5
Imaging Techniques of Body Composition: Advantages of Measurement and New Uses
Steven Heymsfield,1Robert Ross, ZiMian Wang, and David Frager
INTRODUCTION
Few technical advances in medicine can claim greater importance than the development and clinical application of computerized axial tomography (CT or CAT) and magnetic resonance imaging/spectroscopy (MRI/MRS). Both CT and MRS led to Nobel Prizes for their inventors (Bloch et al., 1946; Hounsfield, 1973; Purcell et al., 1946), and rapid related advances such as functional MRI (Duyn et al., 1994) and spiral CT (Fishman, 1994) show great promise.
The opportunities presented by both CT and MRI for studying human body composition are no less important than they are for clinical medicine. The unique capabilities provided by modern imaging methods in studying body composition make them among the most important advances of the century. This review provides an overview of the historical development and current
status of imaging methods; a final section provides suggestions for future research.
Historical Development
Students of human biology have expressed interest in body composition since the nineteenth century (Forbes, 1987; Lawes and Gilbert, 1859; von Bezold, 1857). Human shape, form, fatness, muscularity, and chemical composition were of interest to many investigators early in the twentieth century (Moulton, 1923; Spivak, 1915). Advances in radiographic methods led Stuart and colleagues (1940) to report the first use of standard x-ray films to capture fat and muscle "shadows." By the early 1960s, radiogrammetry was a well-developed method that provided investigators with estimates of subcutaneous adipose tissue (AT) layer thickness and muscle widths (Garn, 1957, 1961). Low image contrast and two-dimensional radiographs limited radiogrammetry to rough approximations of body composition components.
G. N. Hounsfield first introduced CT for brain imaging in 1971 and reported his findings in 1973. The theoretical framework and mathematical algorithms needed for image reconstruction were developed earlier by Raden (1917) and Cormack (1980). The historical roots for MRI appeared even earlier than for CT. Bloch et al. (1946) and Purcell et al. (1946) independently described the basic phenomena that ultimately gave rise to nuclear magnetic resonance spectroscopy in 1946. Differences between malignant tumors and normal tissue were first studied using magnetic resonance (MR) methods in 1971 by Damadian. That one could create images of phantoms using the signal from proton nuclear magnetic resonance was demonstrated in 1973 by Lauterber.
By the mid 1970s, CT scanners were being installed in many American medical centers, and by the early 1980s, MRI systems became available on a widespread basis. Unlike radiogrammetry, even early CT provided high-resolution cross-sectional images. Clear anatomic boundaries could be visualized between subcutaneous AT, skeletal muscle, visceral organs, brain, and skeleton. During this early era of CT technology, Heymsfield and colleagues were exploring the validity of anthropometric assessment methods as they applied to hospitalized patients. The installation of a CT scanner in the investigators' hospital provided an important opportunity to examine anthropometric assessment methods with CT as the "reference" standard. Their use of CT to quantify skeletal muscle mass was reported in 1979 (Heymsfield et al., 1979a), and subsequent reports by the group described methods of estimating visceral organ volumes (Heymsfield et al., 1979b) and visceral AT (Heymsfield and Noel, 1981).
The high radiation exposure of CT limited its use until the mid 1980s. Moreover, other methods with little or no radiation and lower cost appeared to provide adequate measures of components such as fat and fat-free body mass (Forbes, 1987; Lukaski, 1987). During this period, epidemiological studies began to appear that linked upper body AT distribution and visceral AT with obe-
sity comorbidities (Björntorp, 1986). The need arose to quantify visceral AT, and CT quickly became the method of choice (Borkan et al., 1982). In addition, Sjöström and his colleagues (1986) introduced the concept of whole-body multicomponent CT. With this method, images are prepared at 22 or more predefined anatomic locations, and total body volumes of various body composition components are estimated by integrating appropriate slice areas. This approach allows the investigator to quantify total-body and regional AT, skeletal muscle, bone, and other organ and tissue volumes.
Use of MRI in body composition research lagged behind that for CT by several years. Foster et al. (1984) were the first to demonstrate that by comparison to cadaver samples, MRI could be used to discriminate between AT and adjacent skeletal muscle. Not until 1988 was MRI first used to characterize the distribution of subcutaneous AT in human subjects (Hayes et al., 1988). Since that time, numerous studies have utilized MRI technology to describe AT and/or lean tissue distribution in adolescents (de Ridder et al., 1992), normal males and females (Fowler et al., 1991; Ross et al., 1992; Sobel et al., 1991; Sohlström et al., 1993), obese males and females (Ross et al., 1993, 1994), diabetic patients (Gray et al., 1991), and elderly populations (Baumgartner et al., 1992). The observations within many of these studies were based on a single MR image. Because multiple images can be obtained without any known health risks to the subject, MRI is well suited for assessment of whole-body AT or lean tissue distribution using multislice models. A principal benefit of multislice acquisitions is that the volume measurement of various tissues can be derived, thereby eliminating the restrictions imposed by observations based on a single image. Four research groups have employed a multislice MRI protocol to evaluate whole-body AT distribution in human subjects. Fowler et al. (1991) acquired 28 MR images over the entire body, while Ross et al. (1992, 1993) reported using a multislice (n = 41 images) model to measure AT and lean distribution in normal male and obese female subjects. Sohlström et al. (1993) recently described AT distribution in normal, healthy women using a 30-image protocol. In addition to a characterization of body composition, multislice protocols are particularly useful when evaluating the efficacy of various interventions that induce changes in AT and lean tissue distribution (Ross and Rissanen, 1994; Ross et al., 1995a; Sohlström and Forsum, 1995).
Components Measured
Body composition can be considered as five levels of increasing complexity: atomic, molecular, cellular, tissue system (anatomical), and whole body (Wang et al., 1992). The first four levels of body composition and their respective components are shown in Figure 5-1. Both CT and MRI are measurement systems designed to quantify components at the tissue-system level of body composition. The major components at the tissue-system level are AT, skeletal
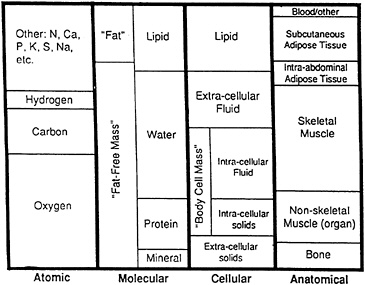
FIGURE 5-1 First four levels of body composition and their main components.
SOURCE: Baumgartner et al. (1995), used with permission.
muscle, bone, visceral organs, and brain (Figure 5-2). The AT component is further divided into subcutaneous, visceral, yellow marrow, and the interstitial AT that occurs between muscle fibers (Snyder et al., 1975).
Both CT and MRI can quantify all of the major components at the tissue-system level. Cross-sectional images are composed of picture elements or pixels, usually 1-mm squares. Slice thicknesses vary, and when considered in three dimensions, the image consists of volume elements or voxels. Each pixel or voxel has a gray scale that reflects the tissue's composition and gives contrast to the image. A later section in this chapter will expand on pixel contrast.
PHYSICAL BASIS OF METHODS
Overview
In vivo body composition methods involve measurement of some property of the human body. A simple formula that describes all in vivo body composition methods is the following (Wang et al., 1995),
(Equation 5-1)
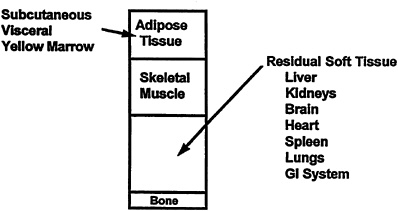
FIGURE 5-2 Main components of the tissue-system level of body composition. GI, gastrointestinal.
where C is an unknown component; Q, a measurable quantity; and f, the mathematical function that links Q to C. All in vivo methods are ultimately based on this general body composition methodology formula. The formula indicates that there are two parts to the equation that are used to estimate a body composition component. The first part is a measurable quantity, Q, and the second, a mathematical function, f. As a description of the physical basis of CT and MRI proceeds, this review is organized according to measurable quantity and mathematical function.
Computerized Axial Tomography
The basic CT system consists of an x-ray tube and receiver that rotate in a perpendicular plane to the subject. The measurable properties of CT are 0.1 to 0.2 amps, 60 to 120 kilovolt peak x rays that are attenuated as they pass through tissues (Sprawls, 1977). Attenuation is expressed as the linear attenuation coefficient or CT number. The CT number is a measure of attenuation relative to air and water. The CT numbers of air and water were defined as -1000 and 0 Housfield units (HU), respectively.
The x-ray beam attenuation is related to three factors: coherent scattering, photoelectric absorption, and Compton interactions2 (Sprawls, 1977). Physical density is the main determinant of attenuation and thus CT number. There is a linear correlation between CT number and tissue density (Heymsfield et al.,
1979c; Wang et al., 1993). Each of the image's pixels or voxels has a CT number which gives contrast to the image.
Image reconstruction is usually done with mathematical techniques based on either two-dimensional Fourier analysis or filtered back-projection, or a combination of the methods.
Magnetic Resonance Imaging
Magnetic resonance imaging is based on the interaction among nuclei of hydrogen atoms, which are abundant in all biological tissues, and the magnetic fields generated, and is controlled by the MRI system's instrumentation. Protons, the nuclei of hydrogen, have a non-zero magnetic moment that causes them to behave like small magnets. In the earth's weak magnetic field, these magnetic moments are randomly oriented and they thus tend to cancel. When a subject is placed inside the magnet of an MRI scanner, however, the field strength is typically ten thousand times stronger than that of the earth, and the proton's magnetic moments align themselves with the magnet's field. The aligned protons are then pulsed with a radio-frequency (RF), and this causes some of the protons to absorb energy and flip. When the RF field is turned off, the protons gradually return to their original positions, releasing energy in the process. Relaxation times refer to the rate at which the absorbed energy is released. The measured relaxation times are used to generate proton (i.e., hydrogen) MR images by computer.
To increase the image contrast between AT and skeletal muscle, MRI data acquisition can be programmed to take advantage of the specific proton density and relaxation times of various tissue types. This is accomplished by varying two time parameters of the RF pulse, time to repeat (TR) and time to echo (TE). By manipulating TR and TE times, one varies the RF ''pulse sequence." Using one such sequence called "spin-echo," the TR parameter can be adjusted to exploit the difference in T1 (Time 1) relaxation times of AT and muscle, which provides the tissue contrast required for high-quality MR images. With few exceptions, it is the spin-echo pulse sequence that has been selected to acquire MRI body composition data.
BODY COMPONENT RECONSTRUCTION
For both CT and MRI, there are two stages in component reconstruction. The first is to determine the amount of the specific tissue of interest in each image. The results from this stage of the analysis are usually expressed in area units (cm2). The second stage is to assemble the area results from selected slices to compute total component volume in cm3.
Computerized Axial Tomography
The cross-sectional CT image can be used to quantify the area of body composition components of interest (Chowdhury et al., 1994; Heymsfield et al., 1979a, b, c; Kvist et al., 1986; Seidell et al., 1990; Sjöström et al., 1986). There are two methods generally used to measure tissue area. The first is to trace visually the component's perimeter, and the CT scanner software then provides the component's cross-sectional area. Some technical concerns related to beam hardening3 and partial volume effects4 should be considered at this stage of the analysis (Chowdhury et al., 1994; Kvist et al., 1986).
Simple structures such as the liver and some skeletal muscles can be quantified using the tracing approach. A recent development is the automated tracing of specific tissue areas using specially designed CT software.
The validity of traced areas by CT is relatively easy to establish. For example, water-filled bottles of known diameter can be scanned and CT cross-sectional area compared to actual area. More complex structures can be created to test scan accuracy. A typical example is the construction of a mid-arm phantom from a human bone embedded in the center of a glycerol-(i.e., muscle) filled wax (i.e., fat) cylinder.
The second method also requires tracing the structure of interest. The CT scanner software can then be used to specify a pixel range for the component of interest. This approach assumes that the traced area consists of two or more components of interest. For example, the area of AT within an encircled region of skeletal muscle can be ascertained by selecting the pixels that range between -190 and -30 HU (Kvist et al., 1986; Sjöström et al., 1986). Most components have a characteristic range of pixel values that can be experimentally established (Sjöström, 1991).
This second approach is useful in separating complex structures that may include more than one tissue. For example, visceral AT is found anatomically between loops of intestine and other abdominal structures. It would be exceedingly difficult to trace visceral AT directly, thus necessitating use of the "pixel range" method. The details of quantifying tissues by CT are provided in the following references: Chowdhury et al., 1994; Heymsfield et al., 1979a, b, c; Kvist et al., 1986; Seidell et al., 1990; and Sjöström et al., 1986.
Kvist and colleagues (1988) developed improved methods of evaluating scans by taking into consideration beam hardening and partial volume effects.
These and other similar studies over the past 15 years have gradually perfected the methods of evaluating body composition by CT.
Once the amount of tissue in a specific slice is known, the total volume of the component can be calculated by compiling data from multiple slices. This is usually done using the formula suggested by Sjöström et al. (1986),
(Equation 5-2)
where C is the component of interest (kg) measured by CT or MRI; d, the assumed constant density (kg/cm3) of the component; Ai, the distance (cm) between scans; and Bi and Ci, the component's area (cm2) in adjacent scans. Other formulae are known, and additional discussion of this topic is presented in the next section.
Magnetic Resonance Imaging
To quantify the area of various tissues in a given image, MRI data are analyzed in a manner similar to that described for CT. Unfortunately, the quantification of MRI data is not as straightforward as it is for CT. Unlike CT where pixel values consistently represent specific tissues regardless of slice position or the individual being assessed, MRI pixel values for a given tissue (i.e., the emitted RF signal of the protons within a pixel) may vary from slice to slice or between individuals. This is because pixel values in MR images are dependent on excitation pulse sequences and a combination of proton density and tissue relaxation values, and these determinants may vary among individuals. Another more important cause of pixel variation is the variation in signal intensities that may occur for the same tissue within a set of images (i.e., seven images acquired at the same time). This variation may arise as a result of heterogeneities in the magnetic field or from other system imperfections.
Recent improvements to both MRI hardware and computer software have reduced artifacts and substantially improved the quality of MR images. However, artifacts still occur, and it is therefore useful to quantify a given tissue with image analysis software that permits visual verification of the results. In other words, the researcher must be able to correct manually for the tissue areas that are not counted by the initial pixel threshold selection. Although these procedures can be accomplished using straightforward image analysis techniques, they add a degree of subjectivity to the quantification of tissues on an MR image that is not usually required when quantifying a given tissue using CT.
The quantification of tissue areas on MR images thus cannot be accomplished by simply identifying the appropriate threshold and asking the software to count the pixels above or below that threshold. Until such time that MRI ac-
quisition procedures improve, manual correction of MR component analyses is required. The reliability of these procedures is discussed later in this review.
The volume (cm3) of a tissue for the whole body or a given region (i.e., legs, arms, etc.) is derived in two steps. First, the volume for each image is determined by multiplying the area (cm2) of the tissue by the slice thickness. Whole-body or regional volume is then calculated using a mathematical algorithm similar to the one described earlier for CT.
VALIDATION STUDIES
Validation of both CT and MRI as body composition measurement systems can be organized into studies that establish the accuracy of a selected area or volume and those that examine the accuracy of whole-body component estimates. Validation experiments can be carried out in phantoms, animals, or humans. The following sections provide examples of previous CT and MRI validation studies in an effort to give an overall analysis of the various potential methods and to summarize the current relevant literature.
Computerized Axial Tomography
Phantoms and Cadavers
A number of studies have validated the accuracy of area and volume measurements by CT in systems ranging from water-filled balloons to in situ cadaver organs. As an example of a validation study, Heymsfield et al. (1979b) examined the accuracy of liver, kidney, and spleen volume and mass measurements by CT. The study was carried out in 4 water-filled balloons; in 12 excised human cadaver organs, including 6 kidneys, 3 livers, and 3 spleens; and in 2 human cadavers while the organs remained in situ. Reproducibility was determined in the first experiment by independent balloon weighing and calculation of CT mass. The coefficient of variation (CV) for weighing the balloon and for estimating CT mass was 1.6 percent and 3.9 percent, respectively. The absolute mean difference between the two methods was 2.6 percent. In the second experiment, the CV for weighing the organs and for estimating organ mass by CT was ±3 percent and ±5 percent, respectively. The mean absolute difference between the two methods was 4.6 percent. In the third experiment, the CV for weighing organs and for estimating organ mass by CT was ±3 percent and ±5 percent, respectively. The mean absolute difference between the two methods was ±5.6 percent. Thus in this study, CT volume and mass agreed with actual volume and mass within ±3 percent to 5 percent.
In a related experiment, Rossner and colleagues (1990) compared AT determinations by CT to those obtained by planimetry of 21 band-sawed slices of the corresponding sections from 2 male cadavers. Linear regression analyses
indicated good agreement between CT-measured and cadaver AT areas and ratios (r values ranged from 0.77–0.94). The authors suggest that the excellent agreement between CT and cadaver AT measurements indicates that CT can be used as a body composition reference method.
Verification of Volume Measurements In Vivo
A simple method of evaluating the overall accuracy of total body CT scans is to compare CT-derived total-body volume to the subject's actual body volume. In one approach, Chowdhury and colleagues (1994) determined the volume of body subcompartments in eight males. A density was assigned to each compartment based on literature values, and compartment mass was then calculated from compartment volume. The mass of all compartments was then summed, and this was compared to actual body weight. The average of the difference between the two measures of body weight was 0.024 ± 0.65 kg, and the error calculated from the squared differences was 0.85 percent of body weight.
Wang and colleagues (1996) compared body volume calculated from 22 CT slices to body volume measured with a combination of underwater weighing and residual lung volume analysis. Whole-body volume derived by CT was highly correlated with body volume measured by underwater weighing (r = 0.990, p = 0.0001, standard error of estimate [SEE] = 1.9 liters, n = 17). The mean body volume measured by CT (74.8 ± 13.9 liters) agreed closely with mean body volume measured by underwater weighing (73.6 ± 13.7 liters), although there was a significant difference between the two results (p = 0.02). The slightly higher body volume estimate by CT was thought secondary to inclusion of trapped respiratory air, which is not included in the body volume estimate by underwater weighing.
Reproducibility
Some reproducibility studies for CT were mentioned earlier. In another study, Kvist et al. (1986) examined each of four subjects twice by CT. A total AT volume error of 0.6 percent was observed. Chowdhury et al. (1994) examined intraobserver "interpretation errors" in four subjects for a large number of CT-measured body composition components. Some examples are for skin, 2.4 percent; total AT, 0.4 percent; and heart, 3.4 percent. An earlier report by the research team (Brummer et al., 1993) indicated interobserver errors of 0.7 percent, 0.4 percent, and 2.1 percent for total AT, skeletal muscle, and visceral organs, respectively.
CT body composition analysis appears to be accurate and reproducible, although there is still a lack of careful human cadaver validation studies in samples of adequate size.
Magnetic Resonance Imaging
Phantoms
Few attempts have been made to validate MRI using phantoms. Ross et al. (1991) verified the surface area calculation of reconstructed images using two polyvinyl chloride tubes 38.1 cm long and 1.78 cm in diameter, filled to capacity with peanut oil and positioned on either side of rats during data acquisition. The mean cross-sectional area (cm2) of the tubes was computed from a set of 12 transverse images and compared with the actual area. The mean area of the tubes obtained from image reconstruction was 2.47 cm2, which differed from the actual value of 2.48 cm2 by only 0.6 percent. The percent error ranged from 0.1 to 1.5 percent.
A comparison of MRI-measured whole-body volume with that obtained by underwater weighing was made in 14 women (Ross et al., 1995b). Good agreement between the methods was observed, as the correlation coefficient obtained was 0.99 (p < 0.001); the associated SEE was 1.5 liters or 1.8 percent.
Animals
Validation of MRI using animal models has been performed by two groups (Fowler et al., 1992; Ross et al., 1991). Using a rat model, Ross et al. (1991) reported a high correlation between chemically extracted carcass lipid and MRI-AT mass (r = 0.97, p < 0.01; SEE = 10.5%). Fowler et al. (1992) compared MRI-AT measurements with those obtained by dissection in a group of lean and obese pigs. The authors observed that the distribution of AT measured by MRI correlated strongly with AT distribution estimated by weighing dissected regional tissue samples (r = 0.98, mean square error [MSE] = 2.1%).
Cadavers
Engstrom et al. (1991) compared the cross-sectional area measurements of skeletal muscle determined from the proximal thigh in cadavers with corresponding MRI-measured cross-sectional areas and reported a correlation coefficient between the two that approached unity ( r = 0.99, p < 0.001). Compelling evidence regarding the accuracy of MRI-AT measurements was reported by Abate et al. (1994), who compared MRI measures of abdominal subcutaneous and visceral AT in three cadavers with that obtained by direct weighing of the same AT compartments after dissection. In this study, the authors subdivided visceral AT into intraperitoneal and retroperitoneal depots. The mean difference between the two methods for the various compartments was 0.076 kg ( ~6%).
Comparison with CT
Attempts to validate MRI have been made by comparing MRI measurements of AT with those obtained by CT using both animal and human models (Table 5-1). Evaluation of the relationships between the two methods in humans generally has been performed by comparing measurements of subcutaneous AT and visceral AT area values obtained from a single abdominal image. The data presented in Table 5-1 reveal that, in general, the correlations obtained between MRI and CT for subcutaneous AT are quite high. Furthermore, given that measurements of the extremities are unaffected by the motion artifacts, it is likely that the CV between MRI-and CT-subcutaneous AT in the leg and arm regions is substantially less than the 5 to 12 percent reported for the abdomen region.
Although the difference between the two imaging modalities for subcutaneous AT is generally low, the CV for visceral AT is higher, ranging from 13 to 20 percent (Table 5-1). It has also been observed that the relationship between MRI-and CT-visceral AT improves with increasing visceral adiposity (Seidell et al., 1990). This may be explained by the increased signal to noise (i.e., from motion artifacts) ratio that results with increasing quantities of visceral AT. The ability of MRI to predict CT-visceral AT in lean subjects is likely poor, due to the low signal to noise ratio. Unfortunately, no data are available that would indicate the MRI-visceral AT area value (cm2) below which substantial differences occur between MRI-and CT-visceral AT. Once again, the use of Fast Imaging protocols that avoid the problems associated with motion artifacts may enhance tissue contrast and improve the ability of MRI to measure visceral AT in lean subjects.
In summary, by comparison with limited cadaver and animal dissection data, it would appear that MRI measures total AT with a SEE in the range of 2 to 10 percent. Comparison with CT suggests that MRI provides images of the abdomen with similar anatomic detail and CVs for subcutaneous AT and visceral AT of about 5 percent and 15 percent, respectively.
Reliability
Adipose Tissue. Several studies have evaluated whether MRI measurements of subcutaneous AT and visceral AT are reproducible. The results presented in Table 5-2 show that for a single MR image in the abdominal region, the CV for repeated measures of subcutaneous AT ranges from 1 to 10 percent. For visceral AT, the CV for repeated measurements ranges from 6 to 11 percent. Taken together, these data suggest that when using MRI, the expected error for measurement of subcutaneous and visceral AT area is approximately 10 percent.
Unfortunately, there is little evidence regarding the reliability of MRI-measured lean tissue. Ross et al. (1994) recently reported that for a single MR image obtained at the level of the proximal thigh, the CV for repeated measurements of lean tissue (skeletal muscle and bone) was 1.2 percent. In addition,
TABLE 5-1 MRI Validation Studies
TABLE 5-2 MRI Reliability Studies*
|
|
|
|
|
|
Coefficient of Variation (%) |
|||
|
Reference |
Subject (N) |
T |
MRI Sequence |
Anatomical Position |
Subcut. AT |
Visceral AT |
Total AT |
LT |
|
Staten et al., 1989 |
Human (6) |
0.5 |
SE |
Mid-abdomen |
5.0 |
10.0 |
3.0 |
— |
|
Seidell et al., 1990 |
Human (7) |
1.5 |
IR |
Umbilicus |
10.1 |
10.6 |
5.4 |
— |
|
Garard et al., 1991 |
Human (4) |
1.5 |
SE |
6 abdomen images |
3.0 |
9.0 |
— |
— |
|
Ross et al., 1991 |
Rat (11) |
1.5 |
SE |
Whole body |
— |
— |
4.3 |
— |
|
Ross et al., 1993 |
Human (3) |
1.5 |
SE |
L4-L5 |
1.1 |
5.5 |
— |
— |
|
|
|
|
|
Whole body |
— |
— |
2.5 |
— |
|
Sohlström et al., 1993 |
Human (3) |
0.02 |
SR |
Whole body |
1.7 |
5.3* |
1.5 |
— |
|
Ross et al., 1994 |
Human (11) |
1.5 |
SE |
Proximal thigh |
— |
— |
— |
1.2 |
|
Abate et al., 1994 |
Cadaver (3) |
0.35 |
SE |
Abdomen |
2.2 |
6.0 |
— |
— |
|
Ross et al., 1995a |
Human (19) |
1.5 |
SE |
L4-L5 |
— |
— |
— |
1.0 |
|
NOTE: MRI, magnetic resonance imaging; T, strength of magnet in Teslas; AT, adipose tissue; LT, lean tissue; SE, spin-echo; IR, inverse recovery; SR, saturation recovery; L4-L5, lumbar vertebrae 4–5. * Reported as nonsubcutaneous adipose tissue. |
||||||||
the authors reported that for lean tissue volume in the leg, derived using 15 images, the CV was 3.9 percent. Although the issue of measurement reliability requires further investigation, these preliminary results are encouraging.
ADVANTAGES AND DISADVANTAGES
Early use of radiogrammetry with conventional x-ray systems was limited by poor image contrast and the availability of only two-dimensional images. Both CT and MRI offer the important opportunity for three-dimensional tissue volume quantification. Image contrast is sharp, and tissue boundaries are relatively clear. Competing technologies, such as ultrasound, cannot delineate tissue interfaces with the same level of accuracy as CT and MRI. No other currently available methods can assess body composition components at the tissue-system level with the same level of accuracy as CT and MRI.
A second major advantage of both CT and MRI is the capability of carrying out cross-sectional imaging. Conventional two-dimensional radiography cannot ascertain the area or volume of structures inside the body cavities. Visceral AT, brain, and heart volumes can all be quantified with CT and MRI. No other current body composition methods can accurately quantify visceral AT.
A third important aspect of CT and MRI is the capability of making regional and whole-body measurements. Ultrasound, which is also capable of estimating tissue-system level components, at present can only provide regional measurements.
A fourth important feature of CT and MRI is the availability of measurement systems. Almost every major medical research center in the United States has both a CT and MRI scanner that is capable of body composition analysis. Many systems are also available in developing countries.
With respect to body composition measurement, MRI offers an advantage over CT in not exposing subjects to ionizing radiation. Multiple MR images can therefore be obtained without known risk to the subject.
Magnetic resonance imaging has the potential to provide criterion data for the development of prediction equations on diverse subject populations. Examples are anthropometric prediction equations for visceral AT and whole-body skeletal muscle mass in which MRI-derived components serve as the reference component estimate.
The lack of radiation exposure with MRI also makes it suitable for longitudinal and intervention studies wherein multiple and/or serial measurements are required.
A disadvantage of some MRI systems is that the small bore magnet precludes study of claustrophobic and very overweight subjects. Open magnet MRI systems are available but are not in widespread use. The magnetic field generated with MRI also restricts study of patients with implanted metal objects.
Another disadvantage of MRI is that motion artifacts can affect tissue contrast in the abdominal region. Although improvements in MRI technology now permit the acquisition of multiple transverse images in a breath hold (i.e., ~20 seconds) (Ross et al., 1995a), reliable determination of AT in the abdominal region can be a problem (Seidell et al., 1990). A related disadvantage is that, due to the subjectivity associated with the determination of tissue areas on MR images, the time required to analyze MR images can be lengthy. The analysis of MRI data using specially designed software on computer workstations improves data analysis capabilities (Ross et al., 1992).
REFERENCE TECHNIQUE FOR HUMAN FAT MEASUREMENT?
Whether MRI or CT might serve as calibration techniques for other methods of body composition assessment is a question of considerable interest. In order to determine body fat by MRI or CT, two key issues must be resolved.
The first issue relates to the conversion AT volume of lipid or fat mass. Lipid is the total lipid solvent-extractable material from tissue. Fat in the current context is nonessential lipid, mainly triglycerides.
Adipose tissue is a body composition component at the tissue-system level, and total lipids and fat are components at the molecular level (Figure 5-1). Two steps are needed to convert AT volume to fat mass: AT volume conversion to AT mass, and AT mass conversion to fat mass. These conversions require knowledge of AT density and fat fraction: AT fat mass = measured AT volume × assumed AT density × assumed AT fat fraction. It has been shown that the normal physiological range for AT density and AT fat fraction is 0.91 to 0.98 g/ml and 0.5 to 0.9, respectively (Martin et al., 1994). Thus the conversion of AT volume to AT fat mass requires a factor that varies over the range of their product, approximately 0.5 to 0.8 g/ml. This variation is considerable and cannot be ignored; successful conversion of AT volume to fat mass requires a good estimate of this factor, which is valid across populations that differ widely in age, gender, and adiposity.
Although there are currently no in vivo methods for estimating either AT density or its fat fraction, it has been shown that these values are closely related to the degree of adiposity. The highest AT densities and fat fractions are observed in the leanest individuals, and the lowest AT densities and fat fractions are observed in the fattest individuals (Martin et al., 1994). Preliminary data in older men suggest that it may be possible to estimate AT fat fraction from overall adiposity, although this observation remains unconfirmed (Martin et al., 1994).
A second source of error when using CT or MRI to estimate total body fat is that once total body AT fat has been estimated, total body lipid is obtained by adding nontriglyceride lipids, a quantity that is variable and difficult to estimate.
Taken together, these observations suggest that the error inherent in the conversion of CT-and MRI-AT volumes to lipid mass precludes their use as a
current reference measure of total body lipid. However, it is important to note that most clinical interest centers on total body fat, and thus this second source of error may not be of primary concern. It should be possible to estimate only total body fat from MRI or CT once the conversion factor(s) for AT volume to AT-fat mass are known.
FUTURE APPLICATIONS
There are many potential future areas of CT and MRI research, and only a few relevant topics are mentioned here.
Spiral (helical) imaging methods represent an important advance in CT technology (Fishman, 1994). Spiral CT was developed to help overcome technical problems with CT, such as patient movement and respiration during a single CT slice. The method allows rapid three-dimensional scanning of a large body segment or even the whole body. Although this capability is valuable in clinical radiographic studies, particularly with contrast agents, the possibility also exists that spiral CT can be used to reconstruct body composition components. It may be feasible to reduce radiation dosages with spiral CT as high image contrast is not needed in body composition research, as it is in clinical studies.
The eventual linkage of MRI and MRS systems will allow study of metabolic processes in vivo. There is already considerable research in this area, although access to large-bore magnets that can carry out both MRI and MRS is still limited. Magnets with high field strengths (up to 5 Teslas) are now either available for human studies or under construction. Imaging and spectroscopy can be carried out on these MR systems for protons (1H), phosphorous (31P), sodium (23Na), carbon (13C), and potentially other elements as well. The availability of combined MRI and MRS systems will allow for a union of body composition and metabolism studies.
Functional MR is an important development in the study of tissue metabolism, particularly of the brain (Duyn et al., 1994). As with MRS, metabolic processes can be evaluated in specific body composition components.
Another important area of future research involves MRI technical developments. What are the potential uses of coronal and saggital MR images in body composition studies? Spin-echo imaging is the traditional scanning sequence of choice for MRI-body composition studies (Table 5-2). This is due primarily to its inherent tissue contrast properties, robust signal strength, and relative insensitivity to artifacts that affect other MR sequences. The principal drawback of spin-echo is the time required for many of the preferred scanning routines. Recent developments in MR technology, however, have addressed this problem. Fast spin-echo pulse sequences can reduce conventional spin-echo by a factor of as much as 16 while maintaining excellent tissue contrast (Mansfield, 1977). Recent developments in Echo Planar Imaging (EPI) promise even greater reduction in the time required to obtain multiple images, as ''snapshot" EPI boasts
20 to 100 µs acquisition rates (10 to 50 images per second) (Jolesz, 1992). At these rates, it would appear that MR applications in body composition measurement hold great promise for the future.
A final important research area is the use of both CT and MRI as reference standards against which useful and practical body composition methods can be developed. The uses of CT and MRI were mentioned earlier as measures of total body lipid and fat. Both CT and MRI may also be useful as reference standards for skeletal muscle, visceral AT, and other components. MRI has the advantage in this area over CT in that it poses no subject risk and thus populations, including children and young women, can be evaluated with little or no concern.
Some early work in this area has already been carried out by a number of investigators. For example, Sjöström (1991) used multislice CT as a reference method for estimating total body AT. The subjects were 19 women and 24 men whose weight ranged from approximately 70 to 130 kg for the women and 73 to 140 kg for the men. Anthropometric prediction equations were developed. Ross et al. (1992, 1994) similarly used MRI-measured visceral AT to develop anthropometric prediction equations.
AUTHORS' CONCLUSIONS
There are many important areas of potential future research that apply CT and MRI, not only in technology development, but also in the application of both imaging methods to the study of biological factors that influence human body composition. Advances in related technologies, such as MR spectroscopy, will also help bridge the gap between static body composition measurements and evaluation of dynamic metabolic and biochemical processes. Taken collectively, these capabilities of CT and MRI will undoubtedly allow both methods to play a central role in future body composition research efforts.
REFERENCES
Abate, N., D. Burns, R.M. Peshock, A. Garg, and S.M. Grundy 1994 Estimation of adipose tissue mass by magnetic resonance imaging: Validation against dissection in human cadavers. J. Lipid Res. 35:1490–1496.
Baumgartner, R.N., R.L. Rhyne, C. Troup, S. Wayne, and P.J. Garry 1992 Appendicular skeletal muscle areas assessed by magnetic resonance imaging in older persons. J. Gerontol. 47:M67–72.
Baumgartner, R.N., S.B. Heymsfield, and A.F. Roche 1995 Human body composition and the epidemiology of chronic disease. Obes. Res. 3:73–95.
Björntorp, P. 1986 Adipose tissue distribution and morbidity. Pp. 60–65 in Recent Advances in Obesity Research, V.E.M. Berry, S.H. Blundheim, H.E. Eliahou, and E. Shafrir, eds. London: John Libby.
Bloch, F., W.W. Hansen, and M.E. Packard 1946 Nuclear introduction. Phys. Rev. 70:460–474.
Borkan, G.A., S.G. Gerzof, A.H. Robbins, D.E. Hults, C.K. Silbert, and J.E. Silbert 1982 Assessment of abdominal fat content by computerized tomography. Am. J. Clin. Nutr. 36:172–177.
Brummer, R.J.M., L. Lonn, U.L. Grangard, B.A. Bengtsson, H. Kvist, and L. Sjöström 1993 Adipose tissue and muscle volume determinations by computed tomography in acromegaly, before and one year after adenectomy. Eur. J. Clin. Invest. 23:199–205.
Chowdhury, B., L. Sjöström, M. Alpsten, J. Kostanty, H. Kvist, and R. Löfgren 1994 A multicompartment body composition technique based on computerized tomography. Int. J. Obes. 18:219–234.
Cormack, M.M. 1980 Early two-dimensional reconstruction and recent topics stemming from it. Med. Phys. 7:277–281.
Damadian, R. 1971 Tumor detection by nuclear magnetic resonance. Science 171:1151–1153.
de Ridder, C.M., R.M. de Boer, J.C. Seidell, C.M. Nieuwenhoff, J.A.L. Jeneson, C.J.G. Bakker, M.L. Zonderland, and W.B.M. Erich 1992 Body fat distribution in pubertal girls quantified by magnetic resonance imaging. Int. J. Obes. 16:443–449.
Duyn, J.H., V.S. Mattay, R.H. Sexton, G.S. Sobering, F.A. Barrios, G. Liu, J.A. Frank, D.R. Weinberger, and C.T. Moonen 1994 Three-dimensional functional imaging of human brain using echo-shifted FLASH MRI. Magn. Reson. Med. 32:150.
Engstrom, C.M., G.E. Loeb, J.R. Reid, W.J. Forrest, and L. Avruch 1991 Morphometry of the human thigh muscles. A comparison between anatomical sections and computer tomographic and magnetic resonance images. J. Anat. 176:139–156.
Fishman, E.K. 1994 Spiral imaging methods assure survival of CT. Diagn. Imaging. (November): 59–67.
Forbes, G.B. 1987 Human Body Composition. Growth, Aging, Nutrition and Activity. New York : Springer-Verlag.
Foster, M.A., J.M.S. Hutchison, J.R. Mallard, and M. Fuller 1984 Nuclear magnetic resonance pulse sequence and discrimination of high-and lowfat tissues. Magn. Reson. Imaging 2:187–192.
Fowler, P.A., M.F. Fuller, C.A. Glasby, M.A. Foster, G.G. Cameron, G. McNeill, and R.J. Maughan 1991 Total and subcutaneous AT distribution in women: The measurement of distribution and accurate prediction of quantity by using magnetic resonance imaging. Am. J. Clin. Nutr. 54:18–25.
Fowler, P.A., M.F. Fuller, C.A. Glasbey, G.G. Cameron, and M.A. Foster 1992 Validation of the in vivo measurement of adipose tissue by magnetic resonance imaging of lean and obese pigs. Am. J. Clin. Nutr. 56:7–13.
Garard, E.L., R.C. Snow, D.N. Kennedy, R.E. Frisch, A.R. Guimaraes, R.L. Barbieri, A.G. Sorenson, T.K. Egglin, and B.R. Rosen 1991 Overall body fat and regional fat distribution in young women: Quantification with MR imaging. Am. J. Radiol. 157:97–104.
Garn, S.M. 1957 Roentgenogrammetric determination of body composition. Hum. Biol. 29:337.
1961 Radiographic analysis of body composition. Pp. 36–58 in Techniques for Measuring Body Composition, Proceedings of a Conference, Quartermaster Research and Engineering Center, Natick, Mass., January 22–23, 1959, J. Broézek and A. Henschel, eds. Washington, D.C.: National Academy of Sciences/National Research Council.
Gray, D., K. Fujioka, P.M. Colletti, H. Kim, W. Devine, T. Cuyegkeng, and T. Pappas 1991 Magnetic-resonance imaging used for determining fat distribution in obesity and diabetes. Am. J. Clin. Nutr. 54:623–627.
Hayes, P.A., P.J. Sowood, A. Belyavin, J.B. Cohen, and F.W. Smith 1988 Subcutaneous fat thickness measured by magnetic resonance imaging, ultrasound, and calipers. Med. Sci. Sports Exerc. 20:303–309.
Heymsfield, S.B., and R. Noel 1981 Radiographic analysis of body composition by computerized axial tomography. Nutr. Cancer 17:161–172.
Heymsfield, S.B., R.P. Olafson, M.H. Kutner, and D.W. Nixon 1979a A radiographic method of quantifying protein-calorie undernutrition. Am. J. Clin. Nutr. 32:693–702.
Heymsfield, S.B., T. Fulenwider, B. Nordlinger, R. Balow, P. Sones, and M. Kutner 1979b Accurate measurement of liver, kidney, and spleen volume and mass by computerized axial tomography. Ann. Intern. Med. 90:185–187.
Heymsfied, S.B., R. Noel, M. Lynn, and M. Kutner 1979c Accuracy of soft tissue density predicted by CT. J. Comput. Assist. Tomogr. 3:859–860.
Hounsfield, G.N. 1973 Computerized transverse axial scanning (tomography). Br. J. Radiol. 46:1016.
Jolesz, F.A. 1992 Fast spin-echo technique extends versatility of MR. Diagn. Imaging 14:78.
Kvist, H., L. Sjöström, and U. Tylén 1986 Adipose tissue volume determinations in women by computed tomography: Technical consideration. Int. J. Obes. 10: 53–67.
Kvist, H., B. Chowdhury, L. Sjöström, U. Tyler, and Å. Cederblad 1988 Adipose tissue volume determination in males by computed tomography and 40K. Int. J. Obes. 12:249–266.
Lauterber, P.C. 1973 Image formation by induced local interactions: Examples employing nuclear magnetic resonance. Nature 242:190–191.
Lawes, J.B., and J.H. Gilbert 1859 Experimental inquiry into the composition of some of the animals fed and slaughtered as human food. Philos. Trans. R. Soc. London 149:493–680.
Lukaski, H.C. 1987 Methods for the assessment of human body composition: Traditional and new. Am. J. Clin. Nutr. 46:537–556.
Mansfield, P. 1977 Multi-planar image formation using NMR spin-echoes. J. Phys. Chem. 10:L55.
Martin, A.D., M.Z. Daniel, D. Drinkwater, and J.P. Clarys 1994 Adipose tissue density estimated adipose lipid fraction and whole body adiposity in male cadavers. Int. J. Obes. 18:79–83.
Moulton, C.R. 1923 Age and chemical development in mammals. J. Biol. Chem. 57:79–97.
Purcell, E.M., H.C. Torrey, and R.V. Pound 1946 Resonance absorption by nuclear magnetic moments in a solid. Phys. Rev. 69:37–38.
Raden, J. 1917 On the determination of functions from their integrals along certain mainfolds. Math. Phys. Klasse. 69:262–277.
Ross, R., and J. Rissanen 1994 Mobilization of visceral and subcutaneous adipose tissue in response to caloric restriction and exercise. Am. J. Clin. Nutr. 60:695–703.
Ross, R., L. Léger, R. Guardo, J. de Guise, and B.G. Pike 1991 Adipose tissue volume measured by magnetic resonance imaging and computerized tomography in rats. J. Appl. Physiol. 70(5):2164–2172.
Ross, R., L. Léger, D. Morris, J. de Guise, and R. Guardo 1992 Quantification of adipose tissue by MRI: Relationship with anthropometric variables. J. Appl. Physiol. 72:787–795.
Ross, R., K.D. Shaw, Y. Martel, J. de Guise, and L. Avruch 1993 Adipose tissue distribution measured by magnetic resonance imaging in obese women. Am. J. Clin. Nutr. 57:470–475.
Ross, R., K.D. Shaw, J. Rissanen, Y. Martel, J. de Guise, and L. Avruch 1994 Sex differences in lean and adipose tissue distribution by magnetic resonance imaging: Anthropometric relationships. Am. J. Clin. Nutr. 59:1277–1285.
Ross, R., H. Pedwell, and J. Rissanen 1995a Effects of energy restriction and exercise on skeletal muscle and adipose tissue in women as measured by magnetic resonance imaging. Am. J. Clin. Nutr. 61:1179–1185.
1995b Response of total and regional lean tissue and skeletal muscle to a program of energy restriction and resistance exercise. Int. J. Obes. 19(11):781–787.
Rossner, S., W.J. Bo, E. Hiltbrandt, W. Hinson, N. Karstaedt, P. Santago, W.T. Sobol, and J.R. Crouse 1990 Adipose tissue determinations in cadavers—a comparison between cross-sectional planimetry and computed tomography. Int. J. Obes. 14:893–902.
Seidell, J.C., C.J.C. Bakker, and K. van der Kooy 1990 Imaging techniques for measuring adipose-tissue distribution—a comparison between computed tomography and 1.5-T magnetic resonance . Am. J. Clin. Nutr. 51:953–957.
Sjöström, L. 1991 A computer-tomography based multicompartment body composition techniques and anthropometric predictions of lean body mass, total and subcutaneous adipose tissue. Int. J. Obes. 15(suppl. 2):19–30.
Sjöström, L., H. Kvist, A. Cederblad, and U. Tylen 1986 Determination of total adipose tissue and body fat in women by computed tomography, 40K, and tritium. Am. J. Physiol. 250:E736–E745.
Snyder, W.S., M.J. Cook, E.S. Nasset, L.R. Karhansen, G.P. Howells, and I.H. Tipton 1975 Report of the Task Group on Reference Man. Oxford: Pergamon Press.
Sobel, W., S. Rossner, B. Hinson, E. Hiltbrandt, N. Karstaedt, P. Santago, N. Wolfman, A. Hagaman, and J.R. Crouse, III 1991 Evaluation of a new magnetic resonance imaging method for quantitating adipose tissue areas. Int. J. Obes. 15:589–599.
Sohlström, A., and E. Forsum 1995 Changes in adipose tissue volume and distribution during reproduction in Swedish women as assessed by magnetic resonance imaging . Am. J. Clin. Nutr. 61:287–295.
Sohlström, A., L-O. Wahlund, and E. Forsum 1993 Adipose tissue distribution as assessed by magnetic resonance imaging and total body fat by magnetic resonance imaging, underwater weighing, and body-water dilution in healthy women. Am. J. Clin. Nutr. 58:830–838.
Spivak, C.D. 1915 The specific gravity of the human body. Arch. Internal Med. 15:628–642.
Sprawls, P. 1977 The Physical Principles of Diagnostic Radiology. Baltimore, Md.: University Park Press.
Staten, M.A., W.G. Totty, and W.M. Kohrt 1989 Measurement of fat distribution by magnetic resonance imaging. Invest. Radiol. 24:345–349.
Stuart H.C., P. Hill, and C. Shaw 1940 The growth of bone, muscle and overlying tissue as revealed by studies of roentgenograms of the leg area. Monogr. Soc. Res. Child Dev. 5 (no. 3, serial no. 26):1–190.
von Bezold, A. 1857 Untersuchungen uber die vertheilung von Wasser, organischer Materie und anorganischen Verbindungen im Thierreiche. Z. Wissenschaftlische Zoologie, 8:487–524.
Wang, Z.M., R.N. Pierson, Jr., and S.B. Heymsfield 1992 The five-level model: A new approach to organizing body-composition research. Am. J. Clin. Nutr. 56: 19–28.
Wang Z.M., S. Heshka, and S.B. Heymsfield 1993 Application of computerized axial tomography in the study of body composition: Evaluation of lipid, water, protein, and mineral in healthy men. Pp. 343–344 in Human Body Composition: In Vivo Methods, Models, and Assessment, K.J. Ellis and J.D. Eastman, eds. New York: Plenum Press.
Wang, Z.M., S. Heshka, R.N. Pierson, Jr., and S.B. Heymsfield 1995 Systematic organization of body composition methodology: Overview with emphasis on component-based methods. Am. J. Clin. Nutr. 61: 457–465.
Wang, Z.M., M. Visser, R. Ma, R.N. Baumgartner, D. Kotler, D. Gallagher, and S.B. Heymsfield 1996 Skeletal muscle mass: Evaluation of neutron activation and dual-energy x-ray absorptiometry methods. J. Appl. Physiol. 80:824–831.
DISCUSSION
WENDY KOHRT: In the MRI procedure, besides the slice-to-slice variability in pixel intensity, isn't there also within-slice variability in pixel intensity?
STEVEN HEYMSFIELD: Yes, there is, and that is a problem. I am only now getting involved with MRI myself for the first time, but I find there is a certain amount of subjectivity involved in, for example, measuring visceral adipose tissue or subcutaneous adipose tissue and so on. We need very good reconstruc-
tion programs that people have developed to make these measurements, but there is subjectivity involved.
One first specifies, say, a certain range of relaxation times in subcutaneous adipose tissue. That might appear on the screen as different colors, but then you see there is a big blotch that has not been included, and then one has to, by hand, incorporate that into the area measurement.
WENDY KOHRT: Yes, since the area you know is fat does not necessarily always appear to be fat when you set a threshold.
STEVEN HEYMSFIELD: That is exactly right. It is a cause of concern, but the comparisons between CT and MRI, and a number of these have been done, are reasonably good.
DONALD McCORMICK: How far off are we from being able to use other nuclei?
STEVEN HEYMSFIELD: I think we are going to hear more. Gerry Shulman is going to talk about 13C, I am sure, but there is a great proliferation of high field-strength magnets now. For example, I know at Columbia we have a 5 Tesla, and I heard that there is at Emory a 5 Tesla as well.
My understanding is that with those higher field-strengths magnets, you can do nuclei such as 23Na, is that correct? So that, then, opens another whole set of interesting, not only physiological measurements, but body composition as well.
DOUGLAS WILMORE: Let me just mention for the group that the place that this really has economic value is for detection of animal composition. If you go to Europe, there are large research facilities in veterinary schools where you can vary food intake or feeding intake for large animals, such as goats and sheep and the like, and scan the animal and look at how much meat you are going to produce or how much fat will be on the meat and the like. That is technology that is growing and evolving and impacting everything in the veterinary schools in a real way.
WM. CAMERON CHUMLEA: Do the high-Tesla magnets have the problem of bore size? I mean the open magnets, as I understand it, are the low Tesla, and so basically we still cannot really get the people who need it most into the machine?
























