Appendix F
Screening for Thyroid Cancer: Background Paper
Karen Eden, Ph.D.
Mark Helfand, M.D.
Susan Mahon, M.P.H.
Between 1951 and 1962 the United States Atomic Energy Commission conducted more than 100 aboveground detonations of nuclear weapons at the Nevada Test Site. Parts of Idaho, Montana, Utah, and Colorado had the highest exposure, but radioactive fallout was deposited throughout the United States. Infants and small children who drank milk or ate fresh vegetables contaminated with fallout were exposed to the highest doses of radiation, and as adults these persons are most at risk for developing thyroid abnormalities.
In 1997, the National Cancer Institute (NCI) released a report estimating the amount of radiation exposure Americans received from the nuclear tests (USDHHS, 1997). The report states that the average dose of radiation received by each American was 0.02 gray (Gy). Average exposures in some Western and Midwestern states were higher as much as 0.16 Gy in some areas. In addition to place of residence, the source and quantity of milk consumed by infants and young children can be used to help predict the dosage of the radioactive iodine (I-131) reaching the thyroid gland.
The NCI findings raised concerns that individuals exposed to higher dosages of I-131 might have a high risk of developing thyroid cancer later in life and that early detection and intervention for thyroid cancer could be useful for those persons.
To justify screening, there must be evidence that screening tests can detect thyroid cancer accurately and safely in asymptomatic individuals, that early treatment decreases mortality or morbidity from thyroid cancer when compared with delaying treatment until symptoms occur, and that the benefits of screening clearly outweigh the adverse effects of the screening program itself. Unfortunately, evidence about the ability of early detection to prevent morbidity and mortality from
thyroid cancer is incomplete. In contrast to the case of screening for breast cancer, for example, there are no randomized, controlled trials of screening for thyroid cancer, either in the general population or in high-risk groups. Instead, the effect of screening must be inferred from observational studies regarding the prevalence of undiagnosed thyroid cancer and the potential benefit of early detection.
In this paper we address whether physicians should screen for thyroid cancer seen in asymptomatic patients thought to have been exposed to I-131. We focus on studies of screening in the general population and in high-risk groups. We examine the accuracy of the tests used for screening, the number of cancer patients detected with screening, and evidence that treatment of cancers found by screening improves outcomes.
Definitions
Screening is "the application of a test to detect a potential disease or condition in a person who has no known signs or symptoms of that condition at the time the test is done" (Eddy, 1991). Studies of screening can be classified according to the setting in which the decision to screen takes place. In clinic-based screening, or casefinding , a screening test is performed in patients who visit a primary-care physician for an unrelated reason. Studies of casefinding programs provide the most realistic estimates of the effects and costs of screening in a clinic or office practice, but there have been very few studies of casefinding for thyroid cancer. Population-based studies contact, recruit, and follow patients in the context of an epidemiologic research effort. Such studies show the extent of unsuspected thyroid cancer in a population sample, but they do not reflect the yield or costs of screening in clinics or providers' offices. We used population-based studies as a benchmark against which the yield and benefits of clinic-based screening programs could be measured. Finally, studies of monitoring in high-risk groups describe efforts to monitor individuals with occupational exposure to radiation or with a history of head and neck irradiation for benign or malignant conditions. Such studies could be less relevant to screening in populations exposed to the much lower doses of radiation from the Nevada Test Site.
Background: Challenges in Developing and Assessing a Screening Proposal
Before the consequences of screening can be estimated, it is necessary to formulate the screening problem. To formulate a strategy researchers must specify the intended population for screening; the screening tests, follow-up tests, and treatments that will be used; and the type of outcomes influenced by the tests. In this section, we enumerate the information gaps, and we suggest a strategy for a "baseline" screening program.
What Is the Target Population? How Can It Be Reached?
For screening to be effective, there should be a substantial prevalence of undiagnosed disease in the target population. It is difficult to estimate this prevalence unless the target population for screening is clearly defined and is similar to populations used for published studies. Current age, place of residence as an infant or young child, and current residence might be used as criteria for screening.
One approach to identifying patients might be for primary-care providers (or public health agencies) throughout the United States to ask questions designed to identify exposed individuals. If this approach is taken, those questions are the initial test for screening, and their sensitivity and specificity for identifying high-risk individuals would need to be measured to estimate the prevalence of disease in the screened population. Another approach would be to target individuals between the ages 35 and 55 who are current residents of counties that had high exposure to radiation; this would omit individuals who had moved away and could include low risk individuals who had moved to those areas as adults. Estimating the effectiveness of this approach would require information on the rate of migration to and from these areas and areas that received lower doses. A third approach would replicate the efforts of epidemiologic studies to contact and track residents throughout the United States and have them report to a single, organized source of care. Finally, an effort to teach and promote thyroid self-examination could be the primary tool for screening. Studies of screening programs do provide information about screening in a defined geographic area, but little if any information is available about the efficacy of the other approaches.
Exposure from the Nevada Test Site detonations occurred more than 30 years ago. Exposed individuals could now be widely dispersed throughout the United States. People who have already been diagnosed and treated for thyroid cancer cannot benefit from screening, so the yield of screening will depend on the probability of having undiagnosed cancer many years after the exposure.
What Test Should Be Done? Who Should Do Them? How Should They Be Interpreted?
To estimate the effect of screening, the choice and interpretation of screening and follow-up tests must be specified. Either a physical examination or an ultrasound examination can be used to screen for thyroid cancer. Both tests identify thyroid nodules that could be cancerous. If a nodule is found, a fine-needle aspiration (FNA) is done to identify cell types found. Individuals found to have malignant cells, or cells that could be malignant, could undergo surgery and other treatments for thyroid cancer.
The interpretation and accuracy of the tests vary. Whether palpation or ultrasound is used, it is necessary to specify how an abnormal result is defined and what action will be taken if the result is normal or abnormal. One variable is the size of the nodule that prompts confirmation by FNA. In some centers most patients
with microadenomas are followed with physical examinations (Tan and Gharib, 1997); in other programs, serial ultrasound test or no tests at all might be done. Recommendations for the management of cystic nodules and of small thyroid cancers and protocols for the management of FNA results also vary. No single protocol has been adopted for screening programs.
How the tests are performed also can affect results. For ultrasound, relevant characteristics might include the resolution of the image and the qualifications and experience of the personnel who perform and interpret the test. For physical examination, a relevant characteristic might be whether examiners were given special training in examining the thyroid and whether standardized measurements were taken as part of the examination. In general, population-based studies and studies of surveillance for thyroid cancer have used structured interviews and examinations by expert examiners, conditions that could be difficult to replicate throughout the nation. Proficiency is also an important influence on the accuracy and cost of confirmatory FNA (Hall et al., 1989).
Which Cancers Require Treatment? What Treatments Should Be Used?
To estimate the effectiveness of early treatment for thyroid cancer we must be able to predict what treatment will be done when a cancer or suspicious nodule is found. Recommendations for treatment of thyroid cancers vary among studies and centers. For example, to manage small, localized papillary carcinomas, which are common in individuals exposed to ionizing radiation, some experts prefer total thyroidectomy; others recommend lobectomy with or without adjuvant therapy with ablative doses of I-131. More aggressive therapies could reduce the recurrence rate but cause higher rates of complication. In a nationwide initiative, individual surgeons' recommendations also might vary, making it difficult to estimate the rate of recurrence or complications that would be associated with screening.
What Health Outcomes Should Be Considered? How Do Screening Outcomes Compare with Usual-Care Outcomes?
Health outcomes relevant to screening for thyroid cancer include mortality and morbidity related to thyroid cancer and to the tests and treatments used in the screening program. Many studies report the number of cases of cancer detected by screening, but few report observed health outcomes in the screened population, and none has made an unbiased comparison of the outcomes of screening with the outcomes of usual care. As a result, the reduction in morbidity and mortality associated with screening can only be inferred from indirect evidence.
Figure F.1 illustrates the type of evidence that could be used to make these inferences. Arcs 1 and 2 indicate direct evidence comparing the mortality and morbidity associated with screening against that of usual care; such evidence is
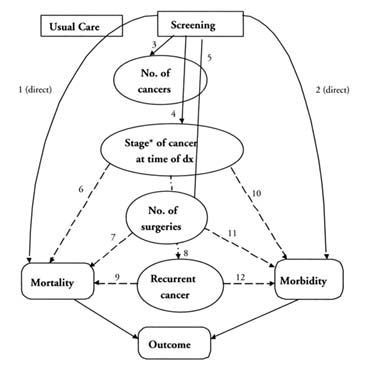
FIGURE F.1 Evidence model. Arcs indicate causal links and lines of evidence. Arcs 1 and 2 represent direct (experimental) evidence linking screening to morbidity and mortality. Arcs 3 to 5 represent evidence from observational studies of screening. Arcs 6-11 represent links for which the available evidence comes from epidemiologic and clinical observational studies not performed in the context of screening.
* ''Stage" means any factor that can be used to predict outcome, including patient characteristics (e.g., age) and features of the cancer (size, histologic type, and presence of local or distant metastases).
not available. Studies of screening do provide evidence about the number of cancers found in a population (arc 3) and, to a lesser extent, the stages of these cancers at the time of detection (arc 4) and the number of surgical operations performed as a result of screening (arc 5).
Does finding these cancers and treating them earlier reduce mortality and morbidity? The stage of cancer at the time of diagnosis, cancer recurrence, and surgery performed are intermediate or surrogate outcomes of screening—they might be related to mortality and morbidity, but they are not a direct measurement of them. Because there is no direct evidence linking screening to health outcome, the effect of screening on mortality and morbidity is inferred. Arcs 6
through 12 illustrate causal links between the intermediate measures and health outcomes. Arc 6 is the relationship of cancer stage at the time of detection to mortality. Arc 7 is mortality due to fatal complications of surgery and anesthesia. Arc 8 is the relationship between stage of cancer at the time of detection and the likelihood of developing recurrent cancer. Arc 9 is the effect of recurrence on mortality. Similarly, morbidity depends on morbidity of cancer at the time of detection (arc 10), morbidity due to complications of surgery (arc 11), and morbidity due to recurrent cancer (arc 12). Arcs 10 and 12 are dashed because most studies report results for usual care rather than screening programs, and so they deal with populations that might not be similar to those included in screening programs.
Lack of information about current practice also makes it difficult to estimate the effectiveness of not screening; that is, of usual care. Screening identifies cancers that would be detected in usual care after some delay. How much is gained by finding these cancers earlier? In the absence of randomized trials, this benefit must be estimated from the length of the delay, the extent to which the cancer advances during the delay, and the effect of advancement on mortality and morbidity. Information about usual care is needed to estimate the length of delay and the rate of advancement during the delay, but such data are sparse. For this reason, the confidence range about any estimate of the benefit of early detection by screening will be wide.
No screening proposal can satisfy all of these concerns completely, and uncertainties do not mean we should not screen for thyroid cancer. Unless a specific proposal is formulated, however, the consequences of screening cannot be estimated.
Baseline Strategy and Assumption
We examined two alternatives to usual care: screening with palpation and screening with ultrasound examination. We assumed that screening would take place in the primary-care setting among patients seeing a provider for reasons other than thyroid disease. We also assumed that providers, health systems, and public health officers could reliably identify individuals exposed to a specified dose of radiation by asking questions about risk factors identified in the NCI study of the Nevada nuclear test.
Figure F.2 depicts the assumptions we made about how screening and follow-up tests would be interpreted and what actions would be taken on test results. For the "palpation" strategy, FNA would be performed if the examiner palpated a nodule. If the FNA result was "malignant" or ''suspicious," the patient would undergo thyroidectomy. If the FNA result was "benign," palpation would be repeated every 6 months. If, over time, the nodule were to enlarge, a repeat FNA would be done. If the FNA result was "insufficient" or "nondiagnostic," FNA would be repeated, possibly under ultrasound guidance. If the FNA was persistently
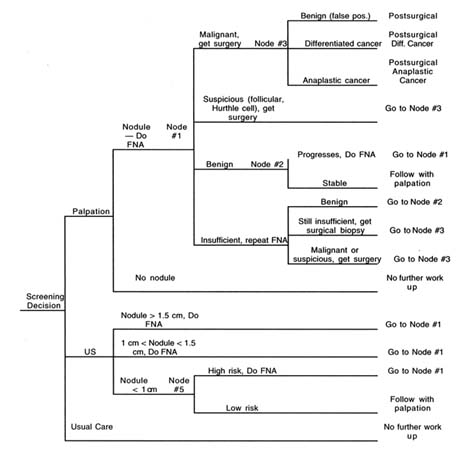
FIGURE F.2 Screening decision tree.
nondiagnostic, a lobectomy would be done to determine whether there was cancer.
These assumptions probably underestimate the use of ancillary tests in the follow-up of individuals found to have nodules. For example, in practice, serial ultrasound examinations, trials of levothyroxine, and scintigraphy are commonly used to evaluate or monitor patients with thyroid nodules, but we assumed that these interventions would not be part of a screening protocol and so did not attempt to assess the benefit or harm they produce.
In choosing between palpation and ultrasound as the first test for screening, an important issue is whether it is worthwhile to pursue small (<1 cm or <1.5 cm)
impalpable nodules found by ultrasound. When palpation is the first test, this issue is moot, because by definition "incidentalomas" or occult thyroid cancers cannot be detected by palpation.
The "ultrasound" strategy is similar to the "palpation" strategy, except that the initial management of a nodule depends on its size. As shown in Figure F.2, if ultrasound is the first test, a decision about how to manage small nodules must be made (node 4). Several experts recommend against routine aspiration of all nodules, but their recommendations are intended for nodules found incidentally in individuals who do not exhibit risk factors for thyroid cancer. This recommendation is depicted as node 5 in Figure F.2, in which patients with additional risk factors proceed to aspiration, whereas "low risk" patients might be followed clinically. However, because individuals who have been exposed to radiation usually are considered "high risk,'' it is possible, in a program to screen individuals exposed to radiation, that aspiration with ultrasound guidance would be attempted in patients found to have occult nodules. If malignant or suspected cytology is found, surgical diagnosis and perhaps aggressive treatment are more likely—again because of the history of radiation exposure.
Thus, the foremost question in choosing between ultrasound and palpation is this: In patients with low levels of radiation exposure due to exposure to fallout from the Nevada experiments, do the potential benefits of detecting and treating occult thyroid cancers outweigh the potential harm posed by additional monitoring, surgery, and medical treatments that will result from screening? Because ambiguity about these decisions could reduce the benefits of screening, a screening recommendation about thyroid cancer should carefully specify what level of exposure makes a patient "high risk" with respect to the aggressiveness of follow-up of small nodules, what size nodules should prompt a work-up, and when aggressive surgical therapy should be applied.
Methods
We reviewed studies of screening for thyroid cancer and studies of the accuracy of tests commonly used to screen for thyroid cancer.
Data Sources
To find relevant articles on screening for thyroid cancer in high-risk populations, we searched the MEDLINE data base for papers published between 1966 and 1998 using the medical subject heading (MeSH) term thyroid neoplasms combined with the MeSH terms mass screening, environmental exposure, radiation-induced neoplasms, power plants, nuclear reactors, radioactive fallout, and nuclear warfare, and the text words screen, screening, power plants, and nuclear reactors. For studies of test performance, we searched the same data base, combining the MeSH terms thyroid neoplasms and sensitivity and specificity. For
recent data on incidence and prevalence of thyroid cancer, we searched for papers published since 1987, and we restricted our focus to papers with the MeSH term thyroid neoplasms and the subheading epidemiology . These searches resulted in a total of 1,353 citations: 904 from the screening search, 249 from the test performance search, and 200 from the epidemiology search. To supplement our MEDLINE searches, reference lists from recent reviews were searched and articles recommended by thyroid cancer panel members were retrieved.
Papers were excluded unless they included information on at least one of the following areas:
-
controlled studies
-
screening in asymptomatic persons
-
health outcomes
-
screening by physical exam, ultrasound, or FNA
-
recommendations for screening based on test results
-
population-based studies
-
size, stage, or type of nodule.
Studies of screening for congenital or familial thyroid disorders were also excluded.
Study Selection
In all, 56 studies were included in our review: Twenty-six addressed either screening in an exposed or unexposed population or surveillance in an exposed population; 23 addressed the accuracy of palpation, ultrasound, or FNA; and 10 addressed the incidence, natural history, treated history, or predictors of mortality in patients with thyroid nodules or thyroid cancer. (The numbers do not add to 56 because of overlap among paper topics.) We found only one study that attempted to examine whether a delay in the initial treatment of thyroid cancer was associated with decreased survival (Mazzaferri and Jhiang, 1994). We also included well-done review articles and meta-analyses about the epidemiology, course, and treatment of thyroid cancer and about the relationship between radiation exposure and the risk and type of thyroid cancer (Caruso and Mazzaferri, 1991; Fraker et al., 1997; Gharib, 1994; Gharib and Goellner, 1993; Giuffrida and Gharib, 1995; Moosa and Mazzaferri, 1997; Ron and Saftlas, 1996; Ron et al., 1995; Schlumberger, 1998; Tan and Gharib, 1997).
Data Extraction
We sought to answer several questions about four topics:
-
Yield of screening. How many individuals with thyroid nodules and cancer does screening identify?
-
Accuracy of tests. What are the sensitivity and specificity of the initial tests for screening (palpation or ultrasound) and of the confirmatory FNA test? What factors affect sensitivity and specificity?
-
Consequences of a screening program. Given the prevalence of disease and the accuracy of the diagnostic tests, how many individuals with thyroid cancer will screening detect? How many follow-up tests will be performed? How many healthy individuals will have false-positive test results that require additional evaluation? How many surgical operations will be done?
-
Effectiveness. Is there evidence that early treatment reduces the burden of illness? Specifically, how do the outcomes of screening compare with the outcomes of usual care? How might reducing the delay in diagnosis affect the potential complications of thyroid cancer?
From each study of screening or surveillance we extracted the following information: the setting in which screening or surveillance was performed, the risk status of the target population, the screening tests used, and the prevalence of thyroid nodules and of thyroid cancer found by screening. When it was available, we abstracted information on the characteristics of the cancers detected by screening (papillary, follicular, undifferentiated, localized, regional, distant metastasis, and so on.)
In studies that measured the performance of screening or confirmatory tests, we recorded the tests used, the gold standard determination of disease, the sensitivity and specificity of the tests, and the presence of biases (such as diagnostic-review bias) that could affect the reported results. We also abstracted the number of patients who underwent surgery to establish a final diagnosis.
Probability of Developing Thyroid Cancer
According to the American Cancer Society, 17,200 new cases of thyroid cancer will be diagnosed in 1998 in the United States (Landis et al., 1998). The incidence of thyroid cancer varies with sex and age. In the SEER registry, the average lifetime risk of being diagnosed with thyroid cancer was 0.27% for males and 0.66% for females (Ries et al., 1997). (For comparison, in a woman of "average risk," the risk of developing colon cancer or breast cancer is 6% or 9.4%, respectively.) In men, the incidence of thyroid cancer gradually increases until age 70-79, at which time the incidence is 8.6 per 100,000 (Ries et al., 1997). For women, the peak incidence, 13.2 per 100,000, is reached in the 50-54 year age group.
The probability of developing thyroid cancer depends on the presence of several risk factors. Exposure to ionizing radiation is the most well-established risk factor for thyroid cancer (McTiernan et al., 1984; Ron et al., 1995). In a population-based study done in Connecticut from 1978 to 1980, about 9% of thyroid cancers were attributable to prior irradiation of the head and neck (Ron et
al., 1987). Most studies of this risk factor involve patients who had received external radiation to the head and neck for benign conditions (Pottern et al., 1990; Ron et al., 1988, 1989; Schneider et al., 1993; Shore et al., 1993; Tucker et al., 1991). In those studies, an increased incidence of thyroid cancer was observed among people who had received radiation doses as low as 10 rad (0.10 Gy) (Ron et al., 1988; Schneider et al., 1993), and the incidence rose linearly up to a dose of 1,000 rad (10 Gray) (Ron et al., 1989).
Mortality and Morbidity of Thyroid Cancer
In 1995 all-stage 5-year survival for thyroid cancer was 92.4% for males and 95.9% for females. In 1995 there were 1,120 deaths due to thyroid cancer in the United States (Wingo et al., 1995); 1,200 deaths are expected in 1998 (Landis et al., 1998). In 1994 the lifetime risk of dying from thyroid cancer was 0.04% for males and 0.07% for females. The risk of dying from thyroid cancer is much lower than the risk of developing thyroid cancer because most people with thyroid cancer, die of other causes.
The risk of death depends on age and on the characteristics of the thyroid cancer. Longitudinal studies of the treated history of thyroid cancer indicate that age at the time of diagnosis, tumor size, local invasion, tumor cell DNA content, and regional or distant metastasis are associated with mortality from thyroid cancer (Fraker et al., 1997). Because most deaths occur in elderly people who have undifferentiated, metastatic cancers, average rates overestimate mortality in younger and middle-aged individuals, who tend to have papillary and follicular cancers (Ron, 1996). Although distant metastases are present in only 5% of thyroid cancers at the time of diagnosis, patients in this group account for about 60% of deaths. At the other extreme, 56% of cancers are localized to the thyroid gland at the time of diagnosis, but only 4 patients per 1,000 in this group die from thyroid cancer within 5 years (USDHHS, 1997).
SCREENING TESTS
History and Physical Examination Palpation
A thorough clinical evaluation for thyroid disease usually includes ascertainment of age, gender, family history of thyroid disease, history of hormonal problems or prior neck irradiation, and visual inspection and palpation of the thyroid gland by a clinician (Ashcraft and Van Herle, 1981; Brander et al., 1992). The goal of palpation is to detect nodules and to assess the size of the thyroid gland. When a nodule is palpated, the examiner notes its firmness and attachment to underlying structures and attempts to determine whether a single nodule or multiple nodules are present. Additionally, nearby lymph glands are palpated to detect enlargement (Khafagi et al., 1988; Spiliotis et al., 1991). The examiner asks whether the patient has noticed it, how long it has been present, and whether the
patient has had difficulty swallowing or has had hoarseness. Although the presence of these conditions increase the likelihood that a nodule is malignant (Holleman et al., 1995; Khafagi et al., 1988; Merchant et al., 1995; Spiliotis et al., 1991), it is usually not possible to tell when nodules are benign or malignant by palpation alone (Ashcraft and Van Herle, 1981).
Three studies of screening in asymptomatic individuals used palpation and ultrasound to detect thyroid nodules (Table F.1). These studies used ultrasound as the gold standard determination of the presence of a nodule; the sensitivity of palpation for all size nodules was 0.10 to 0.31, which indicates that a high proportion of nodules detected by ultrasound were too small to be palpated (Ezzat et al., 1994; Inskip et al., 1997; Mettler et al., 1992). This means that for a person with a nodule of any size, there is a probability of 0.10 to 0.31 that it will be palpated. The specificity of palpation ranged from 0.95 to 1.0. This means that for a person without a nodule, there is a probability of 0.95 to 1.0 that no nodule will be palpated.
One study group consisted of 100 healthy individuals who had no history of exposure to radiation. Twenty-one nodules were palpated in these individuals; 47 patients had nodules 0.5 cm or larger in diameter as shown by ultrasound examination, and 20 had nodules smaller than 0.5 cm. The overall sensitivity of palpation was 31% (21/67). For nodules larger than 0.5 cm the sensitivity was 0.45 (21/47), and for nodules larger than 1 cm the sensitivity was 0.84 (21/25).
In subjects who have been exposed to radiation, the sensitivity of palpation to find nodules could be lower. In one study, 18 nodules were palpated in a group of 1,060 children and adults living near Chernobyl (Mettler et al., 1992); in the same population, ultrasound detected 75 nodules larger than 0.5 cm in diameter (22 nodules, 0.5-0.9 cm, 44 nodules, 1-2 cm, 9 nodules >2 cm). Only 8 of the 18 palpated nodules were confirmed with ultrasound; 10 of the palpable nodules were not seen on ultrasound and were classified as false-positive results. For nodules larger than 2 cm, the sensitivity of palpation was 0.89, but sensitivity for 1-2 cm nodules was only 0.38.
In another study, 1,979 Estonian Chernobyl cleanup workers were examined from 1-9 years after their exposure at the reactor site (Inskip et al., 1997). In all, nodules were detected by ultrasound; of these 175 were larger than 0.5 cm, 88 were larger than 1 cm, and 35 were larger than 1.5 cm. In a study of patients screened 22 years or more after childhood head and neck irradiation (Schneider et al., 1997), palpation identified only 5 of 11 nodules 1.5 cm or larger, while ultrasound found 54 more.
Because the decision to examine and study a nodule is affected by its size, the ability to estimate the size of a nodule can be important. Clinicians often underestimate the size of palpable nodules and cannot reliably determine whether nodules are single or multiple (Brander et al., 1992; Tan et al., 1995). Some studies suggest that palpation is sensitive for nodules larger than 1.5 cm, others confirm the poor results of the studies discussed above. In one study, for
TABLE F.1 Sensitivity and Specificity of Palpation to Detect Nodules (using ultrasound as the gold standard)
|
Author, Year |
Study sample and setting |
P (nodule) |
Palpation by 2 clinicians? |
US Resolution |
Size criteria for nodule |
Sensitivity |
Specificity |
LR+ |
LR- |
PV+ |
PV- |
|
Ezzat, 1994 |
Screening of 84 female and 16 male unexposed adult American volunteers (n = 100) |
0.67 |
y |
10 MHz |
All Sizes |
0.31 |
1.00 |
NAa |
0.69 |
1.00 |
0.42 |
|
Inskip, 1997 |
Screening of 1984 exposed adult clean up workers from Chernobyl (n = 1984) |
0.11 |
n |
7.5 MHz |
All Sizes (FNA if >1 cm) |
0.22 |
0.95 |
4.097 |
0.83 |
0.32 |
0.91 |
|
Mettler, 1992 |
Screening of 1060 residents of villages around Chernobyl (exposed and not exposed). Ages 5, 10, 40, 60 years (n = 1060) |
0.08 |
y |
7.5 MHz |
>.5 cm |
0.11 |
0.99 |
0.99 |
0.90 |
0.44 |
0.94 |
|
Definitions: Sensitivity (also called true positive rate) is the "likelihood that a diseased patient has a positive test." Specificity (also called true negative rate) is the "likelihood that a nondiseased patient has a normal test." LR+ (positive likelihood ratio) = sensitivity/(false positive rate). For example, a positive likelihood ratio of 10 means that a positive test is 10 times more likely to come from a patient with disease as from a patient without disease. LR- (negative likelihood ratio) = (false negative rate)/specificity. For example, a negative likelihood ratio of .10 means that a negative test is 1/10th as likely to come from a patient with disease than from a patient without disease. PV+ (positive predictive value) is "the fraction of patients with a positive test result who have disease." PV- (negative predictive value) is ''the fraction of patients with a normal test result who do not have disease." a In Ezzat, all palpated nodules were confirmed with ultrasound, so this ratio is infinity. SOURCE: Adapted from Medical Decision Making, HD Sox, MA Blatt, MC Higgins, KI Marton, Butterworth-Heinemann, 1988. |
|||||||||||
example, the sensitivity of palpation was 0.50 (14/28) for nodules 1-2 cm in diameter and 0.58 (19/33) for nodules larger than 2 cm (Brander et al., 1992).
Whether a single nodule or multiple nodules are present also can affect decisionmaking about a treatment, especially in individuals exposed to radiation who often have nodules scattered throughout the gland. In one study in which 151 single nodules were palpated 48% (73) of the patients actually had multinodular glands (Tan et al., 1995). Another study found that 63% (20/32) of palpated single nodules were shown by ultrasound examination to be multinodular (Brander et al., 1992)
In two studies of exposed populations, the positive predictive values for a palpated nodule were 0.32 and 0.44 (Inskip et al., 1997; Mettler et al., 1992), respectively. In one study, for example, 139 patients had palpable nodules, but only 44 of these were confirmed by ultrasound (positive predictive value, 0.32). In the same studies, the negative predictive values were 0.92 and 0.94. Because the prior probability of having no nodule was approximately 90% in these studies, a negative test result increases only slightly the probability of having no nodule.
The sensitivity of palpation appears to be 0.31 or less when all sizes of nodules are considered. However, sensitivity increases as size increases, particularly beyond 2 cm. Screening for nodules by palpation appears to have reasonable specificity—above 95%. Nevertheless, fewer than half of individuals thought to have a nodule by palpation actually do have one. For purposes of detecting whether a nodule is solitary, palpation miscategorizes approximately 50% of patients.
Ultrasound
To perform an ultrasound test on the thyroid, the patient lies supine with the neck hyperextended (Tan et al., 1995). A radiologist typically performs the test using an image scanner with 5-10 MHz linear transducers (Brander et al., 1992; Ezzat et al., 1994; Hsiao and Chang, 1994; Tan et al., 1995). An ultrasound test usually reveals the following details about thyroid nodules: echogenicity (reduced, normal, increased), "geneity" (homo, hetero), cystic component (nil, < 50%, 50%, >50%), calcification (present, absent), halo appearance (present, absent, doubtful), and nodularity (solitary, multiple) (Watters et al., 1992; Ashcraft and Van Herle; 1981). The information that a nodule is cystic or solid can be useful clinically. Cystic nodules often are managed by draining with a fine needle, and further evaluation depends on whether the nodule recurs.
Ultrasound is considered to be as accurate as is histologic examination of thyroid tissue for determining whether a thyroid nodule is present. The most important feature of ultrasound is its ability to detect clinically impalpable nodules. This feature makes ultrasound a highly sensitive test for screening, because
such nodules, called incidentalomas or occult nodules, can contain carcinoma ("occult carcinoma"). In choosing between ultrasound and palpation as the first test, the foremost question is whether it is worthwhile to diagnose occult carcinoma, or whether screening is beneficial primarily in patients with relatively large (>1.5 cm) palpable nodules.
Confirmatory Tests: Fine Needle Aspiration
When a thyroid nodule is detected, an FNA confirmatory test often is performed (Bouvet et al., 1992; Cusick et al., 1990; Hamburger and Hamburger, 1985). FNA is a simple, relatively low-risk procedure that provides a cytologic sample to detect cancer, but it should be performed only by physicians experienced with the procedure (Gharib, 1994). It causes minor, local short-term pain and occasionally a small hematoma (Gharib, 1994; Gharib and Goellner, 1993). The use of FNA has greatly reduced the need for surgical excision to diagnose the cause of thyroid nodules (Fraker et al., 1997).
Fine-needle aspiration is usually an outpatient procedure. The physician palpates the thyroid gland while the patient lies supine on a bed. The skin around the thyroid is cleaned with alcohol, and a disposable needle (21-25 gauge) with a 10 mL syringe is inserted into the nodule (Gharib, 1994; Cusick et al., 1990). Suction is applied and the aspirate is sprayed onto glass slides (Haas et al., 1993). To reduce the number of false-negative results, several (2-6) aspirations are usually performed (Gharib and Goellner, 1993). Smears are made using the Papanicolaou, May-Grunwald-Giemsa, and/or Romanowsky-based Liu methods (Cusick et al., 1990; Gharib, 1994; Lin et al., 1997). The slides are reviewed by a cytopathologist who classifies the cells into one of the following groups (Holleman et al., 1995):
-
Benign. Aspirated material adequate and consists of thyroid cell groups without signs of malignancy or consists of cyst fluid.
-
Follicular. Little or no colloid with microfollicular cell groups. Differentiation between follicular adenoma and follicular carcinoma not possible.
-
Suspicious. Signs suggestive but not diagnostic of malignancy in the aspirated material.
-
Malignant. Several clearly malignant characteristics found.
-
Inadequate. (or unsatisfactory). No conclusions because the smear does not contain enough material (fewer than 6 cell groups) or because the smear contains normal thyroid cells, suggesting that the neoplasm was not sampled.
In practice, 70% (range, 53%-90%) of FNA specimens are classified as benign; 4% (1%-10%) as malignant; 10% (5%-23%) as suspicious, follicular, or nondiagnostic; and 17% (15%-20%) as an inadequate or unsatisfactory sample (Fraker et al., 1997).
The result of FNA, along with other clinical information, is used to decide whether to proceed with surgical excision. The frequency of surgery that can be expected in a screening program, and the ratio of cancers to surgery, are important measures of the accuracy of FNA. In studies from major centers, an average of 18% of patients having FNA go on to have surgery (Gharib and Goellner, 1993; Haas et al., 1993; Spiliotis et al., 1991). Of patients who have surgery, it is estimated that 15-32% have cancer (Gharib and Goellner, 1993; Haas et al., 1993). The cancer probability depends on the criteria used to act on FNA results. Some investigators report that only the "malignant" category prompted surgery, but in many studies all patients with a suspicious or follicular FNA result also are taken to surgery (Bouvet et al., 1992; Cusick et al., 1990; Holleman et al., 1995; Khafagi et al., 1988; Morayati and Freitas, 1991).
The rate of nondiagnostic FNA results affects the rate of surgery. Because some authors do not differentiate between "unsatisfactory" and "indeterminate," the term "nondiagnostic" is used here for discussion. In some series, surgery was performed for all nondiagnostic FNAs (Cusick et al., 1990; Piromalli et al., 1992). Others took only patients with nondiagnostic results to surgery if other clinical symptoms were present: hoarseness, rapid growth of a nodule, or fixation to an underlying structure (Holleman et al., 1995; Jones et al., 1990; Khafagi et al., 1988; Lin et al., 1997; Merchant et al., 1995; Spiliotis et al., 1991).
The rate of nondiagnostic samples in referral clinics and hospitals ranges from 1% to 19% (Bouvet et al., 1992; Cusick et al., 1990; Haas et al., 1993; Holleman et al., 1995; Khafagi et al., 1988; Lin et al., 1997; Merchant et al., 1995; Ng et al., 1990; Ongphiphadhanakul et al., 1992; Piromalli et al., 1992; Spiliotis et al., 1991; Takashima et al., 1994). Studies that included a bedside evaluation of the sample with repeated aspiration as needed reported lower rates of nondiagnostic samples (Lin et al., 1997; Takashima et al., 1994). In one study, the researchers reported a nondiagnostic rate of 23% before implementing a bedside evaluation strategy to immediately repeat the test when nondiagnostic results were obtained (Khafagi et al., 1988). Those authors report dropping the nondiagnostic result rate to 12% after the bedside evaluation was in place. One group of investigators (Holleman et al., 1995) suggests that repeating all nondiagnostic FNAs and having two pathologists discuss the results would increase the number of diagnostic results. The probability of a nondiagnostic FNA result diminishes as operators become more experienced with the technique (Haas et al., 1993; Jones et al., 1990; Merchant et al., 1995; Piromalli et al., 1992) demonstrating the importance of having experienced physicians perform the technique.
The probability of nondiagnostic FNA results also is related to the size of the nodule being aspirated. One study found that 27% of the nodules smaller than 1.5 cm were nondiagnostic (Khafagi et al., 1988). In the same study, 16% of the nodules 1.5-3 cm and 13% of nodules larger than 3 cm were nondiagnostic.
Published studies of the accuracy of FNA use the findings from surgery as the gold standard determination of disease. These studies extended from the calculation
of sensitivity and specificity patients who had benign FNA results and did not go to surgery. As Gharib and Goellner (1993) note, because of this diagnostic-review bias, published studies overestimate the sensitivity of FNA for thyroid cancer. Exclusion of those patients also causes FNA specificity to be underestimated.
In published studies, the reported sensitivity FNA for thyroid cancer range from 70% to 97% (Bouvet et al., 1992; Cusick et al., 1990; Haas et al., 1993; Hamburger and Hamburger, 1985; Holleman et al., 1995; Jones et al., 1990; Khafagi et al., 1988; Lin et al., 1997; Merchant et al., 1995; Morayati and Freitas, Freitas, 1991; Ongphiphadhanakul et al., 1992; Piromalli et al., 1992; Spiliotis et al., 1991; Takashima et al., 1994; Watters et al., 1992). Specificity ranged from 52% to 98% for the same studies. The apparent sensitivity and specificity depend on how the investigators classify nondiagnostic FNA results. Examination of sensitivity and specificity results revealed that the surgical decisions related to nondiagnostic FNA results had a strong relationship with sensitivity and an even stronger one with specificity.
To examine this relationship in more detail, studies that document whether patients with nondiagnostic FNA results go to surgery and also that list the histology reports were reanalyzed to report sensitivity and specificity with and without including the nondiagnostic results. A nondiagnostic FNA was classified as "positive" if the patient went to surgery. The results of this analysis are summarized in Tables F.2a and F.2b.
The analysis reveals that sensitivity increases slightly with the inclusion of nondiagnostic FNA results. Most of the patients with nondiagnostic results have benign follicular adenomas, and specificity drops by 4-20 percentage points. This suggests that quite a few more patients with benign nodules went to surgery than represented by specificity results, which typically exclude nondiagnostic FNA results.
In our analysis, the positive predictive value of FNA is the proportion of all surgical patients who prove to have thyroid cancer. Among the studies summarized in Table F.2b, the positive predictive values ranged from 0.28 to 0.71. Figure F.3 shows that the positive predictive value of disease decreased as the prevalence of disease decreased. The patients in these surgical series had clinically apparent signs or symptoms that brought them to medical attention in the usual course of care. Patients identified in a screening program might have a lower probability of disease, so the positive predictive value of FNA could be lower than that shown by Table F.2b and Figure F.3.
Because some patients with benign nodules develop cancer years later, most clinicians follow those patients with periodic physical examinations. Longitudinal studies of patients who had a benign FNA and did not have surgery demonstrate that a benign FNA is a reliable finding. In four studies, patients with untreated, cytologically diagnosed benign thyroid nodules were followed for several years for evidence of thyroid cancer (Jones et al., 1990; Kuma et al., 1994;
TABLE F.2a Sensitivity and Specificity of FNA
|
Author, Year |
Study sample and setting |
Total FNA |
Surg/ FNA |
Repeat FNA? |
US-guided FNA? |
Surgery of Benign FNA |
Nondiagnostic |
Nondiagnostic Surgery |
|
|
|
Patient n |
|
|
|
|
|
|
|
Cusick, 1990 |
395 Scottish patients with thyroid nodules at regional thyroid clinic. |
395 |
77.7% |
y |
? |
57.80% |
6.1% |
100.0% |
|
Holleman, 1995 |
112 Dutch outpatients referred by general practitioner for thyroid nodules. |
112 |
47.3% |
y |
y |
26.10% |
10.7% |
41.7% |
|
Jones, 1990 |
175 British euthyroid outpatients. |
175 |
46.9% |
? |
? |
|
13.7% |
70.8% |
|
Khafagi, 1988 |
618 Australian euthyroid outpatients with thyroid nodules referred to thyroid clinic. |
618 |
41.7% |
n, later y |
n |
38.6% |
33.0% |
31.4% |
|
Lin, 1997 |
3657 Taiwanese outpatients who were referred for palpable thyroid nodules. |
3657 |
10.3% |
y |
y |
7.0% |
3.2% |
48.6% |
|
Merchant, 1995 |
111 British referred for thyroid nodules. |
111 |
50.5% |
y |
? |
43.4% |
13.5% |
46.7% |
|
Piromalli, 1992 |
795 Italian outpatients referred for palpable thyroid nodules. |
795 |
27.2% |
y |
? |
|
5.3% |
100.0% |
|
Spiliotis, 1991 |
1200 Greek outpatients referred for thyroid disease. |
1200 |
16.8% |
? |
? |
13.2% |
13.3% |
6.3% |
|
Definitions: Sensitivity (also called true positive rate) is the "likelihood that a diseased patient has a positive test." Specificity (also called true negative rate) is the "likelihood that a nondiseased patient has a normal test." LR+ (positive likelihood ratio) = sensitivity/(false positive rate). For example, a positive likelihood ratio of 10 means that a positive test is 10 times more likely to come from a patient with disease as from a patient without disease. LR- (negative likelihood ratio) = (false negative rate)/specificity. For example, a negative likelihood ratio of .10 means that a negative test is 1/10th as likely to come from a patient with disease than from a patient without disease. PV+ (positive predictive value) is "the fraction of patients with a positive test result who have disease." PV- (negative predictive value) is "the fraction of patients with a normal test result who do not have disease.'' SOURCE: Adapted from Medical Decision Making, HD Sox, MA Blatt, MC Higgins, KI Marton, Butterworth-Heinemann, 1988. |
||||||||
TABLE F.2b Sensitivity and Specificity of FNA
|
|
Test for Malignant, Suspicious, Follicular |
Includes All Nondiagnostic FNAs as + tests Test for Malignant, Suspicious, Follicular, Nondiagnostic |
|||||||||||||
|
Author, Year |
Sensitivity |
Specificity |
LR+ |
LR- |
p (cancer nodule) |
PPV |
NPV |
sens. w/ nondiag. |
spec. w/ nondiag. |
LR+ |
LR- |
p (cancer nodule) |
PPV |
NPV |
|
|
Cusick, 1990 |
0.76 |
0.58 |
1.84 |
0.40 |
0.58 |
0.720 |
0.64 |
0.78 |
0.55 |
1.73 |
0.39 |
0.58 |
0.71 |
0.64 |
|
|
Holleman, 1995 |
0.84 |
0.52 |
1.74 |
0.31 |
0.40 |
0.533 |
0.83 |
0.85 |
0.45 |
1.56 |
0.33 |
0.40 |
0.49 |
0.83 |
|
|
Jones, 1990 |
0.65 |
0.69 |
2.13 |
0.50 |
0.40 |
0.585 |
0.75 |
0.70 |
0.52 |
1.46 |
0.58 |
0.40 |
0.46 |
0.75 |
|
|
Khafagi, 1988 |
0.89 |
0.72 |
3.17 |
0.15 |
0.20 |
0.436 |
0.97 |
0.91 |
0.52 |
1.91 |
0.17 |
0.20 |
0.28 |
0.97 |
|
|
Lin, 1997 |
0.80 |
0.99 |
59.58 |
0.20 |
0.31 |
0.963 |
0.92 |
0.82 |
0.82 |
4.58 |
0.22 |
0.31 |
0.65 |
0.92 |
|
|
Merchant, 1995 |
0.71 |
0.91 |
8.33 |
0.31 |
0.29 |
0.769 |
0.89 |
0.73 |
0.78 |
3.34 |
0.34 |
0.29 |
0.55 |
0.89 |
|
|
Piromalli, 1992 |
0.95 |
0.84 |
5.83 |
0.06 |
0.33 |
0.740 |
0.97 |
0.95 |
0.65 |
2.72 |
0.07 |
0.33 |
0.54 |
0.97 |
|
|
Spiliotis, 1991 |
0.89 |
0.86 |
6.61 |
0.12 |
0.16 |
0.556 |
0.98 |
0.90 |
0.75 |
3.66 |
0.13 |
0.16 |
0.40 |
0.98 |
|
|
Definitions: Sensitivity (also called true positive rate) is the "likelihood that a diseased patient has a positive test." Specificity (also called true negative rate) is the "likelihood that a nondiseased patient has a normal test." LR+ (positive likelihood ratio) = sensitivity/(false positive rate). For example, a positive likelihood ratio of 10 means that a positive test is 10 times more likely to come from a patient with disease as from a patient without disease. LR- (negative likelihood ratio) = (false negative rate)/specificity. For example, a negative likelihood ratio of .10 means that a negative test is 1/10th as likely to come from a patient with disease than from a patient without disease. PV+ (positive predictive value) is "the fraction of patients with a positive test result who have disease." PV- (negative predictive value) is "the fraction of patients with a normal test result who do not have disease.'' SOURCE: Adapted from Medical Decision Making, HD Sox, MA Blatt, MC Higgins, KI Marton, Butterworth-Heinemann, 1988. |
|||||||||||||||
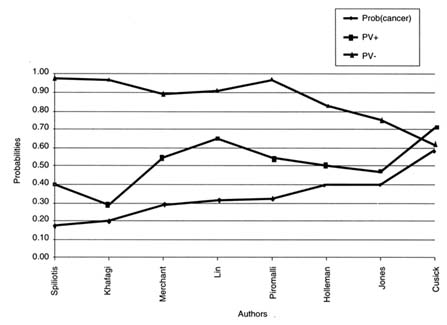
FIGURE F.3 Cancer probability as it relates to predictive values. Notes: Prob (cancer) is probability of thyroid cancer; PV+, positive predictive value, is the fraction of patients with a positive test who have thyroid cancer; PV-, negative predictive value, is the fraction of patients with a normal test who do not have thyroid cancer.
Morayati and Freitas, 1991; Piromalli et al., 1992; Tan and Gharib, 1997). In one study (Jones et al., 1990), 93 patients with benign FNA results were followed for at least 2 years with annual ultrasound and semiannual physical exams. There were no thyroid malignancies found in the follow-up period. In another study, 537 patients with benign FNA results were followed at 6-month intervals for 2-10 years (Piromalli et al., 1992). In this cohort no malignancies were found. An additional 42 patients in this group were lost to follow-up. In a follow-up study of 576 patients with benign FNA results and no surgical treatment (Morayati and Freitas, 1991), there were no documented thyroid malignancies after an average of 4.2 years of follow-up. In a long-term follow-up study by Kuma et al. (1994), cited in Tan and Gharib (1997), only 1 patient of 134 with nodules cytologically diagnosed as benign was diagnosed with a papillary carcinoma during a follow-up period of 9-11 years.
Consequences of Screening
We reviewed studies of screening programs to estimate the likely consequences
of a screening program in individuals exposed to fallout from the Nevada tests. For the screened population, we estimated the probability that a screened individual would be found to have a nodule; the probability that an individual would be found to have thyroid cancer, the distribution of size, histologic type, and spread of cancers; and the probability that a screened individual would undergo surgery. We found no evidence from studies of screening that we could use to estimate other important events related to health outcomes, such as the probability of long-term survival in patients found to have cancer or the rates of surgical complication. As mentioned earlier, these events must be estimated indirectly from studies performed in other settings.
Studies
Of the 26 studies of screening we selected, 12 concerned healthy adults with no history of exposure to radiation. Of these, 4 were population-based studies of healthy adults with no prior exposure to radiation (Brander et al., 1991; Tunbridge et al., 1977; Vander et al., 1968), 4 were studies conducted at a single institution involving unexposed volunteers (Ezzat et al., 1994; Hsiao and Chang, 1994), 1 was a mass screening of healthy adults (Ishida et al., 1988), and 3 were screening programs of healthy adults using casefinding (Bruneton et al., 1994; Miki et al., 1993; Woestyn et al., 1985).
Eight studies concerned individuals exposed to fallout from nuclear detonations. Three studies examined thyroid disease in workers after the Chernobyl nuclear reactor accident (Inskip et al., 1997; Ivanov et al., 1997) and in Chernobyl residents (Mettler et al., 1992). Three papers looked at residents of the Marshall Islands exposed to fallout from hydrogen bomb testing (Hamilton et al., 1987; Howard et al., 1997; Takahashi et al., 1997); 1 examined thyroid disease in survivors of the 1954 atomic bomb blast in Nagasaki (Nagataki et al., 1994); and 1 looked at residents of Utah, Nevada, and Arizona who were potentially exposed to fallout from nuclear weapons testing (Kerber et al., 1993). Time since exposure ranged from 1 year in Chernobyl to more than 40 years.
Six studies concerned surveillance for thyroid cancer in individuals exposed to radiation from medical interventions. Five papers described recall studies of adults who were exposed as children to medical radiation, either for benign conditions (Favus et al., 1976; Ron et al., 1984; Royce et al., 1979; Shimaoka et al., 1982) or for childhood cancer (Crom et al., 1997). One additional study concerned occupationally exposed hospital workers (Antonelli et al., 1995).
Tables F.3a and Table F.3b summarize results of the studies in 4 areas: probability of finding a nodule by palpation or ultrasound, probability of finding cancer, the proportion of nodules found to be cancerous, and the number of surgical operations performed as a result of screening. (Table F.3a provides descriptive data on the studies revealed and Table F.3b presents data probabilities calculated from the same studies).
Probability of Diagnosing a Nodule
The number of nodules found in screening programs depends on the population screened (unexposed or exposed), the test used (palpation or ultrasound), and the threshold size used to define a nodule (0.2 cm to 1.5 cm in various studies).
Unexposed Populations
Studies of screening unexposed adults with palpation find probabilities of nodules in the range of 0.01-0.05 (Brander et al., 1991; Ishida et al., 1988; Miki et al., 1993; Tunbridge et al., 1977; Vander et al., 1968). In unexposed populations, palpable thyroid nodules are more common in women, and their likelihood increases with age. In a population-based study in Whickham County, England (Tunbridge et al., 1977), 5.3% of women had palpable thyroid nodules. The probability for 18-24 year-old women was 4.7% and increased steadily to 9.1% for women over age 75. In the same study, only 0.8% of men had palpable thyroid nodules. In the United States, the probability of thyroid nodules for subjects enrolled in the Framingham study was similar (Vander et al., 1968): The all-age probability of palpated thyroid nodules among adult males was 1.5%; it was 6.4% among adult females.
More nodules will be diagnosed if ultrasound is used as the first test for screening. In studies performed in the general population, rates of 0.20-0.27 were observed (Brander et al., 1991; Miki et al., 1993). Women and older persons had higher rates. High-resolution ultrasound screening of 101 asymptomatic Finnish women (aged 49-58) detected nodules in 31 women (Brander et al., 1989). In France, 645 asymptomatic women and 355 asymptomatic men were screened using ultrasound (Bruneton, 1994). Forty-four percent of the women had thyroid nodules; 17.7% of the men had them. The probability of a thyroid nodule was 0.25 for participants under 50 years and increased to 0.42 for persons over age 50.
Exposed Populations
People who have been exposed to environmental and medical radiation have a higher prevalence of thyroid nodules than is found among the general population. Six population-based studies compared the number of nodules found through screening in radiation-exposed populations and in comparison groups (Hamilton et al., 1987; Howard et al., 1997; Kerber et al., 1993; Mettler et al., 1992; Nagataki et al., 1994; Takahashi et al., 1997). People exposed to the highest doses of radiation from the Nevada nuclear tests had a probability of 0.02-0.04 as determined by palpation; those exposed to lower doses had a probability of 0.02. In Marshall Islands tests, the probability in exposed groups was 0.07 (0.02-0.39) compared with 0.02 in people living farthest from the test site (Hamilton et al., 1987). Howard and co-workers (1997) found an even greater difference: 0.23 in exposed Marshall Islanders compared with 0.06 in unexposed
TABLE F.3a Studies of Screening for Thyroid Neoplasms
|
Author, year |
Study sample and setting |
Exposure |
Time since exposure |
Tests performed |
Definition of a nodule |
Group |
|
Population-based studies |
||||||
|
Brander 1991 |
253 randomly selected adults in Finnish town |
Unexposed |
— |
Questionnaire, PE, US |
> 0.5 cm |
|
|
Brander 1989 |
101 women in a Finnish town, 1988 |
Unexposed |
|
|
> 0.5 cm |
|
|
Ishida 1988 |
Mass screening: 152,651 Japanese women |
Unexposed |
— |
|
|
|
|
Tunbridge 1977 |
2,779 adults in an English town |
Unexposed |
— |
|
|
|
|
Vander 1954, 1968 |
5,108 adults in Framingham, MA without previous thyroid nodules |
Unexposed |
— |
|
|
|
|
Kerber 1993 |
2,473 adults in Nevada, Utah, Arizona |
Fallout from nuclear weapons testing |
7 to 35 years |
Interview, PE; FNA & 123I scan if palpable nodule |
palpable |
Dose = 50- >400 mGy (n=1418); Dose = 0-49 mGy (n=1055) |
|
Hamilton, 1987 |
2,273 residents of 14 atolls of Marshall Islands |
Fallout from BRAVO atomic bomb test on Bikini Island |
33 yrs |
PE |
>1 cm |
Most exposed islands (n = 1903); Least exposed (2 furthest atolls; n = 370) |
|
Howard, 1997 |
Marshall Islands residents PE: 253 exposed, 227 comparison US: 177 exposed, 47 comparison |
Fallout from nuclear weapons testing |
PE: 1-40 yrs; US @ 40 yrs |
PE (1954 to 1994) plus ultrasound (1994) |
1 cm or 0.5 cm plus features of malignancy |
Exposed (PE n = 253; US n=117); Unexposed (PE n = 227; US n = 47) |
|
Takahashi, 1997 |
Residents of Marshall Islands |
Fallout from nuclear weapons testing |
42 yrs |
PE, US |
|
BRAVO cohort (n = 815); EOT cohort (n = 1062); AT cohort (n = 216) |
|
Author, year |
Study sample and setting |
Exposure |
Time since exposure |
Tests performed |
Definition of a nodule |
Group |
|
Mettler, 1992 |
1,061 adults and children, population sample, Belarus |
Chernobyl |
4.5 yrs |
PE, US |
PE: dx of 2 MDs. US: >0.5 cm |
Exposed (n = 597); Unexposed (n = 481) |
|
Ivanov, 1997 |
167,862 Chernobyl cleanup workers |
Chernobyl |
1 to 8 yrs |
|
— |
1986 workers (mean dose 0.17 Gy; n = 77,663); 1987 workers (mean dose 0.10 Gy; n = 58,694); 1988-90 workers (mean dose 0.04 Gy; n = 31,565) |
|
Inskip, 1997 |
1,984 Chernobyl cleanup workers |
Chernobyl |
4 to 9 yrs |
PE, US, +FNA if >1 cm |
|
|
|
Nagataki, 1994 |
1,978 adult residents of Nagasaki, Japan |
Atomic bomb |
40 yrs |
|
> 0.5 cm |
Exposed (n = 1,043); Unexposed (n = 935) |
|
Case finding studies |
||||||
|
Bruneton, 1994 |
1,000 healthy adult volunteers in France, 57% over 50 years of age, most of whom had an ENT infection within 3 months |
Unexposed |
— |
US |
> 0.3 cm |
|
|
Woestyn, 1985 |
300 healthy adults in Belgium referred for US of abdomen |
Unexposed |
— |
PE, US |
Prob > 0.3 cm |
|
|
Ezzat, 1994 |
100 healthy adult volunteers in California |
Unexposed |
— |
PE, lab, US |
FNA done if > 1 cm |
|
|
Hsaio, 1994 |
200 adults undergoing routine PE in Taiwan |
Unexposed |
— |
PE, US |
> 0.2 cm |
|
|
Author, year |
Study sample and setting |
Exposure |
Time since exposure |
Tests performed |
Definition of a nodule |
Group |
|
Horlocker, 1986 |
1,000 patients being evaluated for suspected hyperparathyroidism in Rochester, Minnesota |
Unexposed (46 had had head or neck irradiation) |
— |
PE, US |
|
continues |
|
Miki, 1993 |
451 Japanese adults at employee physical or breast CA screening |
Unexposed |
— |
|
|
|
|
Carroll, 1982 |
67 individuals undergoing carotid US |
Unexposed |
— |
US, palpation if abnormal US |
|
|
|
Clinic-based monitoring in exposed groups |
||||||
|
Ron, 1984 |
443 adult volunteers in Israel exposed to 9 rads, mostly for benign conditions |
Head and neck irradiation |
About 30 yrs |
PE, 99mTc scan if PE positive |
Palpable |
|
|
Royce, 1979 |
217 exposed adults and 243 controls in Pennsylvania |
Head and neck irradiation |
9 to 42 yrs |
Questionnaire, PE by 2 MDs, 99mTc if PE pos, surgery if + scan or nodule >1.5 cm |
Palpable |
Exposed (n = 214); Unexposed (n = 243) |
|
Favus, 1976 |
1,056 adults in Illinois |
Head and neck irradiation |
12 to 58 yrs |
Questionnaire, PE, 99mTc scan |
Pos PE or 99mTc scan |
|
|
Shimaoka, 1989 |
1,500 adults in New York |
Head and neck irradiation |
not given; in 1979 mean = 25.6 yrs |
|
|
|
|
Crom, 1997 |
96 adult volunteers in Tennessee |
Radiation therapy for childhood cancer (2-60 Gy) |
5.6 to 22.8 yrs (median = 10.6) |
Questionnaire, PE, lab studies, and US |
|
|
|
Antonelli, 1995 |
50 exposed Italian male workers compared to 100 unexposed hospital workers and 100 unexposed shipyard workers |
Occupational exposure to x-rays in hospital workers |
Duration of exposure: at least 10 yrs (mean = 22 yrs) |
Questionnaire, PE, US |
> 0.5 cm (by 2 operators); 131I scan & FNA if > 1 cm |
Exposed (n = 50); Unexposed (n = 200) |
TABLE F.3b Studies of Screening for Thyroid Neoplasms
|
|
|
|
Palpation |
|
|
|
Ultrasound |
|
|
|
|
|
Author, year |
Definition of a nodule |
Group |
Nodule p (range) |
Cancer p (range) |
Surgery n |
P(Ca/ Nodule) |
Resolution MHz |
Nodule p |
Cancer p |
Surgery n |
P(Ca/ Nodule) p |
|
Population-based studies |
|||||||||||
|
Brander 1991 |
> 0.5 cm |
|
0.05 |
0.000 |
|
0.00 |
7.5 |
0.27 |
0.000 |
0.004 |
0.00 |
|
Brander, 1989 |
> 0.5 cm |
|
|
|
|
|
7.5 |
0.17 |
|
|
|
|
Ishida 1988 |
|
|
0.04 |
0.001 |
|
0.03 |
|
|
|
|
|
|
Tunbridge 1977 |
|
|
0.03 |
|
|
|
|
|
|
|
|
|
Vander 1954, 1968 |
|
|
0.04 |
0.000 |
0.009 |
0.00 |
|
|
|
|
|
|
Kerber 1993 |
palpable |
Dose = 50- >400 mGy (n = 1418) |
0.03 (0.02-0.04) |
0.003 (0.000-0.008) |
|
0.10 |
|
|
|
|
|
|
|
|
Dose = 0-49 mGy (n = 1055) |
0.02 |
0.004 |
|
(0.00-0.27) |
|
|
|
|
|
|
Hamilton, 1987 |
>1 cm |
Most exposed islands (n = 1903) |
0.07 (0.02-0.39); solitary |
|
— |
|
|
|
|
|
|
|
|
|
|
0.03 |
|
|
|
|
|
|
|
|
|
|
|
Least exposed (2 furthest atolls; n = 370) |
0.02 |
|
— |
|
|
|
|
|
|
|
Howard, 1997 |
1 cm or 0.5 cm plus features of malignancy |
Exposed (PE n = 253; US n = 117) |
0.23 |
0.07 |
0.135 |
0.30 |
7.5 |
0.25 |
|
0.014 |
|
|
|
|
Unexposed (PE n = 227; US n = 47) |
0.06 |
0.02 |
0.033 |
0.33 |
|
0.26 |
|
|
|
|
Takahashi, 1997 |
|
BRAVO cohort (n = 815) |
0.16 |
0.02 |
|
0.06 |
7.5 |
0.33 |
|
|
|
|
|
|
EOT cohort (n = 1062) |
0.14 |
0.02 |
0.016 |
0.07 |
|
0.30 |
|
|
|
|
|
|
AT cohort (n = 216) |
0.042 |
0.02 |
0.023 |
0.17 |
|
0.12 |
|
|
|
|
|
|
|
Palpation |
|
|
|
Ultrasound |
|
|
|
|
|
Author, year |
Definition of a nodule |
Group |
Nodule p (range) |
Cancer p (range) |
Surgery n |
P(Ca/Nodule) |
Resolution MHz |
Nodule p |
Cancer p |
Surgery n |
P(Ca/ Nodule) p |
|
Mettler, 1992 |
PE: dx of 2 MDs. |
Exposed (n = 597) |
0.031 |
— |
— |
— |
7.5 |
0.08 |
|
|
|
|
|
|
Unexposed (n = 481) |
0.02 |
|
|
|
|
0.08 |
|
|
|
|
Ivanov, 1997 |
— |
1986 workers (mean dose 0.17 Gy; n = 77,663) |
|
0.000 |
|
|
|
|
|
|
|
|
|
|
1987 workers (mean dose 0.10 Gy; n = 58,694) |
|
0.000 |
|
|
|
|
0.001 |
|
|
|
|
|
1988-90 workers (mean dose 0.04 Gy; n = 31,565) |
|
0.000 |
|
|
|
|
|
|
|
|
Inskip, 1997 |
|
|
0.02 |
|
0.005 |
|
7.5 |
0.11 |
0.001 |
0.008 |
0.01 |
|
Nagataki, 1994 |
> 0.5 cm |
Exposed (n = 1,043) |
|
|
|
|
7.5 |
0.10 |
0.008 |
|
0.08 |
|
|
|
Unexposed (n = 935) |
|
|
|
|
|
0.05 |
0.001 |
|
0.02 |
|
Case finding studies |
|||||||||||
|
Bruneton, 1994 |
> 0.3 cm |
|
|
|
|
|
13 |
0.35 |
|
|
|
|
Woestyn, 1985 |
Prob > 0.3 cm |
|
|
|
|
|
5.5 |
0.19 |
0.000 |
|
|
|
Ezzat, 1994 |
FNA done if > 1 cm |
|
0.21 (0.09 solitary) |
|
|
|
10.5 |
0.67a |
|
|
|
|
Hsaio, 1994 |
> 0.2 cm |
|
|
|
|
|
7.5 |
0.16 |
|
|
|
|
Horlocker, 1986 |
|
|
0.08 |
0.009 |
0.689 |
0.113 |
10 |
0.41 |
0.013 |
0.689 |
0.032 |
|
Miki, 1993 |
|
|
0.013 |
|
|
|
10 |
0.20 |
0.002 |
0.002 |
0.01 |
|
Carroll, 1982 |
|
|
0.06 |
|
|
|
7.5 |
0.13 |
|
|
|
|
Clinic-based monitoring in exposed groups |
|||||||||||
|
Ron, 1984 |
Palpable |
|
0.05 |
0.000 |
0.019 |
0.00 |
|
|
|
|
|
|
Royce, 1979 |
Palpable |
Exposed (n = 214) |
0.06 |
0.004 |
0.028 |
0.07 |
|
|
|
|
|
|
|
|
Unexposed (n = 243) |
0.05 |
0.008 |
|
0.16 |
|
|
|
|
|
|
Favus, 1976 |
Pos PE or 99mTc scan |
|
0.13 (0.08 single) |
0.057 |
0.256 |
0.38 |
|
|
|
|
|
|
Shimaoka, 1989 |
|
|
0.34 |
0.01 |
0.057 |
0.03 |
|
|
|
|
|
groups. Mettler and co-workers (1992) found no difference in the probabilities of palpable or ultrasound-detected nodules in exposed versus unexposed population groups when highly contaminated villages near Chernobyl were compared with presumably unexposed control villages 4.5 years after the accident. In survivors of the Nagasaki atomic bomb blast, probabilities by ultrasound screening were 0.05 in unexposed groups and 0.10 in an exposed group (Nagataki et al., 1994).
Irradiation for benign medical conditions has been shown to result in an increased probability of thyroid nodules. Surveillance studies of people irradiated as children for benign conditions have found probabilities of 0.05-0.34 by palpation and 0.23-0.38 by ultrasound detection (Favus et al., 1976; Ron et al., 1984; Royce et al., 1979; Shimaoka et al., 1982). Antonelli and co-workers (1995) found a higher prevalence of nodules in hospital workers exposed to long-term, low-dosage x rays than was found in two unexposed control groups.
Nodule Size Distribution
Table F.4 shows the distribution of nodule sizes found in screening studies of exposed individuals. The information in the table can be used to estimate the additional number of nodules requiring follow-up when smaller nodules are considered to be significant.
Probability of a Thyroid Cancer Diagnosis
The yield of thyroid cancer in a screening program depends on the same factors that influence the probability of finding nodules. Moreover, the sensitivity of FNA and other test used to select patients for surgery can affect the probability
TABLE F.4 Distribution of Nodule Size in Screening Studies of Exposed Patientsa
|
Study |
Total Nodules |
<0.5 cm |
|
0.5-0.99 cm |
1.0-1.49 cm |
|
>1.5 cm |
|
Inskip, 1997 |
201 |
12.9% |
|
43.3% |
26.4% |
|
17.4% |
|
Howard, 1997 |
117 |
NA |
|
89.7% |
|
10.3% |
|
|
Mettler, 1992 |
81 |
|
30.0% |
|
|
70.0% |
|
|
Shimaoka, 1982 |
19 |
NA |
|
47.4%b |
|
52.6%c |
|
|
Schneider, 1997 |
157 |
|
74.5% |
|
|
25.5% |
|
|
NA Not available. a All studies used ultrasound except Shimaoka. b 0.5-1.0 cm. c >1.0 cm. |
|||||||
ability of finding thyroid cancer. In general, more cancers are found in radiation-exposed subjects than in the general population and in subjects screened with an ultrasound test versus those screened by palpation. The decision to evaluate small nodules also will increase the yield of cancer diagnosis in screening programs. When higher resolution ultrasound is used, still more nodules and cancers will be detected.
Unexposed Populations
In the general population, 1-5% of nodules are found to be carcinomas; the probability that a nodule is cancerous appears to be higher for larger nodules detected by palpation than for smaller nodules found by ultrasound (Ishida et al., 1988; Miki et al., 1993).
Three population-based studies examined the rates of cancer found in unexposed people (Brander et al., 1991; Ishida et al., 1988; Miki et al., 1993). In a population of healthy Japanese women, 1 per 1,000 screened by palpation had thyroid cancer (Ishida et al., 1988); in a separate study of healthy Japanese adults who underwent an ultrasound examination at a routine physical examination or at a mammography screening center, 2 per 1,000 had thyroid cancer (Miki et al., 1993). In the Framingham study, no cancers at all were detected by palpation in a population sample of 5,108 American adults (Vander et al., 1968). Screening in 253 healthy Finns by palpation and by ultrasound revealed no cancers (Brander et al., 1989).
Exposed Populations
In comparison studies, more cancers are found by palpation in exposed than in unexposed populations. The Nevada Test Site study found probabilities of cancer of 0.008 in the most-exposed group and 0.004 in the least-exposed group (Kerber et al., 1993). Howard and co-workers (1997) found more cancers in exposed Marshall Islanders than they found in a comparison group (0.07 vs. 0.02), and Takahashi and co-workers (1997) found no difference in probability in exposed and unexposed groups—both probabilities were 0.02. These results involve palpation screening only, and in the Marshall Islanders, only nodules larger than 1 cm were counted.
In a study of Chernobyl cleanup workers conducted 1-8 years after exposure, 2.8 per 1,000 patients screened by ultrasound had cancer (Ivanov et al., 1997). Ultrasound screening for nodules 0.5 cm in diameter in Nagasaki survivors revealed cancer rates of 0.10-0.05 in the exposed verses the unexposed group, respectively (Nagataki et al., 1994).
Table F.3b lists the proportion of nodules found to be cancerous in exposed and unexposed populations. The proportion of cancers is higher for exposed populations and for larger nodules. In several studies, a nodule found by screening in
exposed subjects was more likely to be malignant than was one found in an unexposed subject. In contrast to the probabilities seen in unexposed populations (0.01-0.05), nodules found in people exposed to radiation in the study of areas near the Nevada Test Site had a 0.27 probability of being malignant; in Nagasaki, this probability was 0.11 in the exposed group and 0.02 in the unexposed group. Absolute probabilities vary from study to study, but within studies a marked difference between exposed and unexposed individuals is observed consistently.
Size of Neoplasms Found Through Screening Exposed Populations
Because screening is intended to find cancers in an earlier stage than would be found in the course of usual care, the size of cancers found in a screening program is important. Early detection of thyroid cancers will improve survival only if the cancers found have a better prognosis than would have occurred if they were detected in usual care. No population-based study of individuals exposed to fallout reported this information. Only one other study, a recall program of medically irradiated people, reported sizes of thyroid cancers found (Favus et al., 1976). Of 60 cancers found by palpation and scintigraphy, 21 were under 0.5 cm, 28 were 0.6-1.5 cm, and 11 were larger than 1.5 cm. In a follow-up study of a subgroup—patients diagnosed before the start of the screening program—those with more clinically apparent symptoms had a higher risk of recurrence than did those diagnosed earlier, in the course of usual care (Schneider et al., 1986).
Stage and Histology of Cancers in Exposed Populations
No cases of undifferentiated thyroid cancer were reported in five population-based studies of exposed subjects (Howard et al., 1997; Inskip et al., 1997; Ivanov et al., 1997; Kerber et al., 1993; Takahashi et al., 1997). In a study of U.S. residents exposed to fallout radiation from the Nevada Test Site (Kerber et al., 1993), all cancers found were papillary. A study of Marshall Islanders (Takahashi et al., 1997) found 5 papillary cancers and 1 follicular cancer in exposed people. In 47 thyroid cancers detected in 167,862 Chernobyl cleanup workers (Ivanov et al., 1997), 42.8% were papillary, 33.3% were follicular, and 14.3% were other types of carcinoma. This last category is not explained further. Two cancers found in a smaller sample of Chernobyl workers (Inskip et al., 1997) were histologically confirmed to be papillary. None of these studies report information on other clinical features of the cancers found, such as lymph node involvement or distant metastasis.
Surveillance studies of medically irradiated subjects provide some information on histology of thyroid cancers found through screening. In one large series (Favus et al., 1976), all 60 thyroid cancers found in a surveillance program of patients exposed to radiation for benign conditions in childhood were papillary, follicular, or a combination of both (which would now be classified as papillary).
In 45 cases, one lobe was involved, and in 15, both lobes were. There was thyroid capsule invasion in 12 cases, blood vessel invasion in 5, and lymph node involvement in 17. No distant metastases were found. In two other surveillance studies that provide histologic information (Crom et al, 1997; Royce et al., 1979), all cancers found were papillary and follicular.
Probability of Undergoing Surgery
Unexposed Populations
Two studies of healthy, unexposed individuals provide information on surgery performed as a result of screening by palpation in unexposed populations. These results suggest that, of 1,000 unexposed people screened by palpation, between 1 and 8 will have surgery. In the United States, the Framingham study reports 45 surgical operations in 5,108 adults screened by palpation (Vander et al., 1968). None of the individuals proved to have a carcinoma. In another study of healthy Japanese workers, 1 person had surgery; 451 individuals were screened (Miki et al., 1993). This study was unusual in that the decision to proceed to FNA was made based on ultrasound diagnosis of features suggestive of cancer; as a result, very few FNAs and surgeries were performed relative to other studies.
Exposed Population
Studies of Marshall Islanders exposed to fallout radiation show much higher rates of surgery among the screened population. Hamilton and co-workers (1987) report 53 cases of surgery in 1,903 exposed Marshall Islanders screened by palpation. A decade later, in a subset of the same population, Howard and co-workers (1997) report 55 operations in 253 very highly exposed Marshall Islanders. Ten of 1,984 Chernobyl cleanup workers had surgery as a result of screening by palpation (Ivanov et al., 1997), but this study was done only a few years after the accident; continued monitoring could result in higher rates of surgery.
Recall studies of palpation screening in people who received head and neck irradiation in childhood show the highest rates of surgery among screened populations. For example, Shimaoka and co-workers (1982) report 85 operations as a result of palpation screening of 1,500 patients; Royce and co-workers (1979) report 6 in 214; Ron (1996) reports 8 in 443; Favus et al. (1976) report 195 operations in a study of 1,056 recalled patients. These surgery rates are about 10 times higher than those found as a result of screening of unexposed people.
Few data are available to estimate the false-negative rate for surgery in screening exposed populations. The rate can be estimated from information on the FNA specificity and from the ratio of surgery to cancers found in studies that report this information. In individuals exposed to fallout, approximately 1 in 3
patients undergoing surgery had cancer (Howard et al., 1997; Inskip et al., 1997). In patients who underwent external radiation for benign medical conditions, the proportion was 0.20 (Ron et al., 1984; Royce et al., 1979; Shimaoka et al., 1982).
Effectiveness of Screening
Screening in a population is justified if there is evidence that early detection and treatment before clinical symptoms are apparent will reduce mortality and morbidity or improve quality of life. Other issues to be considered include consequences of false-negative and false-positive test results, acceptability of the test to the screened population, and the risks of treatment.
There have been no randomized, controlled trials that address the question of whether screening for thyroid cancer improves patient outcomes. Because thyroid cancer is rare and has a long latency period, such trials are unlikely to be done in the future. Case-control studies can be used to judge the effectiveness of screening, but we could find no studies that evaluated screening programs using that model.
As shown in Figure F.1, stage is an important intermediate measure used in many studies as a substitute for direct evidence about mortality and morbidity. In theory screening is more likely to find a cancer that it is smaller, that has not yet metastasized, or that has metastasized less widely, than would be likely to be found without screening. In the absence of controlled studies, the only way to estimate the extent of a benefit would be to know how much earlier, compared to usual care, screening will detect cancers. In this context ''earlier" means not only at an earlier time, but also at an earlier stage as judged by size, histology, or extent of spread. The studies of screening we reviewed contained no data on which to base such estimates.
Effect of Early Detection on Mortality
Three observational studies have attempted to address prognosis with reference to mortality. These papers show that given a particular size, cell type, and extent of spread—and controlling for age—the prognosis of cancers associated with exposure to radiation appears to be similar to that of cancers that occur in unexposed individuals (Schneider et al., 1986), that in an observational study of an unexposed population, the average size of cancers found by screening was smaller than that of a comparison, unscreened group (Ishida et al., 1988), and that in a statistically controlled study, delay in treatment was associated with lower survival-rate in an unexposed cohort (Mazzaferri and Jhiang, 1994).
In the observational study, Ishida and co-workers (1988) compared sizes of thyroid cancers found through screening with those found in the course of usual care. In the screened group, made up of healthy Japanese women without exposure to radiation, 58% of palpated tumors were 2 cm or smaller. The comparison group consisted of outpatients at a thyroid cancer clinic. In the clinic patients
there were fewer cancers under 2 cm, and more tumors larger than 4 cm. In the screened group, all but 1 of 216 thyroid cancers were differentiated, and 85.5% were papillary. In the comparison group of 229 patients with thyroid cancer, 70.3% of the cancers were papillary, and there were 9 (3.9%) undifferentiated carcinomas. After 1.5-8 years of follow-up, 96.7% of screened patients were disease-free, compared with 85.6% in the comparison group. None of the screened patients died of thyroid cancer, but 12 patients (5.4%) in the clinic group did.
Flaws in the selection of the comparison group limit the usefulness of the article (Ishida et al., 1988). It is not clear whether the clinic patients had already been followed for many years. It appears that the investigators reported the sizes of the cancers in the clinic patients at the time of the study, rather than at the time of diagnosis, which could have been years earlier. The mean age of the clinic patients is given, but it is not clear whether the age distribution was similar in the screened group. Finally, the investigators apparently did not study whether cancers or cancer deaths occurred in screened individuals who were not diagnosed to have cancer on the initial and second screenings. Undifferentiated cancers that developed later in screened patients could have been excluded from the "screened" groups and, in fact, might even have been included in the "clinic" group. These flaws make comparison of tumor sizes and follow-up mortality meaningless.
In the statistically controlled study of a cohort of patients under the care of U.S. Air Force physicians, Mazzaferri and Jhiang (1994) record the time from the first manifestation of cancer to initial therapy. Patients who died of cancer had a median delay of 18 months, compared with 4 months for those who survived 30 years. A simple linear regression of the logarithm of delay in treatment on cancer death had a correlation coefficient of 0.49. The results suggest that a delay of 1 year increased the probability of dying of cancer by about 5 percentage points (from nearly 0 to 5%); a delay of 10 years instead of 1 year increased the probability of dying of cancer from 5% to approximately 12%.
What is the relevance of these findings to screening? First, the average tumor size was 2.5 cm, and the prognosis was inversely related to the size of the nodule at the time of diagnosis. Although the study did not directly estimate the rate of growth of untreated cancerous nodules, it stands to reason that earlier detection of these very large tumors could improve the outcome.
Second, the study documents that, in practice, treatment often was delayed for many years. The reasons are not made clear, and may have occurred after a clinical diagnosis was made. Long delays, followed by a poor outcome, could have been the result of the presence of malignant nodules that were inadvertently managed conservatively for many years, perhaps because an accurate diagnosis was not made initially. In any case, this finding argues (as the authors conclude) for more aggressive initial management of large nodules, once they are diagnosed, but it does not necessarily mean that diagnosing these nodules earlier than was done with usual care would substantially improve outcomes.
Third, the benefit of early detection was apparent only in patients with large nodules, and it should not be overgeneralized to patients with occult nodules or even smaller palpable nodules. If true, this finding suggests that screening be focused on finding large (>1.5 cm), potentially palpable, but clinically unsuspected nodules.
Effect of Screening on Morbidity
Stage at the time of detection, recurrence of cancer, and complications of surgery can affect morbidity (Figure F.1). There are no data from studies of screening about the effect of early detection on recurrence rates or on the frequency of surgical complications in the screened population.
Recurrence of Cancer
We found no studies that directly compare rates of recurrence in screened versus unscreened populations. Most screening studies involve one-time screening and do not follow patients over time for evidence of recurrence or other outcomes. One follow-up study of surveillance for thyroid cancer in patients exposed to external beam radiation for benign conditions of the head, neck, and thorax (Schneider et al., 1986) reports a lower recurrence rate in patients diagnosed after a screening program was begun compared with those diagnosed through usual care—reflecting factors such as smaller tumor size in cancers discovered through screening.
Factors associated with risk of recurrence, such as age at diagnosis (Krausz et al., 1993; Mazzaferri and Jhiang, 1994; Schindler et al., 1991; Schneider et al., 1986; Simpson, 1987; Tubiana et al., 1985), tumor size (Mazzaferri and Jhiang, 1994; Noguchi, 1995; Simpson, 1987; Schindler et al., 1991; Schneider et al., 1986), male sex (Noguchi et al., 1995; Schindler et al., 1991; Tubiana et al., 1985), and local invasion or metastases (Mazzaferri and Jhiang, 1994; Simpson et al., 1987; Schneider et al., 1986; Schindler et al., 1991; Simpson et al., 1987; Tubiana et al., 1985), are generally the same as those associated with increased mortality. Follow-up studies of thyroid cancer patients report recurrence rates of about 10-30%. About two-thirds of recurrences come within 10 years of initial diagnosis, but recurrence can occur throughout a patient's lifetime.
A thyroid cancer recurrence does not necessarily mean increased mortality (Krausz et al., 1993). Cure rates remain high even for recurrences, except for patients who have metastases at the time of recurrence (Mazzaferri and Jhiang, 1994). Few studies relate factors at initial diagnosis to mortality at recurrence, but those that do find survival of a recurrence affected most strongly by age. A Japanese study (Noguchi et al., 1995) with follow-up periods of 10-30 years examined risk factors in patients who died after recurrence with patients who survived
a recurrence. Only age at initial diagnosis correlated with survival of a recurrence. Similarly, an Israeli study (Krausz et al., 1993) found only that age at initial diagnosis was a significant risk factor for mortality after recurrence. Another study of Japanese patients (Asakawa et al., 1997) found increased mortality of recurrent thyroid cancers to be associated with age at diagnosis and shorter period between initial diagnosis and recurrence. Tumor size and spread at initial diagnosis do not appear to be associated with mortality from recurrence.
Even though recurrent thyroid cancers are usually highly curable, Mazzaferri (1987) makes the point that a recurrence, even when cured, is never an insignificant event for the patient, in terms of psychological costs and quality of life.
Harms of Screening
Uncertainty about effectiveness is of particular concern when significant harms are associated with screening. Almost no information about quality of life or morbidity related to the diagnosis and treatment of thyroid cancer has been published. In general, false-positive test results can cause anxiety. Hypothyroidism, caused by thyroid ablation and treatment for hypothyroidism, unexpected complications of surgery or radioiodine therapy, and even preparation for tests used to find recurrences (Dow et al., 1997a,b), can cause morbidity and affect the quality of life of patients with thyroid cancer, but the consequences of most of these events and conditions have not been systematically studied.
The long-term complications of thyroid surgery are hypocalcemia, a serious, difficult-to-treat condition due attendant to hypoparathyroidism; and hoarseness, due to injury to the recurrent laryngeal nerve. The frequency of these complications depends on the extent of the procedure and the experience of the surgeon. Complication rates vary among centers (Fraker et al., 1997). For the most extensive procedure, total thyroidectomy, the risk of hypocalcemia range from 7% to 32% in four surgical series with long-term follow-up (Fraker et al., 1997). In the same study the risk of recurrent laryngeal nerve injury ranged from 0% to 7%. The study reported the experience of highly skilled surgeons at major centers. Major surgery of the thyroid is generally considered difficult, and results of experienced surgeons are thought to be much better than the "average" results of surgeons who perform thyroid surgery only occasionally. Less extensive surgery, such as "near total" and subtotal thyroidectomy, causes fewer complications, but may be associated with higher rates of tumor recurrence and mortality.
Summary
Table F.5 summarizes the findings of our review. The table shows estimates of relevant probabilities and of the number of significant events per 10,000 individuals screened. Many of the estimates, such as those for test performance and
TABLE F.5 Summary of Evidence Regarding the Benefits of Screening for Thyroid Cancer
|
|
Probability |
Palpation |
Ultrasound |
References |
|
Probability of having a nodule |
|
|
|
|
|
Any size nodule |
0.35 |
|
|
|
|
0.5-1.0 cm |
0.12 |
|
|
|
|
1.0-1.5 cm |
0.05 |
|
|
|
|
>1.5 cm |
0.02 |
|
|
|
|
Probability that a nodule is cancer |
|
|
|
|
|
nodules smaller than 1 cm |
0.03 |
|
|
|
|
nodules larger than 1 cm |
0.10 |
|
|
|
|
Cut-off for a significant nodule |
|
1.0 cm |
0.5 cm |
|
|
Probability of cancer given cut-off |
|
0.0007 |
0.011 |
|
|
Sensitivity for nodules |
|
|
|
|
|
0.5-1.0 cm |
|
0.00 |
1 |
|
|
1.0-1.5 cm |
|
0.55 |
1 |
|
|
>1.5 cm |
|
0.65 |
1 |
|
|
Specificity for nodules |
|
|
|
|
|
0.5-1.0 cm |
|
|
0.98 |
|
|
1.0-1.5 cm |
|
0.98 |
0.99 |
|
|
>1.5 cm |
|
0.98 |
1.00 |
|
|
Fine needle aspiration (FNA) |
|
|
|
|
|
Sensitivity for cancer |
0.8 |
|
|
|
|
False positive rate |
0.35 |
|
|
|
|
Lobectomy or subtotal thyroidectomy |
|
|
|
Fraker et al. |
|
Complication (recurrent laryngeal nerve injury) |
0.0005 |
|
|
|
|
Complication (hypocalcemia) |
0.0005 |
|
|
|
|
Total thyroidectomy |
|
|
|
Fraker et al. |
|
Complication (recurrent laryngeal nerve injury) |
0.04 |
|
|
|
|
Complication (hypocalcemia) |
0.1 |
|
|
|
|
Morbidity and mortality prevented by screening |
|
— |
— |
No data |
|
Summary |
|
|
|
|
|
Events per 10,000 screened |
|
|
|
|
|
Diagnosed to have a nodule (true positives) |
|
405 |
1900 |
|
|
Diagnosed to have a nodule (false positives) |
|
386 |
271 |
|
|
Undergo at least one FNA |
|
791 |
2171 |
|
|
Undergo FNA but do not have cancer |
|
751 |
2076 |
|
|
Undergo lobectomy |
|
102 |
696 |
|
|
Cancers diagnosed |
|
32 |
85 |
|
|
Cancers missed |
|
38 |
35 |
|
|
Surgical complications |
|
5 |
13 |
|
|
Death prevented in 5 years |
|
No data |
No data |
|
surgical complication rates, are derived from studies performed in specialized settings that are not likely to be representative of the results of a program of screening in the general population.
Data were insufficient to estimate the effect of screening on mortality or morbidity from thyroid cancer and from recurrences of thyroid cancer. The information needed to make such a determination involves detailing survival rates by risk category among patients found to have cancer during the course of usual care and estimating the effect of early detection on the distribution cancers among people according to category.
As shown in Table F.6a, the SEER study provides estimates of 5-year survival by sex and by the extent of spread (localized, regional, or distant) found among cancers diagnosed in usual care. It also provides estimates of the proportion of cancers found in each risk category. These data can be used to estimate overall survival for males and females with thyroid cancer found in the general population. Although the SEER data provide incomplete information about risk (there are no data by histologic type, for example), these are the only population-based data available about the distribution through risk categories of cancers found during usual care.
To determine whether early detection improves outcome, it would be necessary to estimate how often cancers are detected earlier, and how much earlier they are detected. Specifically, it would be necessary to know the average delay in diagnosis through usual care compared with that from screening and the rates of growth or spread of the cancers between the time they would be found by screening and the time they would be found in the usual course of care.
Table F.6b shows data elements—but not actual data—in one possible causal chain linking earlier diagnosis to improved survival. The improvement in survival could be estimated if we knew the distribution of tumor sizes in the usual-care population and in a screened population; the average duration of delay in diagnosis in usual care, relative to screening; the rate at which tumors in one size category progress to a larger size category; and the relationship between the size of the cancer and the likelihood that the cancer is localized. Because data about these variables are lacking—studies of screening have not demonstrated to what degree the cancers found by screening have a better prognosis—we could not make a reliable estimate of the benefits of screening.
How large is such a benefit likely to be? Table F.6c depicts a hypothetical example showing the potential relationship between earlier detection and 5-year survival for adult females. As shown in Table 6a, in the general population 60% of thyroid cancers were localized at the time of detection; 31% had spread to regional nodes. If screening increased the proportion of cancers that had no regional or distant metastases from 60% to 70%, the overall 5-year survival for thyroid cancer would increase from 0.947 to 0.952. Put differently, 184 people with thyroid cancer would need to be treated to prevent 1 death in 5 years. As seen in Table F.5, 32 cancers would be found per 10,000 people screened. Therefore,
TABLE F.6 Hypothetical Relationship Between Efficacy of Early Detection and Five-Year Survival from Thyroid Cancer
|
a. SEER data |
||||||
|
|
Five-year survival |
Proportion of cancers in each risk category |
Overall Survival |
|||
|
Risk categories |
Total |
Males |
Females |
|
Males |
Females |
|
localized |
0.997 |
0.994 |
0.998 |
0.60 |
0.596 |
0.599 |
|
regional |
0.937 |
0.913 |
0.947 |
0.31 |
0.283 |
0.294 |
|
distant |
0.448 |
0.403 |
0.475 |
0.05 |
0.020 |
0.024 |
|
unstaged |
0.766 |
0.773 |
0.761 |
0.04 |
0.031 |
0.030 |
|
5 year and overall survival |
|
|
|
0.931 |
0.947 |
|
|
b. Consequences of screening (categories of information needed to estimate effect of screening on detection of disease by stage) |
|
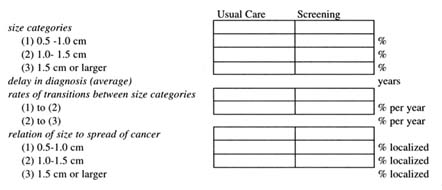 |
|
c. Hypothetical improvement in survival in relation to risk categories if screening increased proportion of cancers with no metastases from 60% to 70% compared to usual care (adult females only) |
|||
|
|
Usual Care |
Screening |
|
|
Risk categories |
|||
|
localized |
0.6 |
0.7 |
|
|
regional |
0.31 |
0.21 |
|
|
distant |
0.05 |
0.05 |
|
|
unstaged |
0.04 |
0.04 |
|
|
Contribution to 5 year survival |
0.947 |
0.952 |
|
|
Number needed to treat to prevent 1 death in 5 years |
|
184 |
|
|
Number needed to screen to prevent 1 death in 5 years |
|
57,445 |
|
1 death would be prevented for every 57,445 individuals screened. Screening 57,000 individuals could also result in 26 surgical complications (Table F.5). The implication is that, in the future, studies of screening should attempt to clearly document the stages at which cancers are detected, and an appropriate comparison group should be identified to determine whether screening is beneficial.
References
Antonelli A, Silvano G, et al. 1995. Risk of thyroid nodules in subjects occupationally exposed to radiation: a cross sectional study [see comments]. Occupational & Environmental Medicine, 52(8):500-504.
Asakawa H, Kobayashi T, et al. 1997. Prognostic factors in patients with recurrent differentiated thyroid carcinoma. Journal of Surgical Oncology 64(3):202-206.
Ashcraft MW, Van Herle AJ. 1981. Management of thyroid nodules. II: Scanning techniques, thyroid suppressive therapy, and fine needle aspiration. Head & Neck Surgery 3(4):297-322.
Bouvet M, Feldman IJ, et al. 1992. Surgical management of the thyroid nodule: patient selection based on the results of fine-needle aspiration cytology. Laryngoscope 102(12 Pt 1):1353-6.
Brander A, Viikinkoski P, Nickels J, Kivisaari L. 1989. Thyroid gland: US screening in middle-aged women with no previous thyroid disease. Radiology, 173(2):507-510.
Brander A, Viikinkoski P, Nickels J, Kivisaari L. 1991. Thyroid gland: US screening in a random adult population. Radiology, 181(3):683-687.
Brander A, Viikinkoski P, Tuuhea J, Voutilainen L, Kivisaari L. 1992. Clinical versus ultrasound examination of the thyroid gland in common clinical practice. Journal of Clinical Ultrasound, 20(1):37-42.
Bruneton J, Balu-Maestro C, Marcy P, Melia P, Mourou M. 1994. Very high frequency (13 Mhz) ultrasonographic examination of the normal neck: detection of normal lymph nodes and thyroid nodules, Journal of Ultrasound Medicine 13:87-90.
Carroll, BA. 1982. Asymptomatic thyroid nodules: incidental sonographic detection. American Journal of Roentgenology 138(3):499-501.
Caruso, D, Mazzaferri E L. 1991. Fine needle aspiration biopsy in the management of thyroid nodules. The Endocrinologist 1:194-202.
Crom D B, Kaste SC, et al. 1997. Ultrasonography for thyroid screening after head and neck irradiation in childhood cancer survivors. Medical & Pediatric Oncology 28(1):15-21.
Cusick EL, MacIntosh CA, et al. 1990. Management of isolated thyroid swellings: a prospective six year study of fine needle aspiration cytology in diagnosis. British Medical Journal 301(6747):318-21.
Dow KH, Ferrell BR, AnelloC. 1997a. Balancing demands of cancer surveillance among survivors of thyroid cancer. Cancer Pract., 5(5):289-95.
Dow KH, Ferrell BR, Anello C. 1997b. Quality-of-life changes in patients with thyroid cancer after withdrawal of thyroid hormone therapy. Thyroid., 7(4):613-69.
Eddy D 1991. "How to think about screening," in Eddy, D. ed, Common Screening Tests. Philadelphia: American College of Physicians, pp. 1-10.
Ezzat S, Sarti DA, Cain DR, Braunstein GD. 1994. Thyroid incidentalomas. Prevalence by palpation and ultrasonography. Archives of Internal Medicine, 154(16):1838-1840.
Favus MJ, Schneider AB, et al. 1976. Thyroid cancer occurring as a late consequence of head-and-neck irradiation. Evaluation of 1056 patients. N Engl J Med, 294(19):1019-1025.
Fraker DL, Skarulis M, Livolsi V. 1997. Thyroid Tumors. In DeVita, Jr., VT, Hellman, S, Rosenberg, SA., eds. Cancer: principles and practice of oncology. Philadelphia: Lippincott-Raven, pp. 1629-1652.
Gharib H. 1994. Fine-needle aspiration biopsy of thyroid nodules: advantages, limitations, and effect. Mayo Clinic Proceedings, 69(1):44-49.
Gharib H, Goellner JR. 1993. Fine-needle aspiration biopsy of the thyroid: an appraisal. Annals of Internal Medicine, 118(4):282-289.
Giuffrida D, Gharib H. 1995. Controversies in the management of cold, hot, and occult thyroid nodules. American Journal of Medicine, 99(6):642-650.
Haas S, Trujillo A, et al. 1993. Fine needle aspiration of thyroid nodules in a rural setting. American Journal of Medicine 94(4):357-61.
Hall TL, Layfield LJ, Philippe A, Rosenthal DL. 1989. Sources of diagnostic error in fine needle aspiration of the thyroid. Cancer, 63(4):718-725.
Hamburger JI, Hamburger SW. 1985. Declining role of frozen section in surgical planning for thyroid nodules. Surgery 98(2):307-12.
Hamilton TE, van Belle G, LoGerfo JP. 1987. Thyroid neoplasia in Marshall Islanders exposed to nuclear fallout. Jama, 258(5):629-635.
Holleman F, Hoekstra JB, et al. 1995. Evaluation of fine needle aspiration (FNA) cytology in the diagnosis of thyroid nodules. Cytopathology 6(3):168-75.
Horlocker TT, Hay JE, et al. 1986. Prevalence of incidental nodular thyroid disease detected during high-resolution parathyroid ultrasonography. In Medeiros-Neto J, Gaitan E (eds.), Frontiers in Thyroidology. Vol. II. Plenum Publishing Corp. pp. 1309-1312.
Howard JE, Vaswani A, Heotis P. 1997. Thyroid disease among the Rongelap and Utirik population—an update. Health Physics, 73(1):190-198.
Hsiao YL, Chang TC. 1994. Ultrasound evaluation of thyroid abnormalities and volume in Chinese adults without palpable thyroid glands. Journal of the Formosan Medical Association, 93(2):140-144.
Inskip PD, Hartshorne MF, et al. 1997. Thyroid nodularity and cancer among Chernobyl cleanup workers from Estonia. Radiation Research 147(2):225-35.
Ishida T, Izuo M, Ogawa T, Kurebayashi J, Satoh K. 1988. Evaluation of mass screening for thyroid cancer. Japanese Journal of Clinical Oncology, 18(4):289-295.
Ivanov VK, Tsyb AF, et al. 1997. Leukaemia and thyroid cancer in emergency workers of the Chernobyl accident: estimation of radiation risks (1986-1995). Radiation & Environmental Biophysics 36(1): 9-16.
Jones AJ, Aitman TJ, et al. 1990. Comparison of fine needle aspiration cytology, radioisotopic and ultrasound scanning in the management of thyroid nodules. Postgrad Med J, 66(781):914-917.
Kerber RA, Till JE, Simon SL, et al. 1993. A cohort study of thyroid disease in relation to fallout from nuclear weapons testing. JAMA 270(17):2076-2082.
Khafagi F, Wright G, et al. 1988. Screening for thyroid malignancy: the role of fine-needle biopsy. Medical Journal of Australia 149(6):302-3, 306-7.
Krausz Y, Uziely B, et al. 1993. Recurrence-associated mortality in patients with differentiated thyroid carcinoma. Journal of Surgical Onocology 52(3):154-8.
Kuma K, Matsuzuka F, Yokozawa T, Miyauchi A, Sugawara M. 1994. Fate of untreated benign thyroid nodules: results of long-term follow-up. World J Surg. 18:495-8. Cited in Tan and Gharib, 1997.
Landis SH, Murray T, Bolden S, Wingo PA. 1998. Cancer statistics, 1998. CA Cancer J Clin, 48(1):6-29.
Lin JD, Huang BY, et al. 1997. Thyroid ultrasonography with fine-needle aspiration cytology for the diagnosis of thyroid cancer. Journal of Clinical Ultrasound 25(3):111-8.
Mazzaferri EL. 1987. Papillary thyroid carcinoma factors influencing prognosis and current therapy [published erratum appears in Semin Oncol 1988 Jun; 15(3):X]. Seminars in Oncology 14(3):315-32.
Mazzaferri EL, Jhiang SM. 1994. Long-term impact of initial surgical and medical therapy on papillary and follicular thyroid cancer. [see comments] [published erratum appears in Am J Med 1995 Feb. 98(2):215]. American Journal of Medicine 97(5):418-28.
McTiernan AM, Weiss NS, Daling JR. 1984. Incidence of thyroid cancer in women in relation to previous exposure to radiation therapy and history of thyroid disease. J Natl Cancer Inst, 73(3):575-581.
Merchant WJ, Thomas SM, et al. 1995. The role of thyroid fine needle aspiration (FNA) cytology in a District General Hospital setting. Cytopathology 6(6):409-18.
Mettler FA, Williamson MR, et al. 1992. Thyroid nodules in the population living around Chernobyl. JAMA 268(5):616-9.
Miki H, Oshimo K, et al. 1993. Incidence of ultrasonographically-detected thyroid nodules in healthy adults. Tokushima Journal of Experimental Medicine, 40(1-2):43-46.
Moosa M, Mazzaferri EL. 1997. Occult thyroid carcinoma. The Cancer Journal, 10, 180-188.
Morayati SJ, Freitas JE. 1991. Guiding thyroid nodule management by fine-needle aspiration. Family Practice Research Journal 11(4):379-86.
Nagataki S. Shibata Y, et al. 1994. Thyroid diseases among atomic bomb survivors in Nagasaki [published erratum appears in JAMA 1995 Jan 25;273(4):288]. JAMA 272(5): 64-70.
Ng EH, Tan SK, et al. 1990. Impact of fine needle aspiration cytology on the management of solitary thyroid nodules. Australian & New Zealand Journal of Surgery 60(6):463-6.
Noguchi M, Yagi H, et al. 1995. Recurrence and mortality in patients with differentiated thyroid carcinoma. International Surgery 80(2):162-6.
Ongphiphadhanakul B, Rajatanavin R, et al. 1992. Systematic inclusion of clinical and laboratory data improves diagnostic accuracy of fine-needle aspiration biopsy in solitary thyroid nodules. Acta Endocrinological 126(3):233-7.
Piromalli D, Martelli G, et al. 1992. The role of fine needle aspiration in the diagnosis of thyroid nodules: analysis of 795 consecutive cases. Journal of Surgical Oncology 50(4):247-50.
Pottern LM, Kaplan MM, et al. 1990. Thyroid nodularity after childhood irradiation for lymphoid hyperplasia: a comparison of questionnaire and clinical findings. Journal of Clinical Epidemiology, 43(5):449-460.
Ries LAG, Kosary CL, et al. eds. 1997. SEER Cancer Statistics Review, 1973-1994, National Cancer Institute. NIH Pub. No. 97-2789. Bethesda, MD.
Ron E 1996. Thyroid Cancer. In Shottenfeld, D., Fraumeni, Jr., JF, eds. Cancer Epidemiology and Prevention. 2nd Edition. New York: Oxford University Press, pp. 1000-1021.
Ron E, Lubin E, Modan B. 1984. Screening for early detection of radiation-associated thyroid cancer: a pilot study. Israel Journal of Medical Sciences, 20(12):1164-1168.
Ron E, Kleinerman RA, et al. 1987. A population-based case-control study of thyroid cancer. J Natl Cancer Inst, 79(1):1-12.
Ron E, Modan B, Boice JDJ. 1988. Mortality after radiotherapy for ringworm of the scalp. Am J Epidemiol, 127(4):713-725.
Ron E, Modan B, et al. 1989. Thyroid neoplasia following low-dose radiation in childhood. Radiation Research, 120(3):516-531.
Ron E, Lubin JH, et al. 1995. Thyroid cancer after exposure to external radiation: a pooled analysis of seven studies. Radiation Research, 141(3):259-277.
Ron E, Saftlas AF. 1996. Head and neck radiation carcinogenesis: epidemiologic evidence . Otolaryngology—Head & Neck Surgery, 115(5):403-408.
Royce PC, MacKay BR, et al. 1979. Value of postirradiation screening for thyroid nodules. A controlled study of recalled patients. JAMA 242(24):2675-8.
Schindler AM, van Melle G, et al. 1991. Prognostic factors in papillary carcinoma of the thyroid. Cancer 68(2):234-30.
Schlumberger MJ. 1998. Papillary and follicular thyroid carcinoma. NEJM 338:297-306.
Schneider AB, Recant W, et al. 1986. Radiation-induced thyroid carcinoma. Clinical course and results of therapy in 296 patients. Annals of Internal medicine 105(3):405-412.
Schneider AB, Ron E, Lubin J, Stovall M, Gierlowski TC. 1993. Dose-response relationships for radiation-induced thyroid cancer and thyroid nodules: evidence for the prolonged effects of radiation on the thyroid. Journal of Clinical Endocrinology & Metabolism 77(2):362-369.
Schneider AB, Bekerman C, Leland J. 1997. Thyroid nodules in the follow-up of irradiated individuals: comparison of thyroid ultrasound with scanning and palpation. J Clin Endoc Metab 82:4020-4027.
Shimaoka K, Bakri K, et al. 1982. Thyroid screening program; follow-up evaluation. New York State Journal of Medicine, 82(8):1184-1187.
Shore, R. E., Hildreth, N., et al. (1993). Thyroid cancer among persons given X-ray treatment in infancy for an enlarged thymus gland. American Journal of Epidemiology, 137(10):1068-1080.
Shore RE. 1992. Issues and epidemiological evidence regarding radiation-induced thyroid cancer. Radiation Research 1312(1):98-111.
Shore RE, Hildreth N, et al. 1993. Thyroid cancer among persons given X-ray treatment in infancy for enlarged thymus gland. American Journal of Epidemiology, 137(10):1068-1080.
Simpson WJ, McKinney SE, et al. 1987. Papillary and follicular thyroid cancer. Prognostic factors in 1,578 patients. American Journal of Medicine 83(3):479-88.
Spiliotis J, Scopa CD, et al. 1991. Diagnosis of thyroid cancer in southwestern Greece. Bulletin du Cancer 78(10):953-9.
Takahashi T, Trott KR, et al. 1997. An investigation into the prevalence of thyroid disease on Kwajalein Atoll, Marshall Islands. Health Physics 73(1):199-213.
Takashima S, Fukuda H, et al. 1994. Thyroid nodules: clinical effect of ultrasound-guided fine-needle aspiration biopsy. Journal of Clinical Ultrasound 22(9):535-42.
Tan GH, Gharib H, Reading CC. 1995. Solitary thyroid nodule. Comparison between palpation and ultrasonography. Archives of Internal Medicine, 155(22):2418-2423.
Tan GH, Gharib H. 1997. Thyroid incidentalomas: management approaches to nonpalpable nodules discovered incidentally on thyroid imaging. Annals of Internal Medicine, 126(3):226-231.
Tubiana M, Schlumberger M, et al. 1985. Long-term results and prognostic factors in patients with differentiated thyroid carcinoma. Cancer 55(4):794-804.
Tucker MA, Jones PH, et al. 1991. Therapeutic radiation at a young age is linked to secondary thyroid cancer. The Late Effects Study Group. Cancer Research, 51(11):2885-2888.
Tunbridge WM, Evered DC, et al. 1977. The spectrum of thyroid disease in a community: the Whickham survey. Clinical Endocrinology, 7(6):481-493.
USDHHS (U. S. Department of Health and Human Services, National Cancer Institute). 1997. Estimated exposures and thyroid doses received by the American people from iodine-131 in fallout following Nevada atmospheric nuclear bomb test. NIH Pub. 97-4264.
Vander JB, Gaston EA, Dawber TR. 1954. The significance of nontoxic thyroid nodules. Preliminary report. New England Journal of Medicine 251(24):970-973.
Vander JB, Gaston EA, Dawber TR. 1968. The significance of nontoxic thyroid nodules. Final report of a 15-year study of the incidence of thyroid malignancy. Annals of Internal Medicine, 69(3):537-540.
Watters DA, Ahuja AT, et al. 1992. Role of ultrasound in the management of thyroid nodules. American Journal of Surgery 164(6):654-7.
Wingo PA, Tong T, et al. 1995. Cancer statistics, 1995 [published erratum appears in CA Cancer J Clin 1995 Mar-Apr; 45(2):127-8]. CA: a Cancer Journal for Clinicians 45(1):8-30.
Woestyn J, Afschrift M, Schelstraete K, Vermeulen A. 1985. Demonstration of nodules in the normal thyroid by echography. British Journal of Radiology 58(696):1179-1182.











































