| This page in the original is blank. |
4
Safety Net Providers
Definition Of Safety Net
For the purposes of this report, safety net providers can be described by any of the following:
- A substantial proportion of the care they provide is for individuals who lack insurance coverage and who cannot afford to pay for care themselves.
- They rely primarily on Medicaid and Medicare revenues and charitable sources of funds.
- They offer specialized or essential health services not generally offered by other providers, including intensive medical services for indigent individuals (e.g., people with HIV and AIDS); public health services, such as health education; and support services, such as transportation, translation services, child care, and other services.
In general, the safety net includes the following groups of providers:
- hospitals (public, children's, teaching, and community hospitals serving low-income individuals),
- community and migrant-worker health centers,
- health services programs for homeless children and adults,
- local public health departments providing clinical services,
- school-based clinics,
- some home health agencies, and
- some individual primary care practitioners in private practice.
The safety net is not an organized national entity, but rather a composite of different agencies, organizations, and individuals in each community across the country (Baxter and Mechanic, 1997). The mix of financing, concentration of organizational responsibility for care for low-income and uninsured groups, and the demand for uncompensated care are different in every community. The mix of services also differs depending on the community's provider base, its commitment to serving low-income and uninsured groups, and individual providers' ability to participate.
This chapter of the report describes the sources and amounts of financing for safety net providers and then describes the general utilization rates and patterns for four types of safety net providers: community health centers, children's hospitals, health departments, and school-based health centers. The chapter
also describes some of the most significant budgetary and other challenges to safety net providers in the late 1990s, including changes in the structure and delivery of Medicaid.
Sources Of Funding For Safety Net Providers
For several decades, safety net providers have helped to increase access to primary and preventive health care for underserved and vulnerable people who experience financial, geographic, or cultural barriers to care. Groups served by safety net providers include uninsured children and adults, homeless families and individuals, migrant farmworkers, adolescents, people who live in rural and frontier areas, residents of public housing, and others (HRSA, 1997a).
Over the past 30 years, the federal government and several states have taken legislative and other steps to build the health care infrastructure supporting safety net providers in underserved areas. Typically, funding for these providers comes from a blend of public and private funding streams that subsidize free or low-cost care. Public sources of funding may include the Medicaid program, federal and state service delivery and research grants, local tax dollars, and state uncompensated care pools. Private sources may include foundations and philanthropic organizations, charities (e.g., hospitals whose missions include serving patients regardless of health insurance coverage or ability to pay), and other sources that are not part of an organized philanthropic funding program (e.g., individual donations).
|
I worry about the whole collapse of any sort of safety net for families and kids. We have hospitals being converted from not-for-profit to for-profit, which eliminates emergency room obligations. Community health centers are under an enormous squeeze in trying to deal with increasing numbers of uninsured families. Federal and state dollars flowing to local health departments and local providers have decreased, and managed care is taking some Medicaid dollars out of health departments and moving people into different systems. These are complex changes which need to be addressed because they affect people in very real terms on a daily basis. Patrick Chaulk Annie E. Casey Foundation, Baltimore, MD Public Workshop, June 2, 1997 |
Until recently, cost-shifting allowed many mainstream providers serving the general population to offset the costs of uncompensated care. As purchasers have turned to managed care for cost savings, the cross-subsidies and excess revenue sources that could support uncompensated care are disappearing. Purchasers have been negotiating deep discounts in contracts with mainstream hospitals and group practices, forcing those who formerly provided care for uninsured individuals to refer these patients to safety net providers. Uncompensated care costs are becoming more concentrated among fewer hospitals and other traditional safety net providers, and there also is a significant increase in the amount of uncompensated care provided by individual physicians (Cunningham and Ha, 1997).
Table 4.1 presents the main sources of public funding for safety net providers up to 1996. These figures represent total federal funding amounts; matching funds from the states and age-specific breakdowns were not available.
After Medicaid, discussed in Chapter 5, the largest source of funding in the past has been Disproportionate Share Hospital (DSH) payments. Because of concerns that DSH funds were not all being used to provide care for uninsured and low-income individuals, these payments were significantly reduced by the Balanced Budget Act of 1997.
TABLE 4.1 Sources and Amounts of Funding for Selected Safety Net Programs in Health Services, United States, 1992-1995 Program
|
|
Source of Funding |
|
Total Funding (in millions of dollars) |
||||
|
|
Federal |
State |
Local |
1992 |
1993 |
1994 |
1995 |
|
Medicaid1 |
√ |
Ö |
NA |
115,200 |
127,400 |
137,100 |
151,300 |
|
Medicaid DSH2 |
√ |
Ö |
|
17,526 |
17,016 |
16,890 |
18,990 |
|
Medicare DSH3 |
|
|
|
2,200 |
2,700 |
3,400 |
3,800 |
|
Supplemental Nutrition Program for Women Infants, and Children4 |
√ |
NA |
NA |
2,566 |
2,820 |
3,160 |
3,451 |
|
Bureau of Primary Health Care Programs5 |
√ |
Ö |
Ö |
1,698 |
1,798 |
1,99 |
2,507 |
|
Community health centers, migrant health centers, health care for the homeless, public housing primary care |
|
|
|
|
|
|
|
|
Title V Maternal and Child Health Care Services block granta,6 |
√ |
Ö |
Ö |
547 |
552 |
575 |
572 |
|
Vaccines for Children7 |
√ |
NA |
NA |
280 |
|||
|
NOTE: All programs are administered by the U.S. Department of Health and Human Services. NA = not applicable. a Federal grants only; state matches not available. b Program not in existence SOURCES: 1 Kaiser Commission on the Future of Medicaid (1997); 2 The Urban Institute (1997) (calculations based on data from Health Care Financing Administration Form 64); 3 ProPAC (1997); 4 U.S. House of Representatives, Committee on Ways and Means (1996); 5 HRSA/BPHC (1997a); 6 HRSA/MHCB (1997b); 7 CDC (1997). |
|||||||
Disproportionate Share Hospital Payments
When DSH payment provisions were enacted, they were intended to offset the costs of uncompensated care provided by community hospitals and other hospitals caring for a disproportionate share of low-income individuals, including uninsured patients and patients covered by Medicaid. Because Medicaid's reimbursement levels were low and because these hospitals also tended to serve few privately insured individuals, they were unable to shift or otherwise subsidize the costs of uncompensated care.
From the late 1980s to the mid-1990s, the number of uninsured individuals increased and the total costs of uncompensated care climbed steadily (see Figure 4.1, Table 4.2). After passage of OBRA (Omnibus Budget Reconciliation Act) 1987 DSH provisions, DSH payments grew from approximately $400 million in 1988 to $19 billion in 1995, with the federal government's share of these payments in 1995 approaching $11 billion (Holahan et al., 1997).
The DSH funds, however, have not always been targeted to hospitals serving low-income individuals. Rather than helping safety net hospitals solve their financial problems, some states used the DSH funding to substitute for other state expenditures through intergovernmental transfers and other methods (Holahan et al., 1997). Only about two-thirds of the funding reached safety net hospitals (Coughlin and Liska, 1997; Ku and Coughlin, 1995).
Congress capped DSH payments at 12 percent of Medicaid program expenditures in 1991. In the Balanced Budget Act of 1997, future federal funding for DSH was reduced by a projected $10 billion. The savings helped Congress to finance part of the $24 billion in allocations set aside over five years for states to implement children's insurance programs (the State Children's Health Insurance Program, or SCHIP). A limited amount of SCHIP funding (up to 10 percent) may be spent on administrative costs, outreach, provider subsidies (including safety net), and direct services. Although safety net providers believe that efforts to increase the number of insured Americans are essential, these efforts are unlikely to eliminate the need for subsidies for the uninsured. Even if SCHIP is fully implemented, millions of children will remain uninsured, and the numbers of uninsured adults are likely to continue to increase.
For example, the Congressional Budget Office has estimated that states' efforts under SCHIP could result in fewer than 2 million newly-insured children by 1999, far below the 11 million children who were estimated to be uninsured in 1996. Moreover, at current rates, more than 2 million currently insured individuals will lose coverage between now and 1999. As commercial payers continue to negotiate severely discounted payment rates, mainstream providers may be forced to reduce or eliminate charity care. Thus, the availability of care for the increasing numbers of uninsured children and adults will be further concentrated among safety net providers.
Community Health Centers
Under Section 330 of the Public Health Service Act, community health centers (CHCs) have a congressional mandate to serve uninsured and underinsured individuals and families. More than 2,200 health center service sites deliver preventive and primary health care to more than 9 million people in underserved urban and rural communities. They adjust their charges according to a patient's ability to pay (Hawkins and Rosenbaum, 1997).
CHCs are governed by community boards and tailor their services to meet the specific needs of the communities and the special populations that they serve, including migrant and seasonal workers, homeless individuals, and people living with AIDS. Most CHCs are private, not-for-profit corporations. In addition to primary care and preventive services, they offer a comprehensive array of expanded services such as outreach, translation services, home visits, care management, and other support services (HRSA, 1997a).
In addition to the federal funds administered by the Bureau of Primary Health Care of the Health Resources and Services Administration, CHCs are supported by Medicaid, Medicare, federal grants,
UNCOMPENSATED CARE COSTS NEARLY DOUBLED FROM 1987 TO 1995
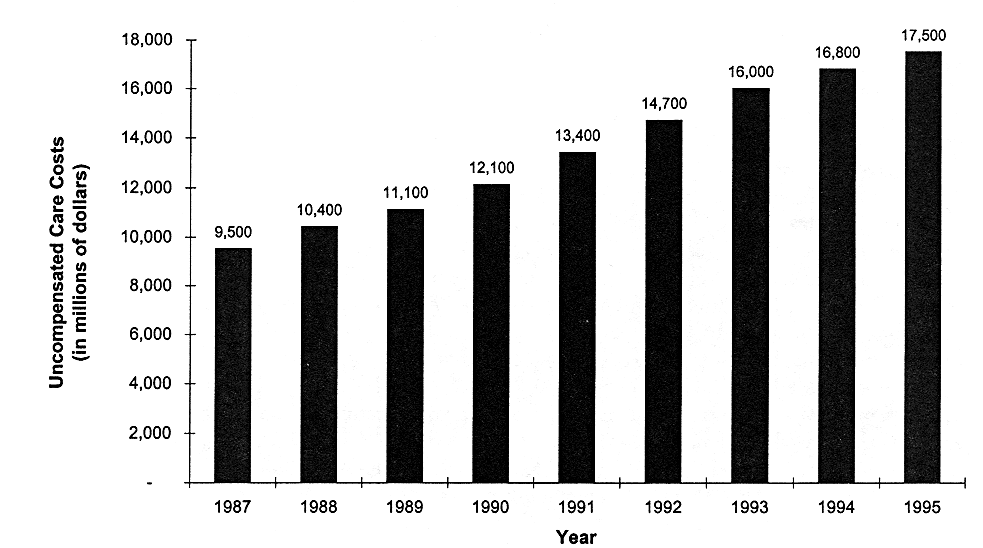
FIGURE 4.1
National cost of uncompensated care in registered community hospitals, United States, 1987-1995. SOURCE: AHA (1995).
TABLE 4.2 National Cost of Uncompensated Care for Registered Community Hospitals, United States, 1987-1995
|
Year |
Uncompensated Care Cost (in millions of dollars) |
Number of Hospitals |
|
1987 |
9,500 |
5,597 |
|
1988 |
10,400 |
5,499 |
|
1989 |
11,100 |
5,448 |
|
1990 |
12,100 |
5,370 |
|
1991 |
13,400 |
5,329 |
|
1992 |
14,700 |
5,287 |
|
1993 |
16,000 |
5,252 |
|
1994 |
16,800 |
5,206 |
|
1995 |
17,500 |
5,166 |
|
SOURCE: AHA (1995). |
||
state and local sources, private insurance payments, and patient payments (see Figure 4.2 and Table 4.3). In 1995, 3.8 million individuals-more than 40 percent of all patients served by CHCs—were uninsured. Medicaid patients accounted for more than one third (38 percent) of the patient visits to CHCs in 1995.
The number of patients served by CHCs almost doubled between 1980 and 1995 (5 million to 9.3 million) (NACHC, 1997). During the same time, the funding required to support increases in staffing levels did not keep pace, often resulting in long waits for appointments. Medicaid reimbursements for CHCs have been increasing, but the amount of grant funding provided to support innovative programs and offset the costs of uncompensated care has fallen off since 1990 (see Figure 4.3 and Table 4.4) (Hawkins and Rosenbaum, 1997).
The Balanced Budget Act of 1997 introduced provisions that will change the structure of Medicaid and make a significant impact on community health centers. Cost-based reimbursement was important to CHCs because CHC patients tend to have multiple problems and their treatment tends to be more expensive, and also because CHCs offer more expanded services than most commercial plans, including translation, case management, and other support services.
Originally, Medicaid had to reimburse 100 percent of the cost of serving Medicaid patients, although many Medicaid waivers changing the amount and structure of reimbursement were already in effect by the time the Balanced Budget Act was enacted. In 1997, Congress changed the cost-based reimbursement provisions for Federally Qualified Health Centers, including CHCs. It eliminated the minimum payment standards that states previously were required to meet in setting reimbursement rates for community health centers, as well as for hospitals and nursing homes (Schneider, 1997). By 2002, Medicaid agencies will be required to reimburse only 70 percent of CHC patient costs, and by 2003, this requirement will be completely phased out (Schneider, 1997).
In environments in which Medicaid is shifting to managed care, CHCs are seeking to be included in provider panels and networks that serve low-income individuals. Medicaid managed care is having other effects on CHCs as well. Through default enrollment mechanisms in state mandatory Medicaid managed care programs, individuals who do not go through a process of choosing a primary care provider are assigned providers automatically. If these individuals are unaware that their assigned provider is not the CHC and seek care there, Medicaid will not provide reimbursement for services provided by the center.
With such a competitive health care marketplace, it remains to be seen whether CHCs can be sustained by capturing an expanding share of Medicaid patients. The changes in Medicaid reimbursement, particularly the loss of cost-based reimbursement, reductions in federal grant support, and increases in the number of uninsured families seeking care will combine to produce significant and ongoing financial challenges.
Children's Hospitals
Because they are philosophically committed to taking care of all children regardless of their parents' ability to pay for care, many children's hospitals are described as safety net providers. There are three primary types of children's hospitals:
- freestanding children's acute-care hospitals;
- nonfreestanding units such as a pediatrics department in a larger community hospital, a distinct children's center within an academic health center, or some other model; and
- freestanding children's specialty and rehabilitation hospitals.
The United States has approximately 45 freestanding acute care children's hospitals, 222 pediatrics programs at teaching hospitals, and about 20 freestanding specialty and rehabilitation hospitals for
THE NUMBER OF MEDICAID PATIENTS DOUBLE AND THE NUMBER OF UNINSURED PATIENTS INCREASED SUBSTANTIALLY AFTER 1990
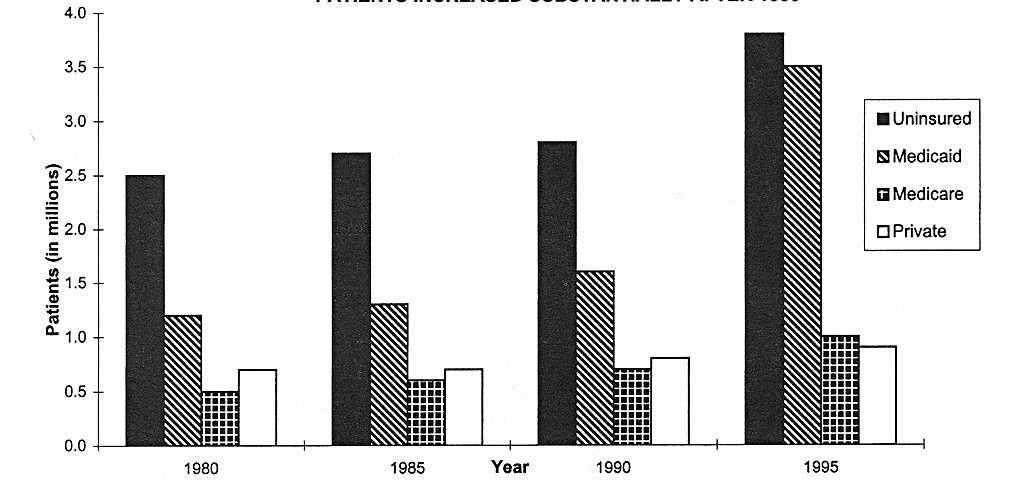
FIGURE 4.2
CHC patients by payer source, United States, selected years, 1980-1995. SOURCE: NACHC (1997).
TABLE 4.3 Insurance Status of CHC Patients, United States, Selected Years, 1980-1985
|
|
Numbers of Patients (in millions) |
|||
|
Insurance Status |
1980 |
1985 |
1990 |
1995 |
|
Uninsured |
2.5 |
2.7 |
2.8 |
3.8 |
|
Medicaid |
1.2 |
1.3 |
1.6 |
3.5 |
|
Medicare |
0.5 |
0.6 |
0.7 |
1.0 |
|
Private |
0.7 |
0.7 |
0.8 |
0.9 |
|
Total |
4,900,000 |
5,300,000 |
5,900,000 |
9,200,000 |
|
SOURCE: NACHC (1997). |
||||
THE NUMBER OF PATIENTS INCREASED WHILE GRANTS DECREASED
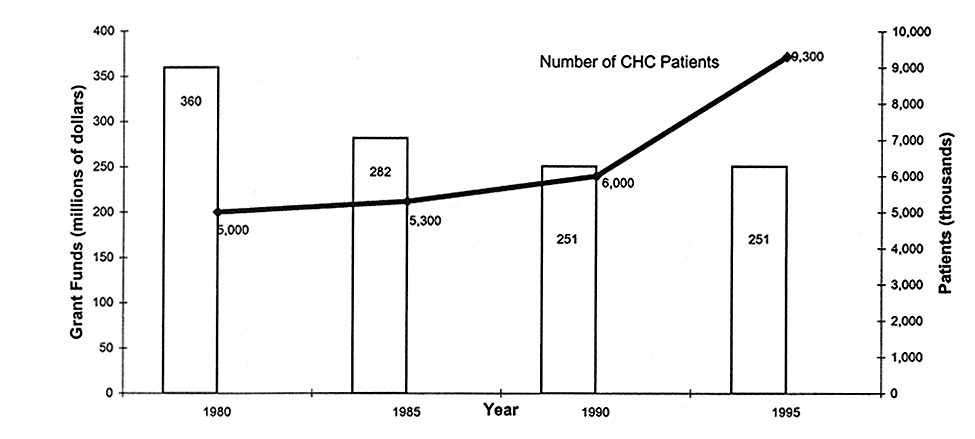
FIGURE 4.3
Community health center (CHC) federal grant funds and number of patients, United States, selected years, 1980-1995. SOURCE: NACHC (1997).
TABLE 4.4 Community Health Center (CHC) Federal Grant Funds and Number of Patients, United States, Selected Years, 1980-1995
|
Year |
Grant Funds (in millions of dollars) |
Patients (in thousands) |
|
1980 |
360 |
5,000 |
|
1985 |
282 |
5,300 |
|
1990 |
251 |
6,000 |
|
1995 |
251 |
9,300 |
|
SOURCE: NACHC (1997). |
||
children. Public financing, primarily through the Medicaid program, provides a higher proportion of revenues for the specialty and rehabilitation hospitals than for hospitals that provide acute care (Figure 4.4).
Most of the data in this section were collected by the National Association of Children's Hospitals and Related Institutions (NACHRI) and come from freestanding children's hospitals, which have their own administrative and financial reporting systems. (Data for pediatric patients from nonfreestanding units are not readily available.) Freestanding acute care children's hospitals make up only 1 percent of all hospitals in the United States, but they deliver 18 percent of inpatient days of care for children who need to be hospitalized. In 1993, they provided 3.2 million days of inpatient care at a cost of more than $7 billion, along with more than 8.3 million visits to outpatient clinics (Gage et al., 1995).
Because the developmental needs of children are better served by fewer overnight visits, outpatient and ambulatory visits are increasing as alternatives to inpatient care (Table 4.5). The increases in revenue for inpatient and outpatient care are comparable (Figure 4.5). The data also indicate that as the proportion of Medicaid patients is increasing, the proportion of uninsured patients is decreasing (Table 4.5).
Another trend for children's hospitals is the growth in regionalized pediatric medical specialty centers, or centers of excellence. Patients from a large metropolitan area, from a multi-state region, or from all over the country may be referred to these centers. A high percentage of the hospitalized children are those with chronic health problems and special health care needs such as cystic fibrosis, cerebral palsy, HIV infection, or other conditions. According to data from NACHRI, 70 to 80 percent of the hospitalizations for complex children's health conditions take place in children's hospitals or general hospitals with pediatric residency programs, which together make up only 5 percent of the total hospitals nationwide (Neff and Anderson, 1995).
Public Health Departments
In 1989, in its report entitled The Future of Public Health, the Institute of Medicine (IOM) defined the mission of public health as ''fulfilling society's interest in assuring conditions in which people can be healthy" (IOM, 1989, p. 7). The IOM report described the core responsibilities of public agencies as protecting the nation's health through the application of scientific and technical knowledge to prevent disease and to promote health. Public health agencies thus have responsibilities for the assessment, monitoring, and surveillance of health problems; for collecting information that can be used to direct resources to areas of need; and for designing and implementing programs that will improve the health of the public (IOM, 1989, 1997).
|
Title V of the Social Security Act, the maternal and child health block grant, ensures that in every state there is a unit that focuses on the health of women, children, and adolescents. Depending on your state or community, public health programs for children may be called maternal and child health, family health, or community health, but they are all involved in ensuring access to care. The dollars flow through local health departments, health centers, visiting nurses associations, school-based clinics, and other groups-whoever is out there in a community, we'll work with them. Catherine Hess National Association of Maternal and Child Health Programs, Washington,DC Public Workshop, June 2, 1997 |
REHABILITATION HOSPITALS HAVE A HIGHER PROPORTION OF PUBLIC FUNDING
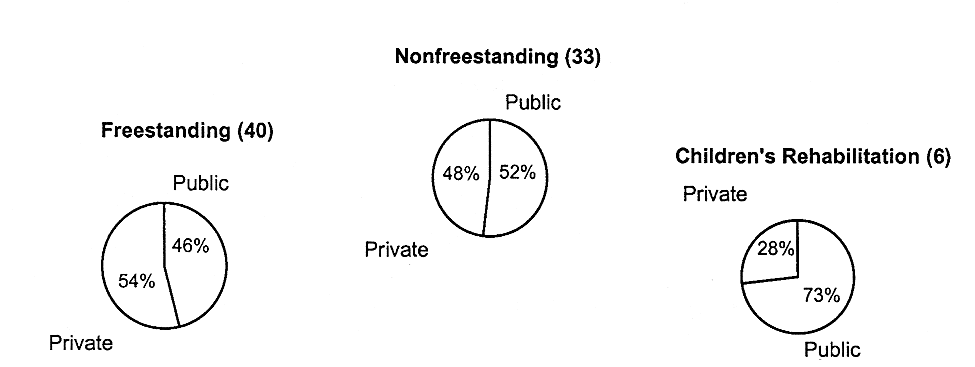
FIGURE 4.4
Percentage of revenues from public and private sources for children'shospitals, United States, 1995. Public sources include Medicaid and other state and local sources. Private includes insured and self-paying individuals.Data are based on survey responses from children's hospitals. SOURCE: NACHRI(1997).
HOSPITAL REVENUES HAVE INCREASED STEADILY SINCE 1991
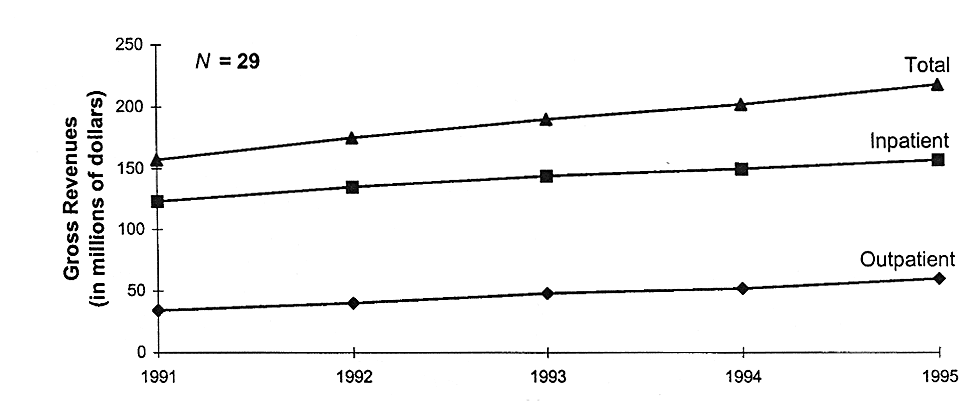
FIGURE 4.5
Average gross revenue per freestanding acute-care children's hospital, United States, 1991-1995. SOURCE: NACHRI (1997).
TABLE 4.5 Trends in Hospital Admissions, Length of Stay, and Percentage of Care Devoted to Low-Income Patients, Freestanding Children's Hospitals, United States, Selected Fiscal Years. 1990-1995
|
|
Fiscal Year |
||
|
|
1990 |
1993 |
1995 |
|
Total number of hospitals |
50 |
50 |
50 |
|
Average length of stay (days) |
6.6 |
6.4 |
5.5 |
|
Admissions |
|
|
|
|
Total no. of admissions |
422,039 |
455,015 |
458,308 |
|
Average no. of admissions per hospital |
8,441 |
9,100 |
9,166 |
|
Outpatient visitsa |
|
|
|
|
Total no. of outpatient visits |
5,769,724 |
7,424,988 |
7,841,756 |
|
Average no. of outpatient visits per hospital |
115,394 |
148,500 |
156,835 |
|
Emergency room visits |
|
|
|
|
Total no. of emergency room visits |
1,967,837 |
2,140,735 |
2,163,084 |
|
Average no. of emergency room visits per hospital |
39,357 |
42,815 |
43,262 |
|
Low-income patient care |
|
|
|
|
Average percentage of care devoted to low-incomeb patients |
40.3 |
46.7 |
47.2 |
|
Average percentage of care devoted to Medicaid patients |
34.2 |
41.4 |
44.6 |
|
Average percentage of care devoted to uninsured patients |
7.2 |
5.3 |
4.9 |
|
NOTE: Averages are based on data from 40 hospitals for all 3 years; totals are extrapolated to the industry. a Outpatient visits include emergency room visits. b Low-income patients include those with Medicaid, those who self-pay, and those who do not pay (bad debt). SOURCE: NACHRI (1997). Data are from the NACHRI annual survey of the nation's 50 freestanding children's hospitals. |
|||
State and local health departments also form an integral part of the safety net. Using funding from a variety of sources, they provide a variety of services relevant for children's health: immunizations, well-child clinics, nutrition programs, Medicaid's Early and Periodic Screening, Diagnosis, and Treatment Program (EPSDT), school-based health clinics, and other services (see Figure 4.6 and Table 4.6).
|
There are health departments that do classic public health functions, but in many areas of the country they also deliver health services, some of which are funded by Medicaid, some by state dollars, some by Title V or grant dollars or Title XX. We don't have a system in this country: we have a series of funding streams with a lot of cracks. Shelly Gehshan National Conference of State Legislatures, Washington, D.C. Public Workshop, June 2, 1997 |
PUBLIC HEALTH DEPARTMENTS RELY MOSTLY ON STATE AND LOCAL FUNDING
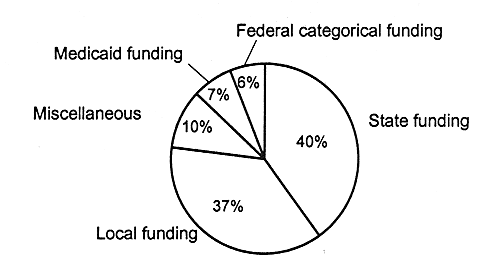
FIGURE 4.6
Sources and percentages of funding for local health departments, United States, 1992-1993. SOURCE: NACCHO, 1995.
TABLE 4.6 Percentage of City and County Health Departments Offering Selected Health Care Programs (N = 2,092), United States, 1992-1993
|
Program |
Percentage of Health Departments with Specified Program |
|
Immunizations |
96 |
|
Well-child clinic services |
79 |
|
Supplemental Nutrition Program for Women, Infants, and Children |
78 |
|
EPSDT |
72 |
|
Testing and counseling for sexually transmitted diseases |
71 |
|
Family planning services |
68 |
|
School-based health clinics |
25 |
|
SOURCE: NACCHO (1995). |
|
Efforts to analyze changes in the rates of utilization, in the characteristics of the populations served by health departments, and in the sources of financing are hampered by a lack of data. State and local health departments often have inadequate computer systems, and activities to develop reporting systems or performance measures are generally underfunded (IOM, 1989, 1997). Thus, health departments often cannot track patients within their own systems; for example, they may not be able to identify whether a patient has already been seen at a clinic in another location in the city or county.
Moreover, as for all safety net providers, continuity of care is often difficult to maintain because of the geographic mobility of these patients. It is not uncommon for low-income patients to move frequently and to have no telephone, so it may not be possible to send appointment reminders or to schedule follow-up visits.
Health departments face many challenges in their role as safety net providers. Although they play a large role in meeting the national health goals set out in Healthy People 2000, health departments continue to face cuts in funding. Many are shifting from the provision of direct services to contracting
with managed care organizations in the hope of achieving cost savings (Lipson and Naierman, 1996). Other health departments are seeking to form networks with CHCs, public hospitals, and other traditional safety net providers so that they can continue to serve their traditional patient populations.
School-Based Health Centers
During the 1995-1996 school year, more than 900 school-based health centers provided care to children and adolescents. According to a national survey, 65 percent of the centers delivered both primary and mental health care, with the remaining 35 percent providing primary care only (Making the Grade, 1997). Most centers have multidisciplinary teams of nurse practitioners, clinical social workers, physicians, and other health professionals working cooperatively with school nurses, athletic coaches, counselors, teachers, and school administrators to help the health center become an integral part of the school's activities.
School-based health centers operate in 43 states and the District of Columbia. Nationally, the majority (43 percent) are in the northeastern and mid-Atlantic states. The 10 states with the largest number of centers are New York, Florida, Texas, Connecticut, Pennsylvania, Maryland, California, Massachusetts, Michigan, and Arizona.
State governments are a primary source of financial support for these centers. In 1995-1996, 34 states allocated $41.9 million in state and federal block grant funds, which was an increase of 8 percent from 1994. The primary sources of these funds included Maternal and Child Health Block Grants and state categorical sources. Other sources of federal support are the Preventive Health Block Grant and funds provided through the Drug-Free Schools and Communities Act. Support also is provided through Medicaid, although that amount has not been tracked.
The centers are located in all types of schools. High schools are the primary sites, housing 41 percent of all centers; 32 percent are in elementary schools, and 17 percent are in middle schools. Studies have shown that the students who use school-based health centers are similar in gender, ethnicity, and age to the rest of the school population (McCord et al., 1993) although they are more likely to be uninsured (Kisker and Brown, 1996).
Implications
In a market-driven health care system, the impact of providing unreimbursed or partially reimbursed care is profound. No managed care organization will compete to care for uninsured individuals, and government subsidies to care for low-income and uninsured individuals are generally being reduced.
Uncompensated care costs are not generally broken down by age group, but the number of uninsured children has been increasing steadily for several years. With the new children's health insurance programs initiated through the Balanced Budget Act of 1997, states that increase their Medicaid eligibility thresholds and otherwise subsidize coverage for previously uninsured children can raise the rates of insurance coverage and thus reduce the burden of providing uncompensated care among safety net providers. However, in order for SCHIP funds to make significant reductions in the numbers of uninsured children, states must draw down all of the available funds, actively pursue effective outreach and enrollment strategies, and also minimize the risk of replacing existing private coverage.
Over the next several years, it will be important to measure the extent to which the new children's health insurance programs alleviate the pressure on other sources of funding for uncompensated care. Unless better data systems are developed, with more consistent age breakdowns, this will be extremely difficult to measure. Thus, the advent of the SCHIP program offers a unique opportunity to track and measure changes in the number of uninsured children and to assess the program's effectiveness from its onset. Lessons learned from the evaluation of the program will have important implications for the likelihood and nature of future insurance expansions.
The lack of consistent data also could limit the evaluation of changes in SCHIP funding in terms of
their impact on safety net providers. Not all safety net providers will be able to make a successful transition to the competitive health care marketplace. Success may be based on the degree to which providers can offer and market strong primary care services, can compete for Medicaid managed care contracts, and can negotiate payment arrangements that not only cover their costs but also contribute to their financial health.
References
AHA (American Hospital Association). 1995. Annual Survey Data, 1980-1995. Chicago: AHA.
Baxter RJ, Mechanic RE. 1997. The Status of Local Health Care Safety Nets. Health Affairs 16(4):7-23.
CDC (Centers for Disease Control and Prevention). 1997. National Immunization Program. Atlanta: CDC.
Coughlin TA, Liska D. 1997. The Medicaid Disproportionate Share Hospital Payment Program: Background and Issues. Washington, D.C.: Urban Institute. [http://newfederalism.urban.org/html/anfl 4.html]
Cunningham PJ, Ha TT. 1997. A Changing Picture of Uncompensated Care. Health Affairs 16(4):167-175.
Gage LS, Hawkins D, Willson PD, Finerfrock B. 1995. America's Essential Providers: The Foundation of Our Nation's Health Systems. Alexandria, VA: National Association of Children's Hospitals and Related Institutions.
Hawkins DR, Jr., Rosenbaum S. 1997. The Challenges Facing Health Centers in a Changing Health care System. In The Future U.S. Health care System: Who Will Care for the Poor and Uninsured? Edited by S. Altman, U. Reinhardt, and A. Shields. Chicago, IL: Health Administration Press.
Holahan J, Wiener JM, Liska D. 1997. The Medicaid Reform Debate in 1997 Washington, D.C.: The Urban Institute. HRSA (Health Resources and Services Administration). [http://newfederalism.urban.org]
HRSA (Health Resources and Services Administration). 1997a. Bureau of Primary Health Care in 1997. [http:// www\.bphc.hrsa.dhhs.gov/bphc.map ?112,190]
HRSA. 1997b. Data provided to the Institute of Medicine by the office of Larry Dickson, Maternal and Child Health Bureau. Personal Communication.
Institute of Medicine (IOM). 1989. The Future of Public Health. Washington D.C.: National Academy Press.
IOM. 1997. Improving Health in the Community: A Role for Performance Monitoring. Washington, D.C.: National Academy Press.
Kaiser Commission on the Future of Medicaid. 1997. The Medicaid Program at a Glance. Washington, D.C.: Kaiser Commission on the Future of Medicaid.
Kisker EE, Brown RS. 1996. Do School-Based Health Centers ImproveAdolescents' Access to Health Care, Health Status, and Risk-taking Behavior? Journal of Adolescent Health 18:335-343.
Ku L, Coughlin TA. 1995. Medicaid Disproportionate Share and Other Special Financing Programs. Health Care Financing Review 16(3):27-54.
Lipson DJ, Naierman N. 1996. Effects of Health System Changes on Safety Net Providers. Health Affairs 15(2):33-48.
Making the Grade. 1997. National Survey of State SBHC Initiatives, School Year 1995-96. Washington, D.C.: The George Washington University.
McCord MT, Klein JD, Joy JM, Fothergill K. 1993. School-Based Clinic Use and School Performance. Journal of Adolescent Health 14:91-98.
NACHRI (National Association of Children's Hospitals and Related Institutions). 1997. Annual Report on Utilization and Financial Indicators of Children's Hospitals. Alexandria, VA: NACHRI.
NACHC (National Association of Community Health Centers). 1997. Data provided to the Institute of Medicine by the office of Dan Hawkins, NACHC, Washington, D.C.: NACHC.
NACCHO (National Association of County and City Health Officials). 1995. 1992-1993 National Profile of Local Health Departments. Washington,D.C. : NACCHO.
Neff JM, Anderson G. 1995. Protecting Children with Chronic Illness in a Competitive Marketplace. Journal of the American Medical Association 274:1866-1869.
Prospective Payment Assessment Commission (ProPAC). 1997. Report and Recommendations to the Congress, March 1, 1997. Figure 1-5, p. 30. Washington, D.C.: ProPAC.
Schneider A. 1997. Overview of Medicaid Provisions in the Balanced Budget Act of 1997, P. L. 105-33. Washington, D.C.: Center for Budget and Policy Priorities [http://www.cbpp.org/908mcaid.htm]
Urban Institute. 1997. The Medicaid Disproportionate Share Hospital Program: Background and Issues (no. 14). By Teresa A. Coughlin and David Liska. Washington, D.C.: Urban Institute.
U.S. House of Representatives, Committee on Ways and Means. 1996. 1996 Green Book. Washington, D.C.: U.S. Government Printing Office.
















