6
Adapting Measurement of Functional Capacity to Work to SSA's Disability Decision Process
This panel was asked to discuss:
-
the criteria for a ''successful" measurement of functional capacity to work;
-
the feasibility and practicality of designing and administering (safety, cost, etc.) measures of functional capacity to work;
-
technical issues of incorporating reliability, validity, sensitivity, and specificity in the context of SSA's disability decision process; and
-
the feasibility and manner of linking these measurement approaches to work requirements in the context of SSA's disability decision process.
Virginia Reno
Director of Research, National Academy of Social Insurance
A discussion about the practical application of new measures of functional capacity to SSA's disability decision process calls for assessing the effectiveness of trying to shift far from the medical assessment tools that SSA uses, or at least that model, to focus more heavily on functional assessment. One needs to step back and ask a prior question, that is, why does SSA want to revamp its disability assessment to make it more "functional" (or less "medical") in nature? What is the evidence or experience suggesting that a more functional assessment will be better than the current process?
Certainly, in many other contexts of disability policy there has been a shift away from medical assessment toward much more functional assessment of
people's capacities. Often this new focus on functioning has produced positive outcomes. In almost all such cases, however, the new emphasis on functional assessment is about the delivery of services—health care, vocational rehabilitation, helping people find jobs that match their abilities, or job accommodations. In each case, the purpose of the intervention is to maintain or improve a person's functioning. The functional assessment helps to determine whether intervention is warranted, and if so, what regimen of services, equipment, or environmental changes would appropriately aid functioning.
The Social Security program, in contrast, is not about delivering services. Rather, it is about providing monthly cash benefits that replace part of lost earnings. And it provides benefits only when workers experience severe illness or other impairments that make them unable to work for a long time. The purpose is to help disabled workers pay their bills while they deal with other consequences of their ill health and job loss. SSA has the unenviable task of deciding who among millions of applicants for these benefits have medically determinable impediments to work that are so severe that they meet the very strict test of disability in the Social Security Act—that is, inability to engage in any substantial gainful activity by reason of a medically determinable physical or mental impairment that is expected to last at least a year or result in death. The impairment must be of such severity that the person is not only unable to engage in prior work but is unable to do any other work that exists in significant numbers in the national economy, not just in the area in which the applicant lives. By law, therefore, the Social Security assessment must determine the severity of the impairment. There is an implicit assumption that other systems—such as vocational rehabilitation—will make separate assessments of the appropriateness of services to restore functioning.
SSA has to be equipped to make a lot of these decisions every year. For instance, in 1996 there were about 2.3 million decisions on new claims, about 770,000 reconsideration decisions, and another 5,400,000 decisions on appeals to an administrative law judge. The process, therefore, needs to be one that can accommodate a tremendous number of decisions.
There are reasons to question the presumption that shifting to a "more functional and less medical" assessment for this purpose would be an improvement. This observation is based in part on findings of a disability policy panel that was convened by the National Academy of Social Insurance and which issued its final report, Balancing Security and Opportunity: The Challenge of Disability Income Policy , in 1996 (Mashaw and Reno).
Three sections of that report are particularly useful for thinking about how we define and evaluate disability for different purposes. First, the panel adopted a conceptual model of work disability that is analytically useful for understanding possible causes of work disability. It is also useful for considering how service interventions at any of the four levels in the model might remedy work disability. That is, remedies might be effective at the level of: (1) the impairment, (2) the person's skills and abilities, (3) the tasks of work the person can rea-
sonably be expected to do, and (4) the broader environment in which he or she lives and works. These are all elements of work disability.
Second, the panel considered legal definitions of disability that are used in public programs and private contracts to define who is eligible for specific assistance provided by that program. Unlike the generic conceptual model of work disability, legal definitions vary depending on the purpose of the program. If the purpose of the program is to provide assistance with activities of daily living (ADL), the definition of disability is the need for assistance with ADL. Likewise, programs that offer vocational rehabilitation services define disability in terms of the applicant's need for and likelihood of benefiting from those services. Laws that offer remedies against discrimination define coverage in terms of those at risk of discrimination. And programs that provide cash benefits to replace part of lost earnings define eligibility in terms of lost capacity to earn. That is true in private disability insurance as well as in public disability cash benefit systems. Social Security disability insurance falls in this last category of programs that offer wage-replacement benefits. When compared with other public and private disability wage-replacement programs, here and abroad, it is found to have one of the strictest definitions of work disability. And when compared with U.S. private sector programs and public programs abroad, it provides very modest levels of partial wage replacement.
A third part of the panel's report focused on the "assessing the assessment" process that is now used to determine who meets the strict test of work disability in the Social Security Act. It is most directly germane to whether a greater reliance on functional assessment (and a lesser reliance on medical evidence) will make the Social Security decision process work better. Four criteria can be used for assessing the assessment: accuracy (validity), consistency, credibility, and administrative efficiency.
Using these criteria, the Disability Policy Panel evaluated SSA's multistep decision process for determining whether applicants meet the Social Security test of disability. It evaluated both the decision process as a whole and the various steps in the process: initial screens for eligibility (a person's insured status, work status, and application for benefits); the expected duration of the impairment; the use of medical listings; the evaluation of residual functional capacity; and the consideration of vocational factors—age, education, and work experience. In evaluating the decision process, it is important to consider each step, not only in isolation, but as part of the whole decision process, conditional on findings made in the earlier steps. Viewed in this way, the sequential process has some logical coherence. The panel nonetheless concluded that various steps in the decision process could be strengthened, such as updating the medical listings, updating and expanding the assessment of functional capacity to include more nonexertional impairments, and perhaps updating the vocational factors to reflect changing work demands.
Efforts to shift SSA's assessment away from medical evidence toward more use of functional measures should be considered with caution. First, it is impor-
tant to recognize that the "medical listings" are not used in isolation. They are used only after certain findings are made at earlier steps in the sequential process. That is, for disability insurance benefits, the medical listings are considered only if: an individual is out of work (not engaging in substantial gainful activity); yet has recent and fairly steady work experience (is insured); has actually applied for benefits that generally replace a modest portion of his or her prior earnings; will receive those benefits only after being out of work for five months; and has a severe impairment that is expected to last a year or result in death.
At this step of the decision tree, the medical listings branch has some useful attributes. Decisions based on the listings compared to functional assessments tend to have credibility with applicants and the public. They often are less time consuming, can be applied fairly consistently, and are the least contentious decisions. The latter is understandable because the medical listings produce a final decision only in one direction, that is, to allow benefits.
That the medical listings are used only to allow benefits that are being sought (and conditional on the findings listed above) is important. In the panel's deliberations about the respective merits of functional and medical assessments for Social Security determinations, it became clear that some concerns about use of medical listings grew out of experience with use of medical assessments in other contexts—particularly in vocational rehabilitation. That is, an emphasis on diagnosis and medical severity was sometimes used by state vocational rehabilitation agencies to find that an applicant for services would be "unable to benefit from services in terms of a work outcome" as called for in the Vocational Rehabilitation Act, and, therefore, services were denied. The Rehabilitation Act was amended in 1992 to reduce the likelihood of such denials.
Given their many useful attributes in making Social Security determinations, why might one want to reduce reliance on the medical listings for this purpose? What is the problem that needs to be solved? Is it a belief that some people are wrongly allowed benefits based on the medical listings? That is an empirical question that could be investigated by looking at the attributes of current beneficiaries. Some disability insurance beneficiaries who are, in fact, able to go back to work do so, despite the continuation of their impairments. Various work incentive features in the program are designed to aid that transition. Are we concerned about the prospect that some people who would meet the criteria in the medical listings are working and have not applied for benefits? How serious is that problem and who is harmed by it? Does this undermine the validity of the listings? It might seem so if the listings are considered in isolation. But that might change if they are considered as one step in a decision process, conditional upon all of the findings earlier in the process. Or, is concern about the use of medical listings a carryover from battles fought on other fronts of disability policy, particularly in the areas of service delivery and civil rights? Is the concern that in these other arenas, medical findings might be used to deny rehabilitation services or job accommodation that were being sought, while a functional assessment might have produced an allowance? If so, the question needs to be
asked whether and how these concerns apply in the context of Social Security determinations.
Lisa Iezzoni, M.D., M.S.
Associate Professor of Medicine, Harvard Medical School
The distinction between medical and functional assessment of disability is a false dichotomy; the assessment should be viewed as a continuum. Diagnosis or diagnostic information has several values in thinking about people's ability to work. The first is prognosis. Medical diagnosis provides a level of certainty about the expected course of the disease that is useful in making a disability determination. It is clearest when the medical diagnosis points inexorably to death in the near future.
Secondly, diagnostic information is viewed by virtually everybody as highly objective. However, determining the diagnosis is not always easy. In addition, identifying a single, primary diagnosis that is responsible for the disabling condition is not always straightforward. Often no one single medical condition alone is sufficient to consider a person disabled, but multiple, coexisting conditions taken together are disabling.
The impetus behind moving away from medical diagnosis is the view that thinking about function tells something about the whole person. Function reflects how the whole organism is operating; it reveals how people are living their daily lives. From the perspective of risk adjustment, functional status is often more predictive of even the ultimate physiological outcome, death, than some classic medical parameters that doctors look at. For example, studies have found that an ADL score was more predictive of imminent death than an acute physiology score or other medical variables, such as the stage of lung cancer, complications relating to the lung cancer, or the burden of comorbid illness.
The question of determining eligibility is not an either-or situation. The best way to evaluate disability for awarding cash benefits is by combining diagnostic and functional approaches and using a holistic view that not only looks at these clinical variables, but also looks at education, job experience, and other aspects of the patients' lives that influence employability.
Motivation is important in whether people continue to work or not, especially if enabling factors are present, such as assistive technologies and reasonable accommodations. Also, there is a lot of discussion about validity of the assessments. The question is validity of assessments from whose point of view? For instance, face validity from a decisionmaker's point of view may differ from face validity from the point of view of a person who cannot walk. If such persons are asked functional questions, the questions have to make sense to them in the context of how they live their lives. This point was illustrated by an example of a woman who uses a motorized scooter to get around because of health problems. When she was asked during her functional assessment to describe her problems
walking, the question was irrelevant from her perspective. The assistive device is integral to this woman's thoughts about how she leads her life.
In the next 20 years, non-English-speaking people and people from other cultures will become the majority of the population in certain areas of this country. Increased attention will have to be given to language and culture as assessments are conducted to determine disability. Different ethnic groups have very different ideas and attitudes about disability. These issues will become increasingly important as the shifting nature of employment puts greater emphasis on communication skills.
The third and final point relates to the nature of jobs. SSA is trying to implicitly calibrate assessment of functioning against some fuzzy concept of substantial gainful employment. The definition of SGA becomes important. Looking at the problem historically, for years disabled people were trained to so limit their skills and their expectations as to be permanently incapable of meaningful employment. Such efforts only served to reinforce the sense of helplessness and isolation felt by those who were disabled.
The statute calls for enabling workers to retain their dignity and self-respect while they cope with the human and financial losses associated with the lost capacity to earn. If that is part of what SSA is doing, this perspective needs to better inform the process. This is a policy issue. The question that needs to be asked next is whether the policies relating to determinations of disability compensate for the inadequacies of other policies of our government, such as health insurance, that touch on the lives of disabled people. For example, for a patient with advanced multiple sclerosis, having an assistive device for mobility is critical in the person's assessment of disability. So when Medicare denies reimbursement for a motorized scooter on the grounds that it is not "medically necessary," should SSA's policy for disability determinations in this venue compensate for this medical necessity barrier toward getting people the assistive technologies they need to obtain jobs that give them not only income, but also allow them to maintain their dignity?
David Stapleton, Ph.D.
Vice President and Senior Economist, The Lewin Group
A conceptual model of disability was presented in a three-dimensional diagram (Figure 6-1), depicting the relationship between earnings potential, impairment, and "environment," loosely defined as all determinants of earnings potential other than impairment.
The figure makes two assumptions: (1) only two factors (impairment and environment) affect ability to work and (2) impairment, environment, and ability to work are each univariates that can be precisely measured. Environment is a composite index of factors facilitating work (e.g., state of economy, support system, employer accommodations). The figure shows that various combinations
of true impairment and true environmental factors result in an individual being able to achieve a specific level of earnings as represented on the surface of the three-dimensional diagram. If impairments increase, holding environment constant, the individual's earnings decline. As environment is improved, holding impairment constant, individual earnings increase.
A contour line in the diagram, labeled YY', indicates the level of earnings that defines substantial gainful activity (SGA) for SSA programs—currently $500. Conceptually, the current programs require SSA to determine which side of the line each claimant is on. But determining the location of the line is problematic. SSA has defined a line, which might be represented by ZZ'. The perception is that this line, which places heavy weight on impairment and relatively little weight on environment, allows many people who can attain SGA to become beneficiaries (false positives) while some who cannot work are denied benefits (false negatives). The redesign process could be described as trying to determine the true SGA line more exactly, by giving more consideration to functional status—implicitly giving more consideration to environmental factors, because these interact with impairment to determine functional status.
SSA's efforts to redesign the disability decision process can only have limited success. The various reasons can be illustrated with this model.
First, as discussed earlier in the workshop, the workplace has changed in the past 30 to 40 years, and more changes can be expected in the years ahead. In the context of the model represented in Figure 6-1, the problem is not to determine the surface as it is today, but to follow how it changes over time and predict what it is going to be in the next 20 to 40 years. That is a tough and intractable problem.
Second, true impairment and true environment are difficult to measure. That means that SSA is not really using the line ZZ', shown on the diagram but rather a fuzzy line because of errors in measuring both impairment and environment. Putting more emphasis on functional status will add to the fuzziness that already exists because of problems in measuring impairment. In part, this is because of uncertainty about what should be included in environment—to what extent should we consider accommodations, assistive devices, and so on.
The main way the proposed redesign would explicitly capture environment is through use of O*NET. Although O*NET is a very good system and useful for what it was designed for, there are strong concerns about whether it can actively capture environment for the purposes SSA intends. O*NET was designed for people who do not have serious impairments and focuses on ''average" abilities.
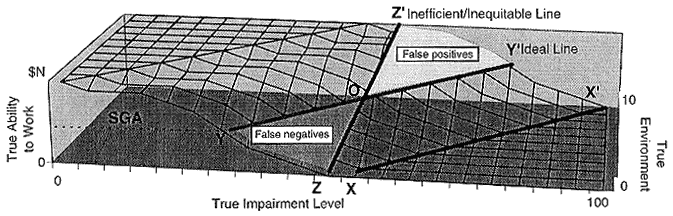
FIGURE 6-1. Impairment level, "environment," and ability to work. NOTE: This chart assumes: (a) that only two factors (impairment and environment) affect ability to work, and (b) that impairment, environment, and ability to work are univariates that can be precisely measured. Environment is a composite index of factors facilitating work (e.g., state of economy, support system, employer accommodations). Impairment is a measure of the severity of individual disabilities. Ability to work is an individual's earnings in the highest-paid job for which she or he is qualified. SOURCE: Unpublished. Reprinted with permission from Abt Associates and the Lewin Group.
Even if true impairment and true environment can be observed, we still would not be able to observe the exact number of eligible and ineligible individuals. One reason is that people who are near the true SGA line have a strong incentive to not reveal what their earnings could be. There are other reasons, such as the state of the economy and the legislative requirement that "any job in the economy" must be considered. The redesign would map out the surface by using a complex process that takes impairment, maps impairment onto functioning, and maps functioning onto requirements for specific jobs, using O*NET, and then looks at what those jobs pay. It is difficult to believe that this complex procedure will result in an estimated surface that is sufficiently accurate for its purpose. People may have less confidence in the redesigned system than in the current system if they perceive that the measurement of disability under the new system is more capricious, which it may be for the reasons described above.
One particular concern about the use of functional status measurement is motivation. Functional status measurements are fine when individuals are motivated to reveal their functional ability. However, SSA will run into trouble when applying functional assessment measures to people who are motivated to show that they "are disabled." By definition, they are so motivated if they are trying to obtain benefits. If SSA goes through with its current plan of adopting increased use of functional status in its redesigned decision process, it needs to carefully assess the effect of motivation on the outcomes of functional assessments. Otherwise, the likely outcome is unanticipated growth in the rolls.
It seems likely that increasing the consideration of environmental factors in the determination process will result in a process that is more complex, not less complex as intended. A more complex process will make uniformity of decisions all the more difficult to achieve in a system that relies on state employees to make most determinations. Deterioration in uniformity will undermine political support for the program.
What policy changes could be supported, given the constraints of measurement? If all agree that impairment can be measured reasonably well, a policy that largely ignores earnings in determining cash benefits might be considered. That is, benefits would be determined on the basis of impairment only—"impairment insurance." Under such a system, SSA might provide full benefits to applicants who are the most severely impaired, regardless of earnings, or at least until earnings are at a very high level. For those who are less impaired, partial benefits can be provided, as is done in some European countries. The Disability Evaluation Study offers the opportunity to estimate the size of the pool of people who would qualify. A less radical departure from current policy would be to determine eligibility for medical benefits on the basis of impairment only, retaining earnings as a consideration for cash benefits.
If such changes to the incentives to work were coupled with more effective rehabilitation and other employment services, we might well see a dramatic change in the employment and earnings of people with disabilities. Better measures of functional status could make a significant contribution to the delivery of
better rehabilitation and other employment services. In determining eligibility for such services and in selecting appropriate services, the individual has an incentive to reveal what his or her real functional capacity is.
GENERAL DISCUSSION AND COMMENTS
Some of the key issues that surfaced during the general discussion are:
-
The Social Security Act requires establishment of a medically determinable impairment and a medical cause and then an evaluation of the functional consequence of the cause. The proposed changes in the determination process are an attempt by SSA to improve the way functional consequences of impairments are measured. It is therefore incorrect to view the current disability determination process as a medical model and the proposed revision as a functional model. Clearly, the contrast between functional and medical assessment should not be overdrawn; medical evidence often is functional in nature. It is not an either-or situation. The value of considering both impairments and functional capacity is obvious; both have something to contribute in the disability determination process.
-
A person with an impairment may be looking for a job and not wanting to receive Social Security Disability Insurance (SSDI) or Supplemental Security Income (SSI), but the impairment makes it difficult to get employment and therefore health insurance. Is there any evidence about the motivation to obtain disability benefits because it may be the only means of getting medical benefits? The Lewin Group is conducting an analysis of a SSI cohort and their earnings over time under the SSI work incentive program. It is finding strong evidence that people on the program were restraining their earnings to keep them below the income threshold. As the income limit went up based on the average Medicaid expenditures in a state, the earnings of the SSI beneficiaries accordingly increased. Because of their earnings they are not receiving much in cash benefits under SSI. This is the first really concrete evidence of a connection between disability benefits and health insurance. People with disabilities are holding back earnings and are staying on SSI to obtain medical benefits. The issues of disability insurance and health insurance need to be considered together because they are inextricably linked.
-
The other side of the link between disability benefits and health insurance is what is called "job lock." People with disabilities who are working and do not have private health insurance keep working past the point where they should in order to keep their health insurance. The question that follows is: what does this link mean in terms of future role of the program. The problem could be compounded by the trend in the
-
labor market toward more part-time jobs, which have traditionally carried no health insurance. People with disabilities are overrepresented in part-time jobs. Moreover, the ADA has civil rights protections for getting a job, but health insurance protection was not included in the final legislation.
-
When all these factors are put together, two questions arise: What do they mean for program growth, and what could they mean for the Health Care Financing Administration, which manages the Medicaid and Medicare programs? Accelerating health care costs and the growing difficulty for a person with severe medical problems in getting health insurance in the private market are likely to be contributing to the growth of the disability rolls. However, empirical analysis does not provide hard evidence of that relationship. On the other hand, people with disabilities use part-time jobs as a mechanism to restrain their earnings in the SSI programs in states where they can retain their Medicaid benefits. Therefore, in some ways all roads to public policy are linked through the health insurance mechanism.
-
Some have suggested that if the system is not broken, why try to fix it. The system may not be broken, but there certainly is room for bringing it up to date and making it ready for the next century. The system would benefit from incremental improvements, both in the medical listings and in the functional assessment measures. The concern of this workshop is how to measure or improve the measurement of functional capacity as it relates to work. The decision process is complex, requiring a great deal of evidence and assessment. It is important to continue to update the medical listings and perhaps incorporate, as appropriate, assistive technology or changes in the environment that have become pervasive enough that they may warrant altering the threshold within the medical listings. Also, the quality of assessments of residual functional capacity as well as the assessment of age, education, work experience, and the demands of jobs in the national economy all need reexamination.











