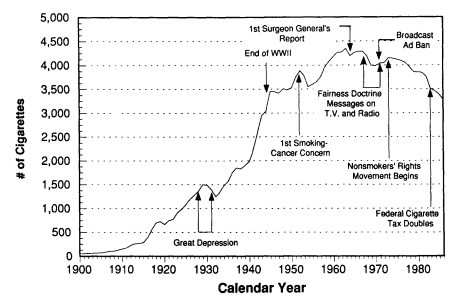
Figure 11-3
Adult per capita cigarette consumption and major smoking and health events: United States, 1900-1986. SOURCES: U.S. Department of Agriculture(1987); U.S. Department of Health and Human Services (1989).
contextual change was responsible for these declines in smoking uptake among minors? A plausible answer is that the broadcast advertising ban had a delayed effect on both incidence and consumption.5 This answer relies on the assumption that advertising works by building a susceptibility to smoking among nonsmokers and by reducing the susceptibility to quitting among smokers. An end to this stimulation of demand could thus be expected to have a delayed effect on consumption, just as demand that has already been stimulated will be reflected only in consumption over time.
Reaction of the Tobacco Industry to Restrictions on Advertising
To investigate the reaction of the industry to the 1971 broadcast media advertising ban, we look at trends in marketing expenditures before and after the introduction of the ban. During the 1960s, tobacco marketing expenditures were relatively stable, exhibiting a 26 percent increase over the decade. The introduction of the advertising ban in the 1970s was not associated with a decline in industry marketing expenditures. Indeed, quite the opposite effect was observed. With rapid annual increases, the marketing budget doubled in a 7-year period. It doubled again over the next 4 years, so that in 1981, a total of $1.5 billion was being spent on tobacco marketing. By 1988 that total had doubled again. In the
next 3 years, expenditures increased further by 42 percent, and there is no indication of a slackening of this almost exponential increase in annual marketing expenditures.
The change in the pattern of marketing expenditures that has occurred since the broadcast media advertising ban is of particular importance. During the 1960s, when there were relatively stable marketing expenditures, the industry allocated around 90 percent of its marketing budget to advertising. By 1991, 45 percent of the total marketing budget was being spent on promotional items labeled as coupons, retail value-added, or specialty item distribution. This represented over $2 billion and was equivalent to the total marketing expenditure in 1984.
In other countries, as in the United States, the introduction of restrictions on advertising has been accompanied by major budgetary increases in marketing and the introduction of new ways to promote tobacco products. In each country, the industry has developed creative ways to circumvent the ban on advertising. For example, there is considerable evidence that sponsorship of sporting events has been an excellent medium by which the industry has been able to promote its brands on television, even with the existence of the advertising ban (Blum, 1991).
The Importance of Beliefs About Health Consequences of Smoking and Environmental Tobacco Smoke
Shifts in Beliefs About the Health Consequences of Smoking
In the 1920s, the health consequences of smoking were not well known. An example of this is given by a dean of medicine at a university who recounted the story of being awakened in the middle of the night so that he could see "a case that you will never see again in your career." It turned out to be a patient with lung cancer. Nor were attitudes about smoking and health much different in the 1930s, when the U.S. population was told, through tobacco advertisements, that "more doctors smoke Camels."
The major studies that were to prove the strong association of smoking with disease were initiated in the 1940s, with the first results being published in 1950. The famous Readers Digest article entitled "Cancer by the Carton" was published in 1953, and the health consequences of smoking appeared on the front covers of major news magazines in that year. Shortly thereafter, a population survey indicated that 41 percent of the U.S. population believed that smoking causes lung cancer, a figure that had increased to 50 percent by 1957. A tobacco industry counteroffensive appeared to lower the proportion to 44 percent in 1958. The release of the first Surgeon General's report on smoking and health (U.S. Department of Health and Human Services, 1964) increased the proportion of believers to two-thirds of the population, including over half the current smokers in 1964. The Surgeon General's report marked the start of the official public
health campaign against smoking in the United States. In the years since then, the proportion of smokers who believe that smoking causes lung cancer has increased to around 90 percent (U.S. Department of Health and Human Services, 1989).
The late 1960s saw the publication of the first data suggesting that nonsmokers who were exposed to environmental tobacco smoke might also have an increased rate of lung cancer. By 1974, some 30 percent of U.S. adult smokers believed in this association. This level increased gradually over the next 4 years. The release of the Surgeon General's report on the issue in 1986 appeared to effect an increase in the proportion of believers to over 80 percent.
Trends in Initiation and Cessation
Prior to the official start of the public health campaign against smoking in 1964, the dissemination of information about the health consequences of smoking was the only anti-smoking intervention. Accordingly, we are able to assess its importance for smoking behavior by studying trends in initiation and cessation of smoking over the period.
Prior to the 1940s, cessation of smoking was rare among those who had become addicted. The incidence of cessation, defined as the number of smokers who quit successfully in a given year, started to increase among all birth cohorts of both men and women in the mid-1940s (U.S. Department of Health and Human Services, 1994b). For both genders, the incidence pattern can be described as a positively accelerating trend through the 1950s to 1970, so that between 1950 and 1964, the annual rate of successful cessation increased at least threefold among all older birth cohorts.
Changes in beliefs about the health consequences of smoking also appear to have had an effect on the incidence of the uptake of smoking, but in the 1950s and 1960s only among men over the age of 20 (U.S. Department of Health and Human Services, 1992). After the mid-1960s, there was a dramatic decline in uptake among all adults, so that by the mid-1980s very few nonsmoking adults in the United States were starting to smoke. This suggests that the message about the long-term health consequences of smoking is not very salient for children and adolescents, although it is for adults (Gilpin et al., 1994).
The Role of Health Professionals in Tobacco Control
The strong justification for spending public monies to undertake tobacco control comes from the enormous health consequences that result from regular use of tobacco. The central role of health professionals in conveying those consequences to the public has been well documented (U.S. Department of Health and Human Services, 1994b). Thus it is essential that health professions be the cornerstone of a tobacco control movement (although see the discussion of this
issue by Prokhorov in this volume). The tobacco industry recognized the importance of physicians in the 1930s when it advertised that more doctors smoked Camels, and later advertised that dentists advised the public to smoke Viceroys.
In every country that has seen a decline in smoking prevalence, the first group that has reduced its prevalence is the medical profession. It would appear that physicians are very important role models for health behavior in society. If physicians smoke, the population is less likely to be concerned about the health hazards of smoking. In the United States, some 60 percent of physicians smoked in 1949. By 1964, some 30 percent of doctors smoked. Today, it is estimated that less than 6 percent of physicians in the United States smoke. Physicians' rate of quitting appears similar to that of other highly educated groups in society. This rapid decline in smoking prevalence among the medical profession has been brought about by the virtual elimination of smoking among medical students (U.S. Department of Health and Human Services, 1994b). Indeed, the trends in smoking among physicians, and particularly among medical students, can be used as a barometer for the level of tobacco control activity in a country.
In addition to being role models, health professionals can play an important part in convincing smokers to quit and nonsmokers not to start smoking, as shown in Table 11-2. Over two-thirds of smokers visit a physician each year in the United States. While they may seek care for a specific problem not be related to smoking, the physician has an opportunity, and many would say a duty, to counsel them about preventing future disease.6 The physician's role is to help reinforce the smoker's motivation to quit and to provide support on each subsequent visit. Unfortunately, physicians are much more likely to counsel a patient on smoking if the patient presents them with a problem that could be smoking related. Efforts to increase this kind of activity have not yet been able to generate widespread physician involvement in assisting patients to quit.
School-Based Smoking Prevention Programs
Since the 1964 Surgeon General's report started the official public health campaign against smoking, prevention of the uptake of smoking has been recognized as crucial to major long-term reductions in prevalence among the population (U.S. Department of Health and Human Services, 1964). To this end, the 1964 Surgeon General's report advocated the conduct of programs directed at educating high school and college students about the health hazards of smoking. Early programs assumed that young people who started to smoke had somehow either not been exposed to or not paid attention to information on the health effects of smoking. Efforts were concentrated on presenting the information as vividly as possible; educational aids included films, posters, and pamphlets, which focused on arousing fear of the long-term effects of smoking. However, by the late 1970s there was general agreement that these smoking prevention programs had little impact on the probability that an adolescent would become a smoker
TABLE 11-2 Other Progress Toward Successful Cessation of Smoking
|
Prediction |
n |
% Progressed |
Adjusted Odds Ratio |
95% Confidence Interval |
|
Workplace restrictions |
||||
|
Indoor worker no ban in 1992 |
666 |
20.5 |
1.0 |
|
|
Indoor worker ban in 1992 |
665 |
30.0 |
1.82 |
1.05 + 3.17 |
|
Not working indoors one or both yearsa |
727 |
27.5 |
1.61 |
0.99 + 2.60 |
|
Home restrictions |
||||
|
Not generally banned |
1,486 |
20.3 |
1.0 |
|
|
Generally banned |
572 |
38.0 |
2.03 |
1.39+ 2.96 |
|
Belief in harm of ETSb |
||||
|
Not ETS concern |
375 |
14.9 |
1.0 |
|
|
ETS concern |
1,683 |
27.9 |
1.65 |
1.03 + 2.63 |
|
Personal motivation to quit |
||||
|
Not motivated |
1,362 |
30.3 |
1.81 |
1.22 + 2.69 |
|
Motivated |
696 |
17.7 |
1.0 |
|
|
Perceived nonsmoker annoyance |
||||
|
Not an issue |
1,665 |
24.6 |
1.0 |
|
|
Smoke + annoys |
393 |
30.3 |
1.46 |
0.89+ 2.39 |
|
Assistance and physician's advice |
||||
|
No assistance or advice |
1,364 |
25.9 |
1.0 |
|
|
Physician advice |
423 |
20.8 |
0.75 |
0.44 + 1.30 |
|
Physician advice with assistance |
115 |
33.0 |
1.5) |
0.81 + 2.76 |
|
Assistance, but not from physician |
156 |
38.3 |
2.31 |
1.30 + 4.08 |
|
a This group is not relevant to assessing the relative importance of workplace restrictions. b Environmental tobacco smoke. SOURCE: Pierce et al. (1994a). |
||||
(Goodstadt, 1978; Thompson, 1978). An alternative approach was based on the observation that those adolescents who did start smoking were those who were not performing as well at school. Programs implementing this approach aimed to change student attitudes toward school, family, or community. However, long-term evaluations failed to demonstrate any impact on reducing adolescent smoking.
Both of the above approaches have given way to a focus on the social environment as a major determinant of behavior. Programs with this focus emphasize developing community norms, as well as individual skills, to identify and
resist social influences to smoke. While there has been considerable variation on this theme, usual components of these programs have included training in identifying and interpreting tobacco marketing messages; practice in saying ''no" to peer pressures to smoke: and training that fosters general assertiveness, decision-making, and communication skills. In addition, these programs have sought to present the negative short-term consequences of smoking and the socially salient advantages of being a nonsmoker.7
These school-based approaches have been extensively researched through a series of randomized controlled trials, which appear to have been successful in the short term. However, these lower initiation rates had completely disappeared by the time the intervention groups had reached adulthood. The conclusion from these studies is that school-based programs can be very effective in the short term, but we should not expect to be able to inoculate students against ubiquitous social influences toward smoking by providing a few classes at an important point in their development. In order for these school interventions to have long-term impact on the uptake of smoking, they need to be supported by other tobacco control efforts that reduce the environmental influences promoting smoking.
Use of Cigarette Pricing for Tobacco Control
The price of a commodity is known to affect its consumption in the marketplace. Price has not been used as a tool of competition among the cigarette manufacturers, but there have been price or tax changes on a number of occasions, offering the opportunity to assess the impact of price in tobacco control efforts.
During the years before the United States entered World War I, pictures of the war tended to show soldiers relaxing after a difficult time at the front, frequently smoking cigarettes. Cigarettes became viewed as an aide to help soldiers endure the strain, "to soothe the nerves and to deaden the loneliness," in the words of a reporter of the time. In addition, General Pershing became an ardent advocate for the provision of free cigarettes to the troops. The tobacco industry was fond of quoting him: "I'll tell you what we need to win the war: we need cigarettes just as much as bullets." As a result, the Red Cross became one of many associations raising money to dispatch free cigarettes to allied soldiers. Across the United States, soldiers received free chewing gum, toothpaste, and cigarettes.
There was a marked increase in the incidence of initiation of smoking among males aged 16 through 20 in 1917 and 1918 (Pierce and Gilpin, 1995). This increased uptake rate among nonsmokers disappeared when the free cigarettes were discontinued with demobilization. The war years were also associated with a major increase in per capita consumption of cigarettes. However, unlike initiation rates, the level of consumption did not decrease to previous levels after the
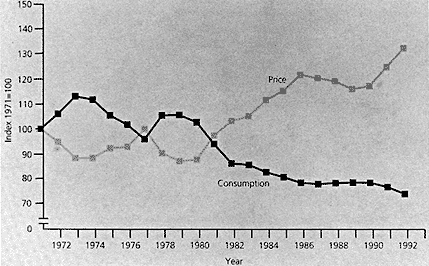
Figure 11-4
Cigarette consumption and real price: United Kingdom, 1971-1992. SOURCE: Townsend (1988).
end of the war. The most likely interpretation is that the young men who started to smoke because of the availability of free cigarettes during the war were unable or unwilling to quit when they returned to civilian life.
This war phenomenon was repeated during World War II. Free cigarettes were again available to the troops. There was a marked increase in the incidence of initiation among young men (Kennett, 1987). With demobilization, the incidence level declined to what it had been previously; again, however, there was no similar return to prewar levels in per capita consumption.
Numerous studies indicate that the demand for cigarettes generally decreases with increasing price; an example is shown in Figure 11-4. Economists use the price elasticity of demand for cigarettes to estimate the impact of an increased excise tax on consumption.8 These models suggest that a price elasticity of between -0.2 and -1.3 has existed in the United States and member countries of the Organization for Economic Cooperation and Development over the past 20 years (U.S. Department of Health and Human Services, 1989). Thus, a 10 percent increase in price could be expected to produce a reduction in consumption of between 2 and 13 percent. Variation in the level of response to a price increase may be associated with the amount of public agenda setting that accompanies the price increase. For example, in California in 1988, a 25-cent increase in the excise tax led to a 9-cent increase in price, which was associated with a 13 percent decrease in consumption. This tax increase was the subject of a major
advertising campaign and an initiative voted on in a general election. In contrast, in 1991 a 4-cent increase in tax was subsumed into a major price increase by the cigarette industry. There was no public discussion of the tax or price increase and no identifiable effect on consumption.
From the mid-1980s through 1993 in the United States, the tobacco industry introduced generic "no-name" cigarettes at a lower price while it systematically increased the price of its premium brand products. Thus, the smokers who converted to generic cigarettes could be assumed to be price sensitive. Heavier smokers, older women, and those with lower disposable incomes were much more likely to switch to generic brands. Importantly, many young people preferred to smoke the more expensive premium brands, even though the price differential was as high as 30 percent. This suggests that the price of cigarettes in the United States does not represent a recognizable drain on disposable income for many new smokers during the early years of the uptake process. Presumably, the daily consumption level is low during these years, and the smokers are less addicted and better able to adjust their consumption level to their budget. Teenagers are price sensitive, though, as was demonstrated with the reduction in adolescent smoking following the very large tax increases in the late 1980s (Ferrence et al., 1991).
Efforts to Control Access By Minors
The first major efforts to control access to cigarettes by minors occurred in the United States in the late 1890s with the formation of the anti-cigarette league.9 By 1910, the league had been successful in introducing legislation banning the sale of cigarettes to minors in many states.
Today, all states have laws prohibiting the sale of cigarettes to persons under the age of 18 (U.S. Department of Health and Human Services, 1994a). Many surveys have demonstrated that these laws have overwhelming public support among adults (both smokers and nonsmokers). However, one survey indicated that 80 percent of adults thought it was either very easy or somewhat easy for teenagers to buy cigarettes near where they live. In 1993, 40 percent of Californian 12 to 13 year olds reported that it would be easy for them to get cigarettes if they wanted to (Pierce et al., 1994a). By age 16, 85 percent of adolescents said it was easy to get cigarettes.
Of those who have bought cigarettes, 35 percent have bought from a vending machine, 55 percent from a supermarket, and 94 percent from a small convenience store such as a 7-Eleven. Worse still, Californian small store owners break open packs and sell single cigarettes to adolescents. This action breaks four different laws (Klonoff et al., 1994; Pierce et al., 1994a). However, it is being done with impunity, since chances of being prosecuted are almost nonexistent. While all states have legislation banning cigarette sales to minors, small business owners have significant financial incentives to ignore the law, and po-
lice do not see enforcement of this law as a priority issue. Thus, we have no experience with providing major barriers to access to cigarettes by minors.
Use of Mass Media for Counteradvertising
The major tobacco control success stories involving the mass media have been in encouraging people to stop smoking. The first use of the mass media to counter the tobacco industry's marketing messages occurred between 1967 and 1970, when a young attorney successfully argued that the Fairness Doctrine applied to cigarette advertising (U.S. Department of Health and Human Services, 1989). Over this period, television stations were required to show anti-smoking commercials as public service announcements if they allowed paid cigarette advertisements. Although there was a plan for a 1 to 3 ratio, the effective ratio of anti-smoking messages to cigarette ads was 1 to 12. Nevertheless, this period was the first during which there was a sustained decline in per capita consumption (see Figure 11-5). The requirement for anti-smoking messages is widely believed to have provided the disincentive for the tobacco industry to conduct a vigorous fight against the broadcast media advertising ban. Following on this success, large-scale paid media campaigns have been undertaken in Australia and in California, with published evaluations demonstrating a major impact on smoking prevalence (Pierce et al., 1990, 1994a).
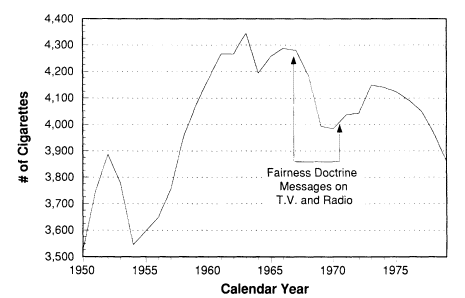
Figure 11-5
Adult per capita cigarette consumption: United States, 1950-1979.
SOURCE: U.S. Department of Agriculture (1985, 1989).
Not all mass media campaigns have been effective. The media are, after all, merely channels through which people receive information and entertainment. It has been estimated that there are up to 1,500 persuasive messages each day aimed at any given individual in the United States. Advertisers have closely studied behavior and know where to put a message to maximize our chances of being exposed to it. We are not passive as an audience, however. We actively seek some messages, avoid others, and let the majority flow by us, paying attention to one here and there that catches our attention and interest.
The amount of money that needs to be spent to ensure that a target audience is exposed to and pays attention to a given message depends on how the message is packaged. To minimize the money needed for mass media campaigns, tobacco control programs have sought to produce television advertisements that viewers will remember forever after seeing them once. However, what is recalled is a version of the original message. One cannot predict how the media message will be processed to fit the individual's experience or how it will relate to other salient messages the person has received. Powerful messages focusing on the health consequences of smoking appear to have been very important in promoting a community atmosphere that encourages smokers to quit. In addition, many smokers think about quitting when they see such advertisements and will take an immediate action, such as picking up the telephone and asking for help in quitting. This window of willingness to change can be quite brief, and the emotional impact that demands an action response to the message is generally gone in a few days. Linking such messages with telephone counseling help lines is an effective way of extending the life of a message (Pierce et al., 1992; Zhu et al., 1996). If assistance in quitting is quickly available to these responding smokers, it becomes possible to double the rate of successful quitting.
Another mass media approach that has been used is to challenge the credibility of the tobacco industry. This approach, which has been used extensively in California, argues that the industry needs to present itself in a very positive light to sustain its influence on legislators and others in thwarting tobacco control efforts. Negative advertising on the image of the industry is seen as one means of reinforcing community norms against smoking. These norms appear to play an important role in influencing smokers' willingness to attempt to quit and in influencing nonsmokers' willingness to experiment with smoking (Pierce et al., 1993, 1994a).
The third area in which the mass media have been extensively used is in advertising to prevent the uptake of smoking. Typically, tobacco control programs have emphasized images that are salient to confirmed nonsmokers. Unfortunately, there are very few success stories in this area. The tobacco industry typically outspends these campaigns by orders of magnitude as high as 25 to 30 times. Furthermore, the industry, in conjunction with advertisers, has carefully honed its messages and their presentation so that it is virtually impossible for tobacco control programs to win the image war with adolescents. Recall that
adolescents did not respond well to messages about long-term health effects of smoking (U.S. Department of Health and Human Services 1989, 1994a). They appear to qualify their willingness to experiment with the notion that they will quit before they suffer health problems. The inability of tobacco control programs to influence significantly the proportion of adolescents who start smoking is the major failing of the field to the present time. In recent years, adolescent smoking appears to have been increasing in the United States (Gilpin and Pierce, 1996).
Thus tobacco control efforts urgently need to develop a new approach for adolescents. The advertising message that is most successful is the one that ties the product to the values of the target group. The "cool," "fun," and ''relaxing" image has been staked out extremely well by the industry. However, this industry message may be vulnerable in the area of "lack of control." Many adolescent smokers report considerable difficulty in trying to quit, and for this age group in particular, such a loss of control could serve as an effective disincentive to start smoking.
The Role of Restrictions on Smoking Behavior
One of the major goals of tobacco control is to protect nonsmokers from the harmful effects of environmental tobacco smoke. As discussed earlier, the majority of the population in the United States believes that environmental tobacco smoke is harmful to nonsmokers. When the U.S. Environmental Protection Agency (1992) released its report concluding that environmental tobacco smoke is a carcinogen in the same category as asbestos, a significant additional impetus was added to the drive for clean indoor air legislation. We have a great deal of experience in developing public health legislation to protect the innocent, and rapid changes in this regard are being observed across the United States. In California, for example, in 1993, two-thirds of workers reported having a completely smoke-free workplace, and over 90 percent reported having a smoke-free work area. Since 1994, California has had statewide legislation that mandates smoke-free workplaces for all workers in the state.
There is considerable evidence that smoke-free workplaces lead to a reduction in the smoking level of heavy smokers (Borland et al., 1992). The evidence suggests that California's worksite policies assist heavy smokers in reducing their level of addiction, which in turn makes it easier for them to quit successfully in the future (Farkas et al., 1996a, 1996b; Gottlieb et al., 1990; Petersen et al., 1988; Pierce et al., 1994a; Stillman et al., 1990; Woodruff et al., 1993).
Application of these Lessons to the New Independent States
How should the tobacco control movement in the NIS react to the significant
new threat posed by the introduction of the transnational tobacco companies into their economic system? Recommendations on how to react depend on an assessment of the strength of support for tobacco control in the region. An analysis of smoking prevalence suggests that Eastern Europe may be in a position similar to that of the United States in the mid-1950s. The 1955 national survey in the United States reported a 50 percent prevalence rate for men and a 23 percent prevalence rate for women (Haenszel et al., 1955). As in the United States of that time, it would appear that the more highly educated in the NIS may have started to quit smoking. If the pattern of diffusion of cigarette smoking through society is the same as in Western countries, the more highly educated will have been the first to start smoking and the first to start to quit. The data indicate that in the United States during the mid-1980s, more highly educated men smoked at half the rate of the less well educated (Pierce et al., 1989).
However, in the NIS these promising indicators need to be balanced with other data, such as research suggesting that over half the male medical students in Eastern Europe smoke. As noted earlier, medical students in the United States were the most responsive to the start of the official campaign against smoking in 1964. In the 15 years from 1964 to 1980, smoking prevalence among medical students decreased to less than 2 percent (U.S. Department of Health and Human Services, 1994b). This decline is unprecedented in the smoking literature. It also suggests that the willingness of future physicians to start smoking is a strong statement about the medical community's tolerance of smoking behavior. A high level of tolerance can only be interpreted as a lack of strong beliefs about the health consequences of smoking among the profession.
The tobacco control movement clearly has had some legitimacy within some communities in the NIS. Recently, both the Moscow City Council and the Russian Parliament were prepared to ban cigarette advertising, which would have extended an earlier ban implemented by the Soviets in 1980. However, the willingness of legislators to promote tobacco control goals must be expected to change with the entry of the transnational tobacco companies into the economy. There is considerable evidence in the United States that the distribution of tobacco industry largesse is sufficient to weaken the enthusiasm and resolve of most legislators (Moore et al., 1994; Glantz and Begay, 1994). The tobacco industry often represents its expansion-related activities as very important to the local economy. The power of this argument, possibly supported by industry contributions to key members, has already been attested to by the unwillingness of the Russian Press Ministry to enforce legislation banning tobacco advertising.
Therefore, tobacco control would appear to have at best a tenuous grip within Eastern European communities. The initial goal of developing a tobacco control movement must be to build support among health professionals, as well as the public, for tobacco control.
In the United States, the building of a strong tobacco control coalition took over 15 years. The health effects of tobacco were plenary topics at meetings of
cancer specialists in the late 1940s. While these efforts continued to be widespread through the 1950s, it was not until the first Surgeon General's report (U.S. Department of Health and Human Services, 1964) that there was a clear indication of the acceptance of the gravity of the issue by the profession. The length of this process was determined by the continual need to bolster the evidence linking smoking with disease. In most countries, there is a need to document the link between smoking and disease, both locally and internationally, in order to build broad-based support for tobacco control.
There is some evidence from Australia that the government health department's early use of strong television commercials on the health consequences of smoking had the effect of galvanizing the medical community toward tobacco control. Given that Eastern European government authorities have shown a willingness to try to ban cigarette advertising (although not to enforce such a ban), they may be willing to allow public service announcements presenting the health side of the issue. The most effective counteradvertising focusing on health impacts includes testimonials from famous actors dying of lung cancer (from the United States) and a commercial that has proved extremely successful in crossing cultural boundaries (the "Sponge" commercial, developed in Australia in 1977) (Pierce et al., 1986).
Another mass media theme that might be effective would be to challenge the apparent perception among Eastern European youth that most young Americans smoke. One way to do this might be to use current anti-smoking advertising from the United States, with voice-overs addressing the misperception.
A key approach, given the current state of the economies in the region, would be to focus on the price of cigarettes. There does appear to be a price inflation level that is acceptable to consumers. The pricing strategy that has worked best for the industry has been to increase the price of cigarettes by small increments at regular intervals. Whenever there is an excise tax, the industry appears to reduce the amount of its own price increase. However, as discussed earlier, pricing can be an effective component of a tobacco control strategy. At the same time, it is important to note that if the increase is too large, it runs the risk of fostering a black market in the area, as it has appeared to do in Canada in recent years.
The advantages of a taxation policy can be maximized if, say, 10 percent of the revenues can be earmarked for use in tobacco control, with the rest being used to assist in other needy areas of the health system or even placed in the general revenues. Both Victoria, Australia, and California are examples of how a creative tax policy has supported the development of an aggressive tobacco control movement (The Catalonia Declaration, 1995).
References
Albright, C.L., D.G. Altman, M.D. Slater, and N. Maccoby 1988 Cigarette advertisements in magazines: Evidence for a differential focus on women's and youth magazines. Health Education Quarterly 15:225-233.
Alexandrov, A.A., V.Yu. Alexandrova, A.D. Vaganov, A.Yu. Rytenko, A.V. Prokhorov, and E.V. Zaikin n.d. The Prevalence of Smoking in Moscow Children and Adolescents. Unpublished manuscript.
Altman, D.G., M.D. Slater, C.L. Albright, and N. Maccoby 1987 How an unhealthy product is sold: Cigarette advertising in magazines, 1960-1985. Journal of Communication 37(4):95-106.
Blum, A. 1991 The Marlboro Grand Prix: Circumvention of the ban on tobacco advertising. New England Journal of Medicine 324(13):91 3-917.
Borland, R., J. P. Pierce, D.M. Burns, E. Gilpin, M. Johnson, and D. Bal 1992 Protection from environmental tobacco smoke in California: The case for a smoke-free workplace . Journal of the American Medical Association 268: 749-752.
Connolly, G.N. 1994 Tobacco Trade and Eastern Europe. Paper presented at the Ninth World Conference on Smoking and Health, October. Paris.
Ernster, V.L. 1985 Mixed messages for women: A social history of cigarette smoking and advertising. New York State Journal of Medicine 85:335-340.
Evans, N.J., E. Gilpin, J.P. Pierce, D.M. Burns, R. Borland, M. Johnson, and D. Bal 1992 Occasional smoking among adults: Evidence from the California Tobacco Survey. Tobacco Control Journal 1:169-175.
Farkas, A.J., J.P. Pierce, E. Gilpin, S.H. Zhu, B. Rosbrook, C. Berry, and R.M. Kaplan 1996a Is stage of change a useful measure of the likelihood of smoking cessation? Annals of Behavioral Medicine 18(2).
Farkas, A.J., J.P. Pierce, S.H. Zhu, B. Rosbrook, C. Berry, and R.M. Kaplan 1996b Addiction versus stage of change models in predicting smoking cessation. Addiction 91(9).
Farquhar, J.W., P.D. Wood, H. Breitrose, W.L. Haskell, A.J. Meyer, N. Maccoby, J.K. Alexander, B.W. Brown, Jr., A.L. McAlister, and J.D. Nash 1977 Community education for cardiovascular health. Lancet 1:1192-1195.
Ferrence, R.G., J.M. Garcia, K. Sykora, N.E. Collichaw, and L. Farinon 1991 Effects of Pricing on Cigarette Use Among Teenagers and Adults in Canada, 1980-1989. Toronto: Addiction Research Foundation.
Flynn, B.S., J.K. Worden, R.H. Seeker-Walker, G.J. Badger, B.M. Geller, and M.C. Costanza 1992 Prevention of cigarette smoking through mass media intervention and school programs. American Journal of Public Health 82(6):827-834.
Gilpin, E.A., and J.P. Pierce 1994 Measuring smoking cessation: Problems with recall in the 1990 California Tobacco Survey. Cancer Epidemiology. Biomarkers and Prevention 3:613-617.
1996 How long will today's new adolescent smoker be addicted to cigarettes? American Journal of Public Health 86(2):253-256.
Gilpin, E.A., L. Lee, N. Evans, and J.P. Pierce 1994 Smoking initiation rates in adults and minors: United States, 1944-1988. American Journal of Epidemiology 140:535-543.
Glantz, S.A., and M.E. Begay 1994 Tobacco industry campaign contributions are affecting tobacco control policymaking in California. Journal of the American Medical Association 272:1176-1182.
Goodstadt, M.S. 1978 Alcohol and drug education: Models and outcomes. Health Education Monographs 6(3):263-279.
Gottlieb, N., M. Eriksen, C. Lovato, R. Weinstein, and L. Green 1990 Impact of a restrictive work site smoking policy on smoking behavior, attitudes and norms. Journal of Occupational Medicine 32:16-23.
Haenszel, W., M.B. Shimkin, and H.P. Miller 1955 Tobacco Smoking Patterns in the United States. U.S. Department of Health, Education, and Welfare Public Health Monograph No. 45, PHS publication 463. Public Health Service, Office on Smoking and Health.
Kennett, L. 1987 GI: The American Soldier in World War II. New York: Charles Scribner's Sons.
Kholmogorova, G.T., and A.V. Prokhorov 1994 West goes east: The new tobacco situation in Russia. Tobacco Control 3(2):145-147.
King, K.W., L.N. Reid, Y.S. Moon, and D.J. Ringold 1991 Changes in the visual imagery of cigarette ads, 1954-1986. Journal of Public Policy Marketing 10(1):63-80.
Klonoff, E.A., J.M. Fritz, H. Landrine, R.W. Riddle, and L. Tully-Payne 1994 The problem and sociocultural context of single-cigarette sales. Journal of the American Medical Association 271(8):618-623.
Mazis, M.B., D.J. Ringold, E.S. Perry, and D.W. Denman 1992 Perceived age and attractiveness of models in cigarette advertisements. Journal of Marketing 56(1):22-37.
Moore, S., S.M. Wolfe, D. Lindes, and C.E. Douglas 1994 Epidemiology of failed tobacco control legislation. Journal of the American Medical Association 272:1171-1175.
Petersen, L., S. Helgerson, C. Gibbons, C. Calhoun, K. Ciacco, and K. Pitchford 1988 Employee smoking behavior changes and attitudes following a restrictive policy on worksite smoking in a large company. Public Health Reports 103:115-120.
Pierce, J.P., T. Dwyer, G. Frape, S. Chapman, A. Chamberlain, and N. Burke 1986 Evaluation of the Sydney "Quit for Life" Anti-Smoking Campaign: Part I, achievement of intermediate goals. Medical Journal of Australia 144:341-344.
Pierce, J.P., M.C. Fiore, T.E. Novotny, E. Hatziandrev, and R. Davis 1989 Trends in cigarette consumption in the United States: Educational differences are increasing. Journal of the American Medical Association 261(1):56-60.
Pierce, J.P., P. Macaskill, and D. Hill 1990 Long-term effectiveness of mass media-led antismoking campaigns in Australia. American Journal of Public Health 80:565-569.
Pierce, J.P., M. Anderson, R.M. Romano, H.I. Meissner, and J.C. Odenkirchen 1992 Promoting smoking cessation in the United States: Effect of public service announcements of the Cancer Information Service Telephone Line. Journal of the National Cancer Institute 84(9):677-683.
Pierce, J.P., A. Farkas, N. Evans, C. Berry, W. Choi, B. Rosbrook, M. Johnson, and D. Bal 1993 Tobacco Use in California 1992: A Focus on Preventing Uptake in Adolescents. Sacramento: California Department of Health Services.
Pierce, J.P., N. Evans, A.J. Farkas, S.W. Cavin, C. Berry, M. Kramer, S. Dealey. B. Rosbrook, W. Choi, and R.M. Kaplan 1994a Tobacco Use in California: An Evaluation of the Tobacco Control Program, 1989-1993. La Jolla: University of California, San Diego.
Pierce, J.P., L. Lee, and E.A. Gilpin 1994b Smoking initiation by adolescent girls, 1944 through 1988: An association with targeted advertising. Journal of the American Medical Association 271:608-611.
Pierce, J.P., and E. Gilpin 1995 A historical analysis of tobacco marketing and the uptake of smoking by youth in the United States: 1890-1977. Health Psychology 14(6):500-508.
Prokhorov, A.V., and A.A. Alexandrov 1994 Prevention of adolescent smoking in Russia. European Journal of Public Health 4:169-174.
Ray, M.L. 1982 Advertising and Communication Management. Englewood Cliffs, NJ: Prentice Hall.
Rice, D.P., and W. Max 1993 The cost of smoking in California, 1993. Tobacco Control.
Russell, M.A. 1978 Cigarette smoking: A dependence on high-nicotine boli. Drug Metabolism Reviews 8(1):29-57.
Schooler, C., and M.D. Basil 1990 Alcohol and Cigarette Advertising on Billboards: Targeting the Social Cues. Paper presented at the International Communication Association Conference. June. Dublin.
Schooler, C., M.D. Basil, and D.G. Altman 1991 Billboard Advertising for Alcohol and Cigarettes: Targeting with Social Cues Working Paper. Stanford, CA: Communication Department, Stanford University.
Stillman, F.A., D.M. Becker, R.T. Swank, D. Hantula, H. Moses, S. Glantz, and H.R. Waranch 1990 Ending smoking at the Johns Hopkins Medical Institutions: An evaluation of smoking prevalence and indoor air pollution. Journal of the American Medical Association 264:1565-1569.
Tennant, R.B. 1950 The American Cigarette Industry: A Study in Economic Analysis and Public Policy. New Haven, CT: Yale University Press.
The Catalonia Declaration 1995 Investing in Heart Health: Declarations of the Advisory Board of the Second International Heart Health Conference. June 1. Barcelona, Catalona.
Thompson, E.L. 1978 Smoking education programs 1960-1976. American Journal of Public Health 68(3):250-257.
Tilley, N.M. 1985 The RJ Reynolds Tobacco Company. Chapel Hill, NC: University of North Carolina Press.
Townsend, J. 1988 Price, Tax and Smoking in Europe. Geneva: World Health Organization.
U.S. Department of Agriculture 1985 Tobacco Situation and Outlook Report. Washington, DC: Economic Research Service, National Economics Division.
1987 Tobacco Situation and Outlook Report. Washington, D.C.: Economic Research Service, National Economics Division.
1989 Tobacco Situation and Outlook Report. Washington, D.C., Economic Research Service, National Economics Division. September.
U.S. Department of Health, Education, and Welfare 1964 Smoking and Health: Report of the Advisory Committee to the Surgeon General of the Public Health Service. Public Health Service publication 1103. Washington, DC: U.S. Department of Health, Education, and Welfare, Public Health Service, Centers for Disease Control.
U.S. Department of Health and Human Services 1988 The Health Consequences of Smoking: Nicotine Addiction. A Report of the Surgeon General. Department of Health and Human Services publication No. CDC 88-8406.
1989 Reducing the Health Consequences of Smoking: 25 Years of Progress. A Report of the Surgeon General. U.S. Department of Health and Human Services publication CDC 89-8411. Rockville, MD: U.S. Department of Health and Human Services, Public Health Service, Centers for Disease Control, Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health.
1991 Strategies to Control Tobacco Use in the United States: A Blueprint for Public Health Action in the 1990's. Smoking and Tobacco Control Monographs 1. NIH publication 92-3316. Bethesda, MD., Public Health Service, National Institutes of Health, National Cancer Institute.
1992 The National Health Interview Survey Design, 1973-84, and Procedures, 1975-1983. U.S. Department of Health and Human Services publication PHS 85-1320. Hyattsville, MD: U.S. Department of Health and Human Services, Public Health Service, Centers for Disease Control, National Center for Health Statistics.
1994a Preventing Tobacco Use Among Young People: A Report of the Surgeon General. U.S. Department of Health and Human Services publication S/N 017-001-00491-0. Atlanta, GA: U.S. Department of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health.
1994b Tobacco and the Clinician: Interventions for Medical and Dental Practice. Smoking and Tobacco Control Monographs 5. Bethesda, MD: NIH publication 94-3693. U.S. Department of Health and Human Services, Public Health Service, National Institutes of Health, National Cancer Institute.
U.S. Environmental Protection Agency 1992 Respiratory Health Effects of Passive Smoking: Lung Cancer and Other Disorders. EPA publication EPA/600/6-90/006F. Washington, DC: U.S. Environmental Protection Agency, Office of Research and Development, Office of Health and Environmental Assessment.
Whelan, E. 1984 A Smoking Gun: How the Tobacco Industry Gets Away with Murder. Philadelphia, PA: George F. Stickley Company.
Whiteside, T. 1971 Selling Death: Advertising and Public Health. New York: Liveright.
Woodruff, T.J., B. Rosbrook, J.P. Pierce, and S.A. Glantz 1993 Lower levels of consumption found in smoke-free workplaces in California. Archives of Internal Medicine 153:1485-1493.
Zaridze, D.G., V.V. Dvoirin, V.A. Kobljakov, and V.P. Pisklov 1986 Smoking patterns in the USSR. In D.G. Zaridze, and R. Peto, eds., Tobacco: A Major International Health Hazard. IARC publication 74. Lyon, France: International Agency for Research on Cancer.
Zhu, S-H., G.T. Tedeschi, C.M. Anderson, and J.P. Pierce 1996 Telephone counseling for smoking cessation: What's in a call? Journal of Consulting and Development (submitted for publication).
Notes
-
prevalence increased from less than 1 percent among 12-year-olds, to 7 percent among 13- to 14-year-olds, to 18 percent among 15- to 17-year-olds, and to 29 percent among 18- to 22-year-olds.
-
9.
While some have interpreted this movement as a precursor of the temperance movement, an alternative explanation is that it grew in popularity because of the type of advertising the tobacco
|
|
industry undertook in the early years. Through the 1870s and 1880s, a picture of a scantily clad woman was included with each pack of cigarettes. This use of "soft pornography" was reported to have young boys scrambling after cigarette packs. There was widespread consternation over what was perceived to be a powerful corrupting influence of the cigarette industry on boys. The first editorial on the subject appeared in the New York Times in 1879, and as concern grew, strong public statements were issued by eminent educational leaders of the day. |



























