1
Introduction
LEGISLATIVE AND EXECUTIVE BRANCH HISTORY
House Report 105-610 outlined the basis for the Institute of Medicine (IOM) study of the VA National Formulary noting that:
Serious concerns have been raised about the impact of the VA's new National Formulary. The Committee has learned that the formulary prevents physicians from meeting the unique health care needs of individual veterans and is overly restrictive. To address these concerns, the Committee directs the VA to contract with the Institute of Medicine to conduct an independent analysis of the effects of the National Formulary on the quality of care.
Specifically, the study should be completed within 6 months and should provide the Committee with an estimate of potential costs to VA health care associated with the National Formulary for drugs, biologic products, devices, prosthetics and pharmaceutical treatment guidelines. The study should also include a comparison of the new VA formulary to private insurance formularies for drugs and devices and other government formularies, such as Medicaid.1
These four concerns—restrictiveness of the formulary, effect on quality of care, effect on costs, and comparison to other public and private-sector formularies —were expressed in the report that accompanied legislation from the House Committee on Appropriations that provided funding for the Departments of Veterans Affairs and Housing and Urban Development for Fiscal Year (FY) 1999 (Public Law 105-276, approved 10/21/98). House Report 105-610 also directed the Secretary of Veterans Affairs to report separately on the nonformulary waiver process operated by each Veterans Integrated Service Network (VISN, 1 of 22
|
1 |
House Report 105-610. |
regional VA health care systems comprising the national Veterans Health Administration [VHA]). The Secretary's response, submitted to Congress in February 1999, was based on a December 1998 survey of all 22 VISNs. It described basic features and statistics of the nonformulary waiver process.
The language of House Report 105-610 and of a Senate request to the U.S. General Accounting Office (GAO) (see below) was developed between January and June 1998. In preparation for the FY 1999 appropriations legislation, the House Appropriations Committee and both House and Senate Committees on Veterans Affairs, in hearings and in questions to the Department of Veterans Affairs (VA), identified a number of concerns regarding the National Formulary and the availability of pharmaceuticals to veterans. These dealt with issues such as the selection of drugs for the formulary, access of veterans to needed drugs, the effects of the formulary policy on quality of care to veterans, on costs to the VA health system, and on comparisons with other private or public-sector formulary systems. The VHA submitted detailed responses to the congressional committees' questions. These responses became part of the available record on the VA pharmacy benefit. The charge to the IOM committee on the VA pharmacy formulary analysis reflected the concerns expressed in this record and the House report.
On October 16, 1998, Senator Rockefeller, ranking minority member of the Senate Committee on Veterans Affairs, wrote to the acting Comptroller General formally requesting an examination of the VA National Formulary by the U. S. General Accounting Office. Noting that the language of House Report 105-610 had not been included in the House-Senate conference report, Senator Rockefeller asked the GAO, in addition to the IOM study, to compare the VA National Formulary to formularies of health maintenance organizations and Medicaid, to assess the fairness of the drug selection process and the timeliness and convenience of the nonformulary process, and to investigate whether the VA Medical Advisory Panel (MAP), the VISN formulary committees, and the VA Pharmacy Benefits Management Strategic Healthcare Group (VA PBM) were working together to the best advantage of veterans health care. The GAO initiated this study, structured as a program audit of the VA National Formulary system, in early 1999 and issued its first report on the audit late that year. Completion of the audit is anticipated shortly after release of this IOM report and should provide useful additional information about formulary systems in the VHA (see “VA's Management of Drugs on Its National Formulary,” GAO, 1999).
History of the IOM Study
After unsuccessful efforts by VA pharmacy leaders in the fall of 1998 to persuade the House and Senate and VA leadership to consolidate the GAO and IOM assignments into one study (MAP/VISN minutes, Jan. 13, 1999), a draft statement of work for the IOM study was prepared by the VA. In meetings in January 1999 between VA PBM staff and GAO and IOM, the problems of the 6-month timetable for the IOM study and the similarity of the two projects were
discussed. Consultation with Congress ultimately resulted in the structuring of the GAO study as a program audit of the National Formulary system, as noted above, and in an extension of the timetable and definition of the IOM study as described below (VA PBM/MAP minutes, Feb. 3, 1999).
A January 26, 1999 VA task order to the IOM outlined a report addressing the four essential questions, that is, restrictiveness, effects on quality of care and costs, and comparison to other formulary systems. The task order stated that VA pharmaceutical costs were experiencing double-digit inflation, that the VHA budget was “straight lined through the fiscal year 2002,” and that management of the pharmacy benefit in terms of cost, adverse drug reactions, and clinical outcomes was key to continuing to treat the same or more veterans within the planned budget. (Ultimately, the VHA appropriation was increased for FY 2000). The task order also stipulated that an analysis of the VA system was to consider the nonformulary process a part of pharmacy benefits. The VA formulary system was understood to mean the National Formulary, VISN formularies, VA medical center formularies, and the nonformulary process as well as drug treatment guidelines. The IOM was to work with and have unimpeded access to VA PBM members to obtain relevant data and information in a timely manner. The 6-month timetable was deleted.
The final IOM-VA contract, effective April 12, 1999, included deliverables responding to the following questions and designed to implement the original language of congressional concerns from House Report 105-610 2 :
-
“Is the National Formulary overly restrictive and does it prevent physicians from meeting the unique health care needs of veterans?
-
What are the potential costs to VA health care associated with the National Formulary for drugs, biological products, devices, prosthetics, and with pharmaceutical treatment guidelines?
-
What are the effects of the National Formulary and related policies on quality of care?
-
How does the VA National Formulary compare with private insurance formularies for drugs and devices and with other government formularies (e.g., Medicaid)?”
A prepublication report was scheduled for release in the 13th month of the project and a final National Research Council (NRC)–IOM peer-reviewed report by the 15 month. The report was to be book length, address the four defined questions, and include the IOM committee conclusions and recommendations. In a subsequent action, Congress specified July 11, 2000, as the delivery date for this final report (House Report 106-379, Conference Report to accompany H.R. 2684, a bill which became P.L. 106-74, the appropriation for the VA
|
2 |
This contract reflects the agreement between the VA and the IOM, resulting in minor differences between its language and the House report language quoted on the first page of this introduction. |
[and other agencies]). An interim report at month 6, was to address the issue of how the VA National Formulary compares with private insurance and government formularies. The format of the interim report was left to the IOM committee. The committee decided it should be a short document, which would not require NRC–IOM peer review, accompanied by a detailed briefing. The interim report and briefings were delivered on January 28, 2000, by the IOM committee chairman, Dr. David Blumenthal, to the VA, the Senate and House Committees on Veterans Affairs, and Congressman Frelinghuysen of the House Committee on Appropriations. The interim report is reproduced in Appendix A of this final report.
The IOM Committee
As specified in the IOM plan of action, a committee of 14 members was assembled to carry out the IOM-VA contract. Because of the subject matter of the study, the organization of the VHA, and the demographics of the veteran population, certain disciplinary backgrounds and areas of experience and expertise were sought. Two members with extensive knowledge of, and experience with, the veteran population were selected. They worked for the Disabled American Veterans (DAV) and the Paralyzed Veterans of America (PVA), two veterans service organizations (VSOs) that are particularly suitable because they represent significant numbers of veterans, especially those with service-connected disabilities who are intensive users of, and dependent on, the VHA.
Veterans who use the veterans health care system are disproportionately minorities and more likely to be old, sick, and disadvantaged. The VHA is emphasizing primary and ambulatory care (Fonseca et al., 1996; Hisnanick and Gujral, 1996; Kazis et al., 1998; Kizer, 1999; Wilson and Kizer, 1997). For these reasons, committee members with expertise in clinical medicine and nursing who had backgrounds in geriatrics and general medicine and experience in caring for minority populations were appointed. Among these members were directors of major academic units or departments of clinical epidemiology, clinical pharmacology, general medicine, nursing research, and health care policy. Some of these experts were also leaders of their institutional or managed care organization pharmacy and therapeutics (P&T) committees.
Some members of the IOM committee were selected because of experience working in managed care organizations (MCOs) with formularies and pharmacy benefit plans. Their experience was especially relevant to understanding VISNs, which are essentially regional veterans MCOs, and to comparing the National Formulary with private-sector formularies. Committee members from national pharmacy benefits management (PBMs) organizations were appointed for similar reasons. With the help of these individuals, the IOM identified elements of restrictiveness for a national survey carried out in early 2000 by the Academy of Managed Care Pharmacy.
Several members of the committee were senior members of the U.S. academic or commercial pharmacy community with wide experience in P&T com-
mittees and the profession of pharmacy, at both the practicing and the leadership levels. The IOM committee also included a member with national Medicaid drug benefit and drag utilization review (DUR) experience and current experience with private-sector DUR and drug standards at the U.S. Pharmacopoeia, as well as a senior health economist and professor of health policy and management.
The IOM contractual agreement with the VA authorized a subcontract to assist the committee in assessing the effect of the VA formulary system on costs, one of the major deliverables of the project. The IOM determined that the Department of Health Care Policy of Harvard Medical School had the necessary expertise and experience to carry out this work. Two health economist members of the department, with support from other departmental staff, became official consultants to the IOM and submitted an analysis of the National Formulary's impact on health care costs. The agreement also provided support for a paper on formularies used by MCOs and Medicaid to assist the committee in comparing the VA National Formulary with formularies in these other systems, another major deliverable of this project. The IOM decided that this task should be carried out by an experienced Ph.D. graduate student from Brandeis University studying in this area. He also became an official consultant to the IOM.
The IOM committee met three times to review information, identify and discuss issues, and review drafts of the interim and final reports. These meetings consumed a day and a half each time—September 30 and October 1, 1999, December 13 and 14, 1999, and March 8 and 9, 2000. At the first meeting, the committee was briefed on the National Formulary system by the VA PBM staff and representatives of the VHA MAP and by GAO staff responsible for its program audit of the VA National Formulary. A member of the IOM committee and IOM staff attended an August 1999 meeting of the VA MAP and PBM in Chicago and reported back to the committee. The committee also spent additional days reading the medical and pharmacy literature; assimilating data from the consultants, the VHA, the VA National Formulary, and other systems; and preparing this report. The committee enjoyed good cooperation and responsiveness in the provision of data from the VA PBM, both from the central office in Washington, D.C., and from the operational VA PBM headquarters located outside Chicago. Members of the MAP and other individual staff from VA facilities around the United States also contributed much useful information. Where data that could have allowed better analysis, or firmer, more extensive conclusions were not available or were incomplete, this is noted in the relevant chapters of this report.
FORMULARIES AND FORMULARY SYSTEMS: HISTORY AND DEFINITIONS
Traditionally, formularies were lists of remedies and their formulas (Weintraub, 1978), that is, books containing medicinal substances with specific formulas for converting raw materials into finished dosage forms, especially for individual consumption (Rucker, 1988). A Sumerian tablet discovered in Nippur, dating to about 3000 B.C., is the oldest known example of a formulary (Sonne-
decker, 1972). European examples date from Florence in 1498. Many early formularies were called pharmacopoeias (literally, a book to make remedies). The term had not yet taken on its present meaning of a compendium of drug standards for purity and strength. The first formularies in the United States were issued in the eighteenth century. These included the Lititz Pharmacopoeia (1778) used by the American continental army's military hospitals and Coste's Compendium Pharmaceuticum (1780) used by the French forces supporting the American Revolution. These were followed by the Pharmacopoeia of the Massachusetts Medical Society (1808), Seamans Pharmacopoeia Chirurgica for the New York Hospital (1811), listing 145 agents; the Pharmacopoeia of the New York Hospital (1816), which for the first time attempted to incorporate the opinions of the medical staff and listed 430 items; and the Pharmacopoeia of the United States (USP) (1820), listing 217 drugs, primarily from the Massachusetts formulary. In the ensuing years, hospitals and localities continued to issue formularies or phamacopoeias—for example, Bellevue Hospital (1868), the cities of New York and Brooklyn, the State of Kentucky, the Commonwealth of Pennsylvania (the late 1800s), German Hospital (1902), Syracuse University Hospital (1925), and the USP convention about every 10 years after 1820. The Syracuse University Hospital formulary was notable in that it involved a formulary system in which 45 physicians and 1 pharmacist established a scientific basis for drug control and elimination of duplication in a drug therapy program (Dillon, 1999).
From the seventeenth through the nineteenth centuries, crude preparations (e.g., decoctions, extracts, and infusions) of natural substances, called galenicals, were removed from formularies. Beginning in the late nineteenth century, purification and standardization of the potency of active ingredients began to be represented in formularies as a result of improved chemical manufacturing and the introduction of pharmacology as a medical school discipline in the 1890s. The Formulary and Therapeutic Guide of the New York Hospital (1933) included selection and regulation of drugs for a facility and preferential generic nomenclature. Secret remedies, drugs differing only in name, and exaggerated claims were eliminated, and the formulary was used as a tool for improving the economics of drug prescribing and use in the hospital, as reported by Hatcher and Stainsby (1933). At about that time, the American College of Surgeons (1936) adopted and issued the first “Minimum Standard for Pharmacies in Hospitals ” by Western Reserve pharmacists Spease and Porter. The American Society of Hospital (now Health-System) Pharmacists (ASHP), the American Pharmaceutical Association (APhA), the American Medical Association (AMA), the American Hospital Association (AHA), and others issued standards and policy statements beginning in 1959. In that year, the ASHP also published the American Hospital Formulary Service, a loose-leaf binder containing clinical, technical, and dosing information to serve as a reference on all drugs for pharmacists and other heath care professionals. Other standards and policy statements have followed at intervals (see American College of Physicians [ACP], 1990; AHA, 1974, 1975, 1999; AMA, 1994; ASHP, 1981, 1983, 1988; ASHP et al., 1964; Francke, 1967; Hoffman, 1984; King, 1987; Sonnedecker, 1972, 1976; Wein-
traub, 1978). These statements supported formularies in principle, but also staked out the prerogatives and responsibilities of the several issuing professional organizations.
Advances in the science of medicine and pharmacology allowed improvements in the quality of formularies (Rucker, 1982, 1986; Rucker and Visconti, 1978). Coincident with this evolution, the Veterans Administration implemented formularies in its hospitals and considered systemwide standardization of some pharmaceuticals by the 1950s (VA M-2, Professional Service, 1955). In the 1950s, the Joint Commission on Accreditation of Hospitals (then JCAH; as of 1987, Joint Commission on Accreditation of Healthcare Organizations [JCAHO]) encouraged hospitals to form P&T committees and establish formularies (Goldberg, 1997). The JCAH and the Medicare program made guidance of drug use by P&T committees a requirement for U.S. hospitals in 1965 and 1966. In 1986, Medicare Conditions of Participation explicitly required formularies for hospitals wishing to participate in Medicare (and Medicaid) (Liang et al., 1987). By the 1970s, 60% of large, mostly academic hospitals (Rucker and Visconti, 1978), and 82% of Medicare-approved community hospitals (Rolands and Williams, 1975) had formularies. Continued surveys documented this growing use over the next several decades (Rascati, 1992; 96.2% of 130 community hospitals).
In the 1970s also, formularies began to be applied beyond the confines of the inpatient hospital sector in significant numbers. Initially, these formularies in staff or group model HMOs were similar to hospital formularies in control and standardization of drugs. They reflected staff and P&T committee views on drug use. Many states operated formularies of several different types in managing their Medicaid programs, with varying success (Meyer et al., 1974; National Pharmaceutical Council [NPC], 1973). Particularly after the stimulus of the federal HMO Act of 1973 (42 USC, 300 et seq.), which supported HMOs, new forms of MCOs such as independent practice association (IPAs) and network models, were developed, and many of these, including some very large managed care health systems, began to use formularies to control their inpatient and outpatient pharmacy benefits (Dillon, 1999). This trend continued during the 1980s and 1990s. Use of formularies by HMOs to help manage drug benefits grew from 39% in 1989 to 67% in 1992, to 80.6% in 1994, and to 92.9% in 1997.
These trends led to considerable state (Herstek, 1999; and see Chapter 5 of this IOM report) and federal (Omnibus Budget Reconciliation Act [OBRA], 1990, 1993) legislative activity to require public disclosure and limit formulary restrictions among other things. Over the same period, a number of foreign countries, including Germany, Canada, and Australia, established national or regional formularies—some limiting the numbers of drugs, others enforcing the formulary with differing levels of strictness. This brief history traces the steps in the development of formularies from their original status as lists of formulas for medications to their much more complex current forms and purposes. Facility,
TABLE 1.1 Potential Advantages and Disadvantages of a Formulary System
|
Advantages |
Disadvantages |
|
|
health system, local, or national formularies are not new inventions. They have an extensive history in the United States and elsewhere.
Modern Formularies and Formulary Systems
A modern formulary is a continually revised compilation of pharmaceuticals that meet pharmacopoeial standards. The IOM committee decided to start with this simple definition of a formulary and then, in defining and describing a formulary system, to identify the elements that a system might employ in managing a formulary to achieve policy objectives. As a practical matter, most modern hospital settings use formularies and formulary systems. Historically, formularies have served ancient societies, city states, and other political jurisdictions, the American revolutionary army, and professional groups, among others. Today, formularies and formulary systems affect most of the 76.6 million Americans enrolled in HMOs and the more than 230 million covered by PBMs and other drug management systems (Cook et al., 2000; Novartis, 1998, 1999). They should be considered, then, as operational components of organized health care delivery systems. As care is increasingly managed and more attention is paid to quality and cost, formularies and evolving formulary systems have played important roles in the pharmacy benefits of delivery systems, whether they are hospitals, clinics, HMOs, PBMs, or others (ASHP, 1988). The committee recognizes both the benefits and the risks of implementation of a formulary and formulary system (see Table 1.1). Any formulary requires careful implementation to maximize the benefits while minimizing the risks.
A formulary system is a method whereby the medical management or administration of an organization, working through a P&T committee or an equivalent group (or groups) of physician and pharmacy experts, objectively evaluates, appraises, and selects from among numerous available drug entities and drug products, those that are considered most useful in patient care. The
pharmaceutical products, listed with nonproprietary and proprietary names, are those that are preferred for use or, in some cases (for example, in health plans), for coverage or reimbursement (AHA, 1974; Nash et al., 1993). Involved, knowledgeable physicians make clinical decisions and, together with system managers, may provide information on procedures, safety, and efficacy and systematic drug evaluations based on contemporary treatment guidelines and pharmacoeconomic principles. These are the critical elements of a formulary system that define its function as a standard of care for drug therapy. Simply stated, the P&T committee should select items for the formulary based on an objective evaluation of their relative therapeutic merits, safety, and cost, minimizing duplication of the same basic drug type, drug entity, or drug product (ASHP, 1992).
Economic Focus of Formularies
Prescription drug costs outpaced the growth in overall health care costs in the 1990s (Levit et al., 1999). Although estimates may vary, they all show an increase in trends for drug costs. According to data provided by the Health Care Financing Administration (HCFA), drug expenditures increased by 9% in 1994– 1995, while total health care costs increased only 5.3%. In 1997, total health care costs increased 4.8%, but prescription drug costs rose 14% (Iglehart, 1999). Total prescription drug retail sales for 1999 are estimated at $121.6 billion for 2.97 billion prescriptions, 18% higher than in 1998 ( www.nacds.org/news/ releases/nr_082999_projections.html). As noted elsewhere, VHA drug expenditures have experienced double-digit annual increases in recent years. Disproportionate increases in drug expenditures reflect increases in drug utilization and higher prices of newer drugs. Reacting to these trends, more and more formulary systems are performing economic analyses (Glennie, 1993; Mannebach et al., 1999; Roberts and Summerfield, 1986; Segal and Pathak, 1988). Compared with more traditional formulary systems, recent systems emphasize the economic efficiency of different drugs and include disease management as well as drug selection strategies. These revised formulary systems typically include integrated drug utilization review, nonformulary exceptions procedures, and the use of treatment guidelines to assist in containing costs.
Types of Formularies and Their Restrictiveness
As noted above, almost all organized health care settings or systems use formularies to serve various objectives,—quality drug treatment, cost control, drug price negotiation, among others. Formularies differ, therefore, but fundamentally they are lists of drugs that may be “open,”—that is, they contain many drugs and drug products, and those that are not listed are generally available and reimbursed,—or “closed” (in whole or in part),—that is, they contain fewer drugs and drug products, and those that are not listed are generally not available nor reimbursed. Management of access to, and reimbursement of, drugs is more
pervasive in closed formularies. Elements of restrictiveness, controls, or other modifications comprise the formulary system that is employed in the management of access and reimbursement to achieve the objectives for the pharmacy benefit of a health care system. These elements can include, for example, genetic substitution, therapeutic interchange, tiered copayments, and preferred or excluded drugs, among others. Some pharmacy benefit controls, such as limits on number, value, or frequency of prescriptions, are also elements of restrictiveness used in parallel to a formulary and are considered relevant to the question of restrictiveness raised by the Congress and the VA. In the remainder of this section, the committee expands this basic description and provides further details on formularies, formulary systems, and relevant controls.
Open formularies may include a great variety of drugs and drug products, and not place limits on, or require clinical justification of, drugs that are approved, prescribed, or stocked. They generally do not require generic substitution or therapeutic interchange.3 Coverage, approval, and reimbursement of drugs and drug products are explicit for entities listed and generally assumed for those not listed. In some cases, an open formulary is termed “intermediate ” or “mixed” if it allows or encourages generic substitution. In other cases, some drugs or drug products listed in the formulary are promoted as “preferred” to prescribers (sometimes called an “incentivized” or “managed” formulary when preferred products are promoted by economic rewards for the payer). In some circumstances, certain drugs are available only after a trial of another drug, a step protocol (Goldberg, 1997; Kreling et al., 1996; Nash et al., 1993).
Current formularies are often closed; that is, the drugs and drug products listed are limited, and entities that are not listed are not covered, approved for use, or reimbursable except through a prior authorization, nonformulary exceptions, or waiver process. Drugs require clinical justification for inclusion in such a formulary, and generic substitution and therapeutic interchange of formulary for nonformulary drugs are encouraged or required. The smaller number of drugs and drug products in such formularies (generally from 300 to 1,000 drug dosage forms [Goldberg, 1997]) means limitations on the number of drugs in therapeutic classes. If a formulary is partially closed, it is restricted in one or more ways for some drugs and drug products and open for others.
Closed or partially closed formulary systems employ a variety of management features. Only a few representatives from one or more therapeutic classes
|
3 |
Generic substitution is the exchange of drug products that have the same, chemically identical, active ingredient(s) and are identical in strength, concentration, dosage form, and route of administration to the drug prescribed. Therapeutic interchange is the authorized exchange of various therapeutic alternates by pharmacists under arrangements between pharmacists and authorized prescribers who have previously established written guidelines or protocols within a formulary system. Therapeutic alternates are drug products of different chemical structures that are of the same pharmacologic or therapeutic class and can be expected to have similar therapeutic effects and safety profiles. See later sections of this chapter for details. |
may be selected, and the remainder of the class members excluded. One or more entire therapeutic classes may be eliminated in rare instances. Some classes may be allowed only with prior authorization or use of a step protocol (occasionally also referred to as a “managed ” formulary). Drugs may be accepted on a restricted and temporary basis to allow their evaluation. Only one brand of dual licensed products may be approved for use. Potentially toxic or expensive drugs or drugs for specific indications may be restricted to prescribers with special experience or expertise, to particular settings (specialty services or inpatient care), or to use in relevant diagnoses or stages of disease for which the drug is approved and clinically indicated. These latter evidence-based restrictions can improve patient care and educate prescribers. Evidence-based restrictions can also promote cost-effective use of certain drugs in some classes, when clinically appropriate. Limits may be set on the number of prescriptions, quantity of drug, or day's supply per prescription, or caps may be enforced on dollar value, quantities, and the like. These latter restrictions are often considered benefit controls.
Generic substitution and therapeutic interchange are tools used within a formulary system to gain enhanced compliance with formulary or preferred formulary products. A nonformulary process of some type is also considered essential to allow products that are not on the formulary to be dispensed and reimbursed. Formularies may be either positive—drugs and drug products are explicitly listed for coverage or approved for use or reimbursement—or negative—drugs are specifically identified for exclusion, which is often the case in Medicaid (Goldberg, 1997; Lyles et al., 1997; NPC, 1998; Rucker, 1999; Shepard and Salzman, 1994). Drugs or drug classes that are specifically designated as excluded in a formulary (for example, cosmetic, life-style, or contraceptive drugs) are not covered or dispensed through that formulary—that is, not only are they nonformulary, but they are not available through any drug exceptions process. They must be purchased at retail, out-of-pocket expense by the patient.
Formulary Control
Pharmacy and therapeutics committees are responsible for formularies and formulary systems in most organized delivery systems. P&T committees began in the 1930s, reportedly at Western Reserve University (Weintraub, 1978). Their role in evaluating drugs for inclusion in hospital formularies was described in 1959 by the AHA and ASHP (Summers and Szeinbach, 1993). They took on important regulatory and legal status in 1965 when they were required by the JCAH for hospital accreditation. Thereafter, the Medicare program ruled that only those inpatient drugs in official compendiums or approved by a P&T committee would be reimbursed (Weintraub, 1978). Medical, hospital, and pharmacy professional groups and organizations have described policies for the structure and function of P&T committees (ASHP, 1992).
A P&T committee is recognized as an advisory committee to the medical staff that represents the official line of communications and liaison between the medical staff and the pharmacy department. It is typically composed of an or
ganization's physicians, pharmacists (who tend to be the most influential on drug matters [Ascione et al., 1998]), and additional members of the health professions such as nurses, administrators, quality assurance coordinators, and others as appropriate. A physician usually is the chair of the committee. A pharmacist acts as secretary (ASHP et al., 1992). Among other things, the P&T committee must evaluate the medical usefulness and cost of pharmaceuticals and recommend for the formulary those which are most useful and cost-effective in patient care (AMA, 1997; ASHP, 1964). The committee may develop policies and procedures on therapeutics and pharmacy services. It may also play an educational role within its organization. Some organizations appoint outside physicians to their P&T committees, although concerns about the independence of these professionals have been expressed. Formularies developed with little input from practicing professionals may not be effective. Acceptance, and therefore effectiveness, of formulary systems may be jeopardized if P&T committees are perceived not to represent an organization's staff of prescribing physicians (AMA, 1997; Carroll, 1999).
In the academic hospital sector, P&T committees preside over formularies that usually are closed and practice generic substitution (Mannebach et al., 1999). Therapeutic interchange with the prior consent of the authorized prescriber is common also (55%) (Ascione et al., 1998; Nash et al., 1993). The same is true in the managed care sector. Of the plans surveyed in 1997, almost all (92.9%) used formularies: 38.1% were closed, 34.1% were partially closed, 63% required generic substitution, and 35.2 –56.5% allowed therapeutic interchange (Gold et al., 1989; Hoechst Marion Roussel, 1998; Kreling and Mucha, 1990; Novartis, 1998). The 1998 figures from Novartis (1999) were 26.9% closed and 45.4% partially closed, figures that vary by the year and by the cohort of MCOs surveyed. These P&T committees are important in evaluating and promoting drug efficacy and cost-effectiveness, monitoring safety, and providing for an appropriate nonformulary process (American Association of Health Plans [AAHP], 1998; AMA, 1997; American Society of Health-System Pharmacists [ASHP] et al., 1964; ASHP et al., 1991; Hanson et al., 1992; Hazlet and Hu, 1992; Shea et al., 1998). As the primary medical advisor, the P&T committee plays a lead role in clinical decisions and works with other managers to structure and implement the elements that a formulary system may employ to realize pharmacy benefits and health system objectives (ASHP, 1998). The P&T committee, chaired by a physician and representing the medical staff, is an important element in the legal authorization of formulary system actions that could affect clinical care, such as therapeutic interchange (Liang et al., 1988).
GENERIC SUBSTITUTION
Pharmaceutical equivalents are defined as drug products that have the same active ingredient(s) in the same dosage form, route of administration, and strength or concentration (FDA, 1999a). However, pharmaceutical equivalents may not always have the same therapeutic effect or safety profile. Other factors,
such as compounding technology, bioavailability, and patient acceptance or compliance, may be important. Potential problems with substitution of nonproprietary or generic versions of “innovator,” “pioneer,” or “brand name” products among themselves or for the branded, proprietary product were reviewed by Strom (1987). Advances in pharmacological science, changes in federal and state law, and issuance of therapeutic equivalence evaluations by the Food and Drug Administration (1999a), however, have made the practice of genetic substitution routine in public and private-sector formulary systems (Kreling et al., 1996). Reasons for the increased availability of generic drug products and the greater acceptance of generic substitution were described by Nightingale and Morrison (1987).
|
Generic Substitution: The substitution of drug products that contain the same, chemically identical active ingredient(s) and are identical in strength, concentration, dosage form, and route of administration to the drug product prescribed. |
Occasionally, P&T committees conclude that a brand name product and its generic pharmaceutical equivalents may not have reliably similar clinical effects even though they are approved for genetic substitution and listed as therapeutically equivalent by the FDA (1999a). The VA National Formulary identifies several such instances (carbamazepine, digoxin, phenytoin, warfarin). These and a few others have achieved some currency (Covington and Thornton, 1995; Spencer and Crouse, 1999), but the FDA does not agree that there are such problems with generics (see www.fda.gov/CDER/news/ntiletter.htm). Some of these drugs, for example, warfarin, were reviewed by the VA PBM recently and changes made as described in Chapter 3 of this report. Some pharmaceutically equivalent generic drug products may be known not to have the same therapeutic effect. The VA National Formulary includes such an instance (disulfiram). In general, however, academic hospital and other private-sector MCO and PBM formularies identify drugs by their nonproprietary as well as their proprietary names. They require genetic dispensing or provide economic disincentives to the use of more expensive branded products when suitable therapeutically equivalent generic products are available from the FDA list (AAHP, 1998; Hoechst Marion Roussel, 1998; Kreling et al., 1996; Nash et al., 1993; Novartis, 1998, 1999; Sax and Emigh, 1999).
If generic drugs are almost universally less expensive than their brand name counterparts (see Figure 2.6), and if they have the same therapeutic effect, they represent more cost-effective drug choices. As a result, genetics currently comprise about 47% of national prescription drug volume and about 8% of dollar sales (Barents Group LLC, 1999a). The policy of generic dispensing is more effective than would appear from this percentage, given that only about half of drugs in the market have genetic equivalents. Experience with genetic substitution provides reassurance that safe and effective clinical care can be obtained with suitable therapeutically equivalent genetic drug products. Laws and regulations that recognize this in one way or another have been enacted in virtually every state. The 1984 federal Drug Price Competition and Patent Term Restora
tion Act required the FDA to publish and update periodically its evaluations of generic drugs (in the “Orange Book”), although the agency had first issued its final version of the list of approved drugs with their therapeutic equivalence determinations in 1980 (FDA 1999a; 44 Federal Register [FR] 2932; 45 FR 72582). In general, these evaluations are categorized as: either single source drugs considered to have the same therapeutic effects as other pharmaceutically equivalent products because there are no known or suspected bioequivalence problems (for example, designated AA, AN, AO, AP, or AT, depending on dosage form); or because actual or potential bioequivalence problems have been resolved with adequate in vivo or in vitro evidence (for example, designated AB); or as single source drugs that are not considered to have the same therapeutic effects as other pharmaceutically equivalent products (for example, designated BC, BD, BE, BN, BP, BR, BS, BT, BX, or B*, depending on dosage forms, status of review, among others) (FDA, 1999a). The FDA has recently reconfirmed the reliability of generic substitution of its designated equivalent drugs in all therapeutic drug classes, including drugs or classes with narrow therapeutic indices or ratios (that is, with toxic and effective doses that are close together, as defined in 21 CFR 320.33[c]). Generic substitution should no longer be controversial; it should require additional tests or precautions only with very rare exceptions, and it is reliable for all classes of drugs when they are approved for bioequivalence by the FDA (FDA, 1998; Nightingale, 1998; www.fda.gov/CDER/news/ntiletter.htm). The Congressional Budget Office (1998) estimated that generic substitution saved $8 billion to $10 billion on retail pharmacy drug purchases in 1994.
THERAPEUTIC INTERCHANGE
Therapeutic interchange involves substitution of therapeutic alternates, that is, replacing a patient's drug that is not on the formulary with one that is, in order to gain increased compliance with the formulary and its objectives. Therapeutic interchange can be an important part of formulary systems. It is at the core of many of the criticisms of hospital and health plan formu laries and formulary systems. A number of terms that can be con fusing are used in describing therapeutic interchange. In the simplest terms, therapeutic interchange is the exchange of therapeutic alternates to achieve an equivalent drug treatment effect, or therapeutic equivalence. The relevant terms are defined and discussed further below.
|
Therapeutic Alternates: Drug products of different chemical structure but the same pharmacological or therapeutic class. Therapeutic Equivalents: drugs containing the same active ingredient and expected to have the same clinical effects. |
Therapeutic alternates are drug products (as a practical matter, generally brand name drugs) with different chemical structures that are of the same pharmacological or therapeutic class. This means that, as members of the same drug class, they share similar structures, mechanisms of action, and indications for
use (McAllister et al., 1999), and they can be expected to have similar therapeutic effects and safety profiles when administered to patients in therapeutically equivalent doses. They do not contain the same, chemically identical, active ingredient(s), that is, they are not pharmaceutical equivalents (AMA, 1997), as that term is defined in the previous section on generic substitution in this report.
Some commentaries on therapeutic interchange policies (American College of Clinical Pharmacy [ACCP], 1993; ASHP, 1998) refer to therapeutic alternates as therapeutic equivalents or use the term therapeutic equivalence in discussing both therapeutic interchange and generic substitution. The committee does not use the term “therapeutic equivalents ” because this term is officially defined by the FDA (1999a) as meaning the same as “pharmaceutical equivalents” or genetic drugs that can be expected to have the same clinical effects and safety profile when administered to patients as specified in the labeling. To eliminate any possible confusion, the committee decided to accept this definition and refer to drugs with different chemical structures that are exchanged in therapeutic interchanges only as therapeutic alternates.
In developing its evaluations of equivalence in generic substitution, the FDA uses “therapeutic equivalence” to describe the clinical effects of interchange of pharmaceutical equivalents, that is, generic substitution, not the exchange of therapeutic alternates, that is therapeutic interchange (FDA, 1999a). In common usage, however, most people understand therapeutic equivalence to mean any drugs having the same clinical or therapeutic effects or properties. To avoid confusion, the committee decided in this case that it would be clearer not to use the FDA terminology and to use the term “therapeutic equivalence” in this broader, more inclusive way throughout this report.
Some policy statements differentiate between therapeutic interchange and therapeutic substitution. They define the former as the exchange of therapeutic alternates with the permission of the prescriber at the time of interchange, and the latter as exchange according to a previously established policy approved by a P&T committee and some, but perhaps not all, prescribers (Spencer and Crouse, 1999). Exchange without the approval of the prescriber is opposed by organized medicine (ACP, 1990; AMA, 1997), and it is not a common practice in formulary systems. In practice, exchange is often accepted in a tightly organized system where close patient monitoring is possible and likely, such as a hospital or staff model HMO. In these systems, all prescribers and the P&T committee are involved and have agreed to specific interchanges with the provision of an override mechanism. As implemented in less cohesive delivery systems, for example, IPAs, PBMs, or outpatient settings, exchange with specific prescriber permission at the time of dispensing is not opposed by organized medicine or other professional groups. In these less controlled settings, patient monitoring is looser, and P&T committees may be perceived as less representative of a diverse group of physicians. This results in less acceptance of interchange that is authorized by protocol or a P&T committee (ACCP, 1993; Academy of Managed Care Pharmacy [AMCP], 1997; ASHP, 1982, 1998; Carroll, 1999; Zellmer, 1993). Of
course, from the perspective of patients, therapeutic interchange is sometimes involuntary and sometimes a concern.
Because VA data do not always allow certainty about the details of prescriber approval, the committee decided it would be simpler and less confusing to use the term therapeutic interchange only. Details of the interchange could be given when known or relevant. In the committee's view, therapeutic interchange usually means that specific prescriber approval exists before dispensing except in settings where exchange according to a collaborative practice agreement or a preapproved policy and protocol is practical and has been accepted by prescribers. Therapeutic interchange is allowed or encouraged by one-third to one-half of HMOs and PBMs, by the VA formulary system, and by most hospitals' formulary systems. Drug class reviews based on sound scientific data and analysis are generally carried out to support therapeutic interchange among therapeutic alternates in a drug class. The provision of a nonformulary exceptions process is the rule in formularies that are closed or partially closed and allow therapeutic interchange (Hoechst Marion Roussel, 1998; Kreling et al., 1996; VHA Directive 97-047). A smoothly functioning nonformulary exceptions process assists implementation of clinically appropriate exceptions to interchange, as noted below.
Although drugs in a therapeutic class share similar pharmacological and therapeutic properties, they are not identical, and their differences may cause problems when they are interchanged across a large group of patients, some of whom will inevitably have differing physiological and pathophysiological status. Differences may involve, for example, mode and extent of action, adverse effects, and potential interactions with other drugs (ACP, 1990; McAllister et al., 1999). An approved practice of therapeutic interchange can be supported in a number of ways. Education of physicians and patients and adequate advance notice with information and advice on relative dosing should be provided. Careful attention to potential effects on patient compliance is also useful. Adequate provisions for exceptions to conversion, nonformulary access to an alternative, or return to an original drug product, if indicated, are important. Follow-up to identify dosage problems, adverse drug events (ADEs), and other clinical results should be part of the program. Particular attention should be paid to those who are already stable on an original agent or taking multiple agents and those whose physiologic status is compromised. As noted, patient monitoring may be better on an inpatient service. Heightened attention to these considerations may be desirable in ambulatory care settings. Quality and cost considerations may not be significant enough in a number of drug classes to justify potential problems or the dissatisfaction of prescribers. For this reason, monitoring of true savings from interchange has been suggested (ACP in Zoeller, 1991; Carroll, 1999). Therapeutic interchange may be most effective, or cost-effective, when limited to classes having little pharmacological diversity among members, those having substantial diversity in price, or preferably both (ACP, 1990).
LOCAL VA FACILITY AND VISN FORMULARIES AND THE NATIONAL FORMULARY
History of VA Formulary Management Prior to the National Formulary
The Veterans Administration was established in 1930 to provide medical care to veterans in 54 hospitals. In 1946, the VA Department of Medicine and Surgery (which subsequently became the VHA) was created, and agreements between VA hospitals and medical schools were begun (Fonseca et al., 1996). As discussed earlier, P&T committees developed slowly beginning in the 1930s coincident with the American College of Surgeons ' promulgation of standards for hospital pharmacy (1936) and the beginnings of modern hospital formularies in New York (1933). In the 1940s, formulary improvement continued in some U.S. hospitals with removal of outdated medications, but the relatively slow introduction of modern pharmaceuticals and the outbreak of World War II delayed complete formulary revisions (Weintraub, 1978). Indeed, as noted earlier, official pronouncements in this field from the AHA and ASHP did not occur until 1959. It is unlikely, therefore, that the first VA hospitals had much in the way of P&T committees or formularies.
In any case, data summarizing the status of formularies at VA hospitals or other local VA facilities in these early decades were not available to the IOM, although a VA manual, issued in 1955 and mentioned earlier, presumed the presence of a formulary (or the possibility of a formulary) at VA hospitals in the 1950s. VA facilities are not Medicare providers and therefore not required to comply with Title XVIII of the Social Security Act and its regulations on P&T committees, but VA hospitals participate in accreditation by the JCAHO and therefore have been covered by that organization's guidelines regarding P&T committees and formularies. Since the VHA is funded by congressional appropriation and not by third-party payments, which might be affected by facility accreditation status, JCAHO compliance may not have been as influential in encouraging implementation of formularies in the VA hospital system as in other health care systems. Nevertheless, the JCAHO, which has been accrediting VA hospitals since 1953, likely encouraged the installation of formulary systems in VA hospitals. Current VA policy requires VA hospitals to have a P&T committee that carries out at least those functions outlined in the JCAHO accreditation manual for hospitals4 and the 1992 ASHP statement on P&T committees (VA Manual, M-2, Part 1, Chapter 3, Clinical Programs, Pharmacy and Therapeutics Committee, Dec. 13, 1993).
As noted earlier, a study by Rucker and Visconti (1978) of 52 large, mostly academic, private U.S. hospitals and 12 Medicaid programs found that about 40% of hospitals had no formulary whatsoever and that most of the formularies in use had significant deficiencies. This study did not include or refer to VA
|
4 |
Currently the JCAHO does not require or regulate P&T committees, but the VA continues to use the standards set forth in earlier JCAHO accreditation manuals (1993). |
facilities specifically. Nevertheless, there appears no reason to conclude that VA hospitals, many of which are also large and affiliated with medical schools, should have had a markedly better or worse record at that time. According to Kittel et al. (1978), the VHA hospital system at the time of their writing used the American Hospital Formulary Service published by the ASHP to disseminate drug information. This was supplemented by an index of drugs and dosage forms stocked by the pharmacy for each individual hospital. These authors described a project to computerize the formulary index at their VA hospital in a way that could be updated easily after each meeting of the P &T committee and could be used by all six VA hospitals in their district (1 of 29 VA hospital districts at the time). Continuing into the 1980s, VA P&T committees and formulary systems became widespread and firmly entrenched according to those involved with VA pharmacy and formularies during that period (Anonymous, 1988; M. Valentino, VA PBM, personal communication, 1999).
Reorganization of the VA
At present, the VHA consists of 146 medical centers or systems, including 172 hospitals, more than 600 ambulatory care and community-based clinics, 132 nursing homes, 40 domiciliaries, and a number of other programs (Kizer, 1999). The VHA is a unique health care system (and different from private-sector managed care) in terms of its size, cost, and budgeting; diversity of settings; geographic scope; role in the use and training of young physicians; and its permanently eligible patient population. In a 1993 survey of pharmaceutical services, 247 of 326 federal hospitals (76%) responded. The response rate from 156 VA hospitals that participated in this survey was 81% (127 hospitals). A P&T committee was present in 100%, prescribing restrictions in 94%, and a “well-controlled” formulary system existed in 90% of VA hospitals responding. Therapeutic interchange was reported in 76% of responding VA hospital programs. Since this survey heard from about three-fourths of all VA hospitals in operation at the time, it appears that by the early 1990s the VA hospital system was essentially 100% compliant with requirements for a P&T committee and a formulary system (Crawford and Santell, 1994). These results compare favorably with those of Reeder et al. (1997), who found 59.7% of 713 U.S. nonfederal hospitals with a well-controlled formulary and 74.5% with therapeutic interchange programs.
Although a group of VA facilities might decide to implement a formulary jointly (Kittel et al., 1978) or to have a multifacility core formulary (Lowe and Trilli, 1995), the control of formulary content rested with each facility's P&T committee at the time of the Crawford and Santell survey (1994). The local formulary, by agreement of the medical staff and P&T committee, shaped and to some extent limited drug use within a facility by imposing restrictions on the use of some drugs and by listing or not listing specific drugs, among other things. Since drugs could be added to the formulary at local option, limits on prescribing could be mostly temporary, however, lasting until the pharmacy added a new
drug to inventory or purchased it from the VA prime vendor5 or in the local private-sector market (Patterson et al., 1995). Drugs would also be available through the consolidated mail outpatient pharmacy (CMOP), which serves all VA facilities from six locations distributed across the country (OSDBU Fact Sheet No. 314, May 7, 1998). Presumably, drug use could also be influenced by marketing information from pharmaceutical sales representatives and by therapeutic guidelines or other educational efforts issued (and monitored) by the VA PBM. The relative effectiveness of the former and lack of effectiveness of much of the latter in the private sector have been discussed by Avorn et al. (1982) and Avom and Soumerai (1983). This subject has also been reviewed more recently by Chren and Landefield (1994), who found that staff physician interactions with a drug manufacturer significantly influenced physician interest in adding products of that manufacturer to their hospital's formulary.
Impact of the VA Fixed Budget
The pharmacy budget is another significant influence on drug use. The total VHA budget was $17,057,396,000 in FY 1998 and in FY 1999, and $18,978,003,000 in FY 2000. Expenditures for pharmaceuticals were about 6% of the total budget from FY 1990 to FY 1994, or $715,879,000 to $924,482,000, but they had grown to $1,844,742,000 or 11% of the total VHA budget in FY 1999; in recent years, they have been escalating between 11 and 21% annually (GAO, 1999). Prices of pharmaceuticals in the VHA depend on a number of purchasing vehicles. These include the statutorily based Federal Supply Schedule which requires manufacturers to offer brand name products at 76% of the average manufacturer price (AMP). The National Acquisition Center, based outside Chicago, can negotiate contracts below this price or for some supplies and genetic drugs at good prices for VA (and other federal agency) use. VISNs and individual facilities can also negotiate lower prices through blanket purchase agreements (BPAs; see Chapter 5 of this report). Important price differences among brand name members of a drug class, between brand and genetic drugs, or among generic drugs of different manufacture can emerge from these acquisition processes.
Differences in drug acquisition costs presumably explain the presence of therapeutic interchange programs in 76% of VA hospitals. These exchanges are implemented to affect drug use and cost as reported by Crawford and Santell (1994). Individual examples of interchange among members of a particular drug class with significant differences in price at a VA hospital began to be reported in the early 1990s; for example, studies were carried out by Bartlett et al. (1996) in 1993 and by Kellick et al. (1995) in 1994. Other examples are reviewed in Chapter 2 of this report. Occasional restriction of a class and interchange of less expensive drugs from another class were also reported (Lederle and Rogers,
|
5 |
The prime vendor, Amerisource, Inc., is a single organization that provides just-in-time drugs to all VHA facilities (and some other federal agencies) on a national contract. |
1990). Therapeutic interchange is carried out in VA facilities following analysis and a decision by the P&T committee and notice to the medical staff, sometimes without obtaining case-by-case permission at the time of dispensing. In other cases, such permission is part of the interchange process. In either event, a record of the interchange is kept in the pharmacy and a notation made in the patient record. As a matter of policy, the central VHA office does not dictate how conversions are to be carried out. This is left to the individual VISNs (which also do not dictate conversion details) and facilities (VHA response to Item 5, personal communication to IOM, 1999).
Establishing the VA National Formulary
In late 1995, a reorganization of the VHA affected the status of all VA facilities and the relationships of the VA formulary systems, the control of drug use, and pharmacy operations. In October 1995, 22 VISNs were created—essentially 22 MCOs with their own capitation-based budgets. Each VISN on average encompasses 7–10 hospitals, 25–30 ambulatory care clinics, 4–7 nursing homes, 1 or 2 domiciliaries, and various other assets (Kizer, 1999). In the larger scheme of things, this reorganization was intended to promote decentralized management and improved care of veteran populations, to move toward enrolling all veterans with primary caregivers, to consolidate (and close) hospital beds, and to emphasize ambulatory surgery and ambulatory care. At the pharmacy level, VHA Directive 10-95-111, November 7, 1995, required each VISN to implement a VISN-level formulary process by November 15, 1995, and a VISN formulary by April 30, 1996. In part, the VISN formularies were to provide a uniform drug benefit and continuity of care in each network. They also were intended to be the foundation within a year or two for a National Formulary which would provide U.S. veterans with a single national entitlement to drugs and to medical and surgical supplies, supplementable at the VISN or local level.
Coincident with the formation of VISN formularies, the VA Pharmacy Benefits Management Strategic Healthcare Group was established in September 1995 and developed over the course of FY 1996. The VA PBM is located both in Washington, D.C., and outside Chicago and is staffed primarily by pharmacists. Its functions include data collection and analysis to monitor drug costs and utilization, selection and development of drug class reviews and therapeutic guidelines in conjunction with the Medical Advisory Panel, coordination of VISN pharmacy activities, guidance of the transition to a National Formulary, and management of the VA pharmacy benefit. At the same time, VISNs also formed P &T committees (called formulary committees), made up primarily of representatives from local P&T committees. At present, the composition of these committees (primarily pharmacists and physicians) varies widely, but on average, pharmacists predominate. A VISN Formulary Leader Committee of pharmacy leaders from each VISN and the MAP consisting of VA physicians interested in and knowledgeable about drug treatment, were established (VISN Formulary Conference Call Minutes, Jan. 26, 1996). Some members of these
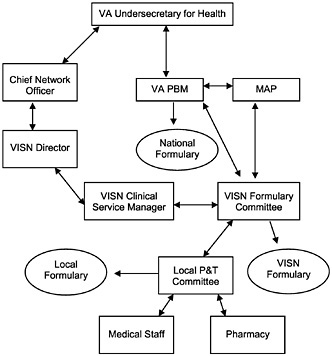
FIGURE 1.1 Reorganization of the Veterans Health Administration. MAP = medical advisory panel; PBM = pharmacy benefits management organization; P&T = pharmacy and therapeutics; VA = Department of Veterans Affairs; and VISN = Veterans Integrated Service Network.
two committees formed a VISN Research Steering Committee and a VISN Data Steering Committee. The first meeting of the MAP/VA PBM was held by conference call on April 3, 1996. Functions of the MAP are defined further below. Figure 1.1 summarizes this recent reorganization and its interrelations, although there are clearly informal ties and communication in addition to the formal ones.
Evolution of the National Formulary
Local formularies provided the foundation for VISN formularies. A formulary template was distributed to VISNs on March 11, 1996 to enable standardized submission of VISN formularies to the VA PBM to assist in development of the National Formulary (VISN Formulary Conference Call Minutes, April 22, 1996). The National Formulary, which presently consists of slightly more than 1,200 items—prescription and over-the-counter (OTC) drugs in 254 drug
classes, as well as medical and surgical supplies—was issued in May 1997 (and has been modified several times since; for example, the original version omitted supplies that were added in December 1997). The official VHA Directive 97-047 followed on October 16, 1997. This directive requires a nonformulary process of each VISN and specifies criteria for granting exceptions. In therapeutic classes where national standardization or committed-use contracts are awarded (for example, any of four closed classes), additional items may not be listed, or listed items deleted, by VISN or local formularies. In other classes, additional items may be added to meet patient care needs as determined by the VISN or local facility. No items on the National Formulary can be made nonformulary at the VISN or local level, although local facilities may restrict National Formulary drugs to certain specialists, settings, or conditions. According to the VA, the objective of the National Formulary is to provide “high quality and best value pharmaceutical products while assuring the portability and standardization of the pharmacy benefit to eligible veterans” (VHA Directive 97-047).
By 1999, when VISN formularies were surveyed by IOM, the local formularies and the VISN formulary were the same in 16 VISNs. In four VISNs, there were differences in a few antibiotics and local restrictions; and in only two VISNs were there more numerous and significant differences among the formularies. Most VISN formularies were larger than the National Formulary, although in at least one instance the VISN formulary and the National Formulary were the same. Apparently, a policy of uniformity within regions is attractive despite the fact that, in theory, local formularies can deviate from the VISN-level formulary and differ among themselves. Of course, the listing of an item on a formulary may not guarantee that it is stocked, only that it will be made available. For example, facilities with patient populations that do not require certain items often do not stock them even though they are listed on the National Formulary (according to a 1999 IOM survey of local facilities). Special facilities such as spinal cord injury centers may have quite different policies from general care facilities on stocking drugs. Local facilities can still add items to their formularies and can request the addition of drugs to the VISN formulary, although such requests are not always granted. Each VISN is required to have an official nonformulary exceptions process based on uniform VHA criteria (VHA Directive 97-047), and some have a standard form for nonformulary requests. The nonformulary process is in part informal and personalized, however, so it is implemented variably depending on local factors, and the standard forms also vary (based on a 1999 IOM survey of local facilities in each of the 22 VISNs).
Despite the directive requiring conformity of closed classes in VISN formularies to the National Formulary, many VISN formularies were not in compliance when the IOM compared 19 drugs in closed classes across VISN formularies and the National Formulary in the spring and summer of 1999. VISN formularies ranged from 74 to 100% conformity; that is, in 16 of the 22 VISNs, from 1 to 5 of the 19 agents were incorrectly included, excluded, or restricted by the VISN formulary. There may be price differentials or local preferences among one or more members of a closed class listed in the National Formulary. In such cases, VISNs
or local facilities may encourage the use of a particular member. The VA PBM does not object to this, although the practice does not explain why some class members are not listed on VISN or local formularies. Comparison of reviewed open or preferred classes also revealed that in about half of the VISNs, from 2 to 7% of the agents in these classes on the National Formulary were not included on the VISN formularies as required. Additions, which are permitted by the VA PBM as expressions of local autonomy, were also common, up to 24% in one case. Elsewhere, the committee comments on the problems inherent in divergence of the VISN or local formularies from the National Formulary.
Although local formularies were not reviewed by the IOM in a similar way, they likely were also not in compliance, since in most cases, all formularies in a VISN are the same. Some of this noncompliance probably stems from different schedules for formulary changes; some, from standardization contracts being established at various times; some, from the natural failures in any very large, complex, and changing system; and some, according to anecdotal reports, from disagreements between VISNs and National Formulary decision makers. It is unclear what implications, if any, minor noncompliance has for cost and quality of care. Enforcement appears to be relatively relaxed with some deference to local autonomy, however, as a matter of policy (M. Valentino, VA PBM, personal communication, 1999).
Medical Staff Input
The MAP works with the VA PBM and the VISN formulary leaders, and together they recommend additions and deletions to the National Formulary. National policy stipulates that new drug products cannot be considered for addition to the National Formulary until a year after FDA approval (except for FDA 1P drugs considered on a case-by-case basis). In this respect the MAP functions as a P&T committee, although it does not conform in structure or authority to ASHP (1992) descriptions of such committees. Its members are exclusively physicians. Appointments to the MAP are approved by the VA Undersecretary for Health on recommendation from the VA PBM and nomination by the VISN chief executives. Local facility P&T committees appear to provide greater opportunity for representation and influence of rank-and-file VA physicians on pharmacy benefit policy.
Although recommendations from the MAP, VISN formulary leaders, and VA PBM are routinely followed, authority to change the National Formulary rests formally with the Pharmacy Benefits Management Executive Steering Board. This board was established by VHA Directive 97-047, but to date has not been created. Decisions are currently made by the MAP-VISN-VA PBM consortium (answers to IOM questions by VHA, 1999). VISNs can request the addition of drugs to the National Formulary, and drugs that most—or many— VISNs add to their own formularies are also reviewed for addition to the National Formulary. Not all requests are granted, nor are all 1P drugs added (see Chapter 2 and Chapter 4 of this report).
Nevertheless, the MAP pursues many activities characteristic of P &T committees. It is made up of expert physicians from VA medical centers around the country, and it is assisted and staffed by the VA PBM. The MAP is charged with developing and coordinating disease state management practices that integrate quality clinical care and cost-effective drug therapy. By considering most frequently occurring conditions in the VHA and those with the top drug expenditures (which include hypertension, diabetes, coronary artery disease, hyperlipidemia, chronic obstructive pulmonary disease, congestive heart failure, prostate cancer, depression, psychosis or anxiety, and peptic ulcer disease, among others), the MAP established priorities for development of therapeutic guidelines and drug class reviews. Close to 30 drug classes have been or soon will be reviewed.
National Formulary Classes
Four classes are closed; that is, they have national standardization, or committed-use, contracts that provide volume-related low prices. Only a few members of the class are listed on the National Formulary. These members must be listed on VISN and local formularies, and other members cannot be listed on VISN or local formularies or dispensed except by nonformulary exception (although, as noted earlier, compliance with these requirements is not complete). These classes are angiotensin-converting enzyme inhibitors (ACEIs) to treat high blood pressure and heart conditions, hydroxymethylglutaryl coenzyme A reductase inhibitors (HMG CoA RIs) to control cholesterol, luteinizing hormone-releasing hormone (LHRH) analogues for treatment of prostatic cancer, and proton pump inhibitors (PPIs) for stomach ulcers and acid reflux. Two classes that were closed are now open, as products within one have become genetic and non-prescription (histamine2 receptor blockers [H2R blockers] for stomach ulcers and acid reflux), or the class has been made “preferred” (alpha blockers for treatment of high blood pressure or improvement of urinary flow in prostatic enlargement). Two classes are preferred, alpha blockers and calcium channel blockers (CCBs) for treatment of high blood pressure and heart conditions, that is, they are open, but they have national contracts that must be honored since prices depend on volume from exclusive use. Prescribing and utilization can also be affected by national usage criteria, or restrictions, which dictate drug usage based on treatment guidelines in classes that are otherwise open.6
When class reviews included specific consideration of closure, in six cases decisions were made to keep classes open or unrestricted (see Table 1.2). The great majority of classes (248) remain open, although closed classes accounted for about 16% of total drug costs in FY 1998 and 10% of total prescriptions and
|
6 |
As work on this report was being completed, a fifth class, oral 5 hydroxytryptamine receptor antagonists for the relief of postoperative and cancer treatment nausea and vomiting, was closed. Because of a challenge to action, this closure and the selection of choice(s) in this class were not announced. |
TABLE 1.2 Drug Classes That Remained Open or Preferred on Review
|
Drug Class |
Reason from VISN Formulary Leaders' Minutes |
Class Status |
|
SSRIs |
Medical staff advised against closing |
Remains open, BPAs in effect |
|
Angiotensin II inhibitors |
Formulary leaders on review of utilization data felt the current arrangement was meeting VISN needs |
Remains open, BPAs in effect |
|
Fluoroquinolones |
Sufficient competition was occurring and closing offered no advantage |
Remains open, BPAs in effect |
|
5-Hydroxytryptamine receptor antagonists (IV) |
Anesthesiologists were against closing the IV class |
Remains open |
|
Ophthalmic beta-blockers |
Drug products in class went generic |
Remains open with a generic multi-source contract |
|
Dihydropyridines |
VISN formulary leaders, after review, felt that VISNs were already moving toward a preferred agent |
Remains as a preferred class |
|
NOTE: BPA = blanket purchase agreement; IV = intravenous; SSRI = selective serotonin reuptake inhibitor; and VISN = Veterans Integrated Services Network |
||
13% of drug expenditures in FY 1999 (GAO, 1999). Some VISNs have pur chasing agreements that influence prescribing and dispensing in addition to the obligations from the National Formulary listings and National Acquisition Center (NAC) contracting. Therapeutic guidelines have accompanied class reviews. Both the formulary status of members of a closed class and the contract prices negotiated by the NAC can have substantial effects on drug utilization as discussed later in this report.
Formulary Relationship to Pharmaceutical Companies
The relationship between buyers and sellers of products in a health care delivery system is a key issue for the VA National Formulary and any other formulary in an organized health care system. Organized buyers include, or have included, major federal government departments such as the VA or the Department of Defense, state programs, MCOs or HMOs, PBMs, group purchasing organizations, hospitals, and other health care facilities and systems. Members of all of these groups use formularies and formulary systems. Sellers are members of the pharmaceutical industry, and the products are pharmaceuticals.
As in any such relationship, prices depend on competition—the ability to choose among competitors, to purchase in volume, and to enforce compliance with market share agreements. By making choices and volume commitments,
formularies and formulary systems are an important component in enabling prudent purchasing. If health care systems lose the ability to discriminate among pharmaceutical products, they will also be handicapped in negotiating prices and purchasing prudently.
Because pharmaceuticals are essential to health care, formularies and formulary systems must be controlled by experts in drug therapy, must safeguard the quality of pharmaceutical care, and must provide, through a waiver process, access to drugs deemed necessary by knowledgeable and informed prescribers. In this way, choices will be made wisely, and the quality of patient care will be protected. These and other objectives of a formulary system are described earlier in this chapter. A formulary system is not necessarily the only way to achieve all of them, but it is an integral part of price negotiation. The purpose of a formulary and formulary system is to achieve value in the purchasing and use of drugs.
REPORT OUTLINE
In subsequent chapters of this report, the concerns of Congress that define the four deliverables of the VA-IOM contractual agreement are considered, and the subject matter discussed in this introduction is expanded. In the final chapter, the committee draws together the material and evaluations from previous chapters in a review of the overall role of the VA National Formulary in veterans' health care. This review is more detailed than the short summary at the beginning of this report. The report concludes with the following material as appendixes: the committee's interim report, a survey carried out by the Academy of Managed Care Pharmacy, additional cost figures and tables, a glossary, and a drug list and drug index (the latter used to define terms and drugs used in this report).
To supplement the information here about the VA National Formulary, VISN formularies, and local formularies, or formulary systems, a detailed description can be found in the first GAO report on this subject, VA's Management of Drugs on Its National Formulary (GAO, 1999), which was requested by the U.S. Senate at the same time that House Report 105-610 requested this IOM study and that will be expanded in a subsequent companion GAO report. The subsequent report is projected to contain the first independent survey of physician perspectives on the National Formulary, which should be a useful addition to understanding the place of the National Formulary in the VHA. Based on the discussion and analyses in this IOM report, the committee comes to conclusions and makes recommendations for the consideration of policy makers in the Congress and the VA, which, it is hoped, may provide some guidance for constructive change in the National Formulary and formulary system. These can be found in the Executive Summary of this report.


























