2
The Institute of Medicine Study on the Future of Emergency Care
Each of the three regional workshops began with an introduction to the Institute of Medicine’s (IOM’s) study on the Future of Emergency Care in the U.S. Health System and an overview of the key findings and recommendations from the three study reports. The information, presented by members of the IOM committee, is summarized here.
EMERGENCY CARE IN THE UNITED STATES
Emergency and trauma care are critically important to the health and well-being of the U.S. population. The emergency care system handles an extraordinary range of patients, from febrile infants, to business executives, to elderly patients who have fallen. It provides not only urgent life-saving care but also primary care services to the millions of people who otherwise lack access to other health care services. In 2003, nearly 114 million visits were made to hospital emergency departments (EDs)—more than 1 for every 3 people in the United States. More than 16 million of those patients arrived at the ED by ambulance.
The emergency care system in the United States has made important strides over the past 40 years: emergency 9-1-1 service now links virtually all ill and injured people to an emergency medical response; prehospital emergency medical services (EMS) teams arrive to transport patients to definitive care; and scientific advances in resuscitation, diagnostic testing, trauma, and emergency medical care yield outcomes unheard of just two decades ago. Yet just beneath the surface, a growing crisis in emergency care is emerging—one that threatens access to quality care for all. EDs across the
country are overcrowded. Ambulances are turned away, and patients, once they are admitted, may wait in hallways for hours or even days before inpatient beds open up for them. Often the specialists that patients need to see are not available. And the system that transports patients to the hospitals is fragmented and inconsistent in the level of quality it provides.
The IOM Committee on the Future of Emergency Care was formed in September 2003 to examine the full scope of emergency care; explore its strengths, limitations, and challenges; create a vision for the future of the system; and make recommendations to help the nation achieve that vision. Over 40 national experts from fields including emergency care, trauma, pediatrics, health care administration, public health, and health services research participated on the committee or one of its subcommittees. In June 2006, the committee released three reports: Emergency Medical Services at the Crossroads; Hospital-Based Emergency Care: At the Breaking Point; and Emergency Care for Children: Growing Pains. These reports provided complementary perspectives on the emergency care system, while the series as a whole presented a common vision for the future of emergency care in the United States.
This study was requested by Congress and funded through a congressional appropriation, along with additional sponsorship from the Josiah Macy Jr. Foundation, the Agency for Healthcare Research and Quality, the Health Resources and Services Administration, the Centers for Disease Control and Prevention, and the National Highway Traffic Safety Administration.
THE COMMITTEE’S FINDINGS
Overcrowding
The emergency care system in the United States is in many ways a victim of its own success. Not only has the hospital ED become the place that people turn to first when they have an illness or injury that demands immediate attention, but it has also been given an increasing number of other responsibilities as well. EDs today provide much of the medical care for patients without medical insurance. Insured patients increasingly turn to the ED during times when their physician is unavailable, such as evenings and weekends, and they are often sent to the ED for tests and procedures that their physician can’t easily perform in the office. In some rural communities, the hospital ED may be the main source of health care for a large percentage of residents. EDs also play a key role in public health surveillance and in disaster preparation and response.
The number of patients visiting EDs has been growing rapidly. There were 113.9 million ED visits in 2003, for example, up from 90.3 million a
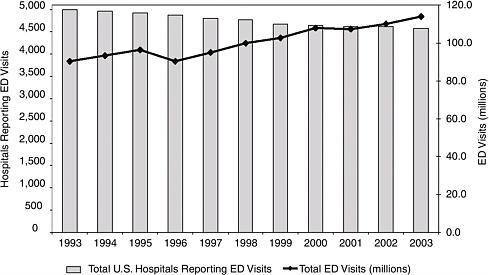
FIGURE 2-1 Hospital emergency departments and emergency department visits.
SOURCE: American Hospital Association Hospital Statistics and National Hospital Ambulatory Medical Care Survey (NHAMCS).
decade earlier. At the same time, the number of facilities available to deal with these visits has been declining. Between 1993 and 2003, the total number of hospitals in the United States decreased by 703, the number of hospital beds dropped by 198,000, and the number of EDs fell by 425 (Figure 2-1).
The result has been serious overcrowding. If the beds in a hospital are filled, patients cannot be transferred from the ED to inpatient units. This can lead to the practice of “boarding” patients—holding them in the ED, often in beds in hallways, until an inpatient bed becomes available. It is not uncommon for patients in some busy EDs to be boarded for 48 hours or more. These patients have limited privacy, receive less timely services, and do not have the benefit of expertise and equipment specific to their condition that they would get in the inpatient department.
Another consequence of overcrowding has been a striking increase in the number of ambulance diversions. Once considered a safety valve to be used only in the most extreme circumstances, such diversions are now commonplace. Half a million times each year—an average of once every minute—an ambulance carrying an emergency patient is diverted from an ED that is full and sent to one that is farther away. In 2004, according to the American Hospital Association, nearly half of all hospitals—and close to 70 percent of urban hospitals—diverted patients at some point during the year. Each diversion adds precious minutes to the time before a pa-
tient can be wheeled into an ED and be seen by a doctor, and these delays may in fact mean the difference between life and death for some patients. Moreover, the delays increase the time that ambulances are unavailable for other patients.
Fragmentation
The modern emergency care system is a relatively new innovation. In the 1950s, for example, emergency medicine was not a recognized specialty, and hospital emergency rooms were generally staffed by internists or primary care physicians, most of them young and inexperienced. There were no paramedics as such—EMS offered little more than first aid, and the local ambulance service often consisted of just a hearse and a mortician.
Since then the emergency care system has developed rapidly. The “emergency room” has become the “emergency department,” and it is now frequently staffed with specialists trained in emergency medicine. Many ambulances employ specialized equipment and EMS personnel trained to stabilize patients and keep them alive until they reach the hospital. But the organization and delivery of these services has lagged behind their technical capabilities, limiting communication and cohesion among the various components of the system. As a result, today’s emergency care system is highly fragmented and variable.
A single population center may have many different EMS agencies— some volunteer, some paid, some based in fire departments, others operated by hospitals or private companies—and these agencies do not always interact with one another effectively. EMS workers often cannot even communicate with police and fire departments because they lack compatible communications equipment or operate on different frequencies. Furthermore, EMS agencies in one jurisdiction are often unable to communicate with those in adjoining areas.
A similar lack of coordination exists between EDs and the EMS services that deliver their patients. Few systems around the country coordinate the regional flow of emergency patients to hospitals and trauma centers effectively, because most fail to take into account such things as the levels of crowding and the differing sets of medical expertise available at each hospital. Indeed, in most cases, the only time an ED passes along information concerning its status to EMS agencies is when it formally goes on diversion and refuses to take further deliveries of patients. As a result, the regional flow of patients is managed poorly, and individual patients may have to be taken to facilities that are not optimal given their medical needs.
Adding to the fragmentation is the fact that there is tremendous variability around the country in how emergency care is handled. Belying its apparent uniformity, there are actually more than 6,000 9-1-1 call centers
around the country. Depending on their location, they may be operated by the police department, the fire department, the city or county government, or some other entity. Moreover, there are no nationwide standards for the training and certification of EMS personnel—or even any national accreditation of the institutions that train them. No single agency in the federal government oversees the emergency and trauma care system. Instead, responsibility for EMS services and for hospital-based emergency and trauma care is scattered among many different agencies and federal departments, including Health and Human Services, Transportation, and Homeland Security. Because responsibility for the system is so fractured, it has very little accountability. In fact, it can be difficult even to determine where system breakdowns occur or why.
Shortage of On-Call Specialists
Emergency and trauma doctors can be called on to treat nearly any type of injury or illness, so it is important for them to be able to consult with specialists in various fields. It has become increasingly difficult, however, for EDs to find specialists who will agree to be on call for the ED, and the resulting shortage of on-call specialists in EDs has had dire and sometimes tragic results.
There is a variety of reasons for the shortage of on-call specialists. Many specialists find that they have difficulty getting paid for their ED services because many emergency and trauma patients are uninsured. Specialists are also deterred by the additional liability risks of working in the ED. Many of the procedures performed in EDs are inherently risky, and physicians rarely have an existing relationship with emergency patients. The result is that insurance premiums for doctors who serve as on-call specialists in the ED are much higher than for those who do not. Finally, many specialists find the demands of providing on-call services too disruptive to their private practices and their family life. After being in surgery all day, they have little desire to be called back into the hospital in the middle of the night, often without the assurance of payment for their services.
Lack of Disaster Preparedness
Any time a disaster strikes, whether it is a natural disaster, a disease outbreak, or a terrorist attack, EMS and hospital EDs are called on to take care of the ill and the wounded. The nation’s emergency care system is poorly prepared to handle such disasters.
The difficulties begin with the already-overcrowded state of the system. With hospitals in many large cities operating at or near full capacity, even a multiple-car highway crash can create havoc in an ED. A major disaster
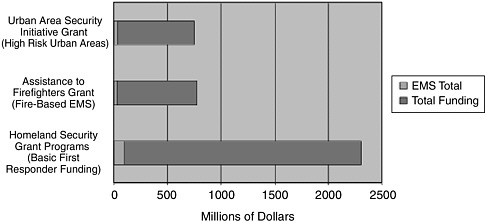
FIGURE 2-2 Emergency medical services receive only 4 percent of first responder funding.
SOURCE: New York University, Center for Catastrophe Preparedness and Response, 2005.
with many casualties is something that many hospitals have limited capacity to handle.
Much of the problem, though, is due to a simple lack of funding. In 2002, for example, hospital grants from the Bioterrorism Hospital Preparedness Program were typically between $5,000 and $10,000—not enough to equip even one critical care room. EMS is particularly underfunded. Although emergency service providers are a crucial part of the response to any disaster, they received only 4 percent of the $3.38 billion distributed by the Homeland Security Department for emergency preparedness in 2002 and 2003 and only 5 percent of the funding from the Bioterrorism Hospital Preparedness Program (Figure 2-2). In general, of the billions of federal dollars being spent on disaster preparedness, only a tiny fraction is spent on medical preparedness, and much of that is focused on one of the least likely threats—bioterrorism.
Due to this lack of funding, few hospital or EMS personnel have received even minimal training in how to prepare for and respond to a disaster. Furthermore, they lack the equipment and supplies necessary to deal with disasters. Few hospitals have negative-pressure units, for example, which are crucial in isolating victims of airborne diseases, such as avian flu. Nor do many hospitals have the appropriate personal protective equipment to keep their staffs safe when dealing with an epidemic or other disaster.
Shortcomings in Pediatric Emergency Care
Children who are injured or ill have different medical needs than adults with the same problems. They have different normal values for pulse, respiratory, and blood pressure measures that change with age. They often need equipment that is smaller than what is used for adults, and they require medication in much more carefully calculated doses. They have special emotional needs as well, often reacting very differently to an injury or illness than adults do. Although children make up 27 percent of all visits to the ED, many hospitals and EMS agencies are not well equipped to handle these patients (Figure 2-3).
A report from the National Center for Health Statistics indicates, for example, that only 6 percent of U.S. EDs have all the supplies necessary for handling pediatric emergencies, and only about half of the departments had even 85 percent of the essential supplies. Training is also an issue. Many EDs, particularly those in rural areas, rely on doctors and nurses without specialized pediatric training to handle pediatric patients. Many EMS agencies require little pediatric training of their personnel.
A number of large cities do have children’s hospitals or hospitals with pediatric EDs that offer state-of-the-art treatment for children. However, the vast majority of ED visits by children are made instead to general hospitals, which are less likely to have pediatric expertise, equipment, and policies in place for the care of children.
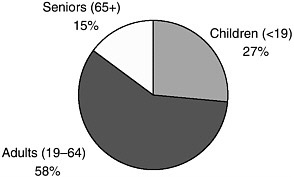
FIGURE 2-3. Emergency department visits by age.
SOURCE: 2002 NHAMCS, calculations by IOM staff.
THE COMMITTEE’S RECOMMENDATIONS
To improve the nation’s emergency care system and deal with the growing demands placed on it, the committee recommended a multipronged strategy. Its reports contain a large number of recommendations, and four key areas are highlighted below.
Creation of a Coordinated, Regionalized, Accountable System
Many of the problems of today’s emergency care system can be traced to its fragmented nature. The emergency care system of the future should be, in contrast, highly coordinated, regionalized, and accountable. This is the centerpiece of the committee’s vision for the future of emergency care.
It should be coordinated in the sense that, from the patient’s point of view, delivery of emergency services should be seamless. To achieve this, the various components of the system—9-1-1 and dispatch, ambulances and EMS workers, hospital EDs and trauma centers, and the specialists supporting them—must be able to communicate continuously and coordinate their activities. When an ambulance picks up a patient, for example, the EMS personnel gather information on the patient, and the information is automatically passed on to the ED before the ambulance even arrives.
The system should be regionalized, in the sense that neighboring hospitals, EMS, and other agencies work together as a unit to provide emergency care to everyone in that region. Patients should be taken to the optimal facility in the region based on their condition and the distances involved. In case of a stroke, for example, a patient might be better served by going to a hospital that is slightly farther away but that specializes in the treatment of stroke.
Finally, the system should be accountable, which means that there must be ways of determining the performance of the different components of the systems and reporting that performance to the public. This will demand the development of well-defined standards and of ways to measure performance against those standards.
The reports call for a series of 10 demonstration sites to put these ideas into practice and test them to determine which strategies work best under various conditions.
Once under way, this coordinated, regionalized, and accountable system should not only address the problem of fragmentation of the nation’s emergency care system, but it should also help the shortage of on-call specialists by routing patients to hospitals with the appropriate specialists. To further increase the availability of specialists in EDs, the report also calls on Congress to find a way to mitigate the effect of medical malpractice suits on services provided to patients in EDs.
Furthermore, the development of a coordinated, regionalized, accountable emergency and trauma care system is hindered by the way that responsibility for emergency care programs is spread out across different agencies of the federal government. The scattered nature of federal responsibility for emergency care makes it difficult for the public to identify a clear point of contact, limits the visibility necessary to secure and maintain funding, creates overlaps and gaps in program funding, and engenders confusion on key policy issues. The report calls for the creation of a lead federal agency that would consolidate many of the government programs that deal with emergency and trauma care.
Improve Hospital Efficiency and Patient Flow
Tools developed from engineering and operations research have been successfully applied to a variety of businesses, from banking and airlines to manufacturing companies. These same tools have been shown to improve the flow of patients through hospitals, increasing the number of patients that can be treated while minimizing delays in their treatment and improving the quality of their care. For example, smoothing the peaks and valleys of patient admissions has the potential to eliminate bottlenecks, reduce crowding, improve patient care, and reduce cost. Another promising tool is the clinical decision unit, or 23-hour observation unit, which helps ED staff determine whether certain ED patients require admission. Hospitals should use these tools as a way of improving hospital efficiency and, in particular, reducing ED crowding.
At the same time, hospitals should increase their use of information technologies with such things as dashboard systems that track and coordinate patient flow and communications systems that enable ED physicians to link to patients’ records or providers. Such increased use of information technologies will not only lead to greater hospital efficiency but will also increase safety and improve the quality of ED care.
Since there are few financial incentives for hospitals to reduce crowding, the Joint Commission on the Accreditation of Healthcare Organizations should put into place strong standards about ED crowding, boarding, and diversion. In particular, the practices of boarding and ambulance diversion should be eliminated except in the most extreme circumstances, such as a mass casualty in a community.
Increase Resources
Increased funding could help improve the nation’s emergency care system in a number of ways. More research is needed, for example, to de-
termine the best ways to organize the delivery of emergency care services, particularly prehospital EMS. And, given that many closings of hospitals and EDs can be attributed to financial losses caused by the cost of emergency and trauma care, Congress should consider providing greater reimbursements to the large, safety-net hospitals and trauma centers that bear a disproportionate amount of the cost of taking care of uninsured patients.
An area in which greater funding is needed is disaster preparedness. To date, despite their importance in any response to disaster, the various parts of the emergency care system have received very little of the funds that Congress has dispensed for disaster preparedness. In part this is because the money tends to be funneled through public safety agencies that consider medical care to be a low priority. Congress should therefore make significantly more disaster preparation funds available to the emergency system through dedicated funding.
Devote More Attention to the Care of Children
Finally, as these improvements are made to the nation’s emergency care system, it will be important to keep pediatric patients in mind in all aspects of emergency care. The needs of pediatric patients should be taken into account in developing standards and protocols for triage and the transport of patients; in developing disaster plans; in training emergency care workers to ensure that they are competent and comfortable providing emergency care to children; and in conducting research to determine which treatments and strategies are most effective with children in various emergency situations.
ACHIEVING THE VISION
There is no “one size fits all” solution to building the best possible emergency care systems from state to state and region to region. In order to explore different approaches and see what works best in different situations, the committee recommends that Congress establish a 5-year demonstration program to provide funding for states or regions to develop coordinated, regionalized, and accountable emergency care systems in various parts of the country. Over time these projects will help identify best practices that can address the problems facing today’s emergency systems and point the way toward a future emergency care system that ensures high-quality, efficient, and reliable care for all who need it.










