3
State of Quality of Long-Term Care
This chapter addresses a specific task in the committee's mandate—to determine the current quality of long-term care in the various settings and the extent to which it has improved or deteriorated in the past several years. The chapter begins with a brief description of the committee's criteria for judging quality of care and the measurement of quality of care in long-term care settings. It summarizes available evidence about the current status of quality of care, focusing in particular on areas of improvement and on the nature and extent of continuing problems. The chapter then discusses whether the legislative and regulatory efforts to improve quality have achieved their objectives, namely improvement of quality in long-term care.
The committee's task was made difficult by the unevenness of available empirical evidence. Although information to judge quality of care in nursing homes is extensive and systematic, for most other settings it is nonexistent or very limited, and lacks uniformity. Moreover, opinions about what constitutes excellent, good, or poor quality care are changing and sometimes conflicting. Some of the available information is open to interpretation, and conclusions are sometimes based on personal and clinical experience rather than empirical evidence. The discussion in this chapter is based on data from national data systems and surveys, on published research and studies in progress, and on testimony received by the committee.
MEASUREMENT OF QUALITY OF CARE
Quality of care in long-term care “is a complex concept confounded by regulations [and] debates about what should be measured to assess quality” (IOM, 1996b, p. 129). Defining quality in long-term care has been a difficult process; it is defined both as an input measure and as an outcome. Since the mid-1960s, quality assessment has been measured in terms of three concepts: structures of care, processes of care, and outcomes of care (Donabedian, 1966). Over the years, nursing home quality has been measured by structural variables such as level, mix, and education and training of staff; and characteristics of the facilities in relation to characteristics of the residents such as demographics, payer mix, and casemix. P rocess measures assess the services actually provided to the residents. Deficiencies in processes of care can be described as overuse of care, underuse of care, or poor technical performance (see, for example, IOM, 1990; Chassin and Galvin, 1998). Other process problems in long-term care have been characterized as neglect (e.g., inattention to weight loss) or even abuse (e.g., physical assault).
Outcomes of care include changes in health status and conditions attributable to the care provided or not provided. Unlike acute care, for which successful outcomes often mean restoring patients to their level of functioning before the onset of illness, successful outcomes in long-term care are likely to be based on criteria such as maximizing quality of life and physical function in the presence of permanent, and sometimes worsening, impairment. The occurrence of specific problems, such as pressure sores or inappropriate weight loss, is generally viewed as evidence of poor quality of care. Because care processes and structural factors are the means through which desired outcomes are achieved, they are key components in defining quality. In principle, health and quality-of-life outcomes are the end results of the structures and processes of care. Outcomes of interest might include overall health status, the presence or absence of specific conditions (e.g., pressure sores), social and psychological well-being, and satisfaction with care. However, using outcomes to assess quality of care is often difficult because of conceptual and practical (e.g., cost) considerations in collecting information on health status and quality of life. As a result, measures of structure and process (e.g., staffing levels or rates of sedative use) are frequently used as proxies for outcome measures of quality of care in various long-term settings. Opinions in the literature and in testimony given to the committee, and even among the committee, vary widely about the empirical evidence linking specific structural features or processes of care to the outcomes in question. At the same time, adequate availability of structural measures, such as staffing
and facility characteristics, is essential to the provision of consumer-oriented long-term care.
In evaluating the quality of long-term care, multiple perspectives have to be considered. Application of the concept of consumer-oriented long-term care requires that the quality of long-term care be judged not only in terms of the structure, processes, and outcomes of clinical care, but also in terms of access to care, the nonmedical personal assistance services that are an important part of long-term care, and the long-term care user's quality of life. Because perspectives can differ among recipients of long-term care services and between care recipients and care providers, one of the challenges is establishing priorities reflecting different perspectives.
Standards for evaluating whether the quality of long-term care is good or bad, improving or deteriorating, are shaped by several considerations including views of the nature and scope of long-term care, the operational definitions of quality, and the ways quality-of-care data and research findings are interpreted. Different observers such as physicians, nurses, consumers, family members, and society also will have different perspectives. Different circumstances will require assessing the views of these and other participants. Long-term care can encompass a broad range of services affecting many aspects of daily life. It is easy to see how observers might differ in their views on the nature and scope of the field and therefore the basis on which the quality of long-term care should be judged. The following are three aspects of long-term care that are relevant to the assessment of its quality:
-
Long-term care is both a health and a social program. Although many long-term care programs are currently identified and judged primarily as either social models or medical models (R.A. Kane, 1999), users' needs do not divide so readily. Some aspects of long-term care are based on services that require knowledge of health conditions and their treatment. Other aspects are aimed at services to help people with functional limitations live in ways that maximize their capability and productivity. Long-term care funding comes partly from health programs, but also from social service and income support programs. For the health services components of long-term care, judgments about quality of care emphasize medical and technical aspects of care. For other aspects of long-term care, judgments about quality of care reflect the opinions and satisfaction of consumers (or their surrogate agents).
-
The potential and actual role of consumers is an essential element in long-term care. As indicated in Chapter 1, long-term care, and therefore the basis for evaluating the quality of such care, is being redefined (at least in some care settings) by the growing recognition of the role of
-
consumers and their involvement in choosing and directing many features of their care and in assessing the adequacy of care.
-
For nursing homes and residential care settings including assisted living, the physical environment of the facility can contribute to the physical safety and functional mobility of residents and, more broadly, to their quality of life. Privacy is an aspect of the physical environment and is intimately tied to the consumer-centered principles the committee endorses.
CURRENT STATE OF QUALITY OF CARE
No single or simple formula is available to guide those attempting to evaluate the quality of long-term care. Evaluators must determine how to interpret a variety of data on health outcomes and provider performance, on many different aspects of care for many individual consumers, and on many providers over a period of time.
Regulatory quality standards often focus on deficiencies in care, defined by the presence or absence of specified problems. When such standards are applied, the quality of care is considered lower if problems are found than if they are not found. At the present time, most measurable standards of quality do not recognize excellence in care with criteria based on positive outcomes, such as maximizing physical functioning or, in the psychological sphere, going beyond minimizing depression and anxiety to maximizing well-being. The following sections examine the state of quality of care in each of the specific long-term care settings addressed in this report.
Nursing Homes
The committee reviewed a large volume of research and investigative reports to examine the quality of nursing home care. In addition, two sources of data are available on nursing home care: (1) the On-Line Survey and Certification Assessment Reporting (OSCAR) System from the federal survey and certification system permits the analysis of longitudinal patterns of deficiencies identified in nursing home inspections; and (2) studies using resident-level data from the Minimum Data Set (MDS), which permits tracing quality indicators in nursing homes. (These information systems are discussed in Chapter 4.) Other research studies provide information on the state of quality, as do recent studies by the General Accounting Office (GAO). Some information also can be inferred from testimony presented to the committee.
Evidence indicates that the quality of nursing home care in general has improved over the past decade, even though nursing homes are serv-
ing a more seriously ill population (Hawes, 1996; Johnson and Kramer, 1998). For example, many facilities have successfully reduced the inappropriate use of physical and chemical restraints. The focus of increased regulatory scrutiny on these two areas of care was a major contributing factor in reductions in both of these. Despite these improvements, serious quality-of-care problems persist in some nursing homes. Pain, pressure sores, malnutrition, and urinary incontinence have all been shown to be serious problems in recent studies of nursing home residents (GAO, 1998a; Mortimore et al., 1998). The committee recognizes that change in eliminating or reducing persistent and serious problems is a long process requiring diligent monitoring and enforced adherence to standards. In a paper prepared for the committee, Johnson and Kramer (1998)1 noted that continuing problems include physical pain and insufficient attention to rehabilitation and restorative nursing. GAO (1999b) and the Office of the Inspector General of the Department of Health and Human Services (OIG, 1999c) reported that national data from the OSCAR system between July 1995 and October 1998 provide evidence of increasing problems with some aspects of care, including lack of supervision to prevent accidents, improper care for pressure sores, and inadequate assistance with activities of daily living.
Data based on state certification surveys of facilities indicate that problems occur in many nursing homes and that they are persistent in a smaller subset of facilities (GAO, 1999b). About one-quarter of nursing homes had deficiencies2 in the highest-severity categories. Figure 3.1 shows the ten most frequent deficiencies for poor quality of care cited in the United States. In 1998, the most frequent deficiency was poor food sanitation (23.7 percent of the 15,401 facilities surveyed) (Harrington et al., 2000b). Failure to remove accident hazards was cited in 18 percent of facilities, poor general quality of care was cited in 17.2 percent, and failure to prevent or properly treat pressure sores was cited in 17.1 percent. Poor care planning, improper resident assessment, failure to prevent accidents, poor housekeeping, failure to protect the dignity of residents, and improper use of physical restraints were also problems in a significant proportion of homes.
GAO (1999b) also found that 40 percent of the facilities that had severe deficiencies in an earlier survey had deficiencies of equal or greater severity
|
1 |
The committee commissioned this background paper from Johnson and Kramer for its use. Much of the analysis in this chapter on the quality of care in nursing homes draws from this paper. |
|
2 |
The Health Care Financing Administration (HCFA) defines a deficiency as a failure to meet a Medicare participation requirement. One or more deficiencies in critical areas result in a finding of substandard quality of care. |
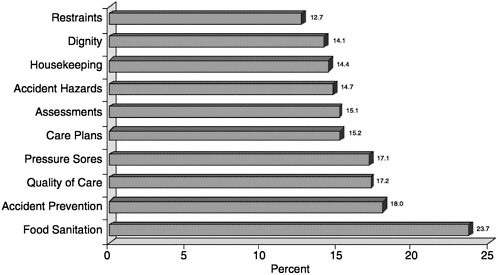
FIGURE 3.1 Top 10 deficiencies of nursing facilities and percent of facilities with the deficiency cited: United States, 1998.
SOURCE: Harrington and Carillo, 2000.
at the time of a later survey. In another study based on the federal and state survey process, GAO (1998a) found that serious and potentially life-threatening quality-of-care problems in the categories of neglect, abuse, malnutrition, and pressure sores occurred in approximately 30 percent of California nursing homes over a two-year period. This study found that another 33 percent of facilities had poor care that caused less serious harm, and 35 percent had more than minimal deficiencies. Overall, GAO found that only 2 percent of California facilities had minimal or no deficiencies, while one in nine was cited for causing actual harm or putting residents in immediate jeopardy (GAO, 1998a). GAO (1998a) also reviewed the medical records of a sample of 62 residents who had died. More than half (34 residents) had received unacceptable care that endangered health and safety. These problems included dramatic unplanned weight loss, failure to properly treat pressure sores, and failure to manage pain. Although problems in California nursing homes may not be representative of national problems, California 's 1,370 nursing homes alone represent about 10 percent of the nursing homes in the United States.
Another study of 14 facilities documented significant problems with nutritional support, care for pressure sores, personal care, pain management, and personal environment and contracture care in 25 to 35 percent of the facilities studied (Kramer, 1998). Kramer also found significant
problems with falls, functional losses, incontinence care, skin breakdown, use of physical restraints, avoidable deaths, antipsychotic drug use, and lack of functional rehabilitation in 10 to 15 percent of the facilities sampled.
Additional evidence comes from complaints to the Long-Term Care Ombudsman Program in some states (OIG, 1999a). The OIG and state ombudsmen link many of these complaints to inadequate nursing home staffing. Abuse, patient neglect, and the hiring of staff with criminal records have been widely reported in the media and by local ombudsmen, although the actual prevalence of such problems is unknown (Kauffman, 1996).
The current state of quality of care, based on some key indicators of quality, is summarized briefly below. This includes use of physical and chemical restraints, pressure sores, malnutrition, continence care, pain, and aspects of care related to quality of life.
Physical and Chemical Restraints
The greatest improvement in nursing home care is in the substantial reductions in use of physical restraints since the reforms in the Omnibus Budget Reconciliation Act of 1987 (hereafter OBRA 87). The Health Care Financing Administration (HCFA) defines restraints as mechanical devices, materials, or equipment that restricts freedom of movement or normal access to one's body. Restraints may cause decreased muscle tone and increase the likelihood of falls, incontinence, pressure ulcers, depression, and other problems. A number of studies have shown the value of reducing the use of restraints (Evans and Strumpf, 1989; Libow and Starer, 1989; Burton et al., 1992; Phillips et al., 1993a; Castle and Mor, 1998).
In the late 1980s, the prevalence of physical restraint use was an estimated 41 percent, with wide variability among facilities (Strumpf and Tomes, 1993). Using 1990 data, Phillips and colleagues (1996) reported a mean physical restraint use of 38 percent in 268 facilities in ten cities. Following the implementation of OBRA 87, Hawes and colleagues (1997b) reported a decrease in average restraint use to 28 percent for the same facilities. Other researchers also have reported declines in restraint use (Ejaz et al., 1994; Sundel et al., 1994; Graber and Sloane, 1995; Levine et al., 1995; Capezuti et al., 1996; Castle and Mor, 1998). OSCAR data show a 41 percent decline in restraint use since the early 1990s, from 21 percent of all residents in 1991 to 12.3 percent in 1998 (Harrington et al., 2000b).
Although the literature suggests an average decrease in physical restraint use since OBRA 87, Johnson and Kramer (1998) note that there is reason for ongoing concern. An average decrease in restraint use may mask persistently high use in some facilities. In 1995, for example, with the rate of restraint use at an average of 20 percent, 21 percent of the
facilities had rates exceeding 25 percent of residents (Castle, 1998a; Castle and Mor, 1998). Moreover, evidence that facility factors such as staffing, occupancy rate, for-profit status, and Medicaid reimbursement policies affect restraint use more than patient needs raises questions about the appropriateness of restraint use (Phillips et al., 1996; Castle, 1998a).
The overuse of psychotropic medications, referred to as chemical restraints, was also targeted by OBRA 87. The average use of antipsychotic and sedative hypnotic medications appears to have declined, and there is no evidence that physical restraint reduction has been accompanied by increased use of chemical restraints (Siegler et al., 1997; Castle, 1998b). Garrard and colleagues (1995) reported a decrease in the use of anti-psychotic medications from a mean of 23 percent prior to OBRA 87 to 15 percent after OBRA 87 in all Minnesota nursing homes. Burton and colleagues (1992) reported a 36 percent decrease in antipsychotic drug use in a sample of Maryland nursing homes between July and December 1990, when OBRA 87 regulations were being implemented. A longitudinal study of Tennessee Medicaid recipients in nursing homes showed a 26.7 percent decrease in antipsychotic drug use following implementation of OBRA 87 (Shorr et al., 1994).
Decreased use of psychotropic medications appears to have been accompanied by improved documentation of appropriate indications for psychotropic drug use. Llorente and colleagues (1998) reported that 70 percent of resident medical records were found to have appropriate documentation, compared with less than 50 percent prior to OBRA 87. There is no evidence of improved behavioral management programs to replace the use of psychotropic drugs (Hawes et al., 1997b).
Quality concerns about psychotropic drug use persist, despite mean decreases in use. As Johnson and Kramer (1998) point out, psychotropic medication use is far more complicated. The arrival of multiple new anti-psychotic medications with improved side-effect profiles may result in increased use of antipsychotic drugs (Lasser and Sunderland, 1998). Few studies are available on the propriety of psychotropic drug use in individual patients.
Pressure Sores
Pressure sores (decubitus ulcers) are bruises or open sores on the skin, usually found on the hips, buttocks, heels, or other bony areas, from pressure or friction on the skin. They range from bruises in early stages to open wounds that may reach the bone at later stages. Severe pressure sores may result in pain or infection, and can be fatal. Because good nursing care can generally prevent pressure sores from occurring and ensure that the skin heals properly, the presence of pressure sores has
been used for decades as an outcome indicator for quality of care in nursing homes (Zimmerman et al., 1995; Mukamel and Brower, 1998). Moreover, a study of three Department of Veterans Affairs nursing homes, with pressure sore prevalence ranging from 2 to 16 percent, found an association between prevalence and staffing patterns, after controlling for casemix, suggesting that pressure sores can basically be eliminated with appropriate nursing care (Rudman et al., 1993).
Data generally indicate, however, that pressure sores are a continuing problem in nursing facilities. They were reported for 7.1 percent of all nursing home residents in 1998, which was about the same as in 1991 (Harrington et al., 2000b). Other studies have reported prevalence rates from 7 to 23 percent, with wide variability among facilities (Zinn et al., 1993; Smith, 1995). In the most recent state surveys, 17.1 percent of facilities had deficiencies related to care for pressure sores (Harrington et al., 2000b), and in 10 states, the number of deficiencies had increased 21 percent from previous surveys (OIG, 1999b). Another study of 254 facilities in 10 states, however, showed some decrease in the prevalence of pressure sores following implementation of OBRA 87 (Fries et al., 1997). No increase in preventive skin care was evident in a pre- and post-OBRA cohort of 268 facilities (Hawes et al., 1997b).
As stated above, the prevalence of pressure ulcers in the population of nursing home residents, as reported in the federal inspection survey and reflecting the residents in the home at the time of the survey, varies by state and by type of facility. Even within states and types of facility variability is noted in the prevalence of pressure ulcers. For example, one unpublished analysis of OSCAR data indicates that among freestanding, non-hospital-based facilities, an average of 6 percent of residents per facility have pressure ulcers on the day of the survey. This varies by state between 3 and 8 percent as the average for these kinds of facilities, but the averages may belie considerable variability. Across the 50 states, 17 percent of facilities had greater than 10 percent of their residents with a pressure ulcer, varying from 1 percent of the facilities in one state to 27 percent in another. Even more variation is observed when these same figures are examined for hospital-based facilities which admit almost all of their patients from hospitals and where most residents do not remain for an extended stay. The risk of acquiring a pressure ulcer is strongly affected by the clinical characteristics of the resident as well as the nursing care provided, and residents entering a hospital-based facility are likely to be more impaired and have more serious medical problems (Vincent Mor, personal communication, May 9, 2000). However, a vast majority of nursing home residents are not such “short-stayers. ”
Since 1995, HCFA's OSCAR data have captured two measures of the rate of pressure ulcers: (1) the number of residents with a pressure ulcer
on the day of the survey; and (2) the number of residents in the facility on the day of the survey who had a pressure ulcer at the time of their admission to the facility. In general, these two figures are highly correlated (0.72), but they are more correlated among hospital-based facilities (0.87) than among freestanding facilities (0.53) (Vincent Mor, Personal Communication, May 9, 2000). This is not surprising because one predictor of pressure sores is previous pressure sores.
Malnutrition and Dehydration
Nutritional problems and dehydration are considered to be serious—and commonly underreported—problems in nursing homes. Inadequate food intake has been found to be a major determinant of mortality in frail elderly people in nursing homes (Blaum et al., 1995; Frisoni et al., 1995). Blaum and colleagues (1995) found that needing assistance with eating was significantly associated with undernourishment among nursing home residents. Malnutrition, starvation, and dehydration have all been documented in recent studies (Kayser-Jones, 1996, 1997; Kayser-Jones et al., 1997; Kayser-Jones and Schell, 1997). Moreover, commercial dietary supplements are being used inappropriately as substitutes for food, perhaps because of insufficient staff for oral feeding and perhaps because of undiagnosed dysphagia or poor oral health (Kayser-Jones et al., 1998). Kayser-Jones et al. (1999) reported that in two nursing homes, fluid intake was inadequate for 39 of 40 residents, contributing to dehydration. (See Chapter 6 for further discussion of this subject.)
Continence Care
Incontinence is a common problem for nursing home residents and requires that they receive assistance in toileting and care to prevent accidents. Incontinence can be reversed in almost half of the individuals who develop it and can be improved in other individuals (Ouslander and Kane, 1984; Ribeiro and Smith, 1985; Palmer et al., 1991, 1994). Bladder incontinence was reported for 50.7 percent of residents in 1998, a 7.8 percent increase since 1991 (Harrington et al., 2000b).
Bowel incontinence, which declined only slightly (3 percent) during the 1991–1998 period, was reported as a problem for 41.6 percent of residents in 1998. In recent nursing home inspections, 10 percent of facilities were cited for deficiencies in incontinence care (OIG, 1999b). Because this problem is reversible in many cases, high prevalence of incontinence suggests poor care.
Research studies help illustrate the problems. In interviews, residents have indicated a preference for assistance in toilet use or changes of wet
linen two times per eight-hour day (Simmons and Schnelle, 1999), but observational studies found that residents were changed less often than this and received toileting assistance even less frequently, an average of only 0.4 to 0.5 times in 8- or 12-hour periods during the daytime (Schnelle et al., 1988a,b; Bowers and Becker, 1992; Simmons and Schnelle, 1999). Residents who were demented and physically or verbally agitated were likely to receive lower levels of assistance (Schnelle et al., 1992b). The low frequency of toileting assistance has been attributed to its being more time-consuming for staff than simply changing residents' wet clothing or bedding. In fact, one study found that “usual” daytime toileting and mobility care required about 11 minutes of staff time per resident over a 12-hour period compared to 46 minutes per resident for a toileting assistance protocol (Schnelle et al., 1995a).
Urinary catheters are sometimes used to control bladder incontinence, but they should be used only when medically necessary because they are associated with infection and discomfort (Ribeiro and Smith, 1985). OSCAR data indicate that urinary catheter use declined by 10.6 percent between 1991 and 1998 for all nursing home residents in the United States (to 7.6 percent of nursing home residents in 1998) (Harrington et al., 2000b). Others examining catheter use following OBRA 87 reforms also found a decline. One study of pre- and post-OBRA period nursing home residents in Virginia found that less than 1 percent of the residents were inappropriately catheterized (Moseley, 1996). Hawes and colleagues (1997b) reported a statistically significant mean decrease in indwelling urinary catheter use from 9.8 percent to 7 percent following implementation of OBRA 87. The decline observed in catheter use may be viewed as a positive development in quality of nursing home care.
Pain Management
Despite widespread agreement that much pain can be ameliorated by appropriate use of medications, undiagnosed and untreated pain has been a widespread problem in many health care settings (AHCPR, 1994; IOM, 1997). Prevalence of chronic pain is estimated in 45 to 80 percent of nursing home residents (Ferrell, 1995; IOM, 1997). A study of Oregon nursing homes found that of the residents suffering from pain, 39 percent were inadequately treated for pain (Wagner et al., 1997), and another study found that more than one-quarter of nursing home residents suffering from cancer received no pain medication even though they had daily pain (Bernabei et al., 1998).
Levels of pain can be particularly difficult to determine, especially among people who cannot easily communicate in words, and methods to identify and assess other signs of distress need further development. In
addition, people in general—and nursing home residents and staff in particular—may have low expectations, believing that pain but not pain relief is to be expected. More effective pain management techniques should be a priority for nursing homes, using, as appropriate, palliative techniques developed by hospices and others.
Hospitalization
As Johnson and Kramer (1998) point out, nosocomial infections, pressure ulcers, and deterioration of functional abilities because of bed rest are common iatrogenic complications of hospitalization of nursing home residents. A potential indicator of improved resident assessment and quality of care would be decreased overall hospitalizations and improved selection of patients for hospitalization. However, appropriate rates of hospitalization are difficult to determine (Castle and Mor, 1996). Mor and colleagues (1997) in a study of 250 nursing homes reported decreased odds of hospitalization of residents between 1990 and 1993, following implementation of the resident assessment system called for in OBRA 87. (See Chapter 4 for more details.) The effect was more pronounced among residents with cognitive impairments. Demonstration projects are now in place and will explore whether enhanced payments and provision of geriatric care through nurse practitioners and other personnel can reduce hospitalizations and lead to improved outcomes.
Quality of Life
Quality of life is difficult to conceptualize, let alone measure. Some commentators view quality of life as the sum of all other domains including physical health, cognitive status, and functional status as well as psychological, social, spiritual, and economic well-being, whereas others make a sharper distinction between quality of life as a psychosocial phenomenon apart from health status (Birren et al., 1991; Frytak, 2000). Quality of life has an inevitable subjective component, necessitating direct input from the persons most concerned —the long-term care consumers—to provide feedback on quality of life domains and to suggest how they should be weighted. But for long-term care consumers, especially residents in nursing homes, several problems require that information on quality of life be sought from multiple sources. Low expectations or fear of being critical of those on whom they are dependent may affect response. Also, some residents are too cognitively impaired to provide reliable information or, in some cases, any information at all. Their quality of life must be inferred from observation and other sources (e.g., family).
The literature contains many statements about what residents find
important for the quality of their lives. Such statements are variously derived from empirical studies using focus groups (NCCNHR, 1985; Abt Associates, 1996), questionnaires to residents or family members (Kane et al., 1986; Kane et al., 1997), “Q-sort studies” with staff (Sano et al., 1999), systematic observations of residents (Lidz et al., 1992; Lawton et al., 1996), anthropological and ethnographic studies (Shield, 1988; Tellis-Nayak and Tellis-Nayak, 1989; Schmidt, 1990; Savashitsky, 1991; Gubrium, 1993), and psychologically oriented research dealing with the search for identity and meaning among nursing home residents (Tobin, 1991). Others have written autobiographical or fictional accounts of life in nursing homes from the perspectives of residents (Tulloch, 1975; Laird, 1985) or nursing aides (Bennett; 1980; Tisdale, 1987; Diamond, 1992: Foner, 1994; Henderson, 1995).
In addition to their emphasis on various aspects of staff behavior and choice, cognitively intact residents have also cited other features that make their lives better or worse in nursing homes, including the quality of food and the ambience at meal time; having a private room or having a compatible or at least not incompatible roommate (Lawton and Bader, 1970; Kane et al., 1997; 1998a); getting outside during pleasant weather; being able to maintain contacts and communicate readily with relatives and friends outside the facility (Kane et al., 1997); getting a good night's sleep; and for some cognitively intact residents, being spared frequent close contact with residents with dementia, particularly those whose behavior and demeanor are frightening or disturbing (Teresi et al., 1993). Residents with advanced cognitive disabilities are unable to report reliably and completely what affects the quality of their lives. On their behalf, observers comment on some things that seem to afford pleasure (e.g., music, other sensory stimulation) and those that bring misery (e.g., forced baths, being physically tied down).
Measuring Quality of Life. One approach to measuring quality of life for nursing home residents, called real experiences and assessment of life (REAL), was developed by researchers at Vital Research in California and tested in facilities under the auspices of a small business grant from the National Institutes of Health (Vital Research, 2000). The REAL is composed of yes-no questions and, in the resident version, generates six factors: help and assistance; communication with staff; autonomy and choice; companionship; safety and security; and food and environment. The survey is administered by staff of the research agency. The Confidence Satisfaction Survey was developed by Life Services Network of Illinois (1997) and uses many of the same items as REAL. This survey is administered by facility staff and sent for interpretation by the network. No standards have been published yet on either of these tools.
In recent years, considerable emphasis has been given to measuring well-being, including quality of life, for people with dementia in nursing homes (Albert and Logsdon, 1999). Some of these measures concentrate on behavioral symptoms exhibited by the person with dementia that tend to render caregiving difficult but may not always equate with a poor quality of life as experienced by the person with dementia (Cohen-Mansfield, 1989). Most of the approaches for examining functioning of the person with dementia rely on the summary reports of paid or family caregivers. Rabins and colleagues (1999) have developed a multidimensional instrument for measuring the quality of life (QOL) of people with dementia through reports from caregivers; it contains five domains: social interaction; awareness of self; feeling and mood; enjoyment of activities; and response to surroundings.
More recently, QOL measures gathered by direct interviews with people with dementia have been developed and tested. Examples include the quality of life–AD scale, a brief 13-item measure, each with a 4-point response set (Logsdon, et al., 1999); and the D-QOL, a longer self-report tool developed by Brod and colleagues (Brod et al., 1999); the latter tool also has five domains: aesthetics, positive affect, negative affect, self-esteem, and feelings of belonging. The work with these three direct-interview tools, as well as work with the REAL mentioned above, gives encouragement to the idea that data can be gathered by direct report from many nursing home residents with dementia.
Finally, the apparent affect rating scale (Lawton et al., 1996, 1999) has been developed as a way of making systematic observations of four mood states in people with dementia: pleasure, sadness, anxiety, anger, and interest. The instrument has been shown to be reliable even, under proper training conditions, when administered by nursing aides. It also has been shown to be sensitive to interventions of the nursing home and changes in staff behavior.
In 1998, HCFA awarded a contract to the University of Minnesota to develop and test measures and indicators of quality of life. The researchers are attempting to measure 11 quality of life domains: dignity, autonomy, individuality, privacy, enjoyment, meaningful activity, relationships, comfort, sense of security and order, spiritual well-being, and functional competence. The first wave field test, underway in 40 nursing homes in five states, is expected to be completed by June 2000 and include data measuring quality of life for about 2,000 residents, half with substantial cognitive impairment. The investigators are collecting data on individual residents from four sources whenever possible: the residents themselves, line staff members caring for each resident, resident observations, and family questionnaires. Analyses will examine the congruence of each data
source as well as the psychometric properties and the reliability and intertemporal stability of the measures (Kane et al., 1999).
Status of Quality of Life. In the past, several studies had found the circumstances of life in nursing homes limited (Diamond 1992; Gubrium, 1993; Henderson and Vespari, 1995). As shown in the previous pages, since the implementation of OBRA 87, quality of care in nursing homes has improved in some categories of care, but in other categories persistent problems remain. For quality of life in nursing homes, the situation is not as encouraging. On the positive side, improvements in care, such as reduced use of physical and chemical restraints, also improve aspects of quality of life, including autonomy and dignity. On the negative side, evidence of deficiencies in care, such as the high prevalence of incontinence, is not consistent with high quality of life. Even though OBRA 87 had beneficial effects on several measures of quality, Kane and colleagues (1997) for example, found that it was difficult for nursing home residents to exercise desired choices or for nursing assistants to enhance residents' choices. Poor quality of life in many nursing facilities continues to be a concern. Until sufficient trained staff is available to allow time and skills to provide the care and personal attention, and until the standards of quality of life included in OBRA 87 are rigorously enforced, problems with quality of care and life will persist in some facilities.
In recent years, efforts have been made to improve the quality of life in nursing homes as well as the ability to measure it. For example, Rader and colleagues have been developing approaches whereby bathing can be a more individualized and pleasant experience for residents (Rader et al., 1996; Hoeffer et al., 1997). Efforts to measure quality of life for nursing home residents with dementia have accelerated in the last few years; the available tools include scales administered to residents, staff, and or family (Lawton et al., 1996; Logsdon, et al., 1999; Rabins et al., 1999).
Innovations. In recent years, new approaches are beginning to be developed to restructure social and physical environments intended to support quality of life in nursing homes. These models represent a departure from the traditional institutional physical environment of nursing homes. A number of architects specialize in nursing home design. For example, they are removing the nursing stations from view, providing lounge space instead of being shared by residents and staff, and using alcoves in the hallways for medicine carts and work space for the nursing staff. To break the monotony of the environment, aquariums and pianos are being introduced (Ouslander et al., 1997). A loose consortium—whose members refer to themselves as “the nursing home pioneers”—is working to improve life in nursing homes, which they consider to require a culture change
(Fagin et al., 1997). Among their strategies are approaches that engage all residents as a community when feasible (Barkan, 1995), give nursing assistants more responsibility and flexibility, and emphasize processes of care that minimize dependence and promote more independent functioning as far as possible (Lustbader, 2000). For example, residents may serve on committees that interview and select staff or attend staff meetings whatever the subject (Burger, 1999).
One well-known innovative experiment, called the Eden Alternative, has brought plants, birds, and a variety of animals, and visits by children into nursing homes. This approach also moved towards empowering staff and developing caregiving teams that would make nursing homes more amenable to individualized care (Thomas, 1994). However, its effectiveness and transferability to other nursing homes with varying leadership, ownership, and casemix have not been rigorously evaluated. Some also fear that it has been grasped too quickly and that facilities introducing it may not be committed to the steady, persistent change needed to alter the quality of life in a nursing home.
Quality of life is also affected by the physical surroundings, which can be pleasing or depressing and can promote independence or dependence. In particular, most residents, prospective residents, and families consider a private room and bath important to independence, dignity, and social interaction (Kane et al., 1998a). A few new facilities are being designed entirely or almost entirely with private rooms.
Another model involves redesigning a facility, emphasizing small neighborhood concepts, or changing staffing patterns to promote continuity and the idea of the universal worker who can perform a variety of tasks (Fagin et al., 1997).3 Variants of this neighborhood approach are found in other facilities. 4
|
3 |
For example, Fairport Baptist in Fairport, New York, now consists of several nine-resident “neighborhoods” with five single rooms and two L-shaped double rooms that maximize privacy. With no central hallways, each neighborhood has laundry facilities, a residential kitchen (where residents have access to the refrigerator), a dining area, and a sitting room but no nursing station. Meals are prepared in the centralized kitchen but are served in each neighborhood. All bedrooms and bathrooms have been decorated with features selected by the residents moving in. Most staff are assigned to neighborhoods to perform a range of tasks (e.g., personal care, housekeeping, serving meals), rather than operating centrally with responsibility for performing a smaller range of tasks for a larger number of residents. The nursing assistants, known as resident assistants, perform a wide range of tasks, including personal care, housekeeping, laundry, serving meals, and washing dishes in the kitchen 's dishwasher. Centralized staff have been drastically reduced or eliminated (including housekeeping and wait staff), and staff ratios on the neighborhoods have increased (e.g., each neighborhood has one full-time staff at night). Residents are actively involved in planning their activities and their lives, including the design of the stained glass windows for a large central chapel under construction. A day care center is prominent in the facility, and the children interact with the residents. |
|
4 |
Some examples are: Evergreen in Wisconsin (Fagin et al., 1997) and Lyngblosten Home in Minneapolis (Wolfe, 1999). The latter is experimenting in a small portion of its facility with a Swedish model called the “service home” to assess if it can be applied to a certified nursing facility. Each resident has a private room and private bath, and all cooking is done in the experimental neighborhood of nine people. |
An example of a successfully restructured nursing facility was reported to the IOM Committee on the Adequacy of Nursing Staff in Hospitals and Nursing Homes (IOM, 1996a, p. 255–256). The model of nursing care delivery implemented at the facility changed nursing care from a task-oriented system to a resident-oriented system by assigning primary nurses and their associates ongoing responsibility to care for a designated group of residents. The number of hours of care did not increase, but the skill mix did; the amount of licensed staff coverage over a 24-hour period increased from 24 to 45 percent. The increase of licensed staff is perceived as having improved the quality of care and the quality of life for residents and quality of work for staff, while remaining cost-effective. Ongoing data collection at that time supported this assertion, documenting notable reductions in the use of restraints and antipsychotic drugs, decreases in hospitalization rates, high resident satisfaction rates, reduced staff turnover rates, and high levels of success with various forms of rehabilitation despite a continuously rising acuity level and an average age of 91 years.
At present, many of these innovative programs are relatively recent and rare. These and other similar examples, however, suggest that cultural change may be possible in nursing homes. Also, current federal and state regulations, despite their many strengths in defining standards of care, are not conducive to these types of changes. For example, the presence of birds or animals could violate state regulations, and some of the staffing arrangements could skirt the boundaries of regulatory acceptability. A facility may also be at risk of violating rules related to food service when residents cook or when residents and staff together determine ways to enhance their meals and snacks. More than 50 waivers of regulations were required in one model to implement its demonstration unit (Wolfe, 1999).
These approaches are intuitively very appealing and appear to avoid some of the quality-of-life problems common in traditional nursing homes. Given this, defensible data describing how life or care is better for residents living in these homes should be collected so that the quality implications of these models can be understood. Although the concepts behind the new care models are very appealing, details about how they work and, more specifically, for whom they work best are still unknown.
Research, demonstration, and evaluation studies are needed to carefully describe the new interventions, and to evaluate their cost-effectiveness and their impact on quality of life and quality of care, when casemix is taken into consideration.
Limitations of the Evidence
Several limitations exist in the empirical evidence reviewed on quality of care in nursing homes. Averaging facilities is problematic—failure to improve in some facilities may be masked by large improvements in others, and vice versa. Average rates do not measure quality of care for individual residents.
As is common with studies using self-selected samples, some believe that the literature on nursing home quality may have problems with bias if results are based on sampled facilities willing to participate in the studies. The assumption is that willing participants are likely to be more receptive to regulatory and nonregulatory efforts aimed at improving quality. Others contend that there is no empirical evidence to support this concern. They advance the argument that many facilities regarded as poor performers are willing to participate in studies; they may be unaware of their relative performance. Also not all studies use convenience samples. Many use random samples of facilities with high participation rates. Other published studies have used data from OSCAR, the survey process, or the MDS. The validity and reliability of these data have been questioned by some. Since much of OSCAR and MDS data rely on reporting from facility staff, underreporting of problem areas is possible. Some items from the first version of the MDS showed adequate reliability; others did not perform as well (Phillips et al., 1993b; Crooks et al., 1995; Hawes et al., 1995b). Validation studies of the MDS version 2.0 found that new and revised items have both reliability and clinical utility (Blaum et al., 1997; Hawes et al., 1997b,c; Morris et al., 1997; Phillips et al., 1997). Problems with state survey reliability have been reported (Abt Associates and CHSRA, 1996; CHSRA, 1997; GAO, 1998a). In the state survey process, measures are derived from assessments by surveyors, pointing to the need for better training for surveyors.
In summary, there is sufficient cause for concern about poor quality of care in a number of nursing homes in the United States. Although care has improved in many facilities since OBRA 87 and there are some interesting models evolving to improve the physical environment, the configuration of staff, and the overall quality of life of residents that should be evaluated, the attention of policy makers must continue to be focused on those facilities that provide inadequate quality of care.
Community-Based Residential Care
As discussed in the previous chapter, a wide range of residential care facilities house people with long-term care needs of multiple levels. As many as one million people live in all types of board and care homes (Newcomer and Grant, 1990; Clark et al., 1994). The area of quality in these settings has received little research attention in the past.
No uniform definitions or criteria exist for judging the quality of care provided in these settings. Given the variations within and across states, comparisons among even similarly labeled facilities can be difficult. Moreover, assessments of the quality of residential care can be further complicated by the inclusion of measures of the physical environment, the ability of residents to remain in place following declines in functional status, and the delivery of services by facility staff versus external agency staff. If these factors are not uniformly incorporated into quality assessments, comparisons of and judgments about the quality of care delivered in these settings can be difficult.
Various studies have indicated that residents in nonmedical residential facilities were not receiving adequate care or protection (GAO, 1989, 1992a,b; Avorn et al., 1989). These studies showed unsafe and unsanitary conditions, improper use of psychotropic medications, and many other problems. These problems are heightened by rising resident acuity and high use of medications, questions about capacity of existing supply of professional staff to meet the needs of more impaired resident populations, and wide variations in regulatory approaches and concern about adequacy of most states' regulatory systems.
Board and Care Homes
Board and care homes have been around for many years and have filled an important need in long-term care for many elderly people and people with disabilities.
The main purpose of the 10-survey of board and care homes described in the previous chapter was to determine whether regulatory systems had an effect on the quality of care provided (Hawes, 1995a). The researchers found that the widespread perception that board and care homes are small, and therefore more “homelike,” is somewhat misleading. Although most homes were small with 2–10 beds, more than three-quarters of the residents lived in homes with 11 or more beds. The majority of homes provided access to a range of services, but most were unable or unwilling to accommodate changing resident needs.
About 99 percent of the licensed homes and 76 percent of the unlicensed homes reported providing medication storage and supervision; 71 per
cent of the residents reported receiving assistance with mediations and 41 percent were taking psychotropic medications. Yet only 21 percent of the homes had a licensed nurse (RN or LPN) on their staff. Nearly 20 percent of the operators in licensed homes and 33 percent in unlicensed homes reported that they did not require any training for staff. Of staff who reported passing medications, 28 percent of staff giving injections were not licensed nurses. The staffing patterns, training of staff, and a lack of appropriate staff knowledge, and some care practices raise concerns about the quality of care provided in board and care homes. There is particular concern regarding the quality of care in some board and care homes that serve people with developmental disabilities and mental illnesses.
The study (Hawes et al., 1995a) found positive effects of regulation on safety, quality of life, and quality of care. States with extensive regulations had fewer unlicensed homes, and operators of the homes were better trained and with prior experience in providing health care and quality of life. Extensive regulation was associated with lower use of psychotropic drugs and use of fewer contraindicated medications, and positively associated with several quality-of-life measures such as preventing a very institutional environment, and the availability of social and recreational aids and supportive aids and devices. The study found no effect of extensive regulation on staff training, availability of licensed nurses on the homes' staff, knowledge of basic procedures and appropriate monitoring of health conditions and medication administration, availability of services, cleanliness, prevalence of safety features, and availability of physical amenities.
Assisted Living Facilities
Assisted living has become a popular subset of residential care facilities. They have been marketed as an option that could combine a capacity for high-quality individual service with physical environments that promote consumer choice, autonomy, dignity, privacy, and continuity with preferred lifestyles. Evaluating success or failure in meeting this objective is difficult because of limited data and the enormous variation among facilities and services. Hawes and colleagues (1999), reporting on the results of a large national probability sample survey of assisted living facilities having 10 or more beds and serving primarily older adults, found that 65 percent of facilities offered low levels of service (e.g., no full-time registered nurse on staff), with another 5 percent offering minimal services (see Chapter 2 for a description of the survey). Thirty-one to 34 percent of the facilities offered high levels of privacy, 40 percent offered low levels of privacy, and 26 to 28 percent offered only minimal levels of
privacy.5 Only 11 percent of the facilities provided high levels of both privacy and service.
Assisted living facilities on a multilevel campus with nursing homes and other programs (45 percent) were more likely to express a willingness to retain residents with greater health care needs and to offer more nursing care; however, they did not report having a more demanding casemix than freestanding programs. Almost half of the administrators interviewed indicated that their assisted living facility would not admit or retain a person with moderate to severe cognitive impairment.
The researchers concluded that there is a gap between the assisted living services currently offered and the philosophy of assisted living, which aims to combine private, residentially oriented buildings with high levels of service and “aging in place,” regardless of changes in health or physical and cognitive functioning. Many facilities that call themselves assisted living fall short on one or more of these criteria. They also concluded that most assisted living in this country was not affordable for the moderate- and low-income elderly population and that affordable facilities were more likely to offer low or minimal levels of service and privacy (Hawes et al., 1999).
In Oregon, the regulatory model for assisted living requires high privacy and autonomy-enhancing features (e.g., locking doors, private-occupancy apartments with bathrooms equipped with roll-in showers, capacity for cooking and refrigerating food, and individualized care plans), and high service capability (e.g., three meals a day and personal care to enhance aging in place).
Quality-of-care problems, however, are reported for some assisted living facilities. A GAO (1999c) review of assisted living services in California, Florida, Ohio, and Oregon found that 27 percent of the facilities reviewed had been cited for five or more quality-of-care or consumer-protection deficiencies or violations during 1996 and 1997. The types of problems identified included providing inadequate or insufficient care; having insufficient, unqualified, and untrained staff; administering or storing medications improperly; and not following state admission and discharge policies. Another issue is holding assisted living settings responsible for developing plans of care. For example, Yee and colleagues (1999) found a need for more social activity and community involvement for residents in a congregate housing-type setting. Other factors that may
|
5 |
High privacy facility is defined as one in which 80–100 percent of the units were private; low privacy facility is one that had no bedrooms shared by three or more unrelated persons, but in which fewer than 80 percent of bedrooms were private; minimal privacy facility is one that housed three or more unrelated individuals in the same bedroom (whether in a room or apartment). |
make the situation more challenging are overbuilding leading to lower occupancy, problems with fiscal solvency, and incentives to accept and retain residents with greater care needs but pressure to preserve high rates of return by containing staff costs.
Among the various potential quality-of-care problems in assisted living settings discussed above, two conflicting concerns are raised. Some observers are concerned that assisted living offers a false promise to consumers of aging in place and that providers will be unwilling and unable to retain residents when their care needs become substantial. Others fear that assisted living settings will retain residents but fail to offer them needed services or, in the worst case, fail even to discern their deteriorating condition and need for services. One potential aid against either problem is ensuring that consumers have accurate and complete information about services available and allowed, policies regarding access to care and changing care needs, and charges. GAO (1999c) concluded that the variation among facilities and services designated as assisted living means that consumers must rely primarily on providers for information about services and policies. Currently, however, consumers often have inadequate information to use in selecting a facility and admission agreements often are misleading about what consumers can expect regarding continuing stays, discharges, services, and costs; and sometimes inconsistent with state law.
Adult Foster Care Homes
Another type of residential care is the adult foster home that typically provides care for a small number of residents (usually three to six) in private homes with a live-in care provider. They are licensed by states under a variety of names, with regulatory differences among states in terms of requirements and options (Folkemer, 1996). In most states, adult foster homes generally serve a low-income clientele, often with mental health problems.
In Oregon, the adult foster care model, introduced in 1982, has proved to be a popular mainstream program. By 1989, two-thirds of the foster home clients were privately paying individuals with higher levels of disability than those covered by Medicaid who, by definition, were eligible for nursing home care (Kane et al., 1991a). Controlling for casemix, a cross-sectional study found more socialization and satisfaction among foster home clients than nursing home residents (Kane et al., 1991a). A longitudinal study comparing Medicaid beneficiaries in adult foster care and nursing homes found no change in functional status for more than 85 percent of the clients, but among those with changes, the nursing home group showed more improvement and the foster care group more decline
(Stark et al., 1995). Although critics question how to interpret these data (e.g., whether functional status was the right outcome to assess), the study seems to suggest that foster care is a viable choice but could be improved by better access to medical and nursing care.
In terms of quality of life, adult foster care homes offer advantages related to homelike settings, but they also have disadvantages related to their small scale and reliance on the live-in caregiver for personal care, cooking, housekeeping, and recreational services, with little margin to cover additional help. In the Oregon program, for example, if one resident is bedridden or needs intensive nursing care, the foster care provider is less likely to be able to devote attention to activities for other residents. It seems probable that consumer satisfaction with adult foster care will depend not only on the intrinsic quality of the home but also on individual lifestyle preferences. Some people welcome the friendliness of a good adult foster home, whereas others prefer the privacy of a residential care setting over joining a stranger's household.
Residential Care for People with Developmental Disabilities.
During the mid-1980s, approximately 70 percent of people with developmental disabilities were cared for in institutional settings. OBRA 87 included a requirement that people with developmental disabilities living in nursing facilities be transferred to alternative settings if they did not need skilled nursing care. Since then, approximately one-quarter of the more than 50,000 people with developmental disabilities who had been living in nursing homes have moved to other facilities (Braddock et al., 1998). In addition, a growing number of states are providing services to people with developmental disabilities under Medicaid home and community-based services (HCBS) waivers. The majority of long-term care users with developmental disabilities now receive their formal care in the community.
Community-based living and smaller facility size have been associated with benefits such as increased community integration, adaptive behavior, choice making, mobility, family satisfaction, improved health, and decreased challenging behavior (Rotegard et al., 1983; Wilson et al., 1991; Heller et al., 1995; Conroy, 1996; Tossebro, 1996; Stancliffe, 1997; Stancliffe and Abery, 1997; Heller et al., 1998). Even for older persons with developmental disabilities, evidence indicates a positive long-term adjustment following movement from nursing homes to community-based settings (Heller, 1985; Heller et al., 1995, 1998). Smaller, community-based facilities are more likely to have policies and practices that support individual choice, to provide more individualized services with increased opportunity for variety and stimulation, to support community participa-
tion, and to involve residents in policy making (Conroy, 1996; Tossebro, 1996; Stancliffe, 1997; Heller et al., 1998).
However, some investigations have found problems with both poor quality and inadequate access to services in Medicaid waiver programs. A study of 1,878 persons with developmental disabilities in California found an elevated risk-adjusted death rate following deinstitutionalization, particularly for the highest-functioning individuals (Strauss et al., 1998; Shavelle and Strauss, 1999). The higher death rates for individuals with developmental disabilities were in part due to problems such as aspiration of food into the lungs or bowel impaction. HCFA investigations determined that similar problems existed in other states, many of which seem to be due partly to states providing inadequate case management services for monitoring quality of care.
Because the few studies that have been undertaken have found quality-of-care problems in all types of residential care, it is suspected that problems are widespread but generally unobserved. In any case, it raises the issue of the need for research on quality of care and particularly outcomes of care.
Home Health Care
Data on the quality of home health care are much less voluminous and systematic than those available for nursing homes. Most of the available data derive from HCFA's National Home Health Agency Prospective Payment Demonstration and from its support of research and demonstration projects using the Outcomes Assessment and Information Set (OASIS), which is now mandated for use by Medicare-certified home health agencies.
Few research studies have actually examined the quality of home health care. Most of the information about quality is available from the state survey agencies under contract by HCFA to regulate home health care. Research funded principally by HCFA has produced some data on processes of care and some on patient outcomes. Because a substantial percentage of home health care is financed by Medicare and because Medicare home health care services have grown rapidly over the past decade, research has focused on Medicare certified home health agencies, and many of the studies have centered around predictors of use and expenditures.
In recent years, GAO has conducted investigative studies of home health care agencies. In a study of home health agencies that had been certified, GAO (1997b) found that very poor care was provided by a number of agencies. Several examples were cited showing problems such as agency administrators with no health care experience, and agencies
serving ineligible patients and falsifying records and staff credentials. On the other hand, GAO investigators found that only 3 percent of all certified agencies are cited by HCFA for being out of compliance with one or more conditions (GAO, 1997b).
In recent surveys by HCFA's Operation Restore Trust which reassessed certified home health agencies in California, HCFA found significant quality-of-care problems that led to the termination of many agencies from the Medicare program. In resurveys of 44 agencies providing high numbers of services and receiving high levels of Medicare payments, HCFA found that 80 percent were out of compliance with at least one of the federal conditions, and 21 of the 44 either voluntarily withdrew from the program or were terminated by HCFA. In these surveys, HCFA found agencies that could not provide lists of active patients, and did not know which patients were receiving care on a particular day, staff that were providing patients with medications not ordered by a physician, therapists who were not qualified, and laboratory services that were not monitored. They also found failures to provide nursing care as ordered and failures to initiate changes in patients' care plans (GAO, 1996a, 1997b, 1998b,c).
On the other hand, a retrospective review of Medicare patient records undertaken for agencies participating in HCFA's prospective payment demonstration revealed problems with potential adverse patient impact in only about 4 percent of the cases (Phillips et al., 1994). In the process of developing OASIS, a prospective study was conducted to assess the care provided for new patients by 44 Medicare-certified agencies in 27 states with approximately 2,600 patients, particularly related to six activities of daily living. The study compared rates of stabilization and improvements in functional status for two groups —those admitted for home health care from the hospital and those admitted from the community. Overall functional status was stabilized for 79 and 92 percent of patients in each group, respectively (Shaughnessy et al., 1994a). Rates of improvement in function ranged from 26 percent for ambulation among patients admitted from the community to more than 54 percent for bathing among those admitted from the hospital. Consistently lower rates of improvement among the group admitted to home health care from the community were attributed to the greater prevalence of chronic functional impairments in this group. Patients admitted from the hospital were more likely to have acute problems for which functional stabilization or improvement would be expected (Shaughnessy et al., 1994a).
Appropriateness of Services
In another major HCFA-funded study, Kane and Finch et al. (1994) examined the costs and outcomes of 2,100 elderly Medicare patients from
three cities who were discharged from hospital to post-acute care settings with one of five diagnoses: stroke, chronic obstructive pulmonary disease, congestive heart failure, hip procedure and hip fracture. They found that in general patients who received home health care had better functional outcomes than those who went home without home health services. Subsequent analyses stemming from this study concluded that at six weeks, six months and one year post-hospital discharge, patients who received home health care experienced significantly higher functional improvement than patients discharged to other post-acute care modalities (rehabilitation facilities, skilled nursing facilities or home without home health care) (R.L. Kane et al., 1998). This study, however, did not examine the nature of home health care provided. Thus, no information is available on the type of personnel who provided care, their level of training, or the degree of physician involvement.
Findings on Process of Care
Under contract to HCFA, Abt Associates conducted the largest empirical assessment to date of process of care deficiencies in Medicare certified home health agencies (Phillips et al., 1994; Jette et al., 1996). The study reviewed retrospectively the records for 4,000 patient episodes drawn from 47 agencies participating in HCFA's prospective payment demonstration. To each episode of care nurse reviewers applied 10 quality-of-care screens, including adequacy of baseline assessment and care planning, addressing all documented problems, addressing all acute problems immediately, delivering all prescribed nursing or therapy services, deterioration of ulcers/wounds, deterioration of ADL status, and adequacy of discharge plan. In cases where reviewers determined failure on a particular screen, they made an additional determination involving three levels of problem: (1) a problem without potential for significant adverse effects on the patient, (2) a problem with potential for significant adverse effects on the patient, or (3) a problem with confirmed significant adverse patient effects.
Overall, reviewers identified no quality problems in 57 percent of cases and at least one quality problem in 43 percent of cases screened (Jette et al., 1996). Two-thirds of cases failed only one quality screen, 28 percent failed two screens, and the remainder failed three or more. Four percent of total cases were judged to have a quality problem with the potential for (3.9 percent) or actual (0.4 percent) adverse effects on patients. However, the researchers estimated that the proportion of cases with potential adverse effects might have reached 14 percent if all records that failed an initial screen had been reviewed by two different nurses. The most frequently failed screens in this study were delivery of all pre-
scribed nursing or therapy services (33 percent of cases) and addressing all documented problems (20 percent of cases). Within the first area, inadequate evidence of patient teaching was the most commonly cited problem and within the second, inadequate evidence of follow-up on cardiovascular problems. As with all record review studies, the researchers could not separate inadequacy of documentation from actual lack of appropriate action on the part of the nurse or agency.
The Abt study revealed “considerable variation in level of quality care observed among the participating agencies” (Jette, 1996: 499). However, agency ownership was not significantly related to the frequency or severity of quality problems identified. Controlling for agency and reviewer characteristics, the likelihood of observed quality problems increased as patients ' condition became less stable and as the number of different services provided to the patient increased. When agencies' status as fee-for-service versus prospective payment providers was considered, the study found no significant difference in the existence of confirmed quality problems with a potential to adversely affect patients (Phillips et al., 1994). Although the study agencies contained a mix of ownership status and geographic representation, the researchers cautioned that as volunteers for a national demonstration, the agencies might not be representative of the home health industry as a whole.
Many of the concerns regarding Medicare-funded home health care are related to the amount and appropriateness of service use and to agency business practices. A GAO (1996a) report highlighted variations in home health service provision by region and agency ownership. Nationally, the number of home health visits per beneficiary per year in 1993 was 57; regionally, the average varied from 79 visits in southern states to a low of 36 visits in states in the Northwest. GAO suggested that some of the regional variation might be explained by the availability of substitute services or by the beneficiary casemix. Variations by agency ownership were equally striking. Proprietary agencies provided an average of 78 visits per beneficiary in 1993, compared to 46 each for government and voluntary nonprofit agencies (GAO, 1996a). A similar pattern was found at the regional level and when patterns of service use were compared for four common diagnoses (diabetes, heart failure, hypertension, and hip fracture). The variations in service use by agency type were greatest for patients with diabetes, a chronic problem, and least for those with hip fracture, an acute problem.
GAO (1996a) did not directly examine the effectiveness of various care plans but suggested that weak oversight might be leading proprietary agencies to provide more services than were needed by beneficiaries. Possible overuse of services was attributed in part to Medicare fee-for-service payment methods (since modified), in part to limited physician
review of the primarily nonmedical home health services, and in part to reduced funding for review of claims and on-site audits. Other GAO (1995, 1998b) investigations have documented financial irregularities and improprieties by specific agencies, including excessive skilled nursing visits, exaggeration of the severity of patient conditions, and services to patients of questionable eligibility.
Although little has been documented about the quality of home health care, many concede that the reports of these problems may not be isolated cases. Because of the rapid growth of home health agencies, with nearly 10,000 certified agencies in the beginning of 1997, the oversight problems are enormous (GAO, 1997b). The committee speculated that individuals living at home are reluctant to complain about poor quality of care for fear of losing their home care workers and receiving no services. Thus, oversight cannot rely simply on individual complaints about quality.
Home and Community-Based Services
Adults
Studies of HCBS usually concentrate on unmet need and its consequences (Allen and Mor, 1997) or satisfaction (Benjamin, 1998; Applebaum et al., 1999). Geron (1996, 1997) looked at satisfaction in terms of a number of issues that members of ethnic-specific focus groups said were important—for example, compatibility with providers, reliability of providers, task competence of providers, and adequacy of total service provision. Adequacy refers to getting enough services; competence refers to how services and care are performed; compatibility refers to the fit between the consumer and caregiver and the consumer's sense that the caregiver cares about him or her personally; and competence refers to the way personal care and homemaking tasks are literally conducted. Typically those who use home and community-based care of all types report high satisfaction (Geron, 1996; Benjamin, 1998; Kane and Huck, 2000). Such satisfaction is also reported for home care and day care delivered as respite services for dementia, though in these instances the respondents are typically family members. Reviewing empirical studies on respite care, Montgomery and Kosloski (1995) stated that “the most pervasive finding in the literature regarding the impact of respite services is that caregivers like the service and generally find programs to be valuable” (p. 50). Satisfaction is also high among general users of adult day care (Weissert et al., 1990).
The extent to which the availability of HCBS actually accounts for keeping people out of nursing homes has been hotly debated and is the subject of decades worth of research (Applebaum et al., 1986; Kane and
Kane, 1987; Weissert, 1997). In some of his writing, Weissert (1997) terms home care a failure because its users enter nursing homes at the same rate as the control groups. This also presupposes that the worth of home care is to be measured by its substitution for some other form of care (e.g., nursing home care or hospital care). These kinds of findings beg the question about the quality of home care itself. For the most part, critiques of home care for older people (Estes and Swan, 1993), as well as for persons with serious mental illness (Horowitz and Reinard, 1997) and for children with chronic illness (Perrin et al., 1997), chronicle lack of third-party payers and poor coverage of care rather than problems in care itself. There are no systematic studies in the literature to suggest that home care is of good or poor quality. The subject has been examined largely in relation to satisfaction, unmet need for care, or burden on family caregivers (which in some ways is another index of unmet need for care). Research on outcomes and other information on which to judge quality of these services is lacking.
Personal Care Services
Researchers have begun to describe the breadth and depth of Medicaid HCBS programs more fully, typically offering statistics on state and national trends (Litvak and Kennedy 1991; Burwell 1999; Miller et al., 1999a,b; Harrington et al., 2000d). Although the Medicaid personal care services (PCS) and HCBS programs have grown significantly over the past two decades (Miller et al., 1999a; Harrington et al., 2000b), the combined Medicaid PCS and HCBS waiver participants are less than the number of Medicaid institutional participants (Harrington et al., 2000a; LeBlanc et al., 2000a).
Wide variation exists among states in the total number of Medicaid PCS optional state plan benefit and 1915(c) HCBS waiver participants, ranging from 10.5 participants per 1,000 population in Missouri to less than 0.7 participant in Louisiana and Indiana (see Table 2.5). When Medicaid officials surveyed were asked if they had an adequate number of HCBS waiver slots or funding allocated for slots to meet the demand, only eight state officials replied that they had enough slots while 42 state officials said they either did not have enough slots or funds to fill the slots (Harrington et al., 2000a). The eight states that reported having adequate slots were: Missouri, Michigan, Rhode Island, North Dakota, Maine, Massachusetts, Alabama, and Arizona. Washington DC was just starting its waiver program so officials stated they did not know if they had adequate slots. Inadequate slots were most often reported for the mental retardation– developmental disabilities (MR/DD) programs. Of the 42 states reporting waivers with inadequate numbers of slots and funds, 37 states had inad-
equate numbers of slots and funds for individuals with MR/DD. In other states, there were inadequate numbers of slots and funds for the aged, those with disabilities, those with traumatic brain injuries, children with special health care needs, and those with HIV/AIDS.
Twenty-eight states report waiting lists in the waiver program, but 14 states could not report and the numbers ranged from 20 physically disabled in South Dakota to 11,000 on the aged and disabled waiver waiting list in Wisconsin. Louisiana reported 7,063 on the MR/DD waiting list and the wait for services was estimated to be 5 years in length. Although states reported that some legislators were sympathetic to the need to expand HCBS, most states with waiting lists had been unable to obtain adequate state funds for the program from the state legislature. Seven other states reported being involved in state litigation cases pertaining to waiting lists for HCBS services (California, Florida, Montana, New Mexico, Oklahoma, Texas, and West Virginia). Two states were under court rulings to either downsize the state facilities for individuals with MR/DD (Tennessee) or provide HCBS services for the mentally ill aged 22–64 (Colorado).
One of the most important reported barriers to the expansion of PCS and HCBS waiver services was the shortage of direct care workers, particularly those working in the home. States with large rural populations faced particularly imposing challenges. State officials identified these shortages as being related to the growing competition in the labor market and the low state Medicaid reimbursement rates for HCBS providers. Wage, benefit, and working condition studies may be needed to assist states in establishing market-based rates for home care providers. Perhaps special federal financial support could be designed to assist state Medicaid programs in increasing their state reimbursement rates for HCBS providers.
In summary, both PCS and HCBS programs appear to be expanding to meet the growing needs of Medicaid participants who are aged or disabled. The problem is that there is a large unmet need in many states based on the reports of state officials and waiting lists. Two major questions remain to be addressed. One is how to ensure that Medicaid participants are offered a choice between institutional and HCBS services and have access to appropriate services in the least restrictive environment. The second is how to ensure equity in access to PCS and HCBS services across states. Should the federal government require states to offer alternatives to institutional care for all Medicaid participants? Alternatively, should special programs be established to give incentives to states to expand access to PCS and HCBS services, while at the same time controlling the growth and expenditures for institutional care? A Blue
Ribbon Panel on Personal Assistance Services (1999)6 reviewed federal and state statutes and regulations for personal care services and home and community-based services. The panel produced several recommendations and strategies for the federal and state governments to implement and promote consumer choice in community-based placement for people with disabilities who require routine, ongoing personal assistance services. The panel also urged HCFA to abandon the link between Medicare and Medicaid certification requirements for providers of home and community-based services.
The committee concludes that research is needed to identify the need for PCS and HCBS services and to examine policy options that would remove the barriers and constraints that states are facing to meet the need for services. The committee believes that HCFA and state governments should work with providers and consumers to undertake research towards developing an appropriate array of community-based long-term care services to meet the needs of consumers and assess the quality of the service and outcomes. At the same time, access to and choice of appropriate services can be argued to be essential to quality of care and quality of life for individuals with disabilities.
Department of Justice regulations implementing the Americans with Disabilities Act (ADA) now require that “a public entity shall administer services, programs, and activities in the most integrated setting appropriate to the needs of qualified individuals with disabilities ” (28 C.F.R. 35.130(d)). In the recent Olmstead v. L.C. case, the Supreme Court held that institutional placement of individuals who could live in less restrictive settings may violate the ADA. The Court indicated that states are required to provide community-based services for persons with disabilities when state professionals determine that such placement is appropriate for the particular individual, the affected person does not oppose such treatment, and the placement can be reasonably accommodated without altering the program through which services are provided. The Department of Health and Human Services issued a letter to state Medicaid Directors regarding the Olmstead decision and informing states about ways to comply by preventing inappropriate institutionalization and providing home and community-based alternatives. Most states have much work that needs to be done to change their programs to ensure choice and access. The challenge is to reduce the reliance on institutional care and to shift services to the home and community when such care is appropriate.
|
6 |
The panel was funded in 1997 by the Robert Wood Johnson Foundation through a grant to the Independent Living Research Utilization Program at The Institute for Rehabilitation and Research. |
Home Care for Children and Adolescents
Children with major medical and technological needs often leave the hospital with careful plans for care and supervision from nurses and other caregivers with expertise in pediatric care. Difficulties often arise for families in providing or arranging long-term care at home and in the community with the loss of connections to hospital programs, limited communications among key providers, changes in home nursing care providers, and changes in the child's health situation. Moreover, many home care providers (mainly nurses) have little training or experience in the care of children. Instead, they may come from a background of providing care for older patients with very different conditions and know little about children's medication doses or equipment needs, or appropriate ways to monitor a child's condition or progress (Feinberg, 1985). At the point of discharge, hospital staff typically choose the nursing team to help the family at home or in the community based on their capabilities in caring for younger patients, but over time as staff change, later nursing personnel may have much less relevant experience. Nursing staff providing home care also have less supervision than hospital staff, and again agencies or programs may lack personnel equipped to supervise home and community care for children. Parents also report that equipment suppliers provide too little information regarding the use of their devices in the home, making it difficult for families to determine when the machine is malfunctioning or what to do about it.
Parents also complain about the interference of some home service personnel in their daily life routines. Although having complex equipment and additional care providers will change any household's activities, at times agency staff interfere inappropriately in how parents discipline their children or indicate disapproval of aspects of the family' s living situations (Perrin et al., 1993).
Children and adolescents receiving long-term care services typically interact with a large number of service providers, including primary and subspecialty medical providers, nursing staff, equipment suppliers, and specialized therapists. A lack of coordination of these services can lead to conflicts among service providers, duplication of some services, and lack of access to others. Although families often learn over time how to coordinate services themselves, problems persist for many. Several programs (see Stein, 1998) exist to help families coordinate services, improving the quality and extent of services received (Stein and Jessop, 1984, 1991). Care coordinators may offer direct care, financial counseling, coordination among medical providers, teaching about the child's care needs, emotional support, coordination among the medical, education, and home nursing systems, help in finding services for the child, and guidance in
teaching families to provide care coordination on their own. Few standards for training and qualifications of care coordinators exist, making assessment of these activities particularly difficult (Perrin et al., 1993).
Parents further report that care plans and services may not change frequently enough, leaving outmoded arrangements in place when the child's and the household's needs have changed. Most conditions leading to long-term care needs for children and adolescents are dynamic, requiring changes in treatments, technological assistance, and monitoring over time. The ability of family members to contribute to a child's care also may change. For example, family members may be able to provide an increased amount of care because they have developed the skills to provide certain services or a decreased amount of care because of changes in employment or family status. Other problems facing families caring for children at home include increased risk of depression and financial hardship (Quint et al., 1990; Thyen et al., 1999).
These shortcomings in home care services, especially for children, point to several likely opportunities to improve the quality of this care. In particular, efforts should be made to ensure that professionals involved in care have appropriate training and skills. Coordination of care should be viewed as an important component of the services available to families, either through trained care coordinators or through opportunities for family members to become care coordinators. Care plans can be used to establish goals for care, select measurable indicators of progress toward those goals, and allocate responsibilities among caregivers. With a person-centered approach to care, families should have the opportunity to participate as full partners in the formulation, implementation, and monitoring of such plans. In addition, family support services should be viewed as part of the array of services contributing to the quality of care.
Emerging Consumer-Directed Service Models
Consumer-directed service models have a brief history compared to traditional institutional and home care. They provide varying levels of consumer involvement and varying mechanisms of support for consumer direction (Flanagan and Green, 1997). Choice is typically between programs that provide cash payments and leave all service management to consumers or programs that allow consumers to delegate all of their service management to an agency. Formal evaluations of consumer-directed service models are still limited. The studies reviewed by the committee vary considerably in their size, methodological rigor, and vulnerability to biases. Nonetheless, the committee believes that taken together, the findings of the evaluation studies to date suggest that a consumer-directed approach may benefit a significant proportion of individuals with dis-
abilities. Some studies have examined the impact of consumer-directed models on factors such as quality of life, control, productivity, use of preventive health care, and cost. Others have examined the impact of cash payment models. The findings from these evaluations are summarized below.
Impact on Users of Services. As noted in other parts of the report, the oldest consumer-directed service benefits are the Housebound and Aid and Attendance Allowance Program, operated by the Veterans Administration (Cameron, 1993). More than 200,000 veterans and surviving spouses received—by choice —cash benefits in place of formally provided homemaker, personal care, and other services. Funds may be spent on whatever consumers believe best meets their health and personal needs. An evaluation of this program suggested that participants received similar hours of care and were no worse off with regard to acute health care utilization than a comparison group receiving traditional services (Grana and Yamashiro, 1987). This evaluation unfortunately did not include measures of quality of care or life.
Most consumer-directed services and their evaluation have focused on personal care services. For example, a 1993 poll of 800 Medicaid beneficiaries who hired independent providers, rather than using agency providers, reported higher levels of satisfaction with care, provider stability, and quality of life (Harris and Associates, 1993). Two studies of personal assistance models in Virginia and California show increased productivity and satisfaction for individuals with physical disabilities. In Virginia, evaluations of consumer-directed personal assistance services compared outcomes for very small samples of individuals who received consumer-directed services through state Centers for Independent Living and those on the waiting list for such services (Beatty et al., 1998a). Consumer-directed services, including funding for personal assistance, as well as assistive technology, home modification, and adaptive equipment, were associated with greater reported control over one's life, greater satisfaction with services, and greater availability of services (Beatty et al., 1998b); increased productivity and employment (Richmond et al., 1997); and greater use of preventive health care (Adams and Beatty, 1998). The individuals on the waiting list tended to have less service needs, as assessed by the Center, than did individuals receiving the services. Although receipt of these services was based on need, it is possible that the frustration of waiting could have been reflected to some extent in the satisfaction scores for those on the waiting list.
In California, Benjamin (1998) interviewed by telephone 1,095 low income people who were aged or disabled or blind and who participated in either a consumer-directed or professionally directed program. Approxi-
mately half of the users of consumer-directed services were 65 years of age and older, and 52 percent had severe disabilities compared to 13 percent of the other group. Generally, users of consumer-directed services scored higher on variables related to service choice and satisfaction and preferred role of provider than did the users of professionally directed services. Also individuals who participated in consumer-directed service to pay for services from family members reported a significantly greater sense of security and interpersonal satisfaction. On dimensions of consumer safety and unmet need, neither model showed a significant advantage over the other.
Tilly and Bectel (1999) reviewed Benjamin's study and four European studies of consumer-directed cash payment service models in Australia (Badelt et al., 1997), Germany (Runde et al., 1996), the Netherlands (Miltenburg et al., 1996), and France (Gilles et al., 1995; Simon and Martin, 1995). They found that in these studies the receipt of cash subsidies was associated with enhanced perceptions of control over services and supports compared to agency services, allowed consumers to compensate relatives for care and to purchase more services, and enhanced overall quality of life. Simon-Rusinowitz and colleagues (1997) interviewed about 490 Medicaid personal assistance clients to assess predictors of consumer interest in the cash option model. Almost one-third of the respondents reported an interest in the cash option. They found that the greatest predictor of interest in a cash option was the individual's willingness to perform employer tasks, followed by a desire for involvement with one's own caregiving. Of those who expressed interest in the option, over half would use the cash to purchase more hours of service, followed by equipment and transportation.
Some studies report a positive association between perceptions of control and quality of life for individuals with disabling conditions (Rodin, 1986; Hofland, 1988). Other research has linked perceived control to health, disability, and quality of life among older adults (Salomon et al., 1998). Nosek et al. (1995) found a similar association between ratings of life satisfaction and control over long-term care, regardless of whether the care was provided in an institution, by an independent provider, or by a paid or unpaid care provider.
Although these consumer-directed options are relatively untested, preliminary evidence suggests their viability for people with disability receiving personal care services. Long-term care service users may be more satisfied with consumer-directed services and may benefit from other aspects of the arrangement, but from a quality perspective, there is little evidence-based research for concluding that consumer-directed services result in better quality of care. There is also a lack of an evidence base regarding the relationship between consumer-direction and con-
sumer risk, both increased and lack of risk. In the absence of such research, those who want to promote or curtail self-direction fall back on beliefs, anecdotes, and assumptions. More research is needed that focuses on the benefits and risks of these models, and on the association between choice and participation in decision making and the quality of care.
Recommendation 3-1: The committee recommends that the Department of Health and Human Services, with input from states and private organizations, develop and fund a research agenda to investigate the potential quality impact associated with access to, and limitations of, different models of consumer-centered long-term care services, including consumer-directed services.
CONCLUSION
Characterizing the quality of long-term care requires coming to grips with different criteria for quality and determining how to make trade-offs among various features of quality. Much more work is needed on these issues, including how to consider safety in comparison to other concerns; whether and how much to consider the quality of the physical environments in residentially based long-term care; and how to incorporate consumer choice and direction into quality assurance and quality improvement efforts. Moreover data and research are very scant for residential care and home care compared to information for nursing homes. Much of the long-term care literature other than nursing homes has focused more on adequacy of access and consumer satisfaction than on quality of care.
Allowing for these current limitations in characterizing quality, the committee's review of the available literature points to several general conclusions about the quality of care in various long-term care settings. Since the enactment of OBRA 87, nursing home care has improved in some areas with less use of physical restraints, better use of psychoactive drugs, and less use of urinary catheters. In other areas, such as prevention and treatment of pressure sores and incontinence care, quality problems remain and appear particularly persistent in some facilities. The quality of life in some nursing homes has been improved by the adoption of more consumer-centered approaches to care, but features such as lack of privacy continue to be problematic.
Residential care presents a mixed picture in terms of both quality of care and quality of life. Some small group homes and assisted living facilities offer high-quality care in settings that afford maximum privacy and dignity. However, others appear to lack adequately trained staff and
to offer neither sufficient amounts of care nor “homelike” settings and the privacy that goes along with it. There are also indications that consumers may receive too little information to make informed choices regarding assisted living services.
Evidence regarding the quality of home health care is more limited than that for nursing home care, but also points to a mixed experience. Moreover, most of the research in this area measures satisfaction and unmet need, and not quality of care. Medicare-funded home health care generally appears to be of adequate quality in terms of the transactions between caregivers and care users. However, the program has suffered from problems of overuse and inappropriate use, leading to new constraints on payments that may adversely affect the availability of services for those with the most complex care needs. Access to HCBS and especially personal care services for people with disabilities needs to be improved and an array of options need to be developed and tested.
This review of the current quality of long-term care has highlighted for the committee several areas of concern, including lack of standard measurement tools and data to use in more systematic assessments of the quality of care in various long-term care settings, evidence of persistent problems in certain aspects of care (e.g., treatment of pressure sores) and in certain facilities, and indications that some problems can be traced to insufficient staff training or inadequate staffing levels. Subsequent chapters address various strategies for responding to these concerns with specific recommendations for improvements. Since no single strategy will be appropriate or sufficient to achieve the broad range of quality improvement goals in long-term care, the aim must be to find the mix of strategies that will most successfully balance differing views and goals.





































