5
Medicaid
Medicaid is the largest single health insurance program for American children. In 1997, more than 22 million children—one of every four children—were covered by Medicaid.
Although children in low-income families make up nearly half of all Medicaid beneficiaries, expenditures for children are less than 20 percent of total Medicaid spending (see Figure 5.1). In 1995, Medicaid spent an average of $1,175 per child, which is the lowest amount per person for any of the groups enrolled in the program (Kaiser Commission on the Future of Medicaid, 1997).
This chapter describes the Medicaid program in the context of its role in financing health care for low-income children. After a brief description of the history and scope of the program, recent trends in Medicaid spending and enrollment are described. Next, the chapter describes the program's impact on access to care. In summary, the chapter describes trends in the program as a result of managed care and recent federal legislation.
History And Overview Of The Medicaid Program
The Medicaid program was created in 1965 as Title XIX of the Social Security Act. It was designed as a federal-state partnership to provide public funding for health care for low-income children and adults.
Specific Medicaid benefits for children were established in 1967, when Congress created the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) Program. The EPSDT program is a comprehensive package of children's medical, ancillary, and support services with an emphasis on regular screenings and preventive services. As discussed later in this chapter, the scope of EPSDT benefits is quite comprehensive compared to the scope of most commercial benefit packages.
In the mid-1980s, the Congress took several incremental legislative steps to expand Medicaid eligibility, first as state options and then as state mandates (see Box 5.1). The number of children enrolled in Medicaid nearly doubled in 10 years, rising from 10 million in 1987 to 18 million in 1995 (see Figure 5.2). The increase was substantial after 1989, when coverage was mandated for all children under age 5 years whose families had incomes up to 133 percent of the federal poverty level, and 1990, when all children under poverty up to age 19 began to be phased in.
In 1989, Congress also began to require states to provide any medically necessary treatment that was indicated through an EPSDT screen, whether or not that service is included in the state's Medicaid plan. Combined with the increase in Medicaid enrollment, this offset the simultaneous decreases in children's
CHILDREN MAKE UP HALF OF THE MEDICAID BENEFICIARIES AND ONE FIFTH OF THE COSTS
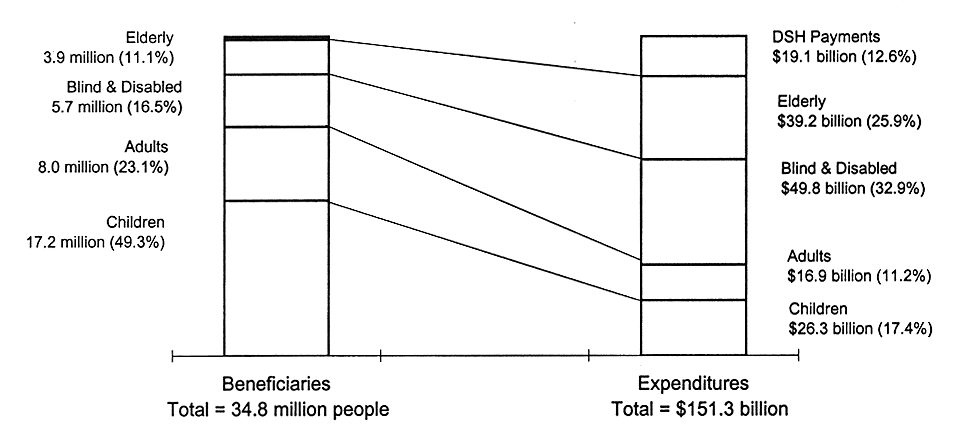
FIGURE 5.1
Medicaid beneficiaries and expenditures, by enrollment group, United States, 1995. Total expenditures exclude administrative expenses. Children are dependent children ages 0-21 years. SOURCE: Kaiser Commission on the Future of Medicaid, 1997. Data are from the Urban Institute analysis of the HCFA 2082 and 64 Statistical Reports.
CHILDREN'S MEDICAID EXPANSIONS RESULTED IN INCREASED ENROLLMENT
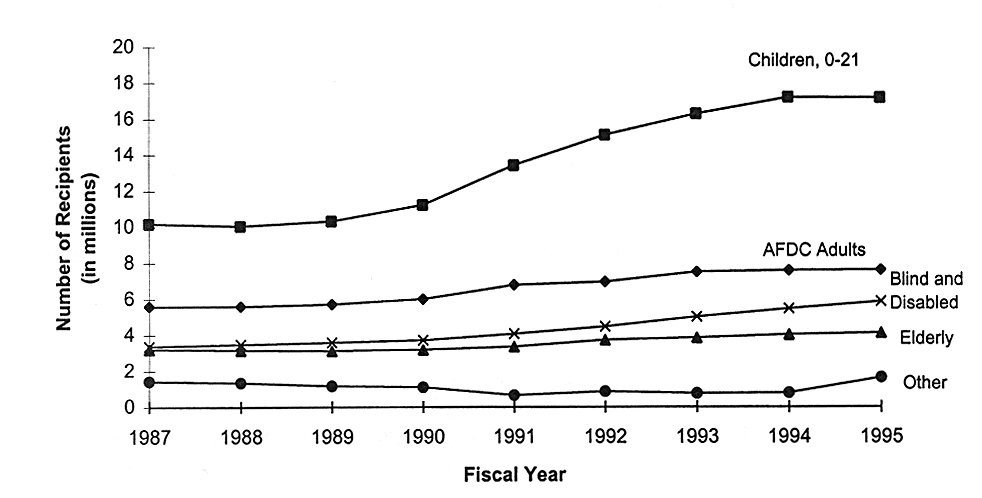
FIGURE 5.2
Trends in the number of Medicaid recipients, by enrollment group, United States, 1987-1995. AFDC = Aid to Families with Dependent Children. SOURCE: HCFA (1997b). Data were provided by the Division of Information Distribution and were derived from the HCFA 2082 Statistical Report on Medical Care: Eligibles, Recipients, Payments, and Services.
coverage through private sources, lowered the number of children without insurance, and significantly reduced the disparities in access to health care for poor children.
However, the increase in enrollment began to alarm governors and state legislatures, who were concerned about the rate of Medicaid cost increases as a proportion of state budgets (see Figure 5.3). In the late 1980s, the number of children enrolled in Medicaid was increasing at the same time that health care costs were rising across the country (see Figures 5.4 and 5.5). Because of the growth in Medicaid as a percentage of state expenditures, most states turned to some form of managed care to control Medicaid costs.
Medicaid represents an average of 20 percent of state budgets, and state officials and policymakers are continuing to experiment with ways to achieve cost savings. Some state policymakers are concerned about the costs of expanding the eligibility for entitlement to Medicaid, whereas 26 other states have expanded their Medicaid programs beyond the minimum federal requirements with a goal of improving access to care for low-income individuals (Gauthier and Schrodel, 1997).
By 1997, Medicaid cost increases seemed to have leveled off, in part because of the shift to Medicaid managed care, and also because of declining welfare enrollment due to welfare reform and the growth in the nation's economy. However, children's enrollment in Medicaid is expected to continue to increase through 2002, when phased-in coverage for older children is complete, and as some states choose to use Medicaid to cover groups of previously uninsured children under the State Children's Health Insurance Program (SCHIP) of the Balanced Budget Act of 1997.
Currently, the Medicaid program comprises 13 percent of all health care spending in this country. Medicaid expenditures totaled $157 billion in 1995: $90 billion from federal funds and $67 billion from state matching funds (GAO, 1997a). During fiscal year 1998, states will spend about $27 billion to purchase health care coverage for children through their Medicaid programs (Mann, 1997). As large-scale purchasers of managed care, states have an increasing ability to negotiate reasonable rates and control costs while increasing access to care.
|
When we think of Medicaid, we should not be thinking about the Medicaid program of 15 years ago. We should be thinking about the new emphasis in the program on managed care, on primary care, on prevention, and on predictable capitated costs for care. States have been increasingly willing to use their Medicaid programs for children's coverage because the move to managed care gives them more predictable costs per child. So they are putting children into systems of care where preventive and primary care are available. Diane Rowland The Kaiser Commission on the Future of Medicaid, Washington, DC Public Workshop, June 2, 1997 |
Eligibility
The Medicaid program is a federal-state partnership with funding and administrative responsibilities shared by the federal government and state governments. It has both mandatory and optional categories of eligibility and services. Mandatory eligibility and service requirements apply in every state, whereas the states have the flexibility of choosing among optional categories at their own programmatic and financial discretion. In essence, the Medicaid program is different in every state.
Eligibility for Medicaid is mandatory for the following groups:
|
BOX 5.1 A Brief History of Medicaid Legislation Concerning Children
|
- Children under the age of 6 years whose families have incomes up to 133 percent of the federal poverty level.
- Older children up to 19 years of age who were born after September 30, 1983, and who live in families with incomes at or below the federal poverty level.
- Children who receive adoption assistance or foster care.
- Pregnant women whose incomes are up to 133 percent of the federal poverty level.
- Infants born to Medicaid-eligible pregnant women.
- Children who receive federal Supplemental Security Income (SSI).
- Children in families that meet the AFDC criteria in place prior to welfare reform.
|
||||||||||||
States have the option of expanding Medicaid coverage to pregnant women and children beyond the minimum federal requirements. In 1997, 26 states had expanded Medicaid eligibility for children by increasing the age criteria, the income criteria, or both (Gauthier and Schrodel, 1997). Under SCHIP, several states will implement further expansions of eligibility.
Medicaid has had strict eligibility requirements on the basis of income, and this has been a problem for families whose income levels fluctuate. Parents who have seasonal work, parents who work in service industries where there is rapid turnover, and parents who are between jobs may not be able to predict their levels of monthly income and may move in and out of eligibility if they are close to the income limits set in their state.
Medicaid administrative systems typically lack the capacity to follow these children and families at
MEDICAID SPENDING AS A PORTION OF STATE BUDGETS NEARLY DOUBLED IN 10 YEARS
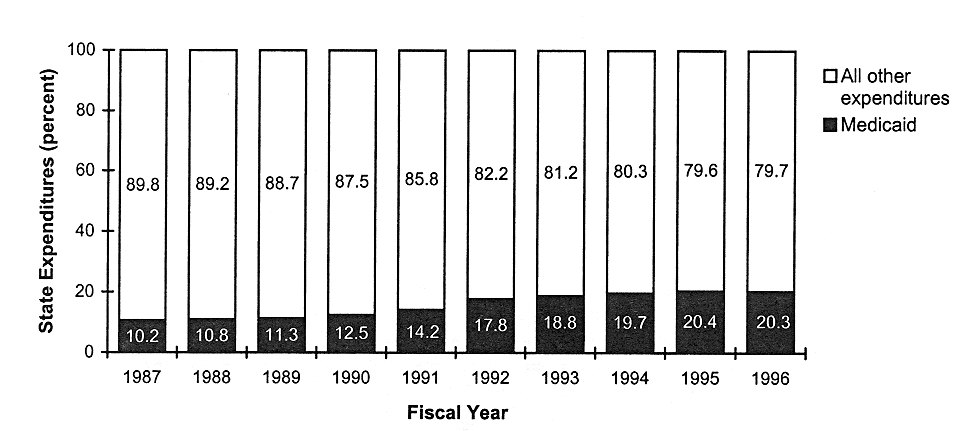
FIGURE 5.3
State Medicaid expenditures as a percentage of total state expenditures, by fiscal year, United States, 1987-1996. SOURCE: NASBO (1997). Data are from NASBO 1989-1997 State Expenditure Reports.
the margins of eligibility. Additionally, many state Medicaid directors believe that their reporting and billing systems not only impose substantial administrative burdens on states, but also fail to provide useful information on utilization and services for planning purposes.
The level of administrative complexity has varied among the states, and some states have been changing the administrative structures of their Medicaid programs. In recent years, a number of states have simplified their enrollment forms, improved their outreach efforts, improved their provider billing and payment procedures, and moved into managed care and capitated payment systems.
|
Family income may fluctuate seasonally, particularly for those below 150 percent of the Federal Poverty Level. It may fluctuate on the basis of periods of employment and unemployment. If families are going to be in Medicaid this month, and they are going to get the premium subsidy next month, but they are not going to qualify for anything in the third month, are we really looking at policies that will help families get coverage for their children that is meaningful on a continuous and ongoing basis? Kay Johnson George Washington University, Washington, DC Public Workshop, June 2, 1997 |
Access To Care
Eligibility and Enrollment
With Medicaid eligibility no longer linked to eligibility for welfare, some states are trying to improve enrollment by reducing the traditional embarrassment some people feel about being associated with
ENROLLMENT AND COSTS PER CHILD INCREASED AT THE SAME TIME
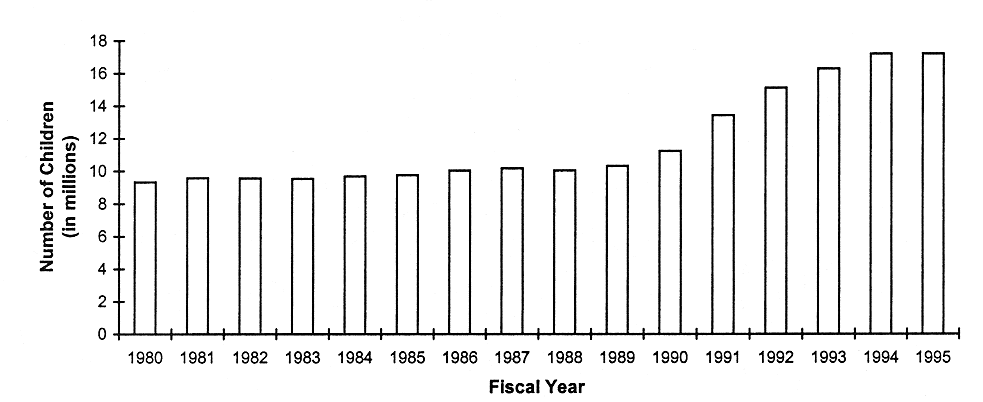
FIGURE 5.4
Trends in the number of dependent children ages 0-21 years receiving Medicaid, United States, 1980-1995. SOURCE: HCFA (1997b). Data were provided by the Division of Information Distribution and were derived from the HCFA 2082 Statistical Report on Medical Care: Eligibles, Recipients, Payments and Services.
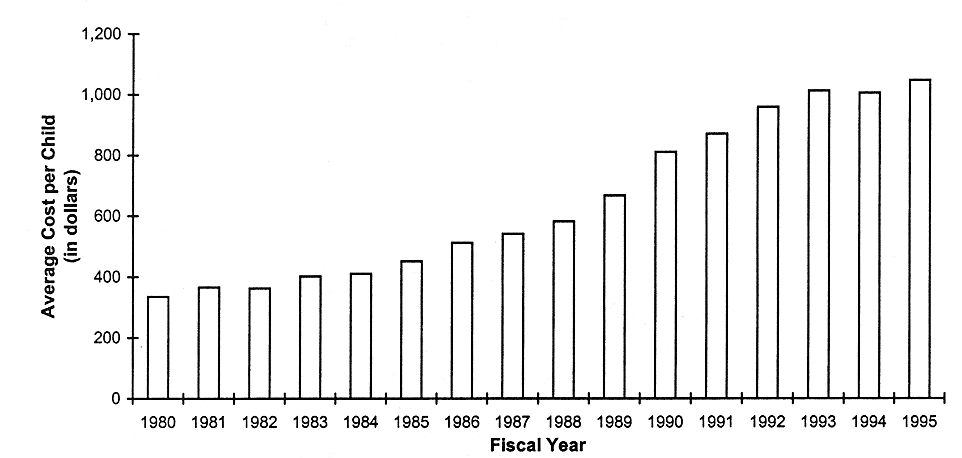
FIGURE 5.5
Trends in the average annual cost per dependent child receiving Medicaid, United States, 1980-1995.
SOURCE: HCFA (1997b). Data were provided by the Division of Information Distribution and were derived from the HCFA 2082 Statistical Report on Medical Care: Eligibles, Recipients, Payments and Services.
welfare, such as by changing the name of the Medicaid program (e.g., Dr. Dynasaur in Vermont). The SCHIP program will pay a limited amount for outreach activities and also includes a ''presumptive eligibility" option that will allow states to immediately enroll Medicaid-eligible children in the program, pending the results of the determination process. In the course of implementing new programs, states are adopting easier application processes, such as mail-in or telephone applications, which may help to enroll more eligible children.
|
In Somerville, Massachusetts, they required every child coming into the school not only to show their immunization record, but to document whether or not they had either Medicaid or private coverage. They were then able to enroll a whole host of kids who were eligible for Medicaid and who had not been enrolled, but who were legally entitled. James Bentley American Hospital Association, Washington, DC Public Workshop, June 2, 1997 |
Historically, Medicaid eligibility was tied to eligibility for cash payments under welfare. For the Aid to Families with Dependent Children (AFDC) program, states set the financial standards for eligibility. Enrollment in the Medicaid program involved the rigorous, inconvenient, and often complex or burdensome administrative procedures of qualifying for welfare. Lengthy applications requiring documentation of income and assets, limited hours and locations for the submission of applications, and other challenges made it difficult to enroll in the program.
Although many states have been developing innovative outreach and enrollment strategies, millions of children who are eligible for Medicaid are not enrolled in the program. Estimates of the numbers of these children range from 2 million (Holahan, 1997) to 3.5 million, or 30 percent of uninsured children ages 0-11 (GAO, 1996). About 80 percent of these eligible children have a working parent, and parents who work and who are not themselves eligible for cash assistance are less likely to enroll their children in Medicaid (GAO, 1996; Summer et al., 1997).
Eligible children may not be enrolled for a variety of reasons. Some working parents are likely to be unaware of the program or unable to leave work to go through an enrollment process. Other parents do not trust the health care system for cultural, racial, ethnic, or other reasons; some find the application process difficult; and some do not want to participate in a program that has traditionally been associated with welfare. Other parents' applications have been denied for procedural reasons other than the lack of eligibility, such as the lack of written documentation of income.
Targeted outreach efforts, culturally sensitive public information campaigns, simpler enrollment procedures, and strategies that distinguish the program from welfare are a few ways for improving the rate of enrollment. Outreach and public education efforts will need to include providers, to allow them to become familiar with program changes and to recruit them to participate.
Provider Participation
Medicaid has no premiums and permits only nominal cost-sharing for its enrollees. However, even when children have Medicaid coverage, providers may not be available to see them. A disproportionate number of low-income children and children who are members of racial and ethnic minorities live in areas where there are shortages of medical providers. Even when providers are locally available, there may be few who accept Medicaid payments, and those few may be too busy to accept appointments.
On average, Medicaid payment rates have been about 40 percent lower than the rates paid by
private insurers (ProPAC, 1992). A substantial number of providers have limited their participation or have not participated at all because of the lower reimbursement levels. Some safety net providers and health care systems argue that they have already absorbed as many Medicaid patients as they can without disturbing the balance of payments from other sources.
Movement of Medicaid enrollees into managed care may begin to increase provider participation and availability. As health plans begin to compete for market share by enrolling Medicaid beneficiaries into capitated programs and as more providers become part of Medicaid managed care plans or networks, more providers will be available to see Medicaid patients. However, unless managed care plans also address nonfinancial barriers, such as transportation, language translation, and child care services, access may continue to be difficult for Medicaid enrollees (Lipson, 1997).
The reduction of Disproportionate Share Hospitals (DSH) funding in the Balanced Budget Act of 1997 could have an independent impact on hospitals that serve relatively large numbers of Medicaid and uninsured patients. Congress capped DSH payments at 12 percent of Medicaid program expenditures in 1991. In the Balanced Budget Act of 1997, future federal DSH funding was reduced by a projected $10 billion.
DSH funds were intended to offset the costs to providers who served a disproportionate share of low-income and uninsured individuals. However, some states used the DSH funding to substitute for other state expenditures through intergovernmental transfers and other methods (Holahan et al., 1997). Only about two-thirds of the funding reached safety net hospitals (Coughlin and Liska, 1997).
The impact of changes in DSH are already visible as safety net providers react to Medicaid managed care and market pressures by trying to become more competitive (Baxter and Mechanic, 1997). Some health plans that are new to the Medicaid market have underestimated the need for expanded services such as case management, language translation, and outreach efforts that are traditionally handled by safety net providers. Thus, they have sought partnerships with community-based providers who know the Medicaid populations and are experienced in providing expanded services. Some community-based providers are entering into partnerships with Medicaid-contracting health plans, and others are developing their own managed care plans (Lipson, 1997).
|
Why do states expand their Medicaid programs? They expand them to poor kids because they know that health insurance matters. It is clear from the Medicaid experience that differentials in access to care between children with Medicaid and children who are uninsured have been markedly changed, in that private patients and Medicaid patients access the health care system in very comparable ways. The uninsured are still lagging considerably behind. Diane Rowland Kaiser Commission on the Future of Medicaid, Washington, DC Public Workshop, June 2, 1997 |
Accountability for Access to Care
Some studies have shown that children with Medicaid coverage have access to health care comparable to that for children who are privately insured (Overpeck and Kotch, 1995; St. Peter et al., 1992). However, access to care varies significantly from community to community (Baxter and Mechanic, 1997), making it difficult to generalize from these studies. Moreover, many studies of low-income
populations are not able to separate out the related effects of income, lack of insurance, generally poorer health status, and exposure to other public health risks, such as poor nutrition or unsafe neighborhoods.
At the state level, accountability for access tends to focus on adherence to eligibility criteria, allowing access only for those who are eligible to enroll in the program. After 30 years of the Medicaid program and at least 10 years of more standardized national data on enrollment and expenditures, the infrastructure of information that can be used to evaluate the impact of the program is fragmented and incomplete. Under a fee-for-service system, it was possible to track utilization through billing information. Under managed care, individual encounter data are needed to determine utilization patterns, but states either may not have access to the data from health plans or may lack the technical capacity to analyze the data (Howell, 1996; GAO, 1997b). Because of these technical problems, information on access under managed care will continue to be difficult to evaluate.
|
Maybe we need private health insurance reform. I'm not saying that we don't. What I'm saying is that Medicaid is a rationing program. Everybody familiar with it knows it is a rationing program. What happens with government-provided health care in all of the developed countries is that they do a very good job of providing inexpensive services, and they skimp on what is expensive. They skimp on heart surgery, the CAT scans—on all of the life-saving technology. For the future, that is exactly what is going to happen to Medicaid and to Medicare. You can see it right now in the budget. Congress wants to cut down on payments to hospitals and doctors, which means they are going to skimp on care for the expensive, sick patients. I don't see any way around that. As a matter of public policy, maybe we are going to have to create global budgets for poor people, but give those poor people an opportunity to get into a better system. John Goodman National Center for Policy Analysis, Dallas, TX Public Workshop, June 2, 1997 |
Scope Of Services
As a condition for receiving federal Medicaid matching funds, Medicaid coverage and services must be in effect statewide and must be comparable for everyone within a particular eligibility group. The following services must be provided for individuals who are enrolled in Medicaid (also see Box 5.2):
- inpatient and outpatient hospital services,
- physician services,
- medical and surgical dental services,
- nursing facility services for individuals ages 21 years and older,
- home health care for people eligible for nursing home services,
- family planning services and supplies,
- rural and federally qualified health clinic services,
- laboratory and X-ray services,
- pediatric and family nurse practitioner services, and
- nurse midwife services.
Although the federal law requires these services to be provided, states have had discretion and a substantial degree of control over the amount, scope, and duration of each service.
|
BOX 5.2 Medicaid Services
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Scope of Benefits
Comprehensive benefits (the EPSDT program) for children enrolled in Medicaid have been in place for several years. These benefits are mandatory for all eligible children, although their provision is not always enforced and the specified benefits are not always available when they are needed.
So, although the intended scope of Medicaid benefits has been comprehensive, children have not always received treatment that was regarded as medically necessary when required by law. For example, if a child were determined by a physician to need an organ transplant, but lived in a state that does not cover the procedure under Medicaid, the parents could face a choice of foregoing the procedure, raising the funds independently, such as through charity donations, or incurring enormous financial costs.
|
Obviously it would be easier if states had more flexibility. On the other hand, if we don't have any regulatory guidelines, I'm afraid we'll see no preventive care, and parents being offered packages that are cheap and that don't cover very much except catastrophic care. If we are going to look after children, we need to look after all of their health care needs. We should define a comprehensive package pretty close to the EPSDT package and include children with multiple problems and serious illness. The cost is minuscule if you spread it over the whole society. Steve Edwards American Academy of Pediatrics, Raleigh, NC Public Workshop, June 2, 1997 |
Early and Periodic Screening, Diagnosis and Treatment Program
Medicaid-eligible children up to the age of 21 are ensured participation in the EPSDT program (see Box 5.3 for a description of EPSDT program services). The EPSDT program was enacted by the U.S. Congress in 1967 and was designed to provide children with comprehensive and periodic physical and mental health assessments as well as to diagnose and treat any problems discovered in the course of routine screenings.
The EPSDT program is unique among programs that provide children's health care benefits. First, it sets a standard of comprehensive care for all enrolled children. Second, the EPSDT program emphasizes age-appropriate preventive strategies and not simply the treatment of acute illnesses and injuries. Third, the EPSDT benefit package was intended to address the needs of chronically and congenitally ill children, including those who need to improve their age-appropriate functioning as well as those who have congenital conditions, need to maintain their limited functional capacity, but who are not expected to improve. In this way, the EPSDT benefit package is significantly different from most commercial benefit packages, which typically provide treatments for illnesses and injuries and coverage for physical, occupational, and speech therapy on a limited and temporary basis to restore lost functioning for acute conditions.
Because responsibilities for the Medicaid program are split across federal, state and local boundaries, information about how many children are receiving EPSDT program services, where they receive them, and the quality of those services is largely inadequate. Another problem discussed at the committee's public workshop is that the screening and diagnostic components of the EPSDT program are provided more frequently than are the treatment components, particularly when the treatment that is considered "medically necessary" is not included among the state's list of allowable expenses (e.g., organ transplants).
|
BOX 5.3 EPSDT Health Services Requirements The Early and Periodic Screening, Diagnosis and Treatment Program (EPSDT) requires states to provide or arrange for the following health services to all Medicaid-eligible children under the age of 21:
|
1.
| Comprehensive, periodic health assessments, or screenings, from birth through age 20, according to medically appropriate periodicity schedules. The medical screen must include:
|
*
| a comprehensive health and developmental history, including assessment of physical and mental health development;
|
*
| a comprehensive unclothed physical exam;
|
*
| immunizations in accordance with the Advisory Committee on Immunization Practices' schedule (AAP, 1993);
|
*
| laboratory tests, including blood lead level assessment; and
|
*
| health education, including anticipatory guidance.
|
2.
| Interperiodic screens to be provided if there is reason to suspect a health problem between regularly scheduled screenings.
|
3.
| Comprehensive preventive, restorative and emergency dental services furnished according to state-defined periodicity schedules;
|
4.
| Periodic hearing examinations, according to medically appropriate timetables, and all follow-up services, including hearing aids;
|
5.
| Periodic vision examinations, according to medically appropriate timetables, and all follow-up services, including eyeglasses; and
|
6.
| Any "medically necessary" diagnostic and treatment services for illnesses or conditions identified during screening. Covered services include all mandatory and optional services available under Medicaid, whether or not an individual state chooses to offer the service to its general Medicaid population. SOURCE: Adapted from box on page 3, NIHCM, 1996. |
|
If state contracts fail to specify the range of interventions and services that should be provided for Medicaid enrollees, health plans may not actually provide all of the required benefits for children covered by Medicaid (Fox and McManus, 1996; Rosenbaum et al., 1997). A 1997 study by the Inspector General of the U.S. Department of Health and Human Services found that only 28 percent of the children enrolled in Medicaid managed care received all of the EPSDT program screens called for in their state, and 60 percent of the children in the study received none of the services called for in their states' periodicity schedules (DHHS, 1997a).
|
There is a great deal of evidence to support the fact that over the past 30 years the children's health benefits package under Medicaid has become the richest children's health benefit package. I don't know of a private insurance package that provides the degree of comprehensive coverage that you get under EPSDT. Kay Johnson George Washington University, Washington, DC Public Workshop, June 2, 1997 |
These figures are not much different from the findings of a 1992 Health Care Financing Administration (HCFA) study, when Medicaid was still predominantly a fee-for-service system. HCFA found that only about 36 percent of the eligible children were reportedly receiving the EPSDT program screens, although the actual numbers may have been higher because providers may not have been accurately coding encounters as EPSDT program screens (Koppelman, 1993).
In addition to covering the costs of EPSDT program services, states are required to provide outreach and education services to inform families of Medicaid-eligible children about services and to assist them in obtaining those services (NIHCM, 1996). These services are typically not provided by health care plans, and as more states move toward managed care, some groups are concerned that children may not get the comprehensive services included in the EPSDT program.
Medicaid Managed Care
The number of Medicaid beneficiaries enrolled in managed care plans increased fourfold between 1991 and 1996 (see Figure 5.6 and Table 5.1). Much of the increase was due to the granting of Medicaid waivers. The 1115 and the 1915 (b) and (c) waivers allowed states to limit Medicaid recipients to particular provider groups, thereby making it possible for them to contract with managed care plans.
As of September 1997, every state except Alaska and New Hampshire had acquired a waiver to begin managed care programs for Medicaid beneficiaries (Epstein, 1997; Zuckerman et al., 1997). More than one third of the nation's Medicaid beneficiaries were enrolled in some form of managed care program as of June 1996. The vast majority of these enrollees were children and single parents, who are generally more easily enrolled in health plans than aged, blind, or disabled Medicaid beneficiaries.
This national shift to managed care has had a tremendous impact on the nature of the program and has significantly changed the role of state Medicaid agencies. A turning point was reached in the early 1990s as states increasingly began to move their Medicaid programs into managed care in search of cost savings, but also to increase access to preventive services. Under a fee-for-service system, the traditional role of state Medicaid agencies was to provide oversight of financial performance and monitoring of providers for overutilization. In the market-driven systems of managed care, the Medicaid agencies' roles have been transformed. Billions of public dollars are being paid prospectively to managed care plans, raising issues of accountability and public trust.
As large-scale buyers of private managed health care coverage, Medicaid agencies are now challenged to use the bargaining skills of other large purchasers in order to negotiate reasonable rates while protecting enrollees. States must be able to develop specific contract language, define the scope of services within existing resources, and establish performance measures for health plans that assure access and quality of care (Landon et al., 1998; Rosenbaum et al., 1997).
|
There is really a shift from thinking of Medicaid as a welfare program, to thinking of it as a purchaser and a payer of services. The further along that road we get, the better we are going to do for our kids. Shelly Gehshan National Conference of State Legislatures, Washington, D.C. Public Workshop, June 2, 1997 |
Under fee-for-service arrangements, Medicaid was a financing stream and a mechanism for reimbursing providers for services. Under Medicaid managed care, state Medicaid administrators are purchasing comprehensive, integrated delivery systems for the first time. This shift to managed care gives them
MEDICAID MANAGED CARE ENROLLMENT QUADRUPLED IN 5 YEARS
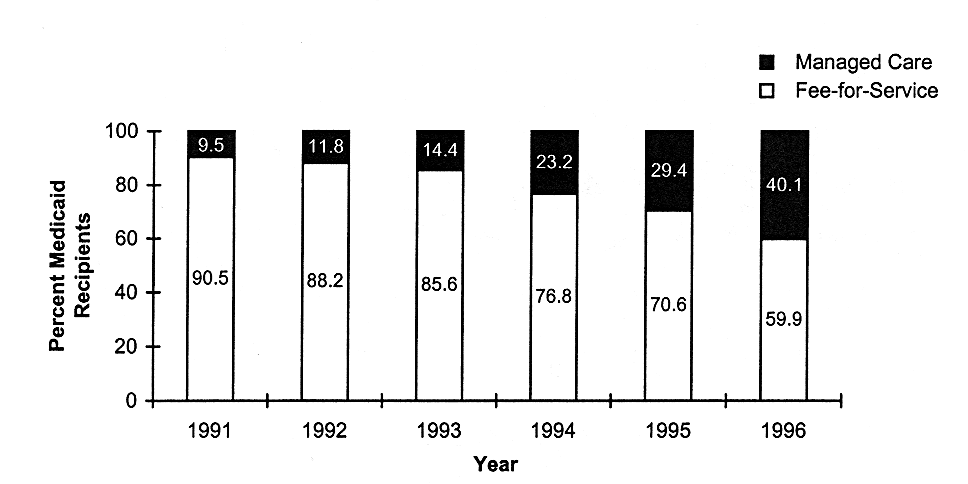
FIGURE 5.6
Percentage of Medicaid recipients enrolled in fee-for-service and managed care plans, United States, 1991-1996. SOURCE: HCFA (1997c). Data were provided by the Division of Information Distribution and were derived from the HCFA 2082 Statistical Report.
TABLE 5.1 Trends in Managed Care and Fee-for-Service Enrollment under Medicaid, United States, 1991-1996
|
|
Year |
|||||
|
Type of Plan |
1991 |
1992 |
1993 |
1994 |
1995 |
1996 |
|
|
Number of Recipients (in millions) |
|||||
|
Total Medicaid Population |
28.3 |
30.9 |
33.4 |
33.6 |
33.4 |
33.2 |
|
Fee-for-Service |
25.6 |
27.3 |
28.6 |
25.8 |
23.6 |
19.9 |
|
Managed Care |
2.7 |
3.6 |
4.8 |
7.8 |
9.8 |
13.3 |
|
|
Percentage of Total Medicaid Population |
|||||
|
Fee-for-Service |
90.5 |
88.2 |
85.6 |
7.8 |
70.6 |
59.9 |
|
Managed Care |
9.5 |
11.8 |
14.4 |
23.2 |
29.4 |
40.1 |
|
SOURCE: HCFA (1997c). Data were provided by the Division of Information Distribution and were derived from the HCFA 2082 Statistical Report. |
||||||
the authority to negotiate specifications for the components and services of a delivery system that must be available as a condition of awarding contracts to health plans.
In addition to controlling costs, managed care arrangements can provide the states opportunities to increase access to services, to improve coordination and quality of care, and to mainstream their beneficiaries into the general health care system. In comparison with fee-for-service Medicaid, managed care with capitation has more regular and predictable expenditures. In theory, managed care can improve access to prenatal and dental care, improve immunization rates, and increase access to preventive health services.
In practice, however, managed care does not automatically improve access to care. Many people in the children's health community are concerned about Medicaid managed care, especially for vulnerable populations such as children with special health care needs. Medicaid beneficiaries are likely to have greater health risks, poorer health status, and limited disposable cash for purchasing health care that may be needed but is beyond what is covered by Medicaid. Although managed care produces cost savings by reducing the overuse of inpatient hospitalization and emergency departments, there may also be a reduced access to pediatric specialists, which is a particular concern for children with chronic medical conditions and other special health care needs (Newacheck et al., 1996).
Impact Of Recent Federal Legislation
Welfare Reform
From the time that Medicaid began until the welfare reform law was enacted in 1996, individuals who were eligible for the Aid to Families with Dependent Children (AFDC) program automatically qualified for Medicaid coverage. Effective July 1, 1997, as part of the Personal Responsibility and Work Opportunity Reconciliation Act of 1996 (P.L. 104-193; also referred to as "welfare reform"), the AFDC entitlement program was replaced with a new cash block grant to states known as Temporary Assistance to Needy Families (TANF) (see Table 5.2).
The welfare reform law included major changes affecting Medicaid eligibility. Eligibility for cash assistance no longer automatically guaranteed Medicaid eligibility. In addition, the law gave states flexibility to modify their Medicaid eligibility criteria in one of three ways:
- reduce eligibility by lowering the income standard to a level that was in effect no earlier than May 1, 1988;
- expand eligibility by increasing income or resource standards by a percentage that does not exceed the percentage increase in the Consumer Price Index; or
- use methods for determining income and resources that are less restrictive than those in effect on July 16, 1996.
The majority of states chose the third option, and most states are choosing whether to expand Medicaid further under the terms of the SCHIP program in the Balanced Budget Act of 1997. The welfare reform law required states to provide 1 year of transitional Medicaid coverage for those individuals who lost their eligibility as a result of beginning to receive child support payments or beginning employment. To further address the changes of welfare reform, the Balanced Budget Act of 1997 provided funding to allow states to continue to provide Medicaid coverage for these individuals for a transitional 1-year period. With federal approval, some states have extended this transitional period to two years.
The delinking of Medicaid and welfare through the law creating TANF acts two ways: ( ) Medicaid enrollment is no longer dependent upon receipt of welfare; and (2) children can be eligible for Medicaid without being on welfare. Parents leaving the welfare rolls to take new jobs may not be aware that their
TABLE 5.2 Comparison of Prior Welfare Laws and the Personal Responsibility and Work Opportunity Reconciliation Act of 1996 (P.L. 104-193), United States.
|
|
Prior Welfare Laws |
P.L. 104-193 / TANF |
|
Medicaid |
* Eligibility determined by receipt of family assistance through AFDC |
* Eligibility delinked from receipt of family assistance through TANF |
|
|
* States also mandated to cover other specified categories of individuals, such as recipients of SSI |
* States may employ more liberal income and resource standards for Medicaid eligibility, within specific range. [*Balanced Budget Act of 1997 restores Medicaid coverage to those SSI recipients who lost coverage because of change in definitions.] |
|
|
* Aliens who were PRUCOL were eligible for Medicaid; those not PRUCOL were eligible only for emergency medicaid services |
* Qualified aliens will be ineligible for five years of Medicaid (except emergency Medicaid); most current legal immigrants already in the U.S. may be deemed ineligible for Medicaid [*Balanced budget Act of 1997 restores eligibility to this group.] |
|
AFDC, JOBS, EA |
* AFDC provided income support to families with children deprived of parental support· |
* Eliminates AFDC, JOBS, and EA, forming a single program TANF |
|
|
* JOBS was an employment and training program for AFDC recipients |
|
|
|
EA provided short term emergency services and benefits to needy families |
|
|
|
* Open-ended funding provided provided for AFDC benefits and EA, while JOBS was a capped entitlement |
* Block grants AFDC, EA, and JOBS into a single capped entitlement to the states |
|
|
* AFDC eligible individuals were guaranteed aid at state-established benefit levels |
* No individual guarantee of benefits |
|
|
* A set percentage of non-exempt AFDC caseload was required to participate in JOBS activities for at least 20 hours per week |
* States must demonstrate that they will require families to work after two years on assistance |
|
|
* States were required to provide basic and secondary education, as well as job training |
* TANF individuals are required to participate in unsubsidized or subsidized job training, hours to be counted toward the work requirement |
|
|
* AFDC benefits were available to each eligible dependent child and parent, regardless of age of mother |
* Unmarried minor parents are required to live in an adult-supervised setting and participate in educational activities in order to receive Federal assistance |
|
|
* Families on welfare received additional AFDC benefits whenever they had another child |
* No provision, no state option |
|
SSI |
* Children who did not meet or equal the Listing of medical Impairments were determined to be disabled if they suffered from physical or mental impairment of comparable severity to an adult |
* Provides a new definition of disability for children, which removes references to maladaptive behavior as a medical criterion in SSA's listing of impairments used for evaluating mental disabilities in children |
|
|
* Aliens who were PRUCOL were eligible for SSI benefits |
* Most legal immigrants will be ineligible for SSI until citizenship, at time of recertification |
|
Food Stamps |
* Six categories of legal aliens were allowed to receive food stamp benefits if they met eligibility criteria |
* Most legal immigrants will be ineligible for Food Stamps until citizenship |
|
|
* Set maximum benefit levels at 100% of the Thrifty Food Plan |
* Sets maximum benefit levels at 103% of the Thrifty Food Plan and retains annual indexing |
|
|
* Able-bodied adults were expected to hold jobs or participate in the Employment and Training Program |
* Able-bodied recipients between 18 and 50 with no dependents must work (at least 20 hours per week) in order to be eligible for food stamps |
|
SOURCE: DHHS(1997b). NOTE: AFDC = Aid to Families with Dependent Children; EA = Emergency Assistance; PRUCOL = Permanently Residing Under Color of Law; SSI = Supplemental Security Income; TANF = Temporary Assistance to Needy Families. |
||
children are still eligible for Medicaid, and state Medicaid agencies will need to find new ways to notify parents about their children's eligibility.
Some observers believe that the changes in the welfare system may result in an increase in the number of Medicaid-eligible children who are not enrolled in the program and that outreach and public education efforts will need to be further strengthened and supported. Early in 1998, the Clinton Administration announced new initiatives to increase outreach and enrollment efforts in Medicaid.
Welfare Reform and SSI Recipients
In 1996, approximately 1 million children under age 18 received Medicaid on the basis of the determination of a disability and associated eligibility for cash payments under the SSI program (SSA, 1997). The 1996 welfare reform law changed the way in which childhood eligibility for SSI is determined by introducing more stringent requirements for SSI eligibility in the following ways:
- establishment of new definitions of childhood disability,
- redetermination of the eligibility status of current children receiving SSI under previous regulations and definitions, and
- continuing reviews of disability status.
With the enactment of the Balanced Budget Act of 1997, Medicaid eligibility (but not cash SSI payments) was restored to many of the SSI recipients who lost coverage under the new welfare law. However, as of August 1997, the new, more restrictive eligibility rules for children with emotional and behavioral problems resulted in the termination of cash disability benefits for more than 95,000 children (SSA, 1997). Eventually, 15 percent of the 1 million children in the program could lose their cash benefits if that rate continues (see Chapter 7, Box 7.1, for a description of the SSI program).
A new option in the Balanced Budget Act of 1997 allows states to create a Medicaid ''buy-in" program for individuals whose incomes are under 250 percent of the federal poverty level and who would otherwise meet the medical eligibility criteria for SSI. The buy-in amounts will be set on a sliding scale based on family income. The new option is geared toward children with disabilities, but it is unclear how many of the children with emotional and behavioral disabilities will eventually be included because of the changes in the determination criteria and procedures.
|
Why not have Medicaid as a secondary insurance? If you need it and you are running out of your own insurance, pay a premium. That motivates you to work. You could still go to work and could pay your taxes into a Medicaid system, like we pay into the Medicare system. Our spend down amount is $1,100 a month. How are we supposed to pay our mortgage and eat? Karen LaPlante Parent, Dublin, VA Public Workshop, June 2, 1997 |
The Balanced Budget Act of 1997
Increasingly, managed care has become the delivery system for both privately and publicly insured children and families. One of the most significant changes made by the Balanced Budget Act of 1997 is
allowing states to move most Medicaid beneficiaries into managed care without a federally approved waiver. States that choose to enroll Medicaid beneficiaries in managed care have the potential to increase children's access to preventive health care services and to increase the comparability of quality in health care to that provided by private insurance.
However, the law specifies that some at-risk groups will still require federal waivers, including children with special needs (those who meet the definition of disability under the SSI program) and children in foster care or other out-of-home placements. These provisions were enacted in response to concerns among the children's health care community about the quality of care for special-needs children, based on clinical experiences in which managed care organizations have limited patients' access to pediatric specialists and support services.
The 1997 law allows Medicaid-only plans for the first time and also includes some general consumer protections. For example, the law requires that beneficiaries must be able to choose from among at least two plans, that the plans must have adequate provider capacity and a range and mix of appropriate providers, and that plans must have grievance procedures and quality assurance assessment and improvement mechanisms.
More than 1,000 pieces of legislation were introduced in state legislatures in 1997 to address some aspect of consumer protection under managed care. The inclusion of federal requirements in the Balanced Budget Act of 1997 for consumer protection for those who are covered by Medicaid was viewed as a landmark.
|
We have a Medicaid system which is providing important services to a substantial share of the population. We have the opportunity to improve that system which is in place, and to offer strategic suggestions on how it can be improved. J. Michael McGinnis National Research Council, Washington, DC Public Workshop, June 2, 1997 |
Implications
Much of the resistance among states to the Medicaid program has been based on the mandated levels of benefits, which are viewed by some states as arbitrary, excessively expensive, and as limiting the ability of states to choose covered services based on the basis of their own preferences and perceived needs. Many providers and children's health advocates, however, view mandatory benefits as the only way of setting minimum national standards and also believe that national as well as state resources must be increased in order to support these standards. This is a fundamental disagreement about the role of government in health care, and debates are occurring in many states as they choose how to participate in the SCHIP program.
The Medicaid program continues to change rapidly. Eligibility requirements are changing in many states as a result of the implementation of new state children's health insurance programs under the Balanced Budget Act of 1997, and managed care is expected to play a major role in the delivery of care under SCHIP. State decisions about Medicaid expansions involve a complex and often difficult process of weighing competing priorities, resolving political and policy disagreements, and making decisions about the allocation of financial and other resources. The new programs will need to be evaluated carefully to determine their long-term impact on access and health status for all children, and particularly for those with special health care needs.
References
AAP (American Academy of Pediatrics) Committee on Child Health Financing. 1993. Scope of Health Care Benefits for Infants, Children, and Adolescents Through Age 21 Years. Pediatrics 91(2):509.
Baxter RJ, Mechanic RE. 1997. The Status of Local Health Care Safety Nets. Health Affairs 16(4):7-23.
Coughlin TA, Liska D. 1997. The Medicaid Disproportionate Share Hospital Payment Program: Background and Issues. Washington, D.C.: Urban Institute. [http://newfederalism.urban.org/html/anfl4.html]
DHHS (US Department of Health and Human Services), 1997a. MedicaidManaged Care and EPSDT . (Report No. OIE-05-9300290). Washington, D.C.: Office of the Inspector General, May 15, 1997.
DHHS, 1997b. Comparison of Prior Law and the Personal Responsibility and Work Opportunity Reconciliation Act of 1996 (P.L. 104-93). [http://aspe.os.dhhs.gov/isp/reform.htm]
Epstein AM. 1997. Medicaid Managed Care and High Quality: Can We Have Both? Journal of the American Medical Association 278(19):1617-1621.
Fox HB, McManus MA. 1996. Medicaid Managed Care for Children With Chronic or Disabling Conditions: Improved Strategies for States and Plans. Washington, D.C.: Fox Health Policy Consultants.
GAO (US General Accounting Office). 1996. Health Insurance for Children: Private Insurance Coverage Continues to Deteriorate. GAO/HEHS-96-129. Washington, D.C.: GAO.
GAO, 1997a. Medicaid: Sustainability of Low 1996 Spending Growth is Uncertain. GAO/HEHS-97-128. Washington, D.C.: GAO.
GAO, 1997b. Medicaid Managed Care: Challenge of Holding Plans Accountable Requires Greater State Effort. GAO/HEHS-97-86. Washington, D.C.: GAO.
Gauthier A, Schrodel SP. 1997. Expanding Children's Coverage: Lessons From State Initiatives in Health Care Reform. Washington, D.C.: AlphaCenter .
HCFA (Health Care Financing Administration). 1995. Medicaid 2082 Statistical Report on Medical Care: Eligibles, Recipients, Payments, and Services, Fiscal Year 1995. [http://www.hcfa.gov/medicaid/mstats.htm]
HCFA. 1996. Health Care Financing Review: Medicare and Medicaid Statistical Supplement 1996. Pub. No. 03386. Baltimore, MD: US Department of Health and Human Services.
HCFA. 1997a. Data provided to IOM by the Division of Information Distribution.
HCFA. 1997b. Overview of the Medicaid Program. [http://www.hcfa.gov/medicaid/mover.htm]
HCFA. 1997c. Medicaid Statistics. [http://www.hcfa.gov/medicaid/hstats96]
Holahan J. 1997. Expanding Insurance Coverage for Children. Washington, D.C.: The Urban Institute.
Holahan J, Wiener JM, Liska D. 1997. The Medicaid Reform Debate in 1997 Washington, D.C.: The Urban Institute. (URL http://newfederalislm.urban.org)
Howell EM. 1996. Medicaid Managed Care Encounter Data: What, Why and Where Next? Health Care Financing Review 17(4):87-96.
Kaiser Commission on the Future of Medicaid. 1997. Medicaid Facts: Medicaid's Role for Children. Washington, D.C.: Author.
Koppelman J. 1993. State Efforts to Improve Health Care Access for Low-Income Children: EPSDT Today and Under Health Reform. Issue Brief 639. Washington, D.C.: National Health Policy Forum.
Landon BE, Tobias C, Epstein AE. 1998. Quality Management by State Medicaid Agencies Converting to Managed Care: Plans and Current Practice. Journal of the American Medical Association 279(3):211-216.
Lipson DJ. Medicaid Managed Care and Community Providers: New Partnerships. Health Affairs 16(4):91-107.
Mann C. 1997. Why Not Medicaid? Using Child Health Funds to Expand Coverage Through the Medicaid Program. Washington, D.C.; Center on Budget and Policy Priorities [http://www.cbpp.org/l119mcaid.htm]
NASBO (National Association of State Budget Officers). 1997. Medicaid. [http://www.nasbo.org]
NIHCM (National Institute for Health Care Management). 1996. Assuring Quality of Care for Children in Medicaid Managed Care-EPSDT in a Time of Changing Policy. Washington, D.C.: NIHCM.
Newacheck, P, Hughes, D, and Stoddard, J. 1996. Children's Access to Primary Care: Differences by Race, Income, and Insurance Status. Pediatrics 97(1):26-32.
Overpeck MD, Kotch JB. 1995. The Effects of U.S. Children's Access to Care on Medical Attention for Injuries. American Journal of Public Health 85(3):402-404.
Prospective Payment Assessment Commission (ProPAC). 1992. Optional Hospital Rates for Private Payers Based on Medicare's Methods. Washington, D.C.: Author.
Rosenbaum S, Shin P, Smith BM, Wehr E, Borzi PC, Zakheim MH, Shaw K, and Silver. KA Johnson, Ed. 1997. Negotiating the New Health System: A Nationwide Study of Medicaid Managed Care Contracts. Washington, D.C.: The George Washington University Center for Health Policy Research.
St. Peter RF, Newacheck PW, Halfon N. 1992. Access to Care for Poor Children: Separate and Unequal? Journal of the American Medical Association 267(20):2760-2764.
Schneider A. 1997. Overview of Medicaid Provisions in the Balanced Budget Act of 1997, P. L. 105-33, Rev. 9/8/97. Washington, D.C.: Center on Budget and Policy Priorities. [http:/www.cbpp.org/908mcaid.htm]
SSA (Social Security Administration). 1997. The Definition of Disability for Children. SSA Publication No. 05-11053, July 1997. [http://www.ssa.gov/pubs/ 105 3.html]
Summer L, Parrott S, Mann C. 1997. Millions of Uninsured and Underinsured Children are Eligible for Medicaid. Washington, D.C.: Center on Budget and Policy Priorities.
U.S. House of Representatives, Committee on Ways and Means. 1996. 1996 Green Book: Background Material and Data on Programs within the Jurisdiction of the Committee on Ways and Means. Washington, D.C.: US Government Printing Office.
Zuckerman S, Evans A, Holahan J. 1997. Questions for States as They Turn to Medicaid Managed Care. Washington, D.C.: Urban Institute. [http://newfederalism. urban.org/html/anf_all.htm]





















