1
The Current Burden of Cardiovascular Diseases in Developing Countries
Economic Development Brings Changes
Although cardiovascular diseases (CVDs) are well known throughout the world, their form and the burden they cause change as a country undergoes economic development. Developing countries begin with a disease burden dominated by nutritional, perinatal, and infectious diseases and, in the process of development, make the transition to one dominated by noncommunicable diseases, particularly CVD (Olshansky and Ault, 1986; Omram, 1971). The four stages of that transition are shown in Table 1-1.
For countries in the earliest stage of development, the predominant circulatory diseases are rheumatic heart disease (Box 1-1), infections, and nutritional deficiency-related disorders of the heart muscle. Regions in this phase include Sub-Saharan Africa and the rural areas of South America and Asia. In the second stage, as infectious disease burdens are reduced and nutrition improves, diseases related to hypertension, such as hemorrhagic stroke (Box 1-2) and hypertensive heart disease (Box 1-3), become more common. Regions in this phase include China and other Asian countries. In the third stage, as life expectancy continues to improve, high-fat diets, cigarette smoking, and sedentary life-styles become more common. Noncommunicable diseases then predominate, with the highest mortality caused by atherosclerotic CVD, most frequently ischemic heart disease and atherothrombotic stroke, especially at ages of less than 50 years. This phase is found in urban India (Reddy and Yusuf, 1998) and the former socialist countries including Russia. In the fourth stage, increased efforts to prevent, diagnose, and treat ischemic heart disease and stroke are able to delay the impact of these diseases to more advanced ages. The regions that have reached this final stage are Western Europe, North America (excluding Mexico), Australia, and New Zealand.
TABLE 1-1 Deaths Caused by Cardiovascular Disease at Different Stages of Development—1990
|
Stage of Development |
Deaths from CVD (% of total) |
Predominant CVDs |
Regional Examples |
|
Age of pestilence and famine |
5–10 |
Rheumatic heart disease, infections. and nutritional cardiomyopathies |
Sub-Saharan Africa. rural India. and South America |
|
Age of receding pandemics |
10–35 |
As above, plus hypertensive heart disease and hemorrhagic stroke |
China |
|
Age of degenerative and man-made diseases |
35–55 |
All forms of stroke; ischemic heart disease at relatively young ages |
Urban India. formerly socialist economics |
|
Age of delayed degenerative diseases |
<50 |
Stroke and ischemic heart disease at older ages |
Western Europe. North America. Australia. New Zealand |
|
SOURCE: Jha et al., forthcoming. |
|||
|
BOX 1-1 Rheumatic Heart Disease: The Unfinished Agenda For countries in the early stages of development, rheumatic heart disease is the most common form of CVD. Indeed, it is thought to affect more than 4 million people worldwide, resulting in approximately 90,000 deaths each year (Michaud et al., 1993). It is caused by group A streptococcal pharyngitis, which if untreated will progress in about 3 percent of cases to rheumatic fever and then cause immunologic damage to heart valves and muscle. Many years later, the thickened or incompetent heart valves disrupt blood flow, which leads to congestive heart failure or death. Although rheumatic fever and rheumatic heart disease have essentially disappeared in developed countries, both remain major causes of CVD in developing countries. In Africa, Latin America, Asia (especially India), and the Pacific Islands, 1-2 percent of school children show evidence of rheumatic valvular disease (Michaud et al., 1993). A high proportion of these children will develop progressive heart failure over the next 20-40 years, then die at 25 to 44 years of age. A range of 20-35 percent of cardiac patients admitted to hospitals in Africa and Asia have rheumatic heart disease, often with heart failure or needing replacement of the heart valve. This surgery is effective at prolonging life, but where it is not available, referrals abroad are costly. For the next 20-40 years, it is likely that developing countries will experience a double burden of CVD: rheumatic heart disease will continue, while atherosclerotic CVD becomes more common. |
For most developing and middle-income countries, the increased incidence of CVD adds to the continuing burden of infectious, nutritional, and perinatal diseases. It is a major setback for health care systems that are already overburdened and underfunded (WHO, 1997, Box 1-4).
Subsets of a population may be at different stages of the CVD epidemic. An ''early-adopter" community such as one with rapid social and economic development may experience an early increase in CVD and thus have a higher level than other parts of the population. The decline in CVD burden may also occur earlier for this community, as shown in Figure 1- 1. The transition of CVD from a disease of the wealthy to one of the poor has been documented in the United Kingdom and the United States (Kaplan and Keil, 1993; Marmot et al., 1991). It was relatively rare in the African-American community in the 1960s, but now its incidence equals or exceeds that in the white population of the United States (NHLBI, 1996). The pattern of disease continues to be in transition for all but the most developed countries.
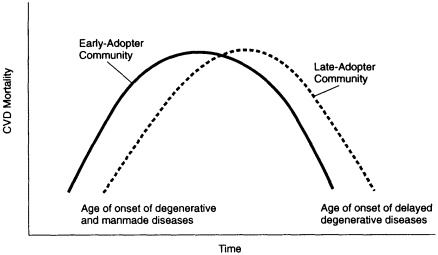
FIGURE 1-1 Theoretical comparison of cardiovascular disease mortality in early-versus late-adopter communities.
ATHEROSCLEROSIS AS THE UNDERLYING DISEASE PROCESS
Vital statistics and hospital admission records show the clinical syndromes of myocardial infarction, sudden cardiac death, atherothrombotic stroke, and peripheral arterial disease to be the leading causes of morbidity and mortality. These diseases share the same pathology, atherosclerosis. This disease process is thought to begin in adolescence with injury to the arterial endothelium and focal accumulation of lipid-filled macrophages known as fatty streaks. These lesions are common worldwide. Some fatty streaks progress by infiltration and proliferation of smooth muscle cells to form the fibrous-capped plaque characteristic of atherosclerosis. The plaques appear to be less common in developing countries. They are clinically silent until the fourth decade of life, when they undergo fissuring, ulceration, and thrombosis, leading to the clinical syndromes of ischemic heart disease, stroke, and peripheral vascular disease. Although the manifestation differs with the artery involved, the clinical syndromes are all related to the same systemic disease process, atherosclerosis (Ross, 1993) (see Appendix B for further discussion of clinical syndromes).
Risk Factors for Atherosclerotic Disease
The risk factors associated with atherosclerotic disease include demographic, familial, behavioral, and physiological characteristics. The roles of
many of these factors in the pathophysiology of atherosclerosis have been defined (Fuster et al., 1996). They can be classified on the basis of whether they are modifiable (Pasternak et al., 1996; Pearson et al., 1993) (Figure 1-2). Nonmodifiable risk factors include age, male gender, and a positive family history of CVD with onset at an early age. Modifiable risk factors can be behavioral (sedentary life-style, a diet high in fat and cholesterol, cigarette smoking) or physiological (elevated low-density lipoprotein [LDL] cholesterol, decreased high-density lipoprotein [HDL] cholesterol, diabetes, hypertension, obesity, postmenopausal status [in women]). The effectiveness of modifying risk factors to prevent disease has been dramatic for some risk factors. For others, the association with atherosclerotic disease is less well understood (see Appendix B).
|
BOX 1-2 A Transition from Hemorrhagic to Artherombotic Stroke As life expectancy increases, acute neurological deficits or strokes may become a significant health problem before there is an increase in coronary heart disease (Reed, 1990). Early in the transition from infectious to noncommunicable diseases, many of the strokes are so-called hemorrhagic strokes, caused by bleeding from an intracerebral artery into the brain. They have a case fatality rate of 80 percent or more (Wolf, 1994). The major risk factor for all forms of stroke is high blood pressure. For hemorrhagic stroke, low blood cholesterol is also a risk factor (Iso et al., 1989; Reed, 1990). As countries develop, their populations may have increased blood pressure before they experience increased blood cholesterol. This would lead to an increase in deaths from hemorrhagic stroke. Later in the transition, stroke mortality may change from the hemorrhagic type to the atherothrombotic type. Atherothrombotic stroke is caused by atherosclerotic plaques in the arteries that supply the brain. These can undergo ulceration or thrombosis, and the pieces of plaque or thrombus that break off may occlude one or more of the arteries to the brain and cause a malfunction. If the blood flow is restored, the malfunction is a transient ischemic attack. If the blood flow is not restored, brain tissue dies as a result of the stroke. This form of stroke has a case fatality rate of approximately 20 percent, but many of the survivors are left with disabilities such as paralysis, inability to speak, or blindness. The risk factors for atherothrombotic strokes are hypertension, elevated blood cholesterol, diabetes, and obesity. Studies of mortality from stroke in rapidly developing country populations have shown consistently high mortality rates and a transition in relative importance from intracerebral hemorrhagic stroke to atherothrombotic stroke with economic development. |
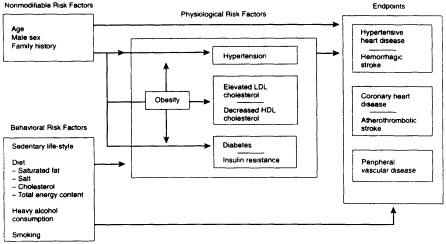
FIGURE 1-2 Relationships among risk factors for cardiovascular disease.
Risk factors that have a causal association with CVD (hypertension, elevated LDL cholesterol, decreased HDL cholesterol, diabetes, cigarette smoking, sedentary life-style) are thought to explain at least 50 percent of the burden of CVD (Pooling Project Research Group, 1978). Interactions among these risk factors can multiply the risk of disease. Additional risk factors have been proposed that help explain the remaining CVD burden. These include the levels of thrombogenic factors such as serum fibrinogen, levels of triglycerides, lipoprotein profiles, levels of serum homocysteine, levels of dietary antioxidants, alcohol consumption, and certain psychosocial factors.
THE GLOBAL BURDEN
Cardiovascular Disease as the Leading Cause of Death
It is likely that CVD became the developing world's leading cause of death for the first time in the mid-1990s. (Murray and Lopez, 1997c)
The Global Burden of Disease Study has estimated the distribution of deaths by region for 1990 (Murray and Lopez, 1997c). Noncommunicable diseases (NCDs) rank first in most developing countries, in developed countries, and worldwide. Moreover, CVD usually accounts for about half of all NCD deaths. The 10 major causes of death in developed and developing countries are listed in Table 1-2. In developing countries, CVD was responsible for slightly fewer deaths than infectious and parasitic diseases in 1990. It is estimated that since that time—with the decreasing incidence of infectious and parasitic diseases and the increasing incidence of CVD in the mid-1990s—CVD became the develop-
ing world's leading cause of death. Even in 1990, CVDs were the leading cause of death for all major geographic regions of the developing world except India and Sub-Saharan Africa.
Although CVD mortality is well known to be high for men and for older age groups, it is also the major cause of mortality in the economically productive age group of 30-69 years and in women (Table 1-3). Not surprisingly, in 1990 CVD caused three times as many deaths in 30-to 69-year-old men and women as did infectious and parasitic diseases worldwide. This is true for all regions of the world, except Sub-Saharan Africa, where the number of deaths from CVD and infectious or parasitic diseases was about equal. Recent data suggest that mortality from stroke in Sub-Saharan Africa is higher than previously reported and confirm the relatively young age of the victims (United Republic of Tanzania, 1997).
|
BOX 1-3 Hypertension: A Global Disease Elevated blood pressure or hypertension emerges as a major cause of hemorrhagic strroke, hypertensive heart disease, and hypertensive kidney failure even before : coronary heart disease and atherothrombotic stroke become major causes of mortality (Whelton et al., 1995). Using a conservative definition for hypertension as blood pressure above 160 mm Hg systolic or above 95 mm Hg diastolic, the prevalence of hypertension, even in Sub-Saharan Africa, ranges from 10 to 33 percent in 30- to 49 year-old men and women (Nissinen et al., 1988). The INTERSALT study carried out in 32 countries, many of them developing, used carefully standardized measurements of blood pressure to confirm substantial prevalence of blood pressures above 140/90 mm Hg in most countries, both developed and developing (INTERSALT cooperative Research Group, 1988). In addition, the level of awareness worldwide is low, as are treatment and control of elevated blood pressure (Marques-Vidal and Tuomilehto, 1997). A practical approach to CVD control is primordial prevention (i.e., prevention of the risk factors themselves) Hypertension may be considered either a risk factor for CVD or disease in itself. This raises the issue of whether hypertension is preventable. Some of its risk factors such as age, male sex, and family history are nonmodifiable. The modifiable risk factors include obesity, sedentary life-style, high-sodium diet, alcohol consumption, and possibly other dietary factors. Clinical trials to prevent the development of hypertension suggest that weight control, increased physical activity, and lower dietary intakes of sodium and alcohol show good potential for primordial prevention (Cutler 1993). Despite their low cost relative to treatment, these strategies have not yet been investigated in developing countries. Without successful primordial or primary prevention, significant disability and mortality are likely to be caused by hypertension. |
Another Measure of Disease Burden
Until recently, quantifying the burden of disease and injury in human populations relied primarily on measurements of mortality. However, using mortality measurements alone ignores significant, nonfatal illness and disability. Because of these and other limitations, different measures for the disease burden have been developed. One of the most commonly used of these is the DALY (disability-adjusted life year), which is a measure of the years of life lost (YLL) due to premature mortality plus years lived with disability (YLD). The years of life lost from premature death are defined as the difference between actual age at death and life expectancy at this age in a low-mortality population. The years of life lived with a disability are adjusted for seven levels of severity of the disability.
When DALYs are used to measure the disease burden, there is a change in the ordering of major diseases or injuries in developing countries (Table 1-4). For developing countries in 1990, CVD ranked fifth as a source of disease burden (measured in DALYs), while it ranked second as a cause of death. Projections for the year 2020 place ischemic heart disease third and cerebrovascular disease fifth among the leading causes of disease burden measured in DALYs for developing countries (Murray and Lopez, 1996). The broader category of CVD would rank even higher than these two subcategories in the global burden of disease and injury. Estimates of the global burden of disease in 2020 can be compared with those for mortality, in which CVD is predicted to be the major contributor in developing as well as developed countries.
TABLE 1-2 The 10 Major Causes of Death in Developed and Developing Countries—1990
|
|
Deaths (thousands) |
||
|
Cause of Death |
Developed |
Developing |
World |
|
Cardiovascular disorders |
5,245 |
9,082 |
14,327 |
|
Infectious and parasitic diseases |
163 |
9,166 |
9,329 |
|
Malignant neoplasms |
2,413 |
3,611 |
6,024 |
|
Respiratory infections |
389 |
3,992 |
4,380 |
|
Unintentional injuries |
552 |
2,682 |
3,233 |
|
Respiratory disorders |
500 |
2,435 |
2,935 |
|
Perinatal disorders |
82 |
2,361 |
2,443 |
|
Digestive disorders |
424 |
1,426 |
1,851 |
|
Intentional injuries |
282 |
1,569 |
1,851 |
|
Genitourinary disorders |
167 |
568 |
735 |
|
SOURCE: Murray and Lopez, 1997c. |
|||
|
Box 1-4 Congestive Heart Failure: The Next Epidemic Congestive heart failure (CHF) develops as a consequence of disease and dysfunction of the heart. Its signs and symptoms vary, but it generally results in failure of the left heart the provide adequate output. This causes fluid to collect in the lungs and leads to shortness of breath. When the right heart is unable to provide adequate output, there is a buildup of fluid in the body (edema, liver enlargement, etc.). Any disease affecting the heart muscle or valves can lead to heart failure. In Africa and South America, heart failure is likely to be caused by rheumatic valvular disease, wher as in Asia it is likely to be caused by hypertensive heart disease. Prevalence estimates from U.S. and European studies suggest that 6 to 10 percent of the elderly population meets criteria for CHF, which increases sharply with age (Rowie et al., 1997). Around 1970, 250,000 new cases of heart failure were diagnosed each year in the United States. In 1988 400,000 new cases—and in 1992 700,000 new cases—of CHF were diagnosed, per year (Abraham and Bristow, 1997). CHF now affects 5 million Americans, is the most common cause of hospitalization in persons 65 years and older, and accounts for $10 billion to 40 billion in health care costs. The majority of CHF cases are due to coronary artery disease or hypertensive heart disease. Developing countries could avoid escalating health care costs currently experienced by developed countries if they could control these diseases. |
TABLE 1-3 Deaths (thousands) Due to Cardiovascular Disease and to Infectious and parasitic Diseases (IPDs) in 30- to 69- Year Olds by Sex and Region—1990
|
|
Men |
Women |
||
|
Region |
CVD |
IPD |
CVD |
IPD |
|
Established market economies |
483 |
42 |
227 |
12 |
|
Formerly socialist economies |
263 |
20 |
163 |
6 |
|
India |
611 |
429 |
481 |
240 |
|
China |
576 |
158 |
439 |
89 |
|
Other Asian and Pacific Island countries |
289 |
147 |
226 |
140 |
|
Sub-Saharan Africa |
183 |
215 |
211 |
228 |
|
Latin American and Caribbean countries |
186 |
62 |
147 |
48 |
|
Middle Eastern Crescent |
285 |
83 |
215 |
85 |
|
Worldwide |
3,028 |
1,128 |
2,201 |
798 |
|
SOURCE: Murray and Lopez, 1996. |
||||
Regional Differences
Populations worldwide have very different levels and presentations of CVD as well as infectious and parasitic diseases. Three factors are likely to contribute to regional differences in CVD:
-
the stage of economic development, which has a role in the predominance of different CVDs,
-
differences in behavior and life-style that expose populations to different levels of risk, and
-
differences in racial and ethnic heritage, which determine genetic predisposition to CVD.
The first factor contributing to regional differences in CVD is the stage of development, as illustrated in Table 1-5. China and India have considerable mortality from rheumatic and inflammatory heart diseases. Sub-Saharan Africa continues to have more mortality from cerebrovascular disease than from ischemic heart disease. These differences are consistent with the level of development of these regions.
The second factor contributing to regional differences in CVD involves the behaviors and life-styles that expose populations to increased levels of risk. The World Health Organization (WHO) Inter-Health Program has documented striking differences in the prevalence of cigarette smoking, hypertension, hypercholesterolemia, and obesity (Berrios et al., 1997; Vartiainen et al., 1991). These differences may determine whether the major CVD is coronary, cerebrovascular, or another presentation. Whereas individuals in developing country populations tend to have a single important risk factor, those in European and North American populations have two or more important risk factors (see Figure 1-3) (Berrios et al., 1997). Since risks for CVD tend to be multiplicative in effect, the greater number of risk factors in developed countries may explain their higher risks.
The third factor contributing to regional differences in CVD is racial and ethnic heritage, which determines the genetic predisposition to CVD. For example, South Asians who migrate to Europe, North America, or other regions of the world have an incidence of CVD that exceeds even the incidence of the countries to which they have migrated (Enas and Mehta, 1995). This suggests a gene-environment interaction (the so-called thrifty gene) in which high caloric intake, a sedentary life-style, or obesity elicits an exaggerated insulin response, that leads to hyperinsulinemia, diabetes, and other physiologic risk factors (McKeige et al., 1993; Neel, 1962). A variation of this observation may be the strikingly low HDL levels and high serum triglyceride levels observed in the Turkish population (Mahley et al., 1995).
TABLE 1-4 Percentage of Disability-Adjusted Life Years Attributable to Specific Causes of Death for Developed and Developing Regions of the World—1990
|
|
Percentage of Total DALYS |
||
|
Disease or Injury |
Developed |
Developing |
World |
|
Infectious and parasitic diseases |
2.7 |
25.6 |
22.9 |
|
Neuropsychiatric disorders |
22.0 |
9.0 |
10.5 |
|
Unintentional injuries |
10.3 |
11.1 |
11.0 |
|
Cardiovascular diseases |
20.4 |
8.3 |
9.7 |
|
Respiratory infections |
1.6 |
9.4 |
8.5 |
|
Perinatal disorders |
1.9 |
7.3 |
6.7 |
|
Malignant neoplasms |
13.7 |
4.0 |
5.1 |
|
Respiratory disorders |
4.8 |
4.3 |
4.4 |
|
Intentional injuries |
4.2 |
4.1 |
4.1 |
|
Nutritional deficiencies |
0.9 |
4.1 |
3.7 |
|
SOURCE: Murray and Lopez, 1997c. |
|||
TABLE 1-5 Deaths Due to Specific Cardiovascular Diseases for Regions at Different Stages of Development—1990
|
|
CVD Deaths (thousands) |
|||
|
Region |
Rheumatic |
Inflammatory |
Cerebrovascular |
Other |
|
Established market economies |
20 |
65 |
788 |
633 |
|
Formerly socialist economies |
25 |
39 |
639 |
341 |
|
India |
70 |
83 |
448 |
490 |
|
China |
163 |
66 |
1,272 |
305 |
|
Other Asian and Pacific Island countries |
10 |
82 |
390 |
406 |
|
Sub-Saharan Africa |
20 |
63 |
383 |
140 |
|
Latin America and Caribbean countries |
8 |
25 |
249 |
160 |
|
Middle Eastern Crescent |
24 |
72 |
212 |
377 |
|
SOURCE: Murray and Lopez, 1997c. |
||||
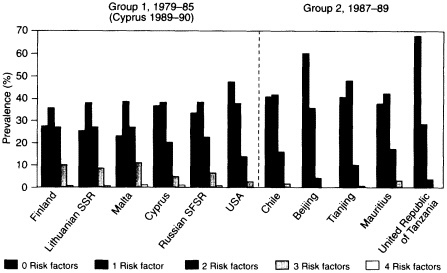
FIGURE 1-3 Risk factors for 35- to 64-year-olds in two groups of Inter-Health countries (data on cholesterol levels and body mass index were not available for Beijing).
SOURCE: World Health Organization, 1991. Reprinted with permission.
Barker and Osmond (1992) have proposed that the adult risk for CVD can be determined to a substantial degree by factors in fetal or neonatal life that "program" metabolic regulation for the early dietary environment and do not appear to adapt to the dietary environment of later life. This would explain why low birthweight or relatively low weight gain in the first year appears to predispose a person to later high risk of CVD. This risk factor overrides the positive results that could be expected from interventions in later life. There is some empirical support for this idea, but it requires further investigation. If this programming is confirmed, it provides yet another reason for improving maternal and infant nutrition and health.
Attributable Risk
What proportion of CVD can be attributed to specific risk factors and thus be prevented if these risk factors are controlled? This is a function of the prevalence of a risk factor and of its relative contribution to CVD. A single risk factor can explain a large proportion of the disease, as in the case of African-American women for whom more than 50 percent of total mortality is attributable to hypertension, which is highly prevalent and contributes a large part of the risk for CVD (Deubner et al., 1975). Control of such risk factors has potential for realizing a sizable reduction in the CVD burden.
CONCLUSIONS
CVD has been the dominant cause of death in developed countries for more than half a century. CVD has also emerged as a dominant disease in developing countries, although this is likely to be only the beginning of an epidemic that will continue to emerge. These diseases already affect large numbers of middle-aged persons, both men and women, and all economic groups. They cause three times as many deaths in 39- to 69-year-olds worldwide as do infectious and parasitic diseases combined. Control of CVD requires an understanding of the changing pattern of disease as a region develops and a focus on the risk factors that have so dramatically influenced CVD in the developed world. Where limited data are available in developing countries, as for atherosclerotic disease, the rich databases of developed countries can provide a strong starting point for addressing important risk factors.













