Executive Summary
Abstract. This report provides an independent assessment of the current policies and potential impact of a pending new federal regulation (the "Final Rule") on the system of organ procurement and transplantation.
One of the most visible and contentious issues regarding the fairness of the current system of organ procurement and allocation is the argument that it results in great disparities in the total amount of time a patient waits for an organ (i.e., the time from registration at a transplantation center to transplant), depending on where he or she lives. Because much of the current debate has centered on the procurement and allocation of livers, the committee focused its examination on this organ.
In an analysis of approximately 68,000 liver patient records, the committee developed several conclusions and recommendations largely specific to liver transplantation policies. Included among these is the fact that, as previously calculated, the overall "median waiting time" that patients wait for organs-the issue that seems to have brought the committee to the table in the first place-is not a useful statistic for comparing access to or equity of the current system of liver transplantation, especially when aggregated across all categories of liver transplant patients. The committee also found that the current system is reasonably equitable within the category of the most severely ill (status 1) liver patients, since the likelihood of receiving a transplant is similar across organ procurement organizations (OPOs) for these patients. Similarly, pretransplantation mortality rates are also quite similar across OPOs, irrespective of the patient's status level. The committee also found, however, that the system can be improved by enlarging the current organ allocation areas to include larger populations. Doing so will likely increase the number of status 1 and 2 patients receiving liver transplants with a concomitant reduction in the number of transplants performed on status 3 patients, who are at much lower risk of imminent death. Such expansion of the geographic area of allocation would have to be done within the limits of cold ischemia time. Preliminary data on existing regional and statewide sharing seem to agree with this projection, indicating that status 1 transplantation rates will be increased, status 2B pretransplantation mortality will be decreased, and the transplantation of status 3 patients will be reduced as a result of broader sharing by smaller OPOs. In general, the committee finds broader sharing is likely to result in more of the most medically urgent patients receiving first attention when waiting for donated livers.
Since the enactment of the National Organ Transplant Act of 1984, the number of people receiving organs has increased annually. In 1998, more than 21,000 Americans—about 57 people a day—were transplanted with a kidney, liver, heart, lung, or other organ. On any given day, approximately 62,000 people are waiting for an organ and every 16 minutes a new name is added to the national waiting list (UNOS, 1999). These numbers represent only the indicated demand for organs. It is likely that there are many more people in need of transplantation who are not currently on a waiting list. Moreover, although the number of donors has increased steadily since 1988, donation rates are not growing as quickly as the demand for organs (GAO, 1997). As a result, approximately 4,000 Americans die each year (11 people per day) waiting for a solid organ transplant (UNOS, 1999).
The disparity between the supply of and demand for transplantable organs has focused attention on the policies and practices regarding the allocation of the scarce supply of organs. Concerns about need, supply, demand, access, and rationing have raised questions about the appropriate role of the federal government in regulating this important public health issue. The polemical nature of the debate has increased public skepticism about the integrity and fairness of the system. Such skepticism may serve to reduce donations and create more serious shortages (Dejong et al., 1995).
One of the most visible and contentious issues regarding the fairness of the current system of organ procurement and transplantation is the argument that it results in great disparities in the amount of time potential liver transplant patients wait for a transplant, depending on where the patient lives. (The term "waiting time" is used throughout this report to refer to the time from registration at a transplantation center to transplant, death, or removal from the waiting list for other reasons.) An additional concern is that minorities and the poor may have less access to organ transplants than do whites of higher socioeconomic status.
In response to concerns expressed about possible inequities in the existing system of organ procurement and transplantation, the U.S. Department of Health and Human Services (DHHS) published a new regulation in April 1998 (42 CFR Part 121, referred to in this report as the "Final Rule") to "assure that allocation of scarce organs will be based on common medical criteria, not accidents of geography" (DHHS, 1998b).
The Final Rule provides a framework within which the transplant system would operate. The stated principles underlying the Final Rule include the need for oversight in a system that permits variance in individual medical practice and the creation of a "level playing field" in organ allocation-that is, organs are allocated based on patients' medical need and less emphasis is placed on keeping organs in the local area where they are procured. A primary stated objective is to equalize waiting times among different areas of the country. To emphasize this, the Final Rule calls for standardized medical criteria to be used to determine the status of a person's illness and when that person can be placed on a waiting list. In addition, the rule aims to improve data collection and analysis so that patients, their physicians, and the public have timely, accurate, and user-
friendly, center-specific data on the performance of transplant programs to help them to assess quality and make transplant decisions.
Issuance of the Final Rule generated considerable controversy in the transplant community. Concerns were expressed that its implementation would increase the cost of transplantation, force the closure of small transplant centers, adversely affect access to transplantation on the part of minorities and low-income patients, discourage organ donation, and result in fewer lives saved. Some opponents of the rule also argued that DHHS had exceeded its statutory authority by establishing a process for reviewing Organ Procurement and Transplantation Network (OPTN) policies and procedures.
In October 1998, the U.S. Congress suspended implementation of the Final Rule for 1 year to allow further study of its potential impact. During that time, Congress asked the Institute of Medicine (IOM) to conduct a study to review current OPTN policies and the potential impact of the Final Rule on:
-
access to transplantation services for low-income populations and racial and ethnic minority groups, including the impact of state policies (under Title XIX of the Social Security Act) regarding payment for services for patients outside of the states in which the patients reside;
-
organ donation rates, reasons for differences in donation rates, and the impact of broader sharing (i.e., based on medical criteria instead of geography), on donation rates;
-
waiting times for organ transplants, including (a) determinations specific to the various geographic regions of the United States and, if practicable, waiting times for each transplant center by organ and medical status category, and (b) assessment of the impact of recent changes made by the OPTN in patient listing criteria and in measures of medical status;
-
patient survival rates and organ failure rates leading to retransplantation, including variances by income status, ethnicity, gender, race, or blood type; and
-
costs of organ transplantation services.
The legislation that called for this study included two additional areas for review: (1) confidentiality of information about the program, and (2) the possible legal liability of OPTN members arising from their peer review activities. As agreed, the U.S. General Accounting Office (GAO) addressed these two issues in a separate report (GAO, 1999). Also as agreed in response to the legislation, GAO assisted IOM by providing data to the committee regarding costs of organ transplantation services.
CURRENT POLICIES AND PRACTICES
The process of organ procurement and transplantation begins when a patient in need of an organ transplant is referred to one (or more) of the 272 organ transplant programs (125 of which perform liver transplants) currently in opera-
tion in the United States. If accepted for transplantation by a transplant program, the patient is placed on that program's waiting list until a donated organ that is determined to be medically appropriate is available. Patients in need of a liver transplant are assigned to one of several classifications—status 1, status 2A, status 2B, or status 3—depending on the nature and severity of the patient's illness (see Table ES-1).
The retrieval and preservation of donated organs, and their transportation (if necessary) from the site of donation to the site of transplantation, is the responsibility of organ procurement organizations (OPOs). There are 62 OPOs currently in operation in the United States. Each is responsible for the retrieval and allocation of organs within a defined geographical area, and in accordance with organ allocation policies (see Appendix C). These geographical service areas vary greatly in their size and population, as well as in the number of organs retrieved and the number of patients transplanted by the transplant centers in their service areas.
TABLE ES-1 UNOS Liver Status for Patients ![]() 18 Years of Age According to Disease Severity
18 Years of Age According to Disease Severity
|
Status 1 |
Fulminant liver failure with life expectancy < 7 days • Fulminant hepatic failure as traditionally defined • Primary graft nonfunction < 7 days of transplantation • Hepatic artery thrombosis < 7 days of transplantation • Acute decompensated Wilson's disease |
|
Status 2A |
Hospitalized in Intensive Care Unit for chronic liver failure with life expectancy < 7 days, with a Child-Pugh score • Unresponsive active variceal hemorrhage • Hepatorenal syndrome • Refractory ascities or hepatic hydrothorax • Stage 3 or 4 hepatic encephalopathy |
|
Status 2B |
Requiring continuous medical care, with a Child-Pugh score • Unresponsive active variceal hemorrhage • Hepatorenal syndrome • Spontaneous bacterial peritonitis • Refractory ascites or hepatic hydrothorax |
|
Status 3 |
Requiring continuous medical care, with a Child-Pugh score |
|
Status 7 |
Temporarily inactive |
|
SOURCE: Keeffe, 1998; data obtained from UNOS website (http://unos.org) initially implemented July 1997, modified January 1998. |
|
The process of identifying which patient on a waiting list should receive an available organ is facilitated by the OPTN. The OPTN, which was created by Congress as part of the National Organ Transplant Act of 1984, maintains a computerized listing of all patients, and certain vital data on such patients, on waiting lists for organ transplantation. When an OPO determines that an organ is available for transplant, it contacts the OPTN or more specifically, the United Network for Organ Sharing (UNOS), which has been the OPTN contractor since the system was created. UNOS then uses a complex, computerized algorithm to determine which patient is the most appropriate recipient of the available organ.
There is general agreement that status 1 liver patients should be given first priority for an available organ and, if no suitable status 1 patient is identified, the organ should be offered sequentially to status 2A, status 2B, and status 3 patients. At the present time, this set of priorities is exercised first (with some exceptions) within the geographical area served by the OPO that retrieved the organ. The organ is offered to a patient outside the OPO's service area (using a similar set of priorities) only if no suitable transplant recipient is identified within its service area. (See Appendix C for a description of current allocation policy.) Thus, despite the general consensus that status 1 patients should be given priority over other patients, the current allocation policies and practices may result in a status 2B or status 3 patient receiving an available organ because he or she is within the service area of the OPO that retrieved the organ, while a suitable status 1 patient in a different OPO service area continues to wait for an organ. This is the basis for much of the debate about the fairness and effectiveness of the current system and one of the major concerns that the DHHS Final Rule was designed to address.
CONCLUSIONS AND RECOMMENDATIONS
The committee developed conclusions regarding the potential impact of the Final Rule on each area listed in its charge, as well as recommendations as to how the Final Rule should be implemented. Because liver allocation was at the center of the debate leading to this study and there are several unique factors related to liver transplantation (e.g., the lack of medical alternatives to transplantation, such as dialysis for kidney patients), and because of the severe time constraints placed on this project by Congress, the committee focused its attention primarily on issues related to the policies, practices, and data concerning liver procurement and transplantation. Unless specified otherwise, the text, analysis, and conclusions and recommendations presented in this report relate to liver transplantation.
The committee views organ transplantation as a valuable, often lifesaving process that should be managed equitably across the nation. It also believes the federal government has a legitimate and appropriate oversight role to ensure that reasonable standards of equity and quality are met. Therefore, the committee offers conclusions and recommendations on several crosscutting issues that must
be addressed to improve the overall system. These issues include the need for better data collection, analysis, and dissemination; the need for better scientific oversight of the entire transplant enterprise; and the need for more rigorous evaluation of the system's performance. The committee's conclusions and recommendations follow.
The Need for Larger Organ Allocation Areas
The committee concludes that the fairness of the organ procurement and transplantation system, and its effectiveness in meeting its stated goals, would be significantly enhanced if the allocation of scarce donated livers were done over larger populations than is now the case. This led to the following recommendation.
RECOMMENDATION 1: Establish Organ Allocation Areas for Livers
The committee recommends that the DHHS Final Rule be implemented by the establishment of Organ Allocation Areas (OAAs) for livers-each serving a population base of at least 9 million people (unless such an area would exceed the limits of acceptable cold ischemic time). OAAs should generally be established through sharing arrangements among organ procurement organizations to avoid disrupting effective current procurement activities.
To arrive at this conclusion and recommendation, the committee reviewed all the literature and testimony submitted to it and conducted an independent analysis of 68,000 records for patients on liver transplant waiting lists. These data described every change in the waiting list status for every patient on a waiting list from 1995 through the first quarter of 1999. These patients were grouped by OPO as the unit of analysis for assessing allocation policies. A mixed-effects multinomial logistic regression model was used to examine the effects of various factors—including age, race, gender, blood type, waiting time, and size of OPO—on the likelihood of a patient either receiving a transplant or dying while on the waiting list. (See Chapter 5 and Appendix A for a complete description of this analysis.)
The committee's analysis revealed that OPO volume (the number of transplants performed within its service area) and OPO size (the population within its service area) are both statistically significant predictors of transplantation for status 2B and status 3 patients. OPOs with small and medium volumes (defined here as those with less than an average of 75 transplants in their service area per year over the 4 years for which data were available) were significantly more likely to provide organs to status 2B and status 3 patients than OPOs that averaged more than 75 transplants per year. In addition, patients served by small OPOs (those with fewer than 40 transplants in their service area per year) had a significantly increased risk of pretransplant mortality while on the waiting list.
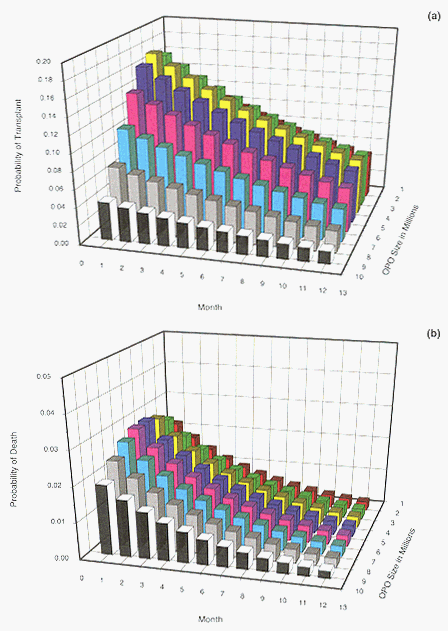
The committee's analysis also provided strong statistical evidence that increasing the size of the population served in liver allocation will result in more opportunities to transplant sicker patients without adversely affecting less sick patients. For status 2B patients, the results of the statistical analysis reveal that both pretransplant mortality and the probability of transplantation falls as OPO size increases up to 9 million people-both desirable outcomes (see Figure ES-1). Results of the statistical analysis also reveal that status 3 patients are less likely to undergo transplantation as OPO size increases up to 9 million with no increase in pretransplant mortality (see Figure ES-2). Thus, the number of status 2B and 3 patients receiving transplants could be reduced to allow more status 1 and 2A patients to receive transplants without an increase in pretransplant mortality for the status 2B and 3 patients. The committee further observed a convergence of these two statistical findings in that all of the OPOs serving 9 million or more people performed a minimum of 75 transplants within their service areas per year. On the basis of this analysis, the committee reached the following conclusion:
Creation of organ allocation areas based on a minimum population of approximately 9 million persons would substantially increase the allocation of organs to patients with more urgent need of a transplant.
The committee recognizes that achieving optimum results in procuring organs for transplantation is highly dependent on good working relationships at the local level among hospitals, OPOs, transplant centers, and others in the community interested in supporting organ transplantation. The OPOs currently in existence have been working diligently for some time to develop and maintain such relationships, and the committee does not want its recommendations to detract from or interfere with present operations where they are working effectively. The committee, therefore, is explicitly not recommending that these larger allocation areas be created by consolidating existing OPOs into fewer, larger organizations. Rather, it is recommending that allocation over larger populations be achieved through changes in policies and procedures and through sharing arrangements among OPOs.
Appropriate Consideration of Patient Waiting Times
Disparities in overall median waiting times for liver transplants have been cited as an indicator of the unfairness of the current system. However, for the reasons set forth below, the committee concluded that this is not an appropriate measure of the fairness of the system. Moreover, the committee also concluded that waiting time was not an appropriate consideration in determining priorities in the allocation of livers within certain classifications of less severely ill patients. This led to the following recommendation.
RECOMMENDATION 2: Discontinue Use of Waiting Time as an Allocation Criterion for Patients in Statuses 2B and 3
The heterogeneity and wide range of severity of illness in statuses 2B and 3 make waiting time relatively misleading within these categories. For this reason, waiting time should be discontinued as an allocation criterion for status 2B and 3 patients. An appropriate medical triage system should be developed to ensure equitable allocation of organs to patients in these categories. Such a system may, for example, be based on a point system arising out of medical characteristics and disease prognoses rather than waiting times.
Because status 3 patients greatly outnumber those in other status groups, the overall median waiting time—for either an OPO or a transplant center—is primarily determined by the waiting times for these patients. However, these are the patients with the least urgent need of transplantation, as well as the patients, on average, with the longest periods of time on the waiting list. These facts led the committee to the following conclusion:
Overall median waiting time, which has dominated the policy debate, is a poor measure of differences in access to transplantation. Status-specific rates of pretransplantation mortality and transplantation are more meaningful indicators of equitable access.
The committee examined the 68,000 patient records described above to compare the waiting times and mortality rates across OPOs, for each of the patient status groups. Waiting times were typically only about 3-4 days for status 1 patients, 40-70 days for status 2 patients, and 100-400 days for status 3 patients. Moreover, there was far less variability in waiting times across OPO areas for status 1 patients than for status 2B and status 3 patients. Similarly, pretransplant mortality did not vary substantially across OPO areas for all three status levels. From this, the committee reached the following conclusion:
The current system appears to generate reasonably little variation in waiting times across OPOs for status 1 and 2A patients, indicating that waiting time is an appropriate criterion for organ allocation, along with necessary medical criteria, within these categories. Greater amounts of variation occur for status 2B and 3 patients across OPOs.
Further analysis of the waiting list data revealed that status 2B and status 3 patients have a decreased likelihood of either transplantation or death the longer they are on the list. This suggests that many of these patients, despite meeting the criteria for being placed on a waiting list, have little likelihood of receiving a transplant and little risk of dying. It may be that some patients are put on waiting lists at an early stage in their disease condition to accumulate waiting time and move up the priority list. If so, this is contributing to the appearance of an ineq-
uitable allocation system. Eliminating the use of waiting time in status 2B and status 3 patients as a component of the priority score would reduce the incentive to list patients who are in less urgent need of a transplant and would enhance the chances that patients more in need of a transplant would receive one.
Among the status 2B and status 3 patients, there appears to be a subgroup of patients who are more likely to require a transplant within a shorter period of time than the remainder of patients in that status. The remaining patients in that status will live a relatively long time with chronic liver disease, not become medically urgent, and not receive a transplant. Thus, the length of waiting time in status 2B and status 3 is not a good indicator of medical urgency or priority.
Access to Organ Transplantation
The committee was charged to determine what, if any, impact the Final Rule would have on the access of low-income and minority populations to transplantation services. The available studies addressing this issue are limited in number and scope, making this a challenging assignment. Moreover, the data the committee received from the OPTN contained information on race, but not socioeconomic status or insurance coverage; our conclusion regarding low-income patients (below) is based on the limited available studies. Thus, the committee cautions that its findings (which follow) must be considered provisional rather than conclusive.
African American patients are less likely than white patients to be referred for evaluation and are placed on waiting lists at a slower rate, as are low-income patients of all racial and ethnic groups.
African American kidney patients on waiting lists are transplanted at a lower rate than white patients, but similar disparities have not been shown for liver patients.
The evidence is inconclusive that the Final Rule would result in the closure of smaller transplant centers located in areas that are more accessible to the residences of prospective transplant patients. Moreover, even if this were a result of the Final Rule, there is no evidence demonstrating that this would have an adverse impact on the access of minority and low-income patients to organ transplants.
The most important predictors of equity in access to transplant services lie outside the transplantation system-that is, access to health insurance and high-quality health care services.
Organ Donation
The committee was asked to assess whether implementation of the Final Rule, particularly efforts to achieve broader sharing, would affect organ donation rates. The committee found that many elements affect donation rates, most of which have little to do with local allocation policies. Thus, local preference seems not to be a significant factor in the decision to donate. The committee found little or no evidence to support the assertion that people would decline to donate, or that health professionals engaged in organ procurement would be less diligent in their efforts, if they knew a donated organ would be used outside the donor's immediate geographic area.
The committee heard testimony that the presence of a transplant center in a community enhances the community's awareness about organ transplantation and increases organ donation in that community. However, the fact that local transplant centers are important in stimulating organ donation does not lead to the conclusion that local use of donated organs is an important consideration of donors. Further, the committee notes that areas participating in broader sharing arrangements have experienced increased donation rates. It may be that the perception of fairness and effectiveness in distribution is as important as other factors in affecting donation rates beneficially.
The committee believes strongly that the effectiveness and productivity of organ procurement is highly dependent on good working relationships at the local level. However, it finds no evidence that broader organ sharing arrangements will lead to reduced rates of donation.
Organ Failure and Patient Survival
The committee was asked to determine the potential impact of the Final Rule on patient survival rates and organ failure rates leading to retransplantation. A number of biological factors influence short-term outcome as well as long-term function of transplanted organs. Not all organs are the same; for example, some organs are more sensitive to ischemic time than others, but ischemic times have not been rigorously evaluated in the past. The committee undertook a comprehensive assessment of the existing literature and made judgments based on this information that are in general agreement with current practices (see Table ES-2).
The committee's analysis of data on posttransplant mortality of recent liver transplant patients revealed that patients receiving transplants at centers served by lower-volume OPOs had higher mortality rates relative to larger-volume OPOs. In addition, the 1999 UNOS report on graft and patient survival rates showed that low-volume transplant centers had lower than expected 1-year graft survival rates. Although these findings may suggest a positive correlation between transplant volume and patient survival, the committee did not believe it had enough data to reach a conclusion regarding the impact of the Final Rule on survival.
TABLE ES-2 Summary of Literature on Cold Ischemic Time for Solid Organs
|
Organ |
Medically Acceptable Cold Ischemic Time* (simple cold storage using appropriate preservation fluids) (hrs) |
|
Liver |
12 |
|
Pancreas |
17 |
|
Kidney |
24 |
|
Heart |
4 |
|
Lung |
6-8 |
|
* The committee defines medically acceptable cold ischemic time as the duration of cold ischemia that has been associated in clinical experience with an appropriate and acceptable percentage of acute and long-term graft function and survival. The times presented in this table are based on the committee's review of peer reviewed literature. Longer times are sometimes reported in clinical practice with acceptable outcomes. Outcomes vary as a function of many other factors, including age of donor and quality of organ. |
|
Costs
The committee examined whether implementation of the Final Rule would increase transplantation costs because of the combined effects of sharing donated organs over a greater geographic area and using donated organs in patients who are more severely ill. Based on information obtained by the GAO about organ recovery practices from officials at six OPOs, the committee learned that costs vary considerably among transplant centers and OPOs. The cost of transporting an organ, for example, depends on the mode of transportation used (ground or air), the distance that the organ must travel, and whether the transplant team travels to the site of donation to retrieve the organ. The committee concluded that organ procurement costs would likely increase, but was not able to estimate by how much.
The committee also concluded that status 1 patients incur higher costs than status 2B or 3 patients, and this, too, would increase the cost of implementing the Final Rule. Again, the committee was unable to estimate the amount of the increase.
Expenditures for organ procurement and transplantation are likely to increase as a result of broader sharing. The committee is not, however, able to estimate with confidence how large the increase might be because it is not clear how the Final Rule will be implemented and how many patients in each status will be affected. Any increase in expenditures must, however, be weighed against the additional health benefits
of broader sharing, which the committee believes will be substantial and could outweigh any net increase in expenditures.
Oversight and Review
During its deliberations, the committee came to the conclusion that the system of organ procurement and transplantation is not functioning as well as it could because responsibility is dispersed among many different participants without an effective means of holding them accountable to the patients that the system is designed to serve. The committee believes that the purposes of the National Organ Transplant Act would be better served if there were enhanced oversight and governance of the system, aided by improved efforts at assessing the performance of all key components. In addition, the committee concluded that, although a considerable volume of data is collected, some important data elements are missing, there is often a lengthy time lag in the data that are available, and these data are not readily accessible to patients, the health services research community, or the general public. These concerns led the committee to a series of important, related recommendations.
RECOMMENDATION 3: Exercise Federal Oversight
The Department of Health and Human Services should exercise the legitimate oversight responsibilities assigned to it by the National Organ Transplant Act, and articulated in the Final Rule, to manage the system of organ procurement and transplantation in the public interest. This oversight should include greater use of patient-centered, outcome-oriented performance measures for OPOs, transplant centers, and the OPTN.
RECOMMENDATION 4: Establish Independent Scientific Review
The Department of Health and Human Services should establish an external, independent, multidisciplinary scientific review board responsible for assisting the Secretary in ensuring that the system of organ procurement and transplantation is grounded on the best available medical science and is as effective and as equitable as possible.
RECOMMENDATION 5: Improve Data Collection and Dissemination
Within the bounds of donor and recipient confidentiality and sound medical judgment, the OPTN contractor should improve its collection of standardized and useful data regarding the system of organ procurement and transplantation and make it widely available to independent investigators and scientific reviewers in a timely manner. The Department of Health and Human Services
should provide an independent, objective assessment of the quality and effectiveness of the data that are collected and how they are analyzed and disseminated by the OPTN.
The committee believes these measures will greatly enhance public confidence that the system is fulfilling its primary mission—serving the needs of transplant patients. The establishment of the scientific review board would make a particularly important contribution toward ensuring that there is a consistent and coherent view as to how the system should operate, that the policies and practices are based on the best scientific and medical knowledge currently available, and that the interests of transplant patients are given paramount importance.