Executive Summary
As the United States approaches the twenty-first century, drug abuse remains one of our most intractable problems and only a small proportion of the approximately 9.4 million addicted and dependent individuals receive treatment in a given year. Further, despite the great strides made in research on the etiology, course, mechanisms, and treatment of addiction, serious gaps of communication exist between the research community and community-based drug treatment programs. Closing these gaps will not only be critical to improving drug and alcohol treatment, but will also be important to improving the nation's public health. Yet, to address the gaps, strategies are required to forge partnerships among diverse groups, such as researchers, treatment professionals, policymakers at all levels, consumers, as well as the public and private health sectors. These partnerships must be forged in a health care delivery and financing environment that is undergoing rapid change.
Community-based drug and alcohol treatment programs, the mainstay of our current addiction treatment system, developed during the 1970s and 1980s. Since then the financing of care has changed dramatically, and demands for accountability and efficiency are increasingly stressing the ability of these programs to survive. Within this context, this Institute of Medicine committee was charged with examining the community-based drug abuse treatment system with the goal of facilitating new strategies for partnership and increasing synergy among those working in a variety of settings to reduce the individual and societal costs of drug addiction (see Box 1).
|
BOX 1 The Committee's Task The task of the committee was to:
|
The findings and recommendations of the committee are directed toward increasing communication, interaction, and activities, especially research activities, to enhance knowledge transfer between community-based drug treatment organizations (CBOs) and the research community Committee members believe a bidirectional flow of information among treatment providers, researchers, and policymakers will enhance the quality of treatment-based research, increase treatment effectiveness, inform policy, and help CBOs to thrive in an increasingly challenging and complex environment (see Figure 1).
The audience for this report is quite broad and includes federal, state, and local policymakers, drug treatment researchers, community-based treatment providers (including their professional organizations), and consumers, as well as sponsors of research and treatment programs Others with interest in this report will include managed care programs, professionals involved with employee assistance programs, behavioral health researchers, behavioral health providers, criminal justice and social welfare programs, as well as foundations interested in public health, education, and professional training.
An early challenge for the committee was agreeing on a definition of community-based treatment organizations in order to frame the study Ultimately, the consensus achieved among committee members was that program accountability may come the closest to capturing the essence of social Identity In the definition of "community-based " The extent to which a program is accountable to elements of a specific community defines the program's interests, mission, and the social setting it serves In the inquiry
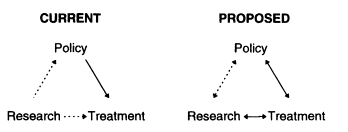
FIGURE 1 Need for bidirectional communication.
underlying its recommendations, this committee sought to include the widest range of drug treatment programs possible and was careful not to exclude from discussions and consideration those programs that defined themselves as community-based. Likewise, the committee was cautious not to exclude, a priori, any significant programs of interest by a determination that they were not "community-based." Thus, the public workshops included representatives from a diverse group, ranging from small local programs that would be considered community-based by the most restrictive definition, to large and complex programs sponsored by entities such as the Department of Veterans Affairs, academic medical centers, state court systems, and managed care organizations.
The committee obtained information from a rich variety of sources. For example, roundtable and workshop discussions with providers, researchers, and policymakers were held and site visits made by the committee and staff to solicit a broad base of input from representative stakeholders in 19 states. These meetings included individuals with expertise at all levels of government, drug courts, Native American health, school-based programs, drug abuse counseling, and research, among others.
New treatment, research, and policy questions flow out of changes in the policy environment as well as the new scientific understanding of brain biology and the mechanisms of addictions. It is important, therefore, to accelerate the exchange of information and knowledge among the research, treatment, and policy areas in order to bring the benefits of treatment research to the drug treatment consumer and to society. The evidence for the barriers between research, treatment, and policy is discussed in Chapter 2. Chapter 3 describes approaches to bridging the gap among stakeholders in this field, including technology transfer, organizational change, practice guidelines, use of consensus conferences and evidence-based reviews, top-down incentives and, most importantly, models that incorporate trust-building experiences. Chapters 4 and 5 address the challenges of the research/practice collaboration from the perspectives of the treatment provid-
ers and the researchers, respectively. The appendixes contain tools to assist those trying to bridge the gaps.
Changing the system will require treatment providers, reseachers, and policymakers working together to ask and answer the right questions and to jointly commit to implementation. Consequently, while this report proposes changes within each area, its most important recommendations are for the joint activities and investments which are necessary to produce systemic changes.
FINDINGS AND RECOMMENDATIONS
The committee's review of the challenges faced by community-based drug treatment providers, current research in this field, models for collaboration between research and practice, community-based organizations, and dissemination strategies led to findings and recommendations in six areas: (1) strategies for linking research and practice, (2) strategies for linking research findings with policy development and treatment implementation, (3) strategies for knowledge development, (4) strategies for dissemination and knowledge transfer, (5) strategies for consumer participation, and (6) training strategies for community-based research collaboration. The committee believes that attention to its recommendations will lead to improvements in clinical practices and will enhance the value of treatment research to clinicians, investigators, policymakers, consumers of treatment, and the public generally. The committee is also aware that many others (e.g., professional organizations, commissions, foundations, policy institutes, and prior IOM committees) have plowed this ground and sown seeds that have not always flourished. However, the value of the potential harvest is so great that it is essential we persevere in its cultivation.
Strategies for Linking Research and Practice
Despite some striking examples of strong collaborations between community-based drug and alcohol abuse treatment programs and research institutions, it was apparent that relatively few investigators work closely with community treatment programs, and even fewer programs participate actively in research.
Research participation becomes a possibility for treatment providers when community-based organizations are compensated for the costs of research participation and when program staff and investigators collaborate in construction of hypotheses, research design, and data collection, analysis, and interpretation.
The level of participation in research collaborations depends on the stage of organizational development of the treatment program, compatibil-
ity of the research with the organization's mission and culture, and its financial stability. Thus, research roles may vary from relatively passive participation (completing surveys and submitting data to state databases) to involvement as a partner in the development of research questions, data collection, and data interpretation. However, incentives for all parties must be strategically aligned if real progress is to be made.
The committee identified barriers to closing the gap between treatment, research, and policy. These barriers range from organizational factors, stigma, and social policy to cultural differences and funding problems, all of which can be strong disincentives for the collaboration needed to advance the field.
A pervasive theme heard in our workshops was the need for communication, mutual respect, and trust. Values of researchers and providers often differ and these differences must be recognized and resolved. The conduct of community-based research is an intensely interpersonal enterprise and trust relationships must be cultivated, at different levels of the organization, with community residents, and often with members of other agencies connected to the CBO. These relationships often take years to build.
The trust necessary for long-term collaboration is generally based on a history of increasing involvement. Successful collaborative programs from other health fields include support for a permanent infrastructure that facilitates long-term development. The National Cancer Institute's Community Clinical Oncology Program (CCOP) uses this strategy to bring state-of-the-art oncology research to community-based cancer treatment programs. CCOP facilitates research collaborations and enhances the ability of treatment programs to apply research findings to the general patient population. Development of a similar mechanism for use in community-based drug and alcohol abuse treatment could catalyze research/practice collaborations and stimulate improvements in practice. CCOPs are not inexpensive and they present a significant managerial challenge. The infrastructure alone at each clinical site can exceed $200,000. However, the infrastructure recommendation that follows does not necessarily require a model with that complexity. It could begin as a demonstration project involving the funding of one full-time-equivalent staff person and some computer support to a small set of diverse treatment sites. This level of support could be the target, whichever of the various network collaboration models was implemented.
Based on these findings, the committee offers two recommendations and identifies certain key characteristics that will facilitate their successful implementation.
RECOMMENDATION 1. The National Institute on Drug Abuse and the Center for Substance Abuse Treatment should support the development of an infrastructure to facilitate research within a network of community-based treatment programs, similar to the National Cancer Institute's Community Clinical Oncology Program (CCOP) networks.
To be successful, the infrastructure and network development will depend on commitment from the community-based treatment programs and researchers. Certain key areas will need to be addressed to foster partnership. For the community-based treatment programs, these include:
Likewise, for treatment researchers, the following approaches are suggested:
RECOMMENDATION 2. The National Institute on Drug Abuse and the National Institute on Alcohol Abuse and Alcoholism should develop research initiatives to foster studies that include community-based treatment programs as full partners.
Issues to be addressed by these initiatives include the following:
Strategies for Linking Research Findings, Policy Development, and Treatment Implementation
State and federal policies sometimes hinder the diffusion of knowledge flowing from research that is relevant to drug abuse treatment. Selective prohibitions on the use of state and federal funds can inhibit the application of proven research findings. Language in the Substance Abuse Prevention and Treatment Block Grant, for example, prohibits the use of federal funds for needle exchange, despite studies demonstrating this improves the effectiveness of outreach to a population at highest risk for HIV infection. A similar restriction on the use of funds for client payments inhibits the implementation of behavioral reinforcement strategies. Local laws and policies restrict the development and operation of methadone services. Moreover, state and federal officials have generally not used funding mechanisms to facilitate collaboration between treatment programs and researchers, to foster adoption of new and effective treatments, or to improve the design of clinical research.
The committee believes that the coordination of state and federal programs is important to facilitate active collaboration and improvement of drug and alcohol treatment. Two recommendations are offered emphasizing the role of states in this collaboration, accompanied by approaches to undergird needed support.
RECOMMENDATION 3. State authorities should provide financial incentives for collaborative investigations between CBOs and academically oriented research centers; and should support structures to foster broad participation among researchers, practitioners, consumers, and payers in the development of a treatment research agenda, including studies to measure outcomes and program operations.
RECOMMENDATION 4. CSAT and the states need to cooperate in the development of financial incentives that encourage the inclusion of proven treatment approaches into community-based treatment programs. This approach should include making additional funds available for implementing targeted treatment approaches.
To improve treatment, the following are considered critical areas to address:
Strategies for Knowledge Development
Practitioners and policymakers requested more research on treatment effectiveness and studies that help programs operate more effectively and identify interventions that serve clients more effectively. The complexity of the contemporary economic and policy environment increases the importance of health services research and the dependence of policymakers on the data and results from research investigations.
The committee's findings suggest that expanding the range of studied treatment settings, treatment modalities, and treatment populations may result in more broadly applicable treatment research findings. These observations led the committee to make two specific recommendations in this area.
RECOMMENDATION 5. CSAT and NIDA should develop mechanisms to enable state policymakers to monitor service delivery in community-based treatment programs and to determine if consumers receive services empirically demonstrated as effective and to ascertain if the treatment dosage and intensity are sufficient to be effective.
RECOMMENDATION 6. NIDA and NIAAA should continue to support "real world" services research and cost-effectiveness studies and include the development of services research in their strategic plans.
Strategies for Dissemination and Knowledge Transfer
The committee found at least four factors that inhibit diffusion of drug abuse treatment knowledge: (1) the structure of treatment delivery systems; (2) the diversity of the clients, providers, and other stakeholders; (3) the stigmatization of people who are dependent on alcohol and other drugs; and (4) an inadequate base of knowledge about technology transfer specific to the field. Differences in perspective among consumers, clinicians, researchers, and policymakers also inhibit knowledge dissemination and use.
Because providers and payers are often unaware of the latest research, the committee found a pressing need to create consensus in the field about which treatments have been proven to be effective and which have been proven to be ineffective. Further, the research agendas of the federal agencies should continue to be fueled by agreement in the field on which models have not received adequate study. The fruits of this consensus process should be widely distributed.
Key to improving knowledge dissemination will be cooperation and collaboration across federal agencies, states, professional organizations, and consumer groups, among others. The committee recommends two general approaches to establish the needed collaboration.
RECOMMENDATION 7. CSAT, NIDA, NIAAA, and AHCPR are the federal agencies that should develop formal collaborations, where appropriate, to synthesize research, reduce the barriers to knowledge transfer, and provide updated information about drug and alcohol treatment strategies to purchasers of health care.
A variety of approaches could be utilized to accomplish these goals. For example, expert panels of investigators, practitioners, program administrators, policymakers, and consumers could be convened by NIDA, NIAAA, and CSAT to generate up-to-date consensus recommendations for community-based drug and alcohol treatment programs based on current research. NIDA-, NIAAA-, and AHCPR-sponsored research on drug treatment knowledge dissemination would help to reduce barriers to the transfer of treatment knowledge and encourage treatment programs and policymakers to adopt proven treatments. Research findings need to be prepared in a form and disseminated within channels that enhance availability and acceptability to community-based treatment programs—especially front-line treatment staff. Continued support for and improvement of electronic and print publications directed to treatment programs and consumers is necessary, and other media, such as public access television should be considered.
CSAT, NIDA, and NIAAA also have an important role in the development of information to enable purchasers of care to take research findings into account explicitly in making purchasing decisions. At the same time, purchasers should develop treatment criteria that ensure treatments of proven effectiveness are adequately funded and should consider withholding funding when the science base shows the treatment to be unequivocally ineffective.
RECOMMENDATION 8. CSAT, in collaboration with state substance abuse authorities, professional organizations, and consumer organizations in the addiction field, should continue the development of evidence-based treatment recommendations (including consideration of short- and long-term outcomes) for use by clinicians of all disciplines involved in the treatment of drug and alcohol use disorders.
To ensure that these treatment recommendations have a positive impact on health care, these agencies and groups should work to encourage
their use. Measurement of the impact of guidelines on clinical care delivery will optimally include short-, intermediate-, and long-term treatment outcomes.
Strategies for Consumer Participation
Consumers are rarely involved in the issues of how drug abuse treatment research is supported and conducted. Although many community-based treatment programs were founded by men and women in recovery and counselors in recovery make up a significant portion of the workforce, there are few advocacy groups for patients and their families. In view of the stigma and legal hazards attached to illicit drug abuse, the reluctance to advocate is understandable but unfortunate. Consumer advocacy for state-of-the-art services has improved care for individuals with cancer, and with HIV/AIDS. Drug abuse treatment may enjoy similar benefits if drug treatment consumers become informed consumer advocates.
RECOMMENDATION 9. CSAT and NIDA, in collaboration with state substance abuse authorities, should develop public awareness programs to encourage consumers and their families to recognize high quality treatment programs so they will begin to demand that treatment programs include research-proven treatment approaches within their treatment models.
These groups should consider a variety of approaches to accomplish this goal. These include:
It is also critically important that representatives of consumers and their families, with the support and assistance of the research, treatment, and policy communities, promote local as well as national advocacy groups to work with state funding agencies, insurers, managed care organizations, and self-insured employers to encourage the use of valid and reliable measures of treatment outcomes. Such measures serve as a basis for evaluating the efficacy of specific treatment modalities and the cost effectiveness of
treatment programs, individual treatment providers and networks of care. State and federal governments, employers, and purchasing alliances could then be encouraged to use these data to inform their health care purchasing and contracting decisions. Consumer groups should also advocate for the development of standards of care in community-based clinics, treatment networks, integrated delivery systems, and managed care networks. Such standards could be used in accreditation of treatment programs and are best if based on findings from clinical research, as well as broadly accepted clinical consensus.
Training Strategies for Community-Based Research Collaboration
In order to foster collaborative research in this field, it is necessary to enhance special skills needed for the next generation of drug abuse researchers. Despite the many prior recommendations for addressing this problem, both clinical and research training programs need to be more attentive to the need for collaboration to improve treatment in this field. The committee made three recommendations specific to preparing trainees for active participation in clinical research studies.
RECOMMENDATION 10. NIDA and other research funding agencies should support predoctoral and postdoctoral research training programs that provide experience in drug abuse treatment research and health services research within community-based treatment programs. Programs funded should have the full and active participation of community-based treatment programs and should include resources to fund the costs of participation for the treatment programs.
RECOMMENDATION 11. University training programs in the health professions should:
|
• |
enhance exposure of students to didactic teaching about substance abuse and dependence; |
|
• |
require didactic teaching as well as supervised clinical experiences in community-based treatment settings; |
|
• |
teach students to interpret substance abuse treatment research and apply research findings in their clinical practices; |
|
• |
work with professional organizations to enhance continuing education about the addictions within the residency training curriculum of the various health professions; and |
|
• |
support researchers seeking to enhance collaborative relation- |
|
|
ships with treatment programs by offering tuition credit for CBO staff involved in funded collaborative research. |
RECOMMENDATION 12. NIDA, CSAT, and other appropriate funding agencies should create research training programs for staff members of community-based treatment programs to strengthen the ability of the treatment programs to include research activities and to adopt the findings of research into their treatment approaches. Training programs should promote research training for clinical staff through fellowships and tuition remission, and incentives for attending professional meetings.
To enhance the likelihood that these recommendations are given serious consideration by the agencies to which they are addressed, the assistance of private foundations is also needed. Foundations could play an important role by developing grant programs to:
TABLE 1 Summary of Recommendations
|
Strategies |
Recommendations |
Primary Responsibility |
|
I. Linking research and practice |
1. Develop research infrastructure and network of community based drug treatment organizations (CBOs) |
NIDA, CSAT |
|
|
2. Research initiative for collaborative studies within CBOs |
NIDA, NIAAA |
|
II. Linking research, policy development and treatment implementation |
3. Promote university/CBO studies and develop treatment research agenda |
States |
|
|
4. CBO incentives to implement targeted treatments |
CSAT, states |
|
III. Knowledge development |
5. Assist states to develop treatment and outcomes monitoring system |
CSAT, NIDA |
|
|
6. Support services research and cost-effectiveness studies |
NIDA, NIAAA |
|
IV. Dissemination and knowledge transfer |
7. Coordinate activities to synthesize research and provide information to payers |
CSAT, NIDA, NIAAA, AHCPR |
|
|
8. Develop evidence-based treatment recommendations—with broad constituency participation |
CSAT |
|
V. Consumer participation |
9. Develop public awareness programs to increase demand for proven treatment |
CSAT, NIDA |
|
Strategies |
Recommendations |
Primary Responsibility |
|
VI. Training for community-based research collaboration |
10. Support pre/post doctoral training for community-based research collaboration |
NIDA, other NIH training programs |
|
|
11. Provide teaching, supervised clinical experience and CME in addiction treatment—for all health professions |
University training programs |
|
|
12. Create research training programs for CBO staff through fellowships and other incentives |
CSAT, NIDA, university programs |















