2
The Gaps Between Research, Treatment, and Policy
A committee member interviewed the director of a substance treatment program in a western state serving 37 male and 15 female substance-dependent patients who live on site for 90 days. They may stay another 30 days in less heavily supervised housing. When it started in 1972 the program aimed at "traditional" alcoholics, but most patients now have alcohol and other substance problems in combination. The staff is small and includes several recovering persons. Because of managed care reimbursement changes in recent months, the program faces a budget deficit this year. Over the years the program has come to rely heavily on block grant funding. Taking public funds, rather than relying on self-pay and other private sources, forces the program to accept more criminal justice referrals.
The program's board of directors primarily comprises older, conservative AA members. They are somewhat suspicious of changes, but they are willing to fund the program's deficit over the next year. Thereafter, if the financial problems are not solved, they probably will direct the program to revert to its former practice of
This chapter was edited by James L. Sorensen with contributions by Lisa Mojer-Torres, Kathleen T. Brady, Thomas Crowley, Emily Jean Hauenstein, A. Thomas McLellan, and Steven M. Mirin.
only housing alcoholic people as they attend AA. All counseling would be discontinued.
Relationship with Research
The program has never been involved in research. The director has no scientific training and has never applied for research funds. His board has encouraged him to apply for such funds, under the belief that if they receive research funds, they could use it for other purposes.
The director reports some interest in research based on his informal observation that perhaps one patient in five "makes it" to a consistently abstinent life. He would like to be able to predict which one out of five would be the successful one, and he would like to see more effective treatments for the other four out of five.
The director feels that involving his program in research might be good for staff morale because the staff is curious and wants to improve. He also worries that doing research probably would mean more work, and he expresses some concern that researchers might find his treatment to be ineffective. However, overall he feels the benefits would outweigh the risks. The director says that the program would be more likely to get into research if there were direct financial benefits. He feels that his Board would oppose introducing any more non-AA treatment as part of a research project.
Information Sharing on Treatment Advances
Regarding information dissemination, this director mentions "NIDA Notes" and says that a similar, brief publication focusing on treatment research would help him. The director receives most of his information about new treatments through peers in the state provider's association. He evaluates new treatment information based on a kind of "gut" feeling and his own extensive experience in the field. He is, for example, aware of naltrexone treatment for alcoholism, and he even attended a meeting sponsored by the drug's manufacturer. However, his program is not using naltrexone because he concluded that for his program, which has no medical or nursing staff, potential benefits from naltrexone would not offset the cost and effort needed to introduce it.
Summary
This man has worked for 25 years to help drug- and alcohol-dependent patients. This was the first time that a researcher had asked his opinion about the research-clinical interface. He provides shelter, support, strong encouragement of AA participation, and a small but caring treatment staff. Changes in his funding and requirements under the state block grant program and from managed care now force him to offer treatment to criminal justice patients with whom he feels less comfortable. Moreover, after 25 years in the field he is not sure that his program can survive financially for the next year. The board of directors is not very supportive of non-AA treatments. His work is consumed with making administrative changes to keep his program alive. He has no ill will toward research, and in fact supports the concept, but his program is struggling so much that it seems to him an unlikely site for conducting treatment research.
OVERVIEW
There are important gaps between the knowledge gained from research, everyday practice in community-based drug abuse treatment programs, and governmental policies about drug abuse treatment at the local, state, and national levels. Much has been learned about drug abuse treatment at each of these levels—research, treatment, and policy. Yet these groups make too little use of one another's knowledge base.
As the site visit report at the beginning of this chapter illustrates so well, there is often a wide cultural and experiential separation between the professionals who conduct empirical investigations and the men and women who apply research findings in treatment and policy settings. Researchers, moreover, study some treatments and leave other treatment modalities, settings, and populations underexamined. Sometimes it takes years for research results to affect treatment delivery. This lag in the diffusion of innovation has been well documented in other areas of health care (Eisenberg, 1986; Ferguson, 1995), but many components of drug treatment seem particularly resistant to incorporating research findings into treatment. Furthermore, relevant studies are slow to reach the desks of policymakers (Millman et al., 1990), and officials do not appear to rely heavily on policy analysis from research organizations (Lester, 1993). At the federal level the commitment to knowledge dissemination has waxed and waned over the years (Backer, 1991), but there are signs of a new upswing of interest in dissemination of information about research-proven drug abuse treatments.
The interactive communications thrust of the NIDA Drug Abuse Treatment Initiative is an example of this new interest.
EVIDENCE FOR THE GAPS
The evidence for the gaps begins with the different perspectives and priorities among researchers, treatment providers, and policymakers. The often overlooked consumer perspective is included as well. Examples of areas where there are clear gaps between research, treatment, and policy include pharmacotherapy, psychosocial interventions, and broader service delivery approaches (i.e., integrating drug and alcohol treatment with other medical treatment and social services, to address the multiple problems of many if not most addicted individuals).
Different Perspectives
Researchers perceive that many research-developed innovations have improved the treatment of drug abuse. For example, methadone maintenance treatment began as a research effort, and relapse-prevention techniques were honed by research investigations. Significant advances have been made in behavioral treatment of drug abusers (Stitzer and Higgins, 1995). The beneficial effect of including contingency-based counseling in methadone maintenance has been reported, as has the finding that contingency management is an effective way to promote abstinence during treatment for both heroin-dependent and cocaine-dependent patients. Studies have found that treatment intensity and systematic follow-up improve treatment results (Fiorentine and Anglin, 1997; Hoffman et al., 1994; Price, 1997; Simpson et al., 1997). Researchers believe that patient outcomes would be significantly improved if these, and other research-tested modalities, were fully utilized in treatment.
Treatment providers have a different perspective. Faced with the challenges of providing services on a daily basis, providers are often frustrated by what they see as the failure of research to provide them with relevant answers to their important questions. Many of their most important questions are in policy- and reimbursement-related areas that, at least until recently, have been under researched. They perceive that current policy provides little incentive for treatment programs to implement new research findings. For example, some states (currently, Idaho, Mississippi, Montana, New Hampshire, North Dakota, South Dakota, Vermont, and West Virginia) prohibit methadone treatment except for detoxification. One representative of a state provider association reported that reimbursement in that state was too low to allow the implementation of effective contingency
models, even if direct payment to consumers were permitted by federal policy controlling the use of block grant money.
Those who define and implement policies have a third perspective and report yet another set of problems. They do not find the research literature easily accessible. They point to the oversupply of information at all levels, too little of which supports the cost-effectiveness of the programs they fund and administer. For information to be effective, they argue, it must respond directly and easily to the needs of increasingly time-pressed individuals and organizations. Providing information on complex and difficult technical issues poses special challenges for all involved (IOM, 1997b). Frustrated by the time lag and the flood of printed material, policymakers tend to rely on familiar sources to select and summarize the information relevant to them as the issues emerge (Young, 1997).
Policymakers and treatment providers both faulted researchers for having no concept of real time. One provider who participated in a multisite study comparing treatment modalities said that some programs were dead when the positive findings were reported five years after the study ended. However, the value of having the right information at the right time was illustrated by the workshop participant who reported that a timely cost effectiveness study resulted in the 600 substance abuse treatment programs in Ohio receiving a 30 percent funding increase for the biennium (Ohio Department of Alcohol and Drug Addiction Services, 1996). A state agency director expressed the need for faster research turnaround this way:
Much research now being published was conceived several years or a decade ago, when a much different system was in place—when today's problems were just beginning. Research funding should support more exploratory, quasi-experimental, clinically relevant studies. Secondary analyses and meta analyses of state agency data might reveal useful information. (Appendix J)
The consumer perspective is often overlooked. There is no popular literature pushing new research findings to consumers, as there is for other chronic disease conditions. Consumers generally have fewer options in selecting drug treatment programs than in other areas of medical care. When choice is available it is difficult to obtain information to make an informed decision and the individual may also find that the treatment of choice is not provided or not covered by their insurance. Few treatment consumers are effective advocates, and former consumers are busy building lives. Individuals needing treatment may want more treatment capacity to reduce waiting lists, more convenient locations and hours for treatment, better integration of drug abuse treatments with other needed medical and social services, counselors with more training, better detoxification facilities, more research into the causes and treatments of drug abuse disorders, and help in reducing
the increased risk of drug problems among children of drug abusers. But, there is little structure for consumer input. The stigma and denial attached to addiction inhibit consumer action and social support.
Despite these handicaps, there is support for treatment and research for problems of drug dependence. Often it is built on the need to defend society from drug abusers, rather than on a need to help "victims" of addiction. Mayors and county officials may lobby their state and federal representatives for help in controlling drug problems with treatment. Judges and district attorneys can also be effective voices for change as they seek treatment resources for the growing drug court movement (Drug Strategies, 1997); but drug abusers rarely lobby for more treatment. Addicted persons are not in a strong position to ask society for help.
Research Findings That Are Underutilized in Treatment
The committee identified several examples of research findings that are not generally utilized or are underutilized in various components of the treatment system. They include pharmacotherapy and psychosocial treatments as well as service delivery approaches. The issues are introduced in this chapter to illustrate the consequences of the gaps between research, treatment and policy. They are discussed in greater detail in a paper by McLellan and McKay included as Appendix D.
Medications in the treatment of drug abuse disorders are underutilized in many community-based treatment settings. Methadone maintenance for treatment of opiate addiction provides an example of the difficulty implementing established findings and knowledge in this field. Adequately designed clinical trials have consistently shown that methadone maintenance treatment is effective only when methadone is given in adequate doses (Ball and Ross, 1991; Caplehorn and Bell, 1991). Despite this research finding, past surveys have found many treatment programs that prescribe inadequate methadone doses (Calsyn et al., 1991; D'Aunno and Vaughn, 1992), although this situation may be improving according to recent reports (Leshner, 1997).
The reasons for this low dosage of methadone may still include lack of adequate information concerning the effectiveness of higher doses, despite public statements of support by such authorities as the National Institutes of Health and Office of National Drug Control Policy. Ambivalent attitudes concerning the use of medications in the treatment of drug abuse disorders may also be a contributing factor. However, while this study was under way, an important and historic event took place which may be a hopeful indicator for change. In 1997 the National Institutes of Health convened a Consensus Development Conference on Effective Medical Treatment of Heroin Addiction, the first NIH conference on this topic. After
hearing from many experts the consensus panel concluded that opiate addiction met the criteria of having effective medical treatment and established diagnostic criteria, and it made recommendations for improving treatment access and identified future research areas and training needs. The consensus statement from this conference is included as Appendix F.
Another example of this gap between research and practice is the underuse of naltrexone, a pharmacologic treatment (opiate-antagonist) which has long been shown to be effective in preventing relapse to opiate addiction in highly motivated patients (Brahen et al., 1978). Several well-controlled studies have also shown naltrexone to be effective as an adjunct to a variety of psychosocial rehabilitation interventions in the treatment of alcohol dependence (Volpicelli et al., 1992). In 1994, naltrexone received Food and Drug Administration (FDA) approval for use in the treatment of alcohol dependence.
However, naltrexone is not widely used in alcohol treatment outside of medical centers and some specialized treatment settings. The manufacturer of naltrexone estimates that approximately 80,000 individuals were treated with naltrexone in 1996 for all indications. Even allowing for a large margin of error, these figures indicate that naltrexone is prescribed for less than one percent of the persons who might benefit. The reasons for this low utilization are unclear, but they likely relate to some of the organizational constraints described above, including lack of available medical expertise, lack of cost reimbursement coverage, and lack of information concerning the cost-effectiveness of adding this medication to current treatment strategies.
A final example of an established research finding that has not been adopted widely in clinical practice is the integration of contingency management strategies in community-based treatment settings. The knowledge that positive reinforcement can increase desired behaviors has been empirically demonstrated in both laboratory and clinical settings. Over the years, these principles have been applied to drug abuse treatment in several ways. In a study of cocaine users, Higgins and colleagues used a system of vouchers which could be traded for material goods which individuals received when the routine urine testing proved negative (Higgins et al., 1994). This research, when compared to noncontingent vouchers, demonstrated a very beneficial effect of the voucher system in increasing drug-free urines. This study has since been replicated (Silverman et al., 1996) in a number of different treatment settings. Despite this, the use of positive reinforcement or a voucher-based system has not been widely implemented in treatment settings. Again, the barriers are multiple, including lack of information concerning the efficacy of these strategies as well as implementation difficulties due to payer policies. Several workshop participants expressed concern about these barriers and one provider reported that the average total
treatment reimbursement in his state was less than the value of one set of vouchers. And certainly there is the public perception that people should not be paid for staying drug free.
Service Delivery Approaches
Drug abuse providers treat persons who are physically, emotionally, socially, and economically unstable. Standard treatments may target only one facet of their need. Service delivery methods, which involve bundling drug abuse treatment with other services that address the multiple disabilities of addicted individuals, have been shown to promote recovery and prevent relapse. Service delivery approaches include, for example, case management, rapid admission, programs geared to the special requirements of treating women with children, as well as so-called ''wraparound services" such as medical care, job training, and social services. Providers who spoke with the committee saw the decline of such services in their communities as a significant barrier to successful treatment. Research based on data from NIDA's Drug Abuse Treatment Outcome Study (DATOS) reports a widening gap over the last decade between the need for services that go beyond basic drug abuse treatment and the supply of such services (Etheridge et al., 1995). An exception to this disheartening decline of supportive services is the DATOS finding that methadone programs are treating more medical problems than in the past. This report also mentions that methadone dosage levels have improved from earlier years (Leshner, 1997). Others have reported the need for and the contribution of supportive services to treatment outcomes (Ball and Ross, 1991; McLellan et al., 1994; Widman et al., 1997).
Adolescents with a drug abuse problem are another special needs population and one that is still growing overall despite the decline at younger ages (Johnston et al., 1997). When there is co-occurring mental illness or physical handicaps in this population the need for integrated services becomes even more important. Yet few are able to receive treatment from a single source. And if they do find treatment they may be subject to conflicting directions of mental health and substance abuse clinicians. Left to the mercies of these disparate systems, many such young people fall through the cracks (National Health Policy Forum, 1998).
Other special needs in consumers of drug abuse services also have motivated a services delivery approach to treatment. For example, drug abusers are at high risk of contracting the human immunodeficiency virus (HIV), and those with HIV have significant medical needs that cannot be managed in many treatment programs (e.g., HIV treatment, tuberculosis monitoring and diagnosis, and treatment of sexually transmitted diseases) (Selwyn, 1996). Many community-based treatment organizations (CBOs)
that treat drug abuse are not equipped to manage on-going primary care for these complex needs. This has motivated some programs to integrate primary care services with drug abuse services for these special populations, typically in university-based settings, but the effectiveness of integrated services requires systematic evaluation. Similarly, drug abusing women and their children require a composite of services to effect positive outcomes (Rahdert, 1996) (see Box 2.1). In the California comprehensive model of care for drug-addicted women, the relationship between services offered and outcome is currently being evaluated (Brindis et al., 1997).
Evaluations of the effectiveness of service delivery methods have identified important variables in determining outcome, including patient factors at treatment, duration and intensity of treatment, and service delivery methods and their determinants (McLellan et al., 1996). Outcome studies of a wide variety of programs and service delivery methods demonstrate, when keeping patient characteristics, treatment intensity, and duration constant, some programs have much more success than others. In another study of subjects receiving methadone only, standard methadone treatment, and enhanced methadone services, the enhanced treatment group demonstrated the greatest improvement in the areas of personal adjustment and public health and safety risk (McLellan et al., 1993).
However, reviews of multimodal service delivery across a variety of settings indicate that many modalities had not been sufficiently evaluated (Floyd et al., 1996). Properly designed research is needed to assess the extent to which improvement in outcome can be expected using various increments of treatment intensity. This requires systematic variation in treatment dose as a key element in determining outcomes. In order to determine the most cost-effective mix of treatment and service delivery methods, much more well-designed health services research must be conducted in this area.
According to a state agency chief and research director who were interviewed by a committee member, state planners would like research in community programs to address such issues as:
Treatment Approaches That Are Understudied in Research
Just as research findings have been underutilized in the treatment community, there are treatment approaches that have been understudied by the research community. In committee roundtables providers said they needed
|
BOX 2.1 Pregnant and Parenting Women She has been hiding her drinking, but doesn't know how much longer she can fool the people around her. She is ignoring the kids and feels guilty, seems like all of the time now. She is terrified that her ex-husband will find out that she's drinking so much and get the judge to take the children away from her. Maybe he should—I'm a lousy mother anyway." Someone told her about a clinic where she could get sober. "Would it work for me? Can I afford it? Who will take care of my kids?" The first place women go to get help is their primary care provider. Here, screening for substance abuse is uncommon, so substance abusing women go unrecognized. When these practitioners do discover their client's substance abuse they often are judgmental. This especially is true if the woman seeking help is pregnant or has young children. The provider has to decide whose rights to consider, the mothers or her children's. Most commonly the rights of the women are secondary. This can lead to loss of custody of her children, her unborn baby, and to prosecution for her. A woman will avoid this punitive environment often putting herself, her baby, and her other children at further risk. Substance abuse is rising among young women and this has brought new challenges to the treatment community. Most treatment models are based on experience with men, and do not work well for women. Research has shown that women have better treatment outcomes if their treatment is based on a family model of care that includes gender-specific treatment. Therapeutic modalities shown to be effective for women include group therapy, treatment separated from males, and the use of female therapists Comprehensive services that include the needs of children like day hospitalization for their mother, residential treatment, and prevention services for them also seem promising. Federal legislation in recent years has spawned the growth of women's services within existing treatment venues and the development of a significant number of new program. The-treatment community in California for example, has used these legislative initiatives to develop a continuum of programs that extend from prevention to residential treatment. The rapid development of women's programs has not permitted systematic evaluation of treatment effectiveness. This is a unique opportunity for the research and treatment communities. Researchers have the chance to study treatment through all stages of its development and implementation. CBOs that treat women may be more receptive to research since their organizations are relatively new, often based on scientific theory, and less entrenched than those providers with a longer treatment tradition. The development of evidence-based treatment for women is an opportunity to set a research agenda that is bidirectional, collaborative, and creates partnerships between researchers and providers. SOURCES: Abcott (1994); Brindis et al. (1997); Brindis and Theidon (1997); Garcia (1993); Grella (1996); Kaufman (1996); Light et al. (1996); Mallouh (1996); Naegle (1968); Pokomi and Stanga (1996); Ripple and Luthar (1996); Samsioe and Abreg (1996); Streissguth (1993). |
practical, relevant research results that they could implement with the resources available to them. Some representatives of community-based drug treatment programs expressed the belief that researchers were not knowledgeable about community-based treatments. They suggested providers should be involved in research from the beginning to help formulate research questions that were important to them, rather than just serving as a research site for investigating researchers' ideas. As the paper by McLellan and McKay points out there is a strong need to identify clinical and policy issues that should be the focus of future research to fill the gaps between what is known and what needs to be known (see Appendix D). The committee found little evidence of research that systematically examines the distribution of treatment research across different kinds of modalities of drug abuse treatment.
The National Institute on Drug Abuse recognizes that very few researchers are studying therapeutic communities, and the research that has been done tends to focus on assessing their overall effectiveness rather than investigating how they work, why, or for whom (Chasnoff et al., 1996). Consequently, NIDA has given a prominent role in its new treatment initiative to increasing research with therapeutic communities (Leshner, 1997).
The treatment modality most commonly available is the outpatient modality. Outpatient programs offer counseling to drug abusers or their families. The term "outpatient" encompasses a variety of treatment programs that may have little in common, except that they do not offer a place to live (Sorensen and Bernal, 1987). The 1990 NIDA-sponsored Alcohol and Drug Research Study found that outpatient "drug-free" treatment accounted for approximately half of the total treatment, and were offered in 71 percent of all facilities (Batten et al., 1993). Preliminary data from a SAMHSA study carried out by the same researchers in 1997 showed that outpatient nonmethadone treatment accounted for more than 60 percent of total treatment in a national sample of drug and alcohol treatment facilities (see Appendix E).
Other nontraditional treatment programs may be more widespread than research evidence would indicate. For example, acupuncture treatment of addiction is commonplace in the growing drug court movement. The National Acupuncture Detoxification Association points out that acupuncture is used in over 200 programs across the United States. There have been many studies of its potential usefulness but until now these studies have generally provided equivocal results because of design, sample size, and other factors. A review of 22 controlled clinical trials of acupuncture for addiction treatment concluded that the strength of positive findings varied inversely with the methodological rigor of the study (Ter Riet et al., 1990). Widespread support for acupuncture has persisted despite these review findings. An NIH consensus development panel reviewed this issue
in November 1997 and concluded there are promising results in some areas (e.g., dental and postoperative pain and chemotherapy nausea and vomiting); in other situations (e.g., addiction, stroke rehabilitation, and asthma), acupuncture may be useful as an adjunct treatment or included in a comprehensive management program. They cited the emergence of plausible mechanisms for the therapeutic effects of acupuncture as encouraging and concluded that "there is sufficient evidence of its potential value to conventional medicine to encourage further studies. There is [also] sufficient evidence of acupuncture's value to expand its use into correctional medicine and encourage further studies of its physiology and clinical value" (NIH, 1997).
Studies of patient factors, treatment factors, and community factors in treatment outcome research are all needed, as are studies of the effect of payment level and political environment on treatment outcome. Treatment provider professionals have a variety of questions that could be addressed in research but are not receiving sufficient attention. Patient factors have been much more widely studied than have treatment setting or modality, perhaps because there are few measures of treatment setting or treatment services. Treatment providers speaking to the committee recommended directing research attention to such challenging problems as community resistance to the placement of drug treatment facilities, the so-called "NIMBY" (not in my back yard) problem. This is a problem that requires measurement of neighborhood and organizational systems, as well as individuals. Several workshop participants commented on the role that the different perspectives of researchers and treatment programs played in determining what research was done. One participant reported that in her state the treatment and research communities held differing views of addiction, one favoring the disease model and the other a behavioral model, which presented a barrier to research collaboration. There are substantially different views about the desired "outcome" of an addiction treatment. For example, studies using an outcome of "percentage improvement'' in needle use will have little credibility with a clinician who believes that abstinence is necessary for recovery to occur.
Many clinical trials exclude the classes of patients that are most prevalent in community-based agencies, and consequently findings from such research do not seem relevant when viewed by treatment providers. To illustrate, studies of treatment techniques for cocaine abusers commonly screen out potential participants who are also abusing alcohol. This not only limits the generalizability of the research, it also reduces the study's credibility to the provider community, because cocaine abusers normally present for treatment with alcohol abuse and a variety of other problems that would have led to their exclusion from much research. Another difficult but important population needing study is the large and seemingly
growing number of individuals with co-occurring mental illness and substance abuse problems.
Stated in the vocabulary of health services research, the treatment community perceives there is a surfeit of "efficacy" research (studies conducted under controlled experimental conditions) and a shortage of "effectiveness" studies (where treatment modalities are studied under real-world conditions). Many of the treatments that receive research attention are resource-intensive interventions studied under rarefied conditions for fixed periods of time.
A comprehensive review of the treatment outcomes literature prepared for the committee is included as Appendix D. This review of what treatment has been studied offers some starting points for filling in the gaps between what is known and what needs to be studied. While the authors acknowledge that the existing literature is disappointing with regard to informing practice at the level of the community treatment program, they identify findings from controlled clinical research that have been significantly and repeatedly related to favorable outcomes and do suggest important directions for treatment practice in the real world. Their findings also suggest that a reader will get substantially different views about the outcome of treatment, depending upon the perspective taken regarding what "outcome" is and when, how, and by whom it is measured. The paragraph below illustrates the significance of this point.
A quality assurance or service delivery evaluation of [an adduction] treatment [program] might conclude that the program "had very good outcomes" since there was no waiting for treatment entry and at discharge, more than 80 percent of the patients were "highly satisfied" with their counselor and clinician. A clinical researcher, having interviewed a sample of patients at admission to the program, and again six months following discharge, might conclude that the program "had mixed outcomes" since at the follow-up point, only 50% of the patients were abstinent (the intended goal of the program), but there was a 70 percent reduction in frequency of drinking and a 50 percent reduction in medical and psychiatric symptoms. Meanwhile, an economist or health policy analyst might have used Medicaid data tapes to compare the health services utilization rates of a sample of discharged patients, two years prior to their treatment admission and two years following their discharge. The conclusion here might be that "treatment had very poor outcome" since there had been no decrease in medical care utilization from the pre- to the posttreatment period, hence no "cost-offset'' to the public. (McLellan and McKay, Appendix D).
Overall, there is a need to distinguish between what has been understudied and what has been studied substantially but found to be ineffective. In this field, as in other areas of health care, therapeutic practices remain
prevalent in the field even though they have not been tested or shown to be effective. There is a pressing need to catalogue the treatments that have been proven to be effective and to develop a research agenda that will stimulate systematic review of the others.
Policies That Impede Treatment
Further, there is a need to review the policies that may put barriers in the way of the utilization of proven treatments and the development of new ones. For example, state regulations can be a barrier to the integration of methadone treatment into comprehensive treatment facilities and laws in some states prohibit methadone maintenance entirely. State regulation is an even greater barrier for treatment providers desiring to use newly developed medications. Each state is responsible for amending its narcotics regulations to permit treatment with new medications. This slow, cumbersome process can take several years and is a barrier to the development and implementation of new treatments (IOM, 1995). And finally, financing policies that bar the use of effective treatment strategies or that contribute to the decline of needed support services (e.g., medical, employment, and social services) should be examined within the context of closing the gaps and making the treatment system work.1
BARRIERS TO CLOSING THE GAPS
There are several sets of barriers to be overcome in order to reduce the gaps in understanding and communication across the research, treatment, and policy communities. Some of these barriers are held in common across the three communities. These barriers became readily apparent in the workshops and other data-collection activities carried out by the committee. Some of the principal barriers are described in the remainder of this chapter, and the following chapter identifies some potential solutions. However, as the British Navy story below illustrates (Box 2.2), innovations, even successful ones, do not sell themselves.
Structural Barriers
Community-based drug treatment organizations must comply with the directives and regulations of their funders. Like other publicly funded orga-
|
1 |
See Chapter 5, Treatment Financing and Trends in Health Insurance, in The Development of Medications for the Treatment of Opiate and Cocaine Addictions: Issues for the Government and Private Sector for a concise review of the complexities of the financing disincentives in this field (IOM, 1995). |
|
BOX 2.2 Controlling Scurvy In the British Navy: Innovations Do Not Sell Themselves In 1601, an English sea captain James Lancaster, conducted an experiment to evaluate the effectiveness of lemon juice in preventing scurvy. The beneficial effect of lemon juice was so clear that one would have expected the British Navy to adopt citrus juice for scurvy prevention on all its ships. But it was not until 1747, about 150 years later, that James Lind, a British Navy physician who knew of Lancaster's results, carried out another scurvy experiment on the HWS Salisbury . The scurvy patients who got the citrus fruit were cured in a few days. Certainly, with this further solid evidence of the ability of citrus fruits to combat scurvy, one would have expected the British Navy to adopt this technological innovation for all ship's crew on long sea voyages. And, in fact it did so. But not until 1795, 48 years later. Scurvy on Navy ship was immediately wiped out. And after only 75 more years, in 1865, the British Board of Trade adopted a similar policy, and eradicated scurvy in the merchant marine. SOURCE: Condensed from a case illustration in Rogers (1995), originally based on a 1981 article by Frederick Mosteller. |
nizations, they must justify their existence to their community, payers, and constituency. Concern with survival naturally diverts attention from the development and expansion of the treatment program. Under these circumstances, involvement in research or adoption of new treatments cannot compete with more immediate concerns.
The typical treatment organization is small, employing less than 30 workers. Resource constraints limit the type and range of services the organization can provide, and it often lacks the financial and human resources to participate in research. Even the introduction of new treatment modalities may be impossible for many CBOs without significant external financial support
The core staff will likely include a mix of counselors in recovery and those who were introduced to the field through graduate training. The number and mix of practitioners are sufficient to support a specific treatment program and achieve a sufficient revenue base. However, implementing new psychopharmacological therapies generally requires adding medical staff, and new behavioral interventions may require trained psychologists who are not a part of current staff (Stitzer and Higgins, 1995). CBOs are frequently unable to afford the additional professional time to implement new treatments (Naranjo and Bremmer, 1996). Even those with enough resources may be reluctant to spend the amounts required.
Managers play an important role in implementing organizational
change. But many forces may impede them in the dissemination and application of research findings. Changes in Medicaid, for example, may mean changes in billing, documentation of patient care, and services provided. Changes in patient mix create new demands on managers. This is especially true in drug abuse, where treatment needs are specifically linked to the drug used. Since drug user choices are influenced by supply forces, there are often rapid shifts as new types of drugs become more readily available. Managers must be cognizant of drug trends in their constituency and adjust treatment services accordingly. Introduction of new treatment is, understandably, less compelling to managers than dealing with immediate challenges in the external environment.
Factors internal to the organization also occupy managers' attention. When managers are therapists, they may have difficulty providing leadership to implement new treatments. Treatment providers may be reluctant to change methods of treatment. Changes in treatment approaches take time and effort, and many front-line treatment providers do not feel they have the time for such retooling. To the extent that manager-providers share these same attitudes, the likelihood of implementing new treatments is decreased. The manager who is not a provider may be less reluctant to introduce change, but may also be less likely to understand the relevance of new treatment findings to the treatment program's constituency. If the manager is receptive to new findings, he or she may lack the technical or leadership skills to ensure their adoption into treatment.
Financial Barriers
Community-based drug treatment organizations are supported primarily by public funds through block grants, Medicaid, other local funding, and private health insurance. An increasing percentage of their clients come from criminal justice sources. Each of these payors has regulations that affect services provided by CBOs. To receive funding, organizations must comply with a multitude of payor-specific criteria—accurate diagnosis, justification of the medical necessity for the provision of services, documentation of care, and reports about client progress. Payers may limit the intensity and length of care provided. Patient care reporting and billing requirements vary widely across payors, but the CBO must meet all requirements in order to be paid for services.
By accepting block grant funding states accept provisions which affect how drug abuse treatment is delivered. Block grants require the states to ensure the provision of prevention services, outreach for injection drug users, and early intervention for those at risk for HIV. Currently, injection drug users and pregnant women receive priority. Treatment providers must provide mandated services to maintain their financial viability. Block grants
also regulate what services can or cannot be provided, for example, generally restricting inpatient care, cash payments to patients, and needle exchange programs. The states pass on these requirements to the treatment provider.
Over-emphasis on drug courts and prison treatment programs can result in treatment funds being carved out or diverted disproportionately into the criminal justice system, with the ironic result that some people needing treatment, especially among the poor, have nowhere else to turn. Communities, in other words, should not require someone to throw a brick through a window in order to get treatment.
Treatment for Addiction: Advancing the Common Good Join Together (1998), p. 17.
Since most drug abuse treatment facilities derive a portion of their funding locally, they must also be responsive to community priorities and community opinions. In most communities, public opinion favors criminal justice intervention rather than treatment intervention. This is evidenced in drug interdiction policies at the federal level and community preferences for jailing those who have committed nonviolent offenses while abusing drugs or alcohol.
In order to maintain funding and community support, community providers must often avoid the use of treatments viewed as controversial. This, for example, could restrict the applicability of contingency management techniques. This apparently effective treatment modality is also controversial because it is viewed as rewarding drug abusers for their actions. Likewise, discharge of patients followed by their involvement in a very public crime has direct implications for local funding of drug abuse. In this environment CBOs proceed cautiously when considering the adoption of new treatments. In summary, many CBOs do not have sufficient organizational resources to implement new treatment findings while also dealing with the complexities of their real world political and financial environment.
Education and Training
A sequence of steps must occur for a provider organization to be successful in adopting new treatments. These steps include becoming aware
of the new treatment, evaluating its utility in the local setting, trying out the new treatment, adopting the new treatment, and confirming that the new treatment works with local clients. These steps to provider adoption of new treatments require that education and training in the new treatment be provided by the organization. A number of factors contribute to making this a very challenging objective.
There are at least three categories of providers within the drug abuse treatment community: (1) licensed practitioners, educated, at a minimum, at the master's degree level and who have received specific education in drug abuse treatment; (2) nonlicensed practitioners (many with college training in another field) who receive on-the-job training in the provision of drug abuse treatment; and (3) the recovering drug abuser who also has received on-the-job training. (Recovering providers can also be in the other two categories.) One survey of 1,328 drug and alcohol counselors found that about 45 percent of respondents had graduate degrees. Nearly one out of two respondents (46 percent) identified themselves as in recovery. Counselors without degrees (81 percent) and those with associate degrees (72 percent) were more likely to report that they were in recovery. Of those with doctoral degrees 18 percent also reported that they were in recovery (Mulligan et al., 1989).
Professionals with graduate training also receive on-the-job training, but experience is not their only reference point for practice. These providers are more likely to be exposed to a model of life-long learning and to be familiar with the processes of acquiring new formal knowledge to improve their treatment.
Drug abuse treatment providers who gain knowledge primarily through experience and on-the-job training may not be as open or as able to participate in the adoption of new treatments that are outside their experience base. The apprenticeship model of training is more viable where a relatively narrow range of duties are performed and when the work environment is relatively predictable. Predictability is decreasing in jobs in most fields, and this is true in the drug abuse field as well. The introduction of new treatments affecting significant numbers of consumers can be destabilizing to an organization and the providers. Staff may not readily adapt to such a change, especially one that requires a change in their behavioral repertoire that takes them out of their "comfort zone."
Efforts to improve the standards of behavioral health care can also tend to undermine the worker trained in an apprenticeship model. State standards are harder to meet for providers trained in the apprenticeship model. Introduction of state provider-qualification requirements has fueled a debate within the drug abuse treatment community about what constitutes appropriate treatment. This debate may work against the adoption of new treatment modalities in CBOs.
Recovering people fear being taken over by people with letters after their name.
Beny Primm, M.D., Committee Workshop, July 29, 1997, Washington, D.C.
Even when studies document that a treatment can be successfully implemented in a clinical setting, the challenge of the final stage of transfer to treatment programs is often daunting. It requires training staff in delivering the new treatment, changing attitudes of the providers so they embrace the new treatment, and providing evidence that the new treatment is effective in the local clinic situation. Each of these components of training poses problems for the treatment program. Training must be planned, systematic, and protective of the fidelity of the treatment. Researchers who establish treatment effectiveness are sometimes best able to translate the intervention. With the right skills, these researchers can provide the requisite training, anticipate the difficulties, assist in the process of changing provider attitudes, and encourage providers to "own" the research. If this transfer of ownership does not happen the prospects are poor for sustaining the intervention after the researchers are gone (Altman, 1995).
However, few incentives currently exist for researchers to participate in the final processes necessary for a successful adoption. Researchers may not have the skills or may be unwilling to engage in on-site training and mentoring of providers as they implement new treatments. When a CBO is ready to implement the new treatment findings, their research partners have often gone on to other studies. Researchers are generally interested in testing new treatment paradigms, and they are more likely to be funded when they design experimental research. These disincentives have impeded research translation. Neither research translation nor dissemination plans are explicitly weighted in the evaluation criteria for research grants. Dissemination activities count far less than scientific publications for academic promotion. Consequently, there is little organized effort to disseminate research to practice and those who do conduct such activities often do not have the organizational status to successfully carry out this difficult task. This is by no means a problem unique to community-based drug treatment. All too little effort goes into ensuring the use of evidence-based practices in any health care field.
Research is like insurance, it is often sold but seldom bought.
Robert 0. Phillips, NAADAC Southwest Regional Vice President, Committee Workshop, September 8, 1997, Albuquerque, NM
Effects of Stigma
Stigma is a special problem for the drug abuse treatment field in many ways. As with other chronic, relapsing medical conditions, there is no cure for addiction, but the existing treatments allow for successful management of addiction and prevent the development of more expensive medical disorders. The major difference is the public's perception of chronic diseases, such as hypertension, diabetes, and asthma as clearly medical conditions, where addiction is more often viewed as a social problem or character deficit. There is no serious argument against supporting health care systems for hypertension, diabetes, or asthma, but there is still much debate regarding support for treatments of addiction (O'Brien and McLellan, 1996).
People who work in drug abuse treatment programs may face a very personal problem of stigma. In many places working in this field is considered a mark of failure. The existence of the programs is often in doubt. Public drug treatment programs often are inadequately funded and staffed and have long waiting lists. The NIMBY syndrome defeats many efforts to site new drug treatment facilities (see Chasnoff et al., 1996, and Box 2.3).
There are few advocates for drug abuse treatment. Persons who have other chronic disorders, or who have family members with those disorders, benefit from disease specific advocacy efforts like the American Heart Association, the American Cancer Society, or the American Lung Association. These organizations educate the public about these disorders, and they provide some (although usually limited) direct services to their "victims." They raise money to support research and educate policymakers to help obtain additional funds for research and treatment. Because people see those with heart disease, cancer, or birth defects as "victims," they are willing to contribute through private channels and with tax moneys to fight those disorders. Unlike these fields in which patient groups provide a strong voice for treatment and research, generally little is heard from people who suffer from addictive disorders.
Some advocacy groups have been successful however. The Gay Men's Health Crisis and other AIDS advocacy groups have been very successful
|
BOX 2.3 A Closed Door At the request of his state drug abuse authority, one member of this committee opened a methadone clinic in a rural community. At a get-acquainted meeting with the city fathers, he was told bluntly that the community leaders did not want methadone treatment in their area. They were not interested in research data showing methadone's reduction of crime and health-care costs; they preferred that those who needed methadone treatment move to a city with a methadone clinic. |
despite the double societal stigmas of their disease. The National Alliance for the Mentally Ill (NAMI) is an excellent example of effective advocacy efforts lead by family, friends, and supporters of those who suffer from mental illness. The National Alliance of Methodone Advocates (NAMA) also provides a working example of how those most affected by addiction can advocate for themselves.
Another stigmatizing factor is job status. To a greater degree than in other chronic disorders, the field of addiction has in the past had large numbers of workers who have themselves experienced the problem. This included physicians and nurses as well. Of all the health care treatment programs, drug abuse treatment may be the most frequent employer of its own graduates. Historically, and to some extent yet today, the ranks of counseling have been filled with significant numbers of former drug abusers, while the ranks of administrators have been less so (Brown, 1997). This disparity in status is often complicated by co-occurring ethnic differences.
Recovering workers have been increasingly accepted as effective counselors (Christensen and Jacobson, 1994), and there has been a growth in the development of certification programs for drug abuse counselors. Nonetheless, credentialing requirements tend to discriminate against experientially trained staff, and counselors in recovery are challenged to develop a more theoretical perspective and apply research in their clinical work.
The stigma of the field may also contribute to the lack of mainstreaming of substance abuse in the curricula of undergraduate and graduate programs in health-related fields. The recommendations of the 1995 conference on training sponsored by the Macy Foundation represent a step in the right direction as does the inclusion of this training objective, for the first time, in the National Drug Control Strategy (ONDCP, 1998).
The Macy report recommended training about drug and alcohol abuse for all primary care physicians (i.e., family-practice, internal medicine, pediatrics, and obstetrics-gynocology). Internal Medicine residency programs are now required to have this training (Josiah Macy, Jr. Foundation, 1995).
Subsequently an IOM committee also made training recommendations in this area. Their investigation led them to conclude that the lack of courses in addiction starts a cycle of shortages at every stage of the professional pipeline, and that as a result fewer undergraduates are exposed to scientific information about addiction, fewer graduate students and medical students express interest in the field, causing fewer administrators to seek faculty with addiction expertise, resulting in fewer young professionals on the faculty, and ultimately, fewer senior faculty to mentor those who might be interested in practicing addiction medicine or doing research in this field (IOM, 1997a).
Objective 4: Support and promote the education, training, and credentialing of professionals who work with substance abusers.
From Goal 3 of Strategic Goals and Objectives of the 1998 National Drug Control Strategy; ONDCP (1998), p. 27.
There appear to be few opportunities for training in a community setting, for either physicians or other health professionals. One such program, Physicians in Residence, provides a hands-on, five day program for residents which includes training and practice in interviewing, assessment and treatment planning, as well as participation in AA meetings. Residents left the program reporting confidence in their new skills, however, a follow-up evaluation suggested they needed continuing support to integrate and maintain these skills in a work environment where substance abusers were less interested in treatment (Levin et al., 1996). Addiction treatment training, as well as research training in community-based treatment facilities requires more opportunities for hands-on experience and continuing education.
Inadequate Knowledge Base About Technology Transfer
There is little information about spread of innovations in drug treatment and how treatment programs use research findings in their work. A qualitative approach to studying technology transfer occurs more frequently than quantitative procedures, and sophisticated research techniques are the exception rather than the rule. Typically, surveys in this field do not include questions about the adoption of new treatment techniques.
NIDA's main extramurally funded research study on technology transfer, according to Backer (1991), was conducted over a six-year period in the
1980s and concerned a method for providing employment-related training for ex-drug abusers (Hall et al., 1988; Sorensen et al., 1988). This random assignment study found that dissemination methods employing personal contacts (site visits and conferences) produced significantly more adoptions than did printed materials alone. There were also adopter site differences: residential programs were more likely to adopt the employment workshop than were outpatient programs.
Published case studies include a description of the implementation of NIDA's cocaine prevention program (Forman and Lachter, 1989). NIDA also sponsored a project to educate injection drug users about HIV risk reduction outside of drug abuse treatment clinics (Brown, 1995). Their dissemination model included extensive training and technical assistance with a newsletter publicizing the positive outcomes, and annual meetings of program administrators and practitioners. Another case study examined the difficulties of disseminating an alcohol withdrawal protocol and a pharmacotherapy technique (Naranjo and Bremmer, 1996). A case study of an international project called Effective Care in Pregnancy and Childbirth reviews and illustrates the principles involved in ''retailing research" to bridge the barriers across the cultures of researchers and practitioners (Lomas, 1993). Technology transfer in drug abuse treatment appears to be a fruitful field for further work.
Policy Barriers
In the environment described above, it is easy for society to ration drug treatment, or reject certain forms of treatment. The usual argument advanced for funding drug abuse treatment is not that addiction is a treatable chronic disease, but that drug abuse treatment is cheaper than prison and cheaper than treating AIDS. Drug-dependence treatment is relatively cheap, although not readily available. Residential treatment programs provide intake evaluations, group and individual counseling, recreational therapies, urine monitoring, transportation to supervised work, regular reports to licensing and referring agencies, housing, and all meals at a daily cost less than the bill for sleeping overnight at a mid-price hotel and considerably less than the costs of staying in jail (Kaskutas, 1998). As shown in Figure 2.1, all federal spending on drug treatment has increased less than inflation in recent years.
Prejudice against addicts can also lead to policies that prevent the use of improved treatment approaches. Research has shown that prolonged maintenance treatment with methadone and other opioid agonists like LAAM (levo-alpha-acetylmethadol) and buprenorphine reduces mortality and morbidity among drug abusers and reduces crime in the community (see Appendix F). However, methadone maintenance treatment is banned in many
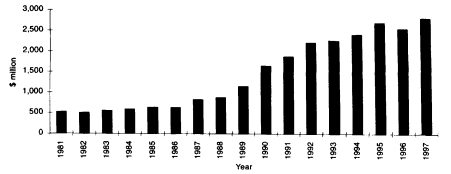
FIGURE 2.1 Federal drug abuse treatment spending, 1981-1997 (millions of dollars). SOURCE: ONDCP (1996, 1997)
communities because of moral disapproval and fear that it will encourage those needing treatment to stay and may attract additional addicts to their community. Similarly, some clinicians still encourage patients to reject methadone maintenance in favor of the less-effective methadone detoxification treatments. Others provide methadone doses that are too low to be fully effective and encourage patients to end maintenance treatment prematurely. Some criminal-justice agencies referring probationers for treatment refuse permission for them to receive methadone maintenance.
The stereotype that drug abusers could change their behavior if they were sufficiently motivated is inconsistent with understanding the complex, multiple factors involved in addiction. When policymakers view drug abusers as untreatable or undeserving of public support, treatment programs, insurance coverage and training programs may be underfunded or abolished.
Dispelling the Myths About Addiction (IOM, 1997a), p. 140.
So, consider the director of the treatment program described at the beginning of this chapter who learns of new research showing that naltrexone improves outcome in alcoholic patients and in heroin addicts on probation. His program is funded for interpersonal treatments by relatively inexpensive counseling staff. He cannot buy the expensive new medication, nor hire a physician to prescribe it, nor a nurse (or pharmacist) to dispense it. The director of such a program may well view the research that determined the effectiveness of naltrexone as impractical.
In one sense that director would be right, since society clearly rations health care in the field of drug dependence on a different basis than rationing occurs in other health care areas. Payment is available only for inexpensive treatments, while the research evidence for efficacy of other treatments is disregarded. Such rationing leads to waiting lists as the agency must cut treatment slots and serve fewer people. Decreasing the length of treatment and increasing counselor caseloads also blocks the utilization of new treatments of proven efficacy.
SUMMARY
Considerable resources flow into drug abuse research but it often takes years before research findings change drug abuse treatment. In a review of outcome studies addiction treatment was shown to be about as successful as treatment of other chronic disorders such as hypertension, diabetes, and asthma. Indeed, less than 50 percent of patients with insulin-dependent diabetes, and less than 30 percent of patients with hypertension or asthma, comply with their medication regimens, with consequently sizable rates of reoccurrence or worsening of condition. These rates are comparable to success rates for treatment of persons with addictive disorders, (O'Brien and McLellan, 1996). Treatment is the most effective way to cut drug use and drug abuse treatment is clearly cost-effective from a societal perspective (Caulkins et al., 1997; Gerstein et al., 1994; SAMHSA, 1997). Despite this evidence, less than 20 percent of those who need treatment are receiving it and there are many barriers to implementing better treatment and providing better access.
With the knowledge explosion taking place in understanding the biology of the brain and the mechanisms of addiction, it is difficult for the best informed and best intentioned treatment provider, researcher, or state substance abuse director to keep abreast of the science. As new treatment questions and new research answers flow out of the new scientific understanding, new policy questions arise. It is important to enhance the exchange of information and knowledge among the research, treatment, and policy areas in order to bring the benefits of treatment research to the drug treatment consumer and to society.
In summary, there are many gaps in communication among treatment, research, and policy, the three key segments of the drug abuse treatment community. These gaps are caused (or exacerbated) by a set of critical barriers to better communication and coordination. Other barriers include lack of advocacy efforts, and lack of training opportunities (and requirements) in substance abuse treatment and research for all health-related professions. In addition, many CBOs lack organizational resources to implement new treatment findings while they are struggling with the complexi-
ties of a shifting political and financial environment. The committee concluded that there are ways to overcome the barriers and narrow the gaps and the following chapter describes a variety of models to aid this effort.
REFERENCES
Abcott AA. 1994. A feminist approach to substance abuse treatment and service delivery. Social Work in Health Care 19(3-4):67-83.
Altman DG. 1995. Sustaining interventions in community systems: On the relationship between researchers and communities. Health Psychology 14:526-536.
Backer TE. 1991. Drug Abuse Technology Transfer. Rockville, MD: National Institute on Drug Abuse.
Ball JC, Ross A. 1991. The Effectiveness of Methadone Maintenance Treatment. New York: Springer-Verlag.
Batten JL, Horgan CM, Prottas JM, Simon LJ, Larson MJ, Elliott EA, Bowden ML, Lee M. 1993. Drug services research survey phase I final report: Non-correctional facilities (revised). Institute for Health Policy, Brandeis University.
Brahen LS, Capone T, Bloom S et al. 1978. An alternative to methadone for probationer addicts: Narcotic antagonist treatment. Contemporary Drug Issues 13:117-132.
Brindis CD, Theidon KS. 1997. The role of case management in substance abuse treatment services for women and their children. Journal of Psychoactive Drugs 29(1):79-88.
Brindis CD, Berkowitz G, Clayson Z, Lamb B. 1997. California's approach to perinatal substance abuse: Toward a model of comprehensive care. Journal of Psychoactive Drugs 29(1):113-122.
Brown BS. 1995. Reducing impediments to technology transfer in drug abuse . In: Backer TE, David SL, Soucy G eds. Reviewing the behavioral science knowledge base on technology transfer. NIDA Research Monograph 155. Rockville, MD: National Institute on Drug Abuse. Pp. 169-185.
Brown BS. 1997. Staffing patterns and services for the war on drugs. In: Fox DM, Egertson J, Leshner AI eds. Treating Drug Abusers Effectively. Malden, MA: Blackwell Publishers. Pp. 99-124.
Calsyn DA, Saxon AJ, Barndt DC. 1991. Urine screening practice in methadone maintenance clinics: A survey of how the results are used. Journal of Nervous and Mental Disorders 179:222-227.
Caplehorn JRM, Bell J. 1991. Methadone dosage and retention of patients in maintenance treatment. Medical Journal of Australia 154:195-199.
Caulkins JP, Rydell CP, Schwabe WJ, Chisea J. 1997. Mandatory Minimum Sentences: Throwing Away the Key or the Taxpayers' Money? Santa Monica, CA: RAND Drug Policy Research Center.
Chasnoff IJ, Marques PR, Strantz IH, Farrow J, Davis S. 1996. Building bridges: Treatment research partnerships in the community. NIDA Research Monographs 166:6-21.
Christensen A, Jacobson NS. 1994. Who (or what) can do psychotherapy: The status and challenge of nonprofessional therapies. Psychological Science 5:8-14.
D'Aunno T, Vaughn TE. 1992. Variations in methadone treatment practices. Results from a national study. Journal of the American Medical Association 267:253-258.
Drug Strategies. 1997. Cutting Crime: Drug Courts in Action. Washington, DC: Drug Strategies.
Eisenberg JE. 1986. Doctors' Decisions and the Cost of Medical Care . Ann Arbor, MI: Health Administration.
Etheridge RM, Craddock SG, Dunteman GH, Hubbard RL. 1995. Treatment services in two national studies of community-based drug abuse treatment programs. Journal of Substance Abuse 7:9-26.
Ferguson JH. 1995. Technology transfer: Consensus and participation. The NIH Consensus Development Program. Joint Commission Journal on Quality Improvement 21(7):332-336.
Fiorentine R, Anglin MD. 1997. Does increasing the opportunity for counseling increase the effectiveness of outpatient drug treatment? American Journal of Drug and Alcohol Abuse 23(3):369-382.
Floyd AS, Monahan SC, Finney JW, Morley JA. 1996. Alcoholism treatment outcome studies, 1980-1992: The nature of the research. Addictive Behavior 21(4):413-428.
Forman A, Lachter SB. 1989. The National Institute on Drug Abuse cocaine prevention campaign. In: Shoemaker P ed. Communication Campaigns About Drugs: Government, Media, and the Public. Hillsdale, NJ: Lawrence Erlbaum Associates.
Garcia SA. 1993. Maternal drug abuse: Laws and ethics as agents of just balances and therapeutic interventions. International Journal of the Addictions 28(13):1311-1339.
Gerstein DR, Harwood H, Fountain D, Suter N, Malloy K. 1994. Evaluating Recovery Services: The California Drug and Alcohol Treatment Assessment (CALDATA). Contract No. 92-00110. Sacramento, CA: State of California Department of Alcohol and Drug Programs.
Grella CE. 1996. Background and overview of mental health and substance abuse treatment systems: Meeting the needs of women who are pregnant or parenting . Journal of Psychoactive Drugs 28(4):319-343.
Hall SM, Sorensen JL, Loeb P. 1988. Development and diffusion of a skill training intervention. In: Baker TB, Cannon DS eds. Addictive Disorders: Psychological Research on Assessment and Treatment. New York: Praeger Scientific Press. Pp. 180-204.
Higgins ST, Budney AJ, Bickel WK, Foerg FE, Donham R, Badger GJ. 1994. Incentives improve outcome in patient behavioral treatment of cocaine dependence. Archives of General Psychiatry 51(7):568-576.
Hoffman JA, Caudill BD, Koman JJ, Luckey JW, Flynn PM, Hubbard RL. 1994. Comparative cocaine abuse treatment strategies: Enhancing client retention and treatment exposure. In: Magura S, Rosenblum A eds. Experimental Therapeutics in Addiction Medicine. Binghamton, NY: The Hayworth Medical Press. Pp. 115-128.
IOM (Institute of Medicine). 1995. The Development of Medications for the Treatment of Opiate and Cocaine Addictions: Issues for the Government and Private Sector. Washington, DC: National Academy Press.
IOM. 1997a. Dispelling the Myths About Addiction: Strategies to Increase Understanding and Strengthen Research. Washington, DC: National Academy Press.
IOM. 1997b. Information Trading: How Information Influences the Health Policy Process. Washington, DC: National Academy Press.
Johnston LD, O'Malley PM, Bachman JG. 1997. Monitoring the Future Study. Rockville, MD: National Institute on Drug Abuse.
Join Together. 1998. Treatment for Addiction: Advancing the Common Good. Boston, MA: Join Together.
Josiah Macy, Jr. Foundation. 1995. Training About Alcohol and Substance Abuse for All Primary Care Physicians. Proceedings of a Conference . Phoenix, AZ, October 2-5, 1994. New York: Josiah Macy, Jr. Foundation.
Kaskutas LA. 1998. Methodology and characteristics of programs and clients in the social model process evaluation. Journal of Substance Abuse Treatment 15(1):19-25.
Kaufman E. 1996. Diagnosis and treatment of drug and alcohol abuse in women. American Journal of Obstetrics and Gynecology 174(1):21-27.
Leshner Al. 1997. Introduction to the special issue: The National Institute on Drug Abuse's (NIDA's) Drug Abuse Treatment Outcome Study (DATOS). Psychology of Addictive Behaviors 11(4):211-215.
Lester JP. 1993. The utilization of policy analysis by state agency officials. Knowledge: Creation, Diffusion, Utilization 14:267-290.
Levin FR, Owen P, Rabinowitz E, Pace N. 1996. Physicians in Residence Program: An evaluation of a novel substance abuse training approach for residents in primary care specialties. Substance Abuse 17(1):5-18.
Light JM, Irvine KM, Kjerulf L. 1996. Estimating genetic and environmental effects of alcohol use and dependence from a national survey: A "quasi-adoption" study. Journal of Studies on Alcohol 57(5):507-520.
Lomas J. 1993. Retailing research: Increasing the role of evidence in clinical service for childbirth. Milbank Quarterly 71(3):439-475.
Mallouh C. 1996. The effects of dual diagnosis on pregnancy and parenting. Journal of Psychoactive Drugs 28(4):367-380.
McLellan AT, Arndt IO, Metzger DS, Woody GE, O'Brien CP. 1993. The effects of psychosocial services in substance abuse treatment. Journal of the American Medical Association 269(15):1953-1959.
McLellan AT, Alterman AI, Metzger DS, Grissom GR, Woody GE, Luborsky L, O'Brien CP. 1994. Similarity of outcome predictors across opiate, cocaine, and alcohol treatments: Role of treatment services. Journal of Consulting and Clinical Psychology 62(6):1141-1158.
McLellan AT, Woody GE, Metzger D, McKay J, Durrell J, Alterman Al, O'Brien CP. 1996. Evaluating the effectiveness of addiction treatments: Reasonable expectations, appropriate comparisons. Milbank Quarterly 74(1):51-85.
Millman J, Samet S, Shaw J, Braden M. 1990. The dissemination of psychological research. American Psychologist 45:668-669.
Mulligan DH, McCarty D, Potter D, Krakow M. 1989. Counselors in public and private alcoholism and drug abuse treatment programs. Alcoholism Treatment Quarterly 6(3/ 4):75-89.
Naegle MA. 1988. Substance abuse among women: Prevalence, patterns, and treatment issues. Issues in Mental Health Nursing 9:127-137.
Naranjo CA, Bremmer KE. 1996. Dissemination of research results regarding the pharmacotherapy of substance abuse: Case examples and a critical review. Substance Abuse 17:39-50.
National Health Policy Forum. 1998. Dual Diagnoses: The Challenge of Serving People with Concurrent Mental Illness and Substance Abuse Problems. Issue Brief No. 718. Washington, DC: National Health Policy Forum.
NIH (National Institutes of Health). 1997. NIH Consensus Development Conference Statement on Acupuncture: November 3-5, 1997. Rockville, MD: National Institutes of Health.
O'Brien CP, McLellan AT. 1996. Myths about the treatment of addiction. Lancet 347:237-240.
ONDCP (Office of National Drug Control Policy). 1996. The National Drug Control Strategy, 1996: Program, Resources, and Evaluation. Washington, DC: Office of National Drug Control Policy.
ONDCP. 1997. The National Drug Control Strategy, 1997: Budget Summary. Washington, DC: Office of National Drug Control Policy.
ONDCP. 1998. The National Drug Control Strategy, 1998: A Ten Year Plan. Washington, DC: Office of National Drug Control Policy.
Ohio Department of Alcohol and Drug Addiction Services. 1996. Cost Effectiveness Study 1992-1996: Final Report. Columbus, OH: Ohio Department of Alcohol and Drug Addiction Services.
Pokorni JL, Stanga J. 1996. Caregiving strategies for young infants born to women with a history of substance abuse and other risk factors. Pediatric Nursing 22(6):540-544.
Price RH. 1997. What we know and what we actually do: Best practices and their prevalence. In: Egertson JA, Fox DM, Leshner A eds. Treating Drug Abusers Effectively. Malden, MA: Blackwell Publishers. Pp. 125-155.
Rahdert ER, ed. 1996. Treatment for Drug-Exposed Women and Their Children: Advances in Research Methodology. NIDA Research Monograph 165. Rockville, MD: National Institute on Drug Abuse.
Ripple CH, Luthar SS. 1996. Familial factors in illicit drug abuse: An interdisciplinary perspective. American Journal of Drug and Alcohol Abuse 22(2): 147-172.
Rogers EM. 1995. Diffusion of Innovations. 4th Edition. New York: Free Press.
Samsioe G, Abreg A. 1996. Ethical issues in obstetrics. International Journal of Fertility 41(3):284-287.
Selwyn PA. 1996. The impact of HIV infection on medical services in drug abuse treatment programs. Journal of Substance Abuse Treatment 13(5):397-410.
Silverman K, Higgins ST, Brooner RK, Montoya ID, Cone EJ, Schuster CR, Preston KL. 1996. Sustained cocaine abstinence in methadone maintenance patients through voucher-based reinforcement therapy. Archives of General Psychiatry 53(5):409-415.
Simpson DW, Joe GW, Brown BS. 1997. Treatment retention and follow-up outcomes in the Drug Abuse Treatment Outcome Study (DATOS). Psychology of Addictive Behaviors 11(4):294-307.
Sorensen JL, Bernal B. 1987. A family like yours: Breaking the patterns of drug abuse. San Francisco, CA: Harper and Row.
Sorensen JL, Hall SM, Loeb P, Allen T, Glaser EM, Greenberg PD. 1988. Dissemination of a job seekers' workshop to drug treatment programs. Behavior Therapy 19:143-155.
Stitzer ML, Higgins ST. 1995. Behavioral treatment of drug and alcohol abuse. In: Bloom FE, Kupfer DJ eds. Psychopharmacology: The Fourth Generation of Progress. New York: Raven. Pp. 1807-1819.
Streissguth PA. 1993. Fetal alcohol syndrome in older patients. Alcohol and Alcoholism Suppl. 2:209-212.
SAMHSA (Substance Abuse and Mental Health Services Administration). 1997. National Treatment Improvement Evaluation Study. Rockville, MD: Substance Abuse and Mental Health Services Administration.
Ter Riet G, Kleijnen J, Knipschild P. 1990. A meta-analysis of studies into the effect of acupuncture on addiction. British Journal of General Practice 40(338):379-382.
Volpicelli JR, Alterman AI, Hagashida M, O'Brien CP. 1992. Naltrexone in the treatment of alcohol dependence. Archives of General Psychiatry 49:876-880.
Widman M, Platt JJ, Lidz V, Mathis DA, Metzger DS. 1997. Patterns of service use and treatment involvement of methadone maintenance patients. Journal of Substance Abuse Treatment 14(1):29-35.
Young WB. 1997. The market for information in health policy: Using the "Just-in-Time" strategy. In: Institute of Medicine. Information Trading: How Information Influences the Health Policy Process. Washington, DC: National Academy Press. Pp. 11-26.





























