| This page in the original is blank. |
1
Introduction
Background
In May 1998 the National Institutes of Health asked the National Academy of Sciences/National Research Council to assemble a group of experts to examine the scientific literature relevant to work-related musculoskeletal disorders of the lower back, neck, and upper extremities. A steering committee was convened to design a workshop, to identify leading researchers on the topic to participate, and to prepare a report based on the workshop discussions and their own expertise. In addition, the steering committee was asked to address, to the extent possible, a set of seven questions posed by Congressman Robert Livingston on the topic of work-related musculoskeletal disorders. The steering committee includes experts in orthopedic surgery, occupational medicine, epidemiology, ergonomics, human factors, statistics, and risk analysis.
This document is based on the evidence presented and discussed at the 2-day Workshop on Work-Related Musculoskeletal Injuries: Examining the Research Base, which was held on August 21 and 22, 1998, and on follow-up deliberations of the steering committee, reflecting its own expertise. We note the limitations of the project, both in terms of time constraints and sources of evidence.
Although reports on the number of work-related musculoskeletal disorders vary from one data system to another, it is clear that a sizable number of individuals report disorders and lost time from work as a result of them.1 For example, the Bureau of
Labor Statistics (1995) has reported that in 1 year there were 705,800 cases of days away from work that resulted from overexertion or pain from repetitive motion. Estimated costs associated with lost days and compensation claims related to musculoskeletal disorders range from $13 to $20 billion annually (National Institute for Occupational Safety and Health, 1996; AFL-CIO, 1997). The multiplicity of factors that may affect reported cases—including work procedures, equipment, and environment; organizational factors; physical and psychological factors of the individual; and social factors—has led to much debate about their source, nature, and severity. In light of the ongoing debate, an extensive internal review of the epidemiological research was recently done by the National Institute for Occupational Safety and Health (Bernard, 1997). That study is part of the work that was considered by the steering committee.
The charge to the steering committee, reflected in the focus of the workshop, was to examine the current state of the scientific research base relevant to the problem of work-related musculoskeletal disorders, including factors that can contribute to such disorders, and strategies for intervention to ameliorate or prevent them. Approximately 110 leading scientists were invited by the steering committee to participate in the workshop, and 66 were able to attend. The attendees represented the fields of orthopedic surgery, occupational medicine, public health, epidemiology, risk analysis and decision making, ergonomics, and human factors (see Appendix A in Part II). Several attendees presented prepared papers; many others presented oral and written responses to the papers or comments on the field of inquiry. Two criteria guided the selection of invitees: that they are involved in active research in the area and that the group, overall, represent a wide range of scientific disciplines and perspectives on the topic.
In designing the workshop, the steering committee considered several approaches to framing the topics. After careful consideration, we chose not to have the presentations focus on specific parts of the body and associated musculoskeletal disorders. Rather, we organized our examination of the evidence—and the workshop discussions (see agenda, Appendix B in Part II)—to elucidate the following sets of relationships between factors that potentially contribute to musculoskeletal disorders: ( 1) biological responses of tissues (muscles, tendons, and nerves) to biomechanical stressors; (2) biomechanics of work stressors, considering both work and individual factors, as well as internal loads; (3) epidemiological perspectives on the contributions of physical factors; (4) non-biomechanical (e.g., psychological, organizational, social) factors; and (5) interventions to prevent or mitigate musculoskeletal disorders, considering the range of potentially influential factors. Our belief was that this approach would provide a framework for reviewing the science base for each set of relationships, as well as the wider interactions among the sets. This approach allowed us to take advantage of both basic and applied science and a variety of methodologies, ranging from tightly controlled laboratory studies to field observations. As a result, we considered sources of evidence that extend well beyond those provided by the epidemiological literature on which the public discussion has focused.
Discussions in each of the five topics (all but topic 4) revolved around a paper commissioned for the workshop and comments of invited discussants; a panel format was used to address the epidemiology of physical factors (topic 4), given the availability of recent reviews of literature on this topic.
The next section presents a conceptual framework integrating the factors thought to be related to the occurrence of musculoskeletal disorders. We used this framework to select and organize topics covered in the workshop.
Framework of Contributors to Musculoskeletal Disorders
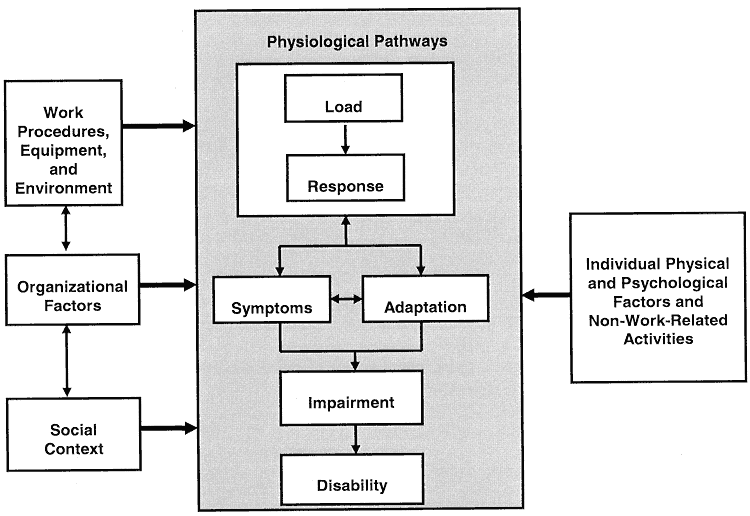
Figure 1 outlines a broad conceptual framework, indicating the roles that various work and other factors may play in the development of musculoskeletal disorders. This framework serves as a useful heuristic to examine the diverse literatures associated with musculoskeletal disorders, reflecting the role that various factors—work procedures, equipment, and environment; organizational factors; physical and psychological factors of individuals; non-work-related activities; organizational factors; and social factors—can play in their development. Its overall structure suggests the physiological pathways by which musculoskeletal disorders can occur or, conversely, can be avoided.
The central physiological pathways appear within the shaded area of the figure. It shows, first, the biomechanical relationship between load and the biological response of tissue. Imposed loads of various magnitudes can change the form of tissues throughout the day due to changes in fatigue, work pattern or style, coactivation of muscle structures, etc. Loads within a tissue can produce several forms of response. If the load exceeds a mechanical tolerance or the ability of the structure to withstand the load, tissue damage will occur. For example, damage to a vertebral end plate will occur if the load borne by the spine is large enough. Other forms of response may entail such reactions as inflammation of the tissue, edema, and biochemical responses.
Biomechanical studies can elucidate some of these relationships. Biomechanical loading can produce both symptomatic and asymptomatic reactions. Feedback mechanisms can influence the biomechanical loading and response relationship. For example, the symptom of pain might cause an individual to recruit his or her muscles in a different manner, thereby changing the associated loading pattern. Adaptation to a load might lead individuals to expose themselves to greater loads, which they might or might not be able to bear. Repetitive loading of a tissue might strengthen the tissue or weaken it, depending on circumstances. The symptom and adaptation portions of the model can interact with each other as well. For example, symptoms, such as swelling, can lead to tissue adaptations, such as increased lubricant production in a joint. These relationships can be described in mathematical models that distinguish external load (e.g., work exposure) from internal load (dose) and illustrate cascading events, whereby
responses to loads can themselves serve as stimuli that increase or decrease the capacity for subsequent responses.
The responses, symptoms, and adaptations can lead to a functional impairment. In the workplace, this might be reported as a work-related musculoskeletal disorder. If severe enough, the impairment would be considered a disability, and lost or restricted workdays would result.
To the left of the shaded area in Figure 1, the framework shows environmental factors that might affect the development of musculoskeletal disorders, including work procedures, equipment, and environment; organizational factors; and social context. For example, physical work factors (reaching, close vision work, lifting heavy loads) affect the loading that is experienced by a worker's tissues and structures. Organizational factors can also influence the central mechanism. Although little studied, hypothetical pathways also exist between organizational influences and the biomechanical load-response relationship, as well as the development of symptoms. For example, time pressures to complete a task might induce carelessness in handling a particular load, with consequent tissue damage. The organizational culture can also create an incentive or a disincentive to report a musculoskeletal disorder or to claim that the impairment should be considered a disability. Social context factors, such as a lack of means to deal with psychological stress (e.g., no spousal support), might also influence what a worker reports or even the worker's physiological responses.
To the right in Figure 1, the framework shows the influence of individual physical and psychological factors, as well as non-work-related activities, that might affect the development of musculoskeletal disorders. For example, psychological factors can affect a person's identification of a musculoskeletal disorder or willingness to report it or to claim that the impairment is a disability. Physical factors might involve reduced tissue tolerance due to age or gender or disease states, such as arthritis, which can affect people's biochemical response to tissue loading.
This framework can accommodate the diverse literatures regarding musculoskeletal disorders by characterizing the pathways that each study addresses. For example, an epidemiological investigation might explore the pathways between the physical work environment and the reporting of impairments or the pathway between organizational factors and the reporting of symptoms. An ergonomic study might explore the pathways between work procedures and equipment and the biomechanical loads imposed on a tissue. This framework also focuses attention on the interactions among factors. For example, the combination of a particular set of work procedures and organizational factors might produce an increase in disorders that neither would alone produce.
Looking at the evidence as a whole provides a sounder basis for understanding the overall dimensions of the problem of work-related musculoskeletal disorders than restricting an examination to any one factor or kind of evidence. It also places individual studies in context, by showing the factors and pathways that they do and do not address.
2
State of the Evidence
The goal of the steering committee was to examine the current state of the scientific research base relevant to the problem of work-related musculoskeletal disorders. As mentioned, we identified five major topics, each of which has been the subject of scientific examination. The resulting literature represents a wide variety of research designs, measures, apparatuses, and modes of analysis. Our representation of the science base therefore covers a wide range of theoretical and empirical approaches. For example, there are highly controlled studies of soft tissue responses that are based on work with cadavers, animal models, and human biomechanics; survey and cross-sectional studies that examine the relationship between musculoskeletal disorders and work, organizational, social, and individual factors; and experimental, quasi-experimental, and time-series studies that are designed to examine the effects of various interventions.
In order to make sense of such a multifaceted body of research, we have extended our analysis beyond the traditional criteria used in epidemiological studies; we rely, instead, on five commonly accepted criteria for establishing causal linkages among factors. Following the discussion of the causal criteria, this review of the evidence is divided into five sections. The first, soft tissue responses to physical stressors, covers material that corresponds to the load and response boxes in Figure 1. The second section, work factors and biomechanics, discusses the biomechanics of the load-response relationship and examines the contributions of work procedures, equipment, and environment to this relationship. The third section covers the epidemiological
evidence relating biomechanical factors at work to musculoskeletal disorders. The fourth section examines the state of the evidence regarding the contributions of the non-biomechanical factors listed in Figure 1—organizational, social, and individual. The final section presents a discussion of workplace interventions; this section covers material relevant to all factors represented in the figure.
Criteria to Determine Causality
Five criteria are normally considered in determining whether scientific evidence supports a causal claim as internally valid—that is, that the purported cause was uniquely responsible for the effect (Campbell and Stanley, 1966; Cook and Campbell, 1979; Cordray, 1986; Einhom and Hogarth, 1986).
- The first criterion, temporal ordering, requires that the cause be present before the effect is observed. It can be assessed by examining the type of control the investigator has over the timing and delivery of the causal agent in an experimental study (e.g., conducted under controlled conditions) and the course of events in an observational study (e.g., one involving systematic observation of events in the real world).
- The second criterion requires that the cause and effect covary. For example, when no force is applied to a tendon, it remains in a relaxed state; in the presence of the cause (a force), the tendon responds.
- The third criterion involves the absence of other plausible explanations for the observed effect. To the extent that confounding factors have been controlled by the design of the experiment or observation, other explanations for the observed effect are less likely. In some studies, it is possible to use random assignment of participants to conditions to control the influence of other factors, but this is not the only means for achieving control. In making a determination of whether factors other than the experimentally manipulated factor (e.g., ergonomic redesign) offer plausible explanations for the observed effect (e.g., a lower average level of sick days in the post-redesign period of observation), it is necessary to identify and test whether other plausible factors might have been operative, mimicking the effect of the target cause (e.g., change in sick leave policy, turnover in personnel). If no other such causes can be shown empirically to be responsible for the effect, it is reasonable to attribute the effect to the cause under investigation. Note that this criterion stipulates that other causal factors need to be plausible, not merely logically possible. Claims of plausibility have merit to the extent that they can be empirically supported.
- The fourth criterion, temporal contiguity, amplifies the first (temporal ordering). To the extent that the effect follows the cause closely in time, the plausibility that other factors are operative is reduced. For example, if a tendon reacts immediately to the presence of force, it is unlikely that other factors (e.g., gravitational pull) are responsible for the sudden elongation. On the other hand, if there is a delay between
- the application of force and the response that cannot be explained by the biomechanical mechanisms associated with tendon structures, other factors may be operative, weakening the strength of the causal claim.
- The fifth criterion is that the size of the cause is related to the size or magnitude of the effect: that is, there is a congruity between the cause and effect. More specifically, a small force or small change in the workplace ought to correspond to a small effect and a large force or major change (e.g., multiple components of the workplace are altered) ought to be accompanied by a large effect (e.g., failure of a tissue or a substantial reduction in work-related injuries). When results from experiments or quasi-experiments violate these expectations, it is necessary to examine how the effect was modified (either enhanced, in the case of a small cause that leads to a large effect, or dampened, in the case of a large cause that produces a small effect). To the extent that a compelling explanation for these anomalies cannot be provided (e.g., delays in the implementation of a workplace redesign), it is plausible to assume that other processes (not related to the suggested cause) are responsible for some or all of the effect.
By applying these criteria to evaluate the credibility of scientific evidence, one need not place heavy emphasis on the types of research design that have been used in a given study. It is a disciplined way to take advantage of the research provided by a wide variety of methods and, thus, it has substantial implications for the manner in which a science base is considered. Rather than focusing on a study's design features, one considers the pattern of data for each study and its associated design on a case-by-case basis. For some studies, it is readily apparent that even the minimal causal criteria cannot be substantiated (e.g., it is impossible to establish that the cause came before the effect). For others, even when there is no conventional experimental control group (created through random assignment), observations before and after the introduction of an intervention can produce valid claims if coupled with other evidence about the change and with probes concerning the presence or absence of other plausible explanations.
In complex domains, single studies can seldom provide a conclusive verification of a causal proposition. It is through replication and synthesis of evidence across studies, preferably with studies that use a variety of methods (each with different strengths and weaknesses), that causal claims gain their inferential strength. In performing such syntheses, greatest weight should be given to the evidence from studies that most completely satisfy the five criteria specified above. Poorly conceptualized and executed studies may have little to offer for assessments of causal claims. In contrast, the evidence from a few well-conceived and well-executed studies can strongly outweigh the "noise" created by a large number of studies that do not satisfy the five criteria for causality. (A similar argument was made in deliberations about the evidence related to the effectiveness of a set of complex public health programs; see Normand et al., 1995).
Finally, inferential strength is gained by examining the evidence from a variety of theoretical perspectives (as well as a variety of research methods), as specified in the framework provided in Figure 1. Establishing that biological and biomechanical pro-
cesses influence tissues, that these forces are present in some work environments or work-related tasks, that their presence is associated with musculoskeletal disorders, and that their influence can be reduced by workplace redesign (or other interventions) should provide a greater understanding of the evidence than can be gained by considering each factor separately. The findings presented in the rest of this section reflect the steering committee's application of the criteria to the research literature.
Soft Tissue Responses to Physical Stressors
Several well-established findings are supported by the papers of Rempel et al. (1998) and Ashton-Miller (1998), presented at the workshop. While certain loads can be tolerated and adapted to, all soft tissues, including muscle, tendon, ligament, fascia, synovia, cartilage, intervertebral disc, and nerve, fail when subjected to sufficient force. Data from cadaver studies provide ranges within which such failures occur, and animal models of some tissue provide support for the laboratory data. Even at levels of force clearly below the failure level, however, there is scientific evidence, from these types of studies, that tissue response to deformation can produce inflammation, failure at microscopic levels, and muscle fatigue.
Injuries to muscle from single-event and repetitive contractions have been documented in humans and in animal models. Local muscle fatigue occurs at low contraction levels when maintained for long periods. Inflammatory muscle responses have been documented in humans subjected to repetitive or prolonged loading. Muscles also are affected by individual factors, such as age and level of conditioning. These effects involve not only the tissue, but also the neuromuscular control system.
Ligaments and tendons also fail from single or repetitive loading. For tendons, disorders can occur at the insertion into the bone, in the tendon proper, or at the junction between tendon and muscle. Animal models have demonstrated the development of inflammatory responses in the tendon sheath and insertion areas (tendinitis and tendinosis).
Cartilage is a tissue known to deteriorate when subjected to abnormal loads. Intervertebral discs, which are a special type of cartilage, fail when loaded, as fissures develop within the substance. Age, gender, and other individual factors influence these processes.
Nerves subjected to tension or compression will respond with pain, dysfunction, and ultimately permanent tissue changes. There is good scientific evidence about both acute and chronic effects of nerve compression and about the effects of vibration on nerves. Critical pressure and duration values have been established for acute nerve compression, but they have not yet been established for chronic compression.
It is important to note that many of the well-designed experimental studies in animals and cadavers have been successfully replicated. The applicability of their findings to humans in the workplace has been addressed by observations of comparable effects in exposed humans. On all of these highly controlled studies, the causal criteria
are met: the load or stress occurs before the response, confounding factors are controlled to eliminate other plausible responses, and the size and temporal proximity of the load and effect can be consistently measured and predicted.
Work Factors and Biomechanics
The relationships among external work factors, loads, and responses (see Figure 1) have been studied extensively, using both theoretical models and human laboratory studies. Theoretical models make use of mathematical models that are widely applied to design mechanical structures in aircraft, automobiles, bridges, and buildings. Some human studies involve postmortem techniques to examine geometry and mechanical properties of tissues and their response and adaptation to various loads. Other human studies use force gauges and electromyography to directly measure forces produced in given activities. It has been shown that activities of work, daily living, and recreation often produce loads that approach the mechanical limits of soft tissue (discussed in the preceding section) and in some cases for some individuals exceed those limits. Up to certain limits, some tissues, such as muscle tissue, are able to adapt to repetitive loading; while the ability of other tissues, such as nerve tissue, to adapt is much less (see discussion of these in Radwin and Lavender, 1998). In general, the results of human studies meet the criteria of temporal order, temporal contiguity, covariance, and the absence of other plausible explanations.
Work entails positioning and exertion of the body to accomplish required tasks. In addition, exertion of the body against an external object may impose significant contact stresses on the surface of the body, which are transmitted to underlying tissues. If the work object vibrates, some of that vibration will be transmitted to the body. Exertion, posture, contact stress, vibration, and varying temperatures are external stressors. The intensities of the exertions are related to the weight, resistance, drag, inertia, and reaction forces of the work objects. Postures are related to the geometry of the workplace and the size of the worker; they range from neutral positions to the limits of the range of motion. Contact stresses are related to force and area of contact. Vibration is related to how a tool is powered, balanced, and mounted. Low temperatures are related to ambient air temperature and to the thermal conductivity of handles and gloves. If ambient air is cold or if a work object is cold, a worker's hand will be cooled. The frequency and duration of exertions and postures are related to production rates and quotas. These exposures may occur not only at work, but also in various recreational and living activities.
These relationships are supported by basic Newtonian mechanics, and they can be observed directly (Chaffin and Andersson, 1990). For example, posture is related to the location of parts, assemblies and controls, size and shape of handles, orientation of work objects, and visual requirements. Posture is also affected by obstructions that workers must see or reach over, under, or around. Posture variations can be observed within a given work situation, but this variation is small in relation to that attributed to
the workstation. If work is located overhead, as often occurs in manufacturing settings, workers will have to stand with their hands above their heads. If the work is located on the floor, workers may have to bend or stoop. It has been observed that work capacity is greatly reduced at very high and very low locations (Snook and Ciriello, 1991; Marras et al., 1997).
It can be shown that the force required to support a work object is related to weight and friction (Armstrong, 1985). Similarly, forces required to depress the keys on a keyboard are related to the stiffness of the keys (Armstrong et al., 1994). However, there may be significant variations from person to person; one worker may strike the keys of a keyboard very forcefully, while another uses a light touch.
It can also be shown that the frequency and duration of exertions are related to work standards and quotas. Production rates are based on estimates of the time required to perform a given task. Allowances may be added to provide time for process variations and to provide sufficient recovery time. Pay incentives, which encourage faster work, may result in insufficient recovery time. The effect may be compounded by production quotas that necessitate overtime. Although external stresses can be produced by activities of recreation and daily living, the duration of exposures rarely equals the 40 to 60 hours per week that commonly occur in work settings.
External loads impose internal loads on underlying tissues (e.g., muscles, tendons, tendons sheaths, bones, ligaments, and nerves). The relationship between external and internal loads has been demonstrated with biomechanical models and observed using instrumentation. For example, intervertebral disk pressures of the lumbar spine up to 1.6 MPa have been calculated and measured. Internal finger flexor tendon tensions have been shown to be three to five times greater than external finger forces (Chaffin and Andersson, 1990).
The relationship between external and internal loads is also based on Newtonian mechanics. Internal loads have been shown to produce mechanical, physiological, and psychological responses, such as tissue deformation, altered metabolism, altered circulatory patterns, and perceived exertion (see discussion of soft tissue responses above). Depending on the duration and intensity of the loads and recovery time, the responses may cause discomfort and impair performance. Fatigue is one such example. While fatigue can significantly affect worker comfort and impair work performance, it is a transient response that dissipates rapidly when work stops. In some cases, however, loads are large enough or last long enough to stimulate acute tissue disorders. Although damaged tissue stimulates a healing response, healing may not occur if the loads continue to be applied.
These processes have been studied in all parts of the body. For example, exertions of the hand entail a complex mechanical equilibrium of the muscles in the forearm and hand that open the fist and those that close the fist. Exertions of the trunk entail a complex equilibrium among all of the muscles in the back and extremities.
The relationships among external loads and internal loads and mechanical, physiological, and psychological responses have been studied extensively, using simulation, direct instrumentation, indirect instrumentation, and epidemiological studies. The
studies support several important conclusions that are in accord with the proposed multifactorial framework presented above (see Figure 1) and that provide a basis for evaluating and controlling biomechanical stresses in the workplace:
- There are numerous ways of measuring and characterizing external loads. For example, force can be measured in terms of the weight of parts, tool reaction force, perceived exertion, muscle electrical activity, or observer ratings. Posture can be measured in terms of joint angles, perceived exertion, observer ratings, or work locations (e.g., keyboard height).
- Internal loads can be estimated by using external loads. For example, a worker must bend or stoop to lift an object from the floor; a worker will exert more force on a stiff keyboard than a light touch keyboard. Understanding these relationships allows prediction of internal loads.
- Predicted internal loads generally agree with measured internal and external loads. For example, measurements of pressure at the L5S1 intervertebral disk agree with predicted values (Marras and Granata, 1997). Predictions of finger flexor tendon loads generally agree with measurements of tendon loads. Measurements of muscle loads using electromyography generally agree with predicted values.
- The importance of a particular response varies from one part of the body to another. For example, tensile, contact, and shear loads and fluid pressures are particularly important in the wrist. It has been shown that internal loads produced on tendons by repetitive handwork are sufficient to cause significant elastic and viscous strain. These loads can be associated with pathological changes in adjacent synovial and nerve tissues. Muscle force and interjoint pressures are particularly important in the low back.
- Although external loads can be measured on continuous scales, most epidemiological studies consider only two levels of exposure—high and low. This approach reflects the operational realities of field studies, which are often limited by availability of workers, exposure groups, and stability of work settings. However, continuous scales would be useful for primary prevention and work design.
Epidemiological Evidence that Physical Factors Can Cause Musculoskeletal Disorders
One of the factors prompting our review of the scientific relationship between biomechanical stressors at work and the occurrence of musculoskeletal disorders has been controversy regarding human studies in working populations. These studies, although numerous, have used diverse methods for measuring both exposure to mechanical factors and the health outcomes of interest. As results have not converged in every regard, some individuals have discounted some or all of the collective evidence.
In an effort to clarify this situation, the National Institute of Occupational Safety and Health (NIOSH) undertook a review of the epidemiological literature (Bernard, 1997), with the intent of examining critically the strengths and weaknesses of available
studies. The study attempted to identify both those areas for which there is strong evidence for convergence of results linking an exposure to musculoskeletal disorders and those areas for which the evidence is weaker or divergent.
A highly representative sample of respected epidemiologists was invited to the workshop to discuss the NIOSH review and the epidemiological studies considered. Seven of these experts from within and outside the field participated in a panel discussion. Both written and presented comments of the panel have been further considered and extensively discussed by the steering committee (using the approach to evidence outlined above). See Evanoff, 1998; Franzblau, 1998; Gerr, 1998; Punnett, 1998; Sandler and Blume, 1998; and Wegman, 1998.
These presentations and discussions led us to the following summaries of the scientific evidence:
- Strong associations between measured biomechanical stressors at work and musculoskeletal disorders were observed in most studies; however, temporal contiguity between the stressors and onset of effects, as well as evidence of amelioration after reduction of stressors, could not always be established, nor could the clinical course of the observed effects. This shortcoming, though inherent to practical requirements of such research, makes it difficult to make strong causal inferences on the basis of the evidence from any individual study.
- Methods used for the assessment of exposures and health outcomes vary, rendering the task of merging and combining evidence more challenging than in some other areas of occupational risk assessment. But this variability does provide the benefit of multiple perspectives on a common set of problems.
- It is not feasible to assess the relative contribution of task and other factors to musculoskeletal disorders in the general population. In addition, high rates of workplace participation complicate characterization of the non-working population (e.g., the prevalence of health-related reasons for not working). Therefore, evidence about the prevalence and incidence of even the most common musculoskeletal disorders in non-working populations, which could be readily compared to results of epidemiological studies of workers, is largely lacking.
- Some published studies that show associations between biomechanical stressors and musculoskeletal disorders are difficult to interpret because of the possibility that plausible but unmeasured factors could explain some or all of the observed differences in rates of musculoskeletal disorders. In other words, whether biomechanical stressors or something else have caused higher rates of musculoskeletal disorders could not be definitively answered. This problem is common to epidemiological research in general.
Despite these limitations, however, the steering committee reached the following conclusions:
- Restricting our focus to those studies involving the highest levels of exposure to biomechanical stressors of the upper extremity, neck, and back and those with the
- sharpest contrast in exposure among the study groups, the positive relationship between the occurrence of musculoskeletal disorders and the conduct of work is clear. The relevant studies have not precisely determined either the causal mechanical factors involved nor the full clinical spectrum of the reported musculoskeletal disorders (which have often been lumped together nonspecifically as musculoskeletal disorders of a body region); nonetheless, those associations identified by the NIOSH review (Bernard, 1997) as having strong evidence are well supported by competent research on heavily exposed populations. Examples include the excesses of musculoskeletal disorders of the upper extremities among sawyers and auto assembly workers and the excesses of musculoskeletal disorders of the back among materials handlers and health care workers who lift patients.
- There is compelling evidence from numerous studies that as the amount of biomechanical stress is reduced, the prevalence of musculoskeletal disorders at the affected body region is likewise reduced. This evidence provides further support for the relationship between these work activities and the occurrence of musculoskeletal disorders.
- Evidence of a role for biomechanical stress in the occurrence of musculoskeletal disorders among populations exposed to low levels of biomechanical stressors remains less definitive, though there are some high-quality studies suggesting causal associations that should serve as the basis for further investigation. In cases of low levels of biomechanical stress, the possible contribution of other factors to musculoskeletal disorders is important to consider. Many of these factors are discussed below.
Epidemiological Evidence That Non-Biomechanical Factors Can Cause Musculoskeletal Disorders
The framework in Figure 1 shows individual, organizational, and social factors as sources of variation that might directly affect the physiological pathways leading from tissue load, through impairment, to disability. This section examines the evidence for and against these relationships.
We note two points about most musculoskeletal disorders: (1) it is highly unlikely that all individuals have equal susceptibility to any disorder, and (2) it would be unusual if organizational aspects of the workplace and social support factors had no role in either the incidence or the time pattern of a disorder. The issues of interest are the magnitude of such effects, relative to biomechanical effects, and the nature of interactions between biomechanical, individual, organizational, and social factors.
The literature on non-biomechanical factors is highly variable in a number of ways that complicate comparisons across studies. First, the number of non-biomechanical factors is potentially unlimited, and different studies typically have examined different, although often overlapping, sets of factors. Second, many of the variables of interest, such as job content, job control, or social support, lack consensus on standard measurement and procedures. Measurement scales are often borrowed from studies of conditions
other than musculoskeletal disorders. As a result, different studies of the same topic use different measures and even different disorders, or different precursors and endpoints for the same disorder. Third, both cross-sectional and longitudinal research techniques have been used, with a variety of sample sizes and with different criteria for causality. This variability is a barrier to mechanical aggregation of studies, a task that requires careful attention to sample size and measurement error. Diversity, however, can be an asset if the findings of a variety of studies reinforce one another. Testing for such convergent validity requires an interpretative framework that acknowledges the potentially complementary strengths and weaknesses of different research methodologies.
Below we review the evidence on individual, organizational, and social factors (see Faucett and Werner, 1998, for supporting material). No evidence was presented that malingering is a large contributor to the overall incidence of musculoskeletal disorders, although it is likely there are individuals who abuse the medical and social systems in this way.
Individual Factors
Faucett and Werner (1998) and the workshop discussants agreed that individuals differ in their susceptibility to the incidence, severity, and etiology of musculoskeletal disorders. Most of the reviewed papers studied upper-extremity musculoskeletal disorders, although some focused on the low back. For some individual factors (age, prior medical conditions) there is high plausibility for the influence of biological mechanisms that could account for the strong relationships observed in epidemiological studies. For a number of other factors, there is equally strong epidemiological evidence, but the mechanism is less clear (body mass index, gender). Still other factors are less well established (genetics, general conditioning) or are limited to a single disorder (wrist physical dimensions for carpal tunnel syndrome).
Overall, the studies complement and reinforce one anothers' conclusions for particular variables that have been studied repeatedly (e.g., aging). However, it is important to note that these relationships, although often statistically significant, rarely show high predictive value. Most studies explain a relatively small percentage of the overall variance in the outcome measures. This is not a paradoxical result, but simply a reflection of the fact that even weak predictors will be statistically significant if they are measured well in large samples.
Organizational and Social Factors
A number of studies have grouped non-biomechanical factors at the workplace and within social support groups as ''psychosocial factors." These are often the factors directly associated with levels of workplace stress, such as job content and demands, job control, and social support. However, variables such as job satisfaction or job enjoyment have also been included. The effects associated with these factors have been examined in the NIOSH review (Bernard, 1997), the commissioned paper pre-
pared for the workshop (Faucett and Werner, 1998), and in a number of other recent comprehensive reviews (particularly from Europe), with quite similar conclusions (see, e.g., Bongers et al., 1993).
Organizational variables of job content and job demands include such factors as job variety, job identity, workload, and time pressure. In the study and evaluation of these variables, both objective measures and subjective perceptions of workers have been used; the latter have been collected in the form of workers' responses on scales. Generally speaking, poor job content (e.g., poor task integration, lack of task identity) and high job demands have been found to be related to higher rates of musculoskeletal disorders. In some cases, these factors covary with physical factors. For example, high levels of time pressure can increase speed of movement and hence the dynamic forces acting on tissues. The effect of job control, also called decision latitude, on reports of musculoskeletal disorders has received moderate support from the literature.
Social support is seen as a mediating variable in studies of psychological stress; it finds strong support in the NIOSH review and the commissioned review, but somewhat less in other reviews presented by workshop discussants. Across organizational and social variables, psychological stress has some causal plausibility, but in general its biological plausibility is weaker than for some other individual and biomechanical factors. Again, the conclusion is that even when statistically significant, these factors are not large.
Interventions
There are a variety of actions that can be taken in the workplace to eliminate or reduce the risk of musculoskeletal disorders. According to the commissioned paper by Smith et al. (1998:2): "These include engineering redesigns, changes in work methods, administrative controls, employee training, organized exercise, work hardening, personal protective equipment, and medical management to reduced exposures." Numerous assessments have been undertaken to determine whether such actions, singly or taken as a program of risk reduction, actually do result in observed benefits to employees and employers.
Intervention studies differ from their epidemiological counterparts in at least one fundamental way: in intervention studies, the effects of occupational risk factors are examined by manipulating attributes of the work condition. One approach is to use the standard experimental paradigm. This involves creating an intervention group that receives one or more of the actions listed above and a control group that receives alternative forms of the intervention or "business as usual." Another research design is the before-and-after paradigm. When multiple observations are obtained before and after introduction of the intervention, the before period serves as the control condition from which the effects of changes in musculoskeletal disorders in the post-intervention period can be assessed. This design is referred to as an interrupted time-series quasi-experiment (Campbell and Stanley, 1966). Although it does not involve random as-
signment to conditions, it represents a relatively strong research design that is often able to provide internally valid evidence about the causal effects of an intervention. That is, because of the control that is exercised over the presentation of the cause (e.g., a work-related design), intervention studies generally fulfill the temporal ordering criteria (i.e., the cause precedes the effect).
Exposure to the cause can be controlled either through random assignment of conditions or through timing of the introduction of the intervention. As with most intervention research, an investigator's ability to control the influence of all plausible threats to validity is reduced as the site of the study moves from the laboratory to the workplace. However, generalization (i.e., external validity) is enhanced for studies conducted in "real-world" settings. Thus, there is a constant tradeoff between internal and external validity.
Overall, there is a great deal of diversity regarding the nature and quality of research methods used in intervention studies (Smith et al., 1998). There are a number of laboratory studies involving the use of random assignment of participants to interventions. However, these studies often involve participants who differ from the target workers of interest on key attributes (e.g., study participants have included well-conditioned athletes). Furthermore, the experimental arrangements are not always representative of the types of work-related tasks that are of most interest. The duration of exposure to a stressor is often short and therefore unrepresentative of the duration and intensity of exposure in workplaces. In assessing the effects of exposure to an intervention, laboratory-based studies often have to rely on short follow-up assessments and measures that reflect symptoms rather than the end-states of most interest (e.g., sick days). As such, the relevance of these studies, despite some of their desirable features (e.g., random assignment), is often questioned.
Field studies conducted in work environments overcome some of the shortcomings of the laboratory studies because of greater realism of the interventions that are tested, longer exposure to the redesign efforts, longer follow-up intervals, and the measurement of important end-states. A few of these studies are classified as true experiments (i.e., experimental versus control conditions); the remainder are designated as less well-controlled studies. But within this latter group, several high-quality quasi-experiments have been undertaken that provide relatively convincing evidence about the effects of multicomponent intervention actions (Aaras, 1994; McKenzie et al., 1985; Jones, 1997). Not only do these studies provide data for extended periods before and after the introduction of the intervention package, they often provide additional evidence about the operation of the causal factor (e.g., workplace redesign) in reducing the amount of load or stress on muscles. Moreover, the patterns of outcome data fulfill the conditions for causal inference: that is, they show sharp reductions in end-state measures following introduction of the intervention (indicating covariation, temporal ordering, temporal contiguity), the size of the reduction (effect) corresponds to the size of the cause (indicating cause-effect congruity), and few (if any) rival explanations can be invoked to explain the effects.
Another class of field studies involves comparisons of alternative forms of intervention (e.g., back school versus exercise) rather than pure control group conditions, where the participants receive little or no specialized attention. Given that two or more interventions are contrasted, each of which might have beneficial effects, there is an increased chance that the results will show no comparative advantage of either intervention or mixed results, where one intervention is superior on some but not all outcome measures.
In field settings, it is not uncommon for an intervention to involve multiple actions to participants in the intervention group. Under this circumstance, it is difficult to determine which of the actions was responsible for any observed effect. It may be tempting to criticize a study because the individual influence of each action could not be uniquely identified. However, from the perspective of the internal validity of the study, this criticism is not strictly applicable. Rather, it is possible to conclude that the design of the study produced valid findings about the "package" of actions. Labeling the specific cause of the findings is an issue of construct validity, a standard that is unlikely to be achieved in actual workplace environments.
The available reviews of the literature (Smith et al., 1998; Lahad et al., 1994) have not examined all of the studies (experiments and quasi-experiments) that have appeared in the literature to date. As such, it is not possible to characterize the quality of the evidence for the full collection of studies. However, there are a number of high-quality studies that can be used to determine whether interventions can reduce the risk of musculoskeletal disorders.
The literature provides evidence that interventions, of various types and complexity, can prevent the development of musculoskeletal disorders in specific industries and occupational groups. For example, there is a set of well-controlled studies that show that hospital workers, nurses aides, and industrial workers benefited from extended exercise programs (Lahad et al., 1994). Among these benefits were greater strength, less absenteeism, and fewer days of reported lower back pain. These effects have been seen for workers with and without prior histories of back pain. Other, less well-controlled studies revealed similar benefits. There is also some minimal evidence pointing to a positive benefit of educational strategies. Other examples are found in the poultry processing and telecommunication industries, where interventions resulted in reductions in the total number of recordable repetitive trauma disorders (according to the criteria of the Occupational Safety and Health Administration [OSHA]), lost workdays, number of days of restricted activity, and employee turnover. In these latter examples, there is also some evidence that the interventions were cost beneficial for employers.
Further evidence for effective intervention is found in several well-designed studies that show that alternative hand tool designs result in improved hand and wrist posture, thereby minimizing the risk of musculoskeletal disorder. And there is some evidence that weight handling devices reduce the risk of musculoskeletal disorders (Smith et al., 1998).
Most of the industry-specific studies used multicomponent interventions (e.g., engineering controls, training, medical management, employee empowerment). Although these studies attempted to provide insights into the relative importance of each component, it is often not possible to identify those features of the overall intervention that are most critical in achieving the observed benefits.
Future Research
Although the research base contains valuable information and shows consistent patterns regarding the relationships between stressors and musculoskeletal disorders, additional research would provide a better understanding of the processes involved. Looking across the areas defined in the framework, there are five interrelated and fundamental issues that deserve additional attention by researchers:
- In all areas, additional research would shed light on the models and mechanisms that underlie the established relationships between causal factors and outcomes. For example, it is obvious that a tissue will fail when loaded above its ultimate strength. How tissue responds to repetitive loading, what triggers inflammatory responses, and how these are influenced by individual factors have not been explained in detail. A similar argument can be made for intervention studies, especially those that involve multiple components. Here, the literature shows that a "bundle" of actions can reduce the risk of musculoskeletal disorders and associated outcomes (e.g., sick days). What is less clear are the mechanisms by which changes to work procedures, equipment, environment, and organization, as well as to social and individual factors, produce the benefits.
- Along with a better understanding of the mechanisms that produce tissue failure and mechanisms that produce reductions in risks, the relationships between symptoms, injury reporting, impairment, and disability should be clarified, as well as how these relationships are influenced by individual, social, legal, and environmental factors. That is, there is a need to conduct more studies that consider multiple factors—workers generally are exposed to multiple factors—and there is likely to be significant interaction between factors.
- The literature identifies a range of procedures and equipment-related intervention strategies that can be effective. It would be helpful to know more about the relationships between incremental changes of the environmental load and incremental responses. Knowledge of these relationships could help to define more efficient and better targeted interventions.
- In order to improve the ability to assess mechanisms, change processes, and interactions among factors, it would help to have more standardization and greater detail in injury reports, better measurement of the attributes of contributors and risks, and better measurement of outcomes and other relevant variables.
- Although a good deal is known about musculoskeletal disorders, a better understanding of the clinical courses of these disorders would be possible with improved models and measures. Better understanding of the course of these disorders would provide information that would assist in formulating strategies for tertiary intervention, by altering the clinical and economic impact of musculoskeletal disorders once they have become manifest. One potential area for research is the contribution of physical conditioning and exercise to developing human resistance and resilience.
3
Seven Questions Posed by Congressman Robert Livingston
The material in Section 2 puts in perspective the state of the evidence with respect to the range of factors that could be contributing to musculoskeletal disorders and describes the extent to which there is a scientific basis for concluding that such disorders originate in the workplace and can be reduced through programmatic interventions. This section presents the steering committee's response to the seven questions posed by Representative Livingston. As our analysis has been at the level of the family of musculoskeletal disorders, our response will be provided across disorders.
Question 1: What are the conditions affecting humans that are considered to be work-related musculoskeletal disorders?
The musculoskeletal conditions that may be caused by (non-accidental) physical work activities include disorders of inflammation, degeneration, and physiological disruption of muscles, tendons, ligaments, nerves, synovia, and cartilage involving limbs and trunk. These entities are included in categories 353-355, 722-724, and 726-729 of the International Classification of Diseases (commonly referred to as ICD-9) (World Health Organization, 1977). Not every disorder in these categories may be caused by mechanical stressors, but all the major musculoskeletal disorders of interest are included in these groupings. Common examples are low back strain, tenosynovitis, and carpal tunnel syndrome.
Question 2: What is the status of medical science with respect to the diagnosis and classification of such disorders?
There is great variation in the diagnostic criteria for the many musculoskeletal disorders, ranging from clinical diagnoses based on symptoms and signs for some, to diagnoses based on structural and functional criteria for others. The diagnostic criteria used in epidemiological studies are often different from those used to make treatment decisions. This difference can lead to classification of cases for research that would be unacceptable when invasive treatment alternatives are considered, but it has little influence on the conclusion of appropriately designed epidemiological surveys. In the classification of back pain, a symptom classification is often used because the precise etiology of the painful process often cannot be identified. For specific disease entities, such as herniated disks, there are accepted diagnostic criteria that are based on clinical symptoms and signs, as well as imaging information. Similarly, there are disease entities for upper extremities for which there are accepted diagnostic criteria; for other disease entities, they are classified broadly on the basis of clinical symptoms and signs.
Question 3: What is the state of scientific knowledge, characterized by the degree of certainty or lack thereof, with regard to occupational and nonoccupational activities causing such conditions?
The relationships among work factors, biomechanical loads, and responses are supported by mathematical models and direct measurements. The mathematical models are widely accepted and applied to design mechanical structures in aircraft and automotive design. Direct measurements have been used to a lesser extent than modeling because they are potentially injurious to human subjects; however, when they have been used they generally support the biomechanical models.
It has been shown that the load forces encountered over time in normal work activities often approach the physiological and mechanical tissue limits. Limits may be exceeded as a result of a single high force or as a result of repeated loads over time. Some tissues have a greater ability to adapt to repeated loads if there is sufficient recovery time between successive loads, while other tissues, e.g., nerves, are less able to adapt.
Biomechanical loads are encountered in activities of work, daily living, and recreation. The contribution of these activities to tissue response is related to their relative duration and intensity. For most people, their main exposure is at work. There is a substantial body of epidemiological literature that shows a disproportionately high incidence of musculoskeletal disorders of all types among persons exposed to high biomechanical loads. Although there can be debate about acceptable exposure limits, there can be little disagreement about the fundamental relationship between extreme work exposures and musculoskeletal morbidity.
Question 4: What is the relative contribution of any causal factors identified in the literature to the development of such conditions in (a) the general population; (b) specific industries; and (c) specific occupational groups?
Data at the population and industry level have been collected for a variety of purposes by different groups using different methods. Some data are based on survey results, some on clinical or medical diagnoses, and some on compensation claims. In the judgment of the steering committee, it is not possible to make useful comparisons on the basis of these data.
The incidence of musculoskeletal disorders in any specific occupational group can be expected to reflect the tissue loads imposed by the work, the tissue tolerances of the mix of individuals doing it, and the other activities in their lives imposing related loads. The relative contribution of the different factors in any occupational group depends on ( 1) the strength of these relationships across the ranges of individuals and activities in that group and (2) the variability of the individuals and activities. For example, gender will not be an important predictive factor if men and women do not, on average, have different tissue tolerances for the loads imposed in that occupational group or if workers in the group are overwhelmingly men or women. The relative contribution in a specific industry will, similarly, depend on the mix of individuals and tasks in it. Unfortunately, measurements of the relevant features of individuals and tasks are typically unavailable, limiting our ability to assess the relative contribution of different factors across groups. The evidence shows that the incidence of musculoskeletal disorders is higher among individuals who perform activities that exceed tissue tolerances. Generally speaking, the more that they perform those activities, the greater are their risks for such disorders.
Question 5: What is the incidence of such conditions in (a) the general population; (b) specific industries; and (c) specific occupational groups?
Current knowledge about the incidence of each of the conditions described in Question 1 in the general adult population is limited because (1) the conditions are clinically diagnosed, typically in doctors' offices; (2) diagnostic criteria for these conditions are not uniformly applied; (3) there are no data collection systems to capture such diagnoses in the health care system; and (4) two-thirds of the adults in the general population are employed, with variable occupational risks. Those who are not employed, including those with various chronic conditions and disabilities, are not a suitable reference population. Data on industry and occupational groups are based on a wide variety of methods that have been collected for different purposes. It is the steering committee's judgment that it is not possible to make useful comparisons on the basis of these data.
Question 6: Does the literature reveal any specific guidance to prevent the development of such conditions in (a) the general population; (b) specific industries; and (c) specific occupational groups?
Specific interventions can affect the reported rate of musculoskeletal disorders in specific industries and for specific occupations. Interventions can also reduce reports of musculoskeletal disorders, the presence of risk factors, and the reporting of comfort and pain associated with work. It is also clear that the effectiveness of interventions can be
improved if they are tailored to specific occupations and work settings. There is a dearth of data on interventions in the general population.
Question 7: What scientific questions remain unanswered, and may require further research, to determine which occupational activities in which specific industries cause or contribute to work-related musculoskeletal disorders?
Looking at this web of evidence, we have reached three major conclusions:
- Musculoskeletal disorders are a serious national problem: estimates of costs range from $13 to $20 billion annually.
- These problems are caused by work and non-work activities.
- There are interventions that can reduce the problems.
We have also identified some focused research projects, the results of which could increase the efficacy of interventions. Some of these projects would produce useful results within specific research areas; others would increase the connections among the areas. It is a strength of the science that it points to these specific opportunities (see the discussion of future research above).
4
Conclusions
The steering committee has explored the complex problem of musculoskeletal disorders in the workplace. We have supplemented our professional expertise with workshop presentations, commissioned papers and other submissions, and discussions with invited workshop participants. We find very clear signals on some topics and weaker signals on others—but little in the way of contradiction. Thus, while there are many points about which we would like to know more, there is little to shake our confidence in the thrust of our conclusions, which draw on converging results from many disciplines, using many methods:
- There is a higher incidence of reported pain, injury, loss of work, and disability among individuals who are employed in occupations where there is a high level of exposure to physical loading than for those employed in occupations with lower levels of exposure.
- There is a strong biological plausibility to the relationship between the incidence of musculoskeletal disorders and the causative exposure factors in high-exposure occupational settings.
- Research clearly demonstrates that specific interventions can reduce the reported rate of musculoskeletal disorders for workers who perform high-risk tasks. No known single intervention is universally effective. Successful interventions require attention to individual, organizational, and job characteristics, tailoring the corrective actions to those characteristics.
- Research can ( 1 ) provide a better understanding of the mechanisms that underlie the established relationships between causal factors and outcomes so that workers who are at risk can be identified and interventions undertaken before problems develop; (2) consider the influence of multiple factors (mechanical, work, social, etc.) on symptoms, injury, reporting, and disability; (3) provide more information about the relationship between incremental change in load and incremental biological response as a basis for defining the most efficient interventions; (4) improve the caliber of measurements for risk factors, outcome variables, and injury data collection and reporting systems; and (5) provide better understanding of the clinical course of these disorders.
By and large, the controversies that we observed reflect the usual disputatiousness of science, which advances when speculative challenges lead to new and clarifying results. One feature of the discourse around musculoskeletal disorders is that it sometimes involves individuals from one discipline (or subdiscipline) who reject entirely the legitimacy of research from another. The steering committee understands the claims made by these often forceful advocates of particular research ideologies. However, we respect the contributions of properly designed research conducted by the variety of disciplines needed for the topic.
The steering committee's task has been to examine the state of the evidence. As such, we have tried to assess the plausible ranges of effects for the various factors that have been studied systematically. We have, however, deliberately avoided providing recommendations for action for three reasons:
- The risk of musculoskeletal disorders depends on the interaction of person and task, as does the effectiveness of options for reducing those risks. A full specification would require much more detailed treatment of person-task combinations than is possible here. We have, instead, focused on the scientific principles that should guide the prediction and prevention of problems.
- We have not reviewed the full range of consequences of musculoskeletal disorders and interventions related to them. For example, we have not evaluated the effects of ergonomics programs on employee productivity, turnover, and morale. Nor have we examined the effects of musculoskeletal disorders on the economic and psychological well-being of injured individuals and their families. Rational decision making must consider the full set of relevant consequences.
- Rational decision making also depends on the relative importance attached to the different consequences. Different people and institutions will have different values and different opportunities for action, at the governmental, employer, and individual levels.
References
Aaras, A. 1994 The impact of ergonomic interventions on individual health and corporate prosperity in a telecommunications environment. Ergonomics 37(10): 1679-1696.
AFL-CIO 1997 Stop the Pain. Washington, DC: AFL-CIO.
Armstrong, T. 1985 Mechanical considerations of skin in work. American Journal of Industrial Medicine 8:463-472.
Armstrong, T., J. Foulke, B. Martin, J. Gerson, and D. Rempel 1994 Investigation of applied forces in alphanumeric keyboard work. American Industrial Hygiene Association Journal 55(1):30-35.
Ashton-Miller, J.A. 1998 Response of Muscle and Tendon to Injury and Overuse. Paper prepared for the Steering Committee for the Workshop on Work-Related Musculoskeletal Injuries.
Bernard, B.P., ed. 1997 Musculoskeletal Disorders and Workplace Factors : A Critical Review of Epidemiologic Evidence for Work-Related Musculoskeletal Disorders of the Neck, Upper Extremity, and Low Back. Cincinnati, OH: U.S. Department of Health and Human Services.
Bongers, P.M., C.R. de Winter, M.A.J. Kompier, and V.H. Hildebrandt 1993 Psychosocial factors at work and musculoskeletal disease. Scandinavian Journal of Work and Environmental Health 19:297-312.
Bureau of Labor Statistics 1995 Workplace Injuries and Illnesses in 1994. USDL 95-508. Washington, DC: U.S. Department of Labor.
Campbell, D.T., and J.C. Stanley 1966 Experimental and Quasi-Experimental Designs for Research. Chicago, IL: Rand McNally.
Chaffin, D., and G. Andersson 1990 Occupational Biomechanics. Second Edition. New York: John Wiley.
Cook, T.D., and D.T. Campbell 1979 Quasi-Experimentation: Design and Analysis Issues for Field Settings. Chicago, IL: Rand McNally.
Cordray, D.S. 1986 Quasi-experimental analysis: A mixture of methods and judgment. New Directions in Program Evaluation 31:9-28.
Einhorn, H.J., and R.M. Hogarth 1986 Judging probable cause. Psychological Bulletin 99(1):3-19.
Evanoff, B. 1998 Work-Related Musculoskeletal Disorders: Examining the Research Base Epidemiology: Physical Factors. Paper prepared for the Steering Committee for the Workshop on Work-Related Musculoskeletal Injuries.
Faucett, J., and R.A. Werner 1998 Non-Biomechanical Factors Potentially Affecting Musculoskeletal Disorders. Paper prepared for the Steering Committee for the Workshop on Work-Related Musculoskeletal Injuries.
Franzblau, A. 1998 The Epidemiology of Workplace Factors and Musculoskeletal Disorders: An Assessment of the NIOSH Review. Paper prepared for the Steering Committee for the Workshop on Work-Related Musculoskeletal Injuries.
Gerr, F. 1998 Workshop on Work-Related Musculoskeletal Injuries: Examining the Research Base Panel on Epidemiology: Risk Factors. Paper prepared for the Steering Committee for the Workshop on Work-Related Musculoskeletal Injuries.
Jones, R.J. 1997 Corporate ergonomics programs of a large poultry processor. American Industrial Hygiene Association Journal 58(2):132-137.
Lahad, A., A.D. Malter, A.O. Berg, and R.A. Deyo 1994 The effectiveness of four interventions for prevention of low back pain. Journal of the American Medical Association 272(16):1286-1291.
Marras, W., and K.P. Granata 1997 The development of an EMG-assisted model to assess spine loading during whole-body free-dynamic lifting. Journal of Electromyography and Kinesiology 17(4):259-268.
Marras, W.S., K.P. Granata, K.G. Davis, W.G. Allread, and M.J. Jorgensen 1997 Spine loading and probability of low back disorder risk as a function of box location on a pallet. International Journal of Human Factors in Manufacturing 7(4):323-336.
McKenzie, F., J. Storment, P. Van Hook, and T.J. Armstrong 1985 A program for control of repetitive trauma disorder associated with hand tool operations in a telecommunications manufacturing facility. American Industrial Hygiene Association Journal 46(1):674-678.
National Institute for Occupational Safety and Health 1996 National Occupational Research Agenda. Publication No. 96-115. U.S. Department of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention, National Institute for Occupational Safety and Health. Washington, DC: U.S. Department of Health and Human Services.
Normand, J., D. Vlahov, and L. Moses, eds. 1995 Preventing HIV Transmission : The Role of Sterile Needles and Bleach. Panel on Needle Exchange and Bleach Distribution Programs, National Research Council. Washington, DC: National Academy Press.
Punnett, L. 1998 Epidemiologic Studies of Physical Ergonomic Stressors and Musculoskeletal Disorders. Paper prepared for the Steering Committee for the Workshop on Work-Related Musculoskeletal Injuries.
Radwin, R.G., and S.A. Lavender 1998 Work Factors, Personal Factors, and Internal Loads: Biomechanics of Work Stressors. Paper prepared for the Steering Committee for the Workshop on Work-Related Musculoskeletal Injuries.
Rempel, D., L. Dahlin, and G. Lundborg 1998 Biological Response of Peripheral Nerves to Loading: Pathophysiology of Nerve Compression Syndromes and Vibration Induced Neuropathy. Paper prepared for the Steering Committee for the Workshop on Work-Related Musculoskeletal Injuries.
Sandler, H.M., and R.S. Blume 1998 Analysis of the Scientific Approach in Assessing Epidemiological Evidence for the Relationship Between Work and Musculoskeletal Disorders. Paper prepared for the Steering Committee for the Workshop on Work-Related Musculoskeletal Injuries.
Smith, M.J., B.-T. Karsh, and F.B.P. Moro 1998 A Review of Research on Interventions to Control Musculoskeletal Disorders. Paper prepared for the Steering Committee for the Workshop on Work-Related Musculoskeletal Injuries.
Snook, S.H., and V.M. Ciriello 1991 The design of manual handling tasks: Revised tables of maximum acceptable weights and forces. Ergonomics 34(9):1197-1213.
Wegman, D.H. 1998 Workshop on Work-Related Musculoskeletal Injuries: Examining the Research Base Panel on Epidemiology: Physical Factors: Summary Comments. Paper prepared for the Steering Committee for the Workshop on Work-Related Musculoskeletal Injuries.
World Health Organization 1977 World Health Classification: Manual of the International Statistical Classification of Diseases, Injuries , and Causes of Death. 9th Revision. Geneva, Switzerland: World Health Organization. 1985 Identification and Control of Work-Related Diseases . Report Series 714. Geneva, Switzerland: World Health Organization.