7
Children's Health Care Needs
Most American children—approximately 70 percent, or about 50 million children—are generally healthy. To help them stay healthy, these children need age-appropriate immunizations, regular preventive care, and professional treatment for acute illnesses and injuries (Ireys et al., 1997; Lozano et al., 1997; Neff and Anderson, 1995; Newacheck and Taylor, 1992). The expenditures for healthy children using the health care services, outlined above, account for about 10 percent of the total childhood medical expenditures (Neff and Anderson, 1995) (see Table 7.1).
Twenty percent of American children—about 14 million children—have mild to moderate chronic problems such as persistent ear infections, respiratory allergies, asthma, eczema and skin allergies, and speech defects (Neff and Anderson, 1995). These conditions may place significant limitations on their ability to function effectively in school and at home. Children with these chronic conditions require more frequent visits to primary care physicians, are more likely to visit emergency rooms, are more likely to need care from specialists, have greater needs for medications, and may also need hospitalization during acute episodes. Their expenses, on average, are two to three times higher than those for the average healthy child.
Another 10 percent—about 7 million children—have one or more severe chronic conditions, such as congenital heart defects, neural tube defects, juvenile diabetes mellitus, sickle cell disease, or HIV infections. Expenditures for this group account for 70 to 80 percent of all medical expenditures for children (Neff and Anderson, 1995).
Some of these children require high expenditures, primarily early in life (e.g., for surgical procedures). Others with severe medical conditions may require lifelong, intensive case management or enhanced medical care from primary care practitioners; regular consultations with pediatric subspecialists; and services from allied health professionals to maintain or to improve their functioning. They may require long-term medications or special equipment and supplies for home care. On average, the cost of care for this group of chronically ill children is five to six times higher than costs for the average healthy child (Neff and Anderson, 1995).
This chapter describes the health care needs of children, including children with chronic medical conditions and special health care needs. The chapter begins with a description of the epidemiology of acute childhood illnesses. It then turns to the health care needs of the most prevalent chronic conditions—dental conditions, mental health and substance abuse problems, and developmental disabilities—and then discusses the needs of children with severe medical problems. The chapter continues with a description of financial and nonfinancial access barriers for children with special health care
TABLE 7.1 Children's Needs for Health Care, United States, 1992
|
|
Percentage of Population |
Number (millions) |
Percentage of Total Expenses |
|
Healthy |
70 |
50 |
10 |
|
Mild or Moderate Chronic Conditions |
20 |
14 |
10-20 (2-3 times) |
|
Severe Chronic Conditions |
10 |
7 |
70-80 (5-6 times) |
|
SOURCE: Neff and Andersen, 1992. Data are from the National Health Interview Survey as cited by Newacheck and Taylor, 1992. |
|||
needs, and then discusses some of the committee's concerns associated with managed care and its effects on access to health care for these children.
|
Certainly when we talk about children's health care status, we need to recognize how different children are, and how different their health care needs are from adults. Children face many obstacles in health care, but one of the hardest to overcome is the way most people view child health issues. When considering therapeutic interventions, medicines must be more finely calibrated, and diagnostic procedures may be more difficult. Young children, who have only a limited ability to communicate, must be examined more closely to diagnose and monitor illnesses. Steve Edwards American Academy of Pediatrics, Raleigh, NC Public Workshop, June 2, 1997 |
Epidemiology Of Illnesses In Children
Acute Illnesses
For most healthy children, a pediatrician, family physician, or other primary care practitioner (e.g., nurse practitioner or physician assistant) is usually the main source of preventive and acute medical care. Depending on the setting for care and the availability of allied health professionals on staff, these primary care practitioners also provide health education for parents and children, refer them for specialty consultations, and coordinate their care, as appropriate. Expanded services such as behavioral counseling, nutrition education, and parenting skills training also may be provided in a primary care setting.
Table 7.2 compares the frequency of acute illnesses and injuries for children with the general population. Infections are the most common acute illnesses of children, especially respiratory infections. Young children (ages 1 to 5 years) have significantly higher rates of acute illnesses than older children (ages 5 to 17 years) or than the general population.
TABLE 7.2 Number of Acute Conditions Per 100 Persons Per Year, for Children and All Ages, United States, 1994
|
|
Children |
||
|
Type of acute condition |
|||
|
Under Age 5 |
Ages 5-1 |
All ages |
|
|
Number per 100 persons |
|||
|
Infective and Parasitic Diseases |
54.7 |
41.9 |
20.9 |
|
Viral infections, unspecified |
20.7 |
11.7 |
6.6 |
|
Common childhood diseases |
8.6 |
2.9 |
1.5 |
|
Intestinal virus, unspecified |
8.3 |
9.5 |
4.6 |
|
All other |
17.1 |
17.8 |
8.2 |
|
Respiratory |
153.8 |
103.4 |
80.5 |
|
Common cold |
68.5 |
29.4 |
25.4 |
|
Other acute upper respiratory infections |
25.1 |
20.3 |
11.9 |
|
Influenza |
37.3 |
46.3 |
34.8 |
|
Acute bronchitis |
11.3 |
4.3 |
4.7 |
|
All other |
11.6 |
3.1 |
3.7 |
|
Digestive system |
10.6 |
8.3 |
6.1 |
|
Indigestion, nausea, and vomiting |
4.1 |
6.0 |
3.2 |
|
Dental conditions |
3.4 |
0.7 |
1.1 |
|
All other |
3.1 |
1.5 |
1.8 |
|
Injuries |
25.6 |
26.0 |
23.8 |
|
Fractures and dislocations |
1.9 |
4.6 |
3.0 |
|
Sprains and strains |
0.8 |
4.9 |
5.5 |
|
Open wounds and lacerations |
5.9 |
5.7 |
4.2 |
|
Contusions and superficial injuries |
5.2 |
5.5 |
4.7 |
|
All other |
11.8 |
5.3 |
6.5 |
|
Selected other acute conditions |
90.3 |
30.3 |
27.5 |
|
Acute ear infections |
62.7 |
13.6 |
9.3 |
|
Fever, unspecified |
10.5 |
4.6 |
2.1 |
|
Skin conditions |
5.9 |
2.7 |
2.4 |
|
Acute urinary conditions |
2.8 |
1.2 |
3.1 |
|
Acute musculoskeletal conditions |
0.8 |
1.5 |
3.5 |
|
All other |
7.6 |
6.7 |
7.1 |
|
Other Acute Conditions |
23.7 |
10.2 |
12.7 |
|
ALL ACUTE CONDITIONS |
358.7 |
220.1 |
171.5 |
|
SOURCE: NCHS, 1995, p. 12. Data are from the 1994 National Health Interview Survey. |
|||
|
People come to the pediatric emergency department when their children are sick. Our triage nurses have determined that about 40 percent of the children who present to our facility have nonurgent issues. Parents who look at a young child with an earache or a sore throat don't say, well, we don't have authorization to be seen tonight in the emergency department. They don't want to wait two weeks to get in to the clinic. They perceive their child's pain as a family and social emergency. These people may be treated as though they don't belong in the emergency department. But a cough and a fever can be a sore throat and a viral upper respiratory infection, or it can be the beginning of a serious pneumonia or an asthma exacerbation. Julius Goepp Johns Hopkins Hospital, Baltimore, MD Public Workshop, June 2, 1997 |
Chronic Conditions
This section describes the distinguishing features of the most prevalent chronic conditions: dental conditions, mental health and substance abuse problems, and developmental disabilities. Figure 7.1 indicates the total number of American children with selected chronic illnesses and conditions.
Concern about the costs of treatment for chronic conditions leads some employers and public officials to choose not to provide coverage for these conditions, or to provide only very restricted coverage. Although certain chronic conditions such as epilepsy or diabetes can be expensive to treat, the incidence of these conditions is limited.
Better risk adjustment methodologies are needed in order to adjust payment rates to reflect the expected costs of care for children with a variety of conditions. With better pricing systems, large employer-based dependent coverage pools and publicly-funded programs (especially those being designed under the authority of the new SCHIP legislation) may be better able to cover expensive conditions or diseases without depleting resources as much as may have been thought in the past.
Children with Dental Conditions
Tooth decay is the single most common chronic disease of children. It affects half of 5- to 9-year-olds in their first teeth and 84 percent of 17-year-olds in their permanent teeth (Kaste, Selwitz, Oldakowski et al., 1996). Untreated tooth decay results in pain, swelling, infection, dysfunction, and poor appearance. The National Health Interview Survey reports that children experience hundreds of thousands of ''bed-days" and "low-activity days" because of tooth decay (NCHS, 1997b).
Dental services for children have been part of publicly funded child health programs for more than 60 years, both through direct service programs and through Medicaid. Medicaid offers dental coverage to more than 20 million children, one of every four U.S. children. Still, approximately 80 percent of decay is found in only 25 percent of children, and most often these children are from low-income families (DHHS, 1996).
The Healthy People 2000 oral health indicators have not improved since the 1986 benchmark. The percentage of children with cavities and the percentage of unfilled cavities in children have not declined. At the same time, the percentage of children who visit a dentist before kindergarten has decreased. Among parents who report that their children have unmet health care needs, 57 percent report that the need is for dental care (NCHS, 1996).
EMOTIONAL AND BEHAVIORAL PROBLEMS ARE THE MOST PREVALENT CHRONIC CONDITION AMONG CHILDREN
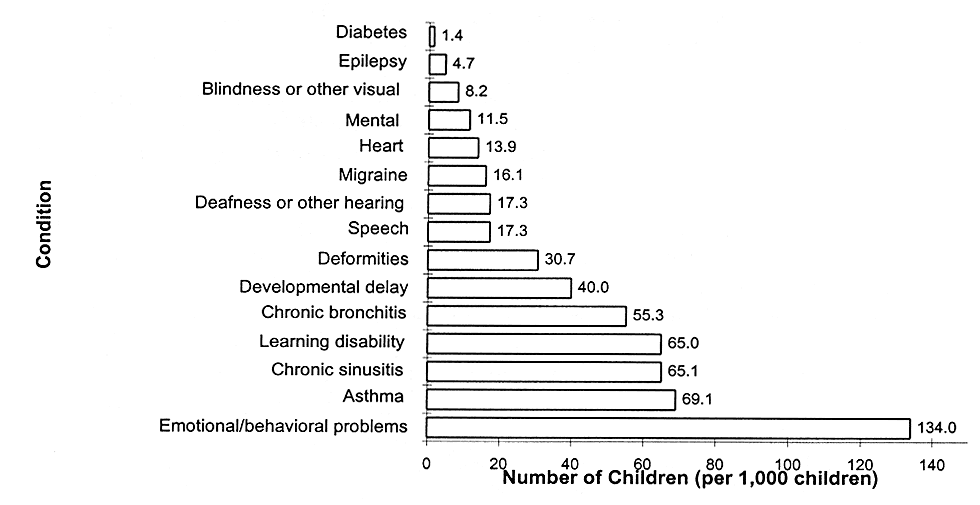
FIGURE 7.1
Number of children, ages 0-171 with selected chronic conditions, United States.
SOURCE: NCHS, 1997a; NCHS, 1995; NCHS, 1994. NOTE: Data are from the the 1988 National Health Interview Survey, Child Health (learning disability, developmental delay, and emotional/behavioral problems); National Health Interview Survey, 1990-92 (nervous system and respiratory conditions); and National Health Interview Survey, 1994 (physical impairments).
1 Data for learning disability, developmental delay, and emotional/behavioral problems, from the 1988 survey, cover children ages 3-17 only.
Children with Mental Health and Substance Abuse Problems
Approximately 12 million children, or 20 percent of all children, experience some type of mental health problem (e.g., attention-deficit-hyperactivity disorder, severe conduct disorder, and depression) or substance abuse problem (alcohol and other drug abuse or dependence) during childhood or adolescence (CMHS, 1996). An estimated 3.5 million children have serious emotional disturbances (CMHS, 1996). Compared with healthy children, children with physical health problems are more than twice as likely to have a mental health problem as well (Alliance for Health Reform, 1997).
Only about one third of children with severe mental health problems receive appropriate services from specialists (IOM, 1997a). Pediatricians and other primary care practitioners may be the first and only health care professionals to be consulted for childhood behavioral and emotional problems. Although some of these practitioners may be willing to provide appropriate care and referrals for these children, others may not have adequate training or time to do so.
A variety of sources—including community mental health centers, the mental health and substance abuse block grant, and state and local funding for mental health services—support services for these children and their families. National policies set by the National Institute of Mental Health and the Substance Abuse and Mental Health Services Administration promote "systems of care" for children
with serious emotional disturbance, with an emphasis on case management, care coordination, individualized treatment plans, and active involvement of family members and other caregivers (IOM, 1997a). Block grant funds are often used to help states organize and coordinate these services.
Although these principles of case management and coordination have been used to develop children's mental health programs in many states, the programs have rarely been evaluated, and data on the implementation and success of the programs have not been collected. Still, this approach may provide a model for comprehensive approaches that could also be applied to other children with special health care needs.
Children with Developmental Disabilities
The Personal Responsibility and Work Opportunity Reconciliation Act of 1996 defines disability as a physical or mental condition or conditions that can be medically proven and that result in marked and severe functional limitations (SSA, 1997a). Children with developmental disabilities have chronic conditions that manifest as single physical, psychological, self-care, language, cognitive, or speech impairments or combinations of these conditions (e.g., cerebral palsy, spina bifida, hearing impairment, visual impairment, and mental retardation). Partly because of differences in definitions and range of severity, estimates of the prevalence of developmental disabilities among children vary from 3 to 17 percent (Boyle et al., 1994; Newacheck and Taylor, 1992).
Data from the National Health Interview Survey indicate that disabled children have 1.5 times more visits to physicians and 3.5 times more hospital days than other children. They miss twice as many school days and are 2.5 times more likely than children without these conditions to repeat a school grade (Boyle et al., 1994).
Children with developmental disabilities have unique and special needs. In addition to the usual health care needs, such as immunizations or care for acute respiratory infections, they often require the assistance of physicians and nonphysician specialists, such as nutritionists or physical therapists. For example, they may require specialized diets, surgical interventions, and specific therapies to prevent complications and to relieve or reduce symptoms.
Although children with disabling conditions may benefit from care provided by specialists in terms of improved health and longevity, several of the committee members believe that increased use of specialists and specialty services can lead to fragmentation of care unless there is an explicit treatment plan that designates responsibilities for care coordination among primary care providers, specialists, parents, and adjunctive practitioners. Care coordination decreases the likelihood of the need for crisis care, reduces duplication and gaps in services, and helps to increase the likelihood that a child will be referred for appropriate medical and adjunctive services to maintain as high a level of independent functioning as possible.
Children with Special Health Care Needs
Although there are many different definitions of children's disabling or chronic conditions, for the purposes of this discussion the committee believes that special health care needs fall into distinct subgroups. The first includes children with severe conditions that are initially costly but whose use of resources decreases over time (e.g., infants with congenital heart defects requiring surgery or premature infants requiring neonatal intensive care). The second group includes chronically ill children who need repeated episodes of care throughout life to maintain or improve functioning, including those with asthma, diabetes, malignancies, sickle cell disease, cystic fibrosis, and neurodevelopmental disabilities such as cerebral palsy, and visual and hearing impairment.
Naturally, children's health care and medical needs—and thus their medical expenses—vary by the diagnosis and the severity of their illnesses. The prospects for medical improvement and improved
functioning vary significantly among children and may change over time with the developmental course of the illness.
|
I tried my best to do everything to have a healthy baby. I did not drink. I did not smoke. I took vitamins. I took prenatal exercise classes. The doctor assured me that I did nothing wrong, that these things just happen. We are grateful that Courtney is now stable. However, as long as she is on this earth she will continue to have medical needs. She takes several cardiac medicines in the hope of keeping her from going into congestive heart failure. Her heart cannot sustain very much stress, and she must be constantly monitored. Karen LaPlante Parent, Dublin, VA Public Workshop, June 2, 1997 |
In general, however, appropriately designed early interventions and disease management strategies can help to improve a child's ability to function, can slow the progression of illness, and often can decrease the long-term costs associated with the condition (Neff and Anderson, 1995). Access to these interventions depends in large part on the structure of the child's health insurance benefit package and on the availability of services and providers in a community. Traditionally, more of the case management services and other expanded approaches have been more likely to be financed by the public sector than by private insurers and health plans (IOM, 1997a).
|
Whether it is children or adults, I don't think we have reached a national agreement on what we do for someone with a very expensive illness. When you pick up tomorrow morning's Washington Post Health Section, it will predictably have some story on a very expensive, new, beneficial treatment, and nobody is willing to say what they are going to ante up for that. James Bentley American Hospital Association, Washington, DC Public Workshop, June 2, 1997 |
Traditional indemnity insurance coverage typically has very limited coverage of the supportive or supplemental therapies (speech, physical, etc.) required for children with severe chronic disease. Most managed care plans provide a core set of preventive and primary care benefits for children, but they differ in the extent to which specialty pediatric services are covered (McManus, 1998).
In recent years, health plans have begun to implement programs specifically for children with special health care needs, often in partnership with public health clinics (AAHP, 1997). Current initiatives include:
- The Blue Cross and Blue Shield Association working in partnership with the National Cancer Institute to refer children to nationally recognized treatment centers after being diagnosed with cancer;
- "ZAP Asthma," in which seven Atlanta-area health plans and local public health clinics will train community health workers to work with 200 families of children with asthma;
- Health Services for Children With Special Health Needs, Inc., a Washington, D.C.-based organization coordinating health care services for Medicaid recipients, including transportation, social services, respite care, and limited-use telephones for families without phone service; and
- Health Partners in Minneapolis working with a local parent advocacy coalition to develop a streamlined referral process and a flexible benefits package for children with chronic conditions.
Although these initiatives are certainly worthwhile, they are only available in a few communities. Evaluations of these programs could yield useful information that can help in the design and development of programs in other communities.
|
Although we have private insurance, there are many charges that our insurance company is refusing to pay. We have an annual out-of-pocket deductible of $2,000 before they begin paying at 100 percent. This 100 percent is for "usual and customary charges." The medical providers bill us directly for the remainder of the charges. Karen LaPlante Parent, Dublin, VA Public Workshop, June 2, 1997 |
Public Coverage For Special Health Care Needs
Historically, the public sector has taken the lead role in financing care for low-income and vulnerable populations. The services needed by families with children with special needs are funded by a mixture of federal, state, and local sources. The services are typically administered at the state and local levels, with significant variation in eligibility, availability of services, coordination among programs, and outreach and public education efforts.
Medicaid pays for health care services for low-income children with and without disabilities and is the major source of federal funds for medical services for special needs children. Medicaid generally covers health and related services for children who receive Supplemental Security Income (SSI), a cash benefit for low-income families with disabled children. It also covers services for children who are institutionalized. States may provide services for children with special health care needs under the Maternal and Child Health Services Block Grant (Title V) of the Social Security Act. This section gives a brief overview of the role of these programs with regard to special-needs children.
Medicaid
Because the benefit package in the Early and Periodic Screening, Diagnosis, and Treatment (EPSDT) program was specifically designed to address the needs of special-needs children (NIHCM, 1995), these expanded services—usually provided by nonmedical agencies or by other professionals such as advanced practice nurses or clinical nutritionists—are more likely to be covered by Medicaid than by private plans.
On a national basis, the average cost of EPSDT benefits for healthy children is typically about $1,000 to $1,500 per year, whereas the cost for special-needs children can approach $5,000 to $6,000 per year (NIHCM, 1995, p. 17). State-specific estimates of costs are generally not available, but average costs are likely to vary significantly by state, region, health care market, as well as by diagnostic and procedural categories.
One of the few states with published cost breakdowns is Washington State. In Washington State's Medicaid program, the average annual cost of care was $3,800 for children with selected chronic conditions, compared with an average of $955 for all enrolled children (Ireys et al., 1997). The proportions of payments for various categories of care (e.g., inpatient, outpatient, home care, drugs, durable medical equipment, and other providers) varied substantially by diagnosis. For example, inpatient costs ranged from 25 to 71 percent of the total. Durable medical equipment accounted for 24 percent of the costs of care for children with cerebral palsy, compared with 12 percent for children spina bifida and 5 percent or less for children with asthma, chronic respiratory disease, and diabetes (Ireys et al., 1997).
The Medicaid program is increasingly using managed care approaches in the delivery of services, most often through contracts with private health plans. An estimated 2.5 million children with chronic special health care needs are enrolled in the Medicaid program, but data are limited to evaluate the impact of Medicaid managed care on these children (Newacheck et al., 1994). Moreover, state Medicaid data tends to be aggregated, and without individual-level encounter data it is difficult to track or evaluate the types or quality of services used by any individual enrollee over time (GAO, 1997; Howell, 1996). The committee's general concerns about managed care are discussed in a later section of this chapter.
Supplemental Security Income
In 1996, approximately 955,000 children with disabilities received SSI payments that made them eligible for Medicaid (Alliance for Health Reform, 1997). SSI benefits are used to preserve the ability of families to take care of disabled children at home by providing cash assistance to help them meet some of their disability-related expenses, to help compensate for lost income, and to help meet basic expenses for food, clothing, and shelter (National Academy of Social Insurance, 1996).
As a result of the welfare reform legislation enacted in 1996, the definition of disability and the process for determining eligibility were tightened for children with behavioral problems (see Box 7.1), thus changing their Medicaid eligibility. The loss of SSI benefits could mean an increased financial burden for parents of disabled children, decrease their access to appropriate services, and ultimately have a significant impact on the children's level of functioning. However, there was controversy about the level of behavioral dysfunction that would merit a monthly federal cash payment and concern that the diagnostic criteria were too generous, as well as difficult to interpret (Koppelman, 1998).
In response to concerns expressed by the disability and children's health communities, the Balanced Budget Act of 1997 mandated Medicaid coverage for all disabled children who lost their eligibility due to changes in the welfare law or who were receiving SSI as of the date of the law's enactment (August 22, 1996). The Social Security Administration is reevaluating the determination criteria and reviewing appeals filed by families who have lost their benefits (see Box 7.1).
Maternal and Child Health Services Block Grant
Title V of the Social Security Act authorizes the Maternal and Child Health Services (MCH) Block Grant, a public health program that allows states to develop model, community-based health programs to improve the health of mothers and children. States are required to match $3 for every $4 that they receive from the federal government, and many states provide funds beyond the required match. More than $1.7 billion was generated in fiscal year 1997 for services at the state and local levels (MCHB, 1997).
The majority of MCH block grant funds are spent on preventive public health services to help meet the Healthy People 2000 national health objectives of the Public Health Service Act. The funds are used to pay for services for children and pregnant women not covered by Medicaid. These include programs offered by local health departments, community and migrant health centers, and HIV prevention and
treatment programs; some also are offered at Women, Infant, and Children (WIC) sites. Title V programs directly operate programs or fund local providers for services, including immunizations and well-child examinations, treatment or referral, school health services and education programs, and others.
State Title V programs are required to coordinate with other federal health, education, and social services programs. As a result, MCH block grant funds typically are used to strengthen linkages among programs and to fill gaps, creating and supporting community-based systems of care for children and their parents. States are required to use at least 30 percent of Title V funds on services for children with special health care needs, and 900,000 children with chronic illnesses and disabilities receive services supported by the block grant (AAP, 1997). These include case management, care coordination, and family support services and a limited number of home-visiting services, supported by the block grant.
Financial Barriers Associated With Special Needs
Even for families with comprehensive benefits provided through traditional private health insurance, out-of-pocket expenses for copayments and deductibles for the required medical services, occupational and physical therapy, and durable medical equipment can be quite substantial (Leonard et al., 1992). Some estimates suggest that expenses for children and families with special health care needs can be as high as 9 to 12.5 percent of the total family income (Leonard et al., 1992).
According to testimony heard in the committee's public workshop, families with these kinds of expenditures may quickly approach an insurance policy's lifetime limit on benefits, perhaps while the child is an infant, leaving the possibility of several decades without reasonable coverage. Families may be forced to choose between medical care and such basic needs as food, shelter, and long-term economic survival.
|
To the best of my knowledge, there is not a single state in this country where a family with severe medical needs doesn't have to wind up with poverty as a definition of when it can get access to some broad scale public program. I don't know of any state or any national program that really gets around that. James Bentley American Hospital Association, Washington, DC Public Workshop, June 2, 1997 |
Caregivers of children with special health care needs must devote significant amounts of their time to coordinating care, often among several agencies and providers. Transportation and related costs can become significant, and frequently one or both parents must miss work to keep appointments (Leonard et al., 1992) (see Box 7.2).
Nonfinancial Barriers For Special Needs Children
Children with chronic health conditions and special health care needs and their families face the same nonfinancial barriers to health care as other segments of society: transportation barriers, racial and cultural barriers, scheduling problems, lack of day care, and other difficulties. However, because of their complicated medical status, these children need more frequent visits to physicians and other health care
|
BOX 7.1 Supplemental Security Income Program Authorized by Title XVI of the Social Security Act of 1965 and begun in 1974, the Supplemental Security Income (SSI) Program replaced state-administered adult assistance programs to provide uniform federal income support to the needy aged, blind, and disabled who were not covered by Social Security. or for those who were only minimally covered. The program is administered by the Social Security Administration (SSA). Eligibility To be eligible for the SSI Program, individuals must meet income and resource requirements, and must satisfy one of the following categorical requirements:
|
*
| elderly—65 years of age or older;
|
*
| blind—defined as those people whose vision is 20/200 or less with a correcting lens in the better eye, or those with tunnel vision 20 degrees or less; or
|
*
| disabled—defined as those people who cannot "engage in any substantial gainful activity because they have a medically-determined physical or mental impairment that is expected to result in death or that has lasted, or is expected to last for a continuous 12-month period."
|
*
| spouse or child of a disabled worker. | |
Children less than 18 years of age (or less than 22, if a full-time student) are also eligible to receive SSI payments, if they are blind or disabled unmarried, and if their family meets the income and resource requirements. Benefits SSI was designed as a program of last resort; beneficiaries must file for all entitled benefits before SSI payments are determined. (It should be noted, however, SSI beneficiaries may not receive TANF Payments. See Table 5.1). SSI payments are adjusted annually to reflect the cost of living (COLA). As of September 1997, the average payment was about $436 per month (Vobejda and Goldstein. 1997). The rationale for the benefits is to help families meet disability-related costs of raising a disabled child, such as medical supplies and equipment to help compensate parents for lost income when they stay |
|||||||||
professionals (Leonard et al., 1992). In short, children with special needs face even greater challenges to access of appropriate health care and other needed services.
|
We take all children. In fact, let's be clear about it—we look for the sick children, because in my opinion, those who have a special health care need, who are in a low-income family, these are the children who are most at risk. Charles LaVallee Western Pennsylvania Caring Foundation for Children Public Workshop, June 2, 1997 |
|
home to care for a disabled child; and to help pay for basic needs such as food, clothing, and shelter. Thus, the purpose is to help support families that choose to care for their disabled children in their own homes. Childhood Disability—Welfare Reform Changes In August 1996, the Personal Responsibility and Work Opportunity Reconciliation Act of 1996 (P.L. 104-193) mandated that the Social Security Administration change its definition of childhood disability and make the definition comparable to that for adults. The revised definition requires a child to have a physical or mental condition or conditions that can be medically proven and which result in marked and severe functional limitations, and requires that the conditions must last or be expected to last at least 12 months or to result in death. Before the law was changed, a child with a condition not listed on the medical listing of impairments could be eligible for SSI if he or she was not functioning at an age-appropriate level as measured by the Individual Functional Assessment and evaluated by SSA. (A child with serious attention deficit disorder, for example would be eligible under this definition.) As a result of the new law, SSA began to review the cases of 260,000 children, more than one quarter of the one million enrolled in the program in 1996. As of September 997, 120,000 children had lost their benefits, and as many as 65,000 more, or about quarter of all SSI children, were expected to lose their benefits when the review has been completed. Families that are denied benefits may appeal, and almost half of them have done so. Of 2,200 cases that were appealed and had reached the first stage of review before September 1997, 67 percent were overturned and benefits restored. The new Commissioner of SSA, Kenneth Apfel, agreed in his Senate confirmation hearing on September 10, 1997, to re-evaluate the implementation of the new eligibility rules within 30 days of his swearing-in. The re-evaluation would be intended to determine whether the problems were due primarily to variations in interpretations of the definitions by states or with the procedures for conducting reviews. On December 17, 1997, Commissioner Apfel released a report reviewing the implementation of the childhood disability provisions of the welfare reform law. After an examination of quality assurance data and other oversight activities, the accuracy of determination decisions was found to vary by state and by impairment The Commissioner directed the agency to review the cases of 45,000 children who had lost their benefits during the redetermination process. In addition, families whose eligibility for SSI was ceased under the new law were given another opportunity to appeal. SOURCES: SSA, 1997a, 1997b; Pear, 1997; Vobejda and Goldstein, 1997. |
For children who are dependent on such technology as respirators, specially trained nurses may be required. It is often very difficult to obtain skilled day care for such children, and it can be difficult to obtain reimbursement for day care. As a result, parents lose days from work or give up their jobs to meet ongoing needs or as a result of intercurrent illnesses and disease relapses (Leonard et al., 1992). Because data on the impact of children with special needs on the parents' productivity in their places of work are not available, it is difficult to estimate the number of parents affected.
Although the treatment needs for each child and the treatment protocols for each chronic illness differ, children with chronic conditions and special health care needs typically see a wide range of practitioners. They are clinically managed by primary care pediatricians or family physicians, typically with an extensive amount of family and community involvement and referrals to specialists as needed. Alternatively, their care may be managed and coordinated by a pediatric specialist associated with a children's hospital or a pediatric specialty center within a larger community or academic health center (Neff and Anderson, 1995). More extensive research is needed to compare the relative effectiveness of
|
BOX 7.2 Caregivers' Time Costs | |
|
* |
personal care (helping with the child's bathing, grooming, eating, and so forth); |
|
* |
providing medical care (i.e., medications, tube feedings, treat wounds); |
|
* |
preparing special or extra meals and cleaning up afterward; |
|
* |
extra or special shopping and running errands (i.e., buying clothes, picking up medications); |
|
* |
extra household chores (cleaning home, snow shoveling, yard work); |
|
* |
escorting this child to get health care; |
|
* |
escorting this child to nonmedical functions beyond what you would have to do if he or she were healthy (i.e., social activities, entertainment) |
|
* |
managing this child's medical conditions (scheduling appointments with physicians, nurses, and social workers); |
|
* |
managing this child's finances (dealing with insurance companies, finding special programs, filling out forms); |
|
* |
waiting in physician's offices; and |
|
* |
monitoring medical equipment (cleaning, making sure it is in working order). |
these strategies. Such studies should take into account the severity of the child's illness, the family's skills and capacity for care taking, and a variety of other factors.
|
I am sad that there are no state and federal programs that assist middle class families in a way that allows them to continue to be middle class families. I have been told many times in the past that our family would have been much better off if we did not work or if we did not have insurance. Then our child would have qualified for assistance. It has been suggested that we get a divorce, place our child into an institution, or put our child in foster care in order to receive assistance toward her medical bills. Caring for an ill child is stressful enough without the sense of financial responsibilities, even when we have insurance. Karen LaPlante Parent, Dublin, VA Public Workshop, June 2, 1997 |
Pediatric subspecialists and intensivists tend to be located in regional medical centers. In many areas, children with complicated health care needs are referred to regional pediatric specialty centers even for routine care because locally available primary care providers may not be able to deliver the needed specialized care or the necessary case management and care coordination may not be not available locally (Schlesinger and Mechanic, 1993). In addition to the travel time and the rearrangement of work and child care schedules, out-of-pocket expenses for transportation and hotel bills can be significant.
Information Technology
The use of information technology holds significant promise for increasing access to health care when consumers and their providers live and work in different communities. For example, electronic consultations using computer-based patient records can reduce the need for families to travel long distances to consult specialists. The term ''telemedicine" is generally applied to the use of information technology when there is geographic separation or distance between the participants. Telemedicine applications include clinical evaluations, consultations, and supervision of providers in other locations (IOM, 1996).
Computer-based patient records can help to facilitate provider access to records, make transfer of records easier, and increase the availability of clinical information for research (IOM, 1997b). Many other uses of information technology are developing in medicine and health care, including some that are consumer-oriented. For those parents and providers who are able to use computers, an extensive variety of patient education materials are available through the Internet. Electronic parent-support groups, children's advocacy groups, and others are becoming increasingly common.
To provide readers with some examples of the uses of information technology by specialty providers, Box 7.3 includes some scenarios based on the actual clinical experiences of one of the committee members, a pediatric gastroenterologist. Research and evaluation have not caught up with the rapid diffusion or variety of uses of information technology in health care, and standard protocols and guidelines have not been developed, with the exception of the standards for electronic transmission of clinical data that are mandated by the Health Insurance Portability and Accountability Act of 1996.
Medical information systems can cost from $500,000 to several million dollars, depending on their features (Ciotti and Zodda, 1996). The expense of installing new administrative software has slowed its implementation, particularly in public clinics. In the past, insurers and health plans have restricted payments for telemedicine consultations and other electronic applications, such as patient education (IOM, 1996). However, the committee believes strongly in the potential of information technology to improve access and quality in health care for children and their families, and the committee urges insurers and health plans to explore its use further.
Access Under Managed Care
As of the summer of 1997, 36 states had mandated managed care arrangements for at least some children with special needs (Alliance for Health Reform, 1997). Some providers and researchers have expressed serious concerns about the potential for incorporating patients with chronic illnesses and serious medical conditions into the typical capitated managed care model (Hughes et al., 1995; Newacheck et al., 1994). Most managed care organizations (MCOs) have traditionally served working adults, who are generally healthy. Thus, MCOs have not tended to have much experience with low-income, chronically ill, or low-income individuals, although some are gaining experience through Medicaid managed care contracts and through developing programs specifically for these groups (AAHP, 1997).
There are few existing studies of children's access to care under managed care and they show many gaps and inconsistencies, making the evidence difficult to interpret. For example, a few studies have compared access to preventive services for low-income children with managed care and traditional coverage. They have found that children enrolled in Health Maintenance Organizations (HMOs) are more likely than children with traditional coverage to receive preventive medical care such as immunizations, vision and other screening tests, as well as more frequent and complete check-up visits compared with children with traditional coverage (Carey et al., 1990; Szilagyi et al., 1990).
A study comparing immunization rates for inner-city infants in Los Angeles found that they were more likely to have current immunizations if they received care in public health clinics rather than in
|
BOX 7.3 Scenarios Demonstrating Increased Access to Care Via Information Technology Scenario 1 J.R. is a 4-year-old child who has always been somewhat slow in his development. He didn't walk until nearly age 3-years and at age 4 he only has a few words in his vocabulary. He has always seemed very clumsy, and since beginning to walk, his parents have noticed that he walks on his toes. The child has otherwise been healthy without any serious illnesses. Because of his good health, he has not been seen by a physician since he was 2. He is brought to the family physician for a routine school physical. During that visit, the physician expresses concern about the child's development, and after examining the child, the physician explains to the mother that the child probably has cerebral palsy. The mother is extremely distraught and uncertain as to the significance of this diagnosis. The family physician suggests that it would be appropriate for the child to be seen and evaluated at a child development center. However, the family lives in a rural region and the nearest child development center is nearly 5 hours away. The physician provides the mother with the appropriate phone numbers and the mother calls the child development center to schedule an appointment. After a preliminary interview over the phone, the mother is directed to an interactive site on the World Wide Web that describes the services provided by the child development center. The website also contains an interactive multimedia tutorial about cerebral palsy that describes what it is, what some of its symptoms are, what can cause it, and some forms of therapy. Built into the tutorial are links to other educational materials, United Cerebral Palsy (UCP), and several moderated discussion groups. While on-line, the mother fills out a series of interactive forms on which she details her child's medical and developmental history. Based on the information provided on the forms, the coordinator at the child development center tailors a multidisciplinary evaluation for the child that includes assessments by a speech and language pathologist, a physical therapist, an educational specialist, a developmental psychologist, and a developmental pediatrician. The coordinator phones the mother and provides her with an outline of the planned evaluation and points her back to the web-site for a complete description of all the services planned for the child. On the day of the assessment, the mother not only comes prepared for the assessment but is also armed with lots of information and many well-informed questions. In this scenario, information technology helps educate and empower the "consumer" as well as optimize the use of resources both from the family's perspective and from the health care system's perspective. Scenario 2 R.W. is a 12-year-old female with severe spastic cerebral palsy. She has been followed by her local family physician for routine health care, but receives specialized care at a large child development clinic affiliated with a children's hospital. During the past 2 years, feeding R.W. has become increasingly difficult |
|
The parents often spend 6 hours each day trying to get her to eat. Despite all these efforts, her intake has declined over the past 6 months and she has lost several pounds. At the suggestion of their family physician, the family schedules an appointment at the child development clinic. During that visit, it is suggested that the family consider having a feeding gastrostomy tube placed to improve R.W.'s nutrition. The family members are quite resistant to this intervention but at the conclusion of their visit, they are provided with the address to the child development clinic's website, which contains a multimedia tutorial on feeding through gastrostomy tubes. Over the weeks following their visit to the child development clinic, the family visit the website several times and review the tutorial on gastrostomy tubes. The tutorial describes the actual procedure of placing the gastrostomy tube including diagrams, videos, and a short virtual tour of the operating and recovery suites. The tutorial also provides links to published follow-up studies concerning the use of a feeding gastrostomy tube in children with cerebral palsy, a link to a moderated listserve run by parents with children with gastrostomies, and the e-mail addresses of several parents who have agreed to serve as lay consultants. The tutorial also includes a direct e-mail link to the developmental pediatricians and pediatric gastroenterologists at the child development clinic to facilitate exchange of information. The family takes advantage of this e-mail consultation service to ask the gastroenterologist several questions concerning the actual operative procedure. After a great deal of soul-searching and deliberation, the family concludes that a gastrostomy is a good choice for their daughter. In this scenario, information technology helps the family make an informed decision concerning the care of their daughter by helping the family assimilate the available information about the proposed treatment as well as helping them communicate with other families that have gone through similar experiences. Scenario 3 K.T. is a 6-year-old female with severe spastic cerebral palsy who had a feeding gastrostomy and Nissen fundoplication (anti-reflux procedure) approximately eight months ago. Two months after her surgery, K.T. began experiencing frequent gagging and retching, and her ability to eat by mouth dramatically decreased. K.T.'s pediatrician and surgeon try a number of different medications without substantial change in her symptoms. The family becomes increasingly frustrated and performs a search on the Internet about gastrostomies. They find a moderated listserve run by parents of children with gastrostomy tubes and post a question on the listserve describing their daughter's symptoms. A number of parents respond stating that most likely K.T. is suffering from "post-Nissen dumping syndrome." These parents offer K.T.'s mother and father several references as well as the web address of a pediatric gastroenterologist who has written about this disorder. K.T.'s parents electronically consult this gastroenterologist, who makes a number of conservative therapeutic recommendations. K.T.'s parents return to their pediatrician and pediatric surgeon armed with information including several references. In this actual case history, parents used information technology to influence physicians and improve the care of their child. This type of exchange reinforces the concept that health care professionals and parents must be collaborators when caring for children with complex needs. |
private physician offices or HMOs (Wood et al., 1994). A national study found, however, that infants were more likely to receive well-child visits and immunizations in private physician offices or HMOs than in public health clinics (Mustin et al., 1994). There is tremendous variation from community to community in the provision of care for low-income groups (Baxter and Mechanic, 1997), and it is very difficult to generalize from the existing studies.
It is well-known that the cost savings under managed care are derived from the increased use of primary care and decreased utilization of specialty and inpatient care. Although this pattern of utilization may be appropriate for children who are generally healthy, its potential impact on children with chronic conditions and special health care needs causes concern (Schlesinger and Mechanic, 1993). Some children's health advocates fear that managed care has an inherent disincentive to provide treatment, although there is little scientific evidence to substantiate this claim. Because the actual costs of inclusion of children with chronic conditions and special needs in managed care plans and networks have not been systematically reported or studied, the issue remains controversial.
Another concern about managed care is that many health plans do not include pediatric specialists in their approved provider networks. As a result, children with complex illnesses may be seen by adult specialists who are trained to care for adults with similar illnesses but who lack the knowledge of the specific manifestations of disease in children and the differences between children and adults (Cartland and Yudkowsky, 1992).
Because at least 36 states now have some form of mandated managed care for at least some children with special needs, several strategies have been proposed to increase the likelihood that their medical needs will be met. These include ensuring that there are a significant number of local pediatric specialists in networks before contracts are negotiated (Newacheck et al., 1994); setting up separate payment systems for children with certain medical conditions or "carving out" these groups (Neff and Anderson, 1995); and developing quality assurance measures that assess quality of care for children with chronic conditions, including clinical practice guidelines and practice parameters, and consumer protections, such as written policies concerning grievances and availability of services (IOM, 1997a; Newacheck et al., 1994).
Long-term strategies include developing better pricing systems, particularly risk adjustment mechanisms that adjust payment rates to reflect the higher expected costs of care for children with chronic conditions. Although health policy and financing experts have been recommending better risk adjustment mechanisms for several years, much work remains to be done to resolve technical and methodological disagreements among proponents of different approaches (Iezzoni, 1997; IOM, 1996).
Despite these technical difficulties and the need for better information involving risk selection and costs of coverage, there is no question that children with special needs typically have additional, nonmedical needs. These include supplemental or adjunctive therapies; specialized transportation, supplies, and equipment; links with schools and other community-based organizations; and family support, including respite care and assistance with out-of-pocket (noncovered) expenses.
Implications For Children's Insurance Expansions
Insurance coverage for children is variable and fragmented, and many controversial issues remain unresolved. It is generally agreed that the most comprehensive and child-specific package of benefits is Medicaid, which offers a full range of medically necessary care for children, including children with special needs. In some cases, privately insured children can receive additional assistance from public sources, even Medicaid, to pay for what their private plan does not cover.
Some opponents of Medicaid believe that if private insurers do not guarantee comprehensive coverage, public programs should not do so either. Others take a pragmatic position that it is less expensive for society in the long run to provide preventive services and early interventions for low-
income children. Still others believe that it is the responsibility of society to provide medically necessary care for all children regardless of their insurance status.
Broadly speaking, traditional private insurance is primarily designed to provide time-limited coverage for acute episodes, whereas Medicaid also covers treatments which may improve functioning and quality of life, but are not expected to result in a cure. Healthy children, as well as children with special health needs, could benefit from the coordination and management of care that are offered in managed care environments, but some in the children's health community are concerned that managed care does not yet have adequate quality assurance methods for special needs children.
Under the new State Children's Health Insurance Program (SCHIP) legislation, states may choose to expand Medicaid, to create or expand a separate state program for children's health insurance, or to use Medicaid for some uninsured children and a separate program for others. Medicaid expansions must provide the existing Medicaid benefits and must be implemented statewide. Other programs do not need to be statewide but must be based on one of the following three options:
|
• |
Benchmark coverage. The standard Blue Cross/Blue Shield preferred provider plan for federal employees, or the commercial HMO plan with the largest insured, non-Medicaid enrollment in the state, or a health benefits plan offered and generally available to state employees. |
|
• |
Benchmark-equivalent coverage. This must include hospital services, physician's services, laboratory and X-ray services, well-baby and well-child care, and immunizations. Some coverage of prescription drugs, mental health services, and vision and dental care is required if it is covered under the benchmark plan being used by the state for this purpose. |
|
• |
Another benefits package approved by the Secretary of Health and Human Services. |
As of April 1, 1998, six months after the SCHIP program began, 8 states had federally approved plans that are expected to cover more than 1 million additional children. Another 15 states had submitted plans to DHHS for approval; of these, only 2 states (Connecticut and Massachusetts) had specifically included programs for children with special needs.
States developing new children's insurance programs have many options for providing coverage for special needs children. The committee encourages states to take advantage of the new program to improve the availability of insurance programs to meet the needs of all children.
References
AAHP (American Association of Health Plans). 1997. AAHP Fact Sheets: Chronic Care. Washington, D.C.: AAHP Medical Affairs Department.
AAP (American Academy of Pediatrics). 1997. Legislative and Regulatory Issue: Maternal and Child Health Block Grant. Washington, D.C.: Author. [http://www.aap.org/advocacy/washing/maternal.htm]
Alliance for Health Reform. 1997. Managed Care and Vulnerable Americans: Children With Special Health Care Needs. Washington, D.C.: Author.
Baxter RJ, Mechanic RE. 1997. The Status of Local Health Care Safety Nets. Health Affairs 16(4)7-23.
Boyle CA, Decoufle P, Yeargin-Allsopp M. 1994. Prevalence and Health Impact of Developmental Disabilities in US Children. Pediatrics 93(3):399-403.
CMHS (Center for Mental Health Services), Substance Abuse and MentalHealth Services Administration , Department of Health and Human Services (DHHS). 1996. Child, Adolescent, and Family Programs. Washington, D.C.; National Mental Health Services Knowledge Exchange Network.
Cartland JDC, Yudkowsky M. 1992. Barriers to Pediatric Referral in Managed Care Systems. Pediatrics 89:183-188.
Carey T et al. 1990. Prepaid versus Fee-for-Service Medicaid Plans: Effects on Preventive Health Care. Journal of Clinical Epidemiology 43:1213-1220.
Ciotti V, Zodda F. 1996. Selecting Managed Care Information Systems. Health care Financial Management, June, 35-40.
DHHS (Department of Health and Human Services, Office of the Inspector General). 1996. Children's Dental Services Under Medicaid: Access and Utilization, OEI-09-00240. San Francisco, CA: US DHHS.
GAO (General Accounting Office). 1997. Medicaid Managed Care Accountability . Washington D.C.: GAO/HEHS/97-86.
HIAA (Health Insurance Association of America). 1997. Source Book of Health Insurance Data. Washington, D.C.: HIAA.
Howell EM. 1996. Medicaid Managed Care Encounter Data: What, Why,and Where Next? Health Care Financing Review 17(4):87-95.
Hughes D.C., Newacheck PW, Stoddard JJ, Halfon N. 1995. Medicaid Managed Care: Can It Work for Children? Pediatrics 95(4):591-594.
Iezzoni LI. 1997. The Risks of Risk Adjustment. Journal of the American Medical Association, 278:1600-1607.
Institute of Medicine (IOM). 1989. The Future of Public Health. Washington, D.C.: National Academy Press.
IOM. 1993. Employment and Health Benefits: A Connection at Risk. Washington, D.C.: National Academy Press.
IOM. 1996. Telemedicine: A Guide to Assessing Telecommunications in Health Care. Washington, D.C.: National Academy Press.
IOM. 1997a. Managing Managed Care Quality Improvement in Behavioral Health. Washington, D.C.: National Academy Press.
IOM. 1997b. The Computer-Based Patient Record: An Essential Technology for Health Care. Revised Edition. Washington, D.C.: National Academy Press.
Ireys HT, Anderson GF, Shaffer TJ, Neff JM. 1997. Expenditures for Care of Children With Chronic Illnesses Enrolled in the Washington State Medicaid Program, Fiscal Year 1993. Pediatrics 100(2):197-204.
Kaiser Commission on the Future of Medicaid. 1997. Medicaid Facts: Medicaid and Managed Care. Washington, D.C.: Kaiser Commission on the Future of Medicaid.
Kaste LM, Selwitz RH, Oldakowsky RJ, et al. 1996. Coronal caries in the primary and permanent dentition of children and adolescents, 1988-91. Journal of Dental Research 75(Special Issue):631-641.
Koppelman J. Personal communication to Institute of Medicine. February 1998. Leonard B, Burst JD, Sapienza JJ. 1992. Financial and Time Costs to Parents of Severely Disabled Children. Public Health Reports 107:302-312.
Lewit EM, Monheit AC. 1992. Expenditures on Health Care for Children and Pregnant Women. The Future of Children (2):95-1 14.
Lozano P, Fishman P, VonKorff M, Hecht J. 1997. Health Care Utilizationand Cost Among Children with Asthma who were Enrolled in a Health Maintenance Organization . Pediatrics 99(6):757-764.
McManus M. 1998. Evaluating Managed Care Plans for Children With Special Health Care Needs: A Purchaser's Tool. [http://www.ichp.edu/mchb/center/policy/index.html
MCHB (Maternal and Child Health Bureau), Health Resources and Services Administration, DHHS. 1997. Maternal and Child Health Bureau- Overview . [http//www.os.dhhs.gov/hrsa/mchb/overview.htm]
Moore CM, Ahmed I, Mouallem R, May W, Ehlayel M, Sorensen RU. 1997. Care of Asthma: Allergy Clinic Versus Emergency Room. Annals of Allergy, Asthma, and Immunology 78:373-380.
Mustin HD et al. 1994. Adequacy of Well-Child Care and Immunizations in U.S. Infants Born in 1988. Journal of the American Medical Association 272:11l1- 1115.
National Academy of Social Insurance. 1996. Restructuring the SSI Disability Program for Children and Adolescents. Washington, D.C.: Author.
NCHS (National Center for Health Statistics). 1994. Health of Our Nation's Children. Vital and Health Statistics 10 (191). Hyattsville, MD: US Department of Health and Human Services.
NCHS. 1995. Current Estimates from the National Health InterviewSurvey, 1994 . Prepared by PF Adams and MA Marano. Vital and Health Statistics 10 (193). Hyattsville, MD: US Department of Health and Human Services.
NCHS. 1996. Healthy People 2000 Review 1995-96. DHHS Publication No. PHS 96-1256. Hyattsville, MD: US Public Health Service.
NCHS. 1997a. Prevalence of Selected Chronic Conditions: United States, 1990-1992. Vital and Health Statistics 10 (194). Hyattsville, MD: US Department of Health and Human Services.
NCHS. 1997b. Priority Area 13, Oral Health. Healthy People 2000 Review 1997. Hyattsville, MD: US Department of Health and Human Services.
Neff JM, Anderson G. 1995. Protecting Children With Chronic Illness in a Competitive Marketplace. Journal of the American Medical Association 274:1866-1869.
Newacheck PW, Taylor WR. 1992. Childhood Chronic Illness: Prevalence, Severity, and Impact. American Journal of Public Health 82: 64- 7 1.
Newacheck PW, Hughes D, Stoddard JJ, Halfon N. 1994. Children With Chronic Illness and Medicaid Managed Care. Pediatrics 93:497-500.
NHCM (National Institute for Health Care Management). 1995. Assuring Quality of Care for Children in Medicaid Managed Care-EPSDT in a Time of Changing Policy. Washington, D.C.: NIHCM.
Pear R. 1997. 135,000 Children to be Struck From Disability Benefit Rolls. The New York Times, February 7, 1997.
Schlesinger M, Mechanic D. 1993. Challenges for Managed Competition from Chronic Illness. Health Affairs Supplement. 1993:123-137.
SSA (Social Security Administration). 1997a. The Definition of Disability for Children. SSA Publication No. 05-11053, July 1997. [http://www.ssa.gov/pubs/l1053.html]
SSA. 1997b. News Release: Statement by Kenneth S. Apfel, Commissioner of Social Security, on SSI Childhood Disability Reviews. [http://www.ssa.glv/press/childhood_statement.html]
Szilagyi PG et al. 1990. The Effect of Independent Practice Association Plans on Use of Pediatric Ambulatory Medical Care in One Group Practice. Journal of the American Medical Association 263(16):2198-2203.
Vobejda B, Goldstein A. 1997. Quick Review Promised for SSI Rules: Thousands of Children Have Lost Benefits. The Washington Post, September 11, p. A9.
Wood D et al. 1994. Access to Infant Immunizations for Poor, Inner-City Families: What is the Impact of Managed Care? Journal of Health Care for the Poor and Underserved 5(2):l12-23.
Zuckerman S, Evans A, Holahan J. Questions for States as They Turn to Medicaid Managed Care. Number 11 in Series, "Issues and Options for States." Washington, D.C.: Urban Institute. [http://newfederalism.urban.org/html/ant_all.htm]





















