3
Health Insurance and Access to Care
Why Access Matters
Children's access to health care is important to children themselves, to their families, as well as to society at large. Health care can influence children's physical and emotional health, growth, and development and their capacity to reach their full potential as adults. All children are at increased risk of developing preventable conditions if appropriate care is not provided when they are sick or injured. When children fail to receive necessary health care, their lives and the lives of their families can be affected for many years.
The Institute of Medicine (IOM) has defined access as ''the timely use of personal health services to achieve the best possible health outcomes" (IOM, 1993, p. 4). The most common way to measure access is by comparing the health care utilization rates for different age groups, different racial and ethnic groups, and so on.
This chapter begins with a general discussion of the evidence that health insurance affects children's access to health care, emphasizing differences in health care utilization rates for insured and uninsured children. Next, other financial and nonfinancial barriers to care are discussed, including family income; family structure; and racial, ethnic, and cultural factors. The chapter also presents three approaches to defining what kinds of health care services should be provided for children, and then describes the services allowed under the State Children's Health Insurance Program (SCHIP).
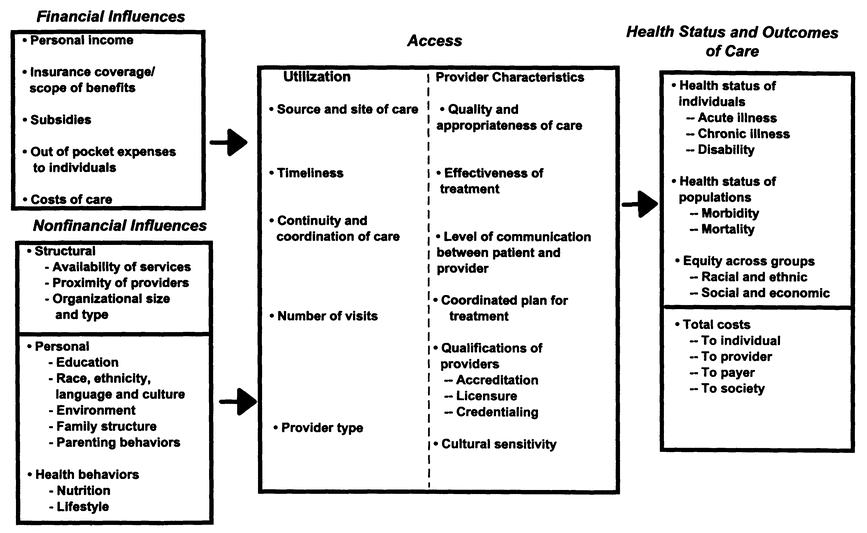
Figure 3.1 was developed by the committee and revised several times throughout the course of the study. It presents the overall framework used by the committee to approach its analysis of a variety of influences on access to health care. This chapter reviews scientific and empirical evidence on the financial and nonfinancial influences represented in the first column of the figure.
Financial Barriers To Access
According to data released in July 1997 by the National Center for Health Statistics (NCHS), more than 7.3 million children—about 1 out of every 10 children—had at least one unmet medical need in 1993. These included dental care, prescription medication, eyeglasses, and mental health care. For 2.7 million children, care was reportedly delayed because of its cost (NCHS, 1997a). Children without health insurance were six times more likely to go without medical care than children with employer-
based (private) insurance. They were four times more likely than children with private insurance or Medicaid to experience a delay seeking care because their parents were concerned about payment.
Health Insurance and Access to Care
Contacts with Physicians
The prevalence of both acute and chronic conditions among insured and uninsured children—and thus their needs for care—are similar (Holl et al., 1995). However, the amount of contact with physicians differs significantly.
Children without insurance coverage are more than twice as likely as insured children not to visit a physician over a 12-month period (Holl et al., 1995). A study based on the 1987 National Medical Expenditures Survey found that uninsured children received care for acute earaches, recurrent ear infections, pharyngitis, and asthma only half as often as children who had either public or private coverage (Stoddard et al., 1994).
|
We don't know very much about the transition to managed care, either in the public or private sectors. But in the fee-for-service world we have very good evidence that children who have Medicaid as a source of coverage have utilization patterns and sources of care that look like those for children with private insurance. Kay Johnson George Washington University, Washington, DC Public Workshop, June 2, 1997 |
Uninsured children with chronic medical conditions also have been found to have insufficient access to routine medical care. According to a national survey sponsored by the Robert Wood Johnson Foundation, nearly one in five uninsured children (17 percent) did not receive medical treatment needed for a chronic illness such as asthma, diabetes, or other conditions (32 percent) serious enough to keep a child from functioning at school (Wood et al., 1990).
Medical Attention for Injuries
Uninsured children are less likely than those with insurance to receive medical care for injuries, even for serious injuries. Among children who are uninsured, one study found that as many as 30 percent of all children with injuries and 40 percent of all children with serious injuries may not receive medical attention (Overpeck and Kotch, 1995). Injured children with Medicaid coverage and children with private insurance were found to have comparable access to medical attention (Overpeck and Kotch, 1995), which is consistent with the findings about access to medical services in other studies (Butler et al., 1985; St. Peter et al., 1992).
Hospital Services
Insured children have been found to have better outcomes from hospitalizations than uninsured children. Among children hospitalized in New York City for similar problems, one study found an in-
hospital death rate that was almost one and one-half (1.46) times higher for uninsured children than for those who were insured (Carr et al., 1992). The uninsured children were more likely to be admitted to the hospital in a critical condition, and their needs for care were more urgent on admission. The study also found that hospitalization and mortality rates were highest in the poorest neighborhoods included in the study and in neighborhoods with the highest percentage of black and Hispanic residents. While each of these factors independently predicted the hospitalization rates, they were also significantly interrelated.
A California study found that newborns who were uninsured were more likely to be sick but received fewer services in the hospital than newborns who had insurance coverage (Braveman et al., 1989). The increased levels of risk for newborns were thought likely to be due in part to the lack of access to prenatal care for the uninsured mothers, who were also more likely to be black and Hispanic.
Figure 3.2 and Table 3.1 present the rates of hospitalizations for children whose conditions could have been treated on an outpatient basis (also known as "ambulatory care-sensitive conditions" or "preventable hospitalizations"). The rates are based on data from 10 states with a total population of 95 million analyzed by the Ambulatory Care Access Project of the United Hospital Fund of New York (Center for Health Economics Research, 1993, p. 57).
Children living in low-income areas have two to four times as many preventable hospitalizations as children living in high-income areas. These rates are likely to be due to poorer general health status, poorer access to preventive and routine care when needed, as well as to lack of insurance among low-income families (Newacheck and Halfon, 1988; Newacheck et al., 1996).
|
If you don't think coverage is important not only to remove barriers, but to restore dignity, go watch a family walk a child into an emergency room and have to ask for services that they can't pay for. They don't enjoy it, and you wouldn't enjoy it either. James Bentley American Hospital Association, Washington, DC Public Workshop, June 2, 1997 |
Preventive Care
Insured children are much more likely to have a usual provider for routine preventive services and to receive recommended and age-appropriate services (Holl et al., 1995; Kogan et al., 1995). Preschoolers who lack insurance are less likely to be fully immunized than insured preschoolers (Wood et al., 1990), and so are children in families with incomes below poverty level (see Figure 3.3). During the course of a year, fewer than half (44.8 percent) of uninsured preschool-age children have any well-child visits, and fewer than one-third receive the recommended schedule of visits for their age (Short and Lefkowitz, 1992).
Racial comparisons of immunization rates show that white children are more likely to be immunized than are black children (see Figure 3.4). These rates are consistent with findings from other studies that have found poverty, minority status, and absence of insurance to be significant predictors of access to adequate primary care (Newacheck et al., 1996). Members of racial and ethnic minorities are disproportionately more likely to be uninsured and poor. While each of these characteristics independently is related to poor health status and lower health care utilization, these characteristics can not be viewed separately when outreach and community-based interventions are designed to increase the use of preventive services.
MOST PREVENTABLE HOSPITALIZATIONS OCCUR AMONG POOR CHILDREN

FIGURE 3.2
Hospitalizations for ambulatory care-sensitive conditions per 1,000 children under age 5, United States, 1989. Data are from 10 states having a total populationof 95 million. High-income areas are zip codes in which fewer than 15 percent of households have annualincomes below $15,000; low-income a reas are zip codes in which 50 percent or more of households haveannual incomes below $15,000.
SOURCE: Adapted from Center for Health Economics Research (1993,p. 57).
TABLE 3.1 Hospitalizations for Ambulatory Care-Sensitive Conditions per 1,000 Children Under Age 5, by Area of Residence, United States, 1989
HIGHER INCOME CHILDREN ARE MORE LIKELY TO BE IMMUNIZED
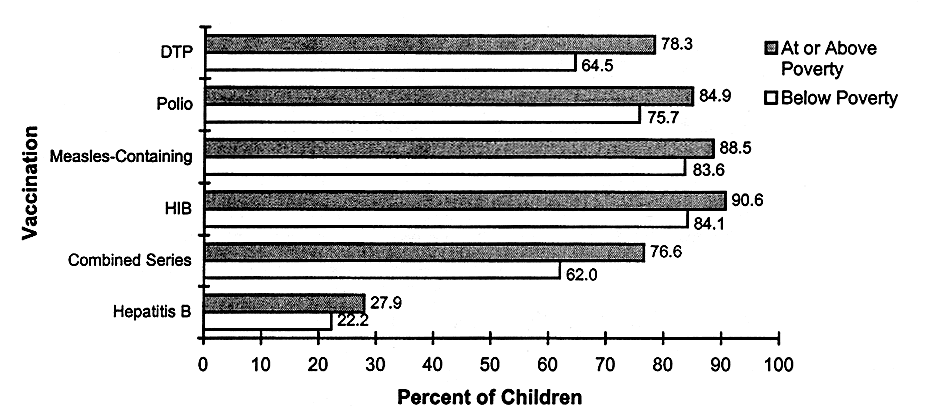
FIGURE 3.3
Vaccinations against selected diseases for children ages 19-35 monthsby poverty status, United States, 1994. Data are from the National Health Interview Survey, supplemented by informationcollected from vaccination providers in the National Immunization Provider Record Check study. NOTES: Poverty status isbased on family income and family size using Bureau of the Census poverty thresholds (see Chapter 2, Table 2.5 in this report).DTP=diphtheria, tetanus toxoids, and pertussis vaccine (four doses or more); polio vaccine is three doses or more; HIB=Haemophilusinfluenzae type b vaccine (three doses or more); combined series (4:3:1) consists of four doses of DTP, three dosesof polio vaccine, and one dose of measles-containing vaccine; and hepatitis B vaccine is three doses or more. SOURCE:NCHS (1997c, pp. 171-172).
WHITE CHILDREN ARE MORE LIKELY TO BE IMMUNIZED THAN BLACK CHILDREN
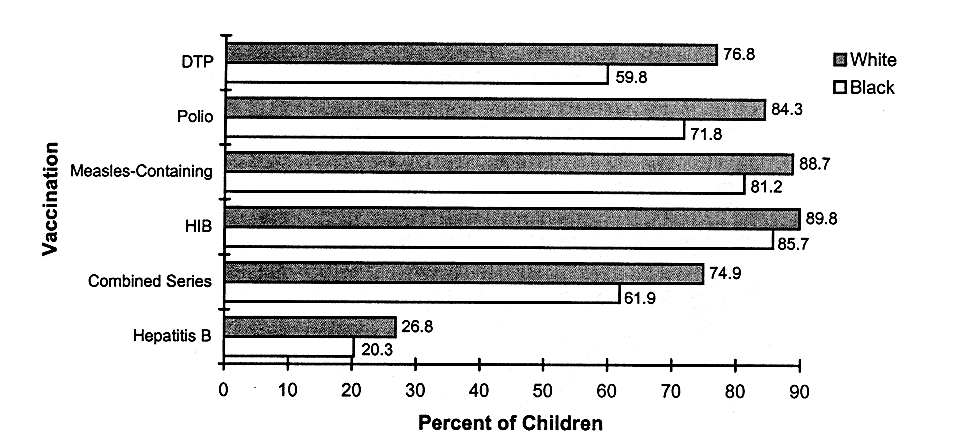
FIGURE 3.4
Vaccinations of children ages 19-35 months for selected diseases,by race, United States, 1994. Data are from the National Health Interview Survey, supplementedby information collected from vaccination providers in the National Immunization Provider RecordCheck study. DTP=diphtheria, tetanus toxoids, and pertussis vaccine (four doses or more); polio vaccineis three doses or more; HIB=Haemophilu influenzae type b vaccine (three doses or more); combined series(4:3:1) consists of four doses of DTP, three doses of polio vaccine, and one dose of measles-containingvaccine; and hepatitis B vaccine is three doses or more. SOURCE: NCHS (1997c,pp. 171-172).
Continuity of Care
One frequently used indicator of access to care is the presence of a usual source of care. Children and families who have a regular source of care are better able to obtain access to health care services when they are needed, and their utilization of services is higher than those without a regular source of care (Aday et al., 1984; Monheit and Cunningham, 1992; Newacheck et al., 1995). Having a regular source of care can also increase the continuity of care, because regular providers who know the children are more familiar with children's and families' medical histories and may be better able or more likely to monitor the progress of treatment through follow-up visits (Aday et al., 1984).
Uninsured children are seven to eight times more likely to lack a regular source for routine health care (Holl et al., 1995; Newacheck et al., 1997). Of the uninsured children who do receive routine care, 24 percent overall and 52 percent of poor children receive the care in a setting other than a physician's office (St. Peter et al., 1992).
Children who do not have a physician's office as their usual source of care are less likely to be taken to a physician when care is needed (Kasper, 1987) and are more likely than insured children to use higher-cost hospital emergency rooms or clinics (Newacheck et al., 1996; Wood et al., 1990). As indicated in Figure 3.5 and Table 3.2, a higher proportion of the total number of visits to emergency rooms are for "nonurgent" reasons than for emergencies. Children without insurance are five times more likely than children with Medicaid or employer-based coverage to use the emergency room as a regular source of care (NCHS, 1997b).
Compared with children who receive routine care at physicians' offices, children who receive routine care at community clinics have less continuity in their care. These children are 10 times more likely to go to a different provider or facility when they are sick and 10 times more likely to be taken to an emergency room (St. Peter et al., 1992).
Dental Visits
Although medical and dental services traditionally have been delivered separately, dental care is increasingly recognized as an important aspect of general health care for children (Lewit and Kerrebrock, in press). Oral diseases affect not only the teeth, gums, and rest of the mouth, but they also can lead to serious general health problems and significant pain, interference with eating, overuse of emergency rooms, as well as lost school and work time. Preventive methods such as the use of fluoride and dental sealant are comparable in effectiveness to immunizations against infectious disease, but these services are not always readily available.
Among parents who feel that their children have unmet health care needs, 57 percent report that the need is for dental care (NCHS, 1997a). Fifty-five percent of all 6- to 8-year-olds have untreated tooth decay, and these rates are even higher among minority populations (NCHS, 1996). The National Institute for Dental Research estimates that 51 million school hours per year are lost due to dental-related illness (Brunelle, 1989).
Uninsured children are 2.5 times less likely than insured children to receive dental care (Bloom et al., 1992; Monheit and Cunningham, 1992; Newacheck et al., 1997). Among children enrolled in Medicaid's Early and Periodic Screening, Diagnosis, and Treatment (EPSDT) program, only about twenty percent actually receive the required dental services (DHHS, 1996).
In the mid-1980s, the RAND Health Insurance Experiment found that reduced cost-sharing for dental services led to increased use of preventive dental services as well as significantly fewer decayed teeth (Isman, 1997; Newhouse et al., 1993). It is well established that individuals who have private dental insurance are more likely to use dental services, including preventive services, than those who are uninsured (Bloom et al., 1992; Newacheck et al., 1997). Yet copayments for dental services are still considerably higher than those for other health services (Lewit and Monheit, 1992).
BOYS VISIT EMERGENCY ROOM MORE THAN GIRLS; WHITES VISIT MORE THAN BLACKS
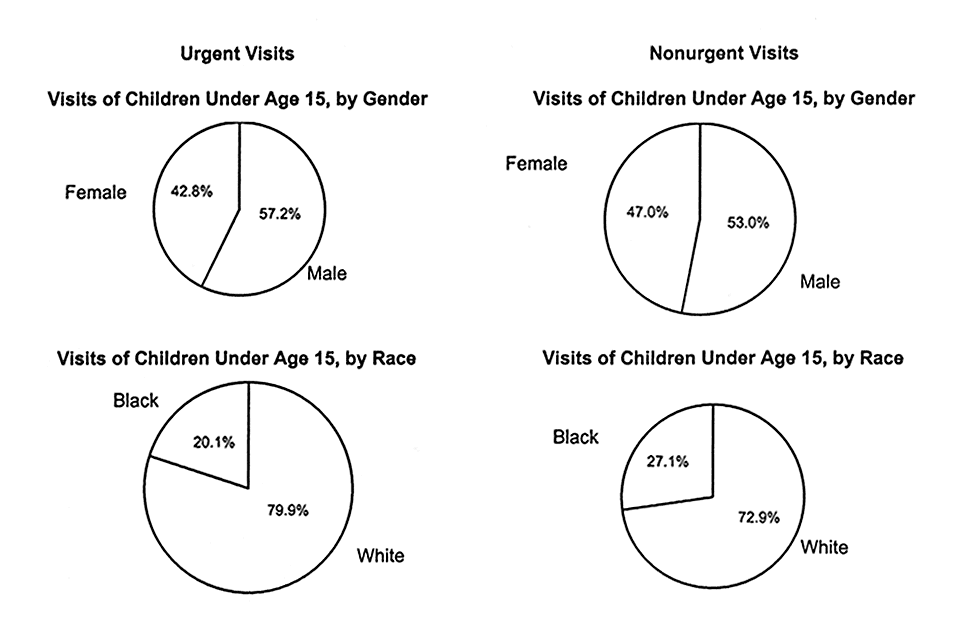
FIGURE 3.5
Urgent and nonurgent emergency room visits for children under age15, United States, 1995.
SOURCE: NCHS (1997b, pp. 4, 6). Data are from the 1995 National Hospital Ambulatory Medical Care Survey, Emergency Department Summary.
TABLE 3.2 Urgent and Nonurgent Emergency Room Visits for Children Under Age 15, United States 1995
|
|
Urgent Visits |
|
Nonurgent Visits |
||
|
Group |
Number (in thousands) |
Percent |
Number (in thousands) |
Percent |
|
|
Gender |
|||||
|
Male |
4,861 |
57.2 |
7,531 |
53.0 |
|
|
Female |
3,638 |
42.8 |
6,679 |
47.0 |
|
|
Race |
|||||
|
White |
6,547 |
79.9 |
9,976 |
72.9 |
|
|
Black |
1,644 |
20.1 |
3,710 |
27.1 |
|
|
SOURCE: NCHS (1997b, pp. 4, 6). Data are from the 1995 National Hospital Ambulatory Medical Care Survey, Emergency Department Summary. |
|||||
Other Financial Barriers to Access
Even when they have insurance coverage, children from low-income families have fewer contacts with physicians than other insured children (Rosenbach, 1989). Low-income, privately insured families bear a greater burden of the direct costs of health care for their children than families who have higher incomes or coverage through Medicaid, because out-of-pocket expenses such as copayments and deductibles represent a higher relative proportion of family income (Newacheck, 1989; Newacheck et al., 1996). Studies have shown that when cost-sharing increases (i.e., when out-of-pocket expenses are higher), the use of outpatient services for a variety of illnesses decreases (Rosenbach, 1989; Valdez et al., 1985).
Out-of-pocket expenses can be particularly burdensome for children with chronic conditions. A recent study sponsored by the Agency for Health Care Policy and Research found that more than 60 percent of insured families with a child with insulin-dependent diabetes mellitus had to pay a deductible for either insulin, syringes, or blood testing strips and that more than 85 percent had a copayment for these items. The annual out-of-pocket expenses were 56 percent higher than those for families with comparable coverage without an insulin-dependent diabetic child ($1,125 compared to $625) (Songer et al., 1997).
Faced with additional expenses from either seeing a provider or paying for medical supplies, many insured families choose to treat a condition at home or to wait and see whether the health condition resolves on its own. According to testimony from several presenters in the committee's public workshop (Appendix C), insured families with large medical expenses may be forced to choose between paying medical bills and other bills and eventually may end up in poverty.
Nonfinancial Barriers To Access
As summarized in Figure 3.1, several other factors have been found to influence utilization, including educational background and other characteristics of parents and families; racial, ethnic, and cultural factors; and the presence of special health care needs. Public health risks as well as structural and organizational characteristics of the health care system also can reduce access to care.
|
If you step back and take an overview of this issue of worrying about coverage, the debate over Medicaid versus tax credits and incentives for people to buy their own insurance is curious. For thirty or forty years, we have known that if you really want to change health status, the surefire way to do it is to increase personal disposable income, improve education, improve nutrition, and make sure people have safe and affordable housing. From a public health perspective, direct access to health care services would come in fifth. Carl Schramm Greenspring Advisors, Inc., Towson, MD Public Workshop, June 2, 1997 |
Parental and Family Characteristics
Children depend on their parents, family members, and other caretakers to determine when they need care and to seek care on their behalf. Studies have shown that several characteristics of parents and families can reduce children's access to care. These include low levels of parental education (Newacheck,
1992; Short and Lefkowitz, 1992; Woodward et al., 1988), an inability to read outreach and other health-related materials (Riportella-Muller et al., 1996), and a lack of skills related to care taking, including a lack of knowledge about prevention and health care needs (Margolis et al., 1995; Newacheck, 1989; Riportella-Muller et al., 1996). Routine preventive services are sometimes neglected for children with chronic health problems and special health care needs (Riportella-Muller et al., 1996).
Low-income parents may be more likely to experience logistical difficulties in arranging care, such as a lack of transportation and lack of a telephone to arrange appointments (Fossett et al., 1992). Regardless of income, parents may have trouble arranging health care appointments because of a lack of child care for siblings or other family members (Riportella-Muller et al., 1996) and difficulty in taking time off from work (Riportella-Muller et al., 1996; Wolfe, 1980).
Family structure also relates to health care access. With the exception of children of young teenage mothers who live with their own mothers (Short and Lefkowitz, 1992), first-born children, only children, and younger children tend to have more outpatient visits (Cafferata and Kasper, 1985; Horwitz et al., 1985; Newacheck, 1992).
Parental health problems or other personal problems and family crises also can compete with children's health care needs as priorities for parental attention (Riportella-Muller et al., 1996). Families who have health and social problems may be less likely to seek health care for a child when it is needed.
Race, Ethnicity, and Cultural Factors
In the increasingly diverse U.S. society, the influences of racial, ethnic, and cultural factors on access to care are gaining a greater degree of recognition. Several studies have shown that nonwhite children have fewer physician visits than white children (Cornelius, 1993; Newacheck, 1992; Wolfe, 1980), independent of the need for care (Horwitz et al., 1985; Riley et al., 1993). Even with insurance coverage, minority adolescents have fewer visits to physicians, are less likely to have a usual source of care, and lack continuity of care in comparison with non-Hispanic white adolescents (Lieu et al., 1993).
Black and Hispanic children are more likely to live in poverty (46.4 percent of black and 39.7 percent of Hispanic children) than white children (12.2 percent). They are also more likely than white children to be uninsured (15.3 percent of black children and 26.8 percent of Hispanic children compared with 10.5 percent of white children in 1995 (see Figure 2.5).
Compared with the distribution of racial and ethnic groups in the U.S. population, there is a shortage of African-American, Hispanic, and Asian-American physicians and other health professionals (Lewin-Epstein, 1991). Health care services are often located outside of a racial or ethnic neighborhood. In areas where there is segregation or racial tension, this may increase an individual's reluctance to seek care outside of the neighborhood (Fossett et al., 1992).
Children with asthma are more likely to require hospitalization (an indicator of ineffective outpatient care) if they are poor, black, or Hispanic, and the outcomes of treatment are often worse (Carr et al., 1992; Perrin et al., 1989; Wissow et al., 1988). For example, a study in New York City found that poor black and Hispanic children who were hospitalized for asthma were three to six times more likely than white children to die from the episode, and also tended to come from lower-income families than the white children (Carr et al., 1992).
Cultural factors also influence care-seeking behaviors. A study of African Americans, Mexican Americans, Puerto Ricans, and non-Hispanic whites in poor areas of Chicago found that African Americans tended to use hospital-based facilities, while Mexican Americans were the least likely of all the groups to have a regular source of care, in large part because of social and cultural barriers such as language and immigration status (Lewin-Epstein, 1991). Hispanics with traditional health beliefs and health care practices may not perceive a need for health care, especially for preventive interventions (Andersen et al., 1986). Southeast Asians who believe in the inevitability of suffering and the
acceptance of a predetermined time of death are less likely to seek care (Hoang and Erickson, 1985; Uba, 1992).
Language and other communication difficulties between families and providers can increase dissatisfaction with care and decrease the likelihood that the family will seek care again (Malach and Segal, 1990; Uba, 1992). Spanish-speaking asthmatics whose clinicians did not speak Spanish were found to be less likely to come to follow-up appointments, less likely to take medications appropriately, and more likely to use an emergency department (Manson, 1988).
Changes in the health care system can reduce the racial, ethnic, and cultural differences in the patterns of care. For example, after barriers to care were reduced through 24-hour availability of care and limiting the waiting time for appointments, a Baltimore study found that the use of health care became more comparable for black and white children (Orr et al., 1984, 1988). Similarly, when language and income barriers were minimized, urban Mexican American and white elementary-school children no longer differed in their use of health care services (Gilman and Bruhn, 1981).
There is growing recognition of the importance of including culturally competent health care as a measure of health care quality (IOM, 1997; Lavizzo-Mourey and Mackenzie, 1996). HEDIS 3.0 (Healthplan Employer Data and Information Set), the most widely used set of performance measures for managed care organizations, includes ''availability of language and interpretation services" as a measure of access to care. Many professional organizations are developing training programs to increase providers' ability to meet the needs of patients from diverse backgrounds (AAPCHO, 1994; AMA, 1994; Tirado, 1995).
Organizational and Systems Barriers to Access
Many aspects of the health care system also can decrease children's access to care. Waiting time for available appointments, lack of 24-hour availability of physicians, travel time, waiting room time, and actual processing time for patients can present significant barriers to seeking and receiving care (Fossett et al., 1992; Riportella-Muller et al., 1996).
For families living in underserved urban or rural areas, access to qualified providers can be even more difficult because provider shortages limit the number of available appointments (Fossett et al., 1992; St. Peter et al., 1992). For example, a study in Chicago found that pediatricians in inner-city residential areas cared for almost twice as many children as pediatricians located in the most prosperous areas (Fossett et al., 1992).
|
We tend to look at this health insurance or access issue as the end product. It really isn't. The end product is really better outcomes for kids. So health insurance becomes one piece of a broader social and public health safety net that we ought to be thinking about for kids. Patrick Chaulk Annie E. Casey Foundation, Baltimore, MD Public Workshop, June 2, 1997 |
As discussed throughout this report, managed care is changing the delivery of American health care. There are relatively few studies of the impact of managed care on children's access to care, and the results are decidedly mixed. For example, there is some evidence that children are more likely to receive preventive services when they are enrolled in managed care plans than when they have traditional indemnity insurance (Carey et al., 1990; Szilagyi et al., 1990). However, studies in the early 1990s
showed that children with special health care needs had difficulties obtaining access to inpatient hospitalization and to specialty pediatric providers in managed care organizations (Cartland and Yudkowsky, 1992; Halfon et al., 1995; Hughes et al., 1995; Newacheck et al., 1994). In recent years, health plans have begun to implement programs specifically for children with special health care needs, often in partnership with public health clinics (AAHP, 1997). It will be important to evaluate the impact of these newer disease management programs in improving access to care.
Access to What? Defining Necessary Health Services
As a matter of principle, the committee believes that all children should have appropriate access to coordinated, effective, and child-appropriate care, including the following health care services:
- generally accepted preventive services for health promotion and disease prevention (anticipatory guidance, health supervision, or maintenance);
- acute care for immediate short-term illnesses and injuries;
- ongoing care for children with chronic medical conditions (e.g., diabetes mellitus, cerebral palsy, and muscular dystrophy);
- rehabilitative care, including allied health services, for children with disabilities; and
- care for children with special needs (e.g., speech disorders).
As shown in Figure 3.6 and Table 3.3, the cost of preventive or "well care" visits is a small proportion of all money spent on health care. The committee believes that a comprehensive scope of benefits with an increased emphasis on prevention is especially important for children because of their developmental needs.
However, scientific evidence and professional consensus do not give clear indications for specific diagnostic tests, treatments, procedures, drugs, specialists, and other services to which children should have access. This is true for all of medical care, but especially for children, in the committee's view. Professional organizations, parents, and purchasers of care have different attitudes and positions about which services are essential for children, and there are many areas of disagreement and uncertainty. Parents, insurers, and policymakers also may have different views on whether a given expenditure is reasonable, but some priorities must be set if payers and policymakers are to be able to make reasoned and equitable decisions in the face of limited resources (Klein et al., 1996).
A complete analysis or comparison of benefit structures for comprehensive care for children would be beyond the scope of this study. However, Boxes 3.1 to 3.3 summarize three approaches to defining recommended services for children. These are the recommendations of a previous Institute of Medicine committee, the National Forum on the Future of Children and Families; the U.S. Preventive Services Task Force guidelines; and the health care services recommendations of the American Academy of Pediatrics. Box 3.4 summarizes the health care benefits allowed under SCHIP.
|
Preventive care is important. Immunizations are important. The health of our children is just as important as the education of our children. It is something we value. Charles LaVallee Western Pennsylvania Caring Foundation for Children, Pittsburgh, PA Public Workshop, June 2, 1997 |
Implications
Evidence is clear that uninsured children receive fewer health care services than children who have insurance coverage. Compared with children who have insurance coverage, uninsured children have fewer visits to physicians, are less likely to be seen by physicians when they are sick or injured, and are less likely to receive adequate preventive services, including immunizations.
Untreated illnesses and injuries can have long-term-even lifelong-consequences. For example, untreated ear infections can lead to hearing loss or deafness. Children who are unable to hear well can have trouble performing well in school and trouble interacting normally with their families and friends. Language or other developmental delays due to untreated neurological problems also can frustrate normal development and social interactions.
Although children who are uninsured have less access to care, it is important to recognize that the presence of insurance alone will not eliminate all of the barriers to accessing appropriate health care services. Children are dependent on their parents to identify problems and seek treatment, and even insured and responsible parents may delay seeking care because of the cost of the out-of-pocket expenses or because it is difficult or inconvenient to schedule appointments. Delays in ambulatory care because of cost may result in diagnosis or treatment later in the course of illness or disease, when treatment may be more complex and more expensive.
Some aspects of the health care system also can create barriers to access, particularly the shortages of providers to serve low-income groups, lack of cultural sensitivity, and inconvenient scheduling. With an increasing emphasis on the quality of care, it is likely that some of these aspects will begin to change over time.
In the meantime, health insurance expansions for children should emphasize benefits that include preventive services and age-appropriate interventions. With health insurance, children are more likely to experience healthy physical and emotional growth, development, and overall health and well-being. Without insurance, their health care needs are far more likely to go unmet.
|
If we get all kids covered, that is not going to solve all of their health problems, but it is going to make solving them a lot easier. John McDonough Massachusetts Legislature, Boston, MA Public Workshop, June 2, 1997 |
WELL CARE ACCOUNTS FOR LESS THAN 4 PERCENT OF HEALTH CARE COSTS
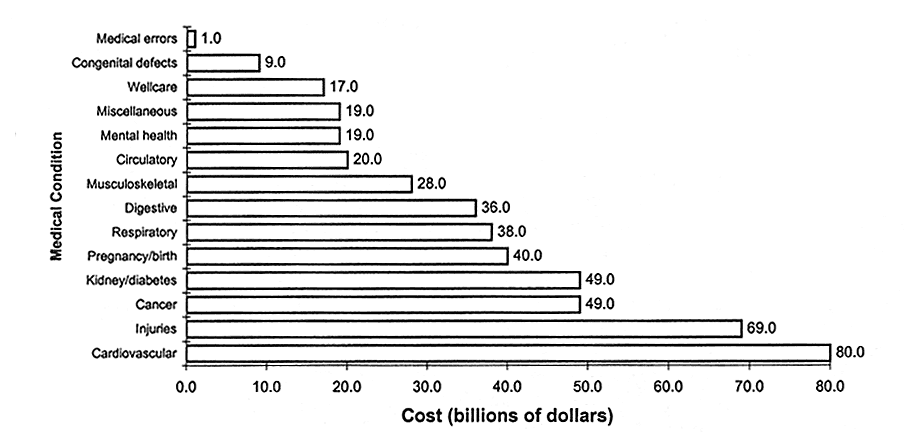
FIGURE 3.6
Drivers of health care dollars, United States, 1993. Miscellaneous includes anemia, unconsciousness, headache, and hormonal disorder other than diabetes. Data from the National Health Interview Survey. Source: Adapted from HIAA (1997, p. 86).
TABLE 3.3 Drivers of Health Care Dollars, United States, 1993.
|
BOX 3.1 Benefits Recommended by the National Forum on the Future of Children and Families
|
1.
| Preventive health services
|
*
| comprehensive prenatal, delivery, and postpartum care, emphasizing continuous risk assessment in pregnancy, education and intervention when problems are detected;
|
*
| regular, routine preventive health care from birth through adolescence, including immunizations, anticipatory guidance and health education, and health screening (beginning with screening of newborns);
|
*
| family planning services and supplies; postpartum care and counseling; and other related reproductive health services; and
|
*
| preventive dental care.
|
2.
| Major medical services
|
*
| services in hospitals and other licensed health facilities, including inpatient care for acute and chronic illnesses, emergency room care, surgery (including ambulatory surgery), and anesthesia;
|
*
| services of physicians and of other licensed providers, such as certified nurse-midwives, obstetric-gynecologic, and pediatric nurse practitioners, and physicians' assistants;
|
*
| diagnostic services, including laboratory and radiology services;
|
*
| mental health and substance (alcohol and drug) abuse treatment services; and
|
*
| acute dental care and noncosmetic orthodontia.
|
3.
| Special services and supplies for persons with extensive or complex health care needs
|
*
| durable medical equipment;
|
*
| extended mental health and substance abuse services;
|
*
| home health care and nursing in specialized day care for mentally fragile children;
|
*
| nutritional services;
|
*
| recuperative stays in long-term care facilities
|
*
| hospice care;
|
*
| home visiting;
|
*
| respite care;
|
*
| coordination of care for chronically ill or high-risk individuals with special health care needs; and
|
*
| occupational, physical, and speech therapy and rehabilitation. SOURCE: Adapted from NRC and IOM, 1996, p. 13. |
|
|
BOX 3.2 U.S. Preventive Services Task Force Recommended Routine Preventive Services for Children (0-10 years)
|
||||||||||||||||||||||||||||||||
|
BOX 3.3 American Academy of Pediatrics Recommended Health Care Services for Children and Adolescents | |
|
1. |
Medical care, including: |
|
(a) |
health supervision with preventive care and immunizations, |
|
(b) |
diagnosis and treatment of acute and chronic illness, developme ntal disabilities, learning disorders. and behavioral problems. |
|
2. |
Surgical care. |
|
3. |
Mental health services. |
|
4. |
Emergency and trauma care services. |
|
5. |
Inpatient hospital services. |
|
6. |
Specialty and pediatric subspecialty consultations. |
|
7. |
Family planning services. |
|
8. |
Pregnancy services. |
|
9. |
Care of all newborns and infants: |
|
(a) |
attendance and management at high-risk deliveries, |
|
(b) |
health supervision, and |
|
(c) |
treatment of congenital anomalies and other illnesses. |
|
10. |
Laboratory and pathology services. |
|
11. |
Diagnostic and therapeutic radiology services. |
|
12. |
Anesthesia services. |
|
13. |
Rehabilitation and early intervention services (e.g., physical, speech. and occupational therapy). |
|
14. |
Home health care, private-duty nursing. |
|
15. |
Hospice care. |
|
16. |
Respite care. |
|
17. |
Long-term care at home or skilled nursing facility. |
|
18. |
Case management and care coordination. |
|
19. |
Medical and social services for suspected physical or sexual abuse or neglect. |
|
20. |
Transfer/transport to hospital or health care facility. |
|
21. |
Dental care and oral surgery. |
|
22. |
Nutritional counseling. |
|
23. |
Prescription drugs, medical and surgical supplies, corrective eyeglasses or lenses, hearing aids. and special nutritional supplements. |
|
24. |
Durable medical equipment and prostheses/braces. |
|
BOX 3.4 Services Allowed Under SCHIP States can choose to expand Medicaid or offer one of the following: (1) one of three "benchmark" packages mentioned identified in the SCHIP legislation; (2) a package actuarially equivalent to one of the benchmark packages; (3) a comprehensive benefits package under an existing child health insurance program [available only to Florida, New York, and Pennsylvania.]; or (4) another benefit package approved by DHHS, Actuarially equivalent packages must include four minimum benefits: | |
|
* |
inpatient and outpatient hospital services, |
|
* |
physicians' surgical and medical services, |
|
* |
laboratory and X-ray services, and |
|
* |
well-baby and well-child care that includes age-appropriate immunizations. |
| Equivalent coverage must have an actuarial value that is 75% of the costs of the following categories: | |
|
* |
prescription medications, |
|
* |
mental health services, |
|
* |
vision services, and |
|
* |
hearing services. |
The following are optional services: | |
|
* |
clinic services; |
|
* |
over-the-counter medications; |
|
* |
prenatal care and family planning supplies; |
|
* |
inpatient mental health services; |
|
* |
durable medical equipment and other medical devices; |
|
* |
disposable medical supplies; |
|
* |
home- and community-based services; |
|
* |
nursing-care services; |
|
* |
dental services; |
|
* |
inpatient and outpatient substance abuse treatment and services; |
|
* |
case management services; |
|
* |
care coordination; |
|
* |
physical, occupational, and speech therapy; |
|
* |
hospice care; |
|
* |
medical transportation; |
|
* |
enabling services (e.g., transportation and translation services); and |
|
* |
any other services specified by DHHS or recognized by state law and prescribed by a licensed physician or practitioner. |
| SOURCE: Johnson and McDonough, 1998. | |
References
Aday LA, Fleming GV, Anderson R. 1984. Access to Medical Care in the U.S.: Who Has It, Who Doesn't. Chicago: Pluribus Press for the University of Chicago.
AAHP (American Association of Health Plans). 1997. AAHP Fact Sheets: Chronic Care. Washington, D.C.: AAHP Medical Affairs Department.
AAPCHO (Association of Asian Pacific Community Health Organizations). 1994. Culturally Competent Health Service Delivery Under Managed Care for Asians and Pacific Islanders. Oakland, CA: AAPCHO.
AMA (American Medical Association). 1994. Culturally Competent Health Care for Adolescents: A Guide for Primary Care Providers. Chicago: AMA.
American Academy of Pediatrics Committee on Child Health Financing. 1993. Scope of Health Care Benefits for Infants, Children, and Adolescents Through Age 21 Years. Pediatrics 91:508.
Andersen RM, Giachello AL, Aday LA. 1986. Access of Hispanics to Health Care and Cuts in Services: A State-of-the-Art Overview. Public Health Reports 101:238-252.
Bloom B, Gift HC, Jack SS. 1992. Dental Services and Oral Health, United States, 1989. Vital and Health Statistics 10:183. Braveman P, Oliva G, Miller MG, Reiter R, Egerter S. 1989. Adverse Outcomes and Lack of Health Insurance Among Newborns in an Eight-County Area of California, 1982-86. The New England Journal of Medicine 330:1421-1425.
Brunelle JA. 1989. Oral Health of United States Children: The National Survey of Dental Caries in U.S. School Children, 1986-87. Bethesda, MD: National Institute of Dental Research. NIH Pub. No. 89-2247.
Butler JA, Winter WD, Singer JD, Wenger M. 1985. Medical Care Use and Expenditure Among Children and Youth in the United States: Analysis of a Probability Sample. Pediatrics 76:495-507.
Cafferata GL, Kasper JD. 1985. Family Structure and Children's Use of Ambulatory Physician Services. Medical Care 23:350-360.
Carey T et al. 1990. Prepaid versus Fee-for-Service Medicaid Plans: Effects on Preventive Health Care. Journal of Clinical Epidemiology 43:1213-1220.
Carr W, Zeitel L, Weiss K. 1992. Variations in Asthma Hospitalizations and Deaths in New York City. American Journal of Public Health 82:59-65.
Cartland JDC, Yudkowsky BK. 1992. Barriers to Pediatric Referral in Managed Care Systems. Pediatrics 89:183-192.
Center for Health Economics Research. 1993. Access to Health Care, Key Indicators for Policy. Princeton, NJ: Robert Wood Johnson Foundation.
Cornelius LJ. 1993. Barriers to Medical Care for White, Black, and Hispanic American Children. Journal of the National Medical Association 85:281-288.
DHHS (U.S. Department of Health and Human Services). 1996. Children's Dental Services Under Medicaid: Access and Utilization. Report of the Office of the Inspector General, OEI-09-93-00240. San Francisco: DHHS.
Fossett JD, Perloff JD, Kletke PR, Peterson JA. 1992. Medicaid and Access to Child Health Care in Chicago. Journal of Health Politics, Policy and Law 17:273-298.
Gilman SC, Bruhn, JG. 1981. A Comparison of Utilization of Community Primary Health Care and School Health Services by Urban Mexican-American and Anglo Elementary School Children. Medical Care 19:223-232.
Halfon N, Inkeles M, Wood D. 1995. Nonfinancial Barriers to Care for Children and Youth. Annual Review of Public Health 16:447-472.
HIAA (Health Insurance Association of America). 1997. Source Book of Health Insurance Data. Washington, D.C.: HIAA.
Hoang GN, Erickson RV. 1985. Cultural Barriers to Effective Medical Care Among Indochinese Patients. Annual Review of Medicine 36:229-239.
Holl JL, Szilagyi PG, Rodewald LE, Byrd RS, Weitzman MD. 1995. Profile of Uninsured Children in the United States. Archives of Pediatricand Adolescent Medicine 149:398-406.
Horwitz SM, Morgenstern H, Berkman LF. 1985. The Impact of Social Stressors and Social Networks on Pediatric Medical Care Use. Medical Care 23:946-959.
Hughes DC, Newacheck PW, Stoddard JJ, Halfon N. 1995. Medicaid Managed Care: Can It Work for Children? Pediatrics 95(4):591-594.
IOM (Institute of Medicine). 1993. Access to Health Care in America . Washington D.C.: National Academy Press.
IOM. 1997. Managing Managed Care: Quality Improvement in Behavioral Health. Washington, D.C.: National Academy Press.
Isman R. 1997. Dental Services in Healthy Families: Issue Paper 1. Sacramento, CA: California Department of Health Services.
Johnson K, McDonough JE. 1998. Expanding Health Coverage for Children: Matching Federal Policies and State Strategies. New York: Milbank Memorial Fund.
Kasper JD. 1987. The Importance of Type of Usual Source of Care for Children's Physician Access and Expenditures. Medical Care 25:386-398.
Klein R, Day P, Redmayne S. 1996. Managing Scarcity. Buckingham, England: Open University Press.
Kogan MD, Alexander GR, Teitelbaum MA, et al. 1995. The Effect of Gaps in Health Insurance on Continuity of a Regular
Source of Care Among Preschool-Aged Children in the United States. Journal of the American Medical Association 274(18):1429-1435.
Lavizzo-Mourey, Mackenzie ER. 1996. Cultural Competence: Essential Measurements of Quality for Managed Care Organizations. Annals of Internal Medicine 124(10):919-921.
Lewin-Epstein N. 1991. Determinants of Regular Source of Health Care in Black, Mexican, Puerto Rican, and Non-Hispanic White Populations. Medical Care 29(6):543-557.
Lewit EM, Monheit AC. 1992. Expenditures on Health Care for Children and Pregnant Women. The Future of Children 2(2):95-114.
Lewit EM, Kerrebrock N. In press. Dental Indicators: The Future of Children.
Lieu TA, Newacheck PW, McManus MA. 1993. Race, Ethnicity, and Accessto Ambulatory Care Among U.S. Adolescents . American Journal of Public Health 83(7):960-965.
Malach RS, Segal N. 1990. Perspectives on Health Care Delivery for American Indian Families. Children's Health Care 19:219-228.
Manson A. 1988. Language Concordance as a Determinant of Patient Compliance and Emergency Room Use in Patients with Asthma. Medical Care 26:1119-1128.
Margolis PA, Carey T, Lannon CM, Earp JL, Leininger L. 1995. The Rest of the Access-to-Care Puzzle: Addressing Structural and Personal Barriers to Health Care for Socially Disadvantaged Children. Archives of Pediatric and Adolescent Medicine 149:541-545.
Monheit AC, Cunningham PJ. 1992. Children Without Health Insurance. The Future of Children 2(2):154-170.
NCHS. 1996. Healthy People 2000 Review 1995-96. Hyattsville, MD: Public Health Service. DHHS Pub. No. PHS 96-1256.
NCHS. 1997a. Access to Health Care Part 1: Children. Vital and Health Statistics, Series 10, No. 196. Hyattsville, MD: NCHS.
NCHS. 1997b. National Hospital Ambulatory Medical Care Survey: 1995, Emergency Department Summary. Prepared by Stussman BJ. Advance Data from Vital and Health Statistics, No. 285. Hyattsville, MD: NCHS.
NCHS. 1997c. Health, United States 1996-1997 and Injury Chartbook. Washington, D.C.: U.S. Government Printing Office.
Newhouse JP and the Insurance Experiment Group. 1993. Free for All? Lessons from the RAND Health Insurance Experiment. Los Angeles: RAND.
NRC and IOM (National Research Council and Institute of Medicine). 1996. Including Children and Pregnant Women in Health Care Reform, pp. 1-32. Paying Attention to Children in a Changing Health Care System: Summaries of Workshops. Washington, D.C.: National Academy Press.
Newacheck PW. 1989. Improving Access to Health Services for Adolescents from Economically Disadvantaged Families. Pediatrics 84(6):1056-1063.
Newacheck PW. 1992. Characteristics of Children with High and Low Usage of Physician Services. Medical Care 30(1):30-41.
Newacheck PW, Halfon NH. 1988. Preventive Care Use by School-Aged Children: Differences by Socioeconomic Status. Pediatrics 82:462-468.
Newacheck PW, Hughes DC, Stoddard JJ. 1996. Children's Access to Care: Differences by Race, Income, and Insurance Status. Pediatrics 97(1):26-32.
Newacheck PW, Hughes DC, Cistemas M. 1995. Children and Health Insurance: An Overview of Recent Trends. Health Affairs 14(1):244-254.
Newacheck PW, Hughes DC, Stoddard, JJ, Halfon N. Children With Chronic Illness and Medicaid Managed Care. 1994. Pediatrics 93:497-500.
Newacheck PW, Stoddard JJ, Hughes DC, Pearl M. 1997. Children's Access to Health Care: The Role of Social and Economic Factors. In Stein REK, ed. Health Care for Children: What's Right, What's Wrong, What's Next. New York: United Hospital Fund.
Orr ST, Charney E, Straus J. 1988. Use of Health Services by Black Children According to Payment Mechanism. Medical Care 26:939-947.
Orr ST, Miller CA, James SA. 1984. Differences in Use of Health Services by Children According to Race. Medical Care 22: 848-853.
Overpeck MD, Kotch JB. 1995. The Effect of U.S. Children's Access to Care on Medical Attention for Injuries. American Journal of Public Health 85:402-404.
Perrin JM, Homer CJ, Berwick DM, Woolf AD, Freeman JL, Wennberg JE. 1989. Variations in Rates of Hospitalizations of Children in Three Urban Communities. The New England Journal of Medicine 320:1183-1187.
Riley AW, Finney JW, Mellits ED, et al. 1993. Determinants of Children's Health Care Use: An Investigation of Psychosocial Factors. Medical Care 31:767-783.
Riportella-Muller R, Selby-Harrington ML, Richardson LA et al. 1996. Barriers to the Use of Preventive Health Care Services for Children. Public Health Reports 111:71-77.
Rosenbach ML. 1989. The Impact of Medicaid on Physician Use by Low-Income Children. American Journal of Public Health 79:1220-1226.
St. Peter RF, Newacheck PW, Halfon N. 1992. Access to Care for Poor Children: Separate and Unequal? Journal of the American Medical Association 267:2760-2764.
Short P, Lefkowitz D. 1992. Encouraging Preventive Services for Low-Income Children: The Effect of Expanding Medicaid. Medical Care 30:766-780.
Songer TJ, LaPorte RE, Lave JR, et al. 1997. Health Insurance and the Financial Impact of IDDM in Families with a Child with IDDM. Diabetes Care 20:577-584.
Stoddard JJ, St. Peter R, Newacheck P. 1994. Health Insurance Status and Ambulatory Care for Children. The New England Journal of Medicine 330:1421-1425.
Szilagyi PG et al. 1990. The Effect of Independent Practice Association Plans on Use of Pediatric Ambulatory Medical Care in One Group Practice. Journal of the American Medical Association 263(16):2198-2203.
Tirado MD. 1995. Tools for Monitoring Cultural Competence in Health Care. San Francisco: Latino Coalition for a Healthy California.
Uba L. 1992. Cultural Barriers to Health Care for Southeast Asian Refugees. Public Health Reports 197:544-548.
United States Preventive Services Task Force. 1996. Guide to Clinical Preventive Services (2nd ed.). Baltimore: Williams & Wilkins.
Valdez RB, Brook RH, Rogers W et al. 1985. Consequences of Cost-Sharing for Children's Health. Pediatrics 75:952-961.
Wissow L, Gittelshon AM, Szklo M, Starfield B, Mussman M. 1988. Poverty, race, and hospitalization for childhood asthma. American Journal of Public Health 78:777-782.
Wolfe BL. 1980. Children's Utilization of Medical Care. Medical Care 18:1196-1207.
Wood D, Hayward R, Corey C, et al. 1990. Access to Medical Care for Children and Adolescents in the United States. Pediatrics 86:666-673.
Woodward CA, Boyle MH, Offord DR, et al. 1988. Ontario Child Health Study: Patterns of Ambulatory Medical Care and Their Correlates. Pediatrics 82:425-434.