Principles
GENERAL CONSIDERATIONS
Any approach to the support of GME, including its direct trainee support and its indirect teaching hospital subsidy, must be based on a foundation of principles. The implementation of a GME funding system also must also take into consideration historical precedent, regional variations, and political realities. At the basic, overall level, if GME and the teaching subsidy to hospitals are a legitimate part of health care services costs, then Medicare, as a responsible health care services financing program, must pay its share of these costs. Notably, Medicare has knowingly been paying more than its share to preserve the viability of the teaching sector, which is experiencing difficulties in recovering its costs from other payers (ProPAC, 1997). If, as the record of statements and decisions from Medicare suggests (Appendix B), GME and the teaching hospital subsidy are general, societal benefits, to a degree separate from providing medically necessary health care services, then Medicare could pay its share, but a decision could be taken not to do so. If Medicare, as a payer, pays its share, other payers should also do so as a matter of national policy. If not, then general public support should be provided in some way. Respecting precedent and recent congressional proposals, the committee has identified eight principles as the basis for a GME payment policy for Medicare, one that allows for, but does not recommend, other funding sources.
Principle 1. Graduate medical education and related health care services represent a reasonable and necessary national investment in the quality of U.S. medicine; they further public purposes and merit continuing public support.
American medicine's high quality and global technological preeminence have benefited from U.S. leadership in the development and diffusion of new medical technology and new procedures and methods of medical practice
(Reuter, 1996a). These advances (testing and improving new kinds of heart surgery, developing new drugs, testing of advanced technology, like MRI, for example) are supported by an infrastructure that depends on the GME mission (Blumenthal and Campbell, 1996). They often owe their conceptualization and application to practice to scientists, medical care givers, and educators at our teaching hospitals. Concentrations of patients, drawn to teaching hospitals because of unusual clinical problems, and the lessons and experiences they provide are also important contributors. With the opportunities in time and resources afforded by teaching hospitals and medical schools, scientists and patients produce the observations and clinical research, through trials and case studies, that advance the understanding of disease and its diagnosis and treatment (Goldfarb 1996; Schroeder et al., 1989). Cooperation with private industry in these endeavors, which has greatly expanded over the last decade, strengthens the U.S. domestic and export pharmaceutical and medical device industries (Blumenthal et al., 1996).
New ideas arising from clinical research are communicated across the country, contributing to needed improvements in a national standard of health care and the development of a consistent approach to care (Pew Health Professions Commission, 1995). Teaching programs, by communicating information and by example, help to create a better standard of practice in their own communities as well. Geographic variations in practice patterns, overuse of technologies, and quality problems in the delivery system have been identified through the efforts of investigators in academic health centers. The existence of an effective network of teaching institutions committed to addressing these issues should be encouraged.
As medicine evolves, different types of personnel are needed. New training programs and new kinds of expertise and professionals develop in the environment created for research and educational purposes. GME keeps clinicians current with progress in health care, and, when new knowledge could be delivered more effectively through new disciplines and specialties, GME helps to create them and train the necessary personnel. Exceptional, complex services are also made available. The GME mission enables the creation of, and its trainees help with the staffing levels needed by, these kinds of care, which are primarily found in teaching hospitals (Jones and Smith, 1997). Although a competitive health care environment is forcing needed reductions of redundancies in expensive services and overcapitalization through mergers and closures (Blumenthal et al., 1996; Gold, 1996), a leaner, reoriented system will still need GME and its support to continue the contributions to health care noted here.
By virtue of their location, tradition, and the educational mission, teaching hospitals provide care with less than the usual concern about the sources, or likelihood, of payment for their services. The populations cared for are disproportionately disadvantaged. The 286 major teaching hospitals provided about $2.5 billion in charity care in 1994, for example, which was 45 percent of
all charity care delivered by all short-term, non-federal hospitals (Jones and Smith, 1997).
The activities that are associated with GME and recognized in direct and indirect reimbursements (see Principle 2) have real though hard to measure costs, and the subsidy to teaching hospitals is based on the known relationship between the presence of training and the extra costs, (Fishman, 1996; GMENAC, 1980; Lave, 1985; ProPAC, 1997; Stedman and Zwellig, 1996). Teaching hospitals in the new competitive health care system are increasingly threatened (PPRC, 1997; ProPAC, 1997; Whitcomb and Cleverly, 1993). Health plans facing today's competitive market place are less likely to pay the subsidy for so called "public goods," such as the educational costs of young physicians who are highly mobile (Reuter et al., 1996). As a result, teaching hospitals are faced with a shrinking private-sector subsidy, although the payment over cost required to support the GME function is still partially in place (Blumenthal and Thier, 1996). If the overall subsidy is reduced enough, one would expect teaching hospitals to economize on the "public good" education, and to turn increasingly to service from their residents to the detriment of the training function.
A national investment in the quality of U.S. medicine is made through GME payments. For these and other reasons, the committee thinks it appropriate that some general, non-Medicare support of GME be available to replace the private sector's diminished implicit contribution and to participate proportionally with Medicare in support of the assets. This might well allow the Medicare support to be reduced, because, as noted above, Medicare is over paying at present. The Medicare GME payment system remains, however, a vital component that continues the government's historic obligation to provide for access to high-quality care settings for Medicare beneficiaries, to contribute fairly to paying all of the costs of the hospital system and not just the marginal costs of the least expensive providers, and to help with the special costs of teaching hospitals (e.g., uncompensated care; sicker patients; special, complex, or technologically sophisticated care; unsponsored research; and inefficiencies of care delivered by trainees, namely extra tests and procedures).
Principle 2. Direct graduate medical education (DME) funding of trainee expenses and indirect medical education (IME) support of the teaching environment are different and worthy of support separately.
GME funding covers the cost of the educational experience and the educational environment. DME support helps to fund the identified expenses of trainees. These costs are incurred in the process of training future generations of health professionals. The types and quality of health care professionals contribute importantly to the quality of the health care system. Residents in teaching hospitals help care for disadvantaged patients and, in general, help with activities that are noted in Principle 1. High-quality graduate apprenticeships are,
therefore, valuable public assets, and support of apprenticeships in the prices of goods and services is not unusual. The committee believes this argues for inclusion of DME in the price of health care.
IME support is not based on identified costs, but on a formula that recognizes the relationship between the teaching environment and the higher costs incurred by teaching hospitals. As will be described later, the formula enriches each Medicare patient's diagnosis related group (DRG) hospital payment rate. This relationship between resident training and increased cost has been observed over a considerable period (COGME, 1990; ProPAC, 1997). These higher costs were noted earlier. The value of the teaching environment extends beyond training, however. GME support sustains an intellectual climate that stimulates improvements in health care. The current division between DME and IME identifies clearly separate but related purposes, both of which are worthy of support as part of the cost of health care.
In the final analysis the current U.S. educational system produces professional practitioners who compare favorably to those produced by other medical systems. GME payment provides vital support for teaching hospitals and academic health centers; contributions to medical advances and quality of care from these institutions are the other products that GME funding buys. The relatively small price paid for these high-quality results in a $1 trillion health care system seems quite reasonable.
Principle 3. GME payment policy should focus on supporting the costs of education and the educational environment, be consistent with the work force needs of the country, and be more neutral than current policy with respect to haping the structure of the health care work force.
Past and current GME Medicare subsidy payments, which now average about $70,000 per resident, have rewarded hospitals for expanding residency programs (Appendix B). This is inconsistent with national work force policy findings of a physician oversupply and recommendations for supply control from the Council on Graduate Medical Education (COGME). Substituting a closed fund for the current open-ended entitlement should have a more neutral effect, that is, it should lessen the stimulus to add residents. Capping overall payment for residents may limit positions because having more residents will result in lower per capita reimbursements. Movement of very high DME per-resident payment toward a uniform payment should also lessen the advantage that residency expansion or maintenance of high resident numbers confers on some hospitals.
In addition, payment strategies that encourage primary care programs or residency programs of shorter duration have had only modest success (Cohen, 1995; Ginzberg, 1996; Greer et al., 1994). The committee thinks that the current differential DME payments (called weighting) that pay more (weight the calculated DME payment amount at 100%) for primary care or the first 5 years
of other residencies do little to affect the applicant pool. Many generalist positions have been unfilled (Eisenberg, 1994). In a rapidly changing health care market, precise plans for the ideal work force composition are uncertain. Observations on variation in the shape and size of the work force in different parts of the country with apparently equivalent health outcomes call into question the validity of descriptions of the appropriate work force size and composition (Goodman et al., 1996; Whitcomb, 1995).
In view of the above, the committee thinks that further conditions should not be added to the current payments related to work force composition. Some professions, such as dentistry and podiatry, do not believe their training positions exceed appropriate supply and do not wish to be caught up in mandates designed for the physician work force. The committee also does not wish to prohibit some redistribution; some regions of the country might properly need more residents to participate in programs aimed at local shortages, for example. Thus the committee concludes that a policy of controlling aggregate payment is preferable to additional attempts to restructure the work force by not paying at all, or paying differentially, for certain residents.
Principle 4. The GME payment system should allow responsiveness to health care system change, such as emphasis on primary and ambulatory care and other innovations. Eligibility for DME payment should be open to all educational and health care services entities that are responsive to change and can provide the best training. Accrediting bodies should assist this process.
The historical emphasis in GME has been on the inpatient setting and training in the teaching hospital. However, there has been of late a marked decrease in inpatient hospital care and a shift to ambulatory settings. Generalist care, managed and team care, more cost-effective care, more population-based and preventive care, and less individual-based medical management are characteristic of these ambulatory settings and of the managed care organizations that are primarily responsible for this new emphasis (Pew Health Professions Commission, 1995; Rivo et al., 1995). Training programs should ensure more exposure of residents to these settings and concepts of care (IOM, 1996b; Peinado and Eisenberg, 1990; Thier, 1994). Health professionals must continue to be technically skilled in managing serious, life-threatening disease, which traditionally has been more likely to be encountered in an inpatient setting. Nevertheless, more and more serious conditions are now being managed outside of the hospital. Few would dispute that concepts of care are changing and that training should adapt to these changes. This argues for readjusting the balance between inpatient and outpatient training and perhaps for incorporating a variety of educational models over the next few years.
The current financial incentives in GME payment policy have made adaptations in training systems slower and more difficult than might be desirable. Permitting alternative options for DME payment and encouraging consortia
among teaching hospitals, medical and osteopathic schools, and other entities that can support a GME experience consistent with changing practice needs would improve the likelihood that the training system will evolve in a responsive manner (Rich, 1994; Rieselberg et al., 1996). Including the amount of time residents spend in appropriate ambulatory sites as part of the IME payment formula—which currently only counts in-hospital time—could eliminate a payment incentive that favors institutions with more in-hospital teaching time. To complement changes in federal policy, the committee urges accrediting bodies to make accreditation available to new entities that are creative and provide the kinds of training settings that are responsive to system change and teach new and more cost-effective ways of providing care. Some managed care organizations appear to be providing such settings now (Ladden et al., 1996; Ludden, 1996, 1997), and others might develop quality programs if supported (G. Moore, personal communication, 20 February 1997; Moore et al., 1994; Veloski et al., 1996).
Principle 5. Medicare should pay its share of graduate medical education support for all its beneficiaries. Other funding sources should address the non-Medicare share proportionately. Support of GME by existing, though diminishing, private-sector payments for health care services in excess of costs may offset the need for an exactly proportional, general, non-Medicare share of support.
Medicare's responsibility for a share of GME expenses dates from the beginning of the Medicare program. Medicare GME payment gives Medicare beneficiaries access to high-quality care in teaching settings, will help beneficiaries in the future through the continued development and improvement of health care (Schweiker, 1982), and fulfills the obligations noted earlier in Principle 1. IME payment is based on a teaching hospital's individual Medicare caseload. The current IME formula of a 7.7 percent increase for each additional 0.1 resident per bed represents more than the true marginal cost increase related to increasing teaching intensity (ProPAC, 1997). The formula could be modified to reflect more closely the true relationship between the resident-to-bed ratio and cost depending on the extent that other payers assumed their share of IME support. In principle, Medicare should not be responsible for more that its share of GME and teaching hospital support. A proportional contribution from a general, non-Medicare source(s) is desirable. Congress should decide how much total support should be available. If general, non-Medicare funding is provided, Congress should assign each funding source, in so far as each fund amount allows, a proportional role within the total.
Principle 6. Nurse clinical DME and physician DME should depend on the same principles and use the same processes.
The committee thinks that funding of GME and its components should be primarily for advanced clinical and postgraduate education. After physicians (as
defined by Medicare) the next largest component of the GME payment system is for nursing. Clinical training of graduate nurses, like that of graduate physicians, contributes to the quality of care of Medicare beneficiaries through the direct provision of services and by enhancing the training environment for others. The rationale for GME support of training pre-entry-level staff is not compelling. Their contributions are less likely to control the future shape or quality of the health care system. They also make lesser contributions to research. Diploma nurse programs, which train non-graduate-level nurses and are currently eligible for GME nursing funds, are generally operated by nonteaching hospitals that receive partial reimbursement for the submitted costs of operating these programs.
Advanced practice nurses, on the other hand, can substitute for physicians in many cases (Green and Johnson, 1995). They contribute to health care delivery by practicing in underserved and rural areas, focusing on geriatric and other primary care, and providing services that residents performed, when resident programs are reduced (Knickman et al., 1992; PPRC, 1994). Advanced practice nurses meet more closely the definition of ''graduate,'' and the committee thinks it is, in principle, more reasonable to include them in GME fund distribution. Given the analogous contributions of graduate-level nurses and physicians and the rationale for conforming to the same principles, it makes sense to structure DME for nurses and physicians in the same way.
Principle 7. Payments should be reasonably consistent from institution to institution and from region to region.
Consistency and the appearance of fairness are important in achieving and sustaining public backing for the expenditure of public funds. The committee does not think that per-resident costs based on cost reports from 12 years ago should vary 10-fold from one institution to another institution (Anderson, 1996).
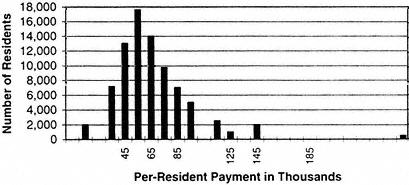
FIGURE 1. Per-resident payment distribution before Medicare share calculation. (FY 1993). Source: ProPAC, 1996b.
Stipends do not vary by anything remotely resembling a factor of 10. This variation reflects, primarily, differences in program structure and costs and idiosyncrasies of allocations from 12 years ago (Anderson, 1996; PPRC, 1993) Resident training costs may indeed vary modestly and appropriately from region to region as a result of varying costs of inputs. Nevertheless, a reasonably standard price is desirable in principle. Movement toward a standard, or average, payment should also have the practical effect of lessening the excessive incentive for institutions and regions with very high DME payment to retain increasing numbers of residents.
DME and associated teaching hospital activities seem more likely to be general, societal benefits (from a well-trained work force, for example) than part of services to individual Medicare beneficiaries. Additionally, the training programs that treat a large proportion of Medicare patients today are not necessarily the ones that produce the physicians who will take care of the most Medicare beneficiaries in the future. This argues for Medicare (and other payers) contributing a proportional share distributed evenly rather than varying by each individual institution's Medicare (or other) caseload for any particular year. A uniform Medicare payment, however, risks substantial DME redistribution; in addition to theoretical considerations, this supports the rationale for a general, non-Medicare payer(s). If such payers contribute proportionally, their payments will be inversely proportional to Medicare's. A general, non-Medicare contribution (if available) would have the same effect in leveling IME support across institutions to the benefit of facilities that have not received GME support because they had low Medicare caseloads, but nevertheless are valuable GME sites and would then be supported by payers representing proportionally the different kinds of subscribers or beneficiaries.
The committee is aware of the issues raised, and the variations in GME payment caused, by the current policies with respect to the calculation of the adjusted, average per capita cost (AAPCC) of Medicare patients in the fee-for-service system, on which Medicare's payment of per capita health plan premiums is based (COGME, 1995a,b; Mullins and Cohen, 1995). The scope of the committee's charge does not include the issues raised by these Medicare capitation calculations, except insofar as the committee expects that the problems will be mitigated by a defined GME fund and other aspects of the committee's plan. In a limited trust fund, inclusion of capitated caseload in the IME formula, as suggested later, can distribute funds to recognize service to managed care plans but cannot increase total expenditures. These issues will be described in detail later, as well as why an annually defined GME fund permits separate consideration of GME and AAPCC policy and practice.
Principle 8. Change should be gradual. Transitions should be designed that avoid funding shifts that are disruptive for the system, the trainees, and the institutions.
Budgetary pressures and plans to restructure the Medicare program may soon lead to changes in GME support. These changes may include reductions in funding for GME if training sources share in program cutbacks. Many policymakers have agreed that GME is a national asset, the quality of which is the foundation for overall health care quality. Educational quality depends on having adequately supported teachers and teaching facilities. Like all education, GME depends on consistent, stable support and having time to adapt to change. Changes made to rationalize the system, to eliminate incentives that distort public policy, and to level support variances should also recognize legitimate differences in local conditions and allow for transitions. Abrupt changes or substantial shifts in funding can have negative effects and disrupt programs.
GME payments vary greatly across institutions. Because substantial changes in payment are possible during corrections, special caution should be exercised to protect individual trainees and teaching institutions. Furthermore, given the length of medical training, longer and more gradual transitions may be warranted than were used to implement Medicare's DRG payment method, the prospective payment system (PPS), for example. In the final analysis, change that comes in response to markets, technologies, or educational practices is preferable to change that is imposed.









