5
The Use of Functional Capacity Measures in Public and Private Programs in the United States and in Other Countries
The key issues for discussion for this panel include:
-
What has been the experience of other programs in the use of functional capacity measures in determining disability?
-
What aspects of their measurements of functional capacity might be relevant for the Social Security Administration's (SSA) needs?
Patricia Owens, M.P.A.
President, Integrated Disability Management, UNUM America
Functional evaluation is presently used in the determination of disability by the SSA. It is used when the severity of a medical impairment in itself is insufficient to allow or deny a disability claim. Proposals under consideration would give functional evaluation a larger role in the disability decisionmaking process.
As used in this context, functional evaluation is a process that estimates the ability of an impaired person to perform work. For example, measures may be made of the person's ability to bend, stand, lift, perform repetitive tasks, concentrate, and produce specific numbers of outputs in given time-frames. The results of these evaluations are then compared to specified functional demands or requirements of jobs, a person's own or others for which they have the required qualifications.
In considering the use and content of functional evaluations, four issues were raised:
-
Functional evaluations may not give sufficient consideration to the personal and heterogeneous nature of disability—same impairment, different person, different disability. More personal discussions, therefore, within a set of very specific guidelines may be an important component in functional evaluation. The person's own view of himself or herself in relationship to the requirements of work are important.
-
Assessments of function are best made by people trained in their conduct as well as knowledgeable about how assessments are used in a disability decision process. Various types of functional evaluation techniques are available, although they differ by type of impairment. However the results are provided, it is important to take motivation into account.
-
Functional evaluations in SSA are done at a moment in time. A static condition is implied. While often impairments are chronic and progressive, improvement in function or adaptation to functional loss over time frequently occurs.
-
Environmental or contextual factors influencing work disability need systematic consideration. There is room in the Social Security programs to take environmental factors into consideration, but the question is how to bring these factors into the process in a systematic manner.
These issues were then described from the perspective of evolving private sector approaches for disability management over time, as distinct from making decisions at a point in time.
Centrality of functional capacity in the disability determination process: A functional capacity assessment is an integral part of work disability decisionmaking in the private sector. Functional capacity limitations, or more properly remaining capacity, arising from physical or mental impairments when compared to functional demands of work, drives private disability decisionmaking within the contractual definition of work disability. A worker's capacity, limitations, and restrictions are all relevant to the initial disability determination.
Ask the person—self-reporting: Who knows better how to describe their function than the person? What people say about themselves and how they feel about their own limitations is a very important part of whether or not they can do work. There is always the worry about the validity of the information and how to validate it. The right questions must be asked. Self-reporting questionnaires must produce valid and reliable information to be used in deciding disability. When the person evaluating function understands the limitations as described by the person, he or she gets sharper insights into ways to remove factors contributing to these limitations, in other words, how to work with the person to manage disability, not just pay a claim.
The assessment and assessors: The assessment of functional capacity in its simplest form asks a physician or other health care professional to estimate the degree of functional loss produced by a medically determinable physical or mental impairment. Conversely, assessors are asked to estimate the degree of remaining capacity. Increasingly, the health care community is being asked to estimate a person's functional capacity in relationship to concrete demands of work and the work environment. For example, how does a respiratory impairment influence climbing a ladder in an environment with high humidity? The health care professionals' role in the functional evaluation process is increasingly important. Clearly, they need to be trained in functional evaluation and, when asked, most want to learn how to make a meaningful evaluation.
Claims payers use the medical functional assessments in comparison to assessments of functional requirements of a job or occupation. These latter evaluations of work demands are increasingly purchased from professionals who look at a person's assessed functional capacity and search for jobs they could do. Job evaluators may also suggest how work requirements can be modified to fit with estimated capacity.
Functional evaluation and assessment is a growing industry, although most often it is still the primary care physician, untrained in disability decisionmaking, who is asked to provide the evaluation. Physicians and others who specialize in functional evaluations use a battery of tests and employ various forms of technological wizardry. The costs of these specialized objective tests range from a standard $500 to much more. Professional job evaluators, whose prices vary, are also readily available.
Disability as a Trajectory Over Time—Disability Management: Disability is not a static event because it is more than a medical condition. It is the adaptation to that medical condition in the environment in which one lives. Therefore, all the factors such as functional limitation, assistive devices to increase function, motivation, and availability of work in the economy, come into consideration. Improvement in work capacity over time becomes an important consideration. Therefore, it is often not enough to establish an inability to work based on a measure of functional capacity at a frozen moment in time.
A case plan that contemplates management over time is essential. This plan should be based on whether and when recovery of function is likely. The plan should also consider when and how accommodation for remaining functional loss could be made. Estimates of both maximum medical and functional recovery are important aspects of a disability management process. These estimates must be made in consideration of pharmacological, surgical, and other interventions that can have dramatic effects on impairment and function. A disability management process provides for functional assessments over time.
Disability management over time is not now done in SSA. SSA is in the business of making disability decisions. Continuing disability reviews (CDR) regularly
and properly planned and conducted in conjunction with the initial disability decision could be an important move to disability management for the SSA. CDRs are currently required and are being undertaken, but perhaps not sufficiently. However, even the CDRs are evaluations at a point in time and not an evaluation of future course. At the present time, after the decision, ''you are disabled,'' a person generally gets lost in the system. Ongoing communication based upon the degree of impairment, recovery, rehabilitation potential, age, and other similar variables, means that functional evaluation and disability decisionmaking is a process, not a one-time event.
Environmental factors (context) such as a person's family, workplace, employers, other employees, community, and transportation influence function and therefore must be taken into consideration. There is room to do that within the current law the way it is written through regulations. Not only are a caregiver and a claim processor important to functional evaluation, as indicated earlier, so are the persons with disabilities. From this perspective, the use of functional assessments can be something very different—a part of the whole.
The workplace: Employers have significant influence on disability; they provide context. Removing barriers, providing transitional work, and job transfers all affect whether persons with functional limitations can or cannot work. Medical limitations are assessed in relationship to work demands. If work demands change, so do limitations. In the private sector a substantial effort is made to include employers in disability management. Employers increasingly understand the bottom-line impact of employee disability.
Place and type of work: The nature and availability of jobs in relation to the number of workers has an enormous effect on the use of functional evaluations. Function needs to be assessed in relation to available work and technology. The increasing numbers of jobs that can be performed in a person's home add new dimensions to matching functional capacity with work demands.
In closing, it is important to emphasize that how to develop the best functional evaluations and when and how to use them in deciding work disability are important questions, but answering these questions alone is only a small step. In fact, a wholesale rush to functional evaluation may in fact bring new problems. If work disability is addressed from the personal civil rights perspective, the issues are quite different. We would be more concerned about mitigating functional limitations by removing barriers through reasonable accommodation.
Motivational issues are not readily solved by functional evaluation, although many professional evaluators say that their tests can detect motivational levels. Motivation continues to be a conundrum. In considering psychiatric disability, depression, for example, is often described as limiting the will to work.
Physicians consistently say they are not trained to do functional assessments and do not understand how disability decisions are made. This problem extends to other assessors as well. How can we see to this training?
The person's functional impairment is only one side of the work disability equation; work is the other. Employment and job placement, including getting support from the business community, need more attention in today's work disability management process.
Finally, public disability programs consist almost exclusively of cash benefits. The cost-effectiveness of providing access to and requiring the use of treatment and rehabilitation, which restores function, along with, or as a condition to, receiving cash benefits has yet to be tested for public policy application.
Richard Burkhauser, Ph.D.
Department of Policy Analysis and Management, Cornell University
The experiences of other countries can shed some light on the search for appropriate Social Security Disability Insurance (SSDI) and Social Security Income (SSI) program eligibility criteria for people with disabilities. This discussion focuses primarily on experiences with disability-transfer programs in four countries—the Netherlands, Germany, Sweden, and the United States (Aarts et al., forthcoming).
Before recommending dramatic changes in our current SSDI and SSI eligibility criteria, one has to ask several questions. Is the current system sufficiently in trouble to warrant such changes? If so, what is the evidence of the failure of the current system to achieve its objectives, and what criteria were used to determine the size of this failure? Without answers to these questions, it is difficult to either put a new system into place or to determine whether or not the new system is superior to the current system.
International evidence suggests that public policies are the most important factors in determining the relative size of the disability-transfer population. Over time, countries have used different eligibility criteria to define their protected population and different processes to implement this protection. Described below are some of the differences across countries and over time in these criteria and processes as well as an overview of the tradeoffs that should be considered in establishing them.
Table 5-1 shows that the working age population receiving disability transfers in the Netherlands, Germany, Sweden, and the United States varies across age groups and over time. As would be expected, since the prevalence of health-related impairments increases with age, disability transfers among working age people increases at older ages in all four countries. Past that similarity, dramatic differences are observed across countries and within each country over time.
TABLE 5.1 Disability Transfer Recipients per 1,000 Workers by Age, in Four OECD Countries, 1970-1995
|
Age |
1970 |
1975 |
1980 |
Growth Change, 1970–1980 (%) |
1985 |
1990 |
Growth Change, 1980–1990 (%) |
1995 |
Growth Change, 1990–1995 (%) |
|
Aged 15–64 years |
|||||||||
|
United States |
27 |
42 |
41 |
52 |
41 |
43 |
5 |
64 |
49 |
|
The Netherlands |
55 |
84 |
138 |
151 |
142 |
152 |
10 |
142 |
-7 |
|
Sweden |
49 |
67 |
68 |
37 |
74 |
78 |
15 |
106 |
36 |
|
Germanya |
51 |
54 |
59 |
16 |
72 |
55 |
-7 |
47 |
-15 |
|
Aged 15–44 years |
|||||||||
|
United States |
11 |
17 |
16 |
45 |
20 |
23 |
44 |
39 |
70 |
|
The Netherlands |
17 |
32 |
57 |
235 |
58 |
62 |
9 |
57 |
-8 |
|
Sweden |
18 |
20 |
19 |
6 |
20 |
21 |
11 |
32 |
52 |
|
Germanya |
7 |
6 |
7 |
0 |
8 |
5 |
-29 |
6 |
20 |
|
Aged 45–59 years |
|||||||||
|
United States |
33 |
68 |
83 |
151 |
71 |
72 |
-13 |
103 |
43 |
|
The Netherlands |
113 |
179 |
294 |
160 |
305 |
339 |
15 |
271 |
-20 |
|
Sweden |
66 |
95 |
99 |
50 |
108 |
116 |
17 |
151 |
30 |
|
Germanya |
75 |
64 |
84 |
12 |
103 |
75 |
-11 |
87 |
16 |
|
Aged 60–64 years |
|||||||||
|
United States |
154 |
265 |
285 |
85 |
254 |
250 |
-12 |
314 |
26 |
|
The Netherlands |
299 |
437 |
1,033 |
245 |
1,283 |
1,987 |
92 |
1,872 |
-6 |
|
Sweden |
229 |
382 |
382 |
67 |
512 |
577 |
51 |
716 |
24 |
|
Germanya |
419 |
688 |
1,348 |
222 |
1,291 |
1,109 |
-18 |
890 |
-20 |
|
a German data refer to the population in the western states of the Federal Republic of Germany. SOURCE: Derived and updated from Table 1.1 in Aarts et al. (forthcoming). Reprinted with permission from Industrial Relations Research Association. |
|||||||||
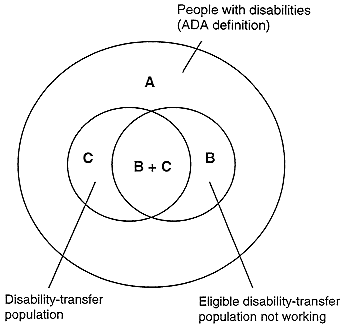
FIGURE 5-1. Targeting social policies on the working age population with disabilities. SOURCE: Burkhauser, 1997. Reprinted with permission of Dr. Richard V. Burkhauser, Cornell University.
Those differences have more to do with the policies that govern the disability eligibility determination process than with changes in the underlying health and disability patterns of those populations.
The preponderance of evidence to date suggests that overall health in each of these countries, measured either by morbidity or mortality scales, has improved significantly over the last 25 years. Yet the number of people on disability-transfer programs relative to the working population has increased in all four countries.
No country demonstrates the power of policy changes to affect the rate of growth in the disability-transfer population better than the Netherlands. No one would suggest that the underlying health of the Dutch working age population has deteriorated at a more rapid pace than that of the other countries in Table 5-1. Yet the growth in the prevalence of the Dutch working age population receiving disability transfers in the 1970s far exceeded that of the other countries. Policy changes in the 1980s slowed this growth, and dramatic policy changes in the early 1990s have turned it around. (See Aarts et al. [forthcoming], for a fuller discussion.)
The dramatic differences in disability-transfer populations seen in Table 5-1 can be explained using Figure 5-1. Circle A represents the entire working age population with disabilities, using the Americans with Disabilities Act of 1990 (ADA) definition, namely, working age people who have a physical or mental impairment that substantially limits one or more major life activities, or a record of such impairments, or who are regarded as having such impairments. This definition is more all-encompassing than that of Nagi or the World Health Organization, since it includes people who have limitations, but may or may not be failing in some socially expected role. Previous studies applying this broader definition to the United States have found that from 8 to 12 percent of the total working age population would be included in the population with disabilities depending on the data set and questions used (Bound and Burkhauser, forthcoming).
When the ADA definition is applied across countries or over time in the same country, the size of the overall population in circle A does not dramatically change. However, two subsets within this population, circle B—the eligible disability-transfer population—and circle C—the actual disability-transfer population—will change dramatically.
Circle A is more or less invariant to policy decisions. It is a function of demographic characteristics, such as age and gender. But it is also affected by the quantity and quality of medical care, the wealth of the country, and the education of the population with regard to their personal health. In the long run, circle A can increase or decrease as a result of medical innovations. It decreased when polio was eradicated and will do so again if a cure is found for AIDS. But circle A can also increase. If medical innovations prolong life but do not offset ensuing impairments and functional limitations, then circle A would increase, as, for instance, it did in the case of advancements in medical care for severe spinal cord injuries.
By contrast, the size of the population in circle B has historically been a reflection of public policy in all four countries in Table 5-1. Eligibility rules vary across the countries. Only in the United States is eligibility limited to those who are totally disabled. In the other three countries, eligibility is offered to those who are partially disabled. The criteria for failure to perform work are also important in determining the size of the circle B population. In the United States, the definition is strict and relates to any substantial gainful employment, while Sweden and Germany use a commensurate work definition. That is, if the impairment prohibits a person from doing the kind of work the person has been doing in the past, this is sufficient to become eligible for disability-transfer benefits. In 1993, in an effort to reduce system growth, the Netherlands abandoned its definition of commensurate work and adopted a "substantial gainful employment" criterion like the one used in the United States. This change in eligibility criteria is one of the reasons for the reduction in the relative size of the disability-transfer population in the Netherlands in the 1990s seen in Table 5-1.
A major distinction between the United States disability-transfer program and that of other countries in Table 5-1 is the availability of immediate benefits.
The United States has a five-month waiting period and no universal short-term disability program, although many individual employers have short-term disability benefits programs. Sweden, Germany, and the Netherlands all have sickness benefits that can continue for several years. Since 1993, however, the Netherlands has required employers to pay for the first six weeks of sickness benefit. When that policy was imposed, the proportion of workers receiving sickness benefits declined.
Labor market considerations affect the size of the eligible population. Prior to 1987, the Netherlands had an elaborate procedure to measure earning capacity in which officials looked at the characteristics of a person's past jobs. They tried to link the characteristics of these jobs to their measure of the person's impairments. They also had a very intricate six-category system of partial disability, starting at the 15 percent disability level. However, if a person was declared to be partially disabled, even if only at the 15 percent level, but was not currently employed, the person received a full disability benefit unless the government could show otherwise. Hence while the Netherlands had an elaborate system of trying to assign a share of disability to each individual, the overriding importance of labor market considerations effectively meant that very few people actually got partial benefits.
Circle C represents the population currently receiving disability benefits. The size of the circle C population depends on application decisions by the potentially eligible as well as on acceptance decisions by program gatekeepers. Applications are sensitive to general economic conditions. They rise in bad economic periods and fall when the economy improves. For individuals, the size of their benefits and their ease of access to them relative to other alternatives is an important factor in their decision to apply. In disability systems that emphasize work through rehabilitation and quotas, such as in Germany and Sweden, even though disability-transfer benefits are relatively generous, transfer rolls remain relatively low because many in the transfer-eligible population work.
The relative size of disability-transfer benefits compared to those offered by other government programs also makes a difference. For instance, transfer benefits in the German disability system are not much different from the benefits offered by other German transfer programs. By contrast, relatively easy access and high benefits relative to other transfer programs in the Netherlands and in the United States have meant that during the trough period of the business cycle, much greater pressure is put on their disability-transfer programs.
Circle B and C populations do not necessarily have to coincide. Some in circle B work and therefore do not apply for benefits, while others in circle B do not know they are eligible and therefore do not apply. Finally, some in circle B have applied for benefits and are eligible, but they are mistakenly denied benefits. This is known as type-2 error.
Circle C is not a subset of circle B, because some of the circle C population are awarded benefits even though they are not truly eligible. This is Type-1 error. These people are currently unemployed and have disabilities, but they are
capable of substantial gainful employment and hence do not actually meet circle B eligibility criteria.
Policy choices make a difference in the size of the two circles and in the degree that they coincide. In its effort to redesign the disability decision process, SSA must decide what it is trying to achieve—for example, reduce the size of circle C, insure that circle B and circle C coincide, insure that circle C is a subset of circle B, minimize Type-1 error, or minimize Type-2 error. If SSA is interested in reducing errors, which is more important—reducing false eligibility or false ineligibility? The discussion at this meeting suggests that we are primarily focusing on reducing Type-1 error. But in making judgments about what we are trying to achieve, it is important to think about the social costs of both types of error when discussing the tradeoffs between added administrative costs and the reduction of such errors.
One important criterion that could be used in any evaluation of a redesigned system is its ability to reduce the uncertainty of outcomes on the part of all parties involved. Ex ante the system should provide better information about the likely outcome for people with disabilities who are required to make the difficult choice of if and when to apply for benefits.
Half of the people with disabilities who have gone through this process and have been denied benefits never work again. There are two reasons why they never work again: (1) the system mistakenly denied them benefits, and (2) the scarring effect of the system itself. If a person invests in trying to get on the program, the rational way to do so is to do everything possible to diminish the possibilities of being judged capable of performing any substantial gainful activity. A person with disabilities planning to apply for benefits has to be unemployed for six months prior to application and during the determination process. Obviously, people out of the workforce for two years are much less likely to get back into the labor force, regardless of their initial condition, than those who try to get back to work before applying for benefits. Therefore, it is possible that a more complex method of reducing errors could lead to worse outcomes, if that system increased the uncertainty of the final outcome to the applicant. Rather than searching for a system that reduces errors based on some gold standard, which in the end will be to some degree arbitrary, a redesigned system should reduce the uncertainty of the process and hence the social costs associated with the disruptions in the lives of people with disabilities.
Ian Basnett, Ph.D.
Department of Medicine and Institute for Health Policy Studies, University of California at San Francisco
This presentation summarizes the basics of the current benefits system in the United Kingdom (UK), its structure, operation, and the likely directions of future change, and offers some conclusions of the review and policy suggestions.
The United States and the UK are facing similar problems with regard to benefits. Both have a system under strain and a method of assessing disability that is certainly considered unsatisfactory by some.
In the UK, disability benefits are included in the government's review of all benefit programs. Spending in the UK on disability benefits has risen substantially and now amounts to about a quarter of all total benefit expenditures. The government's benefits policy is aimed at enabling people to work if they are able to, but it was felt there were not enough positive incentives and mechanisms in the disability benefits system to enable that. The current "All Work Test" is an individually based, functional, all-or-nothing test. There is no graduation between being fully employable and unemployable. There are some perverse incentives that make it difficult for disabled people to take work without risking a drop in income. For example, when a disabled person on the highest level of incapacity benefit takes employment, but subsequently becomes unemployed, the person is eligible only for a lower level of benefit, unless benefit is reclaimed within eight weeks. Like most governments there is also a concern whether the right people are receiving benefits or whether, because of fraud, maladministration, or inappropriate eligibility criteria, ineligible people are receiving benefits.
In the UK, there is a complex array of benefits for disabled people, but in simple terms they can be divided into two types: (1) those designed to compensate for the extra costs of living with a disability, and (2) those that substitute for employment. Access to these can act as "passports" to other benefits, such as housing benefits if other criteria are met, for example, through a means test. The different benefits have different methods for assessing disability; the methods used have changed over time, and more changes are planned.
The main benefit is the Disability Living Allowance, intended to meet the extra costs of living with a disability. This was last changed in 1992, when the Disability Living Allowance replaced two separate benefits and the assessment procedure was changed. Disability Living Allowance has two components, a care component and a mobility component. It is quite common to receive both components. It was designed to target the most disabled and, therefore, those with greatest needs, who are most likely to be poor. It is not means-tested or taxed so that disabled people who are employed can receive this benefit. Children under five and those whose disability arises at 65 years of age and over are only eligible for "Attendance Allowance," the care component of the Disability Living Allowance.
The Disability Living Allowance has increased nearly 90 percent since 1992. The increase is due to a variety of reasons, including: the 1992 changes that extended eligibility, especially to blind people and those with learning difficulties; the previous very low uptake combined with a publicity campaign on the introduction of Disability Living Allowance in 1992; and increasing numbers of people leaving long-stay institutions.
Benefits that substitute for employment are for those people assessed as being unable to work. They are provided mainly via "Incapacity Benefit" (a contributory benefit depending on having paid national insurance contributions) or
"Severe Disablement Allowance" for those who have not made contributions. They were last changed in 1995, when the assessment procedure was substantially revised. They are not means-tested but are taxable.
People with disabilities who are ineligible for Incapacity Benefit or Severe Disablement Allowance may claim income support, the general means-tested benefit available for those not working 16 hours or more a week, designed to raise income up to a minimum level.
Disability Working Allowance is a means-tested, partial-incapacity benefit payable to those who leave Incapacity Benefit or Disablement Allowance to enter training or work. It is payable only while employed for at least 16 hours a week. Incapacity Benefits have tripled over the last 20 years. However, at least part of this increase is accounted for by individuals who previously would have claimed Job Seekers Allowance (unemployment benefit) and by women becoming eligible for contributory benefits for the first time.
Disability is assessed differently in these two benefit areas. The initial assessment for Disability Living Allowance is based on a complex and detailed self-reported form focusing on questions about needs for care and mobility. A "professional" (often the physician) completes a section commenting on how the disability affects the person. Adjudication Officers in the Benefits Agency, who can request further information or a medical examination, make the decision.
Until 1995, the assessment for employment substitutes relied on a combination of functional assessment and other factors, such as education, age, and previous work experience. In 1995, the assessment process changed. Someone previously employed is subject to a test of incapacity in his or her own occupation for the first 28 weeks. Those still disabled after 28 weeks and people not previously employed are subject to the "All Work Test"—a very functional test based on the ability to undertake tasks. Tasks assessed, via a questionnaire, include walking, bending, lifting, and a section on continence and another on mental illness. The measures are similar to those developed for a survey of the population prevalence and severity of disability and were not devised originally for individual assessments. The assessment is based on a self-completed form, a report from one's personal physician, and, if necessary, examination and assessment by the Benefits Agency Medical Service. A Benefits Agency adjudication officer makes the decision. The threshold for work is set at the point at which "it is unreasonable to expect a person to work," not where work becomes impossible. A number of conditions are exempt from the "All Work Test,'' for example, quadriplegia. Claimants are also exempt if they receive the highest level of the care component of the Disability Living Allowance.
The change in 1995 was in part to restrict access to an increasingly popular benefit and believed to be more objective than previous measures. It was unpopular with disability groups, as it was individually based and functional and took no account of other factors.
Likely Directions of Future Change
A far-reaching review of the benefits system is currently underway and a "Green Paper" (for consultation) was published in March, 1998. The review looks at assessments for both areas of disability benefits, and recognizes the fallacy of an all-or-nothing work test. In broad terms, for Incapacity Benefits the measures proposed fall into three areas: (1) helping people with disabilities find employment, (2) removing perverse incentives against working, and (3) changing the assessment process for incapacity benefits. The proposed approach is to focus on what disabled people can do, not what they cannot do. For future claimants, the scale of their employability will be assessed, recognizing that capacity for work is a continuum. People with some capacity for work would then be given the opportunity to receive the assistance they need to help them return to work. With regard to the Disability Living Allowance the Green Paper is vague, promising to involve disabled people in a review of the gateway to Disability Living Allowance and Attendance Allowance.
Conclusion of the Review
Although lacking in detail, the broad direction of the changes in the UK is welcome. Hopefully they will result in an assessment process that has the following features:
-
holistic—assessing an individual's education, skills, and experience;
-
take account of the local labor market and chances of finding employment;
-
replace the All Work Test with an assessment of "employability";
-
consider what a disabled person could achieve given appropriate accommodations, not his or her functional limitations according to an able-bodied norm;
-
allow for a continuum of disability, from able to work full-time to unable to take any employment;
-
assess the impact of impairments in a work setting by experts in vocational. rehabilitation, not necessarily doctors;
-
introduce an individual action plan based on the assessment and other information;
-
redesign benefits to provide income security based on the activities agreed to in an individual's plan, not predetermined rules;
-
involve disabled peoples' organizations in developing the assessment process; and
-
where appropriate, acknowledge and involve the disabled person as an expert in his or her disability in the assessment process.
Involving disability advocacy organizations and the disabled person in the process would be wise as well as politically astute. It would ultimately produce a better process. The new process could be worse than the current one if accommodations do not follow an assessment, or if all of the individual's talents or lack thereof are not assessed and are not sensitive to someone's fluctuating disability or age. Moreover, it is important not to get paralyzed by trying to find the gold standard and to understand that a new process achieves an incremental improvement over what now exists.
Disability is largely a social construct, and functional measures of disability in isolation are not very useful for determining whether somebody is unemployable. An assessment ought to be about employability rather than disability, looking only at functional limitations according to an able-bodied norm. A person with disabilities, therefore, should be assessed based on what he or she could achieve, given appropriate accommodations.
The United Kingdom does not have the further complication that disabled people risk losing their health care coverage should they move off benefits, as in the United States. However, there are still many similarities in the challenges both countries face in reviewing disability benefits, and some similar themes emerge in the thinking about the assessment process. There is a great deal of gray in this area and the redesign efforts in the United Kingdom and in the United States are grappling with reducing it.
GENERAL DISCUSSION AND COMMENTS
Some of the key issues that surfaced during the general discussion are:
-
What can the United States learn from the experience of other countries in terms of techniques or approaches to assessing functional capacity for disability benefits? Clearly, policy questions swamp the technical questions of assessment, and the Netherlands is a dramatic illustration of that. The Netherlands perfected the best system for measuring functional limitations for individuals and developed a concept of earnings capacity and a system to relate conditions to levels of disablement based on kinds of jobs held in the past and jobs that the person could hold in the future. They registered all jobs in the economy. They had a sophisticated computer matching system to determine the percentage of eligibility and tied the benefits to that. After they developed this complex and very sophisticated system, they ignored it all and gave full benefits if the person was unemployed. Even in other countries, such as Sweden and Germany, where the disability programs include partial benefits determination, there is pressure to give full benefits to people who are evaluated as partially disabled but not fully employed.
-
Functional evaluation is an important and necessary way of making a decision about a person's ability to work in certain circumstances. However, SSA also needs to give more attention than has been given in the past to issues around the segmentation in the disability population. Different types of people present themselves for disability evaluation, and there are different ways of evaluating disability in relation to where a person is at any moment in time and what his or her future holds by way of improved function or removing barriers.
-
The purpose of a disability benefit program is important to keep in mind. Is it to compensate for the loss of work, or is it in some way a requirement to compensate for the medical condition by paying for anything it will take to get the person back to work, or is there a different threshold, which is to pay enough for replacement of the minimal gainful employment equivalent? This is a policy question and it goes back to the definition of disability. The SSA has a system that only pays one type of benefit, but it does not divide the world into totally disabled and not disabled. It pays for partial disability; a person can earn up to the SGA limit and still be eligible for some benefits.
-
In the private sector there are two different concepts of assessment techniques—contractual obligation and discretionary obligation on the part of the insurer. The contractual obligation involves assessment to decide if the individual meets the test of disability that is in the insurance contract so that the person can get earnings replacement benefits. The purpose of a subsequent assessment, which was quite different criteria, is to determine what additional services this person should have along with assuring that the person is getting appropriate medical care to help him or her get back to work. One of the primary criterion of this assessment is the person's motivation to get back to work. Case management for these individuals starts at the beginning of the process.















