7
Expansion of the Long-Term Care Ombudsman Program
Consumers of health care and long-term care (LTC) services who cannot effectively speak for themselves need an independent advocate. The LTC ombudsman fills this advocacy role for older individuals in LTC residential facilities—with varying degrees of effectiveness—in all 50 states, the District of Columbia, and Puerto Rico. Many older consumers never enter such facilities; they may receive a broad array of health care and LTC services in such settings as their own homes, acute care hospitals, psychiatric hospitals, adult day care centers, and physicians’ offices. Clearly, not all elderly persons want or need advocacy assistance with respect to community-based care and providers, because many older people are quite able to handle these matters for themselves. However, for those who no longer have such capacities or have exhausted their abilities to negotiate the community-based health care and LTC systems, services like those of the present ombudsman program can be crucial.
Expanding the current LTC ombudsman program to cover these diverse services and settings has been suggested as one way of meeting older consumers’ needs. This chapter explores the conceptual basis and empirical evidence for and against such an expansion. Unfortunately, as the committee discovered, little agreement can be found among experts about what the types and levels of home- and community-based care should be, how “professional” such a system of LTC should be, what constitutes adequate care, how much weight should be given to individual preferences, and what safeguards should be put into place. Actions that may be regarded by some clients as insufficient and perfunctory may be perceived by others as consistent with their individual freedom and choice. Thus, this committee could come to no fixed consensus about all the “next steps” that might be desirable either for advocacy efforts in this arena or for the ombudsman program itself. The committee does, at the end of this chapter, offer two recommendations that are intended to promote
a stronger ombudsman program than exists today and to bring more and better empirical evidence into the debate.
NEED FOR OMBUDSMAN SERVICES BY CONSUMERS OF HEALTH CARE AND LONG-TERM CARE SERVICES
An individual’s need for advocacy assistance is likely to be related to two factors: (1) the individual’s vulnerability and lack of empowerment and (2) the complexity of the system of care with which the individual is having problems (see Figure 7.1). Empowerment denotes an individual’s ability to express his or her views, to feel a sense of personal control, and to influence his or her environment. To the extent that an individual lacks empowerment, he or she is more vulnerable to abuse, neglect, or exploitation. A highly complex system is characterized by a high level of bureaucracy or multiple points of accountability, fragmentation in the provision of services, and limited flexibility. Both lack of empowerment and organizational complexity result in the special necessity to ensure that an individual’s rights are adequately protected.
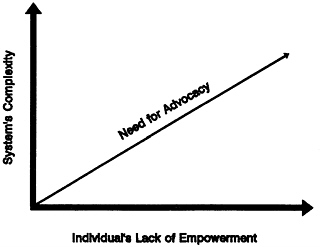
FIGURE 7.1 Relationship of the individual’s lack of empowerment and the system’s complexity to the individual’s need for advocacy.
Even individuals who under normal circumstances have no difficulty expressing their opinions or making their needs known may need an intermediary or proponent should they fall ill or be confronted with an inadequate or nonresponsive system of health care. The need for advocacy may vary over time for a given individual, depending on many factors—his or her physical, cognitive, and emotional health, underlying beliefs and desires about relying on outside assistance, and the complexity and quality of the systems of care to be confronted. For example, an individual who has a broken hip and is trying to arrange for home-delivered meals for a few weeks is much less likely to need an advocate than is an individual with severe cognitive impairment who is trying to appeal an involuntary transfer from a nursing facility.
When the LTC ombudsman program first began in the early 1970s, its efforts were targeted at nursing facility residents because they were viewed as among the most vulnerable consumers, that is, as persons who were relatively “disempowered” and living in very complex “total” institutions. The ombudsman program was viewed as a means of providing a voice through which those residents could resolve problems and experience an optimal quality of life. A few years later, the program expanded to serve board and care (B&C) home residents, since this population was also relatively disempowered and living in a myriad of residential settings of varying character and quality. In this context, it is important to stress that core elements of the ombudsman program to date have been quite facility-oriented. In addition, by federal mandate, the basic target population for the program remains the elderly (i.e., persons 60 years of age and older).
Now, almost two decades after the program first began, it is clear that the health care and LTC systems have undergone sweeping changes—an evolutionary trend that doubtless will continue. The number of vulnerable consumers who are now living outside of residential facilities and who are using increasingly complex systems of care to maintain their independence is unknown. Some of these consumers are indistinguishable in their cognitive or physical impairments from nursing facility residents.
Therefore, the proponents of an expanded ombudsman program foresee a future need for similar ombudsman-like activities and assistance for at least some of the noninstitutionalized elderly population, even though those tasks would no longer be oriented directly to LTC facilities. Moreover, the changing demographics of the U.S. population (the “graying of America”) and patterns within the elderly subset itself (e.g., the increase in numbers of the oldest old) lead some experts and most committee members to predict rising needs for ombudsman-like interventions and programs. Thus, predicting who will need advocacy is essential when considering possible expansion of the LTC ombudsman program.
Vulnerable Populations
Community-dwelling Elderly
Of course, a large proportion of persons over 60 years of age are energetic, competent individuals who function well in their usual and expected daily activities, whether those involve jobs, active retirement, or school. This discussion, however, is intended to draw attention to those members of the older population who are unable to participate fully in such daily activities, and who require one or more kinds of health care or LTC services to maintain an adequate quality of life.
The emphasis in many recent and proposed reforms in health care and LTC service delivery is consistent with the desire of most consumers to remain in their own homes or other noninstitutional, noncongregate settings as long as possible and to consider a move to a nursing facility only as a last resort. As a result, many consumers who have impairments similar to those of nursing facility residents reside in the community. Indeed, those receiving care under state-run Medicaid waiver programs, by definition, experience the level of physical or cognitive impairments that would qualify them for nursing facility care. This is the population of first concern when considering the expansion of the program.
Although community-dwelling elders on average enjoy a higher level of functioning than nursing facility residents, many have equivalent limitations in their ability to perform basic activities of daily living (ADLs). A recent series of Department of Health and Human Services studies found that the average nursing facility resident needs assistance with 3.9 ADLs (out of a possible five), and the average home health consumer needs assistance with 2.5 ADLs. More than 95 percent of nursing facility residents and 56 percent of home health consumers needed help with bathing. Nearly 88 percent of nursing facility residents and 49 percent of home health consumers needed help dressing (Older Americans Report, 1994).
Compared to residents in nursing facilities, home health consumers receive care in a virtually “invisible” setting (U.S. House of Representatives, 1986; IOM, 1990b). Given the sheer number of private homes and privacy concerns, the opportunity for on-site supervision and oversight of health care and LTC service personnel in an individual’s home is severely limited. Additionally, many in-home services may be received simultaneously or sequentially, thus rendering unclear the points of accountability. As with nursing facility and B&C home residents, consumers may fear retaliation if they complain about personnel. They may also fear that lodging a complaint will cause them to lose services and therefore necessitate a move into a nursing facility. Thus, for members of the elderly population who need these home- and community-
based services, the nature of their vulnerability may be different from, and in selected cases, even greater than, that for persons residing in LTC facilities.
Nonelderly Groups
Impaired or disabled persons at younger ages, regardless of whether they reside in LTC facilities or in the community, experience many of the same problems as elderly persons. For those living in the community, considerations include the need for a wide array of home- and community-based services and the problems that may arise when such services are rendered in an invisible setting. Historically, these nonelderly groups have differed significantly from the elderly in their perceptions, definitions, and values about the independence and autonomy of disabled individuals. These viewpoints are reflected in the different services and goals of personal assistance provided to older and younger disabled persons (Simon-Rusinowitz and Hofland, 1993). In keeping with its congressional charge, this committee did not explore issues relating to the nonelderly populations in any depth, so the bulk of this chapter refers specifically to individuals now mandated to be covered through the Older Americans Act (OAA.)
Complex Systems
The systems through which community-based consumers of health care and LTC must maneuver are full of choices that often create complexity and confusion. Although some progress has been made in improving coordination, the system of supports for these consumers still suffers from appreciable fragmentation in financing and delivery. A multitude of public and private agencies and programs at the federal, state, and local levels provide services, but centralized responsibility does not exist at any one level (Pynoos, 1990). Eligibility requirements often vary from program to program. In some areas of the country, particularly rural areas, consumers face the dilemma of having too few choices; sometimes they may be placed on waiting lists for services and sometimes needed services are simply not available.
A typical scenario for an elderly person requiring community-based services illustrates this “complexity.” A home health care consumer may obtain medical monitoring from a visiting nurse, receive assistance with bathing from a home health aide, be placed on a waiting list for a chore aide, attend an adult day care center, be driven to appointments by a special transportation service, have some of these services coordinated by a case manager, and rely extensively on family members or friends for many other personal care needs, especially when the system’s representatives are not available (e.g., on evenings and weekends).
Complexity itself does not tell the entire story. Part of the story is where, and with what types of personnel, the system begins to break down. Kane and colleagues (1991) found that many of the problems in home care focus on paraprofessional providers. These problems include “deficiencies in basic knowledge, failure to perform tasks adequately, intentional injury or abuse, worker tardiness, no-shows, and early departures” (p. 41). Thus, special attention may have to be directed at assisting community-dwelling elders (and their families) with problems in dealing with a wide array of paraprofessional personnel such as nursing aides, personal attendants, and homemakers. The current LTC ombudsman program has already given considerable effort to working with similar types of aides in nursing facilities.
The move toward managed care and the uncertainty of health care reform itself add another level of complexity to the health care and LTC systems. The focus on cutting or containing costs and utilization, particularly in capitated or prepaid practices such as health maintenance organizations (HMOs), has raised concerns about the quality of services provided and about beneficial services withheld. A study of Medicare patients enrolled in HMOs and fee-for-service plans reported that HMO patients appear to receive less resource-intensive ambulatory care than fee-for-service clients and had slightly more negative outcomes (Clement et al., 1994). Shaughnessy (1994) found similar results in a study of Medicare home health care recipients.
Others have argued that prepaid practices can confuse consumers. One study of elderly disenrollees from HMOs found that 23 percent of the disenrollment was due to misunderstandings about how these plans functioned (Rossiter et al., 1989). Prepaid practices also shift the role of the practitioner from that of patient advocate to that of allocator of services, one who must weigh the needs of each patient relative to collective needs and total resources available (Mechanic, 1994). Ironically, LTC ombudsmen may have to assist people in gaining admission to a nursing facility because their HMO or insurer has decided that a less intensive level of care is adequate and refused to cover the costs of nursing facility care.
As a result of the complex health care and LTC systems and despite laws and regulations that promise protection, many consumers of health care and LTC services are simply unaware of their rights. Yurow (1991) conducted an extensive study of the due process rights available to consumers of Medicaid home- and community-based service in order to appeal adverse decisions regarding access to and participation in these federal and state-funded programs. In her extensive analysis, Yurow identified several areas of concern. They included unclear or incomplete state agency policies and directives, lack of consistency in informing consumers of their rights or methods of lodging grievances, lack of encouragement for consumers to assert their rights, and potential lack of impartiality among staff when they hear and decide consumer appeals. These and other findings imply that services like
those of the LTC ombudsman (including assistance in obtaining basic information about available services and consumers’ rights) may be sorely needed by this population at times.
Advocates for Vulnerable Populations
To many, it is clear that at least some community-dwelling elders need assistance in negotiating the health care and LTC systems. Yet a number of sources of help and advocacy may be available to these older persons. To some extent, a variety of mechanisms currently address the need of nonresidential LTC consumers for advocacy, such as information about patients’ rights or complaint resolution.
Family members, concerned friends, case managers, adult protective services (APS), Protection and Advocacy systems (P&As), and other oversight, quality assurance, consumer interest, and advocacy programs all provide valuable information, safeguards, interventions, and advocacy. All of these potential supporters or advocates have strengths and limitations that must be understood if the possible expansion of the ombudsman program is to be put into its proper perspective and context. In particular, the committee examines these programs against three aspects of the mission of the current ombudsman program: (1) to provide an exclusive focus on the interests of the consumer of services, (2) to undertake systemic advocacy as well as individual advocacy, and (3) to prevent as well as solve problems for vulnerable consumers.
Family and Friends
Adult children or grandchildren are often called upon to assist elderly relatives in negotiating the health care and LTC systems. Many regard such informal assistance as the most appropriate and desirable means of providing for the needs of older persons wherever they live. But reliance on family and friends, as a matter of social policy, has considerable drawbacks (Estes, 1993). First of all, family and friends may live in another community or state and have little ability to observe or intervene first hand, regardless of their good intentions. Furthermore, for many individuals, this may be their first encounter with Medicare, a hospital social worker, a home health aide, or an area agency on aging (AAA). They may expend a great deal of energy “learning the system” and still not achieve the desired outcome for their relatives.
Many consumers, particularly older women, do not have family members who can undertake these tasks. Also, their family members or friends may themselves need to be assisted, because of age, infirmity, or other circumstances, in their efforts to advocate for their loved ones. Finally, in
some cases, family members—unwittingly or deliberately—may seek to solve problems that reflect their own needs rather than those of their elderly relatives. This is where significant issues relating to protection of assets, outright misuse of financial resources, or physical or emotional abuse may come into play. For all these reasons, the family cannot be expected to be the sole source of advocacy in difficult cases in community care, any more than the family can be the sole source of advocacy for nursing facility or B&C home residents.
Case Management
Case management is a widespread phenomenon in LTC. However, the term itself is used in multiple and often confusing ways. Typically, case management is defined as a service that coordinates services on behalf of the LTC client (Kane and Caplan, 1993). In OBRA 1981, case management is defined as “management of a specified set of services for a specified group of people,” implying an allocation function. In this legislation the functions of case management include screening, comprehensive assessment, care planning, implementation of the plan (often including authorization of service or purchase of service), monitoring of the adequacy of the plan and the service providers, and reassessment at intervals. These functions have widely become recognized as case management functions.
Part of the confusion about case management stems from the fact that the term is being used by a growing group of privately practicing geriatric care managers who coordinate services for the elderly on a fee-for-service basis (often paid for by worried family members). These managers find adequate home- and community-based help, manage insurance forms and payments for medical and other services, and carry out other tasks needed to maintain the elderly person in his or her home or assisted living facility.
Publicly funded case management agencies, which may be public or private nonprofit, in many states have responsibility for allocating, coordinating, and purchasing LTC services for low-income clients receiving services under Medicaid waivers and state-funded programs. Publicly funded case managers are expected to be both advocates and resource allocators. Various commentators have pointed out the tensions inherent in the same individual performing both an advocacy and a resource allocation role (Estes, 1993; Kane et al., 1991; Kane and Caplan, 1993). For example, case managers have an interest in keeping the cost of the plan as low as possible, whereas the consumer may have an interest in having as much service as possible. Among the strategies suggested (and in place in some jurisdictions) to reconcile the advocacy and gatekeeping functions are well-articulated informed consent processes and disclosure of all premises under which the
case management programs operate (Dubler, 1993). It is a given that community care will be offered within finite resources, and, arguably, any systems advocate will need to take that reality into account. In that sense, it may be possible, some authorities suggest, to maintain both an advocacy and gatekeeping function through case management.
Arguments can be made for and against assigning a major advocacy role for community care to case managers. In favor of this role, case managers in many systems already are well informed about community programs and options and well socialized to the centrality of client preference in development of a care plan. Case managers in some states (for example, Oregon and Wisconsin) are in the forefront of efforts to develop user-friendly, flexible forms of home care such as client-directed home care or client-employed home care.
Several arguments can be made against relying on case managers for community-based advocacy. First, publicly subsidized case management is diversely implemented in the 50 states (Justice, 1994). Some case management programs are much less well-positioned than others in their mission and structure to serve as disinterested advocates. Some case management programs are highly risk-adverse and ease their clients into nursing facilities when it appears that they cannot be cared for in the community at a safety level with which the case managers are comfortable.
Second, some case managers perceive the entire family as the client and make decisions with the family, not necessarily only the older consumer, in mind. This is particularly true in private case management programs when the “client” is the person who is paying.
Third, limited access to case management programs prevent them from being considered a broad-based solution to meet advocacy needs. At present, only those who receive services under designated publicly subsidized programs or who pay privately have access to case management. Income levels for Medicaid waivers range from poverty to 300 percent of poverty. State-funded programs may have no means-test (as in the large, statewide Pennsylvania and Massachusetts programs), but more often they are limited to low-income people. Private case management is an option open mainly, if not exclusively, to families that can afford the fees.
Finally, case managers can have substantial power and some would argue that there must be a counterbalancing force when clients are in contention with case managers. Although most case management programs have appeal mechanisms, quality assurance for case management is in itself at early stages. Sabatino (1992) has pointed out that quality assurance for case management may be more important than quality assurance for each service in the repertoire that the case manager manages. This is especially true because the case manager is expected to be a superordinate point of accountability for the quantity and quality of services received and outcomes achieved.
In summary, although many receiving LTC do not have disinterested case managers, many others do receive needed advocacy services from case managers. However, the sole advocacy function is unlikely to be provided by case managers without major recasting of the case management program.
Adult Protective Services
APS workers generally are mandated to protect incapacitated and dependent adults from abuse, neglect, and exploitation, although the scope of the mandate varies by state. Nonetheless, most APS workers see their charge as to advocate for client self-determination and autonomy. As government agents, however, APS workers are also charged with enforcing societal values of beneficence, or what is thought to be in the person’s best interest.
These two responsibilities often put workers in difficult ethical positions, such as when clients resist accepting services or engage in behaviors that threaten their own health and safety. Workers may be forced to take a stance contrary to the stated wishes of the elderly or incapacitated person if they feel that person is a danger to self or others, particularly if the person’s mental competency is questionable. Additionally, APS workers typically only get involved with a person once a complaint has been lodged. This and, in many jurisdictions, large caseloads severely limit their ability to work preventively.
Protection and Advocacy Systems
As noted in Chapter 2, P&As have been established in all 50 states, the District of Columbia, and U.S. territories to protect the legal and human rights of all individuals with disabilities—regardless of age. They provide some services that are similar to those of the ombudsman program, such as giving general information and program referrals about such issues as discrimination, entitlements, and abuse and neglect.
Unlike the ombudsman program, the mode of operation used by most P&As represents a more distinct legal rights orientation and relies extensively on litigation, or the threat thereof, to resolve disputes. Most P&As offer legal advice and legal representation but do not provide routine visitation.
Other Oversight, Quality Assurance, Consumer Interest, and Advocacy Programs
Yet other mechanisms are available to resolve consumers’ complaints and assure the quality of the care they receive. These programs include the service
provider’s own internal review and monitoring (e.g., patient representative programs, case review by a supervisor, written surveys of consumers, telephone surveys of consumers, and other complaint mechanisms), professional boards (e.g., boards of nursing and Medicaid peer review organizations); state licensure of home care agencies, consumer-driven “Independent Living Centers,” Medicaid fraud control units, home care complaint hotlines, public and private guardianship and conservatorship programs, the police, the state attorney general’s office, consumer protection agencies, and better business bureaus.
Concluding Thought
All of the programs discussed in this section differ widely in legal and budgetary scope, governance, target clients, and other important aspects. Consequently, they offer little overall, systematic coverage of the problems of the elderly (especially of the frail elderly). But, these existing mechanisms should be examined to determine the extent to which they focus on consumers’ interests, allow for systemic advocacy, and contain a preventive element. To the extent that they are collectively deficient in these regards, arguments can be advanced for new responsibilities for one or more of these existing programs or for a new configuration along the lines of the present LTC ombudsman program in order to meet LTC advocacy needs more fully.
The committee concludes that probably no one mechanism can be relied on to handle all the consumer advocacy issues that can and do arise in the area of home- and community-based health care and LTC services for the elderly. The potential problems are varied, the population itself is diverse in both its needs and preferences for assistance, and the possible remedies are quite disparate. Nevertheless, the majority of committee members expressed a strong sentiment that an ombudsman-like advocacy mechanism could be beneficial in meeting the needs of many of the most vulnerable consumers of health care and LTC services. This sentiment was tempered with serious concerns about the many philosophical, operational, and fiscal considerations involved in expanding the current LTC ombudsman program to noninstitutional settings. Some useful—albeit extremely limited—experience has been gained with expansion of several states’ ombudsman program into this arena, to which this discussion now turns.
STATE EXPERIENCE WITH AN EXPANDED OMBUDSMAN PROGRAM
Currently, 13 states have some form of enabling legislation or mandate allowing the state LTC ombudsman to provide advocacy services to individuals other than those who reside in nursing facilities or B&C homes. The following states have expanded ombudsman programs: Alaska, Colorado, Idaho, Indiana, Maine, Minnesota, Nevada, Ohio, Pennsylvania, Vermont, Virginia, Wisconsin, and Wyoming. Although it is no longer in operation, New York City also had a home care ombudsman program for several years. In order to gather information the committee convened a technical panel that commissioned a paper to canvass states with expanded ombudsman programs (Lower, 1994), sponsored a panel discussion at the committee’s symposium, attended presentations of Minnesota’s and Ohio’s experiences with such programs at the National Ombudsmen Resource Center’s national training conference in San Antonio, and visited three states that currently operate expanded ombudsman programs. The committee attempted to evaluate these programs, but each state’s program differs from the others in such fundamental ways that comparable data simply could not be generated or analyzed. Therefore the committee sought to understand the range of experiences presently available with expanded services.
The experiences of states that have expanded their ombudsman program to noninstitutional settings vary widely. Some are charged with serving all older consumers in the state; others are responsible for serving a select group of consumers (e.g., recipients of a state-run home care demonstration program). Some programs have been in operation for more than a decade; other programs are just now being implemented.
Some similarities do exist, however. The programs all face similar budgetary constraints. With few exceptions, they have received no additional funds or staff to carry out their expanded mandate. In addition, no program is well utilized. Other than Alaska and Idaho, most states with expanded ombudsman programs have worked on relatively few complaints outside of nursing facilities or B&C homes. Even states with significant elderly populations and broad mandates—such as Ohio, Minnesota, Pennsylvania, and Wisconsin—have fewer than 300 complaints lodged annually with their expanded ombudsman programs.
The small number of complaints reported are not likely to indicate either the total number of complaints or the entire universe of problems that an ombudsman program may be asked to address. They more likely reflect the restricted implementation and outreach that most programs have been able to achieve as a result of limited funding and staffing. Given the growth in home health care in the past few years and the concerns already expressed by quality-of-care experts about problems that can be expected in that sector
(IOM, 1990a; Sabatino, 1992; GAO, 1994; Shaughnessy, 1994), the committee thought it highly probable that the figures from these expanded-program states reflect only the tip of an iceberg. Complaints could rapidly swell to a huge volume if a program becomes fully operational, well known, and demonstrably effective.
The volume of complaints may also relate to the method of complaint identification. With the exception of the now-defunct New York City home care ombudsman program, no program has tried to use a regular visitation model to identify complaints. Indeed the cost of such an approach may well be prohibitive. Instead, most expanded ombudsman programs employ information and communications approaches, such as a publicized hotline, public speaking engagements, public service announcements, posters, and newsletters, to reach potential clients. Ohio plans to require its Title III providers to disseminate program information. But, in general, the dissemination of information about the services thus far has been low-key and the services are relatively unknown in these states.
In these expanded ombudsman programs, complaints are typically handled over the telephone. Occasionally a worker is assigned for a home visit. Unlike the current program, none of the expanded ombudsman programs currently uses volunteers, perhaps because of uncertainty about the appropriate role of volunteers in this new arena. Some states expressed a reluctance to send volunteer nonprofessionals into private homes where physical risks and volatility of family situations are unknown. More likely, without additional monies the programs were in no position to bring on paid staff to coordinate additional volunteers.
However, the skills needed for complaint investigation, resolution, and mediation are similar across the spectrum of settings and populations (Dize, 1994). Not surprisingly, then, as with the current LTC ombudsman program, ombudsmen in expanded programs typically focus on education about rights, empowerment of consumers, assistance to caregiver support groups, “creative” negotiation and mediation for changes, and referrals to regulatory enforcement and legal services agencies.
In sum, although some states have analyzed and studied their own programs, no comprehensive multistate study on an expanded ombudsman role has been conducted. Indeed, although states appear to be attempting to collect useful information, the committee found little comparable data from these programs to perform such an evaluative study. In general, the committee concluded from its review of these states’ experiences that expansion may be feasible, although existing approaches will need to be modified considerably. The ombudsman program cannot be transported from facilities to community without modification. The committee also concluded from these sketchy state data that expansion would be impractical, and possibly undesirable, without an appropriate increase in funding that would enable such programs to bring on
additional staff and to support the public information, outreach, visitation, and advocacy activities thought to be central to a viable program. This stance reflects the views already discussed in Chapter 3 on compliance and Chapter 6 on adequacy of resources. The next section of this chapter explores the feasibility of expansion in more depth.
FEASIBILITY OF EXPANDING THE CURRENT LONG-TERM CARE OMBUDSMAN PROGRAM
Is it feasible to expand ombudsman services to consumers of health care and LTC services who are not residents of LTC facilities? Philosophical and operational considerations argue both for and against such an expansion.
Conceptual Considerations
Several policy-oriented, or conceptual, questions must be considered when assessing whether the current LTC ombudsman program should expand to serve other consumers of health care and LTC services, such as older persons who receive extensive home health care. They include: (1) What conceptual model would be used in an expanded ombudsman program? (2) Why would such an expansion be opposed? and (3) Why would it be supported?
What Conceptual Model Would Be Used in an Expanded Ombudsman Program?
Generally, the committee adopted the view that, although an expanded ombudsman program might use a different operational model (as discussed further below), the conceptual model of the two programs would remain similar in many respects. As with the current program, the conceptual foci of an expanded ombudsman program would be individual casework, systemic advocacy, and education. The emphasis or weight given to each of these foci, however, may differ from the current program.
It is expected that ombudsmen in an expanded program would continue to become familiar with the problems facing older consumers by working with real people and their problems. Arguably, the real people living in nursing facilities and B&C homes are in different situations than people in their homes. Whereas residents of LTC facilities may feel like “strangers in a strange land,” consumers of home- and community-based health care and LTC services, although similarly impeded by disability or disease, may be likened to “natives in their native land.” Providers enter the consumer’s turf rather than the other
way around. Nonetheless, problems experienced by these consumers are likely to reflect the range of criticisms and grievances that now surface in the current ombudsman program—from involuntary termination of services when an agency decides a consumer is too risky to maintain in the home environment to aides who fail to perform tasks adequately. Most of these problems are resolvable through the same techniques as now employed in the ombudsman program.
The committee believes that the fundamental purpose of the LTC ombudsman program today—upholding and reinforcing consumers’ rights—should continue to be a primary focus of an expanded ombudsman program. Although the rights of nursing facility residents have been codified extensively in federal and state laws and regulations, the rights of consumers of health care and LTC services outside facilities are not explicitly enunciated in the same way. Ombudsmen are used to working within the highly regulatory framework that applies to nursing facilities. In addressing individual complaints, ombudsmen have fairly clear standards against which to assess problems and seek solutions. This is less so in the B&C arena, but B&C regulation is itself advancing toward ever-greater detail.
The case is different for consumers of home- and community-based health care and LTC services, where, although these consumers enjoy the civil rights of any citizen, ombudsmen may have less of a regulatory anchor against which to assess complaints. There is great variability in the regulation of home- and community-based services on a national basis (NAHC, 1994). Despite this variation, the rights of consumers of health care and LTC services that have been codified by some, but not all, states typically fall into five general categories (Sabatino, 1990).
-
Informational rights. The consumer needs to know the extent of the services to be performed, the charge for the service, and the admission and discharge policy. If there is a contract for services, the consumer should be aware of what is or is not covered.
-
Participation and control rights. These rights guarantee a consumer’s autonomy. The consumer must be allowed to participate in the decision making about the care plan and the selection of providers, and he or she should also have the opportunity to participate in other choices about care, including the option to refuse treatment or care.
-
General civil rights and protection. These rights reaffirm the fundamental rights that all citizens enjoy—that individuals should be treated with dignity, have privacy in treatment, be free from physical or chemical restraints, and be assured that their records are confidential.
-
Remedial rights. The consumer should be free to complain without fear of reprisal and should be informed about the complaint process.
-
Quality rights. The consumer should expect safe, “professional” care, at the level of intensity warranted by her or his condition, to obtain the maximum state of health. Workers should be punctual, trained, and “professional.”
These are the same types of rights that LTC ombudsmen currently seek to uphold for LTC facility residents. Naturally, working in noninstitutional environments would require that ombudsmen undergo more training to learn the special nature, rules, and actors involved. However, as already argued, existing ombudsman programs and staffs can be expected in principle to have the generalized knowledge and skills to understand breaches of these rights and to be able to mount effective programs of intervention, correction, and redress.
Finally, the committee believes that much systemic advocacy could be done through an ombudsman-like program. This advocacy would be particularly appropriate because in many states the home- and community-based service “system” will develop at the same time, which will provide an excellent opportunity for the ombudsmen to work proactively. This advocacy will not, however, be without controversy. For example, whether an advocate in the home care arena should engage in systemic advocacy by working to codify structural, process, and outcome standards for services is a matter of debate. Some opponents argue that such codification would serve as an impediment to client autonomy and choice; proponents argue that these vulnerable consumers need stronger protections. It is difficult to foresee on which side the ombudsman would advocate since both positions could be favorable for the consumer.
The emphasis the ombudsmen in an expanded program would give to each focus—individual casework, systemic advocacy, and education—is difficult to predict without further research. Perhaps individual casework would primarily involve referral to other existing advocacy mechanisms. Perhaps the ombudsmen’s time would be better spent on systemic advocacy aimed at giving consumers a stronger voice in care decisions or home care policy. Perhaps the greatest emphasis should be given to education or training of consumers and their surrogates about their rights. The exact equation cannot be determined at this time without better information about the effectiveness of the ombudsmen in pursuing these activities in the new environment of home- and community-based health care and LTC services. In the end, however, more controversial and significant questions may arise in the areas of politics and budgets, as discussed below.
Why Would an Expanded Ombudsman Program Be Opposed?
Presently, the most serious concern with an expanded program is whether it will dilute the ombudsmen’s ability actively to cover nursing facilities and B&C homes. The committee is unanimous that the program should not be expanded at the expense of residents who are currently being served.
Potential duplication of efforts presents a second concern. States with expanded ombudsman programs report that detailed agreements among relevant state agencies, state units on aging (SUAs), and AAAs, are even more vital than in the current ombudsman program to facilitate a clear understanding of each agency’s role in the delivery of health care and LTC services. In particular, it is imperative to differentiate among functions of an expanded ombudsman program and state-supported case management functions, APS, P&As, and legal services agencies.
Also, as in the current program, many providers might express the view that they are best able to handle quality assurance internally. Likewise, many states that operate home- and community-based programs have also built quality assurance into the design of the programs. Quality activities include periodic case reviews, home visits with consumers, consumer satisfaction surveys, licensing or credentialing of agencies and providers, and mandatory reporting of abuse, neglect, and exploitation. Providers and states may worry that the additional layer of quality afforded by the ombudsman program is simply not warranted given the other measures already in place. However, none of these activities is directed explicitly to representing the views of the consumer.
Champions of other patient or demographic groups may also feel threatened or believe that an expanded ombudsman program would duplicate their own advocacy efforts. Examples include P&As and advocates for mental health patients, the developmentally disabled, patients with closed head injuries, or persons with acquired immunodeficiency syndrome. As noted above, the committee did not explore in any detail issues relating to expansion of the ombudsman program to these types of nonelderly patients, but clearly elderly persons may fall within any of these populations, and many may not live in LTC facilities.
Health care reform and the possibility of a federal mandate to develop a separate ombudsman program for health care consumers, as was incorporated in the administration’s Health Security Act and a number of House and Senate bills in the 103rd Congress, may also affect the expansion of the ombudsman program. If a broader ombudsman program were to be mandated at the federal level and pursued through the states—in other words, a public sector program that calls on significant private sector or volunteer inputs—it might have to draw upon the already limited resources that the other advocacy programs now command or could marshall in the future. Thus, the implications of an
expanded ombudsman program for other existing advocacy programs need to be carefully examined.
Problems may arise if consumers have several “advocates” working on their behalf with both duplication and gaps in service occurring. As in the current program, one solution is to encourage ombudsmen and other advocates to work cooperatively with one another. Agreements could be negotiated concerning the populations to be covered and the complaint resolution or advocacy services each would offer; such agreements might spell out referral patterns such that, in total, all relevant client groups would be covered by at least one ombudsman-like program. Presumably, however, such agreements would not be binding on the patient or client groups; consumers ought to be free to choose their own advocates.
Why Would an Expanded Ombudsman Program Be Supported?
In its various factfinding activities and through its own deliberations, the committee developed a keen appreciation of key reasons that proponents of an expanded ombudsman program hold the views they do. Indeed, expansion received significant—but not unanimous—support among committee members, but many expressed concern about the lack of information regarding how to resolve several major operational considerations. One positive argument is that expansion of the ombudsman program would better reflect the changing patterns of LTC service delivery and increasing similarities of clients served. Consumers often use many services in a continuum of care; to achieve continuity as they move between the different levels of care, they may well need advocacy throughout and at different points along that continuum. An ombudsman program that is strictly oriented toward facilities is not able to serve the needs of all vulnerable older individuals. To effectively do so, the program must target its efforts directly to vulnerable older individuals—regardless of LTC setting.
Additionally, the committee observed growing concerns about the quality of health care and LTC services, and judged that these concerns can only be expected to increase. Thus, public officials will feel pressure to “do something” —the same type of pressure that lead to the creation of the ombudsman program in the early 1970s. The U.S. Congress has already held some public hearings regarding the quality of home- and community-based care (U.S. Senate, 1994). News stories on these topics appear with greater frequency now than in the past, and they cover problems such as inadequate care, abusive staff, and unscrupulous agencies. Many proponents of expansion suggest that by developing safeguards in the broader health care and LTC systems now, abuses and scandals will be prevented in the future.
Operational Considerations
As noted above, the committee adopted the view that any operational model of an expanded ombudsman program would differ, perhaps markedly, from the current model. Consideration must also be given to such issues as the current program capacity to expand, target population, organizational placement, staffing, and funding.
Current Program Capacity to Expand
Although an ombudsman program to serve consumers outside of LTC residential facilities could fit conceptually within the same model used by the current LTC ombudsman program, the current program can ill endure another unfunded mandate. In many states, the program does not have adequate coverage of nursing facilities—even when coverage means one visit per year—and the coverage of B&C homes is far less developed than in nursing facilities. Because the ombudsman program has not reached full development even for service to facility-based residents in most areas of the country, expansion into other settings would stretch already scarce personnel and financial resources to their breaking points. Thus, in a very practical sense, expansion is probably not operationally feasible today. Put another way, the program must “expand” into its existing mandates before it considers further expansion.
Furthermore, the committee believes that complete realization of present mandates deserves the highest-priority attention for the ombudsman program—a sentiment reflected in some of the recommendations in Chapters 3 and 6. Nevertheless, the committee also sees several significant arguments in favor of a truly expanded ombudsman-like program, and thus it spent some time elaborating factors relevant to such expansion.
Target Population
The committee agrees that priority should be given to meeting the needs of the present mandated population (i.e., residents of nursing facilities and B&C facilities). The “next” populations and the speed with which they should be brought under the ombudsman umbrella are matters of some contention.
Logically, the first area of expansion would seem to be elderly persons (those over 60 years of age, to match the present definition of the ombudsman program), specifically those receiving various types of home- and community-based services. Even with this group, however, it may not be clear exactly
what home- and community-based services should be included in expanding the purview of the ombudsman program. Skilled nursing or home health aide services for the bedridden stroke patient, physical therapy for a person recovering from knee or hip replacement, or respiratory therapy for persons on continuous oxygen might seem obvious candidates, but Meals on Wheels or subsidized transportation might not. Thus, exactly who would be a candidate for ombudsman services could vary considerably, depending on the nature of the home- and community-based care included in any expansion mandate.
As already suggested, the issue becomes murkier when considering the nonelderly, because expansion has the potential to extend the potential client base immensely. For younger individuals residing in LTC facilities, the arguments for inclusion in the present ombudsman program may be persuasive, particularly insofar as addressing their concerns in a given nursing facility or B&C home may well benefit elderly residents as well (see Chapter 3).
Organizational Placement
The aging network provided a neutral place for the program to operate when it first began in 1973. At that time the network’s primary focus was planning and advocacy. Direct services were limited to nutrition programs—at that time few other formal home- and community-based services existed.
Today, however, the aging network in many states is taking the lead in developing, organizing, allocating, overseeing, and (in some cases) directly providing a wide range of community-based services. Twenty-five SUAs have primary responsibility for managing state- and federally-funded home- and community-based care programs. Sixteen states are developing “single entry point” programs of LTC case-management systems in which consumers will gain access to services through a process of screening, assessment, and care planning. This trend is likely to continue (AoA, 1994b). The potential for conflicts of interest is greatly increased in these states. Those deciding on the appropriate organizational location of any expanded ombudsman program must take into consideration this new and evolving role of the aging network. (For a related discussion, see Chapter 4.)
An ombudsman program, at the federal, state, or local level, may be constrained—either implicitly or explicitly—from intervening on behalf of consumers to challenge eligibility decisions, speak out publicly about long waiting lists, or comment on proposed policy if the program is housed within the agency responsible for such programs and policies. Likewise, consumers may hesitate to contact an ombudsman whose phone number and office location are the same as the case manager whose actions they wish to question.
Another obvious question is whether a program that is broadened to include nonelderly clients should be attached to any entity, whether in the public or private sector, that has the elderly as its chief concern. Logic provokes the observation that, if such a broad growth of an ombudsman program ever were to take place, then it would have to be moved out of agencies or organizations that are operated chiefly for the benefit of the elderly.
As with the current program, expansion should allow states some flexibility in how to go about implementation. The committee is concerned, however, that this will replicate the current problematic variability in program operation across states. As a case in point: the committee had great difficulty in compiling comparable information on complaints in currently expanded ombudsman programs. At a minimum, therefore, a uniform reporting system would be useful, and the committee judges that such a system is best designed and mandated at the federal level. Additionally, the necessity of a national resource center for information and training has already been recognized in the current program. Any expansion proposal should, in the committee’s view, provide for appropriate increases in the activities of that resource center.
Staffing
Staffing needs of an expanded ombudsman program are very difficult to estimate. The reasons are several. First, the potential magnitude of complaints and the types of complaints are not simple to predict based on the limited experiences reported by most states with expanded ombudsman programs. As argued earlier, those data are widely regarded as reflecting the absolute lower boundary on the likely number of complaints in a broader program, even one expanded to include only the elderly receiving home- and community-based health care and LTC services. Many state ombudsmen believe that a full-scale publicity effort for an expanded program would generate more complaints than could be investigated by currently available staff.
In addition, basic staffing at both the state and local level will depend on the structure of the state’s program. Some programs may opt to staff an expanded ombudsman program by relying on hotlines and other centralized means of receiving inquiries and complaints because of the sheer enormity (not to say impossibility) of conducting routine visits to homes and other community settings where elderly or other individuals receive home health care services of various sorts. Finally, ombudsman programs with expanded mandates may or may not use volunteers. If they do, adequate levels of staffing to properly recruit, train, and supervise those volunteers will clearly be required.
Funding
The committee sought to put an approximate price tag on expansion, using information on expenditures for the present program. Chapter 6 argued for a modest increase in federal funding (of approximately $8.8 million) to bring total federal dollars to $32.5 million for this program (or about $39.5 million for FY 1998, taking inflation into account). If the program were expanded in roughly the same time frame and if caseloads in that expanded ombudsman program were to double, then a further increase in federal monies of $39.5 million may be considered a reasonable lower-bound estimate on new dollars needed within a few years. This suggests that a total federal investment approaching $40 million a year might be required to expand the program significantly.
This rough estimate may be criticized on the grounds that some fixed costs of the program would not double, meaning that less than twice the amount of new federal dollars would be needed. However, as noted earlier, many observers believe that new and different types of skills and staff may be needed—ones not now represented in the standard ombudsman program. For the purposes of this discussion, therefore, the committee worked from a simple assumption that these factors would offset each other.
This chapter does not address related financing issues such as a desirable formula for allocating federal dollars across states or the level and nature of a state match, as the committee did not explore these issues with respect to program expansion. Generally, it thought that these matters would demand careful explication as part of a more extensive social and professional debate about the merits of expansion generally, but the set of recommendations in Chapter 6 pertaining to these issues constitutes a good starting point.
CONCLUSIONS AND RECOMMENDATIONS
In conclusion, various arguments are marshalled for and against expanding the current LTC ombudsman program to other settings, as a means of helping to fill deficits in the present system by which people receive health care and LTC services. Opponents raise other jurisdictional and operational points. Given the status of the current program, the various philosophical and operational considerations highlighted above, and the general lack of persuasive evidence on any side, the committee takes a cautious stance about expansion. Specifically:
7.1. The committee recommends that, before any consideration is given by a state to expand its long-term care ombudsman program to serve individuals other than those mandated by the Older Americans Act,
the Offices of the State Long-Term Care Ombudsman programs that are supported with Older Americans Act funds fully implement existing mandates for serving older residents of long-term care facilities.
This recommendation is intended to underscore the need to fulfill existing mandates before taking on added duties, regardless of how worthwhile they might be. The committee favors improving the operation of the current ombudsman program so that it may provide a stronger base for any future expansion. Thus, the committee reemphasizes here the strong recommendations it has made in other chapters of this report about funding, program evaluation, and similar topics.
Moreover, in the committee’s view, before recommending particular directions for a home- and community-based LTC ombudsman effort, it is essential that there be documentation of the needs that could be met through a publicly supported program of mediation and advocacy on a case-by-case basis as well as through systemic advocacy.
Although the Administration on Aging (AoA) has funded demonstrations of ombudsman programs in home care and more recently in the housing arena, these were practice demonstrations of feasibility and contained no rigorous evaluation component. They did not employ established protocols for intervention, comparison groups without the intervention, or measures of effect. Because of these design and methodological limitations, the collective experience of these projects cannot be used to argue conclusively for the need for and benefits of such an expanded ombudsman program. Evidence is also sparse concerning the effectiveness of the program with respect to home care or housing, both in terms of increased protective activities and enlarged advocacy efforts. Finally, it offers little guidance on the best location and structure for ombudsman-like efforts for older people who do not live in institutional settings.
Nevertheless, the committee believes that some interim steps should be taken to clarify further the desirability and feasibility of expansion. To that end:
7.2. The committee recommends that Congress, through the Secretary of the Department of Health and Human Services, direct the leadership of the Administration on Aging, the Agency for Health Care Policy and Research, the Administration on Developmental Disabilities, and the Health Care Financing Administration to develop and support research and demonstration initiatives to determine how ombudsman advocacy services can best be delivered for consumers of health care and long-term care services. Because of the potentially significant role ombudsmen may have in ensuring quality of care in a reformed health care system, the committee also recommends that Congress require that
the Secretary undertake these initiatives during fiscal years 1996–1999 and submit the accumulated results of such research to the Congress no later than January 1, 2000.
Several levels of research are needed. First, a concerted effort should be made to identify and bring together whatever information is available about the effectiveness of the ombudsman program as well as other advocacy mechanisms, such as P&As. As already discussed in Chapter 5, this type of assignment is not easy. However, as more data begin to be collected through the new reporting forms promulgated by the AoA and as states begin to assess their programs in line with the “best practices” ideas advanced in Chapter 5, more information should become available for this purpose. Second, conceptual work, synthesis of existing information, and policy analysis are needed to examine the extent and nature of the need for advocacy. These kinds of analyses should also consider the incentives and challenges of the evolving forms of LTC, including proposed voucher systems, client-directed home care, payment of family members, and capitation.
Studies of case management programs that authorize and purchase health care and LTC services from multiple providers should examine the extent to which clients of these programs need an additional source of advocacy. For example, such investigations should seek to determine the extent to which internal mechanisms of appeal in case management programs work.
Small-scale studies examining the effects of alternative ways to publicize the availability of a community LTC ombudsman function, and the rate at which such a service is used, would be useful for designing programs and for anticipating their likely costs as operational programs. The problems with existing home care hotlines should be investigated to glean lessons for a community ombudsman program.
Based on such preliminary work, a full-scale demonstration should test one or more models of an ombudsman function for community health care and LTC services. Adequate study controls should be applied, so that appropriate comparisons of the models can be carried out and findings and conclusions can be defended methodologically. This approach seems feasible to the committee because the expanded ombudsman function can be made available in some parts of a state and not in others.
Important elements of a rigorous research and demonstration initiative include good baseline data, adequate time for the program being tested to be implemented and tracked, adequate samples of patients and clients, and sufficient time and resources to permit appropriate analyses to be completed. Careful consideration would have to be given to the factors to be controlled for in such studies. The basic goal would be to measure the extent to which problems are identified and ameliorated under various forms of ombudsman efforts and at what costs.
The committee did not discuss in any detail the levels of funding likely to be needed for such an R&D program. The funding levels from the Agency for Health Care Policy and Research for a single Patient Outcomes Research Team (PORT) project may be instructive on this point, as PORTs contain conceptual, data collection, and analysis components similar to those of the main demonstration and evaluation projects contemplated here. Early PORTs were supported at about $1 million per year for five years. Thus, if a reasonably full set of studies were to be implemented, including a meaningful demonstration and evaluation effort, over a four-year period (beginning in FY 1996 and reporting to Congress in FY 2000), $4 million is a tenable, albeit not generous, estimate.
SUMMARY
The committee accepts the conventional wisdom that self-advocacy by consumers is the most desirable solution to many of the problems consumers face. Further, the committee also acknowledges that frail elderly people receiving health care and LTC services, ranging from skilled home health care to various in-home services funded under home- and community-based waivers and state-funded programs, may be vulnerable to neglect, abuse, and poor care. Such consumers of health care and LTC services, especially persons who cannot advocate for themselves when confronted by systems that are complex, fragmented, and cost-conscious, need an independent intermediary and advocate. Such advocates do exist in some places and in some capacities, but they cannot always act expressly on behalf of the consumer, provide both individual and systemic advocacy, nor work preventively.
The 13 states that have expanded ombudsman services to health care and LTC consumers outside of LTC residential facilities have limited experience to date. The committee heard testimony that this is due, in large measure, to inadequate resources to fully implement and operate a viable program. The result, however, is that little empirical evidence is available to support decision making on whether and how the current ombudsman program ought to be expanded.
On the basis of what is already known, however, most committee members believe that some entity or individual—whether or not it is the current LTC ombudsman—is needed to answer questions, to provide systemic advocacy, and to intervene in problem situations for some consumers.
Other activities are in place ostensibly to help address the needs and interests of vulnerable people receiving community-based health care and LTC services. These include: case management programs, the APS efforts available in most states; the home care complaint hotlines mandated by law in 1987, which have been variably implemented across the United States; and licensure,
certification, and survey processes for home health agencies. In addition, public and private guardianship and conservatorship policies are meant to ensure that those unable to make decisions have an agent to act in their best interests.
Of course, all these mechanisms have strengths and limitations. Case management programs are variable in their focus and ability to truly serve as advocates. APS caseloads are large, and the responsibilities of the protective service worker is a rather narrow legal one. Home care complaint hotlines are for the most part poorly publicized and underutilized. Licensure and certification are only as good as the motivations of surveyors and certification programs and the strength of public requirements, regulations, and sanctions; these factors vary significantly across states. Guardianship programs have been criticized as being perfunctory. It is unclear, therefore, whether the solution to these problems is to strengthen one or more of the existing mechanisms, combine and strengthen advocacy functions into a new structure, or create an ombudsman as a superordinate, general operation.


























